ZOOL 463 Final
1/159
Earn XP
Description and Tags
ZOOL 463 Final UofC
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
160 Terms
MODULE 13: GASTROINTESTINAL 1
Gastrointestinal Tract/Alimentary Canal
A long muscular tube that extends from the mouth to the anus and is lined with specialized epithelial cells responsible for secretion, absorption, and transport of nutrients
Sphincters
Refers to the rings of smooth muscle that act as gates, separating the GI tract into distinct functions
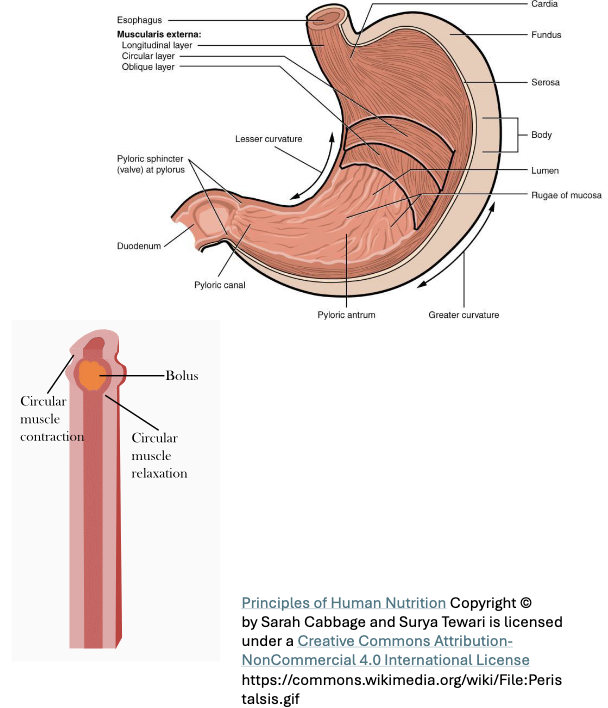
Peristaltic Movement (2)
Coordinated contractions and relaxation of smooth muscle that move food throughout the GI tract
Smooth muscle contraction occurs behind the food bolus, while relaxation occurs ahead of it
Feeding (2)
Feeding is the process by which organisms obtain and ingest food in order to meet nutritional needs
Organisms exhibit diverse feeding behaviours depending on environment and nutrient requirements

Feeding: Challenge & Solution (2)
Most food molecules are large macromolecules such as proteins, carbohydrates, and lipids which are too large to be directly absorbed into the bloodstream
Digestion works to break down these molecules into smaller molecules for absorption and transportation
Digestive System Beyond Digestion: Immune Defense & Tissue Integrity (3)
The GI tract contains protective mechanisms such as mucus layers, acidic environments, digestive enzymes, and lymphoid tissues to prevent infection from pathogens ingested with food
The intestinal lining undergoes rapid cell turnover to maintain a protective epithelial barrier
The small intestine contains immunoglobulin-producing immune cells which contribute to immune protection within the digestive system
Digestion involves several coordinated processes including ___, ___, and ___
Acquisition (feeding)
Processing
Absorption of nutrients
Components of Digestion: Oral Cavity, Pharynx, & Esophagus (3)
Primarily responsible for the mechanical breakdown and transport of food
In the oral cavity, chewing physically breaks food into smaller pieces, while saliva moistens it and begins digestion
The pharynx and esophagus move the food bolus towards stomach through peristalsis
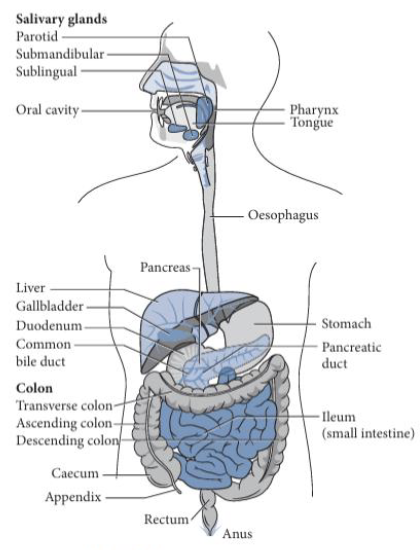
Components of Digestion: Stomach (2)
Muscular organ located in the upper abdomen
Functions as an acidic compartment where food undergoes storage, mixing, and partial digestion
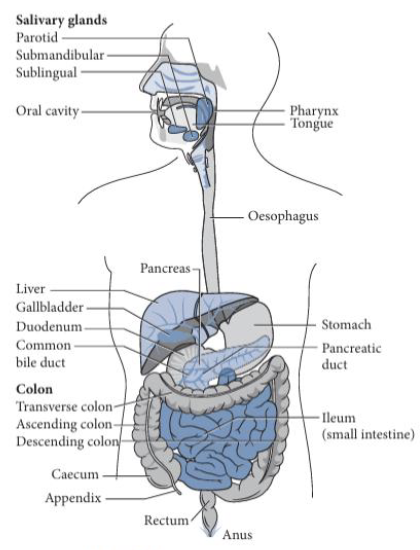
Components of Digestion: Small Intestine (2)
Primary site of digestion and nutrient absorption
Digestive enzymes from the pancreas and bile from the liver break down carbohydrates, proteins, and lipids, while intestinal lining absorbs nutrients
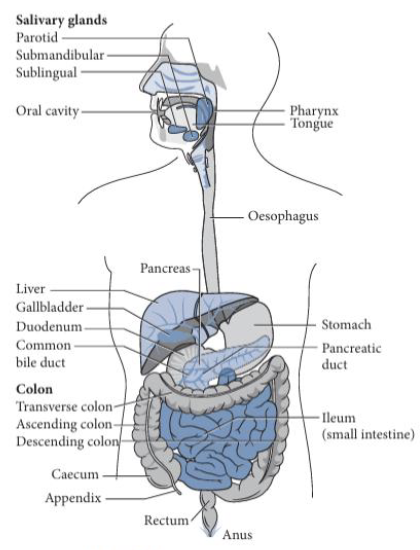
Components of Digestion: Hindgut/Caecum (2)
Plays a role in housing the gut microbiome and appendix
Also contributes to absorption of water and electrolytes and helps lubricate intestinal contents
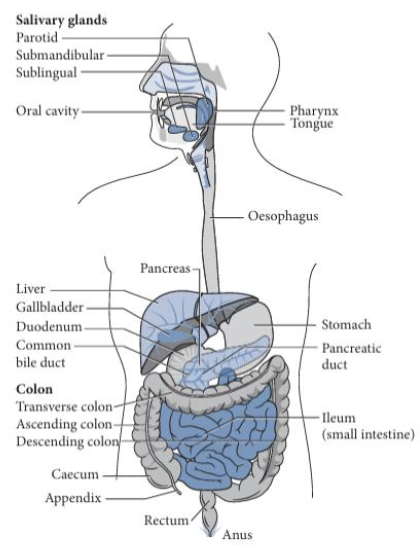
Components of Digestion: Large Intestine (Colon)
*Same function as hindgut/caecum
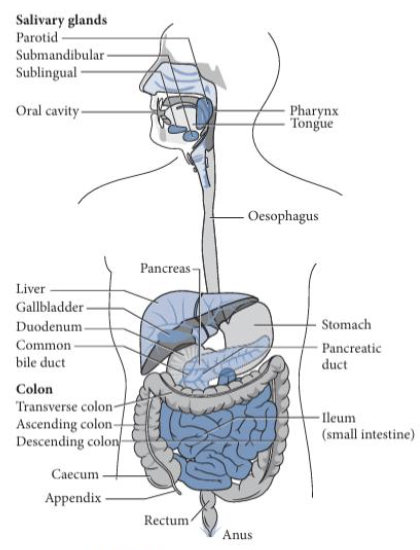
Components of Digestion: Rectum & Anus (2)
The rectum serves as the storage site for indigestible material (feces) before elimination
The anus is responsible for elimination of fecal material
Digestive System Anatomy: The Stomach - Regions (4)
Fundus: Stores undigested food
Body: Main site of mixing and initial digestion
Antrum: Contains partially digested food
Pylorus: Includes the pyloric sphincter which controls the passage of stomach contents into the duodenum (small intestine)
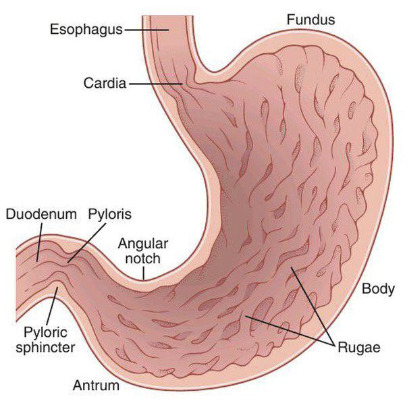
Digestive System Anatomy: The Stomach - Gastric Juice & Chyme Formation (2)
The stomach secretes gastric juice which contains acid and digestive enzymes that begin chemical digestion (especially proteins)
Through continuous mixing and chemical breakdown the food is converted into semi-liquid substance called chyme
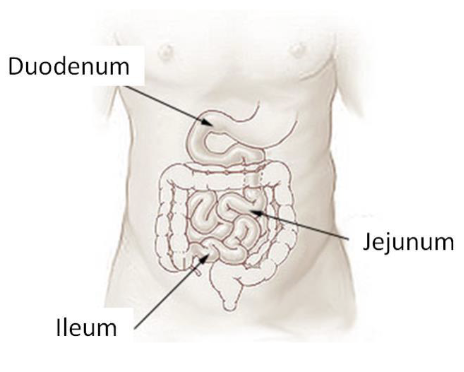
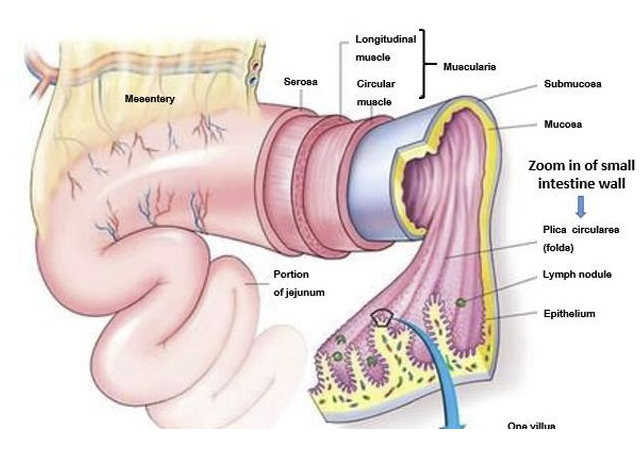
Digestive System Anatomy: The Small Intestine (3)
The duodenum is the first portion of the small intestine (25cm); intensifies chemical digestion
Jejunum and ileum together make up majority of the small intestine (260cm); responsible for absorption of nutrients
The pancreas and liver play roles in digestion by supplying the duodenum with digestive enzymes and bile
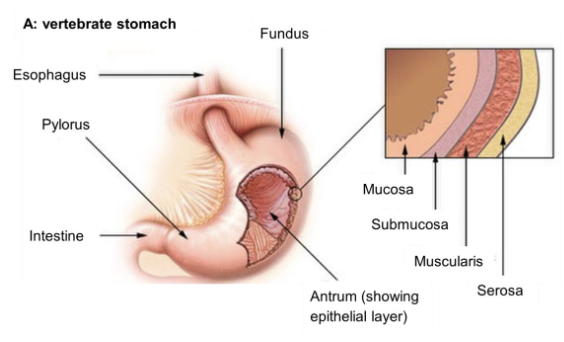
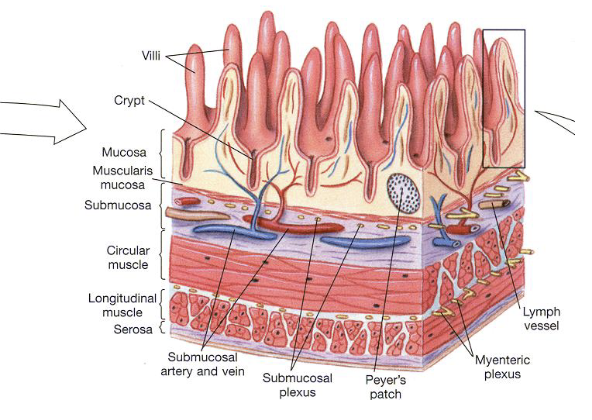
Layers of GI Tract Wall (4)
Mucosa: Innermost layer of the GI tract composed of epithelial tissue
Submucosa: Layer of connective tissue beneath the mucosa that contains blood vessels and lymphatic vessels
Muscularis Externa: Consists of 2-3 layers of smooth muscle responsible for motility
Serosa: Outermost layer of GI tract that provides structural support
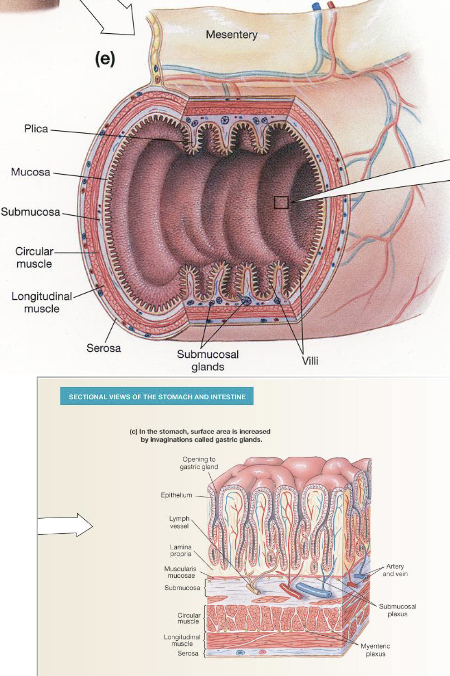
Increasing Surface Area of The Lumen
Structures such as the rugae in the stomach and plicae in the small intestine are folds that project into the lumen and increase surface area for digestion and nutrient absorption
The mucosal layer is the ___
Most variable across the GI tract
Mucosal Layer: 3 Regions
Epithelial Layer: Lines the lumen; structure varies across the GI tract (stomach vs. intestine)
Lamina Propria: Subepithelial connective tissue; contains nerve fibres, blood vessels, and lymph vessels
Muscularis Mucosae: Smooth muscle; separates mucosa and submucosa
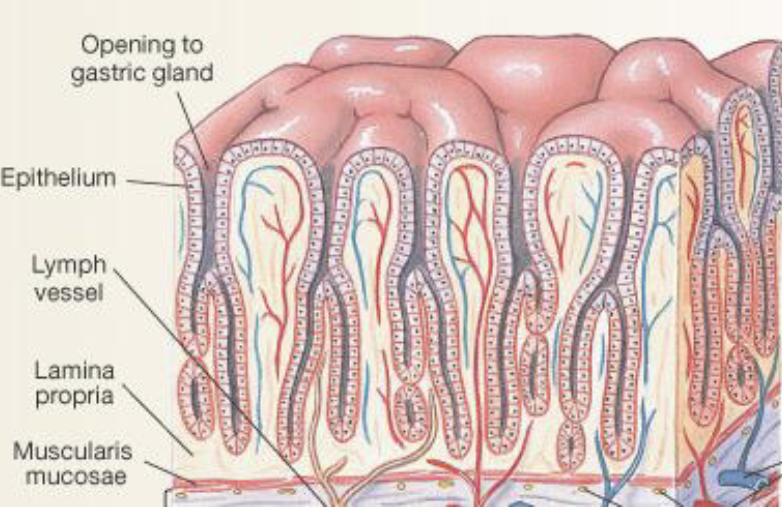
Mucosal Layer: Stomach Epithelium - Gastric Glands (2)
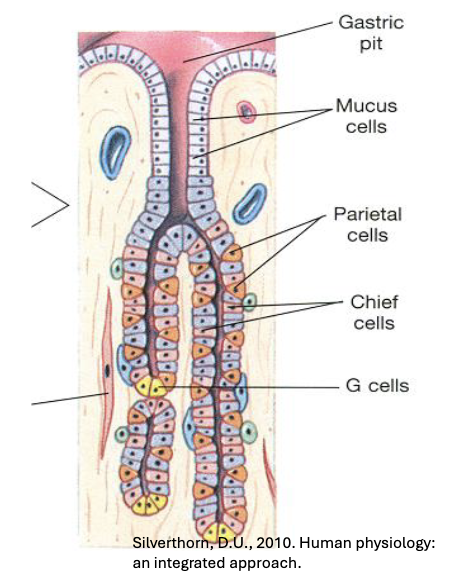
Stomach epithelium contains inward invaginations called gastric glands which extend from the surface into the mucosa
Gastric glands house specialized cells responsible for secretion involved in digestion
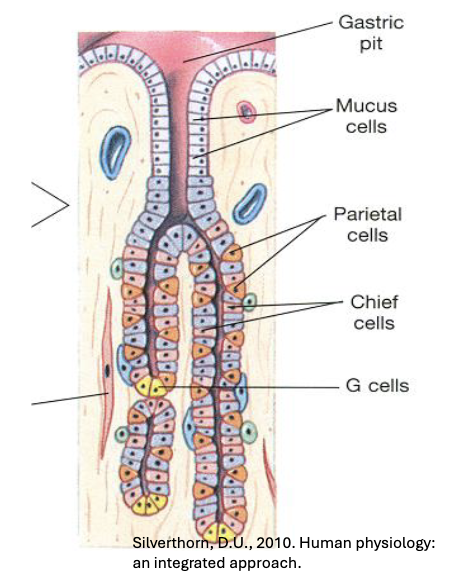
Mucosal Layer: Stomach Epithelium - Four Major Epithelial Cell Types
Mucus (Goblet) Cells: Secrete mucus to protect stomach lining
Parietal Cells: Produce HCL and intrinsic factor (required for vitamin B12 absorption)
Chief Cells: Secrete pepsinogen (inactive precursor of pepsin)
G Cells (Enteroendocrine Cells): Release gastrin
Mucosal Layer: Stomach Epithelium - Role of HCL & Protein Digestion (2)
HCL produced by the parietal cells creates a highly acidic environment that converts pepsinogen into active pepsin
Pepsin is a proteolytic enzyme that breaks peptide bonds in proteins
Mucosal Layer: Stomach Epithelium - Protective Role of Mucus
The stomach lining is protected by a mucus layer rich in bicarbonate that neutralizes acid to prevent damage
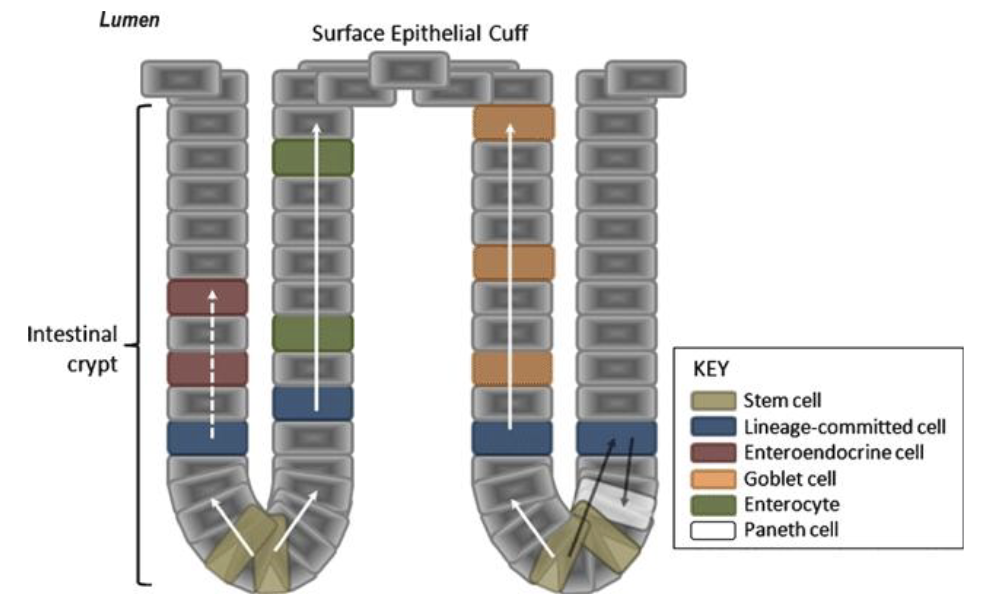
Mucosal Layer: Intestinal Epithelium - 5 Cell Types
Enterocytes: Primary transporting cells
Endocrine Cells: Secrete hormones
Goblet Cells: Secrete mucus
GI Stem Cells: Continuously renews intestinal epithelium; located in crypts and gastric glands
Other Secretory Cells: Includes mast cells that release histamine for immune responses
GI Tract: Cell Junction Differences
Stomach and large intestine have tighter junctions that limit permeability; small intestine is leaky allowing absorption of nutrients
Acidic Stomach: Prevention of Autodigestion - Protective Mechanisms (4)
Bicarbonate-Rich Mucus Barrier
Tight Cell Junctions: Prevent gastric acid and digestive enzymes from leaking into deeper layers
Stem Cell Regeneration/Rapid Epithelial Turnover
Ulcer Formation: If protective mechanisms fail ulcers are formed
Autodigestion: Helicobacter pylori
The bacterium Helicobacter pylori can disrupt the protective mechanisms by damaging the mucus layer (increasing ulcers)
Mucosal Layer: Lamina Propria (3)
Contains wandering immune cells (macrophages and lymphocytes)
Peyer’s patches are specialized clusters of lymphoid tissue found in the ileum that function as immune monitoring sites (detecting pathogens and initiating immune responses)
The lamina propria is part of a larger immune network (GALT - gut-associated lymphoid tissue) which consists of lymphoid follicles distributed throughout the GI tract (including appendix)
Mucosal Layer: Muscularis Mucosa
This layer produces gentle rhythmic contractions that expel epithelial secretions from glands into the lumen and alters surface area by causing villi to move back and forth (enhancing contact between epithelium and luminal contents)
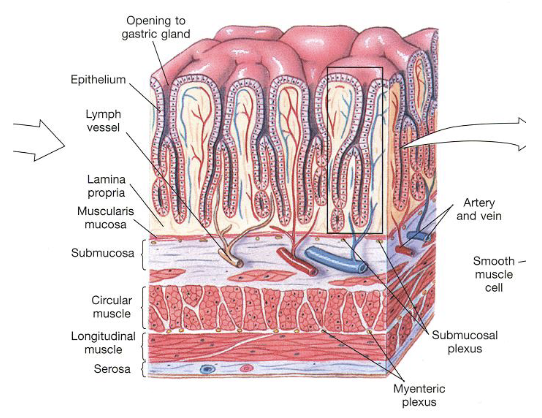
Submucosa: Submucosal Plexus (2)
Contains the submucosal plexus (Meissner’s plexus) a part of the enteric nervous system that plays a role in regulating secretion, blood flow, and local digestive functions
The submucosal plexus innervates both the epithelial layer and muscularis externa (allowing coordinated interactions between secretion, absorption, and motility)
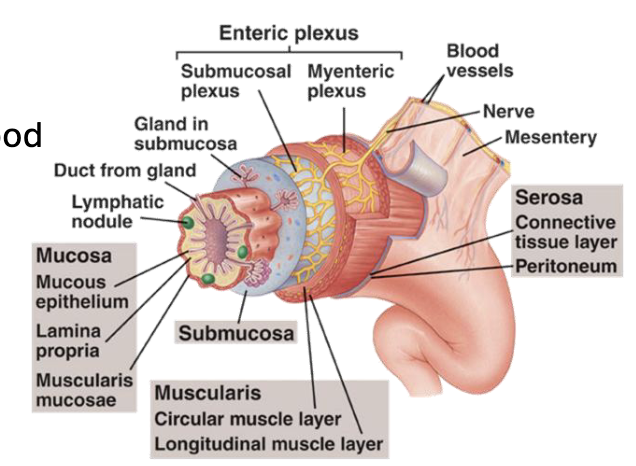
Muscularis Externa: Intestine (2)
In the intestine, the muscularis externa consists of two layers
The inner circular layer contracts to constrict the lumen to push contents forward; the outer longitudinal layer contracts to shorten the tube (aiding in propulsion during peristalsis)
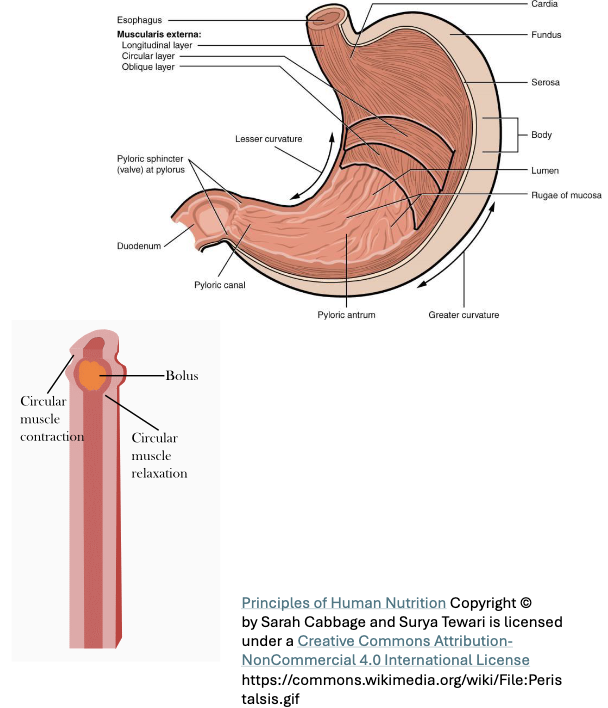
Muscularis Externa: Stomach (2)
In the stomach there are three smooth muscle layers: oblique (inner), circular (middle), and longitudinal (outer0
The additional oblique layer allows more powerful multidirectional contractions which are important for thorough mixing of food with gastric juice to produce chyme
Muscularis Externa: Myenteric Plexus
Myenteric plexus (Auerbach’s plexus) is part of the enteric nervous system and controls coordinated muscular activity
Serosa (3)
Outermost layer of the GI tract that corresponds to the visceral peritoneum; composed of connective tissue covered by simple squamous epithelium (providing smooth outer surface)
The serosa reduces friction between digestion organs and surrounding structures allowing them to slide smoothly within abdominal cavity
In certain regions the serosa is continuous with mesenteries which are folds of connective tissues that anchor the intestines to the abdominal wall and internal organs
MODULE 14: GASTROINTESTINAL 2
Processes of the Digestive System (4)
Motility
Secretion
Digestion
Absorption
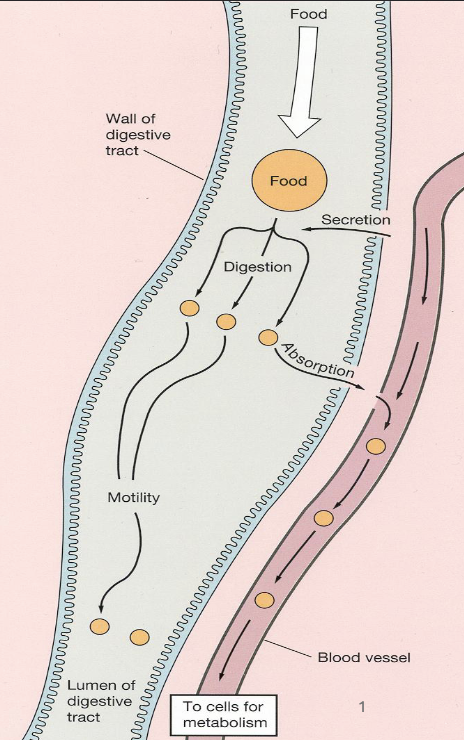
Challenges During Process of Digestion (3)
Autodigestion
Mass Balance
Defense
*Motility and secretion are major contributors in these challenges
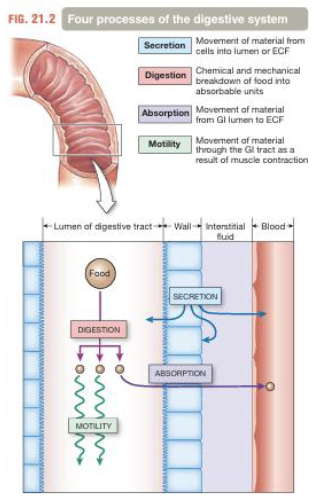
Motility (2)
Refers to the movement of food from mouth to anus (propulsion)
Motility includes mechanical mixing which breaks food into smaller particles for maximal exposure to digestive enzymes
Motility: Contractions (3)
GI smooth muscle contracts as a single coordinate unit because cells are electrically connected by gap junctions
Tonic contractions are sustained contractions that are primarily seen in sphincters (regulate passage of contents between regions)
Phasic contractions are short contractions in the stomach and intestine that mix and propel food during digestion
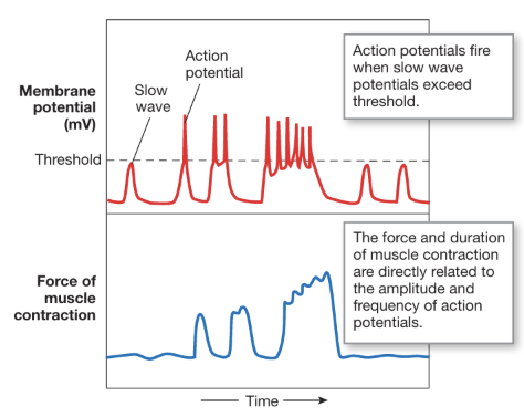
Motility: Electrical Activity - Slow Wave Potential (3)
GI motility is driven by slow wave potentials which are rhythmic cycles of depolarization and repolarization
Slow waves originate from specialized pacemaker cells called interstitial cells of Cajal (ICC) that are located between muscularis externa and enteric nerve plexus
Not all slow waves reach threshold; only when they exceed threshold does an action potential get triggered
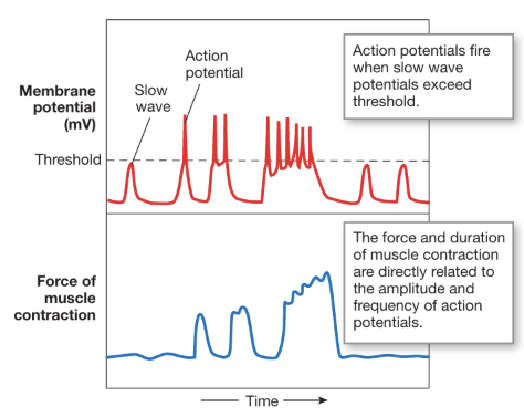
Motility: Electrical Activity - Modulation of Slow Wave Potential (3)
The enteric nervous system and GI hormones modulate slow waves by increasing likelihood they reach threshold
The frequency of slow waves is called the basic electrical rhythm (BER) and ranges from 3-12 waves per minute (varies by region - 3 wave/min in stomach and 12 waves/min in duodenum)
An increase in frequency of APs leads to longer-lasting and more forceful contractions
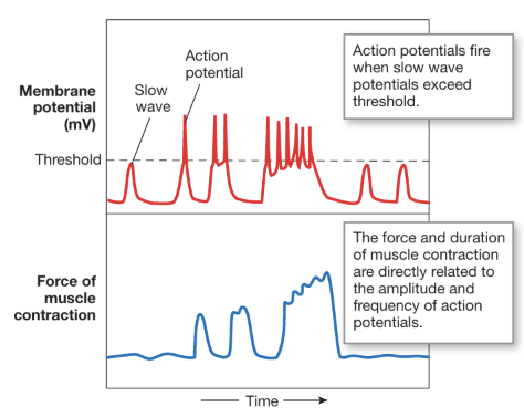
Motility: Electrical Activity - Ion Channel Activation
When slow wave reaches threshold, voltage-gated L-type Ca2+ channels (and others) open to allow calcium influx into smooth muscle
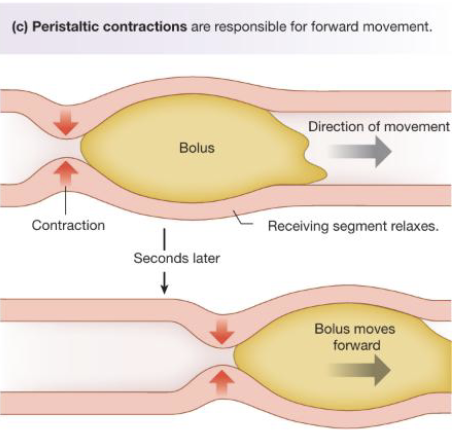
Motility: Peristalsis - Forward Movement (3)
Peristalsis involves a progressive wave of contraction where circular muscle contract behind the bolus of food, pushing it forward into next segment, while circular muscles in front of the bolus are relaxed
This process is initiated by the peristaltic reflex which is triggered by distention (stretching) of the GI wall when a bolus enters a segment
Peristalsis is regulated by hormones, paracrine signals, and the autonomic nervous system to modulate strength and coordination
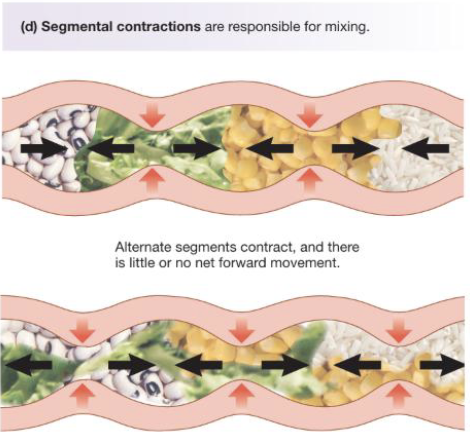
Motility: Segmental Contraction - Mixing (3)
Segmental contractions function to mix rather than propulsion in short segments of the intestine that alternately contract and relax (churn intestinal contents to increase contact with epithelial cells)
In one contracting segment, the circular muscles contract while the longitudinal muscles relax (narrowing the lumen); in the adjacent segment the pattern reverse with longitudinal muscles contracting and circular muscles relaxing (allowing contents to shift between segments)
Segmental contractions occur randomly along the intestine at regular intervals
Motility: Migratory Motor Complex (3)
MMC is a cyclic pattern of GI motility that occurs between meals when GI tract is empty (housekeeping)
Consists of coordinated waves of contraction that progress section to section (stomach through small intestine); takes 90 minutes to reach large intestine
Function is to sweep residual food particles, secretions, and bacteria out of upper GI tract (preventing bacterial overgrowth)
Secretion (2)
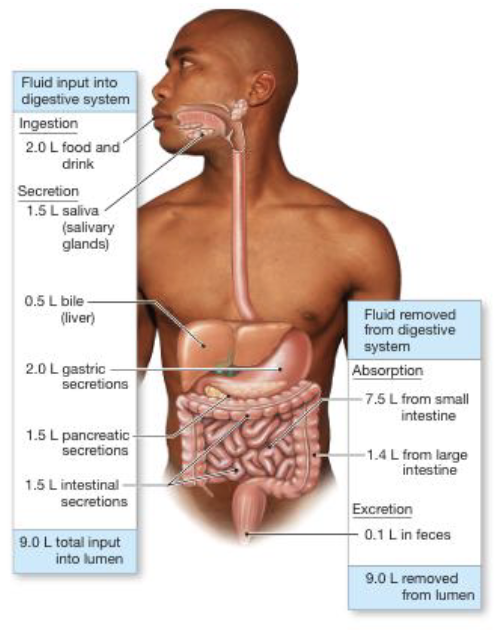
Involves movement of large volumes of fluid into the lumen (volume entering matches volume leaving)
Approximately 2L of fluid is consumed and body secretes 7L of fluid into GI tract; most is reabsorbed (if not dehydration)
Secretion: Fluids & Ions (2)
GI secretion involves the movement of key ions: Na+, K+, Cl-, HCO3-, and H+ that play a role in fluid balance
GI secretion also moves inactive proenzymes (zymogens) which are only activated in GI lumen to prevent autodigestion and helps storage in cells (e.g. pepsinogen to pepsin in stomach)
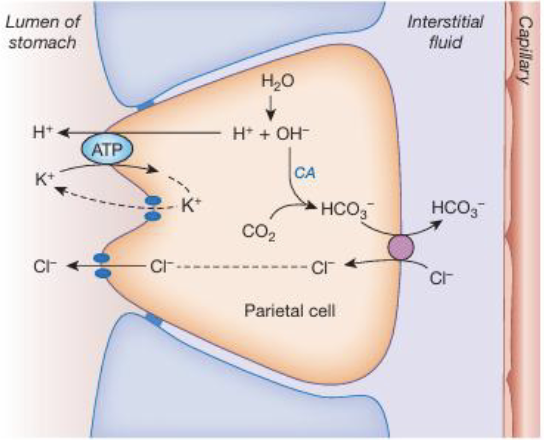
Secretion: HCL in Parietal Cells - Stomach (3)
Inside the parietal cell, carbonic anhydrase catalyzes the reaction: CO2 + H2O → H2CO3 → H+ + HCO3- to produce H+ for acid secretion and HCO3- as a byproduct
H+ ions are then actively secreted into the stomach lumen via H+/K+-ATPase (proton pump)
At the basolateral membrane, HCO3- is exchanged for Cl- (chloride shift); HCO3- enters the blood and Cl- that entered the parietal cell will diffuse into the lumen where it combines with H+ to form HCl
Secretion: HCl in Parietal Cells - Proton Pump Inhibitors
Proton pump inhibitors block the H+/K+-ATPase to reduce acid secretion; used in conditions like GERD and peptic ulcers
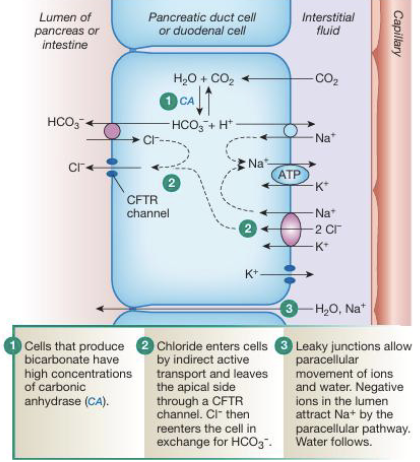
Secretion: Bicarbonate - Pancreas & Duodenum (4)
HCO3- secretion from the pancreas and duodenal epithelium is an exocrine process that produces sodium bicarbonate (NaHCO3-) along with digestive enzymes that will neutralize acidic chyme entering small intestine
Within pancreatic duct and duodenal cells, carbonic anhydrase catalyzes formation of HCO3- and H+
Bicarbonate is transported into lumen via Cl-/HCO3- exchanger where Cl- enters epithelial cells and HCO3- is secreted into lumen
H+ generated intracellularly is transported out of the cell into the interstitial fluid via the Na+/H+ exchanger to maintain pH
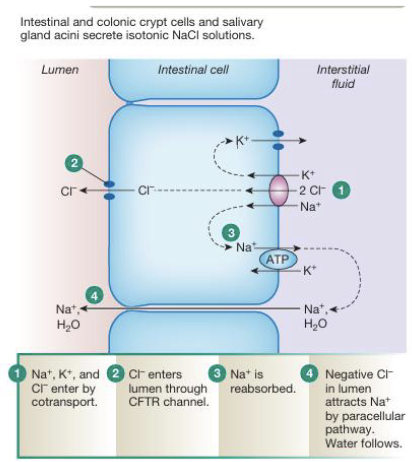
Secretion: Isotonic NaCl Secretion (4)
Cl- enters the epithelial cell primarily via NKCC cotransporter on the basolateral membrane, but can also enter through Cl-/HCO3- exchange
Cl- is then transported into the lumen through the CFTR channel across the apical membrane
Na+ is actively pumped out of the cell into the interstitial fluid by the Na+/K+-ATPase, maintaining low intracellular Na+
As Cl- accumulates in the lumen it creates a negative electrical gradient that pulls Na+ through leaky tight junctions (paracellular pathway) and water will follow osmotically
Secretion: Other (4)
Digestive enzymes are produced throughout the GI tract (mouth, stomach, pancreas, liver, intestine); stomach secretes pepsin and gastric lipase (minimal lipid digestion)
Mucus is secreted along the GI tract to lubricate contents and protect epithelial lining
Saliva is an exocrine secretion that is a hypoosmotic fluid containing water, ions, mucus, and immunoglobulins secreted by three pairs of salivary glands
Bile produced by the liver is stored in the gallbladder and released into the intestine to emulsify fats to aid in lipid digestion
Digestion & Absorption: Anticipatory Stimuli (2)
Digestion and absorption begin before food ingestion through anticipatory (cephalic) stimuli (sight, smell, and the thought of food)
This activates neural pathways to prepare GI tract (increased secretion and motility)
Digestion & Absorption: Background (3)
Digestion involves both mechanical breakdown (mixing & motility) and enzymatic breakdown of macromolecules into absorbable units
Absorption of nutrients occurs primarily in the small intestine; digested fats enter the lymphatic system while ions and water are absorbed in large intestine
Following absorption, venous blood from the GI tract enters the hepatic portal system allowing the liver to act as a biological filter that processes nutrients and detoxifies substances (hepatic clearance)
Digestion & Absorption of Carbohydrates: Amylases & Enzymes (3)
Carbohydrate digestion begins in the mouth with salivary amylase which initiates breakdown of starch and glycogen into smaller polysaccharides
Salivary amylase is denatured in the stomach due to low pH, but carbohydrate digestion resumes in the small intestine with pancreatic amylase that produces disaccharides such as maltose, sucrose, and lactose
These are further broken down at the intestinal brush border by specific disaccharidases (maltase, sucrase, and lactase) into their absorbable monosaccharide end products: glucose, galactose, and fructose
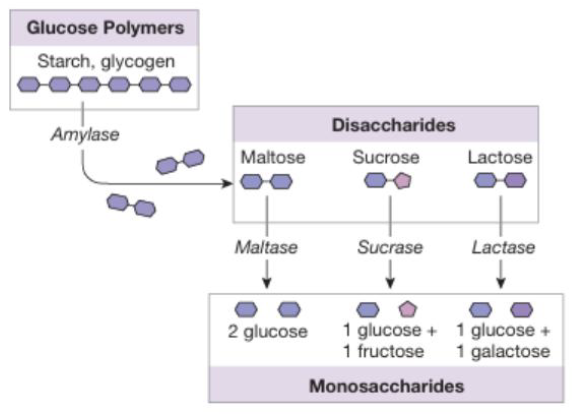
Digestion & Absorption of Carbohydrates: Indigestible Carbohydrates
Carbohydrates such as cellulose and sucralose are indigestible as humans lack the enzymes required to break them down
Digestion & Absorption of Carbohydrates: Transport (3)
Glucose and galactose are absorbed at the apical membrane via sodium-glucose symporter (SGLT) which uses the Na+ gradient to drive secondary active transport
Fructose is absorbed via facilitated diffusion through GLUT5 on the apical membrane
Once inside the enterocyte, all three monosaccharides exit across the basolateral membrane via GLUT2 into the bloodstream
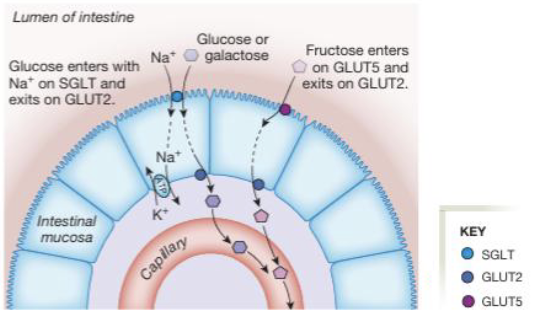
Intestinal epithelial cells use ___ as an energy source because ___
Glutamine
Preserves absorbed glucose for transport rather than being metabolized
Lactose Intolerance (4)
Lactose intolerance results from deficiency of lactase, a brush border disaccharidase that normally breaks down lactose (a disaccharide) into glucose and galactose
Lactase activity is high in juvenile mammals, but typically declines after weaning leading to reduced ability to digest lactose in many adults
When lactose is not digested in the small intestine it passes into the colon where it is fermented by the gut microbiota producing gas and bloating
Undigested lactose increases luminal osmolarity, drawing water in the colon which results in cramping and osmotic diarrhea
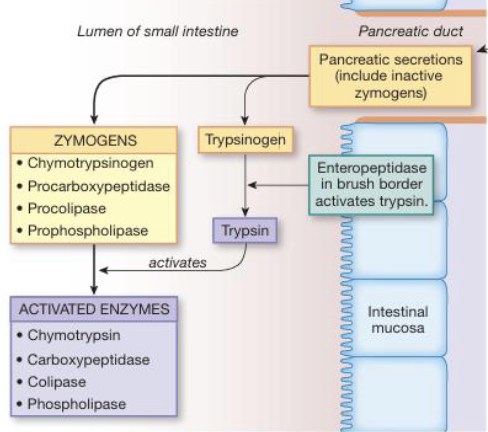
Digestion & Absorption of Protein: Enzymes (3)
Protein digestion begins in the stomach where proteins are denatured and pepsin (activated from pepsinogen) initiates cleavage into smaller peptides
This digestion continues into the small intestine via pancreatic enzymes including trypsin (from trypsinogen) and chymotrypsin (from chymotrypsinogen) secreted as inactive proenzymes
Enzymes act as endopeptidases breaking internal peptide bonds while exopeptidases such as carboxypeptidase and aminopeptidase further cleave terminal amino acids
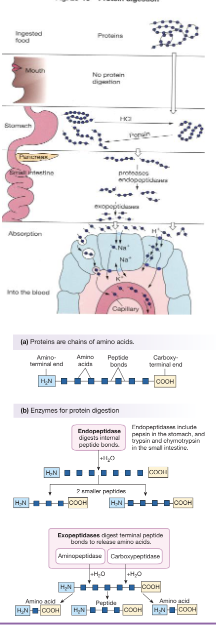
30-60% of protein in the intestinal lumen originates from ___
Endogenous sources (dead cells and secretions)
Plant proteins are ___ digestible while egg proteins are ___
Less
Most digestible
Digestion & Absorption of Protein: Transport (3)
Amino acids are absorbed through solute carrier (SLC) transporters often via secondary active transport coupled with Na+ or H+ gradients
Dipeptides and tripeptides are taken up by the oligopeptide transporter PepT1 which is driven by an H+ gradient
Once inside the enterocyte, small peptides are further hydrolyzed into free amino acids, but some might be transported intact
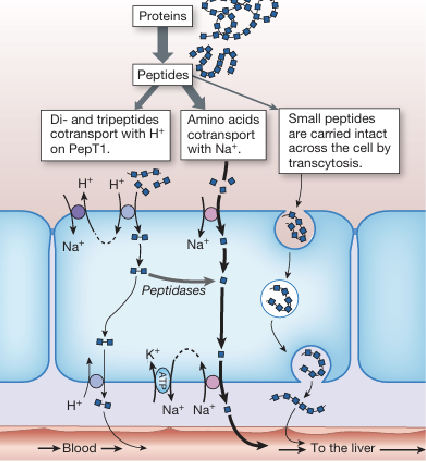
Protein transport mechanisms are significant for ___
Clinical drug absorption (medications utilize peptide transport pathways)
Digestion & Absorption of Protein: Transcytosis of Peptides
In addition to transporter-mediated uptake, larger peptides can be absorbed intact via transcytosis; peptides are taken into enterocytes by vesicles and transported across the cell to bloodstream
Digestion & Absorption of Protein: Transcytosis of Peptides - Clinical Significance (2)
The uptake of intact peptides is clinically significant because they can act as antigens that contribute to food sensitivities, intolerances, and allergies (e.g. gluten)
Advantageous in therapeutics as peptide drugs can be delivered orally such as synthetic analogs of vasopressin (1-diamino-8-D-arginine vasopression)
Digestion & Absorption of Lipids: Overview (2)
Lipid digestion involves processing of triglycerides, cholesterol, phospholipids, long-chain fatty acids, and fat-soluble vitamins (90% dietary fat calories coming from triglycerides)
Intestinal chyme is aqueous and lipids are hydrophobic and efficient digestion requires emulsification; achieved by bile (bile salts, pigments, and cholesterol) which is amphipathic (increases surface area of lipids)
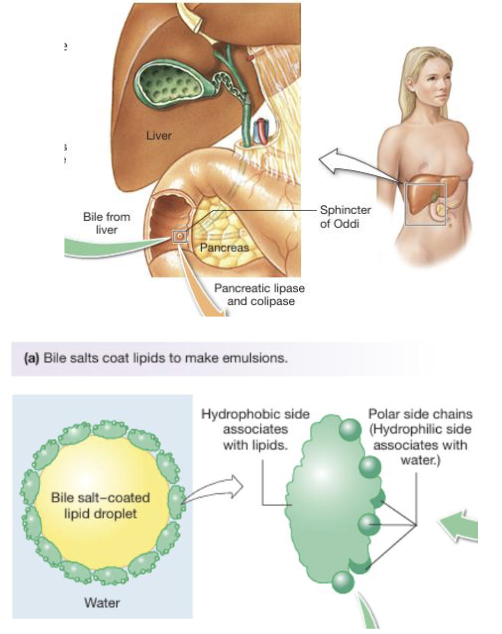
Digestion & Absorption of Lipids: Enzymes (4)
Lipid digestion is carried out by lipases from the mouth (lingual), stomach (gastric), and primarily the pancreas (pancreatic)
Pancreatic colipase is essential as it anchors lipase to the lipid droplet and allows it to function in the presence of bile salts
Pancreatic lipase hydrolyzes triglycerides into one monoglyceride and two free fatty acids which are the main absorbable products
Phospholipids are digested by pancreatic phospholipase while cholesterol is not enzymatically digested and is absorbed in its free form
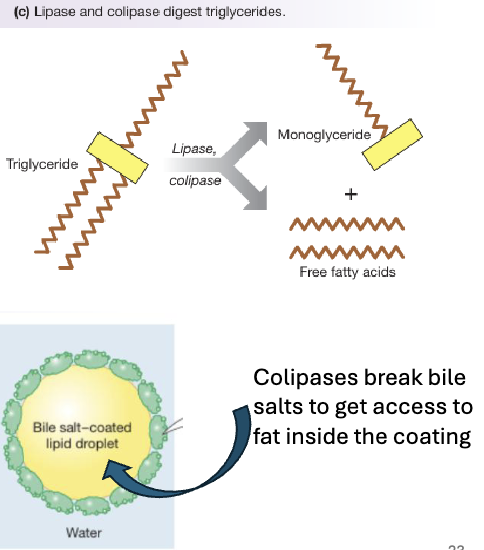
Lipid digestion processes convert dietary lipids into ___ that can be incorporated into ___
Smaller molecules
Micelles (and absorbed by intestinal cells)
Digestion & Absorption of Lipids: Transport (3)
Following digestion, lipid products aggregate to form disk-shaped micelles that transport hydrophobic lipids through the aqueous intestinal lumen
At the brush border, fatty acids and monoglycerides leave the micelles and are absorbed by simple diffusion across the lipophilic plasma membrane of enterocytes
Cholesterol uptake requires a specific transporter while bile salts remain in the lumen and are recycled
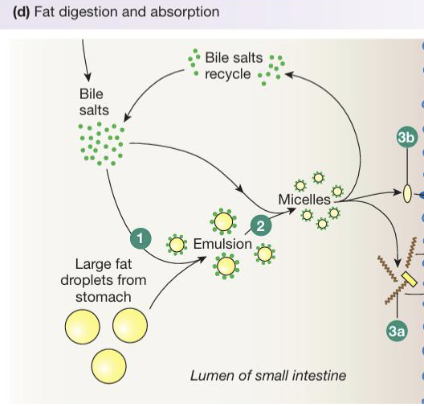
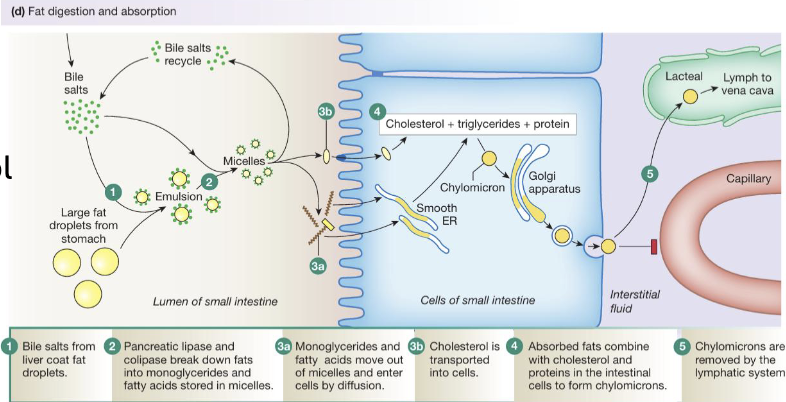
Digestion & Absorption of Lipids: Transport - Chylomicron Formation (4)
After entering enterocytes, free fatty acids and monoglycerides are transported to the endoplasmic reticulum where they are re-esterified to form triglycerides
These triglycerides are combined with cholesterol and proteins in the Golgi apparatus to form chylomicrons which are lipoprotein particles specialized for lipid transport
Chylomicrons are released from the cell via exocytosis, and because they are too large to enter blood capillaries directly they enter lymphatic vessels (lacteals)
From there they travel through the lymphatic system and are eventually drained into the venous circulation via the vena cava
MODULE 15: GASTROINTESTINAL 3
Digestion & Absorption: Other Micronutrients (4)
Nucleic Acids: Broken down by pancreatic and intestinal enzymes into nucleotides, which are further digested into nitrogenous bases and monosaccharides; bases use active transporters and monosaccharides use facilitated transports (GLUTs)
Vitamins: Absorbed based on their solubility; fat-soluble vitamins are absorbed along with lipids, and water-soluble vitamins use Na+-dependent transporters; Vitamin B12 binds intrinsic factor in the stomach and is absorbed in the ileum
Iron: Absorbed as either heme iron (animal sources) or ionized non-heme iron (plant sources) and both sources are exported from enterocytes into interstitial fluid via ferroportin
Water and Ions: Absorbed through mechanisms similar to those in kidneys
Regulation of GI Function: Enteric Nervous System (3)
GI function is primarily regulated through coordinated control of motility and secretion, largely mediated by the enteric nervous system (ENS)
ENS operates as an intrinsic neural network, responding to stimulus independently of CNS input and has two major plexuses
The GI tract is also influenced by extrinsic autonomic inputs from the CNS via sympathetic and parasympathetic pathways
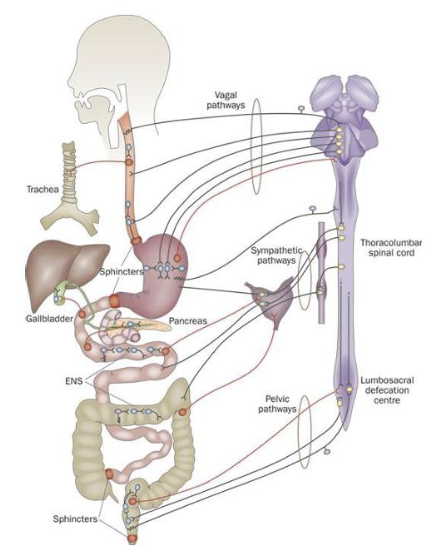
Enteric Nervous System: Plexuses & Reflexes (4)
The ENS has two major plexuses: submucosal located in the submucosa which controls secretion and local blood flow, and the myenteric located in the muscularis externa regulates smooth muscle contraction and motility
The plexuses contain neurons and glial cells that function similarly to astrocytes in the CNS to maintain local homeostasis
ENS has short reflexes which are contained within the ENS (local responses to luminal contents), and long reflexes which involve CNS input
Additionally, the ENS participates in feedforward reflexes where external cues (smell, sight, etc.,) stimulate GI activity in anticipation of digestion
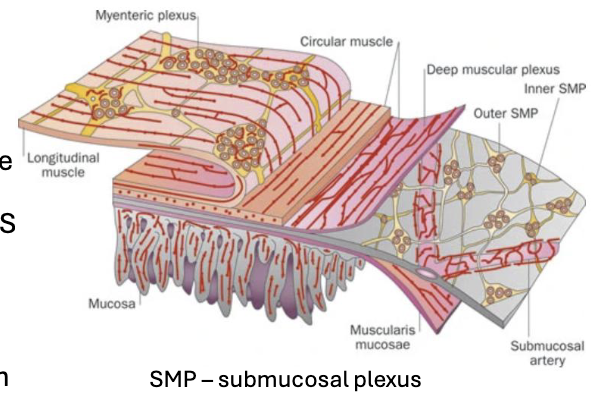
Enteric Nervous System: Parasympathetic input is ___; sympathetic input is ___
Excitatory (enhancing GI activity)
Inhibitory (reducing motility and secretion)
Gastrointestinal Peptides: Three Families
Gastrin Family
Includes gastrin and cholecystokinin (CCK) which are released in response to fats and proteins
Promotes pancreatic enzyme secretion and slowed gastric emptying
Secretin Family
Includes secretin which is released in response to acidic chyme and stimulates pancreatic bicarbonate secretion
Includes incretin hormones GIP and GLP-1 which enhance insulin secretion in response to nutrient uptake
Other
Includes peptides such as motilin which regulate fasting motility patterns by stimulating migrating motor complex
*Gastrointestinal Hormones (3)
GI hormones are synthesized by specialized enteroendocrine cells in different regions with gastrin produced in the stomach, and hormones such as secretin, cholecystokinin (CCK), GIP, motilin produced in the intestine
Hormones exert diverse physiological effects (image)
The release of these hormones is stimulated by the presence of nutrients (biomolecules) in the lumen and by mechanical distention of the GI tract

GI Paracrines & Neurocrines (2)
Paracrines are released from cells to act on nearby target cells (e.g. somatostatin inhibits gastric secretions such as H+ and pepsinogen; histamine stimulates gastric acid secretion and is itself stimulated by gastrin)
Neurocrines are signaling molecules released by neurons within the enteric nervous system and function similarly to paracrines but originate from neural cells (e.g. vasoactive intestinal peptide which modulates smooth muscle relaxation and secretion; enkephalins which influence GI motility and secretion)
Appetite & Satiety (3)
Appetite & satiety are centrally regulated by the hypothalamus which integrates signals from both central and peripheral sources
Within the hypothalamus, appetite is stimulated by orexigenic hormones such as agouti-related peptide (AgRP) and neuropeptide Y (NPY) and is suppressed by anorexigenic hormones including CART (cocaine and amphetamine-regulating transcript) and proopiomelanocortin (POMC)
In addition to central regulators, peripheral signals play a role in modulating appetite with hormones such as leptin, insulin, GLP-1, and peptide YY promoting satiety (and Ghrelin acting as a major orexigenic signal that stimulates hunger)
3 Gastric Events Following a Meal:
Cephalic Phase
Gastric Phase
Intestinal Phase
Cephalic Phase: Initiation (3)
The cephalic phase begins before food is consumed and can last 3-4 hours; initiated by external stimuli such as sight, smell, or anticipation of food
The stimuli are processed in the brain, primarily in the medulla, activating a vagal reflex via the vagus nerve which stimulates gastric secretion and motility in preparation for digestion
During this phase food is masticated (chewed) in the mouth and mixed with saliva to form a bolus that is swallowed
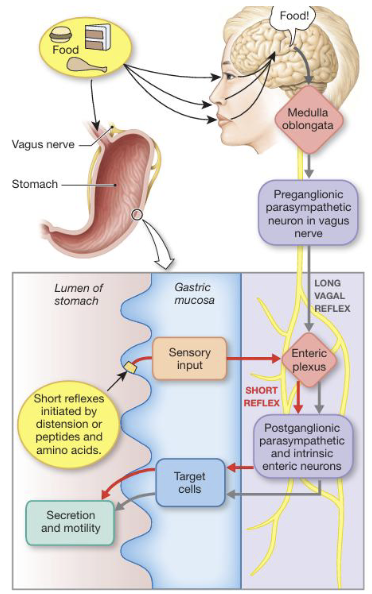
Cephalic Phase: Esophageal Sphincters
The esophagus contains two sphincters, and the lower esophageal sphincter plays a role in preventing gastric acid from refluxing into the esophagus (dysfunction causes GERD)
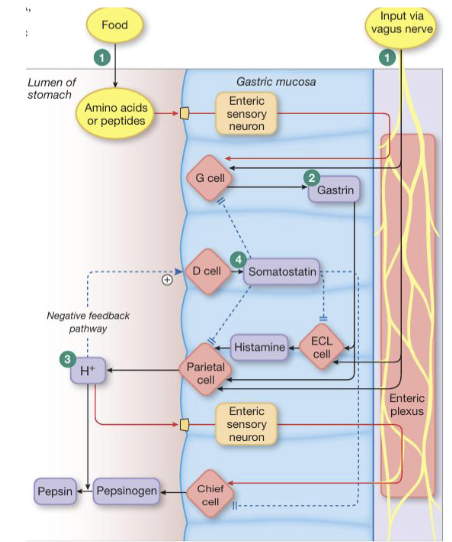
Gastric Phase: Initiation (3)
Gastric phase of digestion begins when food enters the stomach, causing the stomach to relax and expand to accommodate the incoming volume
Nutrients (amino acids and peptides) stimulate G cells to release gastrin which in turn promotes hydrochloric acid (HCl) secretion directly and indirectly through stimulation of histamine release from ECL cells (enhanced through vagal input)
Increased HCl facilitates conversion of pepsinogen to pepsin for protein digestion
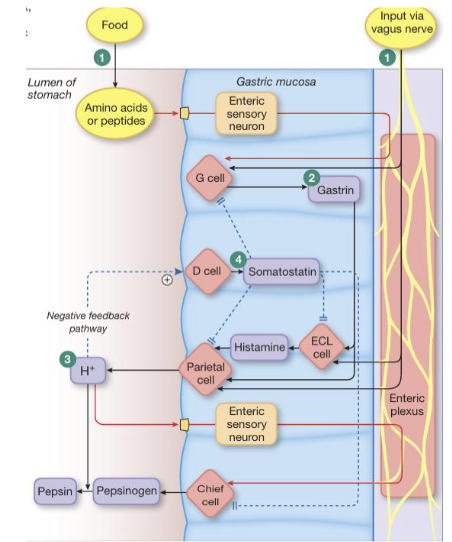
Gastric Phase: Continuation (2)
As acid levels rise, a negative feedback mechanism is activated in which HCl stimulates D cells to release somatostatin (inhibiting further secretion of HCl and pepsinogen)
The stomach protects itself from the acidic environment through mucus and HCO3- secretion along the epithelial surface; maintains a near-neutral pH at the mucosa despite luminal pH of 2
Gastric Phase: Alcohol and NSAID
Disrupt pH balance of the stomach, increasing acid secretion and comprising mucosal protection leading to ulcer formation
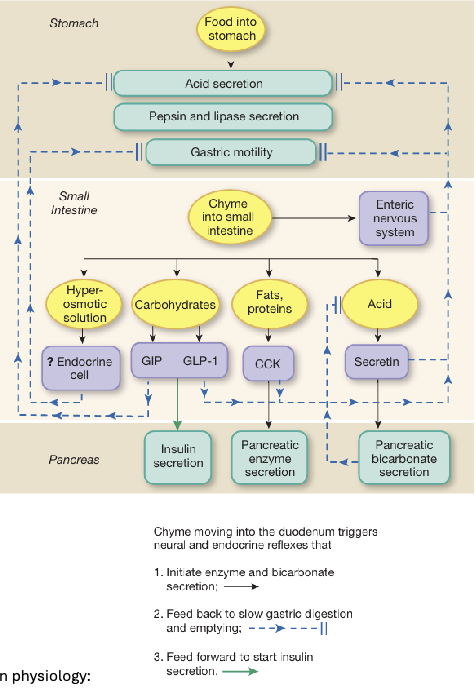
Intestinal Phase (4)
The intestinal phase of digestion begins as chyme enters the small intestine through relaxation of the pyloric sphincter
The presence of chyme activates the ENS which decreases gastric motility, alters secretion, and slows gastric emptying (optimizing digestion and absorption)
Hormonal regulation is critical with secretin and CCK being released, as well as GIP and GLP-1
Hyperosmotic chyme also activates osmoreceptors that further inhibit gastric emptying (ensures intestinal processing is not overwhelmed)
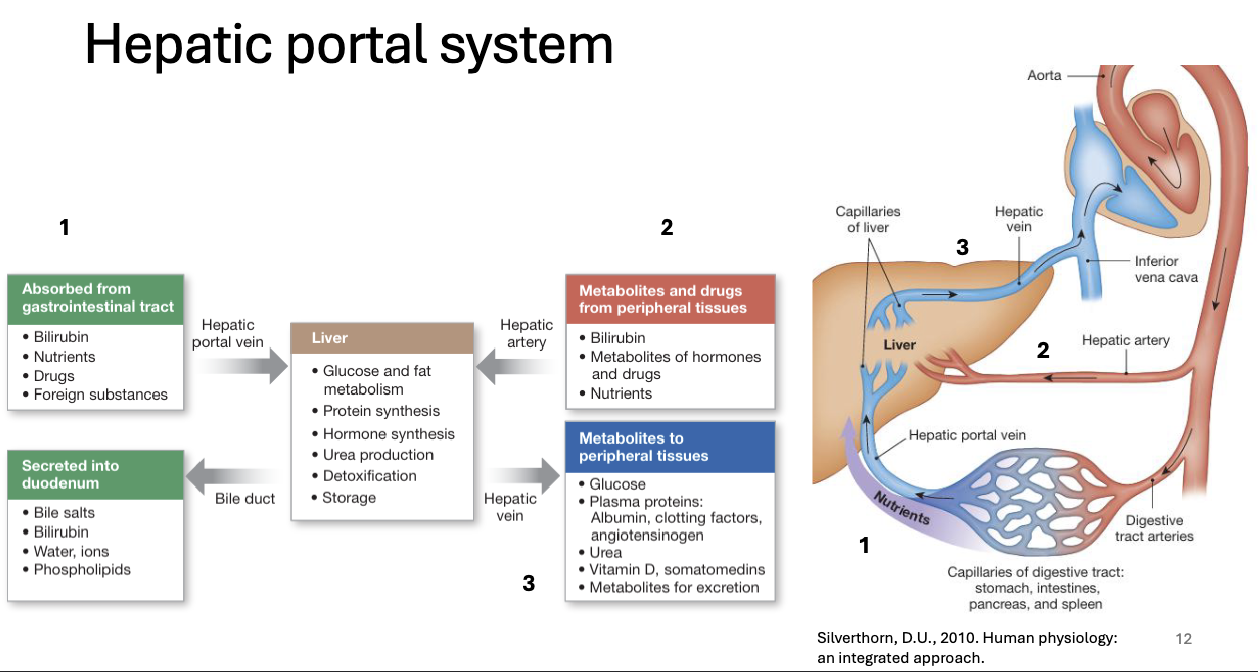
Hepatic Portal System

The large intestine receives ___ of chyme from the ileum, of which ___ is eliminated as feces, and remainder is absorbed as water and electrolytes
1.5L
0.5L
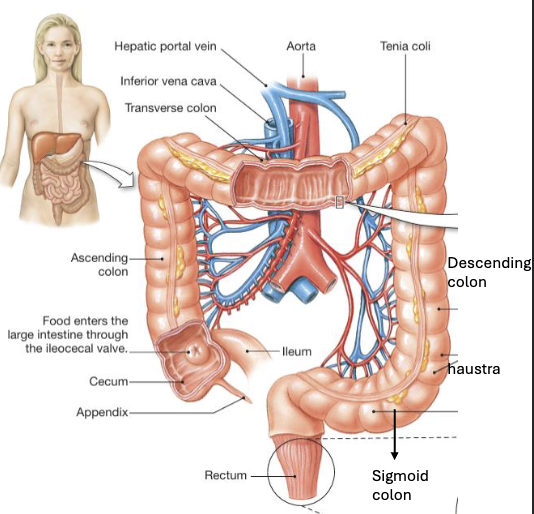
Large Intestine: Anatomy (3)
Chyme enters through the ileocecal valve which is tonically contracted, but relaxes in response to gastroileal reflex when the stomach empties
The large intestine is divided into seven regions: cecum (pouch containing the appendix), ascending colon, transverse colon, descending colon, sigmoid colon, rectum, and anus
Structurally, it is characterized by haustra (pouch-like segments) formed due to discontinuous arrangement of the longitudinal muscle layer (taeniae coli) in the muscularis externa
Large Intestine: Motility (4)
Segmental contractions (haustral contractions) mix the contents to maximize contact with absorptive surfaces
Forward propulsion occur through mass movements (unique colonic contraction) that occurs 3-4 times a day
These movements are stimulated by the gastrocolic reflex where stomach emptying signals the colon to move contents forward
When feces enters the rectum, the defecation reflex is triggered leading to relaxation of the internal anal sphincter (smooth muscle) while the external anal sphincter (skeletal muscle) can be voluntarily controlled
Large Intestine: Digestion & Absorption (2)
Digestion and absorption are mediated by gut microbiota which break down complex carbohydrates and proteins into metabolites such as lactate and short-chain fatty acids that are absorbed by colonocytes
Colonic bacteria also synthesize important vitamins (vitamin K) and fermentation processes produce gases as a byproduct
Large Intestine: Digestion & Absorption - Diarrhea (2)
The large intestine plays a role in fluid and electrolyte balance, and disruptions in motility can cause diarrhea or vomiting
Secretory diarrhea (caused by pathogens such as Vibrio cholerae or E. coli) results from increased chloride secretion leading to water and mucus loss
Large Intestine: Digestion & Absorption - Vomiting (2)
Vomiting is a protective reflex triggered by stimuli such as toxins, drugs, pain, or imbalance coordinated by the medulla
Vomiting involves reverse peristalsis, relaxation of the stomach and pyloric sphincter, increased abdominal pressure, and temporary inhibition of respiration
MODULE 16: GASTROINTESTINAL 4
Comparative Digestive Systems: Invertebrates - Two-Way Guts (3)
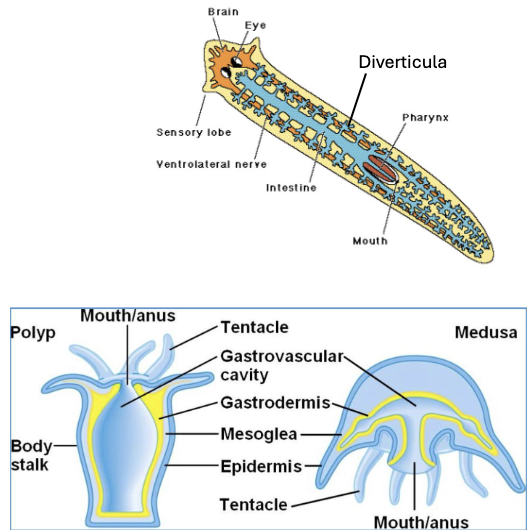
Simple invertebrates such as cnidarians and platyhelminthes possess a two-way digestive system in which food enters and waste exits through the same opening
This forms a gastrovascular cavity rather than a complete digestive tract, which extends throughout the body and allows nutrients to be distributed by diffusion
To increase efficiency, the digestive surface is highly branched through structures called diverticula which expand surface area
Comparative Digestive Systems: Invertebrates - One-Way Guts (6)
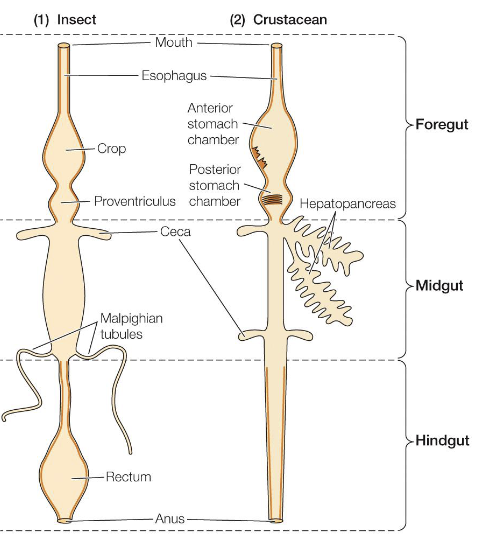
In more complex invertebrates (arthropods), the digestive system is organized as a one-way gut with separate openings for ingestion and excretion
The foregut, which may include a crop or stomach can be slightly acidic (pH 4) and is involved in storage and initial digestion
The midgut is the primary site of digestion and absorption
The foregut and hindgut are lined with chitin, making them impermeable and limiting absorption to the midgut
Structures such as ceca increase surface area and house microbiota that aid in digestion
Malpighian tubules connect to the gut and transport nitrogenous waste (urine) into the digestive tract where it is excreted along with fecal material
Comparative Digestive Systems: Vertebrates (3)
Comparative digestive systems in vertebrates vary significantly depending on diet, metabolic demands, and lifestyle adaptations
Herbivores, carnivores, and omnivores exhibit distinct structural differences that reflect the type of food they consume and the complexity of digestion required
Major variations among vertebrates include differences in stomach structure and the overall length and organization of the digestive tube