Ocular Physiology Midterm 3
1/307
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
308 Terms
Does the aqueous humor or cornea stroma have a greater concentration of lactate?
cornea stroma -- anaerobic byproduct
What moves lactate into the aqueous humor?
MCT (monocarboxylate transporter)
basolateral -- transports into endothelium
apical -- transports to aqueous humor
Which part of the cornea is carbon dioxide primarily produced?
posterior stroma (gradient, anaerobic respiration)
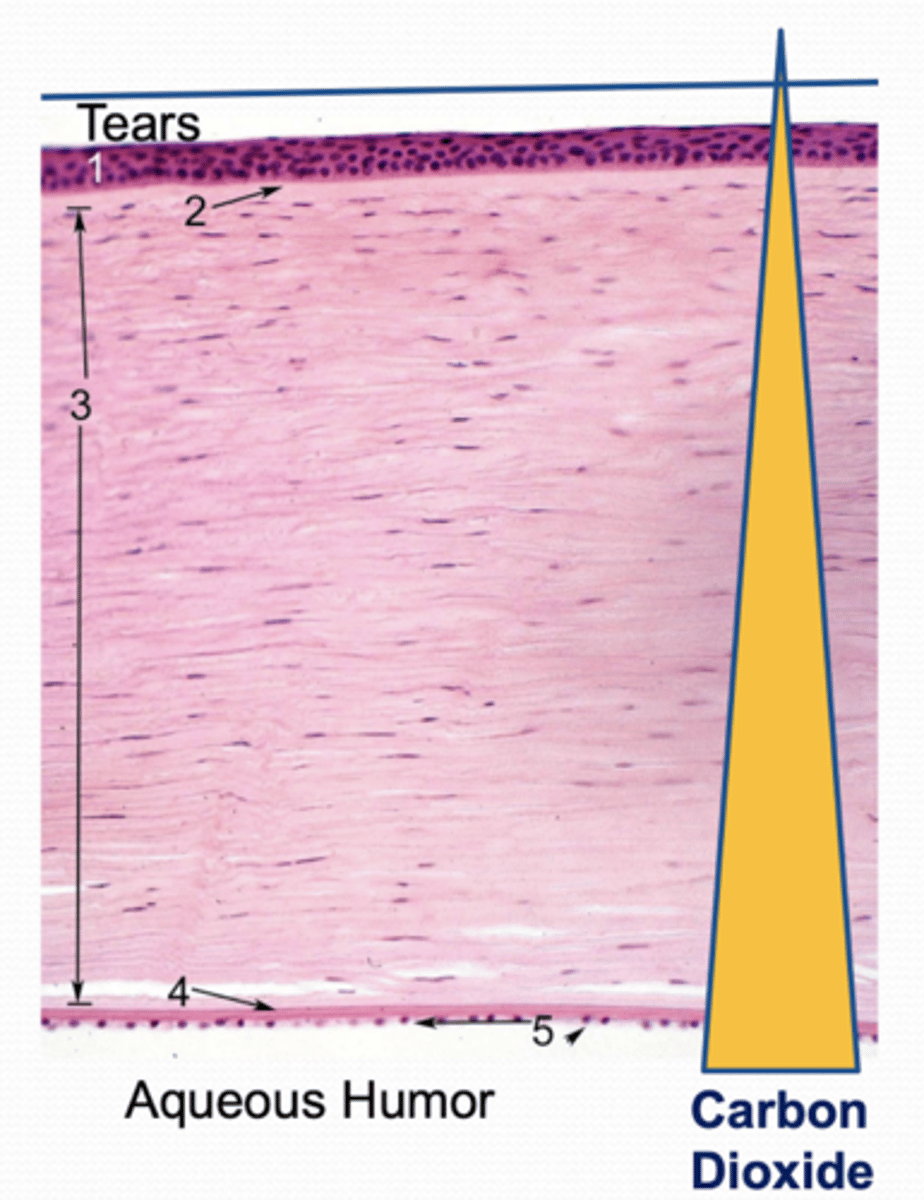
Why does lactate lower the pH?
weak acid -- will produce H+
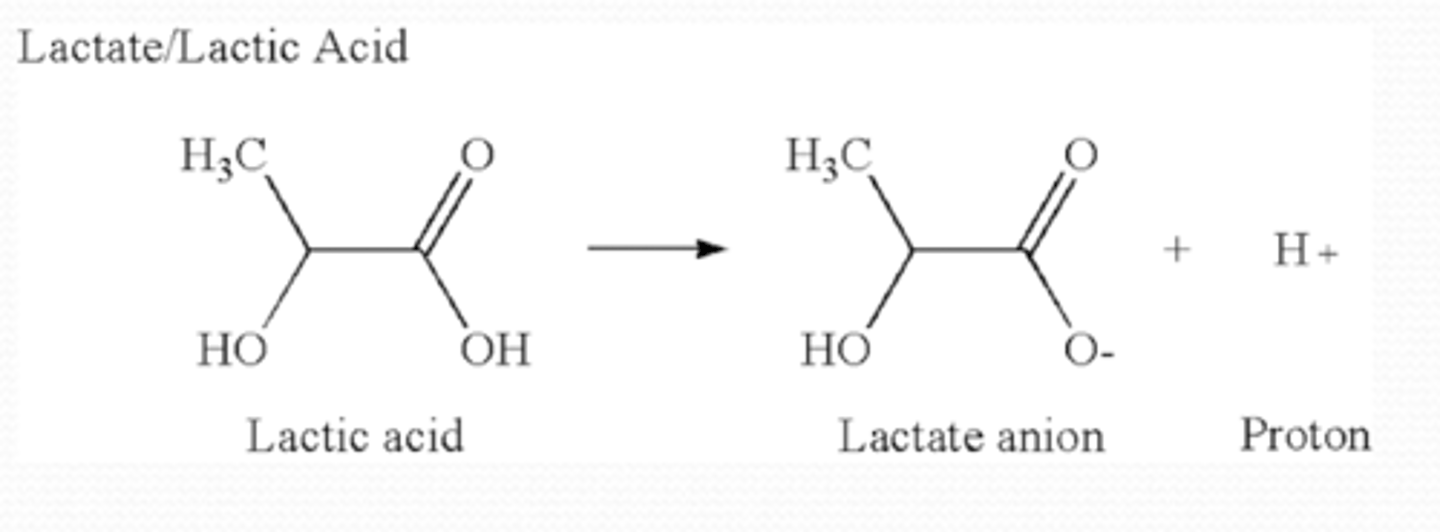
Where is glycogen present in the cornea?
corneal epithelium -- converted to glycogen and packed into cytoplasmic granules for future use
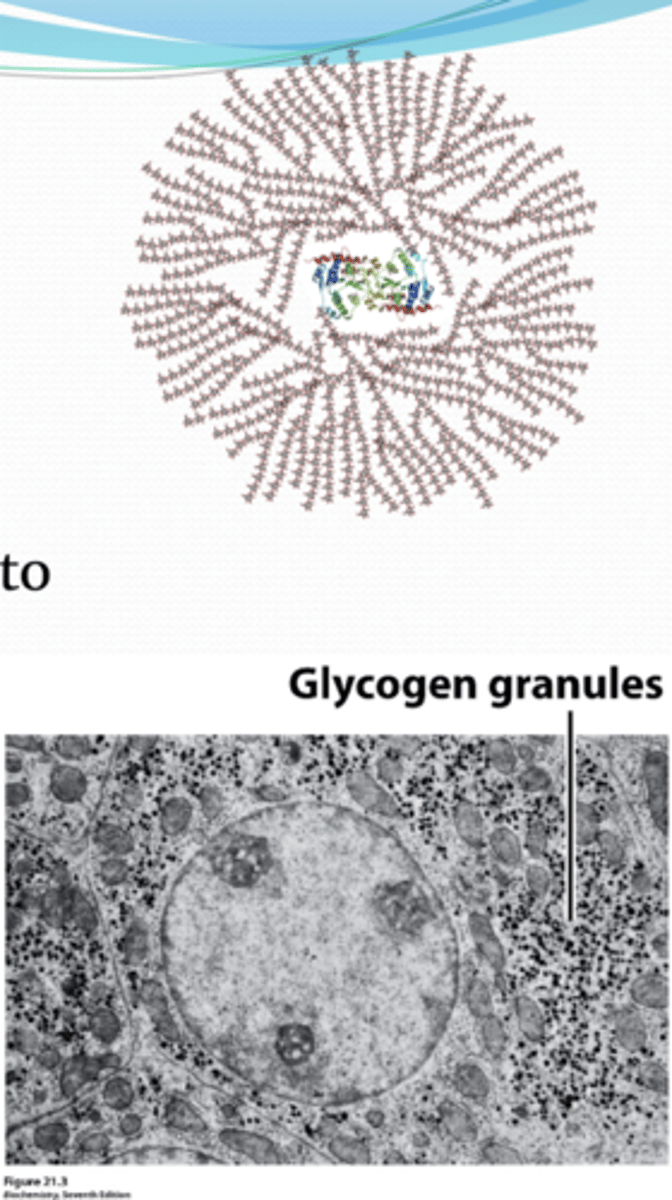
What inhibits the formation of glycogen?
FIH-1 (factor inhibiting hypoxia inducible factor 1)
How does FIH-1 inhibit the production of glycogen?
inhibits the production of enzymes required for glycogen formation
Where is FIH-1 found in the eye?
limbus > cornea (still present in the cornea!)
What happens to the partial pressure of oxygen in the tears when the palpebrae are closed?
decreases
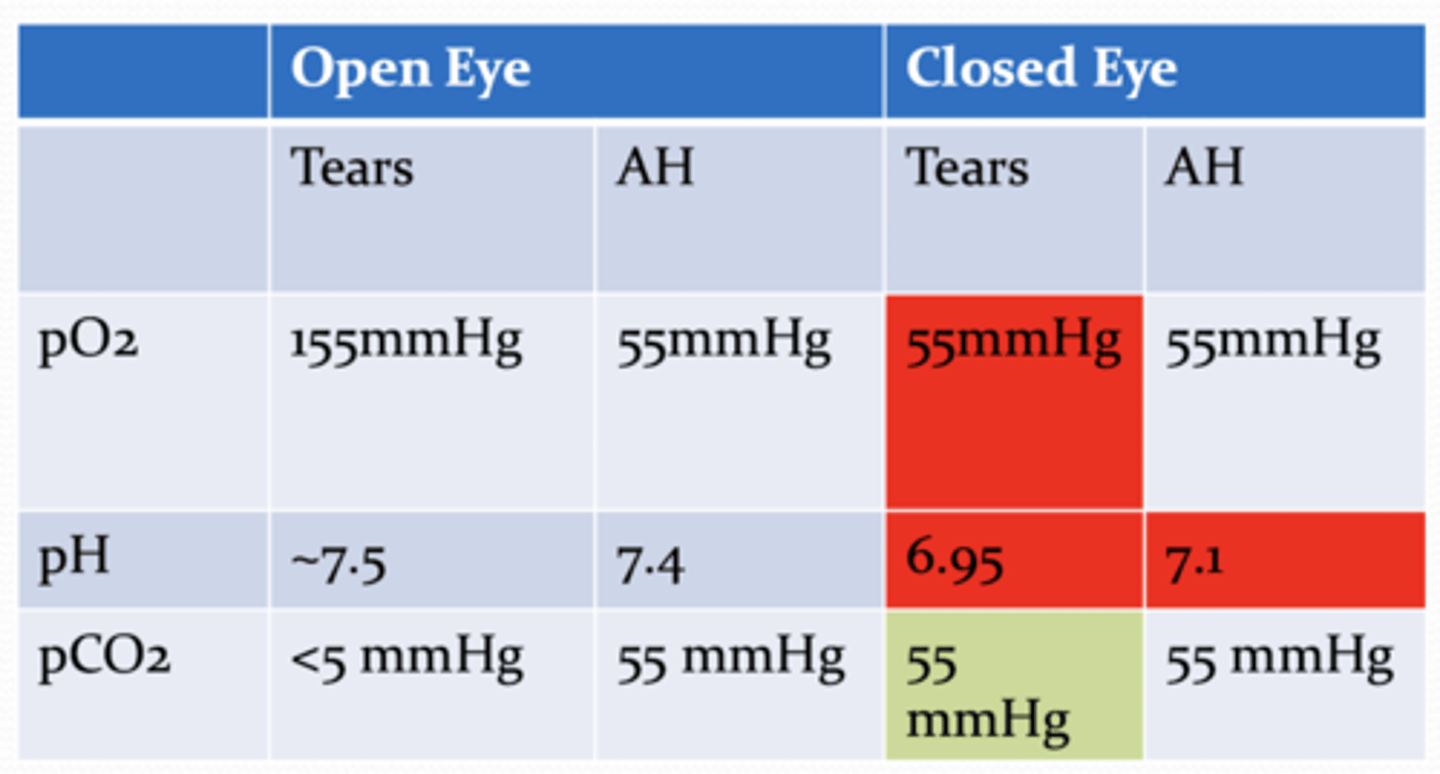
What happens to the partial pressure of oxygen in the aqueous humor when the palpebrae are closed?
remains constant
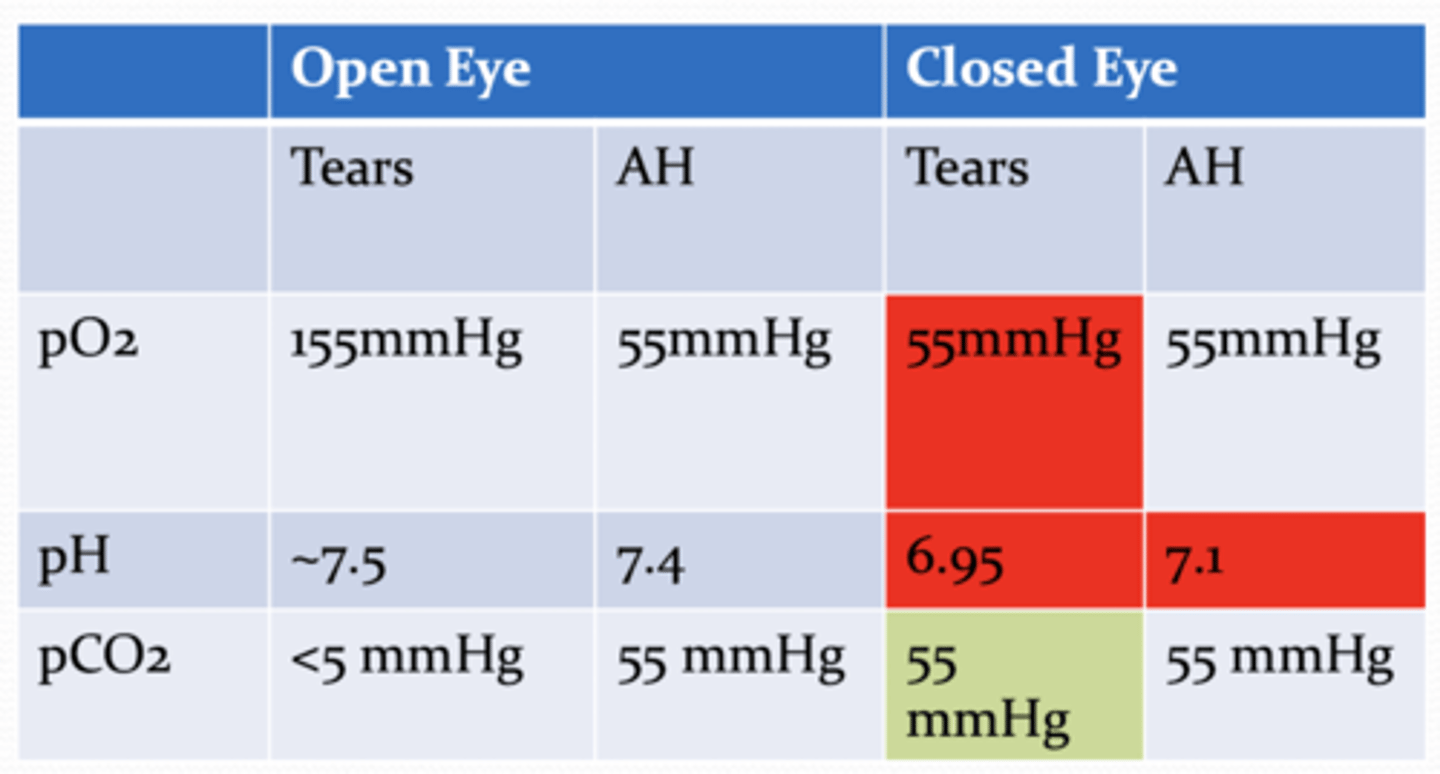
What happens to the pH of the tears and aqueous humor when the palpebrae are closed?
decreases (H+ increases)
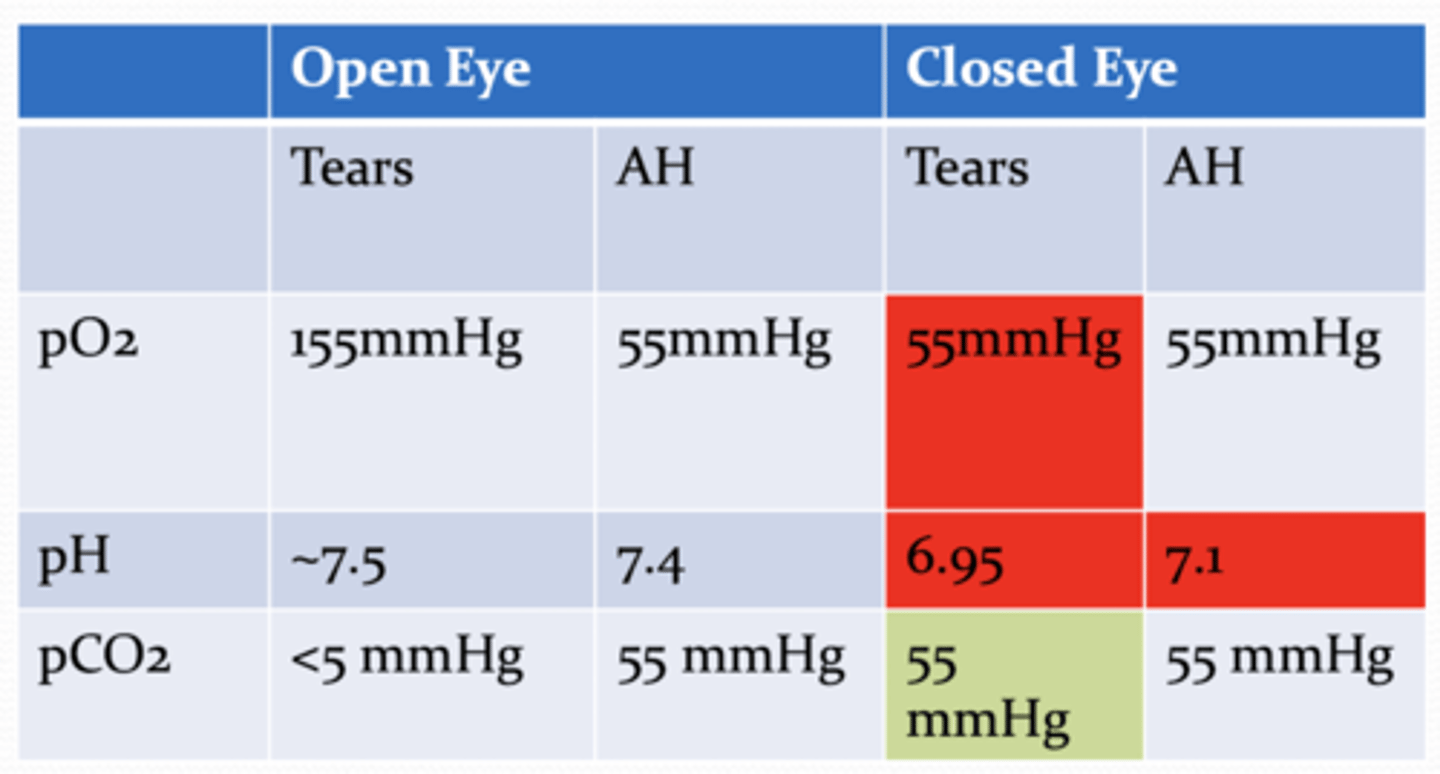
How is endothelium pump function affected by the pH of the cornea?
reduction in pump function
How is the cornea affected by altitude?
decrease in atmospheric pO2 --> increases anaerobic metabolism --> lactate causes edema
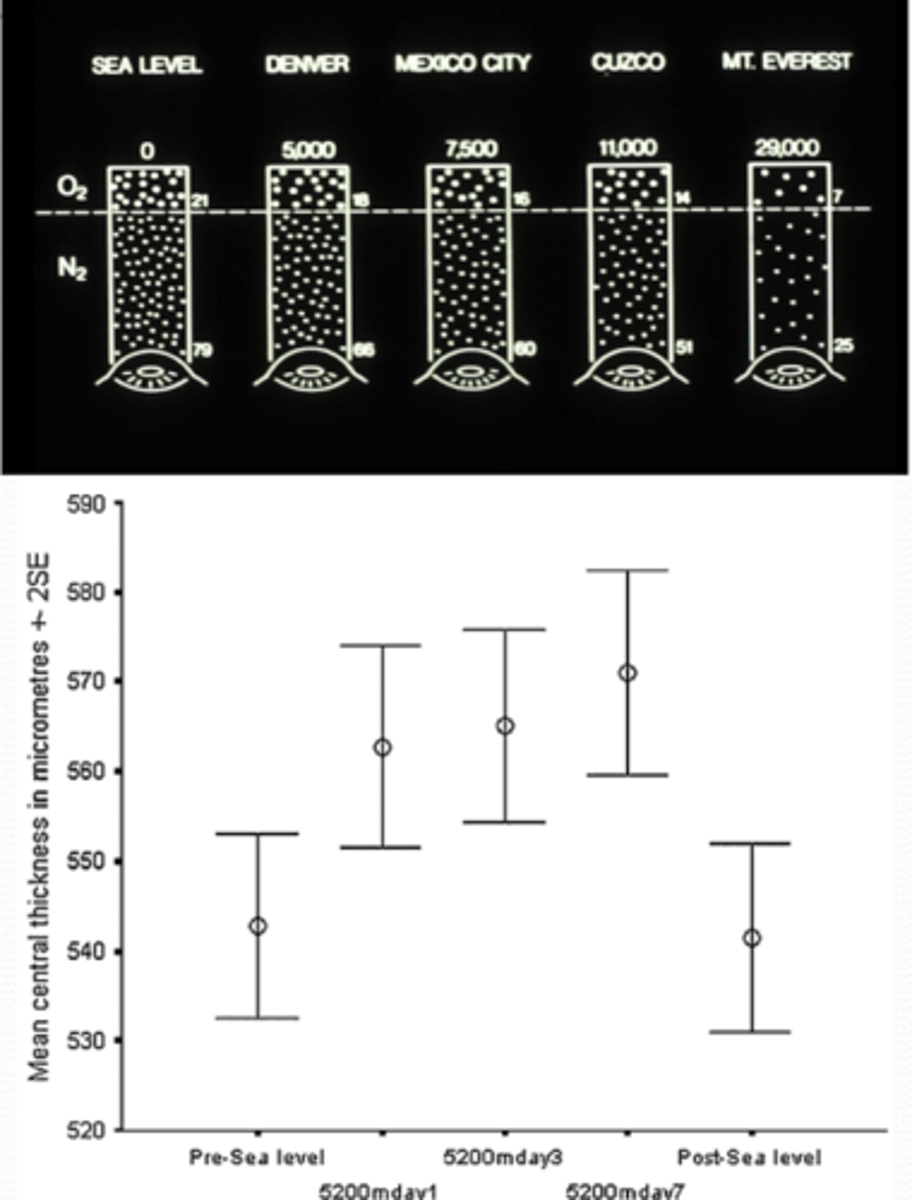
How do contact lens affect the metabolism of the cornea?
decreases pO2 throughout the cornea causing an increase in anaerobic metabolism
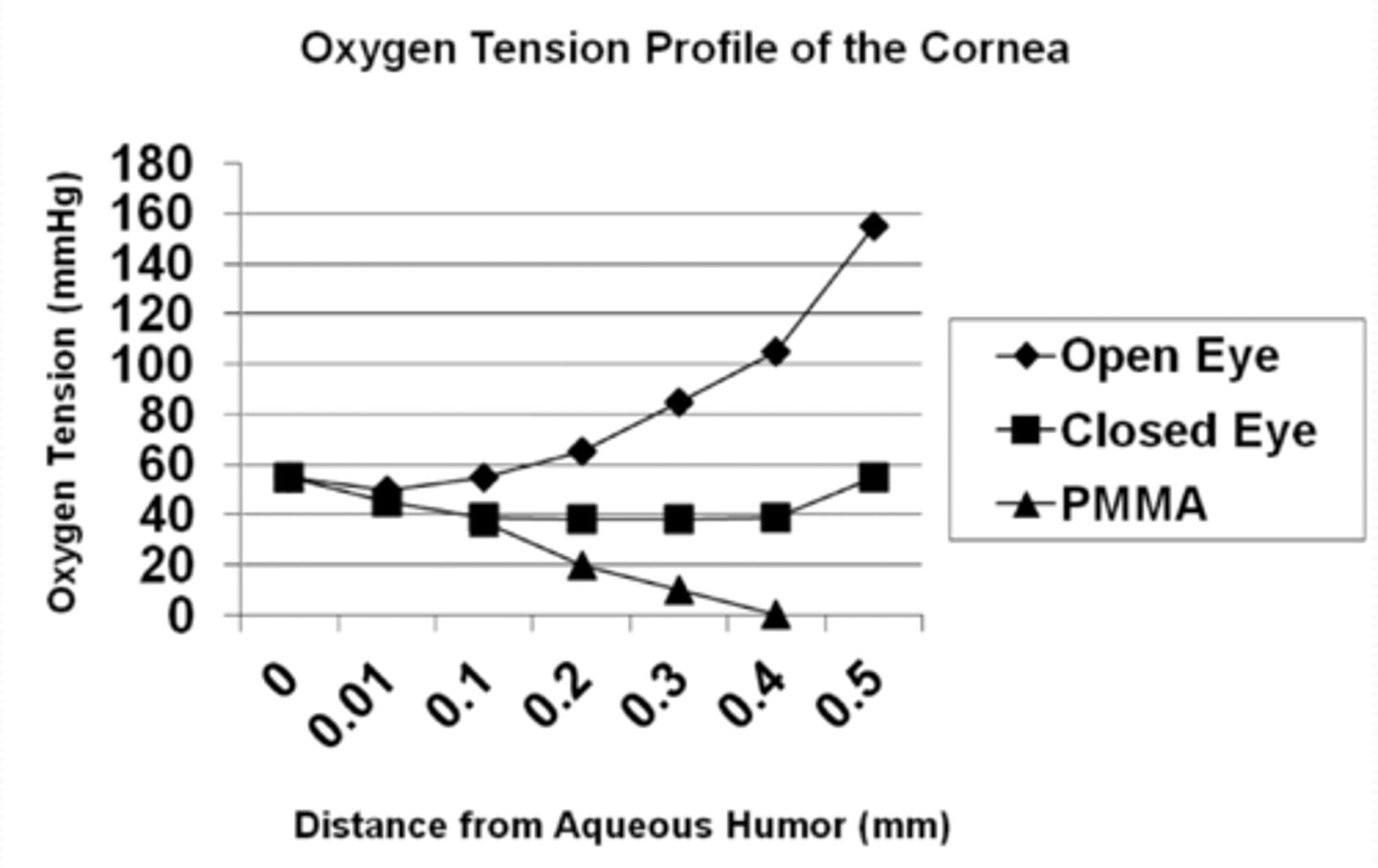
What is the standard minimum O2 exposure to prevent physiological changes?
74 mmHg
How does contact use affect the amount of carbon dioxide in the aqueous humor?
anaerobic respiration --> increased CO2 --> increased CO2 efflux to the aqueous humor
What does deturgescence mean?
relative dehydration of corneal tissue
What are epithelial microcysts?
early signs of epithelial hypoxia (via cls) -- 2-3 months to occur
How does contact lens wear affect epithelial proliferation?
decreases metabolic precursors --> decreases epithelial mitosis and migration
What are corneal stromal striae?
folds in the corneal stroma
What causes corneal stromal striae?
differential swelling of the posterior versus the anterior stroma
What are endothelial blebs?
dark spots -- blebs constitute an immediate index of hypoxia

What causes endothelial blebs?
acute hypoxia

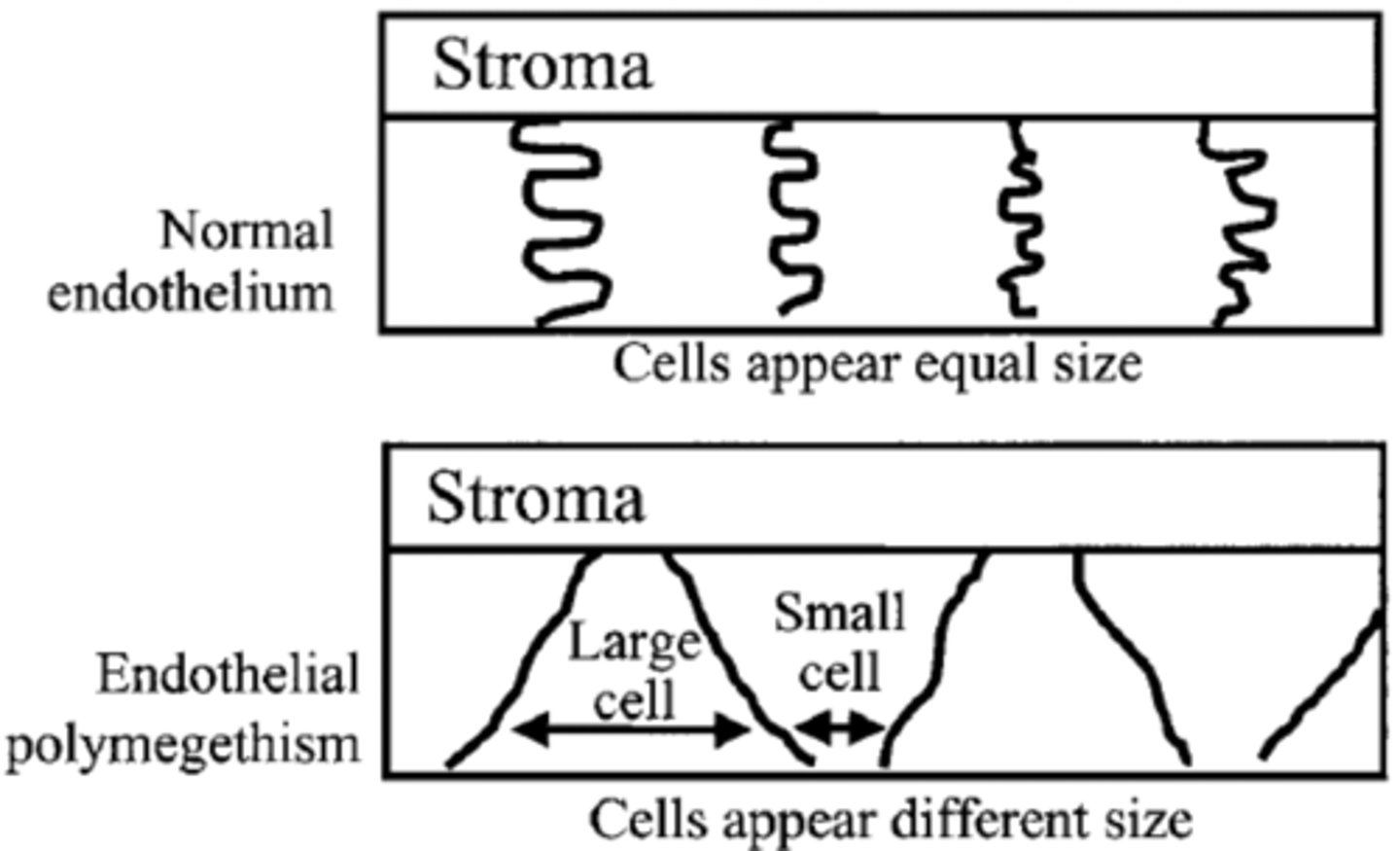
What is corneal endothelial polymegethism?
growth of endothelium (non-uniformity of cell size/shape

What causes corneal endothelial polymegethism?
long periods of contact lens use (hypoxia)
Why would an optometrist prescribe anti-VEGF antibodies?
regression of corneal neovascularization
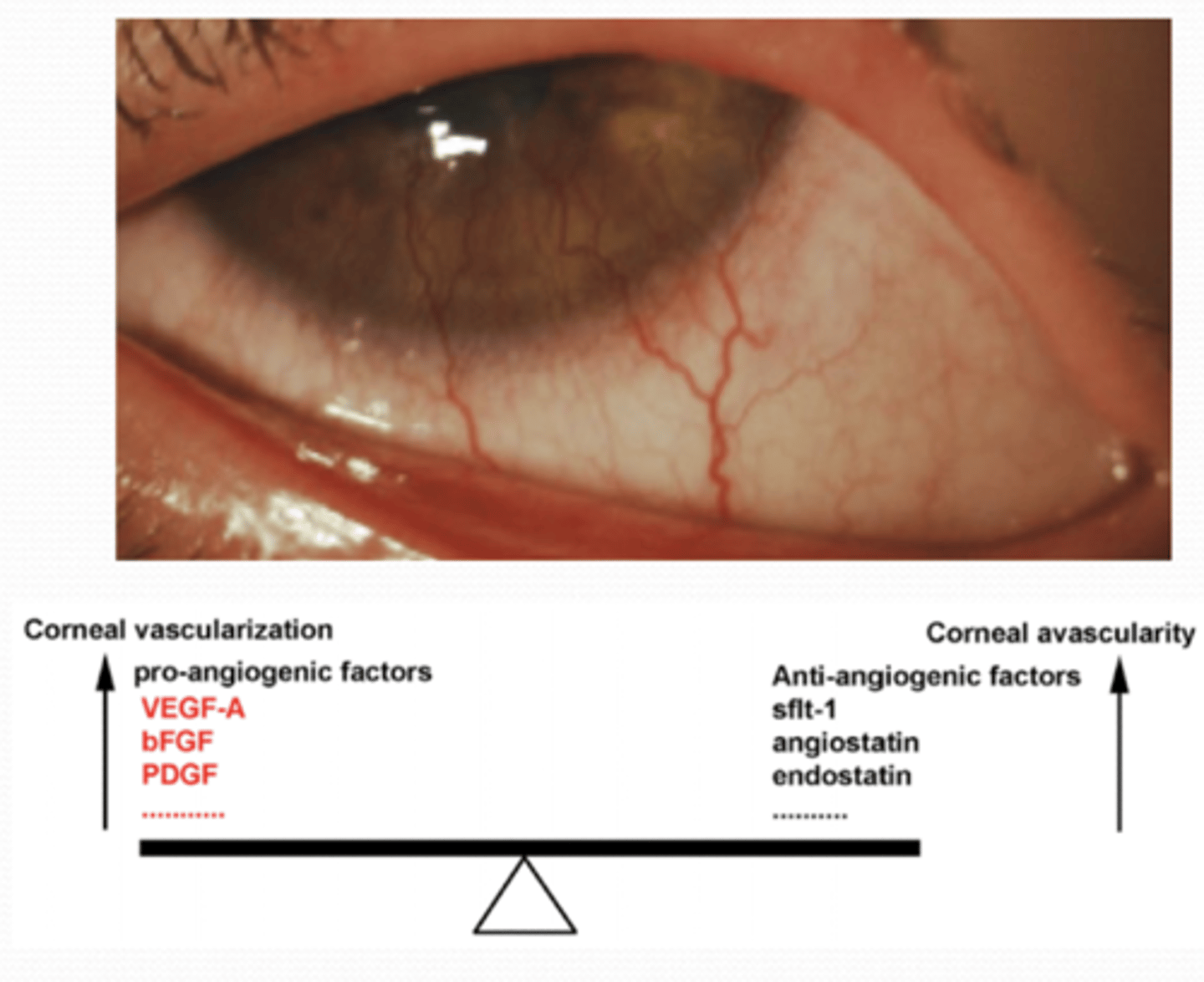
What medications would regress corneal neovascularization?
1. monoclonal anti-VEGF antibodies (Ranibizumab/Lucentis® and Bevacizumab/Avastin®)
2. corticosteroids/NSAIDs
What reaction produces two pyruvate?
glycolysis
What percentage of the cornea is water?
78% water
What are the functions of aqueous humor?
1. provides nutrients to ocular tissues
2. maintains corneal curvature
3. transmits light
4. absorbs UV light
5. transports waste products away
What tissue secretes aqueous humor?
ciliary epithelium lining the ciliary processes -- vasculature is fenestrated
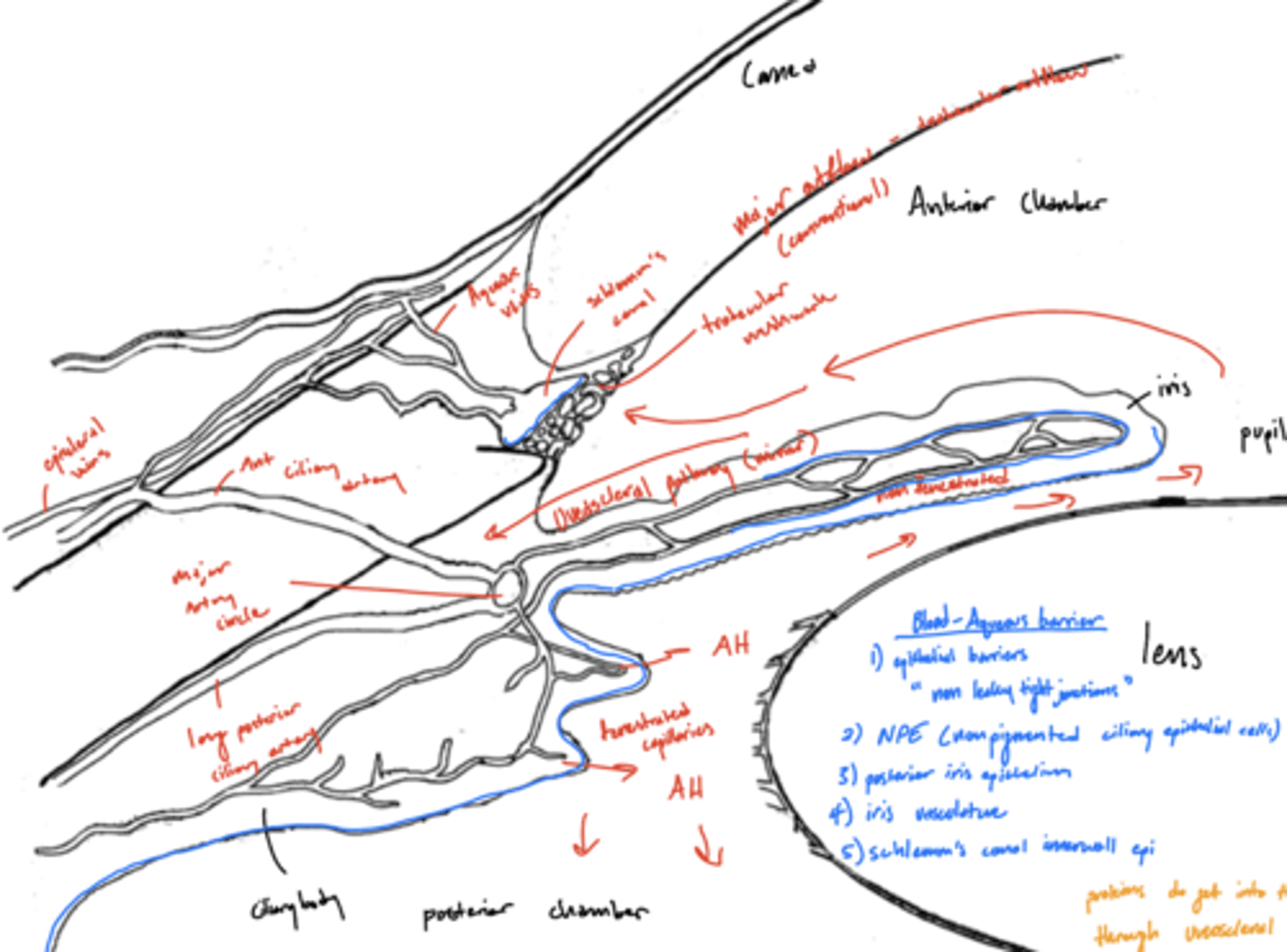
What participates in the blood-aqueous barrier?
non-leaky tight junctions
1. non-pigmented epithelium of the ciliary body
2. posterior iris epithelium
3. non-fenestrated blood vessels of the iris
4. inner wall of Schlemm's canal
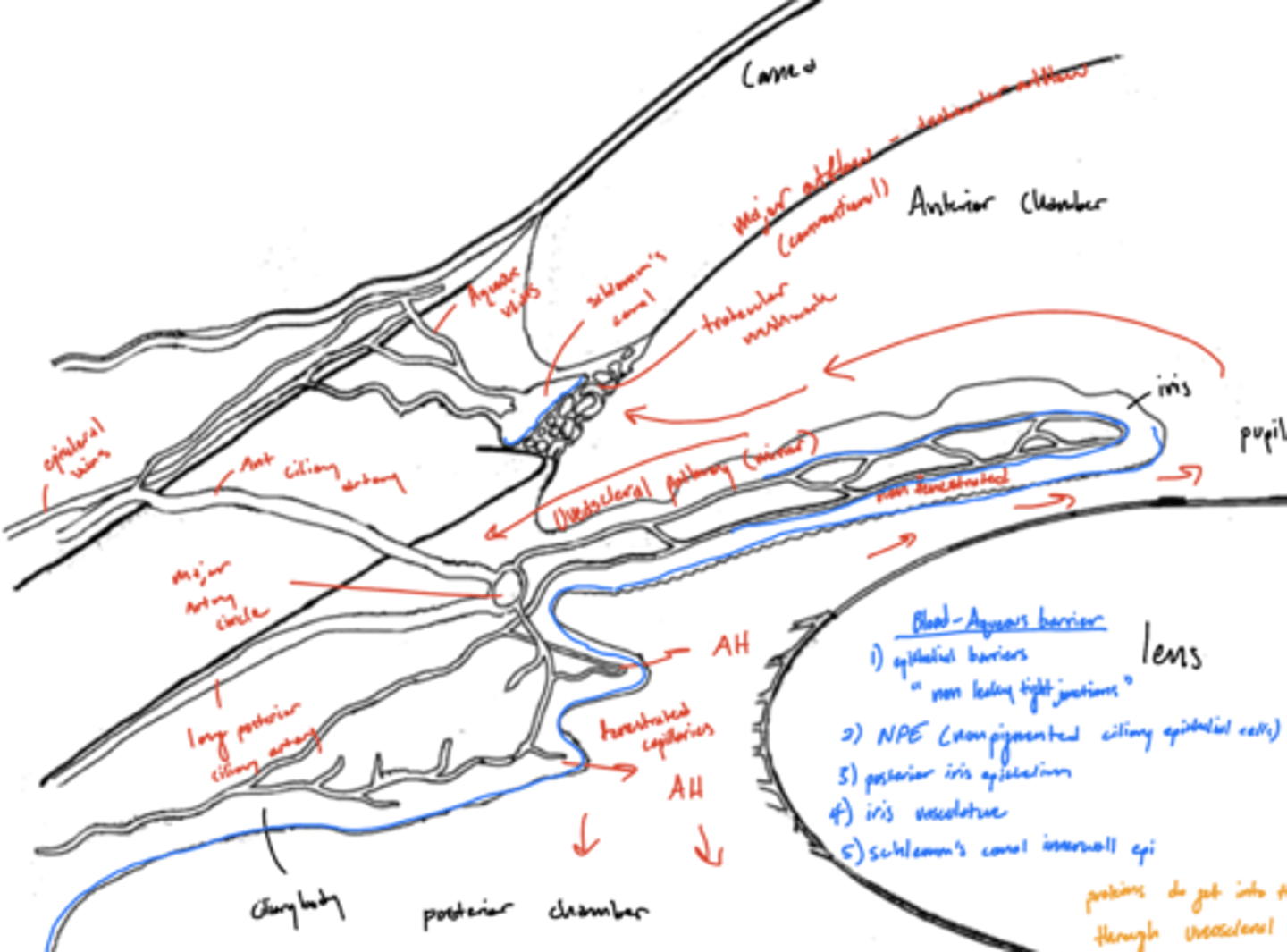
How does aqueous humor travel to the anterior chamber?
1. around lens and through the pupil to anterior chamber
2. diffuse from ciliary body stroma, to the root of the iris, accumulates in the iris stroma and is then released into the AH
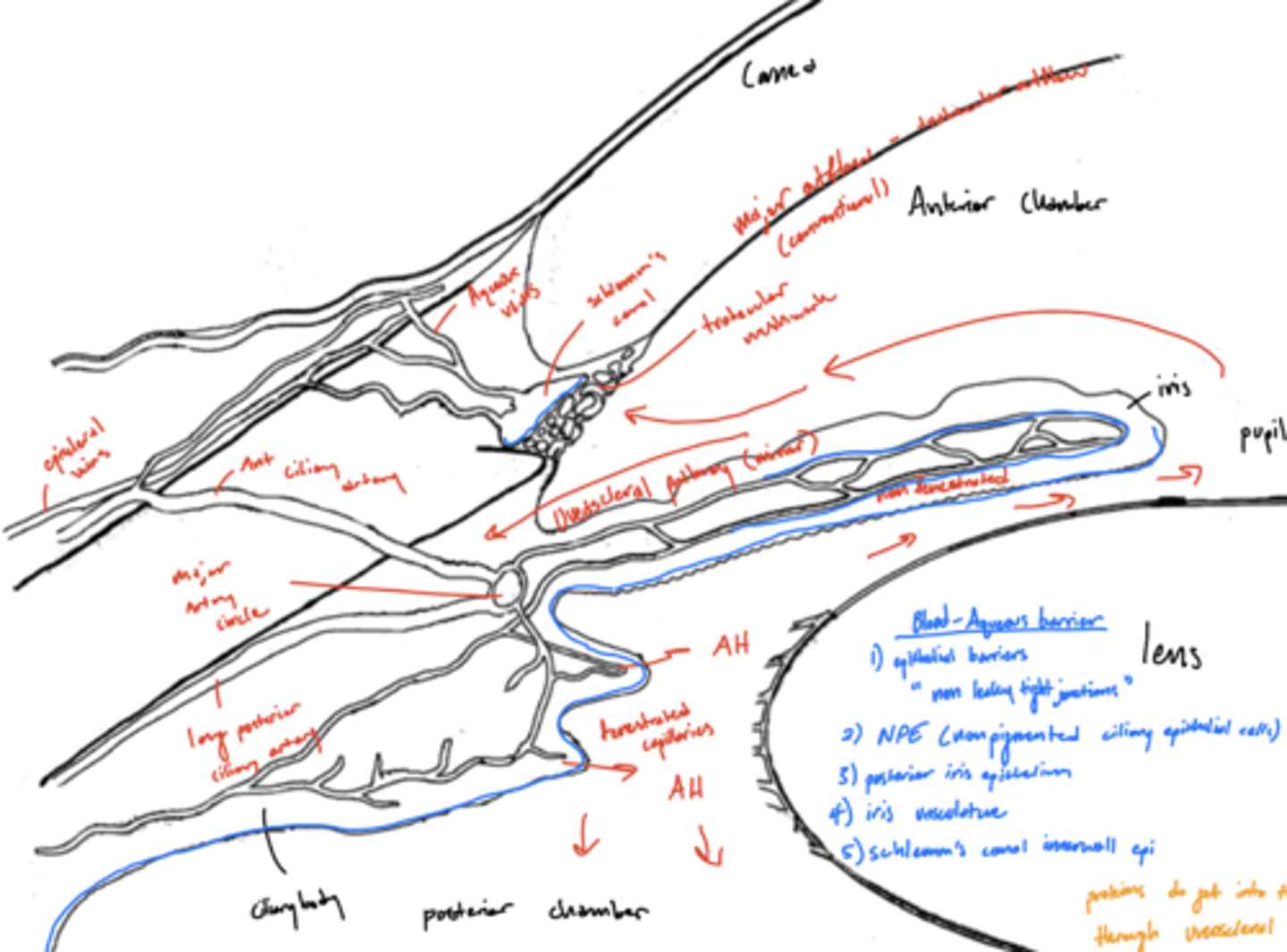
What drives aqueous to the anterior chamber?
convection (temperature) currents differences
why? -- AH is warmer near iris (vasculature), warmer AH is less dense and its buoyancy causes it to rise
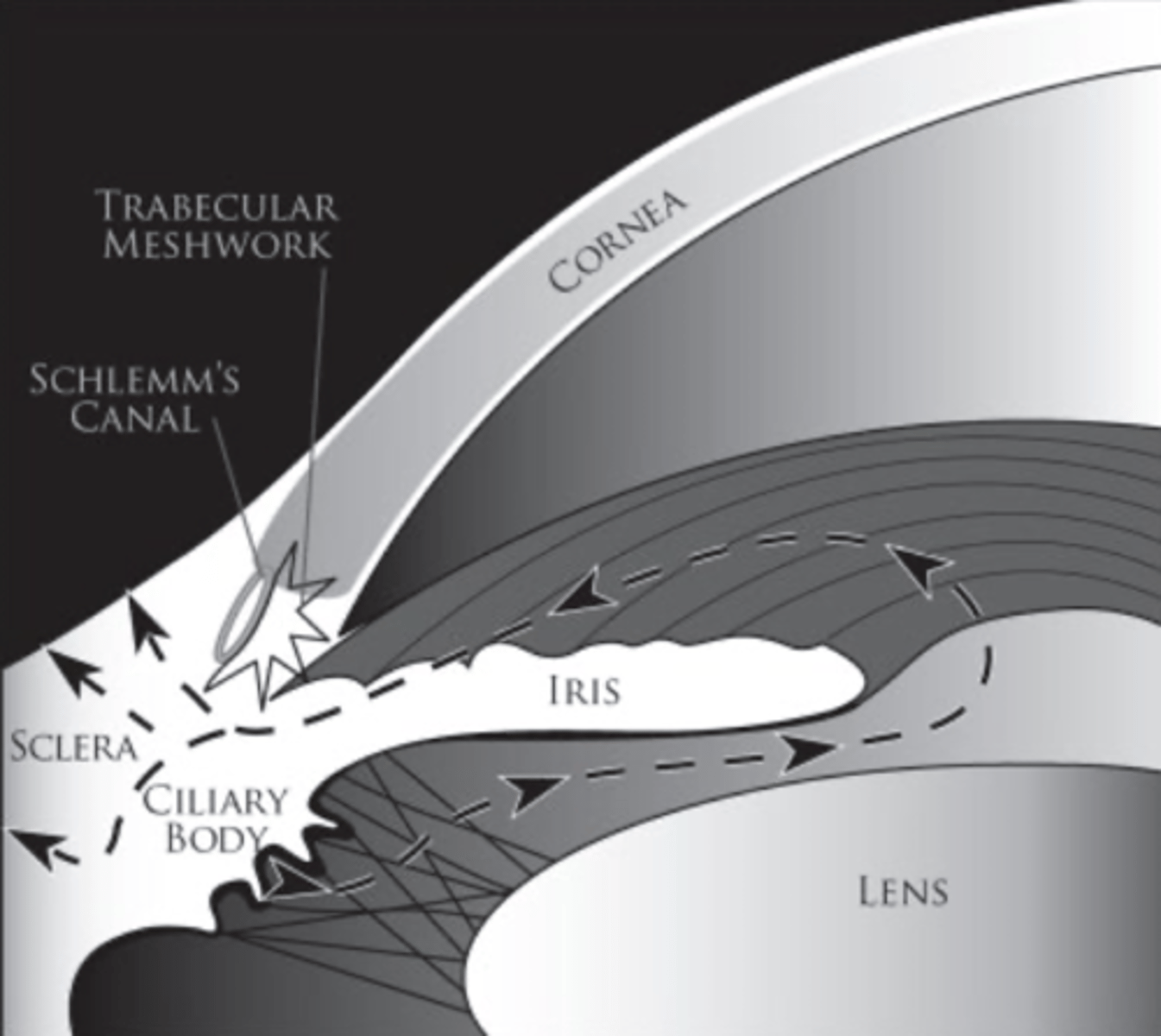
What are the pathways of aqueous drainage?
1. trabecular meshwork, across inner wall of Schlemm's canal... -- conventional route
2. across iris root, uveal meshwork -- unconventional route (or uveal scleral)
What is the conventional route of aqueous drainage?
1. trabecular meshwork
2. across inner wall of Schlemm's canal into its lumen
3. collector canals
4. deep scleral/intrascleral/episcleral plexus
4. episcleral vein
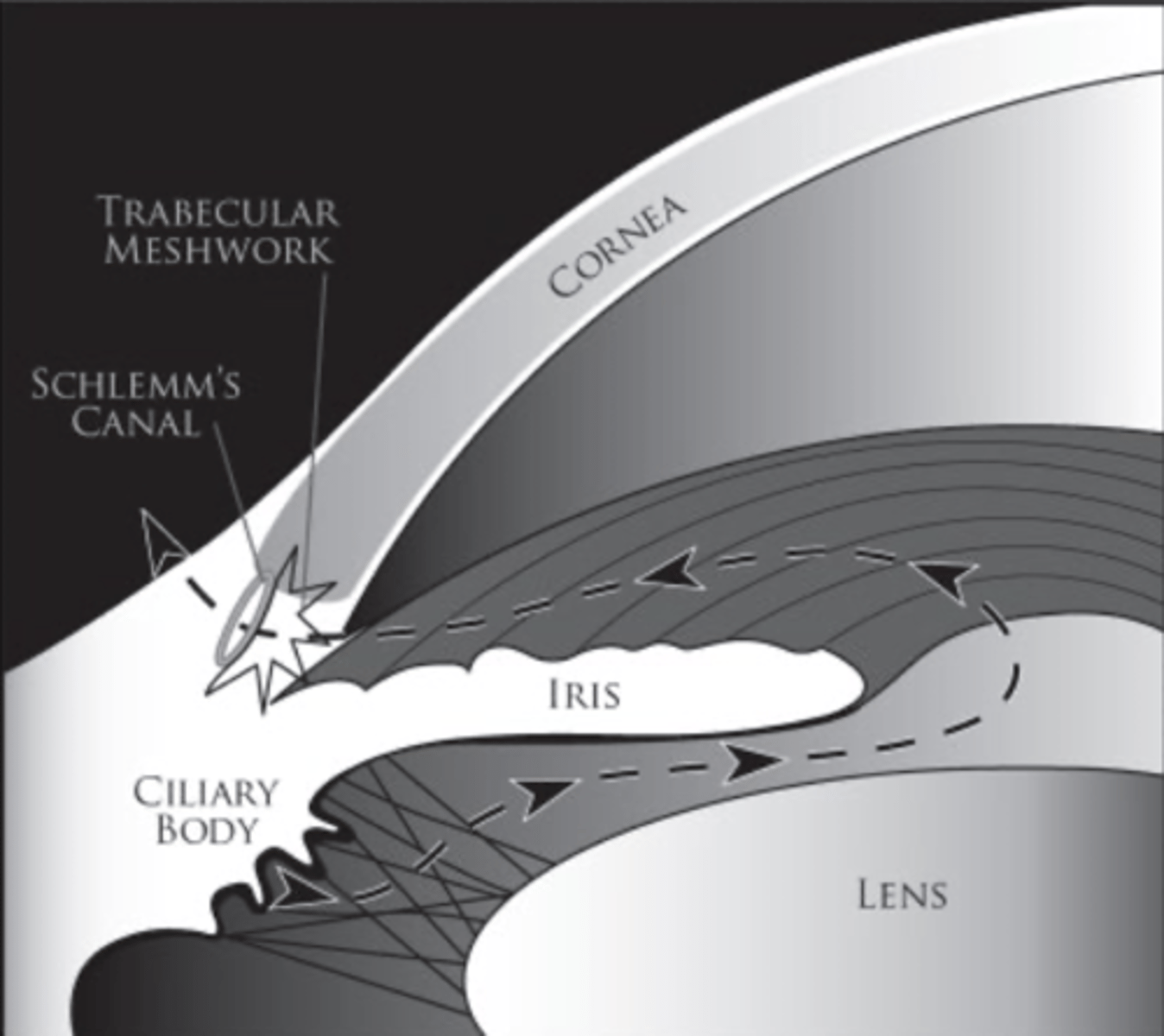
What percentage of aqueous humor is drained via the conventional route?
45-65% majority
What is the unconventional route of aqueous drainage?
1. iris root
2. uveal meshwork
3. anterior face of ciliary muscle
4. connective tissue between muscle bundles
5. suprachoroidal space
6. sclera
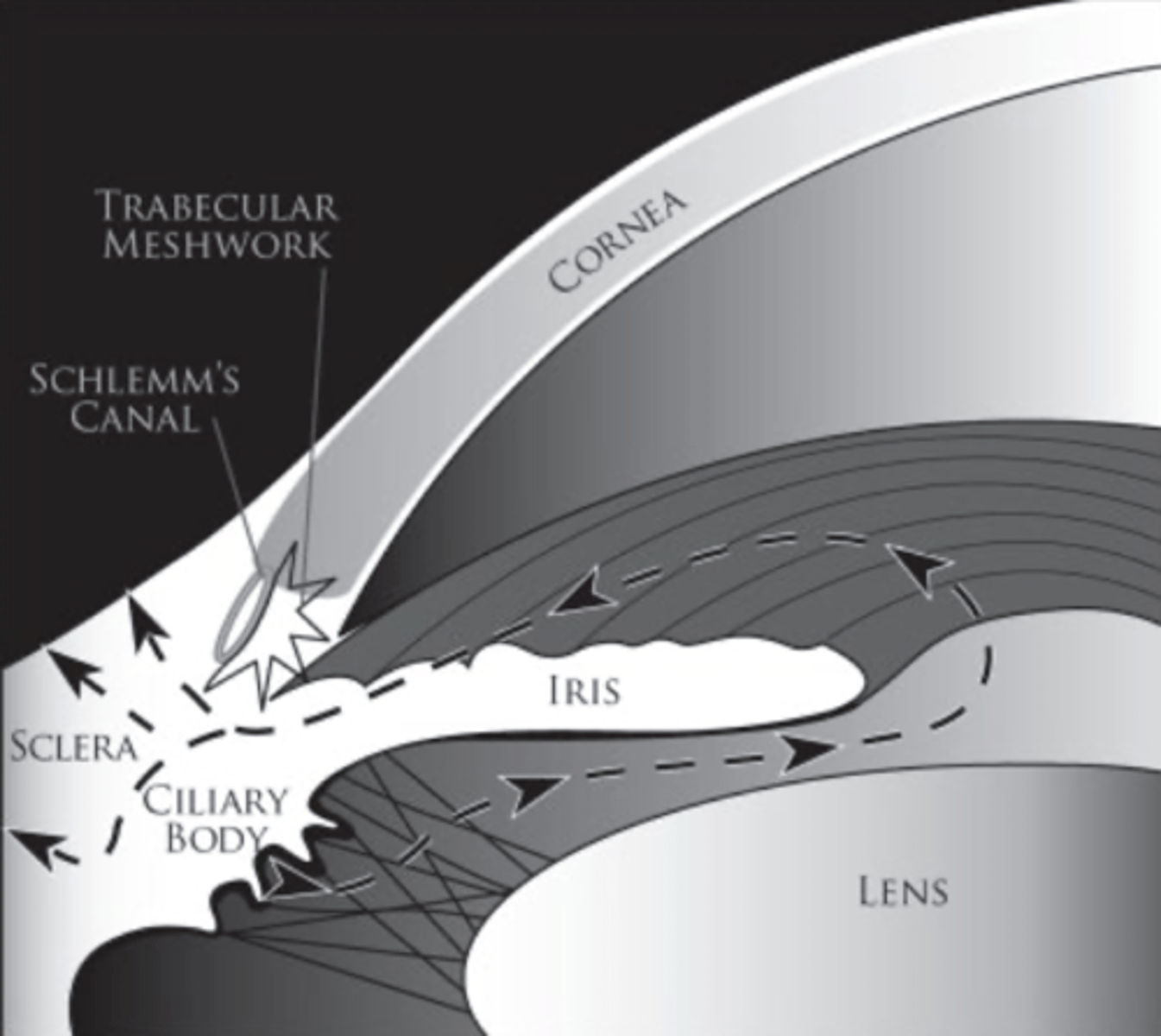
What percentage of aqueous humor is drained via the unconventional (uveal scleral) route?
35-55% minority
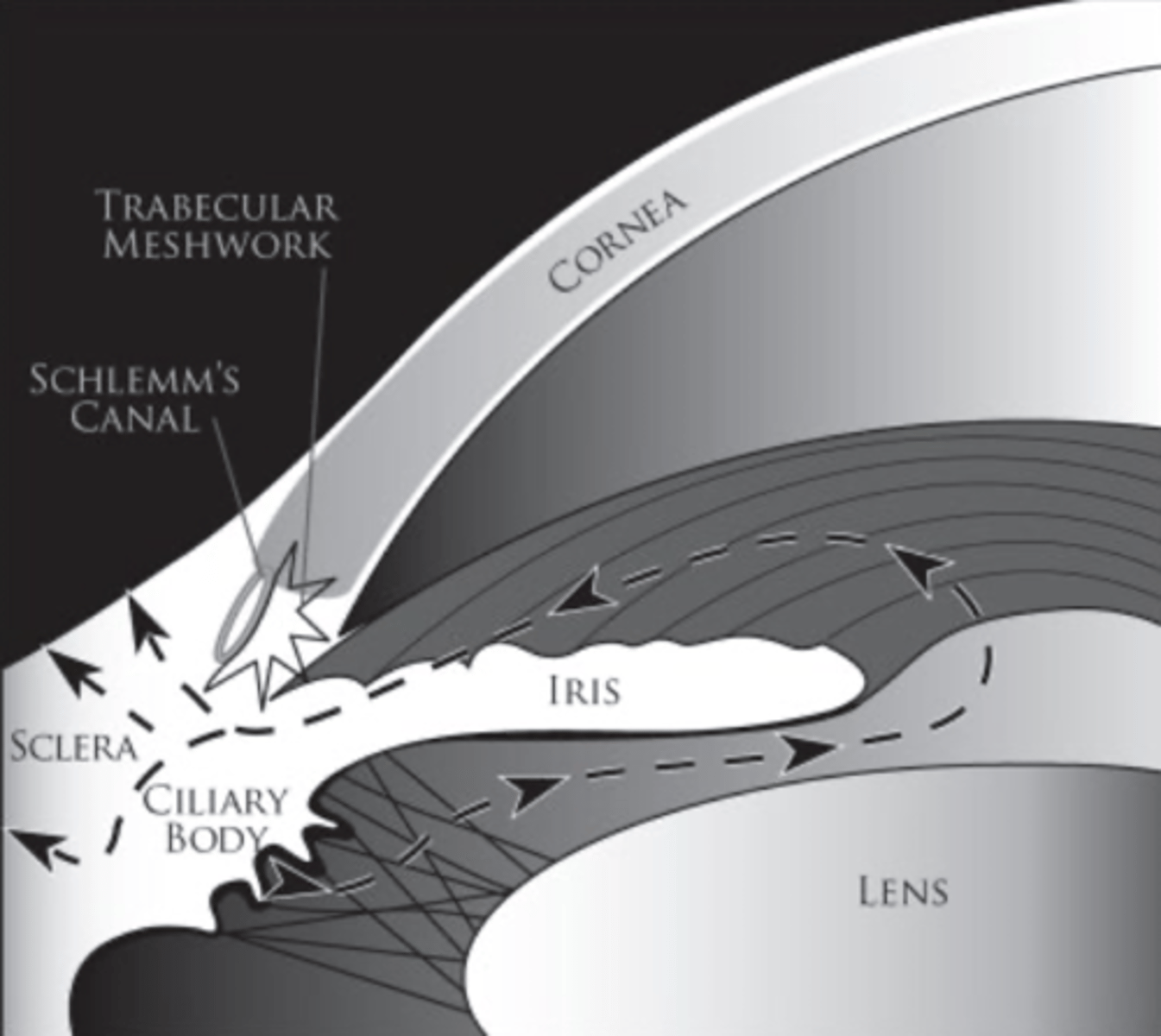
As we age, what happens to aqueous humor drainage via the unconventional (uveal scleral)?
decreases with age
Why is there a blood aqueous barrier?
enables AH to have composition different from the protein filtrate of plasma
Where is protein content the highest in the aqueous humor?
higher peripherally near trabecular meshwork than centrally
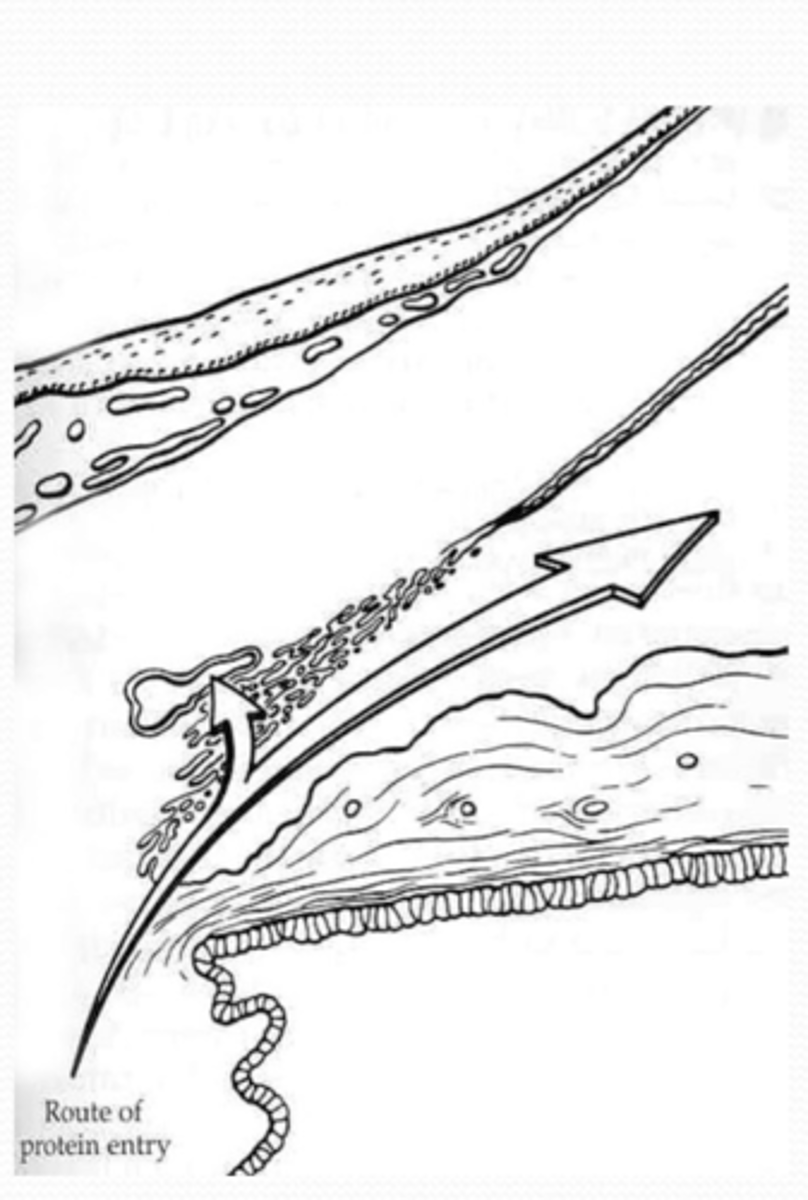
How does protein content differ from aqueous humor and blood?
blood > aqueous humor
What types of proteins are found in the aqueous humor?
1. albumin
2. fibrinolytic and pro-coagulation proteins
3. growth factors and cytokines
4. complement proteins
5. myocilin
What protein is associated with glaucoma?
myocilin
also an extracellular matrix homeostasis
What is the tyndall effect?
scattering of light by colloidal particles within the aqueous humor
What does the tyndall effect tell you?
sign of uveitis -- breakdown of blood aqueous barrier
What is uveitis?
break down of in blood-aqueous barrier -- inflammation of uvea due to ocular tissue damage, pathogens, or toxins
What anatomical structures are within the uvea?
1. iris
2. ciliary body
3. choroid
What are the types of uveitis?
1. anterior uveitis
2. intermediate uveitis
3. posterior uveitis
4. pan uveitis
What does anterior uveitis affect?
1. ciliary body
2. iris
What does intermediate uveitis affect?
1. vitreous
2. peripheral retina
What does posterior uveitis affect?
1. choroid
2. retina
What are the etiologic categories of uveitis?
1. non-infectious
2. infectious
What causes non-infectious uveitis?
idiopathic (many) -- associated with immunological diseases
What causes infectious uveitis?
1. viral infection (HSV, VZV, CMV)
2. microbial (syphilis, lyme disease, mycobacteria)
What is the role of TNF-alpha?
cytokine produced by macrophages for initiating immunity to pathogens, but too high instigates high levels of inflammation, cell death, and tissue degeneration
What produces TNF-alpha?
macrophages
Where are TNF-alpha receptors located?
uveal pigmented cells
What patients have elevated levels of TNF-alpha?
uveitis (inflammation)
How does uveitis break down the blood-aqueous barrier?
disruption of ocular epithelial tight junctions via:
1. reduction of TJ protein/mRNA expression
2. modification of TJ protein
3. enzymatic cleavage of TJ proteins
Why would uveitis break down the blood-aqueous barrier?
loss of TJ's allows access of more immune cells to propagate inflammation pathways
What tight junction proteins are broken down as a part of uveitis?
1. claudin
2. ZO-1/2
3. JAM-1
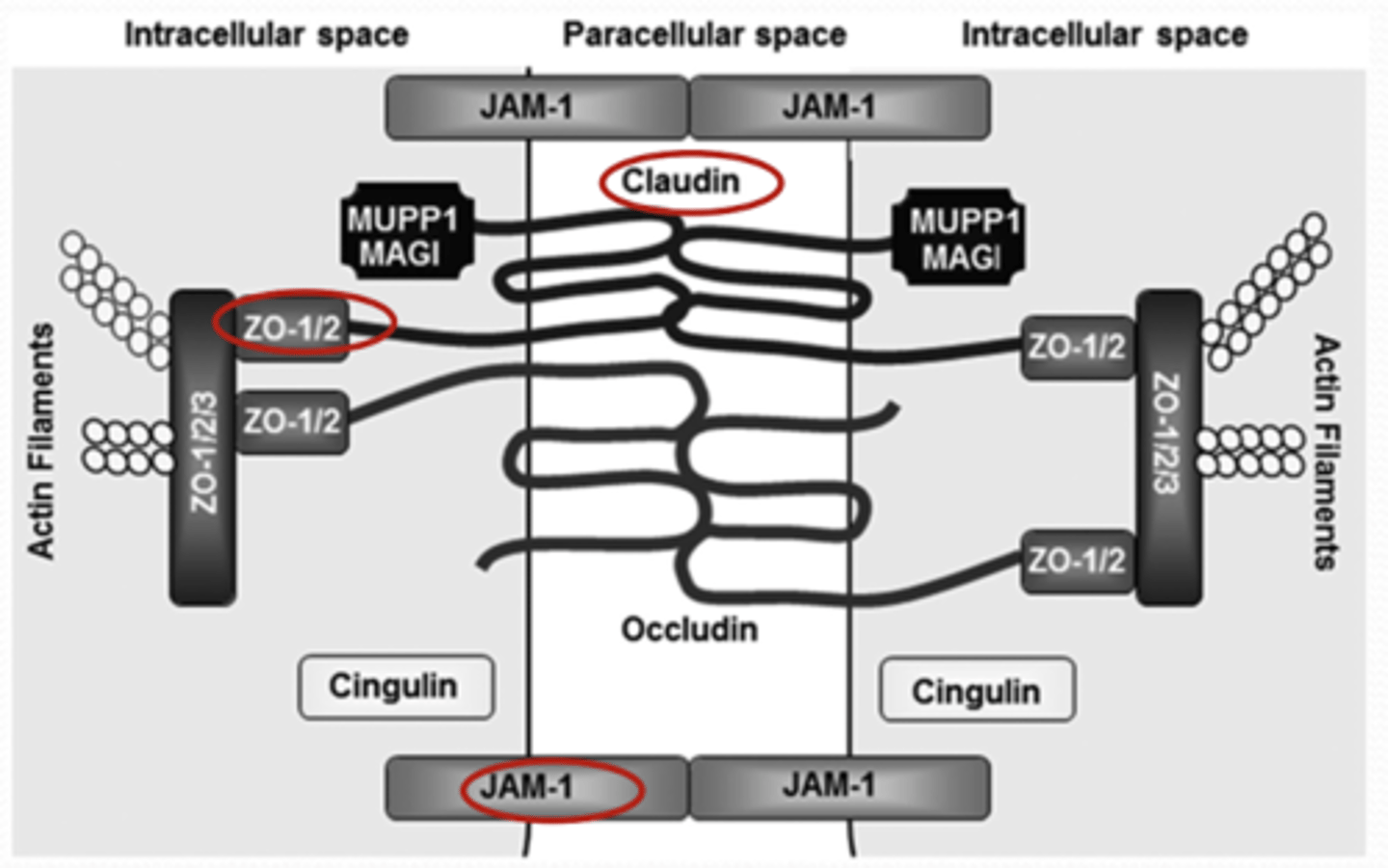
What drugs treat uveitis?
1. anti-TNF drugs
2. corticosteroids
turn off inflammation!
What are anti-TNF drugs?
antibodies designed to prevent TNF from binding to receptors on ocular cells -- prevent signaling pathway
What is ocular immune privilege?
ability to tolerate foreign antigens without instigating an inflammatory immune response -- no rejection reaction (implant)
Why is the eye immune privilege?
1. disrupts vision
2. ocular tissues cannot regenerate and need to be protected from inflammatory pathways (corneal endothelium & retinal neurons)
Why is the eye immunological ignorant?
1. blood-aqueous barrier
2. absence of lymphatic drainage pathways
3. lack of MHC class II, reduced MHC class I
Are resident corneal dendritic cells mature or immature?
both -- depends on presence of MHC II proteins
Where are the majority of immature corneal dendritic cells located?
centrally > peripherally
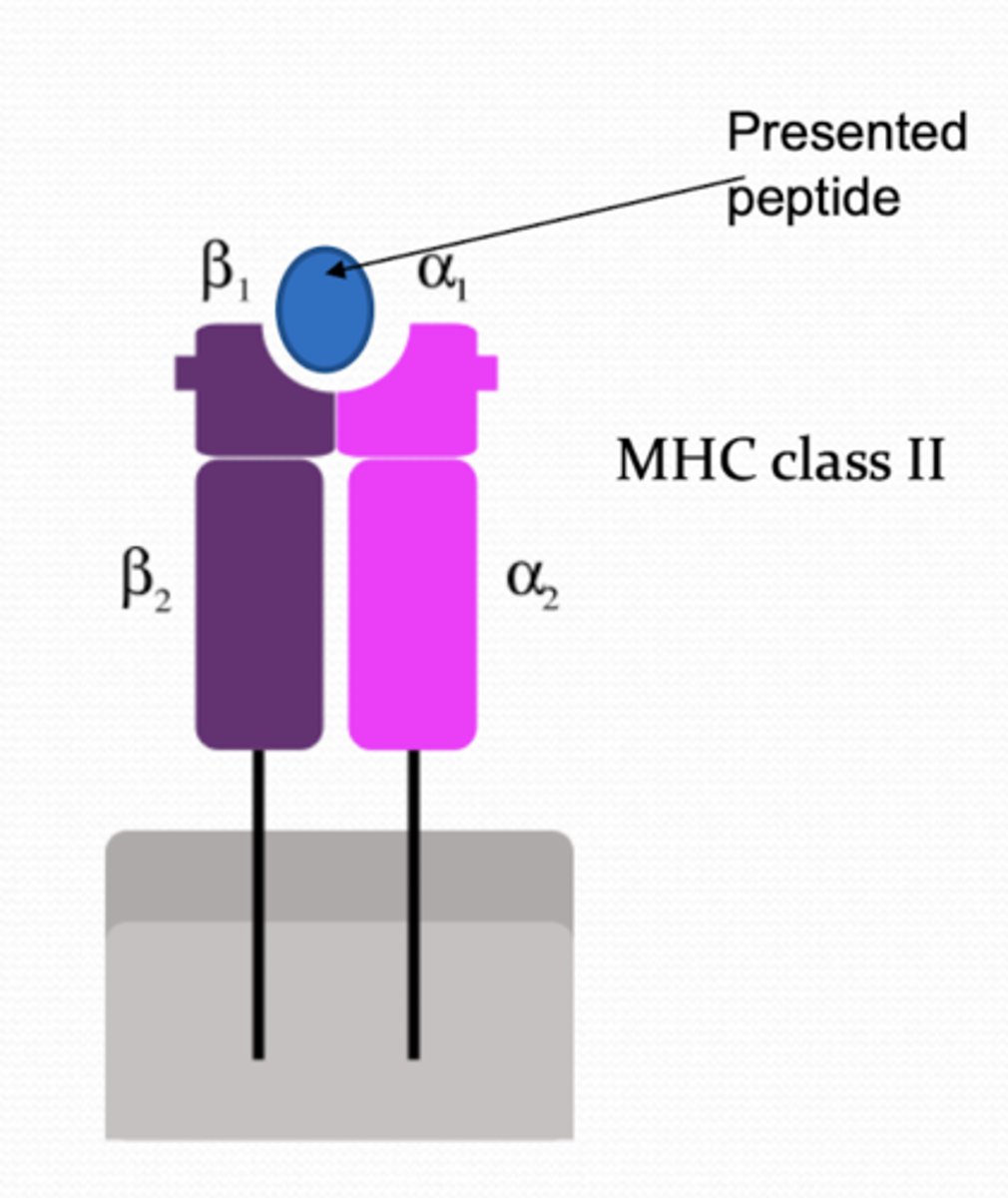
How do corneal dendritic cells present antigens?
1. antigen proteins are endocytosed by DCs
2. combined with MHC II molecules inside cells
3. moved to the cell surface (antigen presentation)
What is peripheral tolerance of eye-derived antigens?
anterior chamber APCs inhibit systemic immune response in spleen
also called ACAID "Anterior-Chamber Associated Immune Deviation"
why eye infections aren't usually accompanied by systemic effects
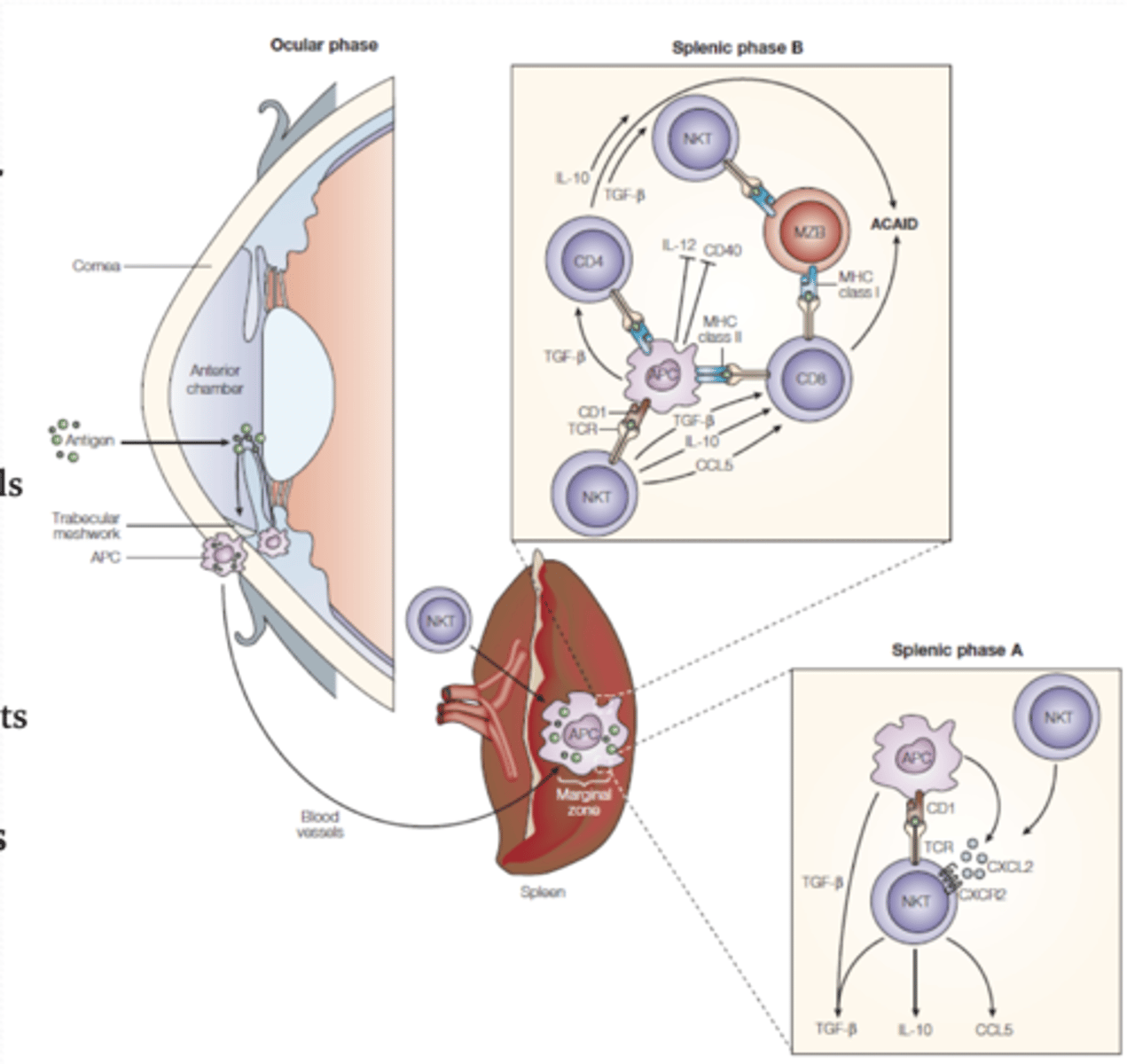
What is anterior-chamber-associated immune deviation (ACAID)?
anterior chamber APCs inhibit systemic immune response
also called peripheral tolerance of eye-derived antigens
why eye infections aren't usually accompanied by systemic effects
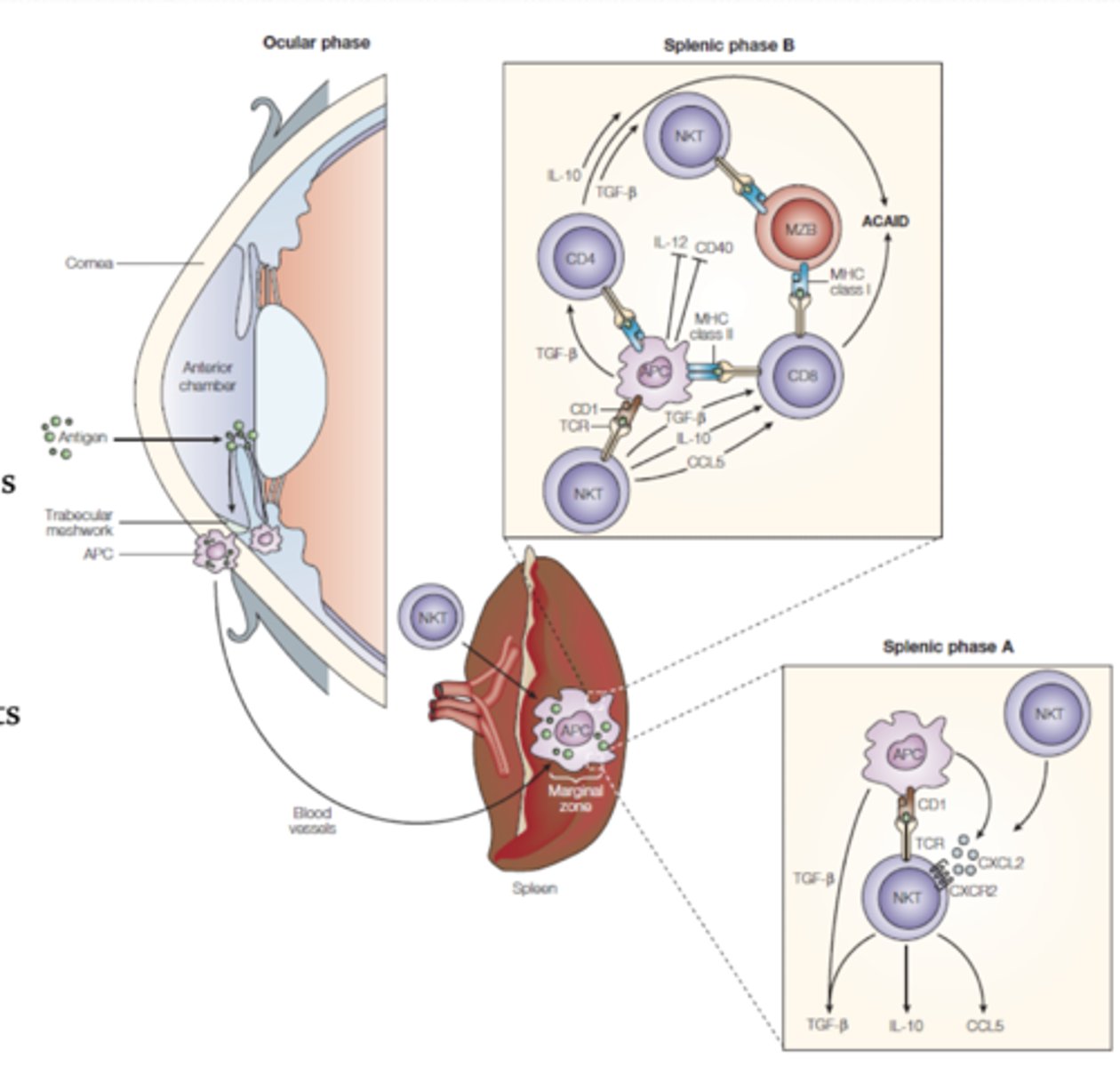
Where do anterior chamber APCs exit the eye?
trabecular meshwork, through blood to the spleen/thymus
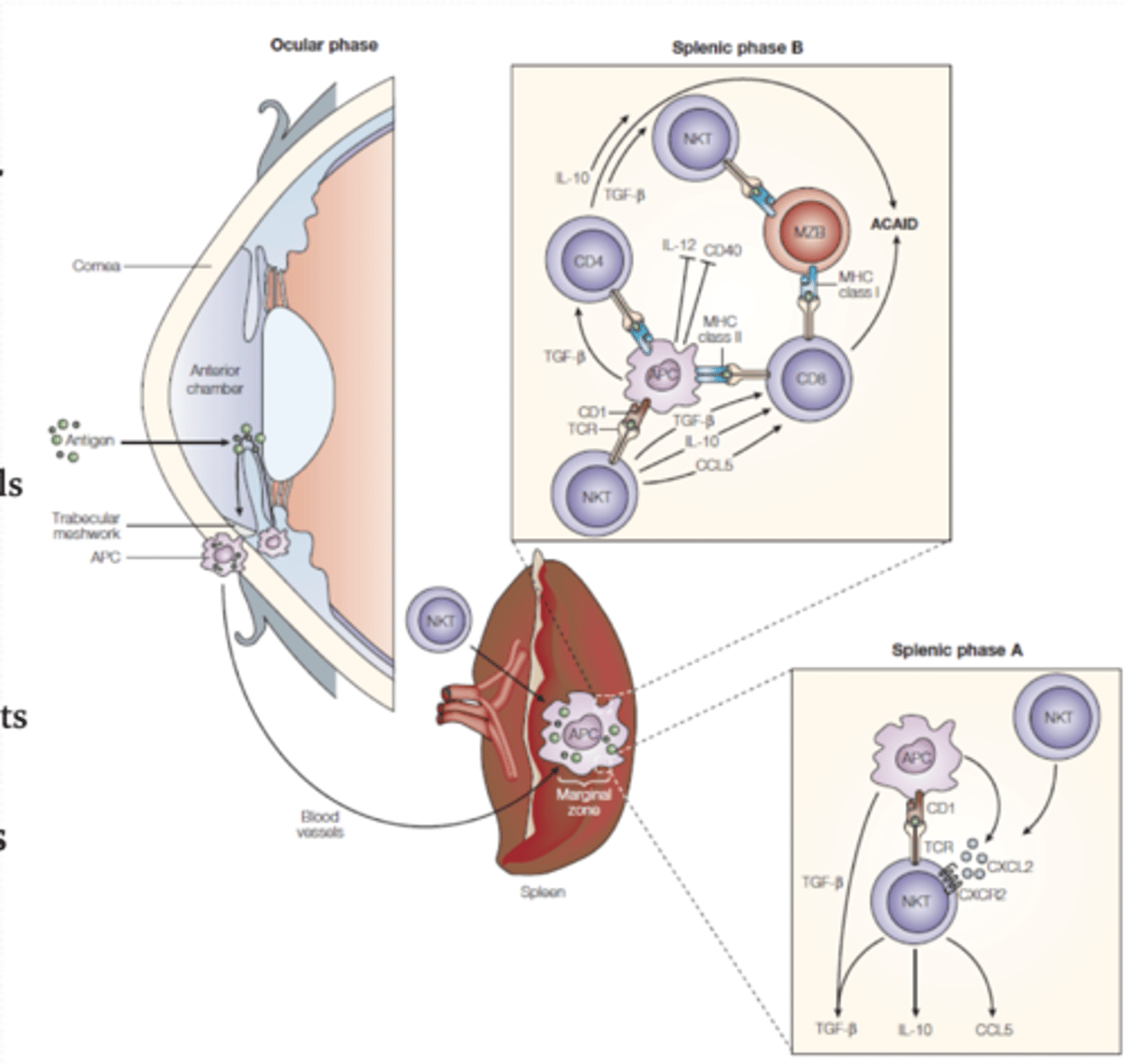
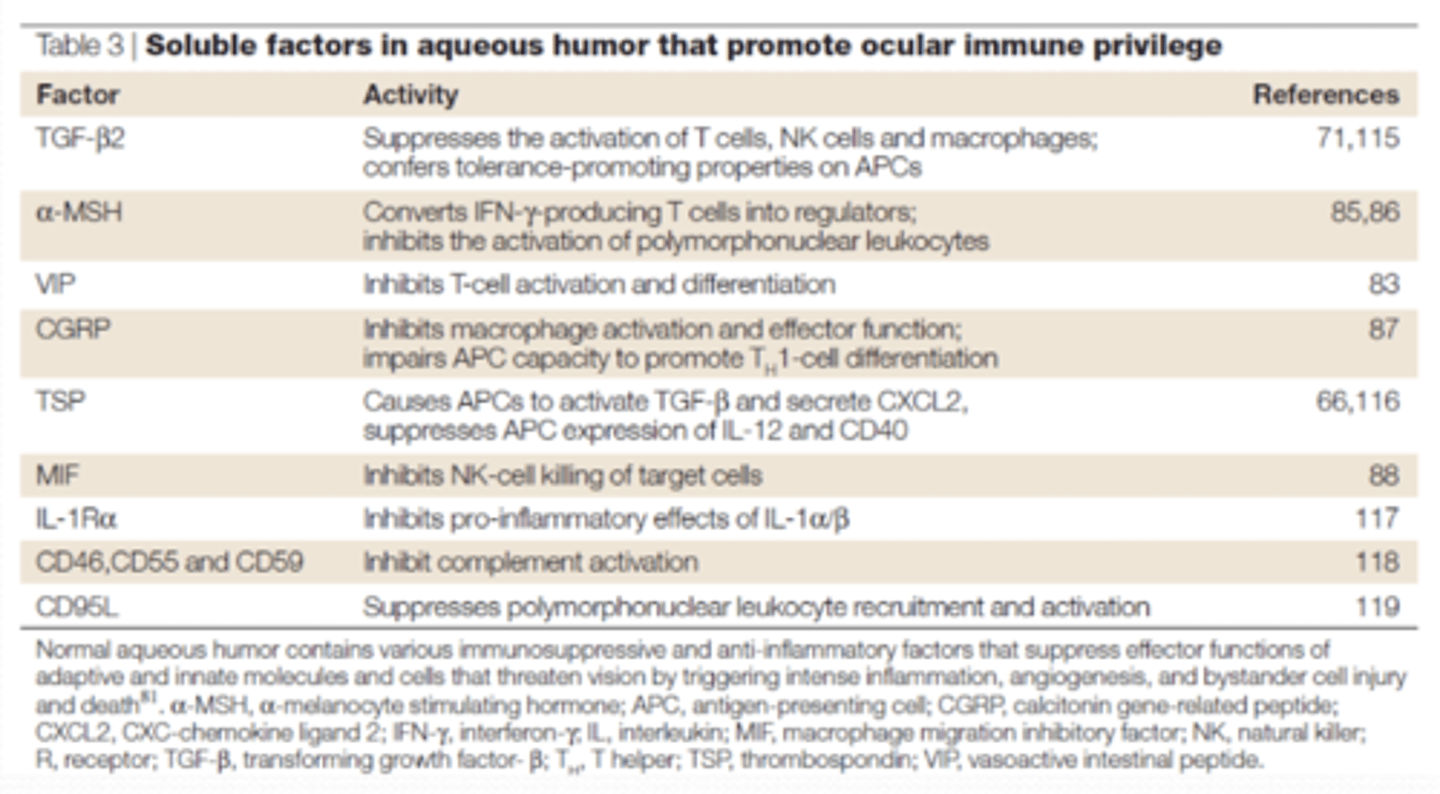
What is the intraocular immunosuppressive microenvironment?
soluble factors (neuropeptides, cytokines, growth factors) inhibit various immunological functions
TGF-beta2
What is the function of TGF-beta-2?
suppresses the activation of T cells, NK cells, and macrophages
What does the ciliary body epithelium (both layers) develop from?
ectoderm
why? -- similar as RPE
What does the ciliary muscle develop from?
ectoderm
What does iris dilator and sphincter muscle develop from?
ectoderm
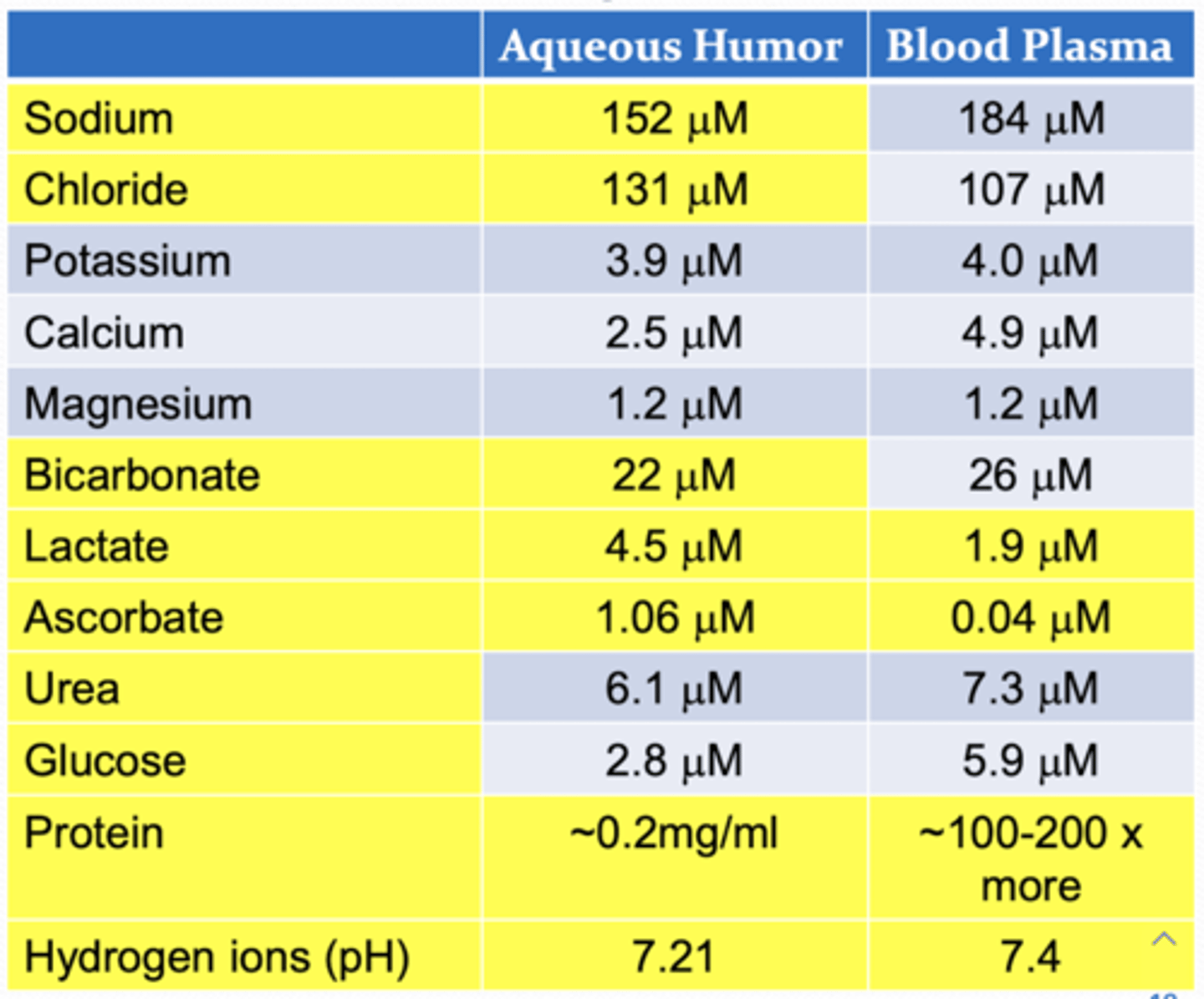
Compared to blood, what molecules have a greater concentration in the aqueous humor?
1. ascorbic acid/ascorbate
2. lactate
What would be the advantage to having ascorbic acid/ascorbate in the aqueous humor?
absorbs UV light (specifically UV-B and UV-A)
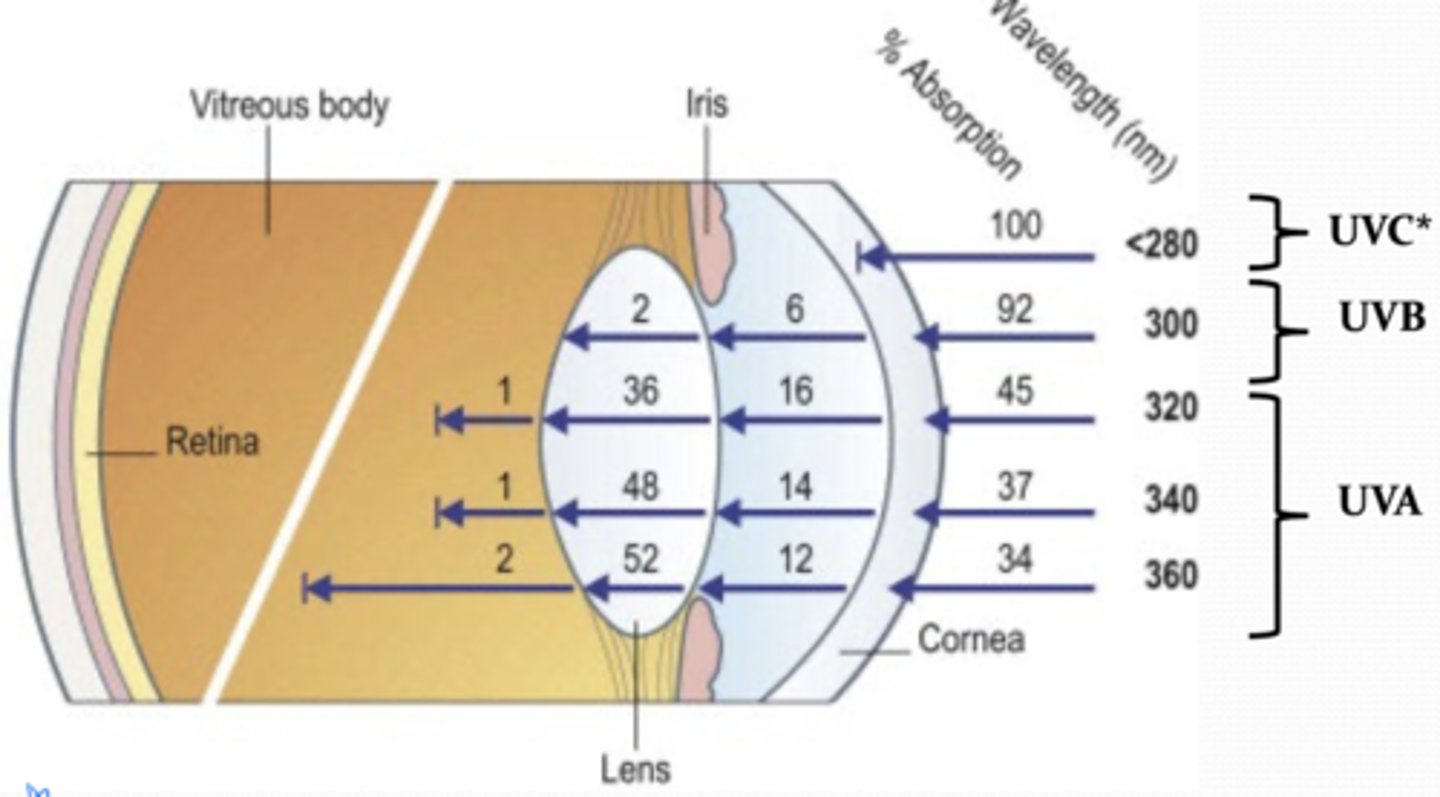
What are the major ions of the aqueous humor?
1. sodium
2. chloride
3. bicarbonate
4. lactate
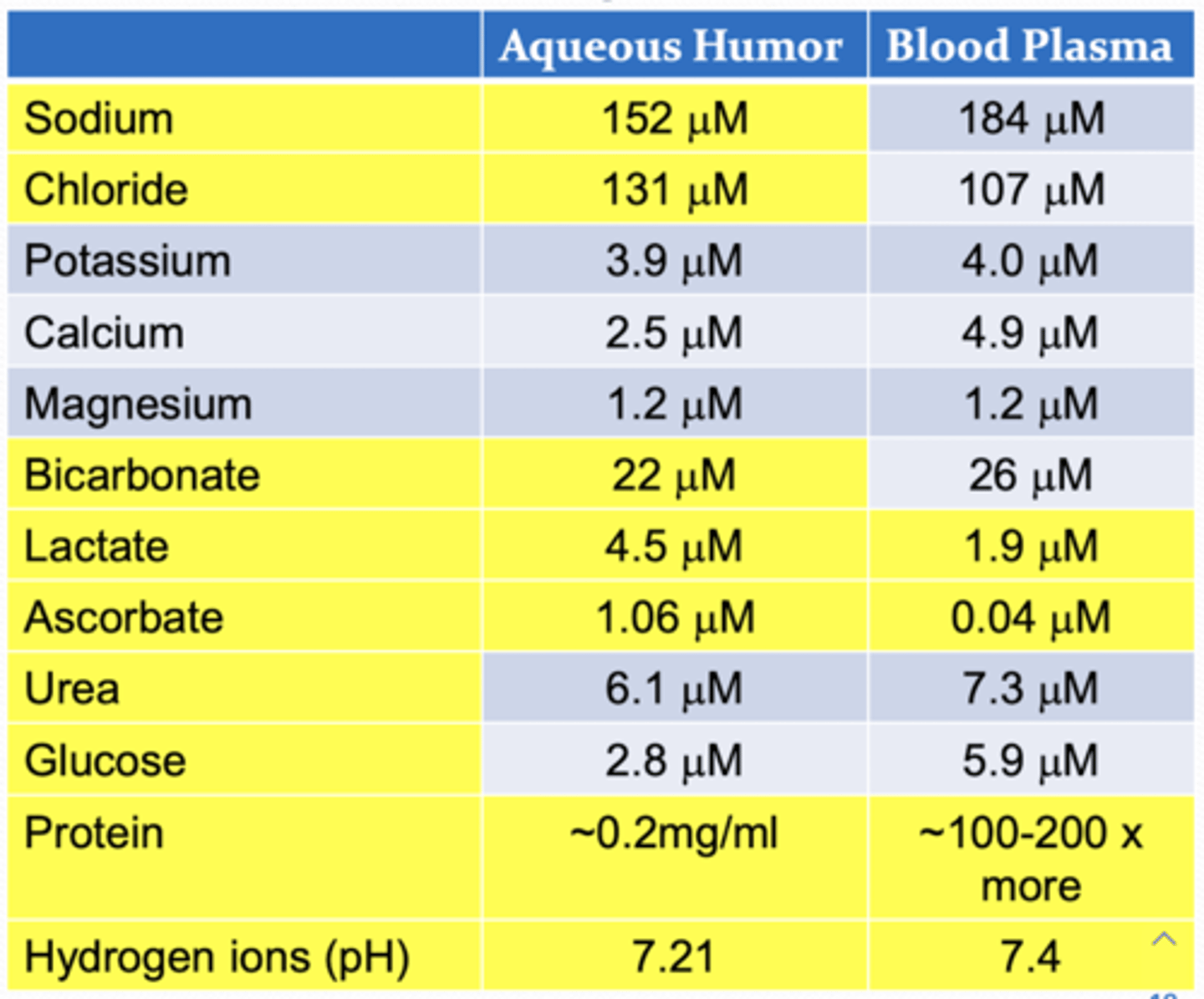
What are the major organic molecules of the aqueous humor?
1. ascorbate
2. urea
3. glucose
4. lactate
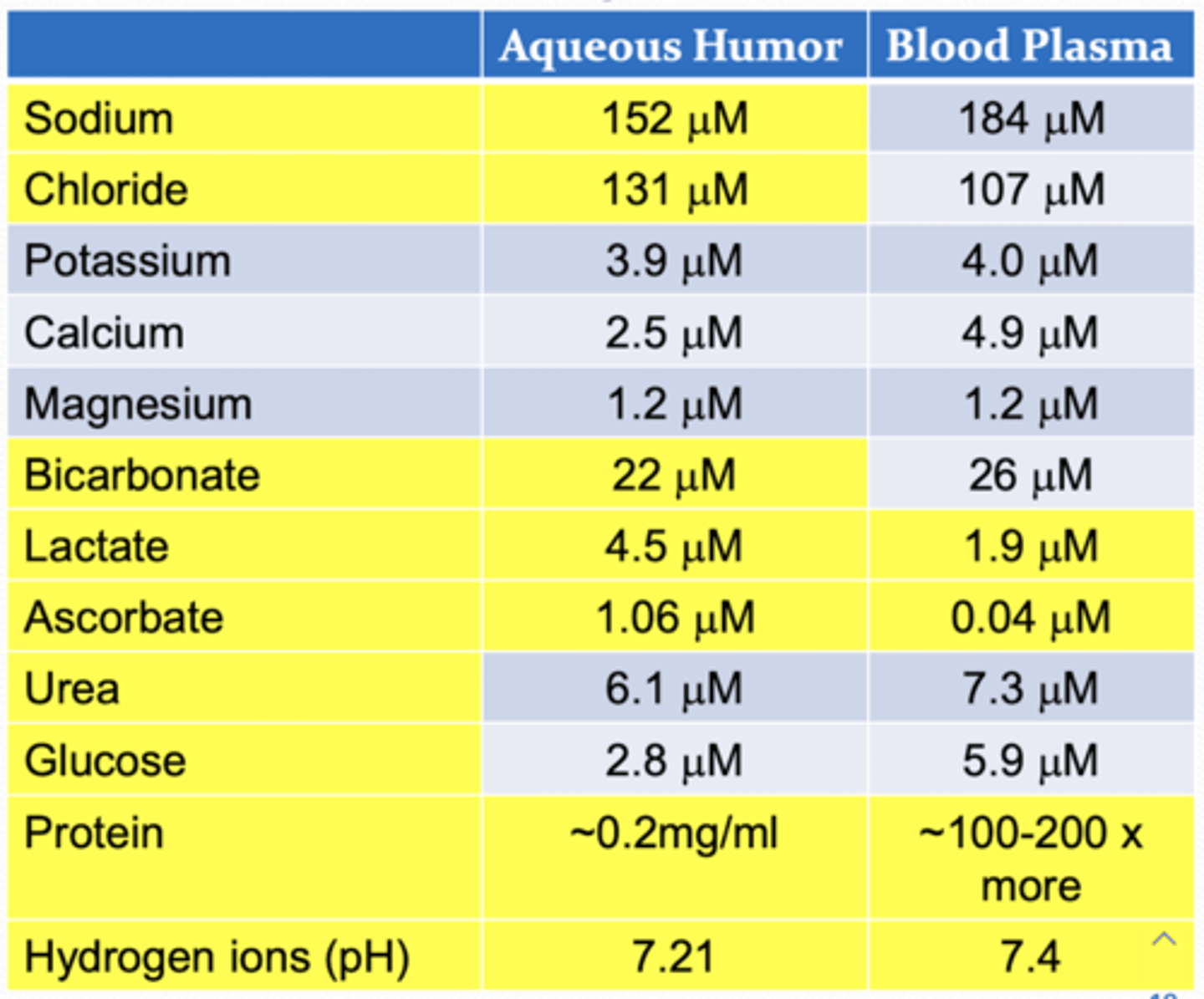
What does the pH of the aqueous humor compared to blood?
AH < blood
AH is more acidic
What are the steps of aqueous humor production?
1. ultrafiltration
2. ion/water secretion
What is ultrafiltration?
production of a reservoir of plasma in the ciliary stroma
During AH production, what does ion/water secretion imply?
ions from plasma ultrafiltrate (in the stroma) goes to the aqueous humor -- occurs at bilayered ciliary epithelium
What does ultrafiltrate describe?
capillary derived solution through fenestrations into stromal spaces
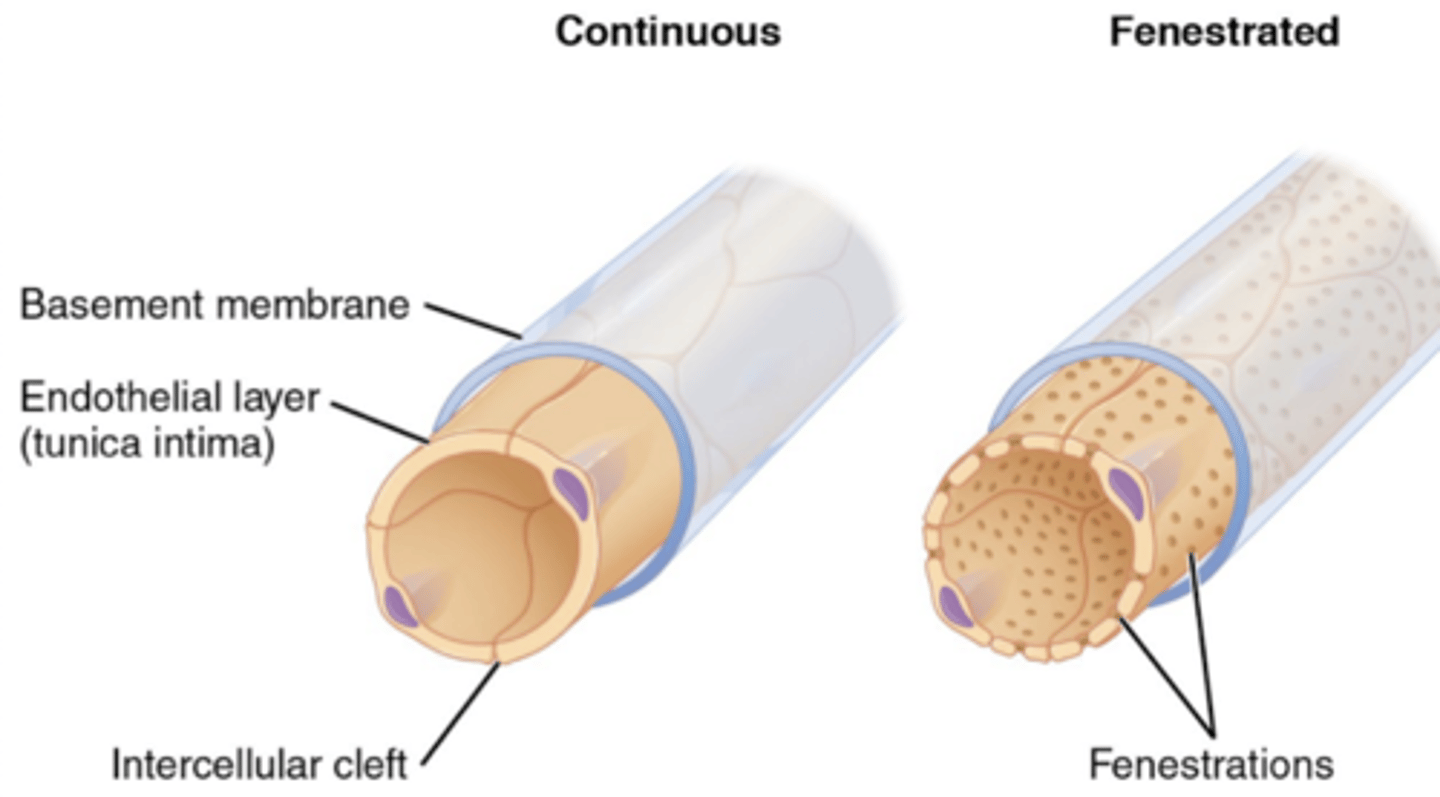
What pushes ultrafiltrate into the stroma (from the capillaries)?
capillary hydrostatic pressure
What pressures is ultrafiltration dependent on?
1. IOP
2. oncotic pressure
3. hydrostatic pressure
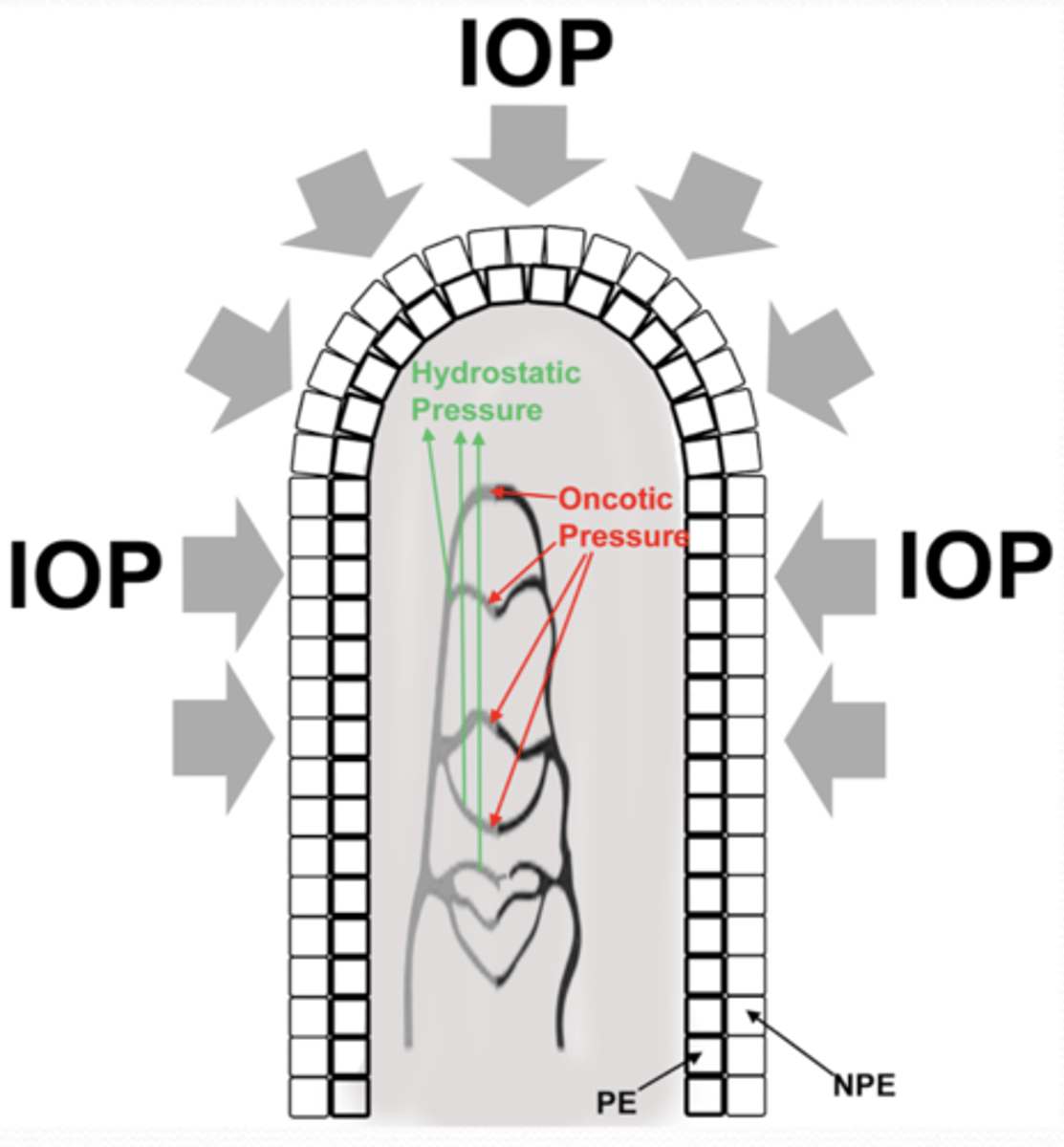
What must happen in order for ultrafiltration to occur?
hydrostatic pressure > IOP + oncotic pressure
as IOP increases ultrafiltration decreases
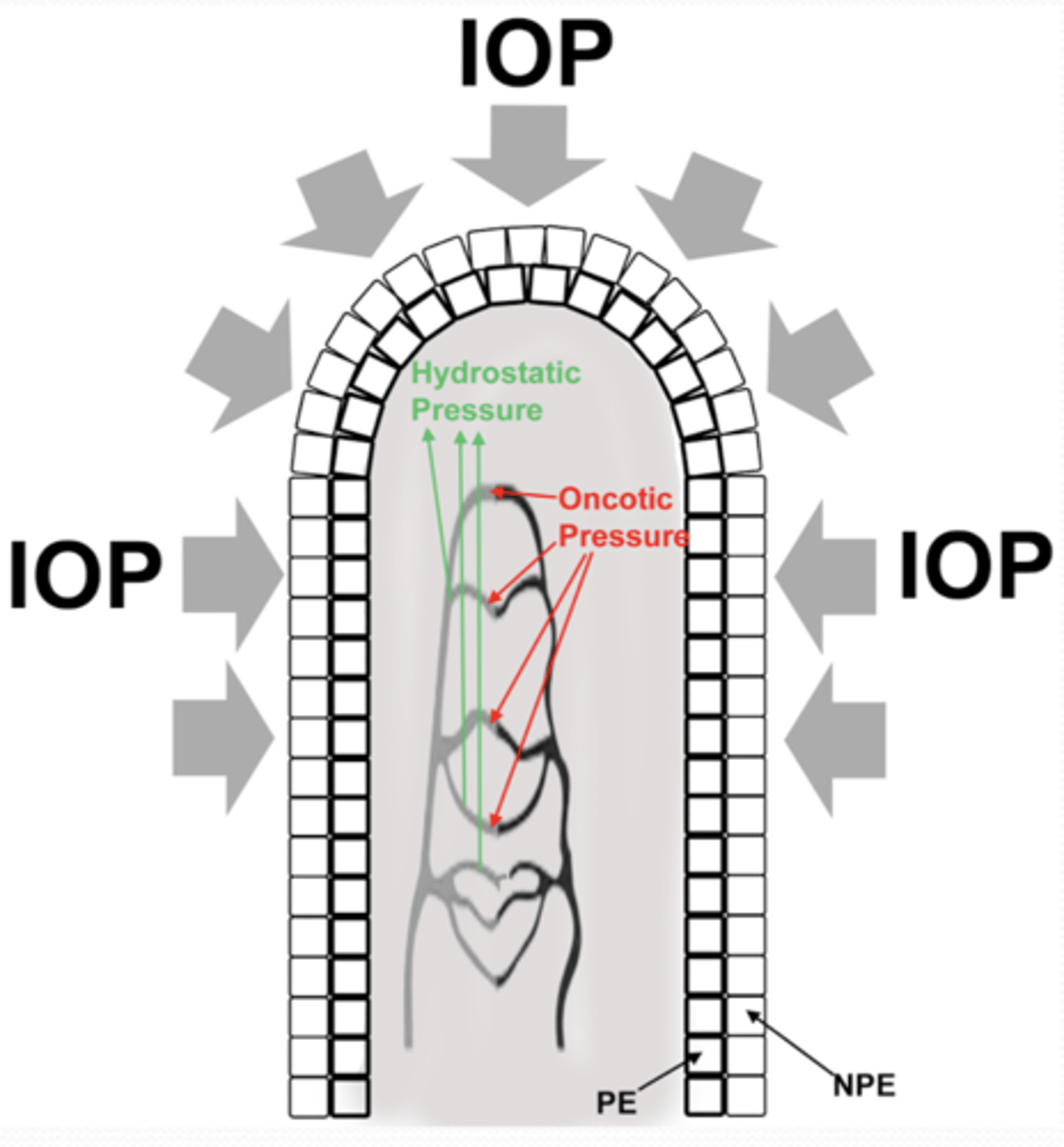
What is a decrease in facility of inflow?
decrease in ultrafiltration due to IOP
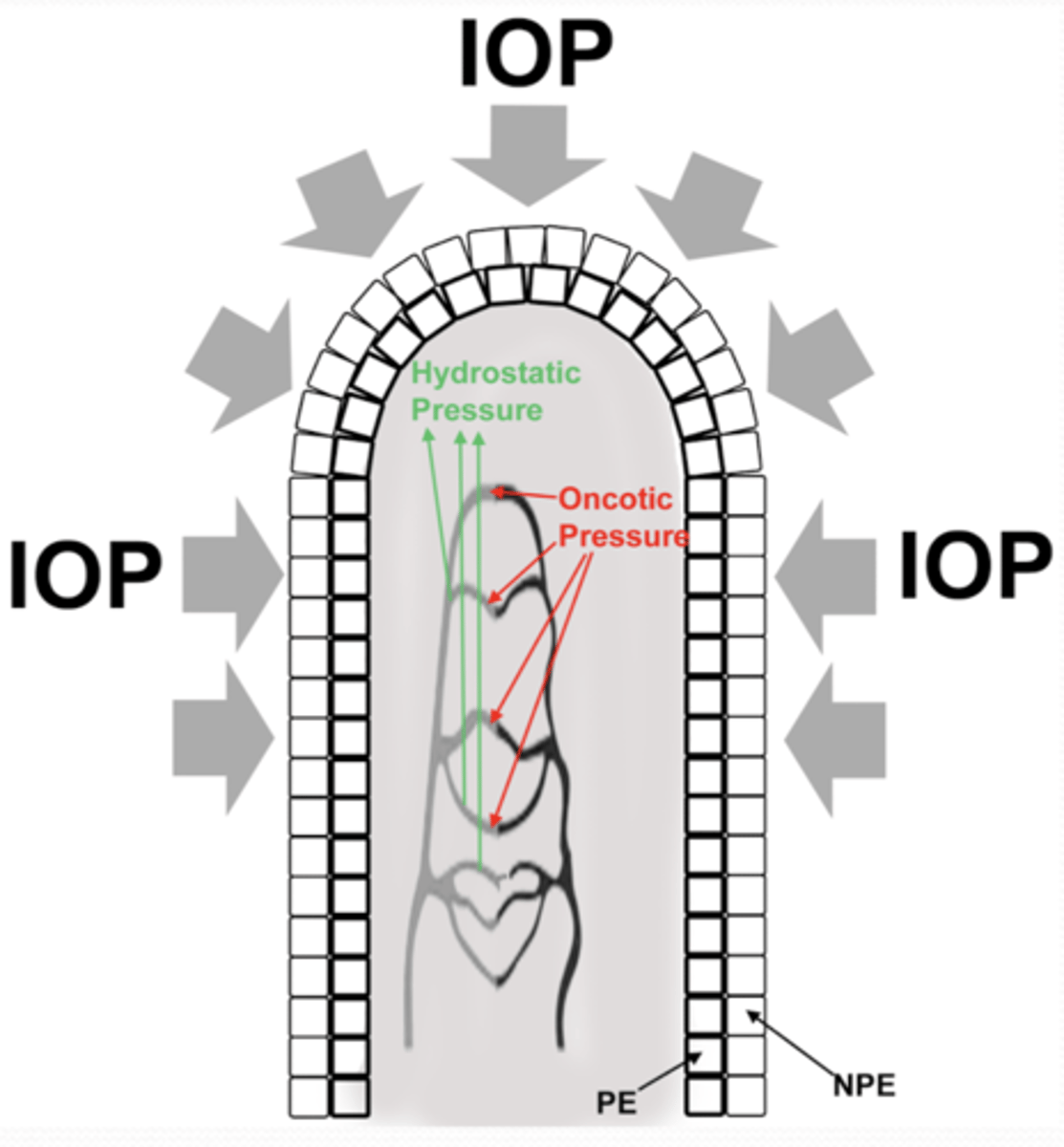
What equation represents hydrostatic pressure?
capillary pressure (Pc) - stromal pressure (Ps) = hydrostatic pressure

What is stromal pressure equal to?
IOP

What equation represents oncotic pressure?
σ[plasma oncotic pressure (Op) - stromal oncotic pressure (Os)]
σ -- stromal protein oncotic coefficient
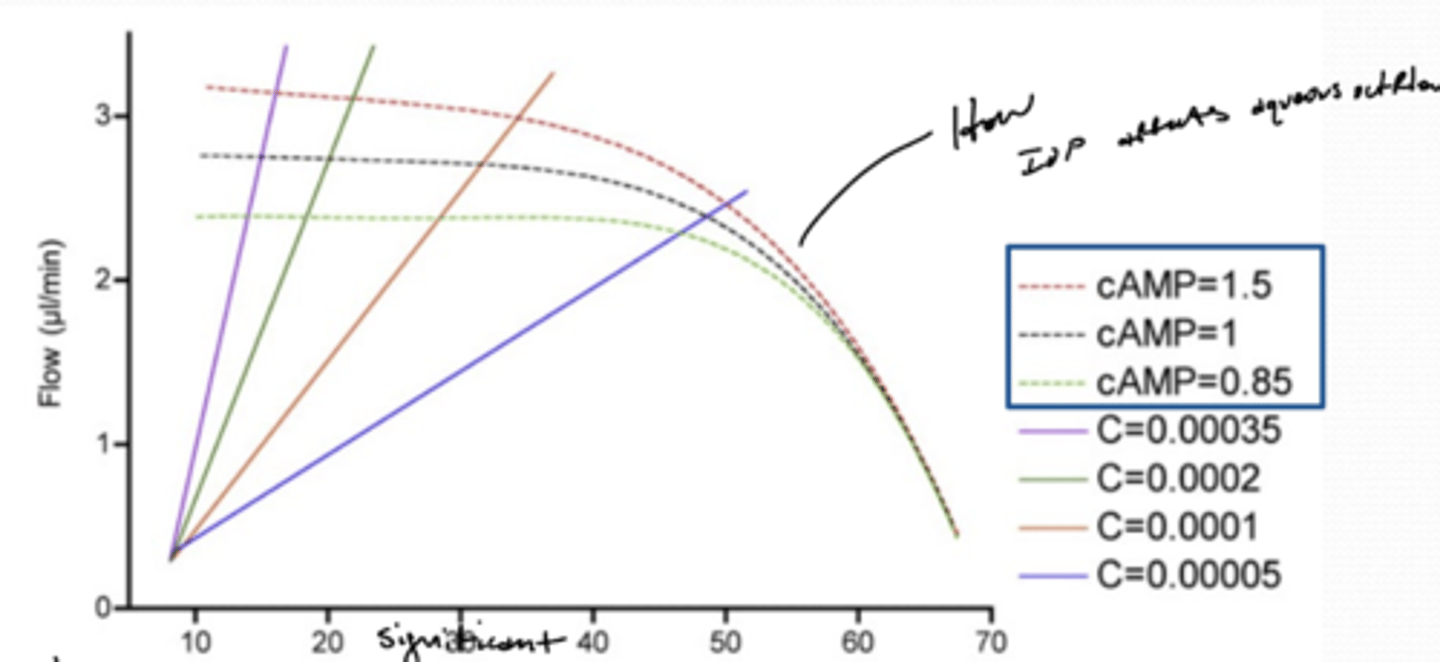
What equation represents ultrafiltration?
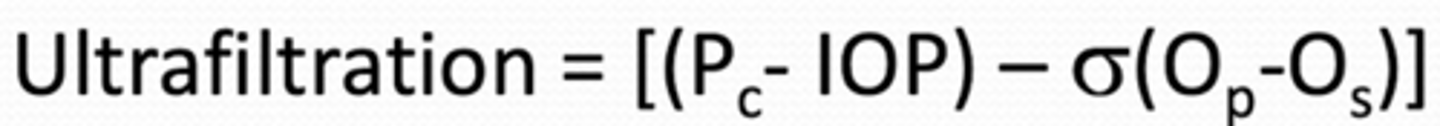
When is aqueous humor production independent of blood flow?
blood flow 75% (of normal) or normal
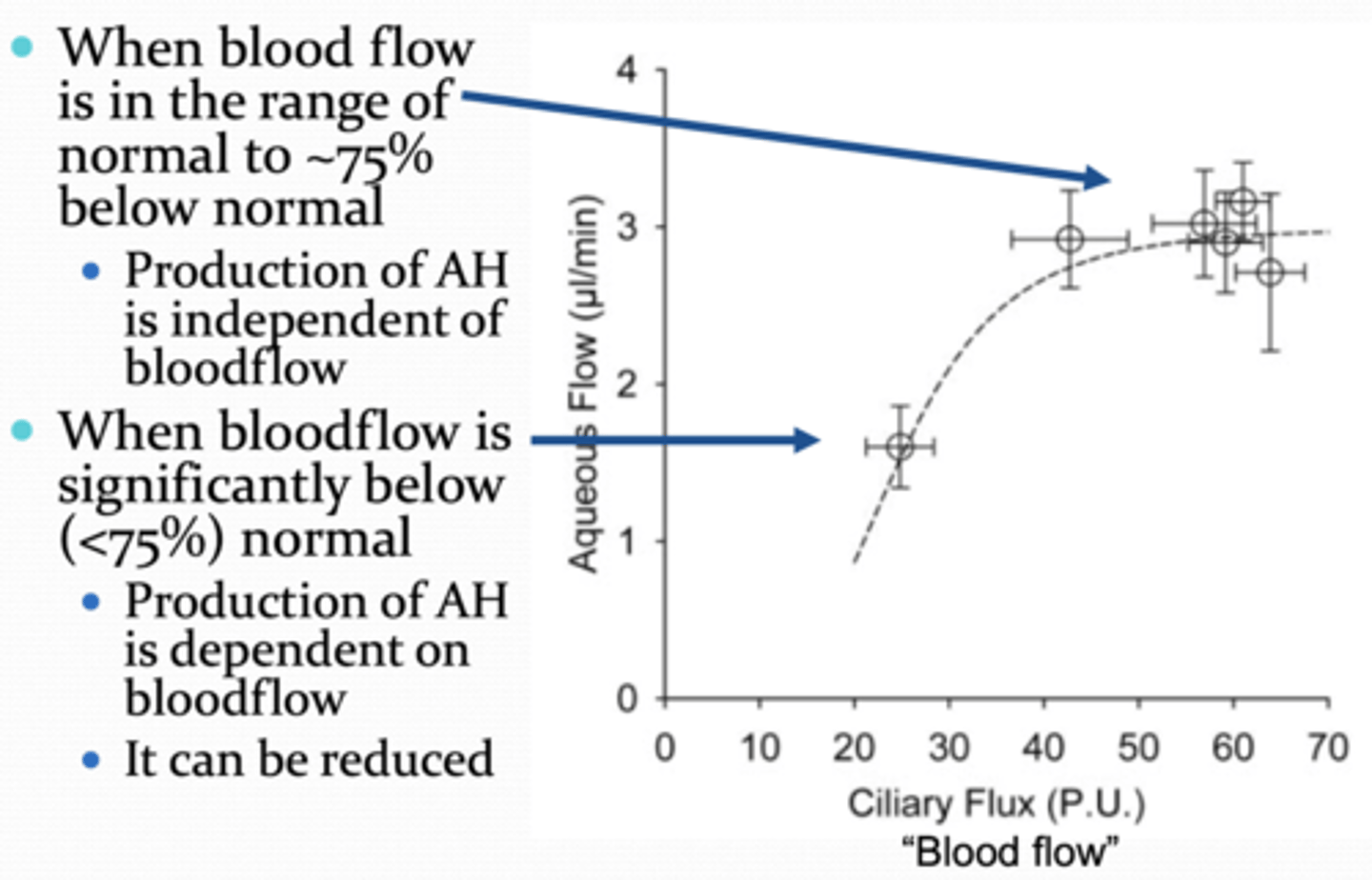
When is aqueous humor production dependent of blood flow?
significantly below 75% (i.e. normal blood flow)
will be reduced
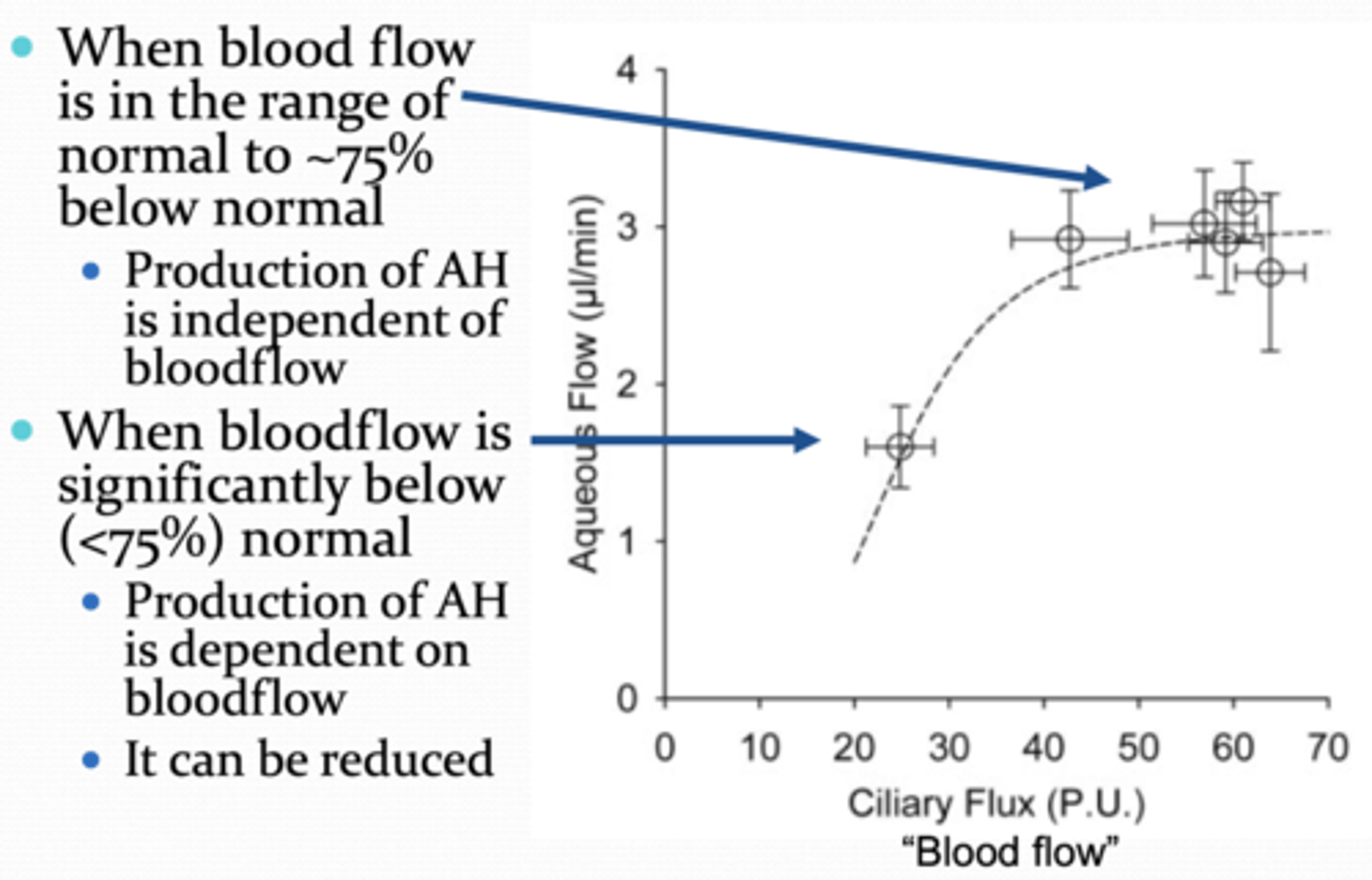
Under normal physiological conditions (in awake individuals), how much aqueous humor is produced per minute?
2.5μl/min
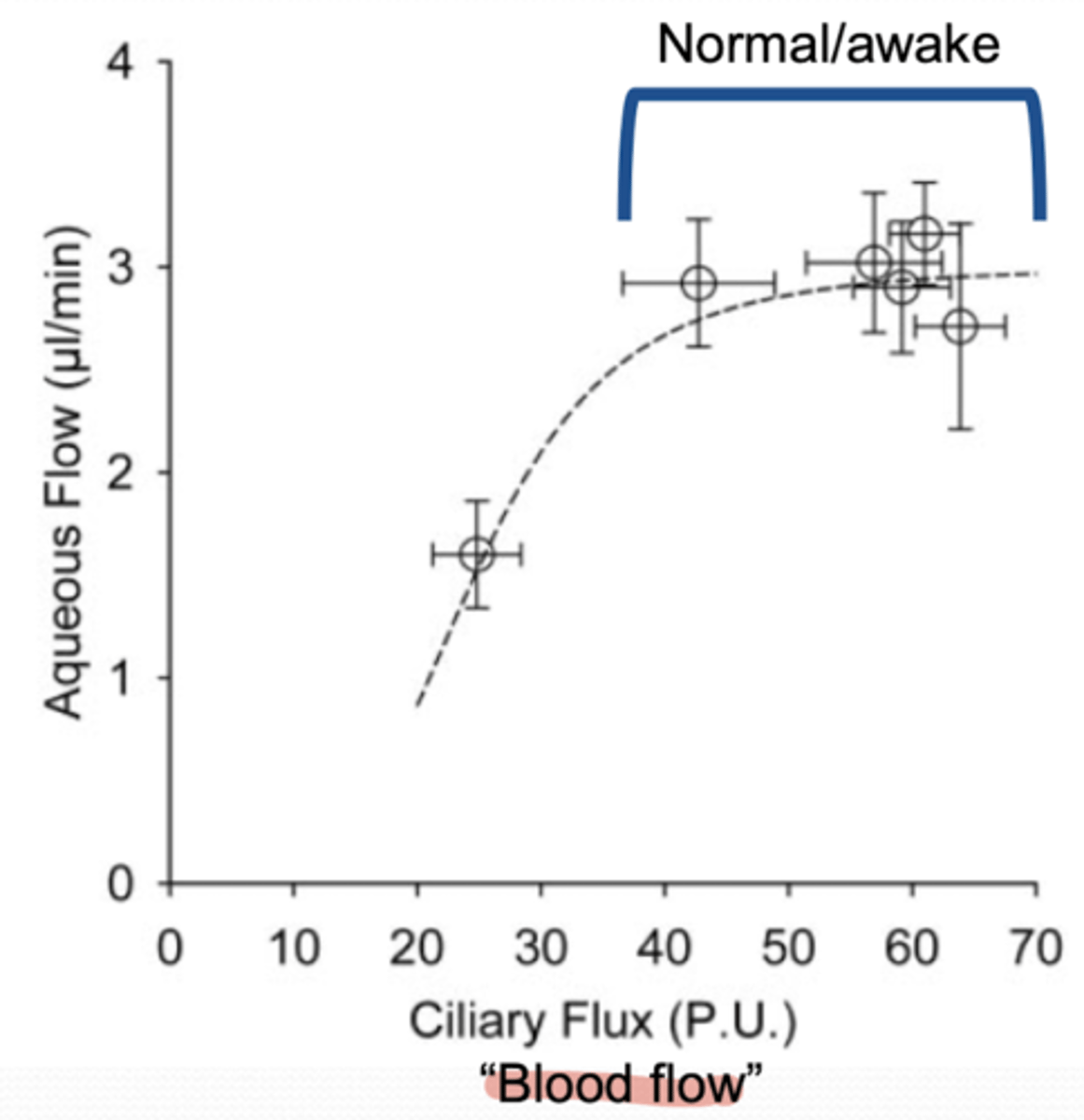
When does IOP decrease aqueous humor production?
IOP is very high -- exceeding ability of blood flow to be autoregulated