Retina Anatomy Part 3
1/59
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
60 Terms
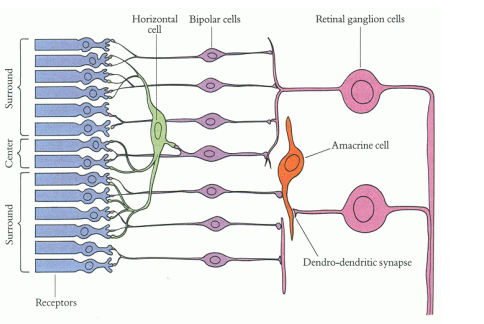
Horizontal Cells
• Interneuron of the outer retina
• Composed of a cell body with a nucleus and one axon with several short dendrites with branching terminals
• Can branch extensively which it allows one part of the retina to influence another part of the retina
• Highest concentration in the fovea region excluding the foveola
• The nucleus of horizontal cells is found in the inner nuclear layer
• Synapses with photoreceptor synaptic terminals (Rod spherules and cone pedicles) and dendrites of bipolar cells in the outer plexiform layer
• Transfers information in horizontal direction parallel to retinal surface
• Horizontal cells are also joined together through gap junctions
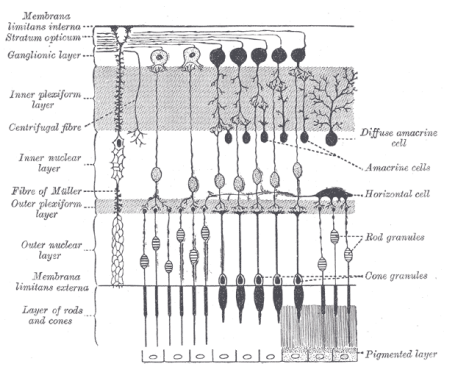
Function of Horizontal Cells
Modulates and transforms information received from photoreceptors
Integrates and regulates activity of multiple photoreceptor cells
Allows eyes to better adjust going from bright to dim and dim to bright illumination
Makes adjustments to signals sent to bipolar cells
Provides inhibitory feedback to photoreceptors with the inhibitory neurotransmitter GABA
3 Types Of Horizontal Cells
HI
HII
HIII
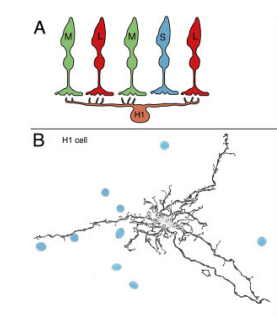
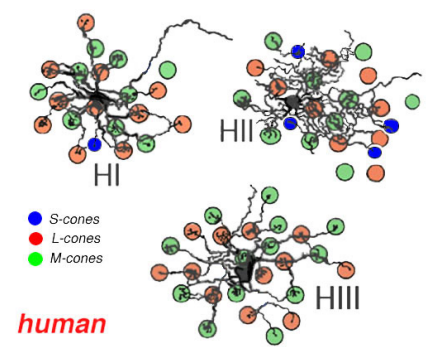
HI
•Dendrites that synapse with 7-18 cones (Number of synapses with cones increase in the peripheral retina) and a large, thick axon ending in a fan-shaped expanse of terminals that end in rod spherules more than 1mm away
•Dendrites synapse with medium and long wavelength cones with little to no contact with short wavelength cones
• Overall function: Enhances visual acuity and contrast
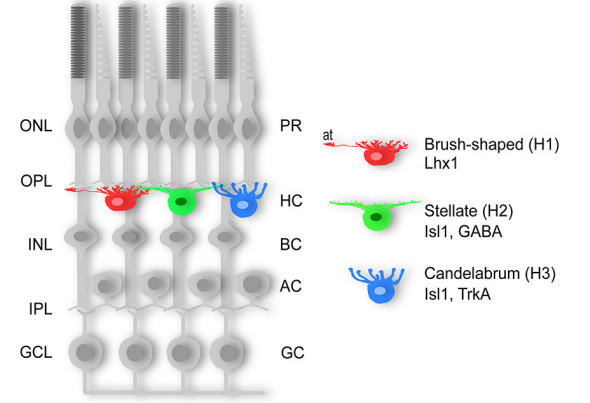
HII
•Makes dendritic connections and some short axonal connections with short wavelength cones in addition to some dendritic connections with long and medium wavelength cones
•Overall function: Enhances visual acuity and contrast
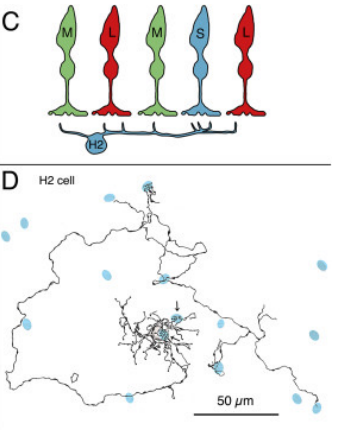
HIII
• Large dendritic tree that synapses with many cones (9-12 cones in the macula region and 20-25 in the peripheral region)
• Makes contact with medium and long wavelength cones with no contact with short wavelength cones
• Overall comes in contact with more cones than a HI cell
• It is unknown where the axon of the HIII cell synapses
• Overall function: Enhances color vision
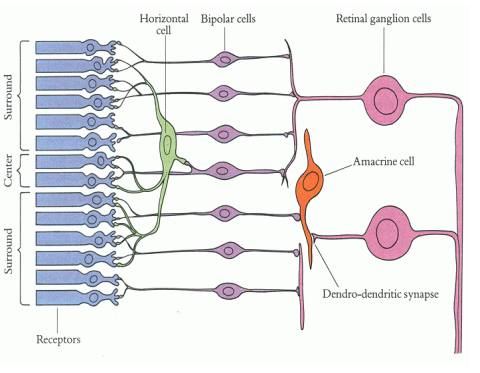
Amacrine Cells
• Interneuron of the inner retina
• Most diverse class of neurons in the retina (There are 30-40 types of amacrine cells)
• First site in the retina where action potentials are generated
• Composed of a large cell body with a lobulated nucleus and a dendrite process with extensive branches (Typically does not have an axon)
• The nucleus of amacrine cells is found in the inner nuclear layer
• Synapses with axons of bipolar cells and dendrites of ganglion cells in the inner plexiform layer
• Carries information horizontally as well as vertically
• Because dendrites of an amacrine cell can branch extensively, one part of the retina can influence another part of the retina
• Amacrine cells are also joined together through gap junctions
Function Of Amacrine Cells
Receives synaptic input from bipolar cells (Connects to axons of bipolar cells)
Provides input to ganglion cells (Connects to dendrites of ganglion cells)
Gives feedback to bipolar cells
Modulates information that reaches ganglion cells from bipolar cells
Provides inhibitory feedback to ganglion cells and bipolar cells with the inhibitory neurotransmitters called glycine and GABA
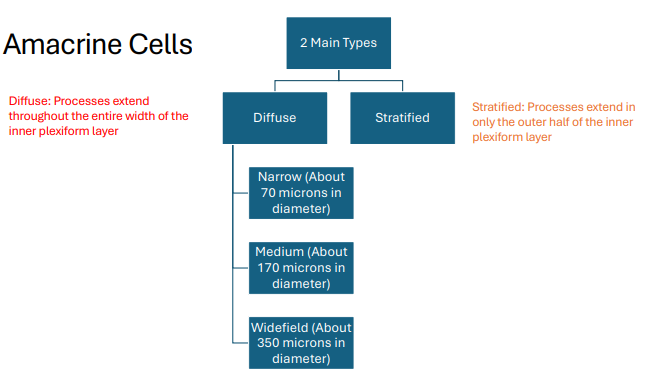
30-40 Types Of Amacrine Cells That Are Either Diffuse Or Stratified
Diffuse: Processes extend throughout the entire width of the inner plexiform layer
Stratified: Processes extend in only the outer half of the inner plexiform layer
AI, AII, A17
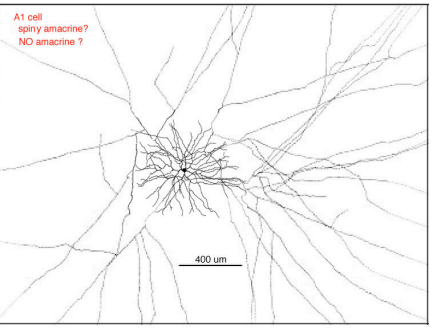
AI Cell
•Diffuse type with widefield diameter
• Spiny with highly branched dendrites and axon-like processes
• Overall function
-Provides long range inhibition of ganglion cells
-Provides inhibitory feedback to bipolar cells
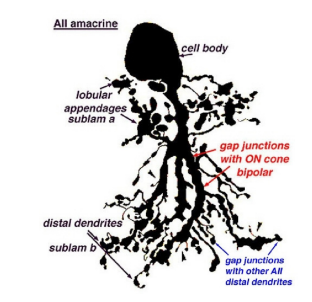
AII cell
• Diffuse type with narrow diameter
• Makes up 10-15% of all amacrine cells
• Most dense in the foveal region
• Overall function
-A major carrier of the signal from the rods as it synapses to ganglion cells. In fact, it is a conduit by which rod signals reaches ganglion cells (An AII cell may receive input from as much as 300 rods through 80 rod bipolar cells)
-Synapses with axon terminals of cone bipolar cells and plays a role with the signals sent to the ganglion cells
A17 Cell
•Diffuse type with widefield diameter
• Synapses with only rod bipolar cells
• Overall function:
-Provides inhibitory feedback to rod bipolar cells
-Interconnects rod bipolar cells in the IPL
-Modifies signal from rod bipolar cells to AII cells
Interplexiform Neurons
•Last major class of retinal neurons to be discovered
•Composed of a large cell body
•Extends into both plexiform layers and conveys information between these layers
Neuroglial cells
• Provides structure and support to the retina
• Plays a role in neural tissue reaction to injury and infection
•Does not participate directly in synaptic interactions and electrical signaling
Three types: Muller, Microglial, Astrocytes
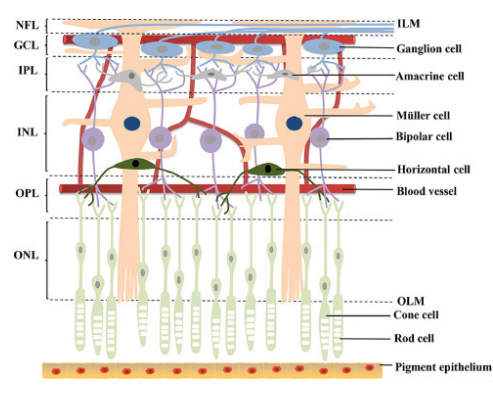
Muller Cells (Neuroglial)
• Most common type of glial cell found in the retina (There are about 10 million Muller cells throughout the retina)
• The nucleus of a Muller cell is found in the inner nuclear layer and projects thick and thin processes in both directions to the internal limiting membrane (The ILM is composed of terminations of Muller cells called footplates) and external limiting membrane (With microvilli extending into the sub-retinal space)
• Surrounds all neural cell types except at the synapses
• Fills in most of the space of the retina not occupied by neuronal elements
Function of Muller Cells
Provides structural support to neuronal cell bodies as they reside in tunnels within the Muller cells
Prevents mechanical deformation of the retina by providing structural support throughout the retina
Controls homeostasis by regulating concentration of potassium ions in the retina
Maintains extracellular pH by getting rid of metabolic waste such as carbon dioxide and ammonia
Recycles glutamate, glycine, and GABA which helps protect neurons from exposure to excess neurotransmitters
Metabolizes, synthesizes, and stores glycogen which is used to fuel aerobic metabolism in neurons
Helps maintain the inner blood-retina barrier
Helps guide light directly to the photoreceptors
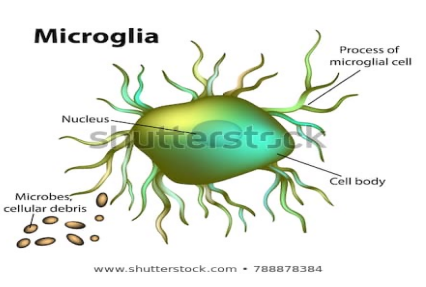
Microglial (Neuroglial)
•Can be found anywhere in the retina as well as any retinal layer
•Increases in response to tissue inflammation and injury
• Overall function - After retinal inflammation or injury, microglial cells will phagocytize degenerating retinal neurons
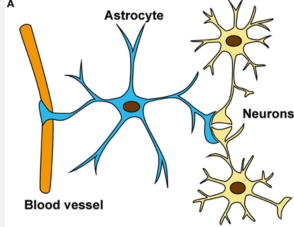
Astrocytes (Neuroglial)
• Almost entirely restricted to the nerve fiber layer with some extension into the ganglion cell layer
• Largest density of astrocytes are found around the optic nerve (Astrocytes decline in density away from the optic nerve)
• Not found at the fovea
Morphology changes based on location in the retina
-Near optic nerve: Flattened cell body with fibrous radiating elongated processes
-Peripheral retina: Symmetrical stellates

Function Of Astrocytes
Provides insulation and support to superficial retinal capillaries and nerve fibers
Helps maintain the inner blood-retina barrier
Controls homeostasis by regulating concentration of potassium ions in the retina
Metabolizes, synthesizes, and stores glycogen which is used to fuel aerobic metabolism in neurons
Contributes to the ILM
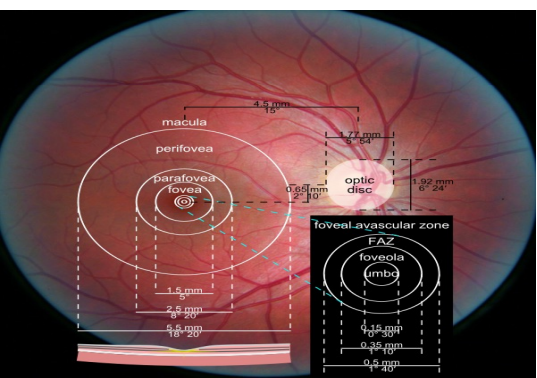
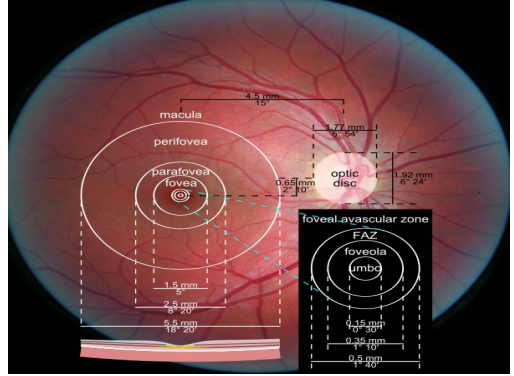
Macula
• Also called the area centralis
• 5.5mm in diameter (About 4DD in size)
• Lies within the temporal arcades, within the superior and inferior arcades, and 1-2mm temp from the temporal side of the optic disc
•Corresponds to 15-20 degrees of visual field
•Includes the perifovea, parafovea, and fovea
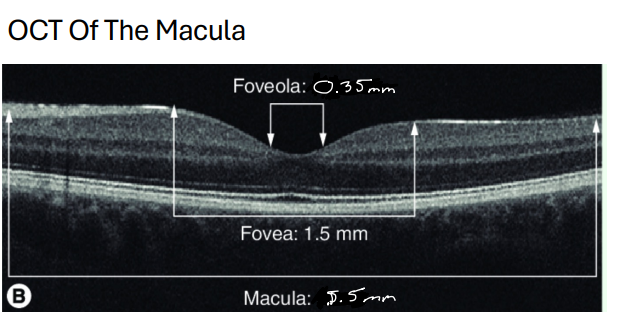
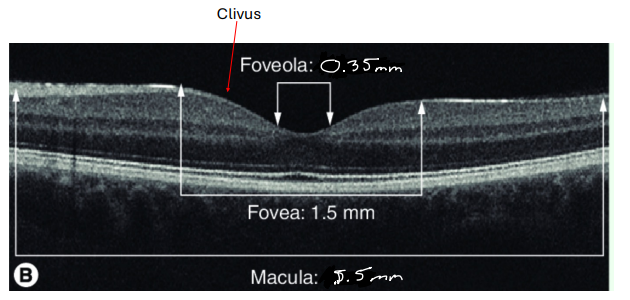
Fovea
• Shallow depression in the center of the macula (Depression is due to displacement of retinal neurons)
• 1.5mm in diameter (About 1DD in size)
• 0.25mm thick
• About 3.7mm temp from the temporal side of the optic disc to the center of the fovea
• Corresponds to 5 degrees of visual field
• Curved wall of the depression is the clivus
• The fovea also includes the foveola and umbo
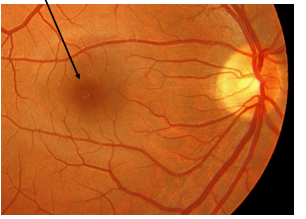
Why Does The Fovea Have A Dark Appearance With A Yellow Hue?
High concentration of the lutein and zeaxanthin, which belongs to the xanthophyll family of carotenoids, is found at the fovea (Also called macular pigment)
*Xanthophylls tend to be yellow in color
Macular pigment is located in the outer plexiform layer, Muller cells, photoreceptor inner fibers, and the rod outer segments
RPE cells are the tallest, most dense, most pigmented at the fovea. Although amount of pigment in the RPE varies from person to person
Choroidal capillary bed is thickest at the fovea
Macular Pigment
• Xanthophylls are found throughout the retina
• There is more lutein than zeaxanthin in the retina outside the fovea while there is more zeaxanthin than lutein at the fovea
• A newborn has very little, if any, of these pigments, and accumulates them from diet
• These pigments act as filters by absorbing damaging short wavelength light and provides antioxidant protection of retinal tissue
Foveola
• 0.35mm in diameter
• 0.13mm thick
• Corresponds to 1.25 degrees of visual field
• The very center of the foveola is called the umbo
• Contains densest population of cones (No rods are found at the foveola)
• Ratio of cone cell to ganglion cell is 1:1 (Specialized for discrimination of detail and color vision)
• Retinal elements/neurons are displaced at the foveola in order to allow light to reach the photoreceptors without obstruction (Even Muller cells are weaker, fewer in number, and diagonally oriented at the fovea especially the foveola)
• The photoreceptor axons are longer at the foveola (Called Henle fibers). They stretch obliquely in order to reach the displaced bipolar and horizontal cells.
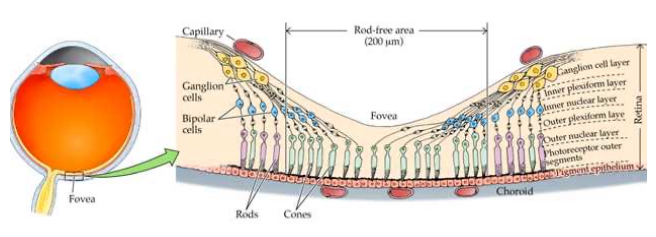
What Layers Of The Retina Are Found At The Foveola?
RPE/Bruch’s complex
Interdigitation zone
Outer segments of photoreceptors
Ellipsoid zone
Myoid zone
ELM
ONL
Henle fiber layer
ILM
Why Is There A Bump Along The Ellipsoid Zone And ELM Directly Under The Umbo?
• Looking at the area of the RPE and interdigitation zone, directly underneath the ellipsoid bump, it is slightly thicker (Subtle) due to longer and more densely packed RPE cells. This contributes to pushing up (Toward inner retina) the outer segments of the photoreceptors which in turn pushes up the ellipsoid zone
• The bump of the ellipsoid zone and ELM is also due to the cones being more densely packed and the outer segment of the cones being more rod like in shape
Capillary Free Zone Of The Macula (Also Called The Foveal Avascular Zone)
• 0.4-0.5mm in diameter
•Includes the foveola and part of the fovea
• Lack of blood vessels in this area further allows light to get to the photoreceptors without obstruction
* The capillary free zone refers to retina vasculature but not the choroid because the choriocapillaris is found in the retinal capillary free zone.
Central Foveal Reflex
•Pinpoint reflection caused by the parabolic shape formed by the clivus (Shape in some patients may not be parabolic so reflection may vary in shape and sharpness)
• Aging and certain macula pathologies may lead to loss of the foveal reflex
Parafovea
•Inner area of the macula that surrounds the fovea
• 0.5mm in diameter surrounding the fovea (Does not include the fovea)
• Largest accumulation of retinal bipolar cells and ganglion cells are found in the parafovea
•Inner nuclear layer is about 12 cells thick and ganglion cell layer is about 7 cells thick in the parafovea
Perifovea
• Outer area of the macula that surrounds the parafovea
• 1.5mm in diameter surrounding the parafovea (Does not include the parafovea and fovea)
• Begins where ganglion cell layer is 4 cells thick and ends when the ganglion cell layer is 1 cell thick
• Here orientation of retinal elements/neurons revert back to a more vertical orientation (Henle fiber layer changes into the outer plexiform layer)
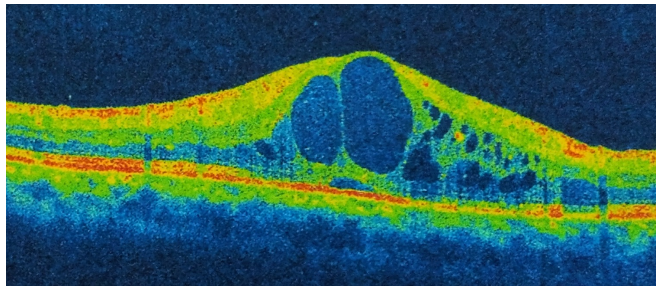
Clinical Example- Cystoid macular edema
Less retinal layer with obliquely oriented retinal elements/neurons.
Muller cells are weaker and fewer in number
No foveal pit → no foveal reflex
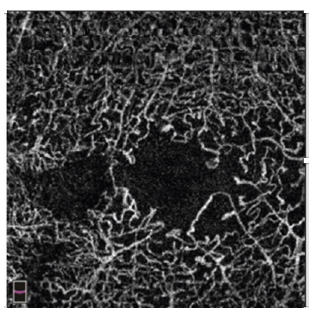
Clinical Example- Enlargement of the foveal avascular zone
Larger fovea avascular zone
Common in diabetics
Further Out In The Peripheral Retina
• Rods disappear and are replaced by malformed cones
• Nuclear layers merge with plexiform layers
• Neural retina becomes a single layer of irregular cells that continue as the nonpigmented epithelium of the ciliary body
• The RPE is continuous with the outer pigmented epithelium of the ciliary body
• The ILM is continuous with the internal limiting membrane of the ciliary body
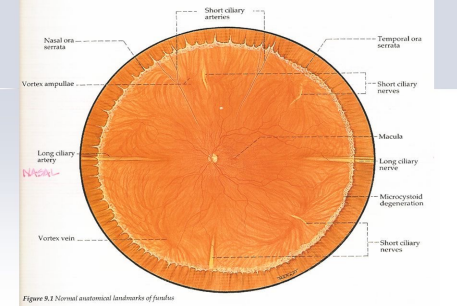
Ora Serrata
•Peripheral termination of the retina
•The vitreous base straddles the ora serrata
•Transition zone between the ciliary body and retina
•The nasal side is more scalloped or serrated than the temporal side (Ora serrata nasally is easier to discern than the ora serrata temporally)
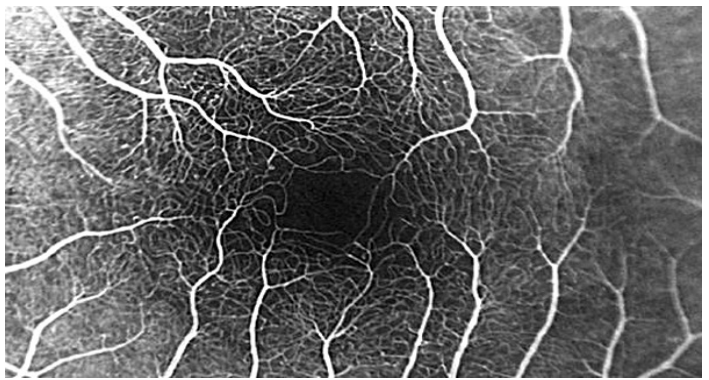
Blood Supply Of The Inner Retina
•The central retinal artery provides the vascular supply to the inner retina via perfusion
•The inner retina is completely vascular (Except at the foveal avascular zone)
•Accounts for 20-30% of the blood flow to the retina
Blood Supply Of The Outer Retina
• The choroidal capillary bed (Choriocapillaris) provides the vascular supply to the outer retina via diffusion through Bruch membrane and the RPE
• The outer retina up until the inner aspect of the outer plexiform layer is completely avascular (The inner aspect of the OPL receives its vascular supply from the central retinal artery)
• Accounts for 65-85% of the blood flow to the retina
Watershed Zone (Receives Dual Vascular Supply)
Outer Plexiform Layer
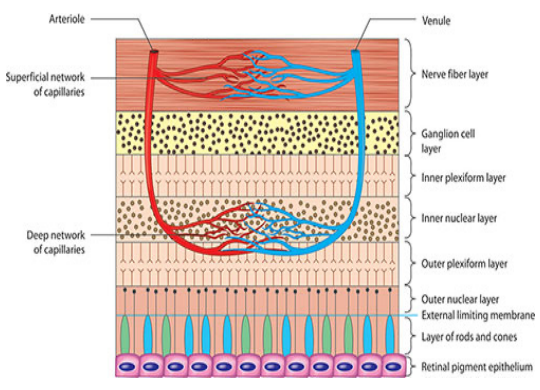
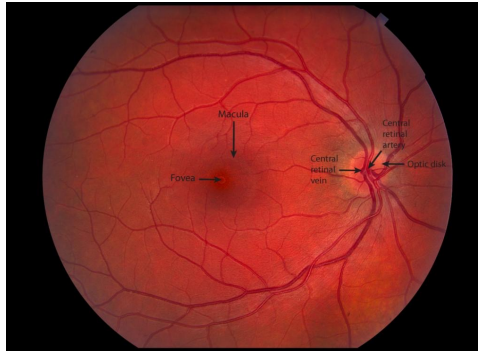
Blood Supply Of The Retina
•Lighter red colored blood vessels: Arteries and arterioles carry oxygenated blood
•Darker red colored blood vessels: Veins and venules carry deoxygenated blood
Inner Retina Blood Flow And Anatomy
•Starts with the ophthalmic artery which branches off the internal carotid artery
•The central retinal artery which branches off the ophthalmic artery enters the optic nerve about 8-15mm behind the globe
• The central retinal artery enters the retina through the nasal side of the optic disc and branches into superior and inferior arteries/arterioles as well as nasal and temporal arteries/arterioles. Bifurcations continue throughout the retina
• Retinal arteries and arterioles are located in the NFL
•From the retinal arterioles, capillaries form
•Retinal capillaries are made up of a single layer of unfenestrated endothelium surrounded by a basement membrane and pericytes which are contractile cells that help with blood flow
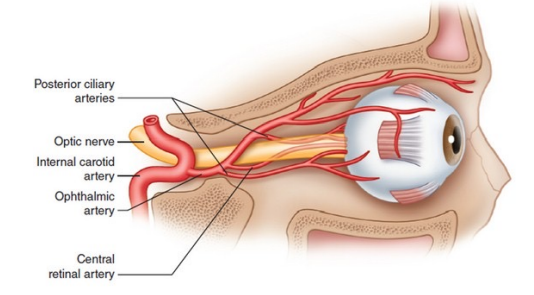
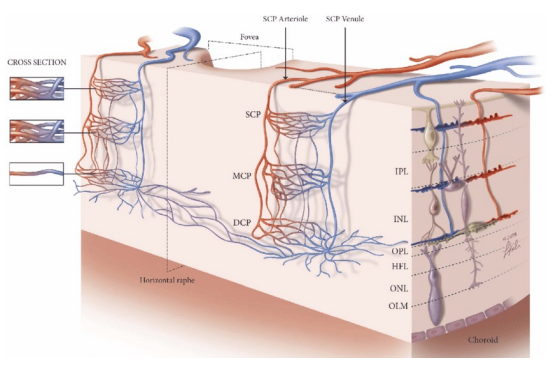
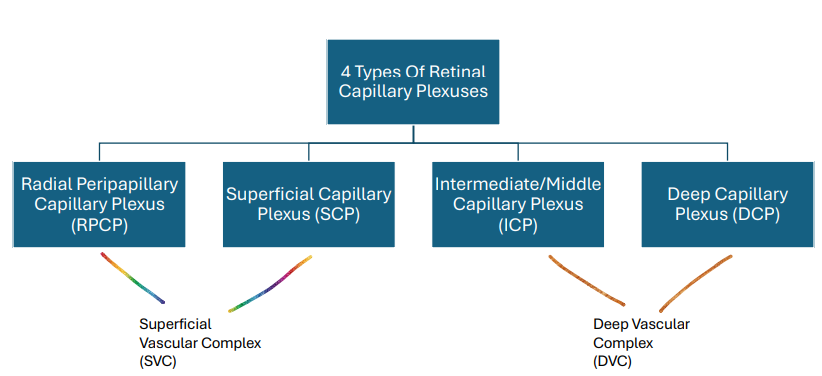
4 types of Retinal Capillary Plexuses
Radial Peripapillary Capillary Plexus (RPCP): Nerve fiber layer
Superficial Capillary Plexus (SCP): Majority found in the ganglion cells layer with part of it found in the inner plexiform layer
Intermediate/Middle Capillary Plexus (ICP): Part of it found in the inner plexiform layer with the majority found in the inner nuclear layer
Deep Capillary Plexus (DCP): Part of it found in the inner nuclear layer with the majority found in the outer plexiform layer
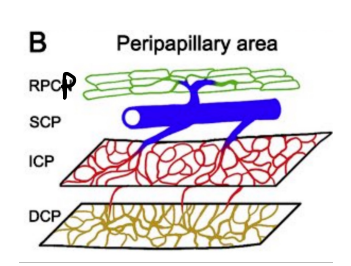
Location of Retinal Capillary Plexuses- Peripapillary area ( around optic nerve)
The radial peripapillary capillary plexus surrounds the optic nerve and follows the retinal nerve fibers
All 4 layers
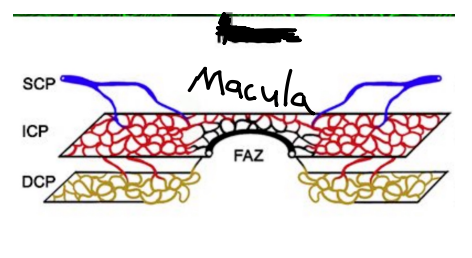
Location of Retinal Capillary Plexuses- Macula
The foveal avascular zone is free of all retinal capillaries
3 layers (missing Radial Peripapillary Capillary Plexus)
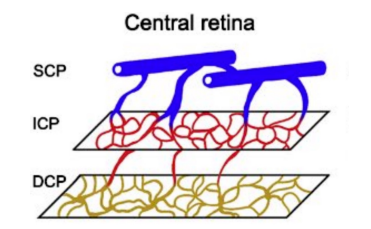
Location of Retinal Capillary Plexuses - Central Retina
3 layers (missing Radial Peripapillary Capillary Plexus)
Location of Retinal Capillary Plexuses - Periphery
2 layers (missing Radial Peripapillary Capillary Plexus and Intermediate/Middle Capillary Plexus)
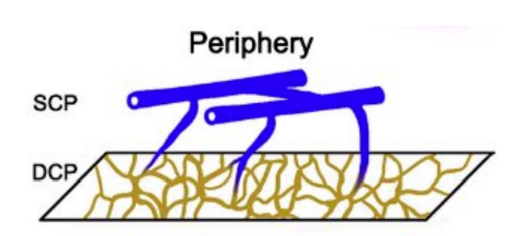
Inner Retina Vasculature
Maintains the inner blood-retina barrier
Should never leak
Inner Retinal Blood Flow
Maintenance of blood flow in the inner retina is controlled by autoregulation (Intrinsic ability of tissue to maintain constant blood flow regardless of changes in perfusion pressure*)
Changes in blood flow can occur due to changes in myogenic factors, endothelial cells within the vessels, and metabolic demands
Again autoregulation involves the inner retinal vasculature but more specifically it involves the arteries and arterioles as opposed to the capillaries.
Capillaries in the inner retina are not really able to autoregulate (Although in theory there is some autoregulation due to the pericytes found in the walls of capillaries)
Inner retinal vasculature has No autonomic innervation
IOP And Inner Retina Blood Flow
•Typically if the IOP of the eye increases, this is going to cause the perfusion to decrease due to constriction of the arteries and arterioles that occur in the presence of elevated IOP
•In response, the arteries and arterioles should dilate in order to keep homeostasis and maintain perfusion
Glaucoma And Inner Retina Blood Flow
• Glaucoma typically presents with IOP that is chronically elevated or IOP that is prone to spike significantly
• There is only so much the arteries and arterioles can autoregulate or they may lose their ability to autoregulate or there may be other issues going on like hypertension or diabetes that causes damage to autoregulation.
• Thus, if there is a breakdown in autoregulation, which happens often times in glaucoma, the arteries/arterioles will ultimately constrict and there will be a decrease in perfusion
Arterial Pressure And Inner Retinal Blood Flow
Typically if the arterial pressure increases, this would lead to an increase in perfusion in the retinal arteries and arterioles. Retinal arteries and arterioles would autoregulate and constrict in order to decrease perfusion and maintain homeostasis.
This is meant to protect capillaries from damage which are weaker and more susceptible to hyperperfusion as they are really unable to autoregulate (Thus, retinal capillaries are dependent on the autoregulation and perfusion that occurs in the retinal arteries and arterioles)
Hypertension And Inner Retinal Blood Flow
• The retinal arteries and arterioles are adept in dealing with a high pressure system as they are able to constrict and dilate (Due to their size and ability to autoregulate) more so compared to the retinal capillaries
• Now, there is going to come a point where arteries and arterioles lose their ability to autoregulate if the blood pressure is chronically elevated or has significant spikes.
This is eventually going to lead to retinal capillary damage as the retinal arteries and arterioles are no longer able to autoregulate the blood flow
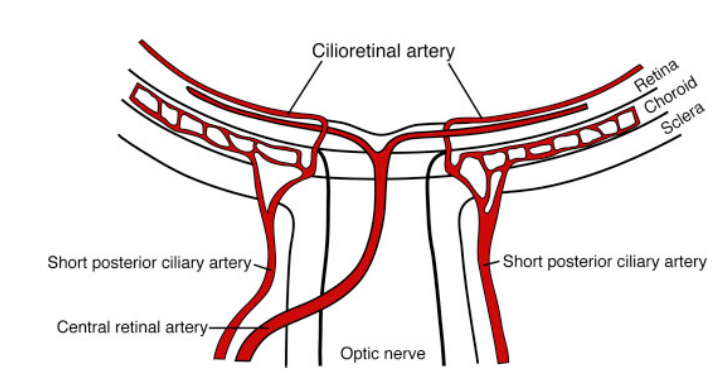
Cilioretinal Artery
•Origin is from the short posterior ciliary arteries (Choroidal vasculature) which branch off the ophthalmic artery
•Enters retina from the temp aspect of the disc and supplies the inner retina
•Found in 15-20% of the population
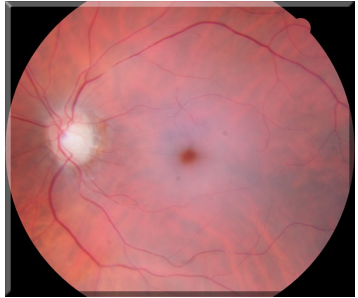
A Patient Presents to Clinic With A Central Retinal Artery Occlusion (CRAO)
Pale
Capillaries (supply inner retina) not getting blood/nutrients
permanent death of capillaries/retinal tissues
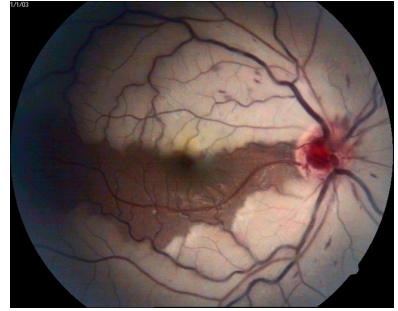
A Patient Presents To Clinic With A Central Retinal Artery Occlusion (CRAO) But With A Cilioretinal Artery?
Why Is Having A Cilioretinal Artery In The Presence Of A Central Retinal Artery Occlusion (CRAO) A Good Thing?
Can get blood flow to parts where cilioretinal artery goes (preserve central vision slightly)
Summary Of Inner Retinal Blood Flow
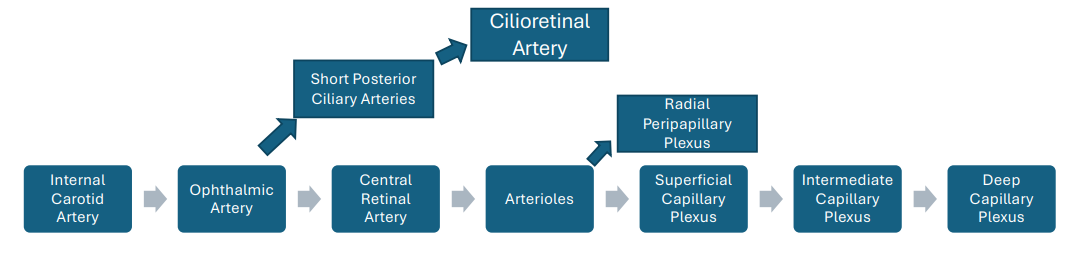
Outer Retina Blood Flow And Anatomy
• Starts with the ophthalmic artery which branches off the internal carotid artery
• Short posterior ciliary arteries branch off the ophthalmic artery and supply the posterior choroid which in turn supplies the outer retina
• Long posterior ciliary arteries branch off the ophthalmic artery and supply the anterior choroid which in turn supplies the ciliary body and iris
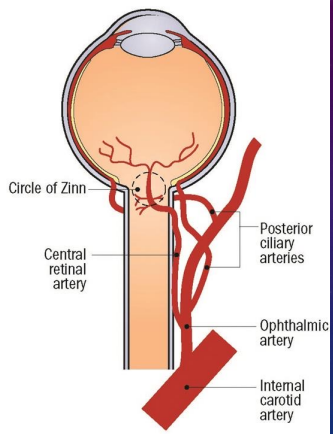
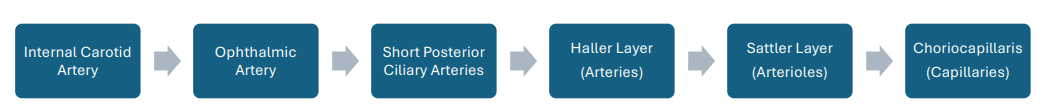
Outer Retina Blood Flow Chart
*Keep in mind that even though the choriocapillaris has capillaries that are fenestrated, the RPE and Bruch membrane maintains the outer blood-retina barrier
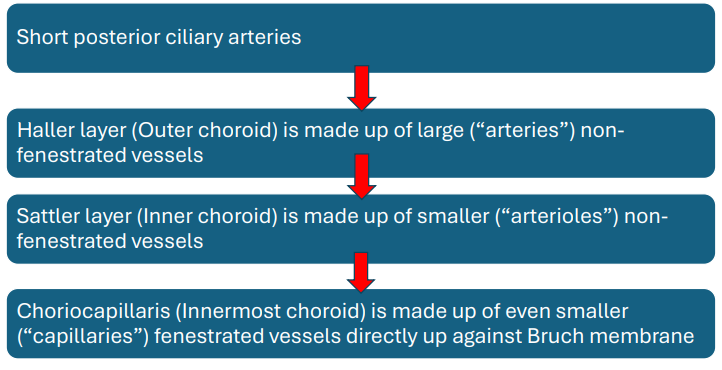
Outer Retina Blood Flow
• Choroidal vessels are not able to autoregulate
• Choroidal vasculature does have autonomic innervation as it is innervated by the parasympathetic nervous system, sympathetic nervous system, and sensory fibers of the trigeminal ganglion (Autonomic innervation is found more so in Sattler compared to Haller layer)
If the parasympathetic nervous system is activated, this will lead to vasodilation and an increase in choroidal blood flow
If the sympathetic nervous system is activated, this will lead to vasoconstriction and a decrease in choroidal blood flow
Activation of the trigeminal nerve has been shown to lead to vasodilation
Why Is Choroidal Vasculature Susceptible To Damage From High Blood Pressure?
• Since choroidal vessels tend not to be able to autoregulate like the retinal vasculature (Although there is debate on this), the choroidal vasculature is going to be more dependent on perfusion pressure
• Systemic changes in blood pressure drive perfusion pressure in the choroid
• Increases in perfusion will lead to damage to the choriocapillaris as well as an increase in leakage as the choriocapillaris is fenestrated
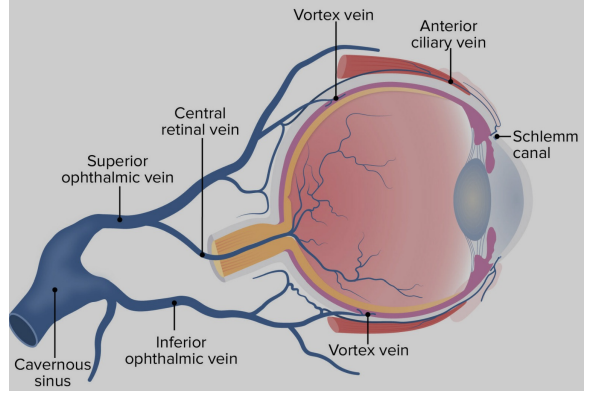
Venous Drainage
• Venous drainage of the inner retina occurs through the branch retinal veins into the central retinal vein. The central retinal vein drains either to the superior ophthalmic vein to the cavernous sinus or directly to the cavernous sinus (Depends on the patient’s eye anatomy)
• Vortex veins of the choroid drain the outer retina and choroid. Vortex veins drain into the superior and inferior ophthalmic veins which end up in the cavernous sinus
Age And The Retina
• Number of retinal neurons will decrease as a patient gets older
• Ganglion cell loss especially at the fovea will increase as a patient gets older (Lose about 0.2% or 0.2 microns per year)
• Rod density decreases (Does not appear to affect scotopic sensitivity)
• Cone density decreases at the fovea (Controversial)
• Number of astrocytes and Muller cells decrease
• Number of RPE cells decrease
• RPE cell loss is accompanied by hyperplasia of adjacent RPE cells (Regular hexagonal shape is lost when this happens)
• Lipofuscin increases at the level of the RPE and the cone inner segments
• Loss of the foveal reflex