CVR: practice questions (week 10)
1/163
Earn XP
Description and Tags
dyspnea, trauma, surgical approach to thorax, effusion, thoracic imaging, upper airway SA
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
164 Terms
What is the low‑pitched, snoring/snuffling sound, originating from the nasopharynx or oropharynx caused by turbulent airflow through partially obstructed soft tissues (soft palate, pharyngeal tissues)?
Stertor
What is the high-pitched, harsh, or wheezing sound produced by turbulent airflow through a partially obstructed upper airway (larynx or trachea), usually heard upon inhalation?
Stridor
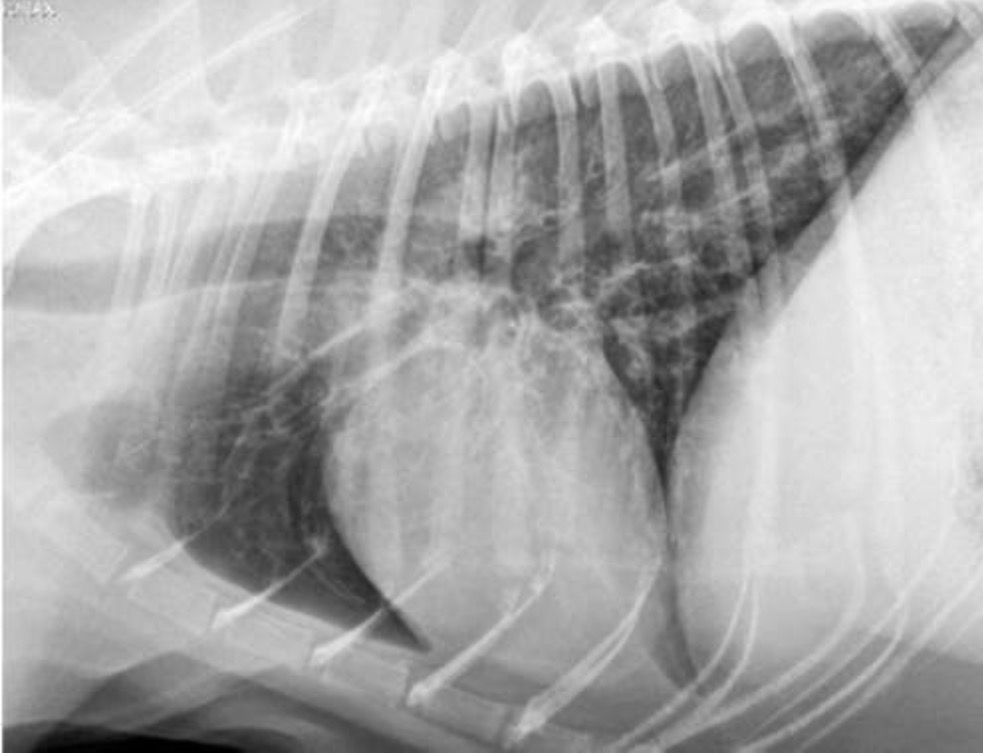
What type of pattern can be seen in this radiograph?
Bronchial → see rings + railroad tracks
What anesthetic protocol would you choose to perform a complete oral cavity evaluation under sedation in a brachycephalic patient with BOAS symptoms?
Pre-med: Acepromazine + Butorphanol
Induce: Dexmedetomidine
What problems will you typically identify in a brachycephalic patient with BOAS?
Stenotic nares, hypoplastic trachea, elongated soft palate, hyperplastic tonsils, macroglossia, everted laryngeal saccules, dental/ocular problems
Which grades in the Functional Grading System for BOAS would require management &/or treatment?
Grade II or III
-assessed after 3-minute trotting exercise tolerance test
If a patient in respiratory distress presents with audible breathing, where is the likely location of the abnormality & what should you do to stabilize the patient?
Upper airway → provide O2, sedate (ace + butorphanol), intubate
If a patient in respiratory distress presents with inaudible breathing, what are the most likely causes?
Lower airway → pulmonary disease (loud auscultation; asthma or heart disease) OR pleural space disease (quiet auscultation; pleural effusion or pneumothorax)
What are the quick physical exam parameters (should take 30-60 seconds) you should assess on a patient that presents to you in emergent respiratory distress?
HR/RR, peripheral pulses, MM color, CRT, extremity temperature
Oxygen delivery increases the partial pressure of oxygen in the blood. How can this help in a pneumothorax?
Decreases the partial pressure of other gases in the blood → makes them diffuse down gradient out of chest back into lungs + out
When is the ONLY time oxygen administration is contraindicated?
Fire!!!
How does administration of oxygen help in patients with head injury?
Early O2 decreases secondary brain injury, edema, & neural death
How does administration of oxygen help in patients with shock?
Decreases reperfusion injury
How does administration of oxygen help in patients with surgical wounds?
Decreases infection rate
Where in the thorax should you perform a thoracocentesis prior to radiographs on a patient with a restrictive breathing pattern (short + shallow)?
7th to 9th ICS → bevel goes down instead of up in this case so we don’t stab the lungs
If we are concerned about lung function, what diagnostic test should we always run?
Arterial blood gas
What are some of the diagnostic tests we should try to run BEFORE stabilizing a patient in respiratory distress?
QATS → PCV/TS/BG/lactate/azo, blood smear, BP, TPR, ABG, ECG, ± thoracocentesis
What are the diagnostic tests we should try to run after stabilizing a patient in respiratory distress?
CBC/Chem/UA, monitor BP/urine output/pulses, POCUS, radiograph, ± contrast studies
While we are assessing acid-base status in a patient in respiratory distress, what other parameter should we calculate?
A-a gradient → tells us if there is a perfusion:ventilation (V/Q) mismatch
How should we treat a patient that presents with flail chest after a traumatic injury?
Place bad side down → administer O2, pain meds, cover wound + protect, thoracocentesis, IV fluids
In a patient that presents with flail chest, what radiographic findings might we see?
Fractured ribs/sternum, pneumothorax, atelectic lung lobes, alveolar pattern/pulmonary hemorrhage, pulmonary contusions
What injury should we expect to find in ALL dogs with thoracic trauma?
Pulmonary contusions
-increased lung sounds with uneven distribution + coughing/hemoptysis
Which arrhythmias would you expect to hear up to 12-36 hours after direct trauma or ischemia in cardiac injuries?
VPCs, Ventricular tachycardia, AIVR
What can CT scans or MRIs show us post-traumatic injury to the thoracic cavity?
Bullae or blebs
Which type of closed traumatic pneumothorax can occur when the chest is compressed while the glottis is closed?
Tension pneumothorax
Which dog breeds are predisposed to spontaneous pneumothorax?
Huskies (deep chested large breeds)
What cavitary lesion (<1cm) that can cause spontaneous pneumothorax occurs after air accumulates in the visceral pleura?
Bleb
What cavitary lesion (>1cm) that can cause spontaneous pneumothorax occurs as a result of destruction, dilation, & convergence of contiguous alveoli, secondary to obstruction of small airways?
Bullae
What best describes blunt thoracic trauma in companion animals?
Non-penetrating injury caused by impacts like vehicular accidents or falls
Which injury in thoracic trauma causes progressively worsening dyspnea is considered life-threatening & often requires immediate intervention?
Tension pneumothorax
A dog presents after a car accident with labored breathing, paradoxical chest wall movement, & multiple rib fractures. What is the most likely diagnosis?
Flail chest
What are the two most common findings secondary to thoracic trauma?
Pulmonary contusion + Pneumothorax
Why can the heart appear “floating” on a chest x-ray in a pneumothorax?
Loss of support from the adjacent collapsed lung
What is the purpose of placing thoracostomy tubes in patients with thoracic trauma?
Allows free air/fluid to evacuate the thorax
What is the main source of air in a closed pneumothorax?
Respiratory tract or esophagus → swallow air
What is the main difference between a closed pneumothorax & a tension pneumothorax?
Tension pneumothorax involves progressive pressure buildup that compresses mediastinal structures, unlike a closed pneumothorax
What is the treatment for a mild closed pneumothorax?
Cage rest + observation
What is the treatment for a moderate closed pneumothorax?
Thoracocentesis
What is the treatment for a severe closed pneumothorax?
Tube thoracostomy + exploratory thoracotomy
What is meant by paradoxical chest wall movement?
Sucking inward during inhalation & bulging outward during exhalation
When should you remove the thoracostomy tube placed in a patient with flail chest?
When collection of fluid is 50cm3 or less in 24 hours
-also when x-ray in 24 hours does not show air or free fluid
What are the main clinical signs seen in a patient with a traumatic diaphragmatic hernia?
Orthopnea + Respiratory distress
What would you expect to hear when you auscultate a patient with a traumatic diaphragmatic hernia?
Muffled heart/respiratory signs (fluid or viscera in pleural space), borborygmus (intestines in pleural space), or tympany on left side of thorax (stomach in pleural space)
What is the goal of initial management in a patient with a traumatic diaphragmatic hernia?
Improve cardiorespiratory status
When is a traumatic diaphragmatic hernia an emergency?
Stomach is in thorax
Where should you begin suturing for a traumatic diaphragmatic hernia repair?
Radial tear at most dorsal margin
Which species is more susceptible to re-expansion pulmonary edema after a traumatic diaphragmatic hernia, which should be corrected by inflating the lungs gradually?
Cats
When do most deaths occur during traumatic diaphragmatic hernia correction?
Pre-operatively during induction (first 24 hours)
Which hernia is where a rupture occurs in the abdominal wall, sucking organs (mainly omentum) into the subcutaneous space?
Paracostal hernia
Which type of hernia is always congenital in dogs/cats & is thought to be a result of faulty development of the septum transversum during embryogenesis &/or closure of the lateral pleuro-peritoneal folds?
Peritoneo-Pericardial hernia
What radiographic signs will you see in a patient with a Peritoneo-Pericardial hernia?
Enlarged cardiac silhouette, discontinued ventral diaphragm, structures with gas in pericardial sac, tracheal elevation
Where are the alar folds in the horse?
Bulbous thickening of the ventral nasal concha that projects into the nasal vestibule that lies within the false nostril
Where are the ethmoid turbinates located in the horse?
Caudal (rear) portion of the nasal cavity, forming part of the ethmoidal labyrinth of the ethmoid bone, close to the cribriform plate
-place a nasogastric tube through the ventral meatus otherwise you will hit the ethmoids + cause a nosebleed
What is the relationship of the epiglottis to the soft palate in the horse?
Epiglottis normally sits above the soft palate, with the soft palate cupping tightly around its base
-creates a mechanical lock, dividing the pharynx into separate respiratory + digestive pathways
What parts of a physical exam are important regarding the respiratory system?
RR, auscultation of lungs/heart/trachea (larynx, middle, bifurcation), bilateral nares airflow, check for nasal discharge
Which lymph node should always be palpated in a physical exam in horses with respiratory issues as they are the easiest to palpate & drain everything from the head?
Submandibular LNs
If a physical exam of a horse with abnormal respiratory sounds reveals normal parameters, what should you do next?
Dynamic examination (exercise)
What diagnostic test should be performed after a dynamic examination reveals abnormal respiratory sounds?
Upper airway endoscopy
During what respiratory phase is a noise occurring if you hear it as the horse’s front feet land?
Expiration
What are the epidermal inclusion cysts that form within the false nostril, which are treated by injecting an irritant or damaging the cyst lining through the mucosa so it cannot recur?
Atheroma
Redundant alar folds present with a normal expiratory flutter + inspiratory noises due to increased airway resistance. How is this diagnosed & treated?
Diagnosis: Tie back alar folds with mattress suture + exercise
Treatment: Bilateral fold resection
Which nasal abnormality right next to the cribriform plate in horses shows clinical signs such as serosanguinous low volume nasal discharge, stridor/dyspnea, & occasionally facial distortion?
Ethmoid hematoma
What is the preferred treatment for ethmoid hematomas in horses?
Formalin injection or laser photoablation
At what classifications of lymphoid hyperplasia in horses will we see signs such as dynamic pharyngeal collapse at high speed & exercise intolerance with inspiratory noises due to negative pressure when the pharynx collapses down on itself?
III + IV
After a dynamic exam of a horse, it presents with a “gurgling” noise & then comes to a standstill. He then swallows & the noise stops. What is your top differential diagnosis?
Dorsal displacement of the soft palate (DDSP)
-expiratory noise
What is the only way to definitively diagnose dorsal displacement of the soft palate (DDSP) in horses?
Endoscopy during exercise
What are the conservative vs. surgical treatment options for DDSP in horses?
Conservative: Tongue tie, cornell collar, figure-8 noseband
Surgical: Tie forward, palatal thermal cautery, staphylectomy, epiglottic augmentation, sternothyrohyoideus myectomy
You are presented with a 12yo TB cross gelding with mild intermittent unilateral epistaxis over the last three weeks. What diagnostic test is most useful to definitely identify the cause of epistaxis?
Endoscopy
After you have performed an endoscopy on a horse, you identify an ethmoid hematoma. What additional first line diagnostic can help plan the treatment for this case?
Radiography → check for invasion past cribriform plate
What surgical approach to the guttural pouch is best for drainage as it is completely ventral & distal to the linguofacial vein?
Modified Whitehouse
Which guttural pouch condition in horses will show intermittent purulent nasal discharge, parotid LN swelling + pain, extended head + neck, & difficulties swallowing/breathing due to collapse of the pharynx, typically in young horses after a strep infection?
Guttural pouch empyema (accumulation of pus)
Which guttural pouch condition in foals up to 1yo shows non-painful distention of the parotid region due to one-way valve function of the ostium (too narrow)?
Guttural pouch tympany (air stuck in GP)
For which upper respiratory disease in horses is radiography better for initial diagnosis than endoscopy?
Guttural pouch tympany → shows enlarged GP with air/fluid
Which guttural pouch condition in horses is diagnosed by episodes of recurrent epistaxis + endoscopy?
Guttural pouch mycosis (Aspergillus spp.)
Which treatment of guttural pouch mycosis will give a horse the best prognosis?
Arterial occlusion → circle of willis, balloon catheter or coils
Which treatment of aerophagia will give a horse the best prognosis?
Modified Forssell’s → omohyoideus + sternohyoideus myotenectomy
What is the indication for a tracheotomy in horses?
Acute upper respiratory obstruction
What is the indication for a tracheostomy in horses?
Permanent impairment of the larynx
What structure forms the caudal boundary of the thoracic cavity?
Diaphragm
What surgical adjustment must be made for all patients with open chest cavities?
Intermittent positive pressure ventilation (IPPV)
What are the surgical approaches for a patient undergoing a lateral thoracotomy?
Intercostal, rib resection, periosteal stripping + rib resection
Which intercostal space should you enter to perform thoracic duct ligation in the treatment of chylothorax on either the left or right side?
8th ICS
Which intercostal space should you enter to perform a cranial lung lobectomy on both the left & right side?
5th ICS
For which surgical procedures would you access the thorax at the 4th intercostal space?
PDA, PS, PRAA → left side
Esophageal FB @ heart base or pericardium → right side
Cardiopulmonary bypass → right side
How would you access the left lateral thoracotomy at the 4th intercostal space?
Sever latissimus dorsi → bluntly separate leaflets of serratus ventralis muscle → cut across intercostal muscles (ventral to dorsal + watch out for neurovascular bundle at caudal margin) → incise pleura
How should you close your patient after performing a lateral thoracotomy?
Place thoracostomy tube → preplace sutures around ribs + tie → routine closure of musculature (do not suture intercostal muscles, do not overlap ribs, close cutaneous trunci with SQ layer in SA) → routine closure of skin
Where should you place a thoracostomy tube in a patient post-lateral thoracotomy?
Make incision in skin + SQ tissue 2-3 ICS both dorsal & caudal to thoracotomy incision
-then tunnel cranially 1-2 ICS, enter pleural space, & position tube
What are the indications for a median sternotomy?
Access entire lung field for exploratory surgery, subtotal pericardectomy, or aortic valve replacement
What is the most used surgical approach to the thorax in dogs for access to the thoracic cavity?
Lateral thoracotomy
What tests are performed initially when evaluating an effusion?
Gross appearance, TNCC, TP, Cytology
What are some of the causes of edema, pleural effusion, & ascites?
Increased vascular permeability, increased capillary hydrostatic pressure, decreased oncotic pressure, & lymphedema
What is the primary site to perform an abdominal tap in cattle?
Cranial abdomen → just caudal to the xiphoid sternum & to the right of the midline
Which diseases may cause pure & modified transudates (high + low protein)?
Right sided heart failure, pericardial disease, hypoalbuminemia, neoplasia, diaphragmatic hernia
Which diseases may cause non-septic exudates?
FIP, neoplasia, diaphragmatic hernia, lung lobe torsion, peritonitis
Which diseases may cause septic exudates?
Pyothorax or septic peritonitis
Which diseases may cause hemorrhagic effusion?
Trauma, bleeding disorders, neoplasia, lung lobe torsion
How can we confirm a chylothorax (leakage from thoracic duct) in a patient?
Compare triglycerides + cholesterol in the fluid vs. the serum
If a patient presents with a low protein transudate with low albumin, what is your top differential?
Protein-losing condition (likely liver issue)
If a patient presents with a non-hemorrhagic exudate with high lymphocytes, what is your top differential?
Chylothorax
If a cat presents with a low cellularity modified transudate, what is your top differential?
FIP (exudative effusion)