Lectures 17 and 18: Auditory System
1/81
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
82 Terms
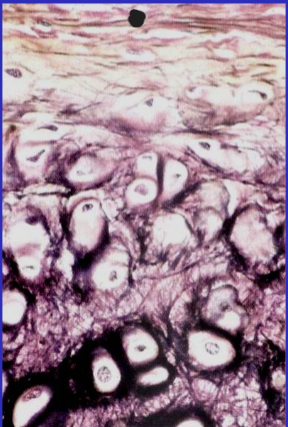
Auricle perichondrium
Auricle elastic cartilage
Auricle
stratified squamous epithelium (keratinized)
hair follicles
elastic cartilage (with elastic fibers)
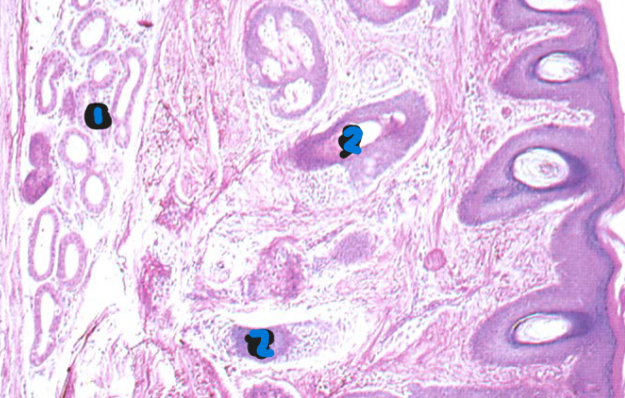
External acoustic meatus
1: Ceruminous glands
2: Hair follicles
external acoustic meatus
derives from pharyngeal cleft 1
stratified squamous epithelium
hair follicles
ceruminous glands (modified apocrine sweat glands)
elastic cartilage, temporal bone
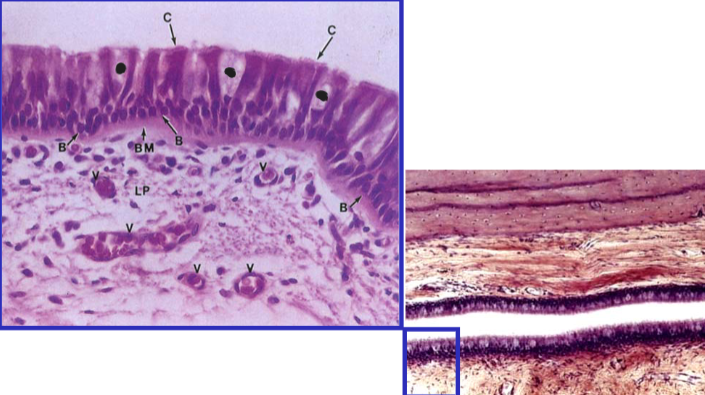
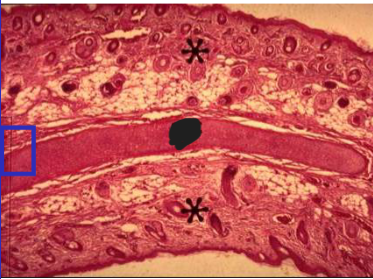
Eustachian tube goblet cells
Eustachian tube
derives from pharyngeal pouch 1
pseudostratified respiratory epithelium
numerous goblet cells
temporal bone, fibrocartilage
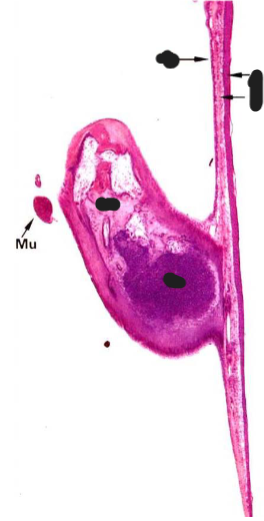
Tympanic Membrane and middle ear ossicles
cuticular layer
fibrous layer
mucous layer
cartilage
compact bone
tympanic membrane layers
cuticular layer of stratified squamous epithelium (ectoderm)
ectoderm that derives from pharyngeal cleft 1
fibrous layer with collagen II and III (mesoderm)
mucous layer of cuboidal cells (endoderm)
endoderm that derives from pharyngeal pouch 1
middle ear ossicles
compact bone formed by endochondral ossification
malleus, incus, stapes articulate with synovial joints
Otosclerosis
Tissue overgrowth and fixation of stapes to oval window (can be inherited)
tympanic membrane
air vibrations through external acoustic meatus oscillate tympanic membrane
during otoscopic exam a cone of light radiates anteroinferiorly from umbo
cone of light is reflection of otoscope illuminator
otitis media (inflammation/infection of middle ear) can scar middle ear ossicles, rupture tympanic membrane, or cause facial nerve palsy and diminished taste
internal ear
spiral lamina spirals around bony modiolus and houses spiral ganglion
membranous cochlea
scala vestibuli – oval window
scala tympani – round window
scala media (cochlear duct)
organ of Corti is sensory organ of auditory system internal ear
spiral ganglion
housed in spiral lamina
collection of neuronal cell bodies of neurons with axons in CN VIII
dendrites of these neurons synapse in organ of Corti
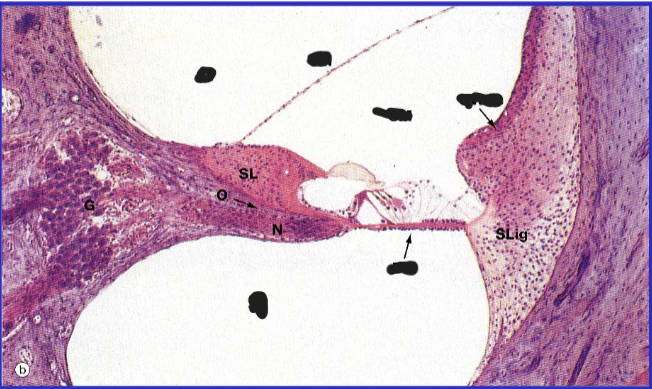

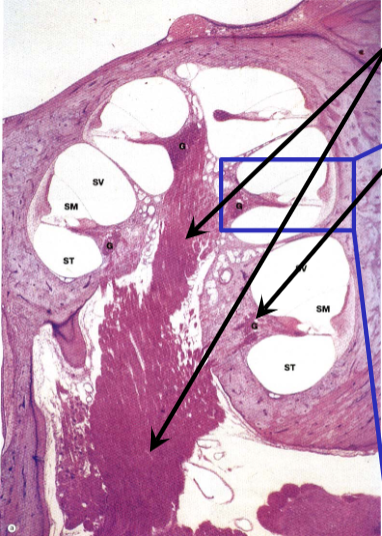

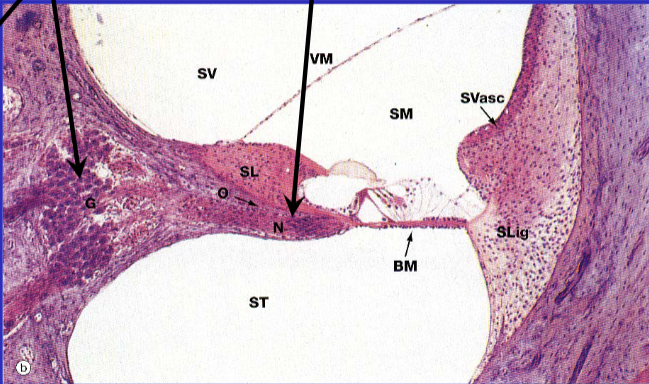

Ear Development
otic placode invaginates to form otic vesicle
otic placode forms otic pit
otic pit forms otic vesicle
statoacoustic ganglion forms from cells of otic vesicle wall and migrating neural crest, and later splits into vestibular and cochlear (spiral) ganglia
otic vesicle forms membranous labyrinth
dorsal component forms utricle, semicircular canals, and endolymphatic duct
ventral component forms saccule and cochlear duct
membranous labyrinth development
cochlear duct surrounded by mesenchyme
mesenchyme differentiates into cartilage by 10 weeks
vacuoles appear in cartilage
membranes separate cochlear duct from scala vestibuli and scala tympani
organ of corti development
by 5 months neuroepithelial cells and tectorial membrane form in cochlear duct
spiral tunnels become tunnel of Corti
middle ear ossicles development
malleus and incus derive from first pharyngeal arch
stapes derives from second pharyngeal arch
mesenchymal condensation by 7 weeks
cartilaginous precursors in mesenchyme remain embedded until eighth month
tympanic membrane development
cuticular layer is ectodermal epithelium from pharyngeal cleft 1
mucous layer is endodermal epithelium from pharyngeal pouch 1
sound frequency localization
frequency of sound determines frequency of oval window displacement and frequency of traveling wave in basilar membrane
each traveling wave maximally activates basilar membrane in specific location in cochlea
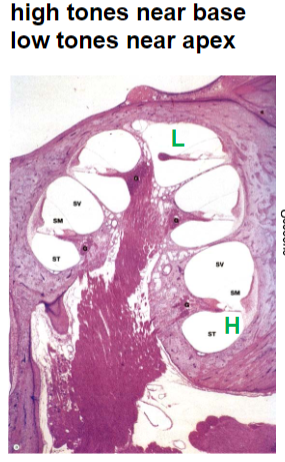
high frequency tones activate near base of cochlea, low frequency near apex of cochlea
retinoic acid establishes BMP7 gradient along developing cochlea
BMP7 higher at apex of cochlea promoting development of low frequency sensing hair cells
this tonotopic representation along the cochlea is conserved through the auditory pathway
interaural time difference
for localizing low-frequency sounds
interaural intensity difference
for localizing high-frequency sounds
endolymph and perilymph
stria vascularis is responsible for maintaining the ionic composition of endolymph through selective secretion and absorption of ions
endolymph of scala media is similar to intracellular fluid, has high concentration of K+ for depolarization
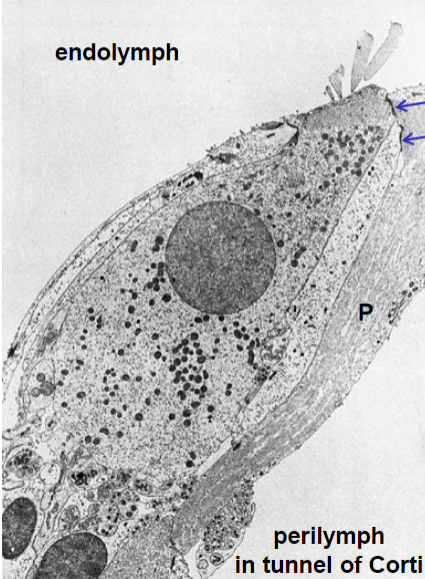
perilymph of scala vestibuli and scala tympani is similar to cerebrospinal fluid, has high concentration of Na+ for neuron viability; also located in tunnel of Corti (between inner and outer hair cells) and basal end of hair cells
tight junctions
at apical end of hair cells with phalangeal cells reticular laminae of phalangeal cells separate endolymph from perilymph
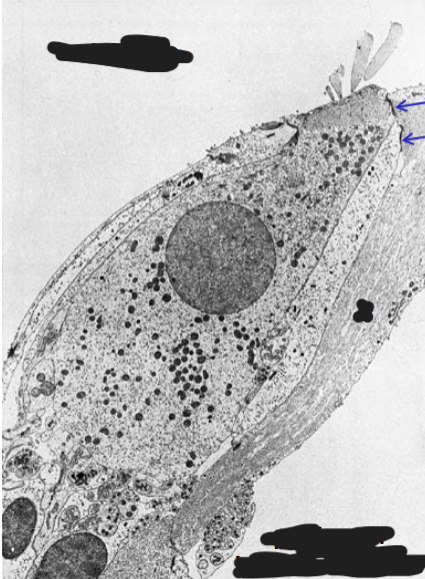
Tight junctions
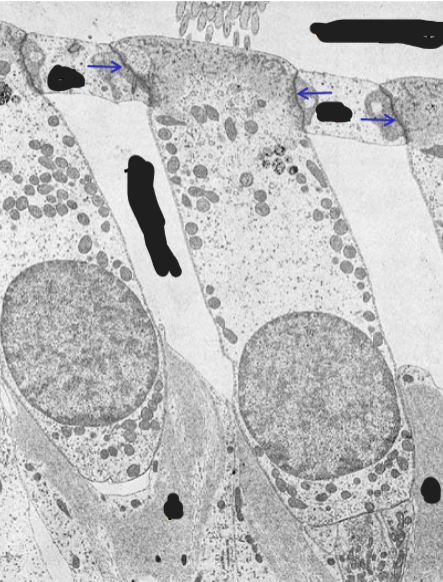
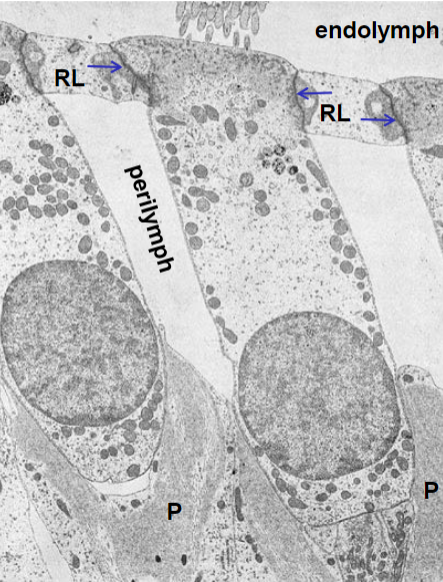
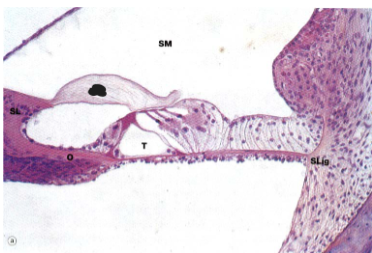
Tectorial membrane
organ of Corti includes
tectorial membrane
supporting cells including phalangeal cells
inner hair cells (single row)
tunnel of Corti
outer hair cells (typically 3-4 rows)
cochlear afferent neurons (type I and II)
olivocochlear efferent neurons
basilar membrane
cochlear afferent neurons
cell bodies in spiral ganglion
innervate hair cells
unmyelinated in organ of Corti
inner hair cell
sensory receptors for sound stimuli
outer hair cells
alter mechanics of basilar membrane by changing length when stimulated
increases sensitivity of cochlear afferent neurons conveying information from inner hair cells
mechanoelectrical transduction mechanism
displacement of basilar membrane relative to tectorial membrane
displacement of stereocilia of hair cells toward tallest stereocilium
mechanically-gated potassium channels open in stereocilia
increased potassium flow into hair cell from endolymph
depolarization of hair cell
voltage-gated calcium channels open at base of hair cell
increased calcium flow into hair cell
increased synaptic vesicle fusion
increased neurotransmitter (glutamate) release
glutamate binds receptors of cochlear afferent neurons
these first order neurons depolarize and increase firing rate
type I cochlear afferent neurons
bipolar
90-95% of neurons in spiral ganglion
synapse with 1-2 inner hair cells each
as many as 20 may converge on 1 inner hair cell
inner hair cells are receptors for sound stimuli
respond to narrow frequency range (high precision)
type II cochlear afferent neurons
bipolar
5-10% of neurons in spiral ganglion
synapse with 10+ outer hair cells each
outer hair cells alter mechanics of basilar membrane to improve
type I cochlear afferent neuron sensitivity
respond to wide frequency range (low precision)
Frequency
coded in the cochlear nerve by the position of the cochlear afferent neurons in the cochlea
with high frequency near the base and low frequency near the apex of the cochlea
intensity
coded in the cochlear nerve by both the discharge rate of the cochlear afferent neurons and the recruitment of additional cochlear afferent neurons as stimulus intensity increases
characteristic frequency
for a type I cochlear afferent neuron the frequency with the lowest threshold intensity
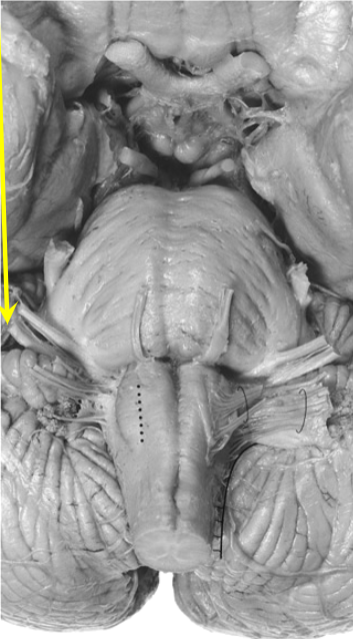
Vestibulocochlear nerve

cochlear nuclei
first order neurons
cell bodies in spiral ganglion
axons in vestibulocochlear nerve
synapse in ipsilateral cochlear nuclei
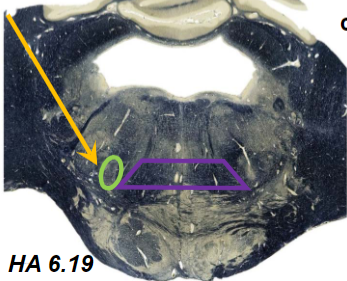
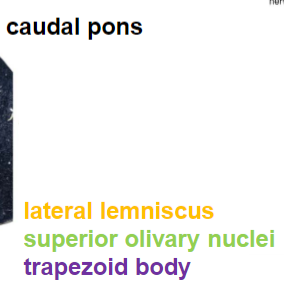
second order neurons
cell bodies in cochlear nuclei
axons in several pontine structures including trapezoid and lateral lemniscus
information ultimately reaches inferior colliculus
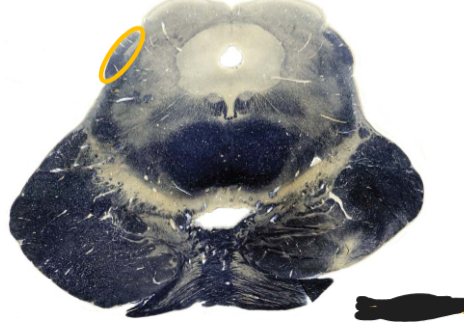
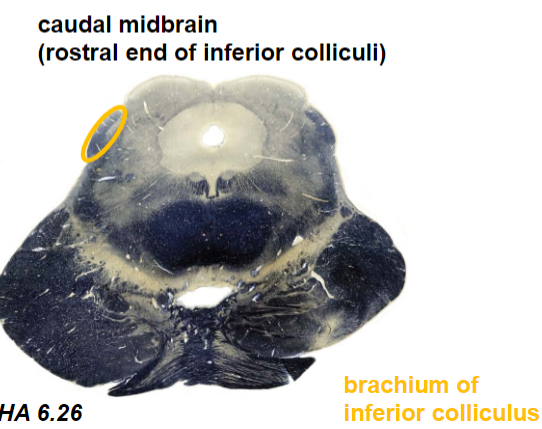
inferior colliculus neurons
cell bodies in inferior colliculus
axons in brachium of inferior colliculus
synapse in MGN of thalamus
medial geniculate nucleus (MGN) divisions
anterior division: involved in complex feature detection (not just simple tones)
posterior division: conveys information about moving or novel stimuli that direct auditory attention
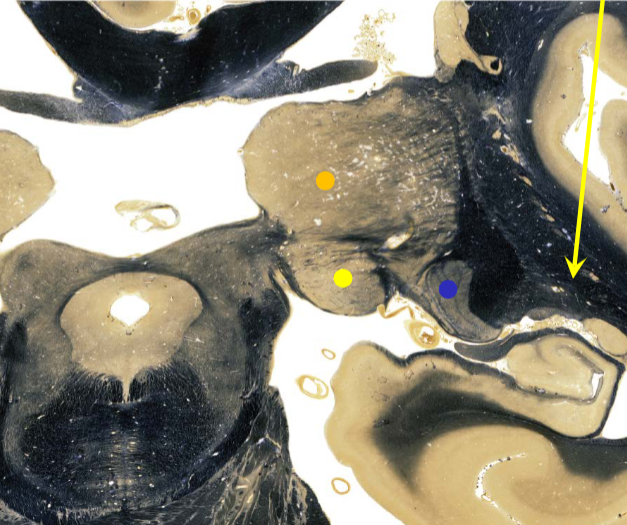

medial geniculate nucleus (MGN) supplied by
thalamogeniculate artery of PCA (posterior thalamus)
sublenticular limb
MGN axons project to primary auditory cortex as sublenticular limb then auditory radiation
sublenticular limb supplied by lenticulostriate arteries
connections between thalamus and cortex

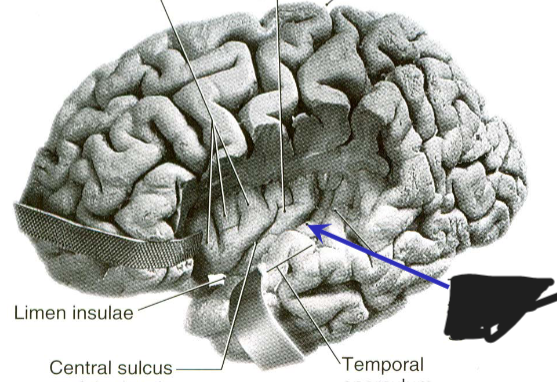
anterior transverse temporal gyrus of Heschl
Primary auditory cortex
primary auditory cortex
Brodmann area 41
anterior transverse temporal gyrus of Heschl
(1-3 gyri of Heschl, 2 is most common)
heterotypical granular cortex
receives axons from anterior division of MGN
contributes to complex feature detection
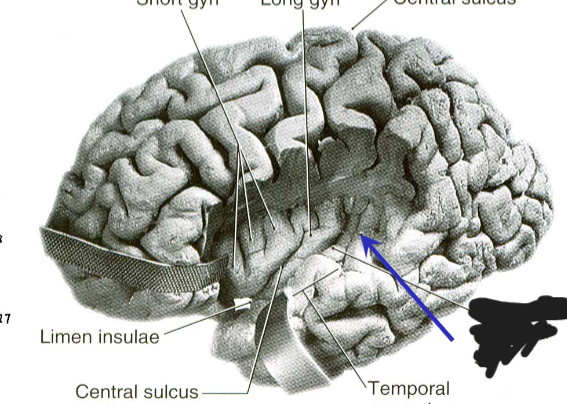
posterior transverse temporal gyrus of Heschl
secondary auditory cortex
secondary auditory cortex
Brodmann area 42
posterior transverse temporal gyrus of Heschl
cortex is less granular than primary auditory cortex
receives axons from posterior division of MGN
contributes to auditory attention to moving or novel stimuli
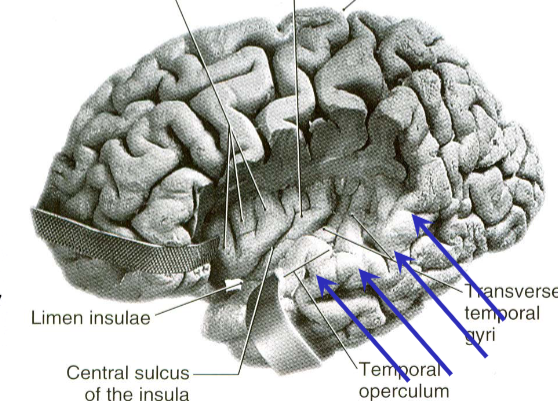
auditory association cortex
Part of Wernicke’s area
auditory association cortex
Brodmann area 22
superior temporal gyrus
part of Wernicke’s area
also receives visual and other sensory information
damage affects language comprehension for speech (but not fluency)
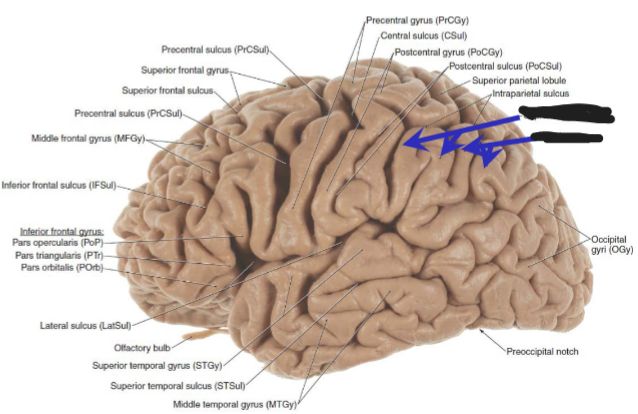
part of Wernicke’s area
Broadman area 39,40
Brodmann area 39,40
angular and supramarginal gyri of parietal lobe
part of Wernicke’s area
damage affects language comprehension for reading and writing (but not fluency)
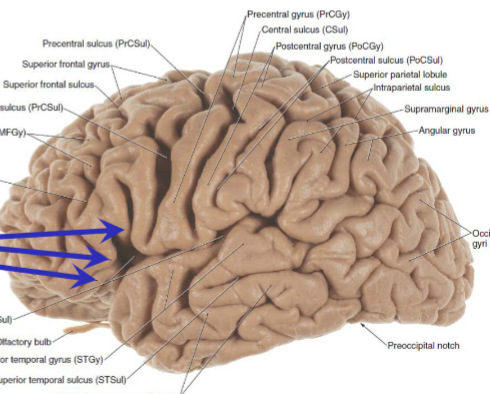
Broca’s area
Broca’s area
Brodmann area 44,45
inferior frontal gyrus
arcuate fasciculus projects from Wernicke’s area to Broca’s area
damage affects language fluency (but not comprehension)
internal ear, cochlear nuclei supplied by
AICA (labyrinthine)
inferior colliculus
quadrigeminal
MGN
thalamogeniculate
primary auditory cortex, auditory
radiation
middle cerebral (inferior trunk)
internal capsule (including sublenticular limb)
MCA lenticulostriate arteries
primary somatomotor cortex, primary somatosensory cortex, and frontal eye field
MCA superior trunk
inferior temporal optic radiation (including Meyer’s loop), primary auditory cortex, and auditory radiation
MCA inferior trunk
primary somatomotor cortex, primary somatosensory cortex, inferior temporal optic radiation (including Meyer’s loop), frontal eye field, primary auditory cortex, and auditory radiation
MCA distal stem
primary somatomotor cortex, primary somatosensory cortex, internal capsule, complete optic radiation, frontal eye field, primary auditory cortex, and auditory radiation
MCA proximal stem
descending auditory pathways
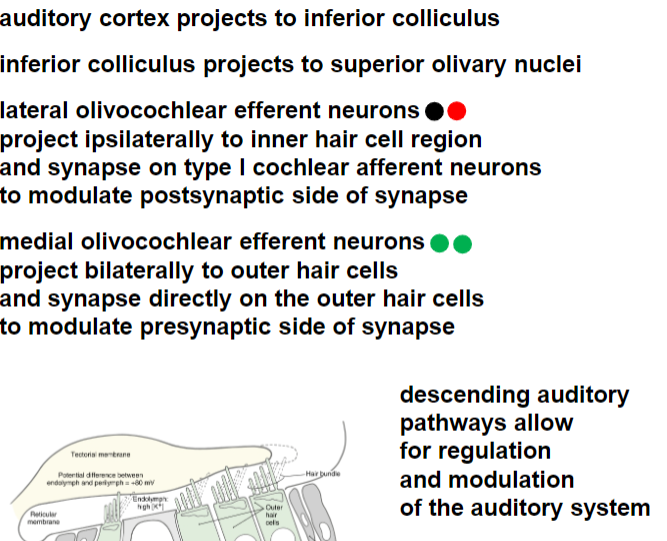
monaural information
routed to the contralateral side

binaural information
handled by central pathways that compare the differences between sounds at both ears

basilar membrane in cochlea tonotopic organization
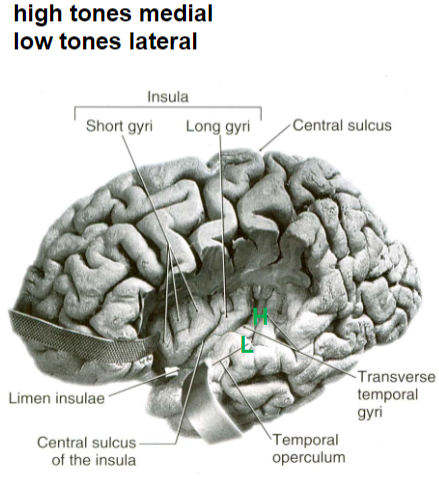
primary auditory cortex tonotopic organization
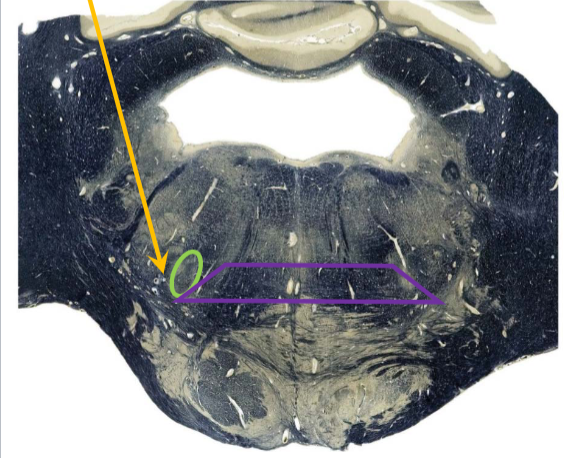
superior olivary nuclei
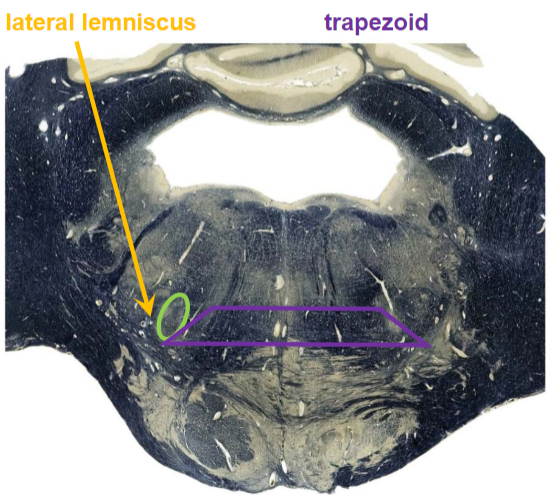
superior olivary nuclei
receives bilateral auditory input
important for localizing sounds in space
bilateralism

orientation of head, eyes, and body to novel sound

for acoustic startle reflex
no voluntary aspects
afferent limb is lateral lemniscus, inferior colliculus, MGN, secondary auditory cortex, superior colliculus
efferent targets are reticulospinal tracts (UMNs), spinal cord (LMNs), facial motor nucleus (LMNs)
middle ear reflex
dampen movement of middle ear bones to compensate for impedance difference between air and fluid
afferent limb: cochlear nuclei neurons, superior olivary nuclei neurons
efferent limb: facial motor nucleus neurons, trigeminal motor nucleus neurons
efferent targets: stapedius muscle, tensor tympani muscle
occurs as sound intensity increases beyond 85 dB
stapedius muscle is attached to stapes, is innervated by CN VII, and diminishes sound intensity when contracted
tensor tympani muscle is attached to malleus, is innervated by CN V, and contracts sometimes when swallowing (it does not contract in response to sound in humans)
in humans the middle ear reflex is mediated exclusively by the stapedius muscle