Cervical Spine
1/87
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
88 Terms
T/F mobility > stability in the cervical spine
T
how many degrees of flexion is the OA joint responsible for?
15-20º
how many degrees of rotation does AA joint do?
50º, >50º may lead to kinking of contralateral vertebral a.
the orientation of facet joints facilitate what movement?
flexion/extension
face joints move by _____.
gliding
what innervates the facet joints?
dorsal ramus of exiting spinal nerve
greatest ROM occurs between what 2 vertebrae? degeneration is most likely between what vertebrae? what is resting position of cervical spine? closed pack position?
ROM greatest at C5-C6
degeneration most likely C4-C5-C6-C7
resting position: slight extension
CPP: complete extension
the IV discs make up __% of the height of the C-spine and give it its _____.
25, lordosis
what does the annulus do? is it innervated?
withstands tension in disc
nucleus has not innervation, outer annulus has some innervation
what is the uncinate process
vertical projection
T/F the facet joints bear a significant amount of weight
F, minimal; a small amount of weight bearing can lead to spondylotic changes
what protects the spinal cord? what are the attachment points for muscles? what is the first palpable spinous process?
vertebral arch
spinous processes and transverse processes
C2
what are common outcome surveys for C-spine?
pain
Neck Disability Index
Fear Avoidance Behavior Questionnaire
what is the MDC and MCID for numeric pain rating scale?
MDC - 2.1 is the amount of change needed to be considered to exceed measurement error
MCID - 1.3 is the smallest difference that patients perceive as beneficial
what is the most studied outcome measure for neck? what is included in it?
Neck Disability Index
10 items - 4 pain related, 4 ADLs, 2 personal care
what are the 5 D’s and 3 N’s for cervical ischemia?
signs of cervical ischemia
dizziness
drop attacks
dysarthria
dysphagia
diplopia
nausea
nystagmus
numbness
what are subjective considerations?
dizziness blackouts or drop attacks
any history of RA - can lead to ligament laxity and cervical instability problems
any neurological sx in LE’s
what are red flags?
cervical myelopathy
neoplastic conditions
upper cervical spine instability
vertebral artery insufficiency
inflammatory of systemic disease
what is the most common inflammatory disorder to affect the cervical spine?
RA, associated with upper c-spine instability and subluxation of the atlas on the axis
what are signs of cervical instability?
severe muscle spasm
reluctance to flex cervical spine
lip of facial paresthesia
dizziness-nausea-vomiting
nystagmus and pupil changes
lump in throat
what is the Sharp-Purser test?
tests the integrity of the transverse or cruciform ligament to determine subluxation of the atlas on the axis
pushing occiput, + if it releves pain
alar ligament test
tests stability of atlanto-occipital junction
should feel spinous process moving opposite direction of where you move head
what is vertebrobasilar vascular insufficiency (VBI)? most common sx? how to test for this?
restriction of blood flow through vertebral arteries, most common cause of sudden onset VBI is trauma (whiplash)
most common sx is pain in the head and neck often unilateral and suboccipital
passively hold rotation position of 10 sec, + if sx appear
subjective patient history
age (spondylosis or spondylotic disease risk)
severity - MOI/insidious (posture if insidious), constant/intermittent, improving/worsening, onset time?
occupation - standing, walking, bending etc., leisure/sports/hobbies
boundaries of pain - neck, arm, interscapular region, C4 and above no arm sx, cervical radiculopathy or myelopathy
radiation of pain - dermatome sensory testing, pain type, pain when coughing/sneezing, paresthesia (pins and needles)
headaches - location, frequency, intensity, duration, relief. often due to upper c-spine
gait deviations and balance - dizziness (semicircular canals or vertebral a.), SNS, CN
sx - aggs/eases, disturbed sleep, sleeping postures, pillows, improving/worsening?
previous history - year of first episode, past tx, mx hx, meds, surgery, accidents, imaging, red flag q’s
where is spondylosis seen in patients?
25 years and older
60% of people >45 years
85% of people >60 years
where does spondylotic disease most commonly occur?
lower cervical spine
cervical radiculopathy vs myelopathy
radiculopathy - injury to nerve roots muscle weakness (myotome), sensory alteration (dermatome), reflex hypoactivity
myelopathy - injury to spinal cord spastic weakness, paresthesias in LEs, proprioceptive and sphincter dysfunction
when to send someone in for imaging
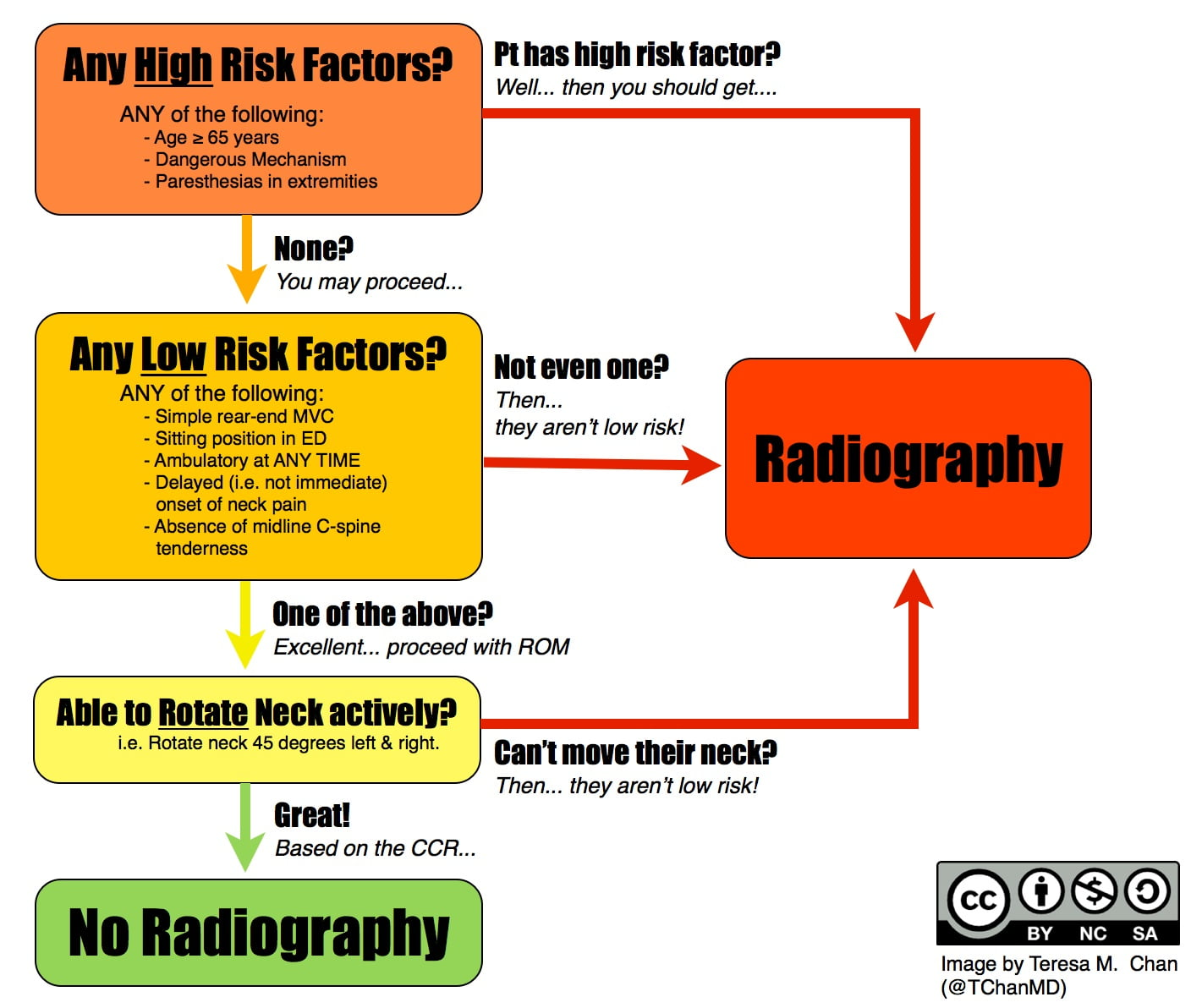
objective
observation/posture
shoulder and thoracic clearing
ROM - active/passive/resistive
compression/distraction
neuro screen
accessory motion
what should you observe in objective exam inspection?
observation of general body posture and willingness to move
resting level of sx baseline
initial view is global then sx area
sitting - standing
do they shift head away from midline
what is tight/short and weak in cervical upper spine syndrome (Vladimir Janda)?
tight/short: pec major and minor, upper traps, levator scap, SCM
weak: lower and middle traps, serratus anterior, rhomboids, deep neck flexors
what to observe in posture posteriorly?
lateral shift, tilt, acromial and scapula heights, scoliosis, muscular size and atrophy/hypertrophy
what to observe in posture anteriorly?
shift, list, muscular size, atrophy/hypertrophy, torticollis
what to observe in posture laterally?
sagittal plane position of head, dowager’s hump (excessive kyphosis), thoracic kyphosis
what are some causes of postural deformities? why is it important to know this?
protective - voluntary/involuntary
non-protective - structural
non-protective - behavioral
identification of postural deformity directs clinician to hypothesize cause and assess adaptive/assistive devices
what should you observe in skin?
trauma and wound healing
incisions - scars
skin color - inflammation, cyanosis, redness
red streaks - infection
tropic changes - PVD
what to observe in active motion testing?
resting level of pain
baseline, sx, quality
ROM
guarding, deviation, crepitus
pain during and after
repeated motions
what to do if full AROM is pain free?
PROM overpressure at end range to establish end feel and stress tissues sufficiently to rule out c-spine
what is flex ROM values? how much larger do the IV foramen expand?
80-90º; up to 2 fingers width
20-30% larger with flexion
what is extension ROM? what could be possible problems if there is no anatomical block? what should you be aware of?
normal is 70º, nose and forehead are nearly horizontal
if there is no anatomical block, reasons for problems could be whiplash or cervical strain
be aware of VBI sx
what is normal side flexion ROM? where does it most occur at (vertebrae)? what to be aware of?
20-45º
most occurs at occiput and C1 and C1-C2
be wary of altered motion like couples rotation or flexion
rotation normal ROM? what to be aware of?
70-90º
SB and rotation are coupled movements and cannot occur alone, rotation and SB occur same side
note extension and SB compensatory movements (VBI sx)
what is the capsular pattern of the cervical spine? what are causes of noncapsular patterns?
lateral flexion and rotation equally limited, extension is limited, flexion is full range and painful
ligamentous adhesions, internal derangements and extra-articular lesions
what are resisted isometric movements? how do you measure it?
same movements that were tested actively, many therapists do not check RROM
measured as strong/weak, painful/painless
what are the cervical myotomes of RROM?
neck flexion: C1-C2
neck side flexion: C3
shoulder elevation: C4
shoulder abduction: C5
elbow flex and wrist ext: C6
elbow ext and wrist flex: C7
thumb ext and uln dev: C8
abd and add hand intrinsics: T1
what is the valsalva test? + test?
moderately reliable and specific for patients with cervical radiculopathy
hold breath and bear down
+ is reproduced sx
what is the shoulder abduction test?
moderately specific, not good screening; unlikely to identify level of cervical radiculopathy
assess sx in sitting
pt actively places hand on top of head
+ is reduction of pain
what is the shoulder depression test?
brachial plexus test
apply compressive force with hand above clavicle on sx side
+ reproduction of radicular sx, unlikely that this test could discriminate b/w radiculopathy and TOS
compression test
narrowing of neural foramen, pressure on facet joint or muscle spasms can cause increased pain on compression, may reproduce radicular pain from cervical spine
sitting apply compression upon the top of the head
if pain note exact distribution of neck or UE
Jackson and Spurling’s tests
Jackson test: apply compression with head rotated to the side of sx, + if produces radicular pain in UE
Spurling’s test: position narrows the IV forman, pt’s head is placed in lateral flex prior to axial compression
Spurling’s has moderate to high specificity for identifying pts with IVF stenosis with referred sx
T/F PROM is greater than AROM in supine
T
what is supine lateral flexion PROM normative values?
75-80º due to relaxation of muscles holding up head
why do muscle length testing? how do you do it?
muscles attaching to the cervical spine and associated structures may cause limitation in ROM and pain
assessing muscle length may help plan tx program
all muscle length tests are done bilaterally for comparison
cranial cervical flexion test
for forward head posture - overuse of platysma, hyoid muscles and SCM
decreased activation and endurance of deep cervical flex m, rectus capitis, ant and lateralis, longus colli and longus capitis
the pressure that pt can hold steady with minimal substitution of superficial muscles is the one that you measure endurance
what is passive intervertebral motion assessment (PIVM)?
provides extent of available PROM, irritability of tissue
accessory motion tests
anterior-posterior glide
specific mobs
anterior glide - PA central vertebral pressure
above mob segment if extension, below is flexion
posterior anterior unilateral pressure
produces minimal rotation of cervical spine, assess response of sx
distraction test
traction force is applied when pt is in sitting or supine, + test is reduction of sx
has good specificity
ULTT
+ ULTT is most likely with nerve root compromise from lateral foraminal stenosis
test good side first, position first shoulder, forearm, wrist, fingers, then elbow last; each phase added until sx are produced
maintain constant depression force on shoulder!
what is a contraindication for ULTT?
cauda equina or SC lesion
the median nerve tension test has a strong association with?
cervical radiculopathy
what is equivalent to the SLR in lumbar spine for the UE?
ULTT
positioning for ULTT of median nerve, anterior interosseous nerve C5, 6, 7?
supine legs straight
scap depression, shoulder abd 90-110 with elbow flexed, forearm sup, wrist/finger ext, shoulder lat rot, elbow exxt, contralateral cervical side flex
sensitivity: 22%, specificity: 97%
where are articular pillars located?
where lamina meets pedicle
what muscle divides the neck into anterior and posterior triangles?
SCM
what are the types of cervical pathologies?
radiculopathy
spondylosis/DDD
facet syndrome
myelopathy
sprain/strain - whiplash associated disorder
is radiculopathy UMN or LMN? sx?
LMN - hyporeflexia or absent DTR’s
decreased sensation dermatomal pattern, muscle weakness following myotomal pattern, biceps reflex diminished increases the changes of cervical radiculopathy from 23% to 59%
what is affected in radiculopathy? what is the most common MOI? common complaints?
nerve root
could be compressive or non-compressive etiology, commonly compressive from spondylosis and disk herniation
reports of numbness, tingling, weakness
myotomes
C5 - lateral forearm
C6 - distal thumb
C7 - distal middle finger
C8 - distal 5th
T1 - medial forearm
what is cervical spondylosis? what could it lead to? what causes it?
general term for nonspecific degenerative changes of the spine
may be the cause of cervical canal stenosis
aging
degenerative changes of discs, facets, vertebral bodies, uncovertebral joints resulting in loss of curve
what is DJD? common sx? what is DDD?
primary findings are bone subchondral sclerosis, joint space narrowing, lipping or spurring
common characteristic is morning sx that lessen throughout the day
DDD: degenerative disc disease, can occur without DJD, and vice versa
what does cervical disc disease entail?
dehydration, fibrosis, mechanical incompetence of the disc
disc height diminishes increasing load on bones and joints
nucleus functions to reduce compression force and annulus functions to withstand tension in the disc
how many facets in c-spine? what are they innervated by? what is facet syndrome?
14 facet joints in c-spine, orientation facilitates flexion and extension, move by gliding and greatest ROM occurs between C5 and 6
innervation: dorsal ramus of exiting spinal nerve
evidence supports these joint capsules can be the source of local and referred pain
what is myelopathy? what increases risk? how does onset present?
compression, most likely to occur at C5-6 level, can lead to spinal cord disease
congenital narrow canal increases risk, usually narrowing of the spinal canal is the end point of degenerative changes
onset is usually gradual and sx may be present in multiple extremities
sx of myelopathy?
LE sx with no history of lumbar dysfunction
loss of muscle tone and decreased girth measurements
ataxia and loss of dexterity with fine motor skills
muscle weakness, hyperactive reflexes, decreased sensation
reports of multiple dermatomal or myotomal weakness
common signs of UMN pathology (myelopathy)?
hyperreflexia UE or LE
sensory changes that are nondermatomal
clonus ankle, Hoffman, Babinski reflex
clumsiness in gait, generalized weakness
cervical spine strain and sprain? MOI?
for conditions that do not fit a particular diagnosis, should refer to a condition where a ligament has been sprained or a muscle strained
may arise from poor posture, may follow performing hard task, sleeping in awkward position, poor ergonomic environment at home or work; whiplash
after trauma, a decreased willingness to move the head could be red flag for?
upper cervical spine instability
neck pain CPG
neck pain with radiating pain
neck pain with mobility deficits
neck pain with movement coordination impairments
neck pain with headaches
neck pain with radiating pain sx
radiating pain into UE
dermatomal/myotomal deficits
neck pain with radiating pain exam findings
cluster findings: ULTT median nerve, distraction test, Spurling’s test, <60º cervical rotation to involved side
all 4 + is 99% specificity
any 3 + is 94% specificity
helps with clinical dx of cervical radiculopathy
neck pain with mobility deficits sx
central and/or unilateral neck pain
decreased cervical ROM and reproduces pt sx
may have referred pain to shoulder girdle
neck pain with mobility deficits exam findings
decreased C/T mobility, accessory motion
pain reproduced with provocation testing (PA mobs)
may see scap mm strength/motor control deficits
neck pain with movement coordination impairments (WAD) sx
MOI of trauma or whiplash
may have referred pain to shoulder girdle or UE
may have concussion sx
dizziness/nausea
HA, concentration or memory difficulties, hypersensitivity to light, sound, temperature, heightened affective stress
neck pain with movement coordination impairments (WAD) exam findings
+ CCF test
+ neck flexor mm endurance test
+ pressure algometry
neck pain in mid-range that can worse at end-range
myofacial trigger points
altered movement patterns, balance, posture
pain with provocation testing
neck pain with headache sx
noncontinuous unilateral neck pain and associated HA
HA aggravated by neck movements or sustained postures/positions
neck pain with HA exam findings
+ CCF test
HA reproduced with provocation testing of upper C-spine
limited cervical ROM
restricted upper cervical mobility with mobs
strength, endurance and coordination deficits of neck mms