VTNE Review: Common Horse Diseases
1/75
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
76 Terms
valvular disease
common in foals (congenital) and in mature horses (degenerative or infectious)
diseased valves may either impede normal flow (stenosis) or allow backflow (insufficiency) which increases the workload of the heart and decreases cardiac output
common causes include endocarditis and ruptured chordae tendinae
clinical signs of vascular disease
murmur
increasing exercise intolerance
± fever (with endocarditis)
± weight loss
± intermittent lameness
± arrhythmias
development of CHF
sudden death
diagnosis of valvular disease
clinical findings
ECG
ECHO with doppler study
exercise testing
if endocarditis
anemia
decreased blood protein
leukocytosis
positive blood cultures
holter monitoring
treatment of valvular disease
depends on severity of symptoms and location of the lesion
degenerative valve disease
usually results in valvular insufficiency or a leaky valve
with every contraction, blood is pumped forward out of the ventricles, but much of the chamber volume is also pumped backward into the atria
increases the volume in the chambers for the next contraction (preload)
as the chambers become overstretched, they must work harder until they begin to fail
treatment of degenerative valve disease
manage the development of CHF and cardiac arrhythmias
furosemide (oral)
digoxin (1-2 times daily orally)
ACE inhibitor: 2 times daily (avoid use in pregnant mares)
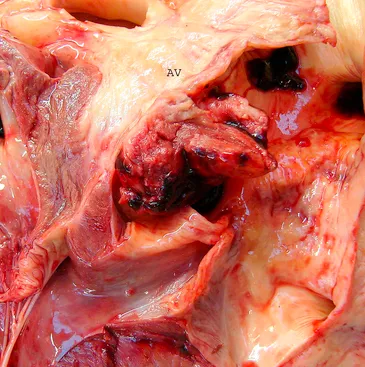
bacterial endocarditis
inflammatory disease of the lining tissue of the heart
most common location for lesions is on the left AV valve or on the left side of the endocardium
jet lesions from mitral insufficiency or ventricular septal defects typically damage the endothelial lining of the heart
circulating bacteria begin to colonize the damaged area, attracting inflammatory cells, and the cellular debris begins to build up at the site
cardiac output decreases, creating a shock-like syndrome
treatment of bacterial endocarditis
IV antibiotic therapy based on culture and sensitivity results for 4 to 8 weeks
potassium penicillin every 6 hours
Gentamicin once daily
extremely guarded prognosis in most cases
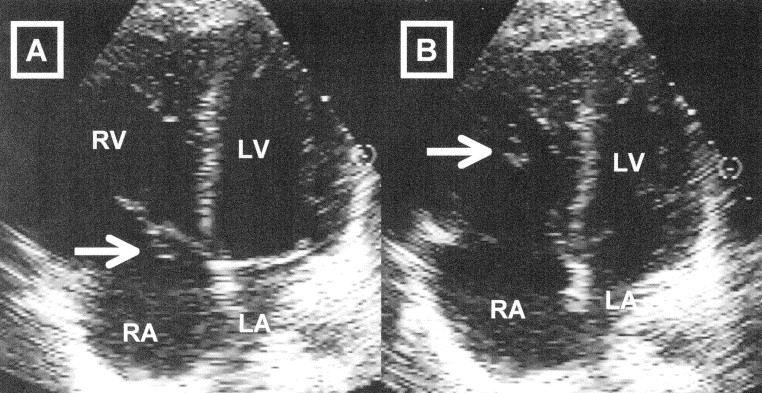
ruptured chordae tendinae
clinical symptoms depend on the number ruptured
tearing of the chordate will result in a flapping of the valve leaflet and produce a valvular insufficiency
greater the number of chordates torn, the worse the leakage of the valve
horse may develop CHF
these horses should not be ridden
clinical signs of ruptured chordae tendineae
increasing exercise intolerance
lethargy
auscultation of murmur
possible sudden death
diagnosis of ruptured chordae tendineae
serum chemistries
ECG
ECHO
treatment of ruptured chordae tendineae
supportive care
as valvular insufficiency worsens, treatment for CHF may be needed
vascular disease
these include thrombophlebitis from catheter placement of IV injections, parasitic thromboemboli in the mesenteric arteries and vascular rupture
clinical signs of thrombophlebitis
heat, pain, swelling at site over vein, fever
clinical signs of parasitic thromboemboli
recurrent signs of colic
clinical signs of vascular rupture
sudden death
diagnosis of vascular disease
CBC: neutrophilic leukocytosis
ECHO: abnorma
culture and sensitivity of infected site
history of poor deworming practices (colics)
necropsy (vascular rupture)
treatment of vascular disease
broad spectrum antibiotics
NSAIDs
surgically remove the obstruction; may include vascular grafting
no general treatment for parasitic thromboemboli
thrombophlebitis
inflammation of the lining of a vein with the formation of clots
often seen in the jugular vein from improper catheter maintenance or other vascular trauma
treatment of thrombophlebitis
high doses of broad spectrum antibiotics or antibiotics based on culture and sensitivity results
hot compresses over the site of inflammation
surgical resection of the vein if medical treatment is unsuccessful
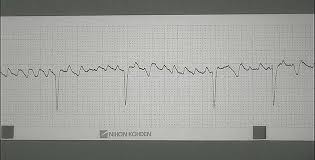
atrial arrhythmias
fairly common in the horse
atrial tachycardia, atrial flutter, and atrial fibrillation are the most likely causes of clinical disease
what arrhythmia is commonly seen in horses at rest?
second degree AV block
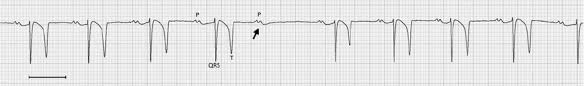
clinical signs of atrial arrhythmia
auscultation os a rapid, abnormal heart rhythm
history of poor or declining performance
exercise intolerance
± pulmonary hemorrhage
± respiratory distress
CHF
ataxia, collapse, or both
diagnosis of atrial arrhythmia
CBC and serum chemistries: may indicate hypokalemia
radiography: usually normal
ECG
Echo: usually normal unless underlying cardiac disease is present
treatment of atrial arrhythmias
provide drug therapy for conversion to normal rhythm:
Quinidine sulfate: oral every 2 hours until conversion or until toxicity develops
digoxin: given concurrently if resting heart rate is more than 90 to 100 bpm or conversion cannot be achieved with Quinidine alone
electrocardioversion
consider resting the horse for 1 to 2 weeks after conversion, although racing horses may return to training within 48 hours of conversion
uneven tooth wear
common dental abnormalities that need attention:
sharp enamel points on the lingual and buccal surfaces
sharp hooks that protrude downward from the first or last tooth of the upper arcade
sharp ramps that protrude upward from the first or last tooth of the lower arcade
wave mouth
step mouth that results from a lack of wear of one tooth, allowing it to grow excessively long
retained wold teeth
clinical signs of uneven tooth wear
bit avoidance
quidding (dropping small, chewed bits of hay)
poor performance
undigested feed in feces
weight loss
prolonged eating time
choke
refers to a condition in which partial or total obstruction of the esophagus occurs, usually caused by feed impaction
often have a history of bolting their feed
may also occur if fed too quickly after sedation
clinical signs of choke
difficulty swallowing
excessive salivation
swelling of the throat
discharge of food from the nostrils
neck extension
differential diagnosis for choke
dysphagia
cleft palate
dental problems
oral foreign body
diagnosis of choke
may be obtained by palpation of the esophagus and passage ( or lack thereof) of the NG tube
radiography
treatment of choke
lavage with gallons of warm water through the NG tube
perform esophageal massage
provide IV fluid therapy
severe cases may need general anesthesia
antibiotics given
NSAIDs given to reduce esophageal inflammation
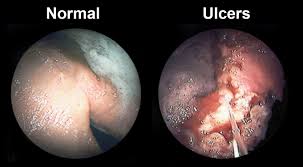
gastric ulcers
horses that have an empty stomach for longer than 6 hours at a time are more prone
feeding concentrate meals predisposes a horse to ulcers by lack of saliva production and constant secretion of HCl acid in the stomach
NSAIDs can cause ulcers in the stomach and the right dorsal colon
clinical signs of gastric ulcers
chronic, low grade colic
anemia, if they are severe and chronic
loss of condition and decreased endurance
some horses may show discomfort when saddled
diagnosis of gastric ulcers
endoscopic examination of the stomach
treatment of gastric ulcers
medication and management changes
omeprazole is very effective
letting horse graze as many hours as possible; feeding small, frequent meals; increasing the amount of forage and decreasing the amount of concentrate fed
colic
many causes
gut sounds may be absent or hyperactive
impaction colic
anatomy of a horse’s gut predisposes it to impactions especially in these areas:
ileocecal junction
pelvic flexure
diaphragmatic flexure
can be caused by a variety of factors:
sand, may accumulate in the cecum
enteroliths
feed
dietary indiscretion, when a horse ingests objects such as a baling twine, rubber, wood, etc
gas or spasmodic colic
often caused by grain overload when bacteria ferment the concentrate and produce gas
typically extremely painful but often resolve spontaneously
pain appears to be intermittent
displacement or entrapment colic
occurs when a portion of the GI tract moves out of normal positioning and may become trapped by another structure
inguinal hernias and nephrosplenic entrapments are examples
infectious or inflammatory colic
occurs as a result of the pain of inflammation of structures in the abdominal cavity
examples: peritonitis and anterior enteritis
necrotic colic
occurs because of lack of blood supply to an area of the intestine
portion of the intestine then dies and feed does not pass through
in the past, major cause was migration of strongyle larvae which cause damage to the intestinal lining resulting in blood clots that may break off and occlude the blood supply to the intestine
clinical signs of colic
pawing
rolling
lying down more than normal
sweating
kicking at abdomen
looking at sides
tachycardia
diagnosis of colic
clinical signs
gray to brick red mucous membranes; poor CRT
increased PCV
treatment of colic
prevent horse from rolling which may cause displacement and torsion
pain relief: Buscpan; Flunixin meglumine; Xylazine
administer NG tube:
water
electrolyes
mineral oil to help relive impaction
psyllium, especially in sand colic
dipyrone: injectable for fever and pain
IV fluids
surgery in severe cases
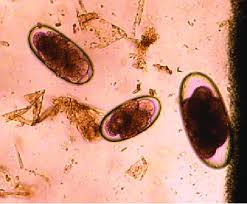
large strongyles
three species that affect horses:
Strongylus vulgaris
Strongylus edentatus
Strongylus equinus
most pathogenical of all intestinal parasites
disease caused by migration of worms, causing inflammation in blood vessels and leading to formation of clots; clots may occlude the vessels, resulting in lack of blood supply to the area and causing local tissue death
effective dewormers: pyrantel, ivermectin, moxidectin, and fenbendazole

life cycle of large strongyles
adults attach themselves to cecum and colon and lay eggs
eggs hatch and larvae crawl in the grass
horse ingests and swallows larvae
larvae migrate through vessels and gut wall
prepatent period is 6 to 12 months
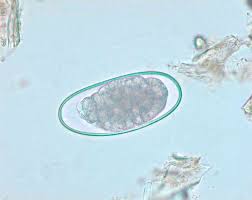
small strongyes
also known as cyathostomes
more than 50 species affect horses
direct damage to the gut wall, impairing digestion and absorption
effective dewormers: pyrantel, ivermectin, moxidectin, fenbendazole
life cycle of small strongyles
adults in colon lay eggs
eggs hatch; infective larvae are consumed by horse
larvae invade the wall of the cecum and large colon
larvae form cysts in the walls of the gut for 1 to 2 months
larvae emerge and mature into adults
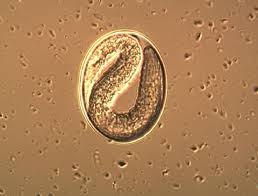
threadworms
Strongyloides westeri
problems mainly in foals
ingestion of larvae in mare’s milk
implicated in foal heat diarrhea
some immunity by 12 to 16 weeks of age; infections minimal
effective dewormer: pyrantel, ivermectin, moxidectin, fenbendazole

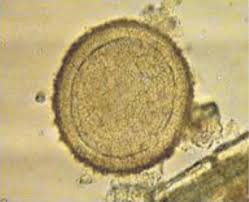
roundworms
Parascaris equorum
most common in foals, clinically irrelevant in horses older than 2 years of age
intestinal blockage
worms actually use the nutrients instead of the horse
may cause intussusception
effective dewormers: pyrantel, ivermectin, moxidectin, fenbendazole
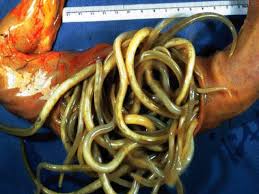
life cycle of threadworms
adults lay eggs in the small intestine
larvae are ingested by the horse
larvae migrate
life cycle of roundworms
adults live in small intestine and lay eggs
foals ingest embryonated eggs
liver and lung migration
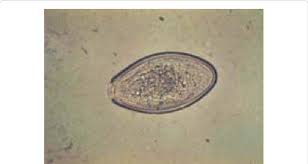
pinworms
oxyuris equi
mostly from irritation of the perinuem; horse itches and rubs tail head
effective dewormers: pyrantel, ivermectin, moxidectin, fenbendazole
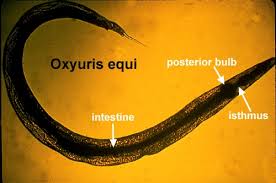
life cycle of pinworms
adults live in large and small colon
female parasites migrate to the anus, rupture, and spew eggs into the environment
infective eggs are ingested; larvae hatch and migrate
tapeworms
Anoplocephala perfoliata; Anoplocephala magna
previously little clinical disease attributed to tapeworms; with newer effective dewormers, competing parasite populations are removed and tapeworms are able to flourish
effective dewormer: praziquantel
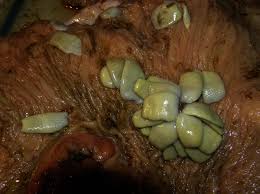

bots
Gastrophilus spp
usually does not cause oo many problmes
may cause ulceration, perforation, peritonitis
effective dewormer: ivermectin, after. the first hard frost
life cycle of tapeworms
horse ingests the mite
larvae are released from the mite and attach themselves to the cecum and small intestine
adults release proglottids into the environment
proglottids release the eggs which are consumed by mites
life cycle of bots
adult fly lays eggs on the horse
horse licks the eggs and ingests larvae
larvae migrate through the oral cavity and tongue
bots are located in the stomach
salmonellosis
may affect horses of all ages, but it is mostly seen in young horses
causative agent is Salmonella spp
organism is present in most horses but it usually causes disease only when the animal is immunocompromised such as in times of stress
illness is caused by a toxin that the bacteria release
clinical signs of salmonellosis
profuse, foul smelling often bloody diarrhea
may become septic
inappetance, depression
fever
abdominal pain
increased heart and respiratory rates
injected sclera
dehydration
treatment of salmonellosis
correction of IV fluid loss; IV fluids with electrolytes, then oral fluids through NG tube
antiserum
NSAIDs
diarrhea control
± antibiotics
probiotics
clostridial infections
similar to salmonellosis but much more severe
animals often ie before the onset of diarrhea
most often seen in foals
caused by Clostridium perfringens type A
bacteria release a toxin that erodes the gut wall
clinical signs of clostridial infections
profound depression and inappetance
severe pain
injected sclera
shock with:
pale mucous membranes
rapid heart rate
weak, thready pulse
fever
profuse bloody diarrhea
treatment of clostridial infections
IV fluid therapy
pain control (Banamine, Ketoprofen, Xylazine)
peniciilin
ehrlichiosis (potomac horse fever)
more commonly found in horses living near large waterways and is also commonly seen in the summer months
caused by Neorickettsia risticii
involves a fluke and it also appears to involve insects that feed on the secretions of snails and flukes
disease causes inflammation of the colon, impaired water absorption, and diarrhea
clinical signs of potomac horse fever
fever, depression
mild abdominal pain
slowed gut movements
diarrhea
some horses experience toxic signs
laminitis is a common sequel
treatment of potomac horse fever
oxytetracycline
maintenance of hydration, possibly IV fluid therapy
banamine to prevent laminitis
which parasite has historically been considered the most pathogenical of all equine parasites?
strongylus spp.
one of the most common causes of explosive diarrhea in stressed, hospitalized horses is what?
Salmonella
one possible consequence of feeding horses soon after sedation or anesthesia. iswhat?
choke
what might predispose a horse to gastric ulcers?
chronic administration of NSAIDs
intense training
high concentrate diets
it is recommended that all horses have their teeth examined and floated how often?
at least yearly
long term use of NSAIDs may result in what?
gastric ulceration
where are you most likely to fnid roundworms?
a nursing foal
which parasite may result in damage to the tail of the horse?
oxyuris equi