Gastric Acid Disorders: GERD & PUD
1/81
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
82 Terms
Anatomy Review of Upper GI
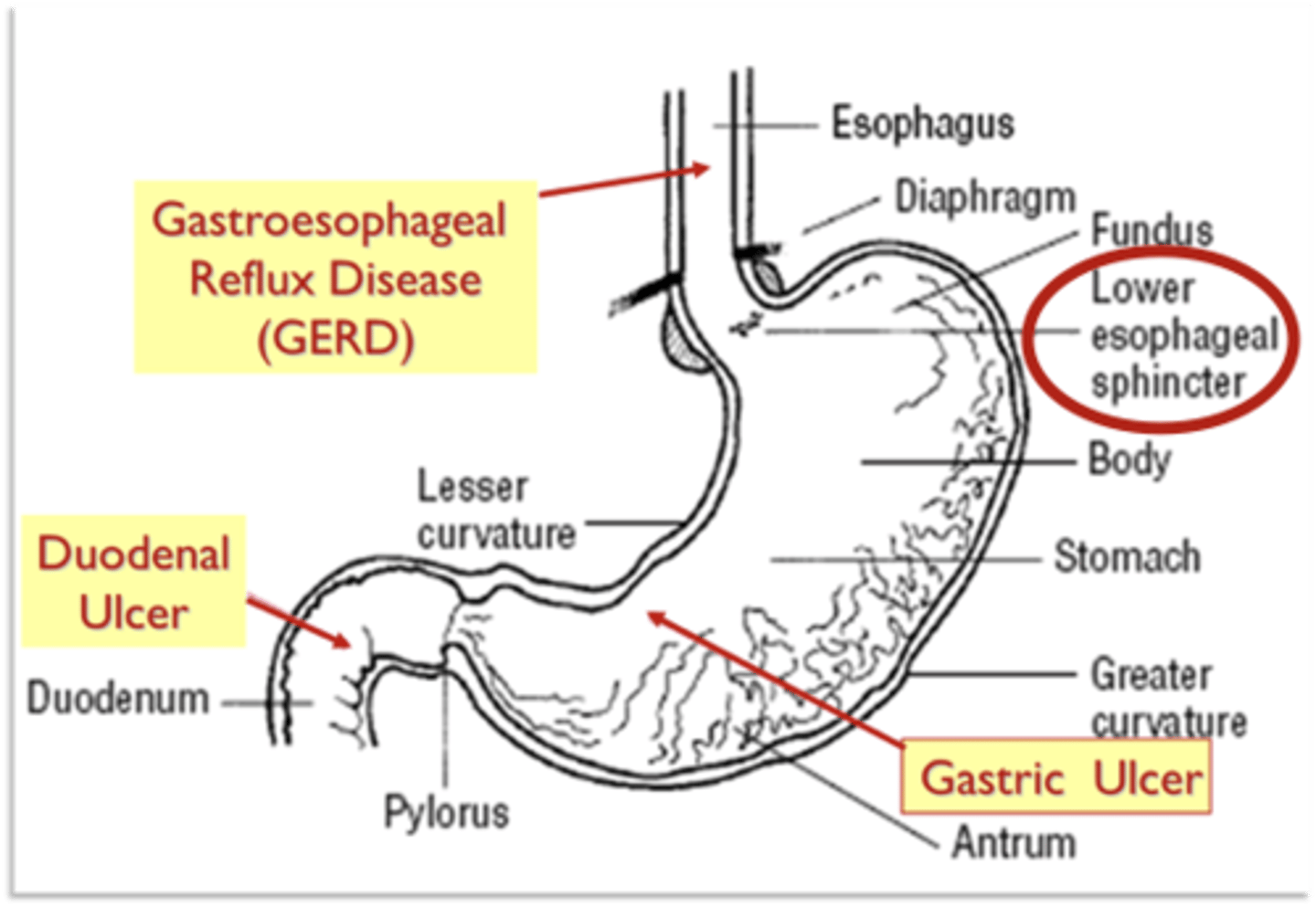
What is in the stomach lining?
Millions of gastric pits that lead to gastric glands that produce gastric juice
What is an important cell type of gastric glands?
G cells: a type of enteroendocrine cell that secretes gastrin
Where does gastric acid come from?
Its secreted by parietal cells in the stomach at a basal rate
-> its secretion increases in response to several stimuli
What active transport protein is on the surface of parietal cells? (Think protein pumps)
Proton Pump (H+/K+ pump)
What does the proton pump do?
Moves one H+ ion out of the parietal cell (into the lumen of the stomach) and one K+ ion back into the parietal cell
Does the proton pump do this movement with or against the concentration gradient?
Proton pump does this against the concentration gradient
-> ATP is required to provide energy for this movement
What else moves into the stomach lumen w/ the proton pump?
Cl- also moves into the stomach lumen and forms HCI
What 3 hormones stimulate gastric acid secretion?
Gastrin, Acetylcholine & Histamine
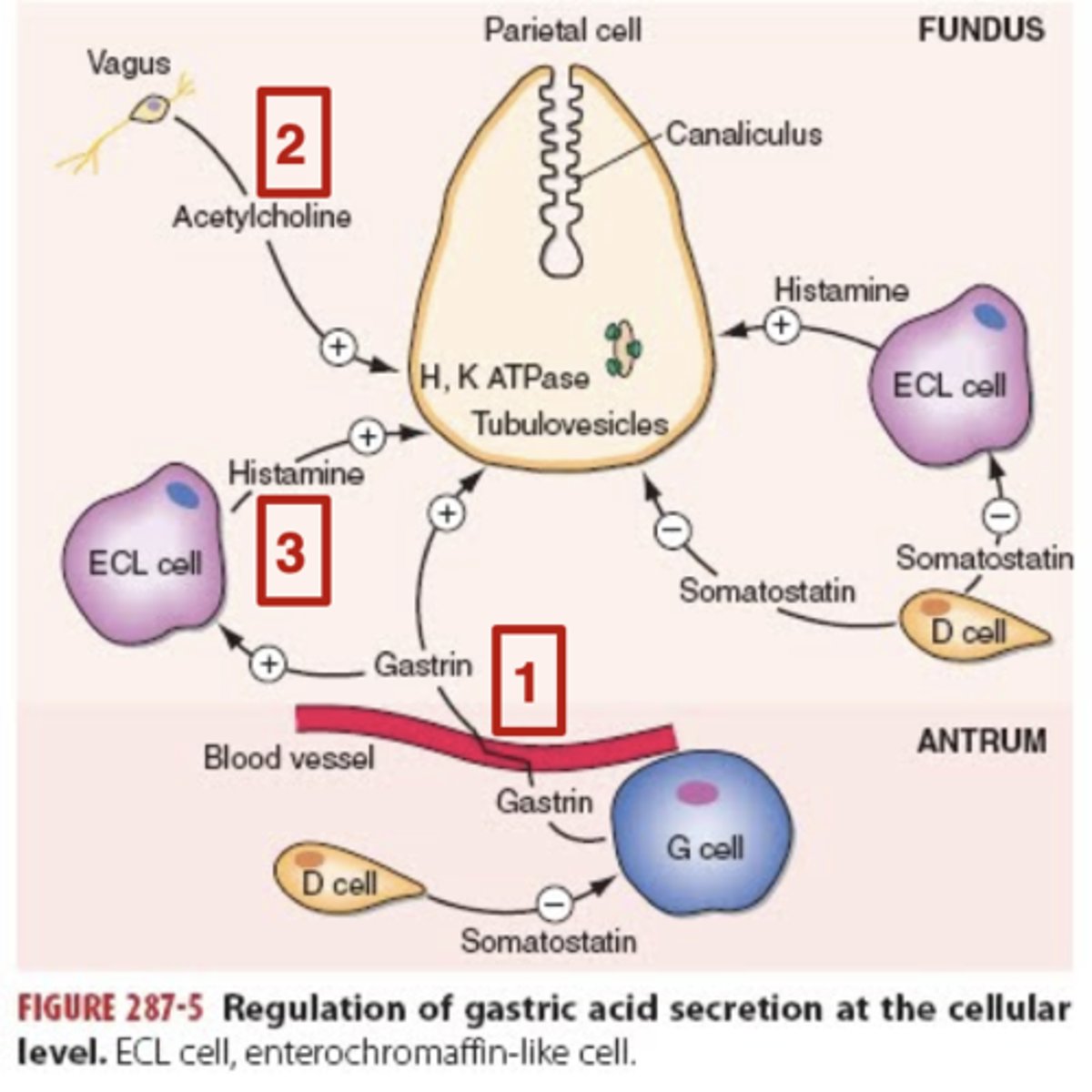
Where is the histamine receptor?
Histamine's receptor is on surface the parietal cells
The specific receptor is the H2 receptor
This is one of the drugs target
What happens when a histamine molecule fits into an H2 receptor on a parietal cell?
The H2 receptor becomes a G Protein-Coupled Receptor (GPCR)
What is the result when histamine binds to its receptor & activates a GCPR?
Parietal cells will cause translocation of proton pumps to the plasma membrane & dramatically increases the # of proton pumps on the cell & stimulate H+ secretion-> decrease in pH of the stomach lumen
What does acid disorder result from?
Imbalance of aggressive/damaging (or potentially damaging) factors & mucosal defense/protective factors
(in a healthy pt. these factors are normally held in balance)
What are aggressive factors?
-Gastric acid
-Pepsin
-Bile acids
-Pancreatic enzymes
-External factors: H. pylori infection, NSAIDs, smoking & heavy use of alcohol
KNOW THESE
What are mucosal defenses?
-LES normal tone
-Esophageal clearance
-Mucosal resistance
-Tight junctions
-Gastric emptying
-Epidermal growth factor
-Salivary Buffering (HCO3-)
-Prostaglandins
KNOW THESE
What is the key to avoiding damage from acid?
Maintain the integrity of the gastric mucosal barrier
-HCO3-
-pH is 7 at surface of mucosa vs. pH of 1-2 in the stomach lumen.
-Epithelial cells joined by tight junctions that prevent HCl from leaking into underlying tissue.
-Mucous cells provide a physical barrier; release mucus. Traps layer of bicarb-rich fluid beneath it.
-Mucus contains mucin proteins, which play a critical role in maintaining the barrier function.
Mucin forms a gel closest to the lumen
What is GERD?
Symptomatic condition or histologic change a/w retrograde movement of gastric contents to esophagus
What is PUD?
Gastritis, erosions & ulcers of the GI tract that requires gastric acid for their formation
(most ulcers form in the stomach or duodenum, w/ duodenal ulcers > common than stomach)
What is the most common cause of GERD?
"Incompetent" LES (Lower Esophageal Sphincter) allows acid reflux
-the normal high pressure of LES is reduced
When does the "incompetent" LES permit reflux of gastric acid?
Every time the pressure in the stomach exceeds the pressure in the LES
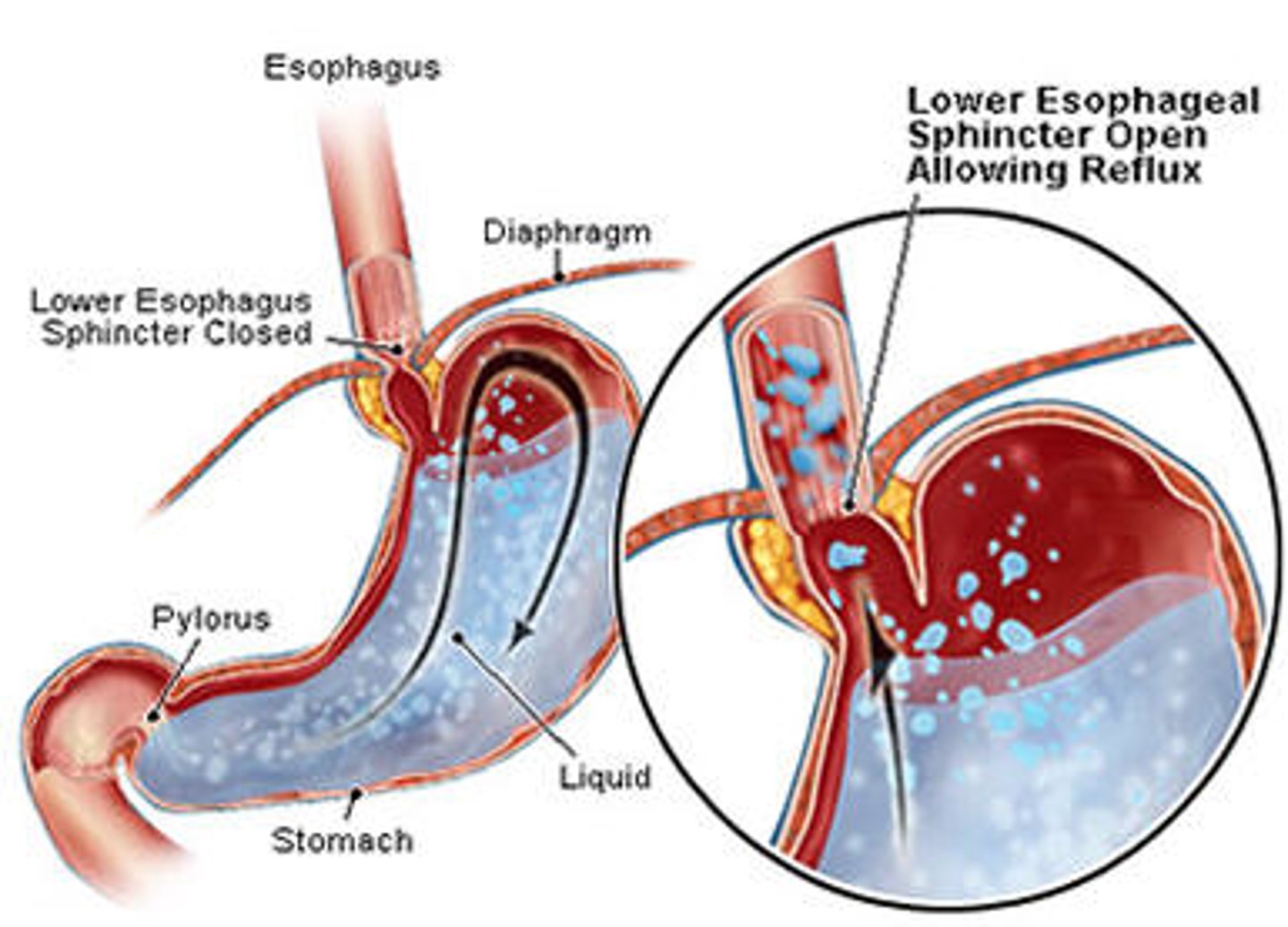
What is the Lower Esophageal Sphincter (LES)?
-High-pressure zone of thickened muscles locate where the esophagus merges w/ the stomach
How does the LES normally work?
LES works in concert w/ the diaphragm to prevent reflux of gastric contents
What does the LES do in resting conditions?
Maintains a high-pressure zone that is 15-30 mmHg above intragastric pressures
(If the LES is "incompetent" -> acid reflux can occur)
What are other causes of GERD?
Anything that alters the normal function &/or tone of the LES or increases abdominal pressure may predispose a pt to GERD
-Certain food or medications
-Smoking
-Obesity
-Hiatal Hernia
-Sleeping positions
What is the hiatus & what normally occurs?
Its an opening in the diaphragm
-> normally the esophagus goes through the hiatus & joins the stomach
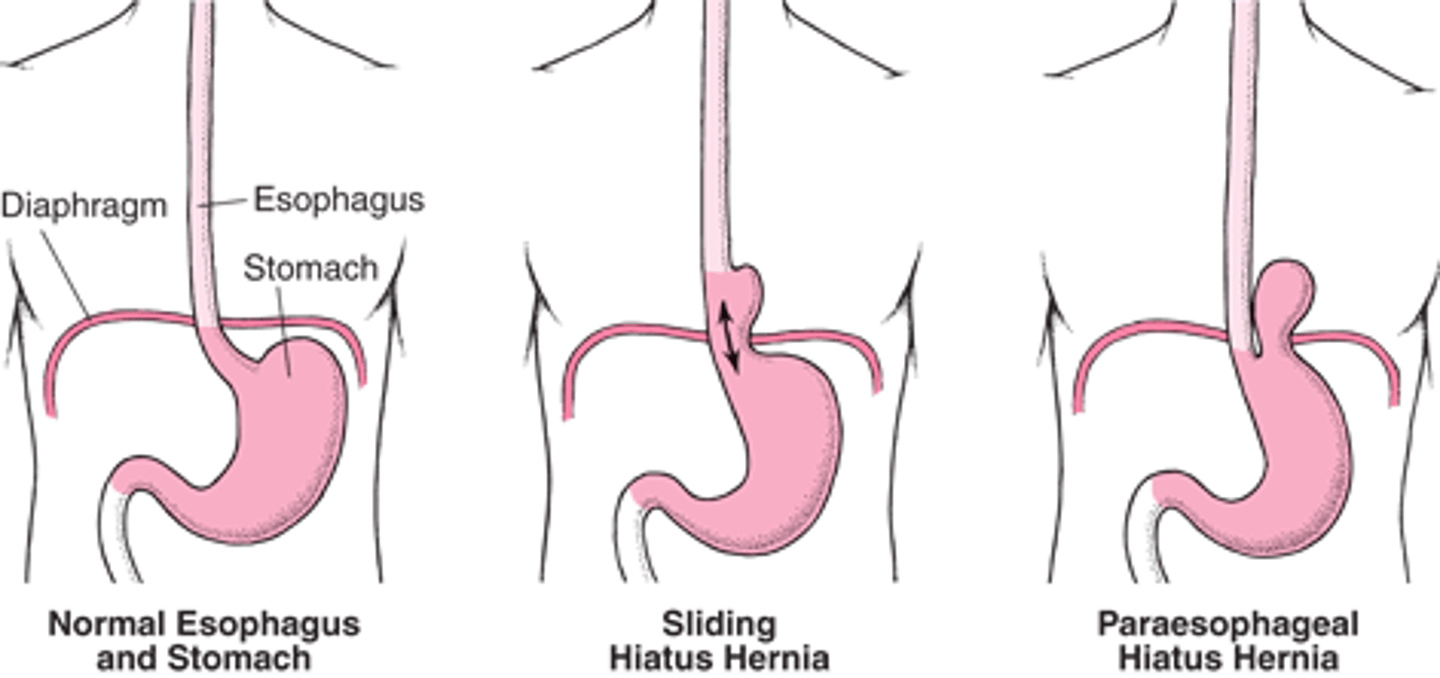
What is a Hiatal Hernia?
When the stomach bulges up into the chest through that opening (hiatus)
What are the 2 types of Hiatal hernia & which is more dangerous?
1. Sliding Hiatal Hernia
2. Paraesophageal (Rolling) Hiatal Hernia (more dangerous d/t the risk of the stomach being incarcerated)
What foods may worsen GERD symptoms?
Decreases LES pressure (relax)
-Some carminatives (pt should be taught to avoid pepermint)
-Chocolate
-Fatty meal
-Coffee, tea, cola
Direct Esophageal Irritants
-Coffee
-Orange juice
-Spicy foods
-Tomato juice
What medications may worsen GERD symtptoms?
Decrease LES pressure
-Ethanol (alcohol)
-Nicotine
Direct Esophageal Irritants
-Aspirin & other NSAIDs
ALSO: Cigarette Smoke
What are typical S/Sx of GERD?
-Heartburn (felt in sternum)
-Belching
-Water brash (hypersalivation)
-Regurgitation w/ or w/o nausea
What are severe S/Sx of GERD?
-Continual pain
-Dysphagia
-Odynophagia
-Vomiting acid in sleep
-Bleeding
-Unexplained weight loss
-Choking
What are atypical (extra-esophageal) S/Sx of GERD?
-Non-allergic asthma
-Chronic cough
-Hoarseness
-Laryngitis
-Chest pain
-Dental erosion
What are sequelae of chronic GERD (what can it lead to)?
-Reflux Esophagitis
-Erosive Esophagitis
-Esophageal Strictures
-Barrett's Esophagus
-Adrenocarcinoma
What happens to the cells in Barrett's Esophagus?
Metaplasia d/t chronic exposure to gastric acid
-Distal esophageal cells (normally stratified squamous cell epithelium) are replaced by columnar epithelium w/ goblet cells & mucus cells
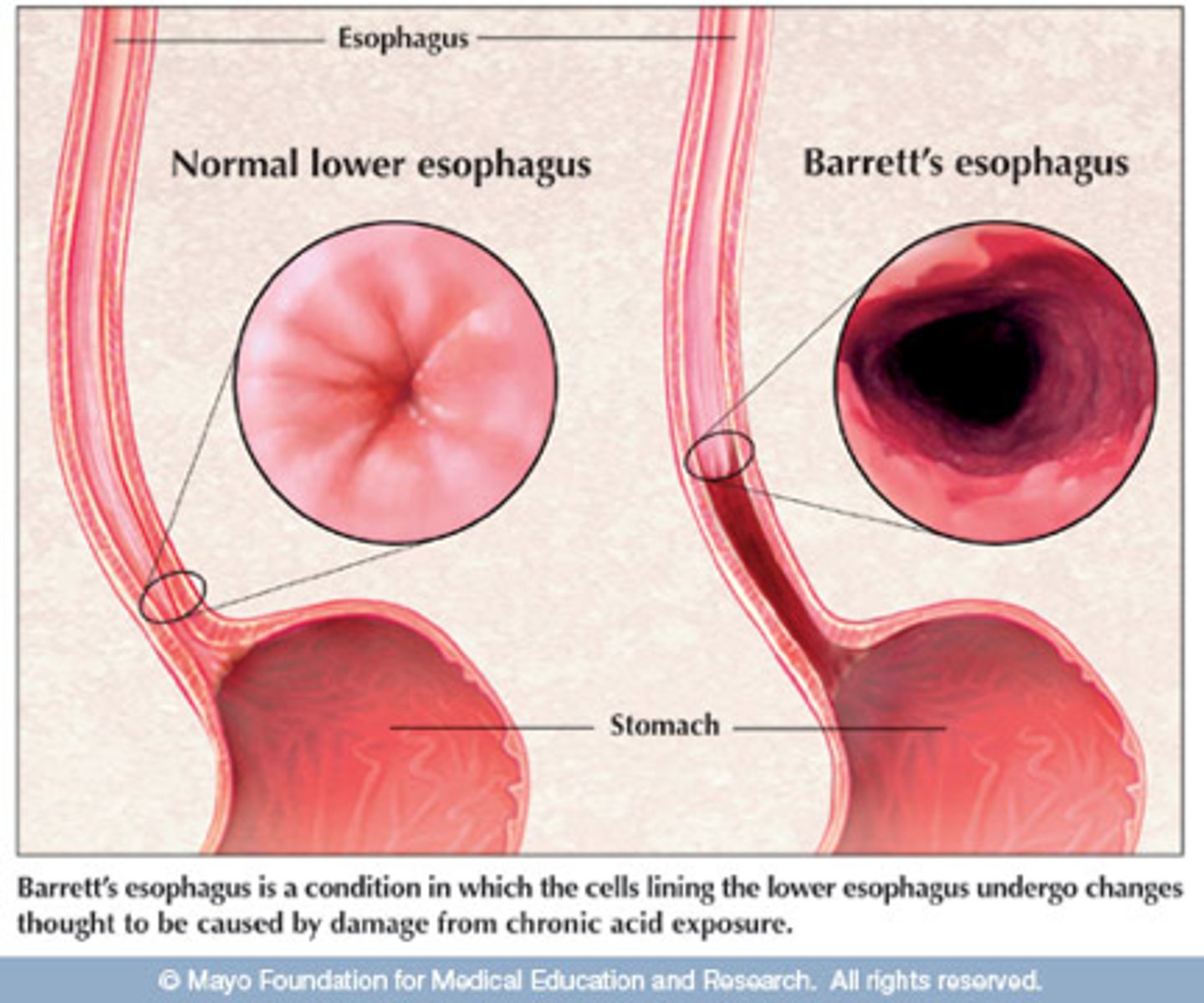
Sequelae of GERD
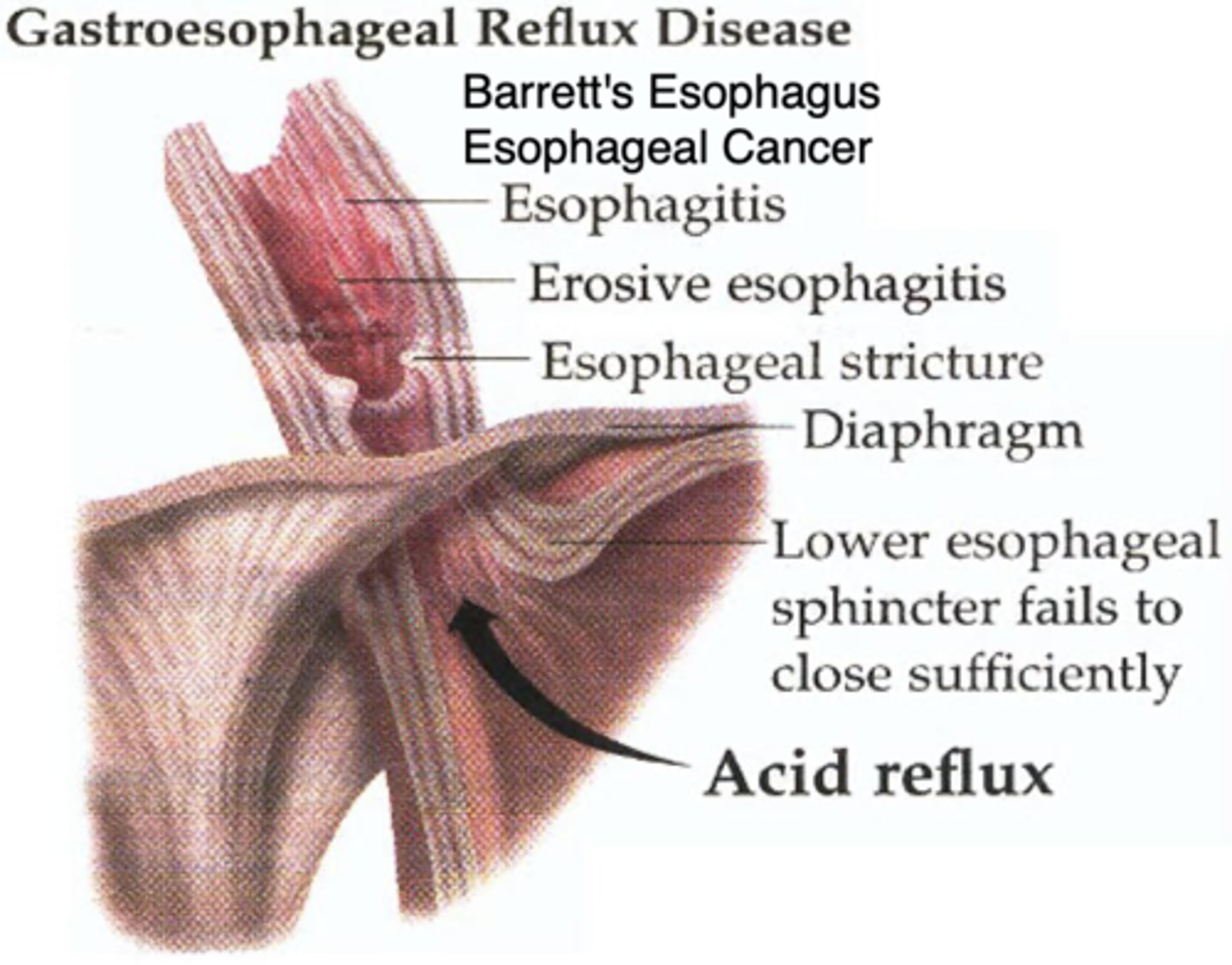
What happens with the metaplastic cells?
They are more tolerant of an acid environment & are more likely to develop into adrenocarcinoma
Pt w/ Barrett's esophagus must be monitored to insure that they haven't developed esophageal cancer
What is Peptic Ulcer Disease (PUD)?
AN Injury to the mucosa of the stomach or duodenum (sometimes esophagus)
Ranges from slight mucosal injury -> severe ulceration w/ bleeding
What is PUD caused by?
An increase in aggressive factors that will tend to injure the mucosa relative to defense factors that tend to protect it
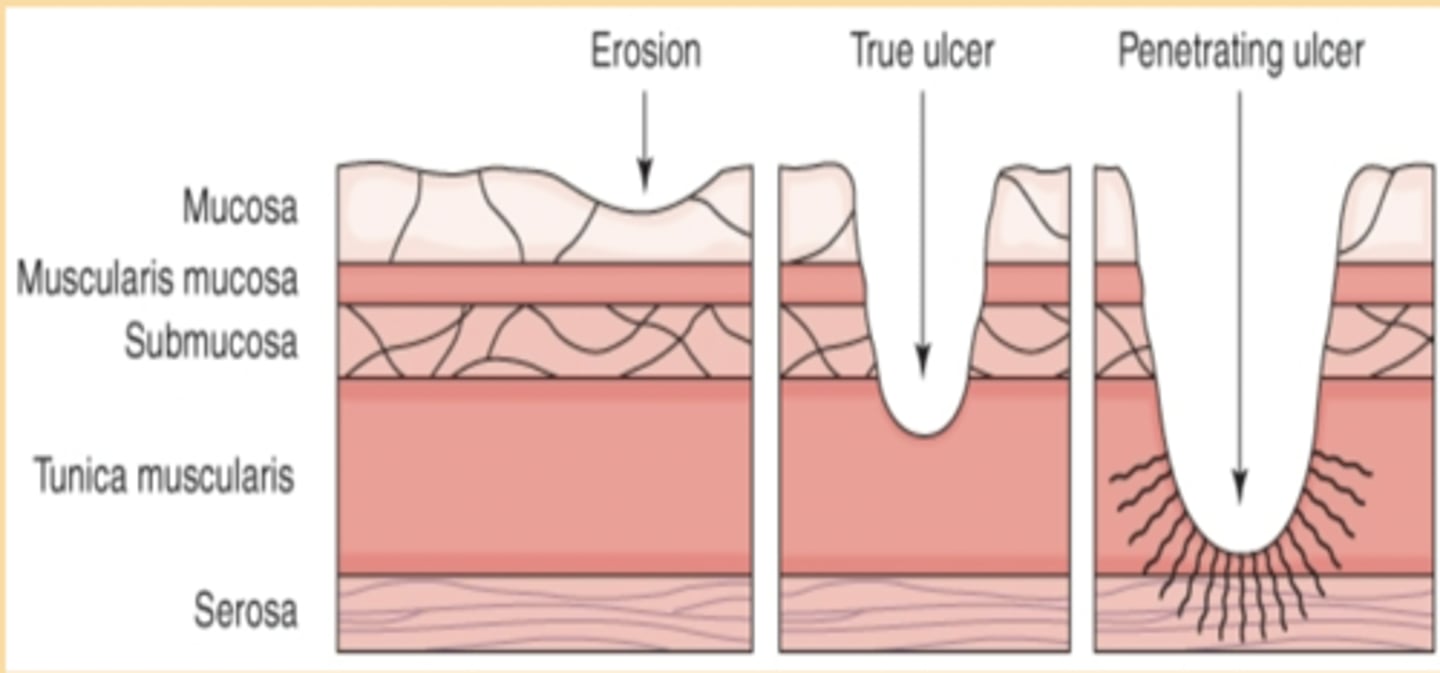
What are common causes of PUD?
-Helicobacter pylori infection (most common)
-Non-steroidal Anti-inflammatory drugs (NSAIDs) (also corticosteroids but they are less commonly used than NSAIDs)
-Increased Smoking
What is H. Pylori? (Charactersistics of thebacteria itsekf)
- Gram(-) bacteria
- Slow growing
What aids in H. pylori mobility & helps it move?
-Helical (corkscrew) shape aids in it mobility
-Flagella help is move below the mucosal surface to colonize the gastric epithelium
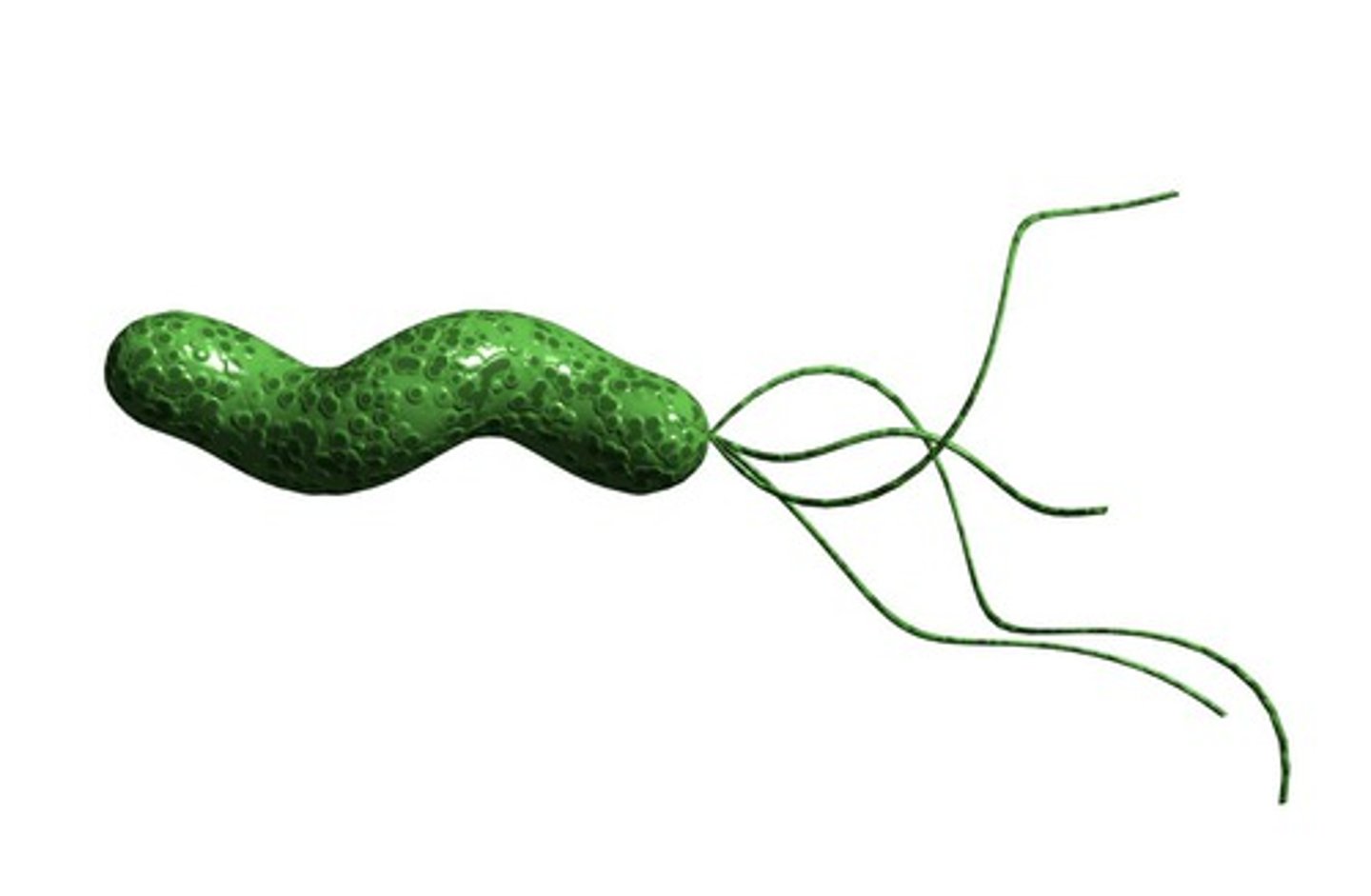
How can a H. pylori infection can lead to PUD?
H. pylori is well-adapted to the gastric environment (lives beneath or within the gastric mucosal layer)
-> will disrupt the mucus layer, neutralizes pH (mucin will "de-gel"), releases enzymes/toxins and adheres to the gastric epithelium
What does H. pylori release and what does it do?
Releases urease enzymes
-> will convert urea to CO2 & ammonia (which will neutralize the stomach acid & irritate/injure the mucosa)
What else does H. pylori promote?
Promotes an inflammatory reaction (which can further cause tissue injury)
What does the mucosal disruption & tissue injury from H. pylori cause?
It will give the bacteria an opportunity to move below the surface of the mucosal layer -> can be the site of an erosion & eventually an ulcer
What is the ulcer formation promoted by?
Its promoted by making the underlying gastric or duodenal mucosa more vulnerable to further damage by acid
What is H. pylori also associated with?
Gastric cancer
How can H. pylori lead to gastric cancer?
It inhibits apoptosis of its gastric pit cells (lack or apoptosis also inhibits cell turnover & healing)
Chronic inflammtion -> Increase risk of cancer
Some strains produce a toxin (CagA) that can degrade p53 proteins, which are normally tumor suppressors
How does H. Pylori cross the mucus layer of the stomach?
H. pylori urease causes: Urea -> NH3 + CO2
HCI is neutralized; pH increases
Mucin will "de-gel" when under conditions of increased pH & can no longer carry out its protective function
H. pylori needs the "de-gelling" & increased pH process to occur so it can move though the mucus layer & to the epithelial cells
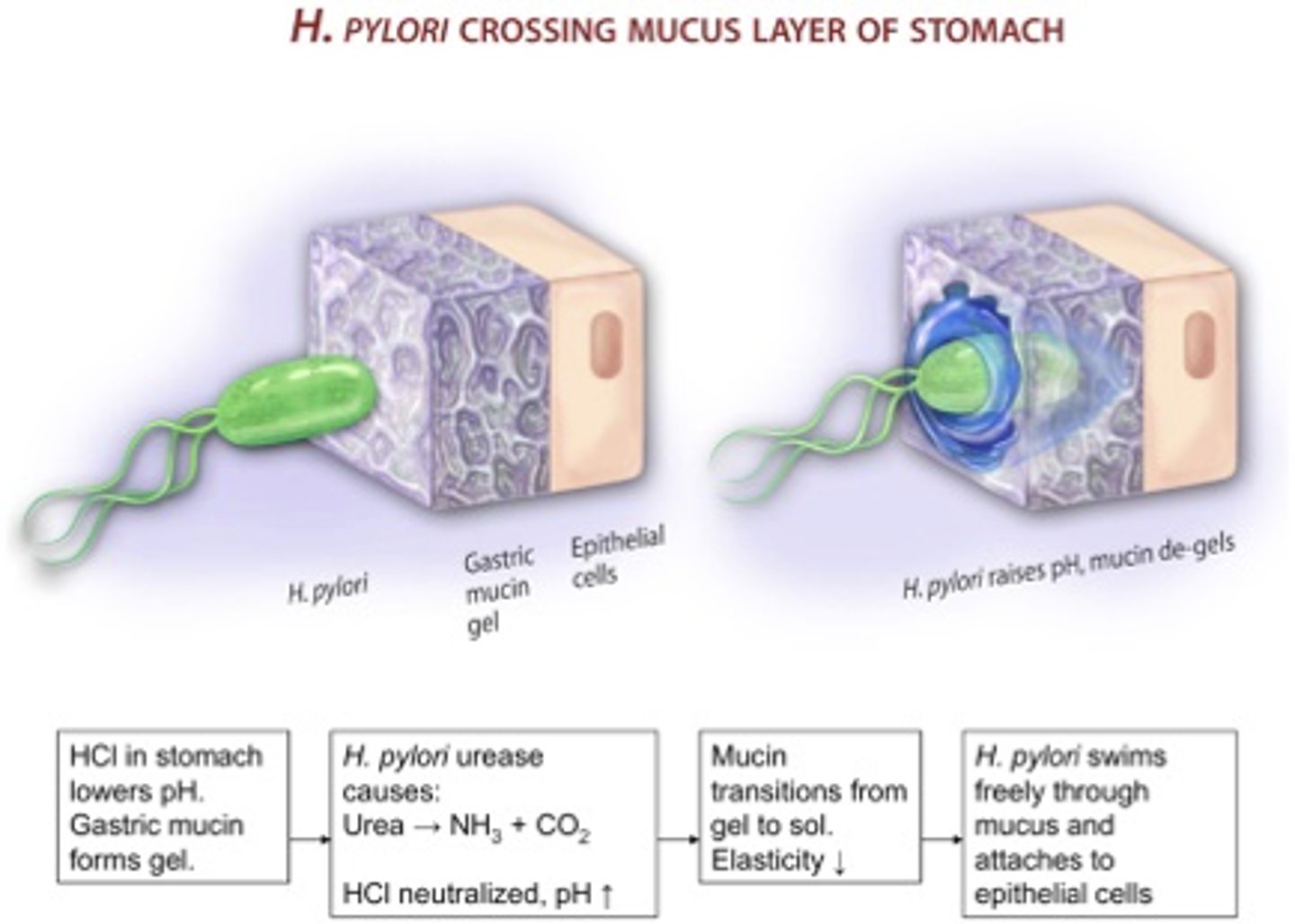
What does Gel + Low/acid pH cause?
H. pylori cannot move
How can H. pylori cause mucosal injury?
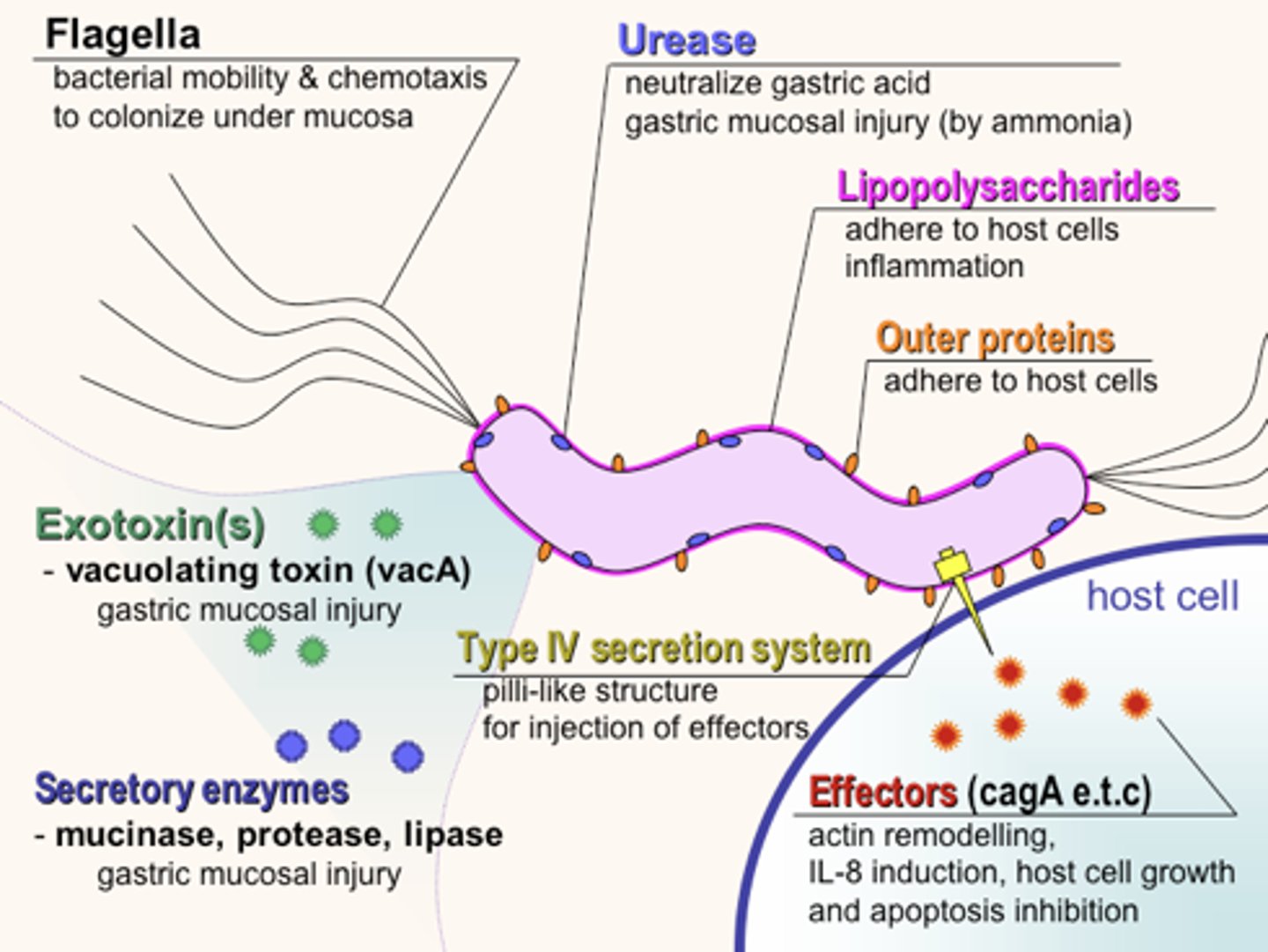
How is H. pylori diagnosed?
-Gold standard: Biopsy via endoscopy
-H. pylori breath test: non-invasive & reliable
-H. pylori antibodies can be measured but are not recommended for dx purposes
What does the H. pylori Breath test take advantage of?
The fact that H. pylori bacteria releases urease that breaks down urea into CO2 & Ammonia
How does the H. pylori breath test work?
There is a pre- & post-test; the pt will blow into a special "balloon"each time
-Pt. swallows a liquid after the pre-test balloon.
-Liquid contains urea made from carbon-13 isotope (13C-urea)
-If H. pylori is present, the 13C-urea is broken down into 13CO2 and NH3.
What is compared in the Pt breath samples?
The pre- & post-ratios of 13CO2 to 12CO2
If the ratio is increased in the post-test sample (more 13CO2 than 12CO2) the test is POSITIVE for H. pylori
When are NSAIDs more likely to cause PUD?
With long-term and or/ high dose therapy (even in long-term 81 mg aspirin)
How can NSAIDs cause PUD?
1. Can cause direct topical injury to the gastric mucosa
2. Promote increased neutrophil adherence to vascular endothelium -> neutrophil-derived ROS & proteases -> damaged mucosal layer
3. By inhibiting COX-1 and COX-2, they also inhibit certain beneficial prostaglandins
What does inhibiting certain beneficial prostaglandins lead to?
1. Deceased submucosal blood flow-ischemia- (inhibits healing of any erosion that forms)
2. Decreased mucosal proliferation
3. Decreased production of mucus & HCO3-/bicarb (allows erosion to form in the presence of HCI acid)
4. Increased secretion of gastric acid & pepsin
NSAIDs inhibits the gastric mucosal-protective prostaglandins
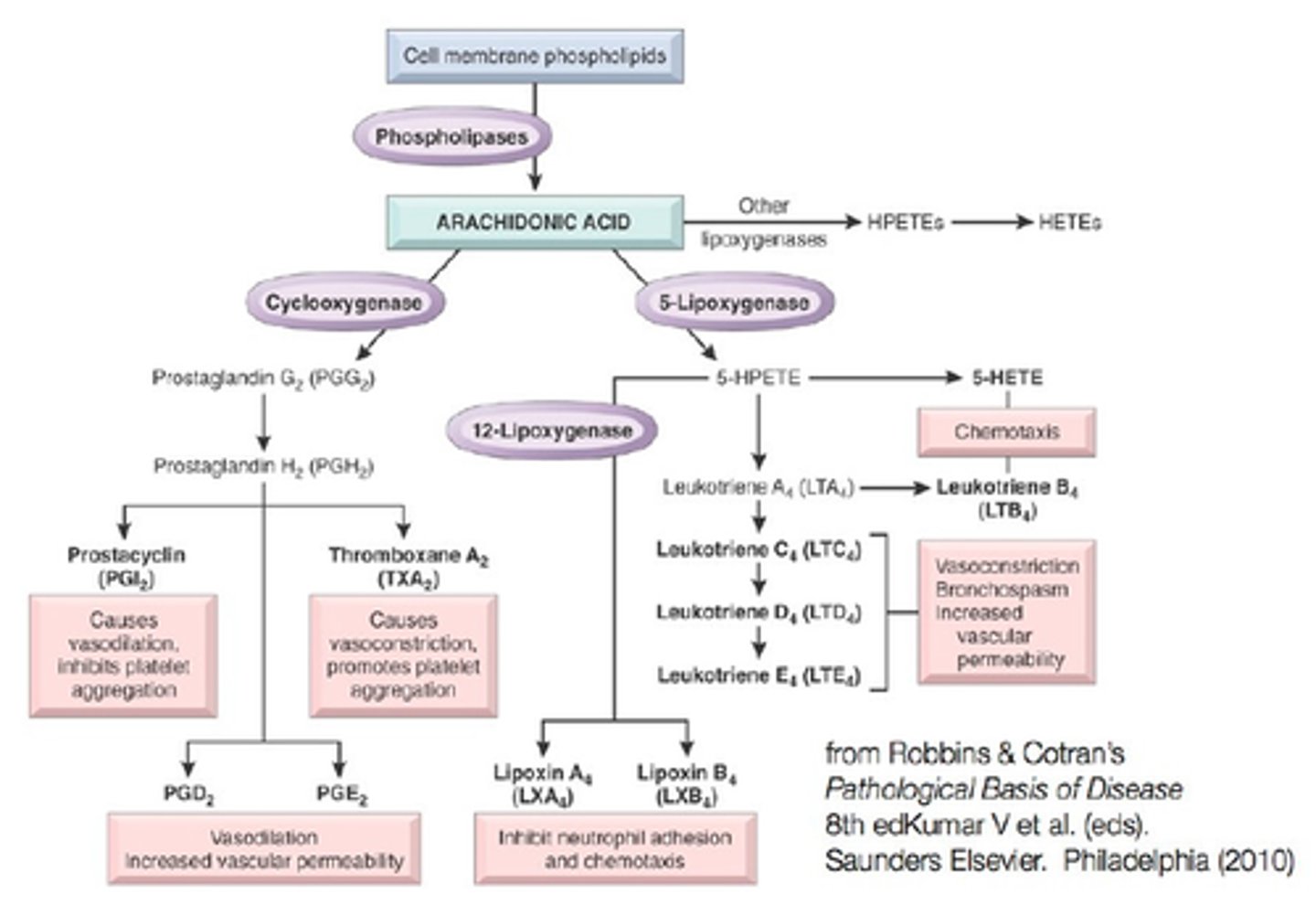
Damage from NSAIDs
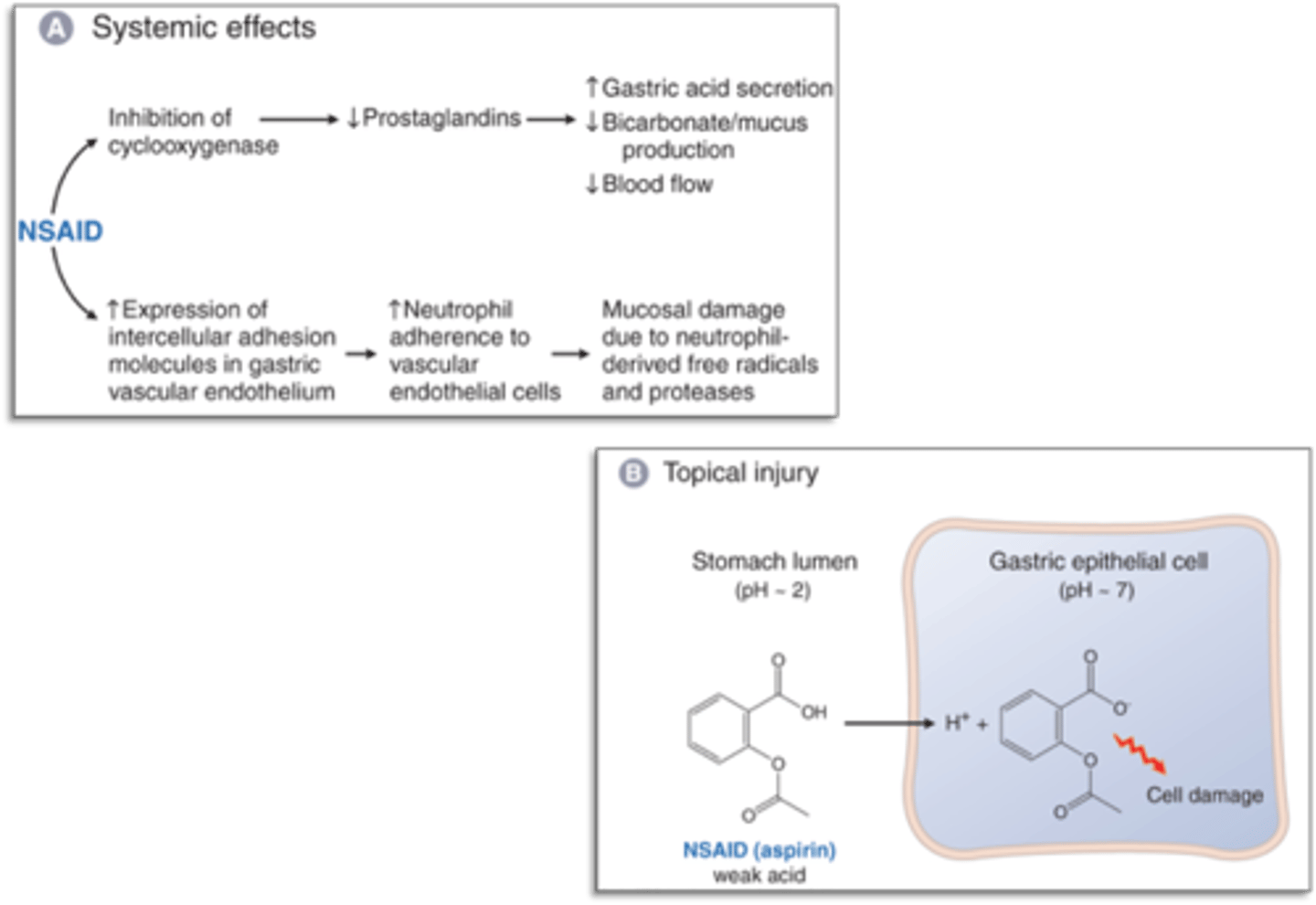
More damage from NSAIDs picture
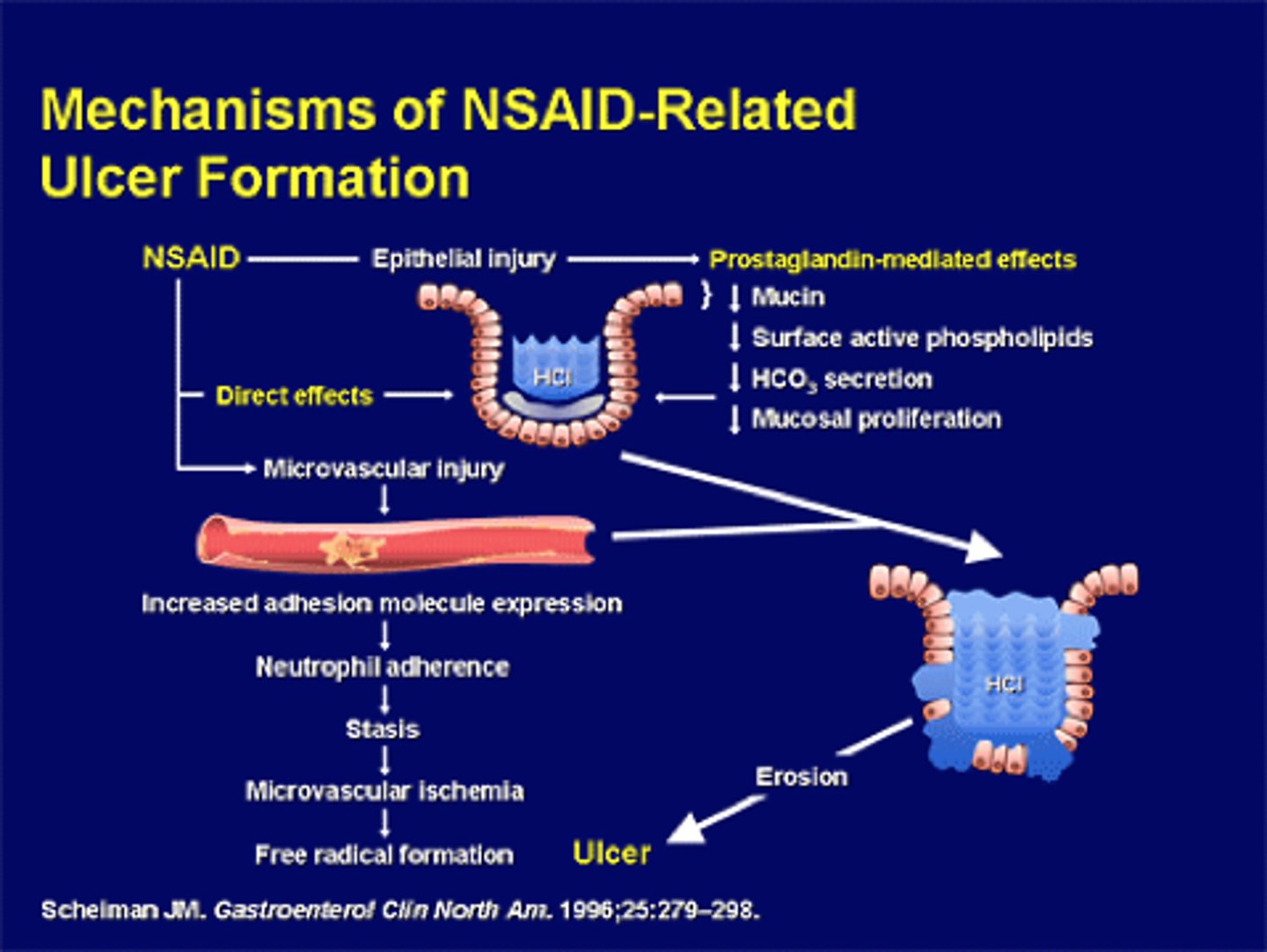
What are risk factors for NSAID-Induced PUD?
-Increased age (esp. >65 y.o.)
-Previous Hx of PUD or related complication
-Combined NSAIDs (multiple NSAIDs, including aspirin)
-Combinations of NSAIDs w/ corticosteroids (also bisphosphonates, anticoagulants, antiplatelet agents, SSRIs)
-Cigarette smoking (heavy EtOH consumption)
What about "stress ulcers" and "stress ulcer prophylaxis"? Don't all hospitalized patients need "stress ulcer prophylaxis"?
NO
Which patients should not receive stress ulcer prophylaxis?
Hemodynamically stable Pt admitted to general-care floor (b/c it will only decrease the rate of GI bleeding)
What symptoms of PUD?
-Epigastric pain (gnawing, dull, aching, often burning, but not always); can be severe
->Gastric & duodenal pain
-C/O Nausea
-Some ulcers can e asymptomatic until the patient suffers a a more serious event (ex; GI bleed)
-If bleeding is present, the labs may show anemia
What is gastric pain?
This pain is aggravated or precipitated by food
What is duodenal pain?
Pain that occurs 1-3 hours after a meal & is relieved by food
What are alarm symptoms that are seen in PUB?
Bleeding, perforation & obstruction
What are alarm symptoms an indication of?
Emergency medical care
Where is bleeding seen in alarm symptoms?
Seen as melena (black or or tarry-appearing stools) or hematemesis ("coffee ground" emesis)
Important Pt Teaching
What is perforation in alarm symptoms?
Upper abdominal pain w/ radiation to back
What is obstruction in alarm symptoms?
Nausea, vomiting & abdominal distension
Additional Info About Meds for Acid Disorders
What are Non-pharmacologic approaches to GERD & PUD?
Lifestyle modifications (esp. in GERD)
Discontinuation of NSAIDs (esp. in PUD)
Surgical Intervention
What are the 4 general pharmacologic approaches to GERD & PUD?
1. Antacids (to neutralize acid)
2. Antisecretory Agents (prevent acid from being produced or prevent stimulation of acid production)
-> H2 receptor antagonist & PPIs
3. Mucosal Protectants (coat/protect gastric mucosa)
4. Antimicrobials (treat H. pylori infection)
What are some lifestyle modifications for GERD?
-Elevate head of bed 4-6" by putting blocks under legs of bed; avoid sleeping on back
-Dietary changes
-Smoking cessation; Avoid alcohol
-If possible discontinue or use caution w/ meds that exacerbate or cause the problem
What are some dietary changes for GERD?
Avoid foods that decrease LES pressure
Avoid foods that have. a direct irritant effect
Eat small meals; avoid eating within 3 hours of laying down
Weight reduction if appropriate
What are advantages of Histamine2 receptor antagonist?
Symptomatic relief for most patients with mild and/or intermittent GERD and non-HP or non-NSAID-induced PUD. Cheaper than PPIs
What are disadvantages of Histamine2 receptor antagonist?
-Tolerance with continued dosing;
-CYP inhibition (depending on specific H2RA);
-Poor protection from PUD re-bleeding
-Only blocks one stimulus of acid production.
Omeprazole Pharmacogenomics: What do the various allele combinations of the gene that codes for CYP2C19 have an effect on?
They can cause a pt to be a rapid, intermediate, poor or ultra rapid metabolizer of omeprazole
What are the clinical implications of a pt being in one of those categories of metabolizers when they have an H. pylori that we are trying to cure?
If the omeprazole is metabolized at a rapid rate, then the active form of the drug will last for a shorter time and not be as effective
-> Pt is less likely to have their H. pylori cured
If the omeprazole is metabolized at a poorer rate, the active form of the drug will last longer and exert more of its effects
-> Pt is more likely to have their H. pylori infection cured
What are the 2 oral medications to eradicate H. pylori-induced PUD and what do they include?
PPI-based regimen x 14 days & Bismuth-Based regimen x 14 days
Both include a PPI & 2 Antibiotics
(the bismuth-based regimen also adds Bismuth subsalicylate)