Genetics - CH.16/15 - Mutation/Repair/Recombination
1/63
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
64 Terms
What are the two sources of genetic variation?
New mutations
Recombination mixing of old mutations
What are the pros and cons of experiencing mutations?
Pro: evolution of useful phenotypes and broadening of genetic information
Con: genetic diseases
Point Mutation:
an alteration ranging from a single DNA base pair to a small number of adjacent base pairs.
What are the two main types of point mutations?
Base insertions and deletions (indels)
Base substitutions
What are base substitutions and what are the two types of base substitutions?
Base substitution - replacement of one base pair with another.
transition
transversion
What is a transition base substitution?
The replacement of one base by another of the same chemical type —> purine to purine or pyrimidine to pyrimidine.
What is a transversion base substitution?
The replacement of one base by another of the opposite chemical type —> purine to a pyrimidine or vice versa.
Synonymous mutation:
Replacement of a codon for an amino acid with a codon for the same amino acid — causes a silent mutation.
Nonsynonymous mutation:
Mutation that changes a codon for an amino acid into a codon for a different amino acid — causes a missense mutation.
What are the two types of missense mutations? How do they work?
Conservative substitution — replacement of an amino acid with one of a similar chemical nature (i.e. both hydrophilic amino acids)
Nonconservative substitution — replacement of an amino acid with one of a different chemical nature (i.e. a hydrophilic amino acid is changed into a hydrophobic amino acid)
Nonsense mutation:
The codon for an amino acid is changed into a STOP codon (aka a nonsense codon).
Frameshift mutation:
The addition or removal of a single base pair in a coding sequence which alters the codon “reading frame” — causes indel mutations.
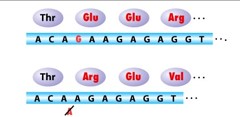
What can cause mishaps in removal of introns from genes?
Point mutations altering the splice site sequences of a gene.
This causes very large insertions or deletions into the reading frame based on where a new splice site is formed or where one is deleted.
How does the Duffy enhancer mutation cause resistance to _________ disease?
A mutation in the Duffy enhancer causes resistance to malaria.
The normal Duffy enhancer causes Duffy proteins to form on red blood cells, which allow the malarial parasite, Plasmodium vivax/knowlesi, to bind to the cell. A point mutation before the Duffy enhancer stops coding for these rbc proteins and the malarial parasite can no longer bind.
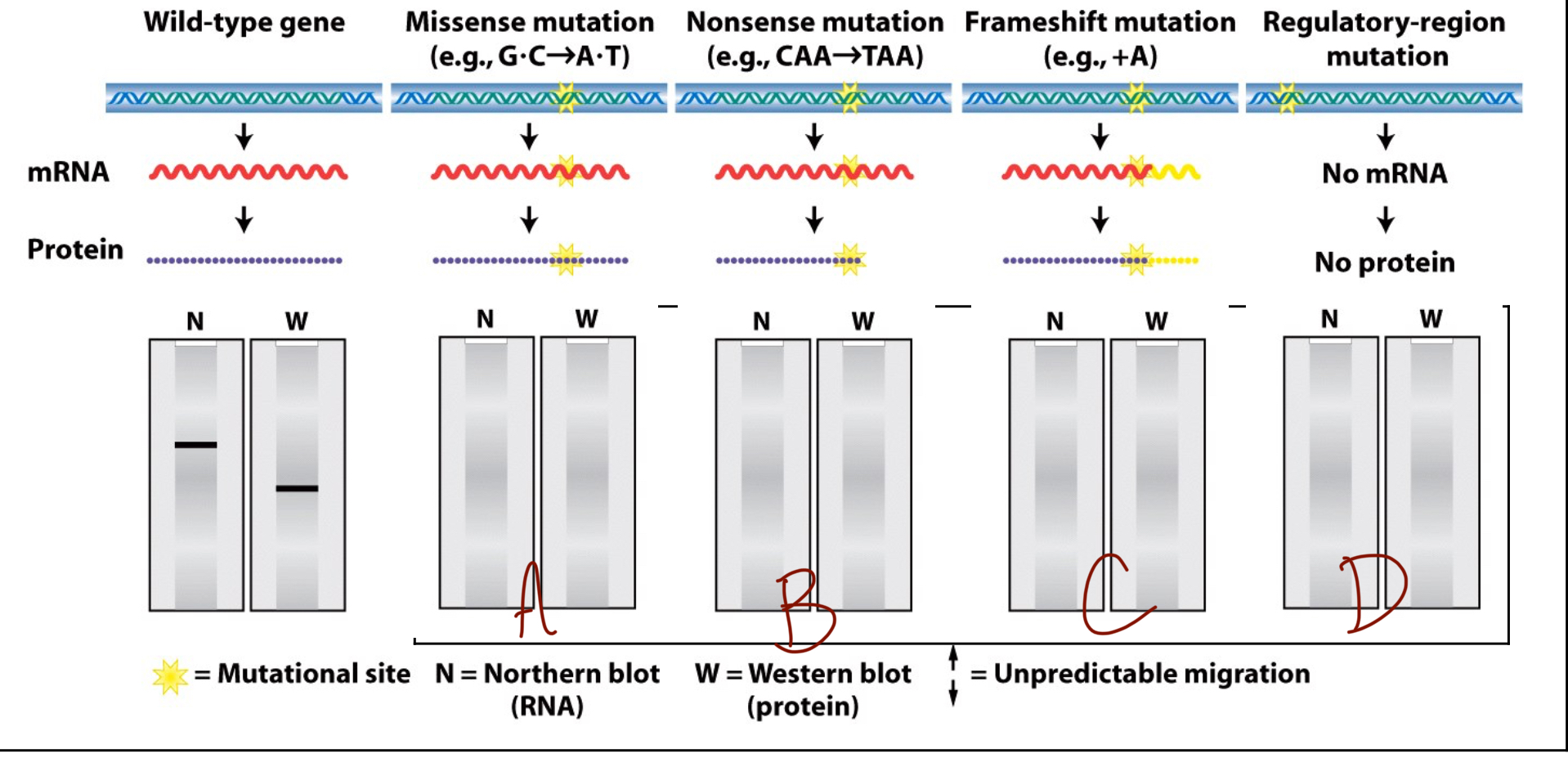
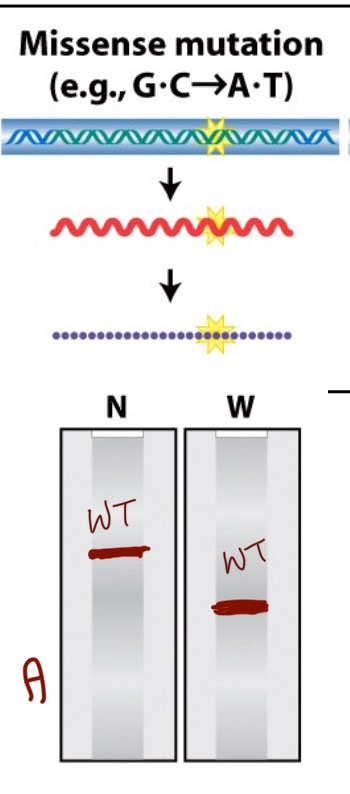
What does the northern/western blot look like for a missense mutation (A)?
Both northern and western blots look like wildtype because there has been no change to the amino acid, only to a single base in the RNA which does not dictate the amino acid.
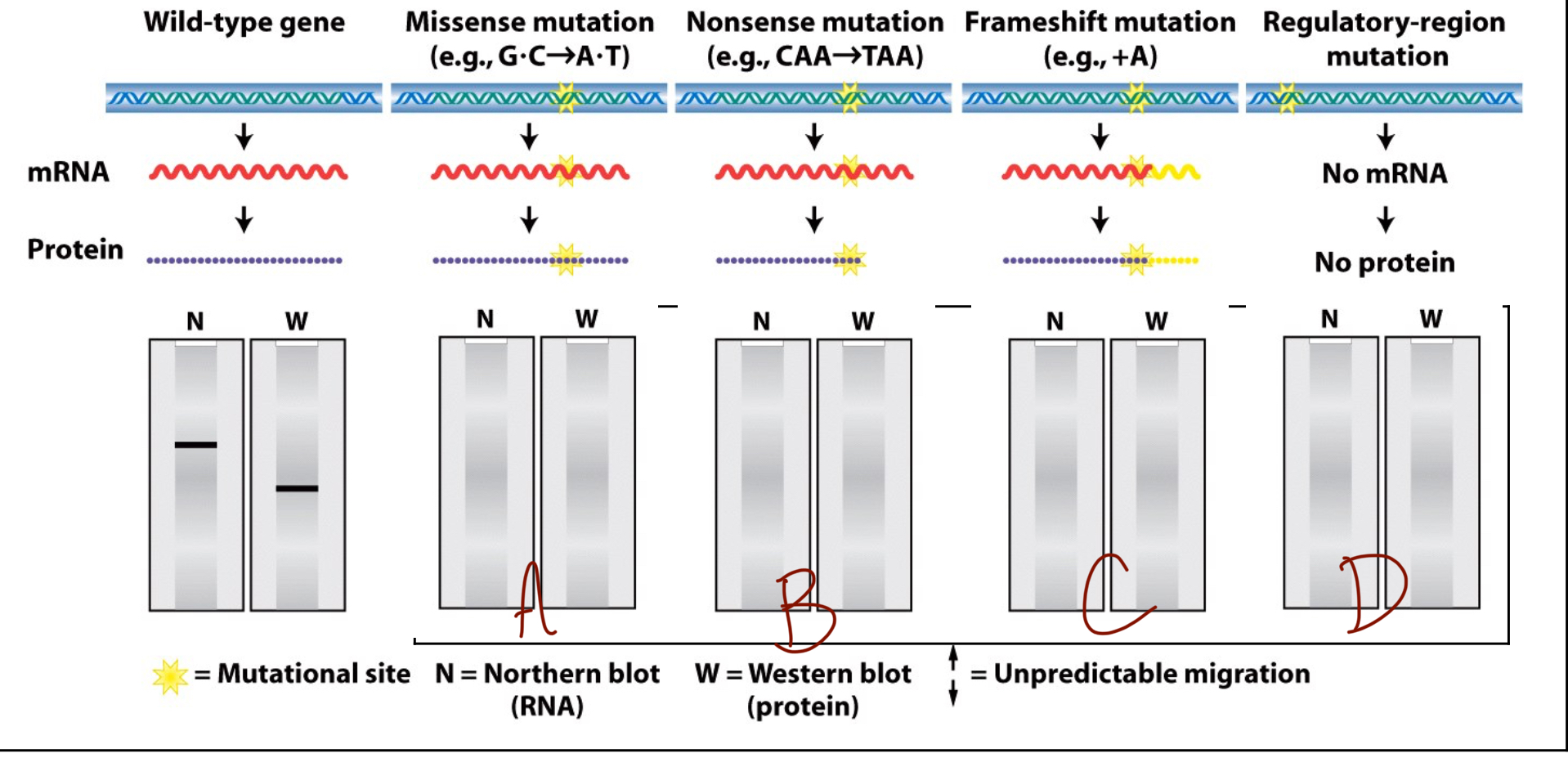
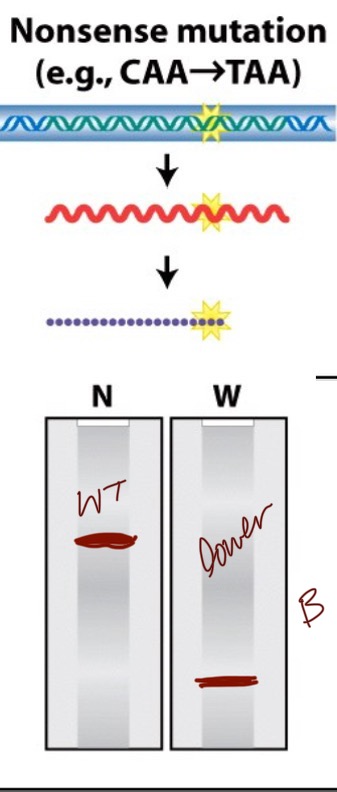
What does the northern/western blot look like for a nonsense mutation (B)?
The northern blot appears to be wildtype but the western blot is lower on the gel than the wildtype. This is because an RNA sequence is still formed of the same length but the STOP codon at the wrong location cuts the protein short.
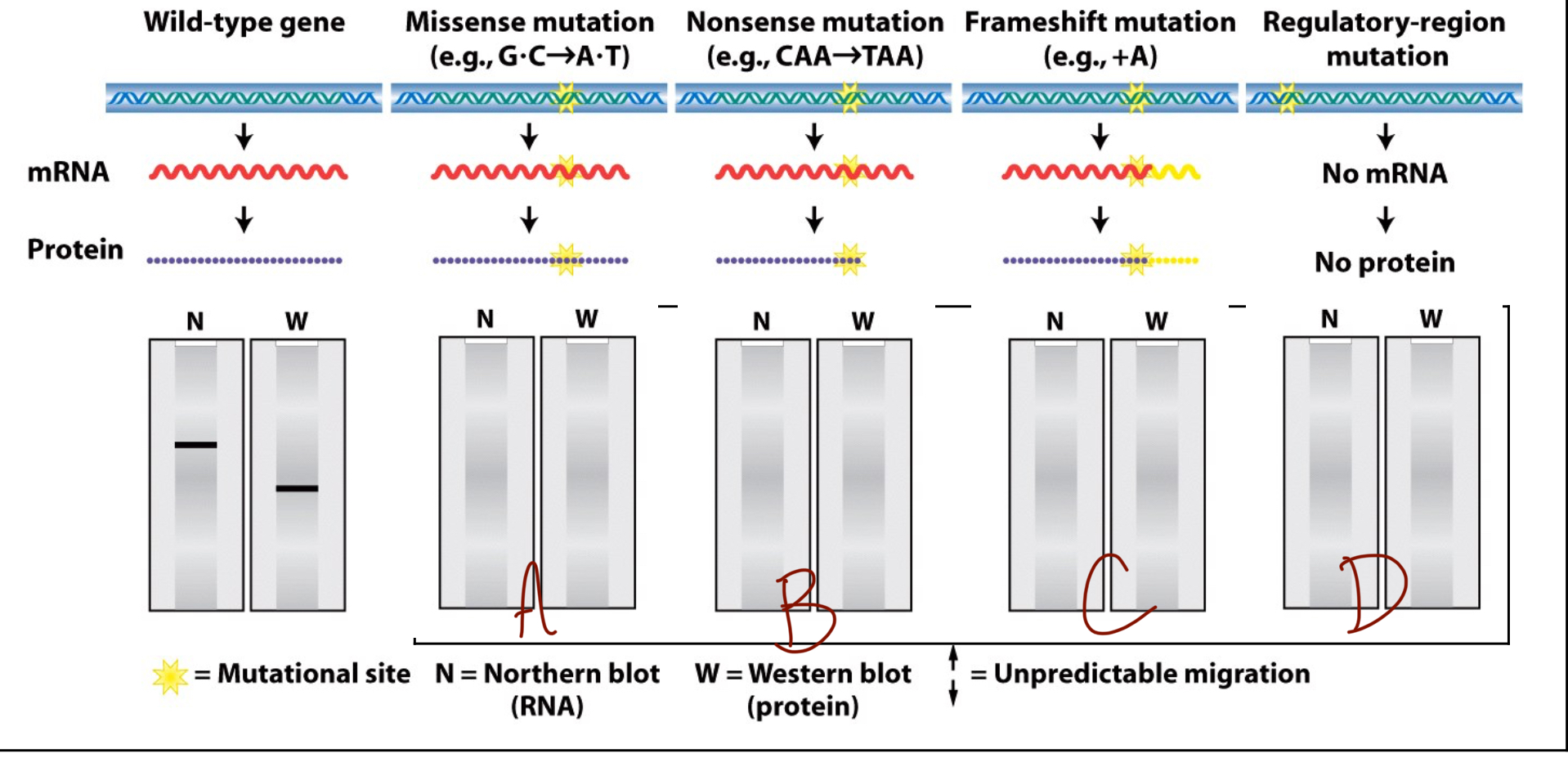
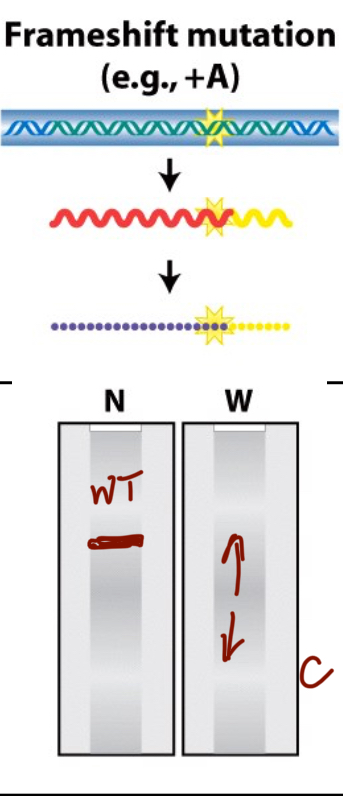
What does the northern/western blot look like for a frameshift mutation (C)?
The northern blot is still wildtype because the RNA sequence is still the same length, but the amino acid sequence is either longer or shorter depending on if the mutation is an insertion or a deletion to the reading frame.
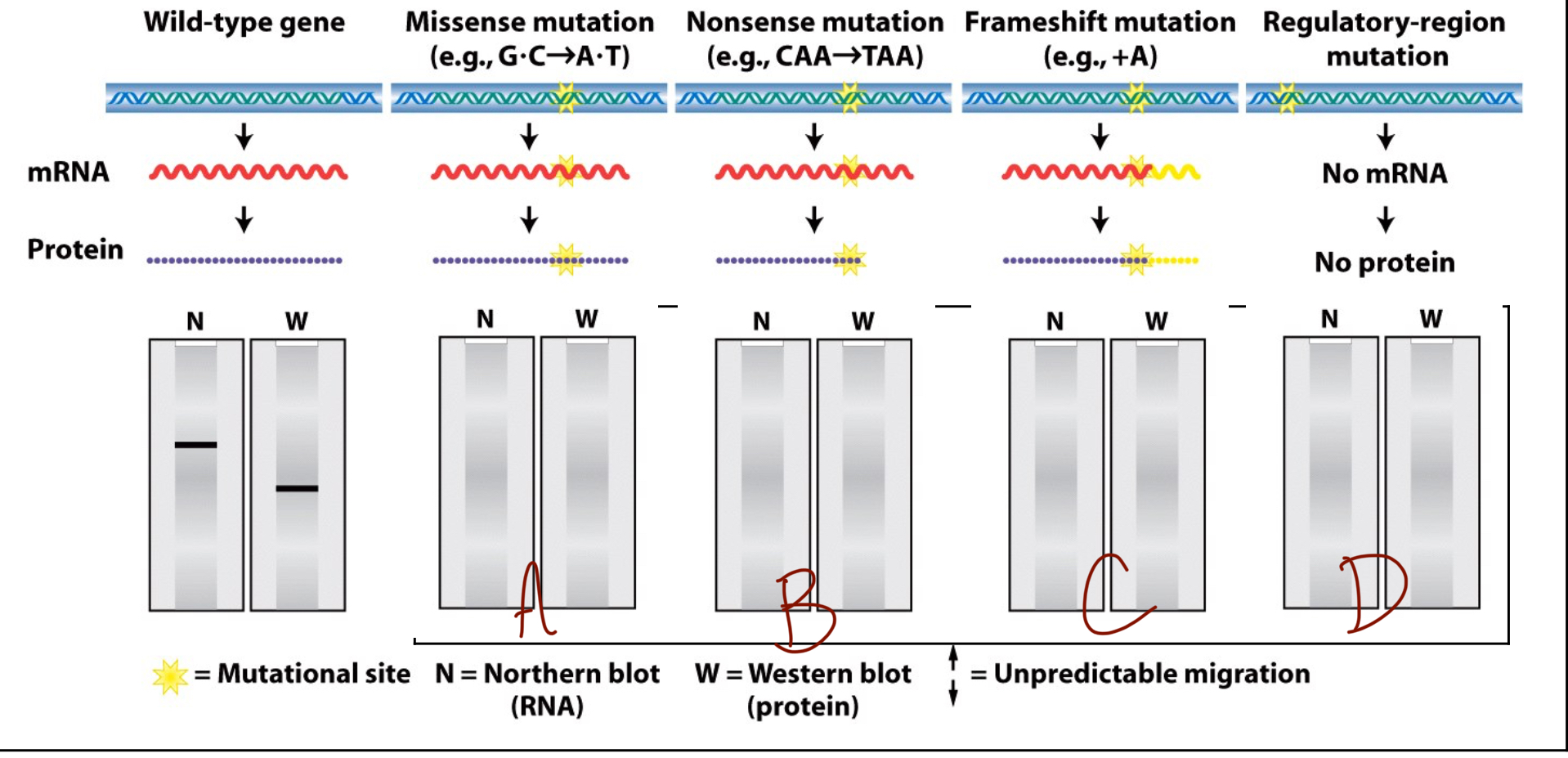
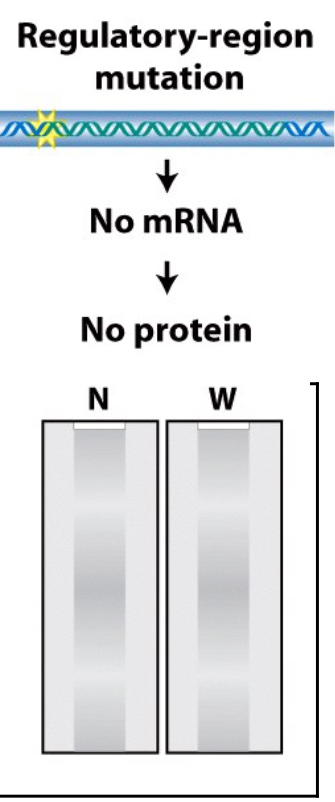
What does the northern/western blot look like for a regulatory-region mutation (D)?
This mutation does not allow an RNA sequence to form, meaning that there is no line on either the northern nor the western blot.
What are the two causes of mutations?
Spontaneous
Induced
Spontaneous mutation:
DNA mutations that are spontaneously/naturally produced in a cell by tautomeric shifts, indel mutations, or spontaneous lesions.
Induced mutation:
Mutations causes by environmental agents which cause mutations — mutagens.
What type of mutation do tautomeric shifts cause and why?
They cause transition mutations:
bases are normally in keto form, but tautomeric changes can lead to rare imino and enol forms of bases which cause errant bases to form during DNA replication.
What does adenine bind to when there is a tautomeric shift?
A rare imino form of cytosine:
C*-A instead of T-A
What does guanine bind to when there is a tautomeric shift?
A rare enol form of thymine:
T*-G instead of C-G
What does cytosine bind to when there is a tautomeric shift?
A rare imino form of adenine:
C-A* instead of C-G
What does thymine bind to when there is a tautomeric shift?
A rare enol form of guanine:
T-G* instead of T-A
What is it believed is the cause of indel mutations?
Slipped mispairing or slippage in repeated sequences.
What strand slips a base loop out to cause addition of a base pair?
The newly synthesized strand.
What strand slips a base loop out to cause deletion of a base pair?
The template strand.
What causes Huntington’s Disease?
A trinucleotide-repeat expansion.
Define genetic anticipation:
Increase in the number of repeats in successive generations infected with a disease (such as Huntington’s): this causes earlier age of disease onset and increased severity of the disease in every successive generation.
Spontaneous lesions:
Naturally occurring damage to DNA resulting from nucleotide depurination and deamination.
also, oxygen radicals
Depurination:
Causes inability to specify the complementary base to be added during DNA replication — the backbone is changed so that a nitrogenous base cannot be added.
Deamination:
Converts a cytosine to a uracil, which pairs with adenine during replication.
Oxygen radicals:
Can cause G to T transversions (different chemical type).
What are the four general mechanisms by which mutagens induce mutations?
Cause the replacement of a base (substitution).
Alter a base so that it specifically mis-pairs with the wrong complementary base.
Damages a base so that it can no longer pair with any base.
Intercalate between a base pair causing the insertion or deletion of a single nucleotide pair (indel).
How does UV light work as a mutagen?
UV light covalently bonds adjacent pyrimidines in the same DNA strand to form photodimers.
Base analogs:
Chemical compounds similar to normal nitrogenous bases which can be incorporated into a DNA strand.
What do base analogs do?
They have distinct base pairing properties that can cause the incorrect nucleotide to be incorporated during replication.
Alkylating agents:
Add alkyl groups to the four types of bases which can result in the occurrence of transition mutations - causes mispairing during replication.
ex. EMS and NG idk what that means
Intercalating agents:
Planar molecules that can insert between the stacked bases at the core of the double helix - causes indels
ex. agent orange, proflavin
What does the Ames Test determine?
It determines the mutagenic potential of compounds
tests for compounds themselves and after they are metabolized by the body.
What are the steps to completing the Ames Test?
extract liver enzymes (from mice)
mix enzymes with auxotrophic bacteria unable to synthesize histidine and whatever chemical compound is under study
Compare the number of “revertants” (colonies surviving on histidine deficient medium due to mutations from the chemical under study) to controls where the compound was not provided
What does it mean during the Ames Test if a chemical added to bacteria WITHOUT liver enzymes grows but it does not grow with liver enzymes?
The chemical itself is a mutagen, but the metabolite of the chemical is not a mutagen.
What does it mean during the Ames Test if a chemical added to bacteria WITHOUT liver enzymes grows and it grows with liver enzymes?
The chemical under study is a mutagen by itself and as a metabolite.
What does it mean during the Ames Test if a chemical added to bacteria WITHOUT liver enzymes does not grow but it does grow with liver enzymes?
The chemical itself is not a mutagen, but the metabolite of the chemical is a mutagen.
How does DNA proofreading work?
DNA pol1 and DNA pol3 excise mismatched base pairs (3’ to 5’ exonuclease activity) and allows a second chance to insert the correct base into the growing strand.
Rate of mutation in a healthy cell:
rate of DNA damage = rate of DNA repair
Direct reversal:
does not require breaking the phosphodiester backbone
does not require a template
requires a specific enzyme
What are two ways that direct reversal fixes DNA damage?
photolyase
MGMT: a methyltransferase enzyme
How does single stranded damage get repaired and what are the three modes of repair?
Single stranded damage is repaired by utilization of the undamaged strand as a template.
Involves:
base excision repair (BER)
nucleotide excision repair (NER)
mismatch repair
Base excision repair:
Repairs damage to a single nitrogenous base using the enzyme glycosylase to create AP site - does not break backbone but leaves a hole where the wrong base was (AP site).
Nucleotide excision repair:
Repairs bulky, helix distorted damage.
most evolutionarily conserved mechanism
Removes only 12-24 nucleotides surrounding damage
Mismatch repair:
Post replication repair found in all cells.
What are the two modes of double stranded break repair
Nonhomologous end joining (NHEJ)
Homologous recombination
Nonhomologous end joining:
error prone but fast (30 min)
Proteins bind to broken ends - protect and create sticky ends for DNA ligase
Homologous recombination:
Error free but slow
uses sister chromatid or homologous chromosome during late S phase of cell division after DNA replication
similar to mechanism of crossing over
Translesion synthesis:
Alternative polymerases are used to bypass pyrimidine dimers or AP-sites for proks and euks:
have larger active site
some are prone to errors
How do cancer cells differ from normal cells?
rapid cell division rate
higher metabolism
abnormal shape
ability to invade new cellular territories
What are the things that mutations change that can increase a cells ability to become cancerous?
increase a cells ability to proliferate or divide
decrease a cells susceptibility to undergo apoptosis
What types of genes are mutated in cancerous cells?
Oncogenes
Tumor-suppressor genes
Oncogenes:
genes that when mutated act dominantly to contribute to tumor formation
gain of function
only one mutation needed to contribute
Tumor suppressor genes
genes that when mutated act recessively resulting in the loss of a gene or protein’s normal function
loss of function
one mutation is fine, but two stops the gene from suppressing tumor creation
p53
Activates DNA repair proteins in response to DNA damage
Arrests cell growth to allow DNA repair, preventing mutations
Initiates apoptosis if DNA cannot be repaired
SERVES TO STOP CANCER FORMATION