Urinary System (Pt 1)
1/36
Earn XP
Description and Tags
Ch 24
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
37 Terms
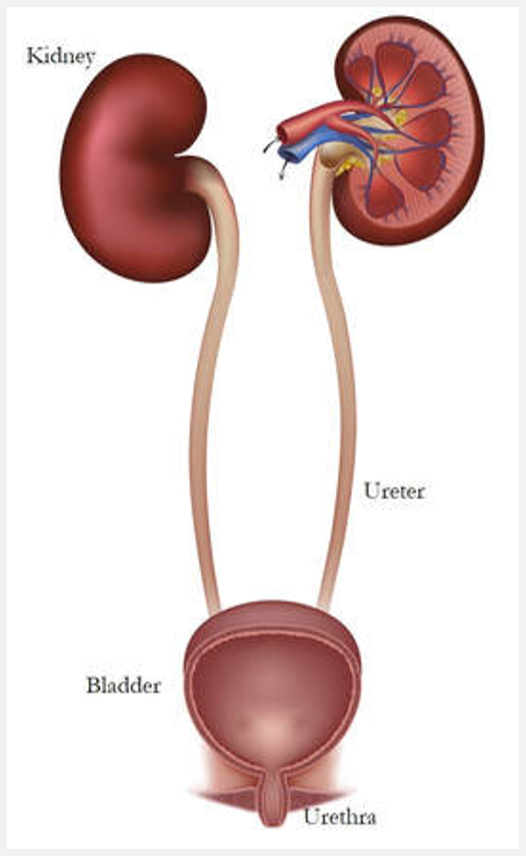
Intro to the urinary system (pt 1)
Components of the urinary system
Kidneys, filter blood
Remove waste products and convert filtrate into urine
Ureters, transport urine
From kidneys to urinary bladder
Bladder, expandable muscular sac
Stores as much as 1 L urine
Urethra, eliminates urine from body
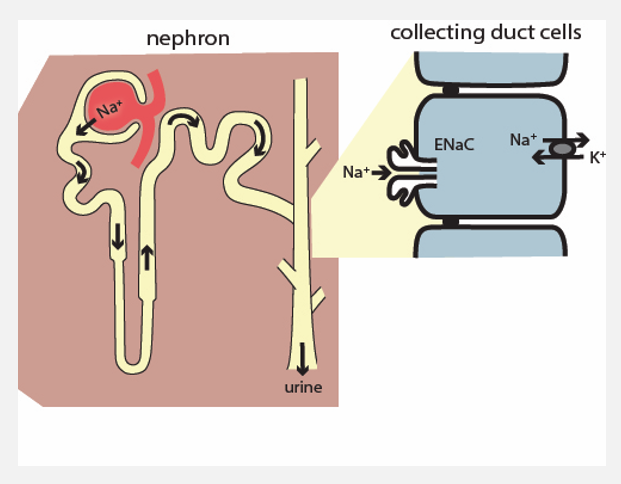
Intro to the urinary system (pt 2)
Processes that occur as filtrate is converted to urine:
Elimination of metabolic wastes
Regulation of ion levels
Ex. Na+, K+, Ca2+
Regulation of acid-base balance
Alters levels of H+ and HCO3-
Regulation of bp
Elimination of biologically active molecules
Hormones, drugs
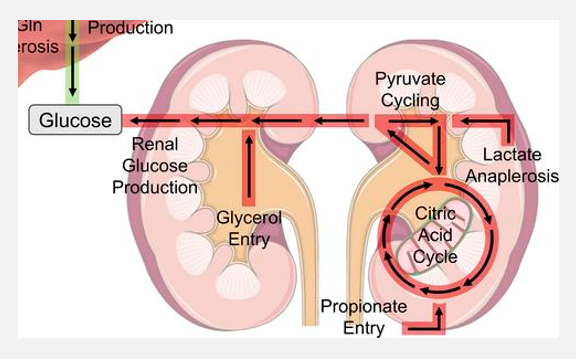
Intro to the urinary system (pt 3)
Other functions of kidney
Formation of calcitriol
Production and release of erythropoietin
Secretes erythropoietin (EPO) in response to low blood oxygen
Stimulates red bond marrow to increase erythrocyte production
Potential to engage in gluconeogenesis
During prolonged fasting or starvation
Occurs in kidney cortex
Produces glucose from noncarbohydrate sources; maintain glucose levels
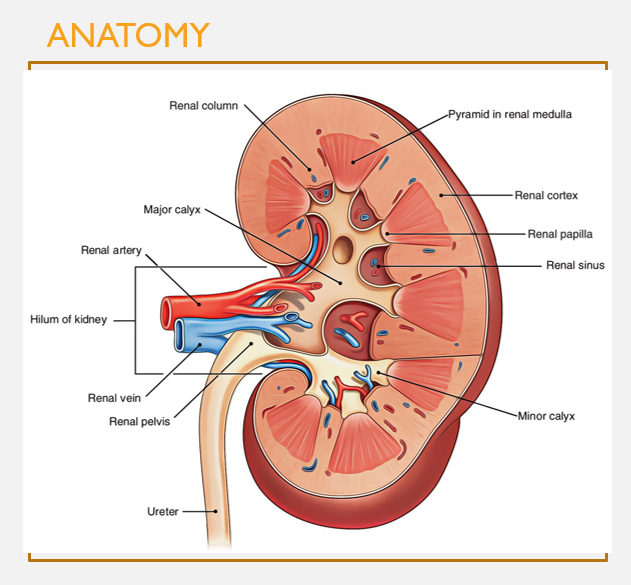
Gross anatomy of the kidneys (pt 1)
FEATURES
Kidneys are 2 symmetrical, bean-shaped organs
Size of hand to second knuckle
Concave medial border, hilum
Where vessels, nerves, ureter connect to kidney
Lateral border convex
Adrenal gland rests on superior aspect of kidney
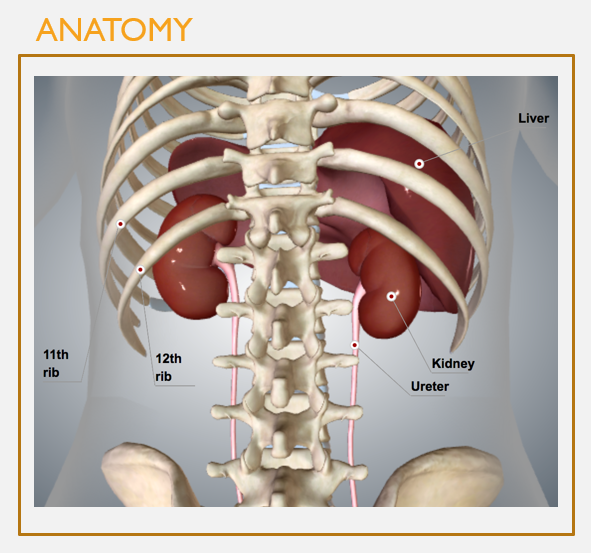
Gross anatomy of the kidneys (pt 2)
FEATURES
Located in the retroperitoneal space (posterior to the peritoneum)
Extend from T12 to L3
Protected posteriorly by the floating ribs
Anchored by various layers of CT
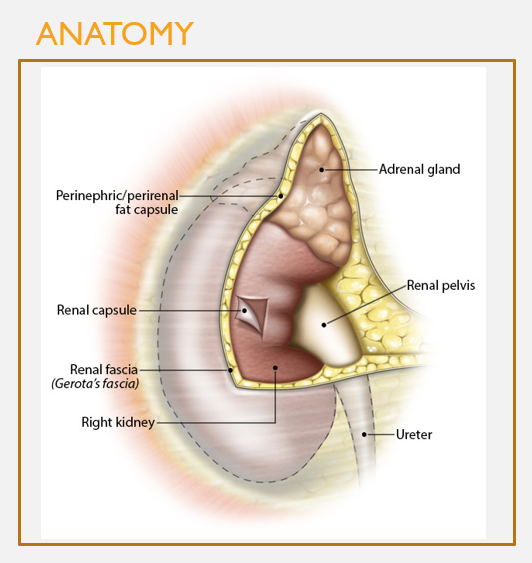
3 connective tissue layers encapsulate the kidneys
FEATURES
Renal fascia:
Most superficial layer
Dense irregular CT
Surrounds both kidneys and adrenal glands
Perinephric/perirenal fat capsule:
Layer of adipose tissue = cushioning effect
Renal capsule:
Directly covers the outer surface of the kidney
Dense irregular CT, helps prevent trauma and pathogen penetration
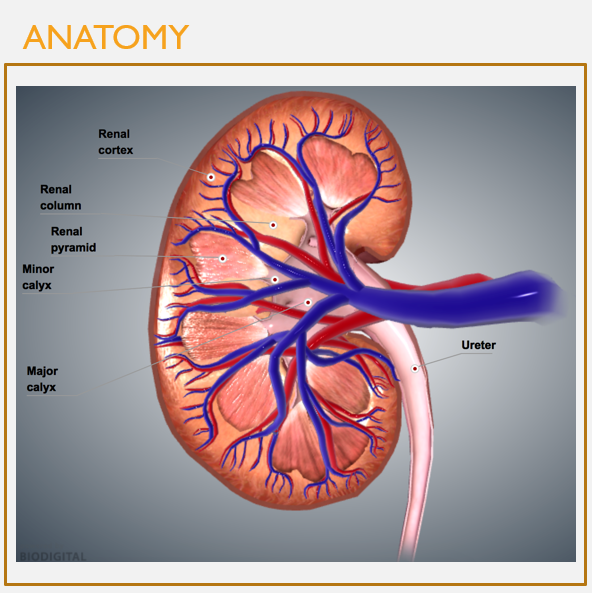
Internal kidney anatomy
FEATURES
Renal cortex: outer regions (granular, reddish-brown)
Renal medulla: inner regions (composed of renal pyramids w/striped appearance)
Renal pyramids: clusters of many nephrons and collecting ducts
Major and minor calyces: collect urine from renal lobes (a pyramid and surrounding cortical tissue)
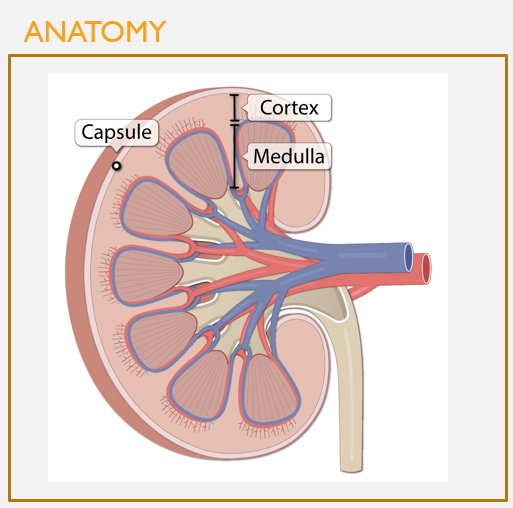
Cortex vs. medulla
FEATURES
The cortex and medulla have diff functions in the kidney
The kidney cortex is the outer portion of the kidney; where filtration of blood occurs
The medulla houses most nephron tubule space, where urine forms and is concentrated
Kidney histology (pt 1)
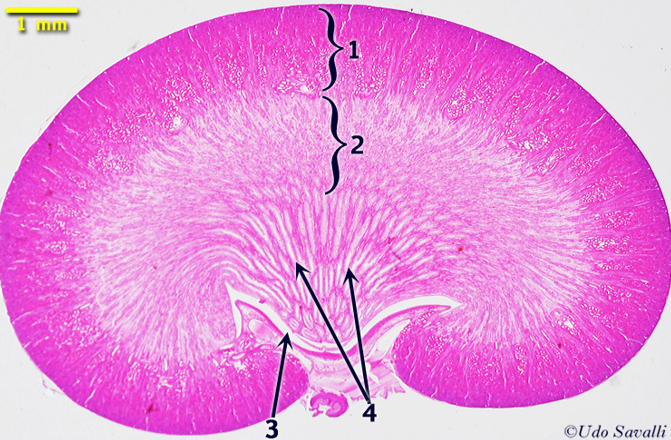
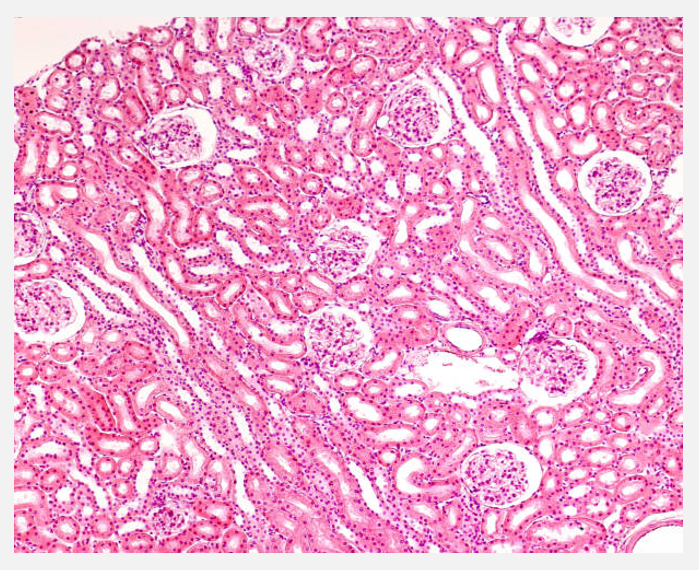
Kidney histology (pt 2)
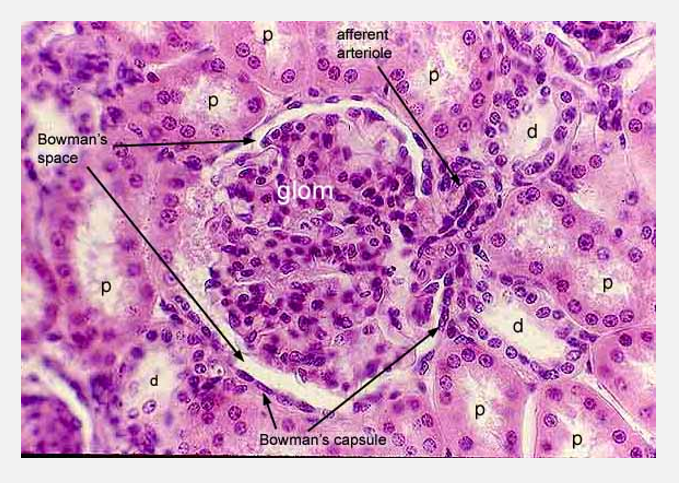
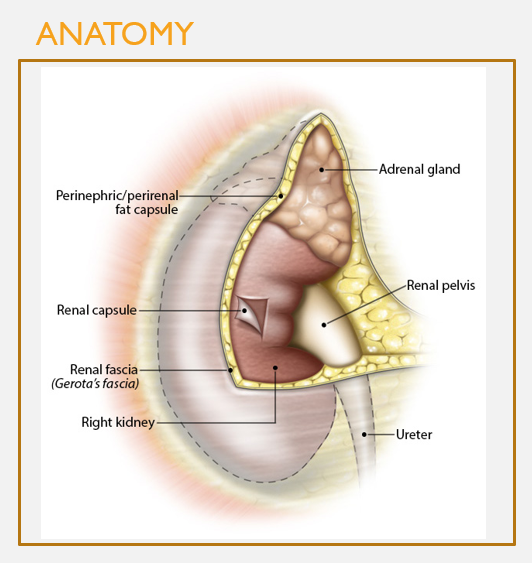
Place the connective tissue layers surrounding the kidney in the correct order, from outside to inside.
A: Renal fascia—>renal capsule—>perirenal fat capsule
B: Renal fascia—>perirenal fat capsule—>renal capsule
C: Renal capsule—>perirenal fat capsule—>renal fascia
D: Perirenal fat capsule—>renal capsule—>renal fascia
B: Renal fascia—>perirenal fat capsule—>renal capsule
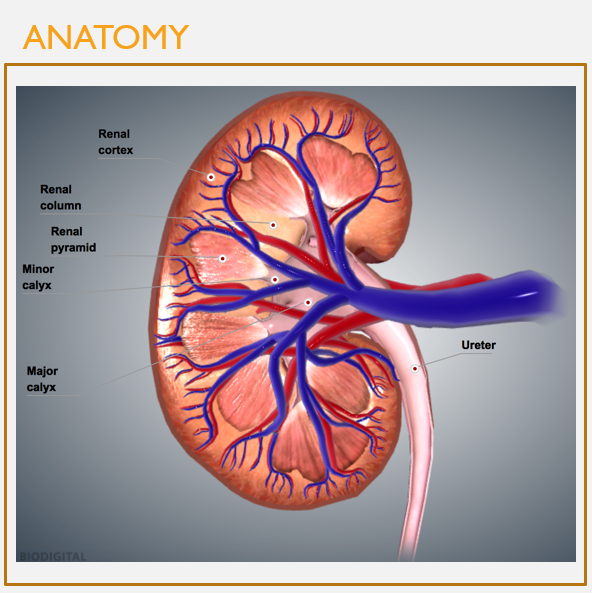
What structures collect urine from renal pyramids?
A: Renal capsules
B: Renal cortex
C: Renal medulla
D: Minor and major calyxes
D: Minor and major calyces
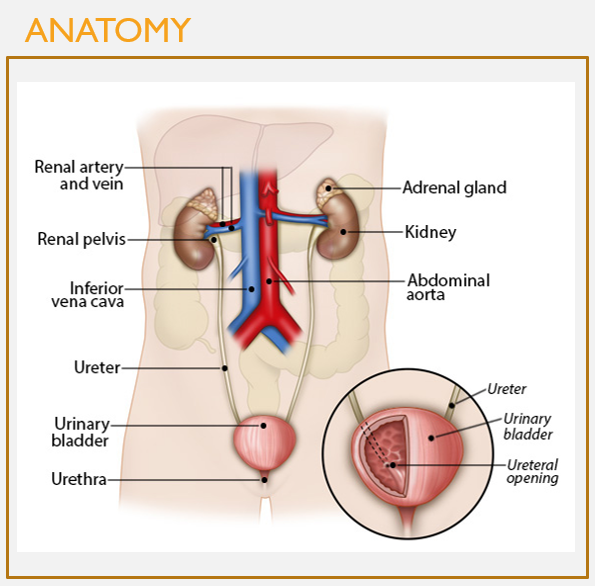
Structures and function of the ureters
FEATURES
Carry urine out of the kidneys to the bladder
Capable of peristalsis
Connect to the bladder at an angle that prevents backflow of urine
Further bladder filling also compresses the distal end of the ureter, further preventing backflow
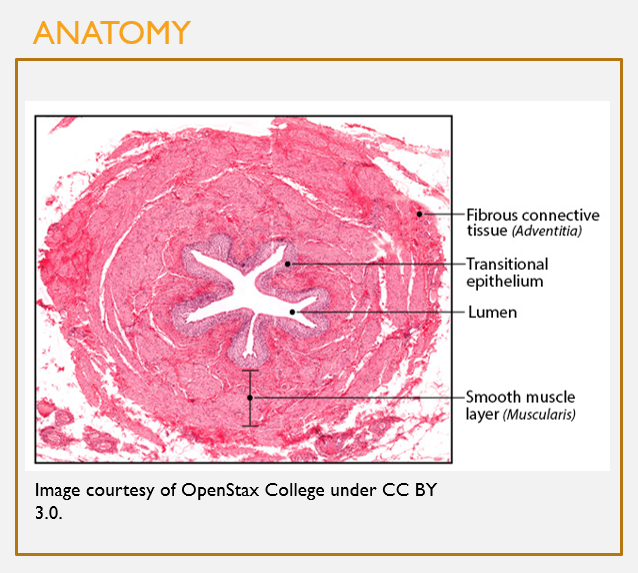
Microscopic anatomy of the ureters
FEATURES
Deepest layer (mucosa):
Transitional epithelium
Readily stretches to accommodate distension from urine filling
Middle layer (muscularis):
Senses distension w/urine filling and triggers reflexive peristalsis
Superficial layer (adventitia):
Fibrous CT
Anchors the ureter in place
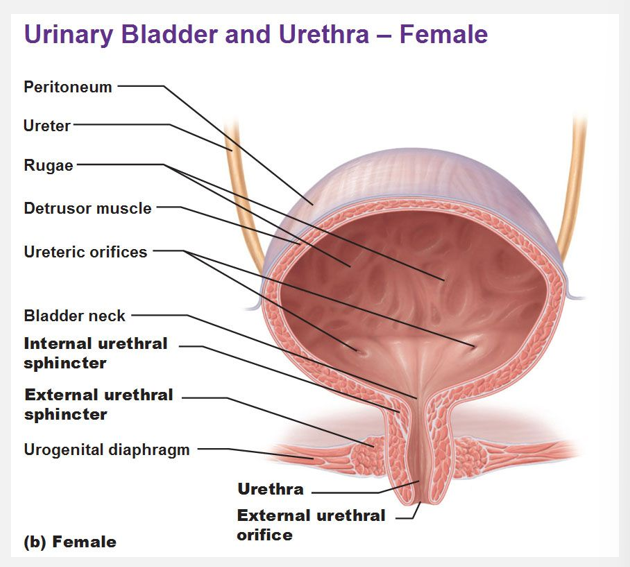
Common features of the bladder in both men and women
Inner mucosa of bladder: transitional epithelium
Middle layer (detrusor): contains muscle that contracts to drive urination
Thick muscle near the urethra forms the internal urethral sphincter
Epithelium transitions to stratified squamous epithelium near the urethra’s opening to the outside
Passes through a ring of skeletal muscle on its way out (external urethral sphincter)
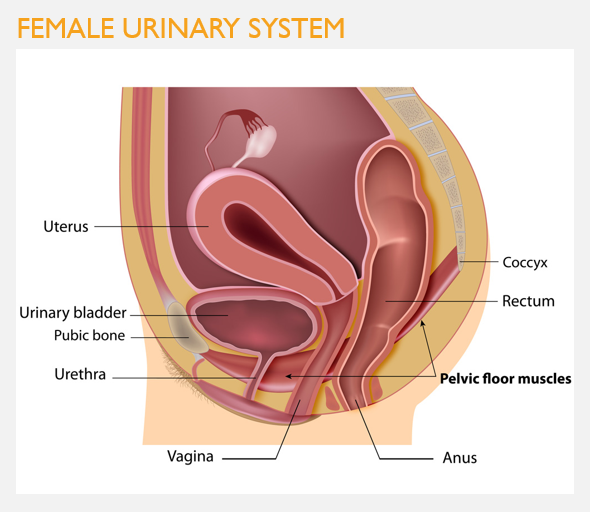
Structure of the urinary system in females
Urethra is only 3-5 cm in length; functions only in transport of urine
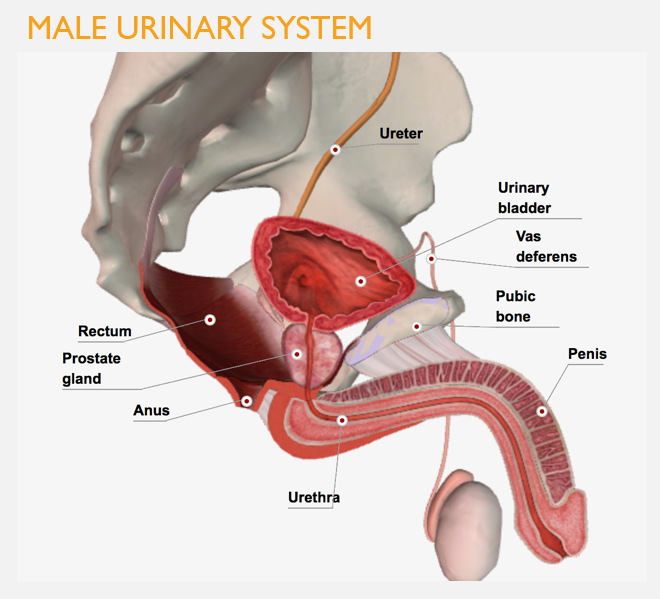
Structure of the urinary system in males
Urethra is longer (20 cm); functions in transport of both urine and semen
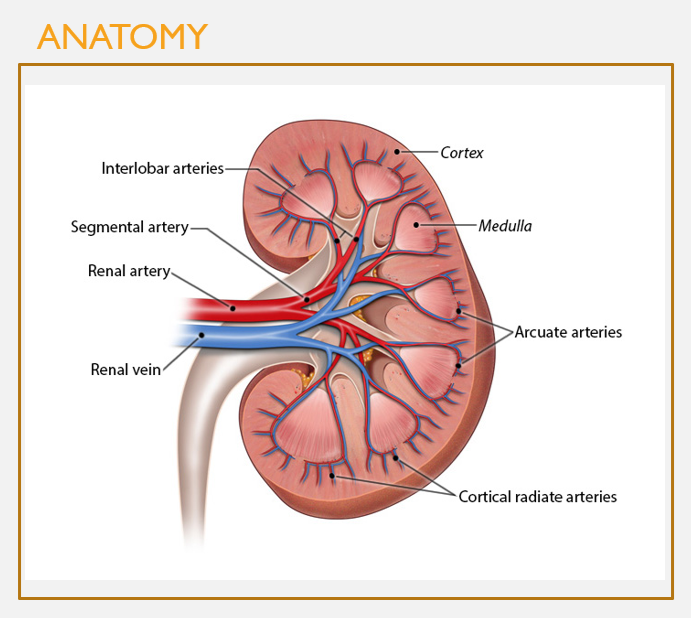
Overall structure of kidney vasculature
FEATURES
Renal artery enters at the hilum
Branches into several segmental arteries, which branch into interlobar arteries
Interlobar arteries travel through the renal columns and branch into arcuate arteries in the cortex
These branch into cortical radiate arteries (interlobular), then microscopic afferent arterioles
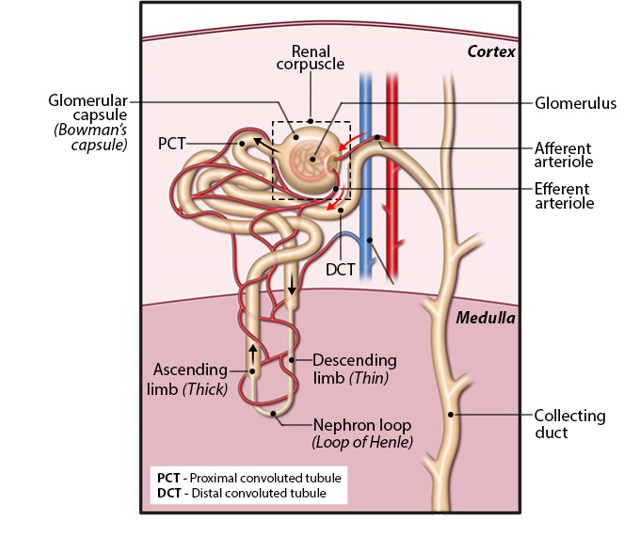
Overall structure of kidney nephrons
Nephron: structural and functional unit of urine formation in the kidney
Afferent arterioles drain into the glomerulus
Filtration occurs when fluid and solutes are forced from the blood in the glomerulus into the space in the surrounding Bowman’s capsule
Blood is drained from the glomerulus by efferent arterioles
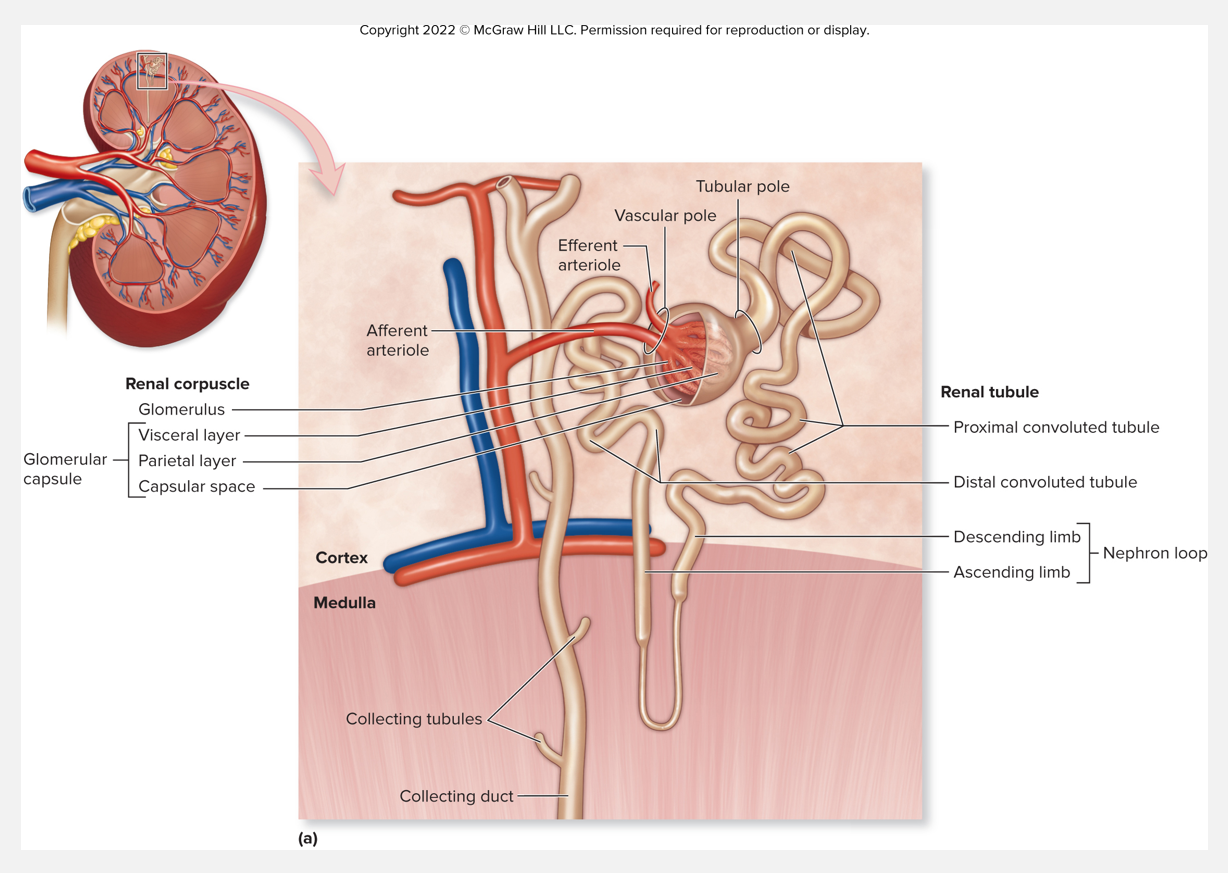
Flow of fluid through the nephron’s tubules
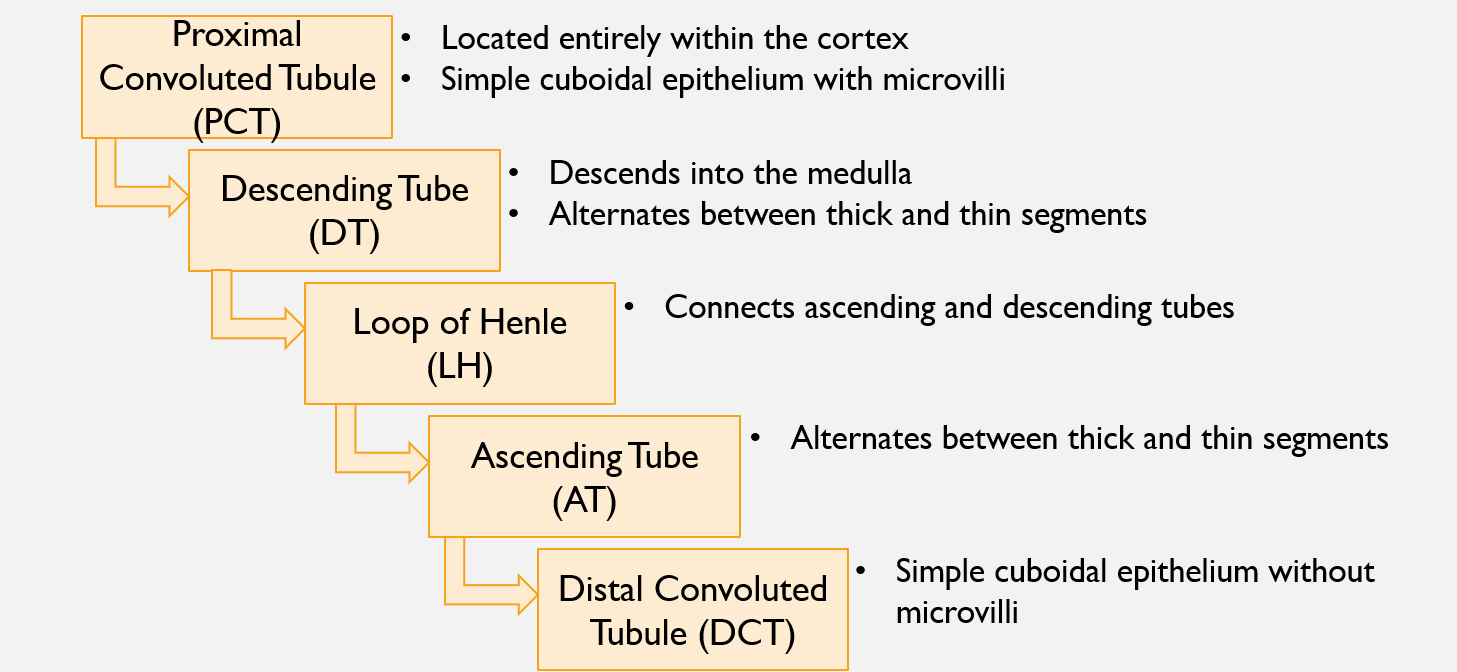
Nephrons (pt 1)
2 types of nephrons: cortical & juxtamedullary
Classified based on 2 factors
Relative position of renal corpuscle in the cortex
Length of nephron loop
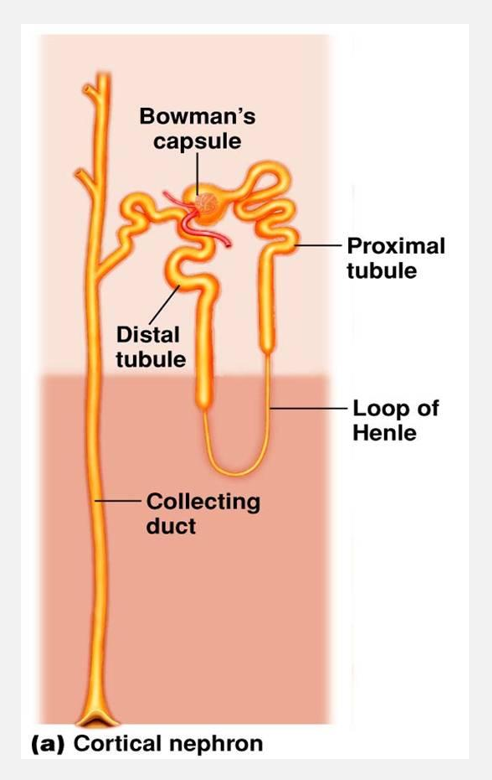
1. Cortical nephrons
Oriented w/renal corpuscles near peripheral cortex
Short nephron loop barely penetrates medulla
85% of nephrons
Main function is for solute reabsorption and excretion
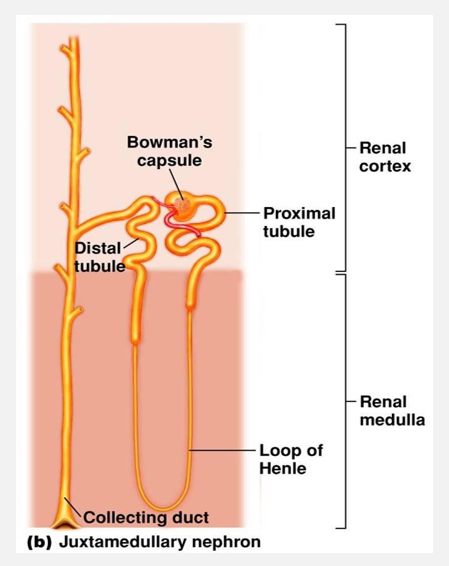
Nephrons (pt 2)
2 types of nephrons (continued)
2. Juxtamedullary nephrons
15% of nephrons
Long nephron loops extend deep into medulla
Main function is to concentrate urine
2 types of nephrons
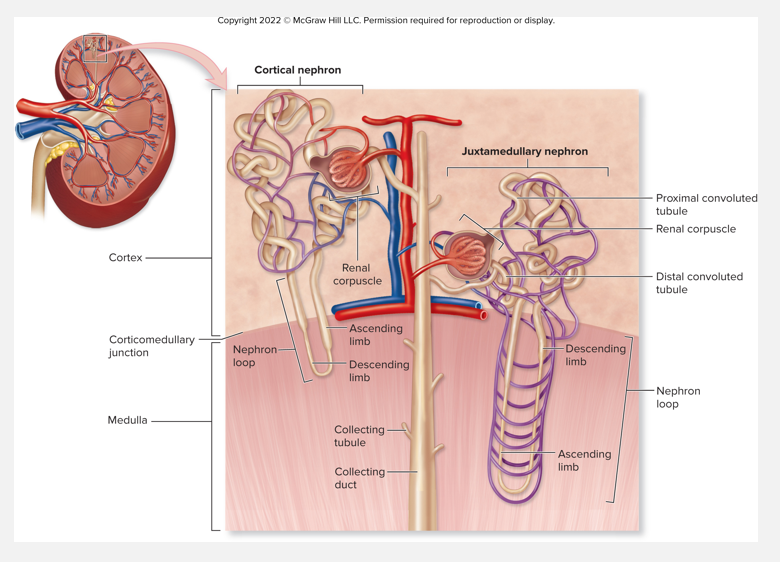
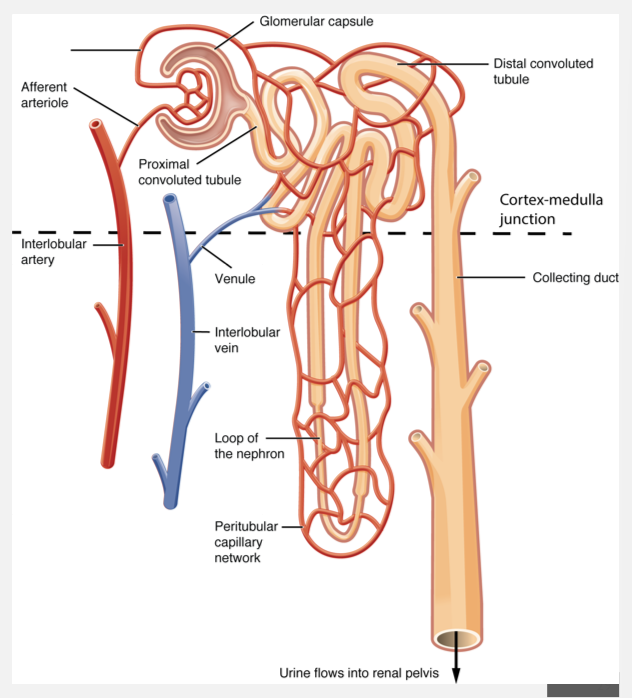
Collecting tubules and collecting ducts
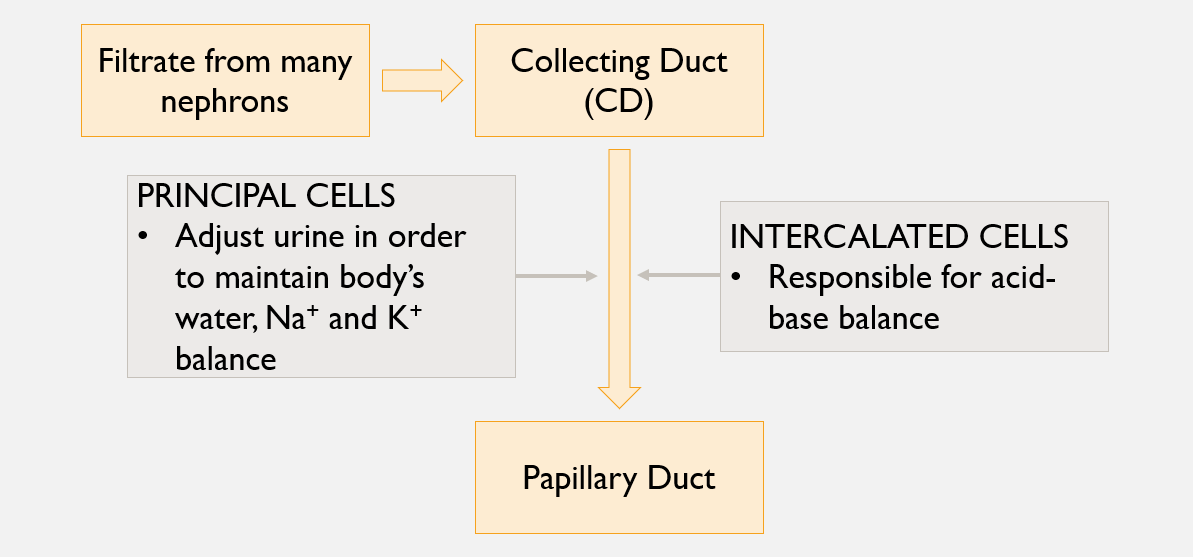
Nephrons drain into a collecting tubule
Multiple collecting tubules empty into larger collecting ducts
Numerous collecting ducts empty into papillary duct w/in renal papilla
Specialized epithelial cells (in CT, CD)
Principal cells
Responsive to hormones aldosterone and antidiuretic hormone (ADH)
Intercalated cells
Specialized epithelial cells
Help regulate urine pH and blood pH
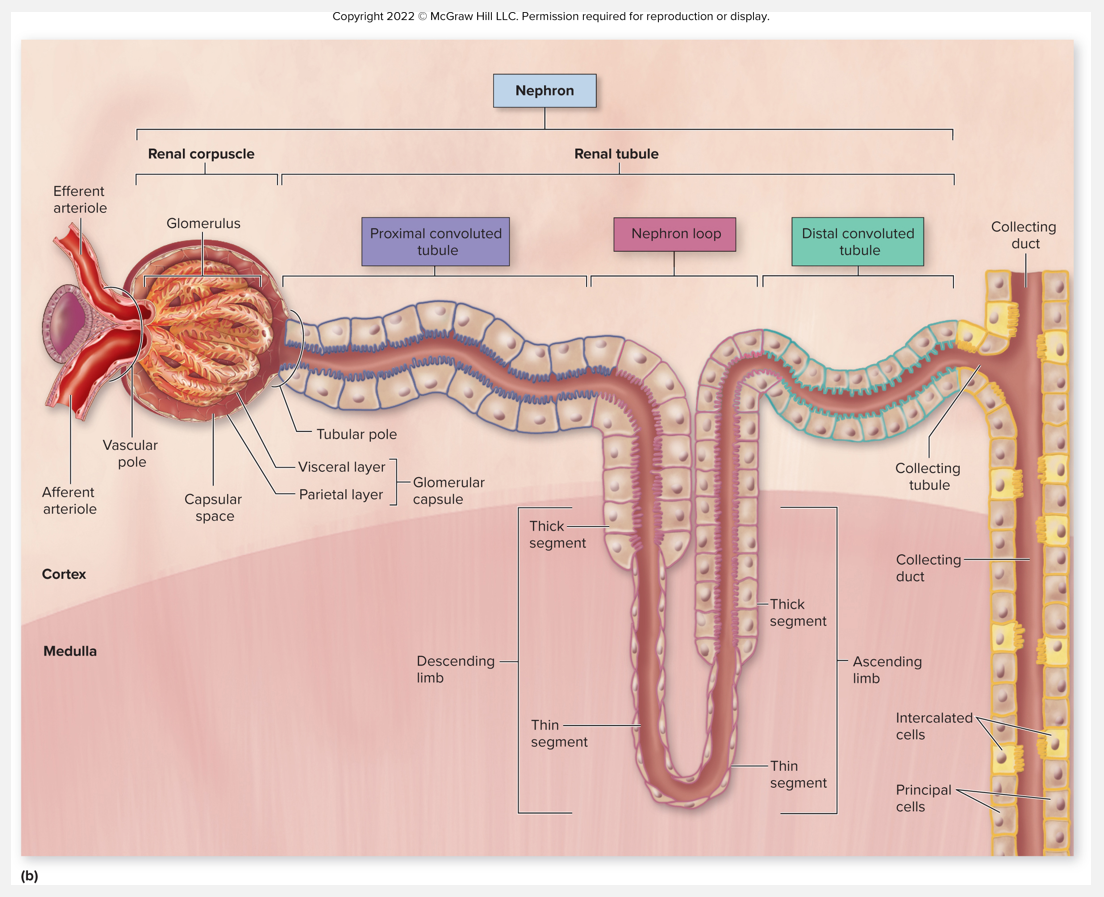
Flow of fluid after filtration through the nephron
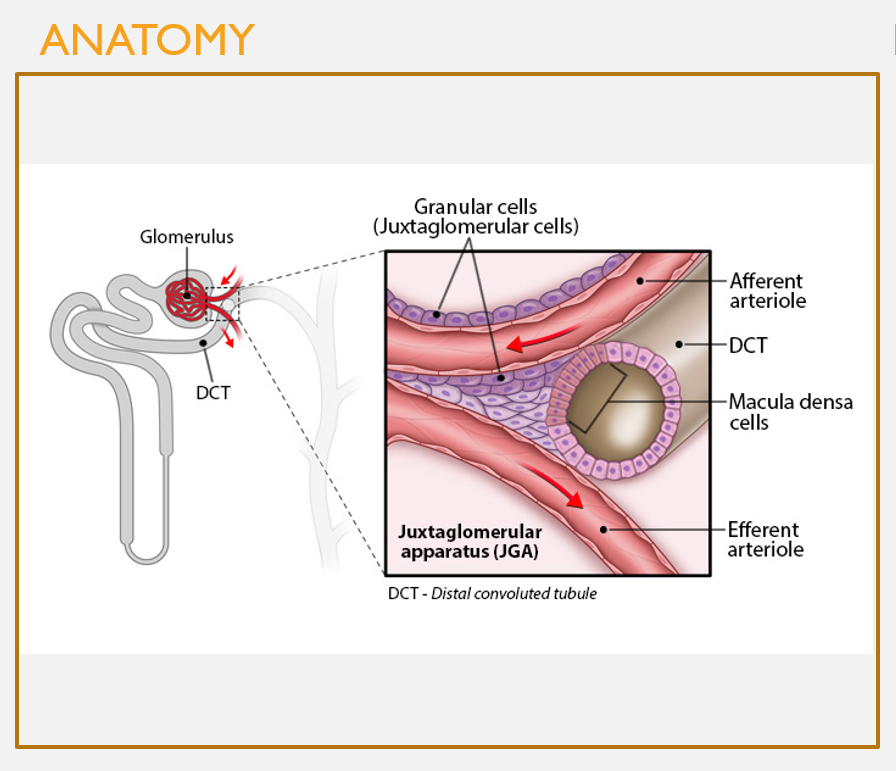
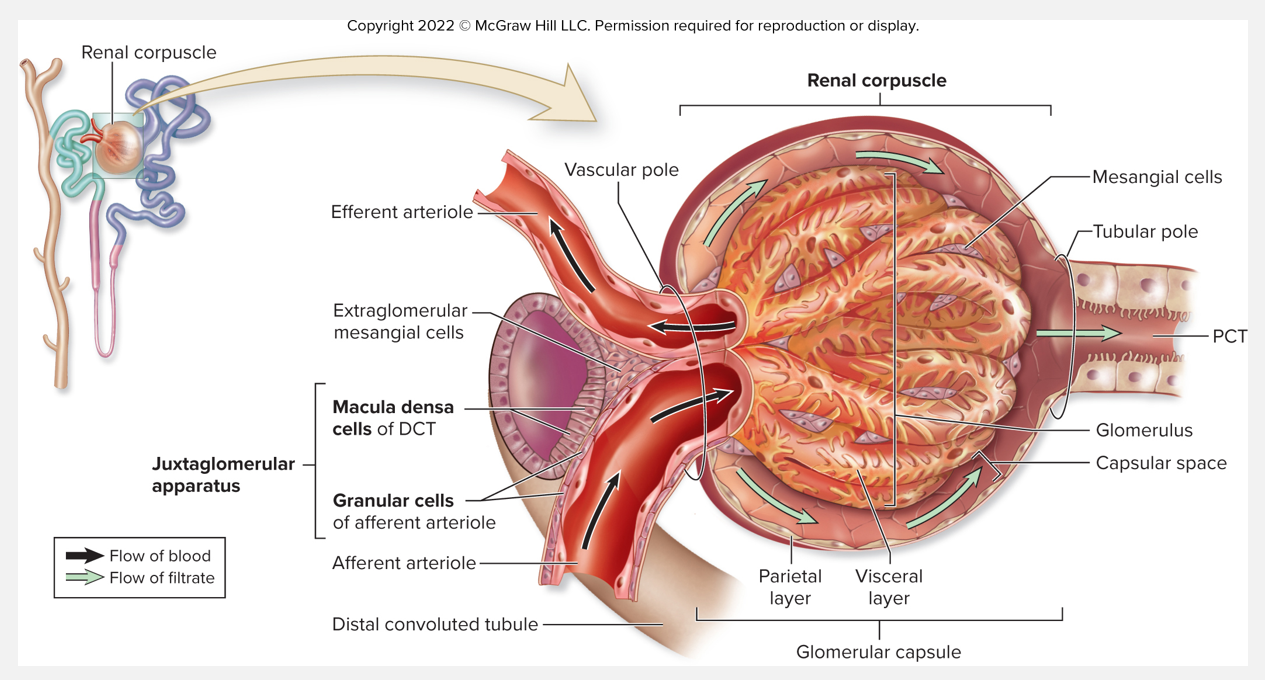
Anatomy of the juxtaglomerular apparatus (JGA)
FEATURES
Occurs when a portion of the DCT comes into contact w/the afferent arteriole
Macula densa cells in DCT: monitor concentrations of Cl- and Na+ in filtrate
Granular (aka juxtaglomerular) cells: respond to changes in bp in the afferent arteriole
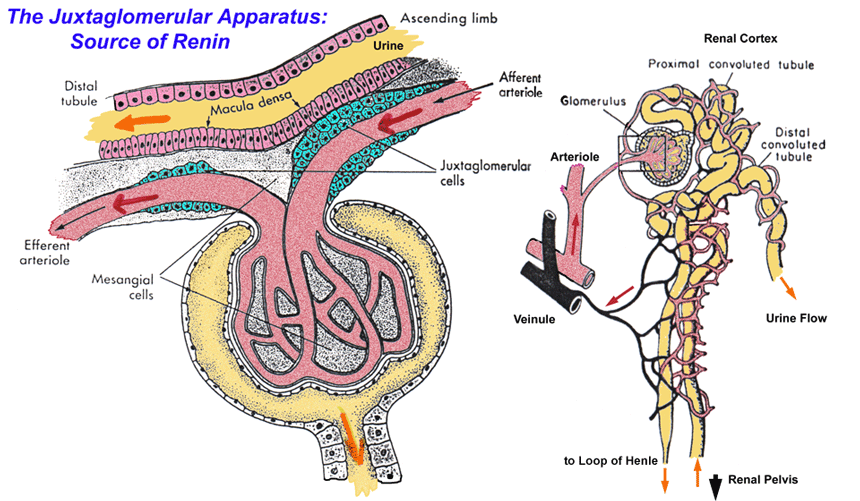
Juxtaglomerular apparatus (pt 1)
Juxtaglomerular (JG) apparatus
Helps regulate blood filtrate formation, systemic bp
JG apparatus components:
Granular cells
Modified smooth muscle cells of afferent arteriole
Located near entrance to renal corpuscle
Contract when stimulated by stretch or sympathetic stimulation
Synthesize, store, and release renin
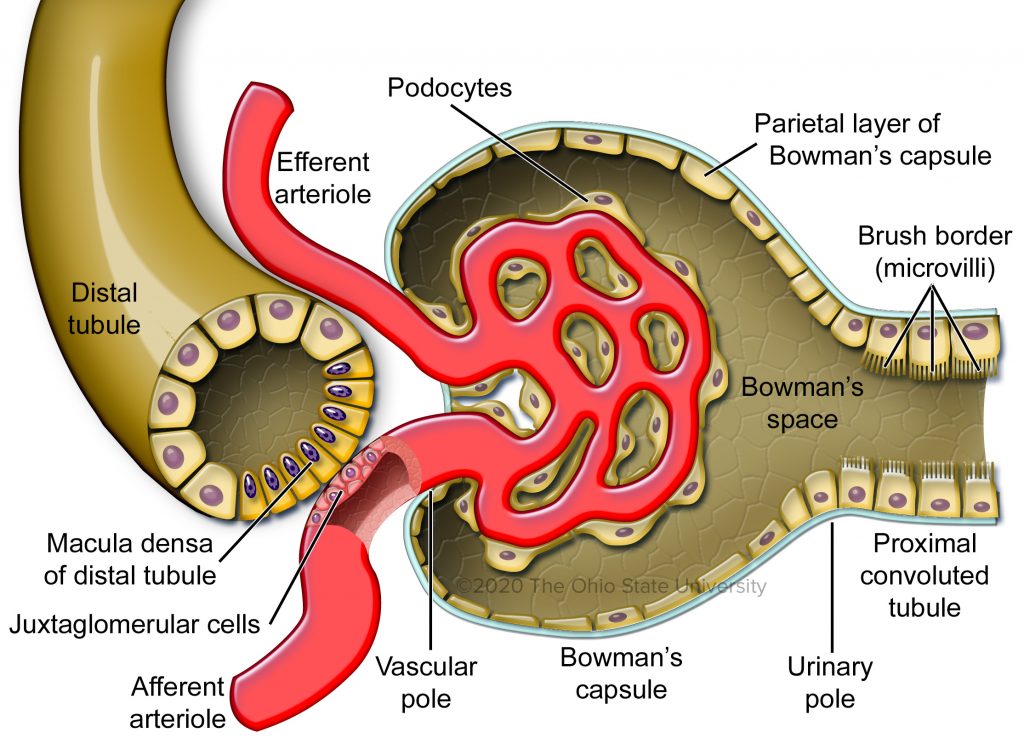
Juxtaglomerular apparatus (pt 2)
JG apparatus components (continued)
Macula densa
Modified epithelial cells in wall of DCT
Located on tubule side next to afferent arteriole
Detect changes in NaCl concentration of fluid in lumen of DCT
Signal granular cells to release renin through paracrine stimulation
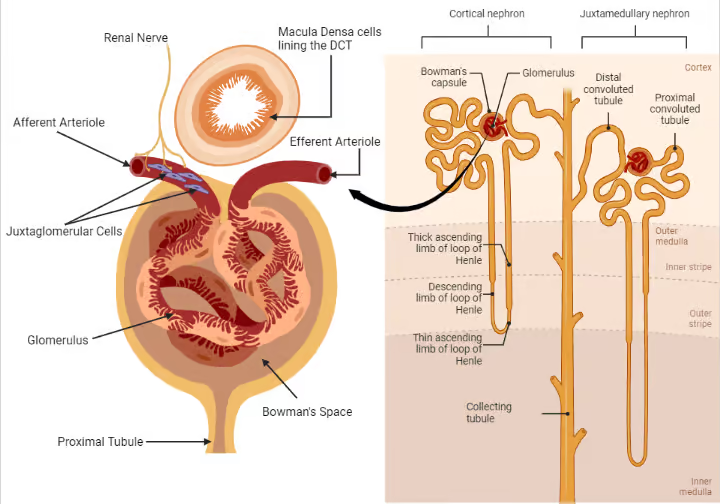
Juxtaglomerular apparatus (pt 3)
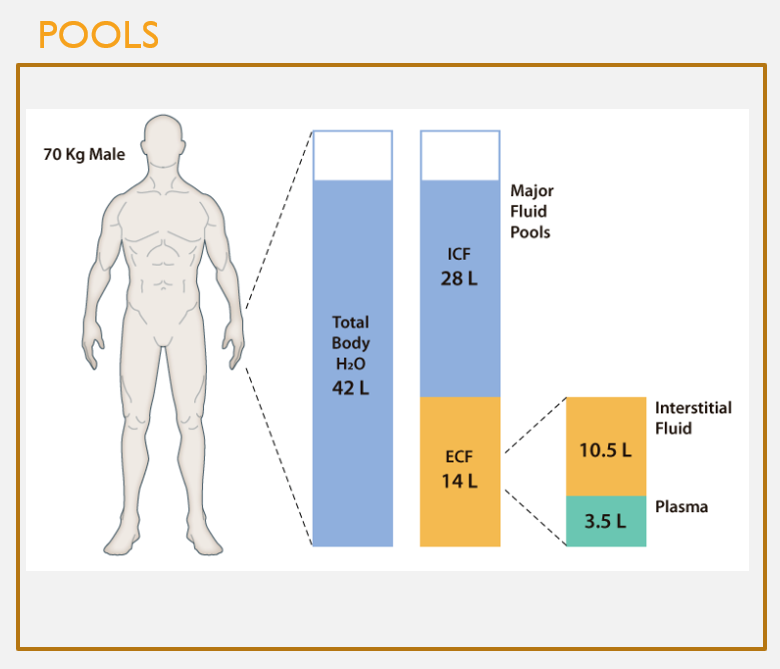
Human fluid pools
FEATURES
Human body composed of 3 interconnected pools:
Intracellular fluid
Inside cells
Intravascular fluid
In blood vessels
Interstitial fluid
Btwn cells
Extracellular
Interstitial + Intervascular
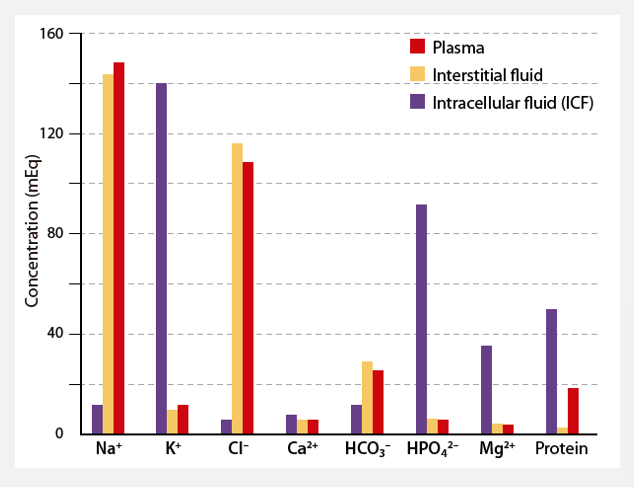
Fluid pool solute profiles are not identical
Intracellular fluid (ICF)
Water, electrolytes, small molecules, non-electrolytes, proteins
20-30% protein, pH 7.00
K+ most common
Extracellular fluid (ECF)
Far less protein, electrolytes
pH 7.40
Na+ most common

Thirst
Thirst is a sensation generated by:
Exercise, eating salty food, dry mouth
A 1-2% increase in osmolarity
Osmolarity — solutes/L, expressed as Osmoles/liter
0.290 to 0.295 Osm/L
Blood loss
Release of antidiuretic hormone (ADH)
Thirst is quenched as soon as water contacts osmolarity receptors in our cheeks — this happens to prevent over-consumption of water
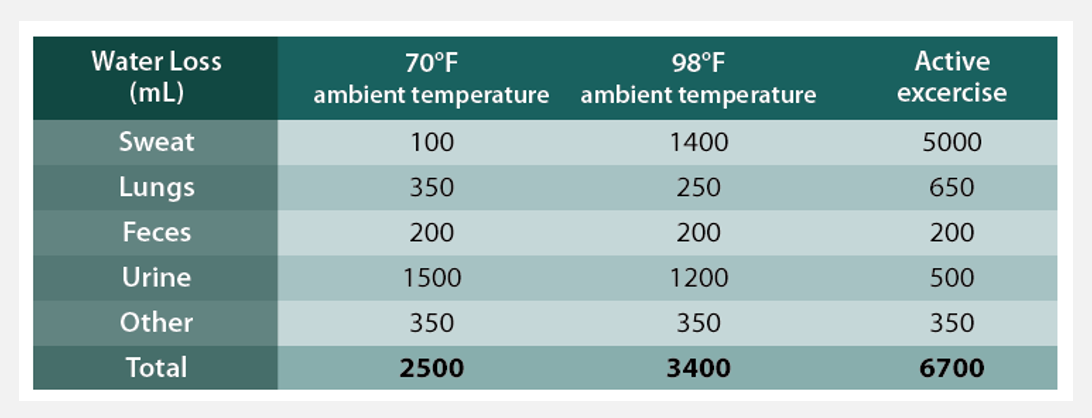
Water loss occurs in various ways
Kidneys (60%)
Sweat (8% or more) - depends on external temp, humidity, and activity lvl
Lungs (28%) - breathing
Feces (4%)
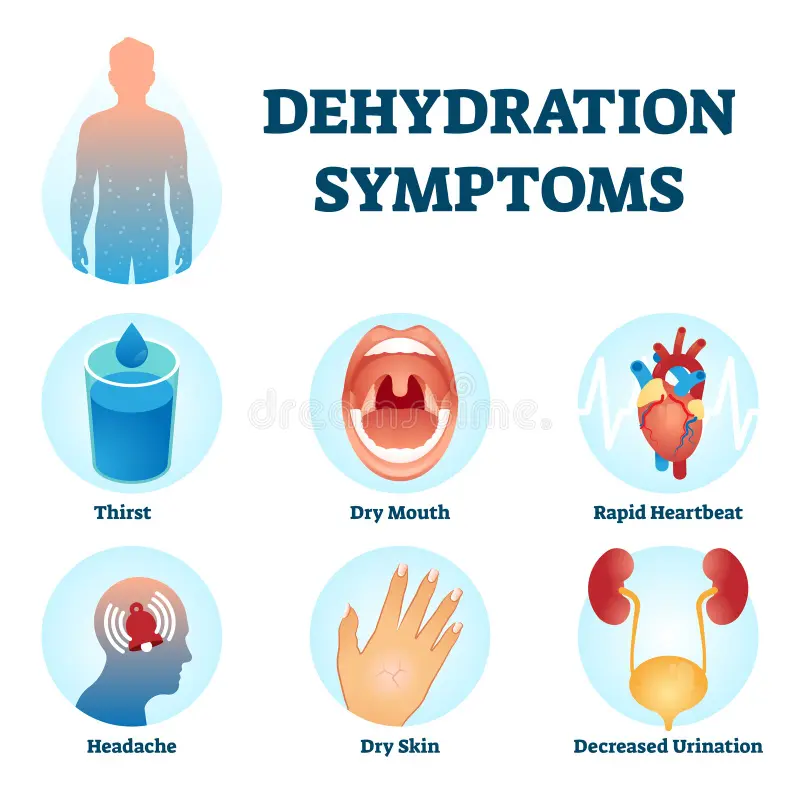
Several clinical disorders can arise from too much or too little water (pt 1)
Dehydration
Excessive water loss via sweating, diarrhea, vomiting, little water ingestion
Clinical symptoms include:
Sticky oral mucosa
Dry, flushed skin
Reduced urine formation
Thirst
Weight loss
Fever, CNS abnormalities and death
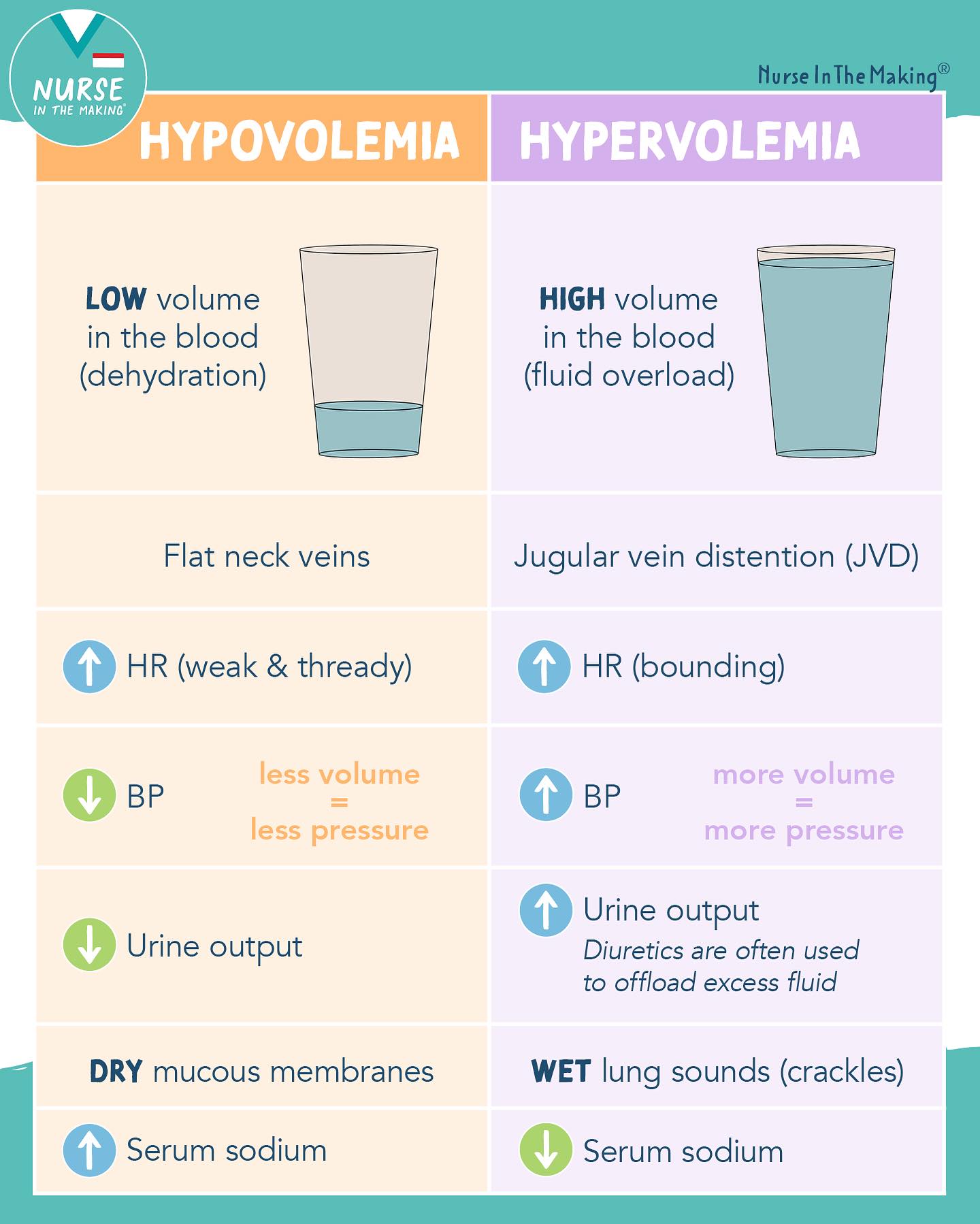
Several clinical disorders can arise from too much or too little water (pt 2)
Hypotonic hydration (rare)
Ingestion of too much water
Decrease in fluid pool osmolarity
CNS dysfunction
Hypovolemia
Loss of plasma volume
Loss of water and solutes
Diabetes, burns, wounds, diarrhea, vomiting
Hypervolemia
Too much plasma volume
Renal or liver failure
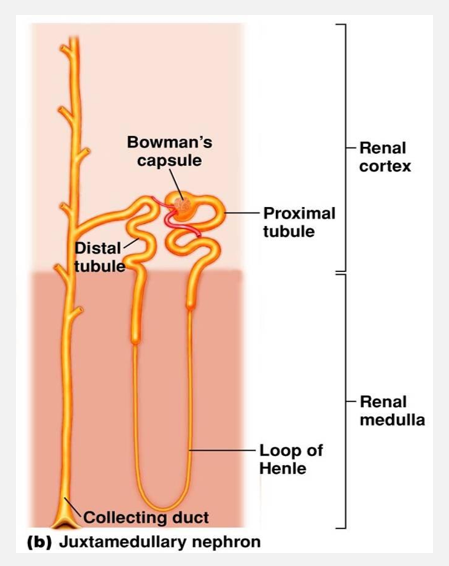
Which nephron’s major function is to concentrate urine?
A: cortical nephrons
B: juxtamedullary nephrons
C: Renal medulla
D: Minor and major calyces
B: juxtamedullary nephrons
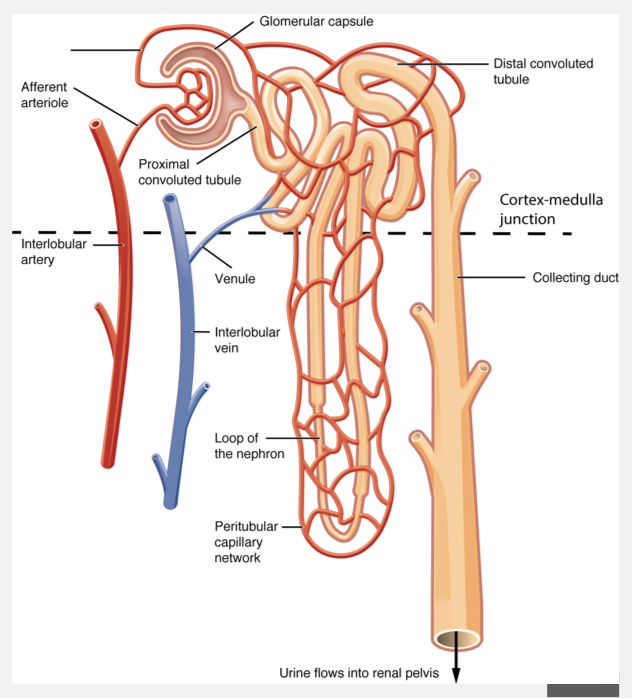
Principal and intercalated cells can be found where?
A: Renal corpuscles
B: Proximal convoluted tubules
C: Distal convoluted tubules
D: Collecting tubules and collecting ducts
D: Collecting tubules and collecting ducts