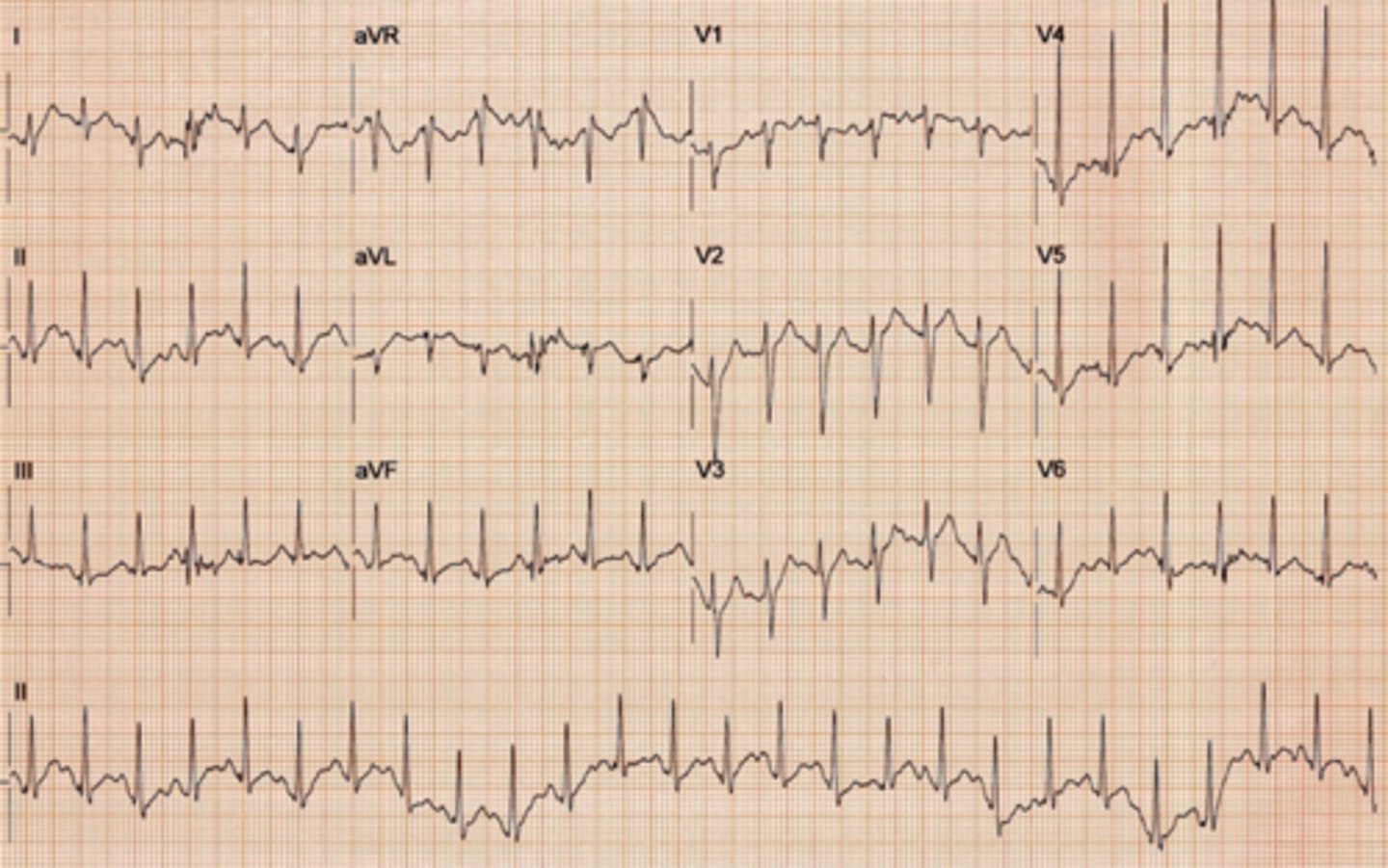
KINE 4415 Test 2: ECG's
1/101
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
102 Terms
Atrial flutter
Originates in an ectopic pacemaker site in the atria, depolarizing at a rate of 250 - 350 beats/minute. The abnormal P waves produced resemble the teeth of a saw (sawtooth deflections). Regular P wave rhythm, R-R rhythm may be regular or irregular.).
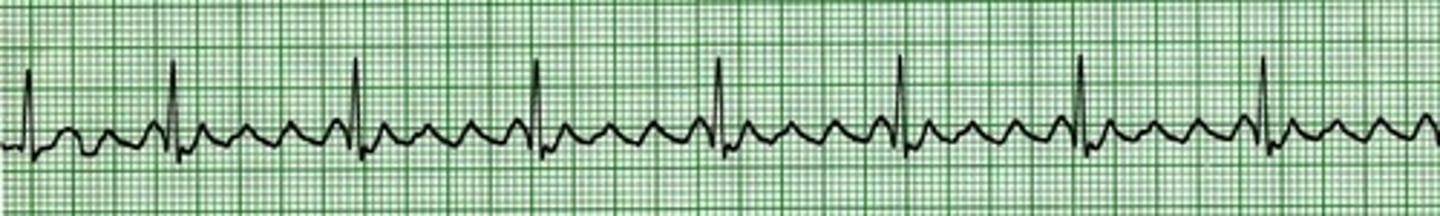
Facts about atrial flutter
•Chronic atrial flutter is uncommon. It usually converts to either atrial fibrillation or sinus rhythm spontaneously or following treatment.
•This rhythm is most likely caused by a reentry circuit.
•Atrial flutter is common after heart surgery. Other causes include valvular heart disease, ischemic heart disease, pulmonary embolism, and alcohol intoxication.
Potential dangers
•There may be a decrease in cardiac output if ventricular rate is rapid.
•Mural thrombi may form due to ineffective atrial contractions and blood stasis, leading to a risk of systemic or pulmonary emboli.
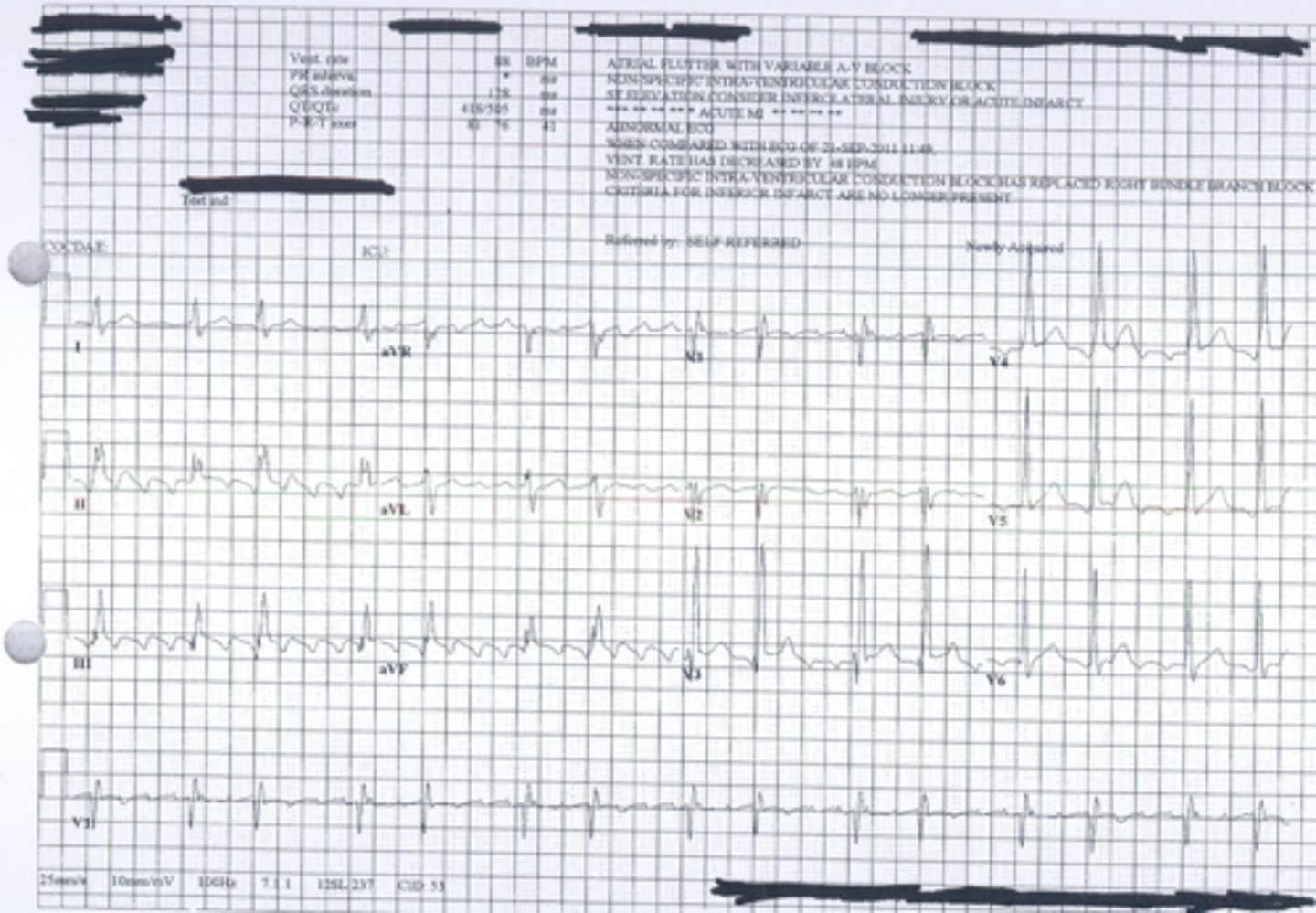
Atrial Fibrillation (controlled rate)
Atrial Fibrillation: A rapid and highly irregular heart rhythm originating in an ectopic site in the atria, depolarizing at a rate greater than 500 beats/minute. The AV node generates and irregularly irregular ventricular rhythm.
Due to the turbidity of the blood moving through the valves blood clots are a common problem with Atrial Fibrillation. You should not exercise or test an Afib patient if they are not already on a blood thinner.
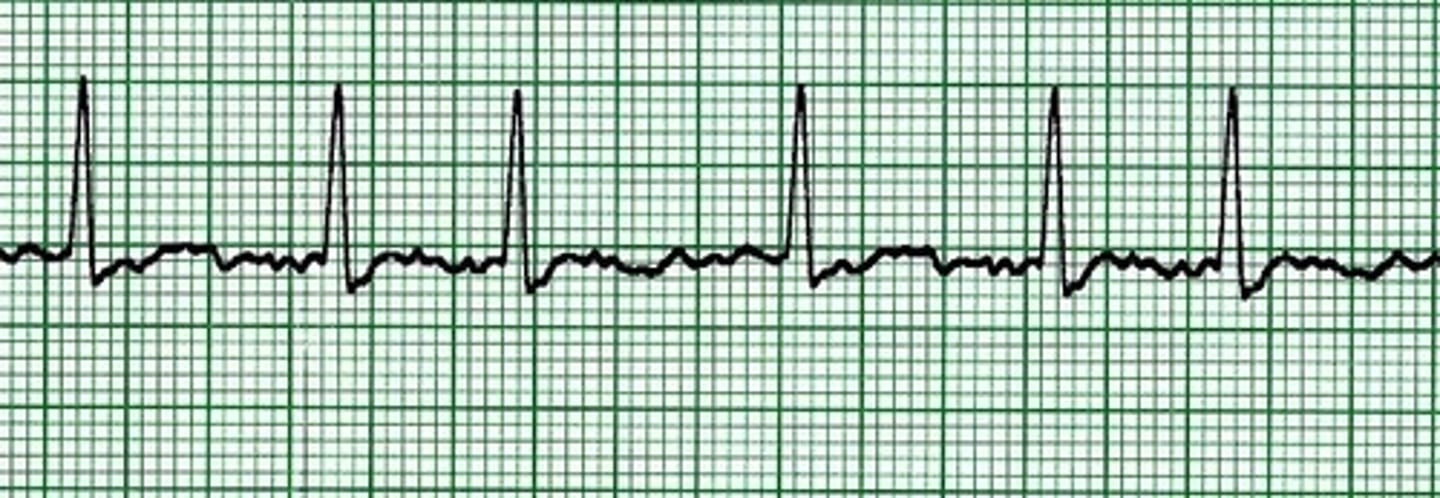
atrial fibrillation
Rhythm: Irregular
Rate: Atrial: Not measurable
Ventricular: 50 beats/minute
P waves: Fibrillatory waves present
PR interval: Not measurable
QRS complex: 0.10 second.
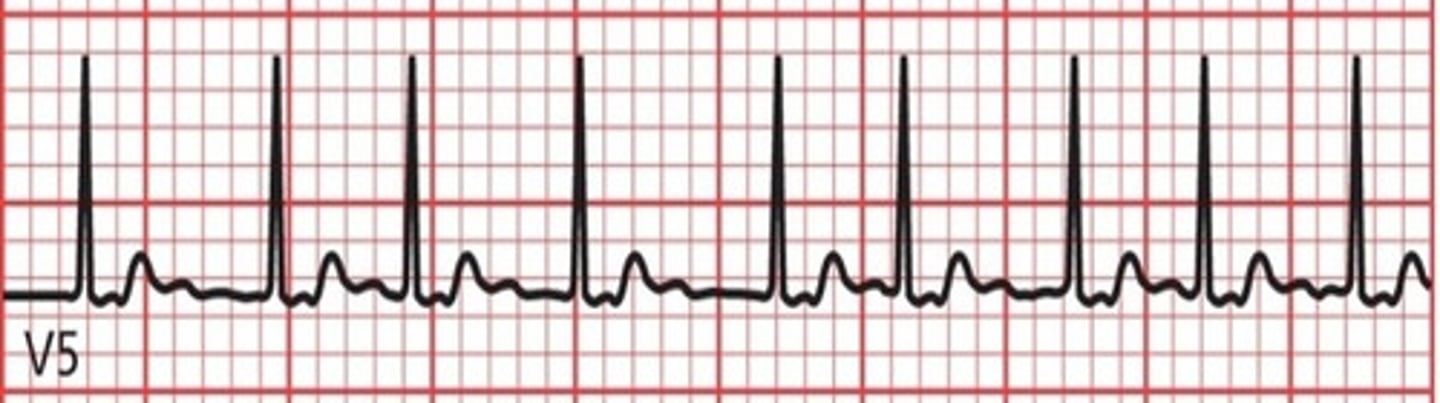
atrial fibrillation
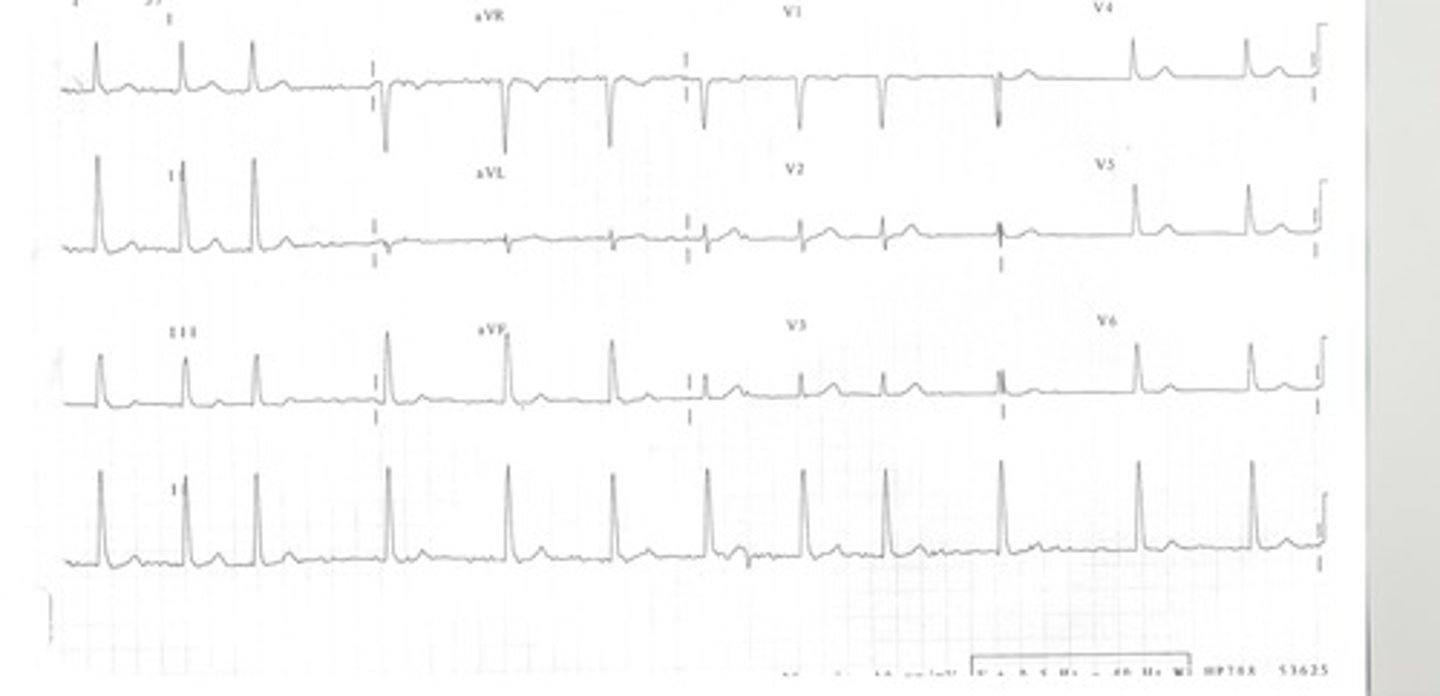
atrial fibrillation
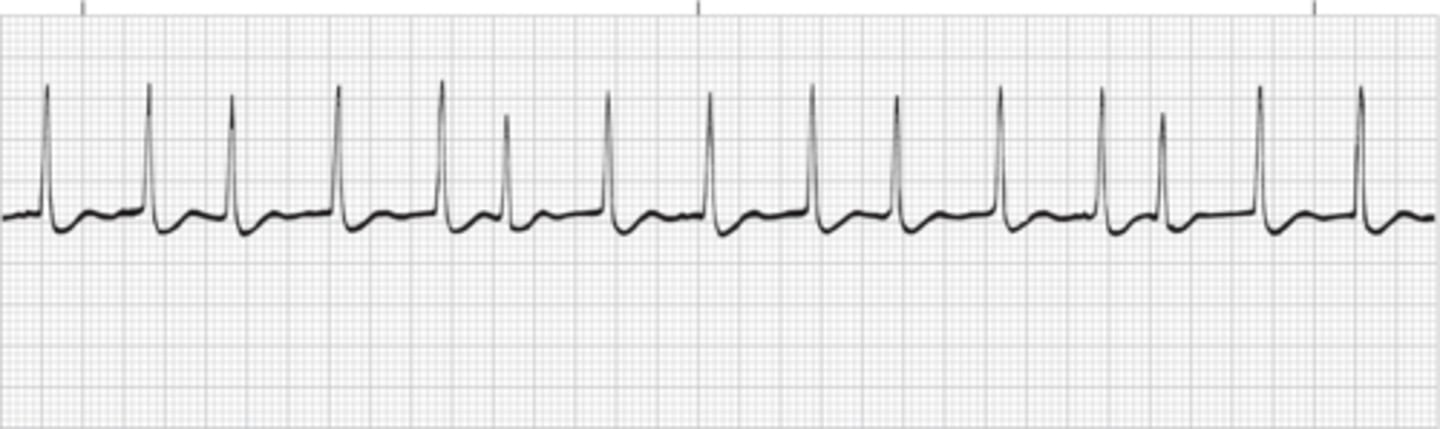
Atrial Fibrillation (A-Fib)
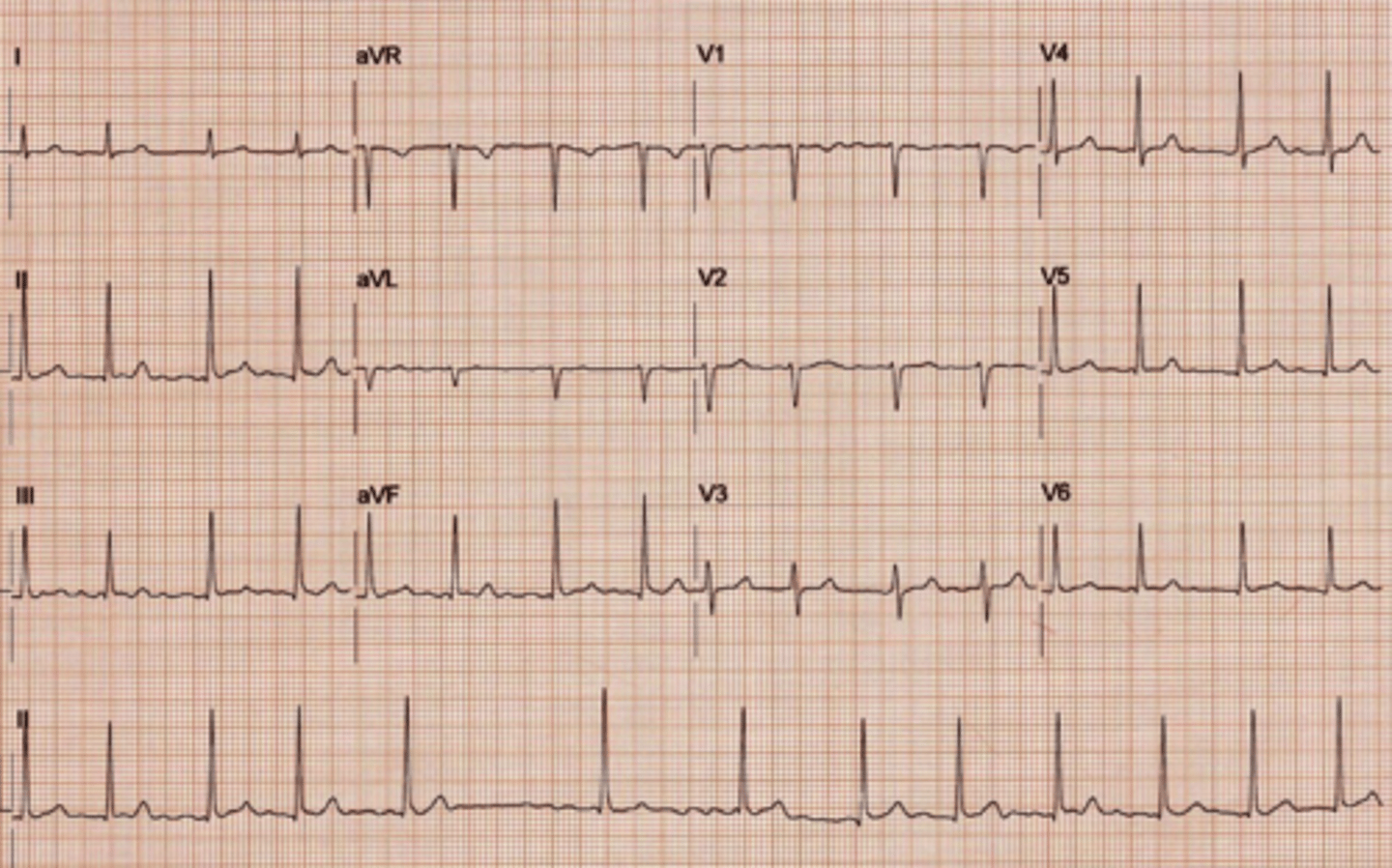
Atrial Flutter
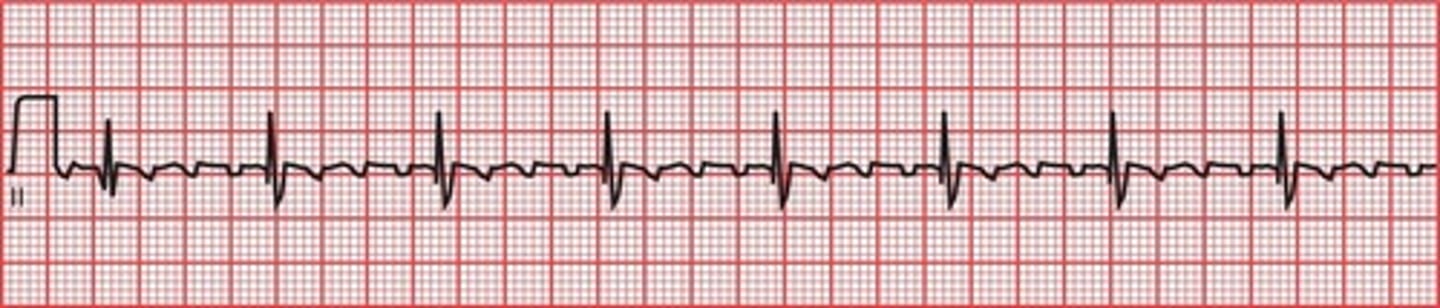
Asystole (ventricular standstill)
A state of no electrical activity
Causes
•Advanced heart block
•V-tach and ventricular fibrillation refractory to resuscitative measures
•Extensive myocardial damage, massive pulmonary embolus
•Hyperkalemia, hypothermia, drug overdose
•Cardiac trauma
Treatment
•Start CPR; establish IV lines; intubate when possible
•Epinephrine 1 mg IV push (may repeat every 3 to 5 minutes)
•Treat underlying reversible causes

atrial paced rhythm
Single lead atria
Pacemakers are needed when the heart beats to slow to meet the demands of the body.
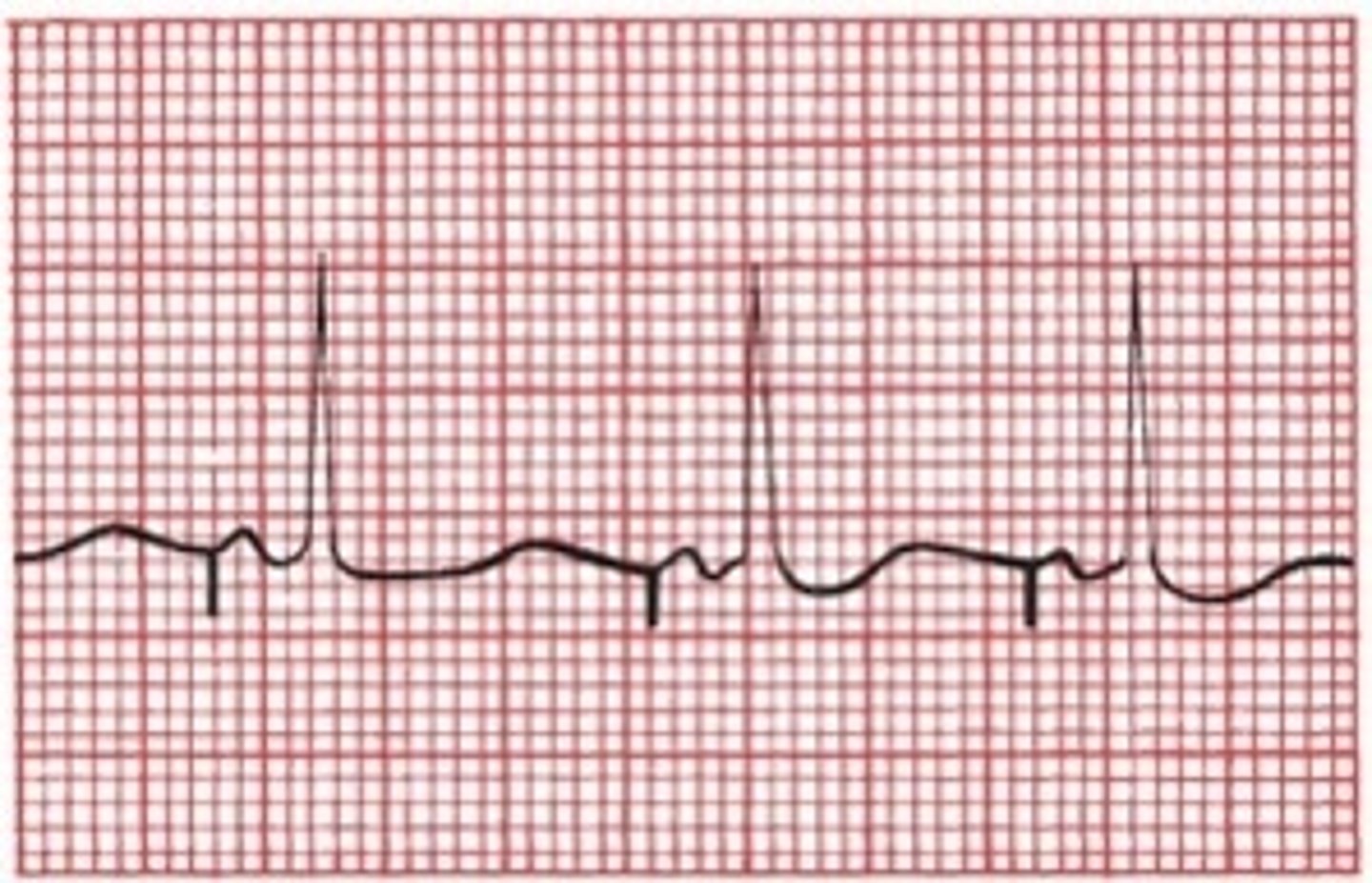
atrial paced rhythm
- spike before P wave
- QRS narrower
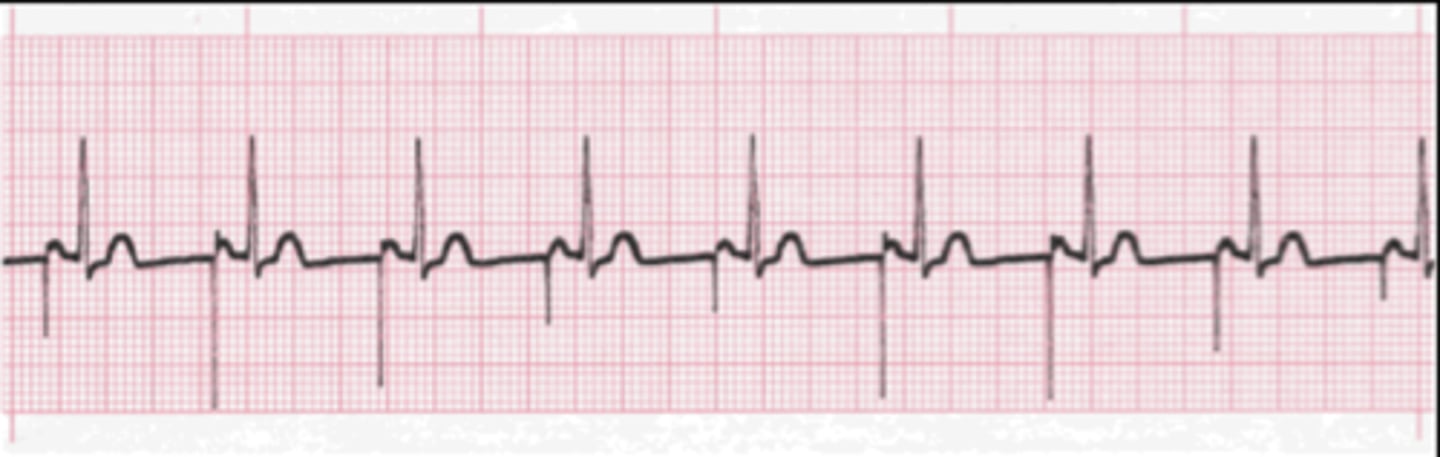
atrial paced rhythm
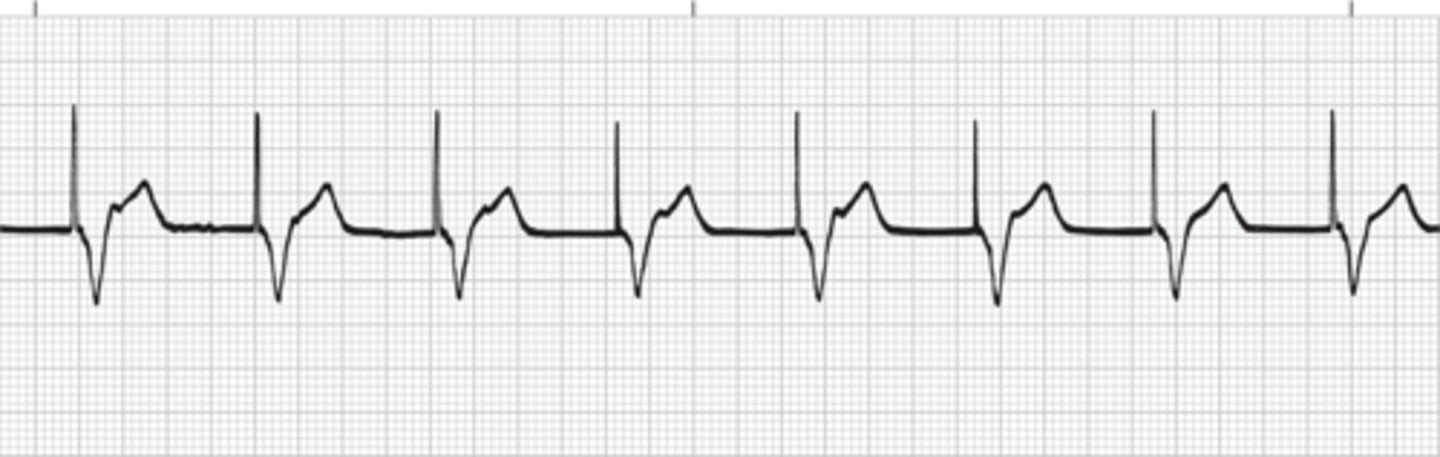
Ventricular bigeminy
When every other beat is a PVC
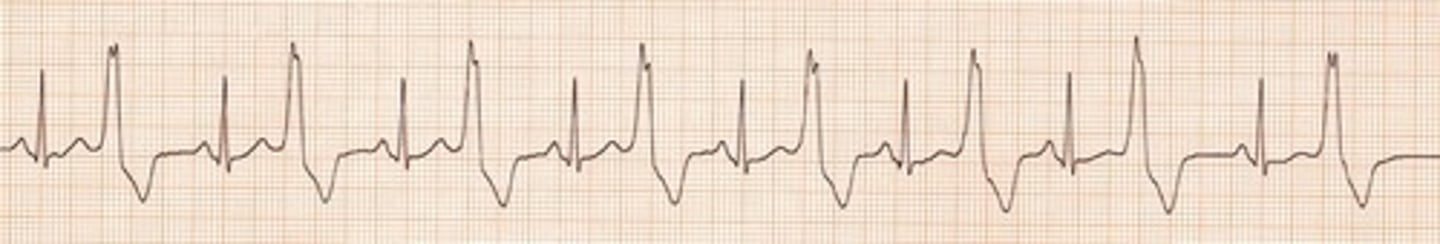
Trigeminy
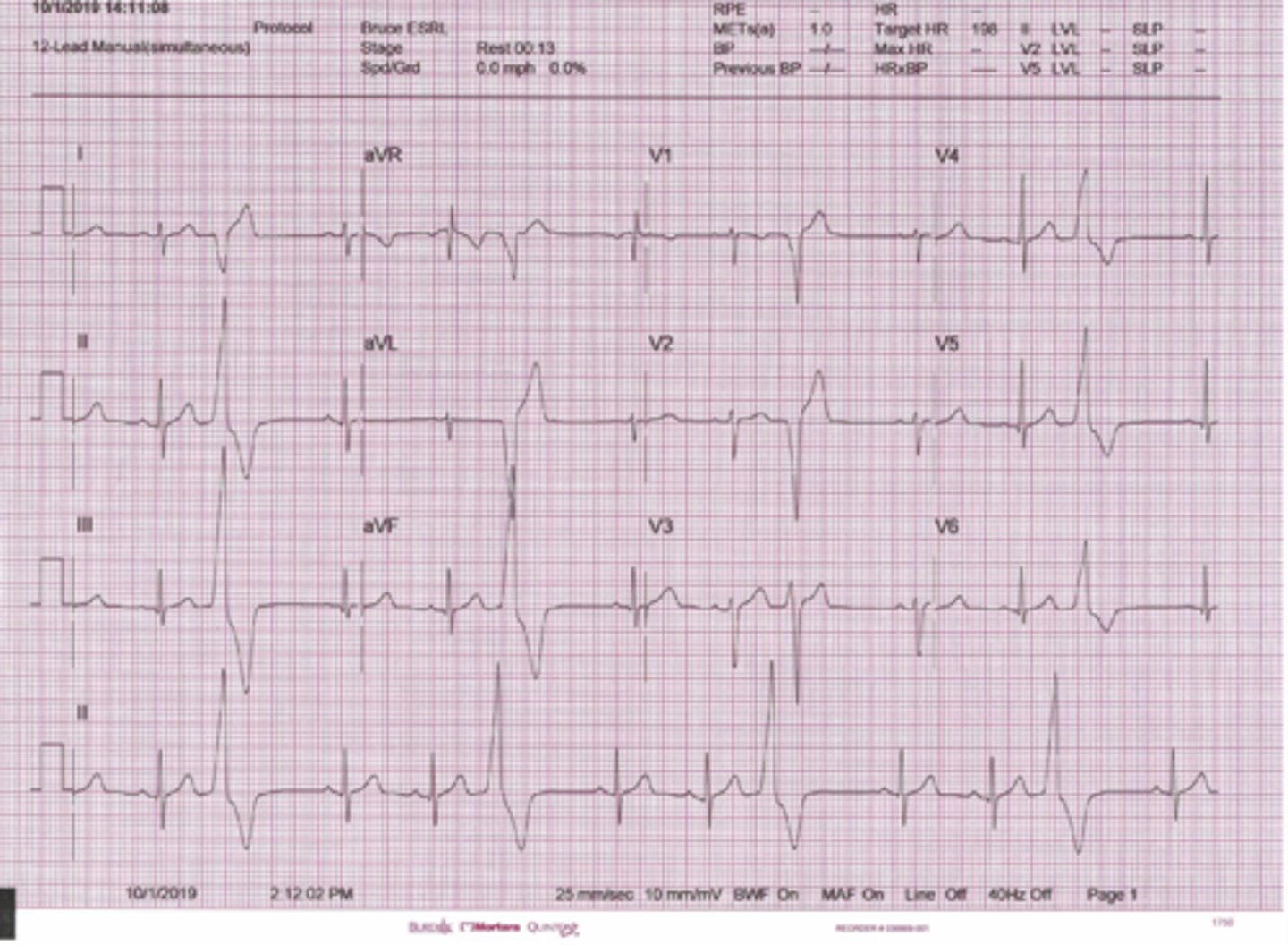
Sinus Bradycardia
P wave is upright
PR interval is 0.16 seconds or 4 boxes
QRS is less than 0.10 seconds long or less than 2.5 boxes.
T wave is upright
Rhythm is regular
Heart rate is 60 or below
Low HR often seen in endurance-trained subjects and patients taking beta-blockers
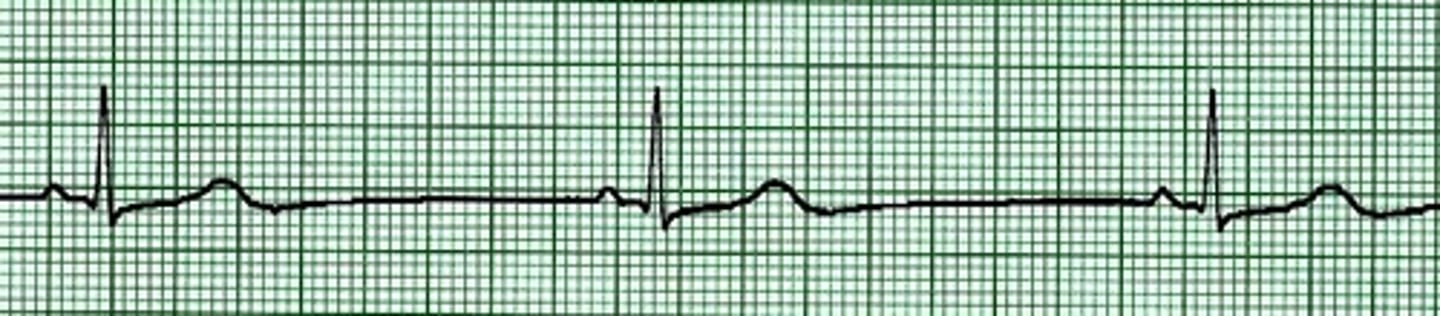
multifocal couplet
-When 2 different looking PVCs occur one after the other
-Each PVC is likely originating from a different ventricular site
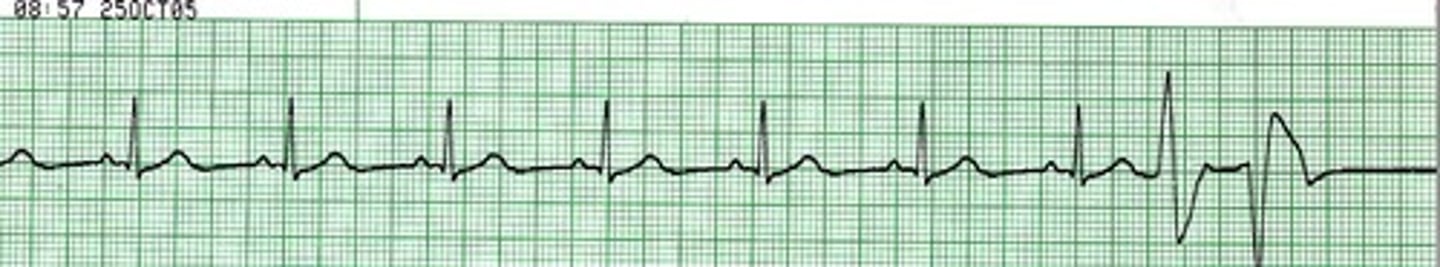
1st degree AV block
prolonged PR interval >0.2 sec
Impulses are delayed in the AV node, but all are conducted to the ventricles.
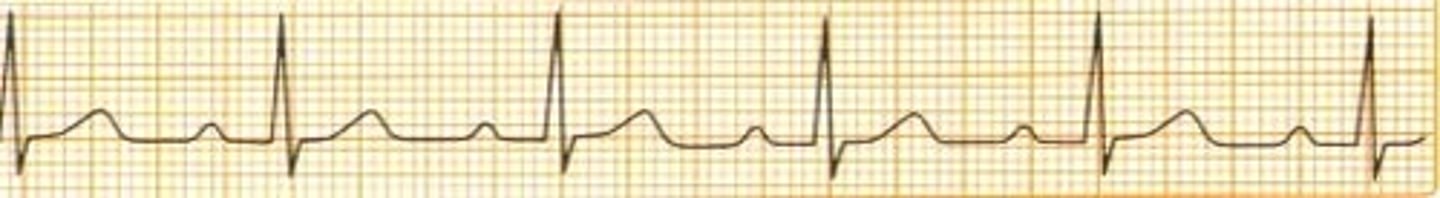
1st degree AV block occurences
•Myocardial infarction, especially inferior wall MI
•Coronary heart disease
•Hyperkalemia
•Increased vagal (parasympathetic) tone
•Effects of drugs such as beta-blockers or calcium channel blockers
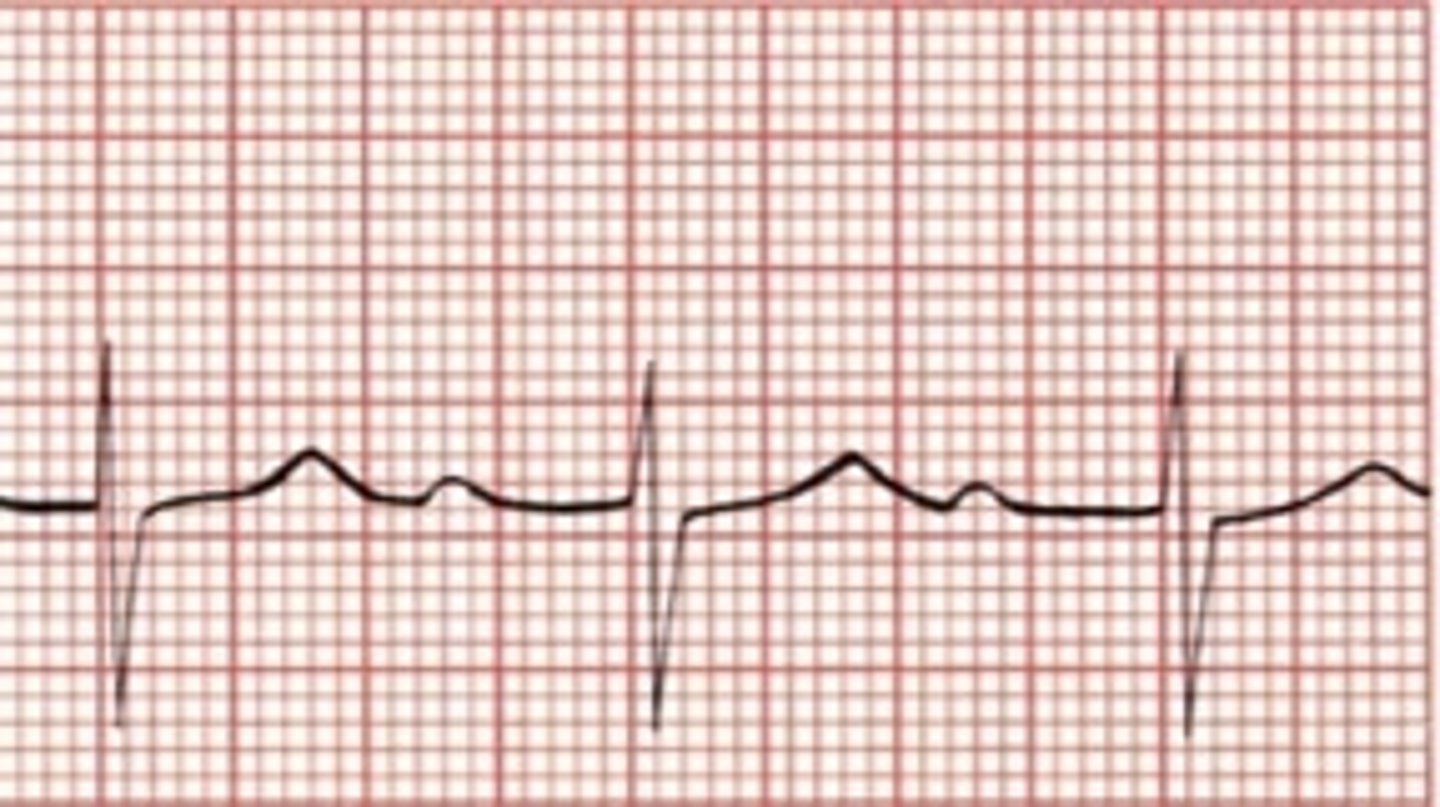
Left bundle branch block (LBBB)
•Wide QRS complex > 0.12 seconds.
•Broad (typically notched) R wave with prolonged upstroke in leads V5, V6, I and aVL with ST segment depression and T wave inversion.
•Reciprocal changes in V1 and V2
•Left axis deviation may
also be present.
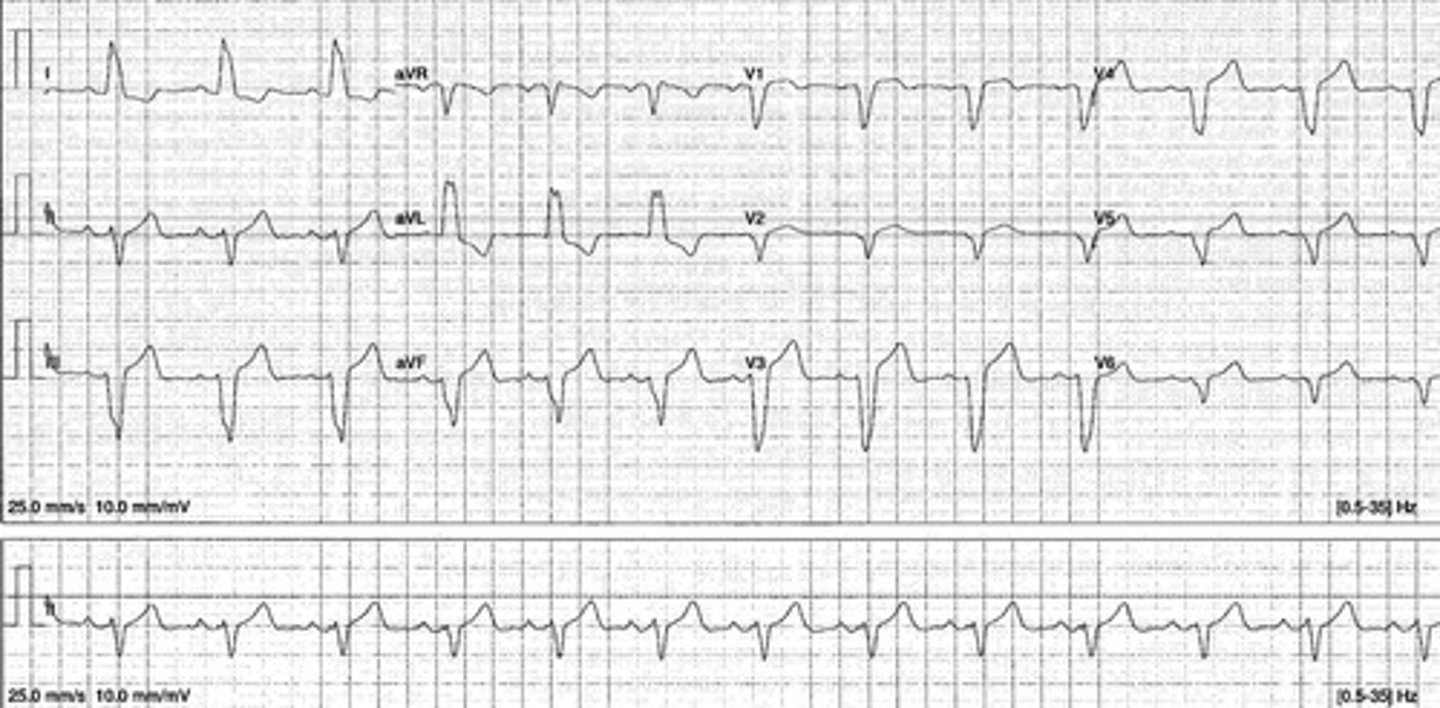
left bundle branch block
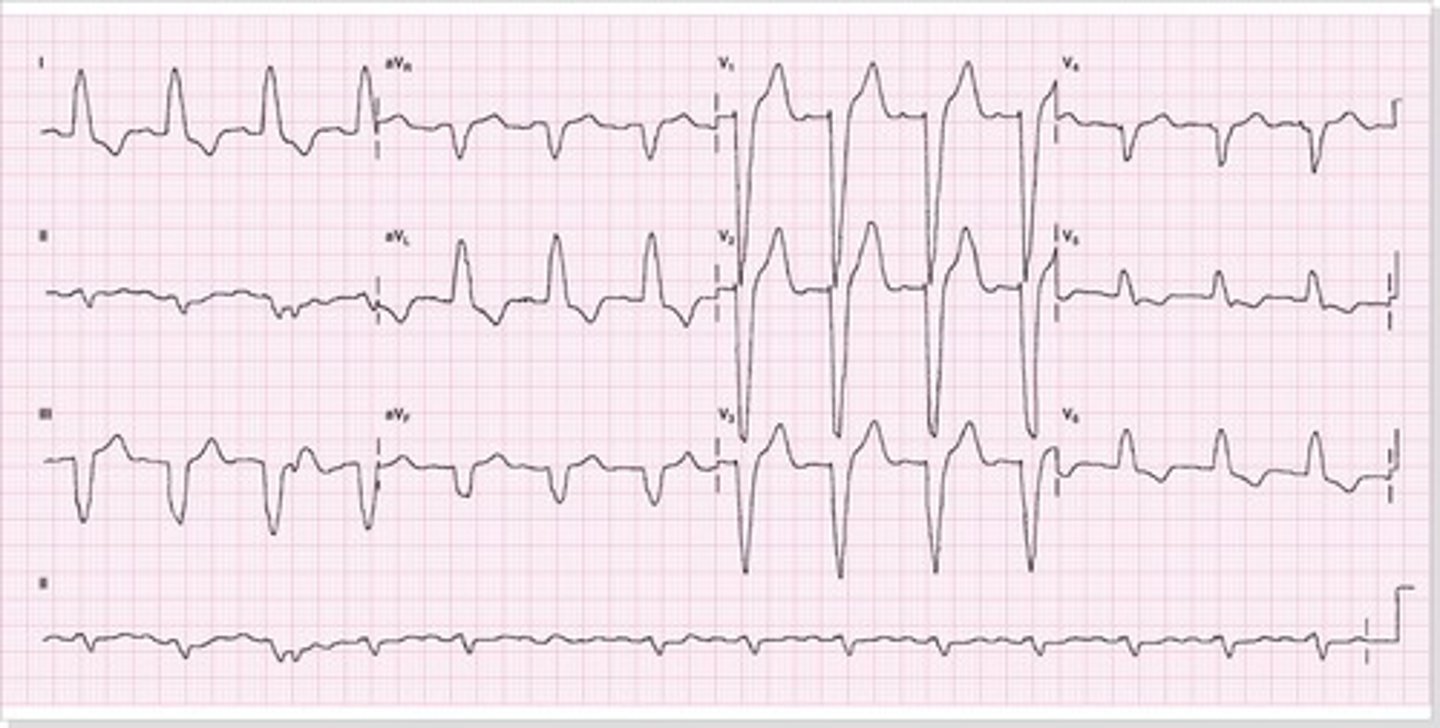
left anterior fascicular hemiblock
•results in leftward shift of electrical axis (-45 to -90 degrees) toward pathologic left axis deviation.
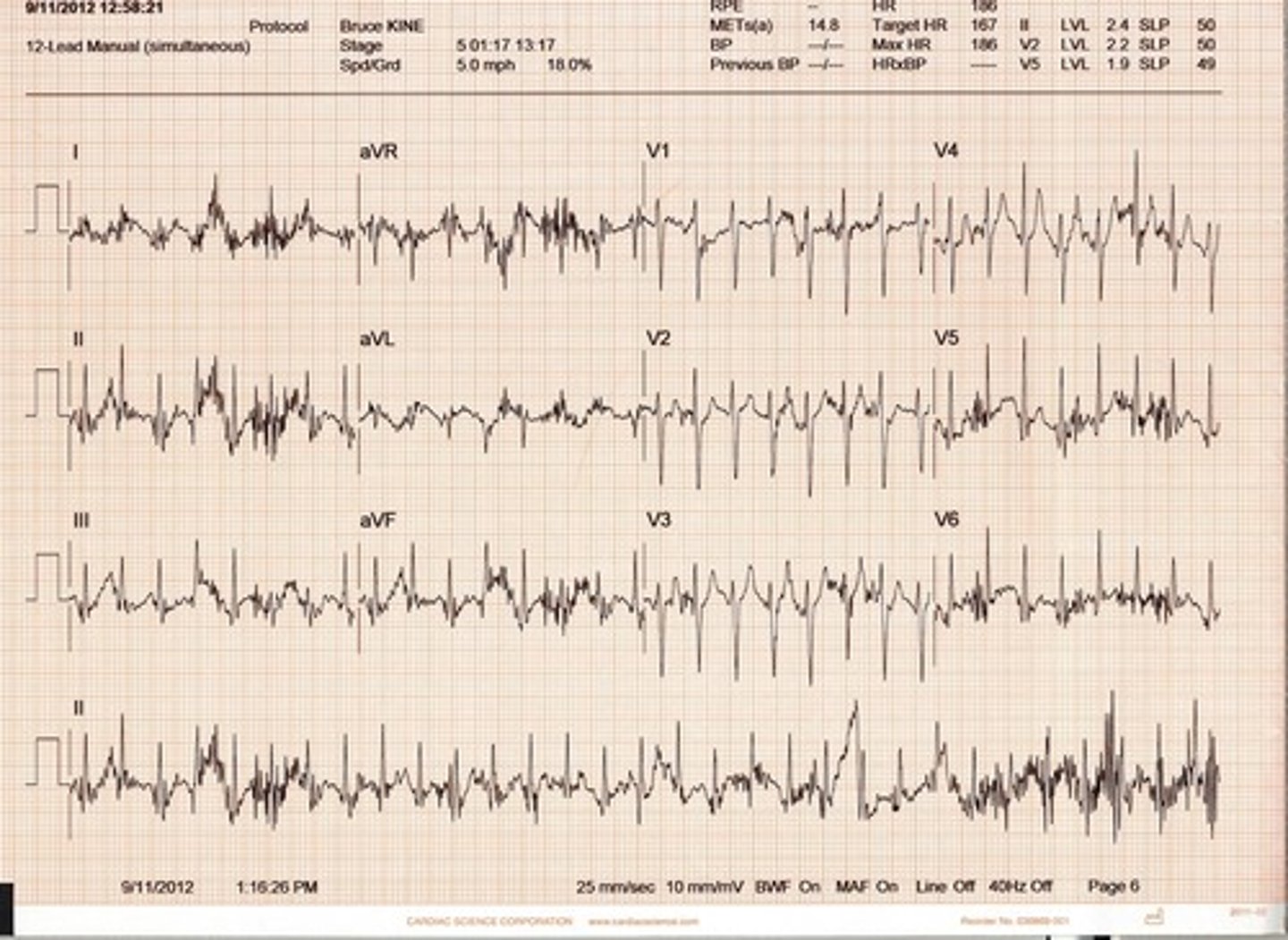
Muscle artifact
fuzzy, irregular baseline
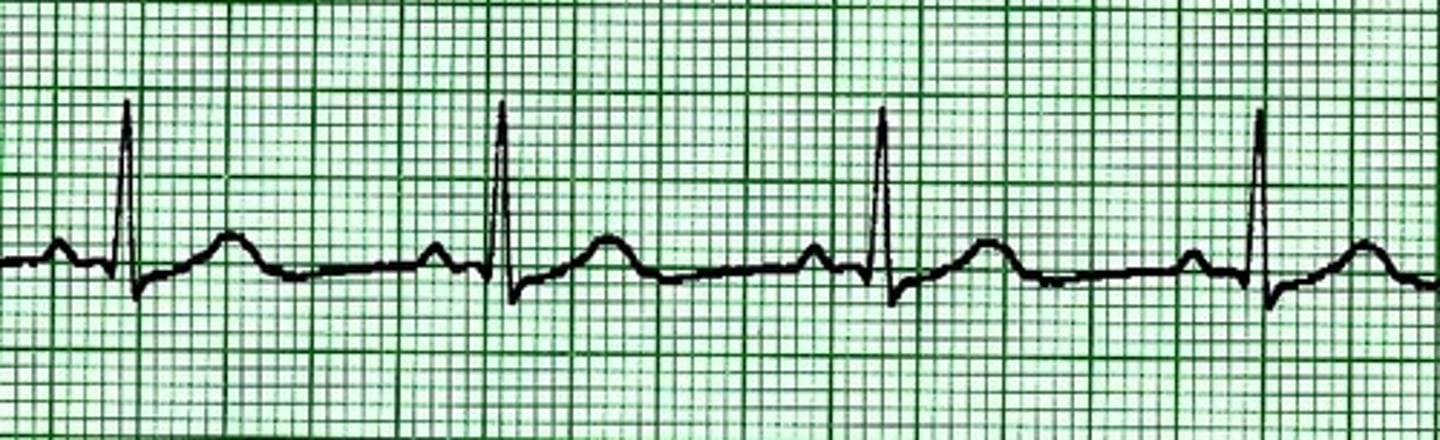
normal sinus rhythm
The following are the normal parameters for each part of the ECG wave. Remember each small box across is = to 0.04 seconds and vertically = 1 mm
PR Interval: 0.12-0.20 seconds. Normal P wave is upright.
QRS complex: 0.06 - 0.10 seconds. Normal QRS is narrow meaning the beat was initiated at or above the AV Node. In some cases the complex may be narrow if it is initiated in the Bundle of HIS just below the AV node. Ex: Third degree heart block with a narrow QRS.
QT interval: 0.36-0.44 seconds. Prolonged QT can lead to Torsades and may be due to hypokalemia or hypocalcemia.
T wave should be upright. It will start slow and end fast. Inverted T waves may be caused by ischemia.
ST segment should be on the isoelectric line. 1 mm ST depression = ischemia. Greater than 1 mm ST elevation may mean ia myocardial injury with the exception of early repolarization of the ventricles in young athletic individuals. If you are young and athletic and do not have this on your ECG it is not a slight against you. Just an occasional normal variance.
Rhythm: Each R wave is equal distance apart. No more than a 4 boxes apart still means normal.
Rate for NSR is between 61-99 bpm.
Bradycardia is 60 or less bpm. Tachycardia is 100 and above.
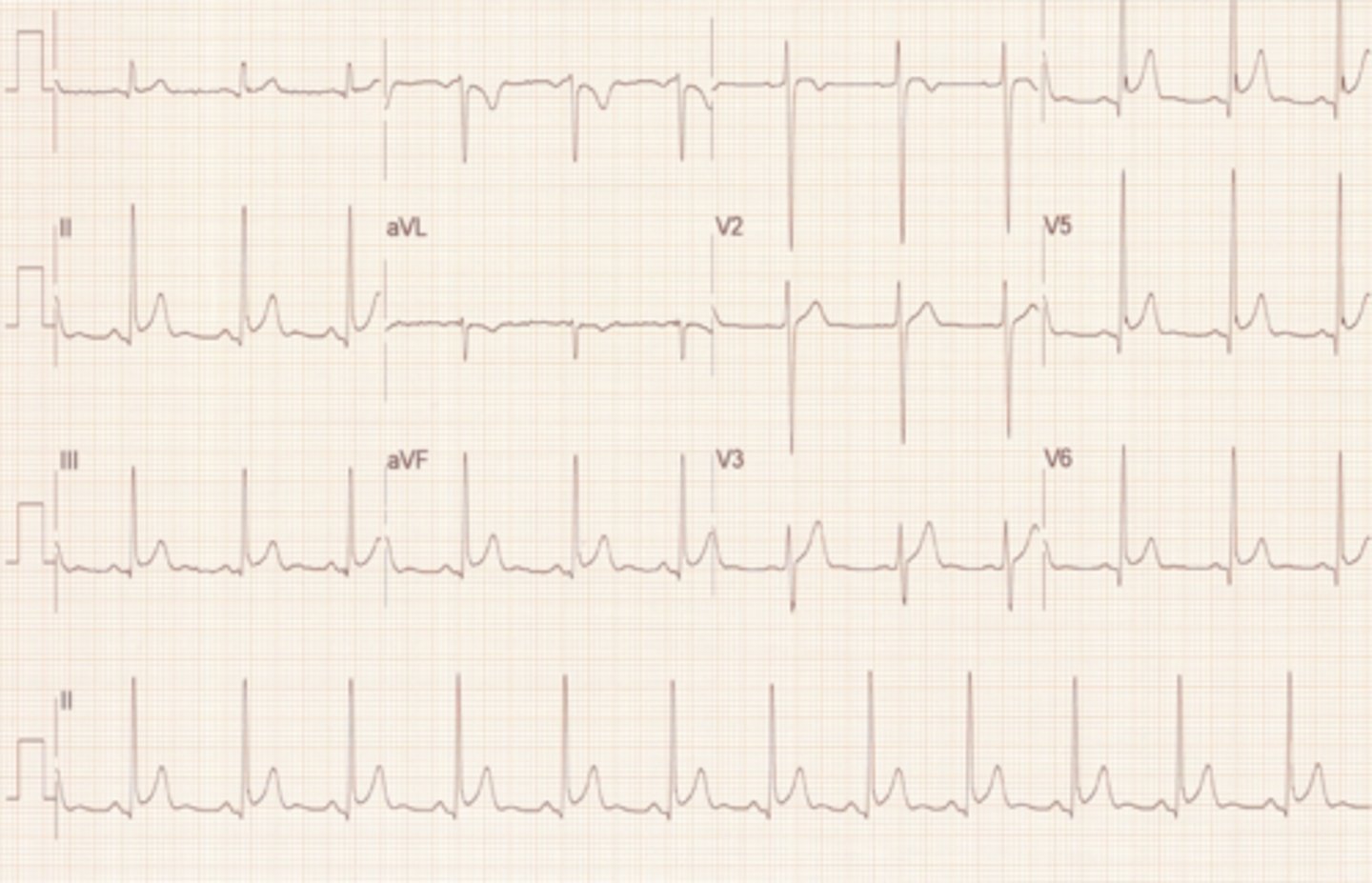
1mm ST elevation in NSR
Normal ECG often seen in athletic individuals
•ST segment is elevated, signifying myocardial injury.
Early Repolarization
Normal ECG often seen in athletic individuals
•Returns to baseline within a few hours, normally.
•Ventricular aneurysm causes persistent elevation.
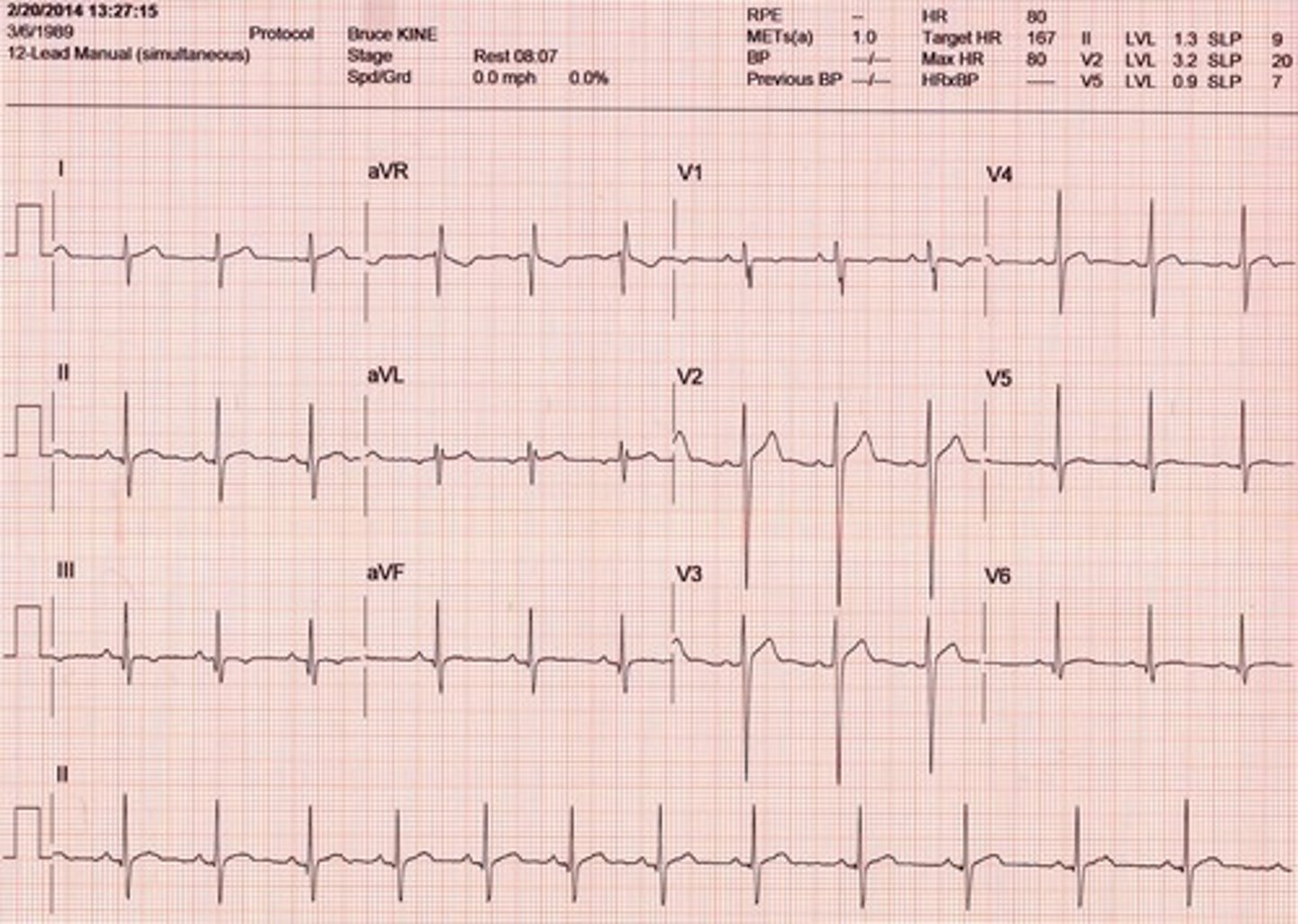
NSR
Junctional Arrythmias
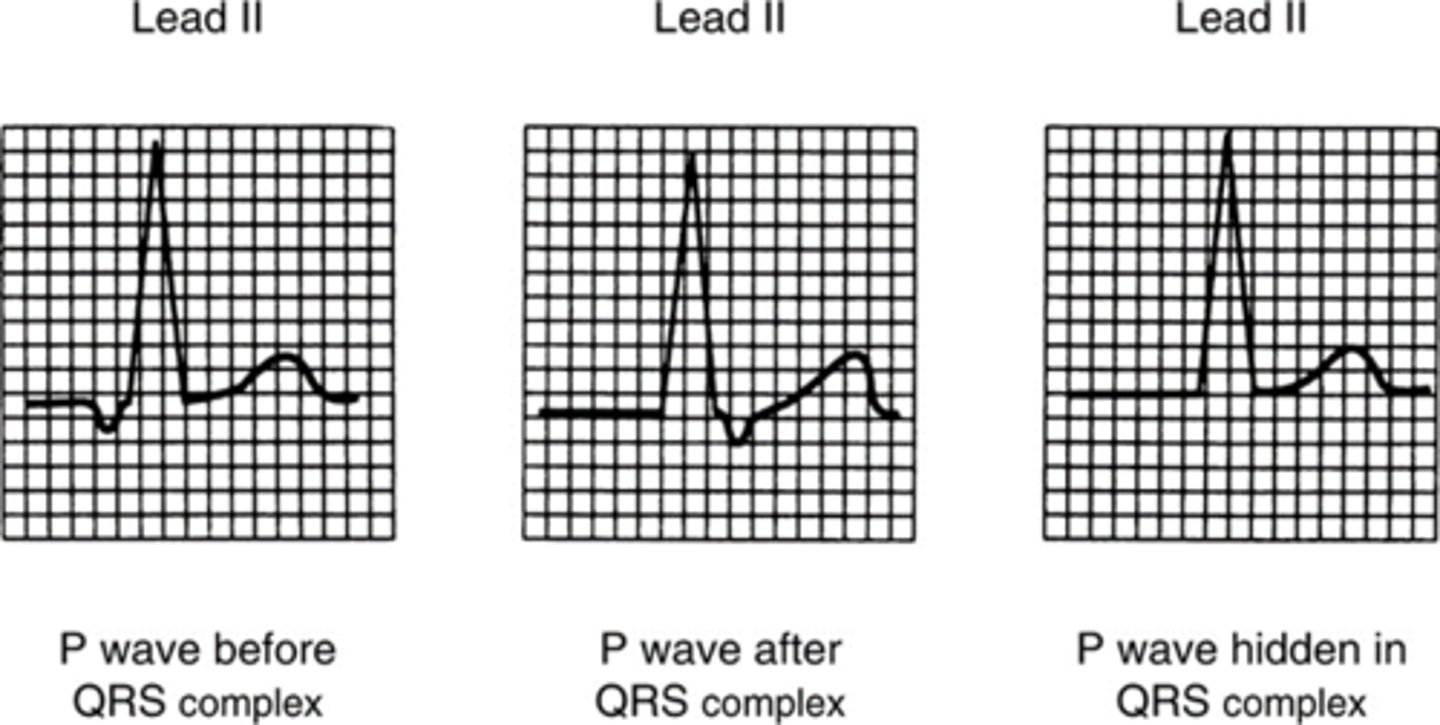
When a junctional focus fires, the wave of depolarization spreads backward (retrograde)into the atria as well as forward (antegrade) into the ventricles. The location of the P wave
in relation to the QRS complex depends
on the speed of antegrade and retrograde
conduction:
•If the impulse arrives in the atria before it arrives in the ventricles, the P wave will be before the QRS complex. The P waves will be inverted (due to retrograde depolarization of the atria) and the PR interval will be short (0.10 second or less). The QRS is normal duration.
•If the impulse arrives in the ventricles before it arrives in the atria, the P wave will be after the QRS complex. The P wave will be inverted and the PR interval will be short (0.10 second or less). The QRS complex is normal duration.
•If the impulse reaches both the atria and the ventricles at the same time, the P wave is hidden within the QRS complex and only a QRS is seen. The QRS complex is normal duration.
Premature Junctional Contraction (PJC)
•Premature beats w/- or absent P waves due to origin at or near the AV Node
•Sometime difficult to decide origin so both terms will work.
PJC
•Increased automaticity of junctional pacemaker cells
•Increased sympathetic tone due to ingestion of stimulants and abuse of drugs
•Hypoxia
•Damage to the AV node related to myocardial infarction
•Electrolyte imbalances, especially low serum levels of magnesium and potassium
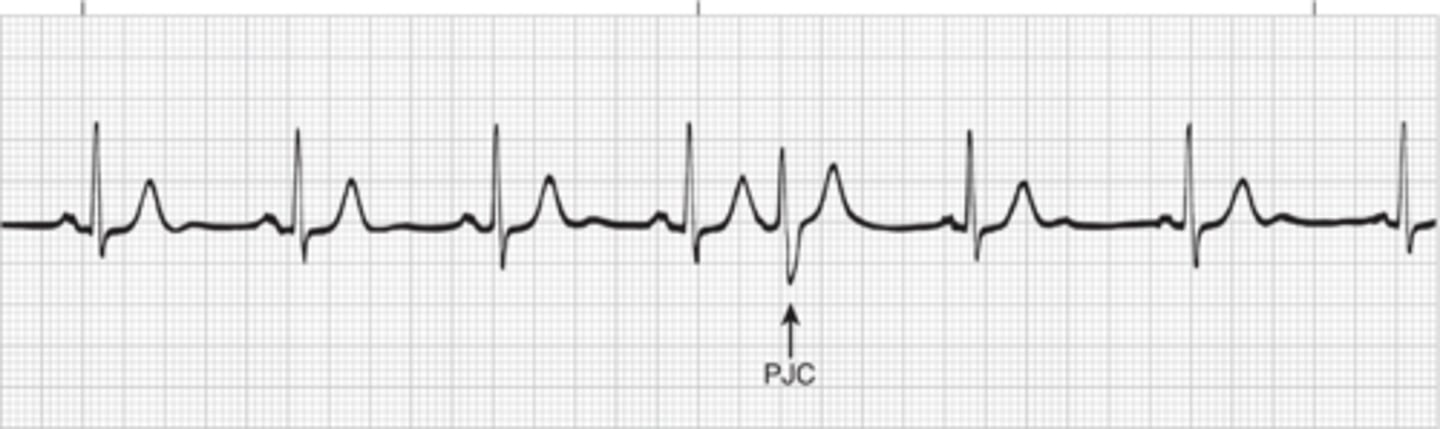
PJC
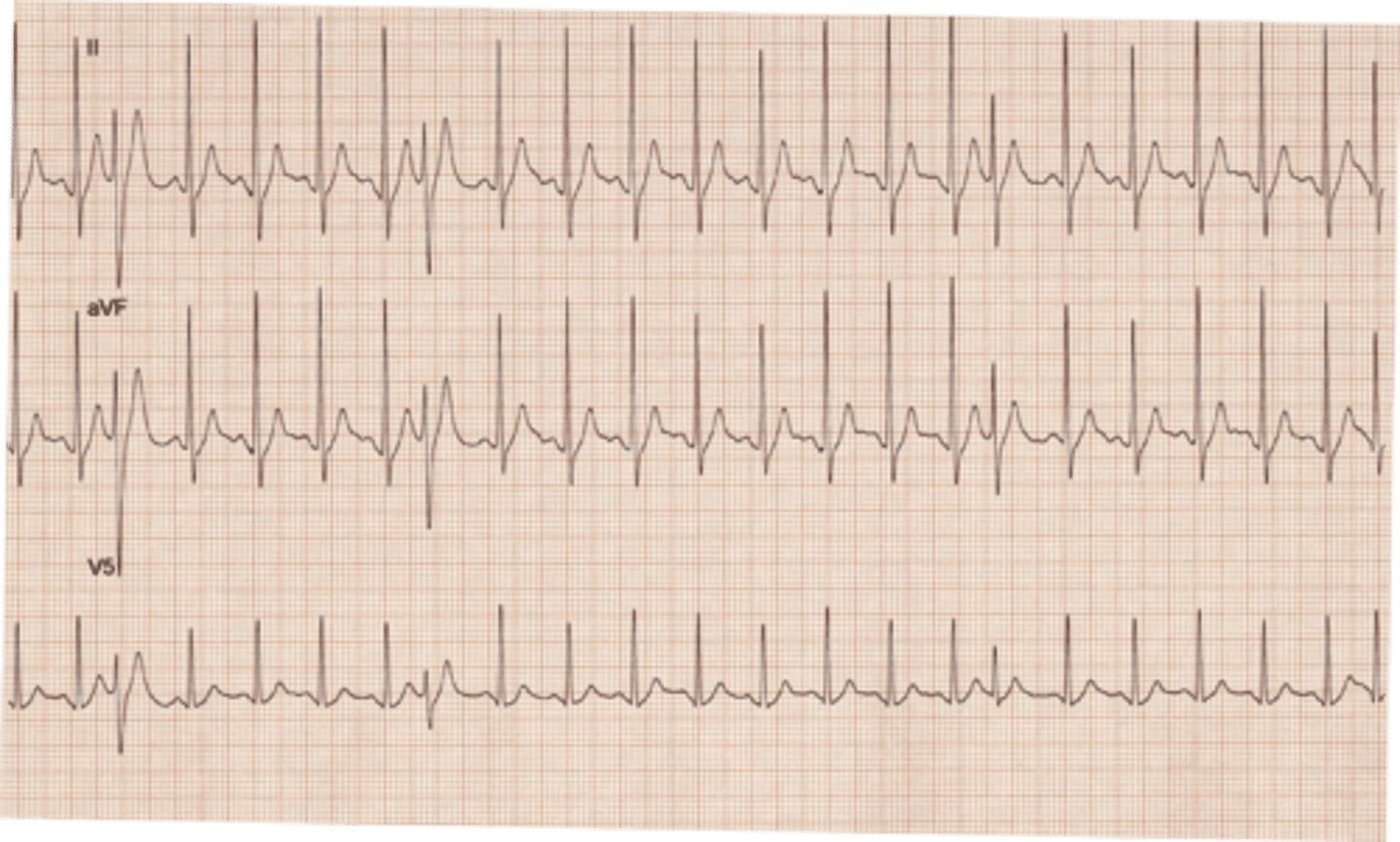
PJC
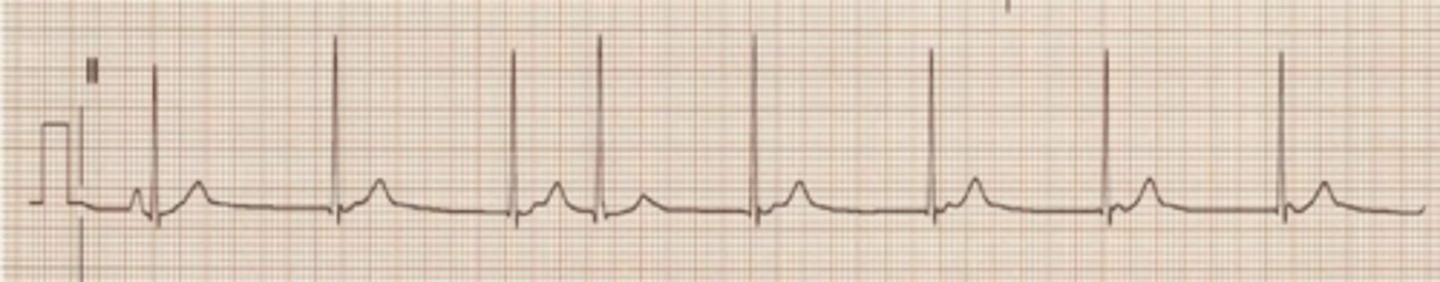
normal sinus rhythm with one premature ventricular contraction
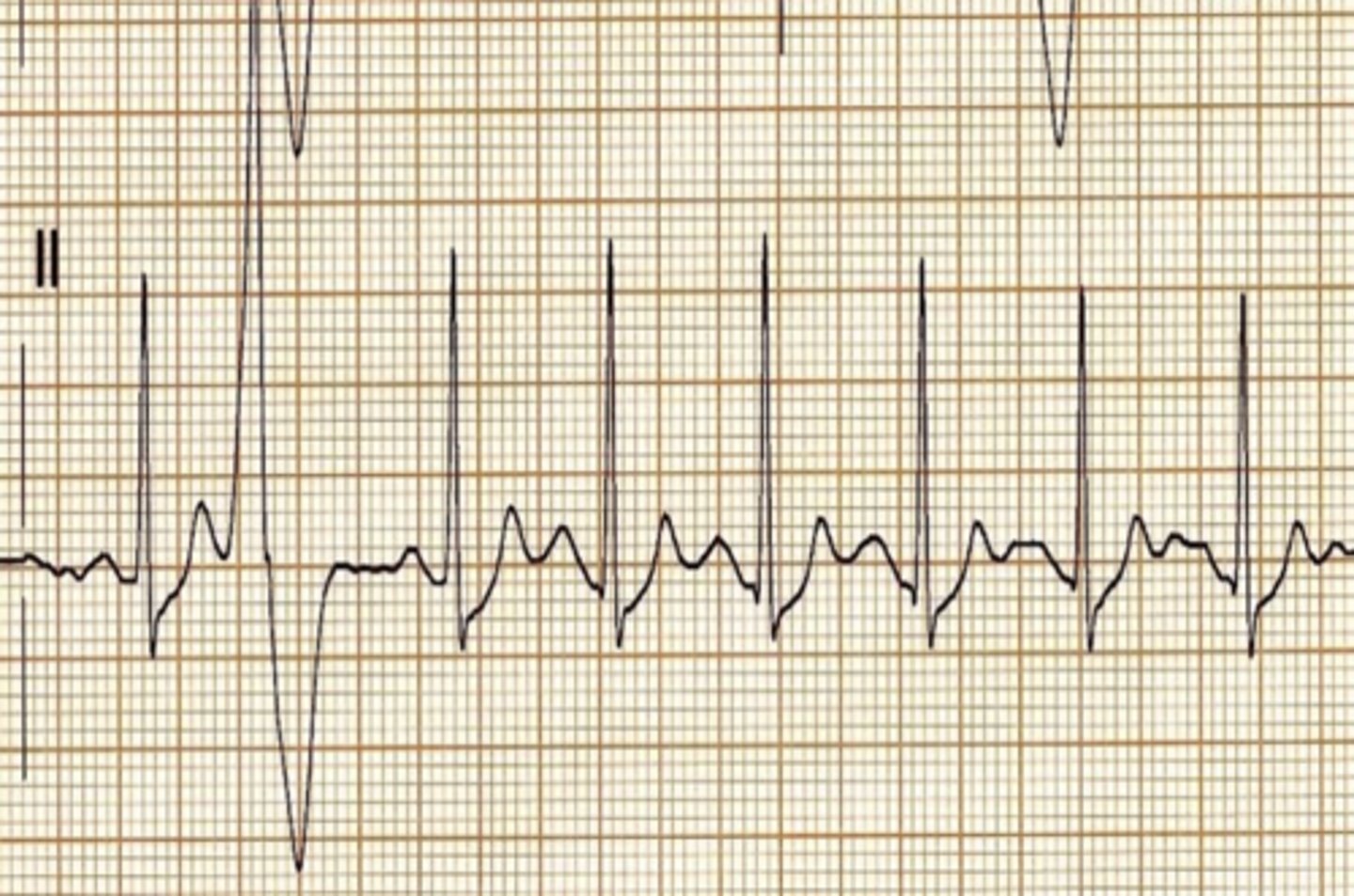
Right bundle branch block (RBBB)
•A wide QRS complex with a duration of ≥ 0.10 seconds in V1.
•rSR’ pattern in V1.
•Inverted T wave; strain pattern or inverted T waves may be present in right chest leads.
•Wide S wave in lead I and V6.
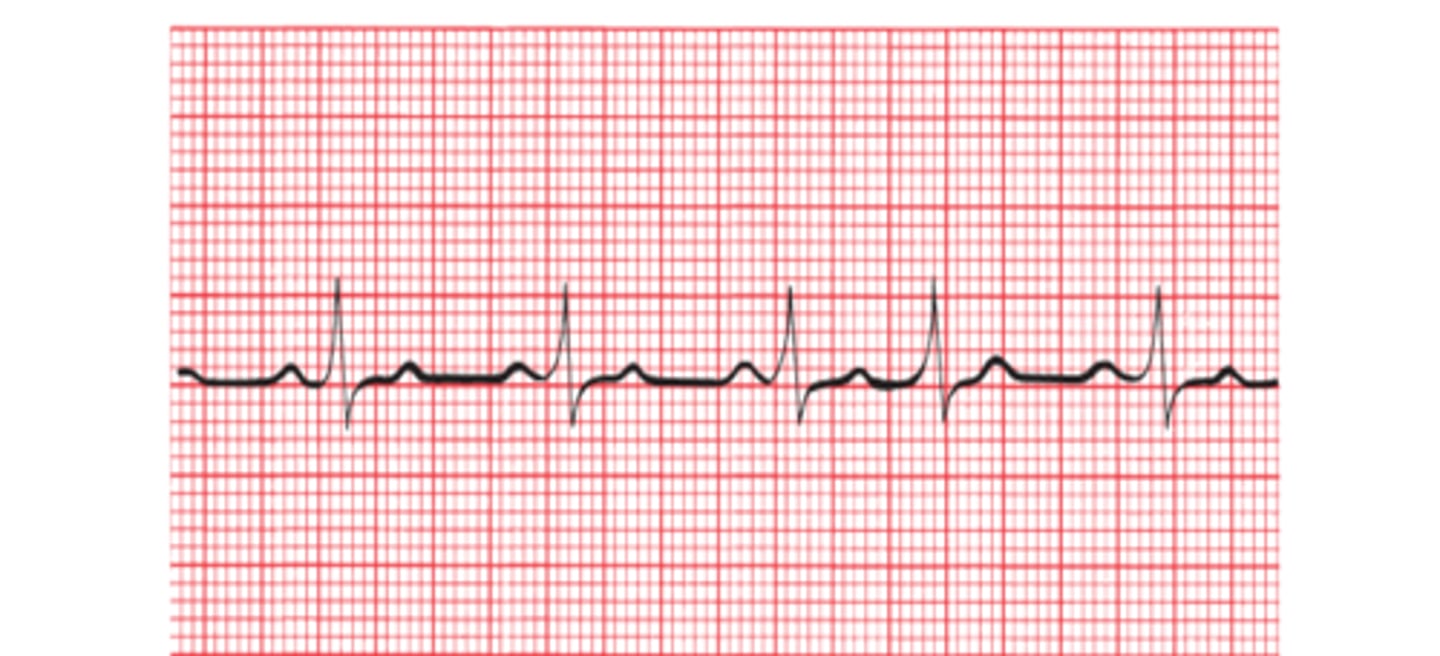
rSR
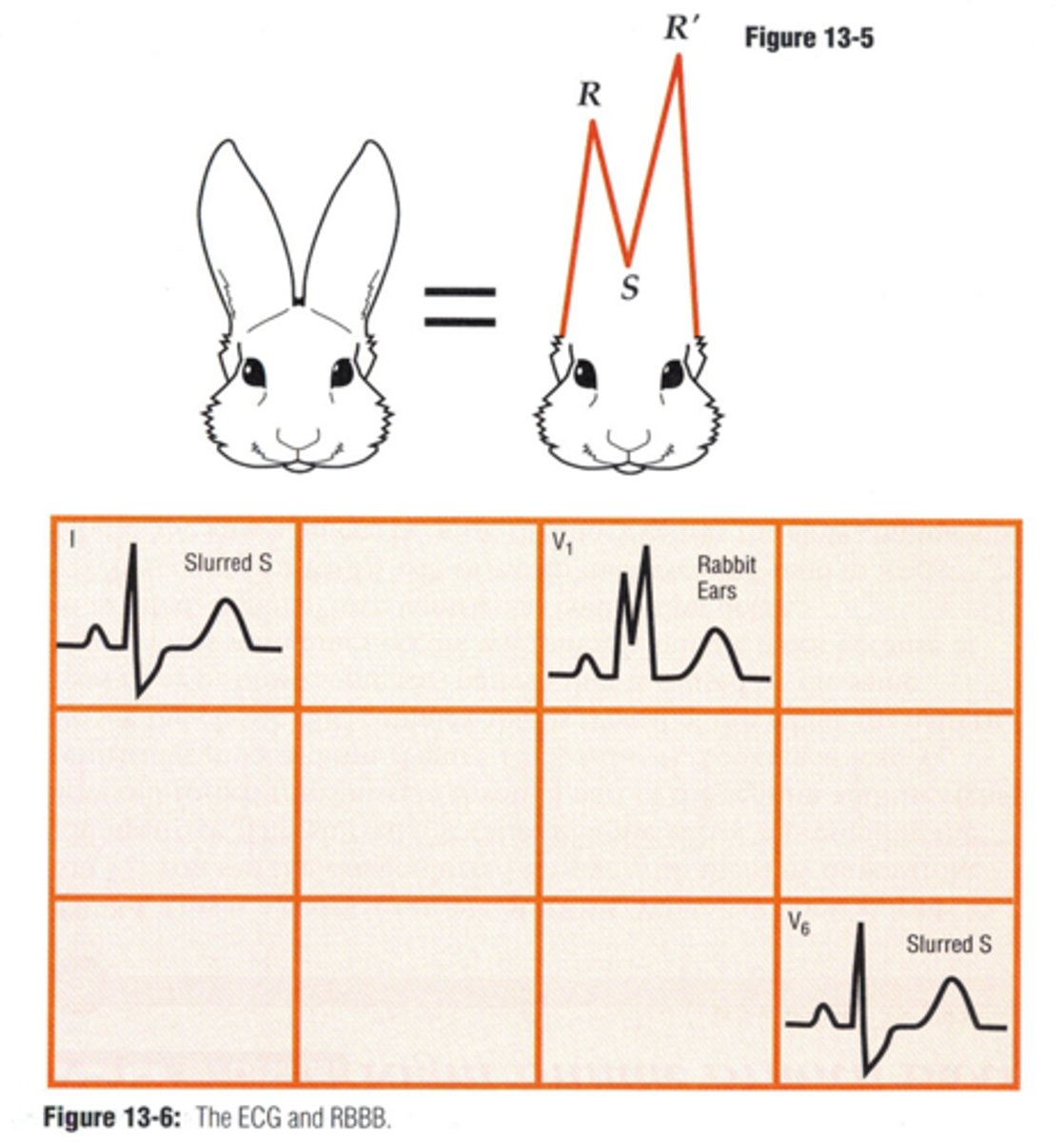
RBBB
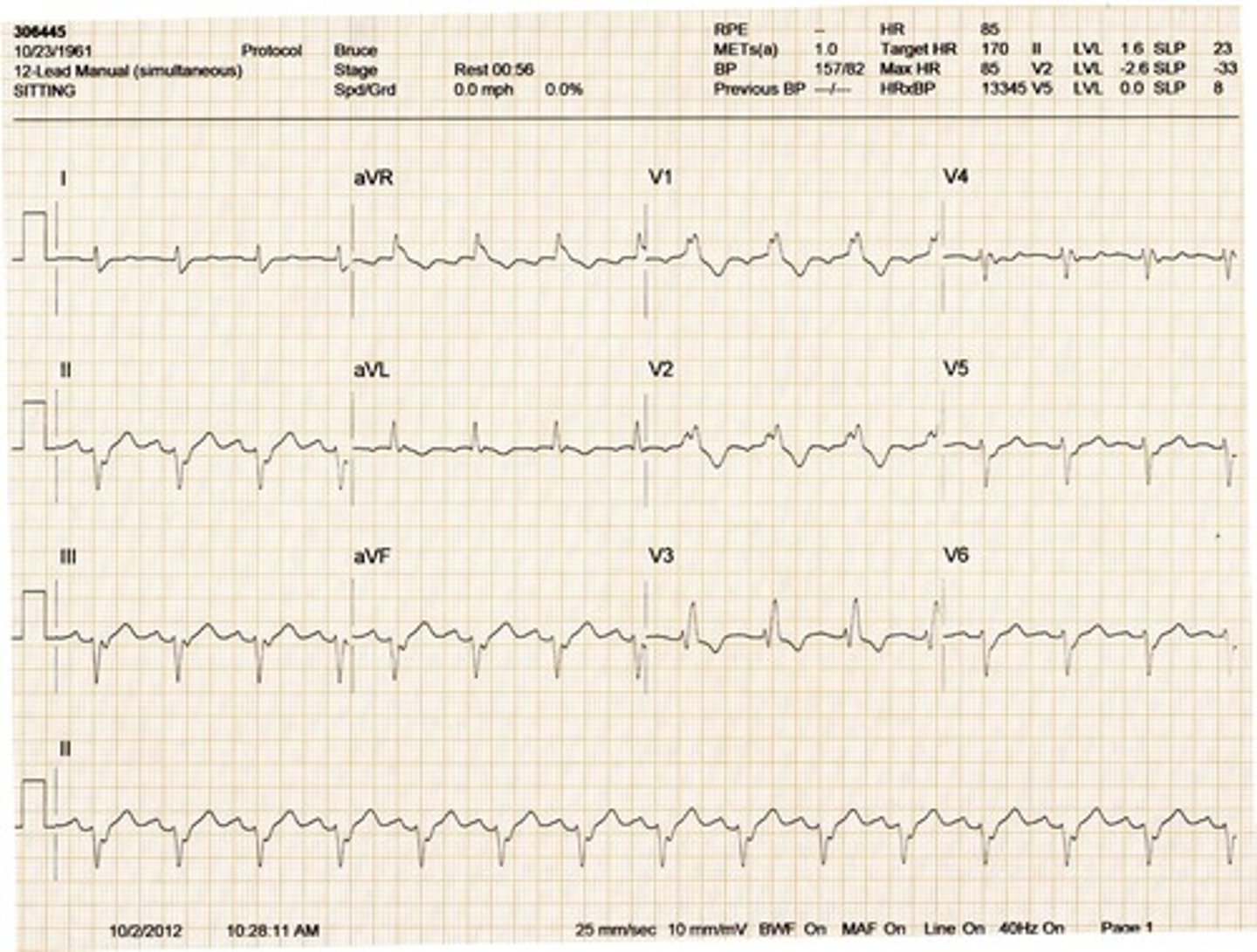
RBBB
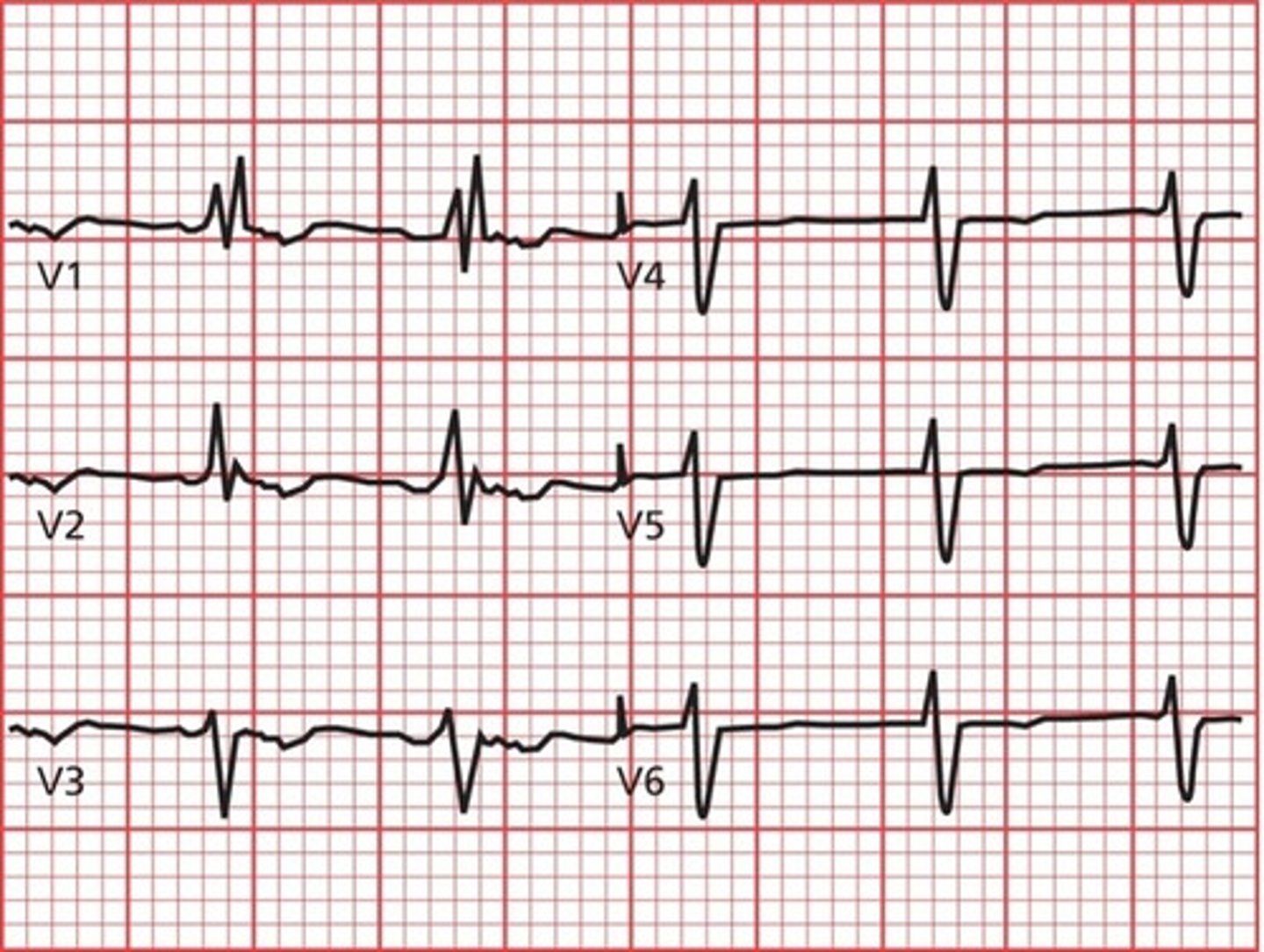
right bundle branch block
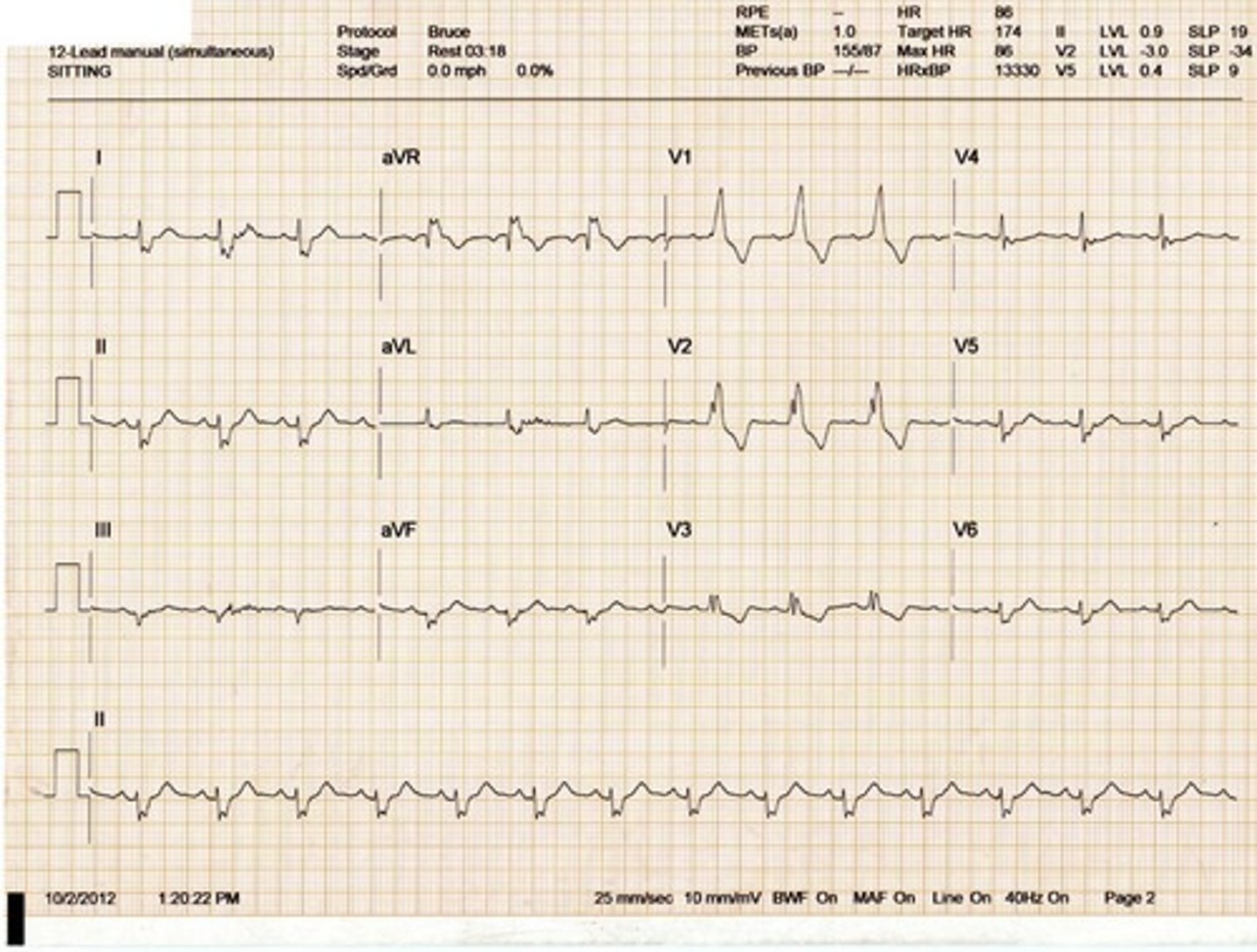
Right Bundle Branch Block
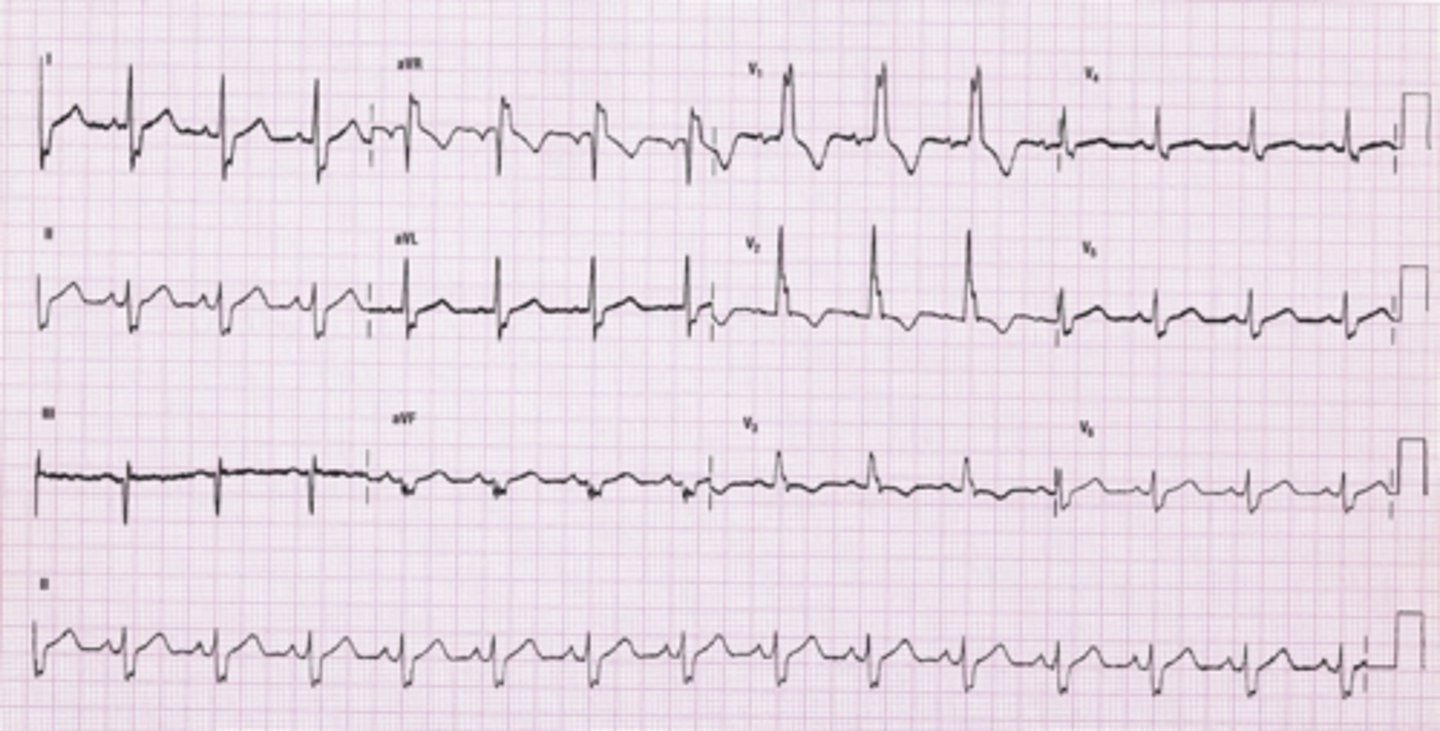
Right Bundle Branch Block
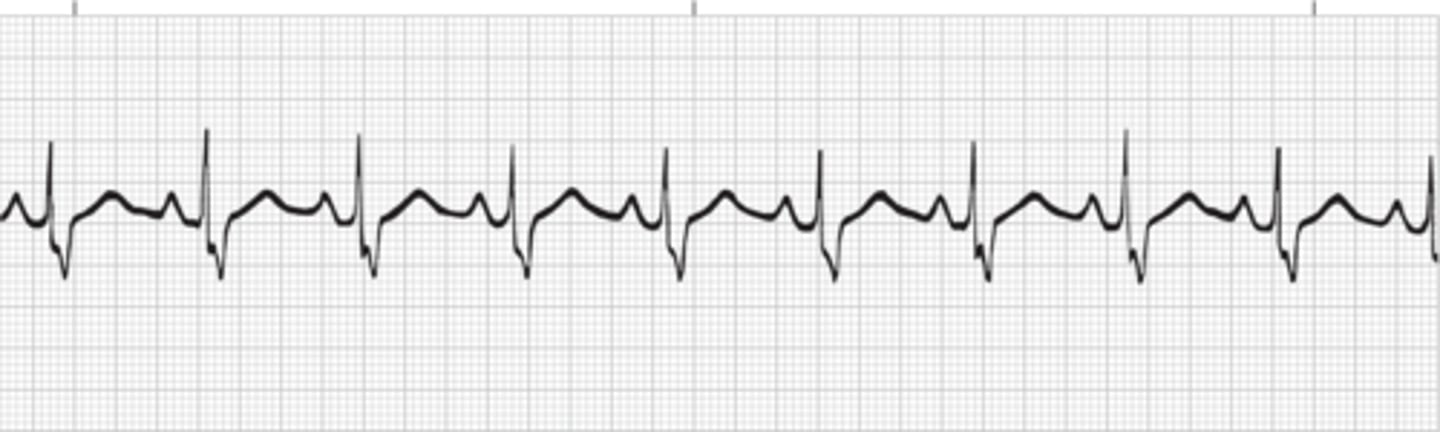
Second-Degree AV Block Type I (Mobitz I or Wenckebach)
Reflected on the ECG by a progressive lengthening (or prolongation) of the PR interval until a QRS is dropped and a P wave appears without a QRS complex. After each dropped beat the cycle repeats itself.
More P waves than QRS complexes. Irregular rhythm. May be a 3:1 or 2:1 block
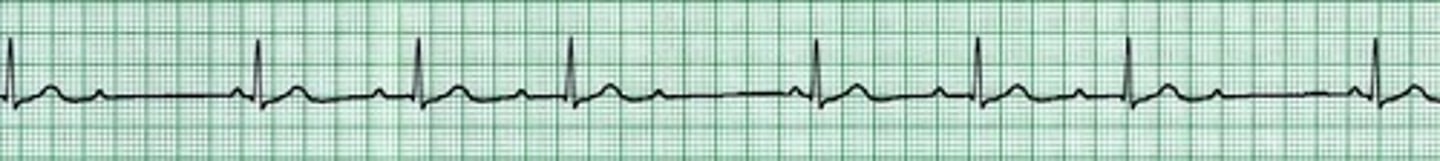
Second-Degree AV Block Type I (Mobitz I or Wenckebach)
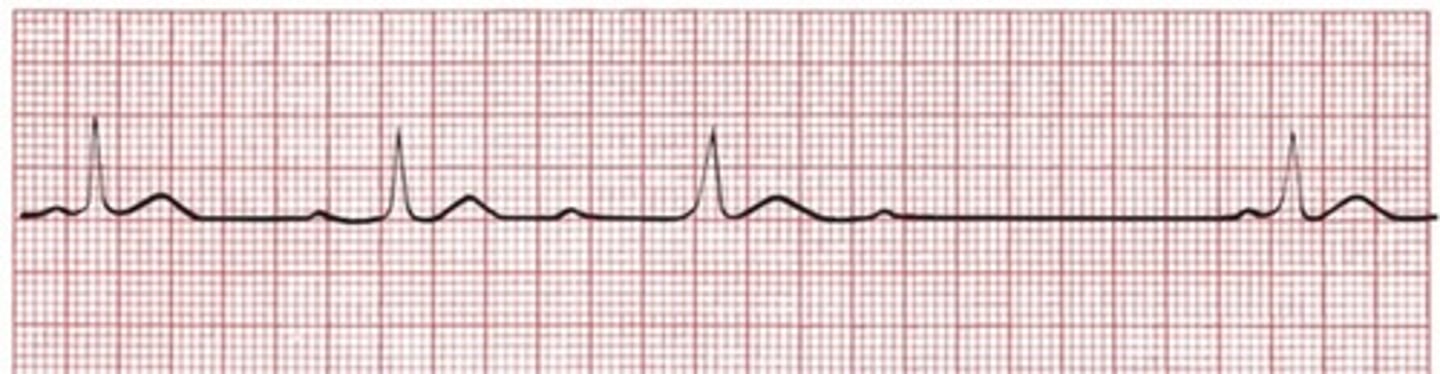
Second-Degree AV Block Type I (Mobitz I or Wenckebach)
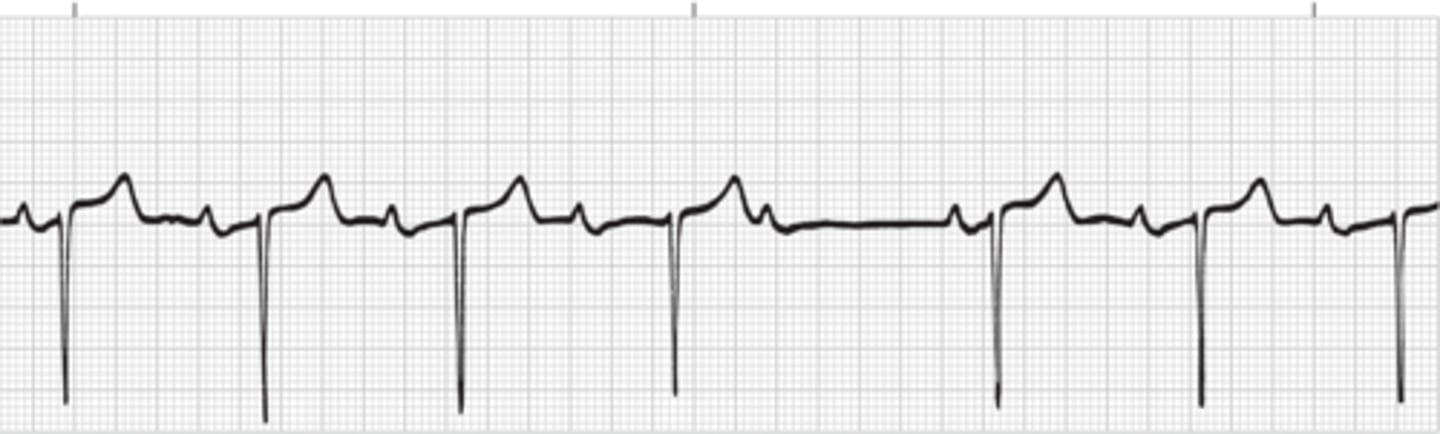
Second-Degree AV Block Type II (Mobitz Type II)
Failure of some of the sinus impulses to be conducted to the ventricles. Two or more normal beats then a P wave without a QRS. The PR intervals are constant with no progressive increase. Varying ratios of P waves to QRS complexes.
Type II is more serious than Type I.
May progress to a third degree AV block which is more serious.
Due to degeneration of the electrical conduction system in elderly patient.
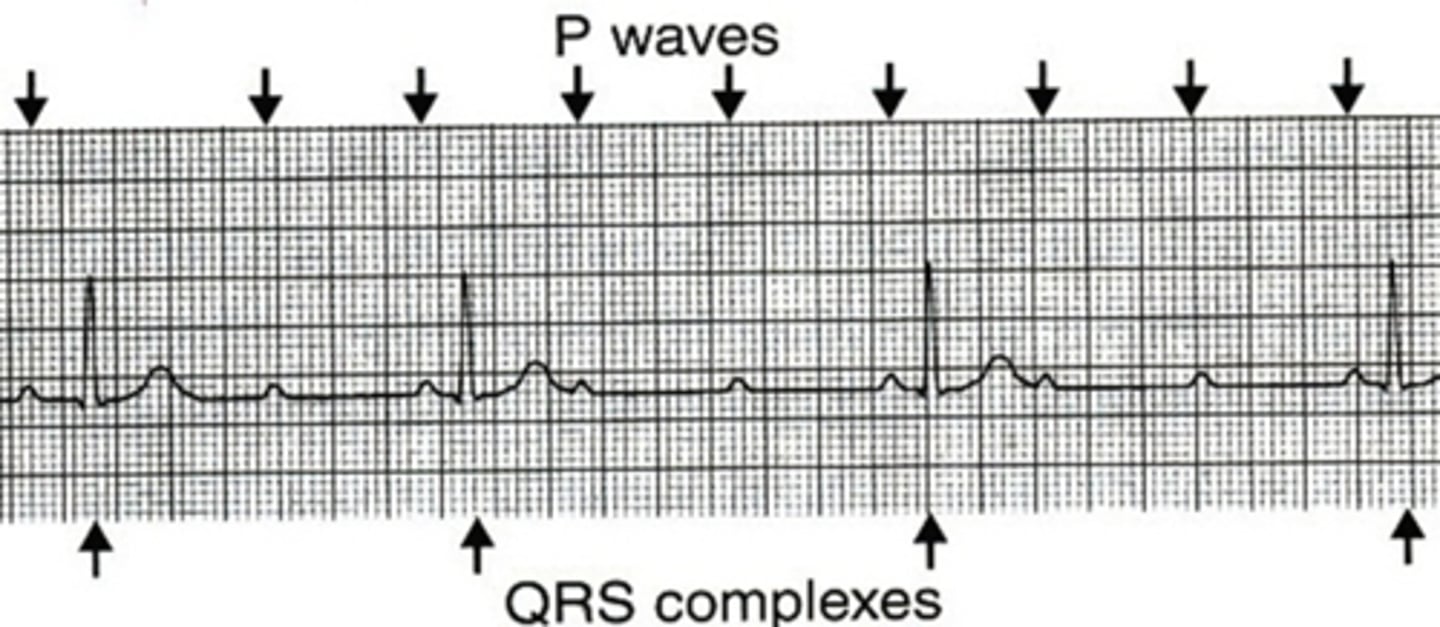
Second-Degree AV Block Type II (Mobitz Type II)
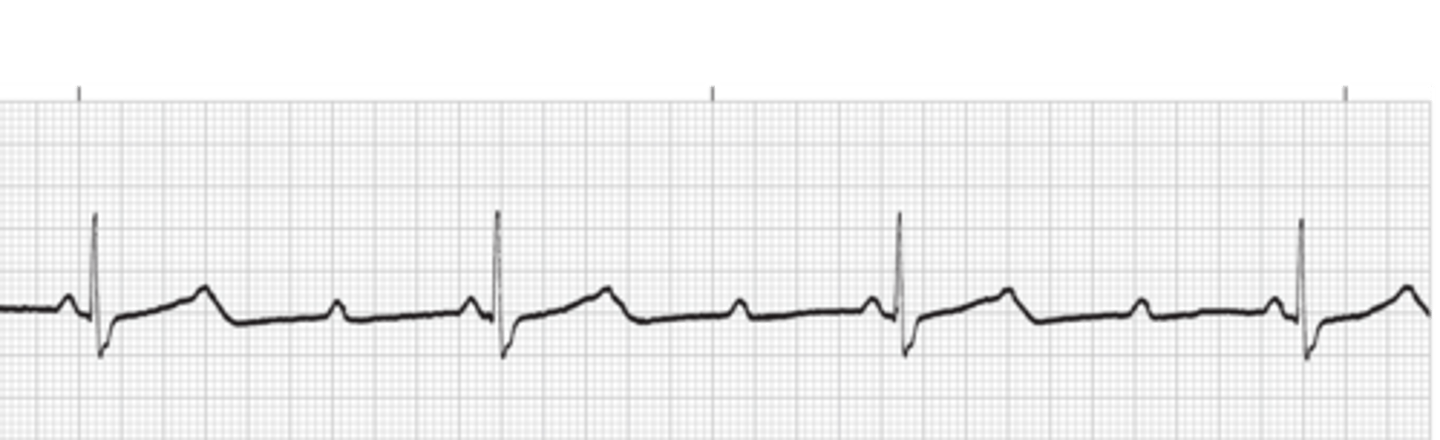
Sinus tachycardia with T wave inversion
This may be an indication of ischemia
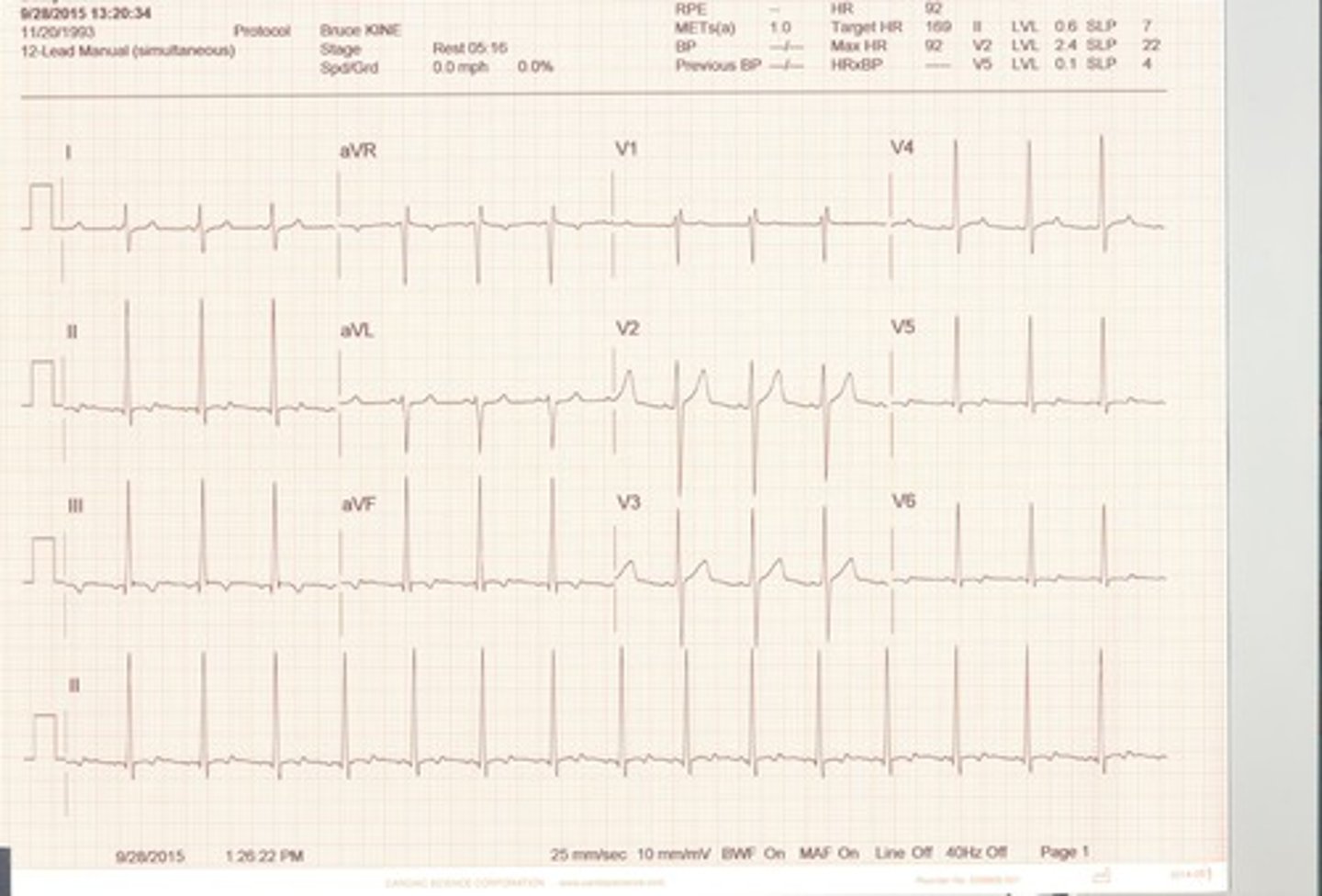
Second-Degree AV Block Type II (Mobitz Type II)
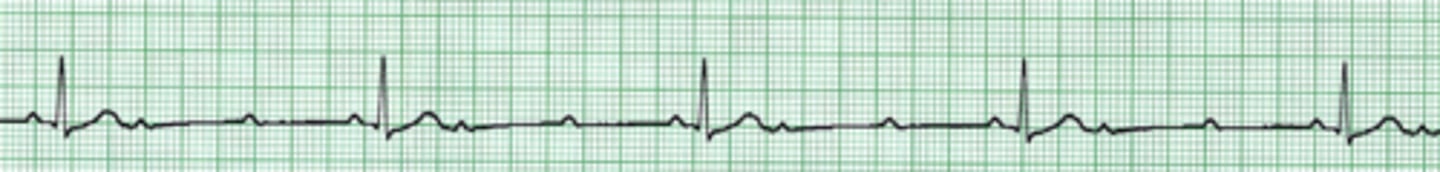
Sinus Tachycardia
P wave is upright
PR interval is 0.16 seconds or 4 boxes
QRS is less than 0.10 seconds long or less than 2.5 boxes.
T wave is upright
Rhythm is regular
Heart rate is 100 and above.
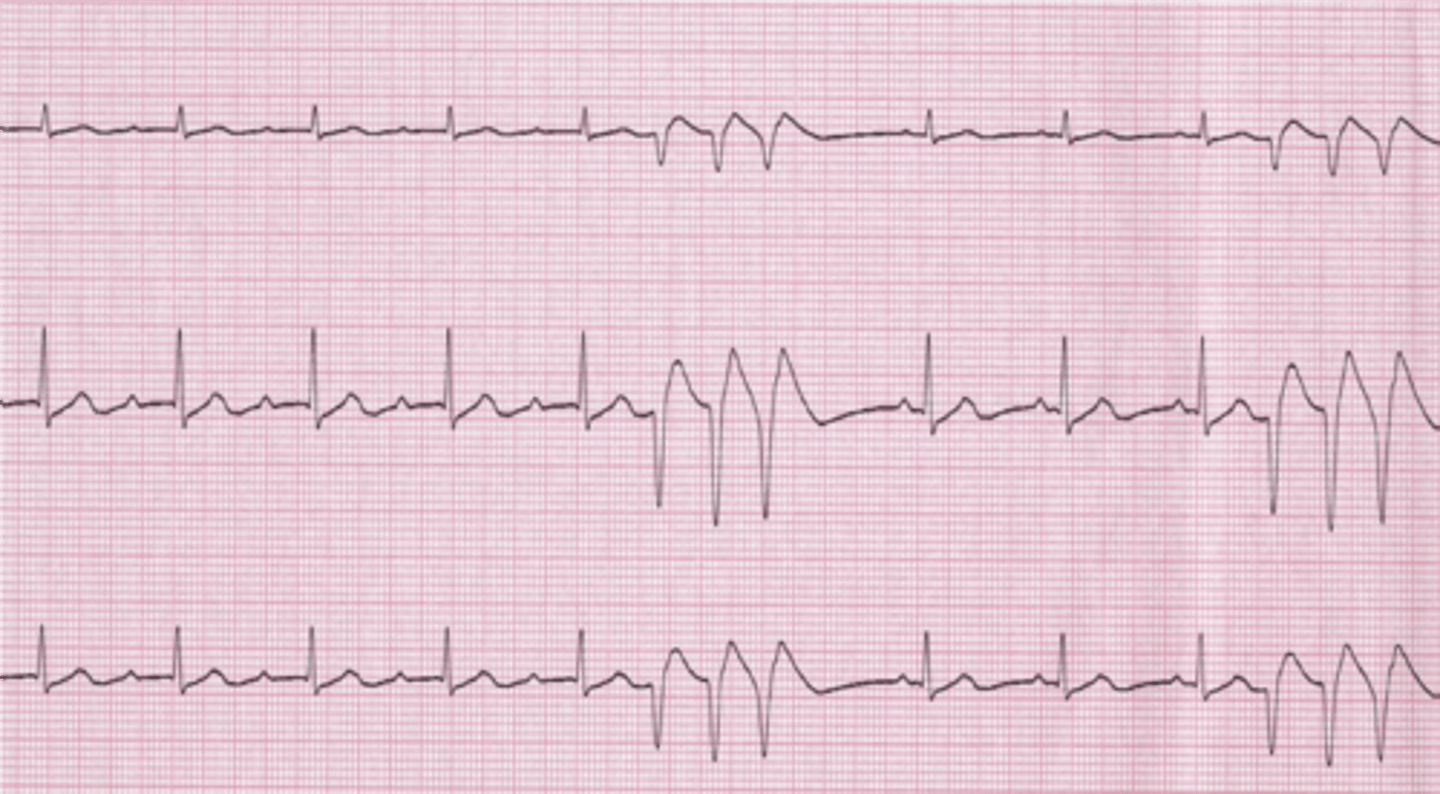
Ventricular tachycardia
A succession of three or more premature ventricular contractions in a row is seen in ventricular tachycardia.
Only the ventricles are firing. No P wave or T wave. Poor cardiac output.
Rate is greater than 150 beats per minute in this example. Dangerous rhythm that requires
Immediate medical attention as the subject is having a heart attack.
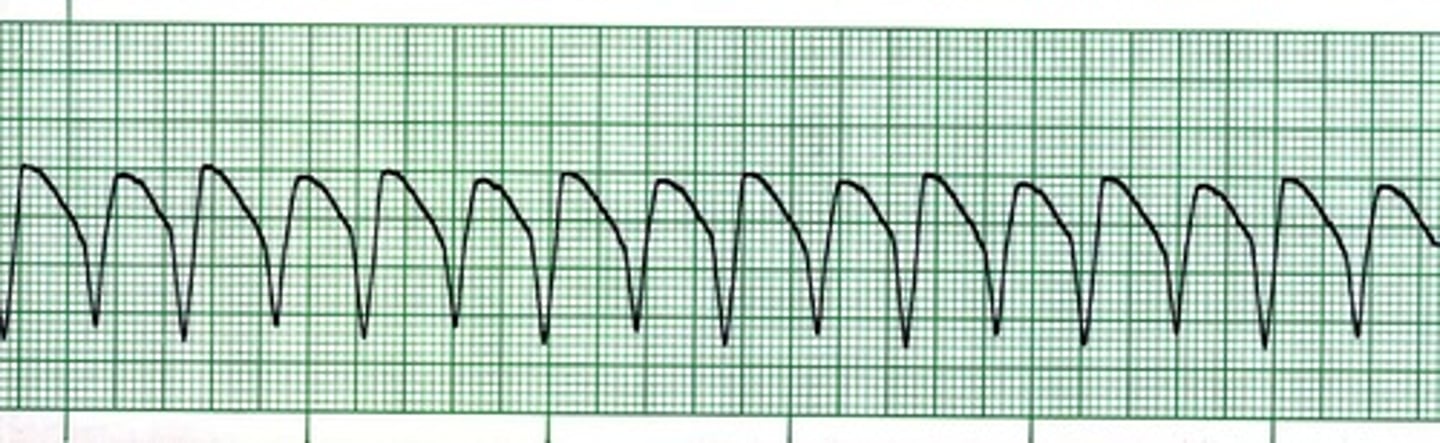
Run of Ventricular Tachycardia
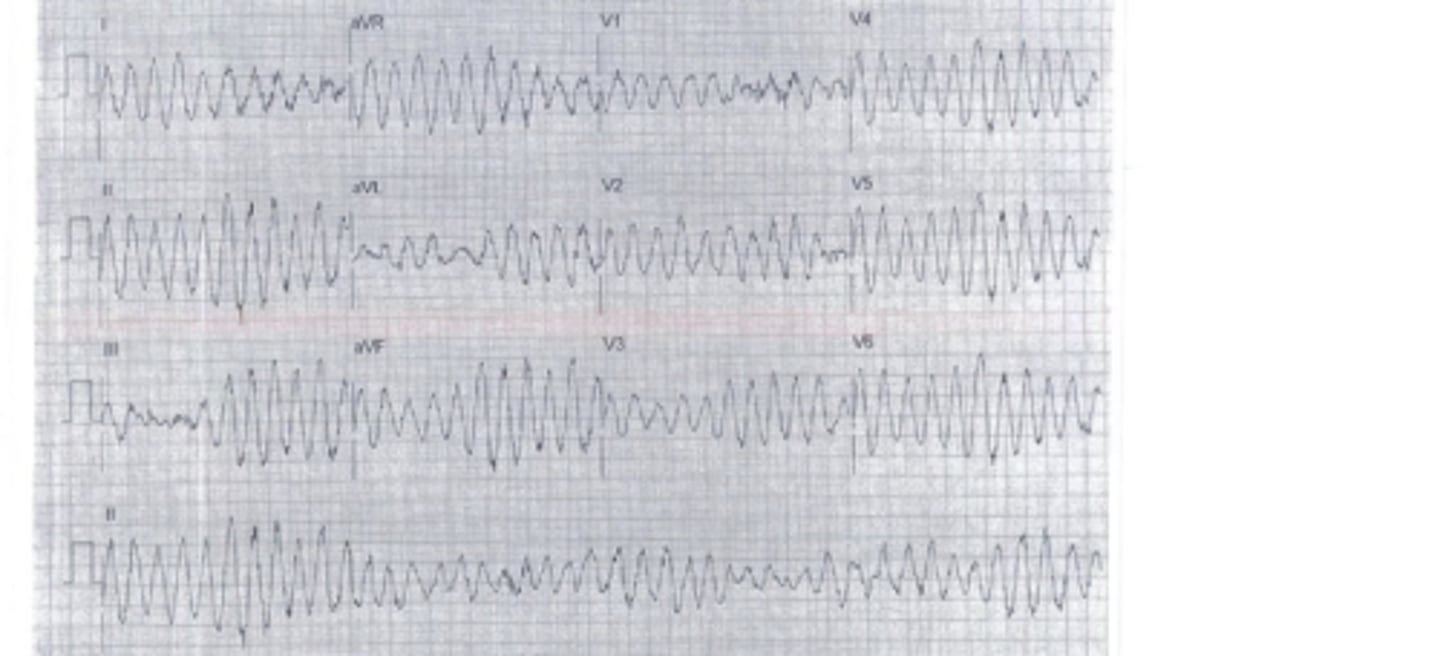
torsade de pointes ventricular tachycardia
form of polymorphic VT and is usually associated with a prolonged QT interval; QRS complex changes polarity as it twists around the isoelectric line.
Usually seen in patients with prolonged QT intervals. QRS complexes spiral around baseline
paroxysmal atrial tachycardia
originates in an ectopic pacemaker site in the atria producing a rapid, regular atrial rhythm between 140 and 250 beats per minute. Atrial tachycardia is often precipitated by a PAC and commonly starts and stops abruptly, occurring in bursts or paroxysms (thus the name paroxysmal atrial tachycardia). The rhythm may be continuous or intermittent. By definition, three or more consecutive PACs (at a rate of 140 to 250 beats per minute) is considered to be atrial tachycardia.
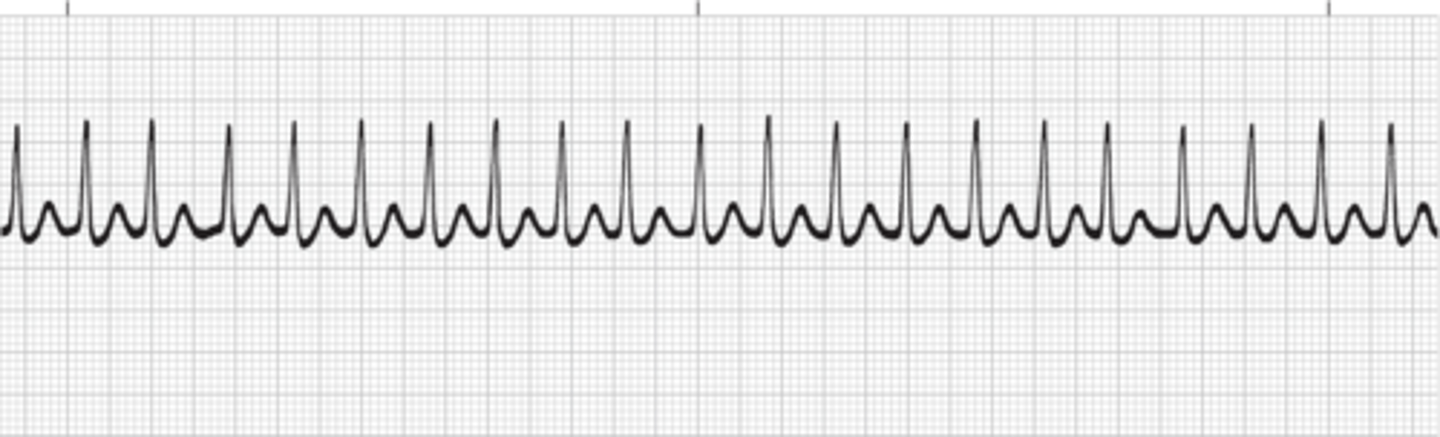
paroxysmal atrial tachycardia (PAT)
Rhythm: Regular
Rate:140 to 250 beats/minute
P waves: Abnormal (commonly pointed); usually hidden in preceding T wave, making T wave and P wave appear as one wave deflection (T-P wave); one P wave to each QRS complex unless AV block is present.
PR interval: Usually not measurable
QRS complex: Normal (0.10 second or less)
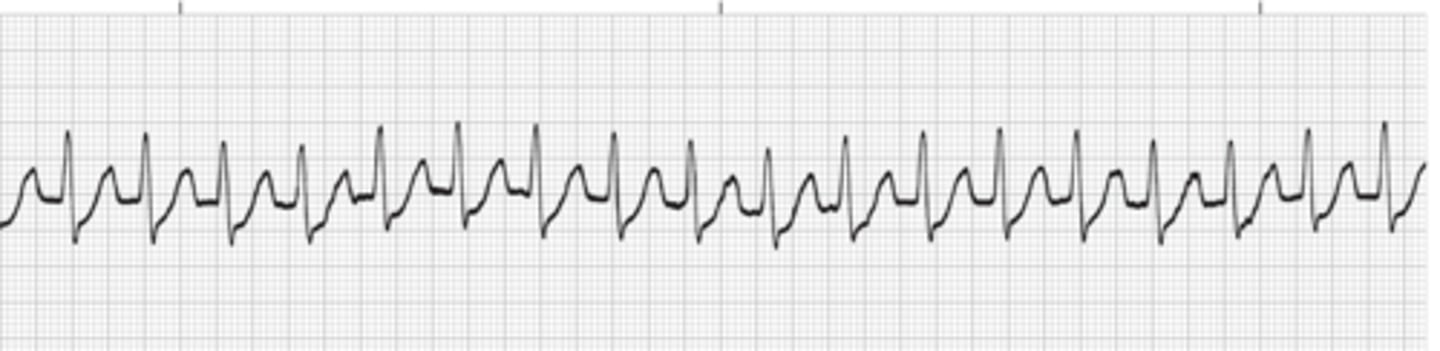
PAT
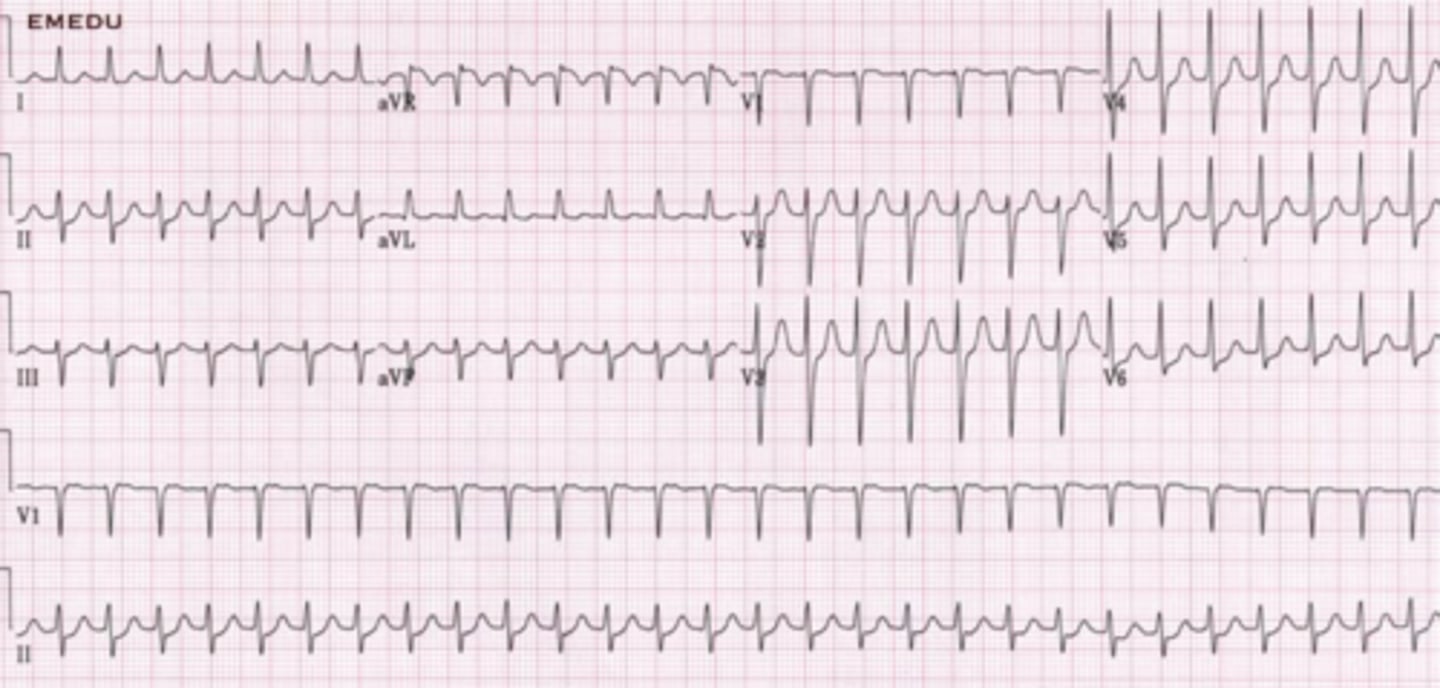
Paroxysmal Junctional Tachycardia (PJT)
originates in an ectopic pacemaker site in the AV junction at a heart rate exceeding 100 beats/minute. PJT is often precipitated by a PJC and commonly starts and stops abruptly. PJT may appear as a sustained, continuous rhythm or occur intermittently in runs of three or more beats. Three or more consecutive PJCs at a rate exceeding 100 beats/minute is considered to be junctional tachycardia
PJT is characterized by an inverted P wave that may occur before the QRS, after the QRS, or be hidden within the QRS complex; a short PR interval of 0.10 second or less; and a normal QRS complex.
•PJT is not a common arrhythmia.
•Paroxysmal junctional tachycardia may occur due to enhanced automaticity of the AV junction or to a reentry circuit.
•Conditions associated with PJT include damage to the AV junction from myocardial infarction (usually inferior wall MI), congestive heart failure, or digitalis toxicity.
•PJT has the same identifying features as junctional rhythm and accelerated junctional rhythm. The rhythms are differentiated by the heart rate.
•A reduction in cardiac output may be present due to the ventricular rate and to the retrograde depolarization of the atria with subsequent loss of the atrial kick. Treatment is directed toward slowing the ventricular rate and reversing the consequences of decreased cardiac output.
•Identify and correct the underlying cause of the arrhythmia.
Rhythm: Regular
Rate: 115 beats/minute
P waves: Inverted before each QRS complex
PR interval: 0.08 second
QRS complex: 0.06 - 0.08 second
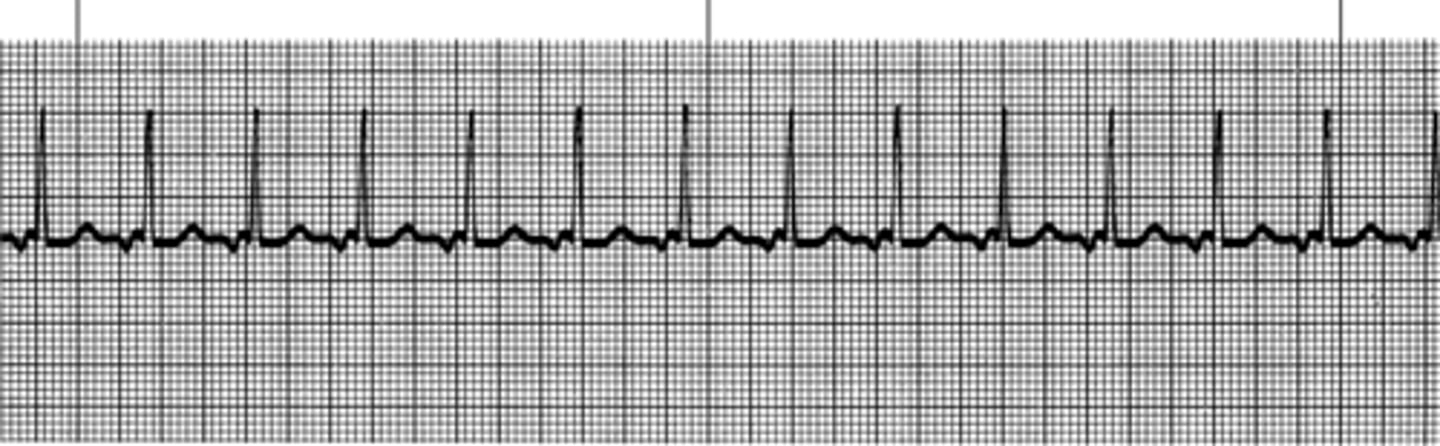
Information
Electrical connections of right and left bundle branches result in uniform contraction of ventricles.
Blocks within the bundle branch system delay ventricular depolarization
Wolff-Parkinson-White
Slurred upstroke on QRS (Delta Wave), creating a wide QRS and short PR interval. This is caused by an accessory pathway in the atria to the ventricles called the bundle of Kent.
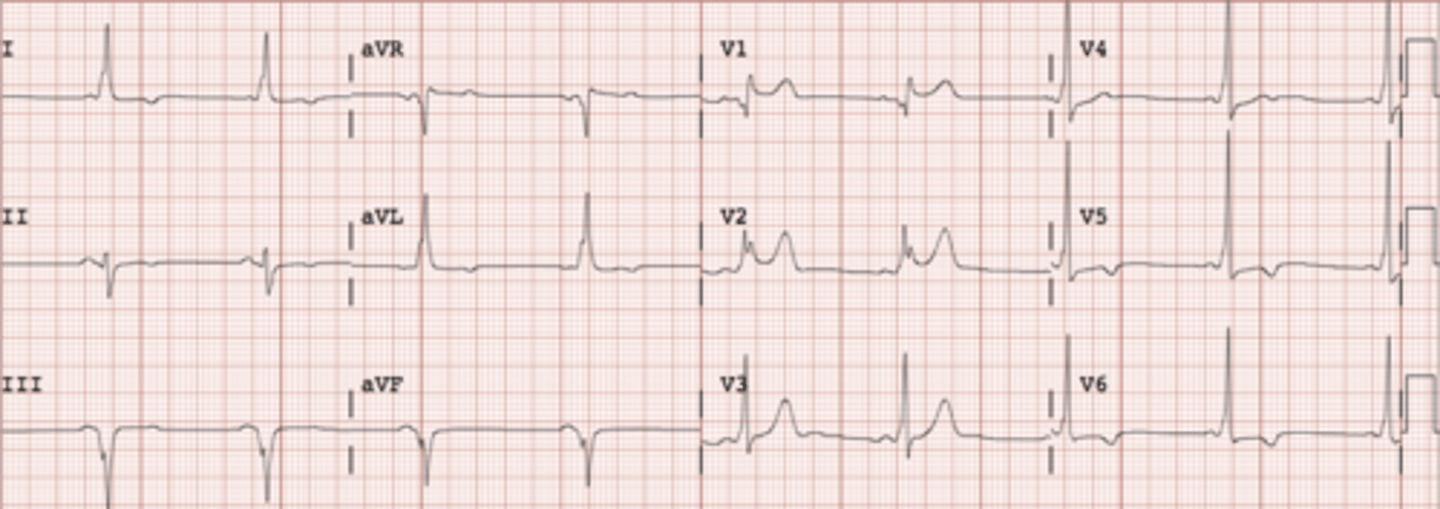
Wolff-Parkinson-White
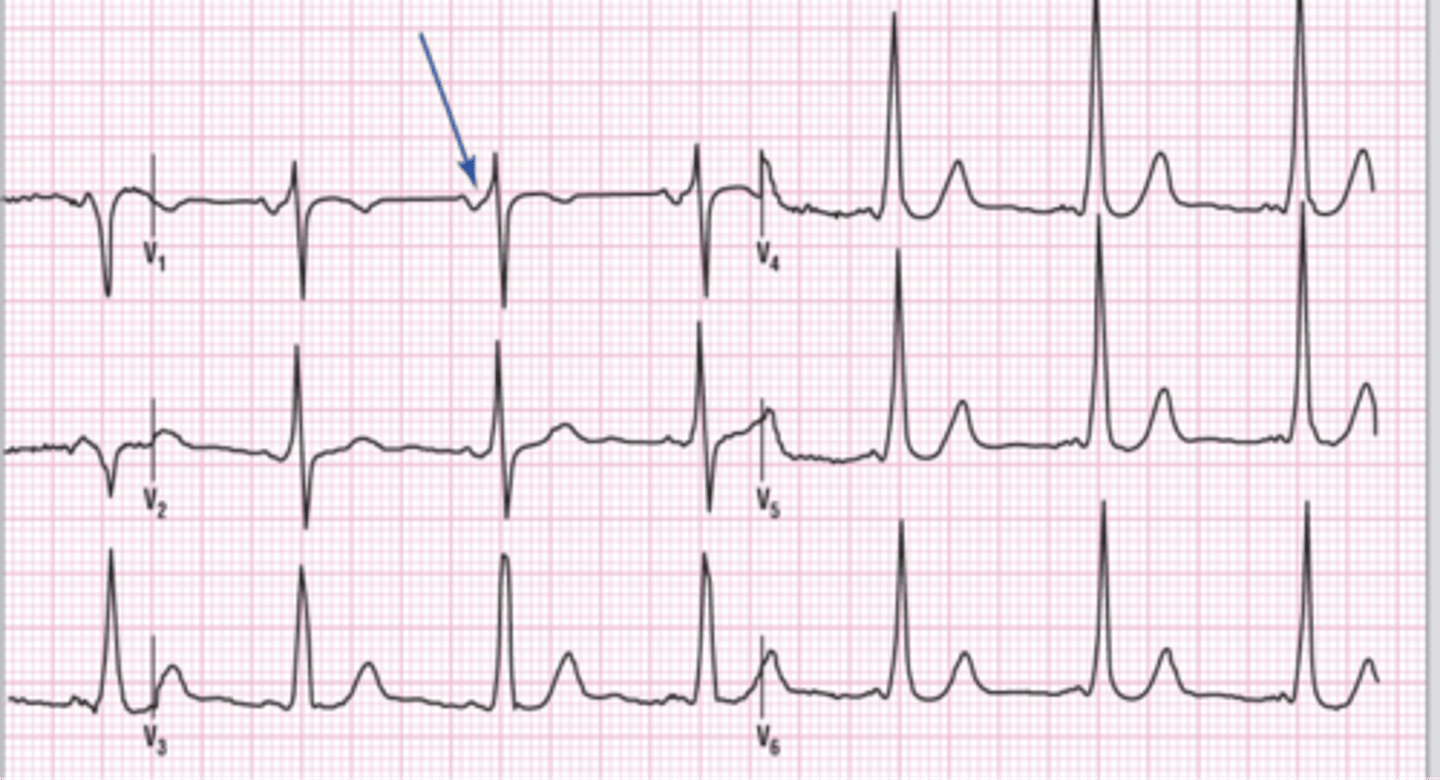
sinus bradycardia with a ventricular escape beat
A ventricular ectopic beat that occurs late instead of early is called a ventricular escape beat. The morphologic characteristics of the late beat are the same as with the PVC. Ventricular escape beats usually occur during a pause in the underlying rhythm. Escape beats act as an electrical backup to maintain the heart rate and require no treatment. No compensatory pause as with a PVC.
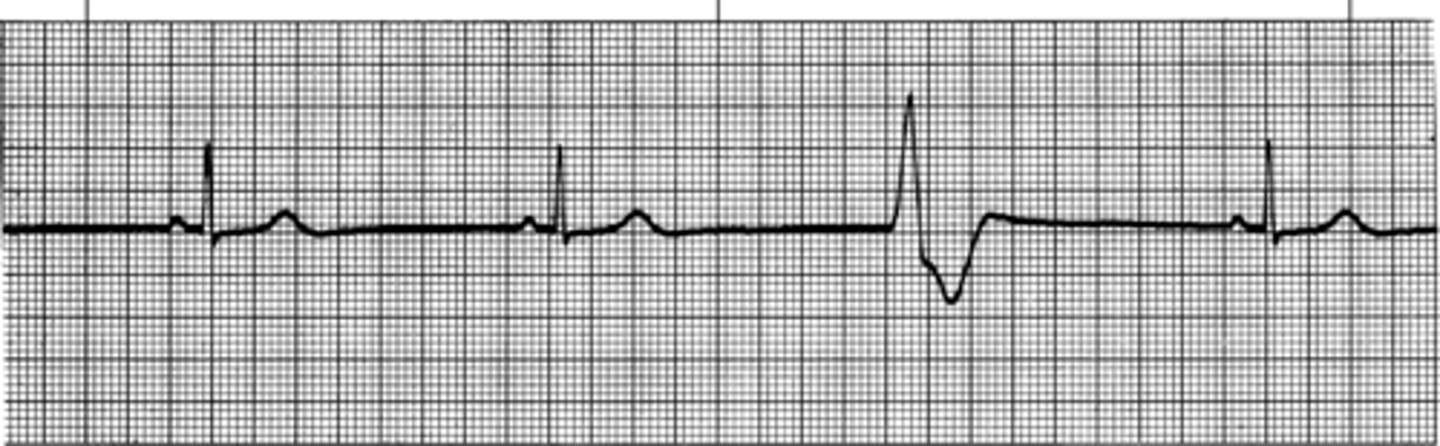
Idioventricular Rhythm
Idioventricular rhythm originates in an ectopic pacemaker site in the ventricles at a rate of 30 - 40 beats/minute (sometimes less). Because the impulse originates in the ventricles, there is no P wave and the QRS complex is wide. IVR may occur as a continuous rhythm or intermittently in runs of three or more beats. Three or more consecutive wide QRS complexes at a rate of 30 - 40 beats/minute are considered to be IVR. The rhythm is regular.
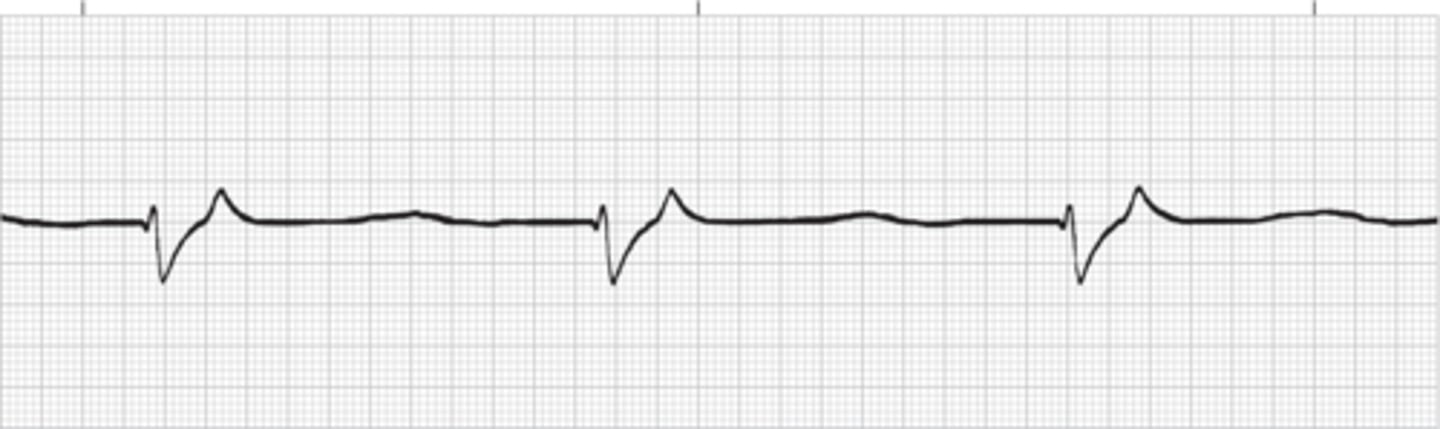
Idioventricular Rhythm
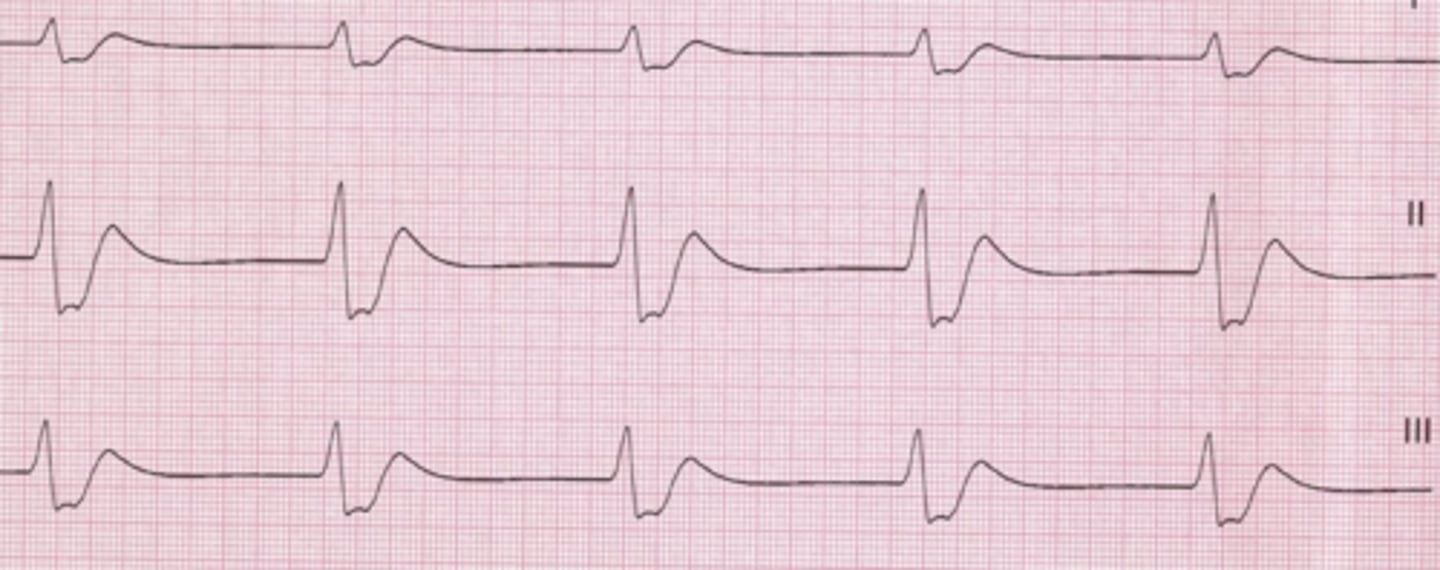
Accelerated Idioventricular Rhythm
Ectopic beats of ventricular origin with a rate of >50and <100 bpm. No visible P waves.

ST segment depression
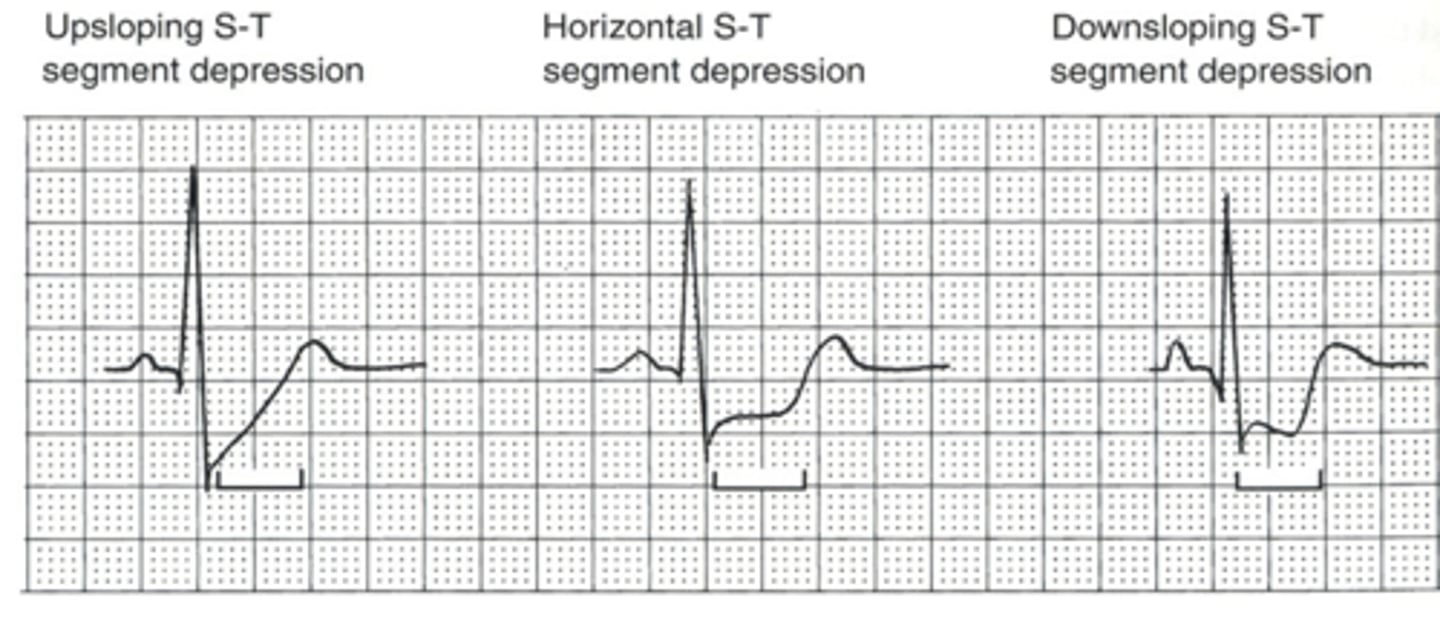
Up sloping ST segment depression
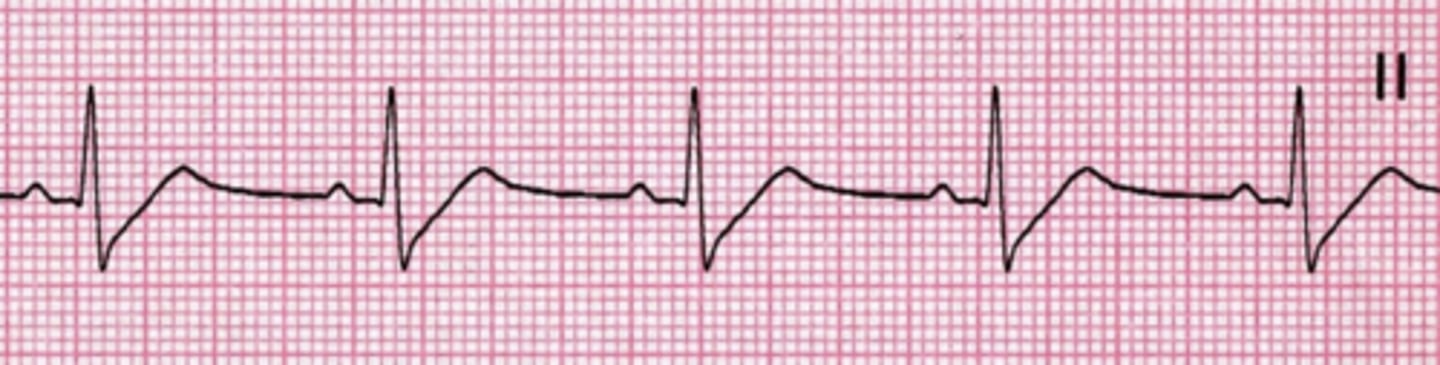
Horizontal and downsloping ST depression
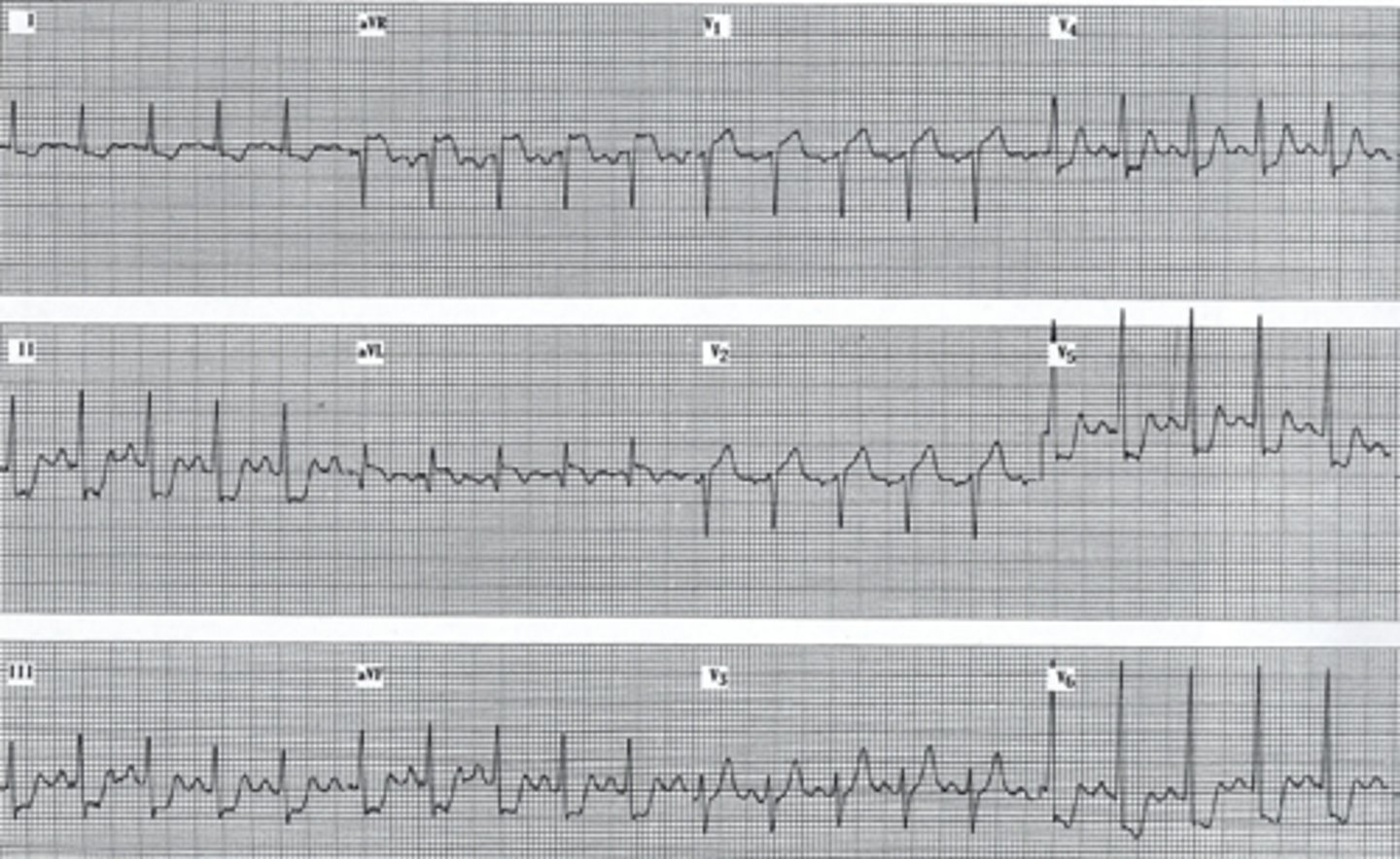
Downsloping ST depression
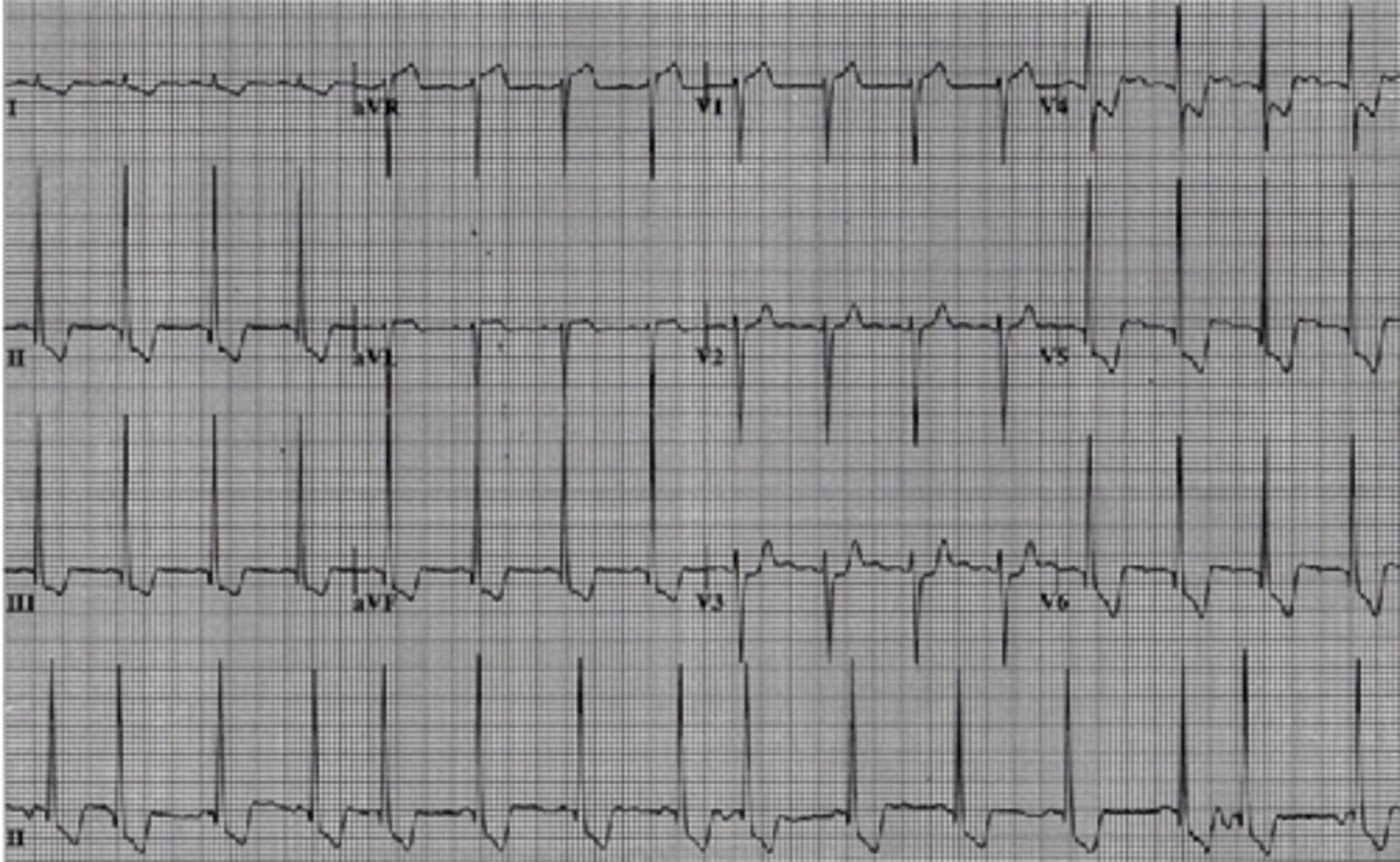
T wave inversion
This may be an indication of ischemia. If a subject goes from a supine to standing position suddenly this may occur briefly and resolve quickly. Chronic T wave inversion equals ischemia.
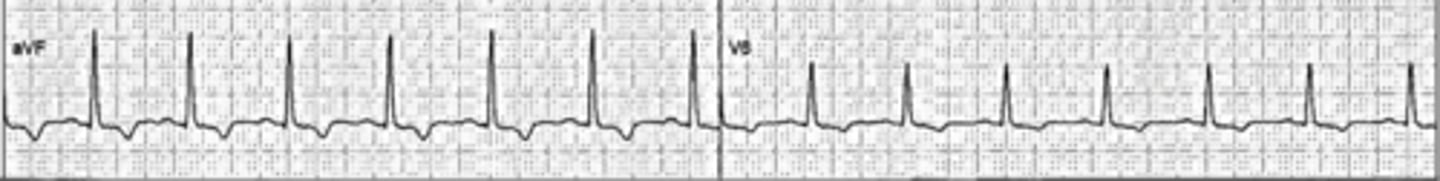
pacemaker
Needed for slow heart rates that are not sufficient to meet the demands of the body
•Vibration and acceleration is best sensor method.
•Best exercise to evaluate pacemaker: Treadmill
•Most common indication for pacemaker implantation is: Under the left clavicle above the heart.
Ventricular paced rhythm
single lead, ventricles
Pacemakers sense and respond to changes in body. The most common sensor method used is vibration and acceleration
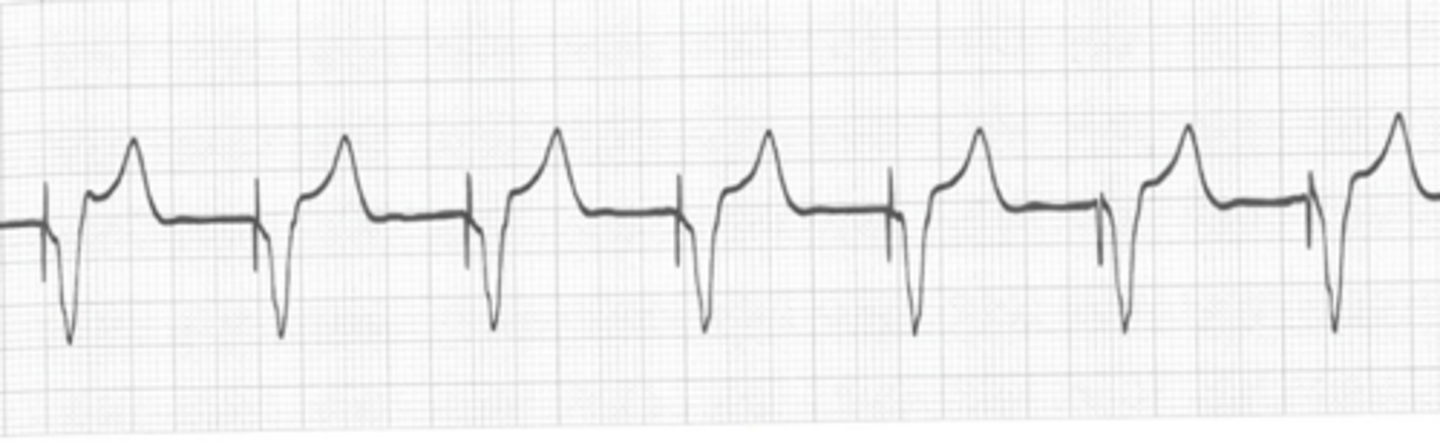
Ventricular paced rhythm
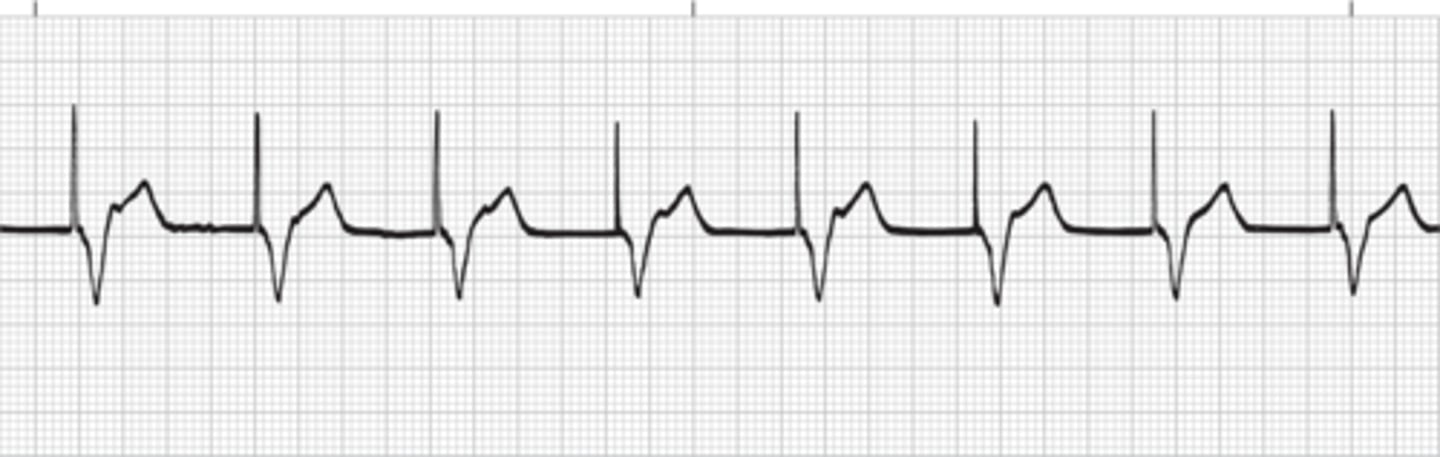
dual chamber pacemaker
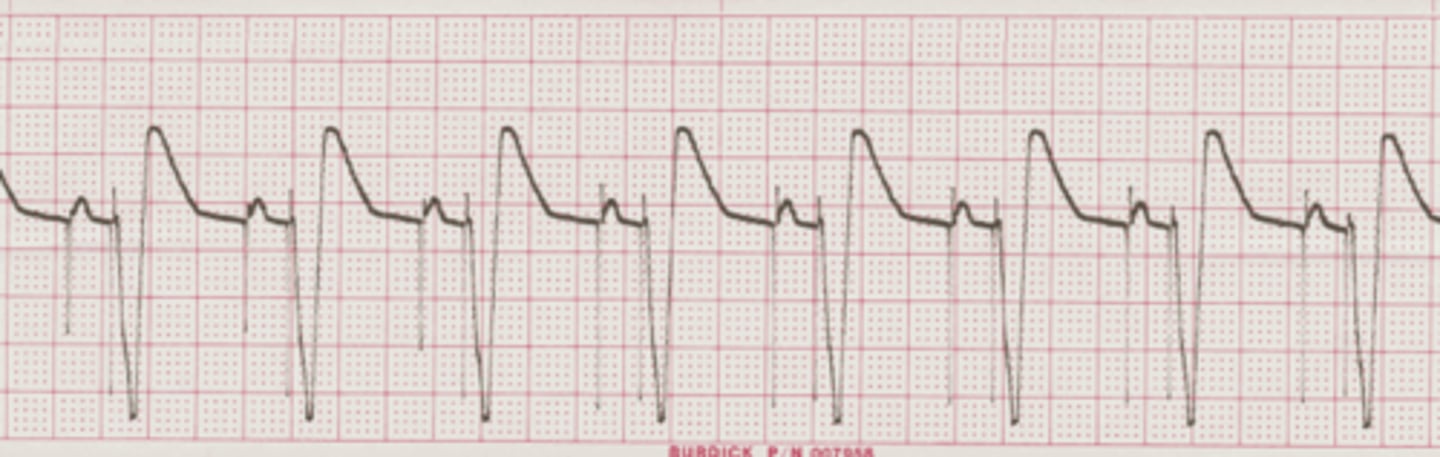
Inferior MI
Right Coronary Artery.
ST Elevation in II, III, and aVF
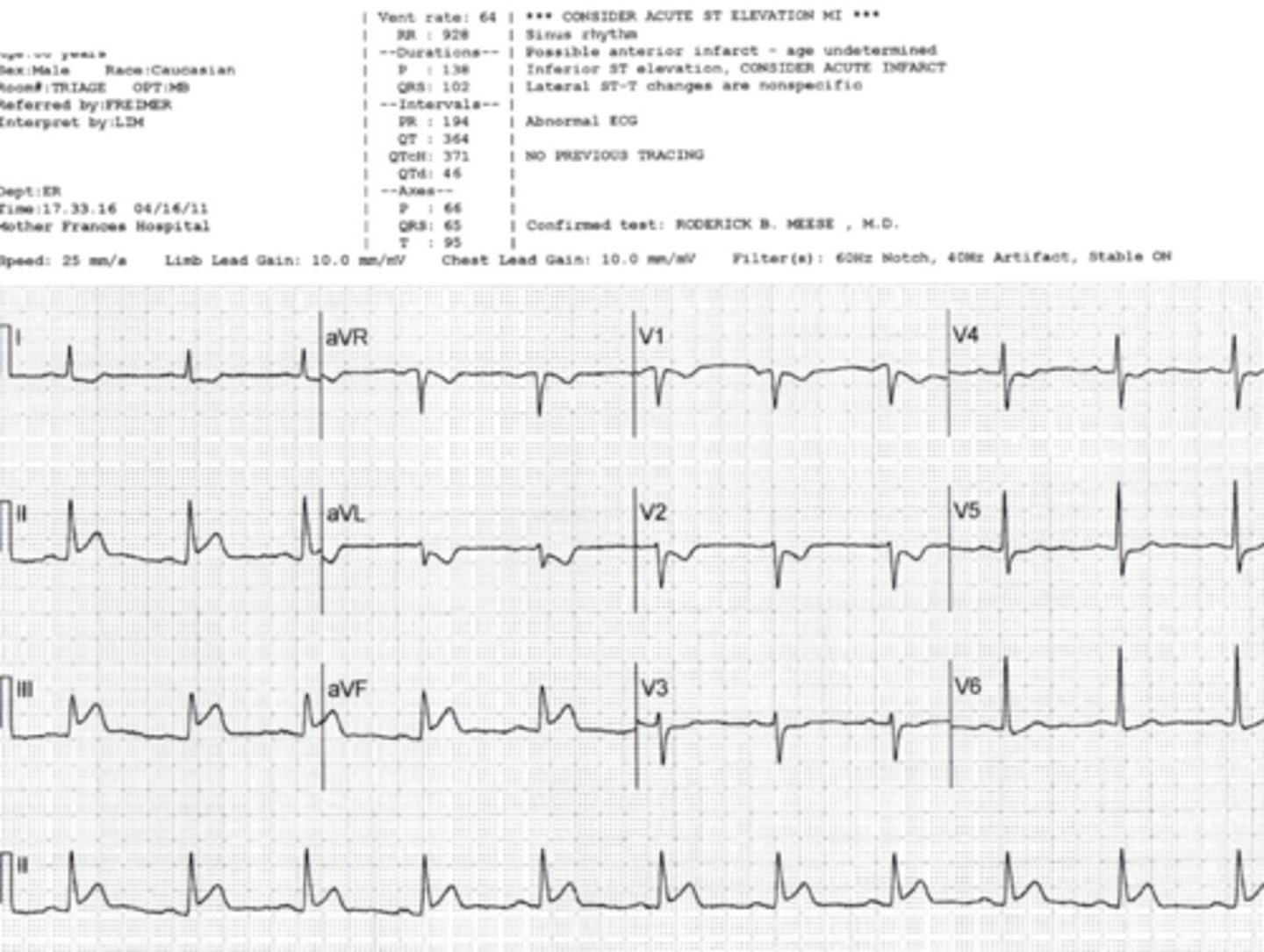
anterior MI
1.Changes occur in precordial leads (V1 to V6); also, in leads I and aVL when left main artery is occluded.
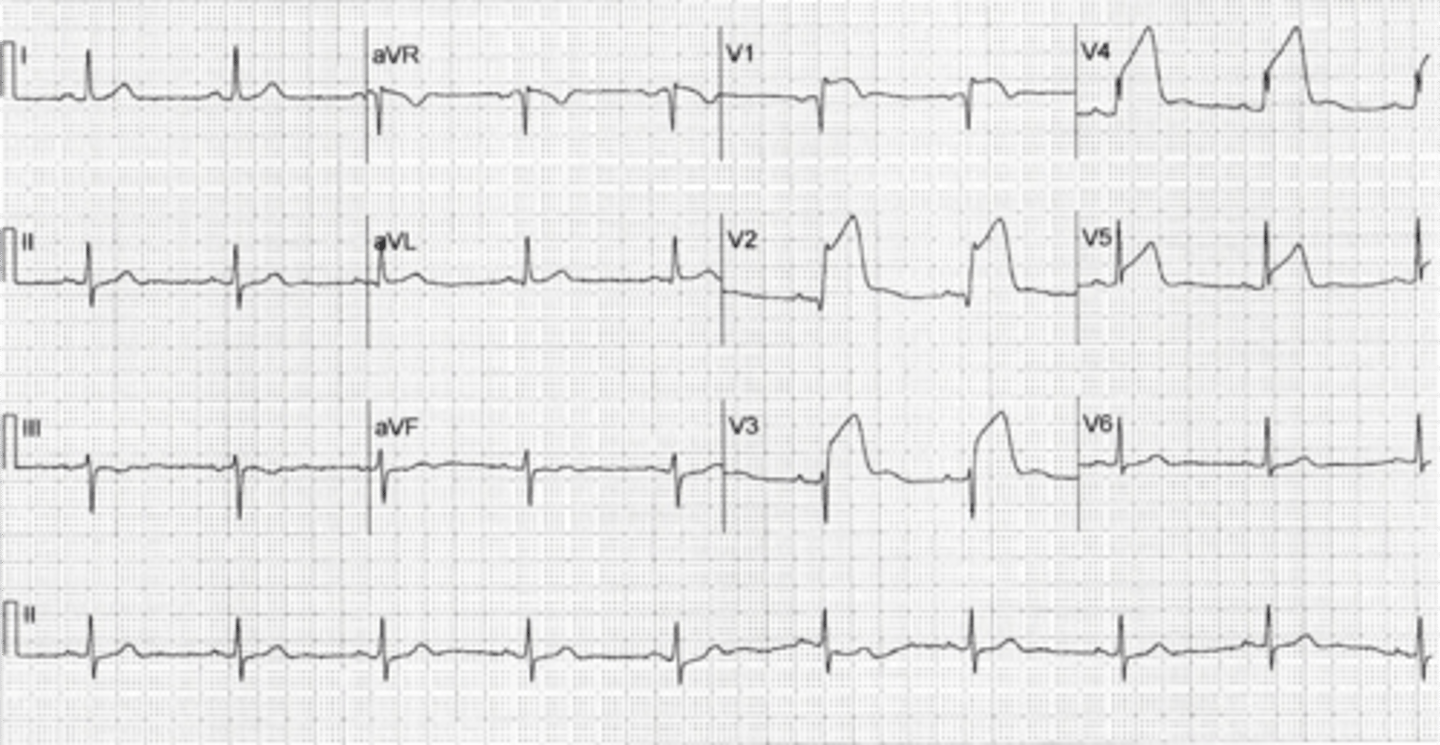
hyperkalemia
•Variety of presentations on EKG.
•Classic: progression to ventricular fibrillation and death
1.T waves peak. Normal: 1/3-2/3 height of the R wave.
2.PR interval lengthens, P wave flattens and disappears.
QRS complex widens until it merges with T wave.
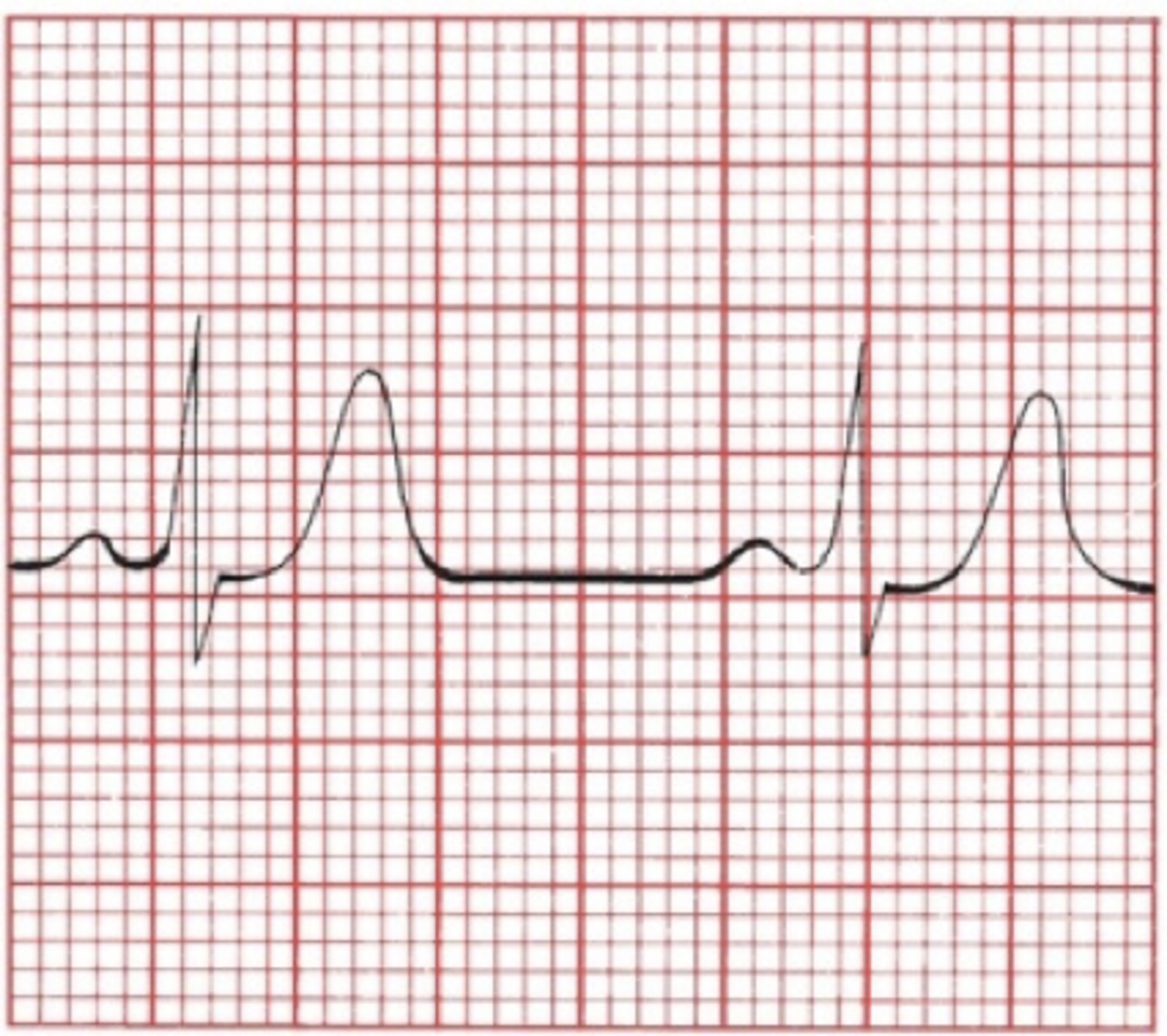
hyperkalemia
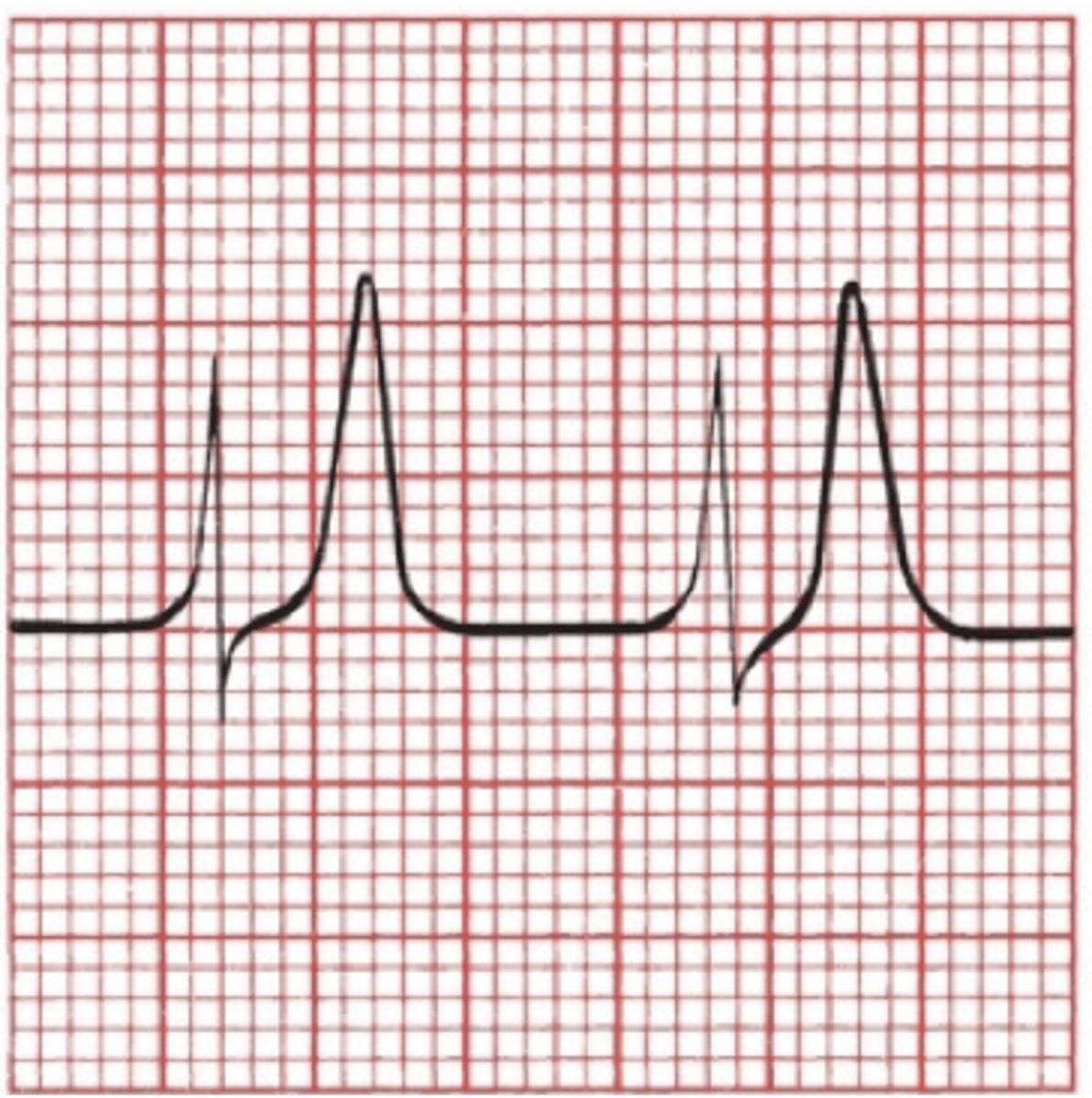
hyperkalemia
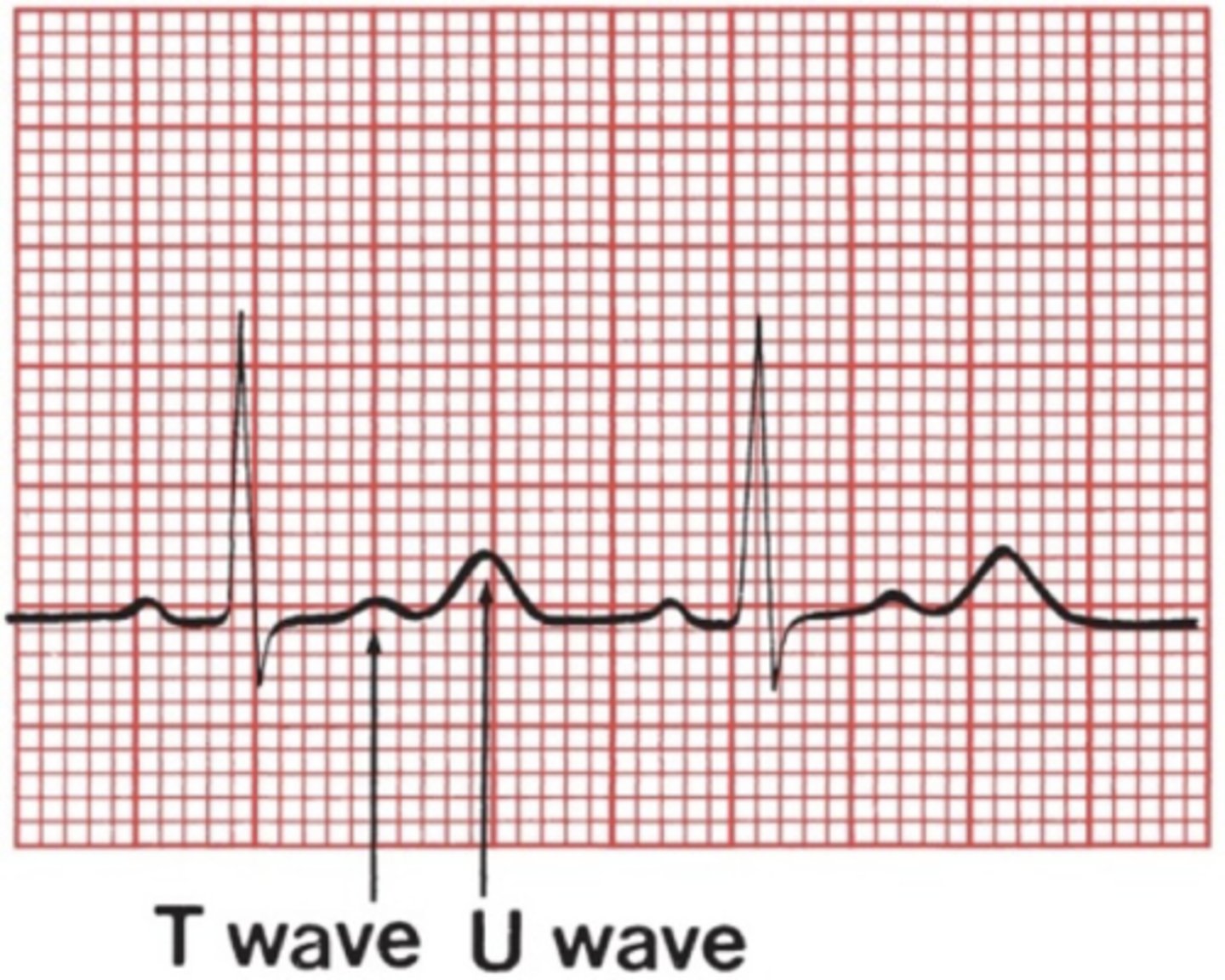
hypokalemia
•EKG changes (in no particular order)
•ST-segment depression or, rarely, elevation
•Flattening of T wave with prolongation of QT interval Normal QT interval: (0.36-0.44) or 9-11 boxes.
•Appearance of a U wave
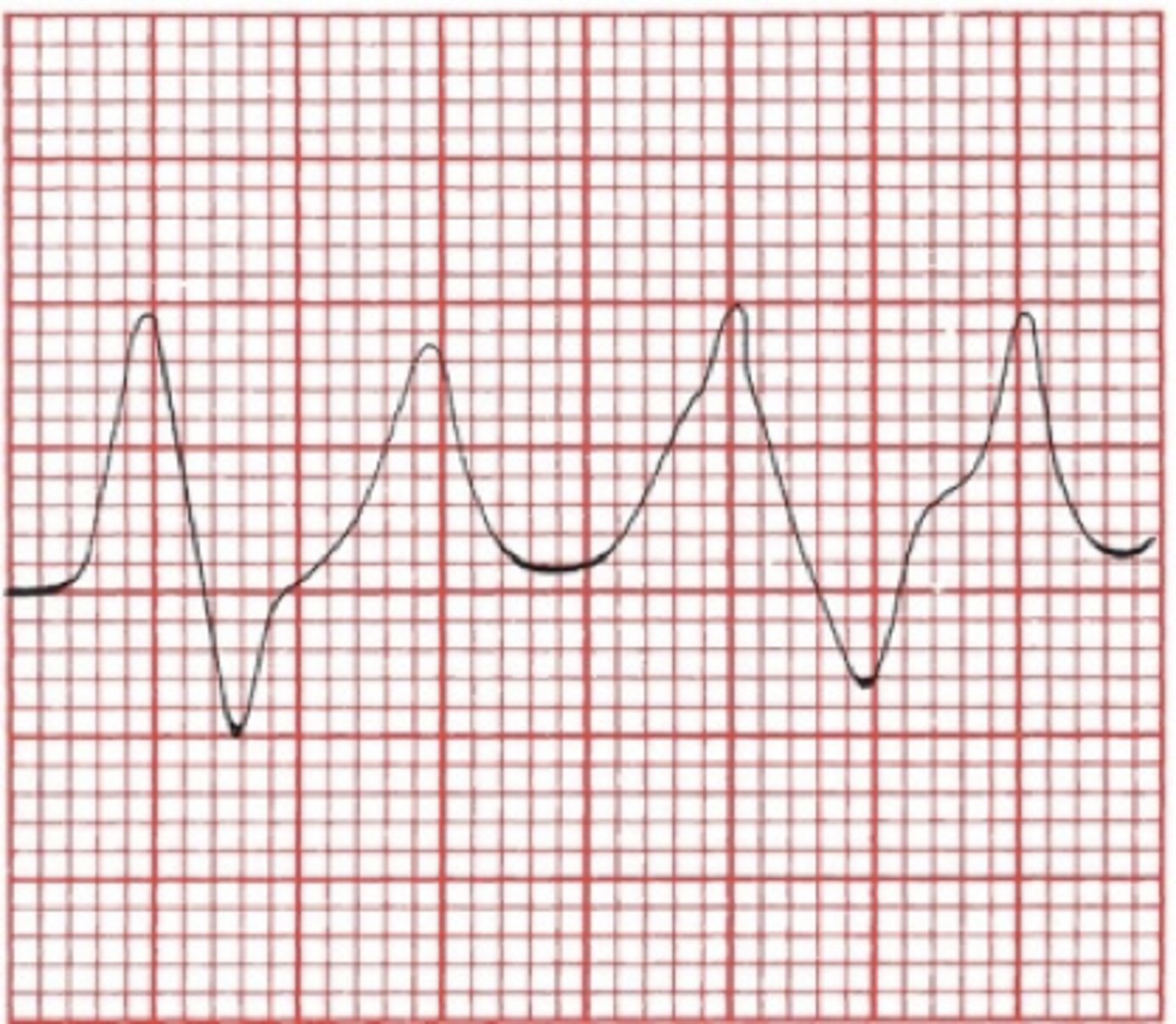
hypocalcemia - leading to torsades de pointes
Calcium Disorders
•Hypocalcemia prolongs QT interval. – Leads to Torsades de pointes
•Hypercalcemia shortens QT interval.
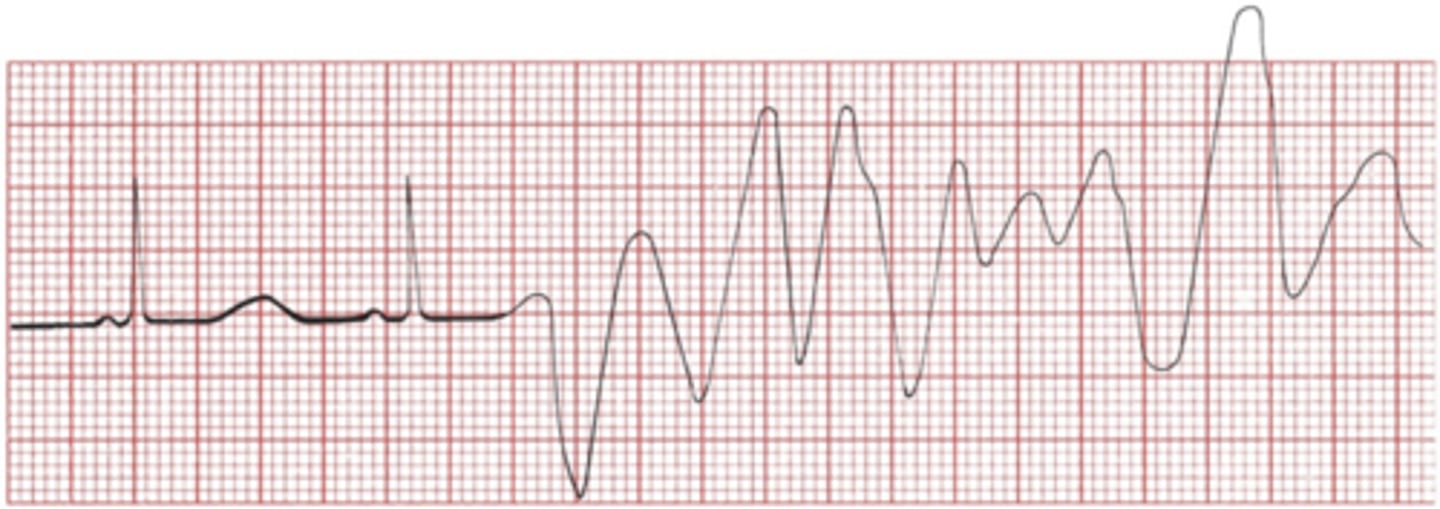
digitalis (drugs)
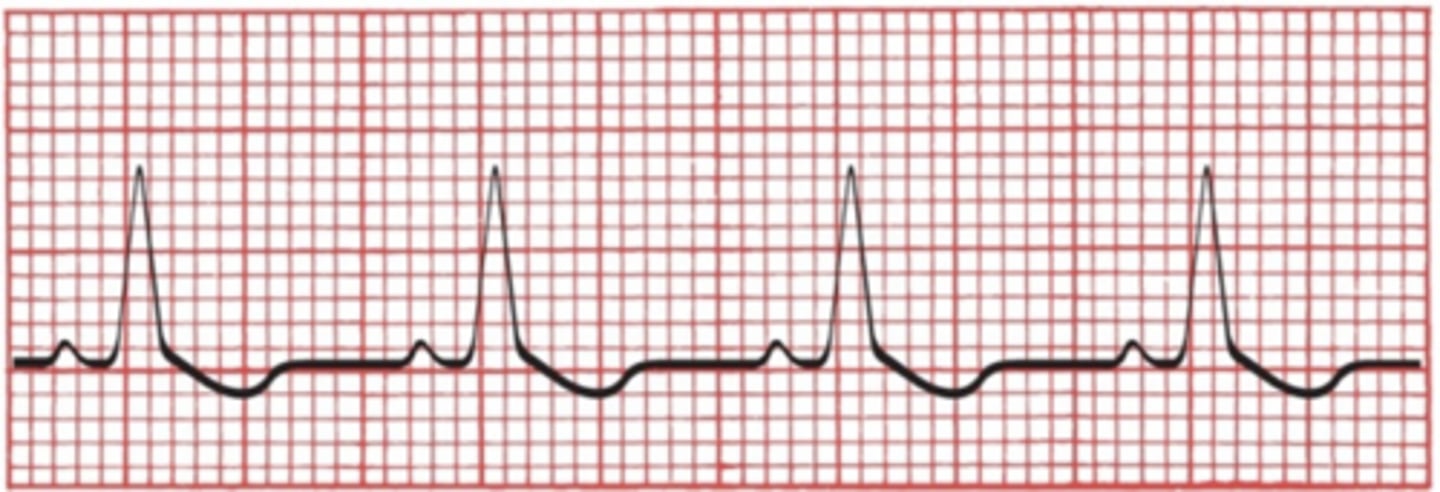
Right Ventricular Hypertrophy
•Typically benign and asymptomatic.
•Symptoms may include:
–Dyspnea
–Dizziness or syncope,
–Edema of the ankles, feet, and legs
–Frequent episodes of sinus tachycardia
•Appearance on ECG
–Right axis deviation may or may not be present (> 100 degrees).
–Tall R waves in V1 and V2 ≥ 7 mm.
–R-S ratio ≥ 1 in V1 and V2
–Right ventricular strain pattern evident in V1 and V2.
–Deep S waves in right chest leads.
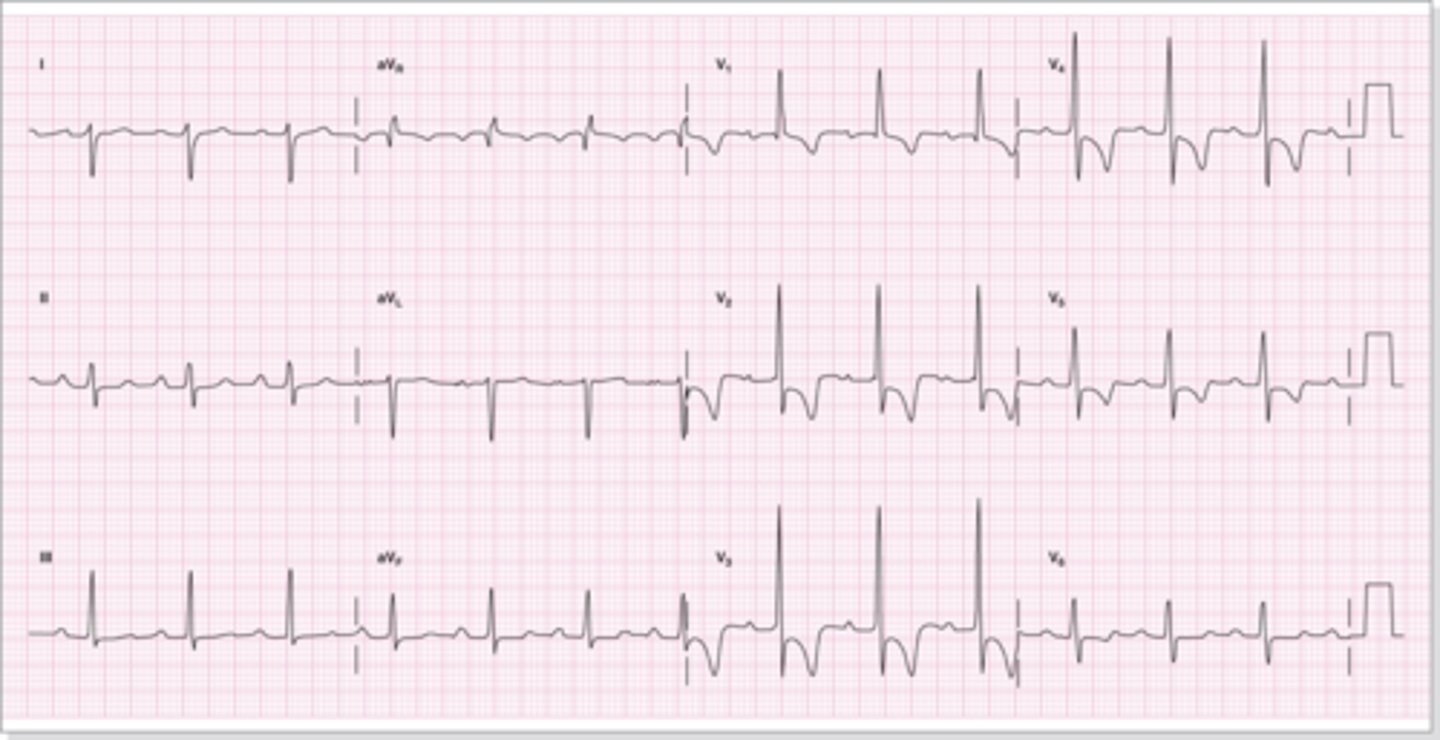
left ventricular hypertrophy
•Appearance on ECG
–QRS complex upper limit of normal.
–Taller than normal R waves.
–Deeper than normal S waves will occur in the right chest leads.
–S wave in V1 or V2 plus the R wave in V5 or V6 > 35 mm.
–Left ventricular strain pattern in the left chest leads.
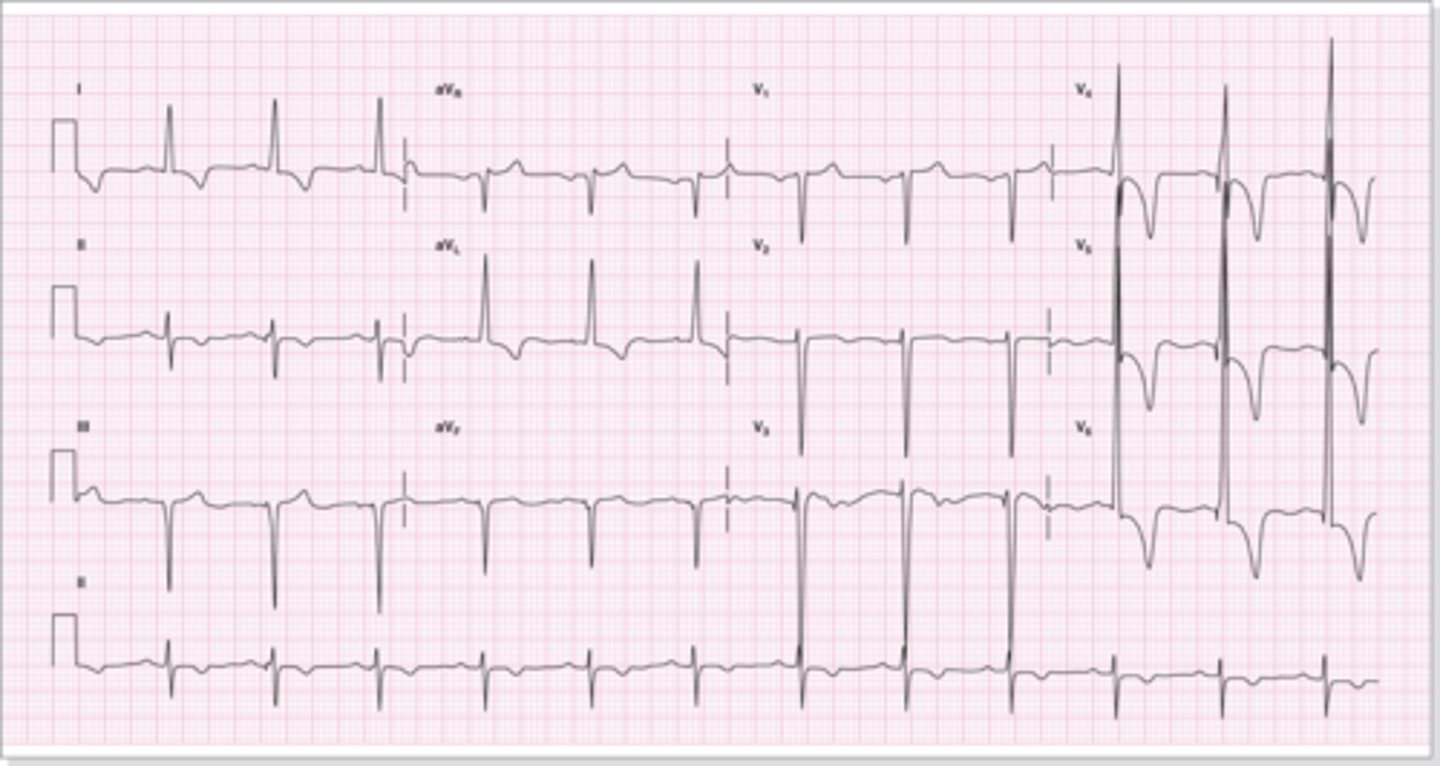
left ventricular hypertrophy
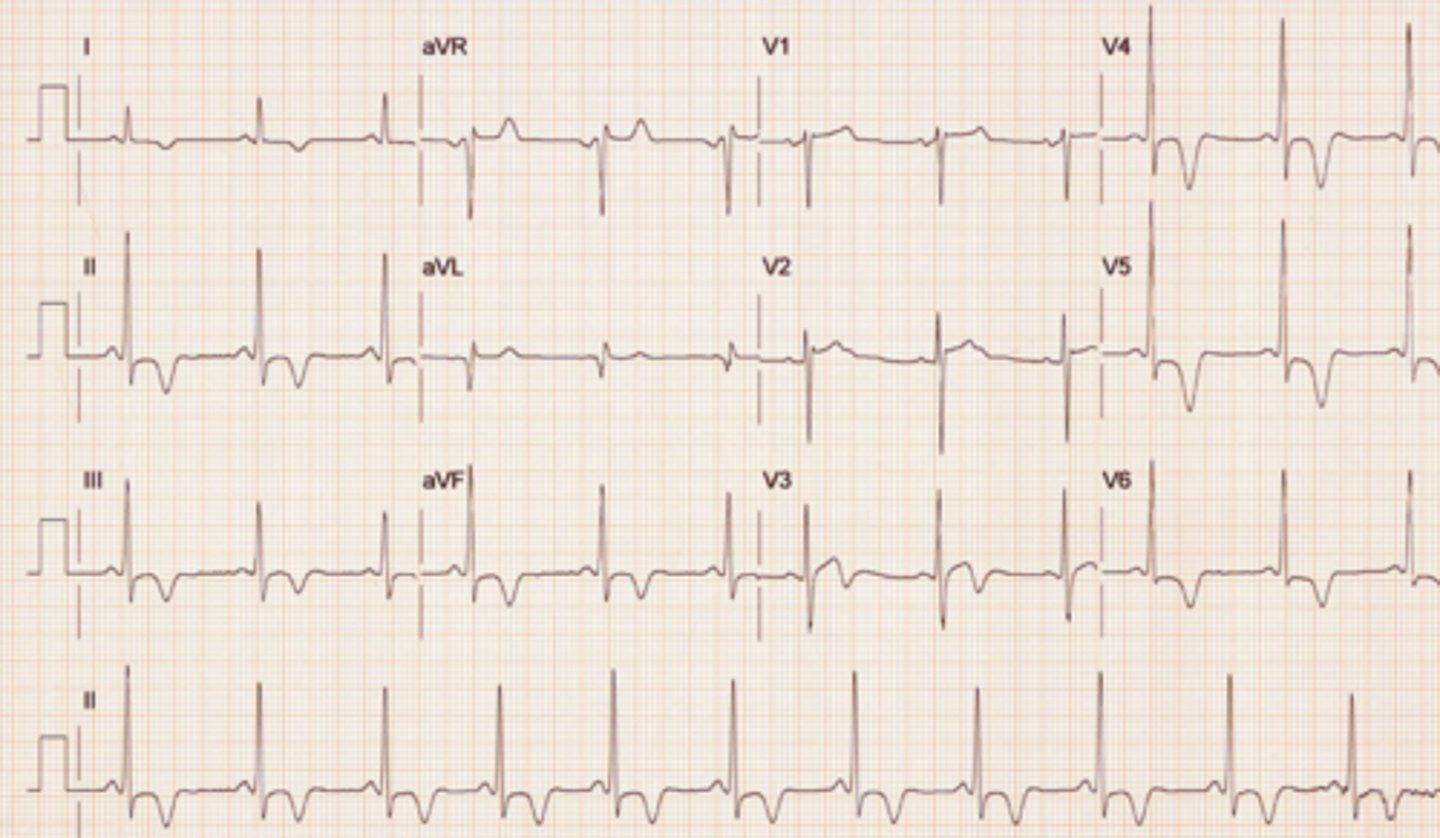
Sinus Arrhythmia
A sinus rhythm in which the rate varies with respiration, causing an irregular rhythm.
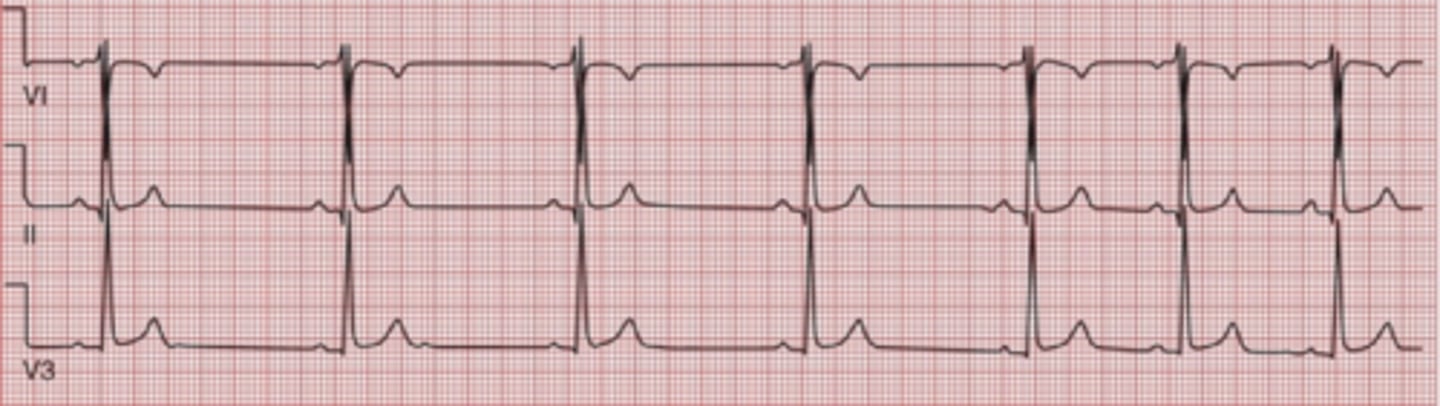
sinus arrhythmia
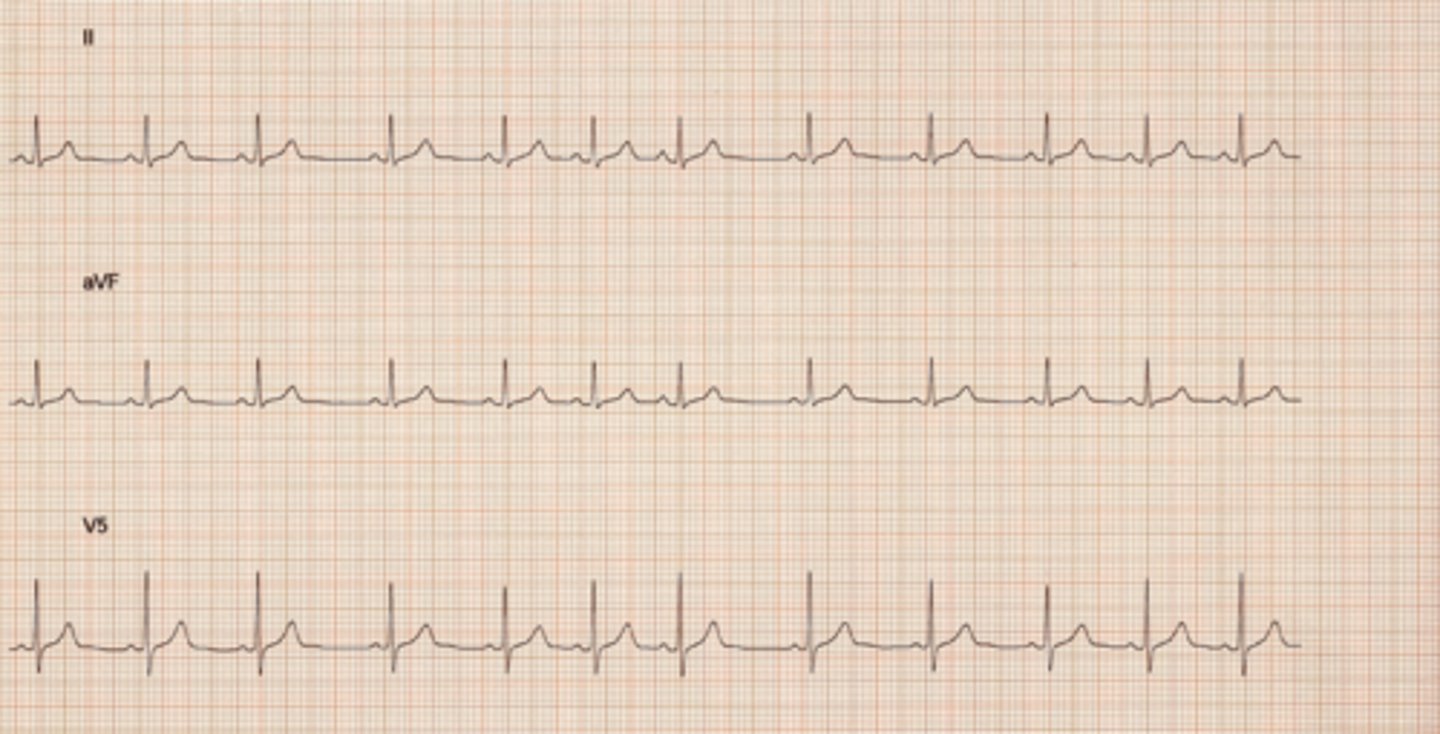
NSR with sinus block
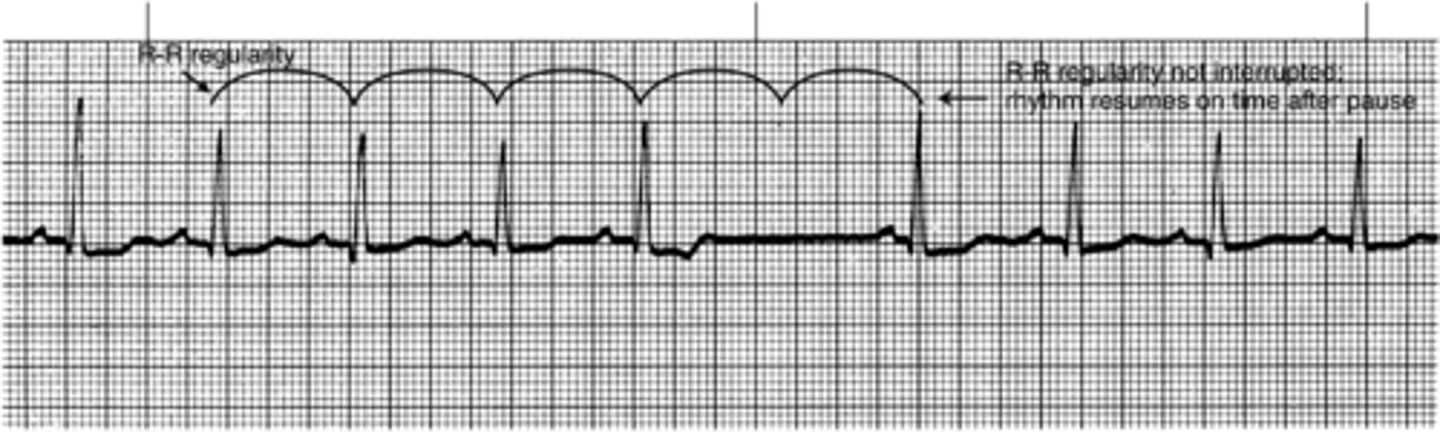
Normal Sinus Rhythm with sinus arrest
Rhythm: Basic rhythm regular; irregular during pause
Rate: Basic rhythm 94 beats/minute
P waves: Normal in basic rhythm; absent during pause
PR interval: 0.16 to 0.18 second in basic rhythm; absent during pause
QRS complex: 0.06 to 0.08 second in basic rhythm; absent during pause
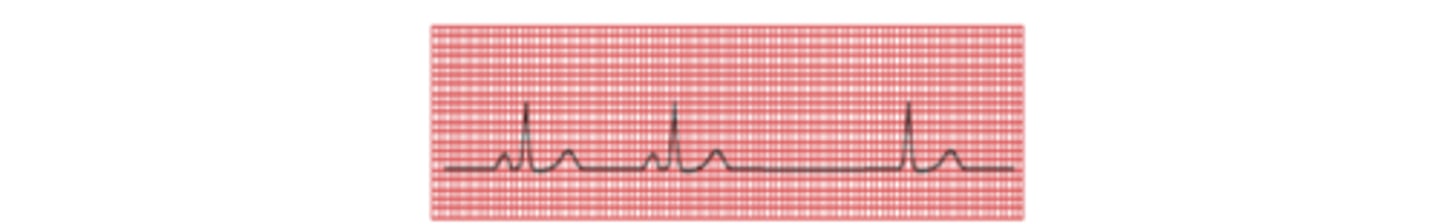
NSR with Sinus Arrest
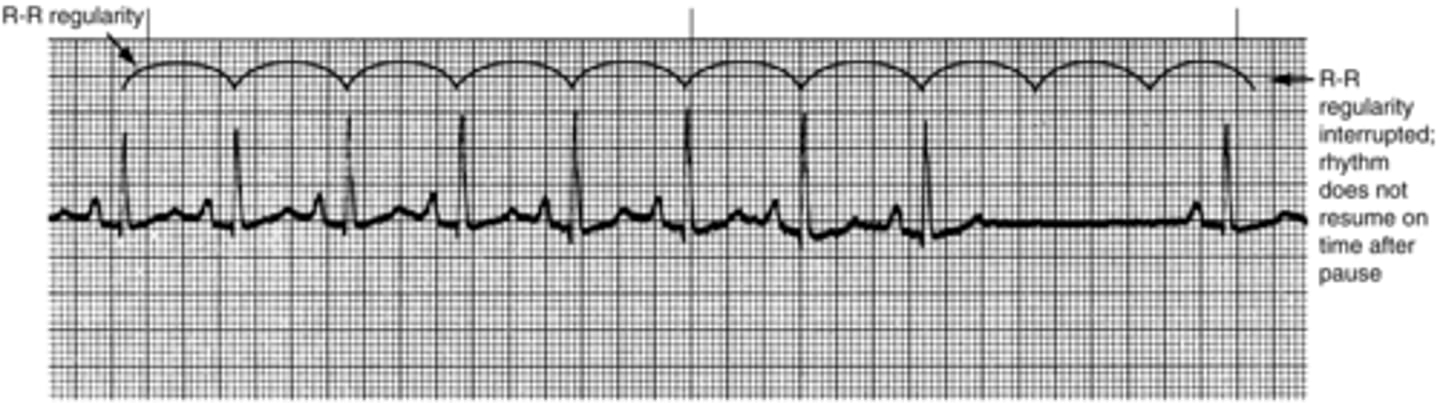
sinus exit block
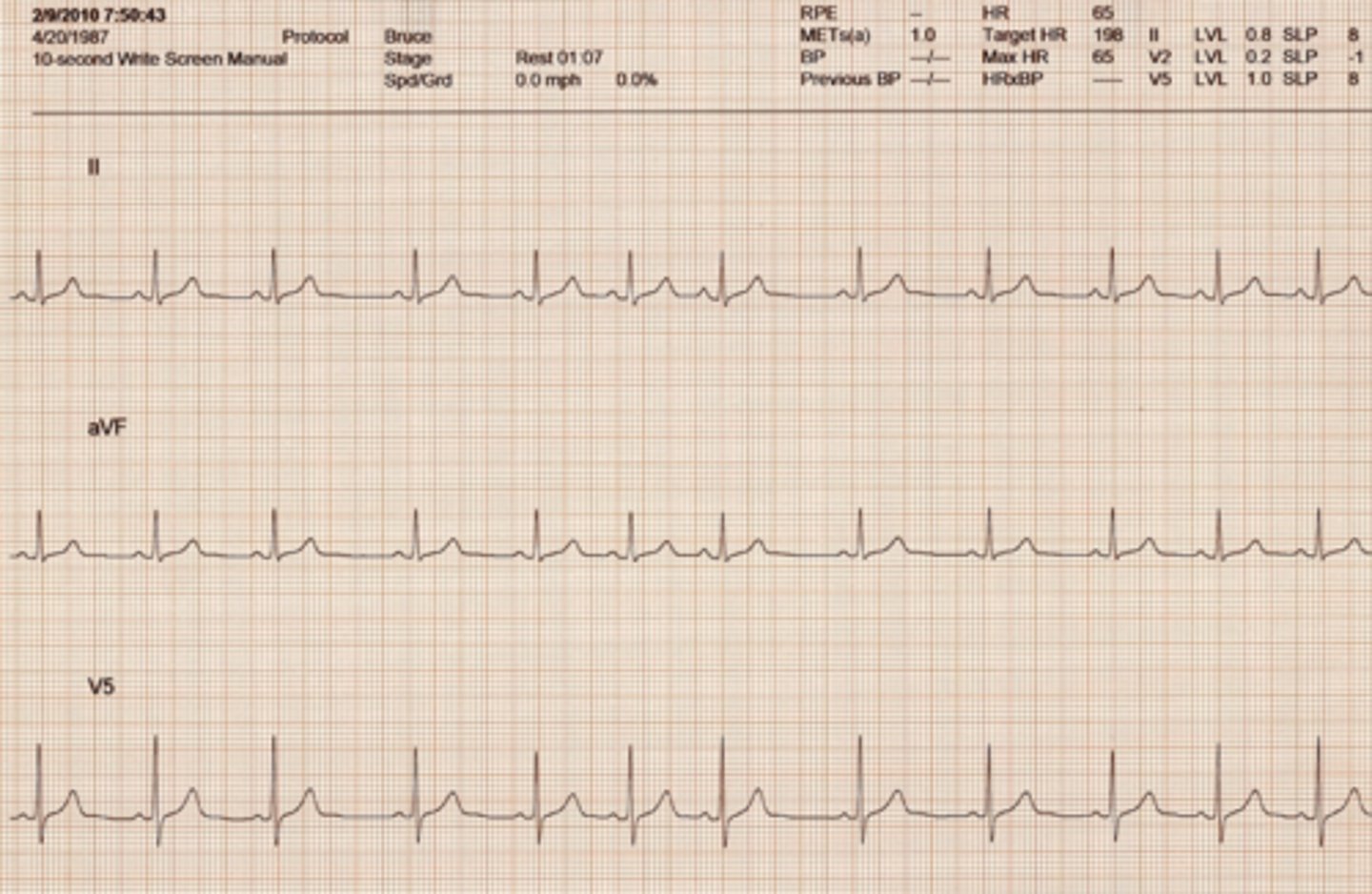
Wandering Atrial Pacemaker
Rhythm: Regular
Rate: 40 beats/minute
P waves: Vary in size, shape, or direction across strip
PR interval: 0.12 - 0.16 second
QRS complex: 0.08 second
The beat is initiated at the SA node and other sites close to it. Thus the difference in appearance but the same PR Interval length.
Slower heart rate.
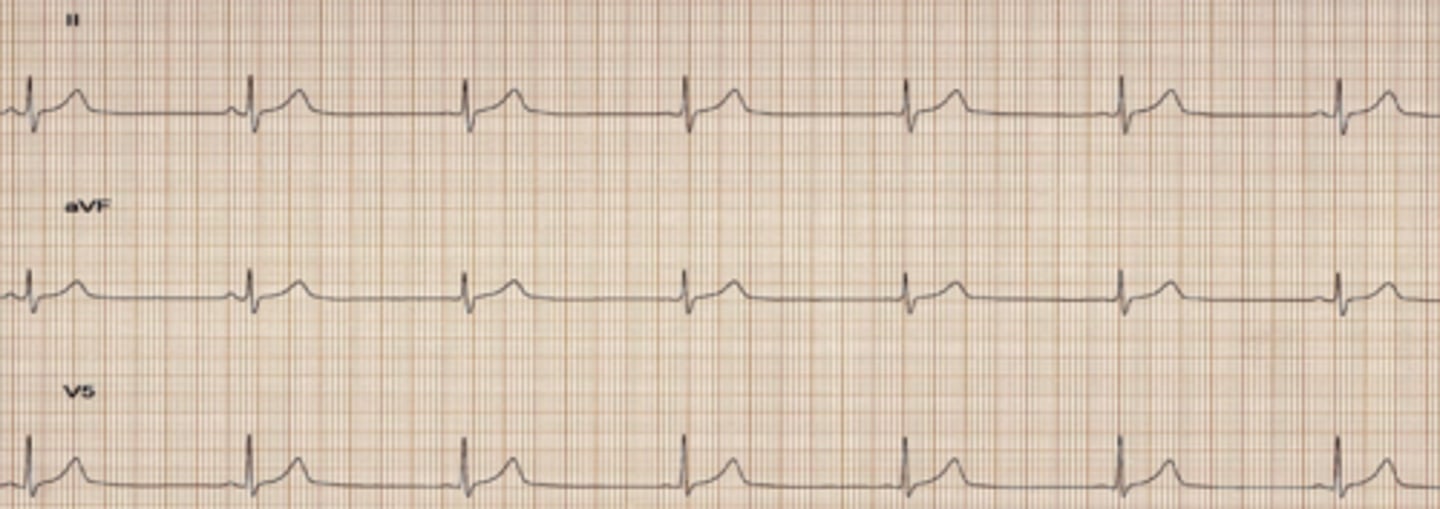
Wandering Atrial Pacemaker (WAP)
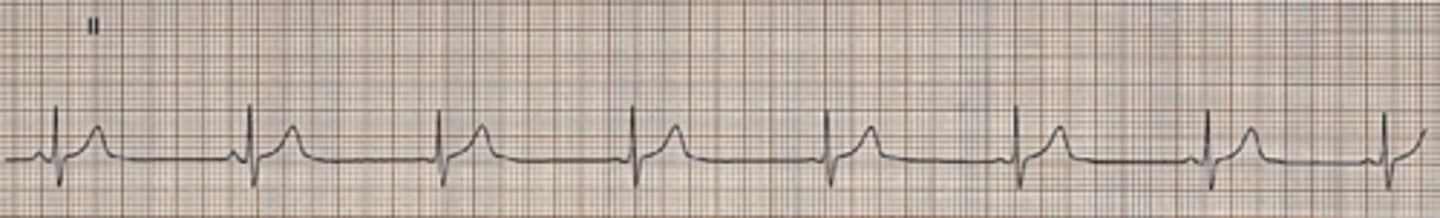
premature atrial contraction
•The nonconducted PAC is the most common cause of unexpected pauses in a regular sinus rhythm.
•Can be confused with sinus arrest or sinus exit block, especially if the P wave of the nonconducted PAC is hidden in the preceding T wave.
•To differentiate between the nonconducted PAC and sinus arrest or block, one must examine the T waves. If the nonconducted PAC occurs very early, the abnormal P wave will distort the preceding T wave. In sinus arrest or block, no P wave is produced and the T-wave contour is unchanged.
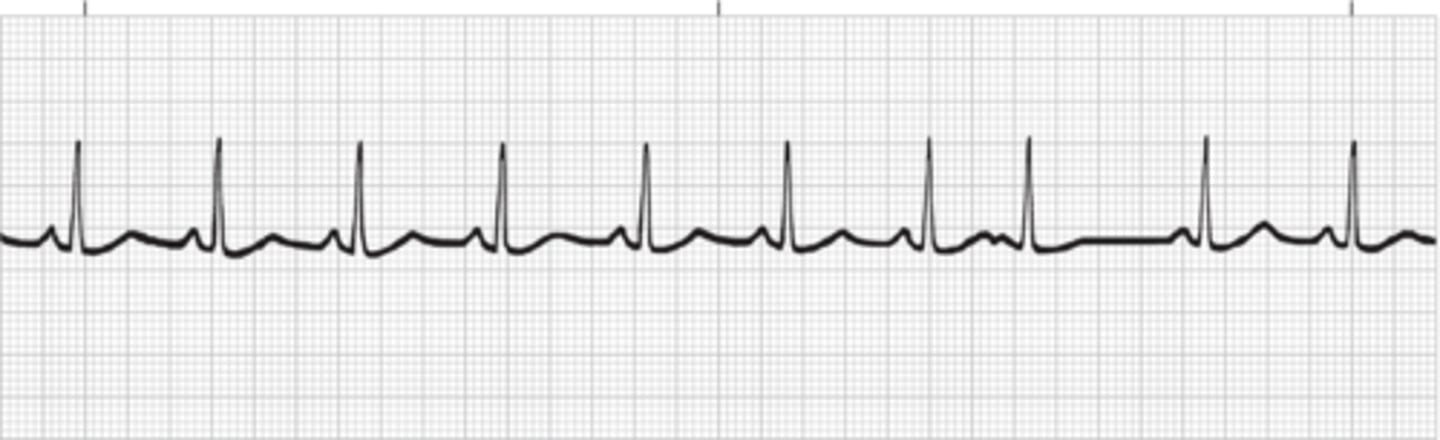
Premature Atrial Contraction (PAC)
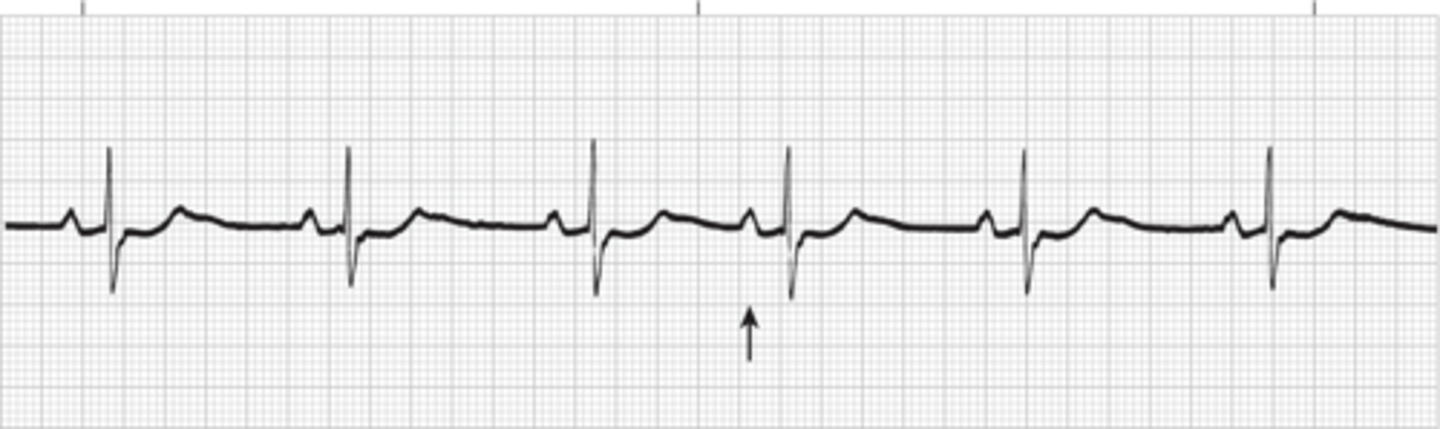
Normal sinus rhythm with a PAC
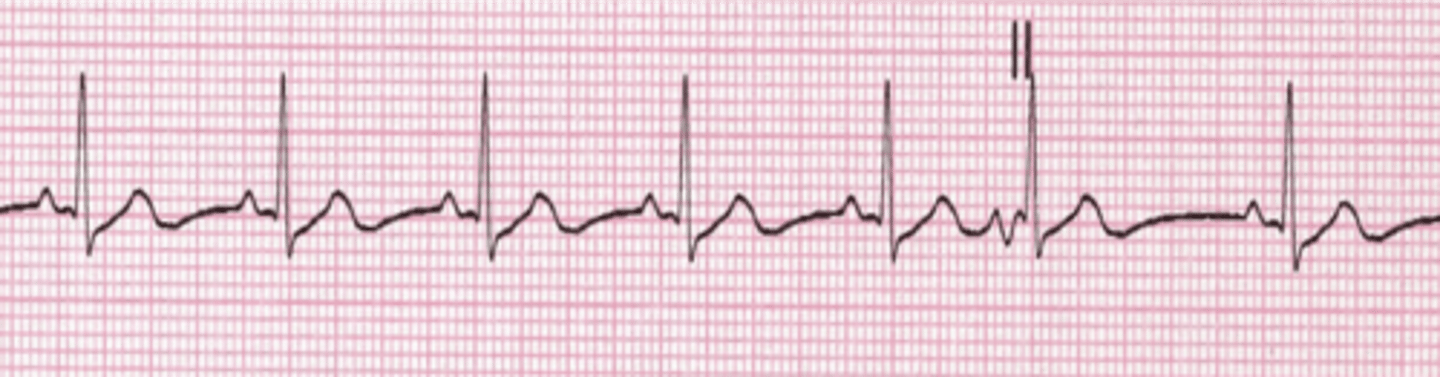
A-fibb
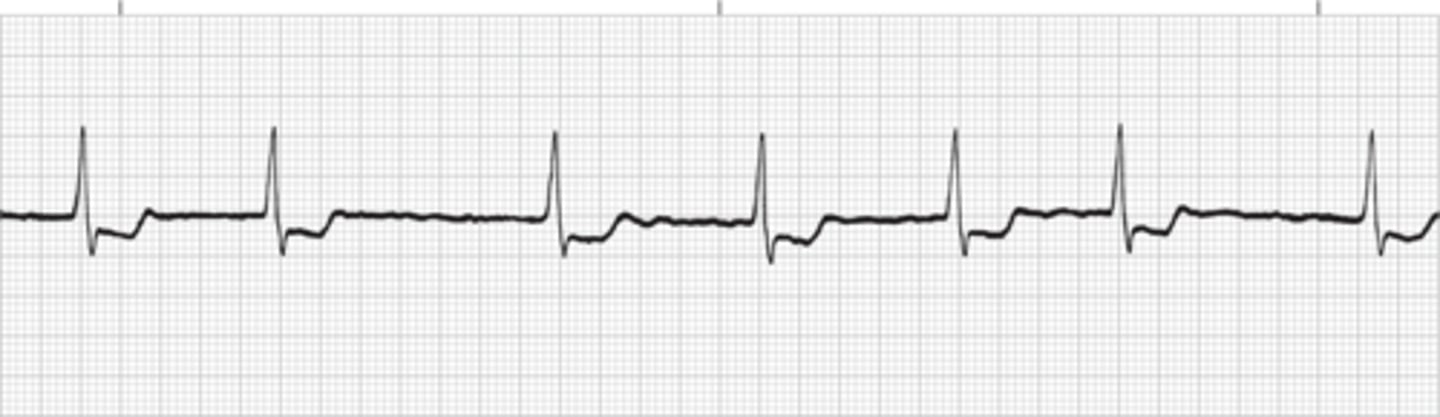
sinus bradycardia with 1st degree AV block
The PR interval is greater than 0.20 seconds; all beats are conducted through to the ventricles.
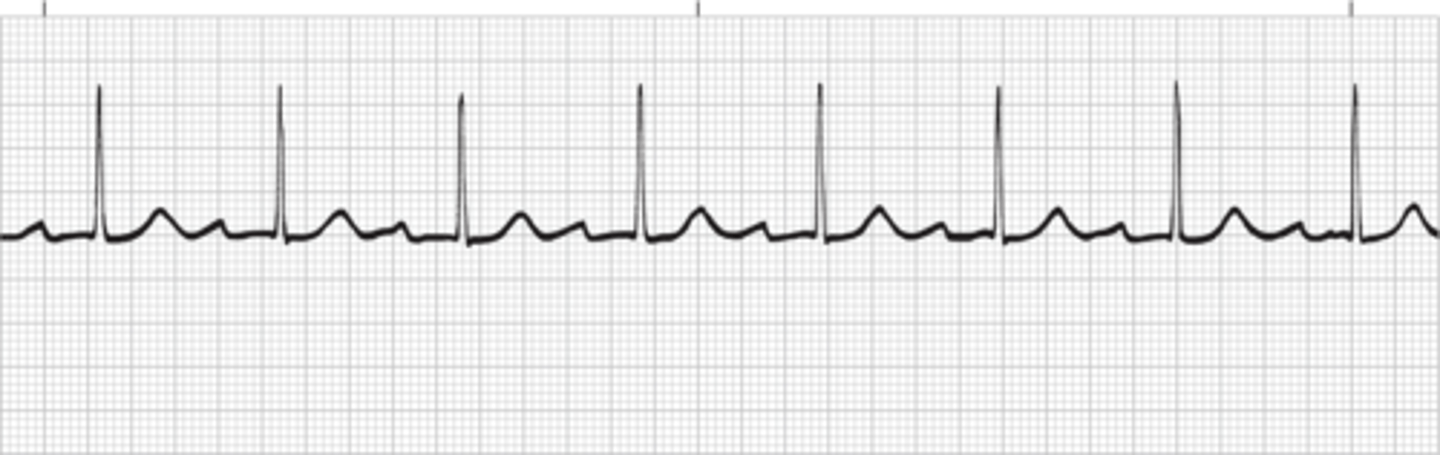
Third-degree AV block
There is no conduction of impulses from the atria into the ventricles. The atria and ventricles beat independently of each other with no relationship between the P waves and QRS complexes. The atria are usually paced by the sinus node, and the ventricles are paced by a junctional or ventricular.
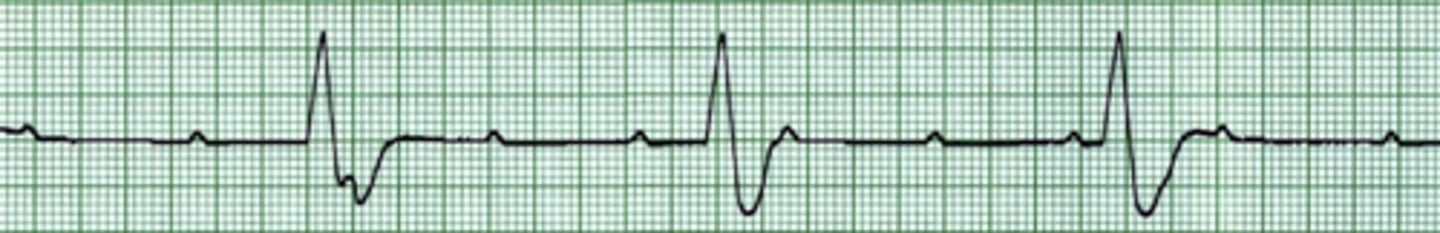
Third-degree AV block
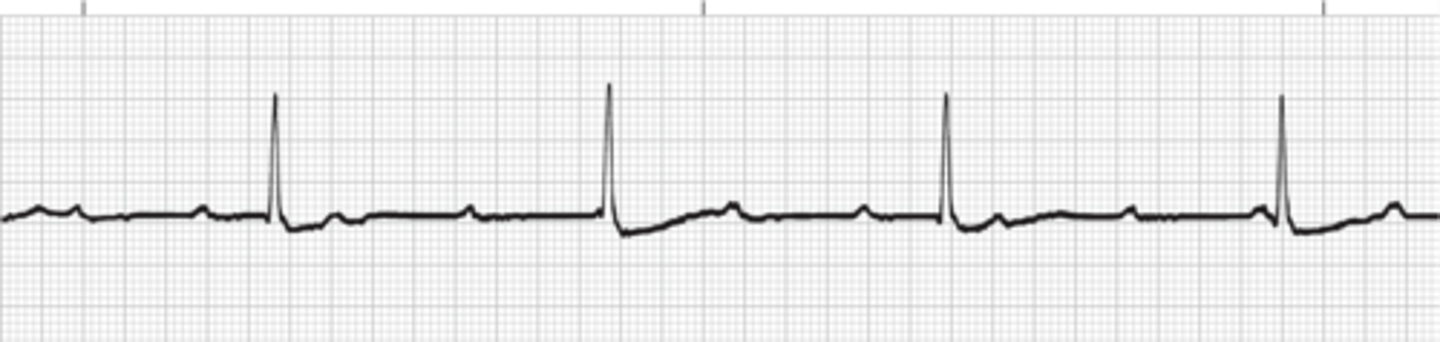
junctional premature complex
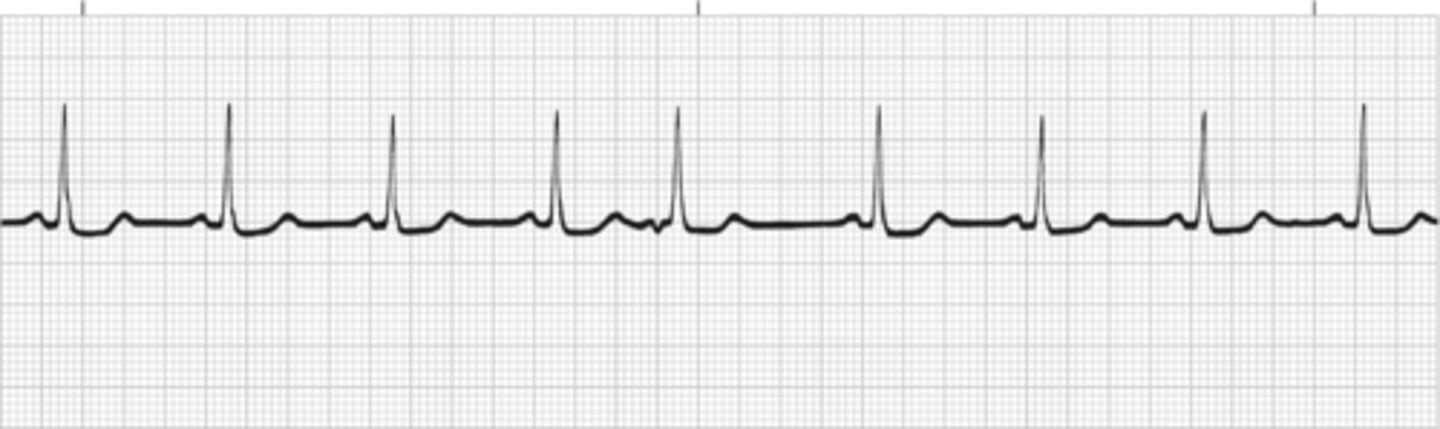
Junctional Rhythm
Junctional rhythm originates in an ectopic pacemaker site in the AV junction at a rate of 40 to 60 beats/minute. It occurs as a regular, continuous rhythm and is characterized by an inverted P wave that may occur before the QRS, after the QRS, or be hidden within the QRS complex; a short PR interval of 0.10 second or less; and a normal QRS complex.
•The rhythm rarely requires treatment unless the rate is too slow to maintain cardiac output.
•If the rate is slow and the patient is symptomatic, atropine can be given to increase the sinus rate and override the junctional focus. Pacing may become necessary.
•Treatment should also be directed toward identifying and correcting the underlying cause.
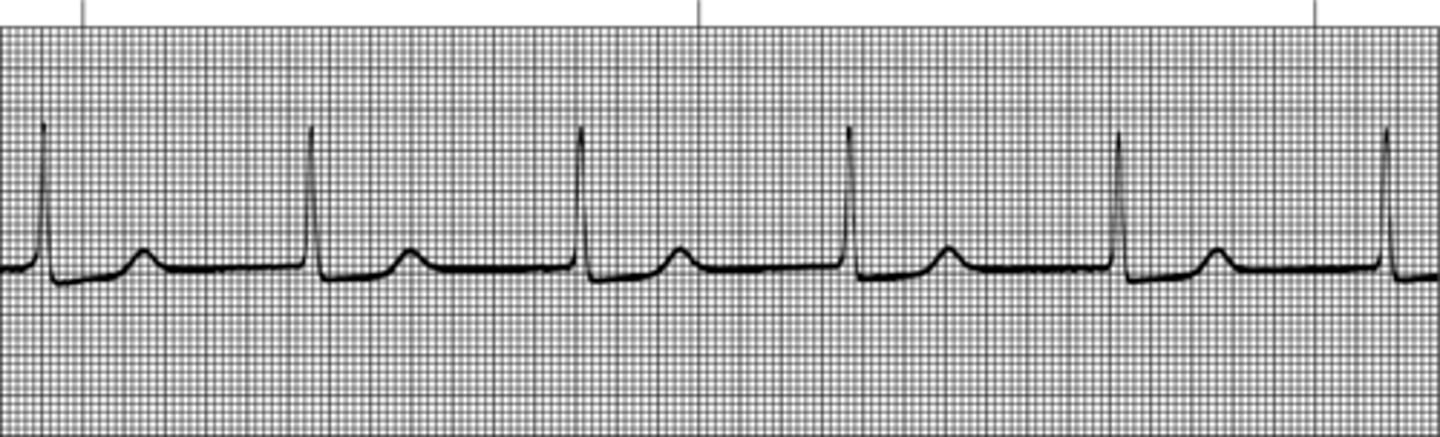
Accelerated Junctional Rhythm
Accelerated junctional rhythm originates in an ectopic pacemaker site in the AV junction at a rate of 60 to 100 beats/minute. The term accelerated denotes a rhythm that occurs at a rate faster than the inherent junctional rate of 40 to 60 beats/minute, but that isn't fast enough to be junctional tachycardia. Accelerated junctional rhythm is a regular, continuous rhythm characterized by an inverted P wave that may occur before the QRS, after the QRS, or be hidden within the QRS complex; a short PR interval of 0.10 second or less; and a normal QRS complex.
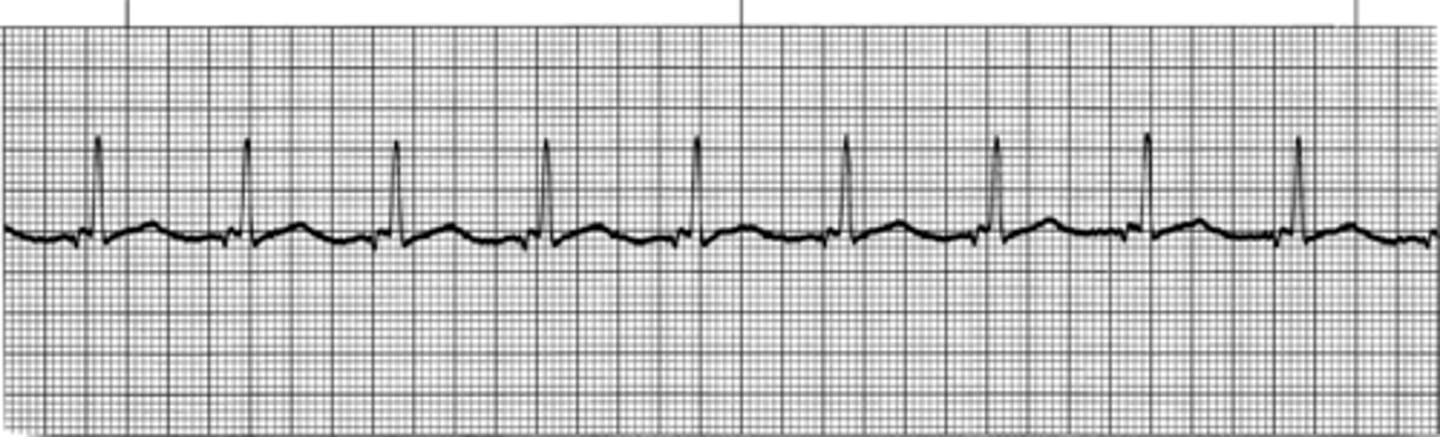
Normal Sinus Rhythm changing to accelerated junctional rhythm
Rhythm: Regular (first and second rhythms)
Rate: 84 beats/minute (first rhythm); 94 beats/minute (second rhythm)
P waves: Sinus (first rhythm); inverted before each QRS (second rhythm)
PR interval: 0.12 second (first rhythm); 0.08 - 0.10 second (second rhythm)
QRS complex: 0.06 - 0.08 second (first and second rhythms)
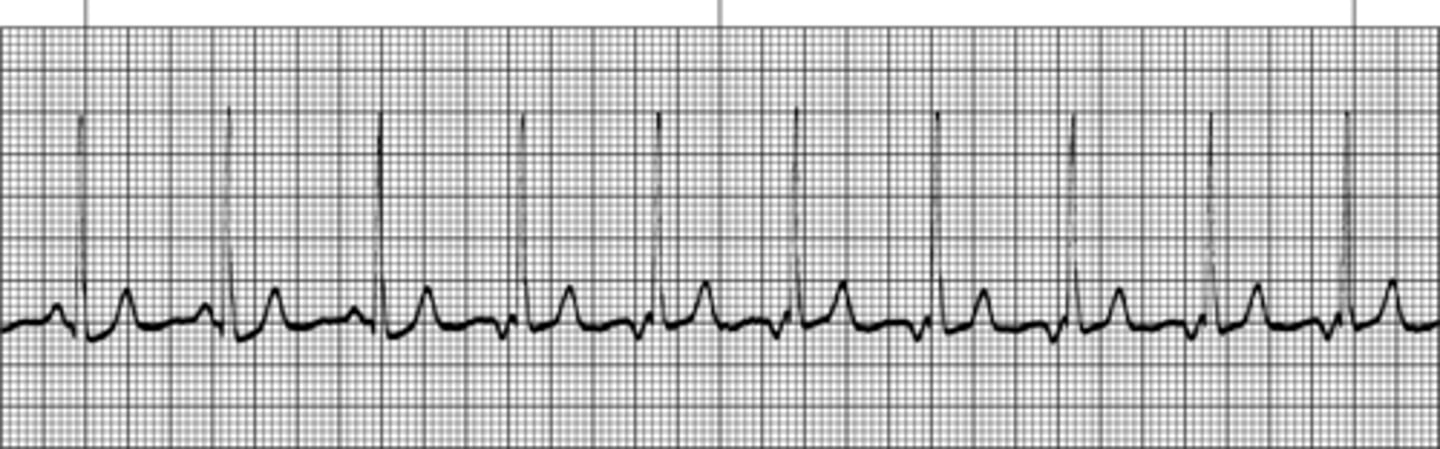
Wandering Baseline
This occurs when the breathing of the subject is heavy. Standard electrode placement is on the area of the breathing muscles. So as the chest expands and returns to normal during breathing the ECG baseline may become altered.
ECG computers work to filter this out on most occasions but it still occurs. This is sinus tachycardia but on the test the answer will be "wandering baseline".