The Reproductive System
1/38
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
39 Terms
Secreted steroid sex hormones:
androgens (males)
estrogens and progesterone (females)
The Scrotum
sac of skin and superficial fascia
paired testes below body temp. for sperm production
Dartos muscle: smooth muscle, pulls Scrotum close to body
cremaster muscles: skeletal muscle - elevate
The Testes
membranes: tunica vaginalis & albuginea
septa: divide testes into lobules
seminiferous tubules: site of sperm production
myoid cells: squeeze sperm and testicular fluids out of testes
Sperm Formation
acrosome: contains enzymes for digesting through the egg’s protective coat
head: contains chromosomes
middle piece: has mitochondria for energy release
tail: for movement
Testicular Cancer
Rare, but most common cancer in men age 15-35
having mumps that lead to orchitis (inflammation of testis) could be a risk factor
cryptorchidism is most common risk factor (non descent of testes)
failure of the testis to make their normal decent is also a risk factor
sign: painless, solid mass in testis
90% cured by surgical removal of testis and often radiation or chemotherapy
Prostate Cnacer
second most common cause of cancer death in males
digital exam screening, PSA levels: biopsy if abnormal
treated with surgery and sometimes radiation, castration, drugs
in clinical trails: cryosurgery, chemotherapy, ultrasound, proton beam therapy
Seminal Glands
smooth muscle contracts during ejeculation
viscous alkaline seminal fluid
duct joints ductus deferens to form ejaculatory duct
Prostate
encircles urethra inferior to bladder
smooth muscle that contracts during ejeculation
secretes milky, slightly acid fluid
plays a role in sperm activation
Bulbourethral Glands
pea size glands inferior to prostate
thick, clear mucus during sexual arousal
neutralize traces of acidic urine in urethra
lubricate glands penis
Semen
sperm and accessory gland secretions
contains fructose of ATP production, protects & activates sperm, and facilitates sperm movements
alkaline fluid
Secreted female sex hormones
estrogen (estradiol, estrogen, estriol): induce secondary sex characteristics, promote oogenesis & follicle growth in ovary, and metabolic effects
progesterone: establish & regulate uterine cycle
Ovulation
ejection of oocyte from ripening follicle
Male Duct System
Epididymis: contracts, expel sperm into ductus deferens, stores sperm cells
Ductus deferens: join duct of seminal vesicle to form ejaculatory duct
Ejaculatory duct
Urethra: transports urine and semen
Female Duct System
Uterine tubes: receives ovulated oocyte & usual site of fertilization
Uterus: receive, retain, and nourish fertilized ovum
Vagina: birth canal, passageway for menstrual flow, copulation
Ectopic Pregnancy
oocyte is fertilized in peritoneal cavity or distal uterine tubes and begins developing there
normally aborted naturally with substantial bleeding
Uterine Tubes
Pelvic inflammatory disease (PID)
spread of infection from reproductive tract to peritoneal cavity
may cause scar tissue and lead to infertility
Uterine Tubes
Cervical Cancer
Risk: frequent cervical inflammation; STIs, including HPV, or multiple pregnancies
Papanicolaou (Pap) smear for detection
Uterus
Prolapse of the uterus
An unsupported uterus may sink inferiorly, until tip of cervix protrudes through the external vaginal opening
causes: overstretching & tearing muscles during childbirth
Mammary Glands
main function is milk production to nourish newborn
Breast Cancer
usually arises from epithelial cells of smallest ducts that eventually metastasize
risks factors:
early onset of menstruation and late menopause
no pregnancies or first pregnancy lat ein life
no or short periods of breast feeding
family history of breast cancer
diagnosis: self-examination, mammography
treatment: radiation, chemotherapy, sorgery
Follicle- Stimulating Hormone (FSH)
Females: triggers the growth of eggs in the ovaries and gets the eggs ready for ovulation
Males: stimulate sperm production
Luteinizing Hormone (LH)
sexual development in children and fertility in adults
Females: helps control the menstrual cycle; triggers the release of an egg from the ovary (ovulation)
Males: causes the Leydig cells of the testes to produce testosterone
Testosterone
stimulates male secondary sex characteristics (muscle mass, deeper voice, facial hair, increases bone density)
Estrogen
Females: secondary sex characteristics (breasts growth, public hair), start menstrual cycles, regulate menstrual cycle
Males: erectile function
Progesterone
Females: maintenance of embryo and uterus during early pregnancy, stays at high levels during pregnancy to stop menstrual cycles
Males: builds bone mass
GnRH
controls the release of the anterior pituitary(FSH & LH release)
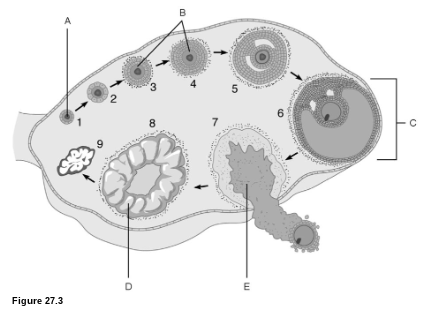
Egg Production: What is D?
corpus luteum
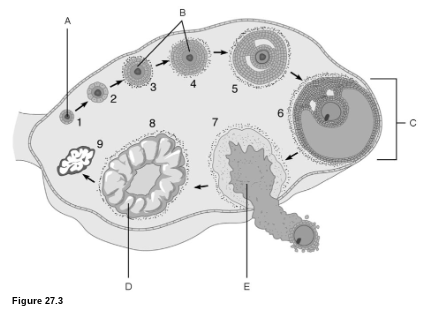
Egg Production: What is C?
mature follicle
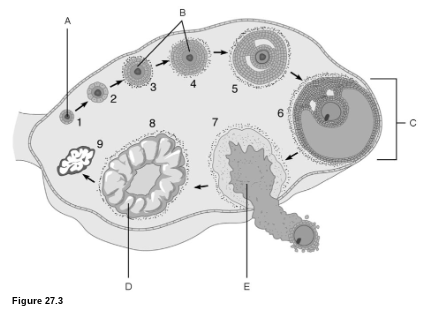
Egg Production: What is E?
ovulation
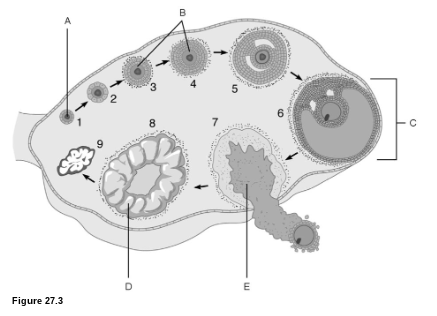
Egg Production: What is A?
primordial follicle
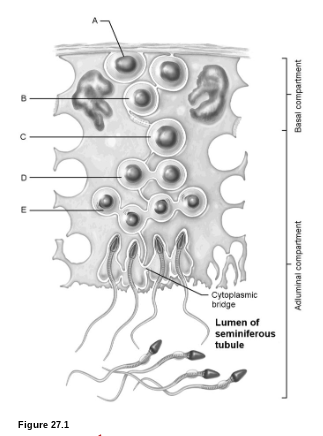
Sperm Production: What is E?
early spermatids
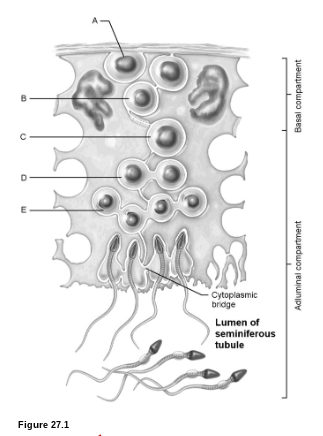
Sperm Production: What is A?
spermatagonia
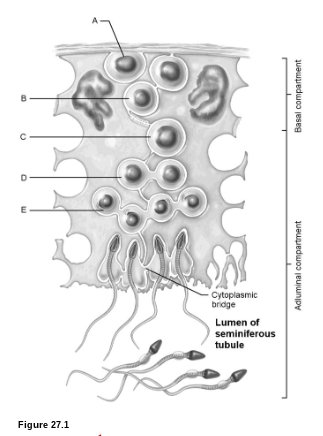
Sperm Production: What is B?
primary spermatocyte
Fallopian Tubes
receives the ovulated oocyte, providing a site for fertilization
Pathway of Sperm
seminiferous tubules
epididymis
vas deferens
urethra
Order of the Layers of the Uterine Wall (inner→outer)
endometrium
myometrium
perimetrium
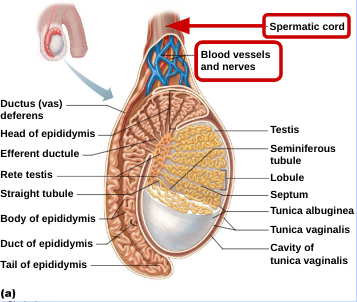
Blood supply
arteries from abdominal aorta
veins form pampiniform venous plexus surrounding arteries - absorb heat from testicular arteries, keep testes cool
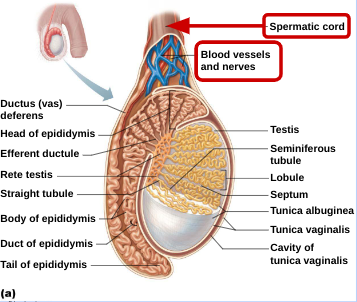
Spermatic Cord
encloses nerve fibers, blood vessels and lymphatics that supply testes
Spermatogenesis
production of sperm (spermatozoa) in seminiferous tubules
most body cell shave 46 chromosomes:
two sets (23 pairs) of chromosomes
one maternal, one paternal: homologous chromosomes
referred to as diploid chromosomal number (2n)
gametes have only 23 chromosomes: haploid chromosomal number (n)
only one member of the homologous pair