Week 1: The kidney
1/36
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
37 Terms
What does the cortical nephrons do?
Removal of waste and reabsorption of nutrients
What does the Juxtamedullary nephorns have?
concentration of urine
What does the Glomerulus do?
filters small solutes from the blood
What does the proximal convoluted tubule do?
reabsorbs ions, water, and nutrients; removes toxins and adjusts filtrate pH
What does distal tubules do?
selectively secretes and absorbs different ions to maintain blood pH to maintain blood pH and electrolyte balance
What does collecting duct do?
reabsorbs solutes and water from the filtrate
What is the ascending loop of henle?
reabsorbs Na+ and Cl- from the filtrate into the interstitial fluid
What is the descending loop of henle?
aquaporins allows water to pass from the filtrate into the interstitial fluid
What does the Kidney do?
makes urine
What does the ureter do?
moves urine
What does the urinary bladder do?
stores urine
What does the urethra do?
releases urine
What is the normal chemical composition of urine?
Urine is an aqueous solution of greater than 95% water, with a minimum of these remaining constituents, in order of decreasing concentration:
Urea 9.3 g/L.
Chloride 1.87 g/L.
Sodium 1.17 g/L.
Potassium 0.750 g/L.
Creatinine 0.670 g/L .
Other dissolved ions, inorganic and organic compounds (proteins, hormones, metabolites).
Describe the function of vasopressin (antidiuretic hormone)
presence of vasopressin increases passive reabsorption of water (your body collect more water)
Where is vasopressin secreted by?
hypothalamus
What does vasopressin trigger?
absorption of water by collecting ducts
What is vasopressin released by
hypovolemia or hypernatremia
What renin secretion can tigger release vasopressin?
Angiotensin II
What can inhibit vasopressin release?
Ethanol
Explain the function of nephrons?
are the functional units of the kidney, with each kidney containing about 1-1.5 million nephrons. Nephrons are responsible for the processes of filtration, reabsorption, secretion, and excretion, which ultimately produce urine.
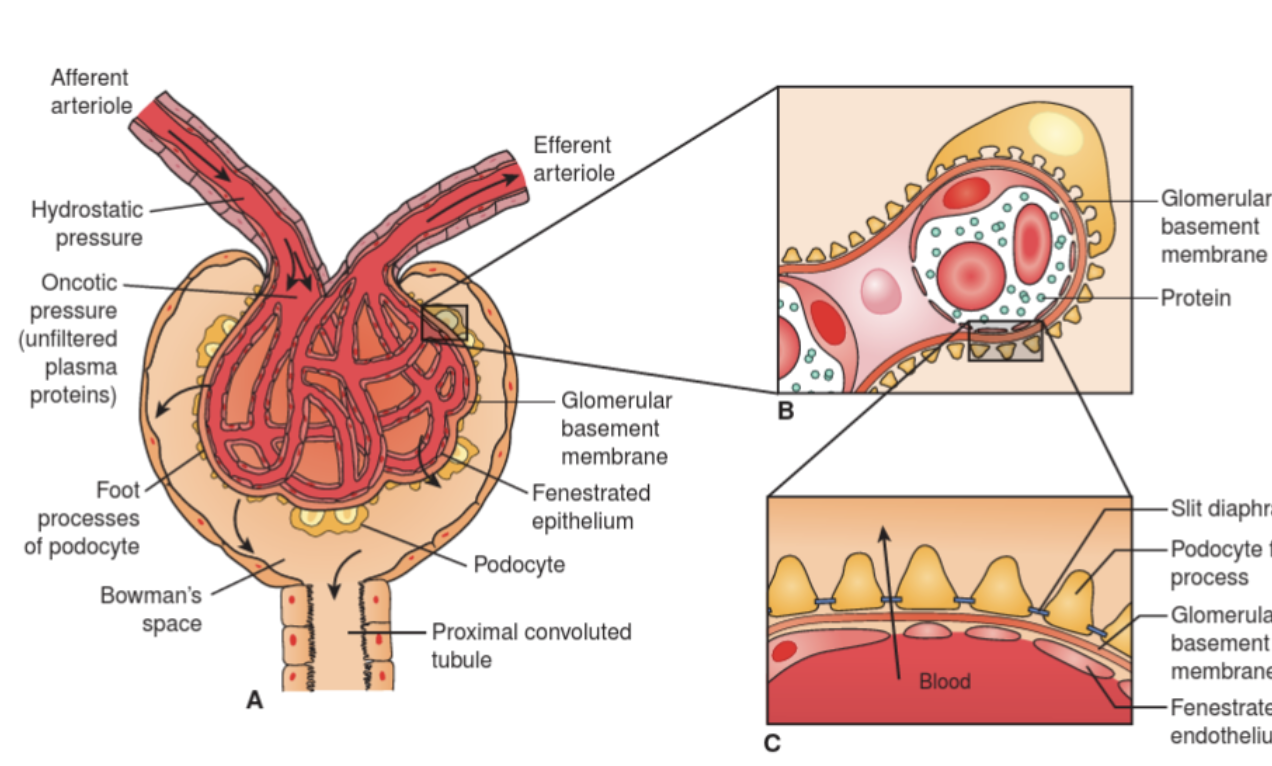
Describe the glomerulus.
Is a nonselective filter.
A ball of tiny capillaries. Capillary blood vessels walls have pores that let small wastes and water pass from the blood into the tubular system. The pores keep larger substance (proteins) in the blood.
A sac called a Bowman’s capsule surrounds each glomerulus. Each glomerulus and Bowman’s capsule together from a renal corpuscle, the filtering unit of the kidneys.
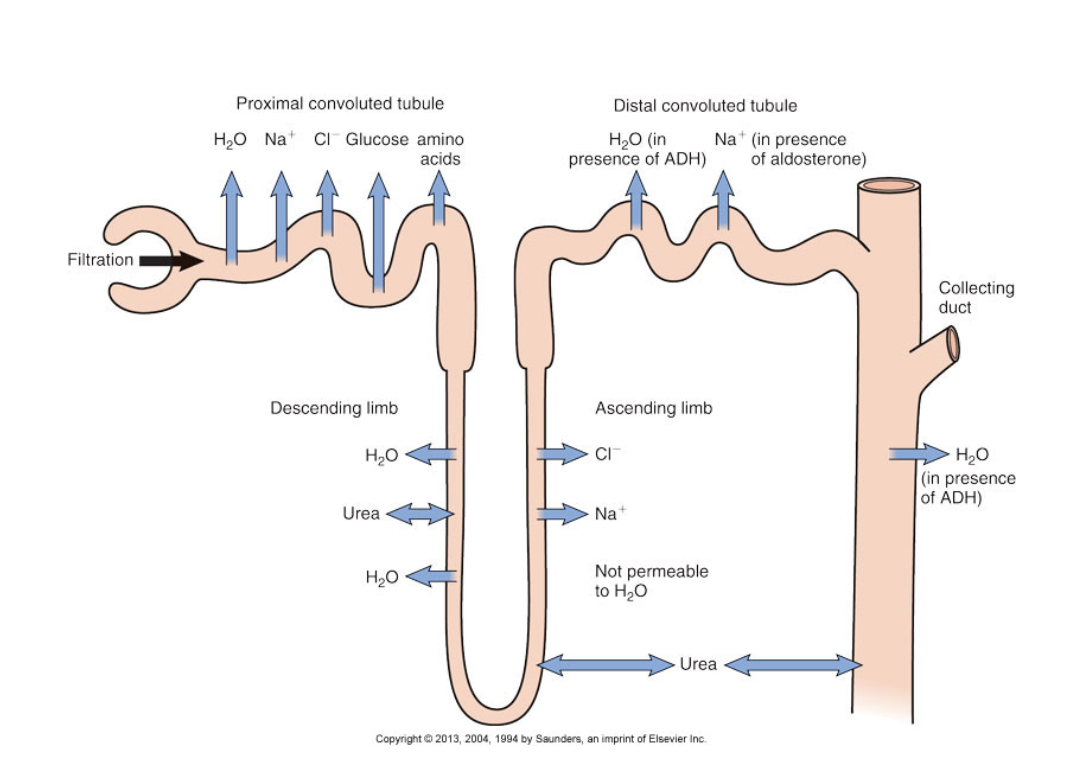
Describe Proximal convoluted tubules.
reabsorbs and secretes substances.
Active reabsorption of glucose, amino acids, salts, bicarb
Passive reabsorption of water, urea, and chloride
Secretion: medications bound to proteins typically, meds attach to tubular cells and transported, H+ ions
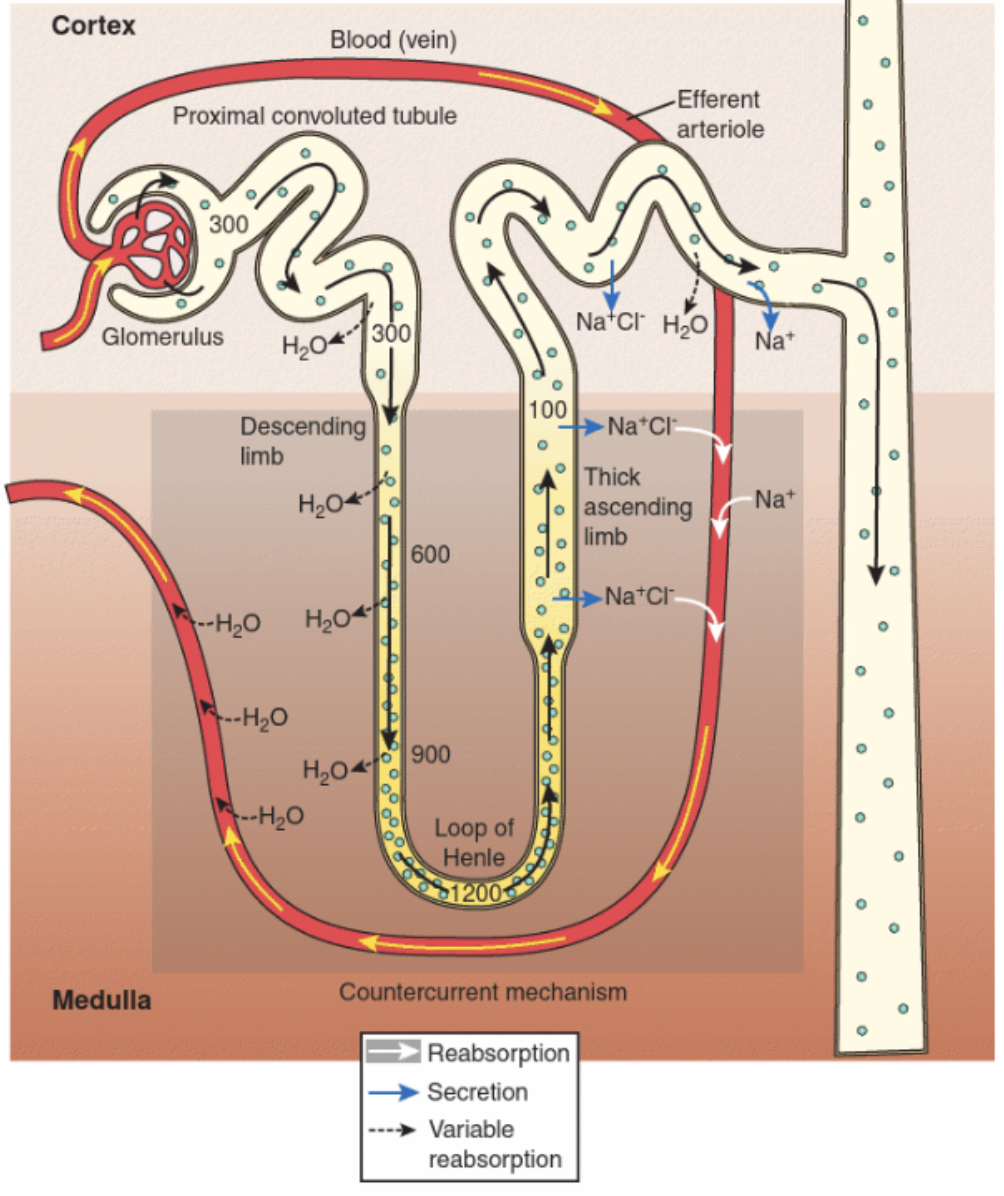
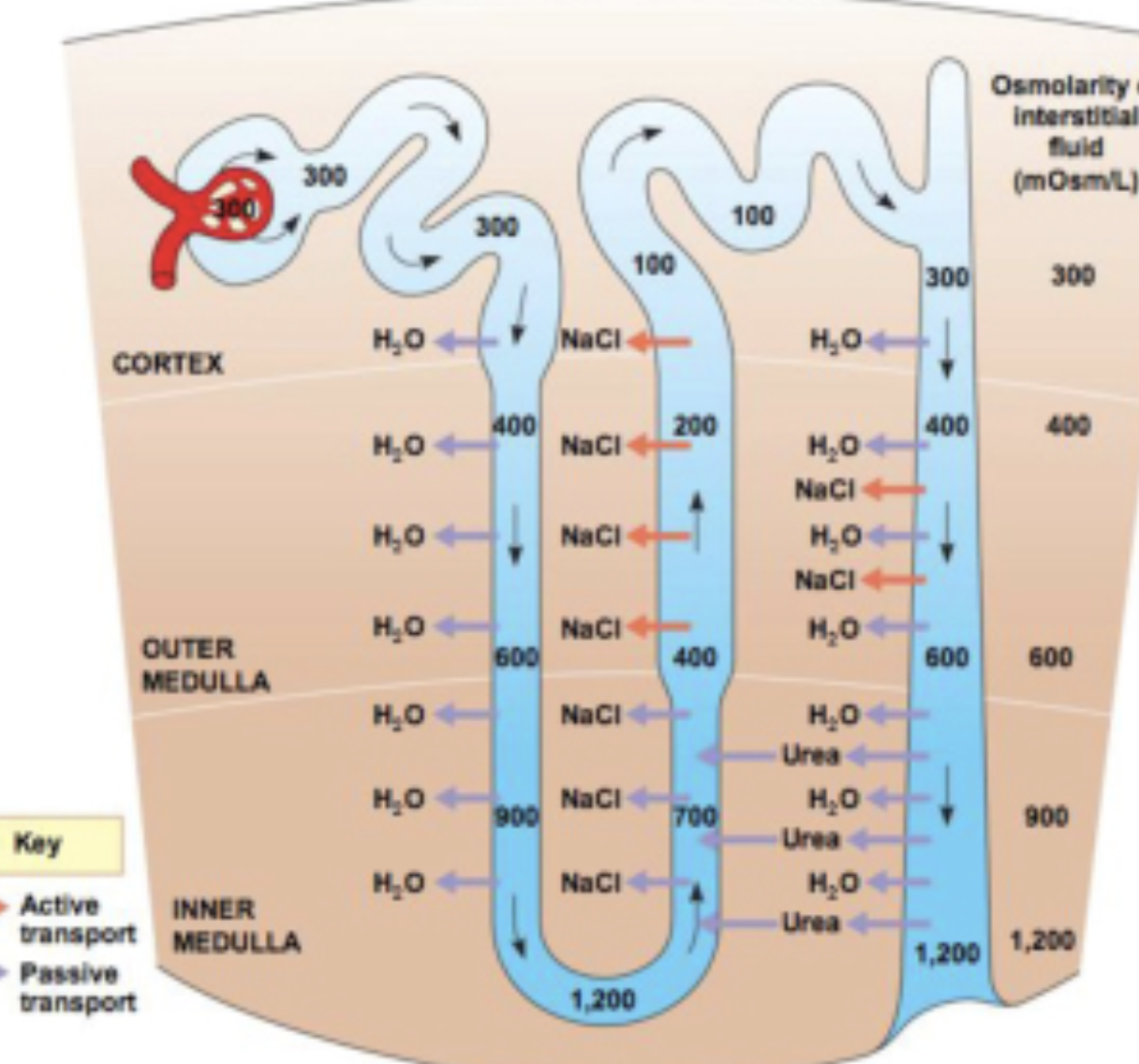
Describe of loop of henle.
Primary function is to concentrate urine.
Goes down into medulla
Descending loop: water passively reasborbed by osmosis
Ascending loop: impermeable to water, Na and Cl are reabsorbed
Describe distal convoluted tubule:
reabsorption of potassium, sodium, calcium, and water.
Ammonia can also be secreted to manage pH
Describe collecting duct.
the final touches, influenced by vasopressin (drug), ammonia can also be secreted to manage pH
How does the kidney manage pH?
kidney help mantain pH balance by excreting acids in the urine.
Kidney also make and absorb bicarbonate, a buffer that will neutralize acid and keep acid-base within a safe range.
H+ freely pass through glomerulus, bicarbonate reabsorbed by secreting H+ (proximal convoluted tubule), H+ secreted by proximal convoluted tubule and will bind to phosphate.
Ammonia produced by cells and H+ will follow (can be done in PCT or DCT)
What does EPO (erythropoietin) do?
hormone made by cells in our kidneys when they detect low levels of O2 in our blood. EPO tells BM to make more RBCs when more oxygen is needed.
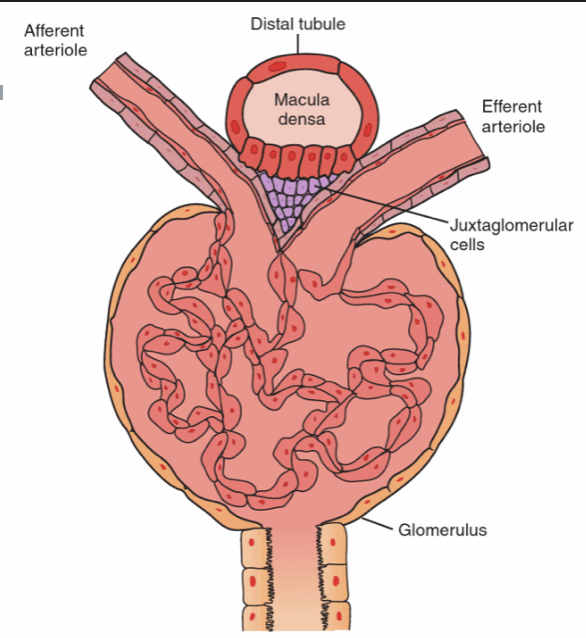
How does the Renin-Angiotensin-Aldosterone System or RAAS work?
juxtaglomerular apparatus detects low bp, Renin secreted by juxtaglomerular cells.
Renin turns hormone angiotensinogen, made by the liver, into angiotensin I.
Angiotensin I is converted (reacts with ACE) into angiotensin II by the lungs.
What does Angiotensin II causes?
constricts (tightens) blood vessels. Vasoconstriction
Vasodilation of the afferent arteriole
Reabsorption of Na
Release of Aldosterone (causes sodium reuptake and K+ secretion) (forcing the kidneys to keep in water and salt.
Release of vasopressin (ADH)
What is diabetes mellitus?
Excessive sugar in the bloodstream (type I and II)
Leads to excessive urination
Body reabsorbs glucose typically unless blood levels > 160-180 mg/dl. Glucose in urine.
What is diabetes insipidus?
Excessive urination
Vasopressin deficiency
Vasopressin resistance
Can produce >20 L of urine daily; no glucose in urine
What is the normal about of urine produce daily?
1-4L
What is Inulin clearance?
as a test that measures the glomerular filtration rate (GFR) by injecting a bolus dose of inulin and collecting timed urine samples to assess inulin concentration in the plasma and urine. It is considered the ‘gold standard’ for estimating GFR, despite being a complex procedure.
100% passes the kidneys
What is BUN (blood urea nitrogen)?
measures the amount of urea nitrogen in your blood. Urea nitrogen is a waste product that forms as your body breaks down proteins. It's carried in your blood and then removed by your kidneys when you urinate (pee).`
What is creatinine?
waste product of muscle metabolism
What is Glomerular Filtration Rate?
Volume of plasma in milliliters that is completely cleared of a substance per unit of time.
It estimates how much blood passes through the glomeruli each minute
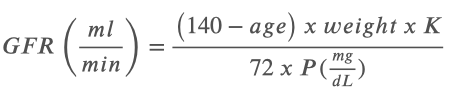
What is eGFR (estimated glomerular filtration rate)?
Estimated glomerular filtration rate
Only needs plasma value for creatinine
Uses gender and age constants to calculate
K= 0.85 for women and 1.00 for men