ANTITUBERCULAR ANTIBIOTICS / ANTILEPROSY
1/71
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
72 Terms
Dapsone
What is the sulfone derivative of sulfanilamide that was later investigated clinically?
Due to its high dosing, which caused toxicity.
Why was Dapsone considered too toxic for clinical use despite being effective for leprosy?
Streptomycin
What was the first antitubercular aminoglycoside discovered by Waksman et al. in 1944?
p-Aminosalicylic acid (PAS)
Which antitubercular drug’s properties were discovered shortly after streptomycin?
Isoniazid
What key antitubercular drug was discovered in 1952?
Ethambutol
Rifampicin
Which additional antitubercular drugs were later discovered after isoniazid?
Because Mycobacterium leprae fails to grow in cell culture.
Why has the development of drugs for leprosy treatment been difficult?
The availability of animal models, such as the infected mouse footpad.
What recent advancement allows in vivo drug evaluations for leprosy?
Due to the increasing emergence of dapsone-resistant strains of M. leprae.
Why have public health officials advocated for combination therapy in leprosy treatment?
Atypical Mycobacteria
- Mycobacteria other than M. tuberculosis and M. leprae that can cause disease.
- Such organisms are not normally considered particularly virulent or infectious
Increased numbers of immunocompromised individuals
Why are diseases caused by atypical mycobacteria increasing?
- Similar geographical distributions
- Are difficult to distinguish microbiologically and diagnostically
Why are Mycobacterium avium and Mycobacterium intracellulare considered a single complex (MAC)?
Mycobacterium avium
Mycobacterium intracellulare
Considered single complex (MAC)
Tuberculosis
What disease does MAC initially resemble?
Overwhelming disseminated form, leading to high morbidity and mortality.
How does MAC affect HIV-infected individuals?
Mycobacterium kansasii
- Is another atypical mycobacterium that causes pulmonary disease, which can spread (disseminate) in immunocompromised patients.
- Unlike MAC infections, which are resistant to most chemotherapeutic agents, these infections can usually be treated effectively with combinations of antitubercular drugs.
Mycobacterium avium
Mycobacterium intracellulare
Mycobacterium kansasii
Examples of Atypical Mycobacterium
Rifampin
What major antibiotic advanced tuberculosis treatment?
Isoniazid and ethambutol (or pyrazinamide)
What drugs are combined with rifampin for tuberculosis treatment?
At least 2 years
How long was TB maintenance therapy without rifampin?
6 to 9 months
How long is TB therapy with the rifampin combination?
- Isoniazid (H)
- Rifampicin (R)
- Pyrazinamide (Z)
- Ethambutol (E)
- Streptomycin (S)
First-line Anti-TB Agents:
- Cycloserine
- Kanamycin
- Capreomycin
- Ethionamide
- p-aminosalicylic acid (PAS)
Second-line Anti-TB Agents:
2HRZE/4HR
Lungs
Regimen 1 and its Site of Action
2HRZE/10HR
Different Parts of the Body
Regimen 2 and its Site of Action
Bacteriologically confirmed rifampicin-resistant TB (BC RR-TB)
Trends of Resistance
Positive for MTB using rapid diagnostic modalities with resistance to rifampicin.
Bacteriologically confirmed multidrug-resistant TB (BC MDR-TB)
Trends of Resistance
Positive for MTB complex with resistance to at least both isoniazid and rifampicin from an NTP-recognized laboratory.
Bacteriologically confirmed extensively drug-resistant TB (XDR-TB)
Trends of Resistance
Positive for MTB complex with resistance to any fluoroquinolone (FQ) and to at least one second-line injectable drug (streptomycin/ amikacin), in addition to multidrug resistance from an NTP- recognized laboratory.
Isoniazid
Antitubercular Agents: 1st Line
- Prepared by reacting the methyl ester of isonicotinic acid with hydrazine
- Its activity is manifested on the growing tubercle bacilli and not on resting forms
- Bactericidal; causes the bacilli to lose lipid content
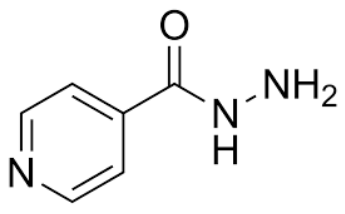
Inhibits the synthesis of mycolic acids, essential components of mycobacterial cell walls.
MOA of Isoniazid
- Isonicotinic acid hydrazide
- Isonicotinyl hydrazide
- INH
Isoniazid is also known as?
Lipid
What is important to mycobacterium tuberculosis (cell wall” peptidoglycan)?
Pyridoxine (vitamin B6)
What supplement is coadministered with isoniazid to prevent peripheral neuritis?
Antagonism of the coenzyme action of pyridoxal phosphate.
What causes peripheral neuritis in isoniazid therapy?
Hepatotoxicity
Which toxic reaction is more common when isoniazid is combined with rifampin?
Acetylation of the primary hydrazine nitrogen
What is the principal inactivation pathway of isoniazid?
- Peripheral Neuritis
- Gastrointestinal Disturbances
- Hepatoxicity
TOXIC REACTIONS OF ISONIAZID
Rifampicin/ Rifampin
Antitubercular Agents: 1st Line
- The most active agent in clinical use for the treatment of tuberculosis
- However, resistance to this drug develops rapidly in most species of bacteria, including the tubercle bacillus
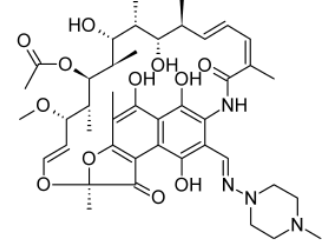
binds to the B-subunit of bacterial DNA-dependent RNA polymerases to prevent chain initiation
MOA of Rifampicin
Because it induces CYP450 enzymes, reducing the effectiveness of these drugs.
Why should rifampin not be combined with oral anticoagulants, benzodiazepines, or theophylline?
Reddish-orange discoloration of urine, stool, saliva, tears, and skin.
What unusual bodily fluid discoloration can occur with rifampin use?
Due to its hepatotoxicity, which may worsen liver function in alcoholics.
Why should rifampin not be used in chronic alcoholics?
Pyrazinamide
Antitubercular Agents: 1st Line
- Has recently been elevated to first-line status in short-term tuberculosis treatment regimens because of its tuberculocidal activity and comparatively low short-term toxicity
- Not active against metabolically inactive tubercle bacilli (not considered suitable for long-term therapy)
- Maximally effective in the low pH environment that exists in macrophages
- 12-24 hours, allowing once-daily or twice-weekly dosing.
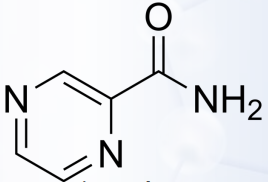
Penetrates Inflamed Meninges
Why is pyrazinamide recommended for tuberculous meningitis?
It interferes with uric acid excretion.
Why should pyrazinamide be used cautiously in patients with hyperuricemia or gout?
Pyrazinamide
Which TB drug in the HRZE/S regimen is the most hepatotoxic?
Ethambutol
Antitubercular Agents: 1st Line
- Active only against dividing mycobacteria
- Has no effect on encapsulated or other nonproliferating forms
- not recommended for use alone, but in combinations with other antitubercular drugs in the chemotherapy of pulmonary tuberculosis
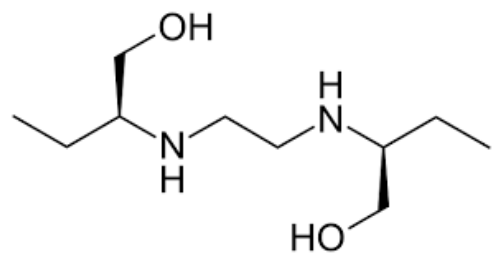
Inhibits the incorporation of mycolic acid into the cell wall.
MOA of Ethambutol
Red-green color blindness
Adverse Effect of Ethambutol
Ethambutol
Which HRZE/S drug is the only bacteriostatic agent?
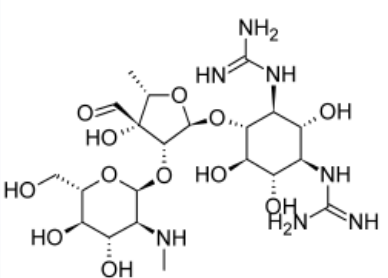
Streptomycin
Antitubercular Agents: 1st Line
- Produced from Streptomyces griseus
- MOA: inhibits the 30s bacterial ribosomal subunit
- Adverse effect: nephrotoxicity, vestibulotoxicity
Streptomyces griseus
Streptomycin is produced from which organism?
It inhibits the 30s bacterial ribosomal subunit, preventing protein synthesis.
What is the mechanism of action (MOA) of streptomycin?
- Nephrotoxicity (kidney damage).
- Vestibulotoxicity (damage to the inner ear, affecting balance).
What are the two major adverse effects of streptomycin?
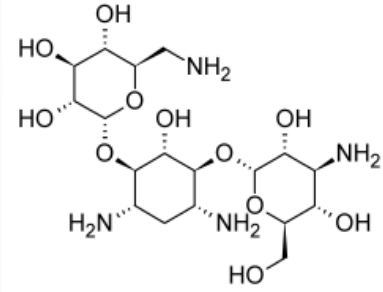
Kanamycin
Antitubercular Agents: 2nd Line
- produced from Streptomyces kanamyceticus
- MOA: inhibits the 30s bacterial ribosomal subunit
- Adverse effect: nephrotoxicity, vestibulotoxicity
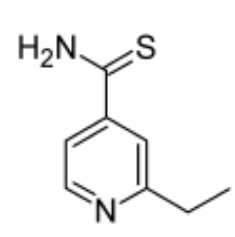
Ethionamide
Antitubercular Agents: 2nd Line
- Has weak bacteriostatic activity in vitro but, because of its lipid solubility, is effective in vivo
- Used in the treatment of isoniazid-resistant tuberculosis
- Highest tolerated dose of this drug is usually recommended due to low potency
GI intolerance
Hepatotoxicity
Visual disturbances
Adverse Effect of Ethionamide
Para-aminosalicylic Acid (PAS)
Antitubercular Agents: 2nd Line
- Orally in the form of its sodium salt, usually as a tablet or capsule.
- Similar to sulfonamides → Prevents the incorporation of PABA into dihydrofolic acid, catalyzed by dihydrofolate synthetase.
- used to be a first-line drug until the introduction of more effective agents
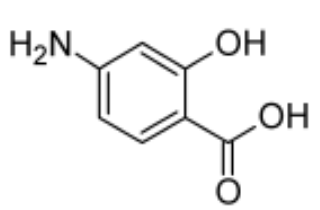
Aminosalicylic acid
4-aminosalicylic acid
PAS
What are the alternative names for para-aminosalicylic acid?
The amino and carboxyl groups must be para to each other and free.
What structural feature is required for PAS activity?
Dihydrofolic Acid
Para-aminosalicylic acid (PAS) prevents the incorporation of PABA into what molecule?
Cycloserine
Antitubercular Agents: 2nd Line
- Isolated from the fermentation beer of S. orchidaceus, S. garyphalus, and S. lavendulus
- MOA: prevents the synthesis of cross-linking peptide in the formation of bacterial cell walls
- Recommended for patients who fail to respond to other tuberculostatic drugs or who are known to be infected with organisms resistant to other agents
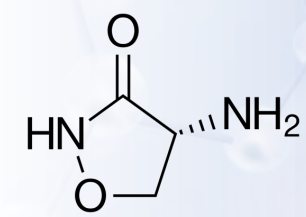
Streptomyces orchidaceus
S. garyphalus
S. lavendulus
Cycloserine is isolated from which organisms?
Prevents the synthesis of cross-linking peptide in the formation of bacterial cell walls.
What is the MOA of cycloserine?
Capreomycin
Antitubercular Agents: 2nd Line
- Isolated from Streptomyces capreolus
- May be used in place of streptomycin when either the patient is sensitive or the strain of M. tuberculosis is resistant to streptomycin
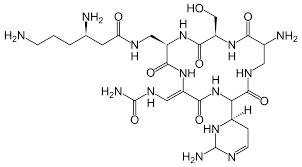
Dapsone
Clofazimine
Anti-leprosy Agents
Dapsone
Anti-leprosy Agents
- Used in the treatment of both lepromatous and tuberculoid types of leprosy
- Drug of choice for dermatitis herpetiformis
- Adverse effects: hemolytic anemia, methemoglobinemia, hepatotoxicity
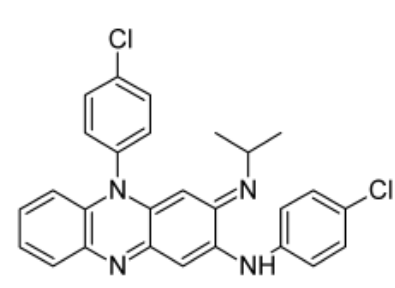
Clofazimine
Rifampicin
Dapsone is used in combination with which drugs for leprosy treatment?
Risk of severe hemolysis.
Why should dapsone not be administered to G6PD-deficient patients?
- Pyrimethamine for malaria
- Trimethoprim for PCP
Dapsone is sometimes combined with which drugs for malaria and PCP treatment?
Clofazimine
Anti-leprosy Agents
- Used in the treatment of lepromatous leprosy, including dapsone-resistant forms
- Frequently used in combination with other drugs, such as dapsone or rifampicin
- Has anti-inflammatory and immune-modulating effects that are of value in controlling neuritic complications and in suppressing erythema nodosum leprosum reactions
- Binds to nucleic acids and concentrates in reticuloendothelial tissue
- May interfere with electron transport processes by being an electron acceptor
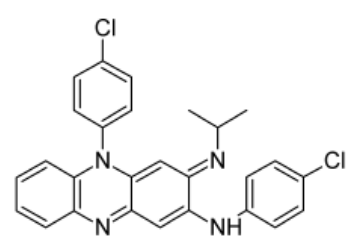
Erythema nodosum leprosum reactions.
What leprosy-related reaction does clofazimine help suppress?