12)personality disorders
1/42
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
43 Terms
personality (4)
def: traits and behaviours that characterize a person
*Personality as enduring patterns of perceiving, relating to and thinking about he enviro and about oneself
*This may vary over context and time
*Idea that ppl have consistent way of perceiving to and thinking about the enviro
“Big Five” Factors—FFM
personality measured by traits and behaviours that characterize a person—often measured using the ‘Big 5’—the five factor model of personality which defines dimensions of personality and ways of perceiving the world
Neuroticism: extent to which s/o is even tempered vs reactive, mood and temperamental
Extraversion: extent to which s/o is talkative/socially active VS silent/passive/reserved
Openness: extent to which s/o is imaginative/curious/creative VS shallow/imperceptive
Agreeable: how kind/trusting/warm VS hostile/mistrustfulness
Conscientious: organized/thorough/careful/reliable VS negaliable/unreliable
*aka OCEAN, these traits can be measured reliably and consistent in ppl over time
*personality thought to be stable way of being in the world over time BUT expression of some of these traits can vary as function of context
*But these traits define the range of possible behaviours--not the lvl
DSM-III & personality disorders (4)
largely ignored by researchers until 1980s
personality disorders first introduced in 1980, in DSM-III
*Personality disorder used be called 'character disorders": way of being in the world that is inflexible and maladaptive to your context, causing yourself or other ppl harm in the context
used as means of distinguishing longstanding maladaptive ways of relating to the world from phasic clinical “syndromes”
*Personality disorder considered longstanding maladaptive way to related to the world, differntiated from disorders like MDD, AUD, etc
—DSM-III devotted Axis II to these conditions *persoanlity disorders recorded as ‘Axis 2 disorders’ Axis I disorders = major forms of dysfunction like MDD
*So clinician would put personality disorders down as smth they think will interfere with treatment for Axis one disorder (ex. MDD--personality disorders
*Personality disorders traditionally not conceptualised as diathesis stress disorders— they were thought of traits (may be genetically determine) that persist via s/o's life
DSM-5 def of personality disorders (5)
*Got rid of axis 2, now personality disorder recognized as significant source of distress that can be treated
“a personality disorders is” an enduring pattern of inner experiences and behaviour that: *lifelong pattern of dysfunction
deviates markedly from expectations of the individual’s culture
is pervasive and inflexible *ppl that can't modulate behaviour across diff situation
has onset in adolescence or early adulthood
is stable over time
and leads to distress and impariment
*since DSM-3 there’s been quite a bit more research—for borderline and antisocial especially, but many of the other PD disorders have been poorly researched
egosyntonic VS egodystonic
Ego-Syntonic: Behaviors that do not cause distress to the person and the person does not see the behavior as a problem.
ex. s/o engages in excessive cleaning because they enjoy it and it feels good to them.
Ego-Dystonic:Behaviors that do cause emotional distress and the person recognizes the behavior as a problem.
Ex: Someone with OCD cleans excessively to relieve anxiety rather than because they enjoy it.
3 cluster groups (for the 10 diff PDs)
Cluster A: Odd/eccentric
unusual behaviors that can range from distrust/suspiciousness to extreme lvls fo social detachment (Ex. paranoid PD, schizoid, schizotypal)
Cluster B: Dramatic/emotional/erratic
Tendency to be dramatic, emotional, etc;
Characterized by erratic behaviours, antisocial activities, and behavior that attract a lot of attention from ppl (Ex. BPD, AD, narcistic PD, histrionic)
Cluster C: Anxious/fearful
May look like anxiety disorder so difficult differential diagnosis
More likely to seeking help than other clusters (except borderline PD)—typically seek help for anxiety problems (Ex, avoidant PD, depednat PD, OCPD)
main contreversies of PD (3)
1)is there a difference btwn Axis I and II conditions? *DSM-5: no, so collapsed the Axis system
2)are personality disorders a difference of degree or a differnce of kind?e
degree: Extreme along a personality continuum *kind: using a threshold for diagnosis, (categorical) more approiate for PD, if defined along big 5 traits
*So categorical vs dimensional model--dimensional camp has been more successful in forcing through
3)what does it mean to be diagnosed with 2+ PDs? *What challenges does this pose for PD diagnosis
categorical VS continuous (4)
many argue better viewed as constellations of traits
—each along a continuum *Bc of problems with reliability, some argue better to view them as constellation of traits--should consider multiple trait dimension and see where ppl fall
proposed as revision for DSM-5
hybrid dimensional-categorical model (*for PD currently?O
PD as conceptualized using five-factor model (3)
PD may represent extreme lvls of normal personality traits that come together in diff combinations
argue that should be classifying PD along the big 5 dimensions
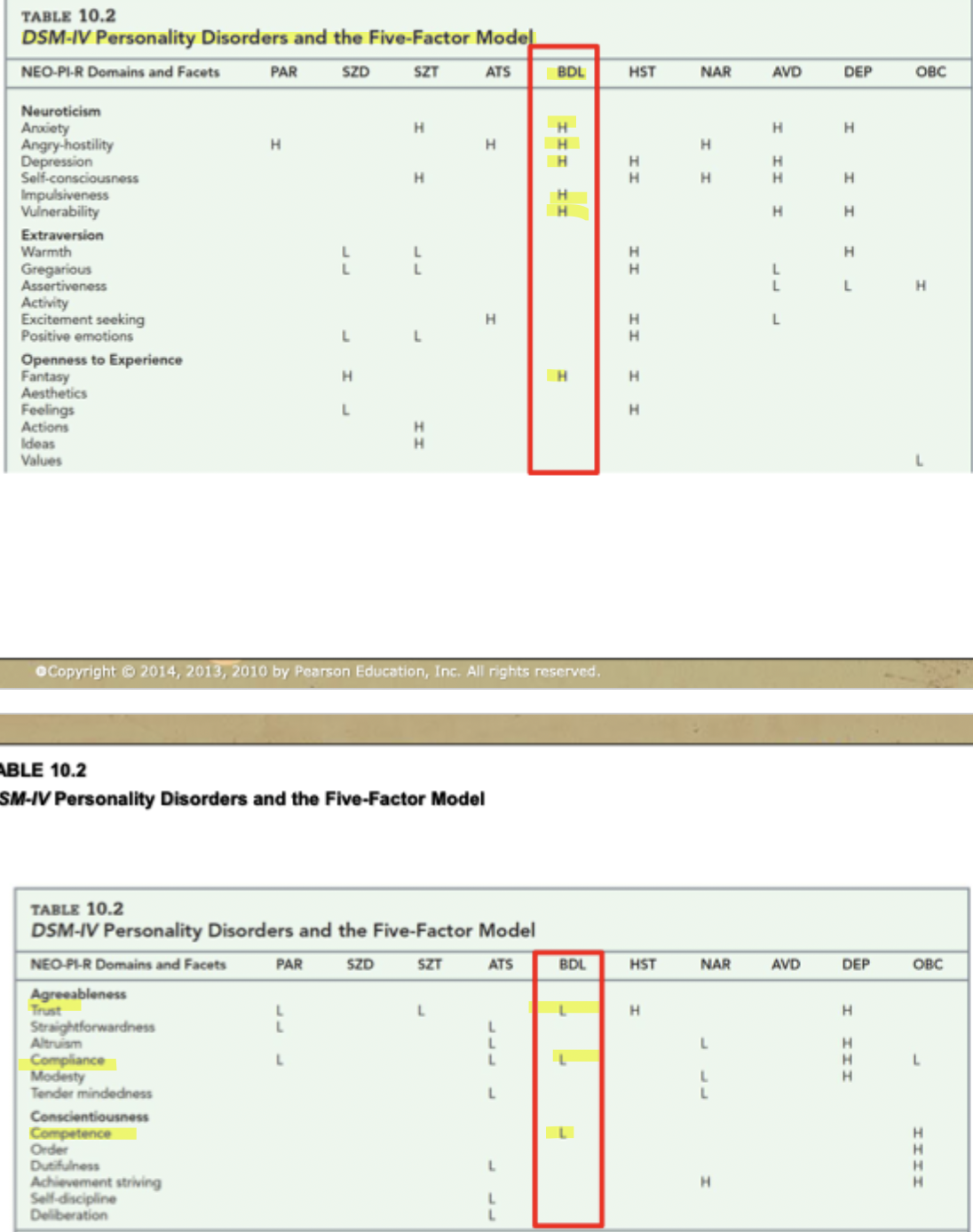
Ex. Borderline Personality Disorder (BDL): high on angry/hostility and depression, high in impulisvity and vulnerability, high on fantasy
VS low on trust, compliance and competence
criticism of this model: does bad job for schizoid but okay for others, assumptions that there is a 'normal personality' (so don't agree that all trait in PD are well captured with the big 5), & all PD correlated with neurosis and very few with openness
*but this model wasn’t used, we still use DSM-5 criteria
proposed revision for the DSM-5
categorical component: reduce list of PDs from 10 to 6
keep: antisocial/psychotic, avoidance, borderline, naracissistic, obsessive compulsive PD, shizptypal *these PDs we have most research on
eliminate: dependant, histrionic, schizoid, paranoid *PDs with most problems with diagnoses, least amount of research
*but this revision wasn’t used, but we ended up keeping all 10
DSM-5: Alternative Model for Personality Disorders (AMPD)
A)moderate or greater impairment in personality functioning—consisting of:
the degree to which there is an intact sense of self (involving a clear, coherent identity, and effective self-directedness *whether feel that they have some agency over their own behaviours
AND interpersonal functioning (reflecting a good capacity for empathy and for mature, mutually rewarding intimacy with others *formalizing that interpersonal dysfunction is the core of PD
*Can't get PD diagnosis unless have moderate impairment in both of those ways—capture swhat make personality psychopathology diff from others--extreme interpersonal dysfunction and incoherent sense of self
B)presence of patholgical personality traits—organized into 5 domains:
1)negative affectivity 2)detachment 3)antagonism 4)disinhibition 5)psychoticism — correlates wll with five factor model *These extreme trait domains correlate pretty well with 5 factor model
a “lvl of funcitoning” scale provided: ‘moderate impairment” the threshold to indicate the presence of a personality disorder *Moderate impairment as threshold to get diagnosis for PD
diagnosis issues: too much clinician leeway (3)
potential for misdiagnosis based on perspective of clinician
few clear behavioural indicators & no discrete time-period (VS for AUD there is 3 or more drinks in 3 hrs or more occasions)
PDs give much more leeway to the clinician
—”disregard for—and failure to honour—financial and other obligations or—commitments; lack of respect for—and lack of follow through on—agreements and promises.”
*ex. how many promises need to be broken for PD diagnosis? So relies on clinical global assements, introduces unreliability bc diff clinicians have diff ideas of how much is too much and this can leads to over diagnosis in some ppl
diagnosis issues: gendered bias in PD diagnosis (4)
clinicians are typically reluctant to diagnose women with APD and to diagnose men with histrionic PD *Almost no men diagnosed with histrionic PD, very few women with APD
agression in APD may take many diff forms in men and women, depending on culture
*types of aggression recognised for APD also types that men are likely to engage in and that women are less likely to engage in
*Women engage in aggression at same lvls but bc not breaking into banks, physically fighting, etc, it looks more like emotional abuse (relational aggression)
“histrionic” (name) explicitly gendered
*Hypocrites: "only women can have..displacement in erratic ways bc womb got dry trying to find water making it's way up to you breath impeding you berating making women act irrational"
Warner (1978) and histrionic PD diagnosis (4)
175 MH professionals diagnose case hist *Gave professionals the same case history but only changed the gender of the patient
½ of cases described as a women
½ of cases described as a man
76% of female cases diagnosed with histrionic PD (VS 49% of male cases)
*found majority of women cases diagnosed with HPD so gender bias still present
Borderline PD, psychopathy and gender differences (4)
80% of individuals identified as BPD are women
men can have BPD —but it may manifest differently in men VS women
25% of male federal inmates diagnosed with psychoapthy *1/4 *Psychopathy: subset of APD
yet very few female federal inmates diagnosed with psychopathy *But based on checklist, men and women they look similar in lvls of psychopathy, but women won't get this diagnosis
—does not seem to represent true prev if look at responses on a checklist
—biases in diagnosis rates or true differences?
problems w/ comorbidity & diagnositic overlap for PDs (4)
comorbidity & diagnositic overlap both problems for PDs
Ex. cluster B
47% met criteria for APD, 57% met for histrionic *within cluster
APD has overlapping symptoms with both schizoid and NPD *btwn clusters (schizoid in cluster A)
huge conceptual overlap *within cluster and btwn clusters
Cluster C PDs and Axis 1 comorbidity (3)
PDs highly comorbidity with ‘Axis 2’ disorders
avoidant & dependant PDs (cluster C): highly comorbid with anx & depression
avoidant PD (cluster c) comorbid with all eating disorders
—highest comorbity for anorexia and binge eating disorder in OCPD
Cluster B PDs and Axis 1 comorbidity (2)
BPD comorbid (cluster B) with unipolar, bipolar disorder & PTSD
Substance use disorder comorbidity with ASPD, BPD and NPD (cluster B)
notion of PD as clinically compelling (4)
clinically, difficult patients present with problems that primarily appear to arise from problems in interpersonal relationships
interpersonal VS intrapersonal *intra=’internal’
they may have anxiety, depression, etc. — but these appear to be secondary to problematic ways of interacting with the world
—this compicates treatment *Ex. Psychotherapy is based on interpersonal functioning, so if have issues with that hard to get the treatment to work and get through to them
RE: 3 clusters of 10 PDs
Cluster A: Odd/eccentric —least well-studied of the PD clusters *Ppl broadly with usual behaviors that can range from distrust/suspiciousness to extreme lvls fo social detachment
— paranoid PD, schizoid, schizotypal)
Cluster B: Dramatic/emotional/erraticTendency to be dramatic, emotional, etc;
Characterized by erratic behaviours, antisocial activities, and behavior that attract a lot of attention from ppl (Ex. BPD, AD, narcistic PD, histrionic)
Cluster C: Anxious/fearful
May look like anxiety disorder so difficult differential diagnosis
More likely to seeking help than other clusters (except borderline PD)—typically seek help for anxiety problems (Ex, avoidant PD, depednat PD, OCPD)
paranoid personality disorder (PPD) (3)
pervasive suspiciousness *paranoia
tendency to see self as blameless
*Ex, in on relationship, always think partner is cheating on them
on guard for perceived attacks by others *Hold long grudges against ppl
diagnostic overlap w/ paranoid personality disorder (4)
occurs more commonly in families of ppl w/ schizophrenia
viewed as a related disorder to schizophrenia—a “cousin”
primary difference is in the severity—often a very fine line btwn the two *schizophrenia more severe
signifigant diagnostic overlap with avoidant PD & BPD *Bc parnoid features of both avoidant PD and borderline PD
schizoid personality disorder (3)
near total lack of interest in intimate involvement with others *Limited interest in intimate relationships
limited emotional responsiveness *Flat affect
—”loners”, percieved as cold, indifferent *no interest in connecting with others
one of the PDs proposed for exclusion
2 disorders w/ overlap w/ schizoid (3)
schzoid PS has diagnostic criteria overlap with schizotypal PD *another cluster A disorder
—recent data suggests it may be more related to asocial disorders (e.g. autism spectrum)
*ASD spectrum: problems with picking up on social cues, but they WANT to engage in social interaction and connections
*Schizoid: don't care about other ppl or want involvement with other ppl
schizotypal PD (3)
cognitive & perceptual distortions
eccentricity of thought/behaviour
*Pervasive interpersonal problems—Want close relationships, but have oddities than make them come off as weird or eccentric
*this makes them socially isolated--other ppl find these things weird of off-putting, but this makes them more entrenched in their odd beliefs--few reality checks from other ppl
BUT their contact with reality is maintained *unlike for schiz
eccentric thought/behaviour seen in schizoptypal PD (4)
—odd beliefs/use odd speech
—magical thinking: *idea that thoughts or behaviours bring about change in the world
*LOTS of superstitious-- ex. Magical numbers, step on a crack will break mother's back, etc.
—telepathy, clairvoyance *More likely to believe in telepathy etc.
—ideas of reference; *interpret ppl's conversation as having personal significance to them
overlap btwn schizotypcal and schizophrenia (5)
great deal of overlap with schizophrenia, but diff severity and quality of symptoms
—eccentric & odd behaviour, but not delusional *maintain contact with reality *Ex. Don't believe that they are the kind of England, but may think they have a strong relationship with the King of England
some argue a mild or prodromal schizophrenia *Schizotypal may be precursor to schizophrenia or related to it but also may just have schizotypal for your whole life with no schizophrenia
familial co-aggregation *with schiz for schizotypal and vice versa
found in both ‘schizophrenia spectrum disorders’ and ‘personality disorders’ sections in DSM *schizotypal PD found in 2 areas in DSM to recognize its degree of overlap with schizophrenia
Ken Kendler— etiology of paranoid & schizotypal (4)
Ken Kendler:
Over 2 yrs: found both paranoid and schizotypal PD are very stable over time— Good test retest reliability
Some genetic heritable component
And they overlap in their genetic risk--share additive genetic risk
Environmental factors seemed transient and not related to expression of these disorder
Histrionic PD (5)
highly dramatic, lively, extraverted personalities
high excitement seeking
low self-consciousness
*Ppl are attracted to these ppl at first but have trouble maintaining these friendships over time
preoccupation with physical appearence *dress 'provocatively’, attempts of flirtation and seduction for those around them
irritability and temper outbursts if attention seeking is frustrated *Try to elicit attention form other ppl--dependant on attention from other ppl and attention-seeking
prev of Histrionic PD (3)
about 2-3% prevalence
sex differences *Gender differences in prev rates
proposed for removal *bc of so little research
*2 theorized subtypes of narcissism
2 proposed subtypes of narcissism disorder:
1)Grandiose Narcissism: Confidence, entitlement, dominance
2)Vulnerable Narcissism: Low self-esteem, sensitivity to criticism, masks shame *unstable sense of self world and esteem; their actions are to mask shame and sensitive to criticism--so reaction to their terrible feelings about themselves
Both subtypes appear/present in similar way, but the vulnerable subtype reacts strongly due to insecurity.
narcissitic PD (5)
grandiosity *key characteristic
preoccupation with recieving attention *wants to receive attentions
self-promoting
lack of empathy
easily offended *Very easily offended: especially about things that challenging their notions of being great
hypercritical and retaliatory is they are not validated
presentation & treatment of narcissitic PD (3)
highly variable clinical presentation *Very variable clin presentation--lots of variability from person to person
this complicates treatment
*they don't often go for treatment of the narcism itself —they go to treatment for smth else (ex. Depression) and then therapist finds out they have narcissistic PD
*the patient gives the therapist lots of unsolicited feedback on the way to do therapy—Ex. You went to McGill for your degree in psychotherapy? "well I went to Harvard
—increased likelihood of dropout, slow symptoms change *Higher rates of therapy drop out, very slow symptom change
prev & gender differnces in narcissistic PD (4)
prev rate of less than 1%
RE: hypercritical and retaliatory is they are not validated *If their sense of themselves as very special and imp, they may retaliate against ppl/do things to undermine their sense of self (Ex. Spread rumors, etc.)
Males with high narcissitive tendencies: more likely to engage in sexual coercion if had their sexual advance rejected
more likely to depict film depictions of SA as more appropriate compared to men lower of narcissistic tendencies
narcissitic PD may be more common in men (than women) --but very little research
etiology of narcissistic PD (grandiose VS vulnerable subtype)
grandiose associated with parental overvaludation
*Psychodynamic theory: Their parents praise them too much which develop in them sense of grandiosity and large self of importance -- grandiose subtype
vulnerable associated with emotional, physical, sexual abuse/intrusive, controlling, cold parenting styles
*Psychodynamic theory: Ppl have vulnerable sense of them they try to mask with grandiosity to build themselves up -- more vulnerable subtype
avoidance personality disorder (4)
avoiding interpersonal contact
—extreme sensitive to criticism and disapproval
avoid intimacy, though they desire it
extreme loneliness, low self-esteem, excessive self-consciousness
*contact with schizoid?
*Schizoid: don't care about other ppl or want involvement with other ppl
*APD: they do desire intimacy, like those on with ASD
overlap btwn avoidant PD and social phobia (6)
differential diagnosis with generalized social phobia—very difficult trying to decipher if the one or the other
substantial overlap but…
can find those with social phobia without avoidant PD
shared genetic vulnerability btwn the both
fear of evaluation is also heritble
distinct diagnoses btwn social phobia VS avoidant PD may not be warranted
dependant personality disorder (3)
inability to function independently
adopt a submissive role in relationships
allow other ppl to assume responsibility for multiple important aspects of their lives
—jobs, classes, clothes, hairstyles
some data suggests more likley to be invovled in abusive relationships—but limited data
dependant personality disorder —comorbidity by gender & cultural differences (4)
relatives of male DPD: increased depression
relatives of female DPD: increased panic
very culture-specific: more prevalence in individualistic cultures (much less prevalent in collectivist cultures)
on the chopping block for removal in ‘DSM revision’
obsesive-compulsive personality disorder (main characterisitcs (4))
extreme inflexibility and a desire for perfection *in all things: Have lists and schedules --these are very imp to them, prioritise making lists and schedules over actually doing the tasks and have very rigid plan for everything
preoccupation with rules & order
often very moralistic and judgmental (about others)
viewed by others as rigid, stubborn, cold
*Are pretty cheap--won't throw things out (will hold on to them forever)
very limited research since 1980s
—proposed for removed in revision
OCPD — most stable characterisitcs (4)
most stable features:
rigidity,
stuboorness
perfectionism &
reluctance to delegate (things to other ppl)
as most common & rigid features
OCPD VS OCD (3)
unlike OCD, OCPD has NOT true obsessions or compulsive rituals (in same way for OCD)
not always associated with anxiety and/or extreme distress
can be egosyntonic *OCD often always egodystonic
RE: Ego-Syntonic: Behaviors that do not cause distress to the person and the person does not see the behavior as a problem.
Ego-Dystonic: Behaviors that do cause emotional distress and the person recognizes the behavior as a problem.

differences in comorbidity btwn OCPD VS OCD (4)
~20% of OCD patients have comorbidity OCPD
~20% of Panic disorder patients have comorbidity OCPD
OCD more liekly to be comorbid with avoidant or dependant PD
*OCPD more common in men VS OCD slighlty more common in women
OCPD may involve perfectionism, preoccupation with details, and/or hoarding—OCD doesn’t involve these things