6. Histamine and Antihistaminic Agents
1/51
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
52 Terms
What is another word for local hormones?
Autacoids
Describe autacoids or local hormones and give some examples.
Released locally
Act at the site/near the site of their release
Histamine, 5-HT/serotonin, bradykinin, eicosanoids
What is the function of histamine?
Important mediator of immediate allergic and inflammatory reactions
Where is histamine distributed and where is it stored?
Distributed: in skin, GIT, mucosa, lungs, brain, CSF
Stored:
Mast cells: skin, gastric and intestinal mucosa, lungs
Non-mast cell: brain, epidermis, gastric mucosa
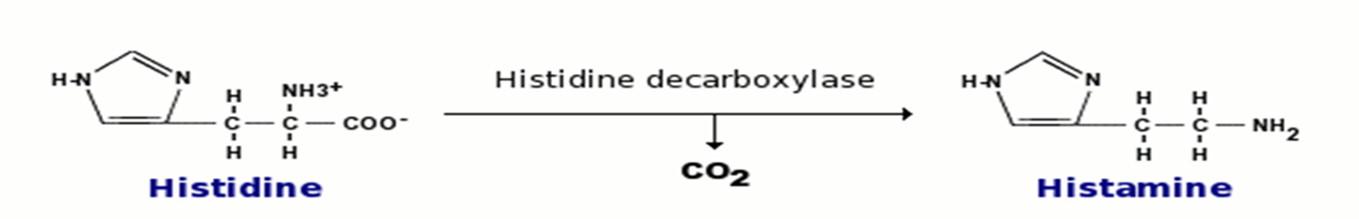
How is histamine synthesized?
Locally from the amino acid histidine
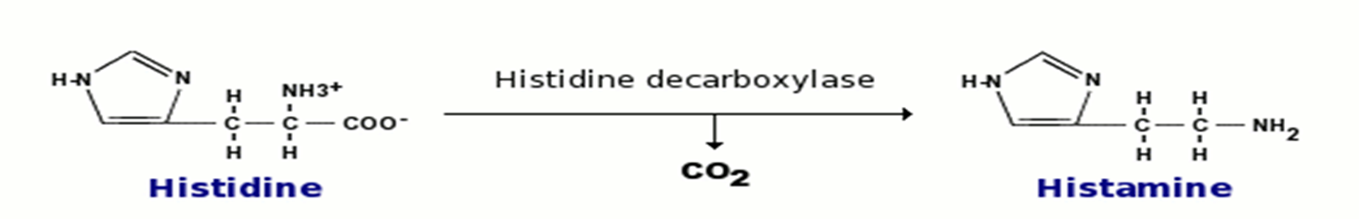
How is histamine degraded?
Rapidly by oxidation and methylation
List the responses of histamine.
Allergic and inflammatory reactions
Gastric acid secretion
Neurotransmission in parts of brain
Histamine has no clinical applications, but agents that _______ the action of histamine (______________/histamine ________ _________) have important therapeutic applications.
inhibit
antihistamines
histamine receptor blockers
List the types of histamine receptors and what category of receptors they belong to.
H1, H2, and H3
G-protein coupled receptors
H1
What are the pharmacological effects of histamine on H1 receptors in smooth muscle?
Bronchial smooth muscles:
Contraction
Constriction of bronchioles
Results in symptoms of asthma
Decreased lung capacity
Intestinal smooth muscles:
Contraction
Constriction results in intestinal cramps
Uterus:
Contraction
H1
What are the pharmacological effects of histamine on H1 receptors on blood vessels?
Vasodilation
H1
What are the pharmacological effects of histamine on H1 receptors on the brain?
Neurotransmitter (involved in arousal and alertness)
H1
What are the pharmacological effects of histamine on H1 receptors on sensory nerve endings?
Stimulation
Causes itching and pain
H1
What are the pharmacological effects of histamine on H1 receptors on exocrine secretions?
Increased production of nasal and bronchial mucus, resulting in respiratory symptoms
H2
What are the pharmacological effects of histamine on H2 receptors on gastric glands/stomach?
Stimulation of gastric HCl secretion
H2
What are the pharmacological effects of histamine on H2 receptors on blood vessels?
Vasodilation
H2
What are the pharmacological effects of histamine on H2 receptors on the heart?
Positive inotropy
Positive chronotropy
H3
What are the pharmacological effects of histamine on H3 receptors on brain?
Pre-synaptically
H1 and H2
What are the pharmacological effects of histamine on H1 and H2 receptors on CVS?
Vasodilation
Positive chronotropism (H2R)
Positive inotropism (H1 and H2R)
H1 and H2
What are the pharmacological effects of histamine on H1 and H2 receptors on skin?
Dilation
Increased permeability of capillaries, that results in leakage of proteins and fluids into the tissues
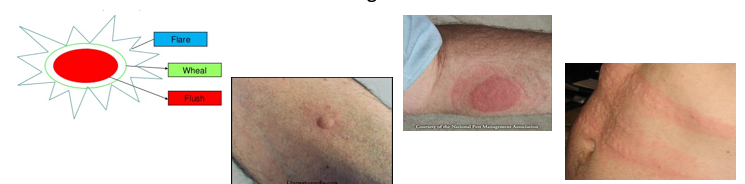
Describe the histamine-triple response (HALO).
Histamine elicits triple response, consisting of:
Red spot: due to intense capillary dilatation
Wheal: due to exudation of fluid from capillaries
Flare: i.e. redness in the surrounding area due to arteriolar dilatation
What type of antihistamine drugs are used? Describe their mechanism.
Histamine (H1) antagonists/blockers
Competitively antagonizes the actions of histamine at the H1 receptors
Describe the antagonism of histamine of the histamine antagonists/blockers.
Effectively block histamine induced bronchoconstriction, contraction of intestinal and other smooth muscles, and triple response (esp. wheal. flare, and itch)
Fall in BP produced by low doses of histamine is blocked (additional H2 antagonists required for complete blockage caused by higher doses)
List the classifications of antihistamine drugs.
First generation
Second generation
Third generation
List the classifications of first generation antihistamines.
Highly sedative
Moderately sedative
Mild sedative
List the highly sedative drugs in the first generation of antihistamines.
Diphenhydramine
Promethazine
List the moderately sedative drugs in the first generation of antihistamines.
Cinnarizine
Pheniramine
Cyproheptadine
List the mildly sedative drugs in the first generation of antihistamines.
Chlorpheniramine
Cyclizine
List the drugs in the second generation of antihistamines.
Cetrizine
Levocetrizine
Desloratidine
Terfinadine
Loratidine
Azelastine
List the drugs in the third generation of antihistamines.
Metabolite of terfenadine
Astemizole
Loratadine (development stage)
Norastemizole and descarboethoxy loratadine (metabolites of astemizole and loratadine)
Fexofenadine (the active metabolite of terfenadine)
Which generation of drugs show sedative effects?
In general, studies of the new generation of drugs show a weaker sedative effect when compared with the first-generation drugs. However, the second-generation drugs, often called non-sedating antihistamines, can also induce sedation (dose dependent)
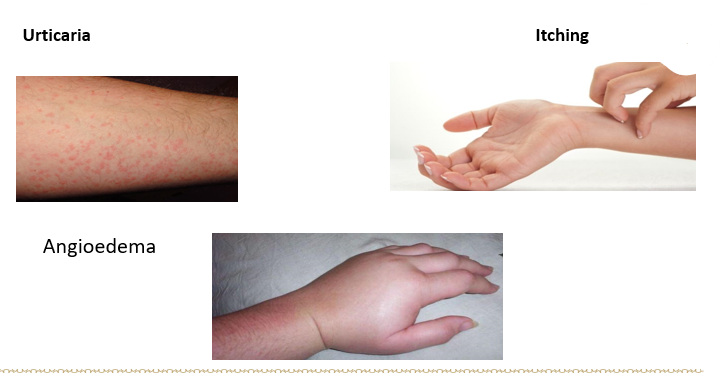
List the antihistaminic actions on allergies/anti-allergy.
Manifestations of immediate hypersensitivity (Type I reaction) are suppressed
Urticaria, itching, and angioedema are well controlled
List the antihistaminic actions on the CNS.
Older antihistamines produce variable degrees of CNS depression, depending on drug’s
ability to cross BBB
affinity for central (compared to peripheral) H1 receptors
List the antihistaminic actions on the anticholinergic action.
Antagonize muscarinic actions of ACh
List the antihistaminic actions on local anesthetics.
Membrane stabilizing property, but causes irritation
List the antihistaminic actions on the blood pressure.
Fall in BP on IV; not evident on oral administration
What are the clinical uses of antihistamines on allergic rhinitis?
Relieves rhinorrhea, sneezing, and itching of eyes and nasal mucosa
What are the clinical uses of antihistamines on common cold?
Palliative (relieves symptoms)
Dries out nasal mucosa
Often combined w/nasal decongestant & analgesics
What are the clinical uses of promethazine and why?
Pre-anesthetic sedation
Prevention of nausea and vomiting
Used for its anticholinergic and sedative properties
What are the clinical uses of promethazine and diphenhydramine and why?
Motion sickness (mild)
Morning sickness (Promethazine)
Drug-induced vomiting (Promethazine)
Post-operative vomiting (Promethazine)
Radiation sickness (Promethazine)
Prevent or diminish nausea and vomiting by both the chemoreceptor (CTZ) and vestibular pathways; effect due to blockage of central H1 and M1 muscarinic receptors
What are the clinical uses of cinnarizine and meclizine and why?
Vertigo
Cinnarizine has additional anticholinergic, anti-5-HT, sedative, and vasodilator properties
Meclizine is useful for treatment of vertigo associated with vestibular disorders
Which antihistamines are used for cough and why?
Chlorpheniramine
Promethazine
Diphenhydramine
Provides relief by sedative and anticholinergic properties
Which antihistamine can give mild symptomatic relief in early cases of Parkinson’s disease?
Promethazine
_____________ or sedatives induce sedation/sleep, especially in children.
Somnifacients
List the advantages of first generation antihistamines.
Effective
Inexpensive
Widely used
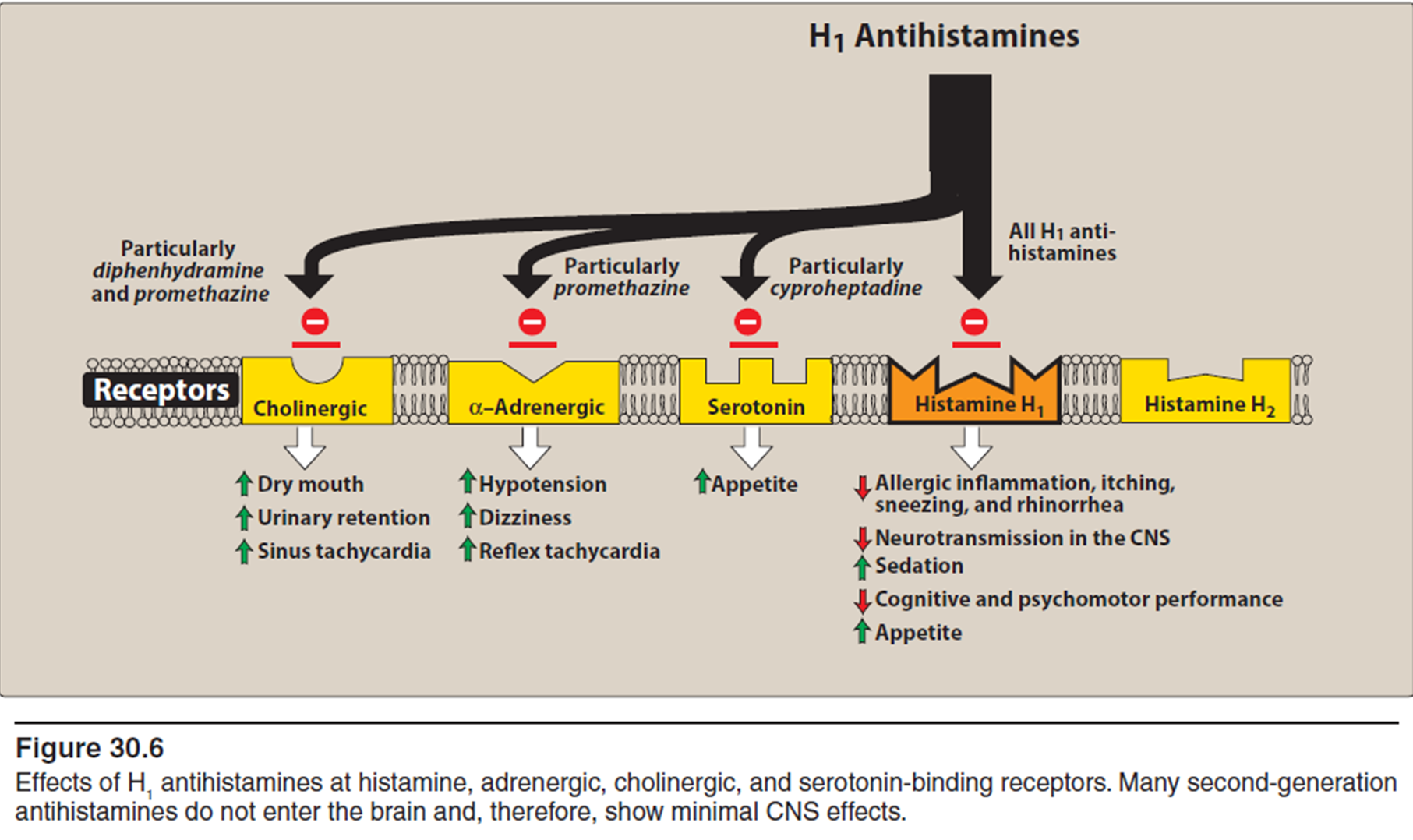
List the disadvantages/adverse effects of first generation anti-histamines.
Tend to interact with other receptors = variety of unwanted adverse effects
(First 5 - frequent but mild)
Sedation
Diminished alertness and concentration
Motor-incoordination
Fatigue
Tendency to fall asleep (cautioned to not operate motor vehicles or machinery)
Dryness of mouth
Alternation in bowel movement
Urinary retention
Blurring of vision (due to anticholinergic effects)
List the advantages of the second generation of antihistamines.
Long acting
Do not cause sedation as they do not cross BBB as readily as 1st gen
Absence of CNS depressant property
Higher H1 selectivity, do not block M1 receptors, so no anticholinergic adverse effects
Additional anti-allergy mechanisms - some also inhibit late phase allergic reactions by acting on leukotrienes
Do not potentiate alcohol or benzodiazepine CNS depressant effects
List and describe the drug interactions of second generation antihistamines.
Lethal ventricular arrythmias in many patients taking either early 2nd gen agents (terfenadine/astemazole) + antibiotics like ketaconazole or erythromycin (CYP3A4 inhibitors)
The antibiotics inhibit metabolism (CYP3A4) and increase conc. of antihistamines
Withdrawn from market due to ventricular tachycardia (Torsades de pointes) occurring w/higher doses or when co-administered with CYP3A4 inhibitors
Grapefruit juice also increases terfenadine’s blood level by inhibiting CYP3A4
List the means of management of anaphylaxis and when they are used.
Adrenaline (I.M): primary treatment; may be repeated every 5-15 mins
Adjuncts: antihistamines; inhibit histamine that would produce bronchoconstriction, etc
Corticosteroids (prednisone): severe allergic case as is anti-inflammatory and immunosuppressant
Nebulized salbutamol and leukotriene inhibitors (montelukast)
Describe adrenaline, its actions, and why it is the drug of choice for anaphylaxis.
Physiological antagonist of histamine
Actions on smooth muscle - opposite of histamine
Acts via β2 receptors on smooth muscle, causing cAMP-mediated relaxation
Therefore, is drug of choice in systemic anaphylaxis + other conditions w/massive release of histamine
Adrenaline followed by a short course of _____________ is indicated for ____________ attending drug hypersensitivity.
glucocorticoids
bronchospasm
Which drug type are the only effective drugs in type II, III, and IV reactions?
Glucocorticoids