Comprehensive Veterinary Cardiology and Respiratory Disease Guide
1/312
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
313 Terms
What is the prevalence of heart disease in cats?
15%
What is a common clinical sign of obstructive HCM?
Tachypnoea and crackles
What can cause pulmonary oedema in obstructive HCM?
High pressure backflow into pulmonary vasculature
What is the treatment for severe left ventricular outflow obstruction (LVOTO) in cats?
Atenolol (beta blocker)
What is a potential complication of dilated left atrium in cats?
Intracardiac thrombus leading to saddle thrombus
What is the significance of cardiac troponin I in heart disease?
It is released upon cardiomyocyte damage
What does NT-proBNP indicate in heart disease?
Myocardium stretch
What is the primary treatment for congestive heart failure in cats?
Furosemide (loop diuretic)
What is the most common acquired heart disease in dogs?
Degenerative Mitral Valve Disease (DMVD)
What is a common clinical sign of DMVD in dogs?
Cough and dyspnoea
What is the typical age range for dogs affected by DCM?
Middle aged to older dogs
What is a common echocardiographic finding in DCM?
Decreased fractional shortening (<25%)
What is the role of pimobendan in heart disease treatment?
It is an inotrope that enhances sensitivity of troponin to calcium
What is a potential side effect of grain-free diets in dogs?
Increased risk of DCM
What is the significance of a gallop rhythm in heart disease?
It indicates heart failure or volume overload
What are the stages of heart disease in cats?
B1 (subclinical), B2 (mild), C (congestive heart failure), D (refractory heart failure)
What is a common arrhythmia seen in dogs with DCM?
Atrial fibrillation
What is a common cause of sudden death in cats with heart disease?
Arrhythmia due to left ventricular fibrosis
What is the significance of left atrial enlargement in heart disease?
It increases the risk of congestive heart failure and thromboembolism
What is a common treatment for arrhythmias in dogs?
Anti-arrhythmics like beta blockers or amiodarone
What does the presence of a left apical systolic murmur indicate?
Mitral valve regurgitation
What is the primary cause of heart failure in dogs with DMVD?
LSHF
What is the treatment for refractory heart failure in dogs?
Torasemide instead of furosemide if needed
What is the role of ACE inhibitors in heart disease treatment?
They help reduce afterload and improve forward flow
What condition can increased pressure in the pericardial sac cause?
RSCHF- right ventricle has thinner wall than left
underfilling of heart
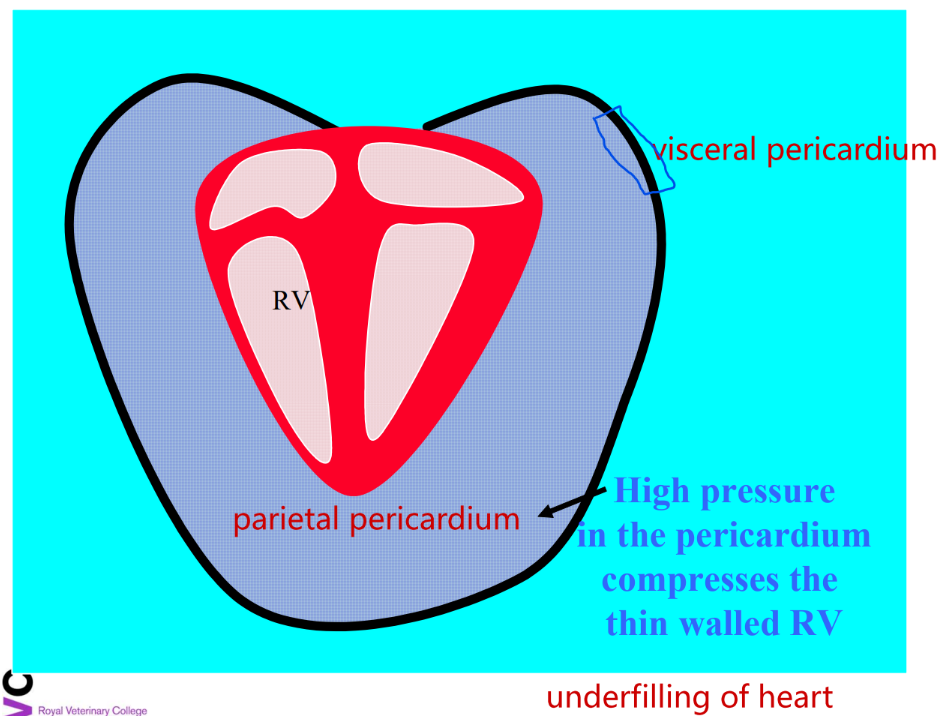
What are common signs of right-sided congestive heart failure (CHF)?
Ascites, jugular pulse or distension, hepatomegaly.
What is a common cause of acute pericardial effusion?
Trauma.
What is the typical ultrasound site for pericardiocentesis?
At the costochondral junction, right side, rib space 5 or 6.
What is the primary complication of cardiac tamponade?
Fluid pressure collapses the right heart.
What does the presence of fluid in the pericardial sac indicate?
Possible cardiac tamponade.
What can cause jugular distension in cattle?
Increased right atrial pressure due to conditions like lymphoma.
What is the prognosis for neoplastic causes of pericardial effusion?
Generally poor, especially with right atrial hemangiosarcoma.

What is a common diagnostic sign of pericardial effusion?
Muffled heart sounds.
What is the significance of pulsus paradoxus?
It indicates varying venous return and can be associated with cardiac tamponade.
pulse drops on inspiration

What is traumatic reticuloperitonitis (TRP)?
A condition caused by foreign bodies penetrating the reticulum, leading to pericarditis.
What are common clinical signs of TRP?
Fever, anorexia, depression, and abdominal pain (grunt when dipping-withers pinch test).
What is the treatment for a foreign body in the reticulum?
Surgical removal, often involving a magnet.

What is the typical age for cows to develop bovine leukemia virus-related lymphoma?
Cows older than 4 years.
What is cor pulmonale?
RSHF secondary to pulmonary hypertension.
What are the signs of pulmonary hypertension in cattle?
Subcutaneous edema and split S2 sound.
Pulmonary artery hypertension → pulmonary valve closes earlier than aortic valve
What can cause thrombophlebitis in horses?
Repeated vessel trauma, thrombogenic solutions, or bacterial contamination.
What is the recommended action if thrombosis is observed in a jugular vein?
Stop taking blood from that vein.
What are the potential outcomes of an ingested foreign object in ruminants?
Fluid in the pericardial sac or traumatic reticuloperitonitis.

What is the significance of electrical alternans in ECG?
It can indicate pericardial effusion.
What is the management strategy for recurrent pericardial effusion?
Removal of the parietal pericardium.
What can cause right atrial myocardium lymphoma?
Bovine leukemia virus.
What are the typical clinical signs of right-sided heart failure?
Jugular distension, weak peripheral pulses, and venous congestion.
What is the emergency situation related to pericardiocentesis?
The right atrial wall can flap and collapse, impairing venous return.
Cardiac tamponade
What are the common anti-inflammatories used in veterinary medicine?
Firocoxib (horses), phenylbutazone, flunixin
What occurs if an infected thrombus detaches?
It can lead to an embolism and showering.
What is the role of anticoagulants in clot management?
They prevent the growth of clots but do not dissolve them.
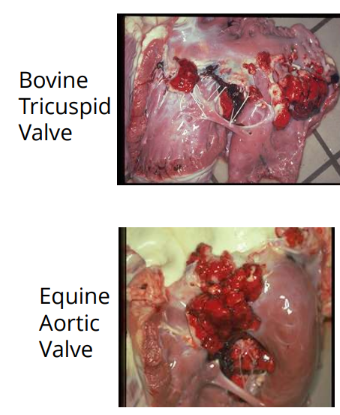
What is the most common location of bacterial endocarditis in large animals?
Tricuspid valve.
What are the clinical signs of bacterial endocarditis?
Fever and murmur.
What is the preferred anticoagulant for emergencies?
Aspirin.
What is the best anticoagulant for long-term use?
Low molecular weight heparin.
What is the prognosis for small animals with bacterial endocarditis?
Guarded prognosis.
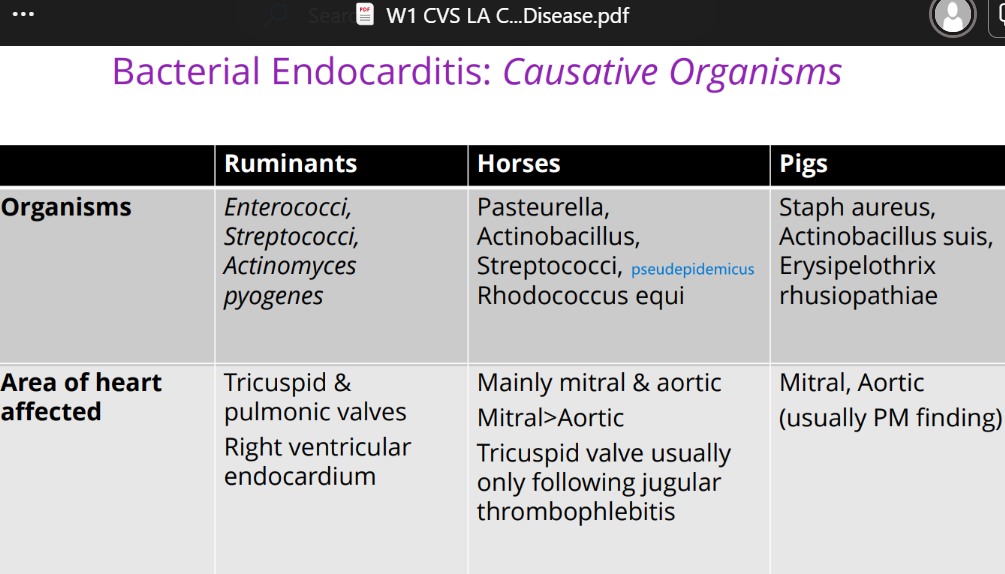
What are common causative organisms of bacterial endocarditis in ruminants?
Trueperella pyogenes, Enterococci, Streptococci.
What are the common signs of exercise-induced pulmonary hemorrhage (EIPH) in horses?
Blood traces and epistaxis after exercise.
What is the treatment for EIPH in horses?
Modify training program and provide a dust-free environment.
What is the effect of furosemide on horses with EIPH?
It reduces circulating volume but is banned for racing in the UK.
What are the common respiratory diseases in dogs and cats?
Canine distemper and cat flu.
What is the primary agent of cat flu?
Feline herpesvirus (FHV-1).
What are the clinical signs of cat flu?
Serous to mucopurulent oculonasal discharge.
What is the treatment for bacterial infections in small animals?
Doxycycline or amoxiclav.
What is the primary agent of canine infectious respiratory disease (CIRD)?
Bordetella bronchiseptica.
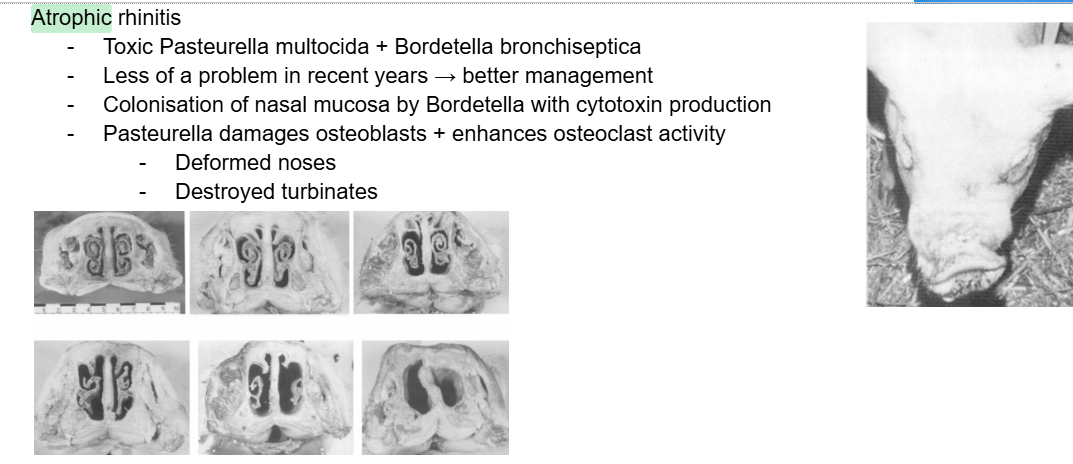
What is the prognosis for pigs with atrophic rhinitis?
Usually good/self-limiting unless complicated. (better managed in recent years)
Pasteurella multocida
B. bronchiseptica
What are common signs of respiratory disease in horses?
Cough, dyspnoea, tachypnoea.
What is the treatment for feline conjunctivitis caused by Chlamydia felis?
Doxycycline and supportive care.
6-8 weeks
active against mycoplasma, bordetella, chlamydia
What are the common causes of epistaxis in horses?
EIPH, aspergillus fumigatus
What are the common diagnostic tools for respiratory diseases?
Blood tests, radiography, and bronchoalveolar lavage (BAL).
What are the signs of severe asthma in horses?
Cough, exercise intolerance, and respiratory distress.
What are the common clinical signs of bacterial pneumonia in foals?
Cough, fever, and increased respiratory effort.
What is the primary treatment for bacterial bronchopneumonia in dogs?
Antibiotics and supportive care.

What is the primary cause of haemorrhagic pneumonia in dogs?
It is caused by a high mortality variant of Canine Influenza virus, often resulting in severe illness.

What are the common clinical signs of EIV in horses?
Serous bilateral nasal discharge, enlarged submandibular lymph nodes, and poor performance.
What is the incubation period for EIV?
1-3 days.
What is the most common strain of equine influenza virus?
H3N8.
What is the recommended supportive care for horses infected with EIV?
NSAIDs such as flunixin or phenylbutazone, along with rest.
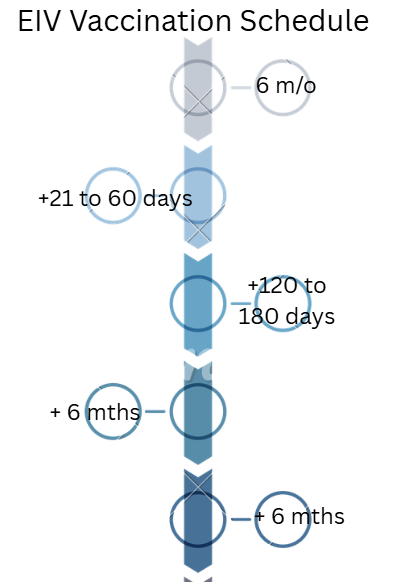
What is the vaccination schedule for horses against EIV?
Start at 6 months, with a second vaccine 21-60 days after the first, a third 120-180 days after the second, then every 6 months.
What is the prognosis for dogs infected with EIV?
Poor prognosis, high mortality rates.
What is the role of serology in diagnosing EIV?
Paired samples taken 10-14 days apart can help confirm infection.
What is the significance of EHV-1 and EHV-4 in horses?
They are the second and third most common causes of respiratory disease in horses.
What are the clinical signs of EHV-1 infection in non-pregnant horses?
Minimal signs, often subclinical.
How is EHV-1 transmitted?
Via respiratory secretions, foetus/placenta, and fomites.
What is the incubation period for EHV-1?
3-7 days.
What are the potential complications of EHV-1 in pregnant mares?
Abortion and chorioretinopathy.
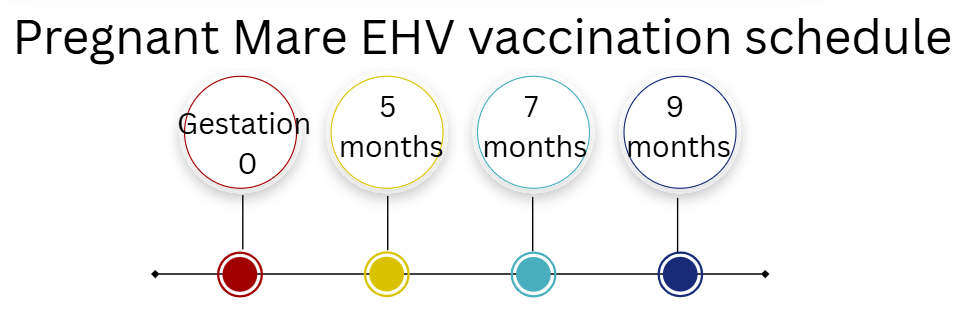
What is the recommended vaccination protocol for EHV-1 in pregnant mares?
Inactivated vaccine at 5, 7, and 9 months of gestation.
EVA- clinical pathology & transmission?
EVA (Equine Viral Arteritis) can cause necrotizing arteritis and is transmitted through contact with aborted foetuses.
What are the clinical signs of EVA?
Periorbital edema, distal limb edema, and possible abortion.
What is the incubation period for EVA?
3-14 days.
What is the treatment for strangles in horses?
Supportive care, drainage of abscesses, and antibiotics if necessary.
What is the causative agent of strangles?
Streptococcus equi equi.
What are the clinical signs of strangles?
Nasal discharge, lymphadenopathy, and abscess formation.
What is the vaccination available for strangles?
Strangvac.
What is the significance of Strep equi zooepidemicus in dogs?
It can cause severe respiratory infections and is not a commensal organism.
What is the treatment for severe infections caused by Strep equi zooepidemicus in dogs?
Fluoroquinolone and penicillin, along with IV clindamycin.
What are the signs of equine rhinitis virus infection?
Subclinical or mild upper/lower respiratory tract signs.
What is the incubation period for equine rhinitis virus?
3-14 days.
What is the recommended isolation period for horses infected with equine rhinitis virus?
3-4 weeks.
What is the importance of monitoring for secondary infections in equine respiratory diseases?
Secondary infections can complicate the clinical picture and worsen outcomes.