Fat-Soluble Vitamins
1/46
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
47 Terms
Properties of fat-soluble vitamins
lipid soluble
absorbed in the presence of fat (if we take a fat soluble vitamin, we must also eat it with fat or else we can’t absorb a lot of it)
absorption/transport is similar to that of fat
can be stored (liver, adipose mostly)
can be toxic in high doses
what is the other name for vitamin E?
alpha-tocopherol (toco- means childbirth and pher- is to bear)
what is the function of vitamin E?
antioxidant
Vitamin E discovery and history
Bishop and Evans needed a fat soluble factor that prevented fetal reabsorption in rats
they discovered that vitamin E helps prevent unsaturated fats from oxidizing
Vitamin E absorption, transport, and excretion
absorbed with fats (emulsification with bile acids)
incorporated into chylomicrons for circulation
processed in the liver
excretion via bile and feces
can also be excreted through the urine, but only after being processed in the liver
alpha-tocopherol significance in digestion
acts as the transfer protein
Vitamin E RDA and UL
RDA: 15 mg/day for adults (alpha-tocopherol form only)
UL: 1000 mg/day
Vitamin E deficiency symptoms
vitamin E deficiency is very rare (usually caused by insufficient fat absorption)
symptoms:
retinopathy
peripheral neuropathy (myelin sheath impairment)
ataxia (myelin sheath impairment)
lower immune function (due to membrane impairment)
Foods rich in vitamin E
vegetable oils
can be destroyed with heat and oxidation
Vitamin E toxicity
Not well researched
possible interference with blood clotting
Very rare
What family of compounds does vitamin A encompass?
Retinoids
Vitamin A functions
light absorbing pigment in the eye (rhodopsin)
Regulation of gene expression (nuclear receptors, meaning they get into nucleus and bind to DNA)
What is rhodopsin and what is its significance?
Rhodopsin is a light-absorbing pigment
It’s for the rod cell photoreceptors at the back of the retina
helps us see in low light
Retinal/retinol cycle
11-cis retinal + opsin = rhodopsin
breaks down in response to light (photo-bleaching): all trans-retinal and opsin
Opsin is responsible for the neuronal signals of vision
We need to regenerate 11-cis retinal to make rhodopsin
Review the visual cycle slide
What is the active form of vitamin A?
Retinoic acid
Retinoic acid production and function
produced in small amounts locally in many tissues
Retinoic acid receptors and Retinoid X receptors
Regulates:
cell differentiation
Growth
Embryonic development
Reproduction
Immunity
Review slide 16 for what we need to know for the exam
Vitamin A discovery history
discovered at UW- Madison by McCollum and Davis in 1913
Vitamin A was the lipid soluble factor needed to support growth in rats
Dietary sources of Vitamin A
animal products (retinyl esters)
Liver (polar bear liver has a toxic dose of vitamin A)
Dairy products
Egg
Fish (tuna, herring, sardines)
Fortified foods (margarine, cereals)
Foods with carotenoids (a plant pigment found in fruits and vegetables like carrots and sweet potatoes)
What structures can be converted into vitamin A by our bodies?
beta-carotene (found in sweet potatoes and carrots)
Alpha-carotene
beta-cryptoxanthin
Conversion of pro-vitamins
conversion of beta-carotene requires the enzyme BCO1 (beta-carotene oxygenase 1)
Converts beta-carotenes to retinal (one molecule of beta-carotene produces 2 molecules of retinal)
12 mcg beta-carotene yields 1 mcg retinol
In what body part is BCO1 most abundant in?
Epithelium in small intestine
Vitamin A absorption
Vitamin A as retinyl esters is sufficiently absorbed in the small intestine as long as enough fats are present
Cooking foods with vitamin A in fat increases absorption
Absorption of carotenoids (pro-vitamin A) is lower
for raw veggies, it can be low as 5%
Less absorption=less likely to experience toxicity
What happens once vitamin A is absorbed?
Retinol and beta-carotene are metabolized in the enterocytes before entering the bloodstream (review slide 22, 23, 24)
Vitamin A RDA
Men: 900 microgram RAE
Women: 700 microgram RAE per day
pregnant: 770 microgram RAE
lactating: 1300 microgram RAE
Tolerable upper intake level: 3000 microgram RAE
Know what RAE actually means! Everyone needs the same amount but different amounts may vary based on source
People who are vegetarians only get it from vitamin A conversion, so they may need to consume more of that source than meat eaters
Vitamin A deficiency symptoms
mostly an issue in developing countries
Night blindness
inability to adapt to darkness
Often the first sign of vitamin A deficiency
Consequence of diminished ability to regenerate rhodopsin (rod cells)
Crude indicator of vitamin A deficiency
Xerophthalmia
excessive dryness of eye caused by mucus production
Leads to corneal and conjunctival scarring, blindness
Bitot spots
white accumulations of sloughed cells and secretions
poor growth
Increases susceptibility to infection
vitamin A is needed for immunity
Vitamin A toxicity
Acute
can result from excessive dose- leads to nausea, vomiting, double vision, and headache
Chronic
develops over months to years (3-4x RDA may be toxic)
anorexia
Hair loss
Skin issues
Increased bone fractures
Eye pain
Liver damage
Birth defects (accutane- pregnant women shouldn’t use this)
what chemical group is vitamin K a part of?
quinones
from what term does the “K” in vitamin K come from?
koagulation
Vitamin K function
primary for blood clotting
essential for the activation of several proteins that participate in the clotting process
participates in bone calcification
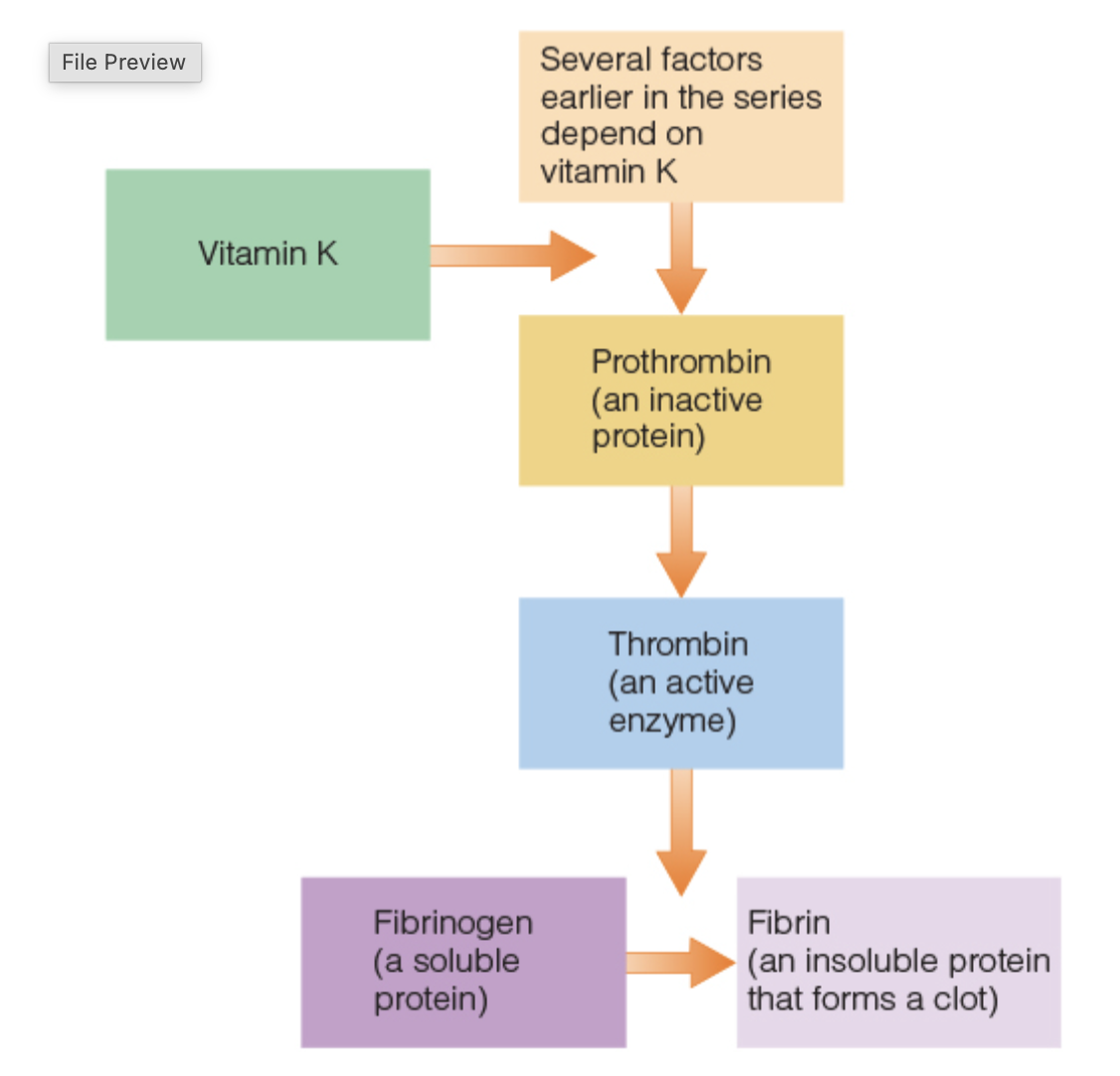
Vitamin K gamma-carboxylation
we tend to recycle vitamin K, so there isn’t much stored
clotting factors like Thrombin require the ability to bind the Ca2+ to be active
gamma carboxylation provides this ability
Vitamin K’s interaction with Warfarin
warfarin was previously used as a blood-thinner (not really used anymore).
Warfarin interferes with the recycling of vitamin K, which makes it less available and reduces gamma-carboxylation clotting factors
vitamin K discovery
by Henrik Dam and Edward A Doisy
discovered by feeding fat-free diets to chickens and saw that they suffered from a hemorrhagic disease
how is vitamin K absorbed?
absorbed in the small intestine
requires fat/bile and pancreatic factors
supplement forms are more readily absorbed than what comes from food
How is vitamin K transported around the body?
transported by chylomicrons
unlike other fat-soluble vitamins, our storage is limited
we use reducing power from NAD(P)H to recycle vitamin K
vitamin K intake recommendations
Adequate intake (different from RDA):
men: 120 micrograms a day
women: 40 micrograms a day
gut bacteria also appear to be able to synthesize vitamin K, although the amount bioavailable and absorbed by us in unclear
toxicity symptoms are not known
those who are using blood thinners need a consistent amount of vitamin K (eating it one night and never again is not enough)
vitamin K food sources
green, leafy vegetables
spinach
kale
broccoli
gut bacteria
likely insufficient amounts to meet needs
vitamin D history
has a long history with UW-Madison
started with Henry McCollum, then Henry steenbuck, and now there are current professors at Madison researching the functions of vitamin D
vitamin D food sources
beef
veal
eggs
fatty fish (salmon, herring, tuna)
liver
the sun (15 minutes of direct exposure to the sun is said to be enough vitamin D for our bodies)
fortified foods (milk/dairy, orange juice, breads and cereals)
vitamin K absorption
absorption from foods
is roughly 50% efficient
occurs in he distal ileum of the small intestine
requires bile acids and fat
incorporated into mixed micelles
packed into chylomicron for circulation
later circulations bound to vitamin D binding protein
vitamin D synthesis
vitamin D is synthesized by the skin
produced the majority of vitamin D from sun exposure (which is why it is recommended that those living in northern latitudes— Wisconsin being one of them— is recommended that they take vitamin D supplements, especially in the winter)
affected by: the amount of UVB radiation, age, race, clothing, sunscreen use
cholecalciferol (vitamin D3) enters bloodstream bound to vitamin D binding protein
vitamin D activation/regulation
vitamin D is a two-step activation process
liver: 25-Ohase (inactive)
+
kidney: 1 alpha-Ohase (inactive)
=
final product: 1,25-(OH)2D3 (calcitrol)- this is the active form of vitamin D
this regulates its own breakdown (negative feedback)
when considering supplements, the patient’s function of the kidney and liver is important because people need the active form
vitamin D function
to maintain normal serum calcium and phosphorus levels in the blood (review slides 21 and 22- 23 is the the most important)
Vitamin D and bone health
calcitrol (active vitamin D) facilitates calcium absorption from the gut, which is needed for bone mineralization
increases expression of cal binding and calcium channels
similar effects on tubules to increase calcium reabsorption from urine
Vitamin' D’s involvement in gene expression
behaves as a hormone (same as vitamin A) and regulates gene expression by binding the vitamin D receptor (VDR)
VDR is expressed in most cell types, suggesting broad functions (nuclear receptor)
Through its action on gene expressions, vitamin D influences immune response and host-defense against pathogens via CAMP (prevents us from getting sick)
vitamin D daily intake requirements
RDA: 600 IU (indicates that there are many ways to get vitamin D) (15 micrograms) for most age groups
prevents deficiency for bone health
older adults (over 50 years): 800 IU a day (20 micrograms)
reduced sun exposure
reduced skin biosynthesis
reduced kidney activity
RDA is not different for pregnant or lactating women
tolerable upper intake level: 4000 IU/day (lower for kids)
requirement can be met with 15 minutes of direct sunlight a day, but highly variable depending on sunscreen use, clothing, time of day, etc.)
Vitamin D deficiency symptoms
inadequate calcium ad phosphorus deficiency in the bone
osteomalacia (soft bones- occurs in adults)
may be caused by kidney, stomach, gallbladder, intestinal, or liver disease affecting vitamin D absorption or metabolism
treatment: sun exposure, supplements)
rickets (occurs in children)
bowed legs, enlarged head and rib cage, and deformed pelvis (this was fairly common in the 1900s because the Industrial Revolution led to a lot of air pollution, resulting in everyone getting lower exposures of vitamin D from the sun)
vitamin D toxicity symptoms
toxicity from sun exposure or foods is unlikely/impossible
tolerable upper intake level: 4000 IU/day
toxicity is most likely to result from excessive supplementation
hypercalcemia
kidney dysfunction
loss of appetite
GI stress