Exam 3: Diseases of the Bovine Forestomach and Abomasum
1/53
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No study sessions yet.
54 Terms
what is the cause of traumatic reticuloperitonitis
perforation of the reticulum by a metallic foreign body
disease of confined cattle
rarely affects other ruminant species
what are the sequela to foreign body penetratiion
attachment to magment if present
acute inflammaton and mild clinical disease (acute localized perionitis)
chronic localized peritonitis and abscess formation
abscess formation in the thoracic or peritoneal cavity, vagal indigestion, pericarditis, and myocarditis
diffuse peritonitis
what are the clinical signs of acute localized peritonitis
partial or complete anorexia
acute drop in milk production
cranial abdominal pain
pyrexia
tachycardia
tachypnea and decreased depth of respiration
reumen hypomotility
free gas bloat
what are clinical signs of chronic localized peritonitis
subtle signs of abdominal pain
partial anorexia and decreased milk production
decreased fecal ouput
poorly digested feed material
what are the clinical signs of reticulopericarditis
cranial abdominal or caudal thoracic pain
abnormal thoracic auscultation
exercise intolerance
distendied peripheral veins and jugular pulsation
peripheral edema
portal hypertension, ascites, diarrhea
what are the clinical signs of diffuse peritonitis
severe signs that are often fatal
tachy
pyrexia
severe dehydration
diarrhea
profound depression
how does TRP present on CBC
neutrophilia with left shift
nyperfibrinogenemia
elevated plasma protein
how will peritoneal fluid evaluation present with TRP
nucleated cells >6000
total protein >3
>40% neu, <10% eos
what are your ancillary diagnostics for TRP
reticular rads and ultrasound
what findings of TRP are seen on ultrasound
reticular reticular motility
abnormal position or contour
perireticular fibrin or abscessation
localized or generalized abdominal effusion
what defines ruminal tympany aka bloat
not excessive gas production!
failure to reructate via mechanical or functional disturbances
what is free gas bloadt
type 1 vagal indigestion
not a disease itself but a manifestation of an underlying disease
sporadic
usually a single animal
what is frothy bloat
primary disease
ruminal gas trapped as small bubbles within abnormally viscous ingestioa
diet related, seen with legumes, heat or rye grass, high carbs
what are the clinical signs of bloat
asymmetrical abdominal distention in the left paralumbar fossa
abdominal discomfort
respiratory and cardiovascular compromise
severe distention compresses diaphragm and venous return
open mouth breething
death in 30min to 4hrs
what structure can you NOT palpate when it is displaced? when does this change
reticulum
if RAD progresses to volvulus, can be felt again
what is vagal indigestion
a functional or mechanical disruption of forestomach or abomasal outflo
-damage to the vagal nerve
-physical or functional obstruction of forestomach or abomasal outflowdecreased milk production, progressive abdominal distention, altered motility, decreased appetite and fecal output, weight loss
site of distubrance classifes into 1-4
describe the 4 types of vagal indigestionn
type 1- failure to eructate
type 2- omasal transport failure
type 3- abomasal outflow failre
type 4- indigestion associated with pregnancy
describe type 1 vagal indigestion
failure to eructate due to esophageal obstruction or physiological disruption
may be accompanied by signs involving other body systems
distention of the left paralumbar fossa easily relieved by tube
abdominal discomfort
rumen hypomobility
rumen fistula until function returns
what is type 2 vagal indigestion
most common
omasal transport failure
common sequela to TRP
disturbed motility due to neurapraxia or neuritis
may be the result of mechanical obstruction of reticulomasal orifice
what are the signs of type II vagal indigestion
abdominal distention with characteristic papple shape
rumen hypermotility intially
frothy ingesta
bradycardia
L shaped rumen on rectal
anorexia, weight loss, decreased fecal production
gradual decline in milk production
what is type III vagal indigestion
aomasal outflow failure
primary impaction, lymphosarcoma, mechanical obstruction, sequela to abomasal volvulus
what are the signs of type III vagal indigestion
difficult to differentiate from type II
rumen hypermotility, frothy ingesta, and bradycardia inconsistently present
ballottement of impacted abomasum through right body wall
what is type IV vagal indigestion
usually occurs in 3rd trimester of gestation
can present as type II or III
only consistent finding is late gestation
what is the use of clin path for vagal indigestion
most important for differentiating between II and III
CBC and fibrinogen
biochem
rumen fluid analysis
how might CBC present for vagal indigestion
elevated PCV and TP due to hemoconcentration
neutrophilia and hyperfibrinogenemia if associated with TRP
persistent lymphocytosis
how might vagal indigestion present on biochem
metabolic alkalosis
hypokalemia and hypocalcemia
azotemia
hypochloremia consistent with type III
what is the use of rumen fluid analysis for vagal indigestion
rumen chloride >30
MOST important factor for abomasal outflow failure
what ancillary diagnostics can be used for vagal indigestion
reticular rads
reticular and abomasal ultrasound
exploratory laparotomy and rumenotomy
what is rumen lactic acidosis
ingestion of larger than normal quantities of highly fermentable carbohydrates causing increased VFA production and decreased rumen pH
alterations in normal rumen microflora
rumen lactate production decreases pH and increases osmolality of rumen fluid
increased absoprtion of fluid from ECF and endotoxin release into systemic circulation
what are the chemical concequences of rumen lactic acidosis
histamine levels increase
ethanol, methanol, tyramine, tryptamine production contribute to CNS depression
thiaminase production may result in development of polioencephalomylasia
what are the lesions of rumen lactic acidosis
acidic rumen pH damages mucosal surfaces in the forestomach and intestine
blood vessels thrombose and sections of rumen mucosa and submucosa slough allowing bacteria to invade
bacteria travel to liver via portal circulation and cause liver abscesses
mycotic ruminits may develop
what are the clinical signs of rumen lactic acidosis
rumen distention
dehydration
diarrhea
signs of endotoxic shock
anorexia, rumen stasis, abdominal pain
neurologic signs
recumbency and death
how might a rumen fluid analysis present with rumen lactic acidosis
milky grey to yellow, sour smelling fluid
pH <5
no normal protozoa
proliferation of gram + rods
ho does rumen lactic acidosis present on bloodwork
consistent with hemoconcentration
elevated liver enzymes
acidemia
generally describe abomasal ulcers
benetrate the basement membrane of the abomasal mucosa, erosions do not penetrate
clinical presentation based on depth and structures
4 types, though individual animals may have multiple
where are abomasal ulcers most commonly seen
cattle under intensive management such as high producing dairy, feedyard cattle, veal and beef calves
stress
describe type 1 abomasal ulcers
local infmallation with serosal thickening and serositis
often subclinical
up to 50% may not have clinical signs → poor performance, abdominal pain, melena
concurrent disease is common
describe type 2 abomasal ulcers
ulceration over sub-mucosal vessels resulting in significant hemorrhage
hallmark sign is melena
positive fecal occult blood
lymphosarcoma or no lymphosarcoma
what are the clinical signs of non-lymphosarcoma type 2 abomasal ulcers
acute drop in milk production
melena and loose feces
pale mucuos membranes
anemia
describe type 3 abomasal ulcers
perforating areas covered by omentum or those associated with LDA → localized peritonitis, omental bursitis
often identified during investigation of concurrent disease
what is type 4 abomasal ulcers
rapidly occuring
areas not covered by omentum
acute generalized peritonitis
surviors often exhibit chronic clinical signs associated with adhesions
what are the clinical signs of type 3 abomasal ulcers
lack signs specific to perforation
intermittent anorexia
melena
abdominal pain
right cranial abdominal pain
abdominal distention
± fecal occult blood
lab data suggestive of peritonitis
what are the clinical signs of type 4 abomasal ulcers
anorexia
agalactia
depression
signs of shock
pyrexia
abdominal pain
low serum protein in the face of hemoconcentration
how are abomasal ulcers diagnosed
hematology for decreased PCV, TP, erythrocyte count and MCHC
serum pepsinogen , though limited value with unknown parasite status
decal occult blood helpful if melena is not obvious
-low for type 1 ulcers
what factors contribute to abomasal displacement
abnormally high VFA accumulation
hypicalcemia
intra luminal gas accumulation
high producing dairy cows in early lactation
often accompanied by other medical conditions such as metritis, mastitis, and ketosis
describe the hallmark clinical sign of abomasal displacement
the ping
right or left depending on direction of displacement
cranial extent 8-10 ICS
caudal extent cranial paralumbar fossa
ventral extent ½ distalce of abdominal wall
what are other clinical signs of abomasal displacement
fluid splash
depression
complete or partial anorexia
decreased milk production
rumen hypermotility
sunken paralumbar fossa
sprung rib
medial displacement of the kidney and rumen on rectal
signs of accompanying disease such as urine ketones, abnormal uterine fluid, CMT
how does abomasal displacement present on ultrasound
fluid filled viscus between left body wall and rumen
rugal folds
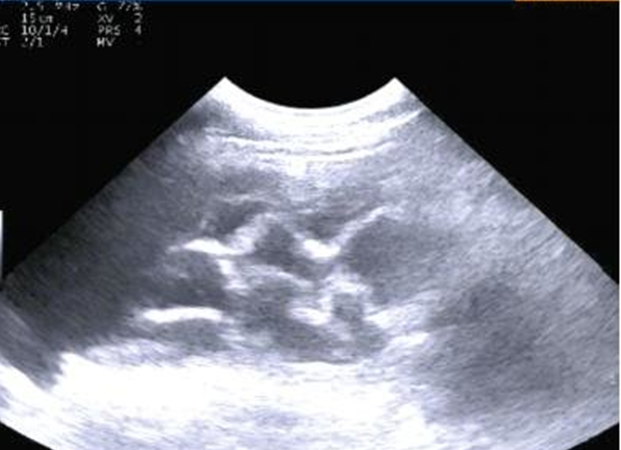
what is important to note abut right displaced abomasum vs left
far less common
signs are similar
SURGICAL EMERGENCY due to likelyhood to develop into volvulus
what is abomasal volvulus
rotation of the abomasum around an axis through the lesser omentum
generally considered a sequela to RDA
not a torsion
rotation most often counterclockwise
obstruction of abomasal outflow
neurovascular compromise
describe the process of an abomasal volvulus
gas accumulates in the abomasum and the pyloric antrum moves dorsally
abomasal body floats dorsally along the right body wall
abomasum and attached structures rotate counterclockwise around an axis through the center of the lesser omentum
any degree of rotation results in neurovascular compromise
what are the clinical signs of abomasal volvulus
right sided ping in 8th ICS to PLF and as far ventrally as the fold of the flank
fluid splash
complete anorexia and scant feces
acute drop in milk production
abdominal pain
absent rumen motility
severe dehydration
abdominal distention
greater curvature palpable per rectum
how does abomasal volulus present on CBC
initially elevated PCV and TP due to dehydration
PCV and TP decrease with compromised abomasal wall intraluminal emorrhage and transudate
how does abomasal volvulus present on chemistry
azotemia
hypochloremia
initial hypokalemia that normalizes
elevated TCO2
evelated anion gap with progression
blood gas will show elevated HCO3, BE and pH