3. Diseases of the iris and retina.
1/76
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
77 Terms
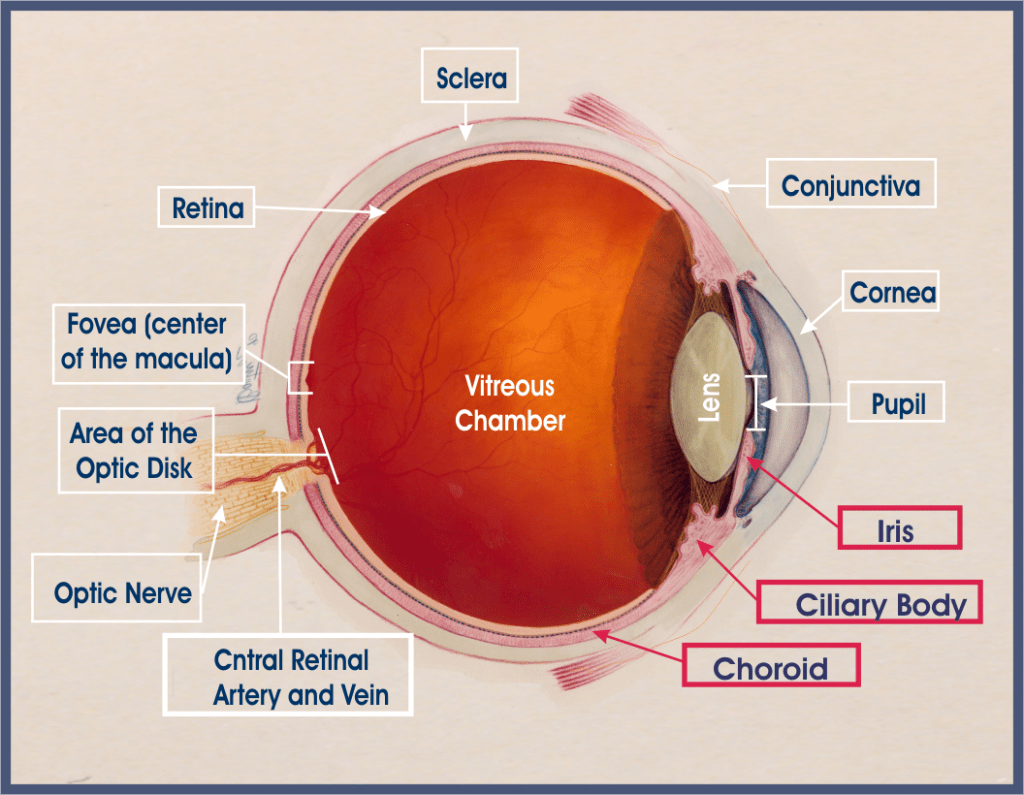
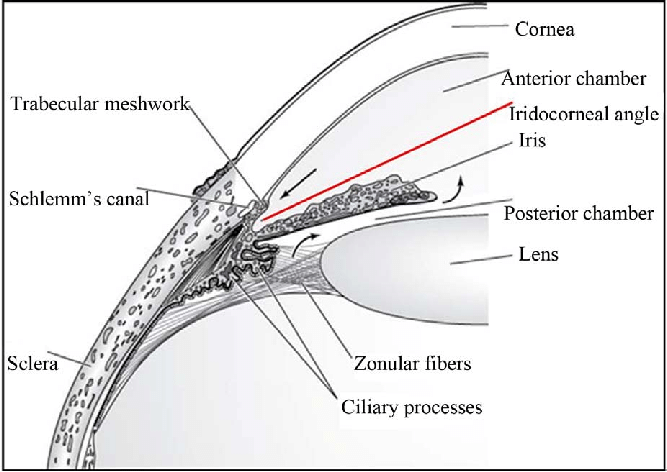
Corpus ciliaris (ciliary body), iris (anteriorly), and choroid (posteriorly)
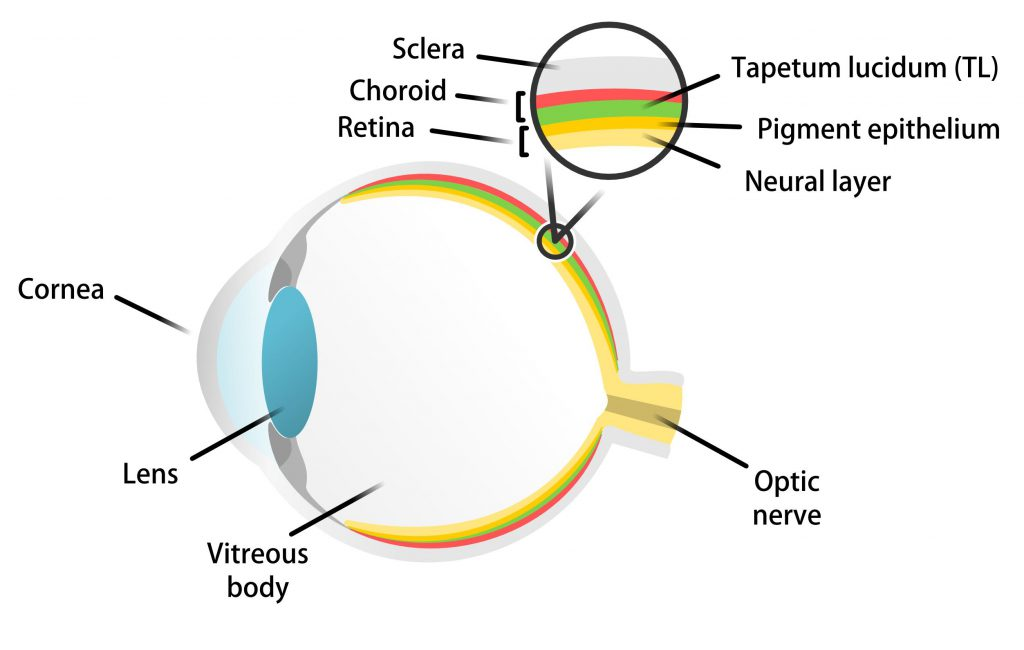
What is the choroid?
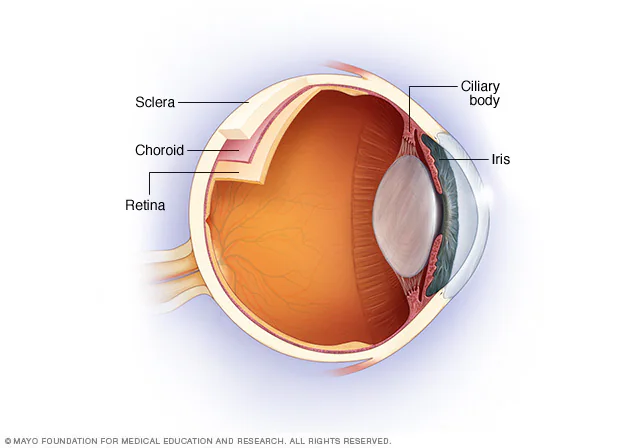
A thin layer of tissue that is part of the middle layer of the wall of the eye, between the sclera and the retina, and connected to the ciliary body
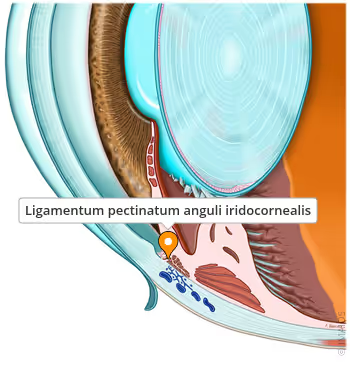
What are examples of diseases of the iris?
Developmental diseases
Uveitis
Colour variations (subalbinotic/blue iris, heterochromia, merle genes [heterochromia, iris hypoplasia])
Persistent pupillary membrane (PPM)
Aplasia/hypoplasia (aniridia, notch coloboma, pseudopolycoria, iridodiastasis)
Iridociliary cysts
Inflammation of the uveal tissue (iris, ciliary body, and choroid)
Can be primary (idiopathic or immune-mediated) or secondary
What are the types of uveitis according to the structures involved?
Anterior uveitis
Posterior uveitis
Panuveitis
Chorio-retinitis
Lens-induced (small lens proteins pass into the aqueous humour)
Immune-mediated (uveodermatologic syndrome/VKH, pigment uveitis)
Infectious
Traumatic
Metabolic (diabetes mellitus)
What are some infectious causes of uveitis in cats?
Bacterial: Bartonella
Viral: FIV, FeLV, FIP
Protozoal: Toxoplasma gondii
Fungal: C. albicans, cryptococcus, coccioides, histoplasma
What are some infectious causes of uveitis in dogs?
Bacterial: Brucella, Borrelia, Leptospira, septicaemia, diphtheria
Viral: Adenovirus, distemper, herpes, rabies
Protozoal: Leishmania, toxoplasma, neospora, trypanosoma
Parasitic: Dirofilaria, toxocara
Fungal: Blastomyces, cryptococcus, coccioides, histoplasma
Ophthalmic examination, fluorescein staining, serum CRP (N: 0-10; bad: >10; uveitis: >20)
Topical anti-inflammatories (corticosteroids like prednisolone or dexamethasone are primary therapy, contraindicated with corneal ulcer)
Topical NSAIDs
Mydriatics (tropicamide; less potent than atropine)
Immunosuppressive (azathioprine)
Systemic ATB (amoxicillin)
Primary (melanocytic, iridociliary, medulloepithelioma, mixed)
Secondary (lymphoma, haemangiosarcoma, melanoma)
Surgery (partial iridectomy), radiation therapy, laser therapy, and chemotherapy
What are examples of diseases of the retina?
Retinal detachment
Retinal dysplasia
Collie eye anomaly
Progressive retinal atrophy/hereditary retinal degeneration
Retinal toxicity
Sudden acquired retinal degeneration syndrome (SARDS)
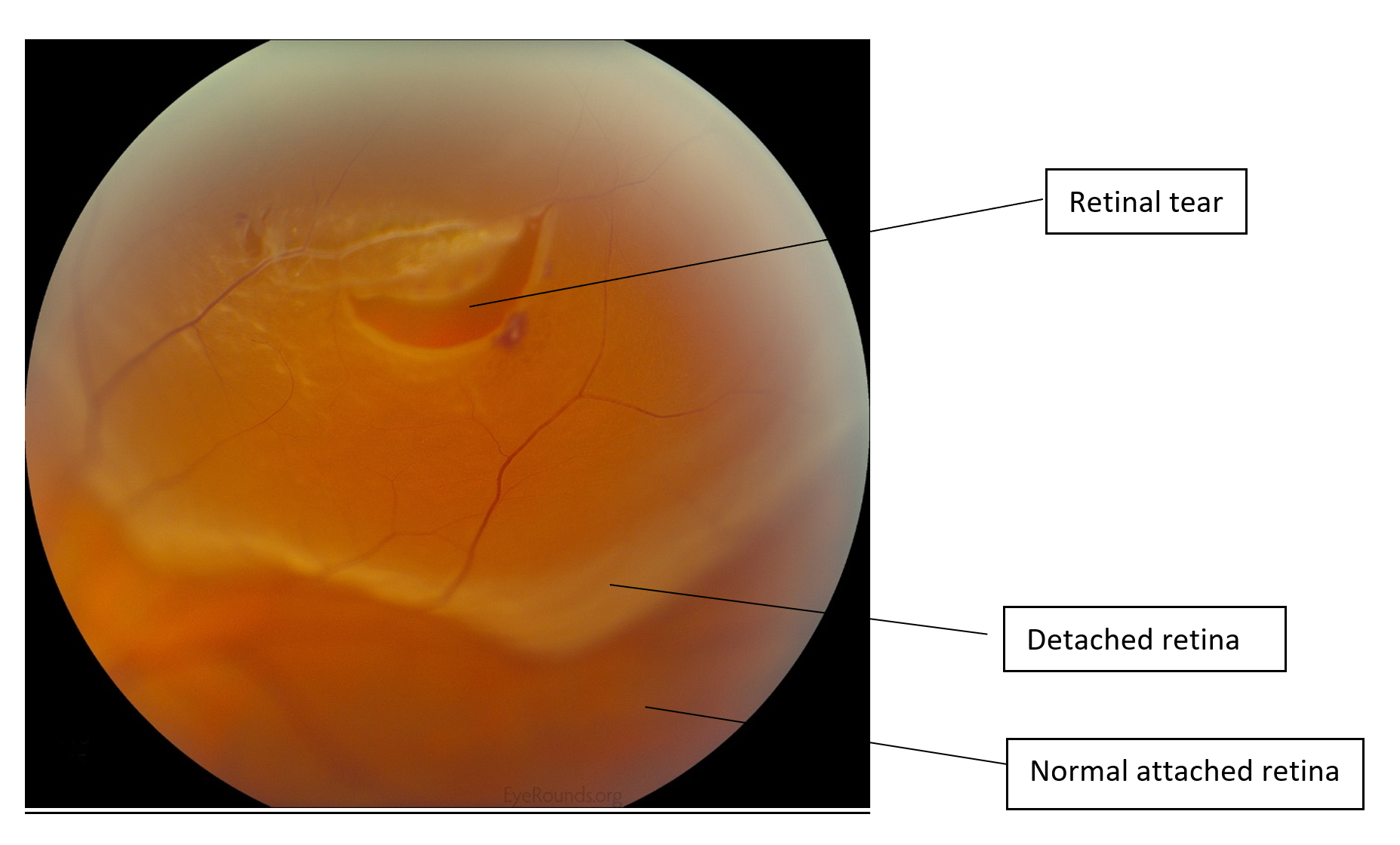
Separation of the retina from the underlying retinal pigment epithelium (RPE) layer containing blood vessels that provide oxygen and nutrients
Visual loss (if partial detachment), blindness (if complete detachment), red eyes (vitreous haemorrhage), pus, and a dilated pupil not responding to light
Ophthalmoscopy/fundoscopy (visualising the detached retina; wrinkled) or ultrasound (USG)
Which surgeries can be used to treat retinal detachment?
Scleral buckle surgery: Placement of silicone band around eye to provide external support & counteract traction on retina.
Vitrectomy: Removal of vitreous gel & any tractional membranes then intraocular gas or silicone oil injection to tamponade retina.
Pneumatic retinopexy: Injection of gas bubble into vitreous cavity followed by laser or cryotherapy to seal retinal breaks, combined w/ postoperative positioning.
An inherited condition where the retina develops abnormally, with unusual growth or changes in one or more of its parts
Viral infections
Vitamin A deficiency
X-ray irradiation
Certain drugs
Intrauterine trauma
Hereditary factors
Retinal Folds: Areas where retina has developed into abnormal folds.
Retinal Rosettes: Clusters of disorganised retinal cells.
Geographic Areas of Dysplasia: Larger, irregular areas of retinal malformation.
Retinal Detachment: severe cases: can cause retina to detach from underlying retinal pigment epithelium (RPE)
A congenital ocular syndrome involving defects of the posterior vascular and fibrous tunics of the eye (choroid, optic disc, sclera)
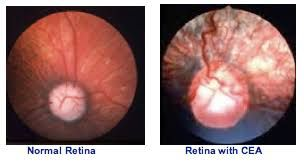
Causal gene testing (4-8 weeks). Diagnosis can be difficult.
What is the treatment for CEA?
None
What are some surgical procedures that might be used to preserve vision in CEA?
Always bilateral, leading to blindness. Early signs include impaired vision in dim light/darkness (night blindness). Progressive form: total blindness, slow pupillary light reflex, cataracts
Vasodilating drugs → Cause tapetal colour change
Ethambutol → Discoloration of the tapetal fundus
Diphenylthiocarbazone → Fundic alterations
Quinine → Vasoconstriction of retinal arterioles and pallor of optic disc
Closantel → Changes to the fundus
Ivermectin and enrofloxacin can also cause blindness
What is the treatment for SARDS?
None
How many layers are there in the retina?
10
What are examples of congenital diseases of the retina?
Collie eye anomaly: choroidal hypoplasia
Primary retinal dysplasia: disorderly proliferation and disorganisation of retinal layers. Focal, multifocal or total
Feline progressive retinal atrophy: autosomal, early-onset retinal degeneration
Canine multifocal retinopathy: multifocal, well-circumscribed grey to tan lesions throughout the fundus of puppies and young dogs. Rarely have significant impact of vision
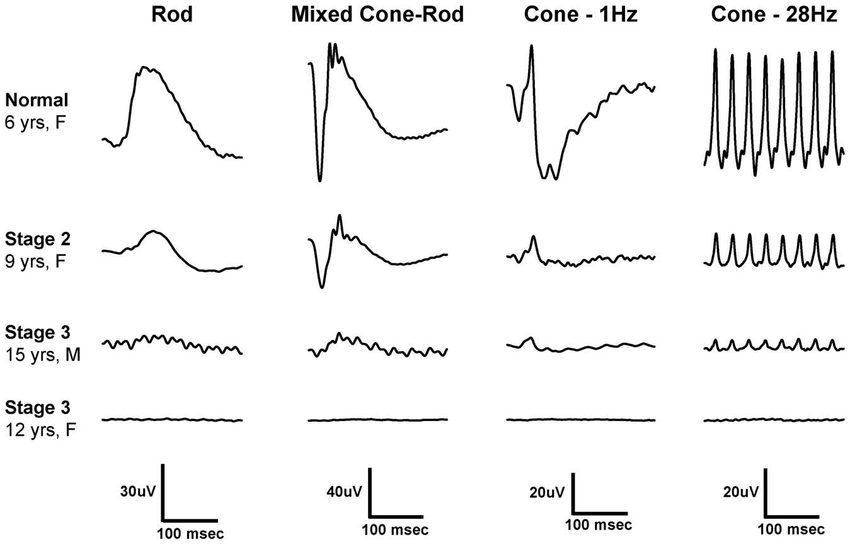
What is electroretinography?
Electroretinography is a test to measure the electrical response of the eye's light-sensitive cells, called rods and cones
What is the difference between hyperlacrimation and epiphora?
Hyperlacrimation: excessive watering due to reflex irritation of the corneal and conjunctival surface as in cases of dry eye, corneal abrasion, corneal foreign body, etc.
Epiphora: watering due to obstruction in the lacrimal outflow pathway