Gastric Motility and Function
1/67
Earn XP
Description and Tags
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
68 Terms
waves of rhythmic depolarization of intestinal smooth muscle cells propagate along length of gi tract
pacemaker potentials of stomach
basal electric rhythmn
differes in various segments
3 cpm in stomach, 12 cpm in duodenum
pacemaker network of cells in stomach small intestine and large intestine
interstitial cells of Cajal
does the pacemaker potential of BER initiate action potentials of its own in smooth muscle
no, stimulation of ENS or hormonal input is needed
what is receptive relaxation and what triggers it
the drop in gastric pressure after eating
stomach must relax as volume increases → reservoir
persists til all solids emptied
NO and VIP are released when mechanoreceptors triggers intrinsic and vasovagal reflexes
why do we have receptive relaxation
it delays gastric emptying until the duodenum is ready
how does the duodenum contribute to receptive relaxation
fat adn protein in duodenum also distend duodenum → release CCK → binds CCK1 → delay gastric emptying
what reflex induces need to defecate shortly after eating a meal
gastrocolic reflex
what reflex relaxes ileocecal valve in response to gastric distension
gastroileal reflex
rapid phasic contractions of stomach
circumferential, start from gastric pacemaker near antrum and move toward pylorus
fluid and small particles <2 mm empty into duodenum
solid meal gastric lag
1 hr before emptying begins
chronic disorder char by delayed emptying of the stomach after eating in the absence of mechanical obstruction like pyloric stenosis
gastroparesis
neuromuscular dysfunction, derangements in extrinsic control, intrinsic nerve dysfunction, cells in local control of gi muscle function and loss of function of smooth muscles
causes of gastroparesis
idiopathic
DM
iatrogeni/post surg
neurological disorders
viral or bacterial infection
gastroparesis association/causes
gastroparesis sx
postprandial fullness, N/V, belching, bloating
tx for gastroparesis
antiemetics, prokinetic drugs, dietary mods, PPI, pyloric botulinum toxin injection
primary role of small intestine
digest components of meal and absorb nutrients into blood stream or lymphatics
what compoounds stimulate smooth muscle contractions in ENS
ACh, substance P
what stimulates smooth muscle relaxation in ENS
VIP and NO
what is the motility pattern of the small intestine during fed state
not to propel but to mix contents with digestive secretions and prolong exposure to absorptive epithelium
propel it slowly
segmentation and peristalsis
once the meal is absorbed the intestine converts to
MMC, migrating motor complex (house cleaning)
describe the migrating motor complex
occurs between meals, fasting state
pattern of motility repeating every 90 minutes to 2 hours
what stimulates the MMC
motilin from M cells during fasting
surpressed during feeding
role and sinificance of the colon
reabsorb water
process feces
colon in fasting states
not part of MMC
biased toward mixing and retaining contents for prolonged periods of time
periodically have large propulsive contractions to transfer contents to rectum and promote urge to defecate
high amplitude propagating contraction of the large intestine
provides mass movement of chyme and feces
poor motility in colon →
greater absorption and hard feces/constipation
excess motility in colon →
diarrhea or loose feces
contains both circular and longitudinal smooth muscle and is under involuntary control
internal anal sphincter
encircle rectum and contains only striated muscle but is controlled by voluntary and involuntary mechanisms
external anal sphincter
resting tone 40-60 mmHg
if passive distension of rectum is large enough →
triggers active contraction of rectal smooth muscles
triggers relaxation of smooth muscle on internal anal sphincter (rectosphincteral reflex) via VIP and NO
if defecation is not desired
skeletal muscle of external anal sphincter contracts by involuntary reflex
increased tone prevents leakage, involuntary control
slow transit constipation
slow movement of feces through large intestine → large dry hard feces bc excess fluid absorption
hirchsprungs disease
congenital megacolon
ENS fails to develop appropriately
defecation reflexes and strong peristaltic motility cannot occur in area of large intestine
segment remains contracted → functional barrier to passage of feces, dams up area and causes megacolon in ascending transverse and descending colon (ganglion cells in myenteric plexus of sigmoid colon is the problem)
stomach secretions
acid, pesinogen, mucus, bicarb, intrinsic factor, water
stomach humoral agents
gastrin, somatostatin
largest portion of the stomach
corpus
stomach area with no acid secreting parietal cells
cardia
most distal region of the stomach
antrum
between cell types and within cell types there is what
cellular heterogeneity throughout (epithelial in antrum vs body very different)
contains gastric glands with variety of secretory cell types and its secretory products
corpus of the stomach
acid, pepsinogen, intrinsic factor
secrete acid and IF necessary for b12 absorption in the ileum
parietal cells (oxyntic)
secrete pepsinogens that are active as pepsins (active by low ph, intitaie protein digestion)
chief cells
chief cells and parietal cells are found in what part of the stomach
corpus
other cell types in corpus
mucus secreting cells in neck of gastric gland
epithelial cell
endocrine cell
enterochromaffin like cells to release histamine
water also secreted
antrum cells
glands DO NOT contain parietal cells
chief cells
epitelial cells
enodcrin cells
g cells → gastrin
d cells → somatostatin
two pathways for acid secretion
direct
stimulate parietal cell directly
indirect
stimulate ECL cell to secrete histamine which acts on parietal cell
Gq → PLC → IP3 and DAG
ACh
CCK2 or CCK1 receptor (Gq)
gastrin
Gs → AC → cAMP → PKA
histamine
stimulation causes cytoskeletal rearrangement of
parietal cells
steps of acid secretion
h-k pump activated (p type atpase)
extrusion of h into lumen in exchange for k
secretion of Cl into gland lumen
results in active secretion of HCL
active secretion of HCL leads to what intracellularly
increased pH → passive uptake of h2o and co2 for conversion to bicarb and h+ by carbonic anhydrase
bicarb gets exchanged for cl- at basolateral surface
gastric acid secretion stimulation summary
Vagus nerve and ENS stimulate parietal directly →ach
ecl cells → histamine
inhibits d cell release of somatostatin (via ach)
stimulates g cells vis GRP
products of protein digestions directly stimulate
g cells to release gastrin
regulation of gastric acid secretion inhibition summary
somatostatin is major
luminal H+ stimulates d cells to release somatostatin
inhibits gastrin
inhibits ecl histamine release
inhibits acid release from parietal cells directly
phase of acid scretoin before food enters stomach
cephalic phase
sights smells and tastes of food
20% of secretion
vagus
phase of secretion after food enters stomach
gastric phase
stimulates vasovagal and enteric reflexes and gastrin
65% of acid secretion
phase pf acid secretion where food is in upper duodenum
intestinal phase
small amounts of gastric acid in stomach
10% acid secreted
what protects the gastric surface
gastric diffusion barrier
what gives gastric diffusion barrier its impermeability to acid
apical membrane and gastric gland tight junctions
3 parts of the gastric diffusion barrier
tight junctions that help make it impermeable to acid at apical membrane
mucous gel on surface epithelial cells
bicarb containing microclimate next to epithelial cells
increased acid secretion due to elevated levels of gastrin usually due to a tumor
zollinger ellison syndrome
what tumors usually cause zollinger ellison syndrome
gastrinoma
pancreatic cell adenoma
what happens with gastrin in zollinger ellison syndrome
gastrin’s release is unregulated/not under phsyiological control
fasting gastrin level is elevated in almost all patients
leads to ulcers
patients lack parietal cells
cannot secrete ____ and ____
pernicious anemia
H+ and IF
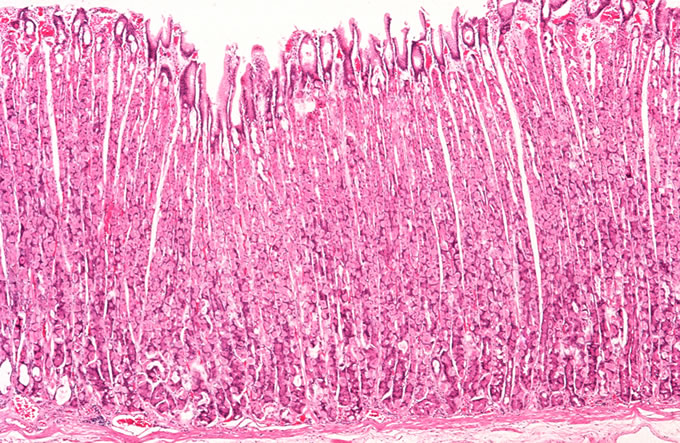
hyperplasia of parietal cells is noted in what
zollinger ellison syndrome
low somatostatin, no D cells stimulated
gastrin secretion is high with almost no H+ secretion
no b12 (cobalamin) absorption
pernicious anemia
no parietal cells