Lecture 19 - Blood and Lymph (in progress)
1/146
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
147 Terms
Connective tissue made up of cellular elements and an extracellular matrix
Blood
Erythrocytes, leukocytes, platelets
Cellular elements
Fluid - mostly water, perpetually suspends the formed elements
Extracellular Matrix (plasma)
Enables formed elements to circulate throughout the body within the cardiovascular system
Extracellular Matrix (plasma)
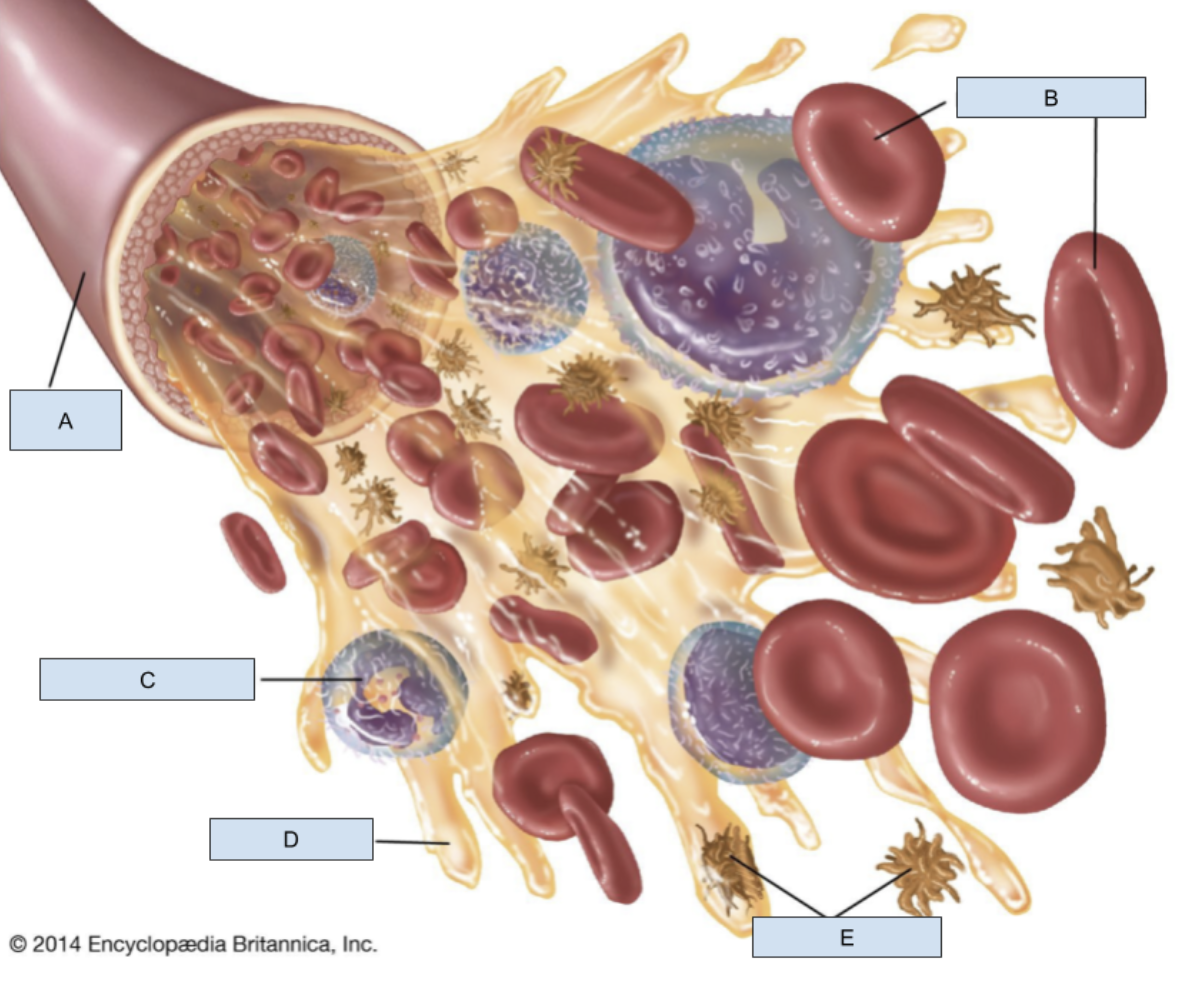
A?
Blood vessel
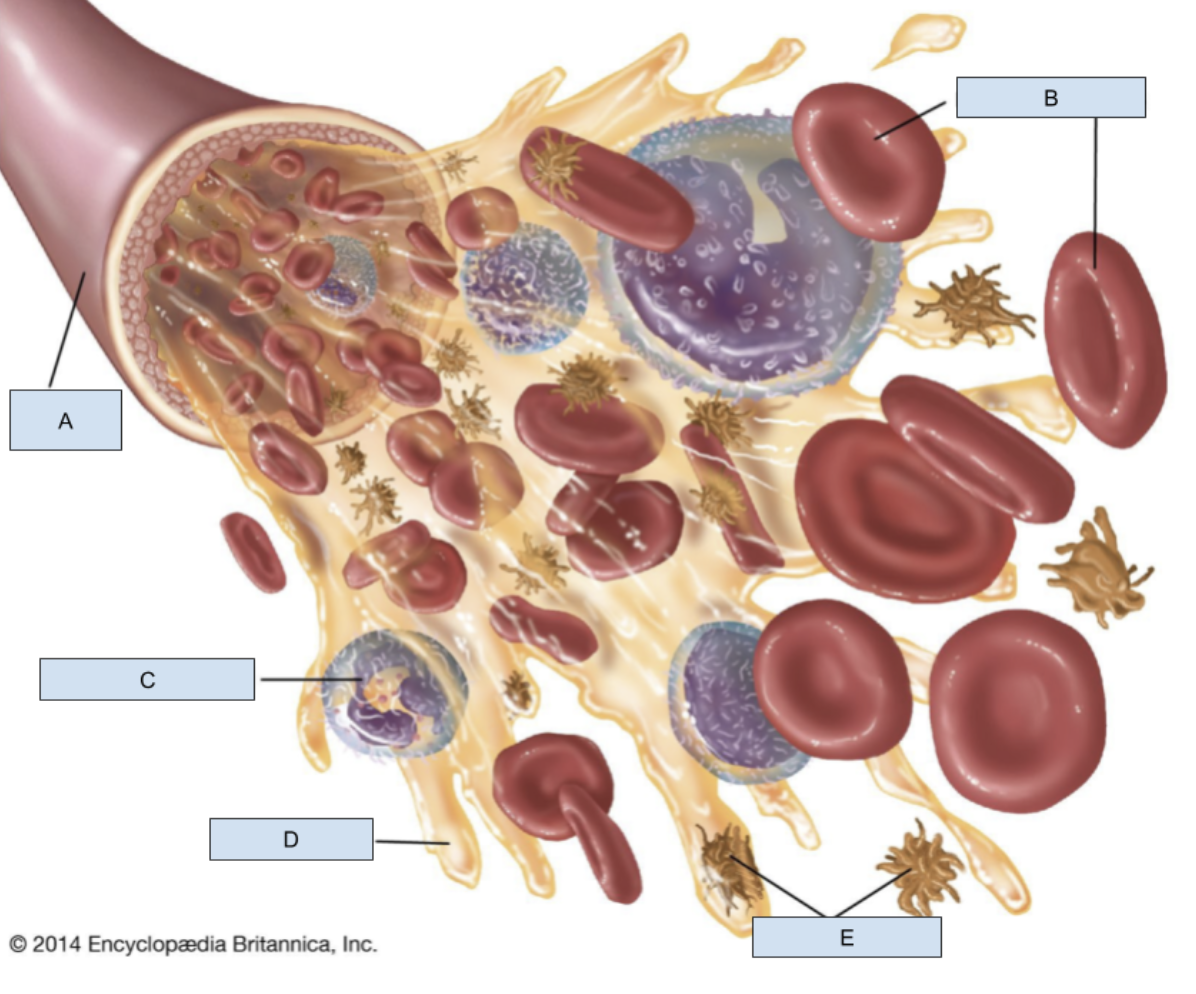
B?
RBCs
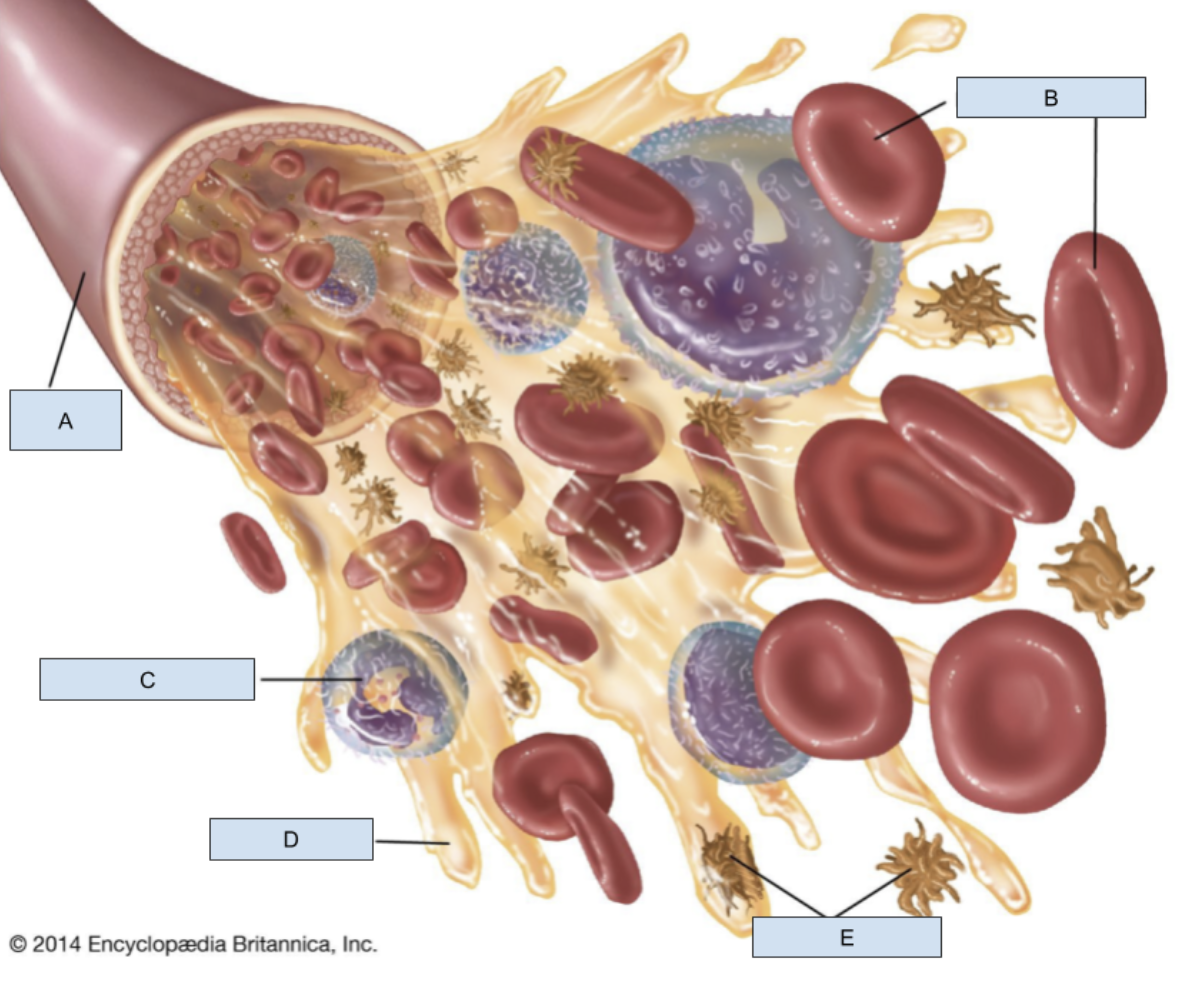
C?
WBC
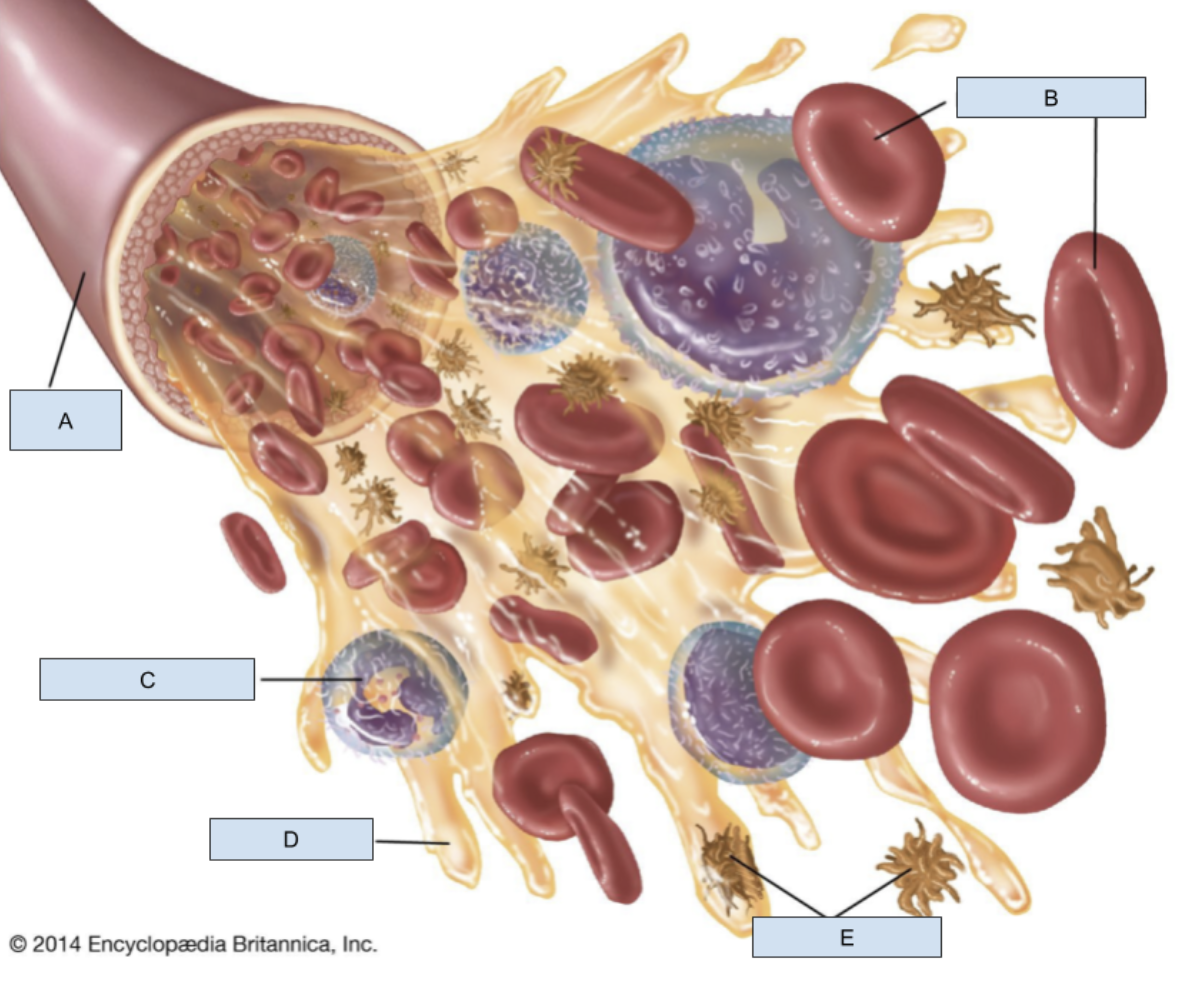
D?
Plasma
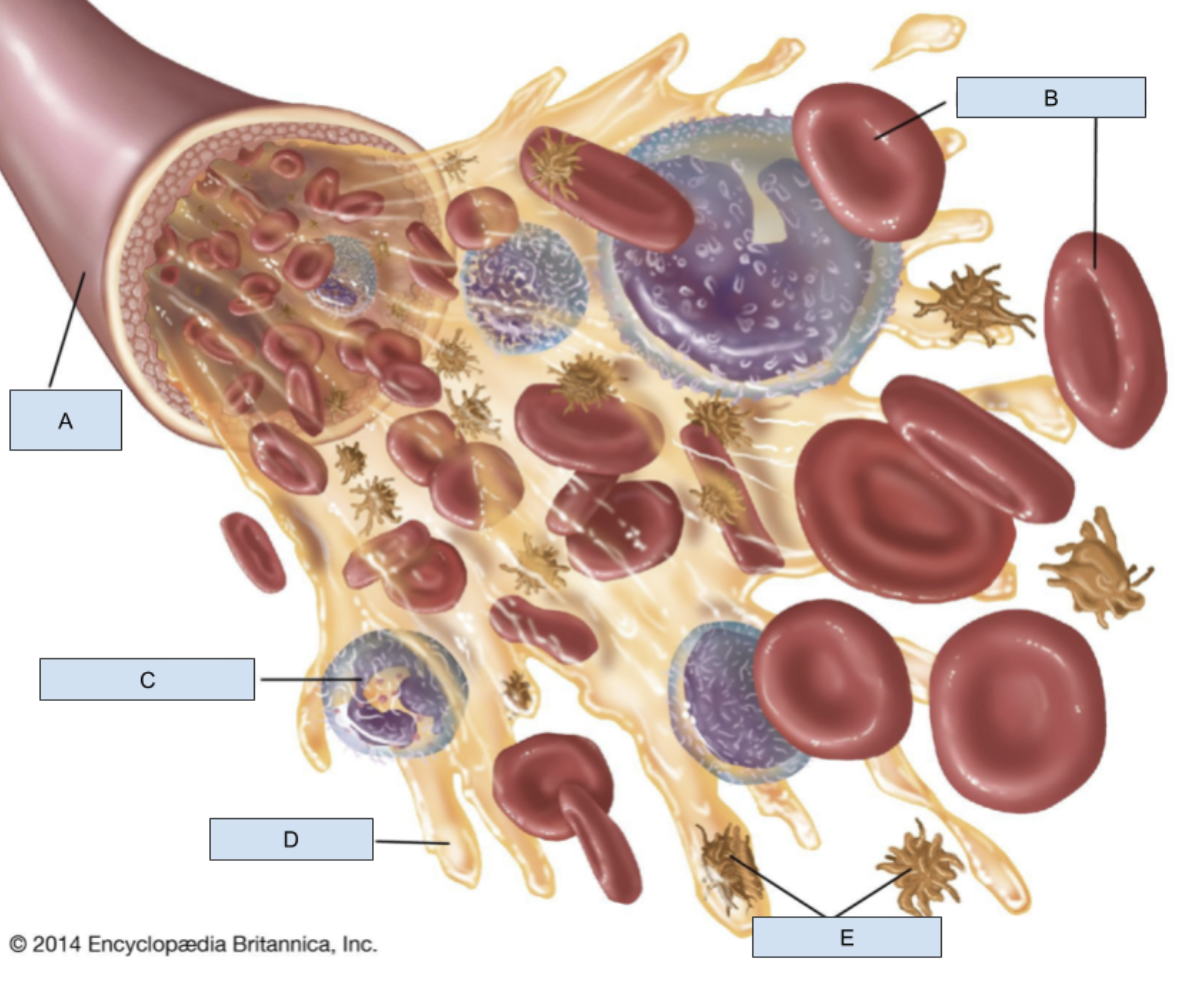
E?
Platelets
% of water in plasma
92%
Dissolved or suspended within plasma water is a mixture of substances, most of
which are
Proteins
Number of protein types in plasma
100s
Most abundant plasma protein
Albumin
What organ manufactures albumin
Liver
Serve as binding proteins clotting (transport vehicles for fatty acids and steroid hormones)
Albumin
Three main subgroups of globulins
Alpha, beta, gamma
Globulins that transport iron, lipids, and the fat-soluble vitamins A, D, E, and K to the cells
Alpha and beta
Globulins involved in immunity, better known as antibodies or immunoglobulins
Gamma
Plasma protein for blood clotting
Fibrinogen
What organ manufactures fibrinogen
Liver
Blood component for gas transport
Erythrocytes
Biconcave disk shape maximizes surface area in which blood component
Erythrocytes
RBC nucleus-free cytoplasm packed with what?
Hemoglobin (Hb)
Iron-rich protein found in red blood cells that is responsible for transporting oxygen throughout the body
Hemoglobin (Hb)
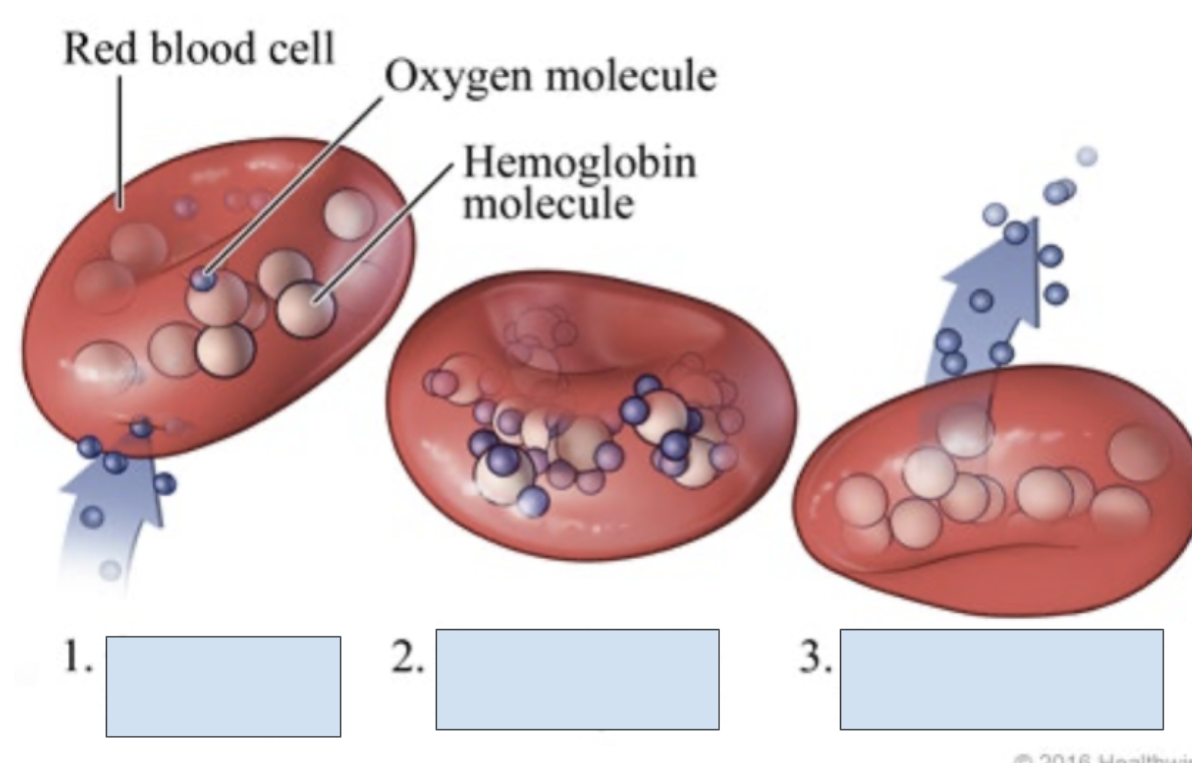
What is happening in step 1?
RBC receives blood from lungs
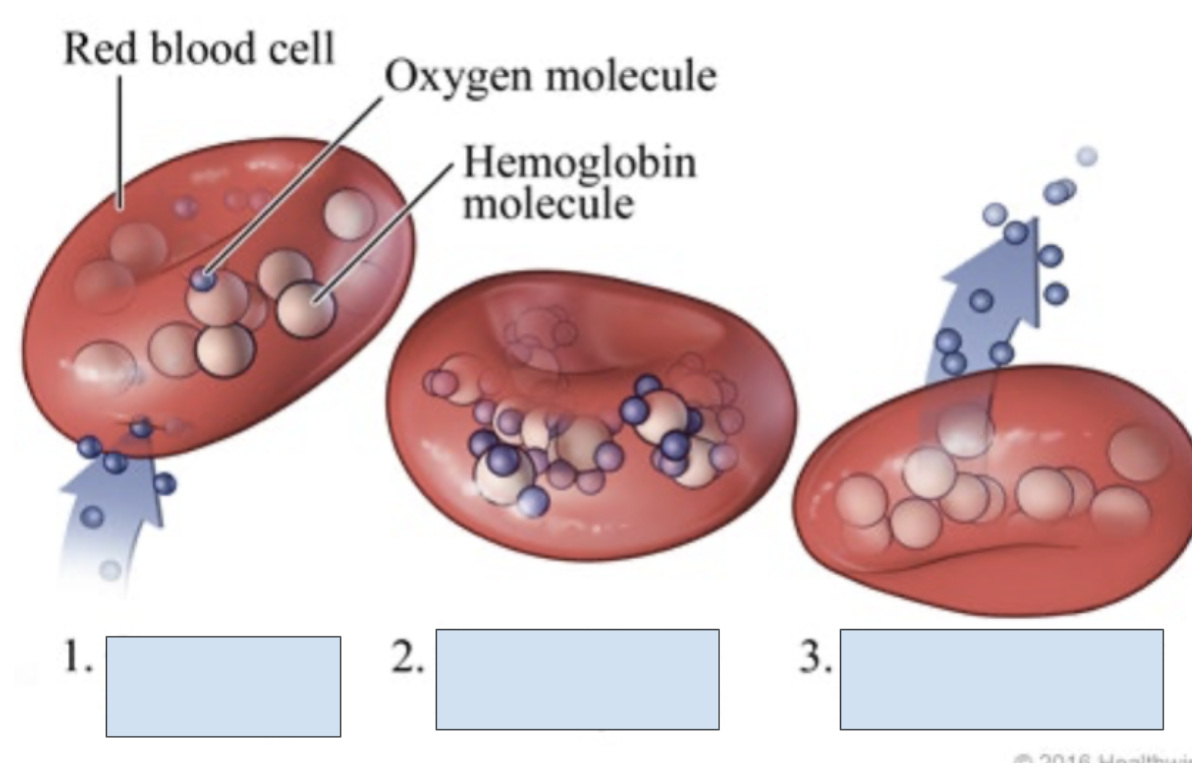
What is happening in step 2?
Oxygen bonds to hemoglobin
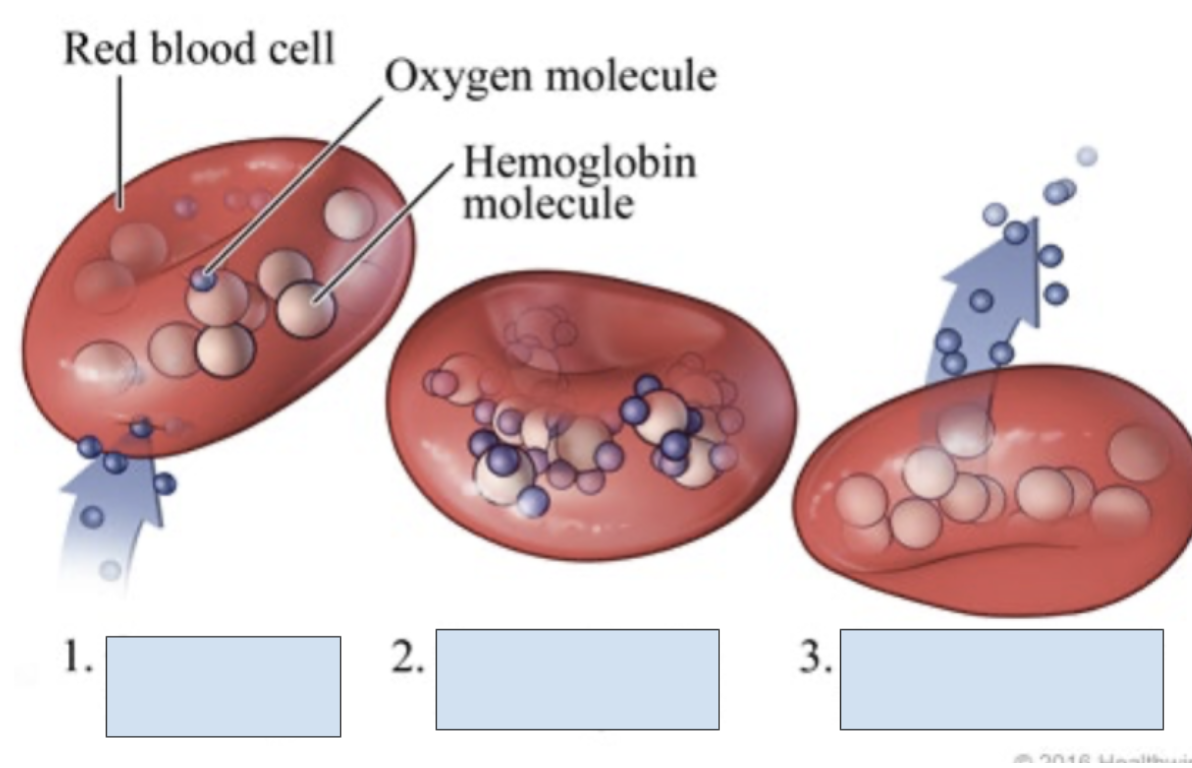
What is happening in step 3?
Oxygen is released to tissue cells
Each Hb molecule can carry _____ molecules of oxygen
Four
What % of CO2 can be carried by RBCs
<2%
Number of circulating RBCs in an adult
25 trillion
Number of hemoglobin molecules on one RBC
260 million
How many days do RBCs remain in the bloodstream
120
Erythrocytes produced per second
2-3 million
Protein released from liver (and kidney) in response to low O2
Erythroprotein
Triggers erythrocyte produced in bone marrow
Erythroprotein
Nutrients needed for erythrocyte production
Folic acid, iron, vitamin B12 (FIB)
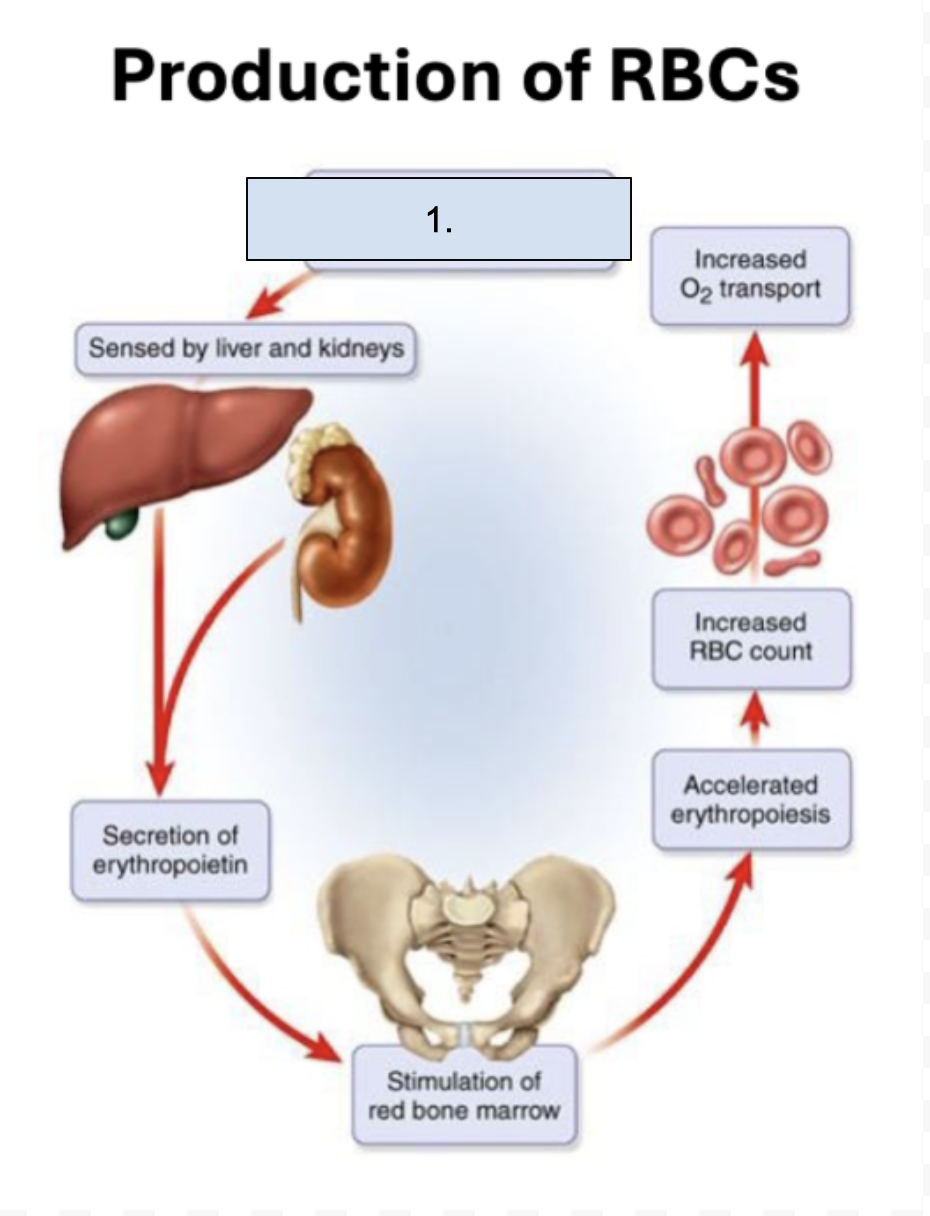
What is happening in this step?
Hypoxemia
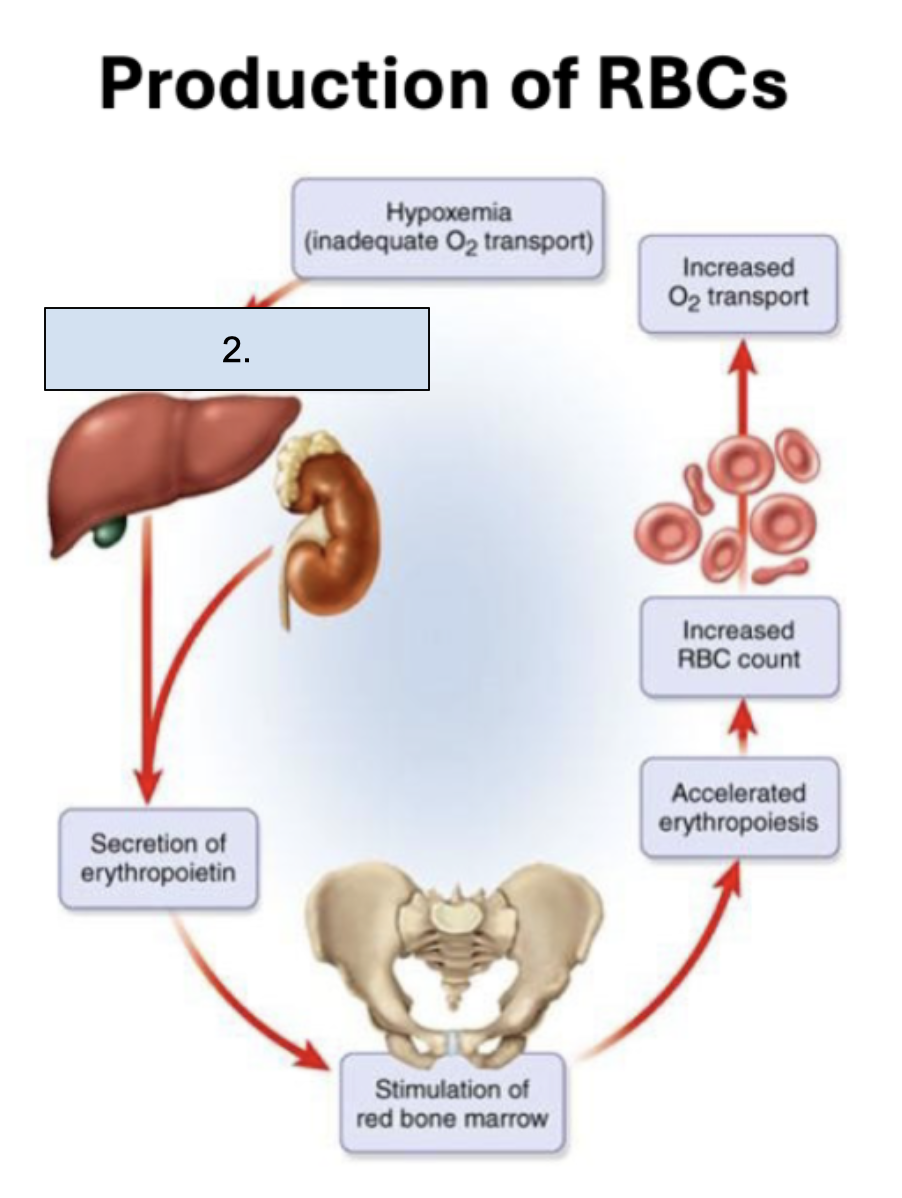
What is happening in this step?
Low O2 sensed by liver and kidneys
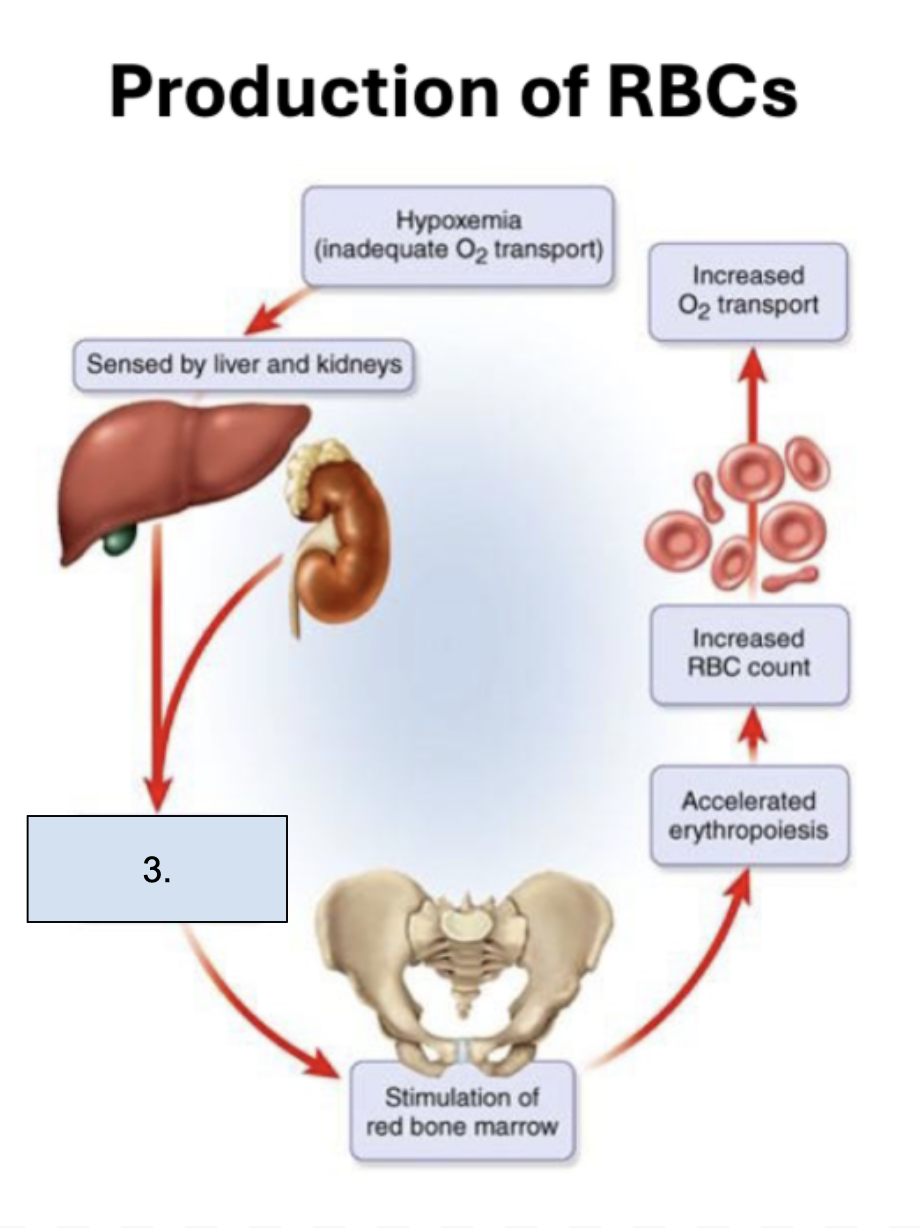
What is happening in this step?
Erythroprotein secretion
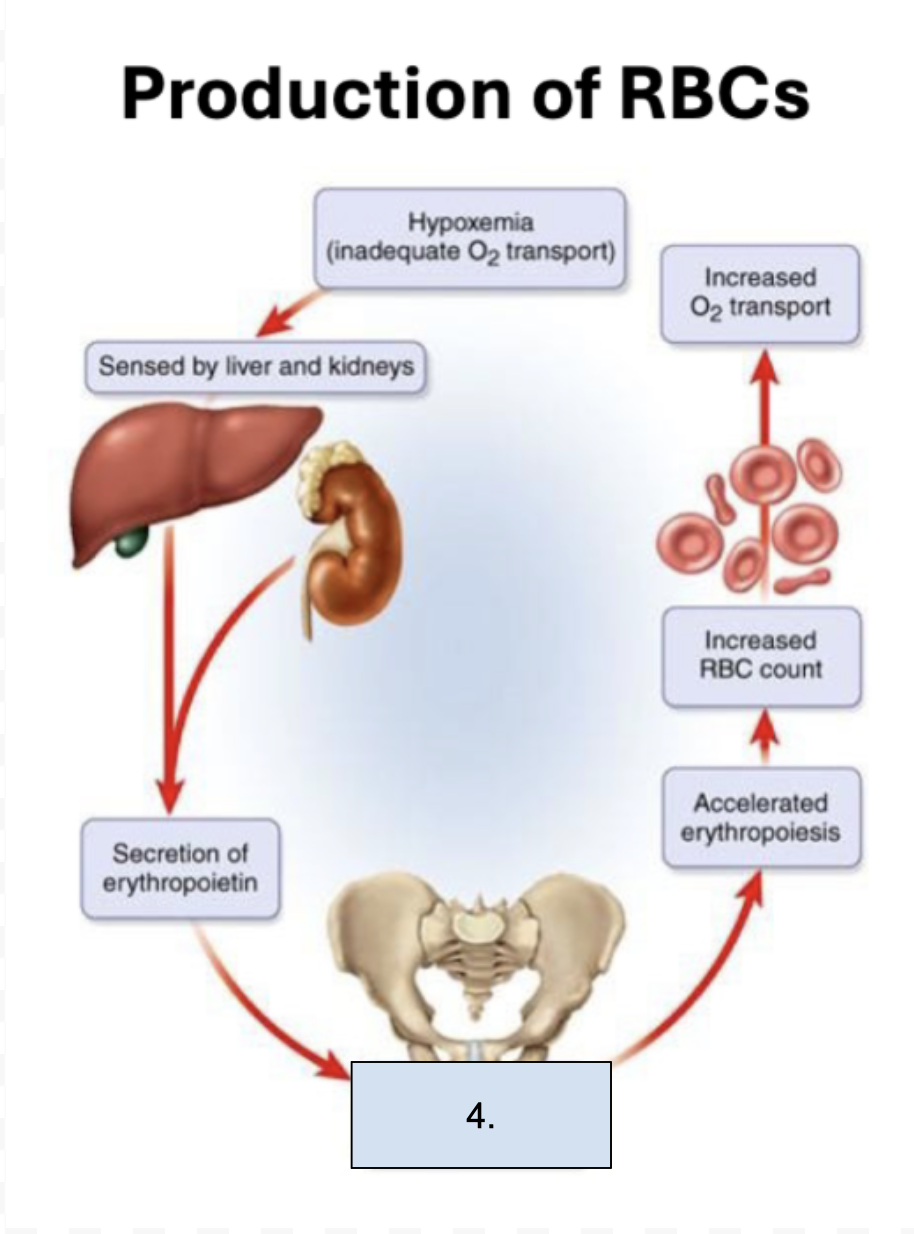
What is happening in this step?
Red bone marrow secretion
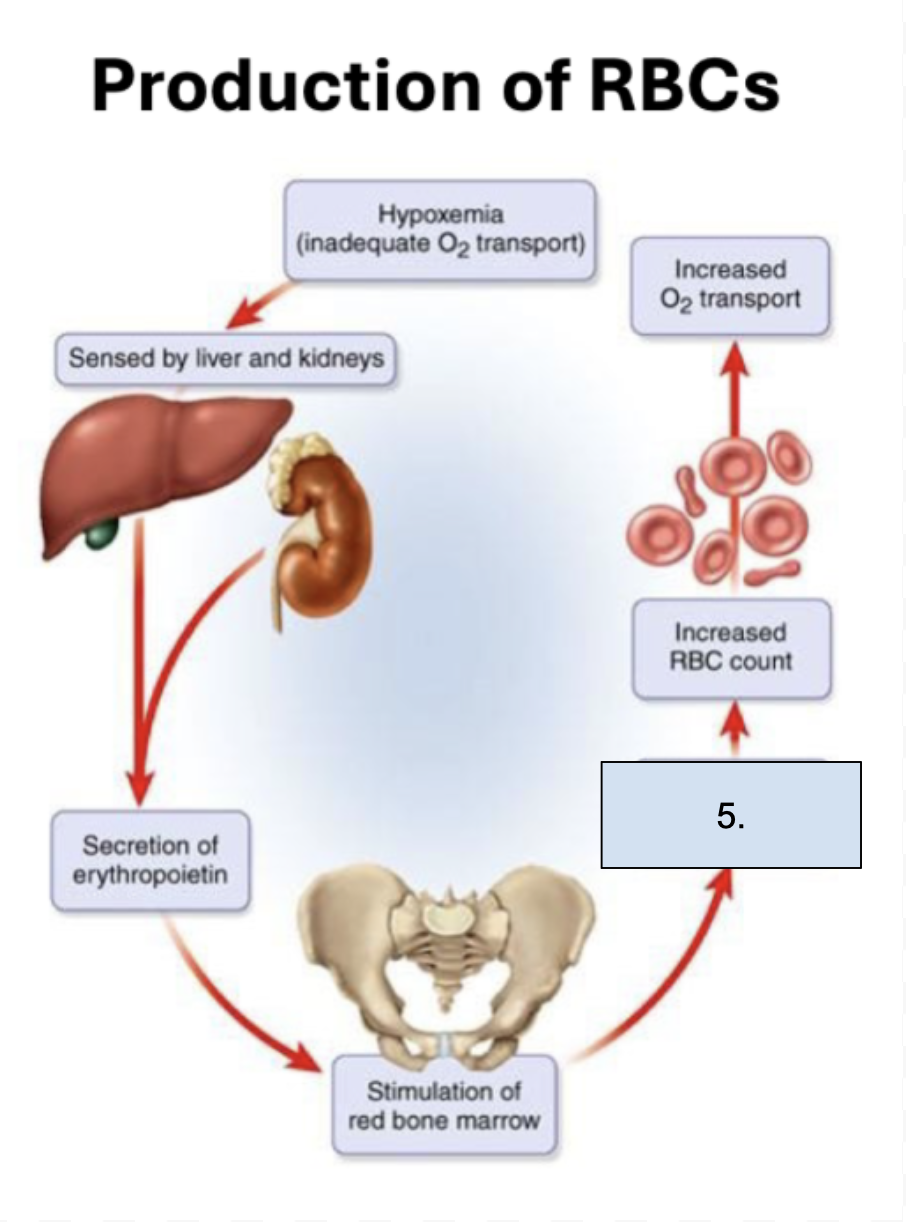
What is happening in this step?
Accelerated erythropoiesis
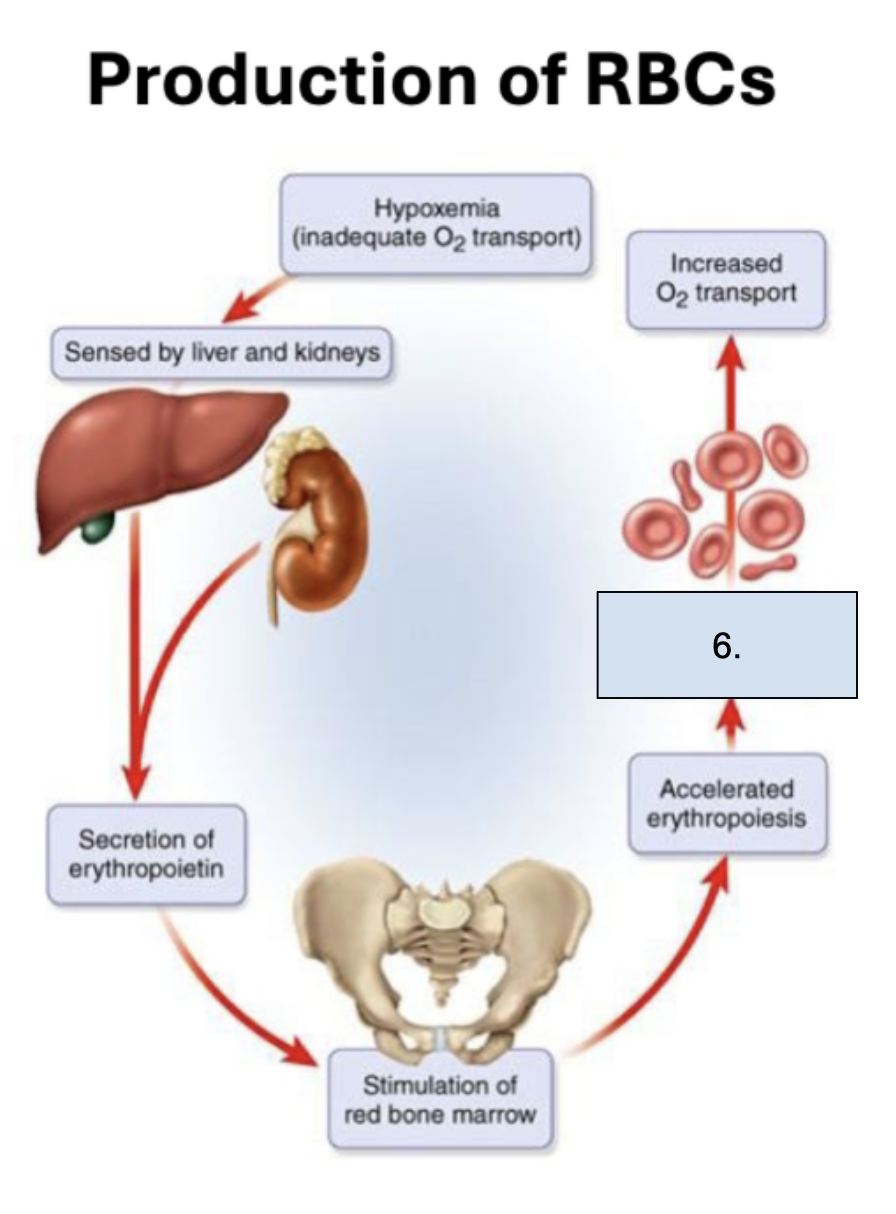
What is happening in this step?
Increased RBC count
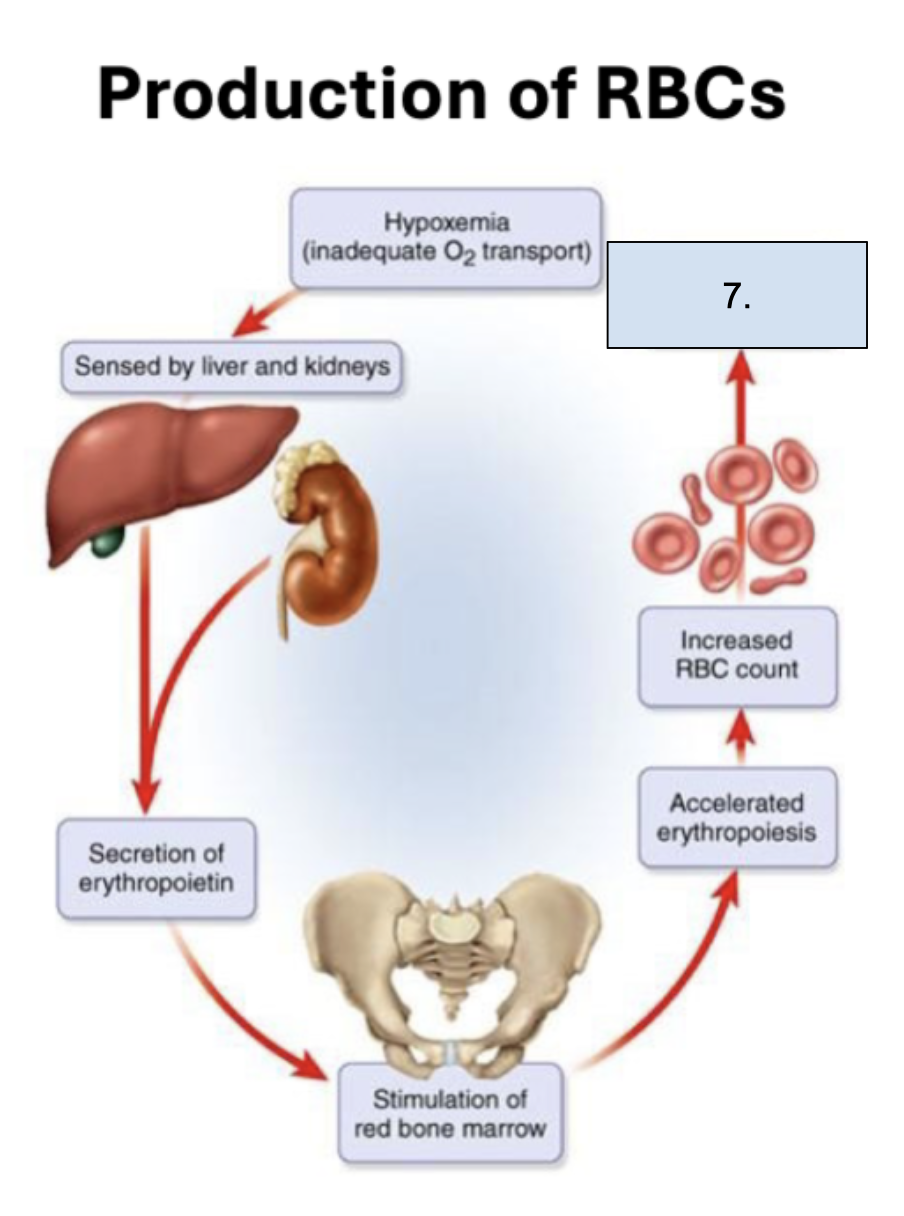
What is happening in this step?
Increased O2 transport
What stores blood cells and removes old RBCs from circulation
Spleen
What cells destroy old RBCs in the spleen
Macrophages
Iron is removed from hemoglobin in what organ
The spleen
What is hemoglobin converted to in the spleen
Bilirubin
What color is bilirubin (tinged)
Yellow
Bilirubin released in blood travels where?
Liver
Once further broken down in the liver, what happens to bilirubin
Excreted in feces and urine
What do WBCs have that RBCs lack
Nuclei and mitochondria
Fashion of movement seen in WBCs
Ameboid
Why do WBCs squeeze through capillary walls
To reach infection
Blood component found in and out of the cardiovascular system
WBCs
Which is more numerous, RBCs or WBCs
RBCs
Range of WBCs in body
5000-10000 per microL
Which is larger, WBCs or RBCs?
WBCs
Only formed elements that are complete cells
Leukocytes
Are monocytes granular or agranular
Agranular (think “cyte”=agranular)
Are lymphocytes granular or agranular
Agranular (think “cyte”=agranular)
Are eosinophils granular or agranular
Granular (think “phils”=granular)
Are basophils granular or agranular
Granular (think “phils”=granular)
Are neutrophils granular or agranular
Granular (think “phils”=granular)
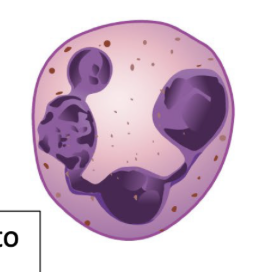
What is this?
Neutrophil
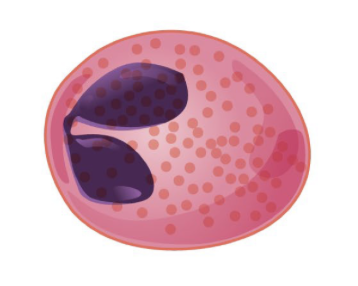
What is this?
Eosinophil
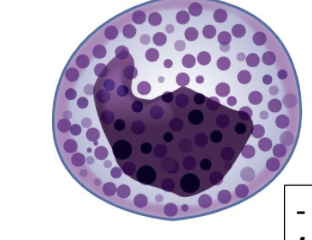
What is this?
Basophil
Rapid responders to the site of infection
Neutrophil
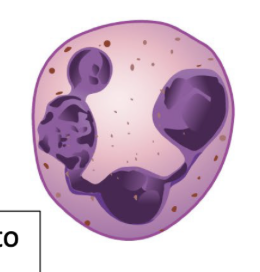
Efficient phagocytes with a preference for bacteria
Neutrophils
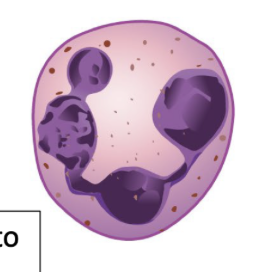
Release antihistamine granules that counteract basophil histamines
Eosinophil
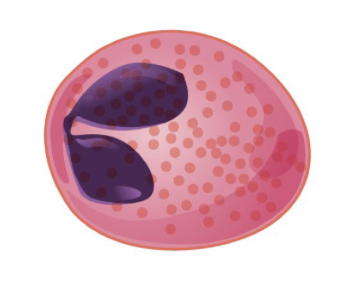
Releases histamine and heparin
Basophil
Inflammatory molecules released by basophils
Histamines
Blood clot opposing granules released by basophils
Heparin
Where are granular leukocytes produced
Red bone marrow
Granular leukocyte lifespan
Few hours to few days
Lobed nucleus and classified by granule stain
Granular leukocytes
Indented or horseshoe-shaped nucleus
Monocyte
Phagocytize debris, foreign pathogens, worn-out erythrocytes, and other dead, worn out, or damaged cells
Monocyte
Release antimicrobial defensins and chemotactic chemicals that attract other leukocytes to the site of an infection
Monocyte
What cells do lymphocytes come from
Lymphoid stem cells
Second most common type of leukocyte, ~20–30% of all leukocytes
Lymphocyte
3 lymphocyte groups
NK cells, B cells, T cells
Cells capable of recognizing cells that do not express “self” proteins or that contain foreign or abnormal markers (non-specific immunity)
NK cells
Cells involved in non-specific immunity
NK cells
Cells that defend the body against specific pathogens; involved in specific immunity
B lymphocytes and T lymphocytes
Cells involved in specific immunity
B lymphocytes and T lymphocytes
Platelets are fragment of large cells called what?
Megakaryocytes
What organ stores 1/3 of platelets for later response to blood vessel ruptures
Spleen
Cells for blood clotting
Platelets
Cells that secrete growth factors essential for growth and repair of tissue (e.g. connective tissue)
Platelets
The percentage of red blood cells in your blood
Hematocrit
Average hematocrit
45%
Hematocrit range
35-55%
Classification system based on the presence or absence of specific proteins (antigens) on the surface of red blood cells
Blood typing
Proteins recognized as foreign by the immune system of another individual
Antigen
Secreted by lymphocytes to bind to antigens and destroy them
Antibodies
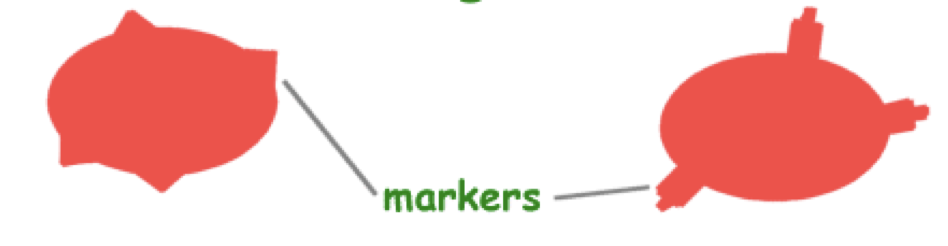
What is this?
Antigen
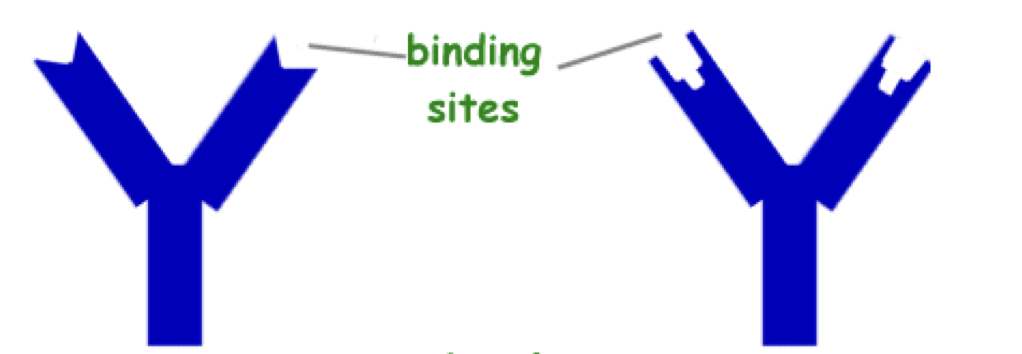
What is this?
Antibodies
What causes blood clumping and artery blockage in blood transfusions?
Mis-matched blood types
Universal donor
Type O
Why is type O the universal donor?
It has no antigens, any recipient antibodies have nothing to attach to