CARD 112 Lecture 20: Urine Formation
1/203
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
204 Terms
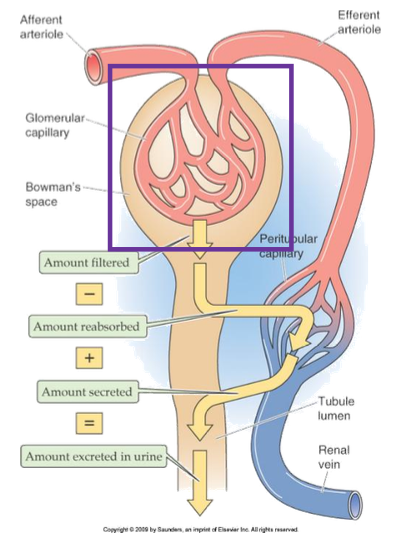
What are the four basic renal processes?
Filtration, reabsorption, secretion, excretion
Where does filtration occur?
Glomerular capillaries into Bowman’s space
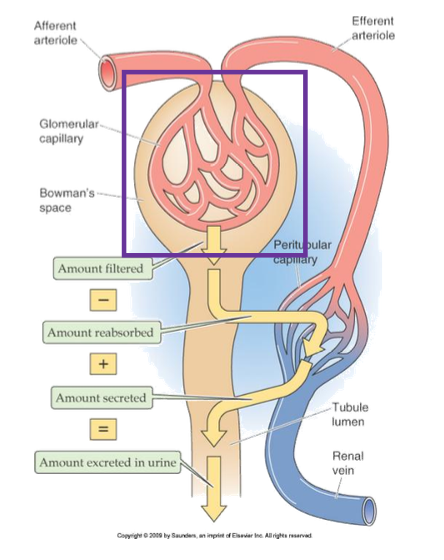
Where does reabsorption occur?
From tubule lumen into peritubular capillaries
Where does secretion occur?
From peritubular capillaries into tubule lumen
What is excretion?
Elimination of substances from the body via urine
What determines the amount excreted?
Filtration – reabsorption + secretion
What vessel brings blood to the glomerulus?
Afferent arteriole
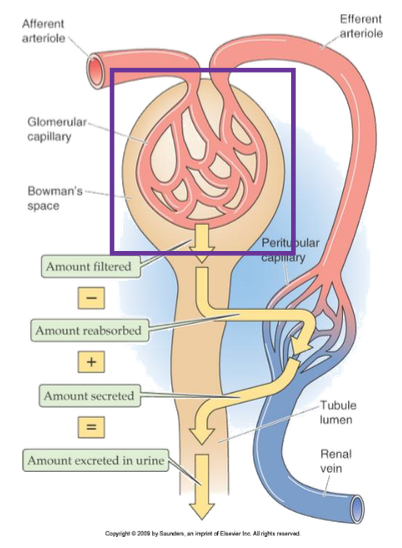
What vessel drains blood from the glomerulus?
Efferent arteriole
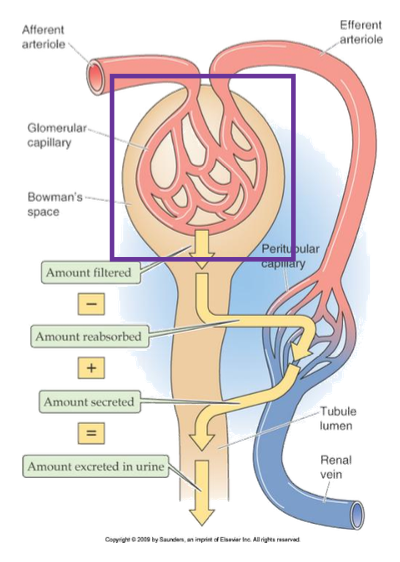
What structure receives filtrate first?
Bowman’s space
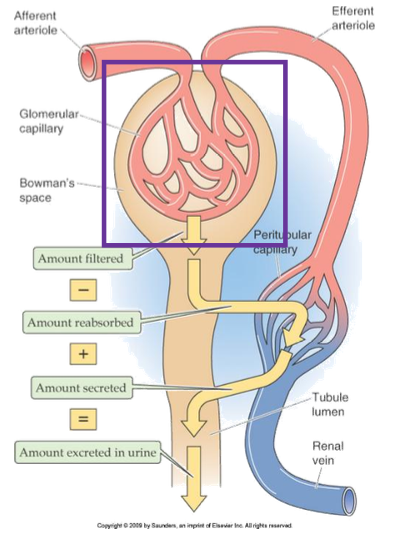
What structure receives reabsorbed substances?
Peritubular capillaries
T/F: Secretion moves substances from the tubule into the blood.
False: secretion moves substances from blood into the tubule.
T/F: Filtration is a passive process.
True (driven by pressure)
T/F: Excretion equals filtration minus reabsorption plus secretion.
True
T/F: Reabsorption always requires ATP.
False: some reabsorption is passive
Filtration occurs from glomerular capillaries into ______.
Bowman’s space
Reabsorption moves substances from the tubule into ______.
Peritubular capillaries
Secretion moves substances from blood into the ______.
tubule lumen
Excretion is the amount of a substance that leaves the body in ______.
urine
What percentage of cardiac output do the kidneys receive?
21%
How much blood flows to the kidneys per minute?
1 L
What percentage of plasma becomes filtrate?
20%
How much filtrate is produced per day?
180 L/day
How much urine is excreted per day?
1-2 L/day
What forces drive filtration?
Starling forces (pressure gradients)
What happens to the 80% of plasma that is not filtered?
It leaves via the efferent arteriole
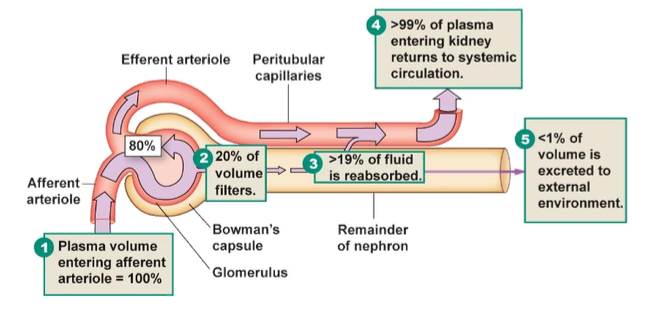
What does high renal blood flow allow?
Precise control of body fluid composition
What is diminished glomerular filtration rate (GFR) a sign of?
Chronic kidney disease (CKD)
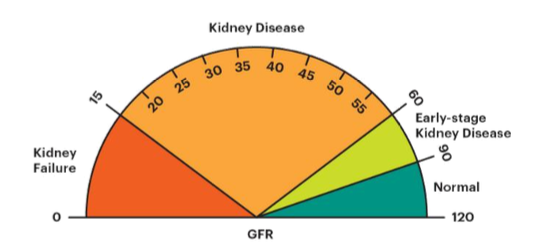
What type of molecules are freely filtered?
Water, ions, glucose, small solutes
T/F: Filtrate is identical to plasma except for proteins.
True
T/F: Only 1% of filtrate is excreted.
True
T/F: Filtration is driven by osmotic gradients only.
False: hydrostatic and oncotic pressures BOTH contribute.
T/F: A decrease in GFR is always harmless.
False: it may indicate chronic kidney disease (CKD)
Filtration is driven by ______ forces.
Starling
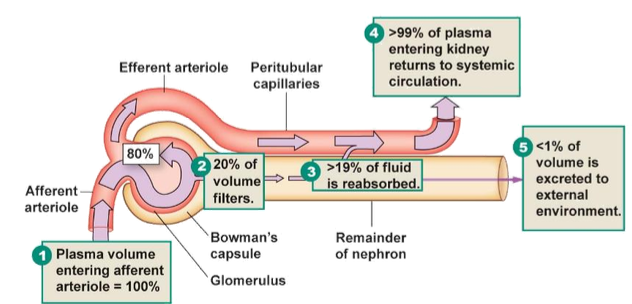
What percentage of plasma is filtered at the glomerulus?
20%
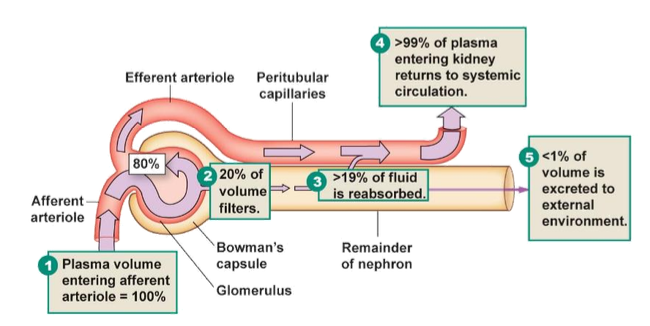
What percentage of filtered fluid is reabsorbed?
99%
What two factors determine GFR?
Filtration coefficient (Kf) and net filtration pressure (NFP)
What determines the filtration coefficient (Kf)?
Surface area and permeability
What determines net filtration pressure (NFP)?
Hydrostatic and colloid osmotic pressures
What happens to glomerular filtration rate (GFR) if surface area decreases?
GFR decreases
What happens to glomerular filtration rate (GFR) if permeability increases?
It increases
What two forces favor filtration in the glomerulus?
Glomerular hydrostatic pressure (PGC) and Bowman’s space oncotic pressure (πBS)
What two forces oppose filtration?
Bowman’s space hydrostatic pressure (PBS) and glomerular oncotic pressure (πGC)
What is the typical glomerular hydrostatic pressure (PGC)?
50 mmHg
What is the typical Bowman’s space hydrostatic pressure (PBS)?
10 mmHg
What is the typical glomerular oncotic pressure (πGC)?
25 mmHg
What is the approximate net filtration pressure (NFP)?
10-15 mmHg
What happens when glomerular hydrostatic pressure (PGC) > glomerular oncotic pressure (πGC)?
Filtration occurs
What happens when glomerular oncotic pressure (πGC) > glomerular hydrostatic pressure (PGC)?
Absorption occurs
What type of pressure draws fluid into capillaries?
Colloid osmotic pressure
What type of pressure pushes fluid out of capillaries?
Hydrostatic pressure
T/F: Bowman’s space normally contains proteins that contribute to oncotic pressure.
False: Bowman’s space oncotic pressure (πBS) is normally ZERO because proteins DO NOT filter.
T/F: Hydrostatic pressure in the glomerulus is higher than in systemic capillaries.
True
T/F: A decrease in πGC increases filtration.
True
T/F: Filtration stops when net filtration pressure (NFP) reaches zero.
True
Net filtration pressure is typically ______ to ______ mmHg.
10’ 15
What is the formula for net filtration pressure (NFP)?
(PGC + πBS) – (PBS + πGC)
(glomerular hydrostatic pressure + Bowman’s space oncotic pressure) – (Bowman’s space hydrostatic pressure + glomerular oncotic pressure)
What is the normal value of Bowman’s (πBS)?
0 mmHg
What happens to net filtration pressure (NFP) along the glomerular capillary?
It decreases as glomerular oncotic pressure (πGC) increases
What causes glomerular oncotic pressure (πGC) to increase along the capillary?
Protein concentration rises as fluid is filtered
What happens when filtration equilibrium is reached?
Filtration stops
What happens to glomerular hydrostatic pressure (PGC) along the glomerular capillary?
It remains relatively constant
What happens to Bowman’s space hydrostatic pressure (PBS) during obstruction?
PBS increases, reducing net filtration rate (NFP)
What happens to glomerular filtration rate (GFR) if glomerular oncotic pressure (πGC) increases?
GFR decreases
T/F: glomerular oncotic pressure (πGC) decreases along the glomerular capillary.
False: it increases as fluid is filtered.
T/F: glomerular hydrostatic pressure (PGC) remains high along the entire glomerular capillary.
True
T/F: Increasing Bowman’s space hydrostatic pressure (PBS) increases filtration.
False: it opposes filtration
T/F: Filtration equilibrium occurs when net filtration pressure (NFP) reaches zero.
True
Glomerular oncotic pressure (πGC) increases because proteins become more ______.
concentrated
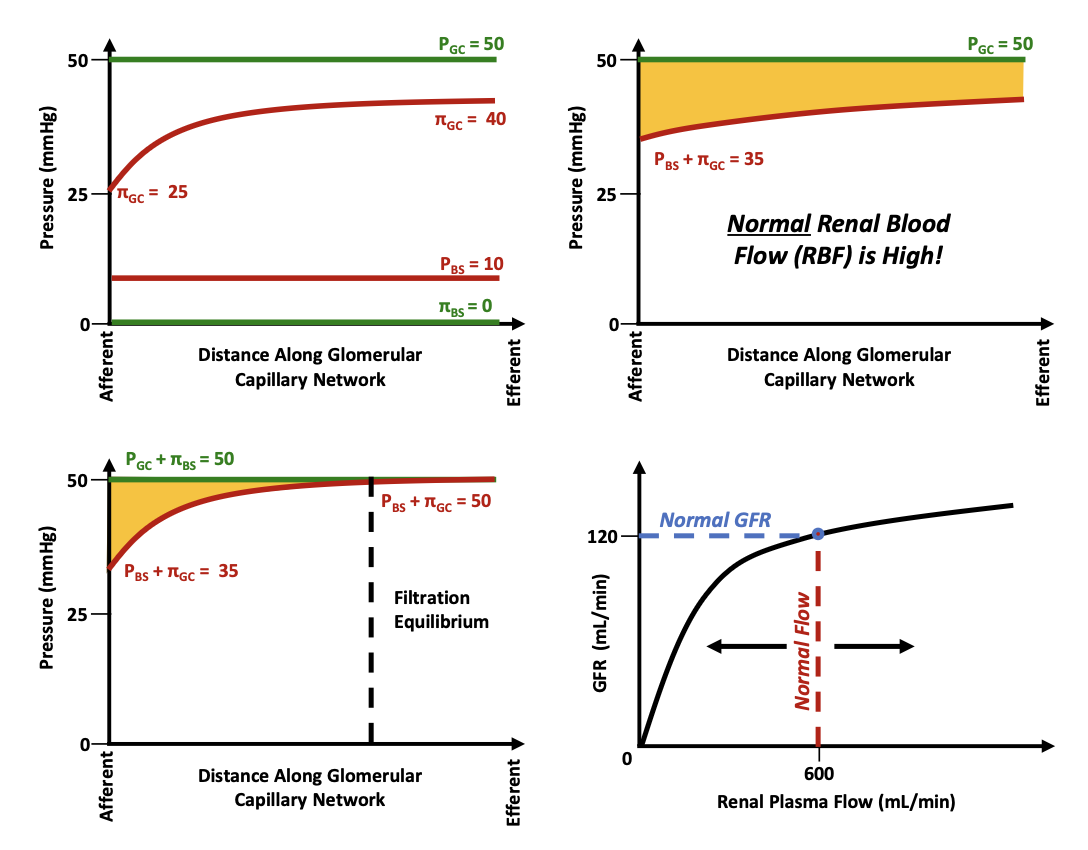
What pressure remains constant along the glomerular capillary?
Glomerular hydrostatic pressure (PGC)
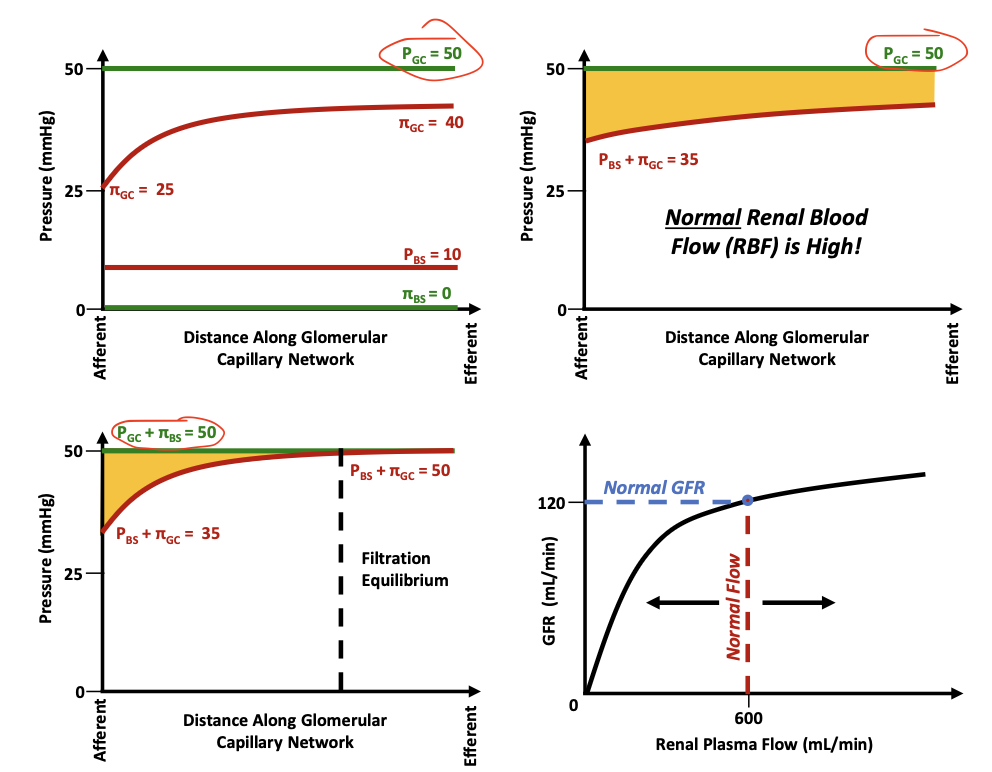
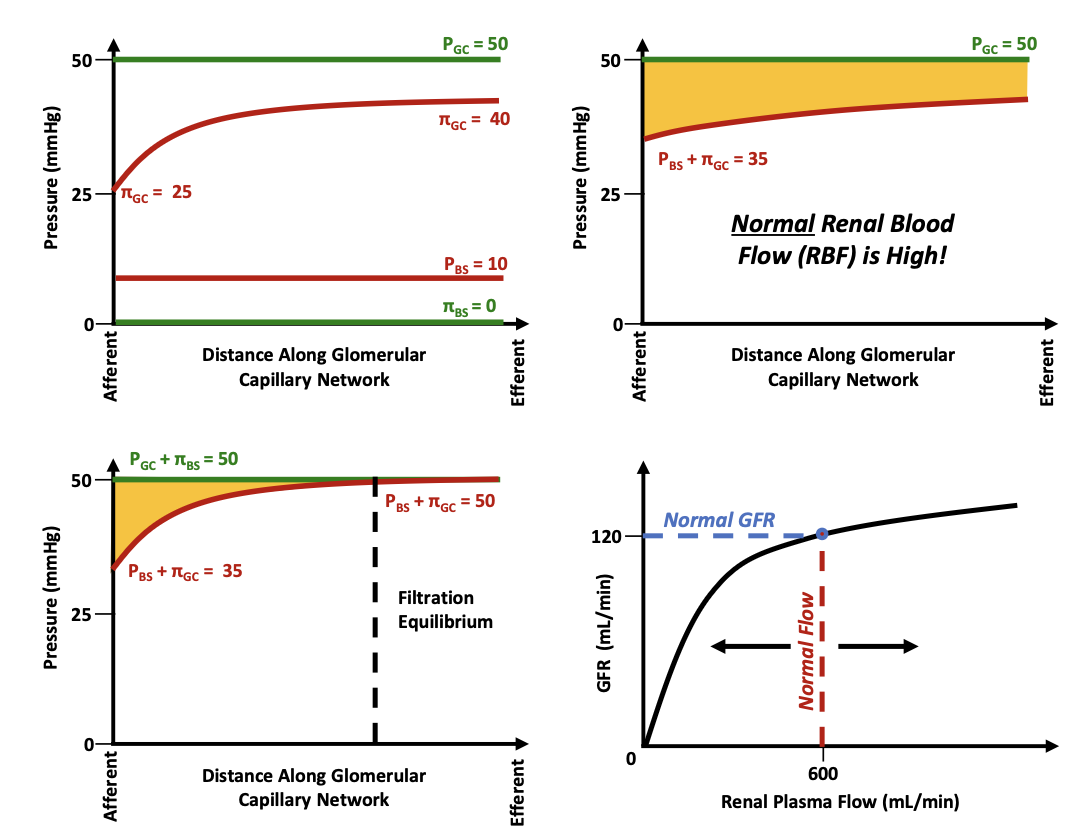
What pressure increases along the capillary?
Glomerular oncotic pressure (πGC)
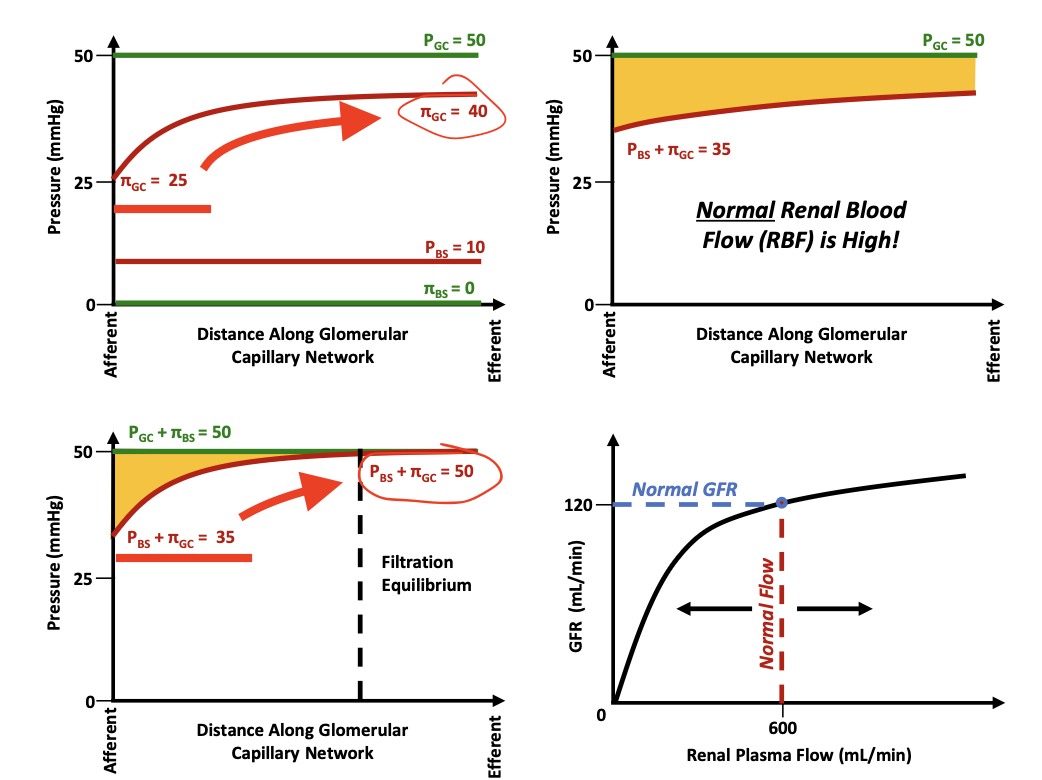
At what point does filtration stop?
Filtration equilibrium
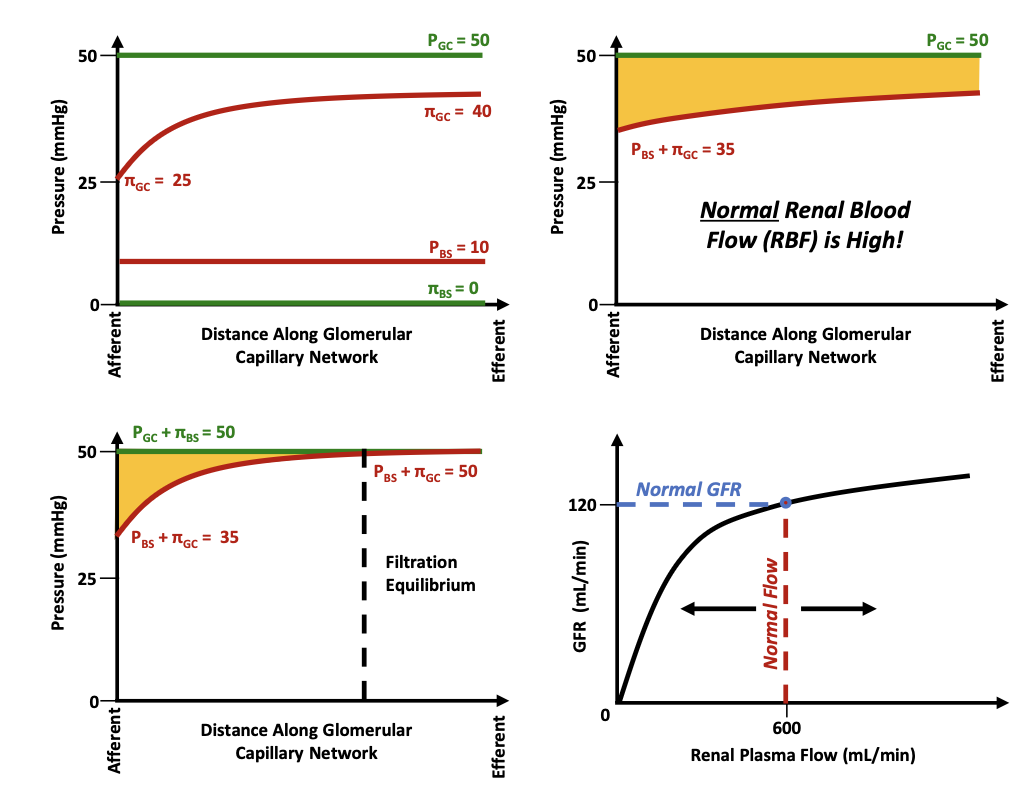
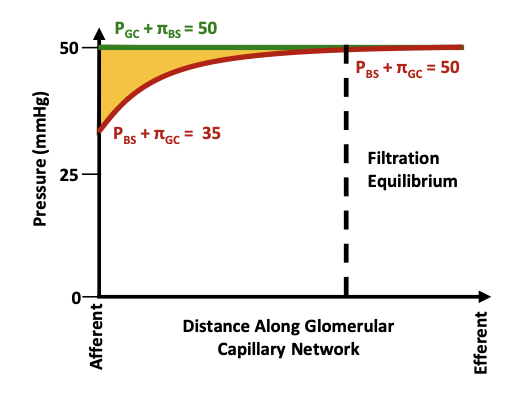
What pressure opposes filtration and rises to ~35 mmHg?
Bowman’s space hydrostatic pressure (PBS) + glomerular oncotic pressure (πGC)
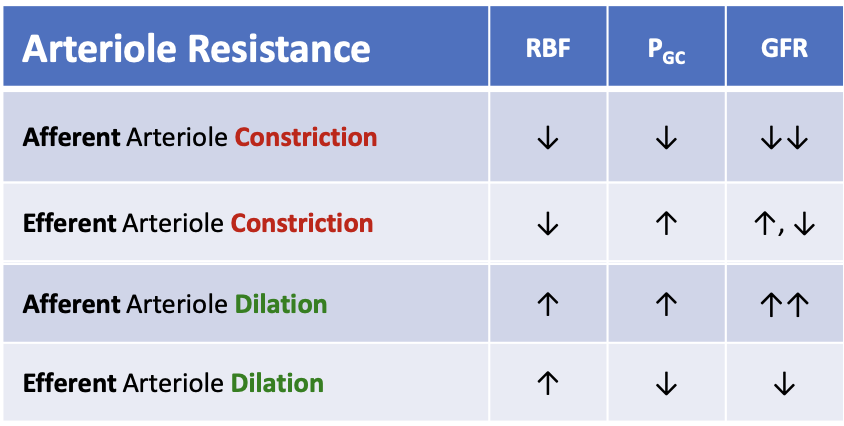
What happens to renal blood flow (RBF) when the afferent arteriole constricts?
RBF decreases
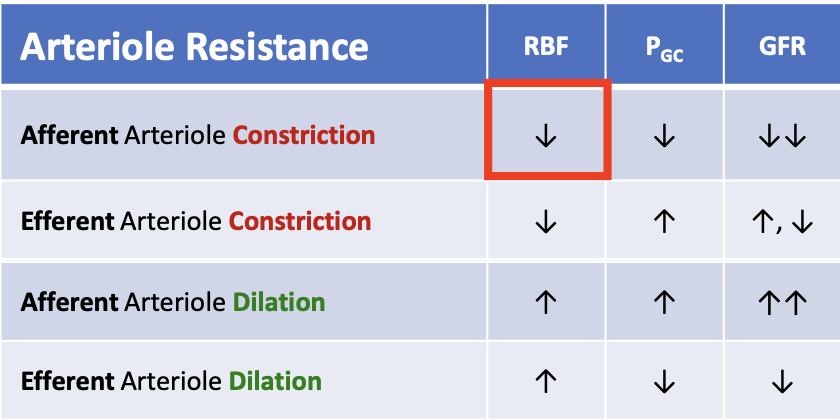
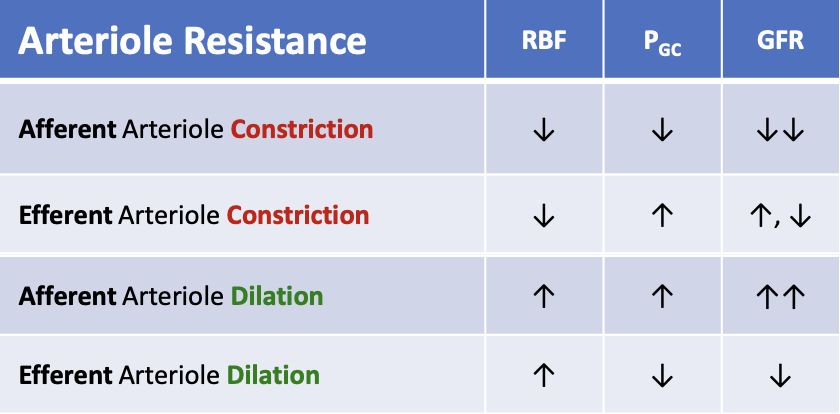
What happens to glomerular hydrostatic pressure (PGC) when the afferent arteriole constricts?
PGC decreases
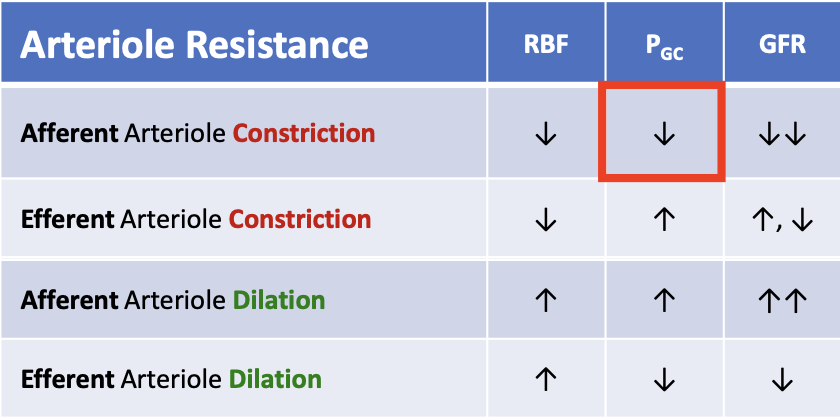
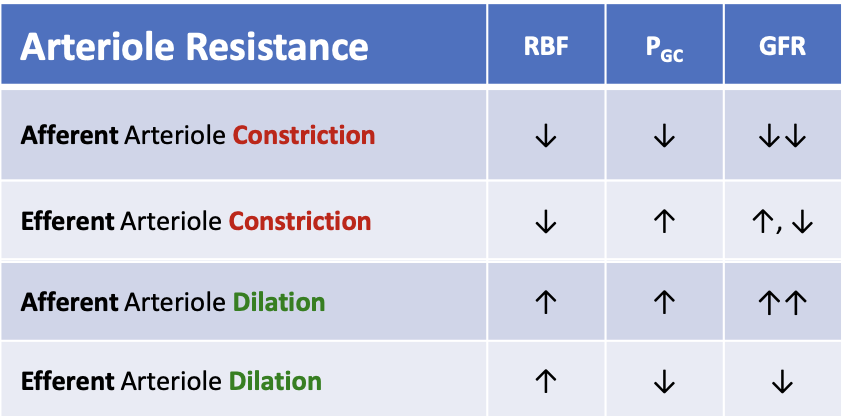
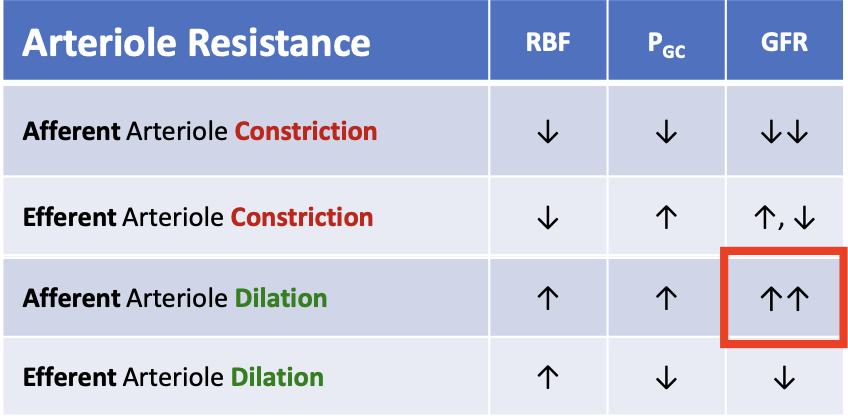
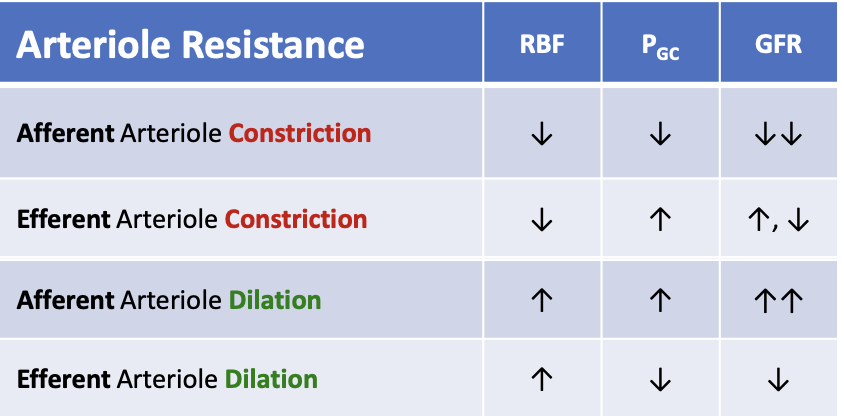
What happens to glomerular filtration rate (GFR) when the afferent arteriole dilates?
GFR increases
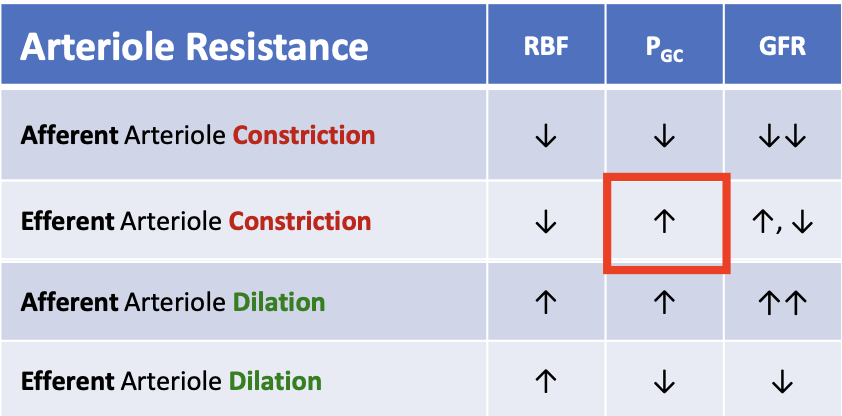
What happens to glomerular hydrostatic pressure (PGC) when the efferent arteriole constricts?
PGC increases
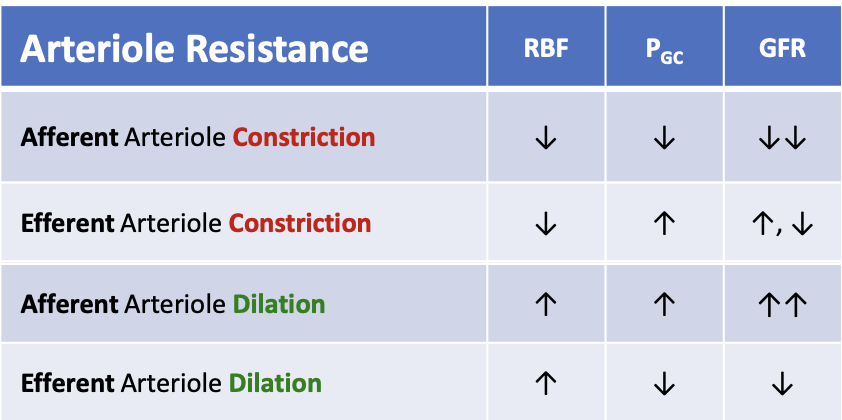
What happens to glomerular filtration rate (GFR) when the efferent arteriole dilates?
GFR decreases
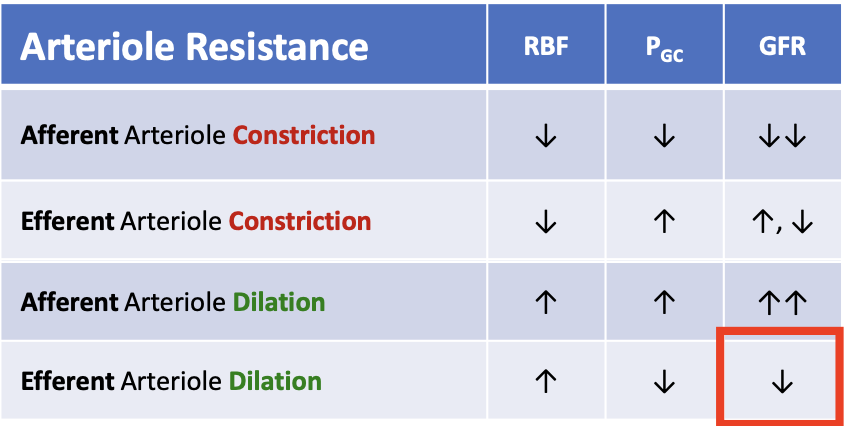
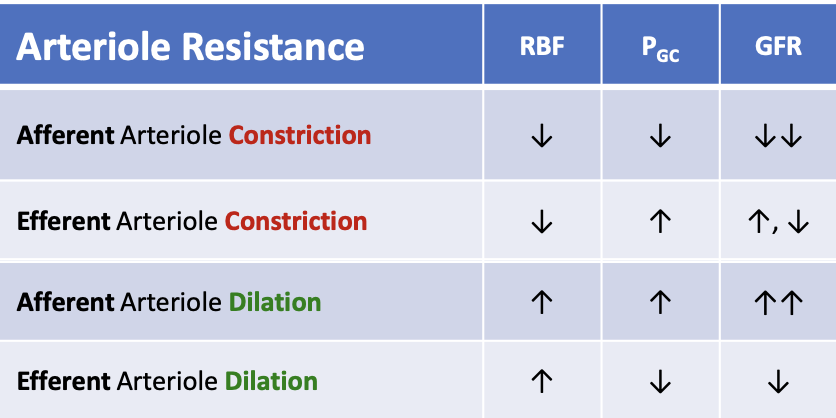
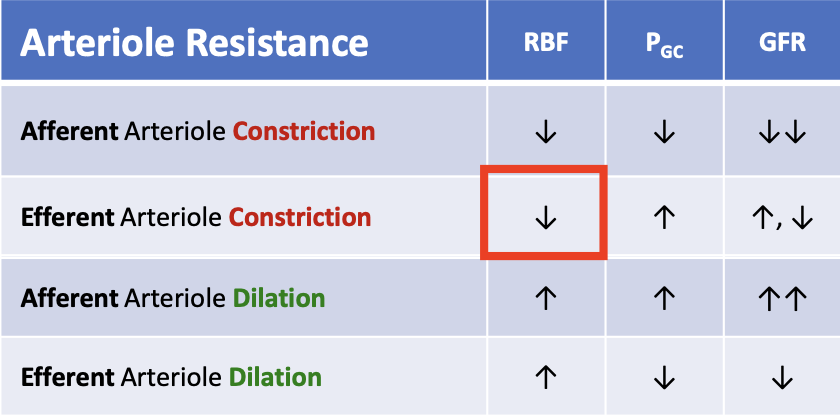
What happens to renal blood flow (RBF) when the efferent arteriole constricts?
RBF decreases
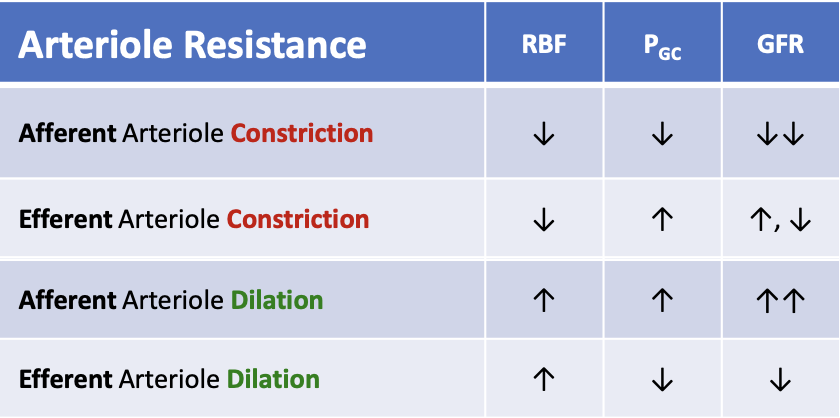
What happens to renal blood flow (RBF) when efferent arteriole dilates?
RBF increases
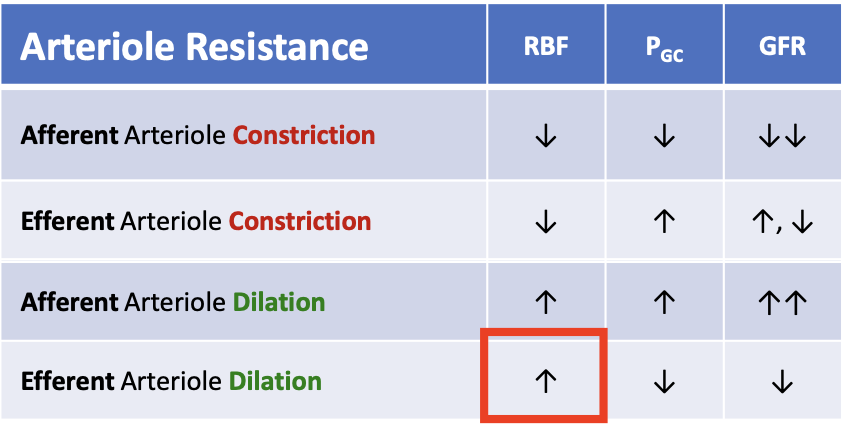
What arteriole change increases both RBF and GFR?
Afferent arteriole dilation
What is the purpose of glomerular filtration rate (GFR) autoregulation?
To maintain a nearly constant GFR despite changes in blood pressure
Between what MAP range is glomerular filtrationr rate (GFR) autoregulated?
80–180 mmHg
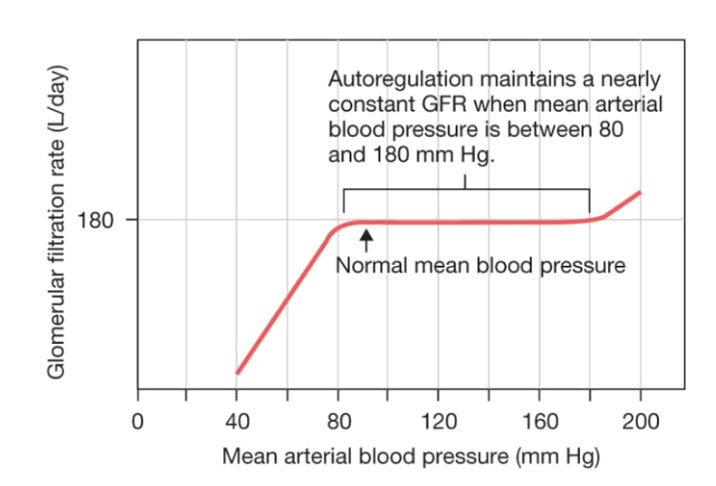
What happens to glomerular filtration rate (GFR) when MAP rises above 180 mmHg?
GFR increases (autoregulation fails)
What happens to glomerular filtration rate (GFR) when MAP falls below 80 mmHg?
GFR decreases sharply
What cells detect stretch in the afferent arteriole?
Juxtaglomerular (JG) granular cells
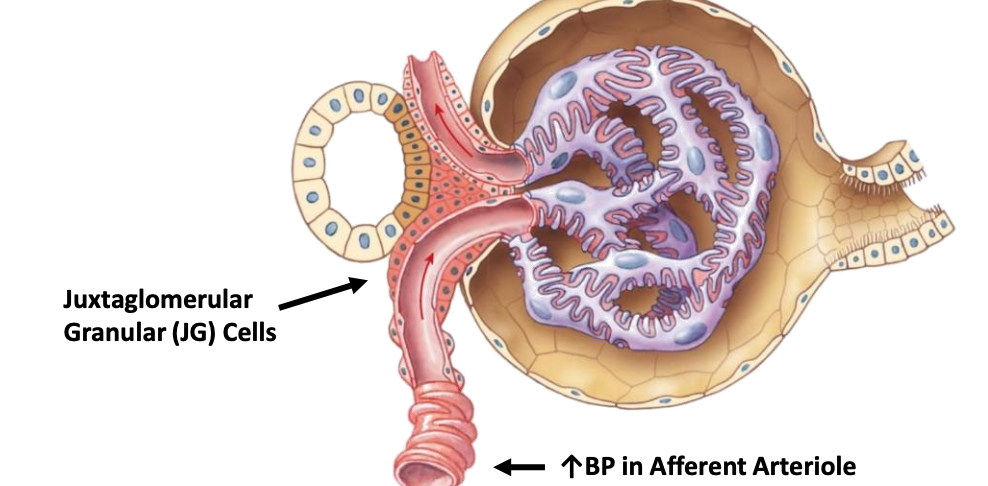
What type of channels open when Juxtaglomerular (JG) cells stretch?
Stretch‑activated cation channels
What ion enters Juxtaglomerular (JG) cells during the myogenic response?
Ca2+
What is the effect of Ca²⁺ entry into Juxtaglomerular (JG) cells?
Vasoconstriction of the afferent arteriole
What happens to renal blood flow (RBF) when the afferent arteriole constricts?
RBF decreases
What happens to glomerular hydrostatic pressure (PGC) when the afferent arteriole constricts?
PGC decreases
T/F: Autoregulation keeps GFR constant between MAP 60–200 mmHg.
False: the range is 80–180 mmHg.
T/F: The myogenic response is intrinsic to vascular smooth muscle.
True
T/F: Stretch of the afferent arteriole causes vasoconstriction
True
T/F: Autoregulation prevents glomerular filtration rate (GFR) from changing during extreme blood pressure changes.
False: autoregulation FAILS outside 80–180 mmHg.
The myogenic response helps stabilize ______.
Glomerular filtration rate (GFR)
What structure senses pressure changes in the kidneys?
Afferent arteriole / juxtaglomerular (JG) cells
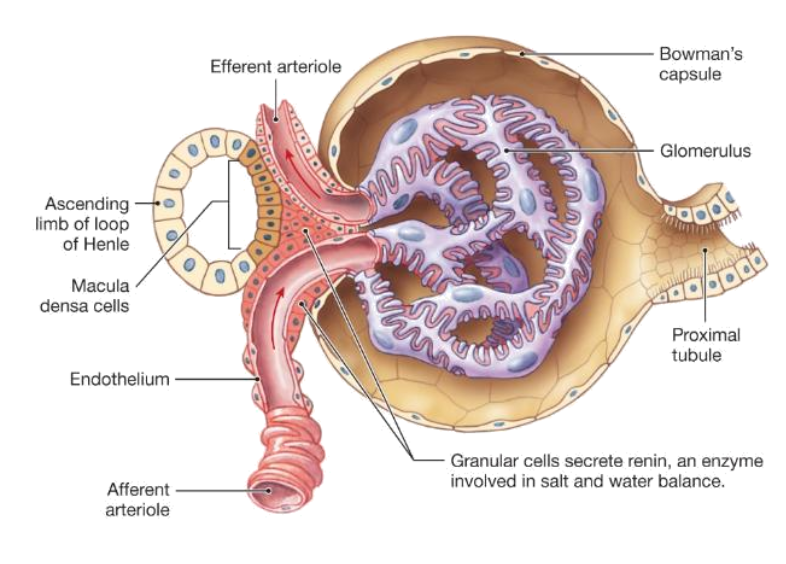
What structure senses NaCl delivery in TGF?
Macula densa
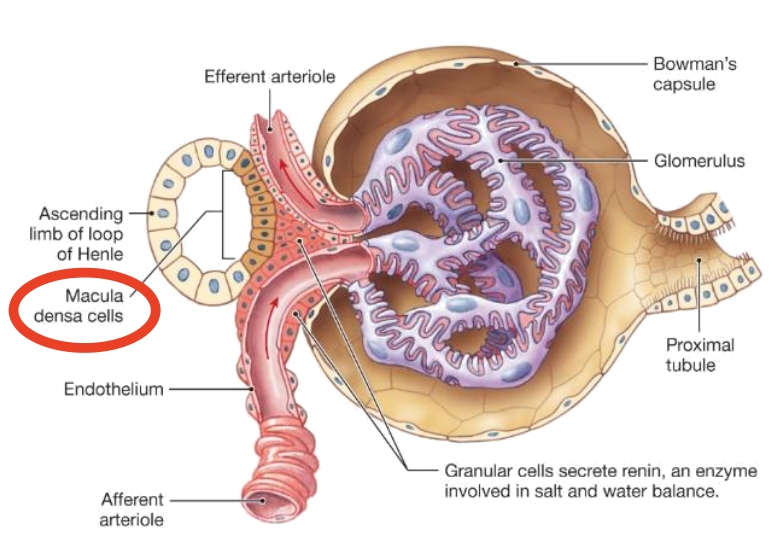
What transporter allows macula densa cells to sense NaCl?
Na⁺/K⁺/Cl⁻ cotransporter (NKCC2)
What happens to macula densa cells when NaCl delivery increases?
They depolarize
What ion enters macula densa cells during depolarization?
Ca²⁺