6. Haemodynamics, cardiac catheterisation, interventional cardiology.
Haemodynamics is the study of blood flow and the forces driving the circulation, and it includes both cardiac and peripheral vascular physiology.
Basic Hemodynamic Parameters
Cardiac Output (CO)
Definition: The volume of blood the heart pumps per minute.
Clinical Relevance: Cardiac output is crucial for assessing the heart's efficiency and overall cardiovascular health. Abnormal values can indicate heart failure, shock, or other cardiac dysfunctions.
Cardiac Index (CI)
Definition: Cardiac output normalized to body surface area, providing a more accurate assessment of cardiac function relative to the size of the individual.
Clinical Relevance: Useful in diagnosing and managing heart conditions, ensuring that therapy is tailored to the individual’s physiological demands.
Heart Rate (HR)
Definition: The number of heart contractions per minute.
Clinical Relevance: Variations can indicate arrhythmias, compensatory responses to systemic conditions, or effects of medications.
Stroke Volume (SV)
Definition: The amount of blood ejected by the heart in each contraction.
Influencing Factors: Preload, afterload, and myocardial contractility.
Clinical Relevance: Key in conditions like heart failure where the heart's pumping capacity is compromised.
Preload and Afterload
Preload: Reflects the ventricular volume at the end of diastole.
Afterload: The resistance the heart must overcome to eject blood.
Clinical Relevance: Understanding these can help in managing patients with hypertension, heart failure, and valve disorders.
Ejection Fraction (EF)
Definition: The percentage of blood pumped out of the ventricles with each contraction.
Clinical Relevance: A primary diagnostic criterion in heart failure; low EF indicates impaired ventricular function.
Cardiogenic Shock
EF in Cardiogenic Shock: Typically 10-20%, indicating severe dysfunction and inadequate perfusion.
Frank-Starling Law
Principle: The Frank-Starling law states that the stroke volume of the heart increases in response to an increase in the volume of blood filling the heart (the end-diastolic volume), when all other factors remain constant. The increased volume stretches the ventricular wall, causing cardiac muscle to contract more forcefully.
Limitation: However, this relationship has an upper limit—beyond a certain point of stretch (e.g., a left ventricular filling pressure around 18 mmHg), increased preload does not improve contractility and can indeed lead to diminished function and congestive heart failure symptoms.
Clinical Application: This principle is critical for managing intravenous fluid therapy, especially in heart failure patients, where careful monitoring is required to avoid overloading the heart.
Measurement Techniques
Ventricular Filling Pressure: Often assessed via right heart catheterization, specifically using a pulmonary artery catheter to measure pulmonary capillary wedge pressure, which indirectly indicates left atrial pressure.
Law of Laplace
Principle: Describes the relationship between the pressure inside a vessel, the tension in the vessel wall, and the radius of the vessel. It mathematically illustrates that the tension (T) necessary to withstand a given internal fluid pressure (P) in a thin-walled sphere is directly proportional to the radius (R) of the vessel and the pressure: �=�×�T=P×R
Clinical Relevance: This law is particularly important in understanding conditions like aneurysms, where increased radius of a blood vessel can lead to increased wall tension, risking rupture. It also helps explain why ventricles with dilated cardiomyopathy are at a disadvantage in generating pressure without hypertrophy.
Blood Pressure Metrics
Normal Values: Typically, a normal blood pressure reading is around 120/80 mmHg.
Hypertension: Defined as a consistently high measurement exceeding 140/90 mmHg. Managing hypertension is crucial as it is a major risk factor for heart disease, stroke, and renal failure.
Hypotension: Defined as blood pressure lower than 90/60 mmHg. While it may be normal in healthy individuals such as athletes, in other circumstances, it may indicate underlying problems, especially if accompanied by symptoms like dizziness or tachycardia.
Shock Index: A simple but useful clinical tool to assess hemodynamic status. A ratio of heart rate to systolic blood pressure, where values greater than 0.8 are suspicious, and values above 1.0 typically indicate a state of shock.
Mean Arterial Pressure (MAP): Represents an average blood pressure in an individual during a single cardiac cycle. It's crucial for ensuring adequate perfusion of organs, calculated as: MAP=(2/3×diastolic)+(3xsystolic)
Pulmonary and Systemic Pressures: Normal pulmonary artery pressures range from 9-18 mmHg, while systemic pressures (represented as MAP) range from 70-106 mmHg.
Pressures (mmHg)
Atrial:
- Right Mean: 2-8
- Right "a" wave: 2-10
- Right "v" wave: 1-10
- Right systolic BP: < 7
- Right diastolic BP: < 8
- Left Mean: 2-10
- Left "a" wave: 3-15
- Left "v" wave: 3-15
- Left systolic BP: < 15
- Left diastolic BP: < 12
Ventricular:
- Right Peak systole: 15-30
- Right End diastole: 2-8
- Left Peak systole: 100-140
- Left End diastole: 3-12
Great vessel:
- Pulmonary artery Peak systole: 15-30
- Pulmonary artery End diastole: 4-12
- Pulmonary artery Mean: 9-18
- Aorta Peak systole: 100-140
- Aorta End diastole: 60-90
- Aorta Mean: 70-106
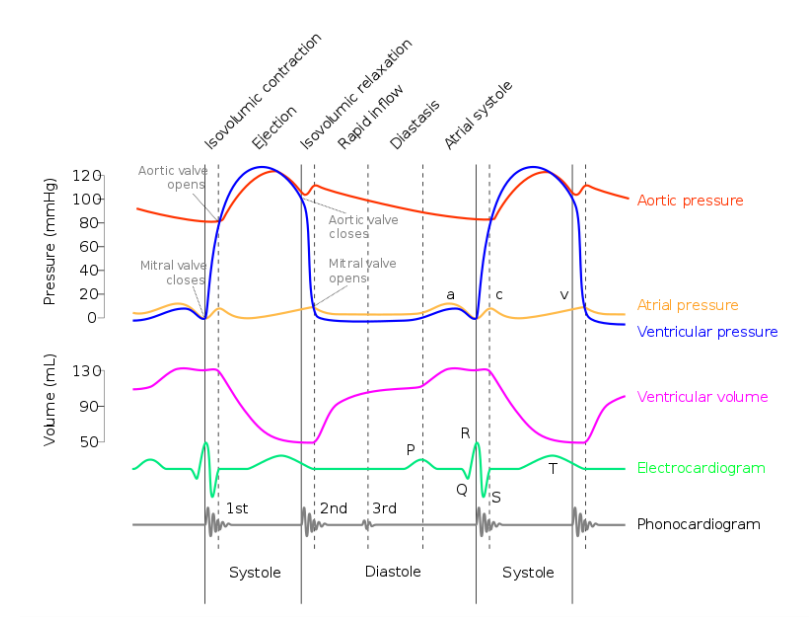
Aortic Pressure: High-pressure curve, peaking after the ventricular ejection phase and dipping down to diastolic pressure before the next cycle.
Atrial Pressure: Shows "a," "c," and "v" waves corresponding to atrial contraction, ventricular contraction (atrial bulging), and venous filling, respectively.
Ventricular Pressure: Rapid rise in systole with a plateau during isovolumetric contraction, followed by a sharp drop during diastole.
Ventricular Volume: Falls sharply during systole as blood is ejected and rises during diastole as the ventricles fill.
ECG (Electrocardiogram): Displays the P wave, QRS complex, and T wave, correlating with atrial depolarization, ventricular depolarization, and ventricular repolarization.
Phonocardiogram: Not clearly labeled but appears to align with heart sounds and potentially murmur timings.
Percutaneous Coronary Intervention (PCI)
Percutaneous Coronary Intervention (PCI) is a cornerstone of interventional cardiology, offering a minimally invasive method to treat coronary artery disease. Here's a detailed linear summary of PCI for your reference:
Percutaneous Coronary Intervention (PCI)
Definition: A procedure to open narrowed or blocked coronary arteries, often involving stent placement.
Indications for PCI
Acute myocardial infarction (MI)
Chronic occlusions of coronary arteries
Occlusion of bypass grafts or previously placed stents
Recurrent ischemia post-cardiac surgery
Timing for PCI
Should be performed within 90-120 minutes of symptom onset, known as the 'golden hour' for optimal outcomes.
Efficacy
Success rate of over 90% in achieving reperfusion
Improves prognosis in acute coronary syndrome by reducing the risk of recurrent MI
Primarily offers symptomatic relief in patients with chronic coronary artery disease
Procedure Steps
Access is gained via the radial or femoral artery.
A catheter is advanced to the site of the coronary artery occlusion.
A guidewire is passed through the occlusion.
A balloon catheter is inflated at the site of stenosis to dilate the vessel.
A stent is deployed to maintain vessel patency.
The balloon is deflated and withdrawn, leaving the stent in place.
Complications of PCI
Radial Approach: Preferred for comfort and reduced bleeding risk, though it may require higher radiation doses.
Restenosis: Occurs less frequently with DES than with BMS.
Stent Thrombosis: A rare but serious complication necessitating extended antiplatelet therapy, especially with DES.
Periprocedural MI: Can occur in a small percentage of cases.
Cerebrovascular Accident: Risk is less than 1%.
Severe Hemorrhage: May occur in about 2% of cases and may require a blood transfusion.
Infection: A potential risk following any invasive procedure.
Death: Very low risk, but present.
Coronary Artery Bypass Grafting (CABG)
Indications: Extensive coronary atherosclerosis, disabling angina, and poor left ventricular function where revascularization can restore myocardial function.
Contraindications: Typically avoided in asymptomatic patients, those with severe comorbidities, or advanced age due to the risk of perioperative complications.
Procedure:
Approach: Involves a thoracotomy via midline sternotomy, the use of cardiopulmonary bypass, and cardiac arrest to allow grafting.
Graft Types:
Arterial Grafts: Such as the internal thoracic artery or radial artery, are preferred due to better long-term patency.
Venous Grafts: Often the great saphenous vein is used.
Complications of CABG
Myocardial Dysfunction:
Due to ischemia, reperfusion injury, or edema.
Management includes medications to support heart function and reduce edema.
Post-Pericardiotomy Syndrome:
Autoimmune response characterized by fever, chest pain, and tachycardia.
Treated with anti-inflammatory drugs and sometimes pericardial drainage.
Perioperative Cardiac Tamponade:
Accumulation of fluid in the pericardium causing pressure on the heart.
Requires urgent drainage to restore normal heart function.
Bypass Occlusion:
Graft failure can lead to myocardial ischemia.
May necessitate repeat revascularization.
Arrhythmias:
Common after surgery, may require medication or pacemaker placement.
Post-operative Acute Mediastinitis:
Infection of the central chest area, a serious complication requiring antibiotics and sometimes surgical intervention.
Mediastinal Hemorrhage:
Bleeding in the chest cavity may require surgical re-exploration.
Perioperative Stroke:
Occurs in about 5% of cases, secondary to intraoperative emboli or hypoperfusion.
Serious Bleeding:
Significant postoperative bleeding occurs in 10-15% of cases, sometimes necessitating blood transfusions.
Mortality:
CABG has a mortality rate of about 2%, varying based on patient risk factors.
Prognosis
A successful CABG graft can last between 8 to 15 years, depending on factors like the type of graft and patient lifestyle.
Valve Replacement
Valve replacement is frequently performed on the aortic and mitral valves and is indicated for severe or symptomatic valvular disease, or in conjunction with other cardiac surgeries.
Types of Replacement Valves
Mechanical Valves:
Offer long-term durability.
Require lifelong anticoagulation therapy to prevent thrombosis.
Bioprosthetic Valves (Biological Valves):
Do not generally require long-term anticoagulation; patients may switch to aspirin after an initial period on anticoagulants.
Have a limited lifespan due to structural deterioration over time.
Valve Replacement Procedure
Can be performed using traditional open-heart surgery or via a less invasive catheter-based approach (e.g., TAVR for the aortic valve).
The choice between mechanical and bioprosthetic valves often depends on patient factors, including age, lifestyle, and the ability to manage anticoagulant therapy.