9. Antimicrobial Therapy
1/41
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
42 Terms
Define and describe chemotherapy.
Treatment of systemic/topical infection with drugs that have selective toxicity for an invading pathogen without harming the host cells
Define and describe antibiotics.
Produced by microorganisms; selectively suppress the growth of/kill other microorganisms at very low concentrations
Define and describe antimicrobial agents (AMA).
AMA = antibacterial agents + antibiotics
Broad term
Includes drugs synthesized (antibacterial agents) as well as those obtained from fermentation of microorganisms (antibiotics)
List the classifications of AMAs.
Chemical structure: sulfonamide, quinolones
Type of action
Mechanism of action
Antimicrobial activity
Spectrum of activity
Source (antibiotic obtained from): fungi, bacteria, etc
List the classifications of AMAs based on their type of action.
Bacteriostatic
Bactericidal
Define and describe bacteriostatic.
Arrest the growth and replication of bacteria, thus limit spread of infection
Adequate in uncomplicated infections (host cells themselves help in eradicating microorganism)
Define and describe bactericidal.
Kill/irreversibly damage the multiplying bacteria so that total number of viable bacteria decreases
Fungistatic and fungicidal also exist
Some primarily static drugs may become cidal at higher concs. (sulfonamides and erythromycin)
List the classifications of AMAs based on their mechanisms of action.
Inhibit cell wall synthesis
Cause alteration of cell membrane integrity
Inhibit ribosomal protein synthesis
Suppression of DNA synthesis:
By inhibiting the synthesis of folate
By inhibiting either DNA/RNA polymerase
By inhibiting DNA gyrase
Mechanism of Action
List drugs that inhibit cell wall synthesis.
β-lactams
Penicillins
Cephalosporins
Mechanism of Action
List drugs that cause alteration of cell membranes integrity.
Polymyxins
Antifungals
Mechanism of Action
List drugs that inhibit ribosomal protein synthesis.
Tetracyclines and Aminoglycosides (bind to 30S ribosomal unit)
Chloramphenicol (inhibits 50S ribosomal unit)
Mechanism of Action
List drugs that suppress DNA synthesis by inhibiting the synthesis of folates.
Sulfonamides
Mechanism of Action
List drugs that suppress DNA synthesis by inhibiting either DNA/RNA polymerase.
Acyclovir
Anticancer drugs
Antiretroviral drugs
Mechanism of Action
List drugs that suppress DNA synthesis by inhibiting DNA gyrase.
Ciprofloxacin
List the classifications of AMAs by antimicrobial activity.
Anti-bacterials
Anti-fungal AMAs
Antiviral
Antiprotozoal
Antihelmintic
Antimicrobial Activity
List antibacterial drugs.
Penicillins
Cephalosporins
Fluoroqinolones
Antimicrobial Activity
List antifungal AMAs.
Fluconazole
Griseofulvin
Antimicrobial Activity
List antiviral drugs.
Acyclovir
Zidovudine
Antimicrobial Activity
List antiprotozoal drugs.
Chloroquine
Metronidazole
Antimicrobial Activity
List antihelmintic drugs
Mebendazole
How are AMAs classified by their spectrum of activity?
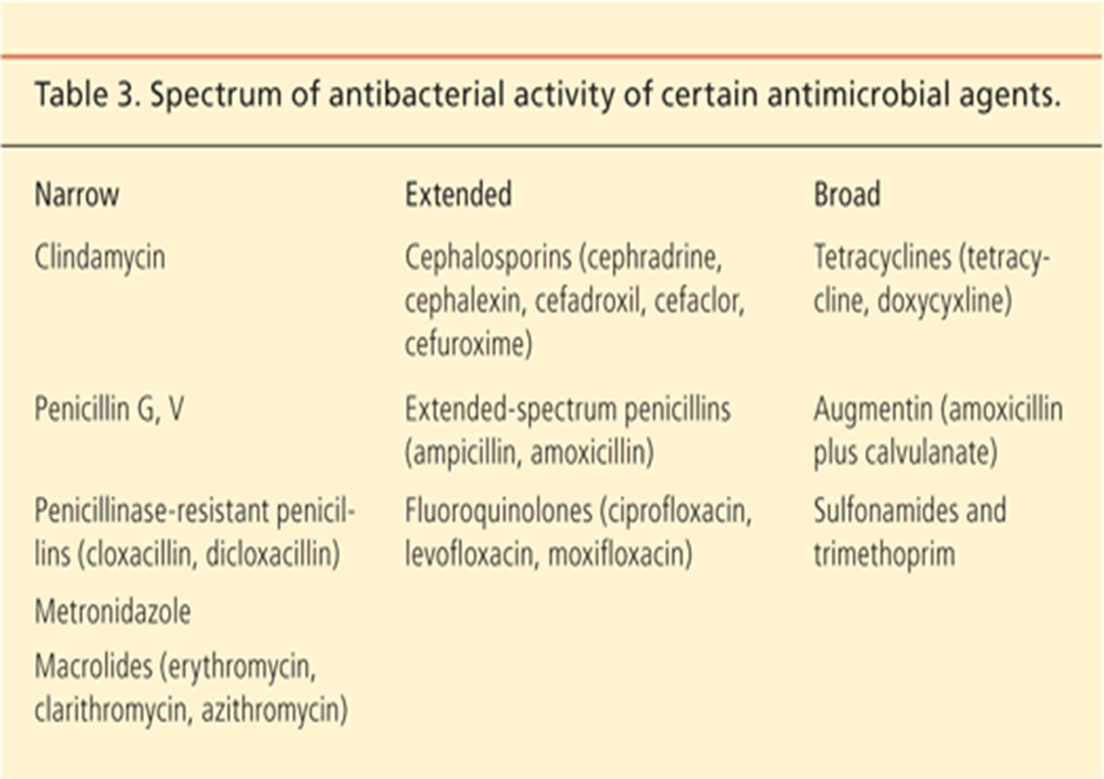
List the concentration and time-dependent effects of AMAs.
Toxicity
Hypersensitivity reactions
Nutritional deficiencies
Drug resistance
Super-infections
Describe the local and systemic toxicity of AMAs.
Local irritancy: at site of administration
Systemic toxicity: almost all produce dose-related and predictable organ toxicities
What does high therapeutic index mean? Which AMAs have a high therapeutic index?
Many-fold increase in dose without apparent damage to host cells
Penicillins
Cephalosporins
What does low therapeutic index mean? Which drugs have low therapeutic index?
Does have to be individualized and toxicity watched for
Aminoglycosides: 8th cranial nerve damage and kidney toxicity
What is very low therapeutic index? Which drugs have very low therapeutic index?
Use is highly restricted to conditions where no suitable alternative available
Polymyxin B: neurological and renal toxicity
Describe hypersensitivity reactions in relation to AMAs. Which AMAs can cause hypersensitivity reactions?
All AMAs capable of causing hypersensitivity reactions
Unpredictable and unrelated to dose
Rashes to anaphylactic reactions
Penicillin, cephalosporins, fluoroquinolones
Describe nutritional deficiencies in relation to AMAs. Which AMAs can cause them?
Vitamin B complex and Vitamin K synthesized by intestinal flora
Prolonged use of AMAs can alter flora; may produce vitamin deficiencies
E.g. neomycin
Define drug resistance and list the 2 mechanisms of drug resistance.
Unresponsiveness of microorganism to an AMA
Phenomenon of tolerance seen in higher organisms
Mechanisms:
Natural
Acquired
Describe the natural mechanism of drug tolerance.
Some microbes always resistant
Lack metabolic process/target site
E.g. Gram negative bacilli are normally unaffected by penicillins
Describe the acquired mechanism of drug resistance.
Development of resistance by an organism that was previously sensitive
Due to use of AMA over a period of time
Depends on drug and microorganism
E.g. Gonococci quickly developed resistance to sulfonamides, slowly-gradually to penicillins)
Describe superinfections.
Appearance of new infection as a result of AM therapy
Microbial flora of body get affected; contributes to host defense by inhibiting pathogenic organisms
Non-pathogenic component of flora, which is not inhibited by drug, may predominate and invade
More difficult to treat; manifested as antibiotic-induced diarrhea and colitis
Which antibiotics are commonly associated with superinfections?
Broad/extended spectrum antibiotics:
Tetracyclines
Ampicillin
Chloramphenicol
Superinfections due to ___________ ________ or _______ are more serious, leading to pseudomembranous colitis.
Clostridium difficile
Candida
Define and describe chemoprophylaxis.
Use of AMAs for preventing the setting of an infection/suppressing contracted infection before it becomes clinically manifest
Often done against all organisms capable of causing infections
List the 3 conditions under which chemoprophylaxis is done.
Prophylaxis against specific organisms
Prevention of infections in high-risk situations
Prevention of infection in general
Chemoprophylaxis
Describe prophylaxis against specific organisms.
Highly satisfactory
Choice of drug is clear-cut
E.g. tuberculosis (children, HIV positive cases: isoniazid alone or with rifampicin is recommended)
HIV infection (health care workers: zidovudine + lamivudine)
Chemoprophylaxis
Describe prevention of infections in high risk situations.
May be valid, satisfactory in certain situation, but controversial in others
E.g. dental extraction, tonsillectomy, endoscopies
Appropriate prophylaxis with amoxicillin/clindamycin may be given few hours before and after
Chemoprophylaxis
Describe prevention of infections in general.
Highly unsatisfactory in most cases
E.g. in neonates after prolonged after prolonged delivery, mothers after normal delivery to prevent post partum infections, viral URTI to prevent secondary bacterial invasion etc
AM prophylaxis may be hazardous (infection by resistant organisms, chances of suprainfections)
Define antimicrobial combination and when they are done.
More than one AMAs used
Frequently used
Should be done with specific purpose, not blindly
List advantages of antimicrobial combination.
To achieve synergism (supra-additive effect) e.g. Sulfonamide + trimethoprim, β-lactamase inhibitor + amoxicillin
To reduce severity or incidence of adverse effects: if combination is synergistic, then dose is reduced, required with AMAs with low safety margin
To prevent emergence of resistance: valid primarily for chronic infections needing prolonged therapy
To broaden the spectrum of antimicrobial action: in mixed infections, initial treatment of severe infections, etc
List the disadvantages of AMA combination.
Increased incidence and variety of adverse effects; toxicity of one agent may be enhanced by another
Increased chances of suprainfections
If inadequate dose of non-synergistic drugs are used, then chances of resistance may be promoted
Increased cost of therapy
Provide casual outlook in diagnosis of infections (rather than rational)