Reproductive Health Exam 2
1/123
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
124 Terms
order of birth
engagement- descent- flexion- extension- external rotation- restitution- expulsion
fetal position maternal
right anterior, left anterior, right posterior, left posterior
the direction the baby's head (occiput) is facing relative to the mother's pelvis.
Anterior: The baby's head is facing the mother's back (towards the sacrum).
Posterior: The baby's head is facing the mother's abdomen (towards the pubic bone).
Left/Right: Refers to the side of the mother's pelvis where the baby's head is located. Left Occiput Anterior (LOA): The baby's head is down, facing the mother's back, and slightly rotated to the left. Right Occiput Anterior (ROA): The baby's head is down, facing the mother's back, and slightly rotated to the right. Left Occiput Posterior (LOP): The baby's head is down, facing the mother's abdomen, and slightly rotated to the left. Right Occiput Posterior (ROP): The baby's head is down, facing the mother's abdomen, and slightly rotated to the right.
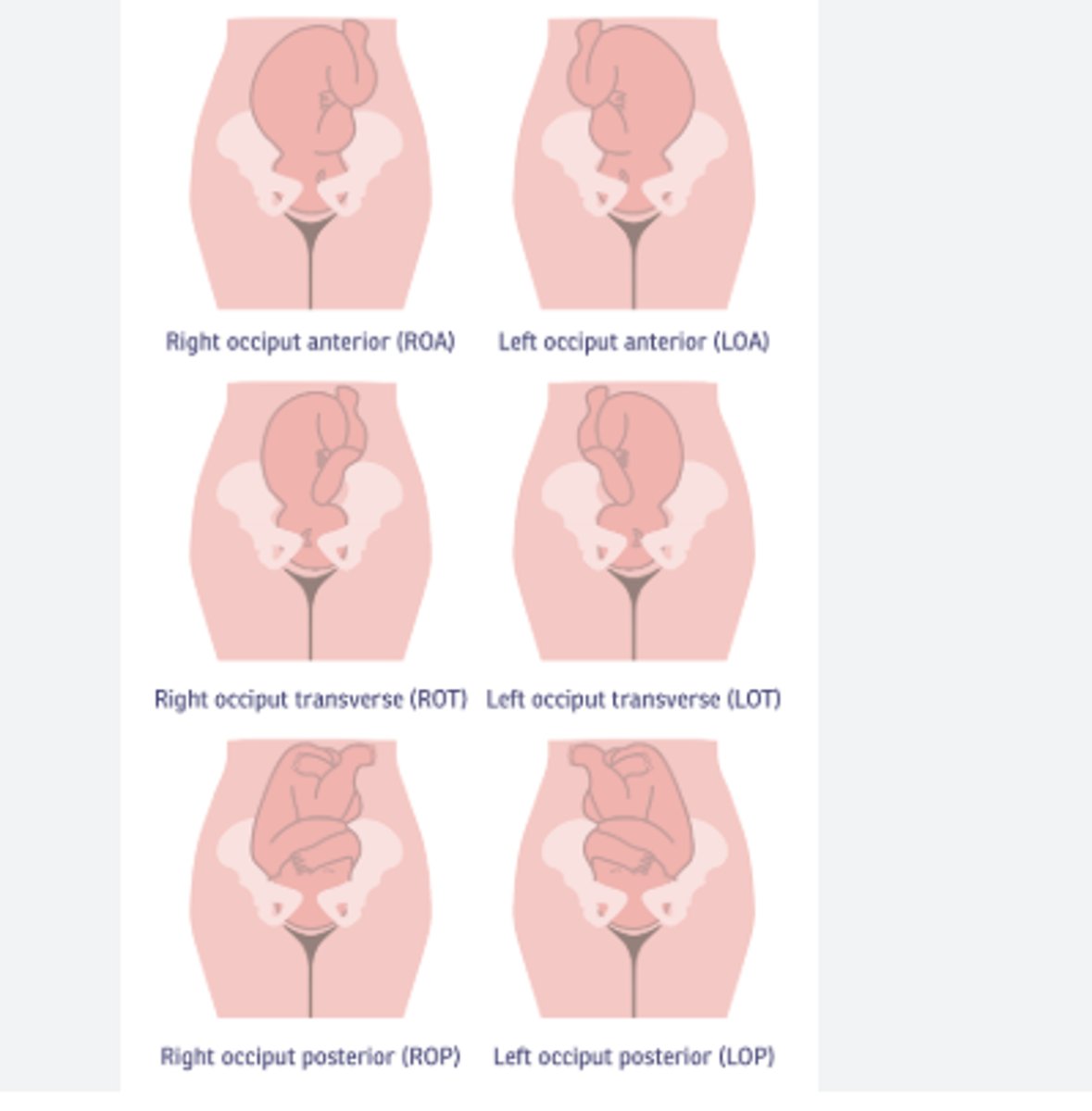
fetus presentation
4 quadrants:
vertex: occiput
face: mementum
breech: sacrum
Shoulder: acromiom
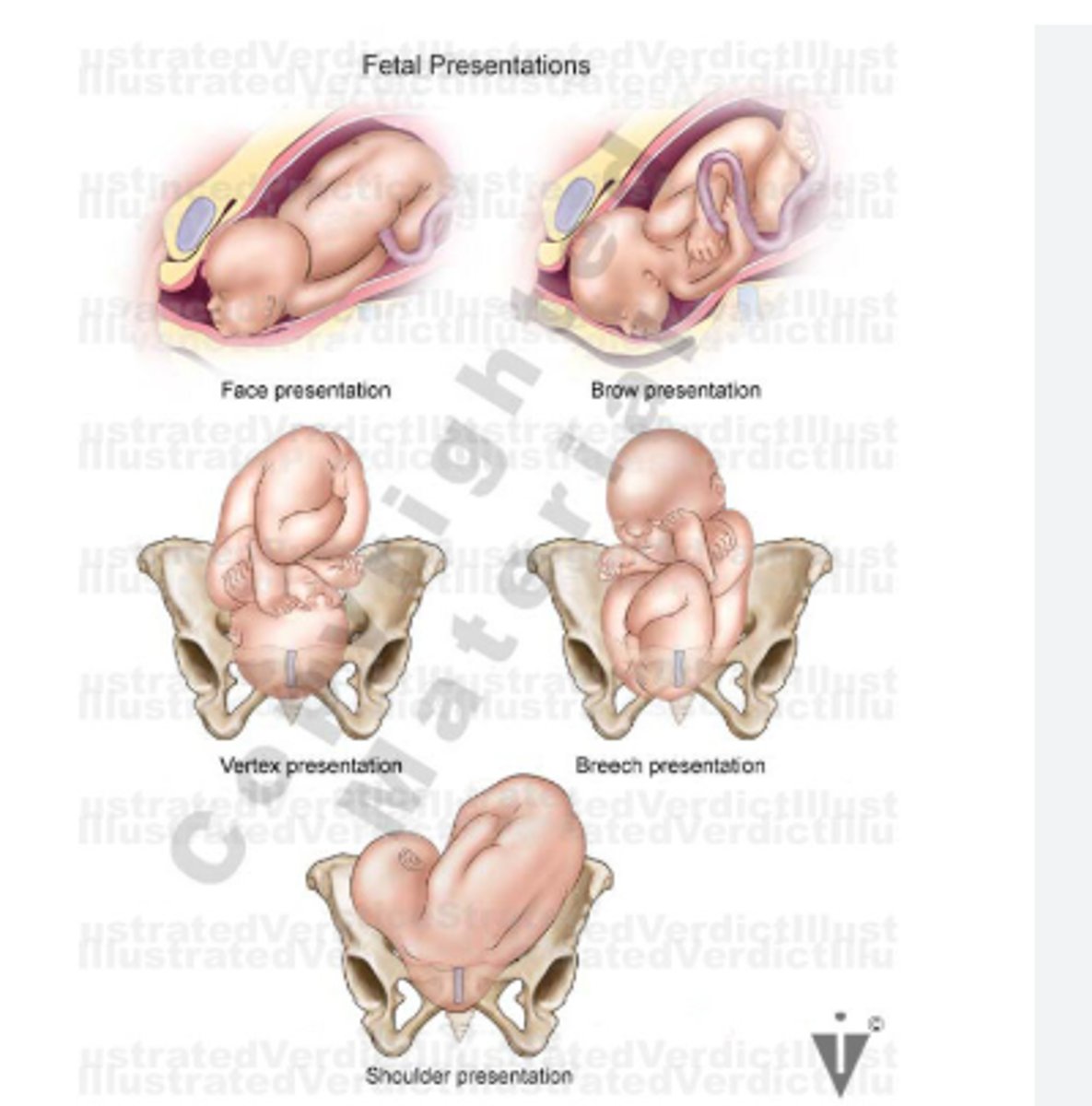
ideal fetal position
left occiput anterior
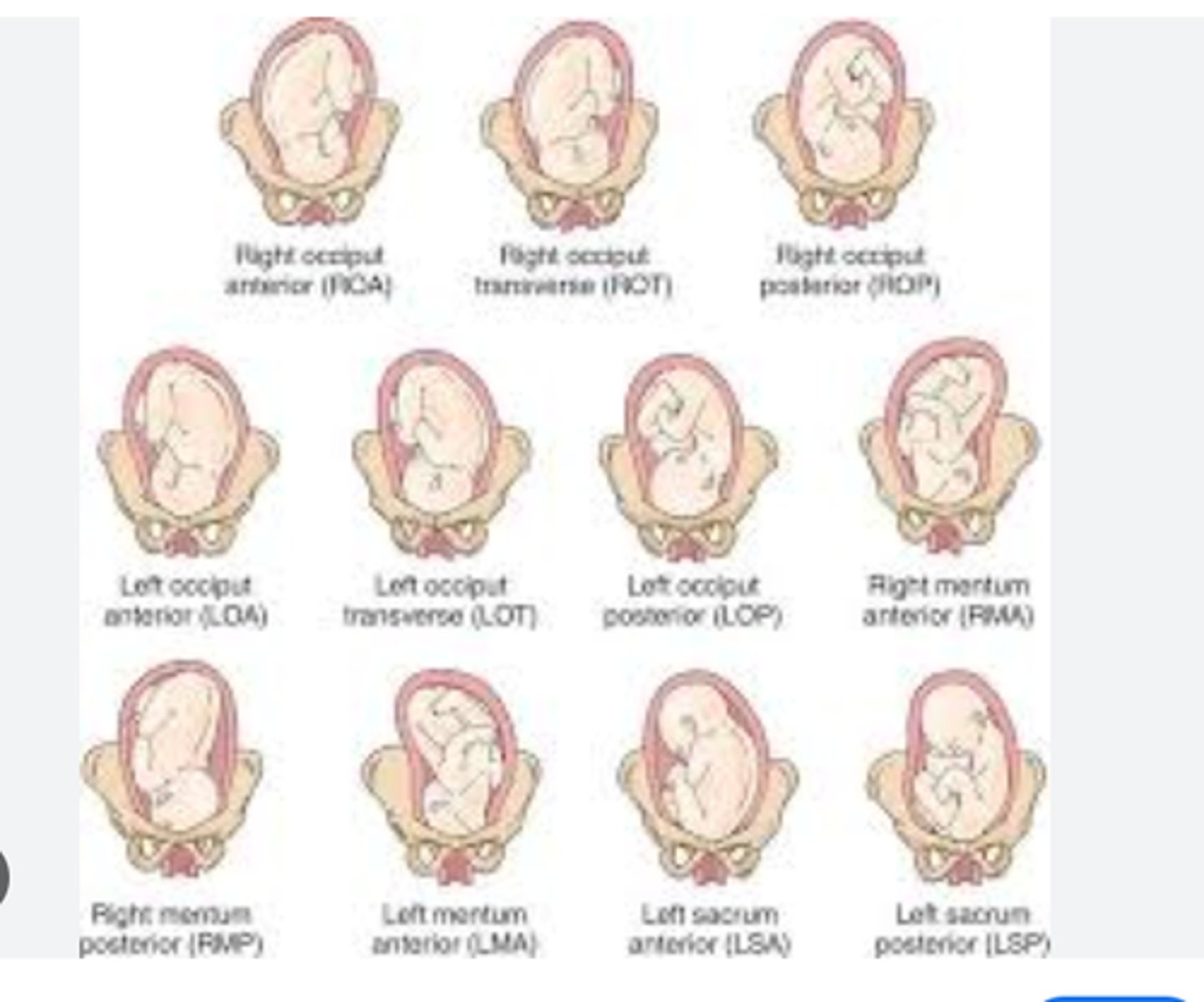
if baby's position needs changed
have mom change positions
5 factors essential for a successful vaginal birth
power, passage, passenger, psyche, position
power
contraction frequency, duration, intensity affect power
pirmary: involuntary contractions leading to dilation and effacement
secondary: voluntary pushing
oxytocin best thing to promote contractions
passage
bony pelvis and soft tissue of the cervix
station of the baby
types of pelvis will affect this
gynecoid pelvis
most favorable pelvis for successful labor.
platypelloid pelvis
pelvis that is flat in its dimensions with a very narrow anterior-posterior diameter and a wide transverse diameter; this shape makes it extremely difficult for the fetus to pass through the bony pelvis
android pelvis
the typical male pelvis; in the woman, the heart shape of the android pelvis is not favorable to a vaginal delivery
anthropoid pelvis
oval shaped, with a wider anteroposterior diameter
passenger
fetal skull shape and size
fontanels are used to identify poisition
fetal attitude: head should be tucked onto chin
fetal lie: should be longitudinal (in relation to mom's spine)
cephalic, breech, or transverse
fetal position
fetal size
psyche
stress and anxiety can cause long labor
position
***avoid supine
upright is good
contractions are best felt at the
fundus
increment phase of contractions
period of increasing strength. longest phase, begins in fundus and spreads through uterus
acme peak of contractions
peak intensity, shortest phase
decrement phase of contractions
relaxation
order of contraction phases
increment- acme- decrement
purpose of vaginal exams
determines dilation, effacement, station
**risk of infection
station of baby
-4 still floating, -3, -2, -1 above pubic symphysis, 0 head is engaged, 1, 2, 3, 4- out.
**IF CERVIX IS DILATING BABY SHOULD BE MOVING DOWN.
signs of impending labor
lightening: fetus descending into pelvis 2 weeks before labor. leads to easier rr, increased urination
braxton hicks, cervical effacemnent, loss of mucous plug, hormone changes, oxytocin, prostaglandin
fetal triggers that lead to birth
fetal cortisol changes, placenta aging, prostaglandins in baby
true labor
regular contraction, increase in frequency and intensity. changes in dilation and effacement
**GO TO HOSPITAL WHEN CONTRACTIONS ARE 5 MINUTES APART, LAST 60 SECONDS, AND ARE REGULAR FOR 1 HOUR
false labor
Irregular contractions without cervical changes.
amnisure ROM test
confirms rupture, very accurate, swab in vaginal canal tests ph
risks r/t c section
PLACENTA ACCRETA IS BIGGEST WITH REPEAT C SECTION
hemmorrahge, VTE, death, newborn respiratory issues, alteration to gut microbiome in newborn
emergent c section
prolapsed cord, rupture of uterus, abnormal FHR patterns
urgent c section
fetal malrepresentation, placenta previa with mild bleeding
non urgent c section
related to complications such as failture to progress and failture to descend
operative vaginal delivery
with forceps or vaccum. use is declining
vaccuum is better
head must be engaged and cervix must be dilated
c section classification
scheduled vs unscheduled
arrest of labor and indeterminate FHR main reasons for unscheduled
1st stage arrest
under 6 cm dilated, membranes ruptured, over 4 hours of adequate contraction or over 6 hours of inadequate contractions
2nd stage arrrest
lack of continuing progress for nulliparious women
3 hours with anestethia or 2 hours without anestethia
fetal indications for c section
breech presentation, brow presentation, occiput transverse position, transverse lie, FHR decelerations/distress, shoulder dystocia, macrosomia
maternal indications for c section
failure to progress, hematologic dz, HIV, active HSV infection, Leiomyomas, eclampsia, placenta previa, post-term, pre-term, vasa previa, multiples, suspected macrosomia, previous uterine surgery, preclampsia, herpes (genital), impediment of labor or arrest of active labor
VBAC
risk of uterine rupture
must be done in a facility that can do a c section
60-80 percent success
induction indications
only when doing so would improve health of mom and baby
if over 41 weeks
risk of uterine rupture and premature seperation of placenta
conditions that must be met before induction
- fetus in longitudinal lie
- no supsected cephalopelvic disproportion
- vertex is engaged
- cervix is ripe and ready for birth
- EGA is at least 39 weeks
oxytocin
most common med for induction
onset of contractions 3-5 minutes after iv is started
continually monitor fhr
monitor fetal and mom response to it and titrate accordingly
TACHYSYSTOLE MOST CONCERNING SIDE EFFECT (can cause fetal hypoxemia and abnormal fhr
most concerning side effect of oxytocin
tachysytole
biggest risk with repeat c section
placenta accreta
cervical ripening
stripping of membranes, manually seperating
mechanical: when little to no effacement and pharm c/i. hydroscopic dilators, transcervial balloon dilators
pharm: when bishop score is under 6. cervidal, misoprostol, c/i if vbac, uterine scar
continue to monitor FHR
bishop score
A Bishop score assesses cervical readiness for labor induction by evaluating dilation, effacement, station, position, and consistency, with scores ranging from 0 to 13, where higher scores indicate a more favorable cervix.
0-1 cm: 0 points
2-3 cm: 1 point
4-5 cm: 2 points
>5 cm: 3 points
Effacement:
The thinning or shortening of the cervix, expressed as a percentage. 0-30%: 0 points 40-50%: 1 point 60-70%: 2 points >70%: 3 points
Station:
The position of the baby's head relative to the ischial spines of the pelvis. -3 to -1: 0 points 0: 1 point +1 to +2: 2 points +3: 3 points
Position:
The position of the cervix relative to the fetal head. Posterior: 0 points Middle or anterior: 1 point
Consistency:
The feel of the cervix on examination. Firm: 0 points Medium: 1 point Soft: 2 points
preciptous labor
labor that lasts less than three hours from the start of uterine contractions to birth
increased anxiety and pain
fetus at risk for hypoxia
carefully examine cervical changes, don't leave patient
amniotomy
artificial rom to augment labor
done by provider
FETAL HEAD MUST BE ENGAGED FIRST
risk for cord prolapse, infection, decels
monitor FHR, contractions, amniotitc fluid
risks with amniotomy
cord prolapse, infection, decels
cephalopelvic disproportion
size/shape/position of fetal head or shape of maternal pelvis prevents going through birthing canal
needs c section
labor dystocia
slow, abnormal progression of labor. leading indicator for c section
leading indicator for c section
labor dystocia
risk factors for labor dystocia
congenital uterine abnormalities, occiput posterior malposition of the fetus, maternal fatigue/dehydration, fear and exhaustion, analgesia and anesthesia early in labor
hypertonic uterus
uncordinated contractions, frequent, painful, ineffective. nulliparious women more likely to have. can lead to low birth weight
encourage rest
part of labor dystocia
hypotonic uterus
not strong enough contractions to dilate. indentiable even at acme phase of contractions. weaker and less frequent during active stage of labor. ambulate often.
fetal dysocia
fetus can't go through birth cancal
risk factors: macrosomia, malposition, twins, abnormalities
most effective position is occiput anterior with head flexed
causes facial bruising on fetus, maternal lacerations, neonatal asphyxia.
pelvic dystocia
small/inadequate pelvic shape
sucess of labor relies on relationship between fetal size, presentation, position, size and shape of pelvis, and quality of contractions
in order for labor to be sucessful what must be correct?
fetal size, presentation, position, size and shape of pelvis, and quality of contractions
what can shoulder dystocia do to the baby?
can cause compression of neck by the pelvis, anoxia, neurological injury, brachial plexus injury, clavical fracture, death
how to fix shoulder dystocia
mcroberts manuever
ensure bladder is empty, straight cath
dont let mom keep pushing
risks for shoulder dystocia
fetal macrosomia, dm, prolonged labor, increased maternal weight gain, previous shoulder dystocia
complications for the mom from shoulder dystocia
severe lacerations
pph
normal fhr
110-160
accerleration
increase in fhr by 15 bpm for 15 seconds or more, can be caused by maternal changes in position
INDICATE HEALTHY AND RESPONSIVE FETUS
decel
temporary decrease in fhr below baseline by 15 bpm
early decel
follows contraction patterns, sign of baby coming into pelvis and vagal response to head compression
not concerning
nadir of contractions and of decel match up
which decels are most concerning
Early decels are generally the most acceptable and typically require no intervention.
Variable decels can be acceptable if they are mild and intermittent but need monitoring.
Late decels are concerning and need prompt evaluation and intervention.
Prolonged decels are also worrisome and indicate the need for immediate assessment and intervention.
variable decel
v shape, means cord compression, could be due to baby or moms position
late decel
placental defiency, over 41 weeks, htn, ect
nadir of decel after nadir of contraction
WORST ONE
nursing interventions for variable decel
Reposition the mother: Move to lateral (side-lying) position to relieve cord compression. If not effective, try other positions like knee-chest or Trendelenburg.
Administer oxygen: 8-10 L/min via a non-rebreather mask.
Amnioinfusion (if ordered): Infuse warm saline into the uterus to cushion the cord (often used if repetitive and severe).
Discontinue oxytocin (Pitocin) if applicable: To reduce uterine contractions.
Increase IV fluids: To improve placental perfusion.
Notify the provider: If the decels are severe or recurrent.
nursing considerations for late decel
Reposition the mother: Move to a left lateral position to improve blood flow.
Administer oxygen: 8-10 L/min via a non-rebreather mask.
Stop oxytocin (Pitocin): To decrease uterine activity.
Increase IV fluids: To improve maternal blood volume and placental perfusion.
Administer a tocolytic if ordered: To decrease uterine activity.
Notify the provider immediately: Continuous late decels indicate fetal distress and may require delivery.
Prepare for emergency delivery: If the situation does not improve.
catogory 1 FHR tracing
normal, continue routine monitoring
category II FHR tracing
FHR factors indeterminate, continue to observe and reevualate
stage III FHR tracing
prompt evaulation needed. resolve situation. provide o2, change postion, ect
DUE TO ABNORMAL FHR TRACING
involution
return of uterus to prepregnancy state, takes 6-8 weeks
uterine atony
boggy uterus, uterus will not contract. do fundal massage first and empty bladder. also breastfeed to release oxytocin
if none of those work: manually provider will do bimanual uterine compression or enter a giant catheter into the uterus to compress
fundal massage
every 15 minutes after birth, use one hand to support pubic bone and the other to press down. risk for postpartum hemmorage is highest in the first hour so this is essential
empty bladder, lower hob
descent of the uterus
1 finger= 1 cm, descends 1 cm/day
immediately after birth it will be halfway between umbulicus and pubis symphysis, then will be palpated at level of uterus within one hour of birth
causes of PPH
tone, trauma, tissue, thrombosis
risks for PPH
multiple gestation, prior PPH, multiparada, placenta previa, placenta accreta, ecclampsia, hemmorrage, intrauterine fetal demise, increaseed amniotic fluid, induction, BASICALLY ANYTHING STRETCHING THE UTERUS AND TISSUE
measuring blood
1 gram= 1 ml of blood
warning signs for pph
low bp, high hr, low oxygen, dizziness, pale, oliguria, not a/o x 4
tone (PPH)
uterine atony.
trauma (PPH)
laceration. visible or cervical. presents as firm midline uterus, increased bleeding without clots, high hr, low bp
hematoma: ruptured blood vessel. usually happens at home. casued by forceps use or long labor. pressure, pain, swelling
tissue (PPH)
part of placenta left. PRIMARY CAUSE OF SECONDARY PPH
occurs after ggoing home. increased risk of endometritis
uterine tenderness, FEVER, abnormal discharge
thrombosis (PPH)
body breaking down clots faster then it can form them, depletes clotting factors. can be caused by HELLP, placental abruption, ecclampsia, hemmorage, intrauterine fetal demise
rubra
red bloody lochia, 1st 3 days
sebrosa
pink/brown, scant, days 4-10
alba
white/clear, scant, day 10
1st degree tear
vaginal mucosa
2nd degree tear
perineal muscles torn
3rd degree tear
anal sphincter torn
4th degree tear
rectum torn
REEDA Perineal assessment
Redness
Edema
Ecchymosis
Discharge
Approximation
*cold sitz baths for first 24 hours, then warm
use peri bottle after using restroom
topical anestesthia
scant bleeding
only when wiped, 1-2 inch stain
light bleeding
4 inch or less stain
moderate bleeding
under 6 inch stain
heavy bleeding
saturated pad in 1 hr or less
endometritis
infection of utuers, USUALLY DUE TO RETAINED PLACENTA
also can be caused by internal fetal monitoring
usually occurs after mom goes home
postpartum psychosis
alteration in perception of reality
very rare
hallucinations, disorganized speech, disorganized and bizzare behavior, can onset within a few days of birth
**highest risk if already bipolar
NEEDS HOSPITALIZED
postpartum blues
Seen early postpartum, peaks by day 5, resolves by 2 weeks usually
Emotional lability, crying for no reason
Requires no treatment, self-limiting
May feel fatigued, restless
Periods of sadness with periods of joy
*self resolving
*still able to care for self and baby
no minumum number of symptoms needed to diagnosis