Menopause and Hormone Therapy
1/20
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
21 Terms
perimenopause
Transition period prior to menopause
→Heavier menstrual flow, Longer duration, irregular menses
menopause
the natural cessation of a woman's menstrual cycles, typically occurring between ages 45 and 55, marking the end of reproductive years
Vasomotor symptoms of menopause
Hot flashes, night sweats
Genitourinary symptoms of menopause
Vaginal atrophy- dyness, burning, irritation
Dyspareunia
Diminished libido
Urinary symptoms- urgency, dysuria, recurrent UTIs
Psychological symptoms of menopause
mood changes
General apporach to menopause treatment algorithm
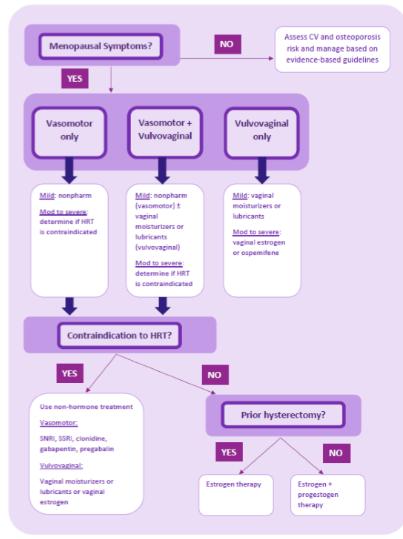
Risks of hormone therapy
Coronary heart disease
Stroke
Venous thromboembolism
Breast cancer
Define the age group and time from menopause onset that is most likely to have a favorable benefit/risk ratio in using hormone therapy
50-59 years or <10 years after the onset of menopause
Which estrogen formulations are systemic
Transfermal, Oral
Which estrogen formulations are local
Vaginal
What has a higher risk of VTW: the estrogen contraceptive patch or the pill?
ethinyl estradiol is more potent so the contraceptive patch (ethinyl estradiol) has greater risk for VTE compared to the pill due to more exposure of potent estrogen
What has a higher risk of VTW: the estrogen menopasal patch or the pill?
menopausal patch (estradiol) has a lower risk of VTE compared to oral options due to bypassion first pass
ET vs EPT
Progestogen is required for women with an intact uterus
Contraindications to hormone therapy
Unexplained vaginal bleeding
Severe liver disease
Known, suspected or history of estrogen sensitive breast or endometrial cancer
MI
Stroke
Dementia
High VTE risk
Initiating treatment >60 years or 10 years post menopause
Vasomotor (hot flashes) treatment - Pharm
Hormone therapy is the most effective treatment option
SSRI/SNRI- relief can occur within 1 week
Gabapentin, pregabalin
Clonidine- lower efficacy and more adverse effects
Veozah (fezolinetant) - Neurokinin 3 receptor antagonist
Vasomotor (hot flashes) treatment - NonPharm
Avoidance of triggers
Cooling techniques
Regular aerobic exercise
Yoga
Perimenopausal Menstrual Symptoms Treatment
Symptom management must be combined with contraceptive if engaging in sex
Combined hormonal contraception
GSM treatment- Vulvovaginal symptoms only
Mild—>Vaginal moisturizers and lubricants
Moderate- Severe —>Vaginal estrogen or ospemifene
GSM treatment- Vulvovaginal + Vasmotor sx
Consider systemic HT
Ospemifene
Improves intercourse pain
BBW: endometrial cancr
Options for women with mdoerate-severe GSM and those who do not respond to lubricants and moisturizers
Low dose vaginal estrogen
Vaginal DHEA
Ospemifene
Systemic HT