3.2 Transport (blood)
1/40
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
41 Terms
What are the three types of vessels?
Arteries- Carries blood away from the heart
Veins- Carries blood back to the heart
Capillaries- Fine networks of tiny tubes linking arteries and veins (facilitates exchange
Describe how the structure of the capillary aid in its function?
Narrow diameter(10 um) of the lumen
- So the red blood cells are in close contact with the capillary wall to reduce diffusion distancea large surface area due to branching
-large surface area to volume ratiothin walls (one cell thick;single layer of endothelium cells)
-Short diffusion distanceFenestrations(gaps in the walls)
- allows larger volumes of tissue fluids to be produced which speeds up exchange between the tissue cells and the blood.
Compare the arteries and veins
Arteries: Carry pulses of high-pressure blood away from the heart to every organ of the body
Veins: Carry a stream of low-pressure blood from the organs back to the heart
lumen thickness enables pressure inside the artery to be maintained and reduces friction between blood cells and the walls of the vessel, enabling the blood to flow freely under low pressure in the veins.
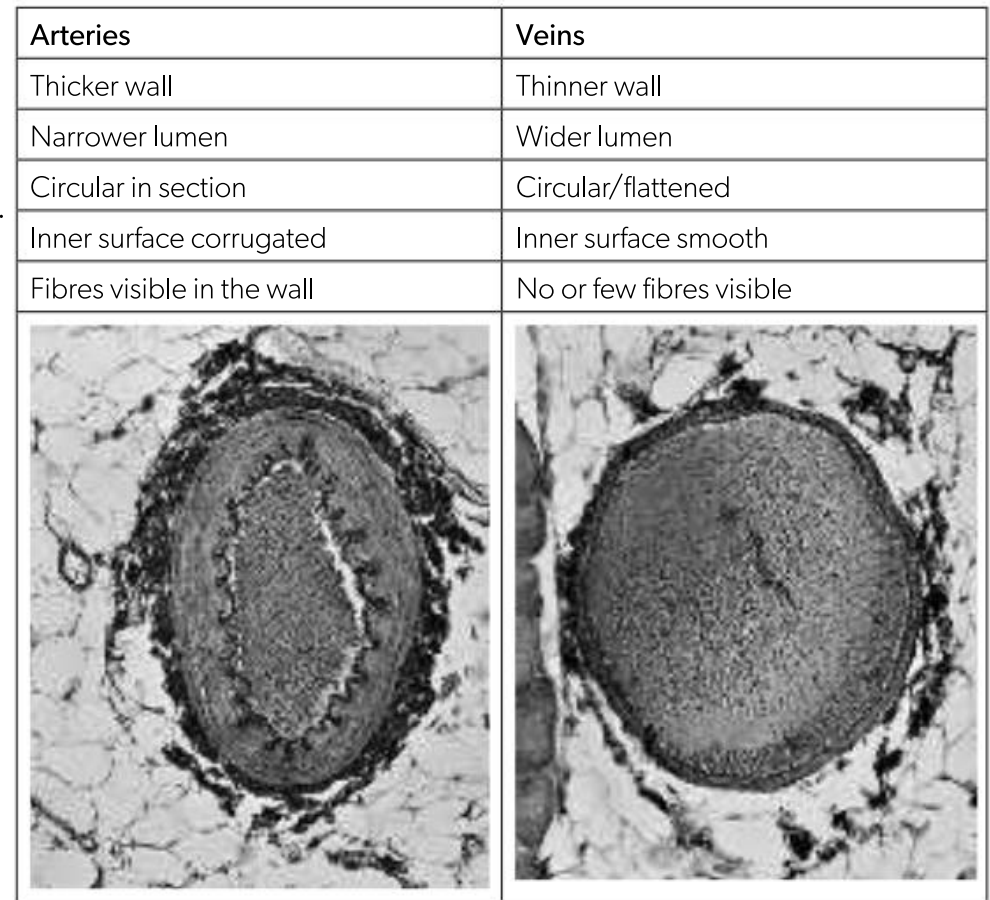
Function and structure of the artery
Function: transports blood away from the heart at high pressure
Elastic in the walls- stretches to accommodate the increased volume of blood as the heart contracts
High wall thickness- withstands blood pressure and prevents rupture of the artery wall
High proportion of elastic fibres- they are first stretched then recoiled keeping the blood flowing and propelling it forward after each pulse passes
With increasing distance from the heart the tunica media progressively contains more smooth muscles and less elastic tissues and recoiling occurs due to the smaller differences in blood pressure
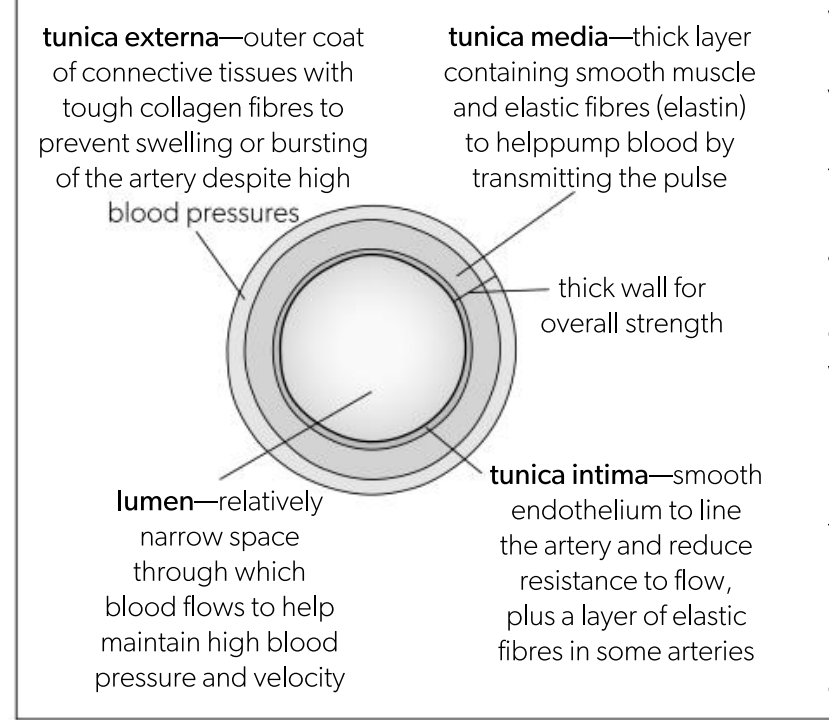
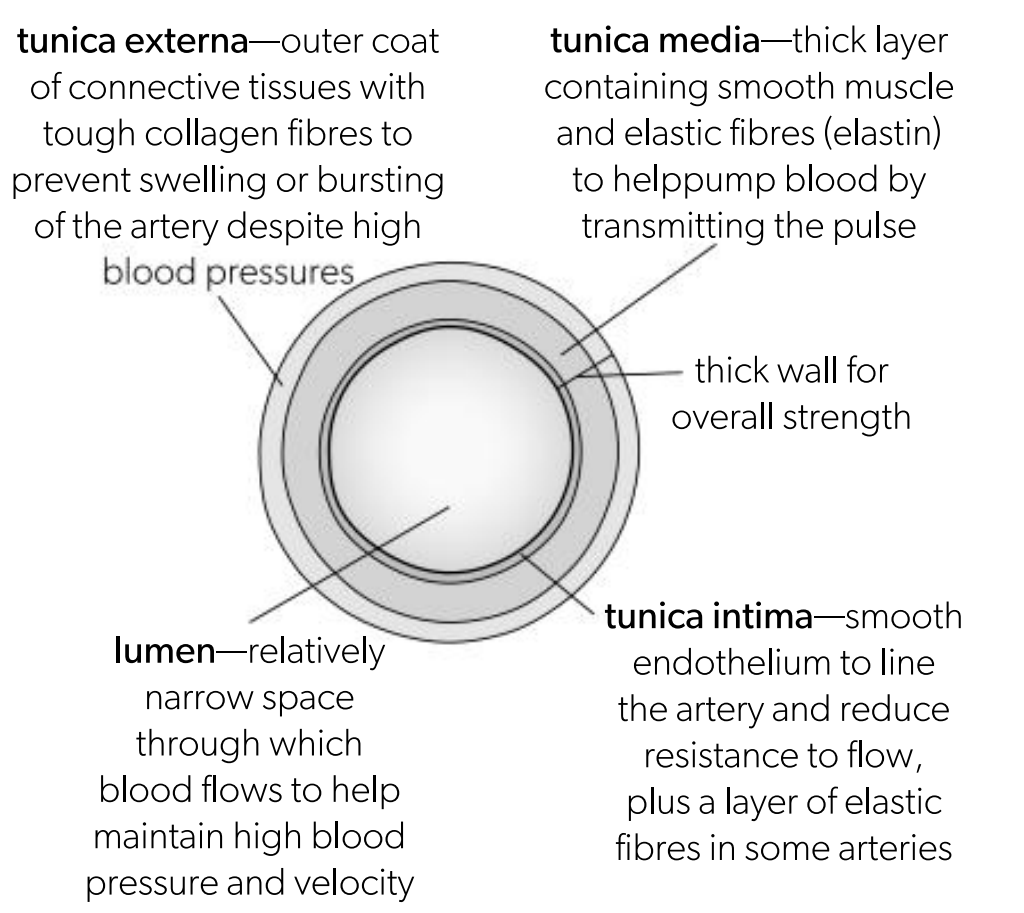
Tunica externa in an artery
Outer coat of connective tissues with tough collagen fibres to prevent swelling or bursting of the artery despite high blood pressures
anchors it to surrounding structures
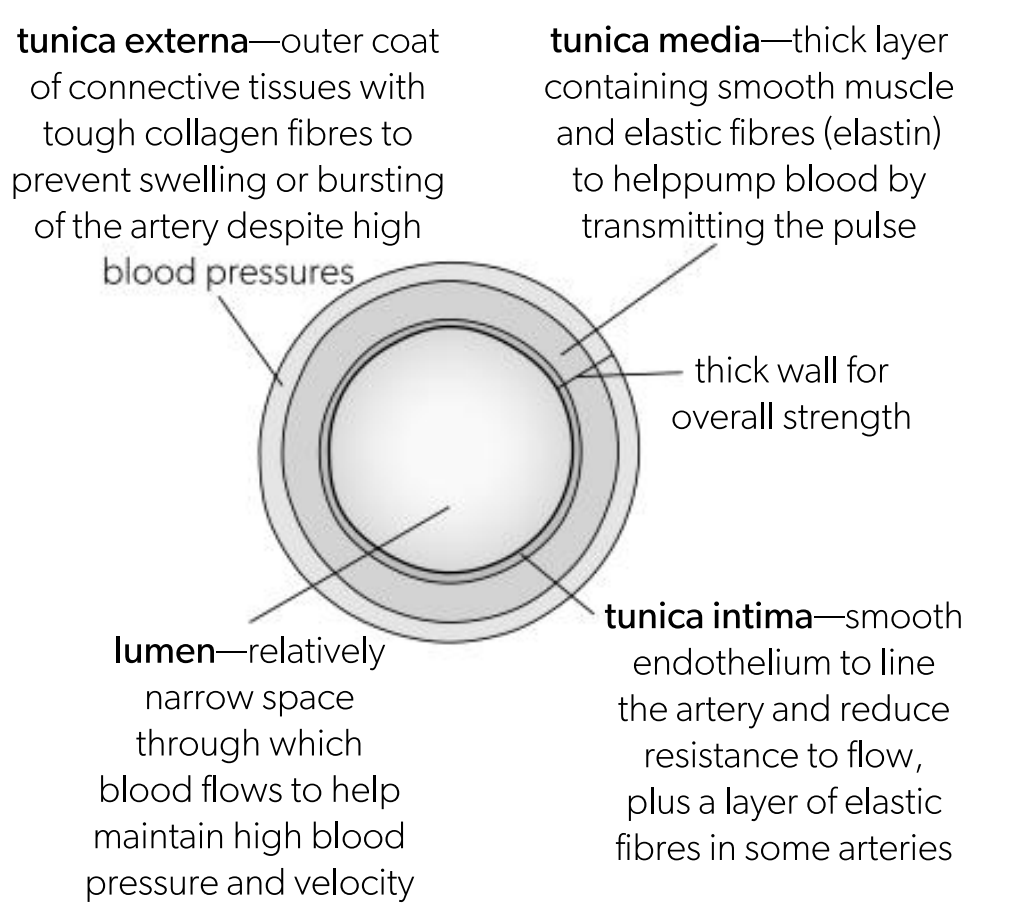
Tunica media in an artery
thick layer containing smooth muscles and elastic fibres to help pump blood by transmitting the pulse
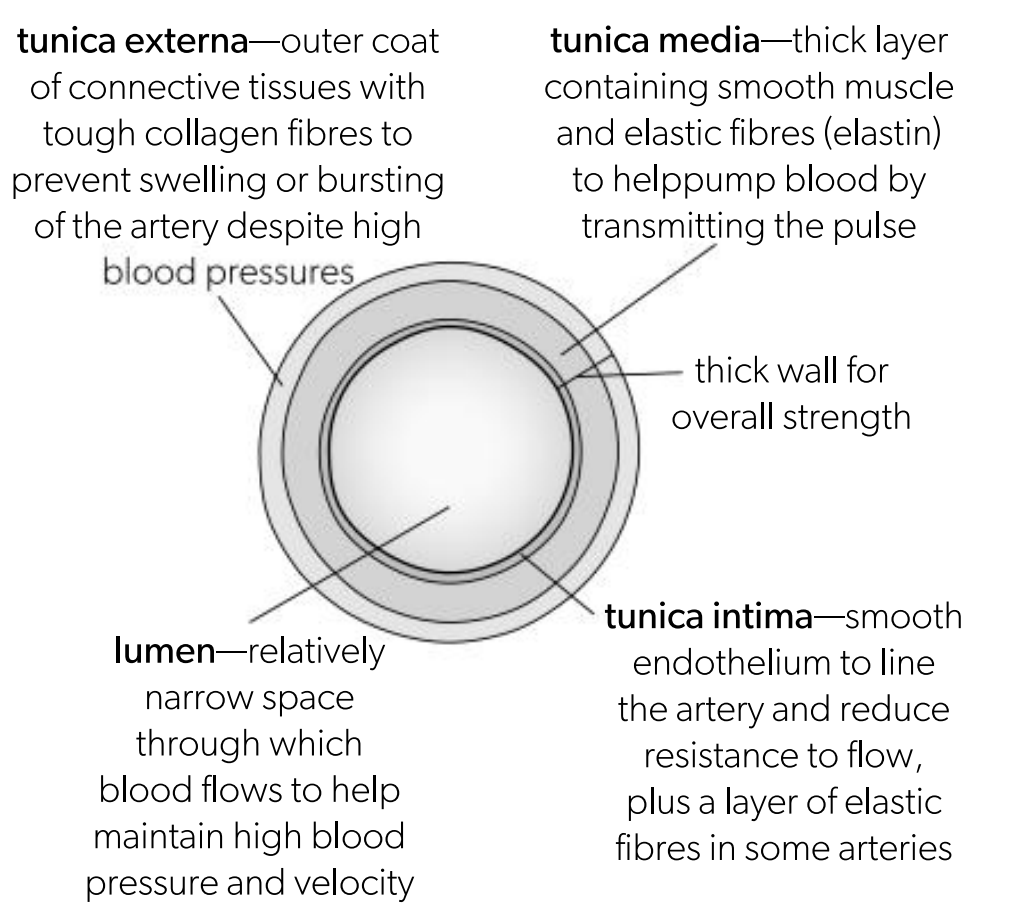
Tunica intima in an artery
Smooth endotheliu to line the artery and reduce the resistance to flow
What are the two arteries where we can find a pulse
cartoid artery (below the air)
radial artery (in the wrist)
Function of veins
Returns blood to the heart
Thinner wall relative to the diameter of the lumen with less smooth muscles and elastic tissues in tunica media
Wall of the vein is flexible, which allows veins to be compressed by the contraction of skeletal muscles.
venous blood flow is aided by skeletal muscles adjacent to veins that become wider when they contract, pressing the vein flatter and raising blood pressure.
Tunica media in veins
thin layer with few elastic or collagen fibbers as blood pressure is low and there is no need for pulse
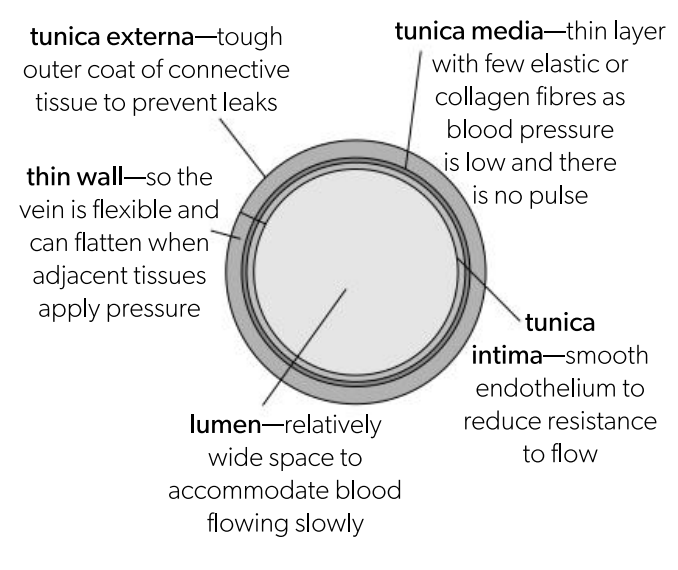
Tunica externa in veins
Tough outer coat of connective tissues to prevent leaks
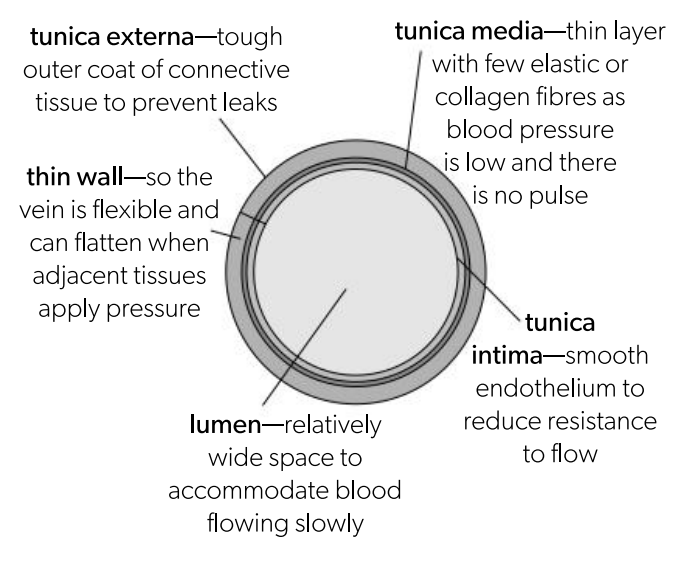
Tunica intima in veins
Smooth endothelium to reduce resistance to flow
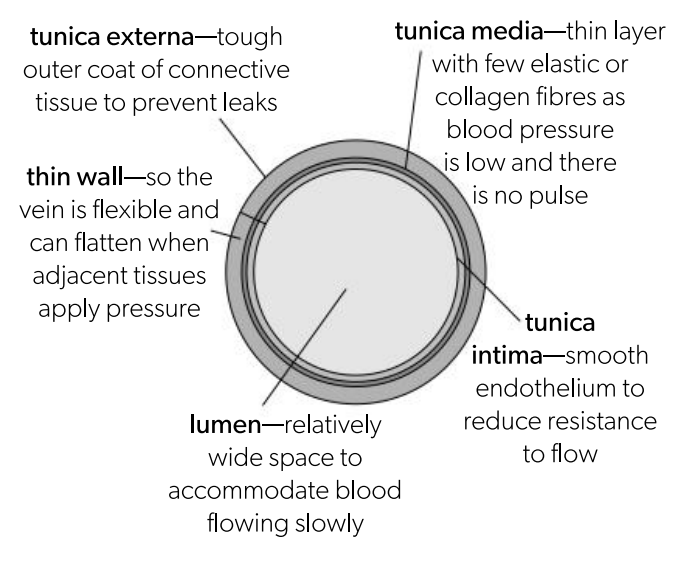
Why is there a risk of backflow of blood and How do valves prevent backflows?
Pressure in veins can drop so low that blood flow stops so there is a risk of backflow towards the capillaries.
To prevent backflow, veins contain one way valves.
Each valves contains of three pocket shaped flaps of tissue which open in the same direction as blood flow and closes if blood tries to flow back in the opposite direction.
State the function of the coronary arteries.
Arteries that branch from the aorta to supply the heart muscle with blood (nutrients and oxygen).
Outline the cause and consequence of a coronary occlusion.
Occlusion is the total blockage of the artery.
Caused when the lumen of the artery becomes narrower and restricts blood flow due to the plaque (deposit of fats and cholesterol)
The atherosclerotic plaque can also:
raise blood pressure (as it impedes blood flow) leading to damage in the arterial wall which is then repaired using fibrous tissue however it reduces the elasticity of the vessel wall. rupture, exposing the damaging tissue underneath
if plaque ruptures, blood clotting is triggered which can cause ischaemia (lack of blood flow)
Factors which effects coronary heart disease
High blood pressure
smoking
obesity
inactive lifestyle
family history
old age
high blood cholestrol concentration
diabetes
Define tissue fluid
Formed when blood plasma is pushed out of the capillary walls into the surrounding tissue.
A mixture of water and solutes, forced out of the blood by ultrafiltration, which surrounds body cells.
Outline what happens briefly when an infection occurs
chemical signals are released by the damaged tissues or by pathogens causing the infection.
These are detected by white blood cells which then squeeze out through the capillary walls and move to the site of infection
What happens at the arteriole?
At the arteriole where the blood enters the capillary, hydrostatic pressure is high, resulting in fluid being pushed out of the capillary wall into the surrounding tissues ny ultrafiltration.
What happens at the venule?
At the venule , much of the fluid is already lost from inside the capillary, decreasing the hydrostatic pressure, resulting in majority of the tissue fluid being drawn back into the capillaries.
Release and reuptake of fluids in tissues
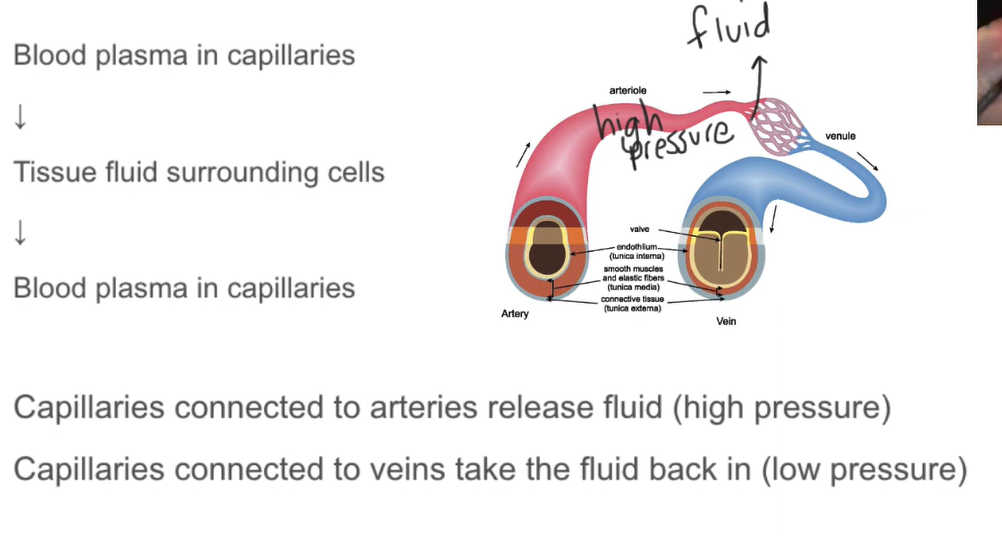
Outline the direction of transport of substances that are exchanged between tissue fluid and cells in the tissue
Into Cells:
Nutrients, hormones, and oxygen move from tissue fluid into cells.
Concentrations are lower in tissue fluid than in blood plasma at arterial capillaries.
Out of Cells:
Excess water and waste products, including carbon dioxide, move from cells into tissue fluid.
Concentrations are higher in tissue fluid than in blood plasma at arterial capillaries.
Exchange of substances between tissue fluid and cells in tissue (mention how)
Oxygen diffuses into cells (concentration gradient)
Glucose moves into cells (sodium-glucose cotransports)
Carbon dioxide moves out of the cells (concentration gradient)
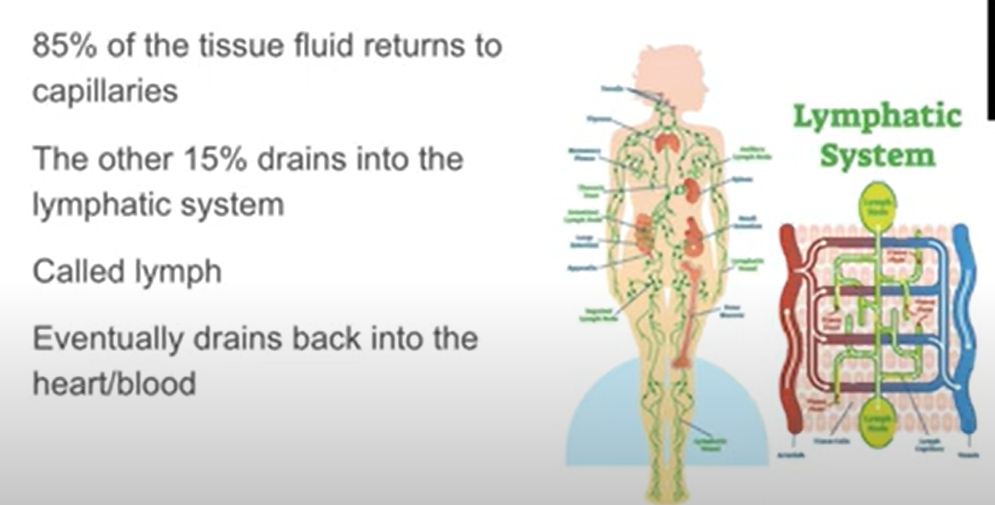
Why is there a need to drain excess tissue into lymph ducts?
Lymphatic Capillaries:
Approximately 90% of tissue fluid drains back into capillaries.
The remaining 10% enters lymphatic capillaries located in the interstitial space.
Lymphatic capillaries have thin, permeable walls made of a single layer of endothelial cells with small gaps.
Lymph Formation:
Once inside the lymphatic system, the fluid becomes lymph.
Lymph is a colorless fluid containing excess tissue fluid, white blood cells, proteins, and other substances.
Its function includes transporting immune cells and removing foreign particles and toxins from the body.
Lymphatic Vessels and Nodes:
Lymphatic capillaries drain into lymphatic vessels (ducts).
Lymphatic vessels rely on surrounding skeletal muscle contractions to move lymph.
Valves ensure one-way flow, similar to veins.
Lymph Nodes:
Lymph nodes act as a filter, trapping or destroying harmful substances.
Dendritic cells sample lymph for pathogens, triggering immune responses.
Larger lymph vessels return lymph to the circulatory system, where waste products and bacteria can be removed by the liver or kidneys.
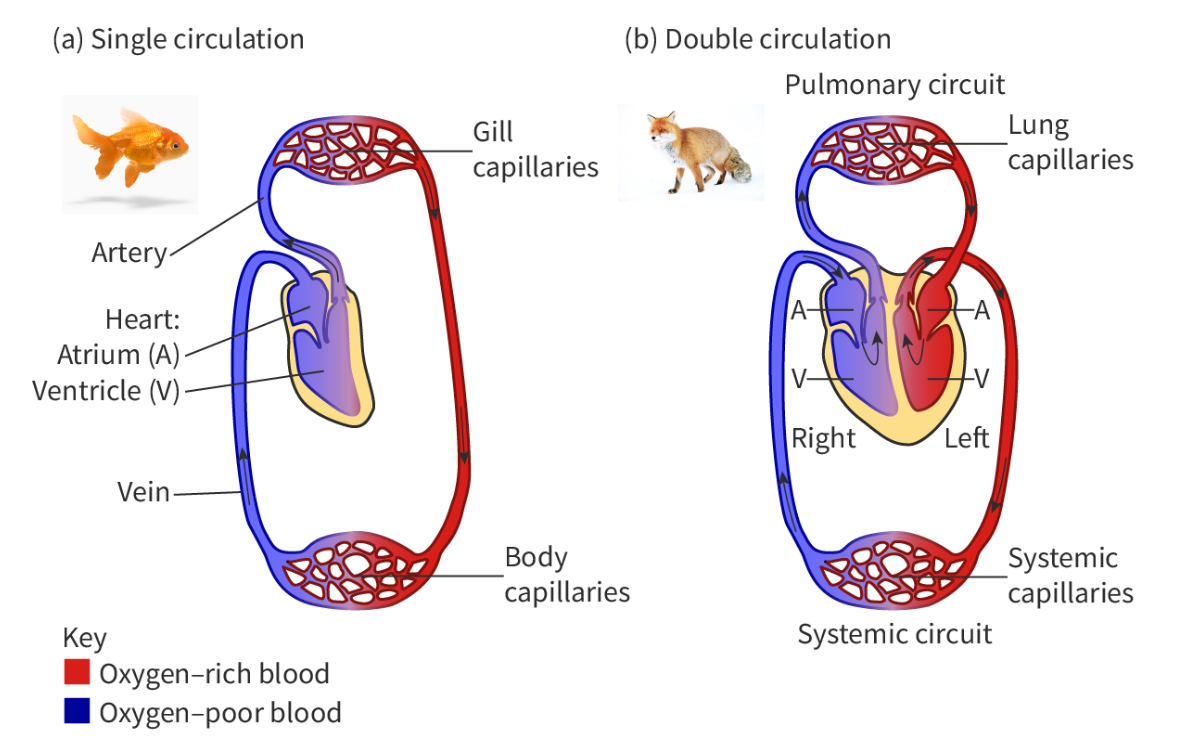
State the function of the heart and lungs/gills in the circulatory system
draw a diagram of the single circulator and double circulatory system
Bony fish have a single circulatory system. This means that to complete one circulation around the body, blood has to pass through the heart once.
In contrast, mammals have a double circulatory system. This means that to complete one circulation around the body, blood has to pass through the heart twice (Figure 1). This double circulation is composed of:
the pulmonary circulation, where blood is pumped from the heart to the lungs, and then returned to the heart, and
the systemic circulation, where blood is pumped from the heart to the rest of the organism and back to the heart
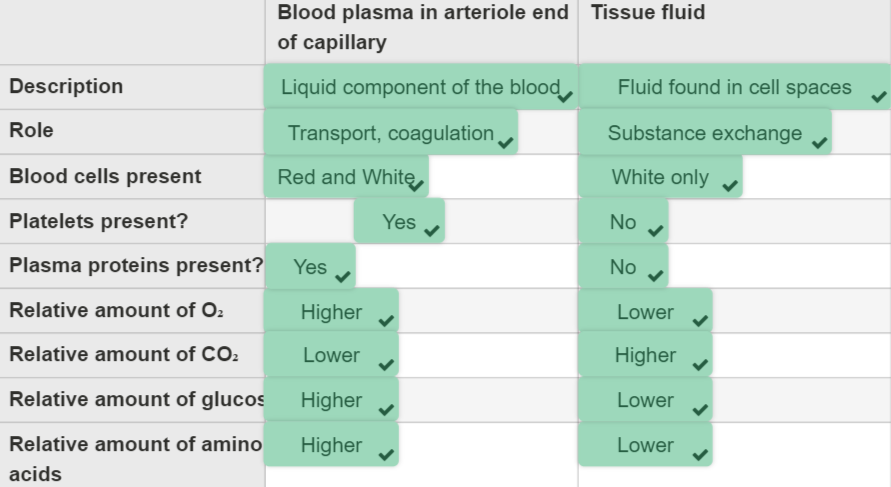
Compare the compositions of blood plasma and tissue fluid
Label a diagram of the heart
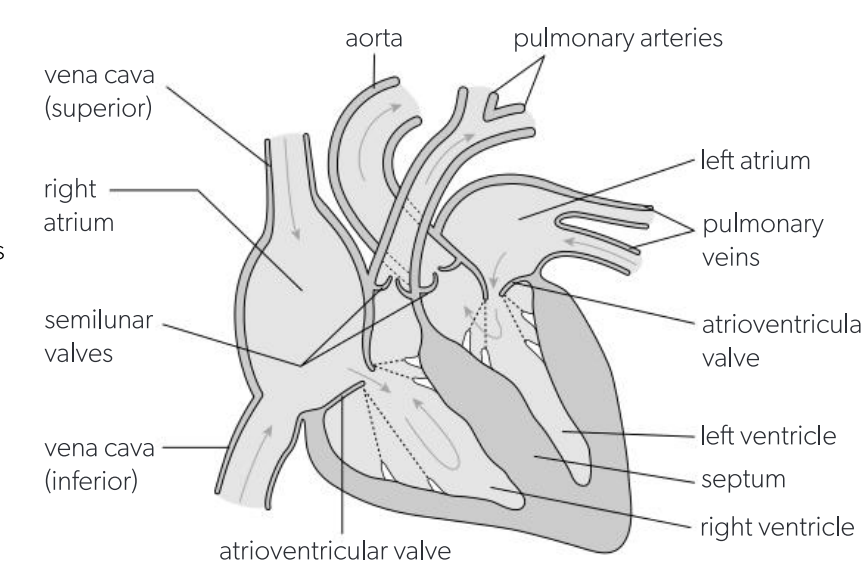
Function of artia
collecting chambers with relatively thin muscular walls, which gradually fill with blood returning in veins to the heart, and then pump the blood into the ventricles
Function of ventricles
Pumping chambers with thick muscular walls that pump blood out into the arteries; pumps oxygen to all organs of the body apart from the lungs
Function of septum
the wall between the left and right sudes if the heart that ensures the heart acts as a double pumo and that dexoygeneated and oxygeneted blood do not mix
Function of valves
atruiventricular valves betwee the atria and ventricles and semilunar valves between the ventricles and the arteries ensure the blood circulates by preventing backflow
Function of cardiac muscle
Muscle tissue with special property of contracting on its own without being stimulated by a nerve
Function of coronary vessels
the many capillaries in the muscular wall of the heart supply oxygen and glucose for aerobic respiration and removes waste products.
the blood running through these capillaries is supplied by coronary arteries and removed by coronary veins.
Function of pacemaker
a region of specialised cardiac muscle cells in the wall of the right atrium that initiates each contracting.
What is the first stage o the cardiac cycle?
The walls of the atria contract, pushing blood from the atria into the ventricles through the atrioventricular valves, which are open.
The semilunar valves are closed s the ventricles fill with blood.
What is the second stage of the cardiac cycle?
The walls of the ventricles contract powerfully and the blood pressure raises rapidly inside them.
This initially causes the atrioventricular valves to close, preventing back-flow to the atria and then causes the semilunar valves to open, allowing blood to be pumped to the arteries.
At the same time the atria start to refill by collecting bloods from the vein.
What is the third stage of the cardiac cycle?
The ventricles stop contracting so pressure falls inside them.
The semilunar valves open, preventing backflow from the arteries to the ventricles.
When the ventricular pressure drops below the artial pressure, the atriventricular valves open.
Blood entering the atriu from the veins then flows on to start filling the ventricles.
The next cardiac cycle begins when the walls of the atria contracts again.
Draw/and or interpret a graph showing blood pressure in the left ventricle and aorta during a typical cardiac cycle
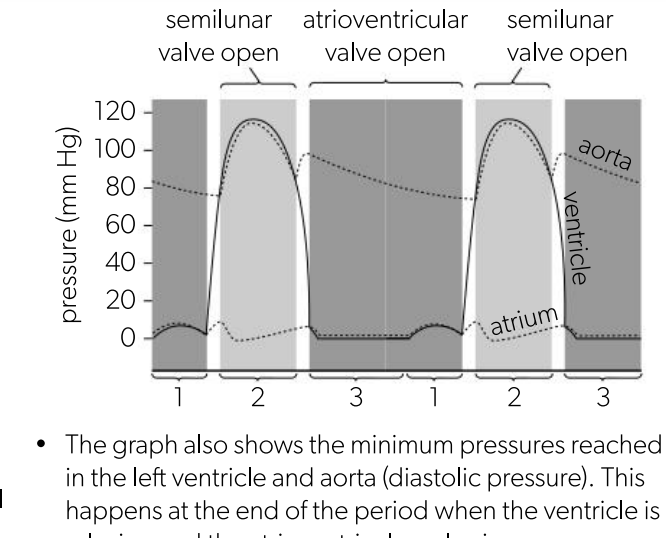
Atrial systole
The sinoatrial (SA) node, our heart’s natural pacemaker, initiates an electrical impulse. This signal spreads across the atria, causing them to contract and push blood into the ventricles through the atrioventricular valves.
Ventricular systole
The electrical signal reaches the atrioventricular (AV) node, which delays it. Then, it travels down the bundle of His and Purkinje fibers, causing both ventricles to contract simultaneously. This pushes blood through semilunar valves into the arteries.
Diastole
After each contraction, there’s a brief period of relaxation. During diastole, the heart refills with blood before another cardiac cycle begins. The atrioventricular valves remain open during diastole to allow blood flow from the atria into the ventricles.