Retina
1/37
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
38 Terms
New onset flashes/floaters. Flashes common in dim illumination or with eye movement. Note shadow in vision? Any recent trauma, previous eye surgery or laser? High myopia or family hx or RT/RD?
RO - retinal tear/ RD/ vitreous hemorrhage with or without PVD, shafer sign (top image) indicates retinal break/detachment. PVD
RO migraine by asking about color/ headache after pattern, lasts approx 20 min, bilateral?
RO uveitis by vitreous cells NOT pigmented. if retinal tear then shafer sign is PIGMENTED.
PVD: natural process where the vitreous gel, which fills the eye, separates from the retina. This separation can cause bleeding into the vitreous gel, resulting in a hemorrhagic PVD.
Approximately 8% to 26% of all patients with acute symptomatic PVD have a retinal break. Shaffer sign indicates 70% change or more to have coexisting retinal break
There is a 2% to 5% risk of developing new retinal breaks in patients with PVD if no retinal break at presentation at initial visit at 6 week follow up.
IF weiss ring not visible, have patient make rapid saccades and then look straight to float the PVD into view.
if vitreous heme accompanied with suspected PVD (7.5% of cases have hemorrhagic PVD), need to do B-Scan to confirm and R/O break/tear/detachment.
Side: Hemorrhagic PVD - symptoms subside within weeks to months, but blood takes weeks to years to reabsorb
Vitreous heme or retinal hemes occur due to increased vitreous traction.
Plan:
RTC 6 weeks for PVD follow up. If have an increase of flashes/floaters or shadow in vision the RTC immediately. Educate patient that fellow eye will develop PVD as well.
If hemorrhagic PVD, RTC 2 weeks for PVD follow up.
If significant VH/schaffer sign (unable to see any breaks) - referral to retinal specialist within 24 hours.
New onset flashes/floaters/blurred vision. Peripheral or central vision loss. Flashes common in dim illumination or with eye movement. Note shadow in vision? Any recent trauma, previous eye surgery or laser? High myopia or family hx or RT/RD?
Retinal Tear: a break or hole in the retina, the light-sensitive tissue that lines the back of the eye. Causes include trauma, myopia, PVD, surgery.
Objective: Full thickness defect often in periphery (most common ST). Also, cells in ant vit, vit heme, PVD, retinal flap, sub retinal fluid. Operculum, pigment or demarcation ring if old
Workup: Scleral depression
Types:
Atrophic retinal holes are caused by retinal degeneration, low risk, usually don’t require treatment esp if asymptomatic and minimal subretinal fluid. Associated with Lattice degeneration.
Operculated holes (full thickness) result from vitreous traction pulling a retinal "plug" forward. Increased risk bc vitreous remains attached to the edges of the hole → TRACTION → RD
Treatment: Laser treatment, 24 hours if horseshoe/operculated, traumatic break, symptomatic lattice degeneration. Monitor if low risk and educate on signs of RD.
Follow up: Tear follow up: if stable, 3 months then 6 and 12 months. If had laser, 2 weeks, 6 weeks, 3 months. RTC ASAP if more symptoms
Asymptomatic, absolute VF defect
age related Retinoschisis: microcystoid degeneration of the neurosensory retina, with splitting at the outer plexiform layer of the retina.
Smooth, dome shaped, translucent, creates absolute field defect, normal underlying vasculature. Low risk for becoming RD. Monitor yearly. Scleral depress shows MOVEMENT
Bilat, smooth, bullous, inf temporal usually. No pigmented cells or hemorrhage. Assoc cystoid degeneration
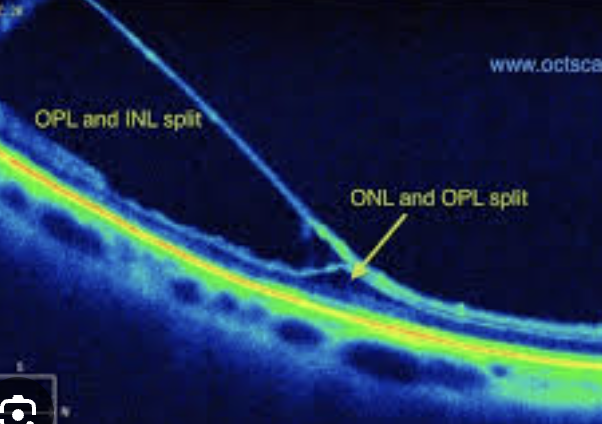
Differential: Different than serous detachment bc not mobile and no pigment demarcation
X-Linked Retinoschisis - Petaloid foveal changes, separation at NFL
Decreased vision if mac involved or asymptomatic. Possible vit heme. Congenital
Workup: Family history, scleral depression looking for detachment or break, OCT, no leakage on F.A., autofluorescence shows areas of schisis. ERG Low B-wave but fine A-wave
Plan: Vitrectomy if vit heme not clearing, surgical repair if → detachment. Amblyopia patching if young kid
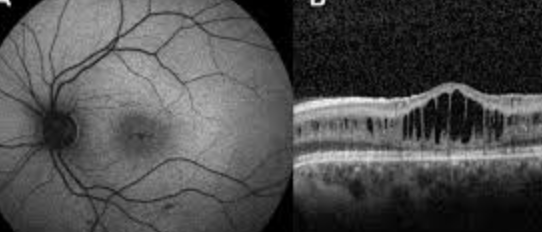
decreased vision, shadow in vision, flashes of light. Not likely to get floaters. visual changes may vary with changes in head position
Exudative (or serous) retinal detachment happens when fluid builds up between the retina and the retinal pigment epithelium (RPE) due to breakdown or blood retina barrier, causing the retina to detach. exudative detachment doesn't involve a break or traction on the retina.
The accumulation of fluid can be due to various factors, including:
Inflammatory conditions: Such as Vogt-Koyanagi-Harada syndrome, posterior scleritis, and uveitis.
Neoplastic conditions: Including choroidal melanomas and metastatic lesions to the choroid.
Vascular problems: Such as central serous chorioretinopathy (CSCR) where fluid leaks from the choroid.
Other: Trauma, eye injury, and certain systemic diseases.
Objective: Exudative detachments typically have a convex, dome-shaped appearance, with fluid shifting depending on the patient's position (bc fluid shifts retina detaches and reattaches as they sit/lie down.)
Workup: FA - determine leakage or pooling at subretinal fluid source. OCT looking for neo. B-Scan, systemic blood work up if inflammatory.
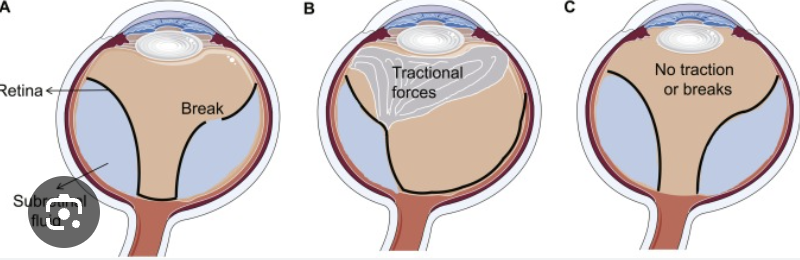
Treatment: treat underlying cause. May have to consider laser therapy
Prognosis for ERD is highly variable and heavily dependent on etiology. Acute, self-limited causes of ERD have a favorable prognosis whereas chronic, irreversible causes have a poor prognosis.[1] Prognosis is particularly poor if there is macular involvement and in cases of metastatic and paraneoplastic disease.
Pigment epithelial detachment
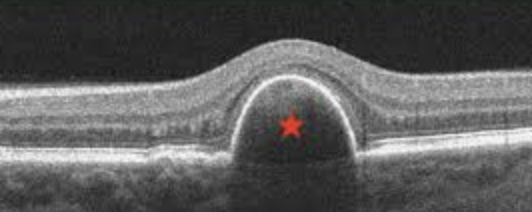
Blurred vision, Distortion of vision (metamorphopsia), Floaters, and Loss of central vision (if the macula is affected)
Pigment Epithelial detachment: RPE separation from bruchs membrane. Causes include: AMD, neovascularization (neo in choroid → PED → anti-VEGF treatment), drusen, CSR, trauma, idiopathic.
Risks: if large PED can result in RPE tears esp if antiVEGF therapy (due to fluid shifts and tissue changes).
Types of PEDs
Serous PEDs: neo or wet AMD (fluid accumulation)
Fibrovascular PEDs: assocuated with choroidal neo
Drusenoid PEDs: nonneovascular or dry AMD
Plan: treat underlying issue: AREDs for AMD intermediate. CNVM refer to retina for antivegf treatment. Follow up q6 months
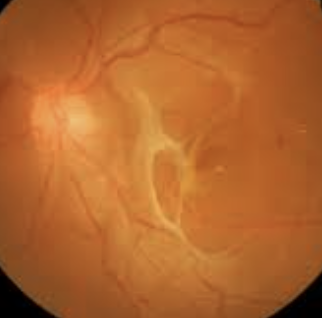
Tractional detachment: traction from scar tissue or other abnormal growths resulting in retinal detachment
Causes: Diabetic retinopathy, sickle cell, retinopathy of prematurity, toxocariasis. DRVOS can also cause abnormal blood vessel growth and scarring in the retina, leading to traction
Cotton wool spot: Obstruction of retinal arteriole causing blockage of axoplasmic flow, causing buildup of debris in the NFL.
Etiology: diabetes, BP, GCA, HIV, heart condition, anemia
Workup: blood pressure, fasting blood sugar, A1C, ESR and CRP for GCA, carotid doppler, CT scan of chest, emboli, HIV
Sidenote: Prolonged high blood sugar levels, can damage the small blood vessels in the retina. Can cause these vessels to swell, leak, or even close off completely.
Sudden, profound, unilateral, painless sectoral VF loss
- Hx of transient vision loss
BRAO: small blood vessel (branch) in the retina becomes blocked, preventing blood flow to that area. This can lead to sudden vision loss or disturbances in a specific part of the visual field. prognosis for BRAO depends on the severity of the blockage, the underlying cause, and the timeliness of treatment. Some patients may regain normal vision, while others may experience permanent vision loss.
Objective: Whitening and edema and CWS in affected section. Narrowed arteries, boxcarring, emboli at a bifurcation
Workup: IVFA, OCT macula, Fundus photo, ERG
Workup up:
BRAO + optic nerve edema or retinitis – Order Blood RPR or VDRL and FTA-ABS or treponemal specific assay, Lyme, toxo and cat-scratch dx RO
CRP, ESR, Platelets if 55 or older to RO GCA
Plan:
Send to the ER for a stroke eval.
Treat underlying dx. Follow up q3-6 months for DFE to monitor. Neo is rare.
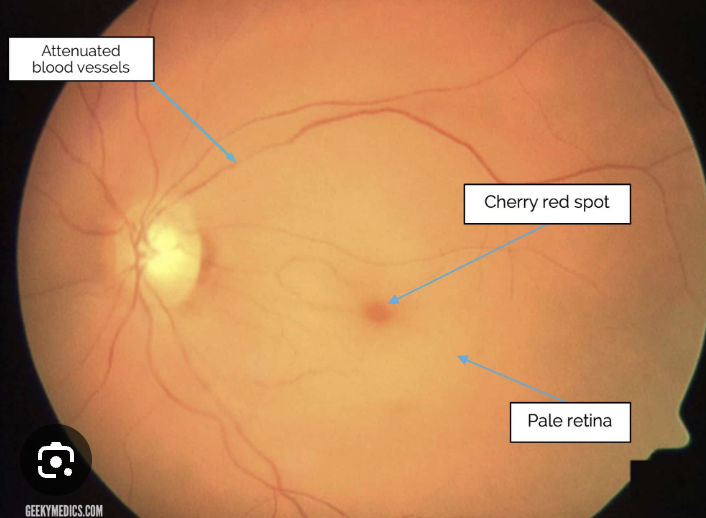
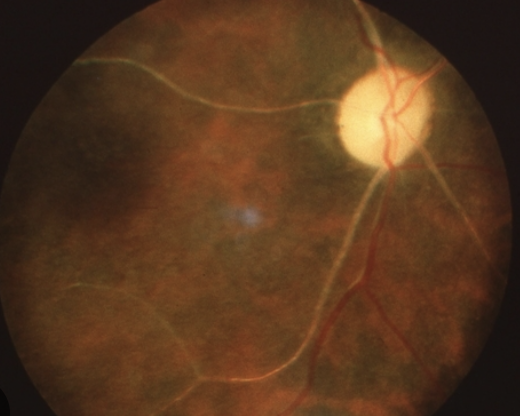
Sudden, profound (CF or LP), unilateral, painless vision loss
Hx of transient vision loss
Vasculitis condition?
CRAO: central retinal artery, the main blood vessel supplying the retina, becomes blocked (“stroke of the eye”. This interruption in blood flow leads to damage to the retina and severe vision loss. Some patients may regain partial vision, but many experience permanent vision loss.
Cause: emboli/thrombus/vascular disease
Ancillary Testing: BP, OCT macula, ERG (abnormal), IVFA, Fundus photo
Plan:
Immediate ESR, CRP , CBC with differential. RO GCA. Blood work for fasting BSL, hemoglobin A1C RO diabetes
Urgent stroke work up if embolism present + Order carotid doppler to determine presence of clinically significant stenosis + ECG
If NVI/NVA/etc present refer to retinal specialist for
anti-VEGF/PRP
RTC: 1-4 weeks, checking for NVI/NVA/NVD/NVE; follow up as indicated by neuro/cardio/internist/retina
Symptoms: blurry or distorted vision, dark spots or floaters, and in some cases, sudden vision loss.
Age? (>55)
Med hx? diabetes, hypertension, hyperlipidemia, inflammatory dx? Factor V Leiden, Prot S defic?
Using contraceptives? Pregnant?
Do you smoke? Cancer?
CRVO: central retinal vein, the major vein that drains blood from the retina, becomes blocked, usually due to a blood clot (thrombosis). This blockage can lead to a backup of blood and fluid in the retina, potentially causing swelling and vision problems.
Objective: macular edema (blurry/distorted vision), retinal hemorrhages (dark spots/floaters), neovascularization → glaucoma
Workup: Gonio - ro NVI/NVA, DFE, IVFA (r/o neo), OCT (mac edema)
Blood work: Blood glc, A1C, CBC with diff, PT/PTT, lipid profile, syphilis RPR or VDRL, FTA-ABS, ANA for lupus, Factor 5 Leiden, antithrombin
2 types: ischemic (non-perfused) or non-ischemic (perfused), each with implications for prognosis and treatment
Non-ischemic: mild decreased in vision, improves throughout the day. May have RAPD
Plan: Monitor. RTC monthly to RO ischemic CRAO conversion. (Acute signs usually resolve over 6-12 months (disc collaterals and pigmentary changes at the macula often persist as residual findings) MONITOR FOR CONVERSION TO ISCHEMIC CRAO – 15% WITHIN 4 MONTHS!!! 35% of pts within 3 years!!
prognosis is good with return of vision to normal or near normal in about 50%
Ischemic: severe vision loss (<20/200) + APD
Prescribe Aspiriin 81 mg po daily
Diamox 250 mg BID - dec IOP/BP
Refer to retina for Anti-VEGF treatments if neo or mac edema present
RTC Monthly for gonio (r/o NVI/NVA) + DFE.
10% risk for fellow eye to develop BRVO/CRVO.
50% of cases develop NVI within 2-4 months → 90 day glaucoma. 5% become neo glaucoma.
Bad prognosis, likely permanent due to mac ischemia
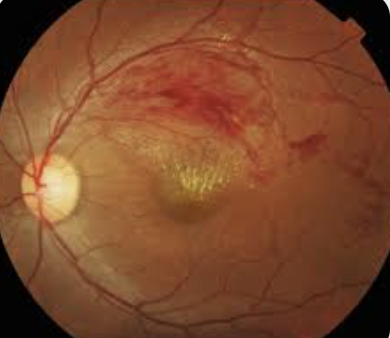
Peripheral vision loss. Blurred or distorted central vision.
BRVO: blockage of one or more branches of the central retinal vein, which runs through the optic nerve. This causes bleeding in the eye. Associated with hypertension, diabetes, and congestive heart failure.
Workup: Macular OCT (R/O macular Edema), BP, FA if suspect neo (NVD/NVE/NVI risk)
IF patient is young, may have underlying dx. Order blood work including: ESR, CRP , CBC with differential, fasting BSL, hemoglobin A1C
Plan:
Order carotid doppler to determine presence of clinically significant stenosis
Refer to retinal specialist for Anti-VEGF if NVD/NVI/NVE
RTC: Monitored every month initially and then every 3-12 months to ensure that complications such as macular edema and neovascularization do not develop.
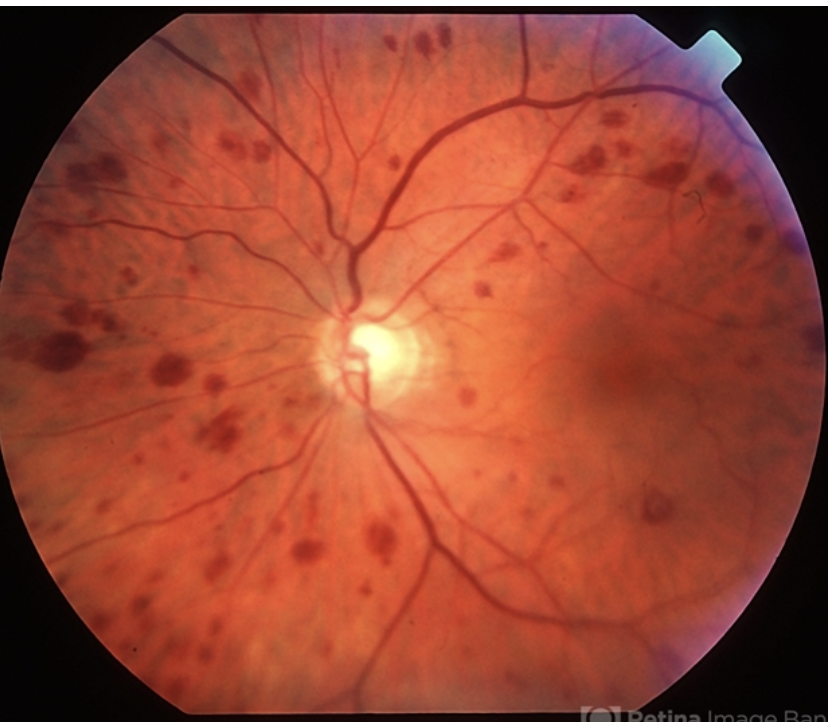
UNILATERAL, decreased vision with associated periorbital or ocular pain, and a history of transient monocular vision loss
- Men 50-80
Ocular ischemic syndrome: occurs when blood flow to the eye is reduced or blocked. This can lead to damage to the retina, optic nerve, and other structures in the eye.
Objective: irregular retinal veins and narrowed arterioles. mid-peripheral retinal hemorrhages, iris neo, and posterior segment neo. NO TORTUOSITY IN BV (way to dif from CRVO).
May have: concurrent episcleral injection, corneal edema, anterior uveitis, neovascular glaucoma, iris atrophy, CWS, spontaneous central retinal pulsations, and/or retinal microaneurysms.
Workup: Blood work , MRI, carotid doppler due to risk of Atherosclerosis (hardening of the arteries), Stroke, Blood clots, and Giant cell arteritis (an inflammatory condition that affects blood vessels
Manage condition with PCP
40% of paitents with OIS die due to cardiovascular disease within 5 years.
RTC: Manage ocular condition of infla, neo glaucoma/IOP increase, Anti-VEGF if neo present. RTC depending on eye problems
Hypertenisive Retinopathy: occurs due to the high blood pressure damaging the small blood vessels in the retina, leading to thickening of their walls, reduced blood flow, and potential retinal damage.
Objective: Narrowed arterioles, flame hemorrhages (rare MA) not confined in a sector, crosses horizontal raphe, bilateral.
Chronic sign:
AV nicking
Copper wiring - Retinal arterioles appear orange or yellow instead of red
Acure Sign: Elschnig spots: focal chorioretinal atrophy from previous choroidal infarcts
Acute sign:: may see Macular Start of exudates
Unilateral Hypertensive retinopathy indicates carotid artery obstruction on the side of NO HR
Workup: BP, DFE, OCT macula, carotid doppler if unilateral.
Plan: Refer to ER if hypertensive crisis (180/120). Refer to PCP for management for BP
RTC: 3 months at first; then every 6-12 months
Diabetic Retinopathy:caused by damage to the blood vessels in the tissue at the back of the eye (retina) due to Poorly controlled blood sugar.
Objective: IRMA, dot blot hemes, exudates, CWS, MA, venous beading
Conversion to Severe NPDR: hemes in 4 quadrants, 2 venous beading quadrants, 1 IRMA
Conversion to PDR:
NVD > ⅓ DD
NVD + pre ret or VH
NVE > ½ DD + pre ret or VH
Any NVI or NVA
CSME grading:
Edema w/in 500 foveal center
Hard Exudates w/in 500 um and assoc thickening
Edema > 1DD w/in 1DD of fovea
Cause: DME arises from the accumulation of fluid, protein, and lipids throughout the layers of the retina.
BV obstruction → ischemia → VEFG → increased leakiness in fragile BV
Free radical inc + inc garbage in long standing diabetes → inflammation → leaky BV
Grading:
Mild: Retinal thickening and hard exudates are present in the posterior pole but fall more than 1,000 μm outside the central macular subfield.
Moderate: Retinal thickening or hard exudates are present within the central subfield of the macula but do not involve the center.
Severe: Retinal thickening or hard exudates involve the center of the macula
Plan: Emphasized Glycemic control with medication, healthy diet and exercise. Continue management with PCP. Follow up as scheduled.
RTC: No DR = annual, Mild NPDR q6-9 mos, Mod-Severe NPDR q4-6 mos, PDR not high risk q2-3 mos
Plan: If CME + CI/Vision reduced then can do Topical NSAID like ketorolac 0.5% QID plus topical steroid QID. Consider Anti-VEGF treatments if severe and not improving.
RTC 4-6 weeks
Hx:
6-10 weeks post surgery including cat, laser, and cryo (Irvine-Gass syndrome)
Trauma, diabetes (CME), vein occlusion, uveitis, ret pigmentosa, vasculitis like Behcet and sarcoid, telangiectasia like Coats and MacTel, AMD, hypertension
Meds: Epinephrine, prostaglandin anaglog
Macular Edema: fluid in the central part of your vision.
BV obstruction → ischemia → VEFG → increased leakiness in fragile BV
Free radical inc + inc garbage in long standing diabetes → inflammation → leaky BV
Workup: OCT, FA, DFE
Plan: Macular edema CI/Vision reduced then can do Topical NSAID like ketorolac 0.5% QID plus topical steroid QID. Consider Anti-VEGF treatments if severe and not improving.
RTC q4-6 weeks to monitor resolution
paracentral scotoma, gray spot, aniseikonic (size difference perception), hyperopic shift metamorphsia, colors faded.
Central Serous Retinopathy: fluid accumulates under the retina, causing a serous (fluid-filled) detachment and vision loss/metamorphopsia. Associated with exposure to corticosteroids, pregnancy, elevated cortisol/aldosterone levels
Objective: RPE mottling, pigment changes, PED
Workup: OCT macula (on FA see smokestack appearance)
RTC 6 weeks to monitor. Plan is observe, usually resolves in 3 months. Discontinue steroid use including creams and nasal sprays.
If chronic + bothersome consider spironalactone and epleronone after doing labs for kidney function. May have symptoms like stomach issues, muscle weakness, cardiac function due to hyperkalemia.
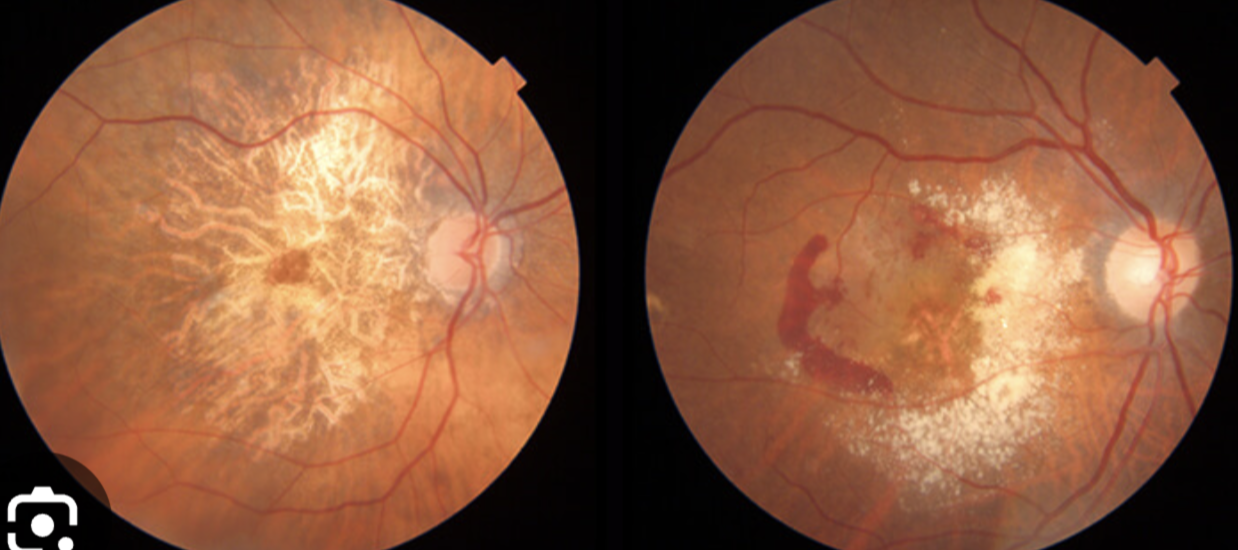
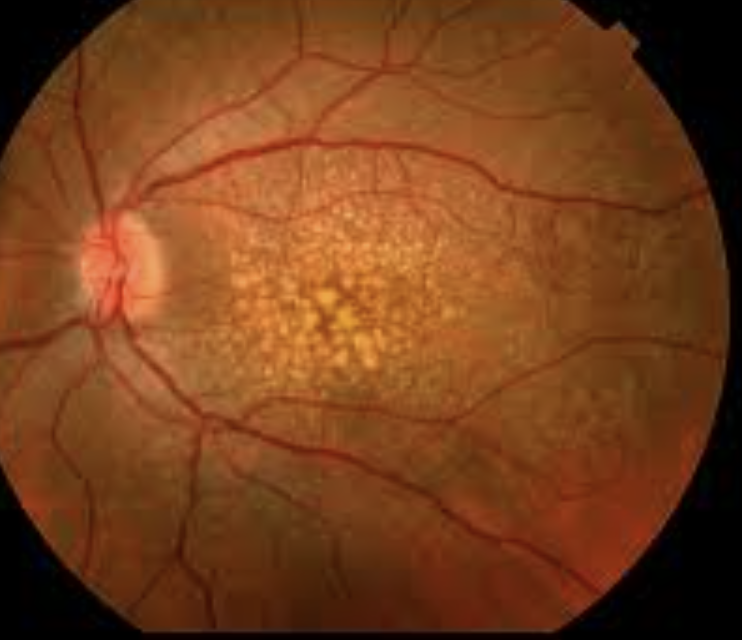
Blurred vision, metamorphopsia, central scotoma,
Age Related Macular Degeneration: acquired degeneration of the retina that causes significant central visual impairment due to damage to the RPE cells (pigment abnormalities), which are responsible for waste removal and supporting photoreceptor function, leading to impaired vision due to drusen formation. Progression to WET AMD can occur when abnormal blood vessels form from choroid.
Risk factors: family history, smoking, >50, white, UV light exposure
Plan: AREDS BID if intermediate. 6-12 months looking for neo. Home monitoring with Amsler. Low vision aid if indicated.
If wet AMD: Referral to retinal specialist for Anti-VEGF treatments. Follow up monthly.
Side note: Occult neo: sub RPE (type 1)
Classic neo: sub-neurosensory retina (type 2)
DDx:
Familial drusen - genetic macular dystrophy disorder characterized by the presence of small yellow-white accumulations of extracellular material under the retinal pigment epithelium in the ocular posterior pole, and affecting multiple members of a family.
Degenerative Myopia:
Rubella: Rubella retinopathy is a part of congenital rubella syndrome and includes unilateral or bilateral pigmentary retinopathy, described as “salt-and-pepper” fundus ranging from finely stippled to gross pigmentary changes
Serpiginous choroidopathy: Geographic atrophy that looks like AMD. bilateral, chronic, progressive, recurrent inflammatory disease of the retinal pigment epithelium (RPE), choriocapillaris and choroid of unknown etiology
Idiopathic polypoidal choroidal vasculopathy: polyp-like lesions in choroidal vasculature around macula or disc. Looks like wet AMD but in younger asian patients and less drusen/geographic atrophy.
Work up: Indocyanine green angiography, OCT
Plan: Spon resolution, anti-VEGF, or PDT
Male toddler, decreased vision on one side
Coats Disease: congenital, nonhereditary eye disorder, causing full or partial blindness, characterized by abnormal development of blood vessels behind the retina.
Objective: Unilateral retinal vascular telangiectasias (Lightbulb vessels). Extensive yellow intraretinal and subretinal exudates. NOT TYPICAL TO HAVE HEME
Risks: Exudative Retinal Detachment, strabismus, Dec VA unilateral, leucocoria
Leucocoria: Retinoblastoma, Coats, Toxocariasis, congenital cataract, RD, Persistent hyperplastic primary vitrous
Workup: OCT/ FA
Plan: Observation if minimal telangiectasic vessel/no exudation.
Referral to retinal specialist for cryotherapy or laser treatment
The prognosis depends on the extent of the disease with milder, older presenting cases, having a better prognosis, of even spontaneous regression, whereas children under the age of three have a poorer prognosis
None or flashes and floaters if advanced. May have sudden severe abdominal or musculoskeletal pain.
Hx of Anemia (fatigue, SOB, pale skin), jaundice (Due to damaged RBC),
Sickle cell Anemia: genetic blood disorder that causes red blood cells to become abnormally shaped (sickle-shaped) and rigid. This leads to a blockage of blood flow in parts of the retina.
Objective signs:
Comma shaped conjunctival vessels
Peripheral sea fan neo (top photo), sclerosed retinal vessels, dull gray peripheral fundus from artery occlusion and ischemia
salmon patches (hemorrhages are caused by sudden occlusion and rupture of a medium sized arteriole by sickled red blood cells, color changes from bright red to orange and later, yellow or white),
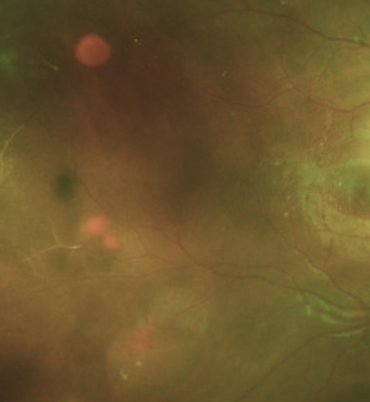
black sunburst- dark pigmented CR scar (RPE migration and proliferation after heme, looks like toxo scar)
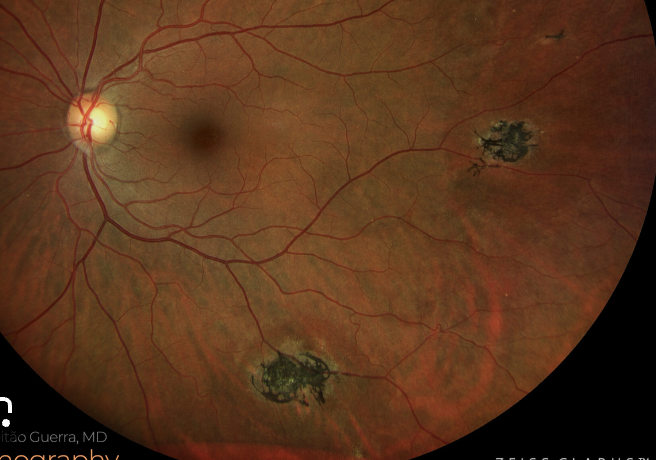
Stages: 1. Peripheral artery occlusion. 2. Peripheral A.V. anastomoses. 3. Neo. 4. Vit heme → fibrosis. 5. Ret detachment
Workup: OCT. Blood work: Sickle cell cont, Hgb low, peripheral smear shows sickled cells, Sickledex, hemoglobin electrophoresis
Plan:
observation if nonproliferative or isolated neo.
Refer vitreous heme/RD for vitrectomy.
If Neo + Vitreous heme refer for PRP to avascular area.
Avoid CAI bc inc sickling.
Ddx.
Sarcoid can have sea fan neo but has regular neo as well. in young african women.
Valsalva retinopathy: intraretinal heme/vitrous heme - rupture in superficial capillaries.
Degenerative Myopia: neo, RD, lacquer cracks
Tilted Disc: anomalous with scleral crescent often inf nasal. Irreg vessel pattern: situs inversus, area of ectasia in direction of tilt (inf nasal). Associated with high myopia and astigmatism. no lacquer cracks. VF ST + doesnt respect midline.
Ddx.
Myopic disc: Posterior staphyloma + lacquer cracks, lattice degen, tilted disc
None or blur from neo
Hx. dx of PEPSI
Pseudoxanthoma Elasticum: elastic fiber disorder → loose skin in neck, heart problems.
Ocular signs: peau d'orange (Mottled fundus appearance like orange tecture, with an orange hue) most common in the temporal midperiphery. Also, optic disc drusen
Ehlers Danlos: CT disorder → hyperelastic skin, loose joints
Ocular signs: Myopia, thin pachs, steep K’s, Keratoconus, Convergence insufficiency, epicanthal folds, hypertelorism, strab, blue sclera, floppy eyelid
Pagets Bone disease : large skull, bone pain, fractures, hearing loss, heart problems.
Sickle cell
Idiopathic
Angioid Streaks: Abnormally thick/calcified Bruchs membrane. Mechanical stress. Break in bruchs → CNVM.
Objective: Breaks in Bruch's membrane. Bilat red brown or gray bands deep to the retina. Spoke like pattern around disc. Risk neo.
May have sub ret hemes, small scars that look like histo spots, drusen.
Workup: DFE, FAF, FA, OCTA for neo
Plan: Referral to retina for Anti-VEGF for neo. Monitor vision with Amsler
If no neo, recommend wearing polycarb lenses to avoid trauma that can cause choroidal rupture (has inc risk).
RTC q6 months for DFE.
Asymptomatic or blur from neo. May experience fever, cough, shortness of breath, chest pain, muscle aches, and fatigue.
Hx of being around ohio mississippi valley or chickens.
Histoplasmosis: Fungal infection breathed in from environment. Histo fungus thrives in soils enriched with bird or bat droppings.
Objective: yellow punched out round spots or chorioretinal scars with pigment clumps.
Triad: PPA + Histo spots + Macular CNVM
Plan: Monitor vision with amsler grid. q6-12 months
If neovascularization present then Anti-VEGF. RTC 4 weeks after VEGF treatment. (wont need lifelong injections like in AMD)
DDx.
Multifocal choroiditis: hypopigmentet spots + inflammation
Toxoplasmos: pigmented choroiretinal lesion + fibrosis + vitreous infla
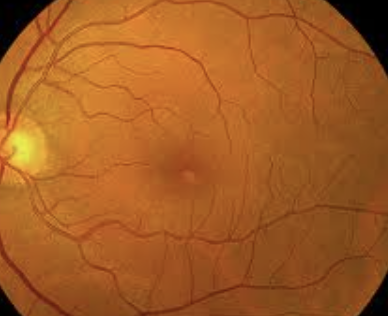
Metamorphopsia/ blurred vision (20/200 or better), blind spot, flashes of light
Vitreomacular traction (VMT): occurs when the vitreous gel in the eye pulls on the macula, the central part of the retina responsible for sharp vision. Mor common in women
Objective: Partial vit detach plus loss of foveolar depression and yellow spot/ring in macula. Pseudocysts, lift from RPE
Workup Macular OCT
RTC 4-6 weeks due to risk of macular hole + amsler
Vitreomacular traction - no fundus appearance change bc normal foveal contour.
RTC 6 months + amsler grid
Blurred or distorted central, Blind spot, Floaters, Loss of depth perception
20/200 or better depending on how much is happening. Metamorphopsia, central scotoma. Women
Hx of trauma, surgery, sun gazing, severe myopia, hx of ERM/Best Dx/RD?
Macular hole: Macular holes are small tears in the macula, the central part of the retina responsible for sharp central vision.
Objective: Separation from the ILM to the outer segments of the photoreceptors (RPE not affected)
Workup: Macular OCT, Watzke Allen (break in line if mac hole. Pseudohole or lamellar hole will report distortion
Stages:
1. Impending hole with yellow ring in fovea.
Sm round yellow spot/ring in fovea, no foveal depression
2. Small full thickness hole.
Yellow ring enlarges
Full thick hole with cuff of sub ret fluid but no PVD.
Yellow deposits in hole at level of RPE
-VA 20/200, try eccentric viewing 20/60
4.Full hole with sub ret fluid and PVD
edematous cuff at margins, operculum visible. VA improves as edema subsides
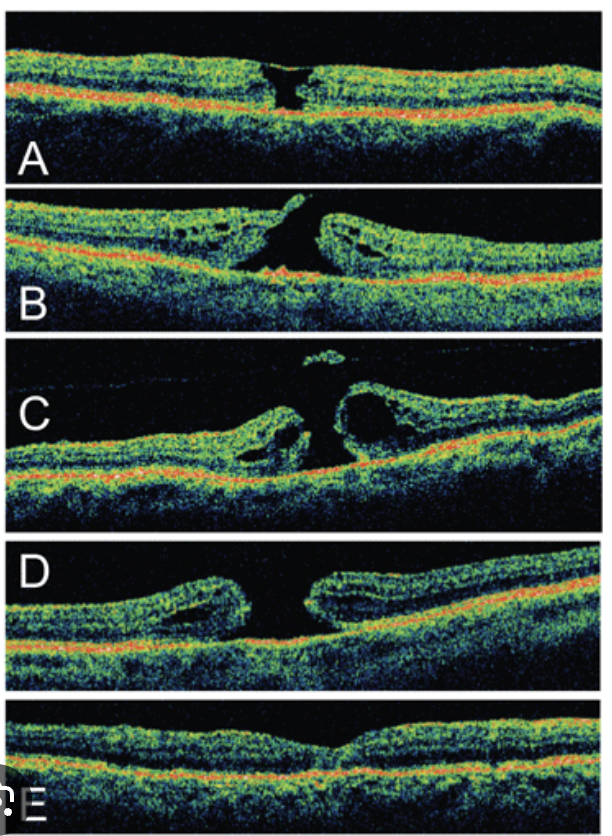
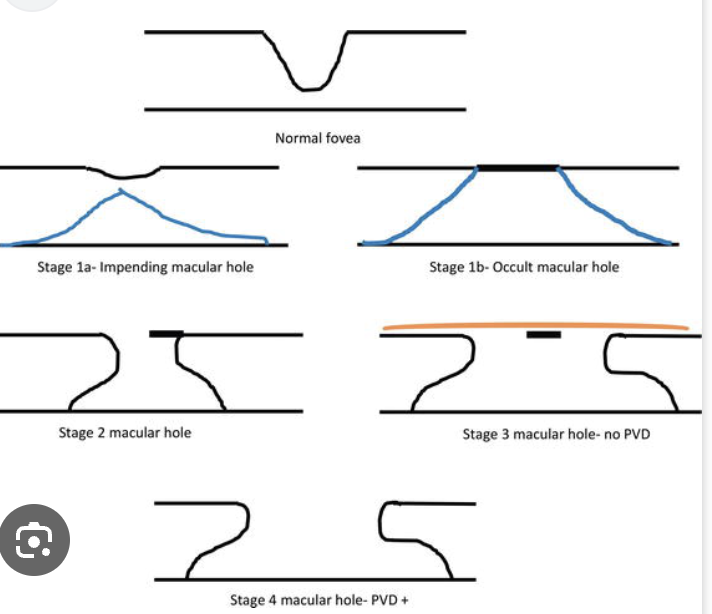
Plan: stage 1: 50% resolve so monitor. '
if a macular hole is getting bigger, getting worse, or causing serious vision problems then recommend pars plana vitrectomy with ILM peel and gas tamponade. Will worsen cataracts.
Consider: Ocriplasmin (recombinant protease that targets fibronectin and laminin, proteins found at the vitreoretinal interface) which works by releasing the vitreous humor from the macula, which can lead to resolution of vitreomacular adhesion and closure of macular holes
RTC q6 months and give amsler grid to monitor for any changes to vision.
Blurred or distorted central vision, Metamorphopsia (seeing straight lines as wavy or distorted), and Reduced color perception.
Lamellar hole: a partial-thickness defect (photoR still attached) in the macula, the central part of the retina responsible for sharp, central vision. (bad VA)
Causes: Chronic CME, characterized by fluid accumulation in the macula, can lead to the formation of a lamellar macular hole. Vitreoretinal traction (pulling on the retina from the vitreous gel), AMD, and Trauma.
RTC q6 months. Observation.
DDx.
Macular Pseudohole - caused by ERM. not full thickness. Caused by ILM contraction around fovea.
Objective: good VA. Notes metamorphosia. ORder macular OCT and do Watze test
blurry or wavy vision, difficulty with reading, and a general decrease in visual acuity.
Epiretinal Membrane/Macular Pucker: collection of cells, primarily glial cells, that form a scar-like tissue on the retina's surface. As the membrane contracts and shrinks, it can distort the retina, leading to blurry or wavy vision, difficulty with reading, and a general decrease in visual acuity.
ERMs often occur naturally with aging, and are more common in people over 50
OTher causes include: PVD, RT/D, trauma, infa
Workup: DFE/OCT macula
Plan: monitor. if become visually significant then refer to retina specialist for membrane peel + Vitrectomy
Dec vision or asymptomatic or Moderate pain/red eye
TRauma? infla? surgery? Red eye?
Choroidal Effusion: Accumulation of blood or subretinal fluid in suprachoroid space.
Objective: Smooth, bullous, orange-brown elevation of retina and choroid. Extends 360 degrees around periphery. Can see ora
Types:
Serous: Associated with operation: wound leak, sclera perforation, bleb.
Trauma - ruptured globe.
Uveitis.
Carotid cavernous fistula
Hemorrhagic: Associated with operation - rupture of SPCAs and anterior displacement of ocular contents.
Can be spontaneous after corneal ulcer.
Workup: B-Scan,
Gonio - RO ciliary cleft -separation of the ciliary body from the scleral spur, creating a direct connection between the anterior chamber and the suprachoroidal space)
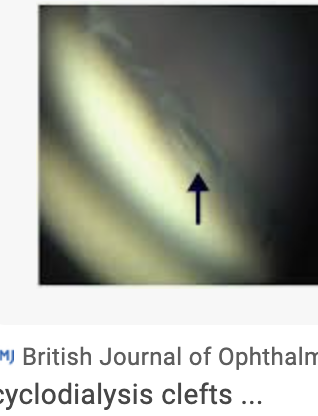
RO rupture by doing seidel sign and look for bleb. DFE to look for subretinal fluid, RD, tumor
Plan: Refer for surgical choroidal drain. If painful red eye and high IOP then brimonidine BID, pred forte 1% QID, cyclo RID.
Reduced night vision, blurry vision, feels like has tunnel vision
Onset?
Retinitis Pigmentosa: RP is most common retinal dystrophy with varying inheritance patterns and is caused by mutations in proteins that are important for photoreceptor function.
Objective: Triad: pale/edematous optic disc, attenuated retinal arteries, bone spicule pigmentation in periphery.
ERM, CME, Keratoconus, PSC + reduced VA earlier in life + May have congenital hearing loss (Has association to Usher syndrome)
Workup: Reduced ERG, Visual field,
Plan: General + Vitamin A (15,000 IU), fish oil and lutein may slow progression. Acetazolamide 250 mg bid if CME present. CE for PSC if indicated.
RTC for routine eye exam
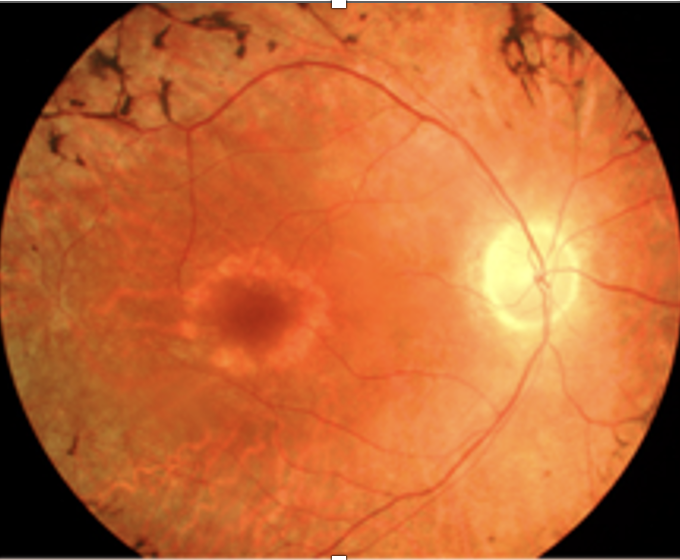
DDx: Leber congenital amaurosis: congenital blindness (looks like RP), has nystagmus, poor pupils, keratoconus. Abnormal ERG
Plan: Recommend gene therapy
Choroideremia: Gene mutation (CHM gene) which disrupts the normal function of the choroid. Choroid is important for providing nutrients and removing waste of the sensory retina → damage to vision. X-linked recessive. males 20 peripheral changes, VA stable till 60s
Objective: Associated with progressive myopia, anhidrosis, skeletal deformities, congenital deafness, dental deformities, hypopituitarism.
Ocular: Pig granules and RPE atrophy. Later, absence of RPE and choriocapillaris. Optic atrophy. PSC, CME
Workup: Abnormal ERG/EOG. FA hypo for choriocap loss, + neo if present. FAF hypo for choriocap loss
Plan: General + avoid smoking. Educate Slow prog then rapid VL in 5th -7th decade.
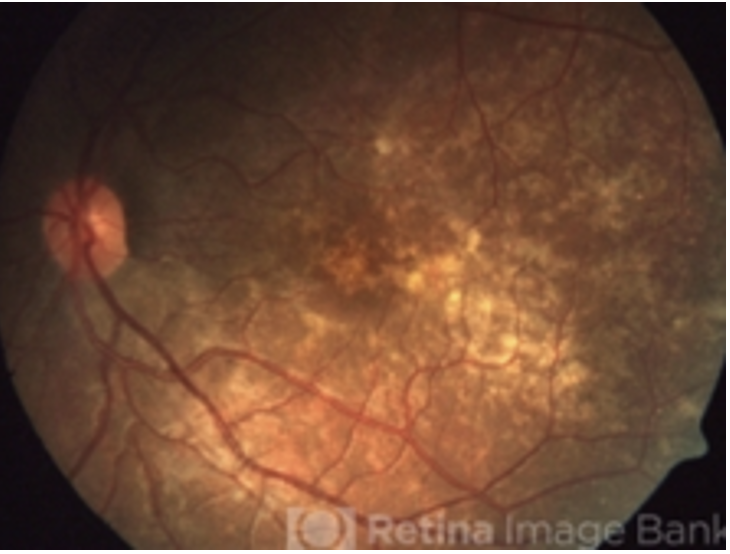
Gyrate Atrophy: AR, deficiency in the enzyme ornithine aminotransferase (OAT), which leads to an accumulation of the amino acid ornithine in the body - damage to the retina
Objective: well defined and scalloped atrophic borders, PSC, progressive myopia, age of onset around 10, PSC
Workup: Abnormal then absent ERG, FAF hypo spots w hyper border, OCT: CME
Plan: Recommend An arginine-restricted diet (nuts, seeds, and certain meats) and vitamin B6 supplements can help slow the progression of GACR. Educate patietn that will get slow profressive vision loss.
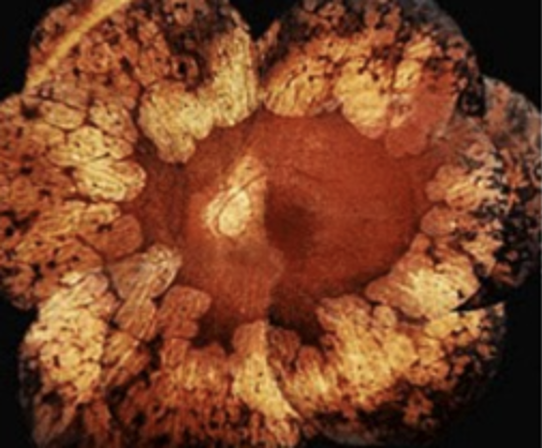
Albinism (X-lined Recessive) - genetic condition that causes a partial or complete absence of melanin, the pigment that gives color to skin, hair, and eyes.
Objective: nystagmus, TID, foveal hypoplasia, 20/40 to 20/400, may have ET strab
Plan: General + contacts/ sun protection/ strab surgery/prism if needed
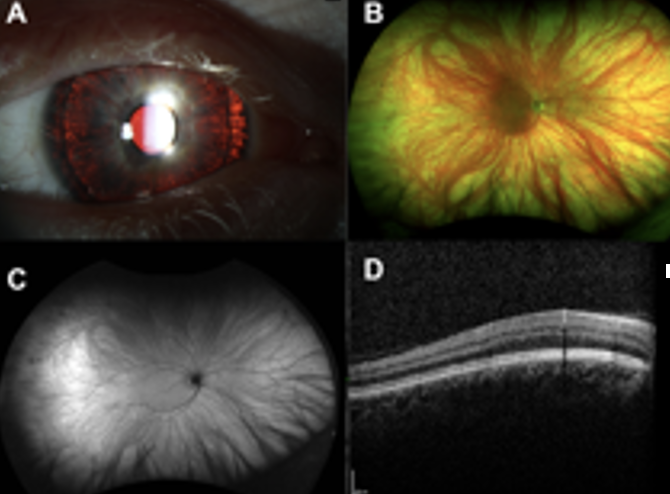
Workup: OCT macula, Visual field, DFE, Fundus photo Genetic Testing, ERG, EOG, blood work (measure ornithine levels)
General Plan: Recommend Referral for low vision consult and genetic counseling. Recommend UV protection. RTC for routine eye exam.
Reduced Central vision/color vision, central vision field loss, metamorphopsia
Cone Dystrophy: caused by mutations in genes that encode proteins essential for the function and survival of cone cells.
Objective: Nystagmus, temporal pallor, pigment clumps in macula
Old: Bullseye macula or geographic atrophy. (early looks normal but poor VA)
Workup: Abnormal ERG for photopic, normal for rods.
Plan: tinted lenses, genetic counseling, low vision aids. RTC for annual exam
Stargardt: Most common hereditary macular disease (AR). Caused by accumulation of a fatty, yellow pigment called lipofuscin in the cells within the macula.
'beaten-bronze' appearance, surrounded by yellowish flecks + geographic macula in bullseye pattern in later stage
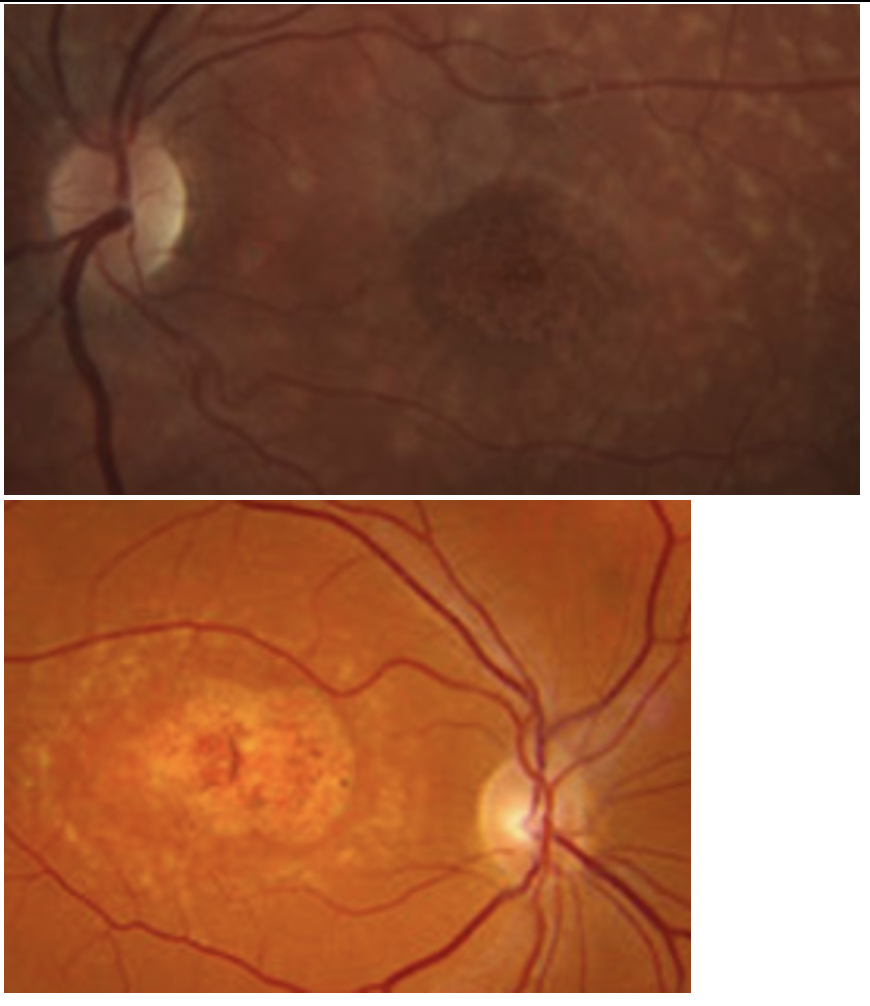
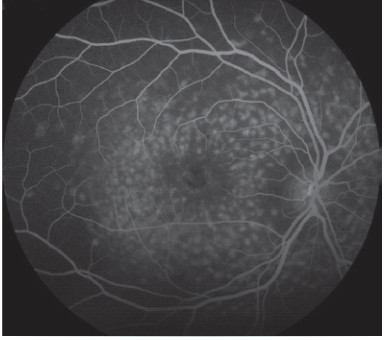
Workup: normal ERG, EOG (abnormal), DFE, HVF, FAF (see lipofuscin), OCT (shows diorganized PR + outer retinal atrophy) Fundus photo, IVFA to see blockage of choroidal fluorescence
Plan: Referral low vision consult + genetic counseling. UV protection + AVOID vitamin A supplementation
Stargardt variant Variant: Fundus flavimaculatus (AD macular dystrophy): Lipfusion spread throughout whole posterior pole. VA normal unless GA present. Caused by accumulation of lipofuscin in the retinal pigment epithelium (RPE) due to mutation.
Plan: no more than recommended Vitamin A amount. Eat fish, leaft greens, fresh fruit, nuts and limit fats and oil time improve retinal function. (diet rich with antioxidants)
RTC for routine eye exam
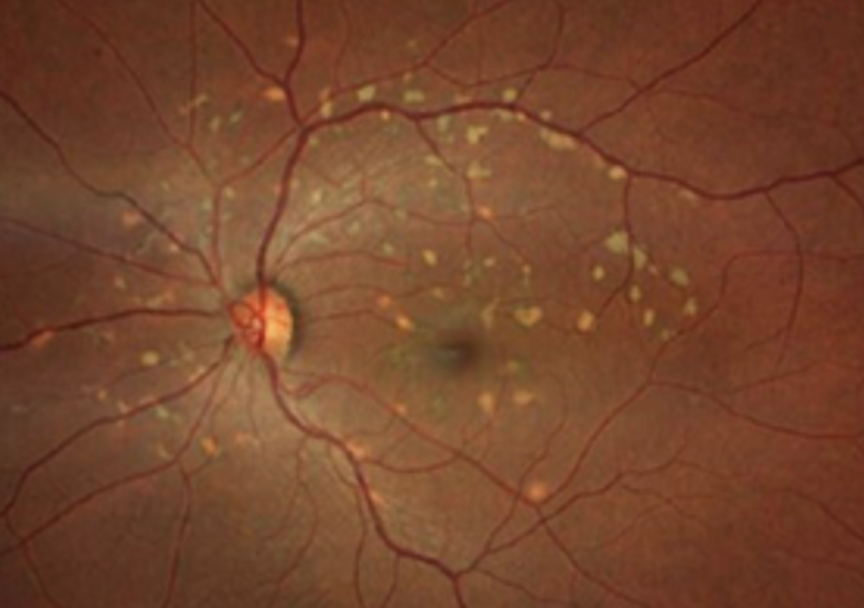
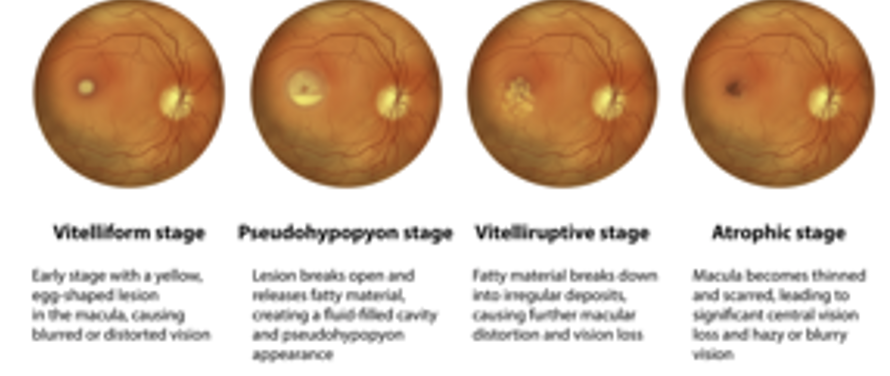
Best Disease (AD): Hereditary macular disease causing RPE dysfunction resulting in progressive macular degeneration. By 50s, may lead to permanent vision loss bc CNVM
Objective: yellow egg shaped lesion at macula
Work up: Abnormal EOG, normal ERG, FAF if suspect CNVM
Plan: Monitor vision with Amsler grid. Polcarb lenses. Refer to retina for Anti -VEGF treatment
RTC q6months or as indicated by retinal specialist
DDx. Vitelliform macular dystrophy: later age of onset, smaller lesion and normal EOG. Same stages
Familial drusen: caused by mutations in genes involved in the metabolism of extracellular matrix proteins, which accumulate in the retina as drusen. Appears in 30s. can be moderate and have bigger drusen around posterior pole
No change in VA, may have CNVM in 50s so monitor with amsler grid. Referal to retinal if indicated
RTC for routine eye exam or as indicated by retinal specialist
Salt and pepper fundus
Kearns Sayre: progressive genetic disorder causing mitochondrial dysfunction. Leads to CPEO (EOM/ptosis), pigmentary retinopathy, heart conduction defects, short stature.
Refer to cardiologist for ERG and management of heart condition.
Syphilis: a sexually transmitted infection (STI) caused by the bacterium Treponema pallidum, that can be treated with antibiotics, but if left untreated, it can cause serious health problems and even death.
Normal ERG normal. Order syphilis blood work up
Rubella: rubella virus, which is spread through respiratory droplets from infected individuals. Causes microphthalmos, cataract, deafness, a congenital heart abnormality
Medications: phenothiazine, thioridazine, and chlorpromazine.
Reduced ERG
Asymptomatic at first. Later, decreased vision, color vision, and dark adaptation.
Chloroquine, Hydroxychloroquine, Plaquenil retinopathy
Objective: Bulls eye macula, loss of foveal light reflex. Ring of depigmentation surrounded by a ring of increased pigmentation
Other signs: Whorl keratopathy, CME, visual field defects central, paracentral, peripheral, poor dark adaptaion
Workup: FAF (dark due to RPE loss) 10-2 HVF, ERG + EOG Abnormal, OCT Macula (flying saucer sign due to disrupted outer layers + loss of foveal contour and RPE atrophy)
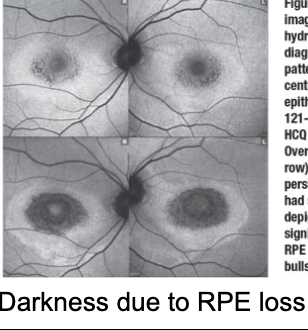
Plan: Baseline eval in first year. RTC yearly to monitor for toxicity. Discontinue if indicated.
DDx: Stargardt (younger + pisciform lesions), Cone dysrophy (younger, photophobic, abnormal photopic ERG)
Sudden vision loss in one eye, asymptomatic in other eye
Foster Kennedy syndrome
Optic disc pallor in one eye in conjunction with disc edema in the contralateral eye caused by an intracranial mass.
Workup: VF, color test, pupils
Order MRI to confirm intracranial mass, refer to neurosurgery for resection.
Follow up monthly for DFE to monitor optic nerve edema resolution.
Dec vision or none
Hx of drug use? Breast cancer? Medications like Tamoxifen? Oral tanning agent?
Crystalline retinopathy - crystals accumulate intraretina which can cause damage to the retina
ischemia can lead to neo/mac edema/vit heme/RD
Workup: DFE, whorl keratopathy (CHAI Tamoxifen), doppler or echo
Imaging: OCT, FA to determine non-perfusion/neo
Plan: Stop causative agent. Consider Anti-VEGF if neo.
DDx. Hard exudates (associated with conditions like Dr.VOS, surrounds retinal vessels, not IN it). Calcific drusen found in Dry AMD subretinal, not intravascular.
Optic Pit is a congenital abnormality that causes a small, oval-shaped depression, often located on the temporal side of the optic disc, that can lead to fluid accumulation and vision problem
Objective: gray, yellow or black round depression on optic nerve temporally or centrally. Can lead to serous detachment or retinoschisis
Workup: DFE, IOP, baseline VF, OCT
Plan: Monitor annually. monitor for any visual changes using amsler grid. If changes occur RTC due to risk of macular hole. Referral to retinal opthomologist for management of serous detachment (laser treatment or PDT)
Notes dec vision, central or paracentral scotoma, dyschromatopsia, metamorphopsia. One or both eyes. VA 20/25-20/200
Hx of sun gazing or welding? Playing with laser when younger?
Solar Retinopathy vs Phototoxic injury: permanent damage to the central part of your vision from staring at the sun or laser/welding. Vision may recover, but by have blind spot/dark spot in vision where damage is located.
Objective: window defect
Workup: OCT macula (shows hyporeflective at RPE and IS/OS junction)
Plan: Observe. RTC annual exam
Choroidal nevus vs choroidal melanoma
Nevus: flat (<2mm thick), overlying drysen, <5mm diameter, well defined borders, no hyperautofluourescne on FAF, disappears with red free.
Melanoma: high risk charactersitics: TFSOMUHHD. If four or more factors are present, 50% chance likely to be melanoma.
Thickness > 2mm.
Subretinal fluid.
Symptoms: photopsia, red vision.
Orange pigment - lipofuscin
Margin within 3mm of disc.
Ultrasound hollowness or thickness
Halo absence.
Diam > 5mm
Workup: FAF (lipofuscin hyper autofluorescence), DFE, OCT (subretinal fluid, also has shaggy photoreceptors). B-Scan (mushroom) to measure thickness.
Plan: initally 3-4 months to look for change then annually. If more then 1mm growth per year then inc risk of melanoma formation
Refer for fine needle biosy then for tx laser/enucleation/radiation to oncology specialist
DDx: CHRPE (flat, crisp margins, usually temporal, depigmented lacunae within lesion, asymptomatic
DDx: Melanocytoma of nerve: black nerve lesion, grows, benign, caused by uveal melanocytes, congenital. (+)APD, enlarged blind spot/arcuate defect, FAF shows hypofluoresence
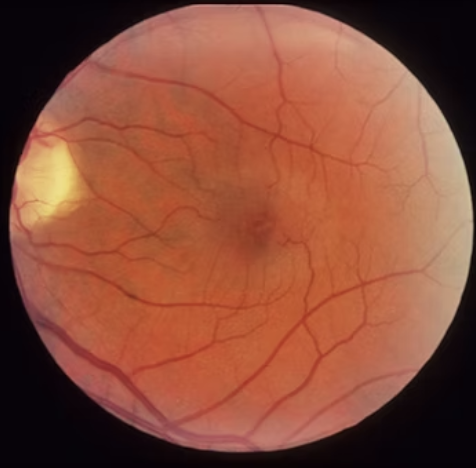
Gradual progressive blurry vision
Macular Telangiectasia: abnormal retinal vasculature abnormality that can cause vision loss, macular edema/exudates, ILM drape, MA, capillary nonperfusion → tortuosity in retinal capillaries.
Type 1: Rare, associated with Coats' disease, typically affects a single eye in male patients.
Type 2 (MacTel): More common, bilateral, and leads to a gradual loss of central vision.
Workup: macular OCT
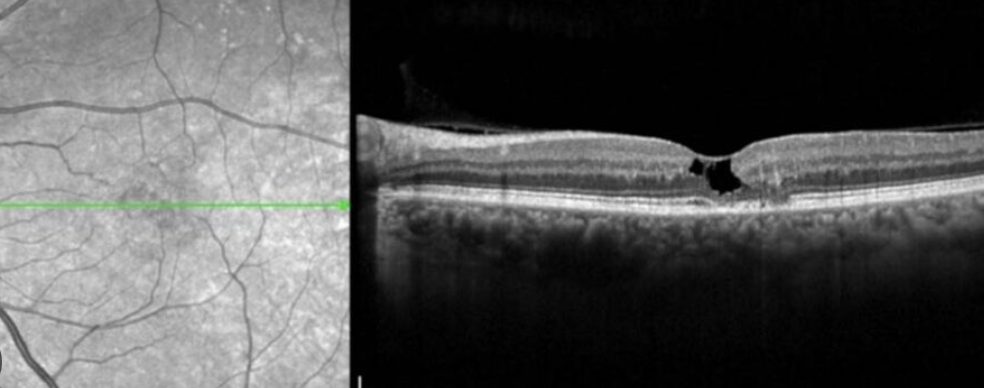
Plan: monitor/observe, Consider Encapsulated cell therapy to slow progression of disease. (40’s and 50s is when notice, gradual vision loss)
First image: Asteroid Hyalosis: consists of multiple vitreous floaters made up of calcium and phosphate crystals. This condition is often associated with diabetes, hypertension, and high cholesterol
Objective: unilateral, older, moves with eye movement, doesn’t gravitate downwards like synchesis scintillans
Plan: RTC 10-12 months, referral to PCP to follow up on diabetes, hypertension, and high cholesterol
DDx: Synchysis scintillans: cholesteral accummulation in the vitreous. Associated with chronic vitreous hemorrhage, chronic retinal detachment, or other ocular conditions like chronic inflammation, hyphema, or trauma.
Objective: bilateral, young, gravitates downward. Treat underlying dx.