6. Haemodynamics, cardiac catheterisation, interventional cardiology.
1/92
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
93 Terms
What does haemodynamics study?
Haemodynamics studies blood flow and the forces driving circulation.
What does haemodynamics include?
Haemodynamics includes both cardiac and peripheral vascular physiology.
Basic Hemodynamic Parameters
Cardiac Output (CO)
Cardiac Index (CI)
Heart Rate (HR)
Stroke Volume (SV)
Preload and Afterload
Ejection Fraction (EF)
Cardiogenic Shock
What is Cardiac Output (CO)?
The volume of blood the heart pumps per minute.
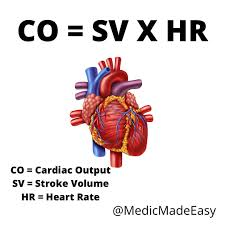
Why is Cardiac Output important in clinical practice?
Cardiac output is crucial for assessing the heart's efficiency and overall cardiovascular health.
What is Cardiac Index (CI)?
Cardiac output normalized to body surface area.
Cardiac Index (CI) is a measure of cardiac output adjusted for body surface area. It is calculated by dividing cardiac output by body surface area. Formula: CI = Cardiac Output / Body Surface Area.

Why is Cardiac Index (CI) clinically relevant?
It provides a more accurate assessment of cardiac function relative to the size of the individual.
What is Heart Rate (HR)?
The number of heart contractions per minute.
How is Heart Rate (HR) clinically relevant?
Variations can indicate arrhythmias, compensatory responses to systemic conditions, or effects of medications.
What is Stroke Volume (SV)?
The amount of blood ejected by the heart in each contraction.
What are the influencing factors of Stroke Volume?
Preload, afterload, and myocardial contractility.
What is Preload?
Reflects the ventricular volume at the end of diastole.
Preload in cardiology refers to the initial stretching of the heart muscle fibers at the end of diastole before contraction. It represents the volume of blood in the ventricles at the end of diastole.

What is Afterload?
The resistance the heart must overcome to eject blood.
Why are Preload and Afterload clinically relevant?
Understanding these factors can help in managing patients with conditions like heart failure, hypertension, and valve disorders.
What is Ejection Fraction (EF)?
The percentage of blood pumped out of the ventricles with each contraction.
Why is Ejection Fraction (EF) clinically relevant?
It is a primary diagnostic criterion in heart failure; low EF indicates impaired ventricular function.
What is the typical Ejection Fraction (EF) range in Cardiogenic Shock?
Typically 10-20%, indicating severe dysfunction and inadequate perfusion.
Cardiogenic Shock is a life-threatening condition where the heart is unable to pump enough blood to meet the body's needs, leading to organ failure. It is often caused by a heart attack or other heart-related issues.
What does the Frank-Starling law state?
The stroke volume of the heart increases in response to an increase in the volume of blood filling the heart.
The Frank-Starling law states that the force of contraction of the heart is directly proportional to the initial length of the muscle fibers before contraction.
Stroke Volume:Stroke volume is the amount of blood ejected by the left ventricle of the heart in one contraction. It increases with an increase in the volume of blood filling the heart.
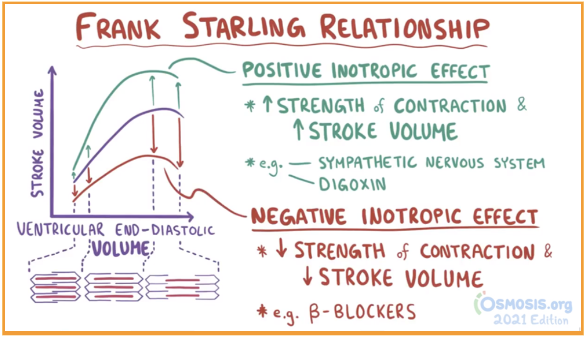
How does the Frank-Starling law explain the increase in stroke volume?
The increased volume stretches the ventricular wall, causing cardiac muscle to contract more forcefully.
What is the upper limit in the (Frank-Starling law) relationship between increased preload and contractility in the heart?
Beyond a certain point of stretch, such as a left ventricular filling pressure around 18 mmHg, increased preload does not improve contractility.
Answer:Yes, preload refers to the end-diastolic volume of the ventricle. It is the volume of blood in the ventricle at the end of diastole before contraction.
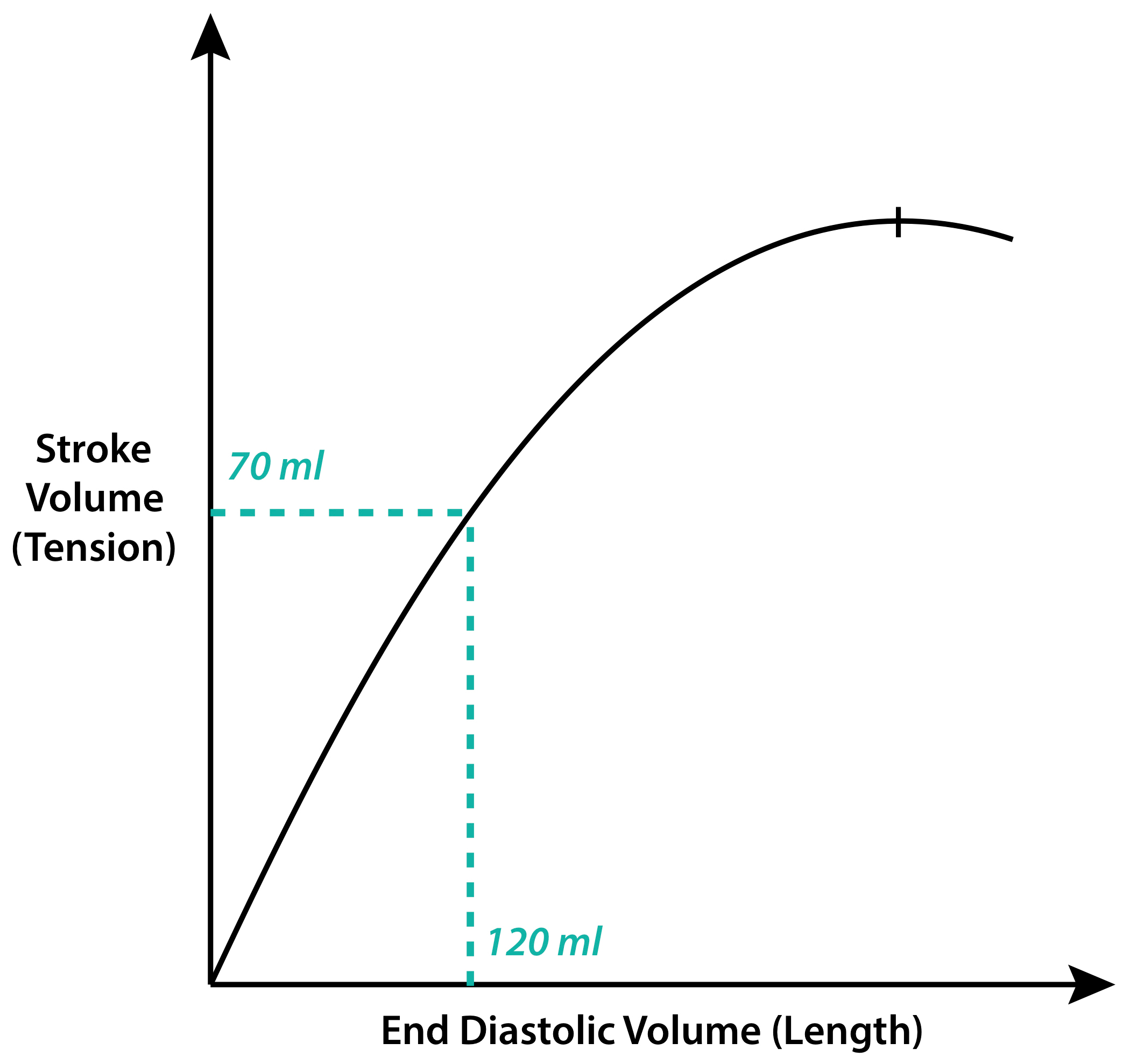
Why is careful monitoring essential in managing intravenous fluid therapy in heart failure patients?
Careful monitoring is crucial to avoid overloading the heart, as excessive preload can lead to diminished function and congestive heart failure symptoms.
How is ventricular filling pressure often assessed?
Ventricular filling pressure is often assessed via right heart catheterization, specifically using a pulmonary artery catheter to measure pulmonary capillary wedge pressure, which indirectly indicates left atrial pressure.
Pulmonary capillary wedge pressure is the pressure measured by a pulmonary artery catheter in the pulmonary capillaries, indirectly reflecting left atrial pressure
Pulmonary capillary wedge pressure indicates left atrial pressure because the catheter is wedged into a small pulmonary artery branch where pressure equilibrates with the left atrium due to the thin walls and direct connection to the left side of the heart.
What does the Law of Laplace describe?
The relationship between pressure inside a vessel, tension in the vessel wall, and the radius of the vessel.
The Law of Laplace describes the relationship between the pressure inside a spherical structure and the tension in its wall.
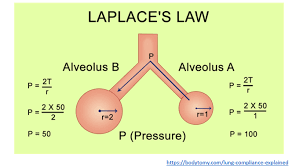
How is the tension in a vessel wall related to the radius and pressure according to the Law of Laplace?
Tension (T) is directly proportional to the radius (R) of the vessel and the pressure: T = P x R.
Why is the Law of Laplace important in clinical practice?
It helps understand conditions like aneurysms and dilated cardiomyopathy, where vessel radius affects wall tension and pressure generation.
Blood Pressure Metrics
Normal Values
Hypertension
Hypotension
Shock Index
Mean Arterial Pressure (MAP)
Pulmonary and Systemic Pressures
What are the normal blood pressure values?
Typically, around 120/80 mmHg.
How is hypertension defined?
Consistently high measurement exceeding 140/90 mmHg.
What is hypotension?
Blood pressure lower than 90/60 mmHg.
Shock Index:
A simple but useful clinical tool to assess hemodynamic status.
Shock Index is a clinical tool used to assess hemodynamic status by dividing heart rate by systolic blood pressure. It helps in identifying patients at risk of circulatory shock.

What is the Shock Index used for in clinical practice?
The Shock Index is used to assess hemodynamic status by calculating the ratio of heart rate to systolic blood pressure.
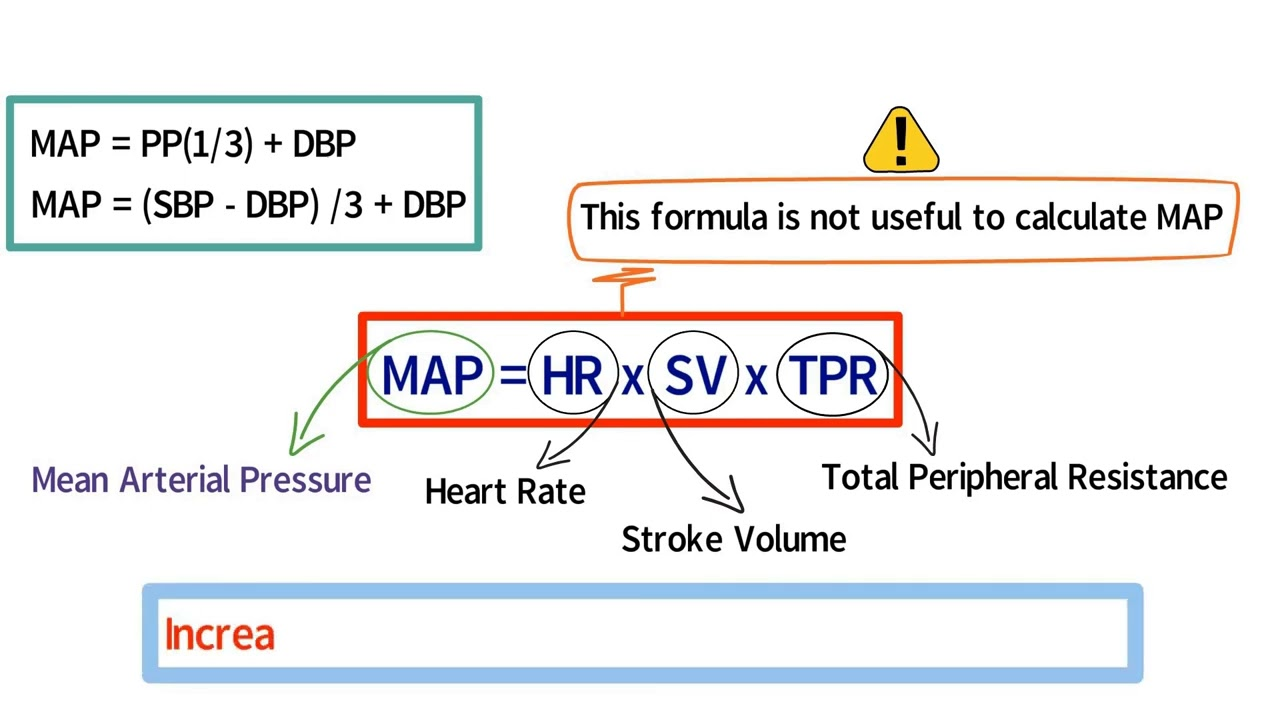
How is MAP is calculated as (2/3 × diastolic) + (1/3 × systolic) and is crucial for ensuring adequate organ perfusion. (MAP) calculated and why is it important?
MAP is calculated as (2/3 × diastolic) + (1/3 × systolic) and is crucial for ensuring adequate organ perfusion.
What are the normal ranges for pulmonary artery pressures and systemic pressures (MAP)?
Normal pulmonary artery pressures range from 9-18 mmHg, while systemic pressures (MAP) range from 70-106 mmHg.
What are the normal pressure ranges (in mmHg) for the atrial pressures?
Right Mean:2-8, Right "a" wave:2-10, Right "v" wave:1-10, Right systolic BP:< 7, Right diastolic BP:< 8, Left Mean:2-10, Left "a" wave:3-15, Left "v" wave:3-15, Left systolic BP:< 15, Left diastolic BP:< 12
Mean Pressure: Represents average pressure in the heart during a cardiac cycle.
"a" Wave Pressure: Reflects atrial contraction pressure.
"v" Wave Pressure: Indicates venous filling pressure in the heart.
What are the normal pressure ranges (in mmHg) for the ventricular pressures?
Right Peak systole:15-30, Right End diastole:2-8, Left Peak systole:100-140, Left End diastole:3-12
Peak systole and end diastole pressures refer to the maximum and minimum pressures within the heart chambers during the cardiac cycle. In this context, the values provided represent the pressure ranges in millimeters of mercury (mmHg) for the right and left sides of the heart.
What are the normal pressure ranges (in mmHg) for the great vessel pressures?
Pulmonary artery Peak systole:15-30, Pulmonary artery End diastole:4-12, Pulmonary artery Mean:9-18, Aorta Peak systole:100-140, Aorta End diastole:60-90, Aorta Mean:70-106
What is Aortic Pressure characteriz
e
High-pressure curve, peaking after the ventricular ejection phase and dipping down to diastolic pressure before the next cycle.
Aortic pressure follows this pattern due to the contraction and relaxation of the heart during the cardiac cycle. The peak represents systolic pressure during ventricular ejection, while the dip corresponds to diastolic pressure when the heart is relaxed and refilling.
Systolic Phase: Aortic pressure peaks during ventricular ejection.
Diastolic Phase: Aortic pressure dips down to diastolic pressure as the heart relaxes and refills.
Yes, there is blood in the aorta during the diastolic phase. The aorta receives blood from the left ventricle during systole and continues to distribute blood to the body during diastole.
Aortic pressure decreases during diastole because the heart is relaxed and refilling, causing a temporary drop in pressure as it prepares for the next cycle of ventricular ejection.
What do the "a," "c," and "v" waves in Atrial Pressure correspond to?
Atrial contraction, ventricular contraction (atrial bulging), and venous filling, respectively.
How does Ventricular Pressure change during the cardiac cycle?
Rapid rise in systole with a plateau during isovolumetric contraction, followed by a sharp drop during diastole.
Ventricular Pressure Changes: During systole, ventricular pressure rises rapidly as the heart contracts to push blood out. In isovolumetric contraction, pressure plateaus as all valves are closed. During diastole, pressure drops sharply as the heart relaxes and refills.
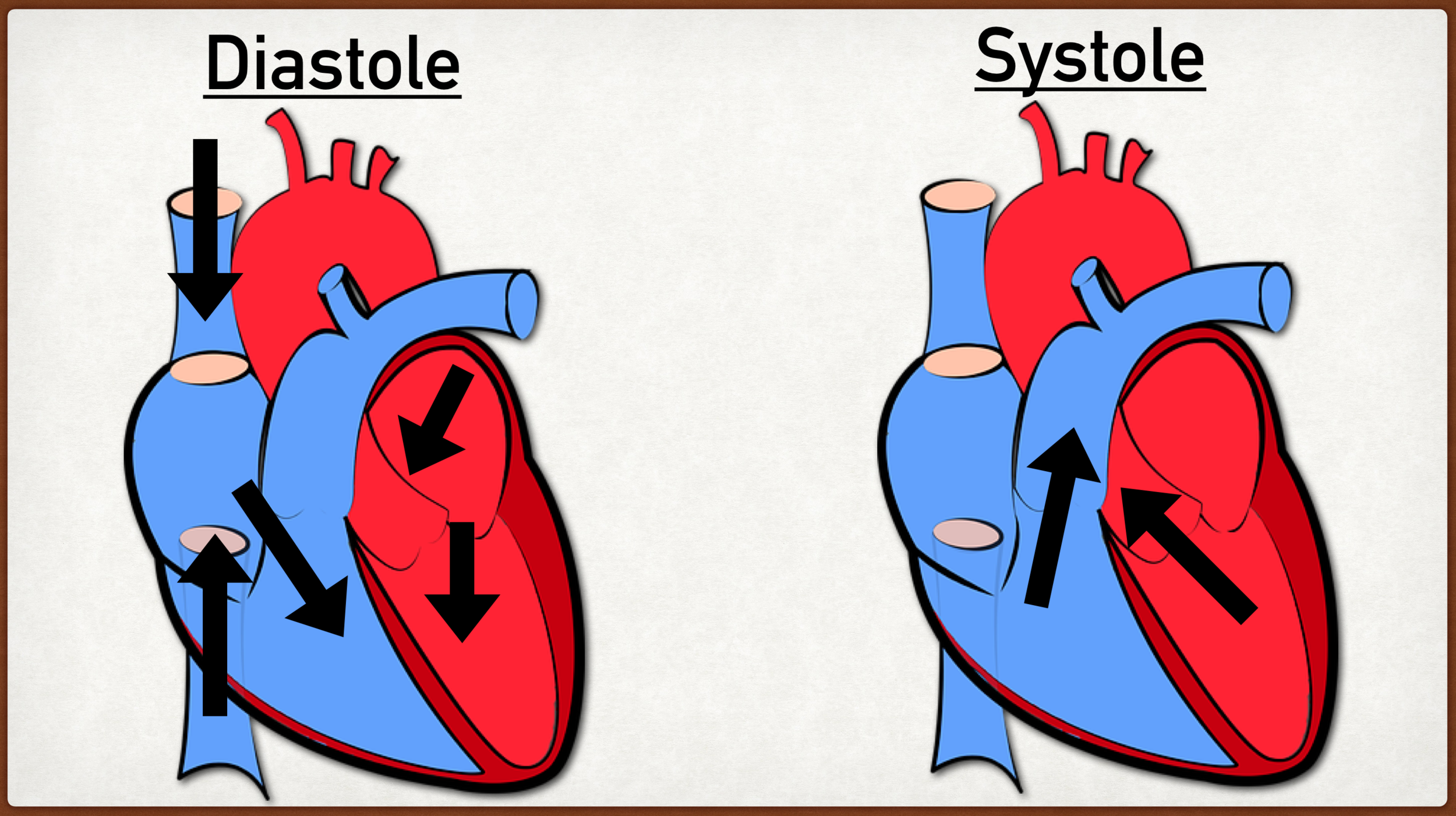
How does Ventricular Volume change during the cardiac cycle?
Falls sharply during systole as blood is ejected and rises during diastole as the ventricles fill.
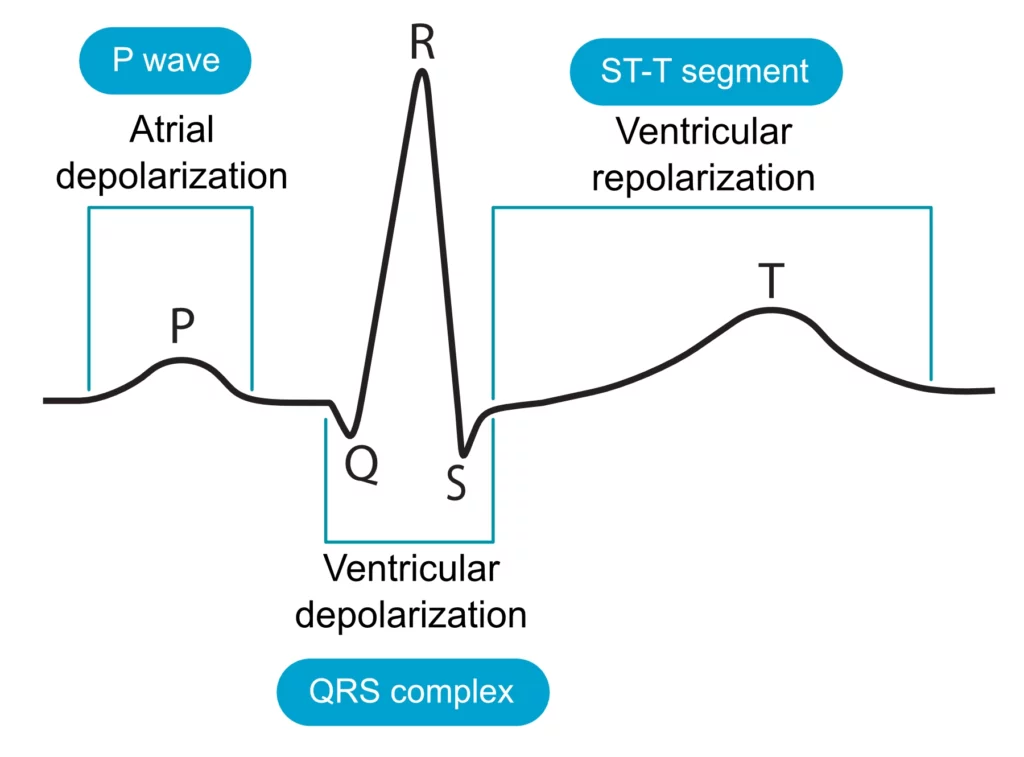
What do the P wave, QRS complex, and T wave in an ECG correlate with?
Atrial depolarization, ventricular depolarization, and ventricular repolarization.
What does a Phonocardiogram align with?
Heart sounds and potentially murmur timings.
What is Percutaneous Coronary Intervention (PCI)?
A procedure to open narrowed or blocked coronary arteries, often involving stent placement.
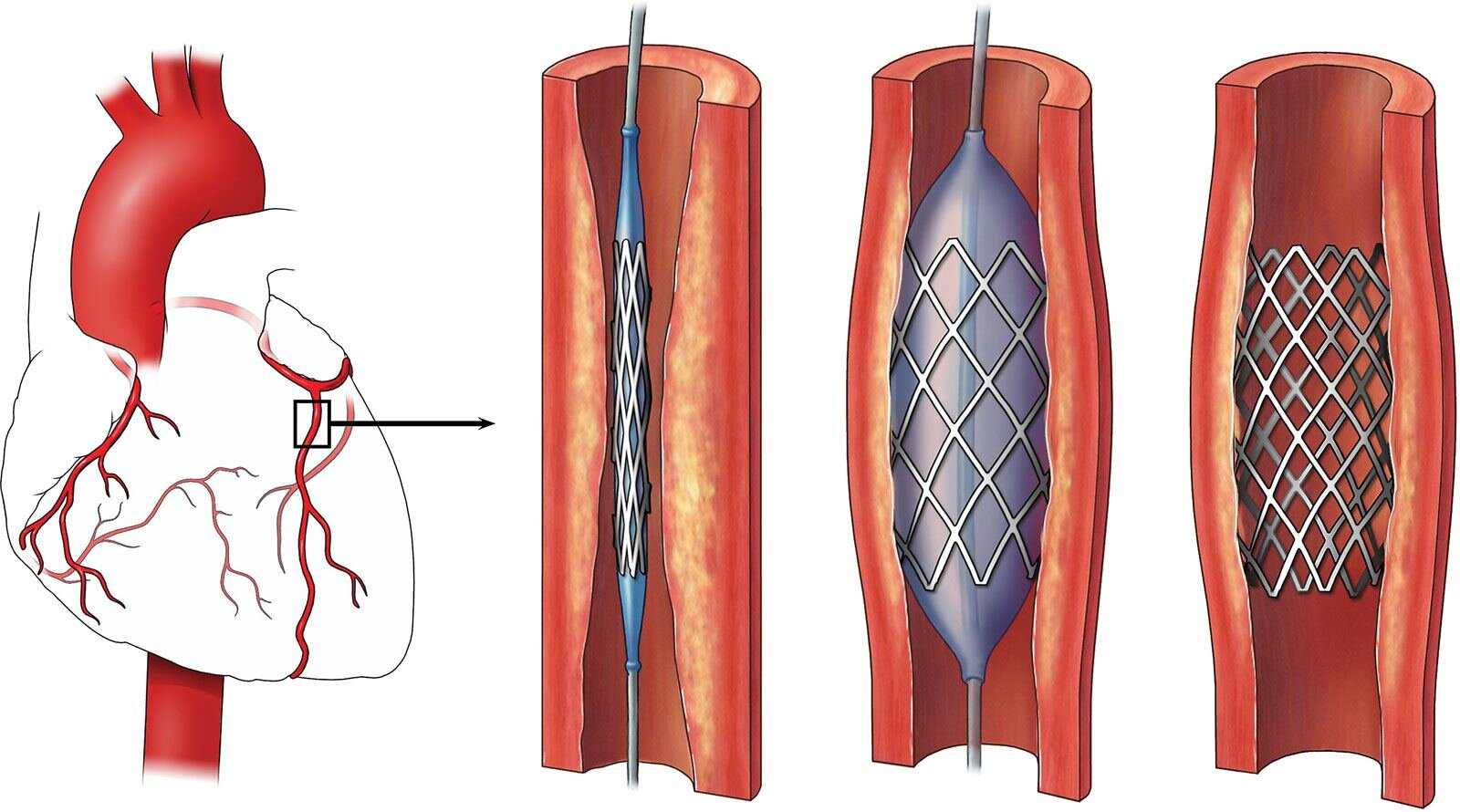
What are the indications for PCI?
Acute myocardial infarction (MI)
Chronic occlusions of coronary arteries
Occlusion of bypass grafts or previously placed stents
Recurrent ischemia post-cardiac surgery
Acute myocardial infarction (MI): Immediate restoration of blood flow to prevent heart muscle damage.
Chronic occlusions of coronary arteries: To improve blood supply to the heart muscle.
Occlusion of bypass grafts or stents: To reopen blocked vessels and restore blood flow.
Recurrent ischemia post-cardiac surgery: To alleviate symptoms and prevent further heart damage.
When should PCI be performed for optimal outcomes?
Should be performed within 90-120 minutes of symptom onset, known as the 'golden hour' for optimal outcomes.
What is the success rate of achieving reperfusion with efficacy?
Over 90%
How does efficacy improve prognosis in acute coronary syndrome?
By reducing the risk of recurrent MI
Acute Coronary Syndrome is a term used to describe a range of conditions associated with sudden, reduced blood flow to the heart. It includes unstable angina and heart attacks (myocardial infarctions).
What does efficacy primarily offer in patients with chronic coronary artery disease?
Primarily offers symptomatic relief in patients with chronic coronary artery disease
How is access gained during the procedure?
Via the radial or femoral artery
Access is gained via the radial or femoral artery.
What is advanced to the site of the coronary artery occlusion?
A catheter
A catheter is advanced to the site of the coronary artery occlusion
What is passed through the occlusion?
A guidewire
A guidewire is passed through the occlusion.
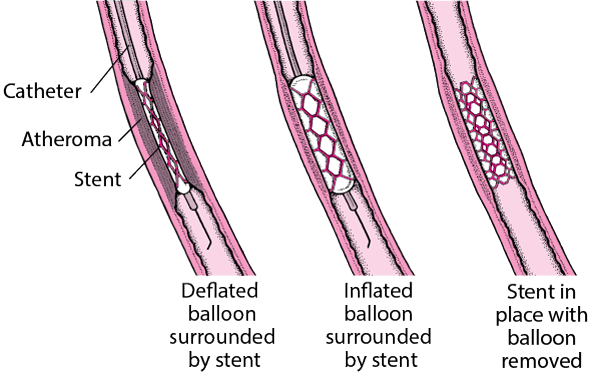
What is inflated at the site of stenosis?
A balloon catheter
A balloon catheter is inflated at the site of stenosis to dilate the vessel.
What is deployed to maintain vessel patency?
A stent
A stent is deployed to maintain vessel patency.
What is left in place after the balloon is withdrawn?
The stent
The balloon is deflated and withdrawn, leaving the stent in place.
Complications of PCI
Radial Approach
Restenosis
Stent Thrombosis
Periprocedural MI
Cerebrovascular Accident
Severe Hemorrhage
Infection
Death
What is the preferred approach for PCI to reduce bleeding risk and increase comfort?
Radial Approach
Which type of stent is associated with less frequent restenosis compared to bare-metal stents?
Drug-eluting stents (DES)
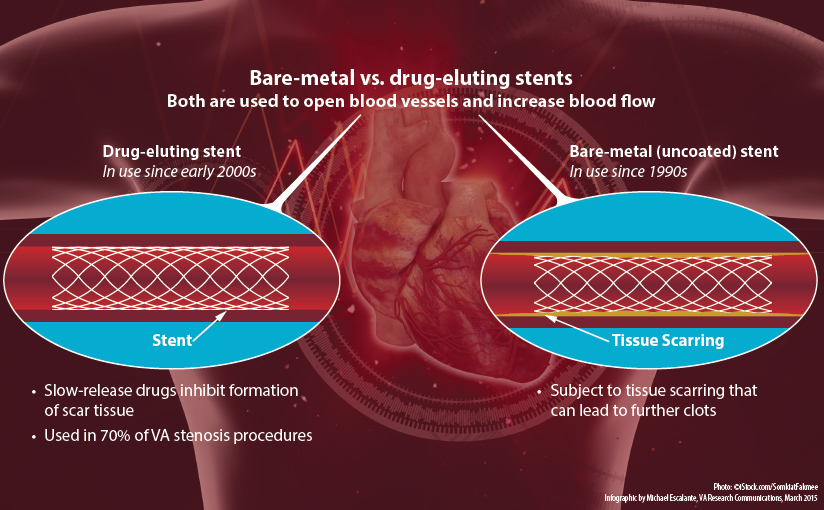
What is a rare but serious complication of PCI that may require extended antiplatelet therapy, particularly with Drug-eluting stents (DES)?
.
Stent Thrombosis
DES have a lower risk of thrombosis due to reduced rates of restenosis, they require longer periods of antiplatelet therapy to mitigate the increased risk of late stent thrombosis due to delayed endothelialization.
What is a potential complication that can occur in a small percentage of cases during the procedure?
Periprocedural MI
Periprocedural MI stands for Periprocedural Myocardial Infarction, which refers to a heart attack that occurs during or shortly after a medical procedure or surgery. It can be a serious complication due to various factors such as stress on the heart during the procedure.
What is the risk of a Cerebrovascular Accident during the procedure?
Less than 1%
What complication may occur in about 2% of cases and could necessitate a blood transfusion?
Severe Hemorrhage
What is a potential risk following any invasive procedure, including this one?
Infection
What is the risk of death during the procedure?
Very low, but present.
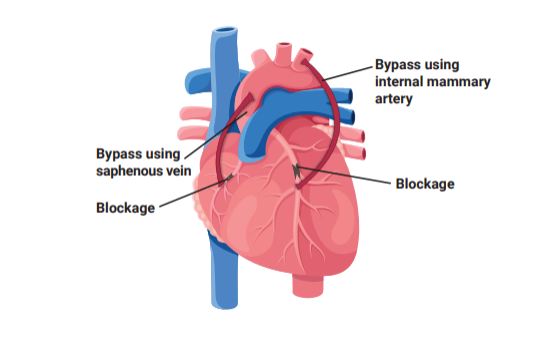
what is Coronary Artery Bypass Grafting (CABG)?
Coronary Artery Bypass Grafting (CABG) is a surgical procedure that improves blood flow to the heart by bypassing blocked or narrowed coronary arteries using a healthy blood vessel graft.
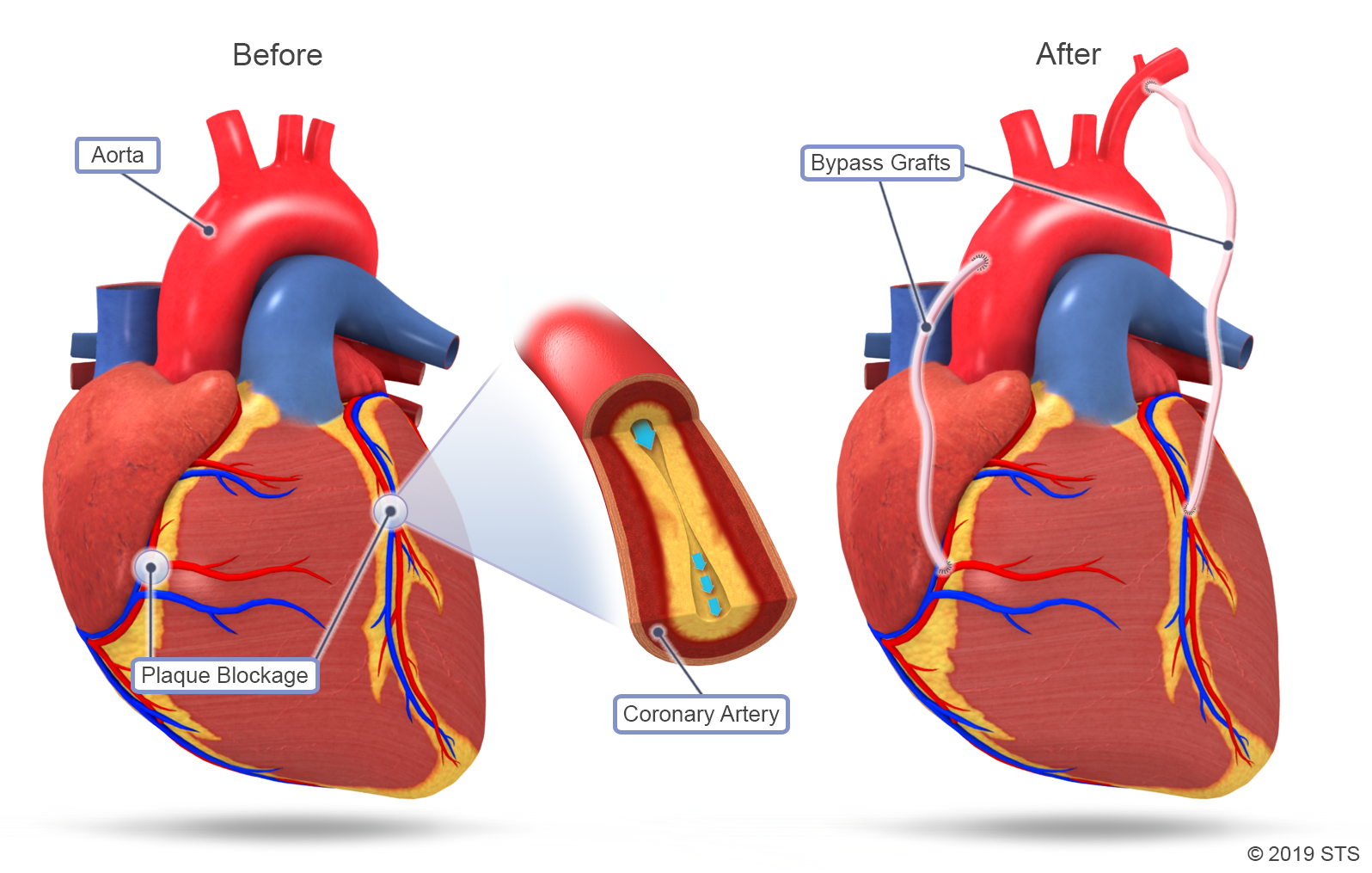
What are the indications for Coronary Artery Bypass Grafting (CABG)?
Extensive coronary atherosclerosis, disabling angina, and poor left ventricular function where revascularization can restore myocardial function.
What are the contraindications for CABG?
Typically avoided in asymptomatic patients, those with severe comorbidities, or advanced age due to the risk of perioperative complications.
What is the approach for CABG?
Involves a thoracotomy via midline sternotomy, the use of cardiopulmonary bypass, and cardiac arrest to allow grafting.
CABG Procedure Overview:
Involves a thoracotomy via midline sternotomy.
Utilizes cardiopulmonary bypass.
Induces cardiac arrest to facilitate grafting.
Yes, coronary artery bypass grafting (CABG) induces cardiac arrest.
This means the heart is intentionally stopped during surgery to facilitate grafting of the coronary arteries.
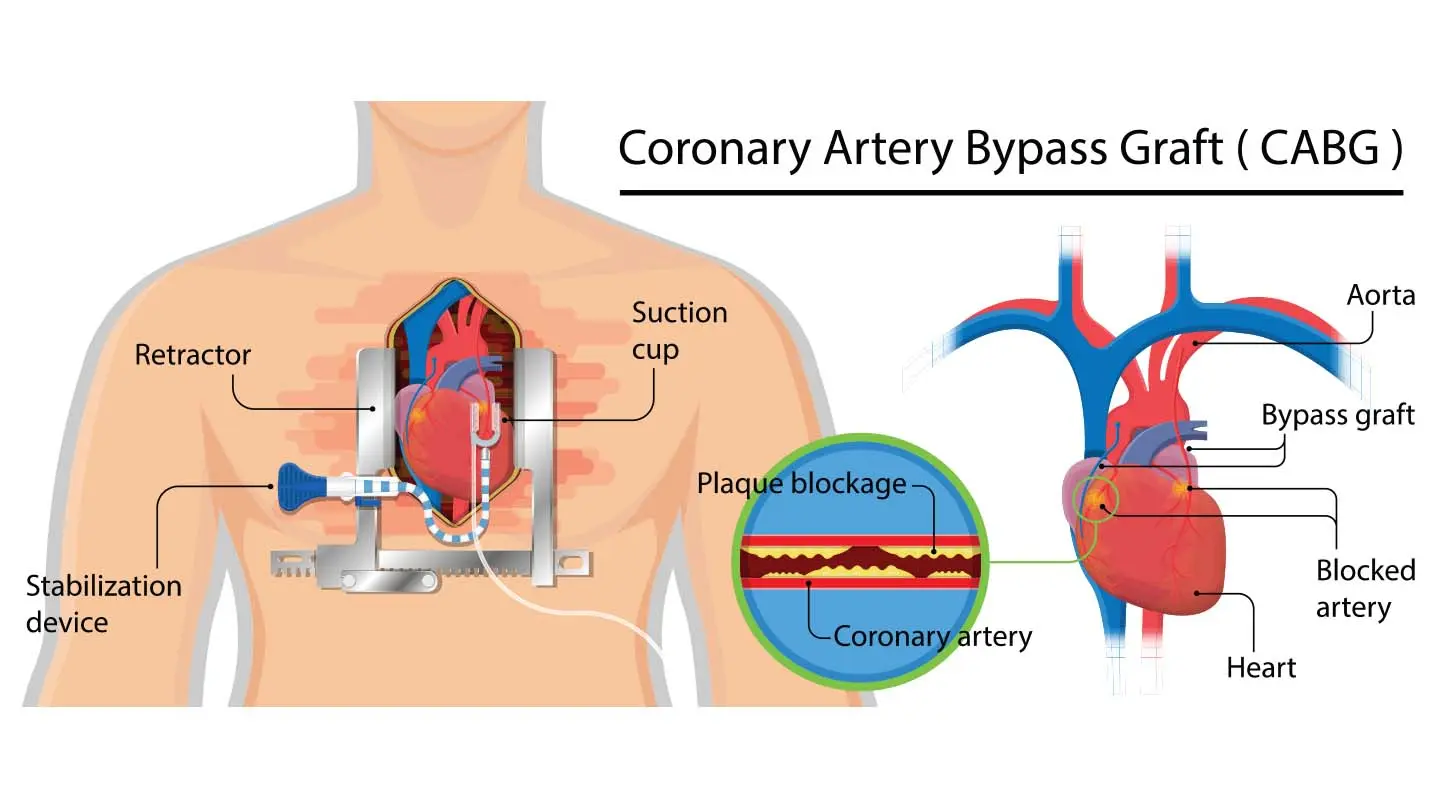
What are the preferred types of arterial grafts used in CABG?
Internal thoracic artery or radial artery, preferred due to better long-term patency.
An arterial graft is a surgical procedure where an artery is used to bypass a blocked or damaged artery, improving blood flow. It can be the internal thoracic artery or radial artery, preferred for their long-term patency.
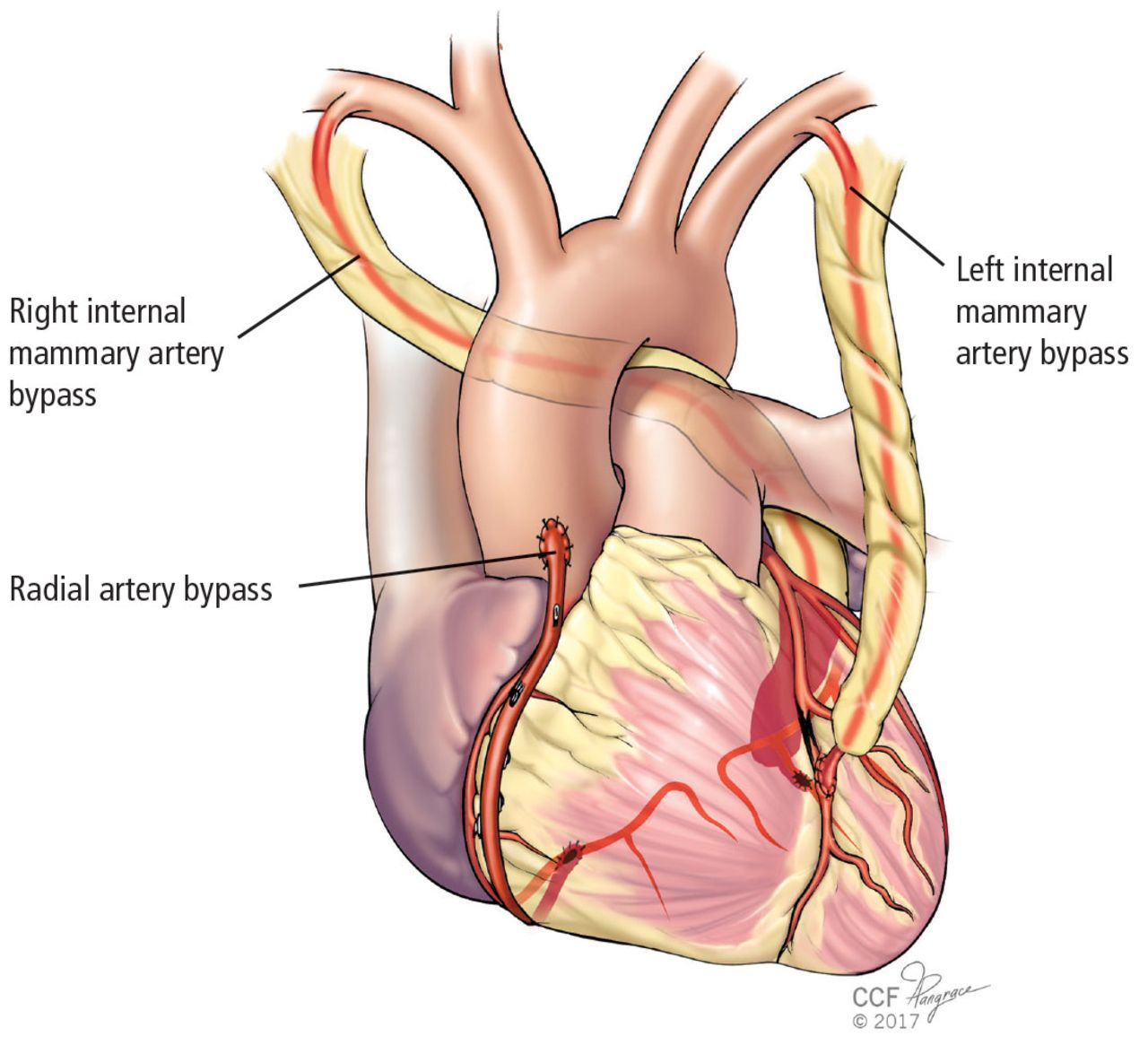
What is a common type of venous graft used in CABG?
Great saphenous vein is often used as a venous graft in CABG.
Complications of CABG
Myocardial Dysfunction
Post-Pericardiotomy Syndrome
Perioperative Cardiac Tamponade
Bypass Occlusion
Arrhythmias
Post-operative Acute Mediastinitis
Mediastinal Hemorrhage
Perioperative Stroke
Serious Bleeding
Mortality
What are the complications of CABG related to myocardial dysfunction?
Ischemia, reperfusion injury, or edema can lead to myocardial dysfunction.
Answer:Coronary artery bypass grafting (CABG) can cause ischemia due to temporary occlusion of blood flow during surgery, reperfusion injury upon restoration of blood flow, and edema as a result of tissue trauma and inflammation.
How is myocardial dysfunction managed in CABG patients?
Management includes medications to support heart function and reduce edema.
What is Post-Pericardiotomy Syndrome in the context of CABG?
It is an autoimmune response characterized by fever, chest pain, and tachycardia.
Post-Pericardiotomy Syndrome in the context of CABG refers to inflammation of the pericardium following cardiac surgery, such as Coronary Artery Bypass Grafting. Symptoms include fever, chest pain, and pericardial effusion.
How is Post-Pericardiotomy Syndrome treated in CABG patients?
It is treated with anti-inflammatory drugs and sometimes pericardial drainage.
What is Perioperative Cardiac Tamponade in the context of CABG?
It is the accumulation of fluid in the pericardium causing pressure on the heart.
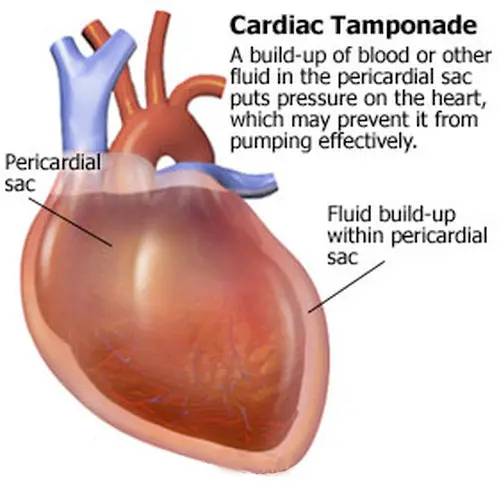
What is the urgent intervention required for Perioperative Cardiac Tamponade in CABG patients?
It requires urgent drainage to restore normal heart function.
What can graft failure lead to in CABG patients?
Myocardial ischemia
Graft failure in CABG patients can lead to complications such as myocardial infarction, angina, or the need for repeat surgery.
Graft failure in CABG refers to the inadequate functioning of the bypass graft used to reroute blood flow around blocked coronary arteries during coronary artery bypass graft surgery. It can lead to complications like myocardial infarction, angina, or the need for repeat surgery.
What is a common complication after CABG that may require medication or pacemaker placement?
Arrhythmias
What is post-operative Acute Mediastinitis in CABG?
Infection of the central chest area, requiring antibiotics and sometimes surgical intervention
What is Mediastinal Hemorrhage as a complication of CABG?
Bleeding in the chest cavity that may require surgical re-exploration
What is Perioperative Stroke as a complication of CABG?
Stroke occurring in about 5% of cases, secondary to intraoperative emboli or hypoperfusion
How often does serious bleeding occur postoperatively?
In 10-15% of cases, sometimes necessitating blood transfusions
What is the mortality rate of CABG?
About 2%, varying based on patient risk factors
What factors can influence the lifespan of a successful CABG graft?
The type of graft and patient lifestyle can influence the lifespan of a successful CABG graft.
Valve Replacement
When is valve replacement typically performed?
Valve replacement is frequently performed on the aortic and mitral valves and is indicated for severe or symptomatic valvular disease, or in conjunction with other cardiac surgeries.
Types of Valves
Mechanical Valves
Bioprosthetic Valves (Biological Valves):
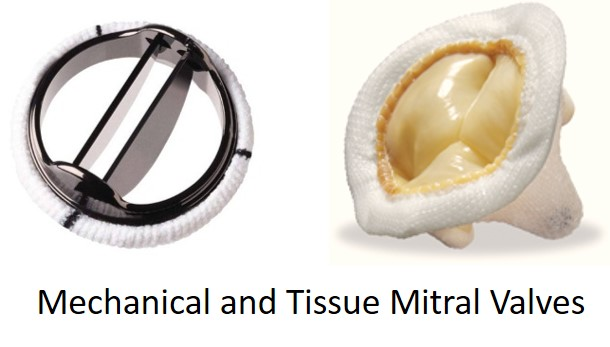
What is a key characteristic of Mechanical Valves?
Offer long-term durability
What is a key consideration for patients with Mechanical Valves?
Require lifelong anticoagulation therapy to prevent thrombosis
Mechanical valves require lifelong anticoagulation therapy due to the increased risk of thrombosis associated with the artificial materials used in the valve construction. Bioprosthetic valves, made from biological tissues, have a lower risk of thrombosis, hence do not require lifelong anticoagulation.
What is a key feature of Bioprosthetic Valves?
Do not generally require long-term anticoagulation; patients may switch to aspirin after an initial period on anticoagulants
What is a limitation of Bioprosthetic Valves?
Have a limited lifespan due to structural deterioration over time
How can Valve Replacement Procedure be performed?
Can be performed using traditional open-heart surgery or via a less invasive catheter-based approach (e.g., TAVR for the aortic valve)
What factors influence the choice between mechanical and bioprosthetic valves?
Patient factors, including age, lifestyle, and the ability to manage anticoagulant therapy