2.3 Reproduction, Fertility and Contraception 🐣
1/60
Earn XP
Description and Tags
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
61 Terms
Function of male reproductive system
make sperm and deliver it to female reproductive system
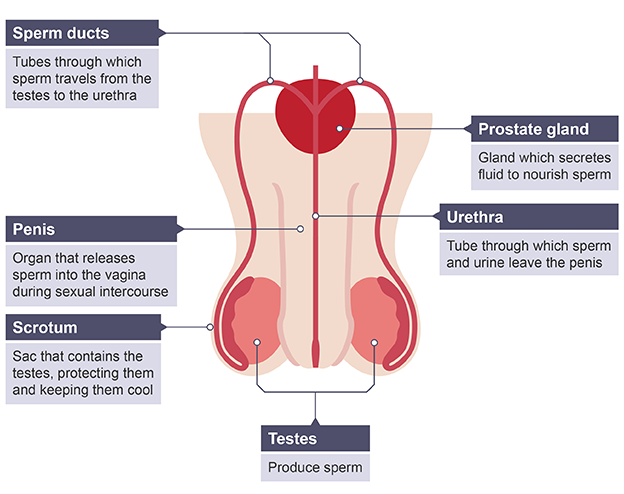
Urethra
Tube through which sperm and urine leave penis
Prostate gland
Secretes fluid to nourish the sperm
Penis
Organ that releases sperm into vagina
Scrotum
Sac that holds and protects testes, slightly lower than body temperature
Sperm ducts
Carries sperm from testis to urethra
Testis
Produces sperm
Sperm
haploid male gametes formed by meiosis
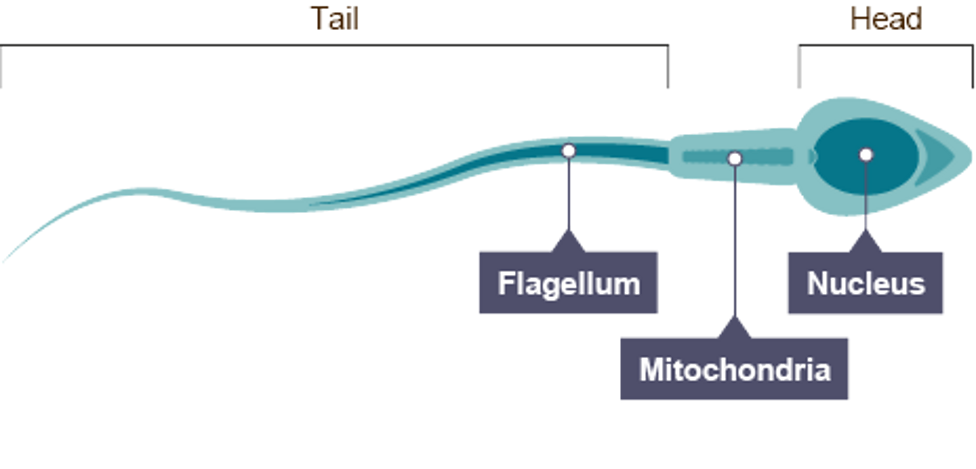
Adaptations of sperm
flagellum allowing it to swim through the female reproductive system
haploid nucleus containing half normal number of chromosomes
many mitochondria to produce energy
Function of female reproductive system
make and release eggs/ ova, protecting and nourishing the foetus until birth
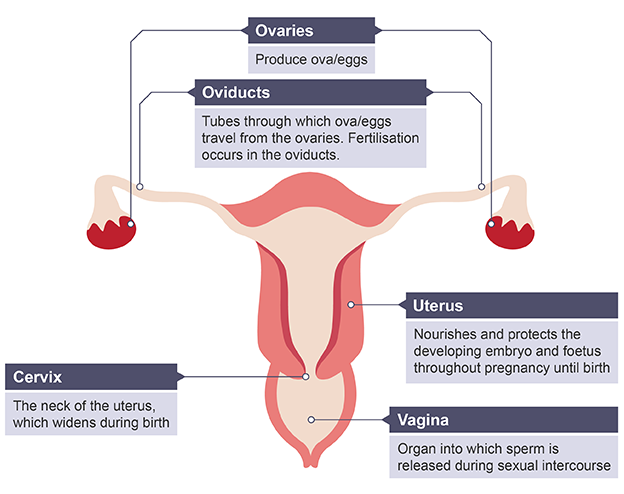
Ovaries
Produce ova (eggs)
Cervix
Opening of the uterus which widens during birth
Vagina
Where sperms is released and travels from
Oviducts
Carries ova from ovaries to the uterus and is where fertilisation takes place
Uterus
Will nourish developing foetus if pregnancy results
Fertilisation
fusion of haploid sperm nucleus and haploid egg nucleus to form diploid zygote, in the oviducts
Zygote
First cell of new individual
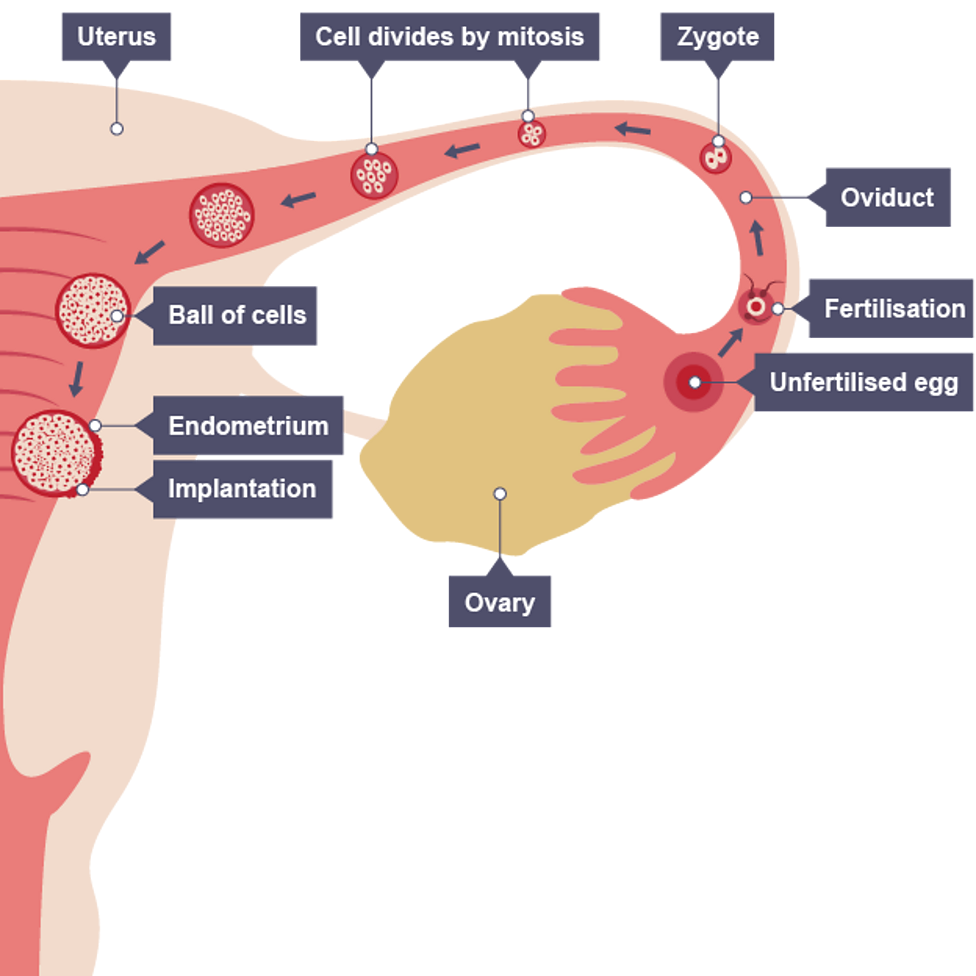
What happens after fertilisation
Zygote travels down the oviduct and divides by mitosis to form ball of cells (embryo)
Implantation when embryo reaches uterus, attaching and sinking into its thick lining to receive nourishment
Placenta, umbilical cord, amnion and amniotic fluid form.
Embryo differentiates to produce variety of tissues and organs
Referred to as foetus when all organs start to form
Placenta
allows useful substances to diffuse from mother’s blood to foetus and waste from foetus to mother’s blood
Adaptations of the placenta
large surface area for exchange between uterus wall
finger like projections that extend into uterus wall, called villi, further increasing surface area
good blood supply
Umbilical cord
attaches placenta to the foetus, contains umbilical artery and vein
Umbilical artery
Carries urea and carbon dioxide from foetus to mother’s blood
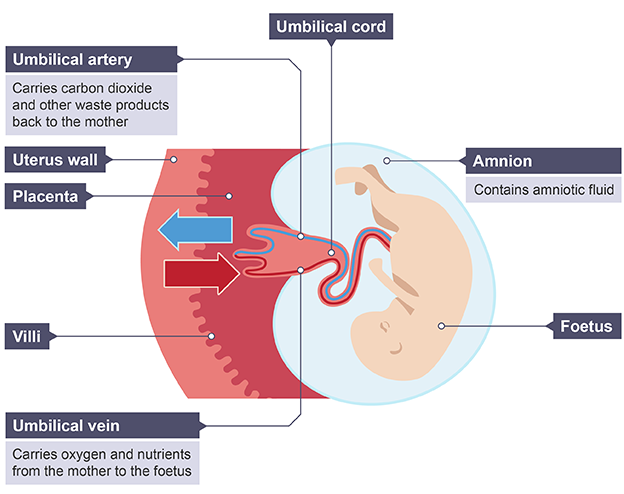
Umbilical vein
Carries oxygen and nutrients from mother’s blood to foetus
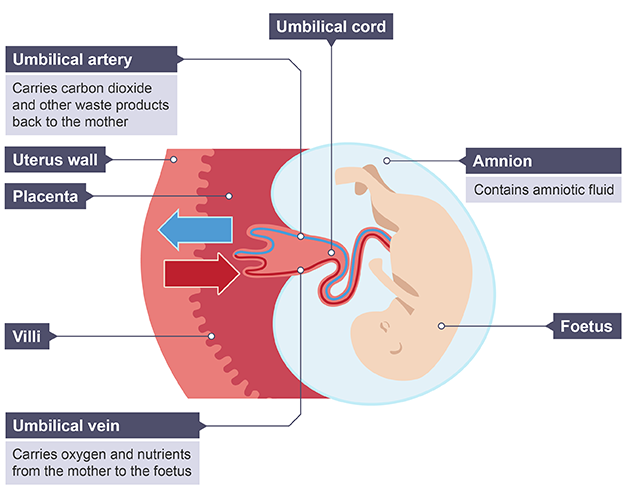
Maternal and foetal blood systems
Close together but not joined, thin membranes separate and allow for diffusion
Amnion
Protective membrane that forms around the embryo and contains amniotic fluid
Amniotic fluid
Surrounds and cushions developing embryo
Male sex hormone
Testosterone, produced in testes
Female sex hormone
Oestrogen, produced by ovaries
Secondary sexual characteristics in males
Testes enlarge
Body becomes more muscular
Voice deepens
Secondary sexual characteristics in females
Sexual organs enlarge, breasts develop
Pelvis and hips widen
Menstruation begins
Secondary sexual characteristics in males and females
Body and pubic hair grow
Sexual awareness and drive increase
Menstrual cycle
28 days cycle (on average) that prepares for pregnancy
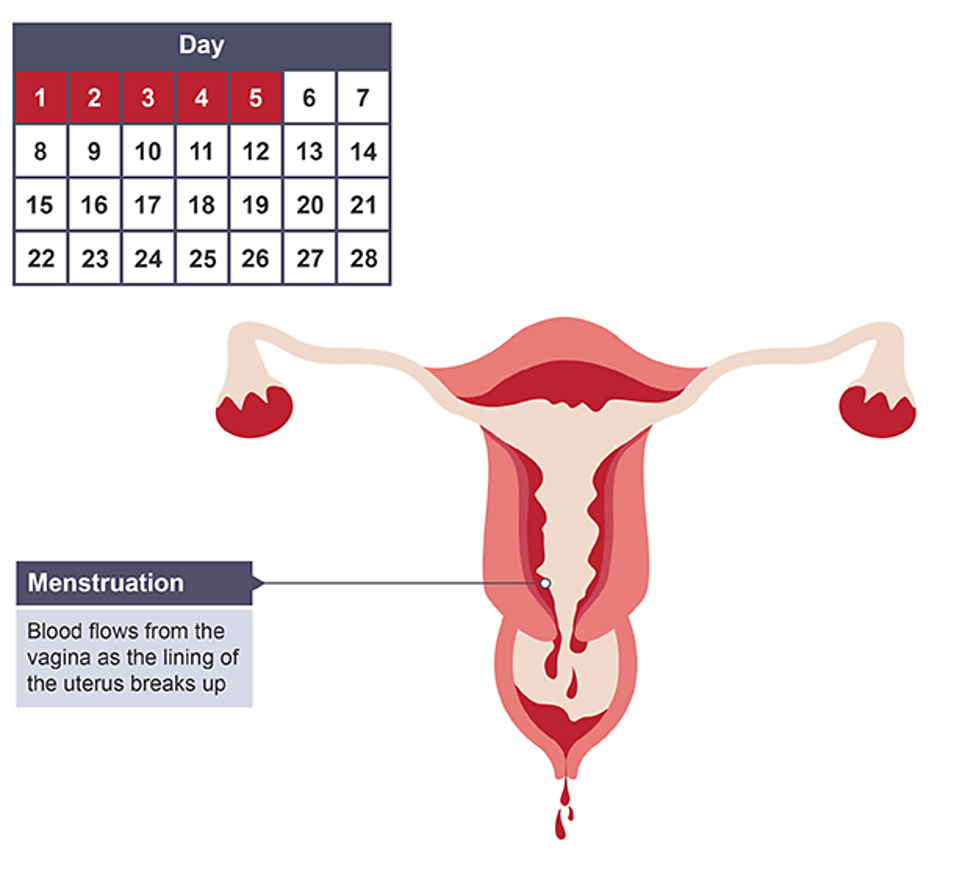
Menstruation
breakdown and removal of blood rich uterine lining through the vagina, at end of each cycle due to low oestrogen/ progesterone
Days 1-5
Menstruation occurs, both progesterone and oestrogen levels are low causing lining to break down
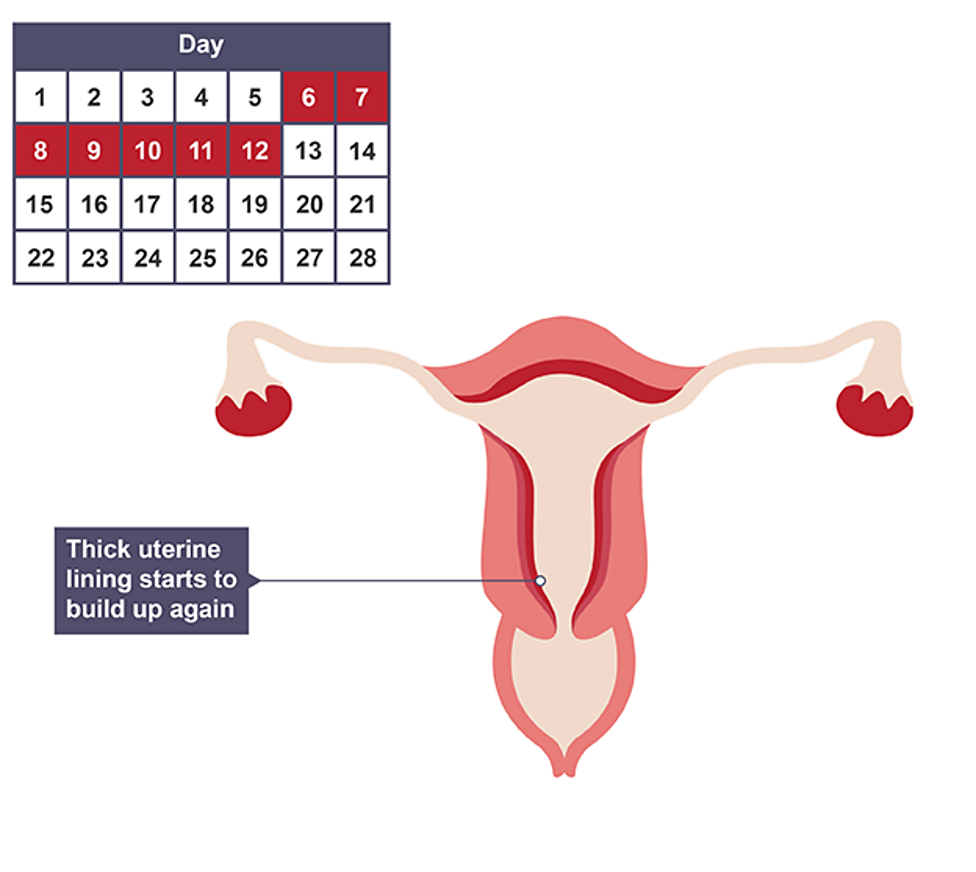
Days 6-13
Oestrogen increases, repairing uterus lining and its initial buildup
Day 14
Ovulation, oestrogen levels peak and cause egg to be released
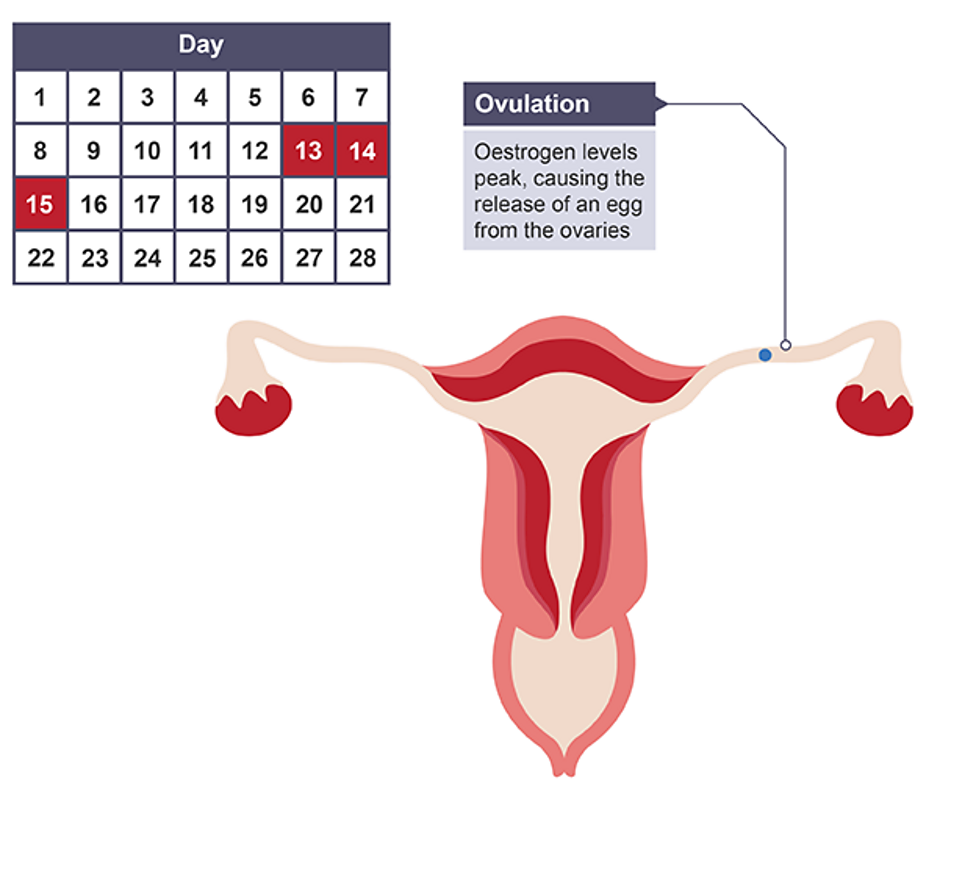
Days 15-28
Progesterone levels peak after ovulation to maintain thick lining
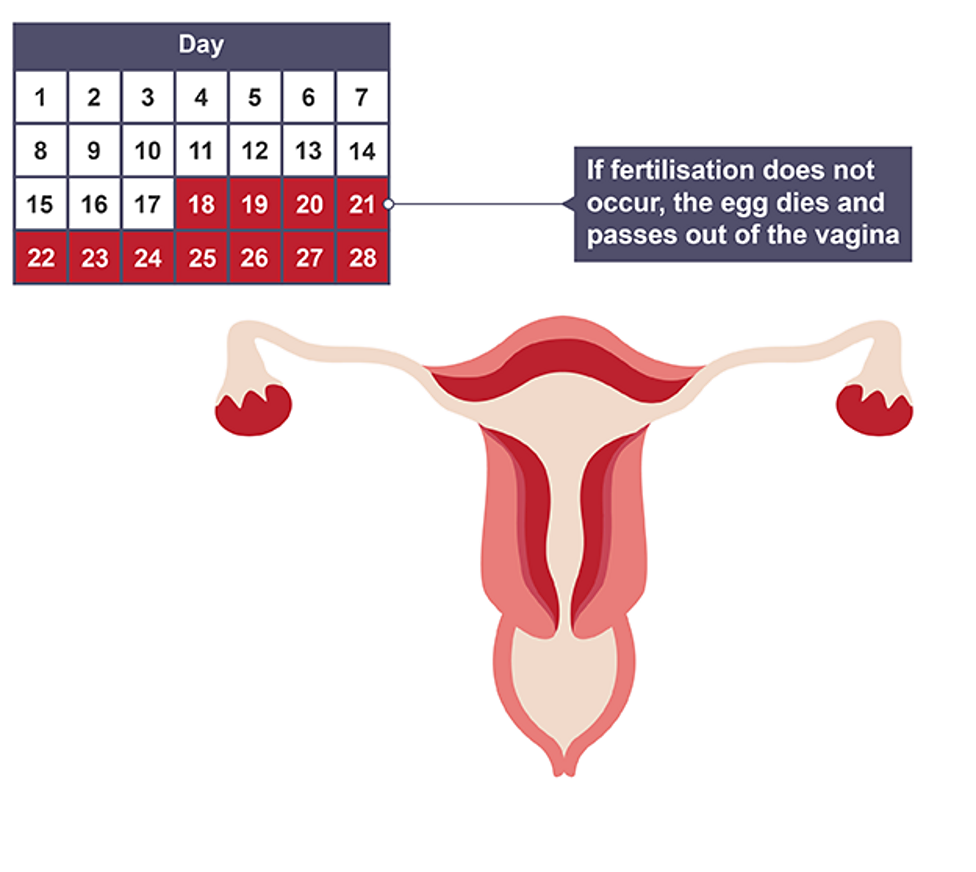
Day 28
If no pregnancy occurs hormone levels decrease and cycle restarts
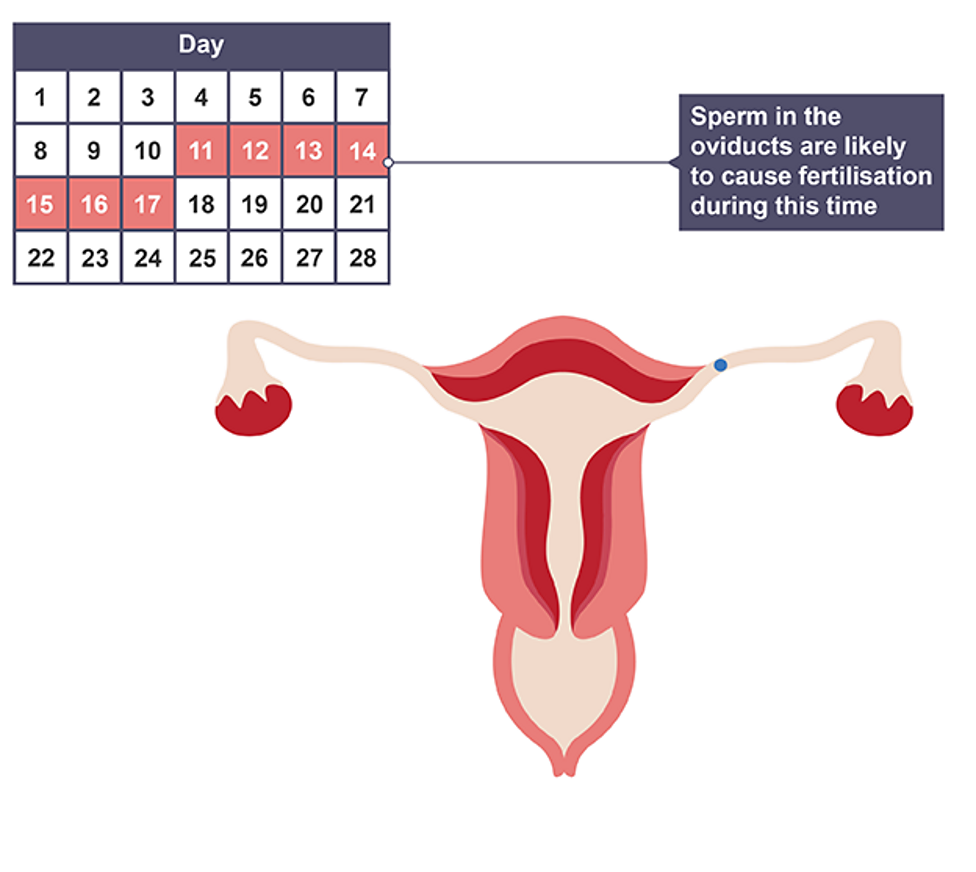
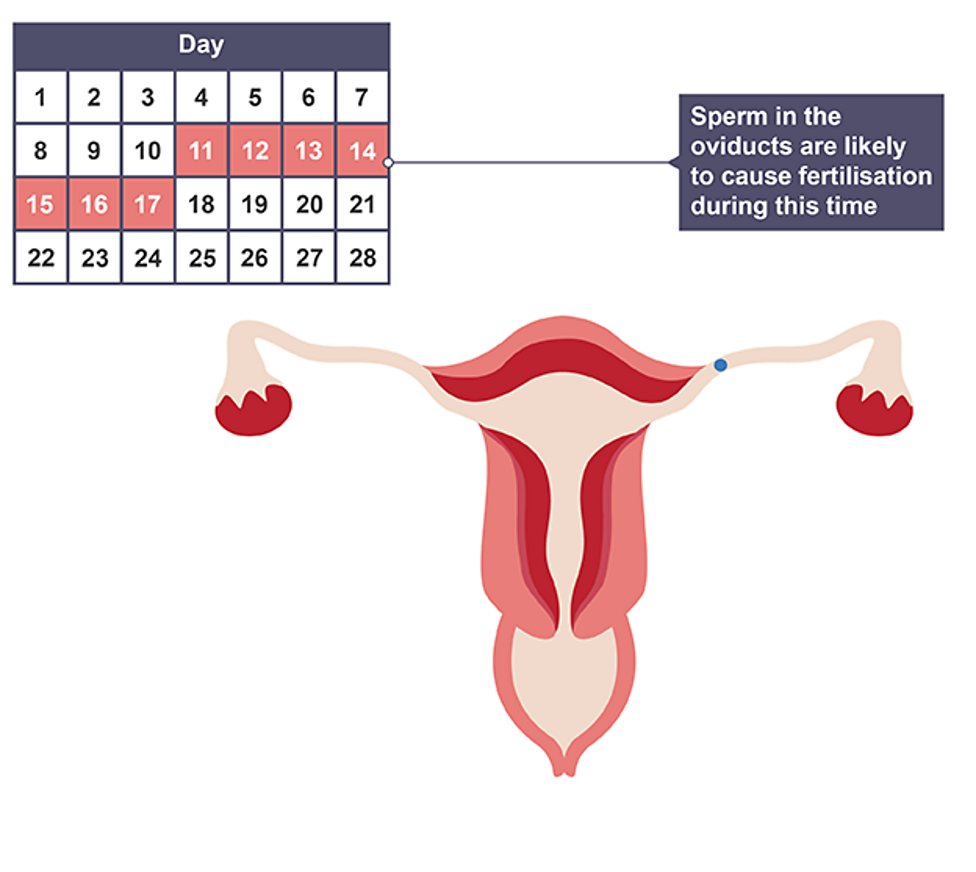
When is fertilisation most likely
Few days before or after ovulation, sperm left in vagina still lives for a few days
Oestrogen
stimulates ovulation and starts buildup/ repair of uterine wall
Progesterone
Continues and maintains buildup of uterine lining
Causes of male infertility
Not enough sperm produced
Non-healthy sperm (can be smoking or drinking)
Impotence
Causes of female infertility
Ovaries don’t produce eggs
Blocked/ twisted oviducts
Complication from previous STI
Uterus lining not developing enough for implantation
Vagina too hostile to sperm e.g too acidic
Treatment for infertility
Fertility drugs
IVF
Fertility drugs
Hormones given to woman which increase egg production and chance of egg being fertilised
IVF - in vitro fertilisation
Fertility drugs given to increase egg production and chance of egg being fertilised
Eggs surgically collected from ovaries and sperm collected
Sperm and egg cells are mixed in a lab
Woman is given hormones to ensure the uterus lining is thick.
Embryos are placed into the uterus
If successful embryo implants into uterus lining
Why several embryos are used in IVF
Higher chance of success, risk of multiple births
Ethical issues of IVF
can be used to screen for abnormalities or selecting characteristics like gender
Why are eggs left over from IVF often frozen
so egg collection process doesn’t have to repeat if first implantation fails or for another child
Contraceptives
Methods used to prevent pregnancy
Mechanical contraception
Male and female condoms
Condoms
Barrier that prevents sperm entering or passing up
Easily obtained and protects against STIs
Unreliable if not used properly
Chemical contraceptives
Contraceptive pill or implant
Contraceptive pill
Taken regularly to prevent ovulation by changing hormone levels
Very reliable
Need to remember and has side effects, doesn’t protect against STIs
Side effects of contraceptive pills
Weight gain, mood swings or increased risk of blood clots
Contraceptive implant
Small tube under skin of upper arm, releasing hormones slowly over time to prevent ovulation
Very reliable, can last up to 3 years
Doesn’t prevent against STIs and can prevent menstruation
Surgical contraceptives
Vasectomy or female sterilisation
Vasectomy
Sperm tubes are cut, preventing sperm entering penis
Virtually 100% reliable
Difficult or impossible to revert
Female sterilisation
Oviducts are cut, preventing fertilisation
Virtually 100% reliable
Difficult or impossible to revert
Natural contrceptives
Rhythm method
Rhythm method
Intercourse is avoided around ovulation
No chemicals used, chosen by those who appose contraceptives for religious or ethical reasons
Not very reliable, especially if cycle is irregular