Health and society year 1 (full set - Albie's flashcards)
1/493
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
494 Terms
Consequentialism
Moral based on the consequence of the action.
Deontology
Moral based on the actions adherence to the rules/duties
Virtue ethics
Right act is one a virtuous person would do, that express the virtues such as compassion and honesty.
What is the definition of medical professionalism?
A set of values, behaviours and relationships that underpins the trust that the public has in doctors.
Describe the regulatory role of the GMC?
To protect, promote and maintain the health and safety of the public by ensuring proper
standards in the practice of medicine.
Outline the role of medical schools and the GMC in ensuring students and doctors fitness to
practice?
• GMC sets its guidance for what medical graduates need to accomplish in Tomorrow's
Doctors.
• This is taught by the medical schools.
• This is examined formally in various exams taken throughout the course, reflective
essays, learning to give feedback and self-reflection, attendance and punctuality, plagiarism.
Benefits of good communication?
• More accurate diagnosis.
• More accurate data gathering.
• Increased adherence with treatment regime.
• More effective patient-doctor relationship.
• Increased patient-doctor satisfaction.
Consequences of poor communication?
• Inaccurate diagnosis.
• Less recognition of ICE.
• Non-adherence to treatment.
• Decreased satisfaction with doctor.
• More complaints.
What makes science social?
• Decisions about research funding.
• Pharmaceutical industry - profits.
• Ethical issues.
• Nature of scientific work - communication.
What is eugenics?
• Improving a population by controlled breeding.
• Encourages good genetics, discourages bad genetics.
Issues with eugenics?
• Thinking about the future based on genetics.
• Designer babies.
• Genetic screening - health insurance, employment, and civil liberties.
• Many conditions are polygenic.
What is patient centred care?
Care that is responsive to the wants, needs, and preferences of the patient.
6 criteria of patient centred care?
• Explores patients main reasons for visit. +establishes rapport
• Seek integrated understanding of patients world - looks at the whole person.
• Finds common ground on problem and mutually agrees on management.
• Enhances prevention and health promotion.
• Enhances the continuing relationship between the patient and the doctor.
• Is realistic i.e
How does patient centered care enhance heath prevention/promotion?
allows a doctor to find the methods of health promotion and preventative care which most appropriately match a patient’s world.
What is the sick role?
States the rights and responsibilities for patient and doctors when they have a consultation.
What is the patient expected to do in the sick role?
• Must want to get well as quickly as possible.
• Should seek professional medical advice and cooperate with the doctor.
• Allowed to stop normal activities and responsibilities e.g. work.
• Regarded as being in need of care and unable to get better alone.
What must the doctor do to uphold the sick role?
• Apply a high degree of skill and knowledge.
• Act for welfare of patient, not self interest.
• Be objective and emotionally detached.
• Be guided by rules of professional practice.
Criticisms of the sick role?
• Symptom iceberg - Patients do not necessarily act on symptoms and go see the doctor.
• Chronic illness and MUS - If cause unknown, patients can't enter sick role due to
uncertainty.
• People try to label themselves as sick.
• Conflict between best interests for the patient and cost to society in allocation of
resources.
What 4 sources are used when making a clinical decision?
• Patient preferences
• Available resources (studies)
• Research evidence (guidelines/systematic reviews)
• Clinical expertise (others)
Why is evidence-based decision making important?
• Deals with uncertainty.
• Medical knowledge is incomplete/shifting.
• Patients will receive most appropriate treatment.
• Constant need for innovation and improvement.
• Improving efficiency of healthcare services.
• Reduces practice variation.
What are the sources of NHS funding?
• Tax finance.
• Some user charges e.g. prescriptions, parking
How is the NHS organised?
• Smaller Integrated care boards (ICB's) that are clinically-led statutory NHS bodies responsible for the planning and
commissioning of health care services for their local area
• Public hospitals and GPs - Sellers.
What is flat of the curve medicine?
increased expenditure on healthcare produces no further benefit
What are meta-ethics?
Study of moral concepts, e.g. right and wrong.
What is normative ethics (moral theory)?
Study of the means of deciding what is right and wrong.
What is applied ethics?
Application of moral theory.
What are the 3 main types of moral theory?
• Consequentialism - Moral based on the consequence of the action.
• Deontology (duty based) - Moral based on actions adherence to the rules.
• Virtue ethics - Right act is one a virtuous person would do.
What are the 4 ethical principles?
• Autonomy - Respect the patient as an individual to make choices.
• Non-maleficence - Not permitted to harm patients.
• Beneficence - Act in a way that positively benefits patient (act in patients best interests).
• Justice - Treat people fairly and equitably.
What is the difference between disease and illness? (the 2 agendas)
What is the difference between disease and illness?
• Disease - What is wrong with the body.
• Illness - Looks at the way that the patient experiences the disease.
why is important to address disease and illness
• Disease - Means you treat the correct condition, improves biomedical health.
• Illness - Can discover how illness is impacting patients life, patient more satisfied,
enhances doctor-patient relationship.
What is autonomy?
• Informing patients with capacity to make their own decisions.
• Respecting wishes regarding patients treatment.
What ethical principles should you think about when assessing patients best interests?
• Beneficence - Act to positively benefit patient.
• Non-maleficence - Act in a way as not to harm the patient.
What does it mean to act in a Patient's best interest
Actions that seek to provide an overall benefit for the patient. Takes into account impact on daily life, family, ability to communicate and future implications
What potential difficulties that might occur when assessing best interest? 4
- lack capacity to communicate with Dr
- Dr and Pt views differ
- uncertain future consequences
- weighing up conflicting goods
informal carers
An informal carer is any person, such as a family member, friend or neighbour, who is giving regular, ongoing voluntary assistance to another person without payment.
What is paternalism?
Interference with a patients autonomy of action/information in order to benefit them e.g coercion + witholding info
exceptions to paternalism
- to prevent serious harm e.g psychological distress
- treatment of infants/children who lack capacity
- adults with mental health problems
- when treatment provides no overall benefit
What is coercion?
Persuading patient to do something by force or threats (e.g. forcing to eat).
What is the Bolam test?
Test of negligence, determines standard of care.
Where can you look at disease distribution?
- Globally
- Regionally
- Locally
Why do we need to study populations?
• To find out about risk (diseases, drugs, etc).
• Need to use evidence of what has previously happened to a population to work out how
drugs act, etc.
What is epidemiology?
The study of the distribution and determinants of health-related states or events in specified populations, and the application of this study to the control of health problems.
What are the 3 types of epidemiology?
• Descriptive - Tell us how things are distributed (who, what where when)
• Analytical - Determining factors for the disease?
• Experimental - Tests a hypothesis to conclude things
What is incidence? + formula
New cases of disease within a period
= total new cases/person years
how to figure out person years for incidence formula?
number of people x follow up period
cumulative incidence formula
= total new cases/total initially free of disease
What is prevalence? (+ formula)
Proportion of people with a disease at a particular point in time
= total diseased / total population
How can epidemiology be useful in smoking research?
• Identify cause of disease.
• Guides preventative action - Identifies targets for intervention.
• Surveillance of populations and smoking can measure effects of intervention.
what role does descriptive epidemiology play in medicine?
to characterise patterns to ultimately generate hypotheses on risk factors/causes of disease
What is illness behaviour?
The way in which symptoms may be differently perceived, evaluated and acted upon by different kinds of persons.
illness
a feeling of poor health perceived by an individual
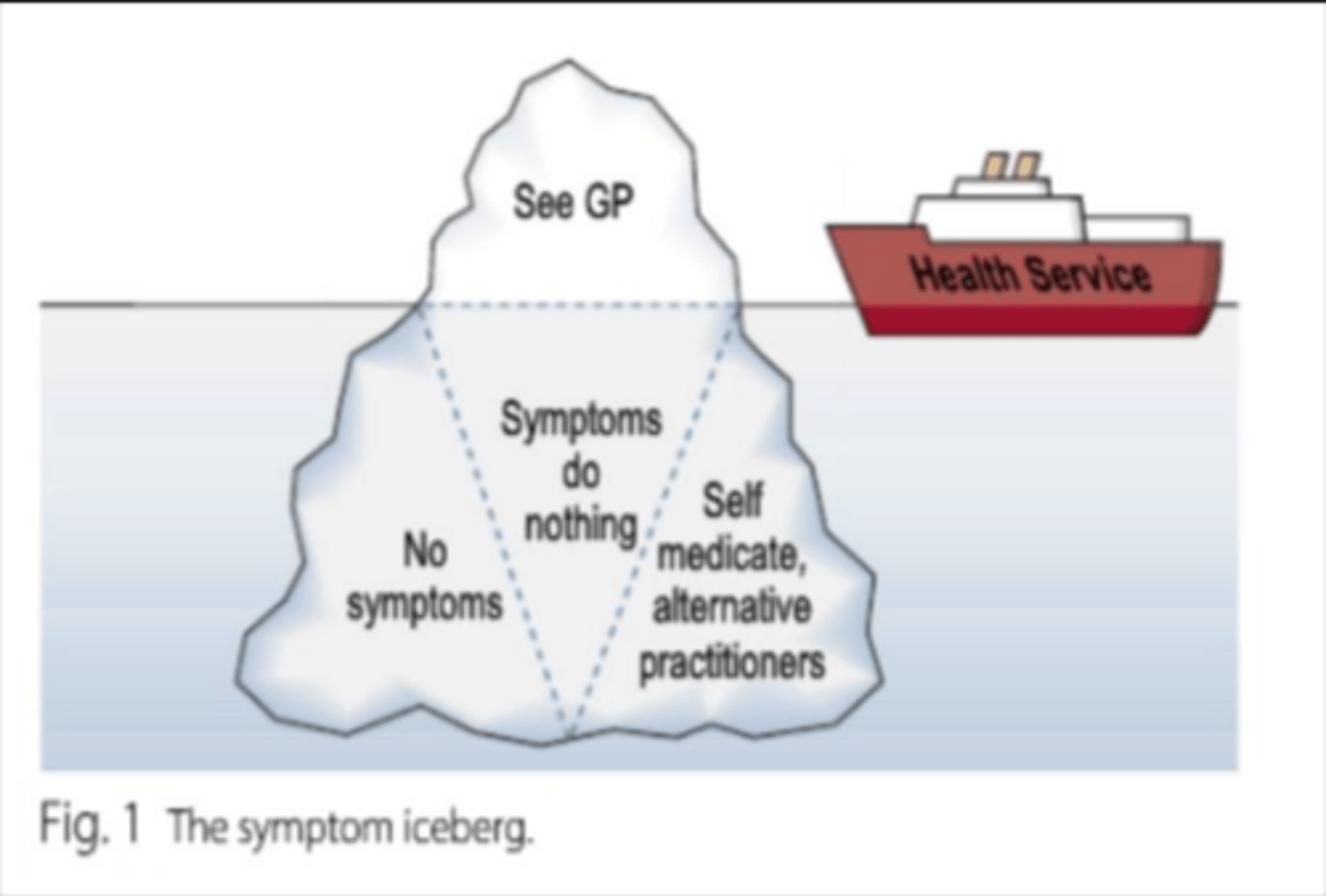
What is the symptom iceberg?
• Only a small minority of symptoms are seen by health professionals.
• Most symptoms managed within community
• Patients only report 5-15% of symptoms.
Who is most healthcare word done by?
Lay people - lay referral system. (community)
What is the lay referral system?
People talk to other people (lay people) before seeking help.
Give examples of lay referral systems?
• Friends
• Relatives
• Pharmacists
• Magazines
• google (80% of people use - FAKE NEWS?!)
What demographic/social factors influence help seeking and illness behaviour?
• Gender
• Age
• Social class
• Race
• Culture
(pretty much everything)
An example of gender influencing illness behaviour?
studies suggested men less likely to seek help from health professionals
An example of age influencing illness behaviour?
studies suggested individuals over 51 more likely to have screening health checks than those younger
Problems with delaying help seeking?
- reduces opportunity for early diagnosis/intervention
- impacts outcomes for both acute/chronic disease
medical pluralism
the adoption of more than one medical system in terms of health beliefs, behaviours, treatments, or institutions
e.g combining biomedicine with traditional/alternative medicine
3 examples of complementary and alternative medicine (CAM's)
• Aromatherapy (aromatic oils)
• Acupuncture (needles)
• Homeopathy (microdoses)
What are Zola's triggers to help seeking behaviour?
• Interference with work or physical activity.
• Interference with social relations.
• Interpersonal crisis e.g. death in family.
• Putting a time limit on symptoms.
• Sanctioning - relative/friends tell them to seek help.
What influences health seeking behaviour?
• Lack of awareness of symptoms e.g indigestion as MI
• Perception and evaluation of symptoms (not severe enough)
• Perceived risk.
• Confirmation from others
• Previous experience.
• Psychological factors - Fear of what it might be.
• Denial.
• Concern about using NHS resources.
What barriers are there to help seeking?
• Provision and availability of services.
• Car ownership, transport cost, availability.
• Disruption to work.
• Attitudes of staff - Previous bad experience.
• Inverse care law - Better off areas get better health provision that poorer areas.
• Geographical distance.
• Perception and evaluation of symptoms (e.g., Afraid that it was serious)
• Time, effort.
• Childcare
• Denial
• Long waiting times.
• Language barrier
What is health promotion?
The process of enabling people to increase control over, and to improve, their health.
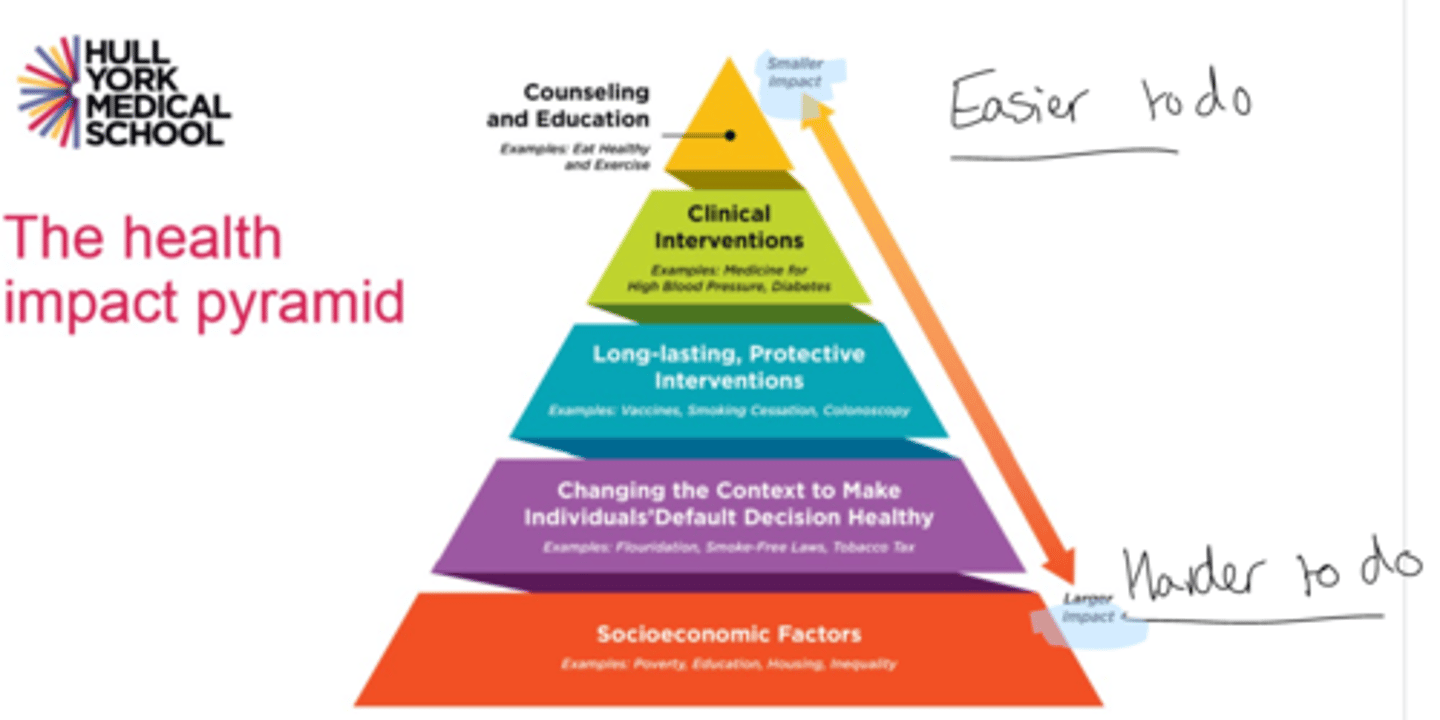
Health Impact Pyramid
upper portions easier to do but have a lesser impact and vice versa
What are WHO's 5 aspects of health promotion?
• H - Healthy public policy.
• A - Action in the community.
• R - Re-orientating health services.
• P - Personal skills.
• S - Supportive environment.
What are the 3 different approaches to health promotion?
Individualistic - encouraging individual responsibility and action
Collective/societal - educates groups on preventative health
Governmental - new legalisation to protect/improve health
3 examples of health promotion (success, easy?, hard to solve)
Success - Cot death (sudden infant death syndrome) was drastically reduced due to health campaigns "back to sleep"
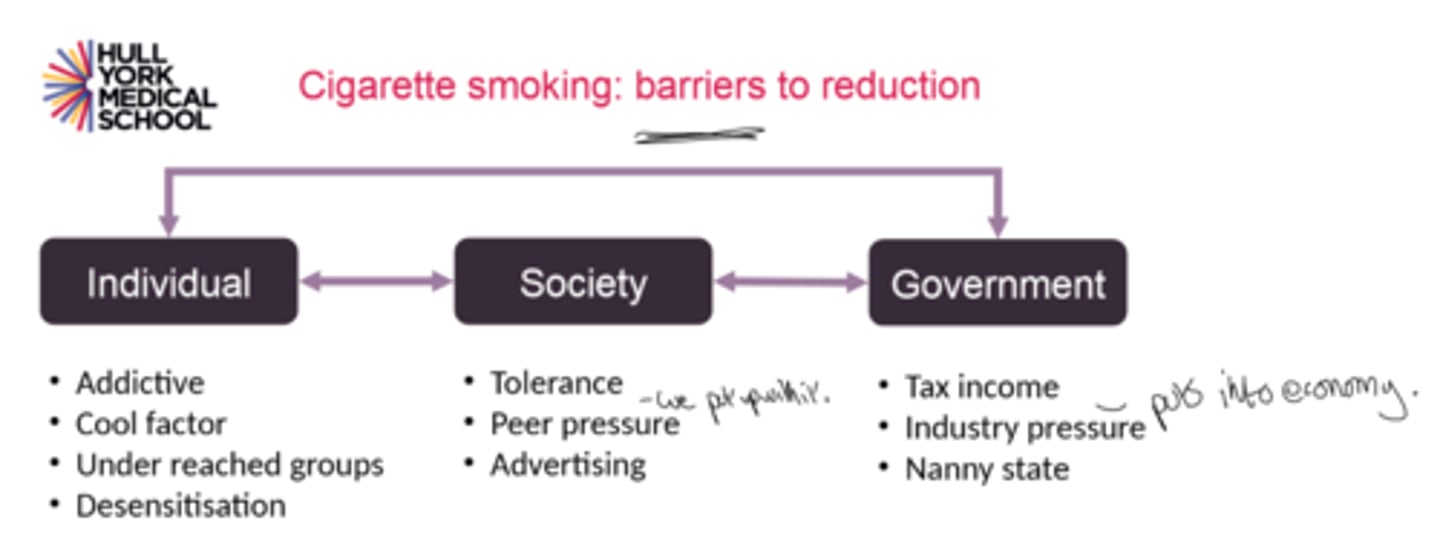
Easy? - smoking not as easy due to barriers to reduction e.g cool factor, tolerance of society, tax income putting into economy
Hard - obesity hard to solve due barriers e.g desensitisation/victimisation
What is primary health prevention?
• Aims to prevent onset of disease.
• Screening risk factors.
• Health protection.
• Health education.
What is secondary health prevention?
• Detect and cure disease at early stage.
- E.g. cancer screening.
What is tertiary health prevention?
Minimise the effects or reduce the progression of irreversible disease.
What is health persuasion?
the process of influencing an individual's attitudes, beliefs, and behaviors related to health
• Includes mass media campaigns, such as sexual health and health eating.
- For example, 5-a-day TV campaign.
How is personal counselling involved in health promotion?
• Opportunistic prevention in consultations.
- For example, working with dietician on food.
What is health protection?
• Legislation to protect public health.
- Includes seat belts, restrictions on smoking in public.
What is prevention paradox?
A preventative measure which brings much benefits to the population but offers little to each participating individual.
e.g cigarette tax
What is advocacy for health?
A combination of individual and social actions designed to gain political commitment, policy support, social acceptance and systems support for a particular health goal or programme.
What is empowerment for health?
In health promotion, empowerment is a process through which people gain greater control over decisions and actions affecting their health.
What is enabling?
In health promotion, enabling means taking action in partnership with individuals or
groups to empower them to promote and protect their health.
What is health literacy?
Health literacy represents the cognitive and social skills which determine the motivation and ability of individuals to gain access to, understand, and use information in ways which
promote and maintain good health.
What are social inequalities in health?
Differences in people's health linked to social inequalities in their lives.
health inequities
the unfair and avoidable differences in health status arising from poor governance, corruption or cultural exclusion.
social determinants of health
The conditions in which people are born, grow, live, work, and age, shaped by the distribution of money, power, and resources at global, national, and local levels

3 intermediaries between social factors and health outcomes
1. Material - stuff you have e.g house, car, food
2. Psychosocial - the stressors/emotional wellbeing
3. Behavioural - eating, smoking, alcohol consumption
What did the black report show? (1980)
• Confirmed social health inequalities are involved in mortality and the extent of this
• Shows health inequalities were widening, despite general improvement
• recommended increasing child benefit, introducing minimum wages + improving housing
How do childhood circumstances influence inequalities?
• Childhood is a period of rapid development and heightened sensitivity to environmental
influences.
• Father's occupation at birth is a strong indicator of life expectancy.
Name some government initiatives to help reduce child poverty?
• Raising National minimum wage.
• Increase child benefit.
• Increase income support.
• Teenage pregnancy strategy.
• Supporting families into work and increasing their earnings
• Providing free school meals to all infant school children
Why has child poverty increased?
• Unemployment/part-time work.
• Lower pay.
• Rising prices of food/necessities
• More single parent families.
• Freezing or abolition of some benefits
• government cuts
• More indirect taxation.
• economic inflation
What is in the marmot report 2010? (4)
• Shows life expectancy has stalled in UK
• People living in deprived areas spend most of their (shorter) lives in poor health
• Funding cuts have worsened inequalities
• urgent health improvement needed in north
Inverse care law
The availability of good medical care tends to vary inversely with the need of the population served
inclusion health
services, research or policies that work to redress inequities by supporting specific vulnerable groups e.g homeless, migrants, sex workers
What is culture?
System of knowledge, experience, belief, attitudes, meanings, signs, and symbols
shared by a group of people
socioeconomic status (SES)
Defines the economic and social position of a person in terms of income, wealth, education, and occupation
What is enculturation?
Process of learning your own group's culture.
What is acculturation?
Process of taking on another groups culture
Why do people self care?
• Many people will self treat before seeing a doctor.
• Many cultures have strong non-western medical traditions.
Why are CAMs (complementary and alternative medicine) used?
• Easily accessible, cheap
• own control over treatment.
• Dissatisfaction with health care.
• Poor doctor-patient relationship.
• Desperation.
• Perceived effectiveness and safety.
What is diagnosis?
Determining the nature of a disorder by considering the patient's signs and symptoms, medical background, and test results.
What is prognosis?
Assessment of future course and outcome of patients disease based on knowledge of similar patients together with the pt's health, sex and prognostic factors
Why is prognosis important? (3)
• It can help diagnostic and treatment decisions.
• It is important for patients to know the likely course of their disease.
• Helps discussing opinions of patients