The Reproductive System
Primary sex organs (gonads): testes and ovaries
Accessory reproductive organs: ducts, glands and external genitalia
Male Reproductive System: Testes produce sperm released through ducts
Testes: within the scortum
Ducts: epididymis, ductus deferens, ejaculatory duct, and urethra
Accessory sex glands: seminal glands, prostate, and bulbourethral glands
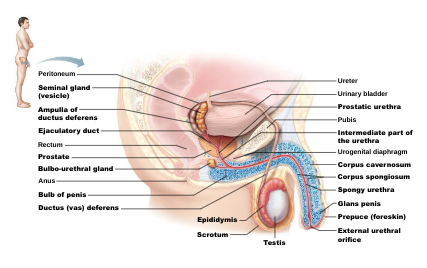 The Scrotum: sac of skin and superficial fascia
The Scrotum: sac of skin and superficial fascia
outside abdominopelvic cavity
paired testes
below body temp.
septum divides into two
3C lower than core body temperature
Lower temperature is necessary for sperm production
Midline septum divides scrotum into two compartments, one for each testis
Dartos muscle: smooth muscle, pulls Scrotum close to body
Cremaster muscles:skeletal muscle - elevate
The Testes:
Membranes:
Tunica vaginalis: outer, derived from peritoneum
Tunica albuginea: inner layer forms fibrous capsule
Septa: divides testes into lobules
1250 lobules each
1-4 seminiferous tubules
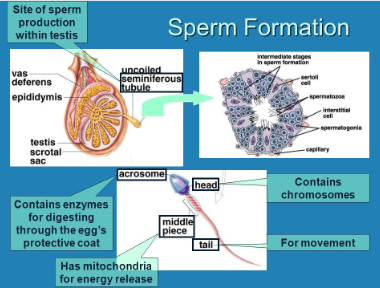
site of sperm production
Seminiferous Tubules:
Myoid cells surround each tubules - smooth muscle - like cells squeeze sperm and testicular fluids out of testes
Epididymis: 3 sections: head, body, tail
Blood supply:
arteries from abdominal aorta
veins form pampiniform venous plexus surrounding arteries - absorb heat from testicular arteries; keeps testes cool
Spermatic cord encloses nerve fibers, blood vessels, and lymphatics that supply testes
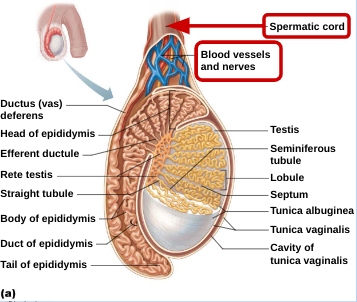
Homeostatic Imbalance:
Testicular cancer
rare, but most common cancer in men age 15-35
having mumps that lead to orchitis (inflammation of testis) could be a risk factor
cryptorchidism is most common risk factor
non descent of testes
sign: painless, solid mass in testis
90% cured by surgical removal of testis and often radiation or chemotherapy
Penis:
corpus spongiosum: surrounds urethra and expands to form glands and bulb
corpora cavernosa: paired dorsal erectile bodies
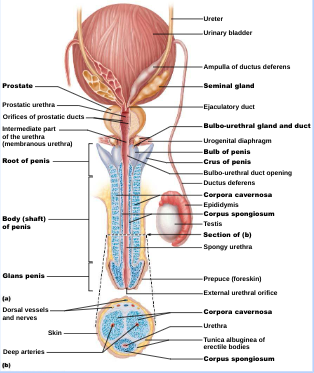
Male Duct System: ducts carry sperm from testes to body exterior
Epididymis: 6m long
microvilli(stereocilia) absorb testicular fluid and pass nutrients to stored sperm
sperm: 20 days to become motile
contracts, expel sperm into ductus deferens
Ductus Deferens(vas deferens): 45 cm long
joints duct of seminal vesicle to form ejaculatory duct
smooth muscle in walls: propels sperm from epididymis to urethra
vasectomy: cutting and ligating ductus deferens (100% birth control)
Ejaculatory duct
Urethra: transports urine and semen
3 regions:
prostatic urethra
intermediate (membranous urethra): in urogenital diaphragm
spongy urethra: runs through penis; opens at external urethral orifice
Male Accessory Glands:
Seminal glands:
smooth muscle contracts during ejeculation
viscous alkaline seminal fluid
duct joints ductus deferens to form ejaculatory duct
Prostate:
encircles urethra inferior to bladder
smooth muscle that contracts during ejaculation
secretes milky, slightly acid fluid
plays a role in sperm activation
Prostate Cancer:
second most common cause of cancer death in males
digital exam screening, PSA levels
biopsy if abnormal
treated with surgery and sometimes radiation, castration , drugs
in clinical trials: cryosurgery, chemotherapy, ultrasound, proton beam therapy
Bulbourethral glands:
pea sized glands inferior to prostate
thick, clear mucus during sexual arousal
neutralize traces of acidic urine in urethra
lubricate glands penis
Semen: sperm and accessory gland secretions
contains fructose of ATP production, protects and activates sperm, and facilitates sperm movement
alkaline fluid
Female Reproductive Anatomy: reproductive role of female more complex because of pregnancy
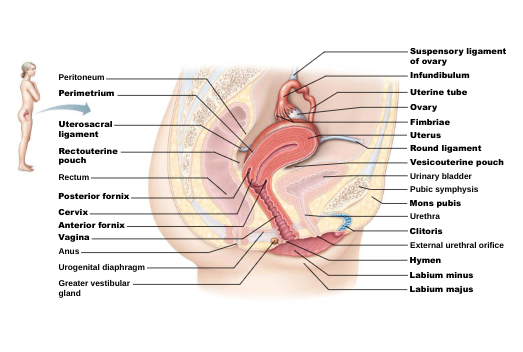
Ovaries: female gonads
Ligaments: suspensory ligament and mesovarium are part of broad ligament that supports uterine tubes, uterus, and vagina
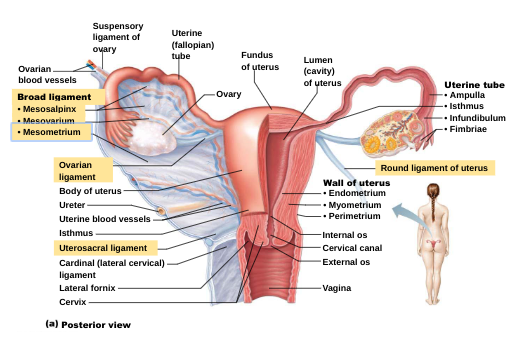
Tunica albuginea:
fibrous, covers ovaries
covered by germinal cuboidal epithelium outer layer (continuation of peritoneum
Two poorly defined regions:
outer cortex: houses forming gametes
inner medulla: contains large blood vessels and nerves
Ovarian follicles: tiny saclike, embedded in cortex
contain immature eeg (oocyte)
go through several stages of development
Ovulation:
ejection of oocyte from ripening follicle
Female Duct System: tube system includes:
Uterine tubes: regions of uterine tube
isthmus: constricted area, joins uterus
ampulla: distal ends, curves around ovary
infundibulum: distal extension near ovary, ciliated fimbriae
Homeostatic Imbalance: Uterine Tubes
Ectopic pregnancy:
oocyte is fertilized in peritoneal cavity or distal uterine tube and begins developing there
normally abort naturally with substantial bleeding
Pelvic inflammatory disease (PID)
spread of infection from reproductive tract to peritoneal cavity
may cause scar tissue and lead to infertility
Uterus:
hollow, thick walled, muscular organ
receive, retain, and nourish fertilized ovum
position of uterus
Anteverted: inclined forward (normal position)
retroverted: inclined backward
Homeostatic Imbalance: Uterus
Cervical cancer
risk: frequent cervical inflammation; STIs, including HPV; or multiple pregnancies
Papanicolau (Pap) smear for detection
Prolapse of the uterus: unsupported uterus may sink inferiorly, until tip of cervix protrudes through the external vaginal opening
causes: overstretching & tearing muscles during childbirth
Uterine Wall: three layers of wall
perimetrium: outermost (visceral peritoneum)
myometrium: middle, layers of smooth muscle
contracts rhythmically during childbirth
endometrium: mucosal lining
simple columnar epithelium
fertilized egg burrows into endometrium
stratum functionalis - shed
stratum basalis - base layer
Vagina:
thin-walled tube 8-10 cm (3-4 inches) in length
birth canal, passageway for menstrual flow, copulation
vaginal secretions acidic in adult females, alkaline in adolescents
Sperm Production:
the golgi apparatus packages the acrosomal enzymes
the acrosome forms at the anterior end of the nucleus and the centrioles gather at the opposite end
microtubules form the flagellum
mitochondria multiply and cluster around the proximal portion of the flagellum
excess cytoplasm sloughs off
an immature sperm that has just been released from a sustentocyte
structure for a fully mature sperm
Egg Production:
Primordial follicle with a primary oocyte
Primary follicle
Secondary follicle
Graffian follicle
Corpus Luteum
Fetal Development: major understandings:
Fertilization:
sperm travels from vagina → cervix → uterus → fallopian tubes
when encounter egg, sperm uses enzymes form acrosome to disintegrate zona pellucida surrounding egg
only one can penetrate to fuse nucleus with nucleus of egg
fertilized egg = zygote
divided into 2 cells = embryo
keeps dividing & traveling down fallopian tubes until reaches uterus
Development:
day 4: solid ball of ~50 cells
day 5/6: blastocyst (hollow ball w/ fluid in center)
day 6/7: attaches to uterus after fertilization
~3 weeks: nervous & digestive system develop
placenta: connection between mother & embryo, function: nourishment, respiration & excretion, barrier to disease, materials diffuse across capillaries
8 weeks = fetus
12 weeks = umbilical cord
8 cm long, 28g
reflexes and movement
4-6 months = specialization
6+ months: can survive
mass doubles, lungs finish
Fetal testing:
ultrasound
genetic tests:
alpha fetoprotein: check for down’s syndrome and spinal bifida
amniocentesis: 16 weeks +
Chorionic Villus sampling: 10 weeks