Degenerative disorders of the spine
1/20
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
21 Terms
Describe the degeneration of the disc (Lumbar disc herniation)
Degeneration starts from 20 years old
Nuceleus pulposus starts to loss fluid and elasticity
Loss of fluid → biomechanics of the spine change
Annulus fibrosus is no longer uniform
Due to large and unfavourable loads (flexion + rotation)
→ Cracking + bulging can occur
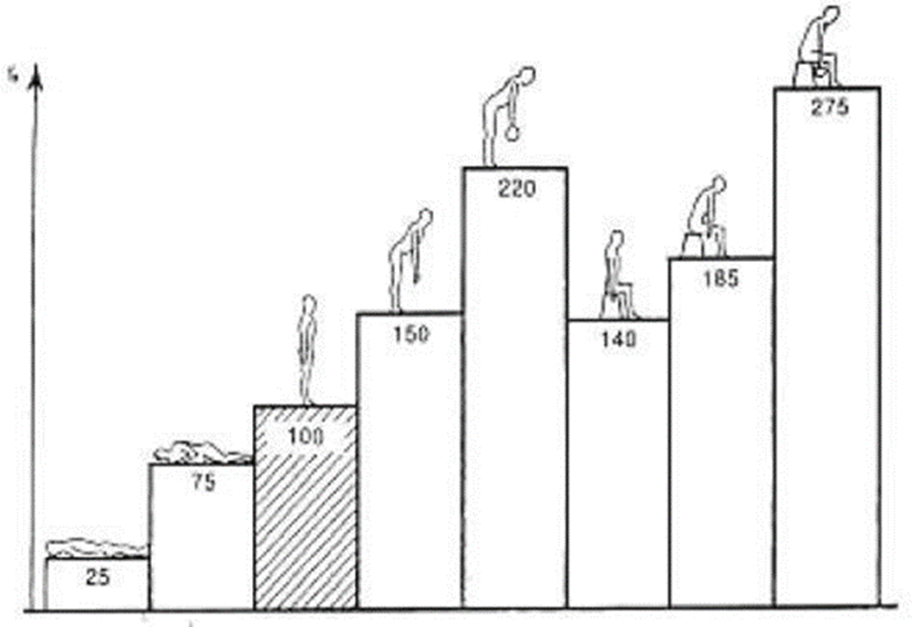
(Forces acting on the disc) = Lumbar disc herniation
1 Compression force
•Caused by gravity and muscle tension
•Depends on posture
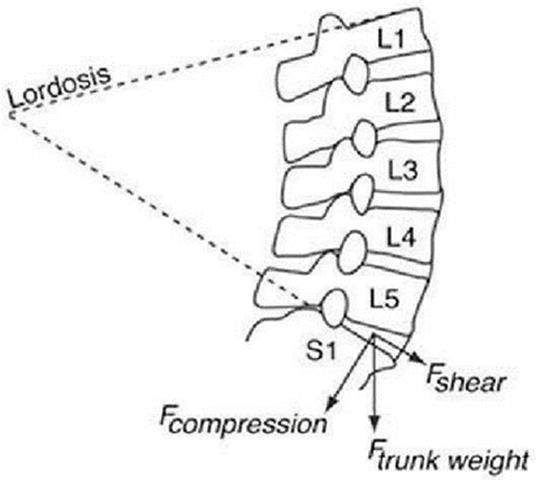
(Forces acting on the disc) = Lumbar disc herniation
2 Shear forces
•L4-L5 and L5-S1 experience the greatest shear forces due to the inclination of the sacrum
•The facet joints cause the greatest resistance in absorbing the shear forces
Increased lordosis → increased inclincation → increased shear forces at L5 and S1
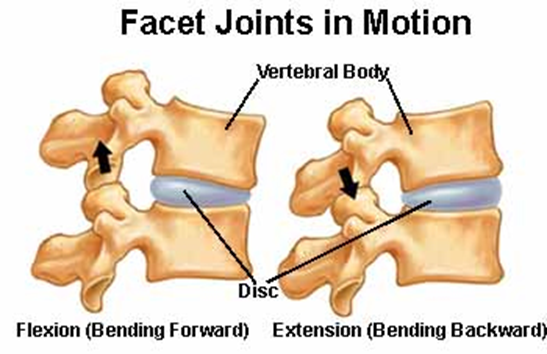
(Forces acting on the disc) = Lumbar disc herniation
3 Torsion
Mostly resisted by the facet joints
Repetitive torsion → damage to the facet joints
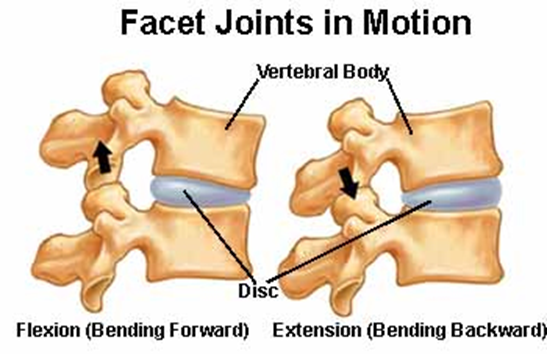
(Forces acting on the disc) = Lumbar disc herniation
4 Bending
•Bending backward → mainly facet joints and vertebral arch experience resistance
•Bending forward → jointcapsule + facet joints + ligaments provide resistance

Mechanism of occurrence of disc injury of Lumbar disc herniation
?
Slowly progressive damage due to:
•Disuse
•Overuse
•Repetitive movements
Symptomatic- non-symptomatic?
Medical imaging?
You cannot develop a discus hernia from bending to twisting the trunk movement. It does not happen immediately but spontaneously especially Bulging herniation
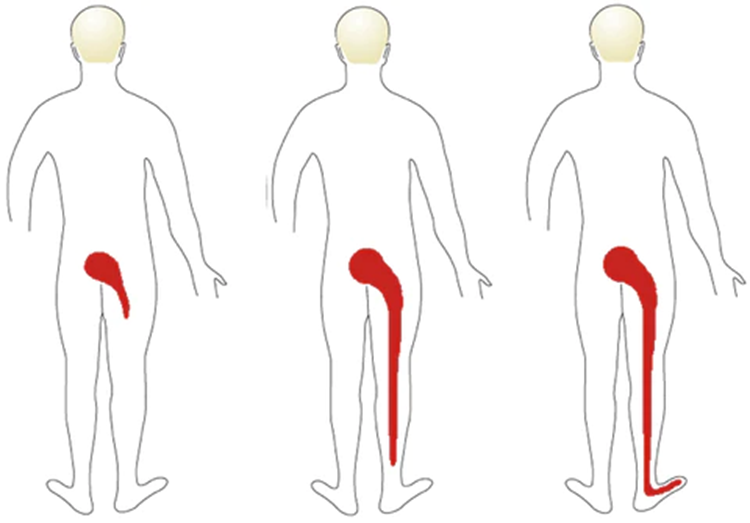
(Mechanism of occurrence of disc injury) = Lumbar disc herniation
ISCHIAS Pain worsens with ?
•prolonged sitting or standing
•Lifting/pressing/ coughing and sneezing
•Specific flexion movements in the spine
Posterior-lateral side of the leg, up to the ankle and foot (L4-L5)
Anterior pain in the thigh region (L2-L3) (more rare)
ISCHIAS Pain
= Numbness
= strong pain and changes
= feeling of ants in the region
= pain increases by laughing or coughing
HAMSTRINGS
= Itching pain
= Nocturnal pain
If people have pain in the anterior pain can be a result of of back pain
What is the difference of HNP (herniated pulposus disc) & disc degeneneration?
Herniated pulposus disc (HNP)
→ Young + middle-aged males
→ Favourable prognosis
→ 70% recovery after 1 year
→ Neurological damage and repair?
Disc degeneration
•Age-related reduction in water in the disc
•Discus tissue becomes stiffer
•Prognosis: rehabilitation and/or infiltrations/surgery needed
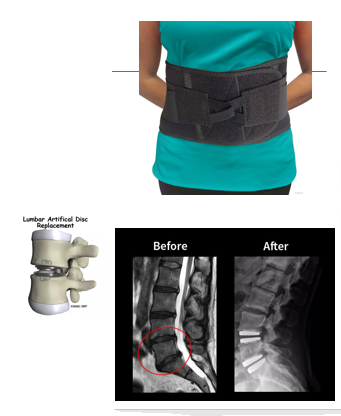
What is the treatment for Lumbar disc herniation?
Initial phase
•Symptomatic
•Most hernia’s improve rapidly within 3-4 weeks
•Physiotherapy
•Lumbosacral orthosis
If symptoms persist
•Up to 2-3 CSI
•Surgery
•Disc prosthesis
•Arthrodesis if both the disc and facet joint are damaged
What happens to the cartilage of (Cervical/lumbar) osteoarthritis?
To cover joint surface and prevent friction between bone pieces
Important shock-absorbing function
OA = degenerative → quality and quantity of cartilage deteriorates
If all the cartilage is gone → joint surfaces friction over each other → extra bone (osteophytes) are formed
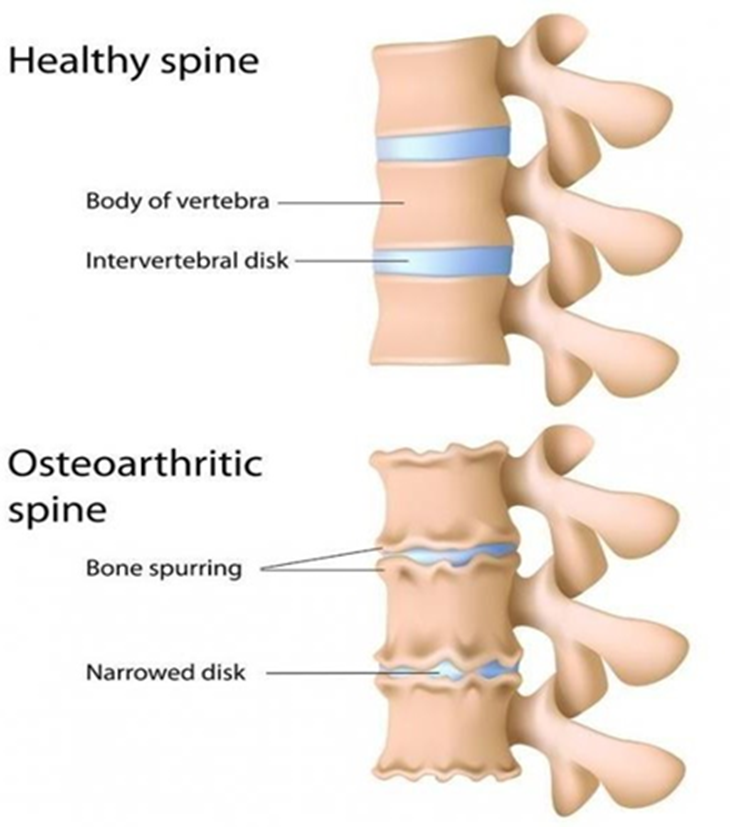
Where in the vertrbrates do Cervical & Lumbar OA happens?
Cervical OA
•Mostly C5-C6 + C6-C7
Lumbar OA
•Mostly (L4-L5)
•Mostly OA of the facet joints
What are the symptoms of Cervical & Lumbar OA?
• Pain at the level of the joint
• For cervical osteoarthritis: possible headaches and dizziness
• Motion restriction of the spine
• Muscle tension paravertebral musculature
• Possible radiation to the upper and lower extremities
Treatment for Cervical/ lumbar OA
Conservative treatment
•NSAID’s
•Physiotherapy
•Weight loss if needed
•Nutritional supplements
•Curcuma (really good)
•Glucosamine (Hydrates the discus and joint)
•Hyaluron acid (new technique)
If neurological signs are present
•Decompression with fusion
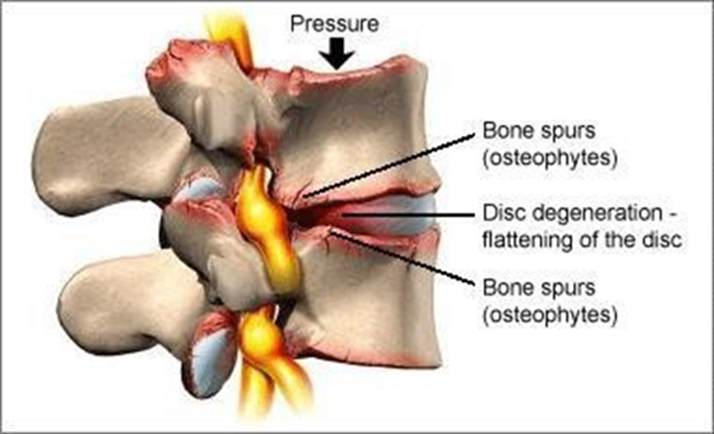
Describe the degeneration of the facet joints
Degenerative changes of the disc → affect functioning of the facet joints
Normal function facet joint: motion-control function
But in case of disc flattening → take over support function of the disc
→ Abnormal loading → risk of OA degeneration increases
→ Osteophytes possible → hypertrophy possible
ALWAYS LOOK FOR ALTERNATIVE
Stop the patient from doing repetitive movements because they will only accelerate the degeneration of the facet joint
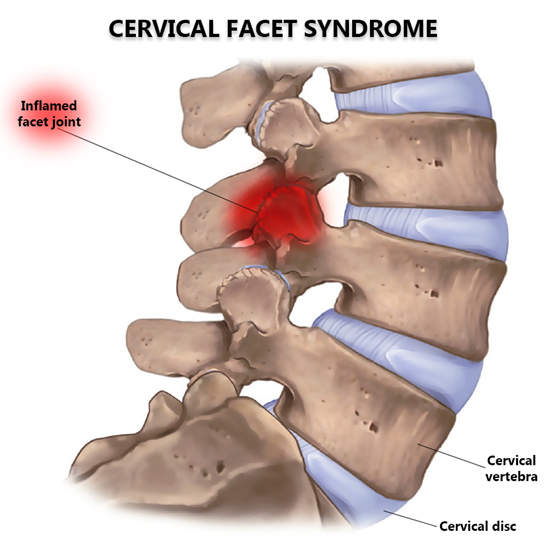
What happend if degeneration of facet joints are accompanied by chronic inflammation?
facet-syndrome
•Unilateral pain + well localized
•Extension pain
Differentiate Facet-syndrome and osteoarthritis
DON’T NEED TO KNOW
Referred pain patterns of facet joints
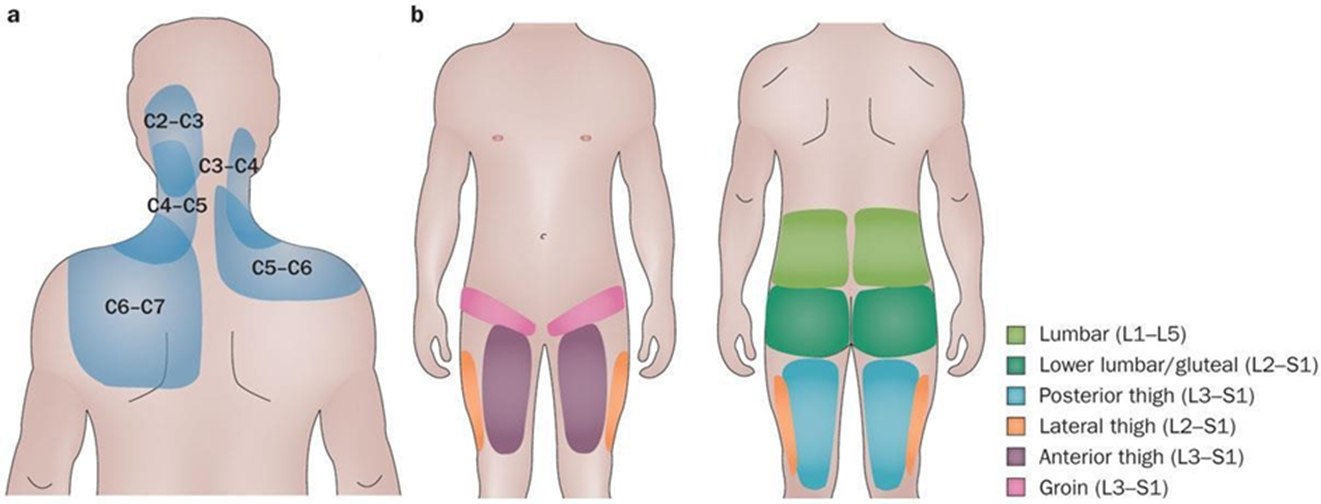
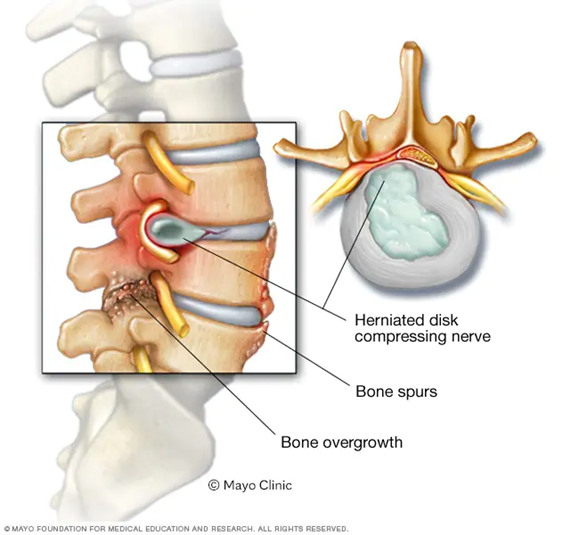
Describe Spinal canal stenosis
decrease in diameter of the spinal canal
Pain in the back + radiating to the buttock + leg region
Sometimes accompanied by motor and sensory disturbances
30% of the >60 y/o, but often asymptomatic
Neurogenic intermittent claudicatio
Radiating sharp pain in both legs
Worsens with standing + walking (with little walking distance..)
Flexion → symptoms diminish
≠ intermittent vascular claudication!
50 – 60 percent do not report back pain = it can be radiating pain
KNOW YOUR MYOTOME AD DERMATOMES
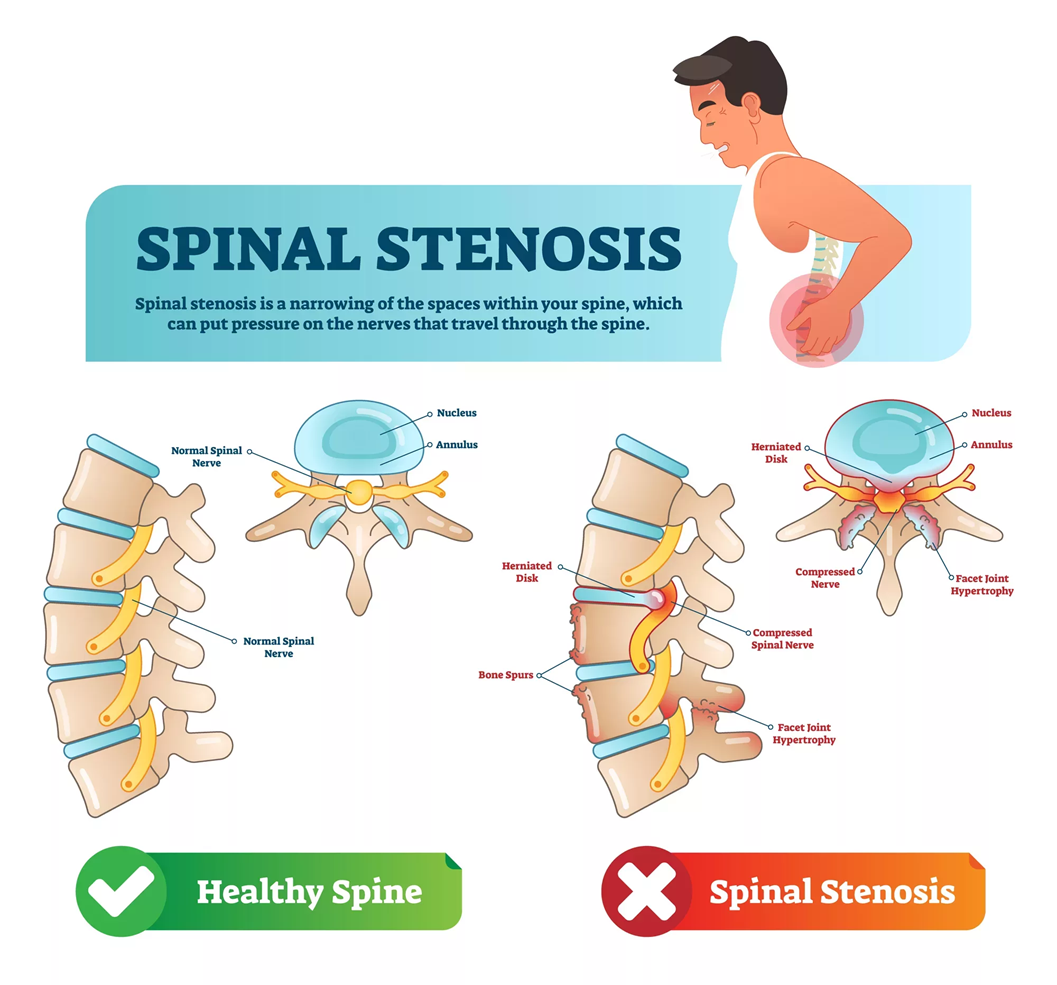
What are the possible (degenerative) causes of Spinal canal stenosis?
•OA of the facet joints
•Osteophyte formation
•Discus bulging
•Thickening of the ligaments
•Degenerative spondylosisthesis
Pain is caused by pressure on the neurogenic structures
There are a lot of causes BUT most important is OA
Problem happens to the height of the nerve root
DON’T NEED TO KNOW
Pain patterns in patients with spinal stenosis
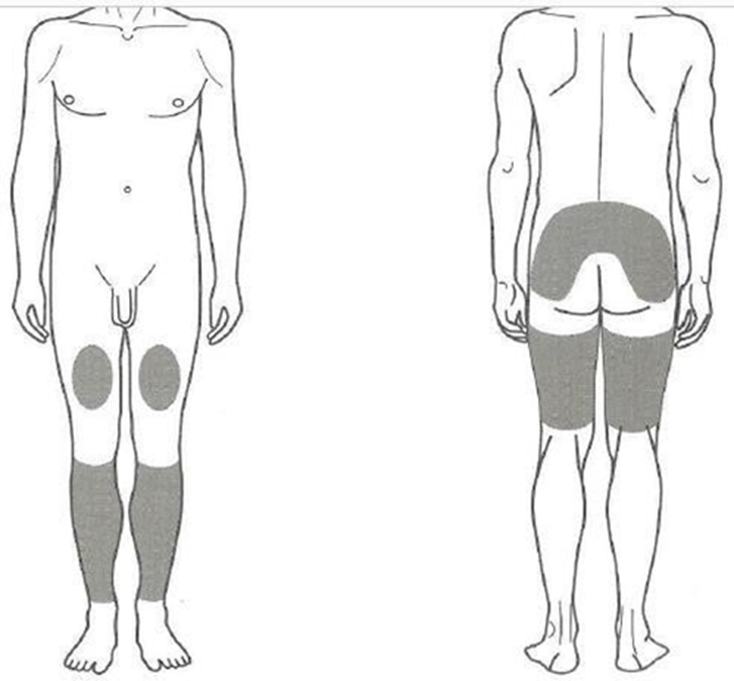
Treatment of Spinal canal stenosis
•Conservative
•Epidural infiltrations
•Physiotherapy = manual therapy
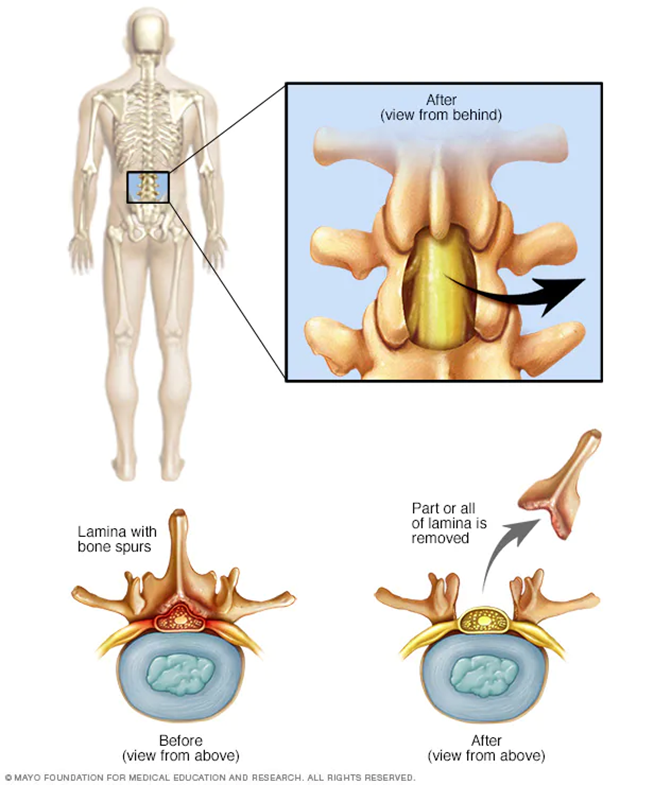
•Surgery
•Decompression techniques
•Laminectomy / facetomy
•Aims to reduce neurogenic claudication
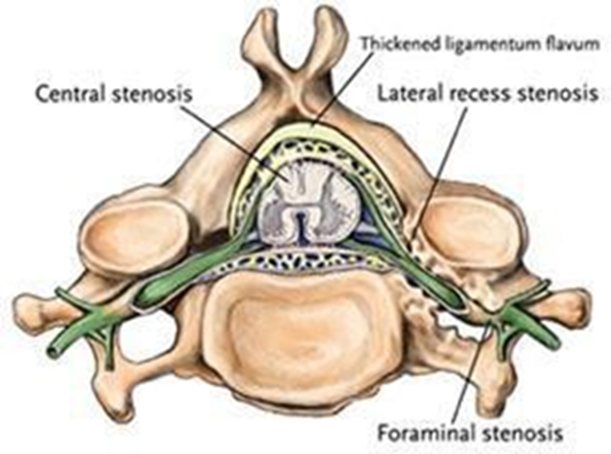
Describe Lateral recessus stenosis
Treatment?
Stenosis in the nerve root channel
Entrapment of the nerve root is not continuous + dependent on changes in posture and movements that narrow the nerve canal
Always unilateral = cannot be in two legs
Treatment → Lateral recessus stenosis?
Surgery is not really a solution for this one but sometimes it is applied bit always opt for conservative treatments