Pharmacotherapy Final Exam
1/213
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
214 Terms
acute pain
pain lasts for a minute up to 3 months (sometimes up to 6 months) and improves rapidly when underlying pathology stops
e.g. acute postoperative pain, soft tissue injury, trauma, labour, bee sting
goal -> recognize and treat pain before it becomes chronic
subacute pain
subset of acute pain, at least 6 weeks, under 3 months
similar nociceptive mechanisms
chronic pain
persistent and recurrent for 3 months or more
hyperalgesia and allodynia maybe 6 months or more
can start as acute pain, but continues beyond normal healing process or
usual course for acute disease little protective mechanism
may be nociceptive, neuropathic, mixed may result in changes to pain receptors
episodic pain
intermittent episodes of pain that occur over a long period, pain-free episodes in between
breakthrough pain
transitory flare of pain occurs in setting of controlled pain
risk factors for progression from acute to chronic pain
anxiety or depression
female gender
younger adults
Hx of poor acute pain management
Hx of poor response to common analgesics
genetic predisposition
nerve damage due to surgery or injury
SCHOLAR-E pain assessment
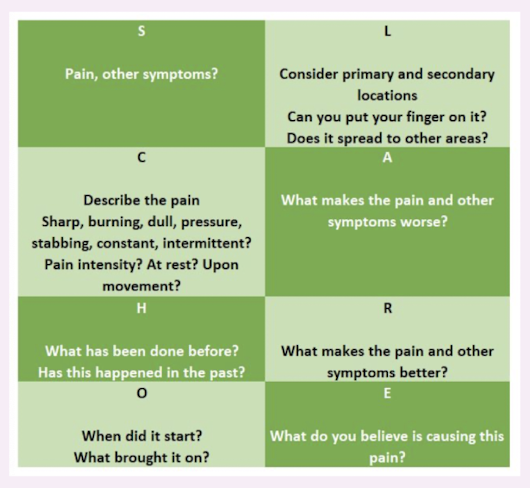
PQRST pain assessment
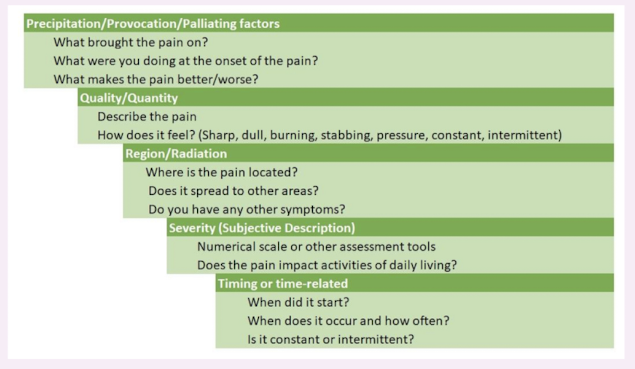

pain behaviour in children
infants may present with increased fussiness and change in eating habits
preschoolers - clingy, immobile, lose verbal/motor skills, lose sphincter control
school-age children - aggressive behaviour, shame, nightmares, withdrawal from social situation
adolescents - oppositional behaviour and depression (chronic pain)
pain in the elderly
assessments can be challenging - solicit information from caregivers and family members if poor historian (e.g. dementia)
pay attention to behavioural cues (e.g. grimacing)
more prone to adverse effects from medications
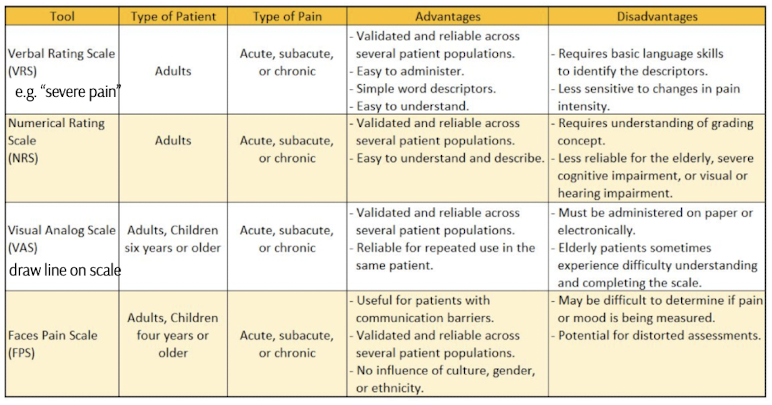
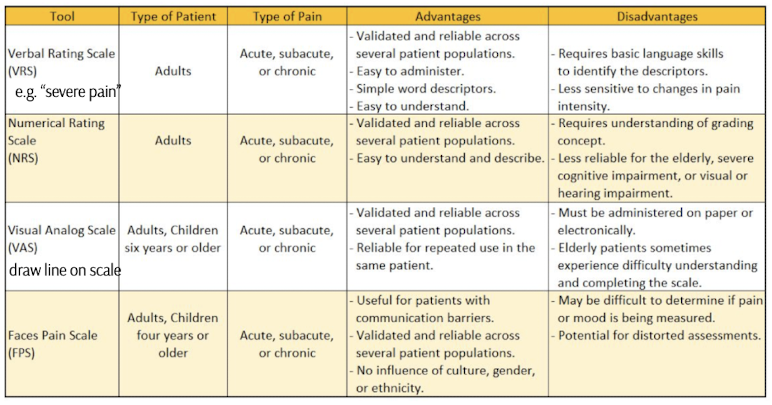
single dimension pain assessment tools
verbal rating scale
numerical rating scale
visual analog scale
faces pain scale
verbal rating scale for pain
A simple pain assessment tool where patients rate their pain on a predefined scale, typically using words such as "none," "mild," "moderate," and "severe."
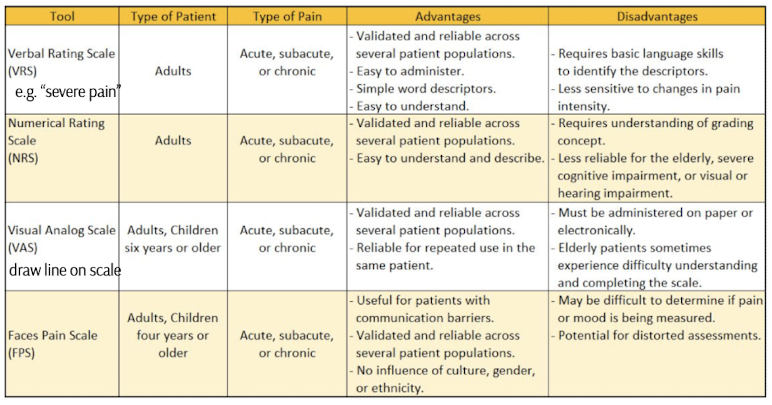
numerical rating scale for pain
A subjective pain assessment tool where patients assign a number to their pain level, usually ranging from 0 (no pain) to 10 (worst pain imaginable).
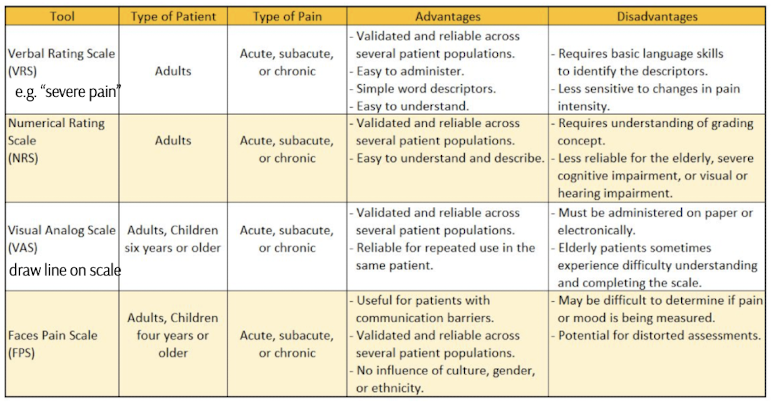
visual analog scale for pain
A pain assessment tool that uses a straight line, typically 10 centimeters long, where patients mark the point that corresponds to their pain intensity, with one end representing "no pain" and the other "worst pain imaginable."
faces pain scale
A pain assessment tool that uses a series of faces with varying expressions to help patients, particularly children, indicate their pain level in a way that is easily understandable.
multidimensional pain assessment tools
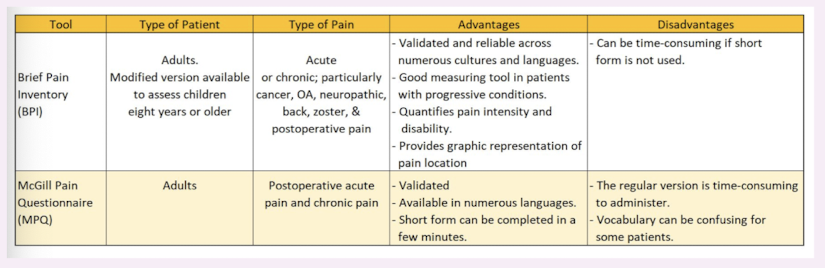
brief pain inventory
McGill pain questionnaire
brief pain inventory
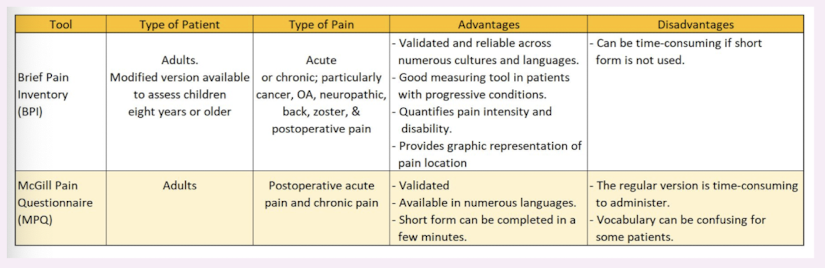
McGill pain questionnaire
acute pain goals of therapy
recognize the patient is experiencing pain
identify and treat that cause of pain
reduce or eliminate pain
minimize adverse effects
prevent progression to chronic pain
non-pharm management acute pain
(P)RICE (cold < 48 hours after injury)
most useful for soft tissue/musculoskeletal injury
application of heat ( > 48 hours after injury)
exercise
CAM options acute pain
acupuncture, massage, chiropractic, osteopathic manipulative therapy transcutaneous electrical nerve stimulation (TENS)
cognitive behavioural therapy
biofeedback
approach to pharmacological management for acute pain
step/ladder approach
1. mild pain -> non-opioid with or without adjuvant therapy
2. mild to moderate pain -> weak opioid or multimodal fixed-dose opioids, with or without non- opioid with or without adjuvant therapy
3. moderate to severe pain -> strong opioid, with or without non-opioid, with or without adjuvant therapy
escalate is pain persists or worsens
acetaminophen
analgesic/antipyretic
used for mild-moderate pain (4-6/10 on the NRS) as monotherapy or combined with other analgesics (additive)
no anti-inflammatory properties
*hepatic impairment - dosing changes based on degree of impairment
acetaminophen adult dosage forms
PO immediate release 325 mg, 500 mg (tabs, caps)
PO extended release 650 mg (Tylenol Arthritis)
acetaminophen pediatric dosage forms
PO 80 mg/mL, 160 mg/5 mL suspension
PO 80 mg, 160 mg chewable tabs, PO 160 mg sachet
PR 120 mg, 160 mg, 325 mg
acetaminophen adult dosing
max 4 g/day, older adults max about 3 g/day
325-500 mg PO Q4-6H PRN or 1 g PO Q6H PRN
extended release 1300 mg PO Q8H PRN
acetaminophen pediatric dosing
weight dosing: 10-15 mg/kg PO Q4-6H PRN
fixed dosing all available (weight dosing preferred)
max 75 mg/kg/day or 4 g/day (maximum of 5 doses/24H
weight dosing: 10-20 mg/kg PR Q4-6H PRN (max 75 mg/kg/day, max 5 doses/24H, children under 12 -> do not exceed 1,625 mg/day)
acetaminophen A/E
acute hepatotoxicity with acute overdose or chronic high doses
allergy - associated SJS, urticaria, angioedema
acetaminophen toxicity doses and symptoms
adults -> doses above 10 g/day or single ingestion above 250 mg/kg
pediatric -> doses above 75 mg/kg/day, above 4 g/day, single ingestion above 150 mg/kg
mild toxicity A/Es: N/V, abdominal pain, fatigue
severe toxicity A/Es: liver failure, jaundice, encephalopathy, coagulopathy
acetaminophen drug disease interactions
increased risk of toxicity with pre-existing liver injury + other risk factors (alcohol > 3 drinks/day, malnutrition, low BMI, fasting more than 1 day)
acetaminophen drug interactions
warfarin -> coagulant effect increased (limit acetaminophen to under 2 g/day if used for more than 3 days)
phenytoin, carbamazepine, alcohol -> increased hepatotoxicity
acetaminophen monitoring and follow up
pain/function - patient monitor daily, pharmacist follow up within 1 week/periodically using pain scale
pharmacist adjust to timing/other management strategies if current dose ineffective
educate importance of max daily dose
patient to monitor allergic reactions
NSAIDs for acute pain
analgesic, anti-inflammatory, antipyretic
used for mild-moderate pain (4-6/10 on NRS), monotherapy or combined with other analgesics (additive), more effective than acetaminophen when inflammation involved
difference is COX sensitivity depending on medication -> use lowest effective dose for shortest period (decrease risk of A/Es)
highly protein bound, metabolized by liver, variable half life
excreted primarily urine, also feces
ASA adult dosing
PO 81 mg, 325 mg (tabs)
dose: 325 - 1000 mg Q4-6H PRN, max 4g/day
pediatric ASA dosing
generally not used (Reye’s Syndrome)
ibuprofen adult dosing
PO 200 mg, 400 mg (tabs, caps)
dose: 200-400 mg PO Q4-6H PRN, max 3.2 g/day (1.2 g/day for self care)
ibuprofen pediatric dosing
PO 50 mg, 100 mg (tabs)
PO 100 mg/5 mL suspension, 40 mg/mL drops
dose: 5-10 mg/kg/dose Q6-8H PRN, max 40 mg/kg/day or 1.2 g/day
naproxen adult dosing
PO 220 mg (tabs, caps)
dose: 220 mg PO Q8-12H PRN max 440 mg/day for self-care
naproxen pediatric dosing
avoid under 12 years old
NSAID A/Es
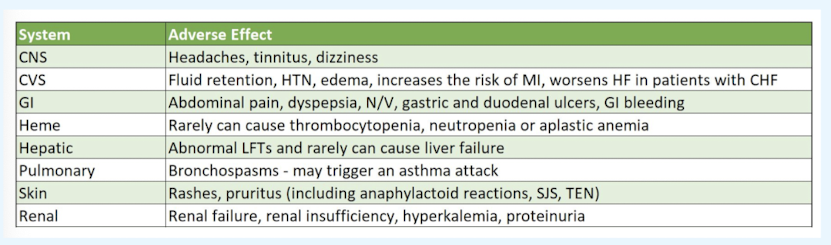
caution with NSAIDs in patients with:
renal dysfunction, CVD, CHF, HTN, asthma, hx of PUD or GI bleed
avoid in severe hepatic failure -> hepatorenal syndrome
pregnancy -> limit in 1st/2nd trimesters, avoid in 3rd trimester
NSAIDs contraindications
ASA-sensitive asthma or hypersensitivity to NSAID/ASA (bronchospasm, rhinitis, urticaria), before/following cardiac surgery, uncontrolled HF, active GI ulcer/GI bleeding/CV bleeding or other bleeding disorders, severe renal impairment, SLE/hyperkalemia
NSAIDs drug interactions
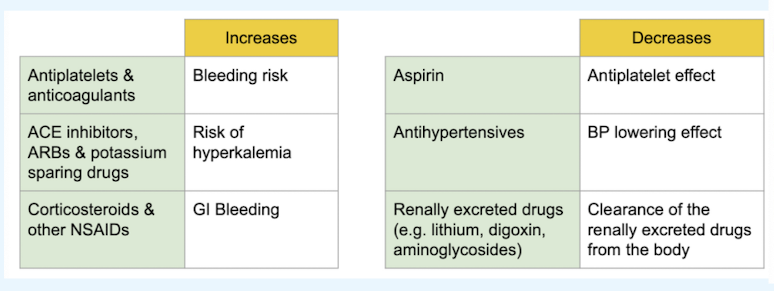
NSAIDs for acute pain monitoring and follow up
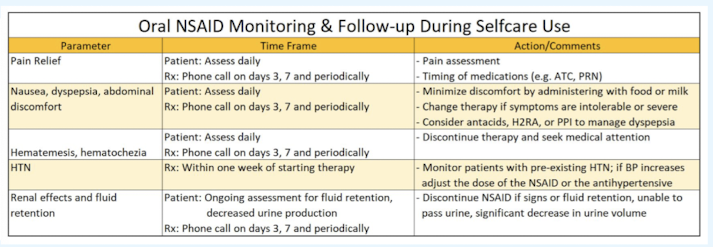
NSAID + acetaminophen combo
acetaminophen 325 mg + ibuprofen 97.5 mg tab
(Combogesic) mild to moderate acute pain
for adults 18+
dose: 1-2 tab PO Q6H PRN, max 12 tab in 24H
topical NSAIDs
for acute musculoskeletal conditions, more effective for smaller joints
similar pain relief to NSAIDs, delayed onset
not recommended to use topical and oral NSAIDs at the same time
topical diclofenac
1.16%, 2.32% gel applied 3-4x/day (OTC)
skin irritation, hypersensitivity, rarely systemic effects
topical non-NSAID analgesics
methyl salicylate, menthol, camphor, capsaicin, troamine salicylate
applied 1-3x/day, limited efficacy, may be helpful during rehabilitation as cooling/heating rubs or accompaniments to massage therapy
limited evidence for arnica montana for pain relief (can reduce bruising) should not be applied to bleeds/open wounds
should not be used at same time as thermotherapy -> burns
skin reactions -> pain, swelling, blistering in products with menthol
muscle relaxants for acute pain
for pain relief when muscle spasm is component of acute injury
MOA: skeletal muscle relaxation via general CNS depression
usually given in combination with NSAID or acetaminophen
e.g. methocarbamol
A/E: dizziness, drowsiness, confusion
not recommended for acute musculoskeletal injuries due to limited effectiveness in pain relief
analgesics in pregnancy
DOC = acetaminophen
brief use of NSAIDs in 1st/2nd trimester (increased risk of ductus arteriosus after this)
analgesics in breastfeeding
NSAIDs and acetaminophen can be used safely
analgesics in older adults
DOC = acetaminophen (limit up to 3.25 g/day for chronic use)
lower doses of oral NSAIDs effective for mild-moderate pain
increase risk of GI bleed, PUD, acute kidney injury, avoid chronic use preferentially
topical NSAIDs for MSK injury -> local pain relief, fewer systemic A/Es
muscle relaxants not well tolerated due to sedation/anticholinergic A/Es
sports-related injuries
common injuries include sprains, stress fractures, overuse injuries
30-50% of sports injuries caused by soft tissue injuries
majority of injuries among adolescents -> sports-related
higher incidence in adolescent males
mechanisms of sports-related injuries
direct injury -> occurs at site of contact
indirect injury -> related to lack of contact and maybe environmental or functional
after initial injury -> regeneration begins 3-6 days after, peaks between days 7-14
non-pharm for sports-related injuries
RICE -> rest, ice, compression, elevation
pharmacological management for sports-related injuries
OTC oral analgesics
acetaminophen, ASA, ibuprofen, naproxen
OTC topical NSAID
diclofenac 1.16% or 2.32% gel applied 3-4x/day
others
prescription NSAIDs
oral muscle relaxants -> pain relief when muscle spasms are part of symptomology
external analgesics -> methyl salicylate, methanol, camphor, capsaicin, etc
red flags for sports-related injuries
eye injury resulting in blurred vision, vision loss, moderate to severe eye pain or discomfort
nosebleed resulting in ongoing bleeding beyond 20 minutes
ruptured eardrum resulting in headache, discharge from ear, slight bleeding or partial hearing loss
head injury resulting in: confusion, unusual eye movements, slurred speech, nausea, loss of consciousness, tinnitus, seizures, vomiting, dizziness, amnesia, headache, drowsiness
sports-related injury patient assessment
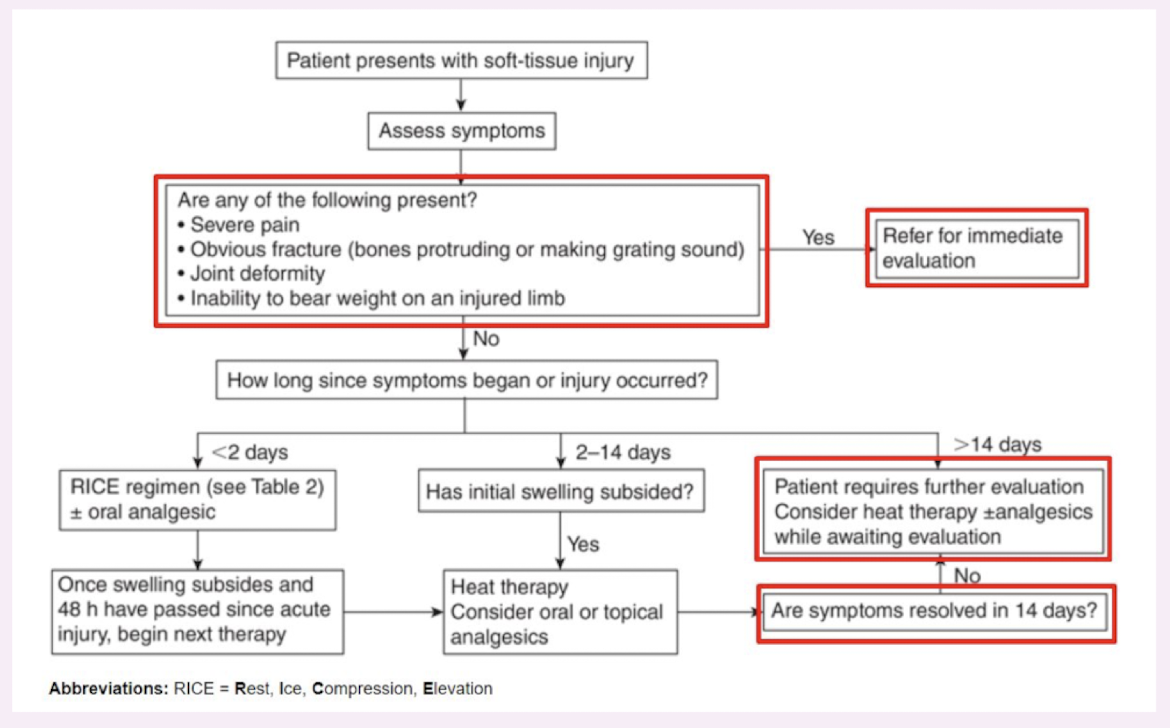
sports-related injuries goals of therapy
relieve symptoms to support a return to normal functioning within 2 weeks
support the healing process
prevent-re-injury or worsening of the existing injury
sports-related injuries monitoring and follow-up
instruct patient to monitor pain and swelling daily
pharmacist to follow up after 7 (initial response to therapy, dose being used) and 14 days
if no improvement -> refer to medical practitioner
if pain is worse despite pharmacotherapy, refer to medical practitioner
monitor -> efficacy and safety from analgesics (depends on chosen agent)
lower back pain pathophysiology
pain of varying severity in spinal area in lower lumbosacral region and can extend to gluteal, hips, lower extremities
improvement within 6 weeks of presentation, slows after that
lower back pain classification
duration
acute = < 4 weeks
subacute = 4-12 weeks
chronic = >12 weeks
categories
nonspecific lower back pain (treatments listed)
back pain with radiculopathy/spinal stenosis
back pain with other specific spinal causes
considerations for lower back pain therapy
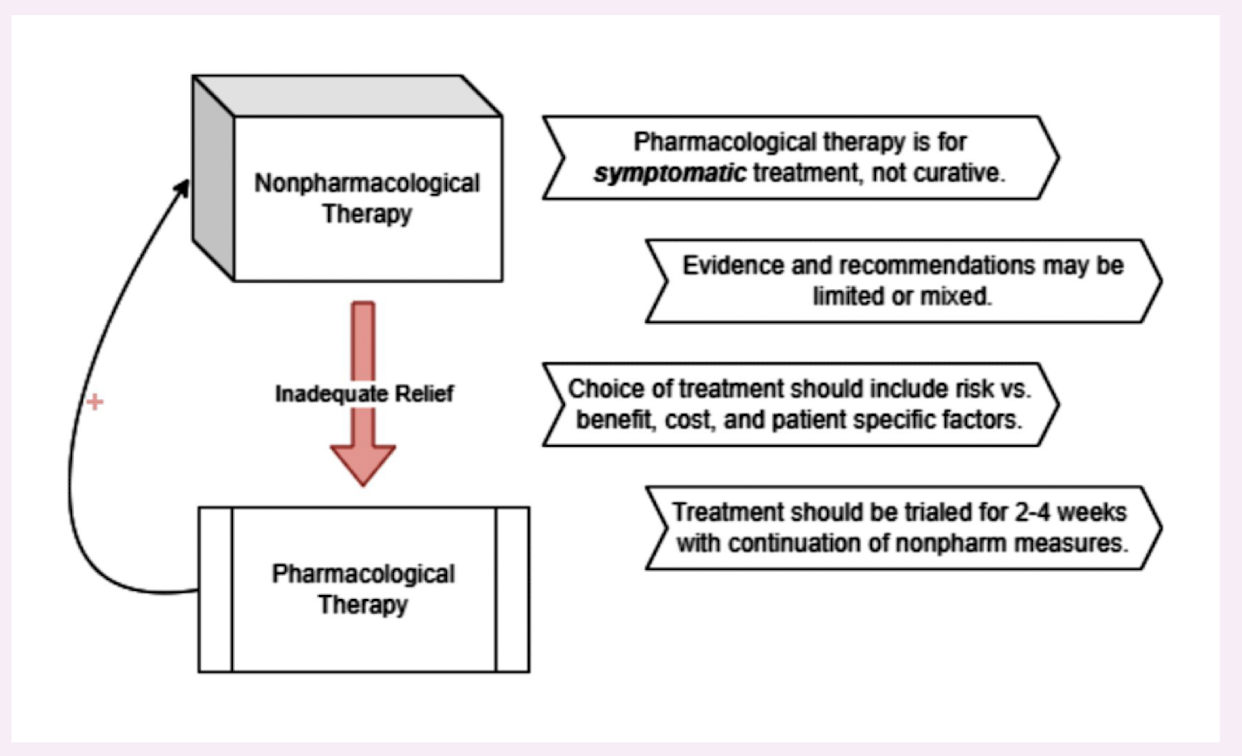
non-pharm management for lower back pain
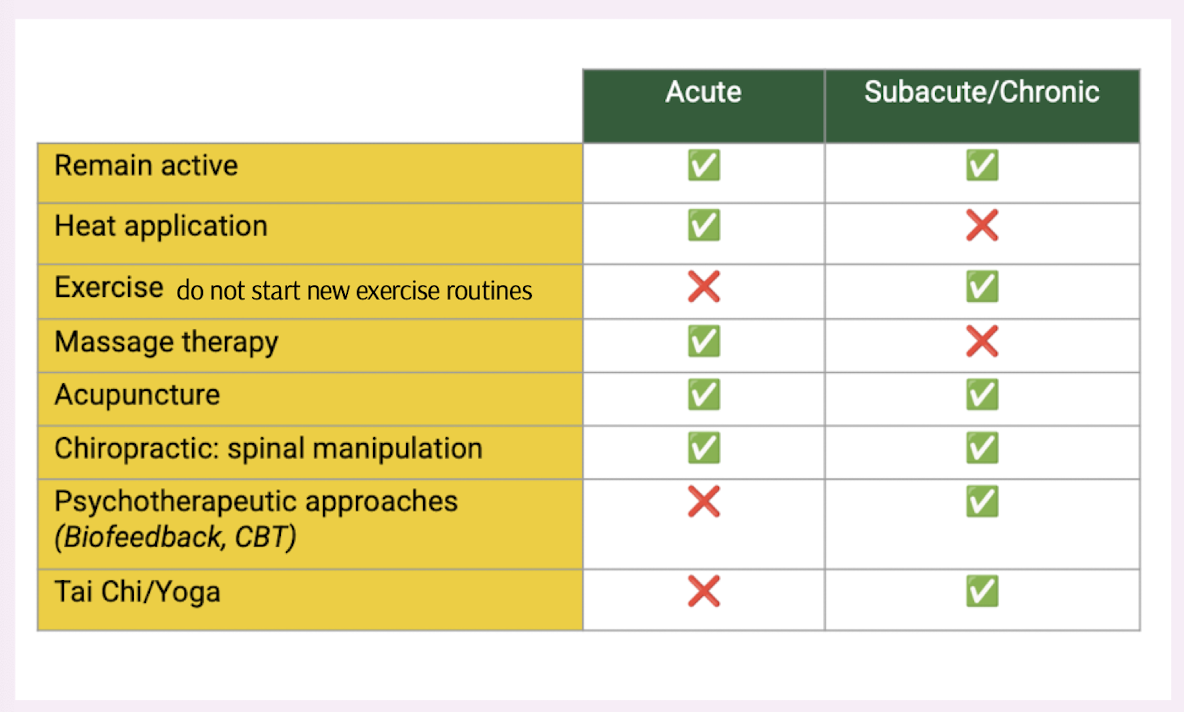
risk factors for lower back pain
age (common 45-64 years old), tall, climbing stairs often, stress
poor general health, heavy lifting, physical disabilities, sciatica, whole-body vibration (e.g. work with jackhammer), obesity, smoking, pregnancy, high physical work demands, arthritis
lower back pain patient assessment
1. red flags
2. yellow flags
3.SCHOLAR-E/PQRST
4. PMHx (e.g. cancer, osteoporosis, uncontrolled chronic medical condition)
5. medication history (e.g. prolonged corticosteroid use)
6. allergies
7. social history (e.g. smoking, exercise, work that requires heavy lifting, truck driving)
8. complete the assessment and refer/offer appropriate management
lower back pain goals of therapy
relieve symptoms and promote rapid recovery
improve function and mobility
enhance quality of life
prevent or minimize re-injury
prevent progression to chronic pain minimize work absence
red flags for lower back pain
history or suspicion of cancer
signs of infection (especially in immunocompromised patients possible fracture (recent trauma, chronic corticosteroid use)
causa equina syndrome
chronic pain (> 3 months)
sciatic conditions
rapid weight loss
neurologic deficit
inflammatory disorders
new onset under age 20 or new onset over age 50
yellow flags for lower back pain
negative pain beliefs
believe pain is severely debilitating
fear of movement/activity
mental health concerns -> depression or anxiety
work-related issues -> belief they will never return to work
passive coping style -> relies solely on passive treatments and avoids active participation in care
social withdrawal
reduced social interactions
poor support systems
lower back pain non-Rx oral NSAIDs
ibuprofen 200-400 mg PO Q6-8H max 1.2g/day for self-care
naproxen 220 mg PO 1-2x/day, max 440mg/day for self-care
lower back back non-Rx acetaminophen
current guidelines do not support acetaminophen for lower back pain, evidence shows limited benefit
lower back pain non-Rx codeine combinations (Tylenol 1)
limited evidence supporting use in lower back pain
not recommended as a routine treatment option
lower back pain Rx options
NSAIDs
muscle relaxants
lower back pain Rx muscle relaxants
limited evidence of benefit
not recommended with NSAIDs
consider only if NSAIDs failed/contraindicated
Rx muscle relaxants preferred to OTC options, if needed use cautiously due to side effects
Rx muscle relaxants
baclofen 5 mg TID increase gradually to max 20 mg TID
cyclobenzaprine 5-10 mg PO TID
lower back pain monitoring
effectiveness -> pain relief, function/mobility improvement, trial each agent 2-4 weeks at optimal dose
safety -> medication-specific AEs, impact on activities of daily living, risk factors for complications
lower back pain follow-up
pharmacist to follow up on days 3, 7, 14, 28
refer to healthcare practitioner as required
lower back pain CAM
Devil’s Claw (Harpagoside 50-100 mg PO daily)
potential interactions with drugs due to CYP2C9/3A4
Comfrey root (topical)
white willow bark* (salicin 120-240 mg PO daily)
cayenne* (topical)
* = can manage chronic
tension-type headaches classifications
primary: no identifiable underlying cause
e.g. tension-type, migraines, cluster headaches
secondary: caused by specific underlying condition or substance
e.g. medication-induced, HTN, infection
cranial nerve disorders: pain from specific nerve dysfunction/damage
e.g. trigeminal neuralgia
tension-type headaches epidemiology
may be episodic or chronic (>15 days per month)
most common primary headache
slightly more prevalent in females
mean onset 25-30 years, peaks in 30's
exact pathophysiology unknown
risk factors: young age, female, poor general health status, work-related stress, sleep disturbances
infrequent episodic tension-type headaches
<1 day/month, <12 days per year
at least 10 episodes when headache occurs
frequent episodic tension-type headaches
1-14 days/month, >12 but less than 180 days/year
>3 month duration
at least 10 episodes when headache occurs
chronic tension-type headaches
>15 days/month
>3 month duration
> 180 days/year
frequent episodic tension-type headaches diagnosis
frequency, duration, other description of frequent episodic TTH + ALL of the following criteria:
duration: 30 minutes-7 days
headache characteristics (need minimum 2)
bilateral location
pressing and/or tightening mild-moderate intensity
not worsened by physical activity
associated symptoms (must have BOTH)
no N/V
no more than ONE of: photophobia phonophobia
not attributed to another disorder
tension-type headaches differential diagnosis
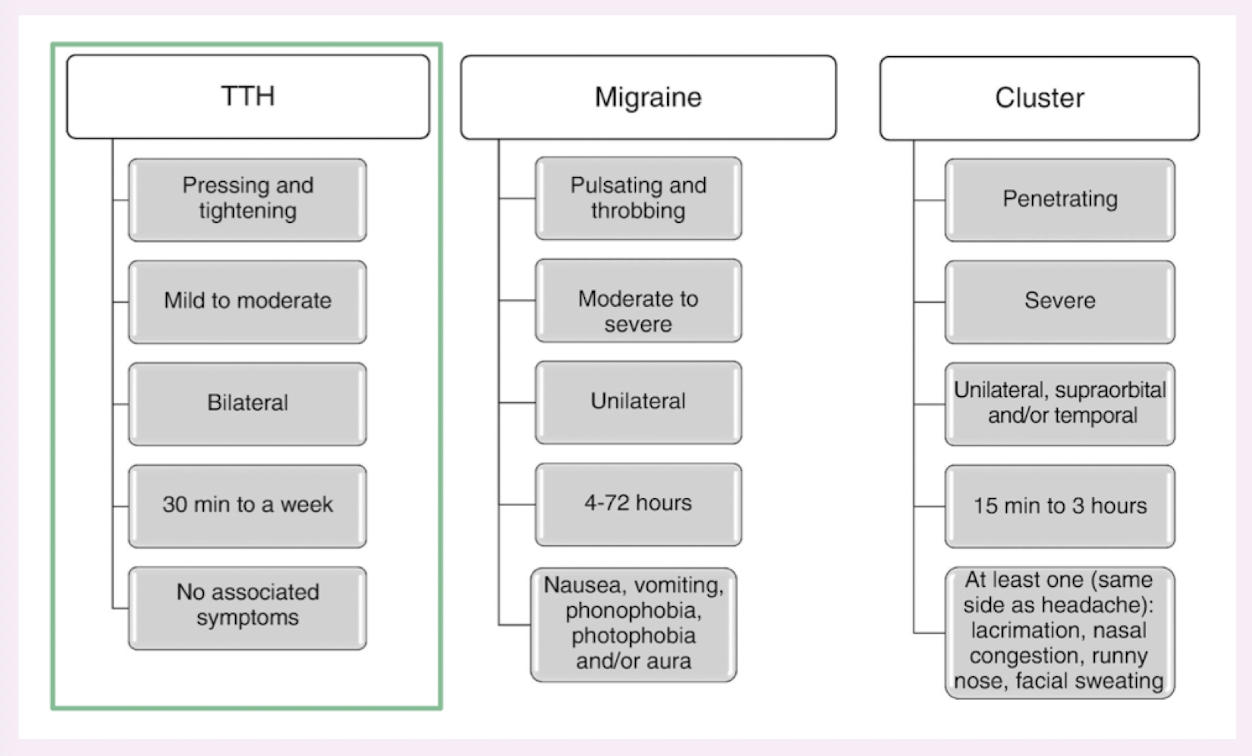
red flags for tension-type headaches
sudden “thunderclap” headache - worst ever experienced
mental status changes (confusion, decreased alertness)
new onset of symptoms >50 years of age
fever with neck stiffness
systemic symptoms (fever, chills)
recent change in headache pattern
pregnancy or postpartum
immunosuppressed individuals
positional changes affect headache severity
triggered by coughing/sneezing
history of cancer
vision changes or swelling around the eyes
eye pain with autonomic symptoms (e.g. eye redness, tearing, facial flushing)
progressive worsening
recent head trauma
medication-induced or painkiller overuse
tension-type headaches assessment
signs of stroke:
F: face drooping?
A: arms - can you raise both?
S: speech - slurred or jumbled?
T: time -> to call 911
1. red flags
2. SCHOLAR-E
3.PMHx, medication Hx, allergies
4. Social Hx (e.g. sleep, stress levels, hydration, EtOH use, physical activity)
5.complete assessment and refer/offer appropriate management
tension-type headaches algorithm
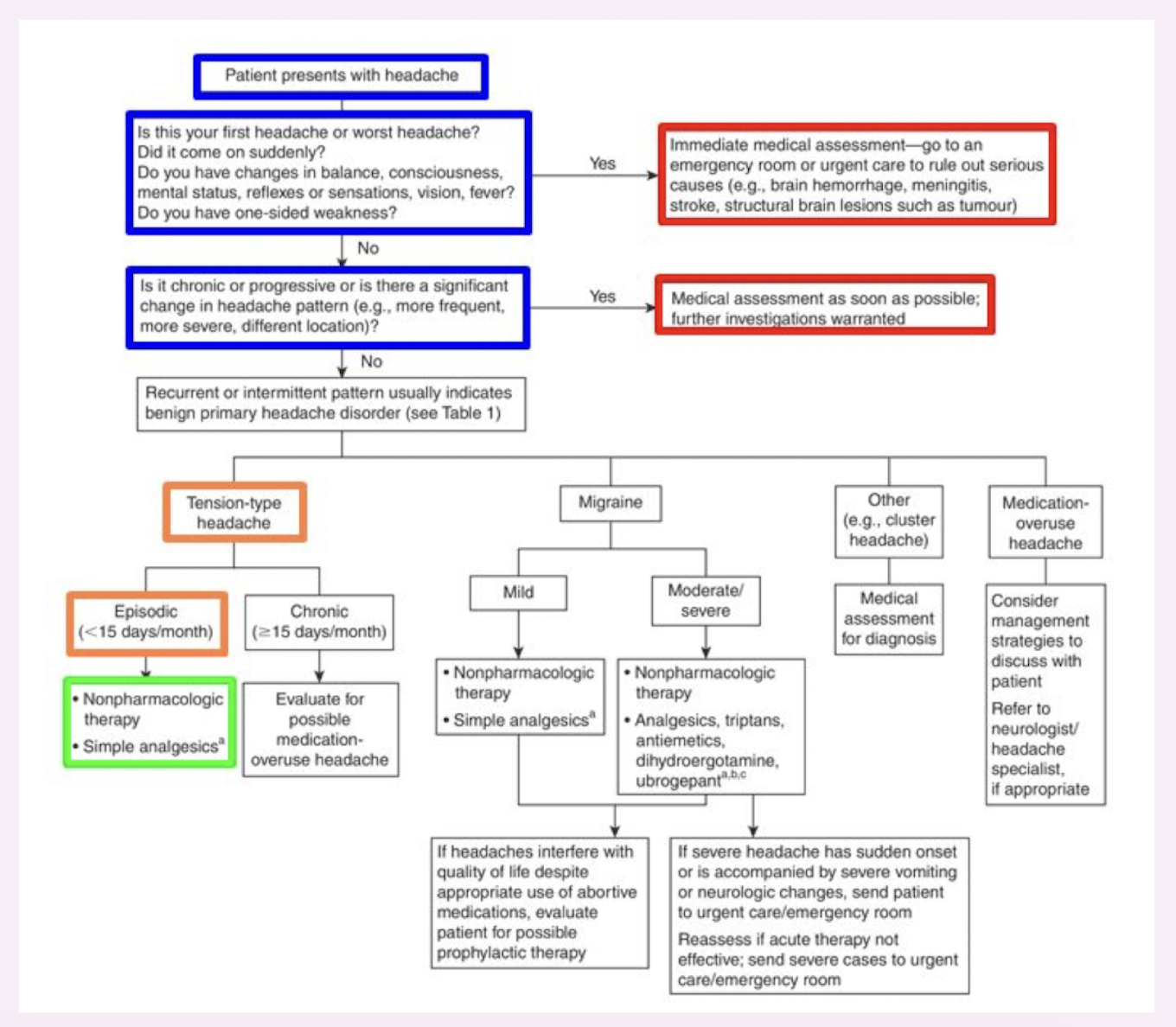
tension-type headaches goals of therapy
achieve timely, consistent pain relief (within 2 hours)
minimize frequency of future episodes
prevent complications and adverse effects of drug therapy
maintain ability to perform daily activities
promote effective self-management to reduce healthcare resource utilization
tension-type headaches monitoring
effectiveness -> pain relief within 2 hours of acute treatment, frequency of headaches, impact on daily activities/function, sleep quality, stress levels
safety -> medication specific AEs, signs of medicaiton overuse headache
tension-type headaches follow-up
patient to daily self-monitor using headache diary
pharmacist to follow up after 7 days and again after 30 days
refer to healthcare practitioner as required
tension-type headaches non-pharm managment
patient education and reassurance
maintain headache diary
track frequency/severity, identify triggers, monitor treatment response
lifestyle modifications
sleep hygeine, regular exercise, hydration, balanced nutrition, stress management, avoiding triggers (e.g. EtOH, chocolate, strong odors)
during an attack
rest in dark quiet room, heat/ice therapy to head, stress reduction
psychological interventions
tension-type headaches pharmacological management
start treatment ASAP treat with analgesics
NSAIDs, acetaminophen
do not use more than 15 days/month to avoid MOH (medication overuse headache)
caffeine combination products (e.g. acetaminophen + caffeine)
provides enhanced efficacy
not greatly favoured due to potential for caffeine withdrawal headache
when to consider prevention therapy for tension-type headaches
patient with:
1. frequent episodic TTH or chronic TTH AND
2.any of the following:
a.simple analgesics are ineffective
b.analgesics are poorly tolerated
c.analgesics are contraindicated
options include: amitriptyline, venlafaxine, mirtazapine
allow 2-3 months for full therapeutic effect
pathophysiology of viral rhinitis (common cold)
entry of virus into nasal cell through receptors -> infects nasal epithelial cells damaging tight junctions/disrupting membranes -> cell death
viral inflammation -> clinical symptoms appear due to injury of nasal mucosal linings
increased vascular permeability, glandular secretion, vasodilation
cholinergic stimulation -> increases mucous gland secretion and sneezing
viral shedding can continue for up to 3 weeks, even after viral replication peaks at 48 hours
symptoms of viral rhinitis
(symptoms peak in 2-4 days, resolve around day 7)
sore throat (mild, dry, sore, scratchy) - generally resolves in a few days (usually occurs first)
nasal congestion and rhinorrhea (later symptom)
discharge is clear and watery at beginning, can become purulent
sneezing during first few days
cough (can last 2-3 weeks or longer, dry initially, can become productive)
headache
chills (first few days)
malaise (later symptom)
fever (infrequent in adults, low fever common in children)
dyspnea (shortness of breath) is uncommon
viral rhinitis patient assessment
1. red flags
2. SCHOLAR-E
what sequence in appearance of symptoms?
any fever or pain symptoms?
any cough? wet or dry? how long has it lasted?
exposure to close contacts who were ill?
variation in symptoms throughout the day?
3. PMHx - personal or family hx of asthma, COPD, immunocompromising conditions
4. medication Hx - immunosuppressive medications
5. Social Hx - e.g. tobacco/marijuana use, environmental/occupational exposure, recent travel
6. vaccination history
7. allergies
8. complete assessment and refer appropriate management
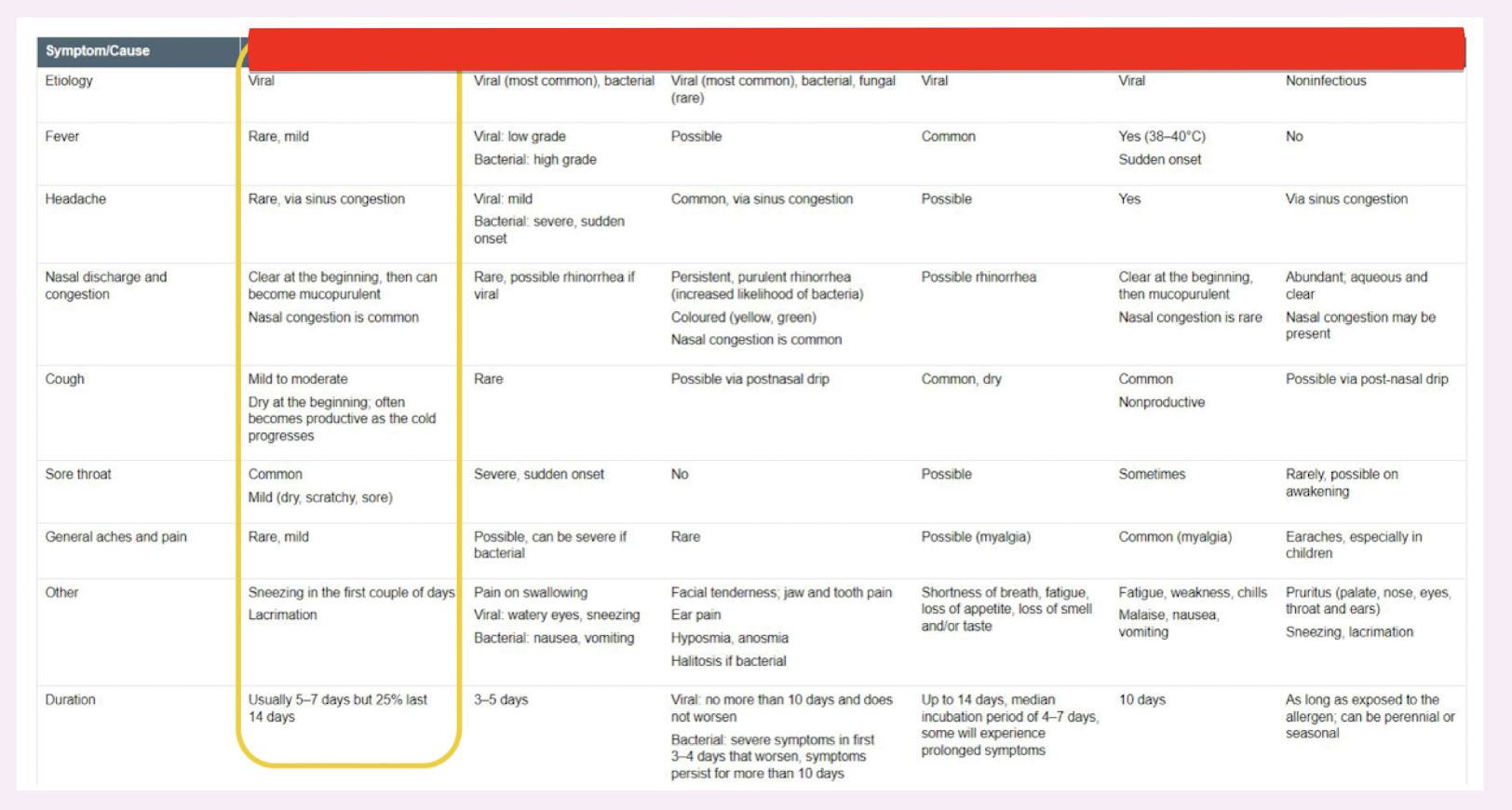
viral rhinitis differential diagnosis (adults)
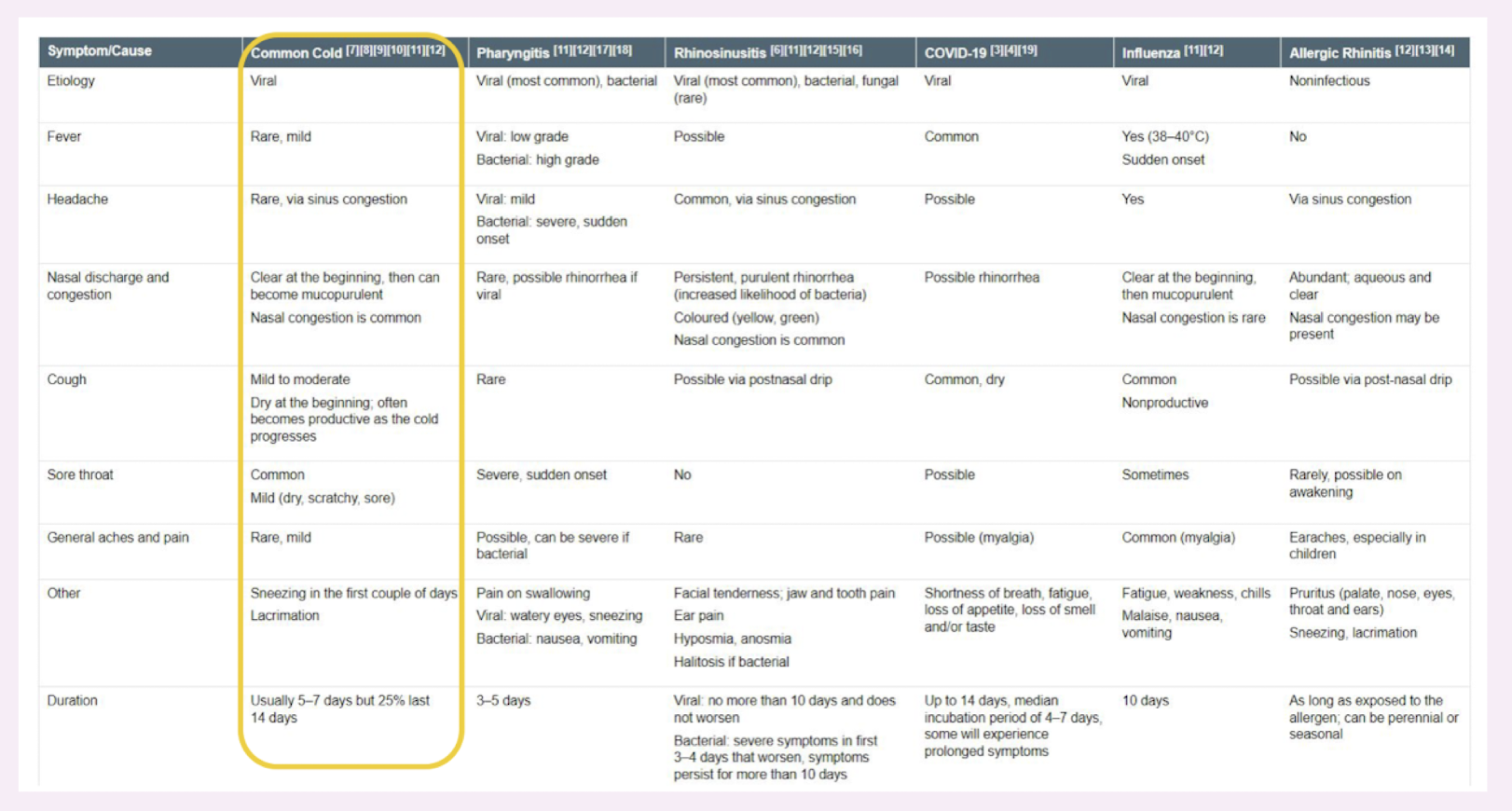
viral rhinitis differential diagnosis in children
croup
early symptoms - mild fever, runny nose, fatigue, sore throat, cough
hoarseness
dyspnea
wheezing that gets louder when breathing in
barking cough that is seal-like (dry and unproductive)
symptoms worse at night
being in a warm shower with steam often helps symptoms
otitis media
fever, particularly a few days into having a cold
earache or child pulling or fingering ear
irritability and/or lethargy
pus coming out of ear
viral rhinitis CPS algorithm

viral rhinitis goals of therapy
alleviate symptoms within 2 weeks
eradicate viral infection or shorten duration of viral infection
lessen interference with activities of daily living
prevent complications of viral infection and adverse effects from medications
prevent person-to-person transmission