EXAM 3 Respiratory and Digestive System Functions and Processes
1/118
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
119 Terms
What are the major functions of the respiratory system?
To supply body with O2 for cellular respiration and dispose of CO2.
What are the four processes of respiration?
1. Pulmonary ventilation (breathing) 2. External respiration 3. Transport of O2 and CO2 in blood 4. Internal respiration
What is external respiration?
Exchange of O2 and CO2 between lungs and blood.
What is internal respiration?
Exchange of O2 and CO2 between systemic blood vessels and tissues.
What are the functions of the nose?
1. Provides an airway for respiration 2. Moistens and warms entering air 3. Filters and cleans inspired air 4. Serves as resonating chamber for speech 5. Houses olfactory receptors.
What is rhinitis?
Inflammation of nasal mucosa.
What are the three regions of the pharynx?
1. Nasopharynx 2. Oropharynx 3. Laryngopharynx.
Where is the pharyngotympanic tube located?
It connects the nasopharynx with the nasal cavity.
Why is the pharyngotympanic tube important?
It equalizes pressure between the middle ear and atmospheric pressure for optimal tympanic membrane vibration for hearing
What structures make up the conducting zone?
The trachea and bronchi up until the terminal bronchioles.
What is the function of the conducting zone?
Transports gas to and from gas exchange sites; cleanses, warms, and humidifies air.
What structures make up the respiratory zone?
The respiratory bronchioles, alveolar ducts, and alveoli.
What is the function of the respiratory zone?
Site of gas exchange.
What are the functions of the larynx?
1. Provides patent airway 2. Routes air and food into proper channels 3. Voice production.
What structure prevents food and liquids from entering the trachea?
Epiglottis.
What are the three layers of the wall of the trachea?
1. Mucosa: ciliated pseudostratified epithelium with goblet cells 2. Submucosa: connective tissue with seromucous glands 3. Adventitia: outermost layer made of connective tissue
What prevents the trachea from collapsing?
C-shaped cartilage rings.
What are the anatomical differences between the right and left main bronchi?
The right main bronchus has a larger diameter, is more vertical, and shorter.
What is the respiratory membrane?
A blood air barrier that consists of alveolar and capillary walls along with their fused basement membranes.
What is the normal thickness of the respiratory membrane?
Very thin (~0.5 μm).
What are alveolar type I cells?
A single layer of squamous epithelium that make up the walls of alveoli.
What are alveolar type II cells?
Cuboidal cells that secrete surfactant and antimicrobial proteins.
What is the difference between the pulmonary and bronchial circulations?
The pulmonary circulation delivers systemic deoxygenated venous blood from heart to lungs for oxygenation via the right and left pulmonary arteries.
The bronchial circulation provides oxygenated blood to lung tissue via the bronchial arteries (part of systemic circuit)
What are the serosal membranes surrounding the lungs?
Pleurae: thin, double-layered serosal membrane in the thoracic cavity
Parietal pleura: membrane on thoracic wall, superior face of diaphragm, around heart, and between lungs
Visceral pleura: membrane on external lung surface
What do the serosal membranes do?
Provides lubrication and surface tension that assists in expansion and recoil of lungs; causes the lungs to move with the thoracic cavity wall
What is atmospheric pressure?
P (atm) Pressure exerted by air surrounding the body (760 mm Hg at sea level).
What is intrapulmonary pressure?
(Ppul) Pressure in alveoli.
What is intrapleural pressure?
(Pip) Pressure in pleural cavity; always negative pressure
How do volume, pressure, and flow relate to each other in the lungs?
Volume changes lead to pressure changes; pressure changes lead to flow of gases.
How do the lungs change for inspiration? Expiration?
Inspiration: thoracic cavity volume goes up → intrapulmonary pressure goes down → air enters lungs
Expiration: thoracic cavity volume down → intrapulmonary pressure up → air exits lungs
What is the relationship between pressure and volume according to Boyle’s law?
Pressure (P) varies inversely with volume (V)
How does the pressure in the lungs compare with the atmospheric pressure during inhalation? Exhalation?
During inhalation – pressure in the lungs is less than atmospheric pressure
During exhalation – pressure in the lungs is greater than atmospheric pressure
What is the major muscle for breathing?
Diaphragm.
What is the main nerve that controls the diaphragm?
Phrenic nerve.
What are the three factors that influence pulmonary ventilation?
1. Airway resistance 2. Alveolar surface tension 3. Lung compliance.
What is the relationship between flow, resistance and pressure?
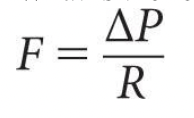
What effect does epinephrine have on bronchiole diameter? Albuterol?
Increases bronchiole diameter.
What is surfactant?
Surfactant is a detergent-like lipid and protein complex that helps reduce surface tension of alveolar fluid by reducing the number of hydrogen bonds between water molecules
What factors influence lung compliance?
Nonelastic scar tissue replacing lung tissue (fibrosis), Reduced production of surfactant & Decreased flexibility of thoracic cage ex: Deformities of thorax • Ossification of costal cartilage • Paralysis of intercostal muscles
What is minute ventilation?
Total amount of gas that flows into or out of respiratory tract in 1 minute.
What is alveolar ventilation rate (AVR)?
Flow of gases into and out of alveoli during a particular time.
What does Dalton's law say about the total pressure of a gas mixture?
The total pressure is equal to the sum of pressures exerted by each gas.
What are the top two major gases in the air we breathe in order of abundance?
Nitrogen ~ 78.6% & Oxygen ~ 20.9%
What are the factors that influence external respiration?
1. Partial pressure gradients and gas solubilities 2. Thickness and surface area of respiratory membrane 3. Ventilation-perfusion coupling: matching of alveolar ventilation with pulmonary blood perfusion
If perfusion to a portion of the lung is greater than ventilation, how do the pulmonary arterioles respond? If perfusion is less than ventilation?
If perfusion is greater than ventilation, pulmonary arterioles will constrict If perfusion is less than ventilation, pulmonary arterioles will dilate
Where in the body is the blood with the highest partial pressure of CO2?
In the blood returning to the lungs in the pulmonary arteries.
Where in the body is the blood with the lowest partial pressure of CO2?
In the blood leaving the lungs in the pulmonary veins.
Where in the body is the blood with the highest partial pressure of O2?
In the blood leaving the lungs in the pulmonary veins.
Where in the body is the blood with the lowest partial pressure of O2?
In the blood returning to the lungs in the pulmonary arteries.
What percentage of oxygen is carried in the blood plasma?
1.5% is dissolved in plasma
What percentage of oxygen is carried inside red blood cells?
About 98.5%.
How many oxygen molecules can each hemoglobin molecule carry?
Up to four.
What is oxyhemoglobin?
Oxyhemoglobin (HbO2) is the hemoglobin-O2 combination; O2 is bound to hemoglobin.
What is deoxyhemoglobin?
Reduced hemoglobin (deoxyhemoglobin) (HHb) is hemoglobin that has released O2.
What factors influence hemoglobin saturation?
PO2, temperature, blood pH, PCO2, concentration of BPG.
In one passage through a bed of systemic blood capillaries, the blood gives up about what percentage of its oxygen?
20% to 25%.
What is venous reserve?
Oxygen remaining in venous blood after passing through a systemic capillary bed; Hb is still 75% saturated at rest.
How does an increase in temperature affect hemoglobin's affinity for oxygen?
Increases in temperature results in a decrease for Hb’s affinity for O2 • Enhances O2 unloading
How does a decrease in temperature affect hemoglobin's affinity for oxygen?
Decreases in temperature results in an increase for Hb’s affinity for O2
What is the Bohr effect? How does pH relate to oxygen unloading?
As cells metabolize glucose, they use O2, causing: • Increases in PCO2 and H+ in capillary blood. Declining blood pH (acidosis) and increasing PCO2 cause Hb-O2 bond to weaken, O2 unloading occurs where needed most
What is hypoxia?
Inadequate O2 delivery to tissues, which can result in cyanosis.
How is CO2 transported in the blood?
CO2 is transported in three forms: 7-10% dissolved in plasma, 20% bound to hemoglobin (carbaminohemoglobin), and 70% as bicarbonate ions (HCO3-) in plasma.
What is the direction of the reaction in systemic capillaries?
CO2 + H2O → H2CO3 ⇌ H+ + HCO3-.
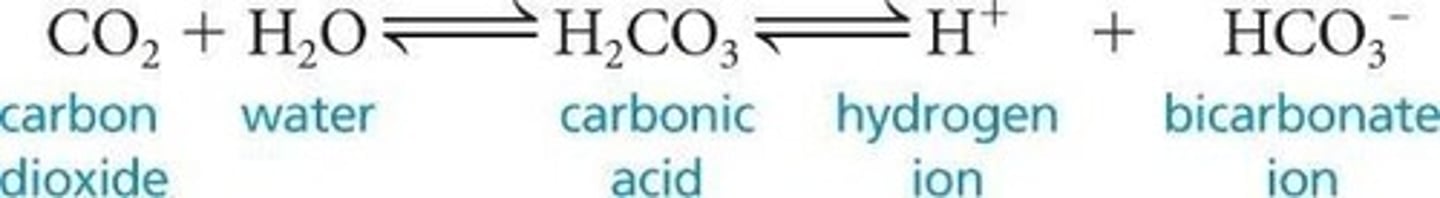
What is the direction of the reaction in pulmonary capillaries?
HCO3- + H+ ⇌ H2CO3 ⇌ H2O + CO2.
What is the Haldane effect?
Increased blood O2 decreases its ability to carry CO2, encouraging CO2 release in the lungs.
How does blood PCO2 relate to blood pH?
↑blood CO2 = ↓ blood pH; ↓ blood CO2 = ↑ blood pH.
How can a change in respiration affect blood pH?
Slow, shallow breathing increases CO2, dropping pH; rapid, deep breathing decreases CO2, raising pH.
What chemical factors influence respiratory rate?
Changing levels of PCO2/pH (most potent) and PO2; rising CO2 levels are the most powerful respiratory stimulant.
How do changes in blood PCO2, PO2, and pH affect respiratory rate?
Decreased PCO2 leads to slow, shallow respiration; declining PO2 has slight effect unless below 60 mm Hg; decreased pH increases respiratory rate.
How does temperature influence respiratory rate?
Increased temperature generally leads to increased respiratory rate.
What is hyperventilation?
Increased depth and rate of breathing that exceeds the body's need to remove CO2.
What is hyperpnea?
Increased ventilation in response to metabolic needs.
What are the main functions of the digestive system?
Take in food, break it down into nutrient molecules, absorb molecules into the bloodstream, rid the body of indigestible remains.
What are the two groups of digestive system organs?
1. Alimentary canal (GI tract); 2. Accessory digestive organs.
What are the accessory digestive organs?
Teeth, tongue, gallbladder, salivary glands, liver, pancreas.
What is digestion?
Breaking large food molecules into small molecules.
What are the two types of digestion?
1. Mechanical breakdown; 2. Chemical digestion.
What is absorption?
The physiological process that moves digested fragments from outside the body into the blood or lymph.
What is peristalsis?
A 'milking' action where adjacent segments of the alimentary canal alternately contract and relax to move food.
What is segmentation?
Nonadjacent segments of the alimentary canal contract and relax to mix and mechanically break down food.
What is the serous membrane of the abdominal cavity?
Peritoneum, which has parietal and visceral layers.
What are mesenteries?
Double layers of peritoneum that are fused back to back.
What are the layers of the alimentary canal wall?
1. Mucosa; 2. Submucosa; 3. Muscularis externa; 4. Serosa.
What is the enteric nervous system?
The intrinsic nerve supply to the alimentary canal.
What are the two nerve plexuses in the wall of the alimentary canal?
1. Submucosal nerve plexus; 2. Myenteric nerve plexus.
What is the role of the parasympathetic nervous system in digestion?
It enhances the digestive process.
What is the role of the sympathetic nervous system in digestion?
It inhibits digestion.
What are the different types of lingual papillae?
Filiform (no taste buds), fungiform, vallate (circumvallate), foliate (contain taste buds).
What is saliva made up of?
Water, electrolytes, enzymes, and other substances.
What is the composition of saliva?
Mostly water (97-99.5%), slightly acidic (pH 6.75 to 7.00), contains electrolytes (Na+, K+, Cl−, PO42−, HCO3−), enzymes (salivary amylase, lingual lipase), proteins (mucin, lysozyme, IgA), and metabolic wastes (urea, uric acid).
What are the functions of saliva?
Cleanses mouth, dissolves food chemicals for taste, moistens food and compacts it into bolus, begins breakdown of starch with enzyme amylase.
Which extrinsic salivary gland is inflamed in mumps?
Parotid.
How do serous and mucous salivary gland secretory cells differ?
Serous cells produce watery secretion with enzymes and ions; mucous cells produce mucus.
What are the layers of a tooth from superficial to deep?
Crown: Enamel > dentin > pulp; Root: Cement > dentin > pulp.
Where does the transition from skeletal muscle to smooth muscle occur in the alimentary canal?
Esophagus.
Where is the gastroesophageal sphincter located and what does it prevent?
At the junction of the esophagus and the stomach; it prevents heartburn.
What is deglutition?
Swallowing.
What are the main functions of the stomach?
Breakdown of food, holding area for food, delivers chyme to small intestine, denatures proteins by HCl, enzymatic digestion of proteins by pepsin.
What are the major cell types of the gastric glands and their secretions?
Mucous neck cells (thin, acidic mucus), Parietal cells (HCl and intrinsic factor), Chief cells (pepsinogen and lipases), Enteroendocrine cells (serotonin, histamine, somatostatin, gastrin).
What does intrinsic factor do and what disease is associated with its lack?
Intrinsic factor is necessary for vitamin B12 absorption; lack causes pernicious anemia.