Microscopic Anatomy of the Periodontium (CH 2)
1/37
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
38 Terms
Microscopic Anatomy of Sulcular Epithelium
The epithelial lining of the gingival sulcus is thin and nonkeratinized
Continuous with oral epithelium extending from crest of gingival margin to coronal edge of junctional epithelium
Permeable, allowing fluid to flow from gingival connective tissue into sulcus---gingival crevicular fluid
Three cellular layers:
Basal cell layer
Prickle cell layer
Superficial cell layer
Joins connective tissue with a smooth interface and no epithelial ridges in health
Sulcular Epithelium
In a healthy state the epithelium is smooth and intact
In health the sulcus is generally 1-3mm deep
Probe measurements are subject to variation for several reasons
Probe insertion pressure
The ability of the probe tip to penetrate tissue
The accuracy of the clinician reading the measurement
Microscopic Anatomy of Junctional Epithelium
Forms the base of the sulcus and joins gingiva to the tooth
The base of the sulcus is made up of the coronal-most cells
In health, attaches to the tooth slightly coronal to the cementoenamel junction
Thin and nonkeratinized, easily penetrable
Easiest entry point for bacteria to invade into connective tissue
Comprised layers of closely packed epithelial cells
Has a sparse extracellular matrix with a thin basal lamina between JE and the tooth surface and JE and gingival connective tissue
Two cell layers:
Basal cell layer
Prickle cell layer
15 to 30 cells thick at coronal zone(the zone that attaches highest on the tooth) and tapers to 4 to 5 cells thick at the apical zone
Cells next to tooth form hemidesmosomes that attach the internal basal lamina with the tooth surface
The attachment of the hemidesmosomes and internal basal lamina to the tooth surface is not static
Cells of the JE can move along the tooth surface
Cells next to gingiva form hemidesmosomes that attach the external basal lamina with gingival connective tissue
Has a smooth tissue interface with connective tissue in health
Why the Teeth Need a Junctional Epithelium
Teeth create break in epithelial protective covering
Protective epithelial sheet covers body
Teeth erupt and puncture protective epithelial sheet
Body attempts to seal opening by attaching epithelium to tooth
Gingival Fibers (Supragingival Fiber Bundles)
A network of rope-like collagen fiber bundles in the gingival connective tissue
Located coronal to the crest of the alveolar bone
Embedded in the gel-like extracellular matrix of the gingival connective tissue
Strengthen attachment of JE to tooth by bracing the gingival margin against the tooth
JE and gingival fibers are known collectively as dentogingival unit
Function of Supragingival Fibers
Reinforce
Reinforce attachment of JE to tooth
Provide
Provide rigidity to free gingiva so it can withstand chewing forces
Connect
Connect free gingiva with root cementum and alveolar bone
Connect
Connect adjacent teeth to one another
Classification of Gingival Fiber Groups
Classified based on:
Their orientation
Sites of insertion
Structures that they connect
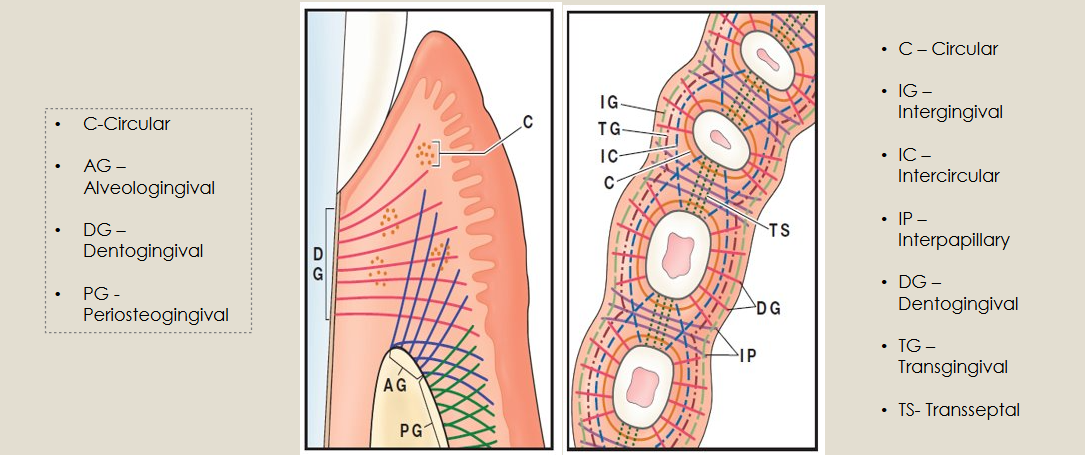
Alveologingival Fibers
Extend from the periosteum of the alveolar crest into the gingival connective tissue of the attached gingiva
Attach gingiva to the underlying bone
Circular Fibers
Encircle the tooth in a ring-like manner
Coronal to the alveolar crest
Not attached to the cementum of the tooth
Support the free gingiva
Dentogingival Fibers
Attached in cementum near the CEJ and fan into the gingival connective tissue of the free and attached gingiva
Support the gingiva
Attach gingiva to the teeth
Periosteogingival Fibers
Extend laterally from the periosteum to the alveolar bone
Attach the gingiva to the bone
Intergingival Fibers
Extend in a mesiodistal direction along the entire dental arch and around the last molars in the arch
Link adjacent teeth into a dental arch unit
Intercircular Fibers
Encircle several teeth
Interpapillary Fibers
Located in the papilla coronal to the Transseptal fiber bundles
Connect the oral and vestibular interdental papillae of the posterior teeth
Transgingival Fibers
Extend from the cementum near the CEJ and run horizontally between adjacent teeth
Link adjacent teeth
Transseptal Group
Cementum to cementum of adjacent teeth
Maintain relationship between teeth
Supragingival Fiber Groups
(looking down on occlusal)
Periodontal Ligament Fibers
Rope-like collagen fibers that stretch across space between cementum and alveolar bone of tooth socket
Have a rich supply of nerves and blood vessels
Composition of the Periodontal Ligament
Components
Cells
Mainly fibroblasts
Some cementoblasts
Some osteoblasts
Extracellular Matrix
A rich gel-like substance with specialized connective fibers
Fiber Bundles
A specialized connective tissue the surrounds the root of the tooth and connects it to the alveolar bone
Origin of the Periodontal Ligament
The PDL is derived embryologically from the ectomesenchymal tissue of the dental follicle that surrounds the developing tooth in its bony crypt
At the time of tooth eruption the cells and collagen fibers in the dental follicle, i.e. the future PDL, are orientated primarily with their long axis parallel to the root surface.
Remodeling of the follicle into a PDL begins at the CEJ and proceeds in an apical direction.
Functions of the Periodontal Ligament
Supportive
Anchor the tooth to the bony socket
Separate the tooth from the socket wall so the root does not traumatize the bone during mastication
Sensory
The PDL is supplied with nerve fibers that transmit tactile pressure and pain sensations
Nutritive
The PDL is supplied with blood vessels that provide nutrients to the cementum and bone
Formative
The PDL contains cementoblasts that produce cementum throughout the life of the tooth
Osteoblasts maintain the bone of the tooth socket
Resorptive
In response to severe pressure, osteoclasts in the PDL can induce rapid bone resorption and sometimes resorption of cementum
Periodontal Ligament Fibers – Five Principal Fiber Groups
Alveolar crest
Horizontal
Oblique
Apical
Interradicular
Alveolar Crest Fiber Group
Extend from the cervical cementum running downward in a diagonal direction to the alveolar crest
Resists horizontal movements of the tooth
Prevents tooth extrusion
Horizontal Fiber Group
Located apical to the alveolar crest fibers
Extend from the cementum to the bone at right angles to the long axis of the tooth
Resists horizontal pressure against the crown of the tooth
Oblique Fiber Group
Located apical to the horizontal group
Extend from the cementum to the bone in a diagonal direction
Resist vertical pressures that threaten to drive the root into the socket
Apical Fiber Group
Extend from the apex of the tooth to the bone
Secures the tooth in the socket
Resists forces that might lift the tooth out of the socket
Interradicular Fiber Group
In the furcation of multi-rooted teeth
Extend from the cementum in the furcation to the interradicular septum of the alveolar bone
Helps stabilize the tooth in its socket
Sharpey Fibers
The ends of the PDL fibers that are embedded in the cementum and alveolar bone
As cementum forms, the tissue calcifies around the ends of the periodontal ligament fibers surrounding them with cementum
As the walls of the tooth socket calcify, it surrounds the ends of the periodontal ligament fibers with bone
Microscopic Anatomy of Cementum
Is a mineralized tissue that covers roots of the teeth and serves to attach the tooth to alveolar bone via collagen fibers of the PDL
Anatomically it is part of the tooth
Functionally it is part of the periodontium
Functions of Root Cementum
Primary function is for periodontal ligament attachment
Sharpey fibers are the terminal endings of periodontal ligaments attached to cementum
Seals ends of open dentinal tubules
Compensates for occlusal attrition to maintain tooth length
Excess deposit in apical third of root is called hypercementosis which appears radiopaque on an x-ray
Composition of Cementum
Comprised of:
Organic substances
50-55% - Primarily Type I collagen and non-collagenous matrix proteins
Inorganic substances
45% -
Hydroxyapatite (calcium and phosphate)
Trace elements
Contains no blood vessel or nerves
Has been shown to contain biologically active mediators
It is believed that growth factor molecules are produced during cementum formation and then stored in the cementum matrix to induce PDL regeneration when needed.
Thickness of Cementum
20 to 50 microns - coronal half
50 to 200 microns - apical region
Cementum deposition continues after eruption
As teeth wear down on the occlusal or incisal surface there is compensatory deposition of cementum in the apical area
Conservation of Cementum During Periodontal Instrumentation
Historically it was accepted that bacterial products penetrate the cementum of periodontally diseased root surfaces
This concept resulted in intentional, aggressive removal of all or most cementum during instrumentation
Current research
Bacterial products are not located within cementum and removal of cementum is not necessary for successful periodontal treatment
Cementoenamel Junction
Relationship of the Cementum to Enamel at the CEJ
Overlap
60% of time
Cementum overlaps the enamel for a short distance
Meet
30% of time
Cementum meets the enamel
Gap
10% of time
There is a small gap between the cementum and enamel
Exposes dentin
Microscopic Anatomy of Alveolar Bone
Part of maxilla and mandible that forms and supports sockets
Anatomy
Alveolar bone proper
Trabecular bone
Cortical (compact) bone
Functions of Alveolar Bone
Protects roots of teeth
Changes in response to mechanical forces and inflammation
Constantly undergoes periods of bone formation and resorption in response to mechanical forces on he tooth and inflammation of the periodontium
The process of bone formation and resorption is called bone remodeling
Components of the Alveolar Bone
Major cell types
Osteoblasts:
deposit, synthesize/secrete
Osteoclasts:
destroy or resorb
Extracellular matrix
Collagen fibers
Gel-like substance
Matrix deposited by osteoblasts is not mineralized and is termed osteoid.
As new osteoid is deposited the old osteoid mineralizes.
Bone matrix undergoes mineralization by the deposition of minerals such as calcium and phosphate, which are subsequently transformed into hydroxyapatite
Alveolar bone has blood vessels and innervation