Pharm E3- Immunizations
1/95
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
96 Terms
What type of immunity is protection transferred from another person or animal as an antibody, and provides immediate protection, but is only temporary (weeks-mos)?
Passive immunity
The following are examples of what type of immunity?
Immune sera → human sources
Mom to baby, transplacental, breast feeding
Immunoglobulin → donated plasma
sterile homologous soln w/ pooled ab
antitoxin → animal sources
heterologous hyperimmune serum
equine sources (horse antitoxin), ovine (sheep)
used w/ snake bites (animals immunized to venom & given to pt to neutralize)
Passive immunity
What type of immunity is protection produced by a person’s own immune system, but offers delayed protection (need to produce antigen specific antibodies)?
*may need boosters or can be lifelong immunity
Active immunity
The following are examples of what type of immunity?
natural disease
vaccines
Active immunity
What type of vaccine?
“weakened” wild virus or bacteria → virulence is disabled
must replicate to be effective
provides stronger response, similar to natural illness
durable response (better memory) & requires fewer doses
Live, attenuated
The following downsides are seen with what type of vaccine?
interferes with circulating antibodies
maternal abs can neutralize vaccine
unstable → more of a storage concern
severe reactions are possible
Live, attenuated
What type of vaccine?
whole micro-organism killed by chemical or heat
does not replicate or cause disease in recipient
minimal effect on circulating antibodies
larger doses required
~ 3-5, protection seen after 2nd or 3rd dose
temporary immunity (humoral)
may need booster to activate B cells & retain immunologic memory
Killed, inactivated
What chemical found in vaccines such as MMR was previously thought to be linked to autism, but has since been proven not true?
Thimerosal (mercury based preservative)
With what patients should live attenuated vaccines be used with caution or avoided?
Infants, pregnant women, & immunocompromised (HIV w/ low CDD4 count, cancer patient on chemo, transplant patient, pt taking long term steroids, biologics, DMARDs, cyclosporine, etc)
What type of vaccine?
fractional → polysaccharide found on external capsule of bacteria
sugar chains on organisms that are big enough for the body to have an immune response to
T cell independent antigens
repeat doses don’t cause booster response
not good for children < 2 y/o → little/no protection
Pure polysaccharide
What type of vaccine?
fractional → conjugate w/ protein & polysaccharide to provide bigger target for immune system to respond to
T cell dependent → increases immunogenicity
good for children as young as 2 months
Conjugate polysaccharide
What kind of vaccine?
viral gene segment inserts into gene of yeast → modified yeast cell produces pure antigen
expensive
may be a better option for allergies
Recombinant
What is the general rule for timing g of vaccines?
All can be administered at the same visit as all other vaccines
What antigen combination is fine to be given simultaneously or at any interval?
2 or more inactive
Inactive & live
Which antigen combination should doses be given at 4 week intervals if not given simultaneously?
(give immune system time to fight off first vax & built immune system for a better response)
2 or more live
In a multi dose vaccine series, what is typically the time interval between the last 2 doses of primary immunizing series?
5-6 months
What might happen if the interval between doses in a multi dose vaccine series is shortened?
Interfere with antibody response & protection (worse / weaker immune response)
What might happen if the interval between doses in a multi dose vaccine series is delayed/longer (within reason)?
Does not diminish effectiveness but response is delayed
don’t need to restart series or add doses
When should a patient who needs radiation or chemotherapy receive live vaccines?
2 weeks before or 3 months after treatment
How should live vaccines & antibodies (Ig) be separated?
If live given first → wait ≥ 2 weeks before giving ab
If ab given earlier than 2 weeks → test for immunity or repeat vaccine
If ab given first → wait ≥ 3 months for live vax
What vaccines can be given with encephalopathy?
Live: contraindicated
Inactive: contraindicated
What vaccines can be given in pregnancy?
Live: contraindicated
Inactive: good
What vaccines can be given in immunosuppression?
Live: contraindicated
Inactive: good (but response is not as strong)
What vaccines can be given in severe illness?
Live: precaution
Inactive: precaution
*wait until illness subsides
What vaccine can be given if a patient recently received blood product?
Live: precaution
Inactive: good
*can have abs that mess with effectiveness of response
Why are vaccines usually not PO?
Protein → will get metabolized in GI tract, making it ineffective
What IM injection site is best for infants & toddlers?
Anterolateral aspect of upper thigh
What IM injection site is best for children & adults?
Deltoid
What IM injection site is generally avoided d/t inadequate responses?
Buttocks
Which vaccine can be taken PO route in babies because there is not a concern with bioavailability due to their immature GI tracts?
Rotavirus
What adverse effects can be seen with vaccines?
Local- pain, swelling, redness (MC w/ inactivated)
Systemic- fever, malaise, HA, nonspecific sx
Allergic rxn (rare, screen before)
What is the FDA reporting system that monitors adverse events that occur after immunization & providers should call and report any clinically significant reactions?
Vaccine adverse event reporting system (VAERS)
What is the federal “no fault” system of HRSA that compensates those who had a bad reaction to a childhood vaccine?
National vaccine injury compensation program (VICP)
What vaccines should all adults receive?
Tetanus, MMR, varicella, influenza
What vaccines are recommended for > 65 y/o?
Pneumococcal
Which influenza vaccine is recommended for > 50 y/o?
IM only, recombinant
Why do infants need to wait until 12 months to get the MMR vaccine (live vaccine)?
Passive transfer of maternal antibodies acquired in the 3rd trimester inhibit the immune response to the vaccine
How do you determine when a premature infant should start receiving live vaccines?
Based on postnatal age (tx the same as term infants)
What vaccines should pregnant women receive?
Influenza recommended for all pregnant / trying during flu season
Tdap during late 2nd or 3rd trimester d/t pertussis risk
*avoid live vaccines
What doses of steroids would make. patient contraindicated to live vaccines?
Prednisone > 20 mg/day or 2 mg/kg/day for > 14 days or equivalent doses of other steroids
Which steroids are not considered immunosuppressive and therefore allows a patient to receive a live vaccine?
Steroids given topically, MDI (inhaled), intra-articular injections, on alternate day therapies or short courses (< 2 weeks)
Which vaccine recommended for healthcare personnel is a 3 dose series (0, 1, 6 mos) given IM & requires serologic testing 1-2 months after the last dose?
Hep B
What is the recommendations for healthcare personnel & the vaccines against tetanus, diphtheria, and pertussis?
Td booster every 10 yrs after primary series OR 1 time dose of Tdap if < 65 y/o
In what healthcare personnel is the varicella vaccine indicated?
No serologic proof of immunity, prior vaccination or history of disease → 2 doses given SC 4 weeks apart
In what healthcare personnel is the MMR vaccine indicated?
Born in 1957 or later w/o serologic evidence of immunity or prior vaccination → 2 doses given SC 4 weeks apart
In what healthcare personnel is the meningococcal vaccine indicated?
Microbiologists who are routinely exposed to n. meningitidis isolates → 1 dose
What ages is the HPV vaccine recommended for?
9-26 y/o (best if before onset of sexual activity)
*can vaccinate 27-45 y/o but were probably already exposed → no effect on existing disease
How should the HPV vaccine be dosed?
2-3 dose series; 4 weeks between doses 1 and 2; 12 weeks between doses 2 and 3
What ages is the influenza vaccine recommended for?
All persons ≥ 6 months w/o a contraindication
What strains does the quadrivalent influenza vaccine cover?
2 A & 2 B strains
What strains did the older trivalent influenza vaccine cover?
2 A & 1 B strains
Which patients should get 2 doses of the IIV influenza vaccine instead of 1 dose?
Children < 9 years old/o getting vaccine for the first time
*4 week interval between doses, can be given simultaneously w/ others
Which influenza vaccines are inactivated vaccines (IIV) approved for persons > 6 months, given IM?
Fluzone, Fluvirin, Fluarix, FluLaval (same strains, approved for different age groups)
Which flu vaccine is better for patents with egg allergies (made w/o egg protein), but is generally more expensive?
Recombinant influenza vaccine - RIV, FluBlok
Which flu vaccine is a quadrivalent, live attenuated influenza vaccine (LAIV) given intranasally approved for healthy persons aged 2-49 y/o?
Flumist
What patients should receive 2 doses of LAIV instead of 1 dose?
Children aged 2-8 getting vaccine for the first time
*6-10 week interval bt doses; if not given simultaneously, space live vaccines 4 weeks apart
What are CIs to flumist?
Severe allergic rxn (egg protein) & concomitant ASA use in children/adolescents
In what patients is flumist not recommended?
Pregnant women, immunosuppressed, egg allergy, children 2-4 y/o w/ asthma or wheezing episode, antivirals w/in 48 hrs
What has the highest fatality rate of any infectious disease, most commonly in the US from bites from bats, raccoons, skunks, foxes?
Rabies
What stage of rabies infection does the administration of vaccine & abs try to intervene?
Incubation
What is the average incubation of rabies infection?
1 - 3 months (longer if lower extremities/farther from brain)
What are the preventative care options for animal bites?
Wound care (wash w/ soap & water, virucidal agent, povidone-iodine), antibiotics (augmentin MC), tetanus prophylaxis
What are the rabies immune globulin options for rabies prophylaxis?
Human derived (HRIG) - preferred in USA
Equine derived (ERIG) - higher risk of allergic rxn
What offers immediate neutralization after rabies exposure and is given IM to infiltrate around the bite site?
Rabies immunoglobulin
What agent used for rabies prophylaxis produces antibodies in 7-10 days of administration & is administered IM?
Rabies vaccine
What agents are rabies vaccines?
Human diploid cell vaccine (HDCV, Imovax)
Purified chick embryo cell vaccine (PCECV, RabAvert)
Where should the rabies vaccine be administered?
Deltoid
Rabies algorithm
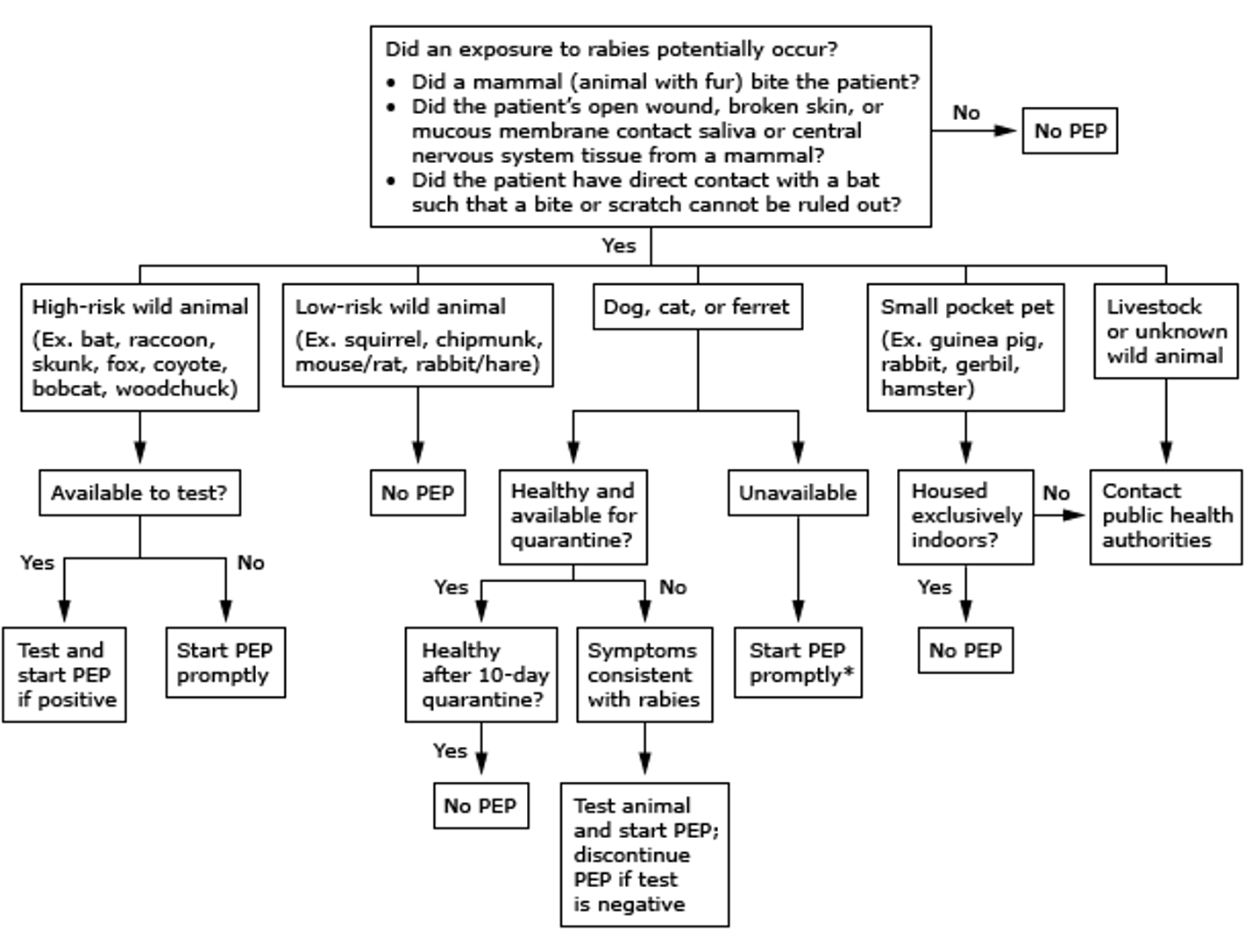
What is the only vaccine preventable disease that is not contagious (derived from environment)?
Tetanus (exotoxin from clostridium tetani)
What vaccine?
toxoid absorbed onto aluminum hydroxide / salts to increase antigenicity
binds to tetanus exotoxin & inactivates it
vaccine against the toxin produced, not the organism**
provides protection for 10 years
given for wound care management w/ diphtheria (Td) ± acellular pertussis
Tetanus toxoid
What is indicated for tetanus prophylaxis with more serious wounds in unvaccinated individuals, but its typically more expensive?
Tetanus Ig
Is TdaP used in adults or kids?
*higher dose of tetanus toxoid
Adults
Is DtaP used in adults or kids?
*high dose of diphtheria toxoid
Kids
What tetanus prophylaxis is indicated for the following patient?
clean & minor wound
unknown vaccination history OR fewer than 3 doses Tdap
Td: yes (single Tdap dose for > 10 y/o)
TIG: no
What tetanus prophylaxis is indicated for the following patient?
clean & minor wound
hx: ≥ 3 doses of Tdap
Td: no (unless > 10 yrs since last dose)
TIG: no
What tetanus prophylaxis is indicated for the following patient?
serious wound
unknown vaccination hx OR fewer than 3 doses of Tdap
Td: yes (single Tdap dose for > 10 y/o)
TIG: yes
What tetanus prophylaxis is indicated for the following patient?
serious wound
hx: ≥ 3 doses of Tdap
Td: no (unless > 5 yrs since last dose)
TIG: no
Tetanus algorithm
I dont think he could have made this chart more confusing!
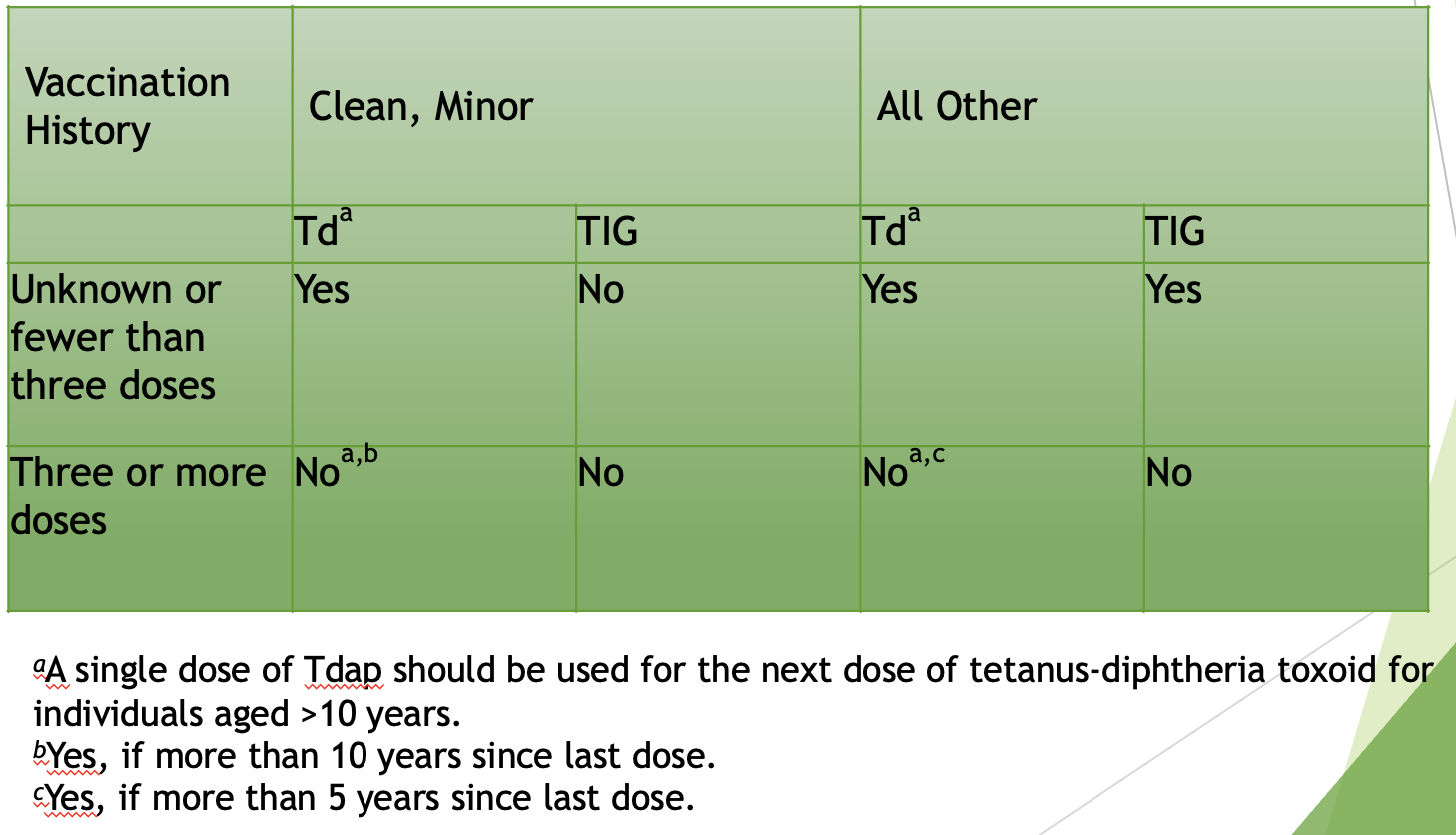
What is the T ½ of immunoglobulin (IgG)?
18-32 days
What adverse effects are seen with IgG administration?
Sensitization (allergic reaction), rate related chills / N / V
*flu like syndrome → pretreat with Benadryl, Tylenol, or steroids; start low & go slow
What patients / conditions would receive immunoglobulin (IgG)?
Primary immune deficiency (can’t produce own IgG), ITP, Kawasaki’s, AI disorders that need additional coverage, etc
What patients would receive RhO(D) immunoglobulin?
*RhO(D) status must be known
RhO(D) negative & exposed to RhO(D) positive RBCs (pregnancy)
What patients should NOT receive RhO(D) immunoglobulin?
RhO(D) positive or have anti-RhO antibodies
What can happen if a mother who is RhO(D) negative is pregnant with a baby who is RhO(D) positive?
Prodcues antibodies attacking fetal RBCs → hemolytic disease of newborn
*give immunoglobulin to reduce/prevent antibody formation
What agents are RhO(D) immunoglobulins?
WinRho, HyperRHO, RhoGAM
What is the antigenic target in SARS-CoV-2 vaccines?
Spike protein → binds to ACE2 receptors to induce membrane fusion
*antibodies bind to the spike protein to prevent this fusion
How do mRNA SARS-CoV-2 vaccines work (Pfizer, Moderna)?
Enters immune cells & gives copy of mRNA to translate & produce just the spike proteins (not the whole virus) & develop antibodies against that
*stays in cytoplasm, does not affect DNA, does not give whole organism like normal vaccines
How do adenovirus vector vaccines for SARS-CoV-2 work (J&J)?
Uses modified adenovirus engineered to express spike protein → may or may not replicate (not always effective)
How do protein adjuvant SARS-CoV-2 vaccines work (Noravax)?
Contains spike protein to stimulate a responce
(“like conjugate vax”)
How does Nirmatrelvir-ritonavir (Paxlovid) work for SARS-CoV-2?
Nirmatrelvir inhibits protease (Mpro) so virus can’t produce mature proteins
Ritonavir inhibits CYP3A4 to boost nirmatrelvir drug levels
How is Nirmatrelvir-ritonavir (Paxlovid) dosed?
BID x 5 days; skip dose if missed by more than 8 hrs
What ADRs are seen with nirmatrelvir-ritonavir (paxlovid)?
Many drug reactions (d/t 3A4 inhibition), mild ADRs, risk for rebound COVID
avoid in renal/hepatic impairment
How does Remdesivir (Veklury) work for SARS-CoV-2?
Inhibits RNA dependent RNA polymerase (RdRP) → mimics ATP to get incorporated into viral RNA & prevent production of proteins (chain terminator)
How is Remdesivir (Veklury) dosed?
Parenteral administration over 3 days
What ADRs are seen with remdesivir?
Hyperglycemia, redcued GFR, increased SCr
What is used in hospitalized patients who cannot receive Paxlovid?
Remdesivir