Pathophysiology
1/98
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
99 Terms
What are the two common causes of joint injuries?
mechanical overloading
forcible twisting or stretching
What is a dislocation?
the displacement or separation of the bone ends of a point w/ loss of articulation
subluxation
partial dislocation
What is dislocation typically the result of? Where is it most often seen?
trauma
most often seen in the shoulder and acromioclavicular (AC) joints
dislocation manifestations
pain
deformity
limited movement/range of motion (ROM)
dislocation diagnosis
hx
pt assessment
radiologic findings
dislocation treatment
depends on the site, mechanism, and degree of injury
reduction, immobilization, surgery
When do fractures occur?
when more stress is placed on the bone that it can absorb
What are the three fracture categories?
sudden injury (most common)
fatigue or stress
pathologic
comminuted fracture
bone broken into three or more pieces
fragments are present at the fracture site
lots of pain, crushing trauma
spiral fracture
the break spirals around the bone
common in a twisting injury
often from domestic abuse or sexual assault
compression fracture
bone is crushed
causes bone to be wider or flatter in appearance
two bones that are crushed/squeezed together
often in vertebrae
open (compound) fracture
if bone sticks out of skin
often needs surgery and IV abx
closed (simple) fracture
bone inside skin
less risk infection
greenstick fracture
incomplete break
transverse fracture
break is in a straight line across the bone
segmental fracture
the same bone is broken in two places, so there is a “floating” piece of bone
fracture clinical manifestations
pain, tenderness at the site
inflammation
loss of function: loss of nerve function (local shock)
abnormal mobility
deformity: long bones: angulation, shortening, rotation
fracture diagnosis
hx: mechanism, time of injury
physical assessment: shortening and rotation of extremities, like feet, is indicative of a fracture
imaging: XR, others may be indicated based on complications
fracture treatment
objectives for treatment
reduction
immobilization
preservation and restoration of function
reduction and internal fixation
closed manipulation
surgical (open) reduction (ORIF)
immobilization and external fixation
immobilization: splints, casts, traction
external fixation: pins, screws
limb-lengthening systems
used to widen or lengthen bones, correct angular/rotational defects, immobilize fractures
preservation and restoration of function
active and passive ROM exercises
compartment syndrome etiology and pathogenesis
condition of increased pressure w/in a limited space that comprises the circulation and function of the tissues
What are the effects of fixed space (compartment) of an extremity?
increasing pressure can lead to death of nerve and muscle cells
permanent loss of function
What is the amount of pressure required to produce compartment syndrome dependent on?
duration of pressure elevation
metabolic rate of tissues
vascular tone
local blood pressures
acute compartment syndrome
can occur after a fracture or crushing injury
chronic compartment syndrome
may develop from exertion in long-duration of activity
compartment syndrome clinical manifestations
severe pain that is out of proportion to the injury
paresthesias, diminished reflexes, loss of motor function
compartment syndrome diagnosis
hx and physical assessment:
pain score
sensory assessment
motor functioning testing
peripheral vascular assessment: doppler pulses
compartment pressure
compartment syndrome treatment
removal of restrictive devices
casts, splints, dressings
elevating extremity to reduce edema
fasciotomy
incision of the fascia to separate it to allow for compartment to decompress
re-establishes blood flow
What does a lower extremity fracture put one at risk for?
venous thromboemboli (VTE)
deep venous thrombosis (DVT) and/or pulmonary embolism (PE)
What is the recommended treatment for a thromboemboli?
thromboprophylaxis
pharmacological or mechanical
How often do VTE related to musculoskeletal system (MSK) injuries/procedures (hospital admissions) occur after discharge?
≥ 2 months after discharge
follow up assessment is indicated
fat embolism syndrome (FES)
refers to multiple life-threatening manifestations resulting from the presence of fat droplets in the small blood vessels of the lung, kidneys, brain after a long bone or pelvic fracture
FES pathogenesis
unclear mechanism
thought to result from fat droplets that are released from the marrow or adipose tissue at the fracture site into the venous system through a torn vein
FES clinical manifestations
respiratory failure: chest pain, SOB, tachycardia, cyanosis
cerebral dysfunction: confusion, change in behaviors, disorientation, seizures
skin and mucosal petechiae: chest, axillae, neck, shoulders
FES diagnosis
arterial blood gas (ABG)
other diagnosis as appropriate
FES treatment
correct hypoxemia
inflammation
maintaining fluid balance
osteopenia
characterized by a reduction in bone mass greater than expected for age, race, or sex
occurs d/t a decrease in bone formation, inadequate bone mineralization, or excessive bone deossification
osteopenia diagnosis
not a diagnosis, but a term used to describe an apparent lack of bone seen on XR studies
osteopenia major causes
osteoporosis
osteomalacia
malignancy (multiple myeloma)
endocrine disorders (hyperparathyroidism, hyperthyroidism)
osteoporosis
characterized by a loss of mineralized bone mass causing increased porosity of the skeleton and susceptibility to fractures
often associated w/ the aging process
imbalance between bone resorption and formation
resorption > formation
bone mineral density (BMD)
peak bone mass
determined by genetics, estrogen levels, exercise, calcium intake and absorption, and environmental factors
osteoporosis pathogenesis
poor nutrition and physical activity
age-related decreased in intestinal absorption of calcium d/t deficient activation of Vit. D may contribute towards osteoporosis
postmenopausal osteoporosis
estrogen deficiency…loss of cancellous bone and predisposition to fractures of the vertebrae and distal radius
males have ~8-10% more BMD
age-related changes: osteoblasts have reduced replicative potential in older adults
secondary osteoporosis pathogenesis
endocrine disorders: hyperthyroidism, hyperparathyroidism, Cushing syndrome, DM
malignancies: multiple myeloma
alcohol use disorder: alcohol is a direct inhibitor of osteoblasts and inhibits calcium absorption
medication use: corticosteroids (prednisone), aluminum-containing antacids, anticonvulsants
osteoporosis clinical manifestations
often a silent disorder…
the first manifestations of the disease typically accompany a fracture
vertebral compression fracture
fracture of the hip, pelvis, humerus, etc.
loss of height
wedging and collapse of the vertebrae: kyphosis
systemic symptoms (weakness, fatigue, pain) are suggestive that osteoporosis is caused by an underlying disease process
secondary osteoporosis
osteoporosis diagnosis
WHO Working Group on Osteoporosis Screening Tool: Fracture Risk Assessment Algorithm
Dual-Energy X-Ray Absorptiometry (DEXA): spine and hip
serial height assessments
osteoporosis treatment
regular exercise
calcium supplementation
Vit. D supplementation
antiresorptive agents
estrogens and selective estrogen receptor modulators (SERMs)
biphosphonates
calcitonin
anabolic agents
osteomalacia etiology
2 main causes:
insufficient calcium absorption from the intestine d/t the lack of dietary calcium or deficiency of or resistance to the action of Vit. D
Vit. D deficiency is often caused by reduced Vit. D absorption as the result of biliary tract or intestinal diseases
cultural: northern China, Japan, northern India (less Vit. D from the diet)
phosphate deficiency d/t increased renal losses or decreased intestinal absorption
chronic renal failure
renal rickets
osteomalacia clinical manifestations
bone pain and tenderness
fractures (w/ disease progression)
muscle weakness (severe cases)
slightly reduced serum calcium levels
osteomalacia diagnosis
XR
lab tests
bone scans
bone biopsy
osteomalacia treatment
treat the cause…
nutrition
sun exposure
rickets etiology
kidney failure
malabsorptive syndromes (celiac disease, cystic fibrosis)
medications (anticonvulsants, aluminum-containing antacids)
nutritional rickets: results from inadequate sunlight exposure or inadequate intake of Vit. D, calcium, phosphate
prolonged breast-feeding w/o Vit. D supplementation
rickets clinical manifestations
bone deformities
unmineralization
enlarged and soft skull
delayed closure of fontanels
deformities are likely to affect the spine, pelvis, and long bones
lumbar lordosis (curving of the lower spine) and bowing of the legs
rickets treatment
nutrition: diet w/ calcium, phosphorus, and Vit. D
supplementation
sunlight exposure
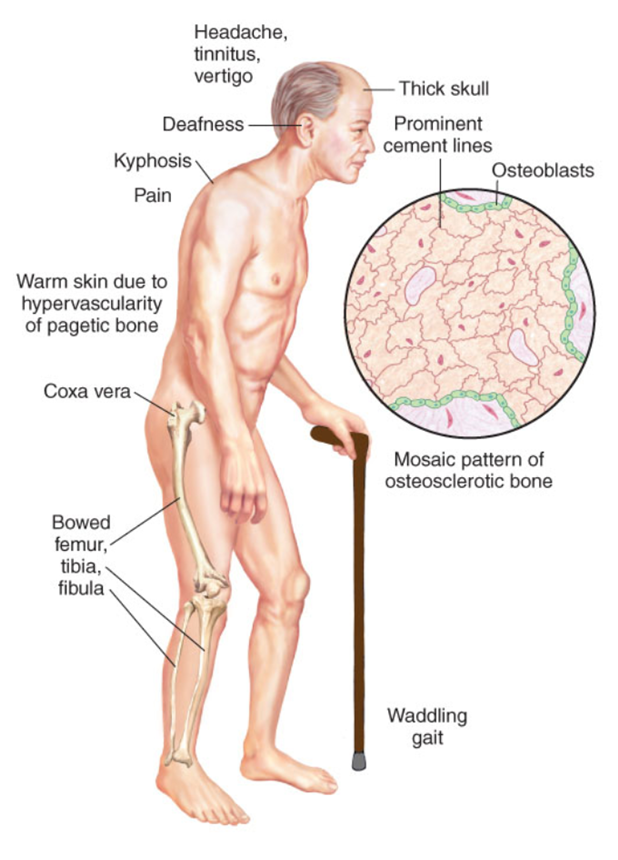
Paget disease overview
osteitis deformans
second most common bone disease
at the onset, marked by regions of rapidly occurring osteoclastic bone resorption
followed by period of hectic bone formation w/ increased osteoblasts rapidly depositing bone in a chaotic manner
poor quality bones…bowing and fractures
localized to the spine, skull, hips, pelvis
Paget disease etiology
genetic and environmental influences
15-40% have 1st degree relative w/ Paget disease
gene mutation
Paget disease clinical manifestations
often asymptomatic
detected during wellness visit or during times of other illness presentation
skull
HA, intermittent tinnitus, vertigo, eventual hearing loss
spine
kyphosis of the thoracic spine
femur and tibia
bowing
coxa vara: reduced angle of the femoral neck d/t softening; waddling gait
nerve palsy syndromes
mental decline
cardiovascular disease
high-output HF
calcific aortic stenosis
most common cause of death
osteogenic carcinomas
femur → pelvis → humerus → tibia
Paget disease diagnosis
based upon bone deformity characteristics and XR changes
bone scans
bone biopsy
differentiate other possibilities
infection vs carcinoma (primary vs metastases)
Paget disease treatment
based upon degree of pain and extent of disease
pain: NSAIDs, anti-inflammatory agents
suppressive agents: biphosphonates, calcitonin
prevent further spread and neurologic deficits
rheumatoid arthritis (RA) etiology
systemic inflammatory disease
genetic predisposition
first-degree relatives
gene: human leukocyte antigen (HLA) loci on the major histocompatibility complex (MHC)
immune-mediated joint inflammation
activation of T-cell-mediated response to an immunologic trigger
antimicrobial agent (virus, bacteria, etc.)
RA pathogenesis
aberrant immune response leading to synovial inflammation and destruction of the joint architecture
initiated by activation of helper T cells, release of cytokines (tumor necrosis factor [TNF], interleukin [IL]-1, an antibody formation
rheumatoid factor (RF) (70% - 80%)
inflammatory response that begins w/ attraction of neutrophils, macrophages, and lymphocytes that then release lysosomal enzymes to destroy the joint cartilage
progressive disorder
vasodilation and increased blood flow causes warmth and redness
joint swelling → reduced joint motion
irreversible
RA clinical manifestations
blend of systemic, articular (joint), and extra-articular (non-joint) manifestations
RA articular manifestations
symmetric and polyarticular
fingers, hands, wrists, knees, and feet
deformities
stiffness and pain
decreased joint motion
pain → fibrosis
subluxation
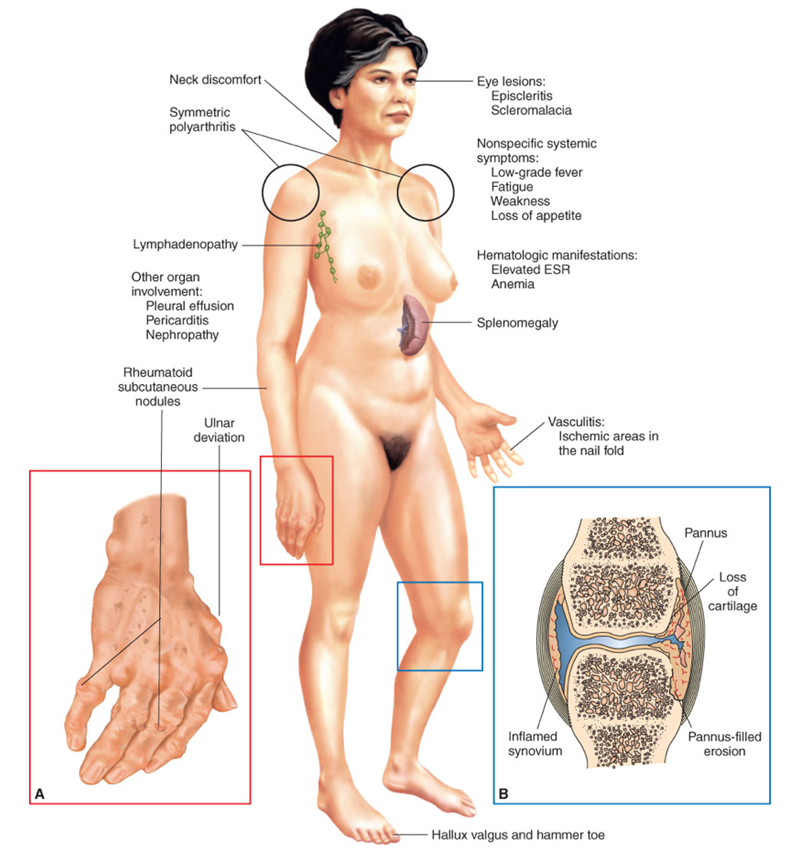
RA extra-articular manifestations
systemic: factor, weakness, anorexia, weight loss, low-grade fever
hematologic: thrombocytosis, anemia
felty syndrome (rare): RA, splenomegaly, neutropenia
rheumatoid nodules
vasculitis
ischemic areas in the nail fold and digital pulp that appears as brown spots
lower extremity ulcerations
neuropathy
visceral organ involvement
eyes
keratoconjunctivitis sicca
episcleritis
uveitis
nodular scleritis
RA treatment goals
prevent/reduce pain
decrease stiffness and swelling
maximize mobility
attempt to halt progression
RA treatment
pharmacological management
disease-modifying antirheumatic drugs (DMARDs)
NSAIDs
corticosteroids
biologics: anti-tumor necrosis factors (anti-TNFs)
surgery
synovectomy
systemic lupus erythematosus (SLE) pathogenesis
characterized by the formation of autoantibodies and immune complexes
B-cell hyperreactivity and increased production of antibodies against self and non-self antigens
autoantibodies can directly damage tissues or combine w/ other antigens to form tissue-damaging immune complexes
autoantibodies
antinuclear antibodies (ANA)
SLE etiology
development of autoantibodies may result from a combination of factors
genetics, hormones, immune factors, environment
How do SLE clinical manifestations occur?
in exacerbations and remissions
SLE musculoskeletal manifestations
arthralgias, arthritis
tenosynovitis
intrapatellar and Achilles tendon ruptures
avascular necrosis: femoral head
SLE integumentary manifestations
malar rash: butterfly rash
photosensitivity
fingertip lesions
nail fold infarcts, splinter hemorrhages
hair loss
SLE renal manifestations
glomerulonephritis
end-stage renal disease
interstitial nephritis
nephrotic syndrome
SLE pulmonary manifestations
pleural effusions
pleuritis
less common: pulmonary hemorrhage, interstitial lung disease, pulmonary embolism
SLE cardiac manifestations
pericarditis
myocarditis
HTN
ischemic heart diease
SLE neurologic manifestations
vasculitis leading to stroke or hemorrhage
seizures
psychosis
SLE hematologic manifestations
hemolytic anemia
leukopenia
lymphopenia
thrombocytopenia
lymphadenopathy
SLE diagnosis
hx, physical, labs
American College of Rheumatology criteria
diagnostics: ANA
SLE treatment priorities
prioritizes managing the acute and chronic symptoms
prevent progression
reduce exacerbations
minimize disability
prevent medication-related complications
SLE pharmacological management
NSAIDs
antimalarial agents
corticosteroids
immunosuppressive drugs
psoriatic arthritis etiology
unknown etiology
genetic, environmental, and immunologic factors appear to affect susceptibility and play a role in disease expression
environmental: infectious agents, trauma
immune: T-cell mediated immune response
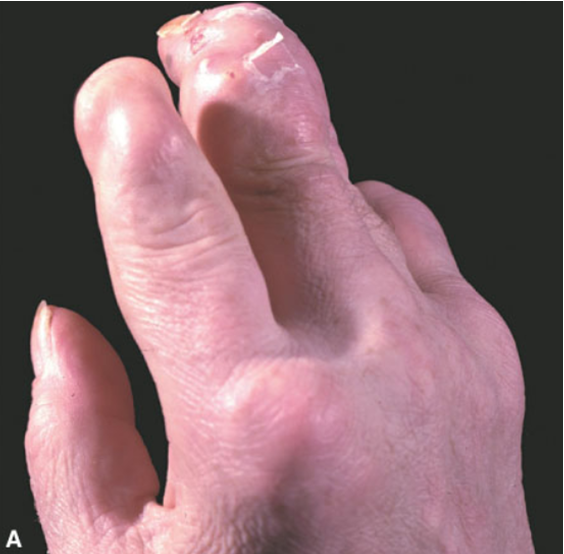
psoriatic arthritis clinical manifestations
manifestations of arthritis w/ psoriasis
detectable skin rash
skin or nail changes
psoriatic arthritis treatment
similar to treatment of RA
pharmacological management
NSAIDs: MSK symptoms
DMARDs: methotrexate, sulfasalazine
TNF inhibitors: indicated when there is inadequate response to DMARDs, NSAIDs, and steroid injections
osteoarthritis (OA) syndrome epidemiology and risk factors
age: primary OA affects 4% of people between the ages 18 - 24 years
85% of people in their 70s
sex: younger males are more commonly affected than females (45 years)
after age 55, female
race
hand OA is more common among Caucasian females
knee OA is more common among African American females
obesity
OA syndrome pathogenesis
alterations in the homeostatic mechanisms that maintain articular cartilage
significant changes in both the composition and mechanical properties of cartilage
increased water and decreased concentrations of proteoglycans (elasticity and stiffness) w/in the cartilage as compared to healthy tissue (early)
cytokine release which destroys the joint space
imbalance between joint building and breakdown
edematous changes in the cartilaginous matrix
cartilage loses its smooth aspect and cracks begin to form
erosion…inability to absorb shock
secondary OA pathogenesis
repetitive impact loading resulting in joint failure
high prevalence specific to vocational or avocational sites
shoulder and elbows of baseball pitchers
ankles of ballet dancers
knees of basketball players
immobilization
cartilage degeneration from the loss of lubrication that occurs w/ joint movement
OA cervical spine manifestations
localized stiffness
radicular vs. nonradicular pain
vascular compression d/t posterior osteophyte formaiton
OA lumbar spine manifestations
low back pain/stiffness
muscle spasm
decreased movement
nerve root compression → radicular pain
spinal stenosis
OA hip manifestations
insidious onset of pain — localized to the groin/inner thigh
may be referred to buttocks, sciatic region, or knee
reduced ROM
gait changes
OA knee manifestations
localized discomfort w/ pain on motion
reduced ROM crepitus
quadricep atrophy
joint instability
joint effusion
OA first carpometacarpal joint
tenderness at base of thumb
squared appearance to joint
OA first metatarsophalangeal joint
irregular joint contour
pain and swelling
OA diagnosis
hx
physical assessment
labs: elevated inflammatory markers (if inflammation is present)
diagnostics: XR findings
narrowed joint space, bony sclerosis, spikes, osteophytes
OA treatment
treatment goals: symptom management
nonpharmacologic management
exercises and strengthening
assistive devices: canes, walkers, splints
pharmacologic management
NSAIDs
intra-articular corticosteroid injections
surgery: severe disease
gout pathogenesis
the result of elevations in serum uric acid levels
uric acid is the end product of purine metabolism
overproduction of purines, augmented breakdown of nucleic acids, and decreased urinary excretion of uric acid
primary gout pathogenesis
90% of cases
overproduction of uric acid or inadequate elimination of uric acid (kidneys)
secondary gout pathogenesis
increased breakdown of nucleic acids
chronic renal disease, thiazide diuretic use
gout attack
precipitation of monosodium urate crystals in the join which initiate the inflammatory response
crystal deposition typically occurs in peripheral sites (great toe)
w/ prolonged hyperuricemia, crystals accumulate in the synovial joints and cartilage
results in cartilage destruction
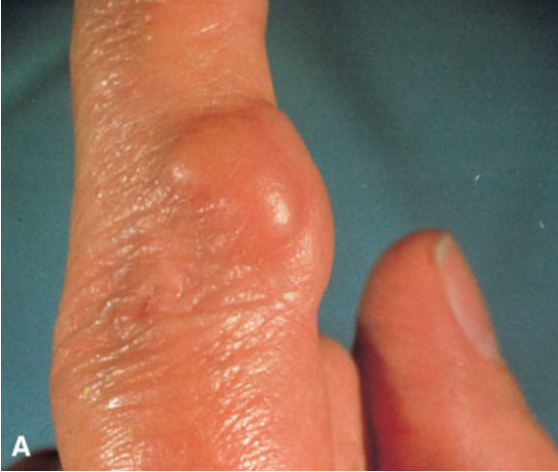
repeated or untreated attacks lead to chronic arthritis and the formation of tophi
large, hard nodules
gout clinical manifestations (4 stages)
Asymptomatic hyperuricemia
Acute gout arthritis
Typically, initial attack affects the first metatarsophalangeal joint
Tarsal joints, insteps, ankles, heels, knees, wrists, fingers, and elbows may also be initial sites
Abrupt onset of pain and inflammation
Intercritical gout
Early stages after the initial attack has subsided…asymptomatic
Chronic tophaceous gout
Recurrent attacks w/ permanent joint changes
gout treatment goals
termination and prevention of acute attacks
correction of hyperuricemia
gout treatment
Nonpharmacologic management
Weight management
Moderation in alcohol consumption
Tobacco cessation
Pharmacologic management
NSAIDs
Indomethacin, ibuprofen
Colchicine
Allopurinol
Corticosteroid injections