2. pulmonary system: Anatomy of the Cardiovascular and Pulmonary Systems_condensed
1/22
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
23 Terms
Ventilation: inspiration and expiration: inspiratory muscles
inspiratory muscles increase the volume of the thoracic cavity by contracting
the result causes a decrease in intrathoracic pressure
homeostasis, air flows into lungs
Inspiration causes an increase in intra pressure (in the chest cavity)
- when you initially expand the volume vis the muscles- it decreases the pressure – as you breathe in you create more space so the molecules have more room to move around – this means atmospheric air rushes into the thoracic cavity
Ventilation: inspiration and expiration: expiration
expiration is the relaxation of the diaphragm and inspiratory muscles, causing a decrease in thoracic cavity volume
the result causes an increase in intrathoracic pressure
homeostasis, air flows out of the lungs
When you breathe out – you decrease the volume in the thoracic volume which increases the pressure – so the air going out to make homeostasis
Respiratory system: muscles of inspiration - primary muscles
diaphragm and external intercostals
Respiratory system: muscles of inspiration - accessory muscles
SCM
Scalenes
Upper Trapezius
Pectorals Major and Minor
Serratus anterior/serratus posterior superior
Rhomboids
Latissimus Dorsi
Thoracic Erector Spinae muscles
if you see that the SCM/scalene/upper trap are hypertrophies it may indicate that they are having breathing problems (pulmonary issues)
Diaphragm (inspiration) (where does it sit, what does it separate, what are the 3 major openings, what nerve)
can sit as high as the level of T4 at rest
separated the thoracic and abdominal cavities
three major openings in the diaphragm to allow for vessels to transverse
venal caval opening: inferior vena cava
esophageal opening: esophagus
aortic opening: aorta
phrenic nerve arises from C3-C5 spinal nerves and is involved with the contraction of the diaphragm
“C3,C4,C5 keeps you alive” - if these are injured the patient may have difficulties breathing on their own
External intercostals (inspiration)
external intercostals
11 external intercostals on each side of the sternum
contraction of these muscles pull the lower rib up and out towards the upper rib, thus elevating the ribs and expanding the chest
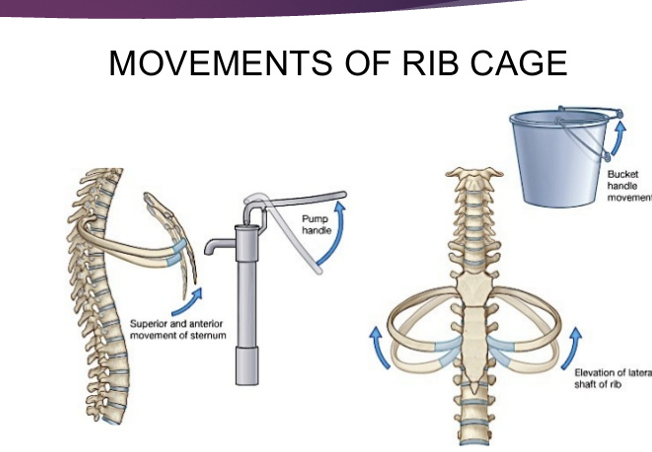
The lower ribs act like a bucket handle – you should find that the lower ribs have a movement that goes up and out
Upper ribs – go up and down (like a pump handle)
muscles of forceful expiration
expiration should be a relaxed, passive process, however…
abdominal muscles
rectus abdominus, internal and external obliques, transverses abdomens
work to raise intraabdominal pressure with huffing of coughing
pressure generated in the abdominal cavity is transmitted to the thoracic cage to allow for greater expulsion of air
internal intercostals
11 internal intercostals are located on each side of the sternum
depresses the rib to aid in forceful expiration
If expiration is problematic its obstructive – this cues you to take a stethoscope to auscultate the lungs to find that
Rib movement
bucket handle movement (lower)
pump handle movement (upper)
clinical: “milking effect”
changes in intraabdominal and intrathoracic pressure assist with venous and lymphatic return to the heart
manual technique
breathing
lymphangions are 6-8x/min for the lymphatic system - this is why we need to belly breathe (creates the internal pressure changes we need to move fluid)
Pulmonary system: pleurae
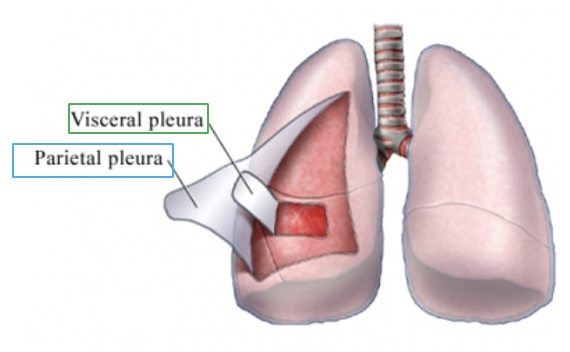
two serous membranes, or pleurae, exist that cover each lung
outer surface of the lung is visceral pleura
inseparable from the tissue of the lung
the pleura covering the inner surface of the chest wall, diaphragm, and mediastinum is called the parietal pleura
normally, the two pleura are in constant contact with eachother
there exists a potential space between the pleura called the pleural space of pleural cavity
a constant negative pressure within this space maintains lung inflation
You cannot separate the visceral pleura from the lung they are conjoined
Pleural space with pleural fluid (prevents pleural friction rubbing – this as a certain sound that we can hear with auscultation)
Clinical: Complications effecting pleural integrity: Pleuritis or pleurisy
an infection with resultant inflammatory response in between the pleura
detected via auscultation as an abnormal pleural friction rub
Clinical: Complications effecting pleural integrity: pleural effusion
refers to buildup of fluid in the pleural space, commonly seen after cardiothoracic surgery
detected via auscultation as diminished or absent breath sounds in the area of effusion, often accompanied by reduced lung volumes
Hemothorax vs pneumothorax vs empyema
hemothorax
blood in the pleural space
pneumothorax
air in the pleural space as result of a collapsed lung\
empyema
infection with pus in the pleural space
If that pleural space is irritated its pleuritis – can be from material in that space that shouldn’t belong (air, blood, pus)
*******pleural effusion (fluid in pleural space) vs pulmonary edema (fluid in lungs)
Auscultation shows absent or diminished breath sounds –
when testing – the lung volumes would be off (there is more pressure on the lungs causes less space of ability to expand)
This is an example of restrictive lung disease but the etiology (cause) is pleural effusion
Thoracocentesis – drains it so you can see whats inside (if its yellow its pus, if its red its blood, ect)
treatment for complications effecting pleural integrity such as pleuritic, pleural effusion, hemothorax, pneumothorax, empyema
treatment: insertion of a chest tube into the pleural space to drain pleural secretions or to restore a negative pressure, to allow for lung inflation
thoracocentesis: a needle aspiration of fluid into the pleural space for patients who have large pleural effusions
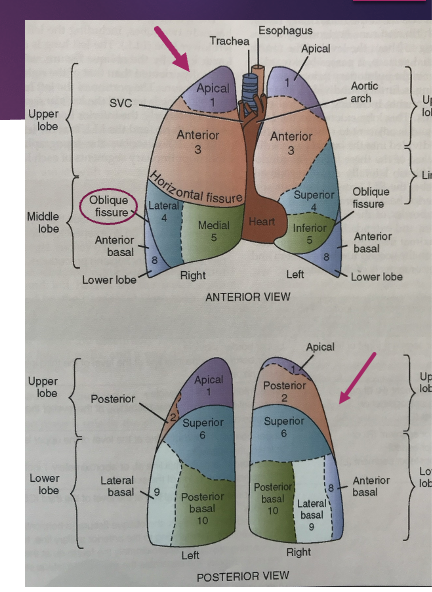
pulmonary system: lobes, tissues, segments - right lung
3 lobes: RUL, RML, RLL
two issues separate these lobes from one another
the RML and RLL are separated by the oblique (major) fissure
the RUL and RML are separated by the horizontal (minor) fissure
each lobe is further divided into segments
Each lobes have segments: the areas of the lungs are important because you asacultate the different areas of the lungs and based on where the fluid is congested you have to position the patient in a certain position
- you don’t have to memorize the different segments but this is why you have them
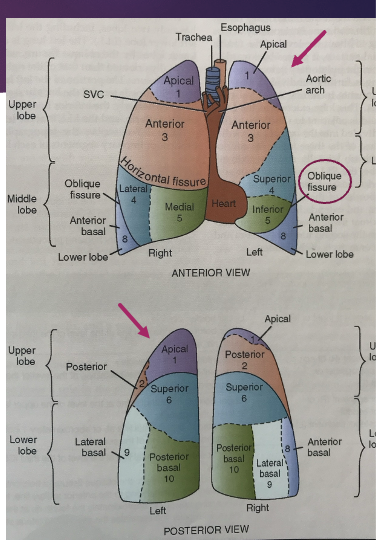
pulmonary system: lobes, tissues, segments - Left lung (what is an additional section added to the left lung)
left lung
smaller than the right lung, how two lobes: LUL, LLL
an oblique fissure divides the LUL from the LLL
the portion of the left lung that resembles the middle lobe of the right ling is called the lingular segment, or lingua
part of the LUL
each lobe further divides into segments
clinical: seasonal allergies
individuals with seasonal allergies who are prone to developing sinus infections are also prone to developing bronchitis if the infection leaves the sinus cavities and drops down the trachea to the bronchioles
upper respiratory infection may lead to a lower respiratory infection
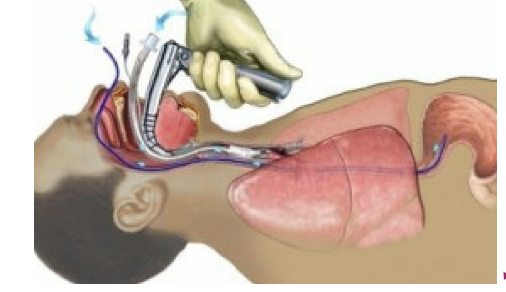
clinical: ETT
endotracheal intubation may cause damage to the structures within the larynx, producing an inflammatory response - laryngitis
hearsness and pain during speech
Pulmonary: lower respiratory tract - airway diameter
airway diameter progressively decreases with each succeeding generation of branching
starting at approximately one inch in diameter at the trachea and reaching 1mm or less at the terminal bronchioles
Pulmonary: lower respiratory tract - Trachea (bifurcation and where and what is it called)
the trachea bifurcated into the right and left mainstream bronchi at the level of the 5th thoracic vertebra or sternal notch of the sternum
carina
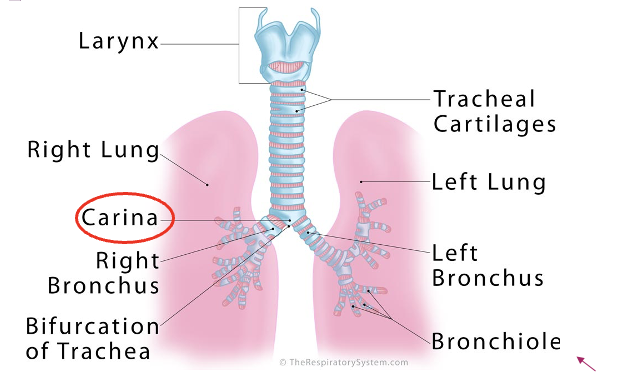
lower segments distal to the trachea
primary bronchi
R/L main stem
secondary bronchi
go to each lobe
tertiary bronchi
go to each segments within the lobes
Carina is an upside down triangle at the first dissection pf primary bronchi
Secondary bronchi go to the lobes (3 on R; 2 on L)
Teriary bronchi go to each segment in the lobes
Bronchiole
Alvioli – most functional unit of gas enchange in the lungs (provide oxygenated blood to the lungs and the circulatory system gives CO2)
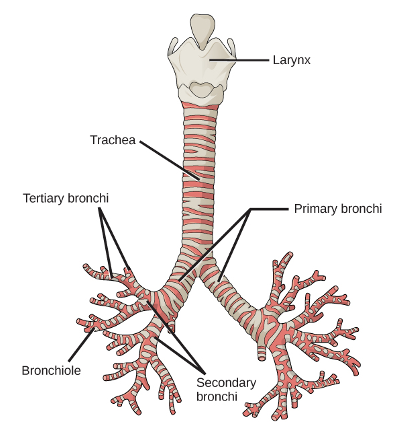
Clinical: aspiration (angles and which lung is more likely to experience aspiration)
aspiration - breathing in air or food - can cause infection if not expelled
the right mainstream branches off at the trachea at approximately a 25* angle
the left mainstem branched off the trachea at approximately a 40-60* angle
which lung is more likely to experience aspiration
R lung is more likely to experience because there is less resistance to fall

Pulmonary: terminal respiratory (acinar) units
The functional unit of the lung is the alveoli, where gas exchange occurs.
Two major types of cells exist along the alveolar wall
Squamous pneumocytes (type I): flat and thin. Cover 93% of alveolar surface
Granular pneumocytes (type II): thick and cuboidal. Cover 7% of alveolar surface- produce surfactant
Surfactant is a lipoprotein that lowers alveolar surface tension at end expiration and thereby prevents the lung from collapsing
Capillaries deliver blood in close proximity to the alveoli. The alveolar capillary interface is where gas exchange occurs.
KNOW SURFICANT