week 7 part 1
1/87
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
88 Terms
chapter 4!!!!!!!!
what is the receptor of proprioceptive information
cerebellum
sensory cortex is composed of…
primary sensory cortex (S1) → where sensory information from the outside enters by way of the spinal cord and brainstem
secondary sensory cortex (S2) → analyses shape, location in space and movement
tertiary sensory cortex/ parieto-temporo-occipital association area (S3) → links sensory information to visual or auditory information → links to events from the past to form a concept
!! not only sensation but also other sensory modalities enter there
secondary sensory cortex vs somatosensory association area???
based on information that enters the sensory cortex, movement is initiated or continued by the…
more frontally situated premotor cortex
prefrontal association cortex (M3)?????
where motor action is planned on the basis of complex information from the sensory areas
signals conveyed from S3 to M3 are usually also influenced by the…
emotional limbic system
secondary motor cortex/supplementary motor area (M2)
has to prepare movement in such a way that the correct muscle groups are used properly
directly influences the spinal cord
if the movements are already familiar through experience and practice, the brain can predict what will happen so it uses existing motor programmes = feedforward
feedback is when a movement is initiated and then adjusted according to the result
basal ganglia
basal nuclei/ganglion are located below the cortex on both sides of the hemispherical midline
consist of the caudate nucleus, putamen and globus pallidus
→ caudate nucleus + putamen = the neostriatum/striatum
→ putamen + globus pallidus = the lenticular nucleus (lentiform nucleus)motor function of the basal nuclei together with the mesencephalon is regarded as separate from the pyramidal tract system = extrapyramidal system (but even though the cerebellum for example is situated outside the pyramidal tract system, it is not seen as part of the extrapyramidal system)
motor function of young children is initially controlled by the extrapyramidal system, while myelination of the pyramidal tracts continues for years after birth
occupy a key position because they receive input from virtually the entire cortex as well as the brainstem
BUT the spinal cord does not directly send information to this system which means that the basal nuclei play only a minor role in external feedback from initiated movement
As movement becomes less automatic and more planned, the prefrontal cortex (M3) and higher sensory areas (S2 and S3) increasingly come into play in motor function. The basal nuclei are also involved in this process, since they send information about planned voluntary movement from M3 to M2. A great deal of information is exchanged with M2, showing the control function of the basal nuclei
associated with a variety of functions, including regulating voluntary motor movements, procedural learning, habit formation, conditional learning, eye movements, cognition and emotion
supply M2 with existing practiced motor programmes and preparing those planned in M2 (?)
also uses internal feedback with M2 → tests the scheme before the movement is initiated
(cerebellum also uses internal feedback with M2 → assesses the efficiency of a motor function before movement is initiated)its dysfunction is seen in parkinsons
important pathways to and from the basal nuclei
Important pathways to and from the basal nuclei . Th thalamus, NC caudate nucleus , Pu putamen , S2 secondary sensory cortex , S3 tertiary sensory cortex , M2a supplementary motor cortex , M2b premotor cortex , M3 prefrontal cortex
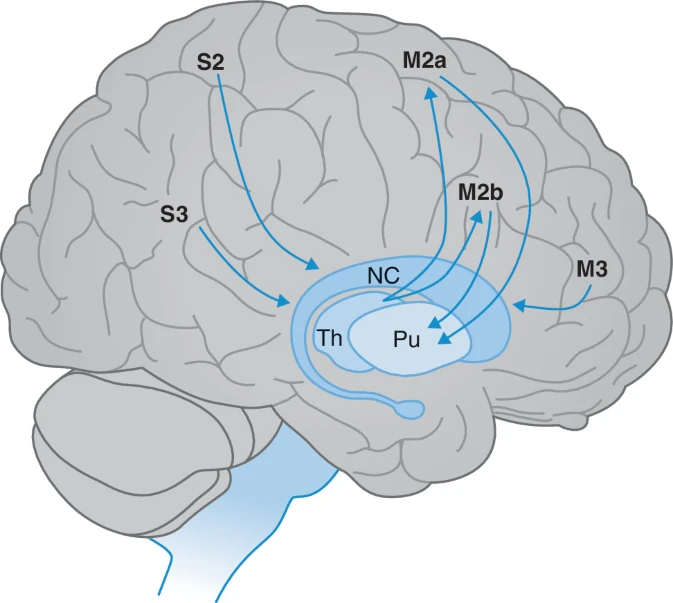
motor function of young children is initially controlled by…
the extrapyramidal system, while myelination of the pyramidal tracts continues for years after birth
As movement becomes less automatic and more planned, the prefrontal cortex (M3) and higher sensory areas (S2 and S3) increasingly come into play in motor function. The basal nuclei are also involved in this process, since they send information about planned voluntary movement from M3 to M2. A great deal of information is exchanged with M2, showing the control function of the basal nuclei
the … and … have a ‘consultative function’ for M2
basal ganglia and cerebellum
statement: cerebellum → internal and external feedback among other things
direct and indirect pathways from the basal ganglia
think of these pathways are response systems (?) not pathways that directly cause motor movement
direct pathway
from the striatum to the globus pallidus then 2 pathways
globus → substania nigra → thalamus
globus → thalamus
thalamus → motor cortex → spinal cord
activates/disinhibits the thalamus
indirect pathway
from the striatum via the globus pallidus (each doesnt synapse (?) there) to the subthalamic nucleus to the thalamus
thalamus → motor cortex → spinal cord
photo doesnt make sense with ^
inhibits the thalamus
!! direct and indirect pathways thus have an opposite effect on motor function, and disorders causing motor defects can generally be explained in terms of an imbalance between these direct and indirect thalamocortical circuits
eg. hyperkinetic disorders such as chorea can be explained as a relative overactivity of the disinhibiting direct system
hypokinetic disorders such as parkinsonism are caused by relative overactivity of the inhibiting indirect system
parkinson’s → malfunction of the dopaminergic cells in the substantia nigra (part of the direct pathway) causing degeneration of nigrostriatal pathways = direct system
sterotactic surgery can improve extrapyramidal motor disorders → the subthalamic nucleus is stimulated in patients with Parkinson’s disease , causing the indirect system to be inhibited
wait so they stimulate the indirect system to INHIBIT it???
but not all motor defects right? only central ones
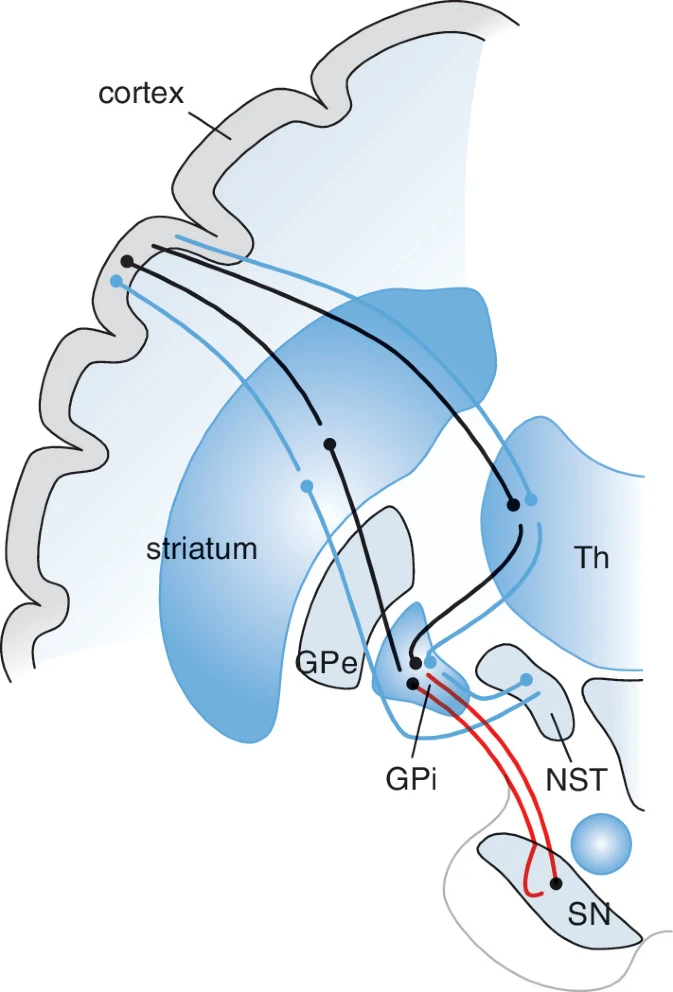
parkinson’s is a malfunction of the…
dopaminergic cells in the substantia nigra (part of the direct pathway) causing degeneration of nigrostriatal pathways = direct system
… surgery can improve extrapyramidal motor disorders
stereotactic surgery
eg. in parkinson, the subthalamic nucleus is stimulated in patients with Parkinson’s disease, causing the indirect system to be inhibited
all information from the basal nuclei to the cortex is transmitted via the…
thalamus
function of thalamus*****
descending motor pathways for posture and balance
the rubrospinal, reticulospinal, vestibulospinal and tectospinal tracts are more under the influence of the basal nuclei (unlike the pyramidal tract) = bulbospinal pathways
bulbospinal pathways → regulate axial and postural motor function and tone
recall that a majority of the pyramidal tract (lateral) decussates and influences the distal musculature
but a small part of it (anterior/medial) does not decussate, instead it branches off at its destination in the spinal cord and influences both sides of the body and mainly the proximal muscles of the trunk and limbs → responsible for posture and balance
the rubrospinal tract is similar to the lateral pyramidal tract in terms of its anatomical course and function
the other pathways are more similar to the medial pyramidal tract, and play an important role in axial and postural motor control
the red nucleus is…****
a part of the brain where the rubrospinal tract (only?) synapses at
tracts:
afferent: corticorubral, cerebellorubral
efferent: rubrospinal, rubroolivary tracts
which bulbospinal tract follows the same anatomical course and function as the lateral pyramidal tract
rubrospinal tract
does the pyramidal tract decussate
most of it (the lateral part) does, but the anterior/medial part doesnt
anterior/medial vs lateral pyramidal tract
recall that a majority of the pyramidal tract (lateral) decussates and influences the distal musculature
but a small part of it (anterior/medial) does not decussate, instead it branches off at its destination in the spinal cord and influences both sides of the body and mainly the proximal muscles of the trunk and limbs → responsible for posture and balance
symptoms in basal ganglia diseases
defects in an extrapyramidal neuron circuit cause loss of function other than damage to the primary motor cortex and the pyramidal tract
symptoms include too much (hyperkinesia, dyskinesia) or too little (hypokinesia) spontaneous movement, and difficulty initiating or sustaining movement (akinesia)
but no paresis
muscle tone is elevated but in a different way than in the case of CMN impairment, recall that it causes rigidity rather than spasticity
problems with movement must be caused by defects in a subcortical circuit of the basal ganglia, whereas abnormal muscle tone is mainly caused by impaired output via the systems descending from the extrapyramidal system to the spinal cord
unilateral defects → symptoms in the contralteral half of the body due to disturbance within the subcortical pathways between the cerebral cortex, basal ganglia and red nucleus
proximal motor functions are influenced on both sides, in principle, due to the other descending tracts from the brainstem to the spinal cord that are influenced by the extrapyramidal system and have a bilateral influence on motor function
problems with movement vs abnormal muscle tone when it comes to the basal ganglia
problems with movement must be caused by defects in a subcortical circuit of the basal ganglia, whereas abnormal muscle tone is mainly caused by impaired output via the systems descending from the extrapyramidal system to the spinal cord
hyperkinesia**********
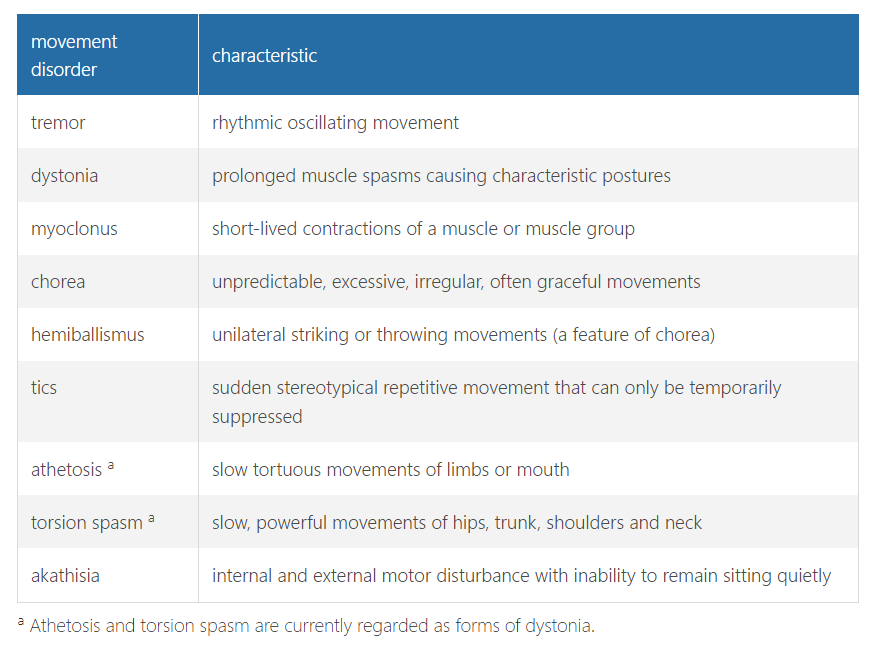
impairments affecting speed of movement and automaticity**********

hyperkinetic disorders
= tremor, dystonia, myoclonus, chorea, tics etc
can be (not always) caused by abnormalities in the basal nuclei
tremor:
classified according to frequency, amplitude and the circumstances under which it occurs, eg.
unilateral resting tremor → consistent with Parkinson’s disease
bilateral action tremor→ consistent with essential tremor
tremor that increases as the target is approached → usually an intention tremor, consistent with a cerebellar disorder
tics → divided into motor, phonic and sensory tics, and also categorized in terms of complexity, into simple and complex
distribution and circumstances are also taken into account in myoclonus and chorea
eg. Sydenham’s chorea is located distally, whereas drug-induced chorea occurs in the face, trunk and arms, and chorea caused by Huntington’s disease is generalized
hypokinetic disorders
hypokinesia or bradykinesia are important features of parkinsons (a hypO-KINETIC - hypER-TONIC disorder, ie hypertonia from rigidity)
recall that extrapyramidal problems can cause rigidity
impairment of the descending pathways from the brainstem (eg. in the cases of both spasticity and rigidity i think?) causes disinhibition not of the anterior horn cells but of the gamma motor neurons controlling the muscle spindles, which changes the muscle spindles’ point of reference (‘turns up the thermostat’), causing permanent hypertonia
however, the symptoms of rigidity and spasticity are very different, check other flashcard
parkinsons patients may experience substantial fluctuations, especially under the influence of medication
there can be off states with hypokinesia and rigidity, and on states with hyperkinesia
tremors in parkinson should not be regarded as hyperkinesia (because they actually dont occur during the off states with hypokinesia and rigidity)
patients with parkinsons feel more comfortable with excessive movement (choreic), probably because these symptoms occur in a stage where the dopamine levels are relatively high and dopamine itself has a positive effect on cognitive symptoms and mood
tremors in parkinson should not be regarded as…
hyperkinesia (because they actually dont occur during the off states with hypokinesia and rigidity)
why do patients with parkinsons feel more comfortable with excessive movement (choreic)
probably because these symptoms occur in a stage where the dopamine levels are relatively high and dopamine itself has a positive effect on cognitive symptoms and mood
parkinsons patients may experience…
substantial fluctuations, especially under the influence of medication
there can be off states with hypokinesia and rigidity, and on states with hyperkinesia
rigidity vs spasticity
rigidity → extrapyramidal, velocity independent, affects both the agonist and antagonist muscles, plantar reflex and tendon reflexes are usually normal
(spasticity generally occurs only during muscle stretch)
WHY IS THERE A TIC (HYPERKINETIC) IN PARKINSONS WHEN ITS A HYPOKINETIC DISORDER
froments sign in rigidity????****
cerebellum functional anatomy
function = balanced execution
do not fucking confuse with the cerebrum (= majority of the brain, the part that has the cerebral cortex)
part of a feedback system
ie. planned movement is checked and adjusted by the cerebellum prior to (internal feedback) and during its execution (external feedback)
since its involved in both internal and external feedback, it receives information from the vestibular nuclei, contralateral cerebral cortex (M2) and from the ipsilateral spinal cord via the spinocerebellar tract
notice how it gets info from the contralateral cerebral cortex but the ipsilateral spinal cord
this is because the left cerebellum controls the left half of the body
divided into 3 parts
spinocerebellum
= vermis (proximal motor function) + medial parts of the hemispheres (distal motor function)
receives information directly from the spinal cord → can control a movement once it has been initiated
feedback to the IPSILATERAL spinal cord is given via the the CONTRALATERAL red nucleus
also from the rubrospinal tract and contralateral cerebral cortex
cerebrocerebellum
= compromises the 2 cerebellar hemispheres
is in contact with the contralateral cortex via the corticopontine pathways
involved in the planning of future movement (internal feedback)
receives information for the direct control of initiated movement from the corticospinal tract as it travels to the spinal cord via the pontine nuclei
this info goes back to the cortex via the contralateral thalamus
vestivulocerebellum
= flocculonodular lobe
completely situated within the cerebellum
controls balance and ocular motor function
cerebellar symptoms
main symptom = axatia = lack of coordinated movement in the absence of muscle weakness → excessive movement that can overshoot OR compensatory movements that do not end in time (disturbed rebound phenomenon)
attempts to compensate for ataxia also fail due to the lack of coordinated movement, leading to cerebellar tremor, especially when approaching a target = intention tremor
antagonistic movements become too large and clumsy + slow
acute stage, patients with cerebellar ataxia complain of dizziness, but that clears up quickly and they then feel unsure of their footing
these were the general symptoms but it can also differ according to where in the cerebellum it exactly is, eg.
hemispheric syndrome → ipsilateral ataxia of the arm and leg
caudal vermis → trunk ataxia with normal limb coordination
saccade dysmetria = eyes do not move smoothly
hypermetria eyes overshoot their intended target
nystagmus (since part of the cerebellum control oculomotor movement***)
might fall back into a chair after getting up and letting go of the chair arm due to truncal ataxia
while turning, a cerebellar disorder may cause the moving leg to swing outwards (i think the book is wrong, circumduction is more for pyramidal diseases ie. paresis while overshooting the step ie. hypermetria is for cerebellar)
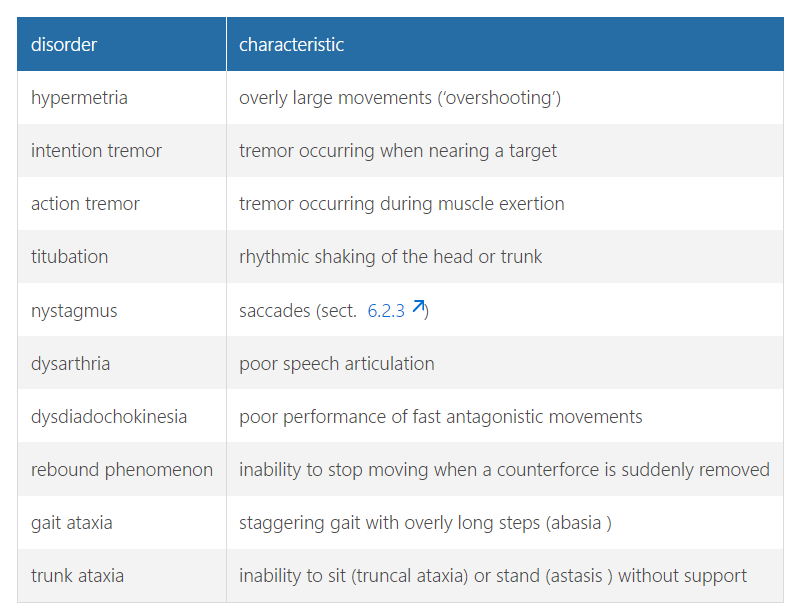
what is the main symptom of cerebellar dysfunction
ataxia (usually upper limb)
other than movement, the basal ganglia and cerebellum also affect…
basal ganglia are not only connected with the motor cortical regions but also with the prefrontal association areas and the limbic system = links ‘motion’ and ‘emotion’
the cerebellum plays a role in cognitive processes and cognitive development. The mind and motor function are therefore more interconnected than was long thought
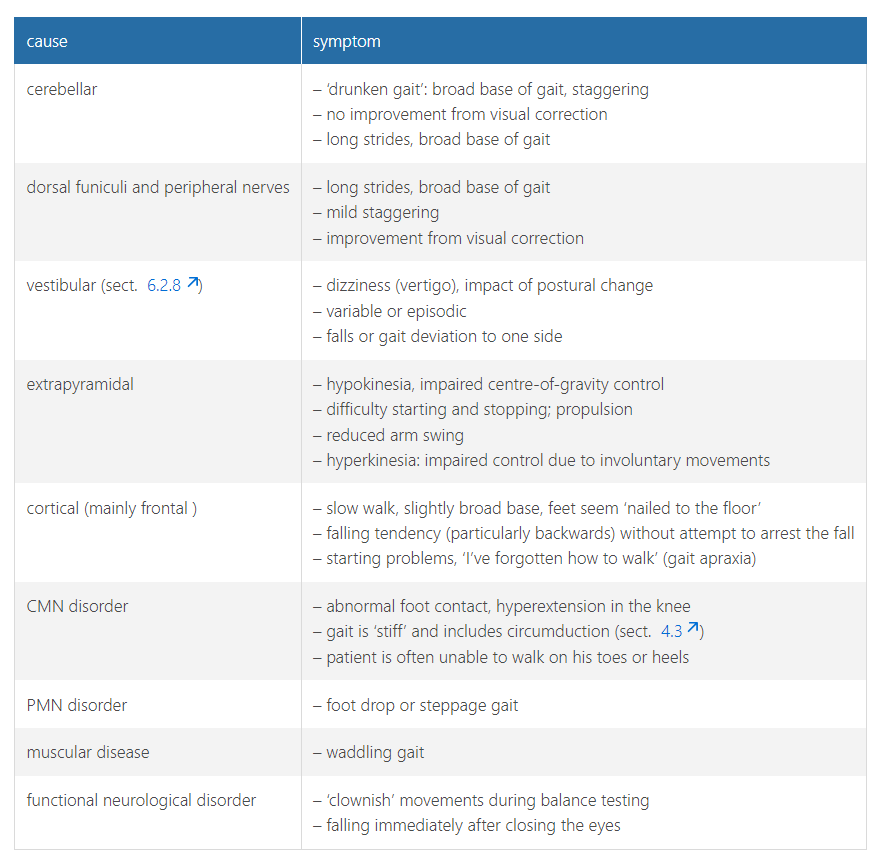
examination of central motor control - central motor function tests***
a extrapyramidal disorder ,
b pyramidal system disorder ,
c cerebellar disorder and
d epicritic system disorder.
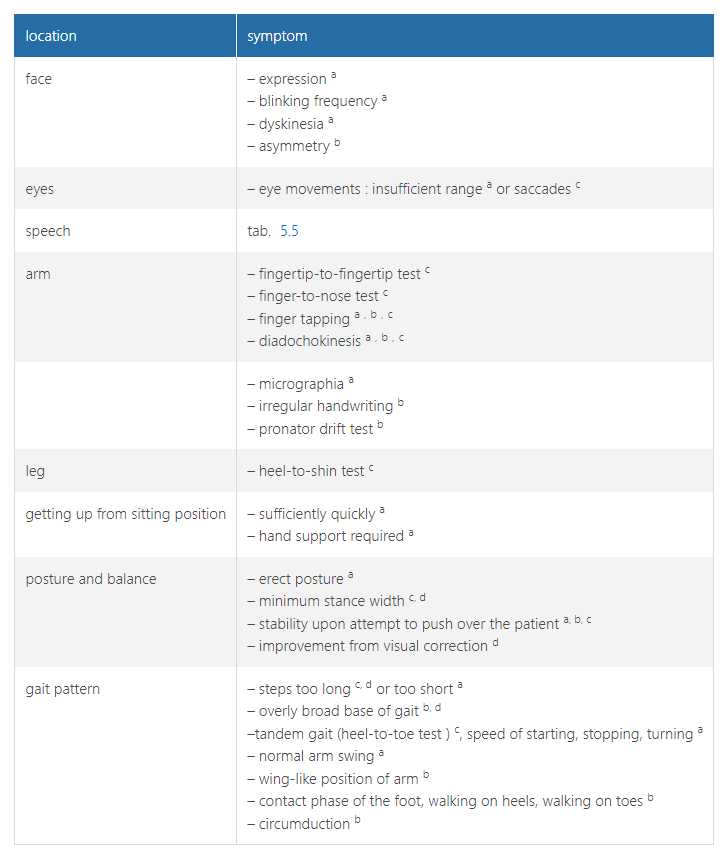

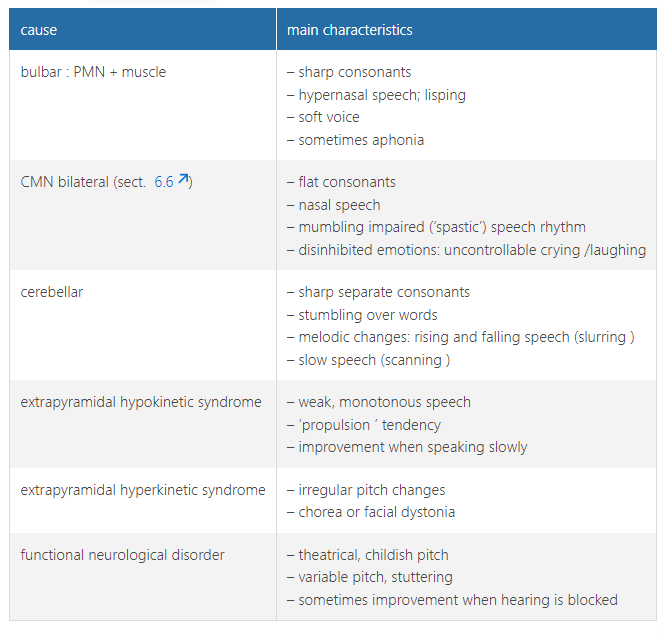
examination of central motor control - main forms of dysarthria (motor speech disorder)***
Impaired speech can be caused by impaired motor function (central or peripheral) or impaired motor control (cerebellar or extrapyramidal)
parkinsons disease symptoms general
facial hypomimia = stolid facial expression
reduced blinking frequency
abnormal posture
during finger tapping (tapping the thumb and index together for 30s) they generally exhibit a progressive decrease in the amplitude of the movements and become hesitant
often find it hard to get up from a chair
arm swings may be less pronounced in one or both arms in the early stages
hyperkinetic syndromes
characterised by facial tics → rapid blinking, winking, raising eyelids or a corner of the mouth and sometimes tongue protrusion
dystonia
may be accompanied by excessive closure of (usually both) eyes and an abnormal contraction of a corner of the mouth
position of the head may be abnormal
torticollis = head tilted to one side (usually slightly backwards)
antecollis = forward hyperextension
retrocollis = backward hyperextension
pyramidal tract involvement often causes…
asymmetry in the lower half of the face
how does the cerebellum affect eye movements
eyes do not move smoothly but jump around (saccade dysmetria) and overshoot their intended target ( hypermetria ). Often nystagmus occurs when the patient is instructed to look at a stationary finger held 45 degrees to the side of the face. The eyes will then simultaneously saccade in the direction of the fixated object. Nystagmus can be interpreted as an intention tremor of the gaze.
how are eye movements affected in extrapyramidal impairment
field of vision in the vertical plane may be restricted, particularly in the downward direction = progressive supranuclear paresis
dyskinesia can cause oculogyric crisis = upward or downward deviation of the eyes
several hypokinetic syndromes make it hard for patients to quickly shift their gaze, eye movements are generally slow or interrupted
actual question: does extrapyramidal impairment cause hypo or hyperkinetic???
upper limb ataxia
cerebellar impairments often cause ataxic symptoms in the arms
check for any intention tremors, especially during the finger-to-nose test
the target will only be missed if the ataxia is severe
If the ataxia is mild and the nose is still missed with eyes open or closed, this should be regarded as a functional neurological phenomenon
recall from theme 1 that if the test can be completed w/ eyes open but not closed then deep sensation is impaired (sensory ataxia)
finger to finger test is more sensitive than finger to nose test
although these tests can be done smoothly by a patient w/ extrapyramidal syndrome, they will be slower
in the case of both cerebellar and extrapyramidal disorders (also CMN impairment) tests involving antagonistic movements (diadochokinesis) will be positive → eg. switching between supination and pronation, rapid finger movements
isnt the cerebellum part of the extrapyramidal tract??? no it isnt they literally stated that
in parkinson’s patients, during finger tapping (tapping the thumb and index together for 30s) they generally exhibit a progressive decrease in the amplitude of the movements and become hesitant
in cerebellar disorders, when trying to grasp something between the thumn and index finger they will make the gap too wide and overshoot the object
also rotations in the wrist will be too large and irregular
also a rebound phenomenon occurs = unable to correct the position of a limb
handwriting → irregular letters, abnormally large letters (macrographia) and untidy handwriting
in extrapyramidal syndromes, the ranges of motion are too small and slow
also unlike cerebellar disorders, this causes abnormally small handwriting (micrographia)
diadochokinesis
the inability to perform rapid alternating muscle movements
actual q: why does it not count as ataxia if they also cant touch their nose with their finger if there eyes are open???
components of the extrapyramidal system
The main components of the extrapyramidal motor system are the nuclei of the basal ganglia. Other structures which are involved include the nuclei of the cerebellum and brainstem, as well as the mesencephalic reticular formation
lower limb ataxia
can be detected by observing gait and heel-to-shin
heel-to-shin → patient is instructed to smoothly place a heel on the knee of the other leg, wait for a second and then smoothly move the heel along the edge of the tibia to the great toe
cerebellar disorder → will overshoot the knee (hypermetria) and there will be an intention tremor → movement will be jerky and the heel will lose contact with the shin
those with sensory ataxia will benefit from visual correction
cerebellar leg ataxia also manifests itself during walking as the patient exhibits too much hip flexion and swings the leg too far forward = hypermetria
truncal movements***
Patients with Parkinson’s disease often find it hard to get up from a chair. They do not automatically move their feet backwards and push themselves up with their hands. Sometimes they have to make a few attempts, falling back into the chair when unsuccessful.
When letting go of the arm the patient may fall backward; in severe cerebellar disorders the patient may not be able to sit unaided because of truncal ataxia. In less severe disorders the rebound of the trunk may be impaired when that of the arms is tested: the patient falls backwards when the arm is released
muscle tone
can be tested by inducing slow passive movement across joints
extrapyramidal problem → resting muscle tone is usually elevated across the entire range of motion and cogwheel rigidity is often present
+ activation of other muscle groups may show rigidity sooner
CMN involvement → spasticity
cerebellar → can cause hypotonia
activation of …. may show rigidity sooner
other muscle groups
muscle stretch reflexes
normal in extrapyramidal impairment
cerebellar → the patellar reflex test may produce pendular reflexes: the lower leg keeps swinging for a while because the movement is not inhibited
low significant tho
CMN → hyperreflexia and babinski
muscle stretch reflexes are… in extrapyramidal impairment
normal
gait and stance
even minor CMN problems can cause impairment of postural reflexes
test by instructing the patient to stand erect with their feet together or as close as possible
if the patient does not sway in this position, start the push and pull test = gentle pushes in various directions
romberg tests deep sensation which is NORMAL in cerebellar disorders
suddenly falling or losing one’s balance after closing the eyes will usually be due to a functional neurological disorder
the types of atasis (insecure standing) and abasia (insecure walking) depend on where the lesion is (CHECK PHOTO)
a heel to toe test just tells you if the CNS is functioning normally
if abnormalities are found then a more detailed examination is needed
while turning, a cerebellar disorder may cause the moving leg to swing outwards
arm swings may be less pronounced in one or both arms in the early stages of parkinson’s
while turning, a cerebellar disorder may cause
the moving leg to swing outwards
figure 5.7!!!!!!!!!!!!!
cerebellar function tests are abnormal in … and … (not disorders)
children below age 12 and the sense of balance declines with age
also standing and walking become harder when people are nervous
those with functional neurological disorders often perform better on … than on …
often perform better on difficult tests than on simple ones and distraction leads to better results
chapter 5 key points
In the case of basal ganglia dysfunction, voluntary movements are often restricted, and in the case of a cerebellar problem they will be too large.
An extrapyramidal disorder can be accompanied by hypokinesia or sometimes hyperkinesia.
Tremors due to basal ganglia dysfunction are linked to hypokinesia.
The increase in tonus in a patient with impaired basal ganglia is different from that in one with spasticity, namely greater stiffness throughout the range of motion with no ‘give’, i.e. rigidity.
The basal ganglia communicate with the ipsilateral cortex, the cerebellum with the contralateral cortex
chapter 8 key points
A number of higher functions can be localized, but even they can be impaired due to a problem further on that impedes the supply of information.
The functions related to perception are located in the posterior part of the cerebrum, those involving action in the anterior part.
In 95 % of people, the language-dominant hemisphere is the left one (that includes half of left-handed people), and it is the seat of mainly analytical functions.
The non-language-dominant hemisphere is no less important, being the seat of emotion, strategic understanding and spatial understanding in particular.
Aphasia can broadly be divided into receptive and expressive aphasia, but both of these elements are usually somewhat impaired in a patient with aphasia. There are also some specific types of aphasia.
Apraxia is the inability to act and is used in various contexts – sometimes wrongly. The performance of actions on command or according to an internal plan originates mainly in the language-dominant hemisphere, even if the non-dominant hand is being used.
Agnosia can take on fairly complex forms. The patient perceives something but fails to recognize it. This is almost always due to an impaired connection between two cortical areas (disconnection).
Speech is altered also as a result of problems in the non-language-dominant hemisphere: it is less musical, more monotonous (aprosodia). The patient understands factual matters but misses emotional undertones, which can lead to distressing misunderstandings.
Spatial disorders are caused by problems in the posterior parts of the non-language-dominant hemisphere. A particular type is problems with dressing, referred to – not entirely correctly – as ‘dressing apraxia’.
Vitamin B 1 deficiency causes severe types of short-term memory disorders, Korsakoff’s syndrome. These are often due to an alcohol problem, but not always.
Transient global amnesia – as far as we know – is a harmless syndrome that does not require any additional tests.
There are two sides to a frontal syndrome: (a) insufficient activity (orbitofrontal) and (b) disinhibition of action and omission (dorsolateral). The patient has no overview and behaves chaotically.
As the posterior cerebral artery supplies part of the hippocampus, infarctions in the posterior cortex can also cause mental phenomena.
Various neurological (especially degenerative) disorders are accompanied by altered consciousness (delusions, hallucinations).
The MMSE and the Frontal Assessment Battery can be used to test the higher functions: these tests are complementary. The MoCA test lies between the two and is essentially a combination of both.
diffuse and local cortical disorders
dementia → deterioration in cognitive funtcion due to general neuron loss
if its local loss, the following may occur:
aphasia → language disorders
apraxia → inability to perform purposive actions
agnosia → inability to interpret sensory information
the presence of a cognitive disorder can only be established if…
primary motor and sensory capability, consciousness and cooperation are all reasonably normal
eg. aphasia cannot be diagnosed if they have a motor disorder that prevents normal speech, apraxia cannot be diagnosed if hemiplegia is present in the same half, and astereognosis (agnosia) is identifiable only if primary tactile sensation is normal
insular***
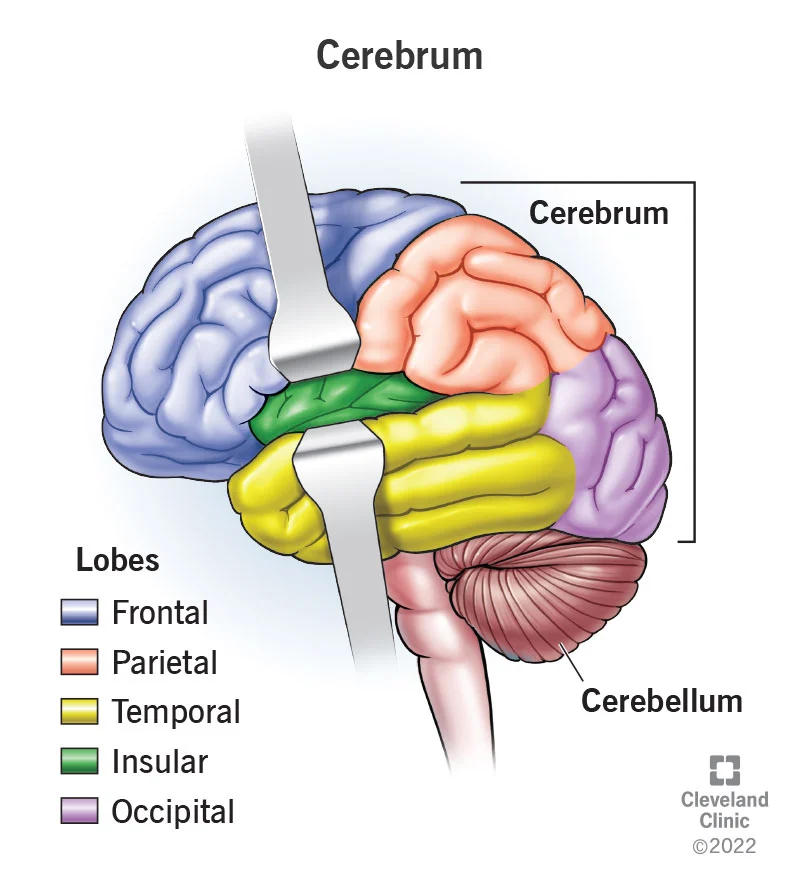
anatomy of the cerebrum
consists of 2 cerebral hemispheres separated by the falx cerebri of the dura mater
rear part = parietal, temporal and occipital lobes → involved in mainly perception and secondarily the initiation of action
Front part = frontal lobes → important for executive functions and the integreert of personality
Perception has 3 stages → information is input (= primary cortical zone), analysed (= secondary cortical zone) and then put into context (tertiary cortical zone)
Secondary areas are also known as association areas
But each area deals with one sensory quality so they’re described as unimodal, several unimodal association areas form a heteromodal association area = tertiary cortex ????? How does that make sense
is it like the stimuli from the unimodal association areas combine in the heteromodal association area/tertiary cortex to form a single concept
The synthesis of information can lead the prefrontal cortex to initiate a voluntary action
The secondary cortical regions (where gnostic sensory info is processed in order to locate things in space = ‘where’) have fairly direct connections to the secondary motor regions
The info comes in → primary cortex → secondary cortex/unimodal association areas process info in order to locate things in space (where) → all info combines in the heteromodal tertiary cortex, sends all information about ‘what’ to → Limbic cortex
‘what’ information can also be relayed via the protopathic system
wait idk if ^is true? is it where → what → limbic? or where AND what → limbic
The secondary cortical regions, in which gnostic sensory information is processed in order to locate things in space (‘where’), have fairly direct connections to the secondary motor regions (fig. 5.1-M2) where movements are generated. The sensory information related to the nature of ‘what’ is relayed via the heteromodal areas, after being linked to other information, to the limbic cortex (fig. 8.2). A substantial amount of information on the sensory ‘what’, especially that relating to emotion, is also relayed via the protopathic system (sect. 4.1.6). There is a similar division into ‘where’ and ‘what’ (see sect. 9.1.2) in the case of the other modalities, but slightly different in each case.
which cortical hemisphere is language dominant
left (usually… roughly 90% of people are right handed, for them language is usually on the left)
left also deals w/ musical analytical capability and the sense of rhythm
right (in 95% of people) is more associated with feeling, expressing and perceiving emotion AND emotional language use such as prosody (= sentence melody, emotional hue of language) and intonation
also regulates attention, visual spatial perception, orientation in the left half of the body and the recognition or evaluation of melodies
where is hemispherical specialisation less pronounced
in the medial regions of the hemispheres
this is where the phylogenetically old (paleocortex = blue) and new (neocortex = grey) parts of the cortex meet in the mesial temporal cortex (medial temporal lobe)
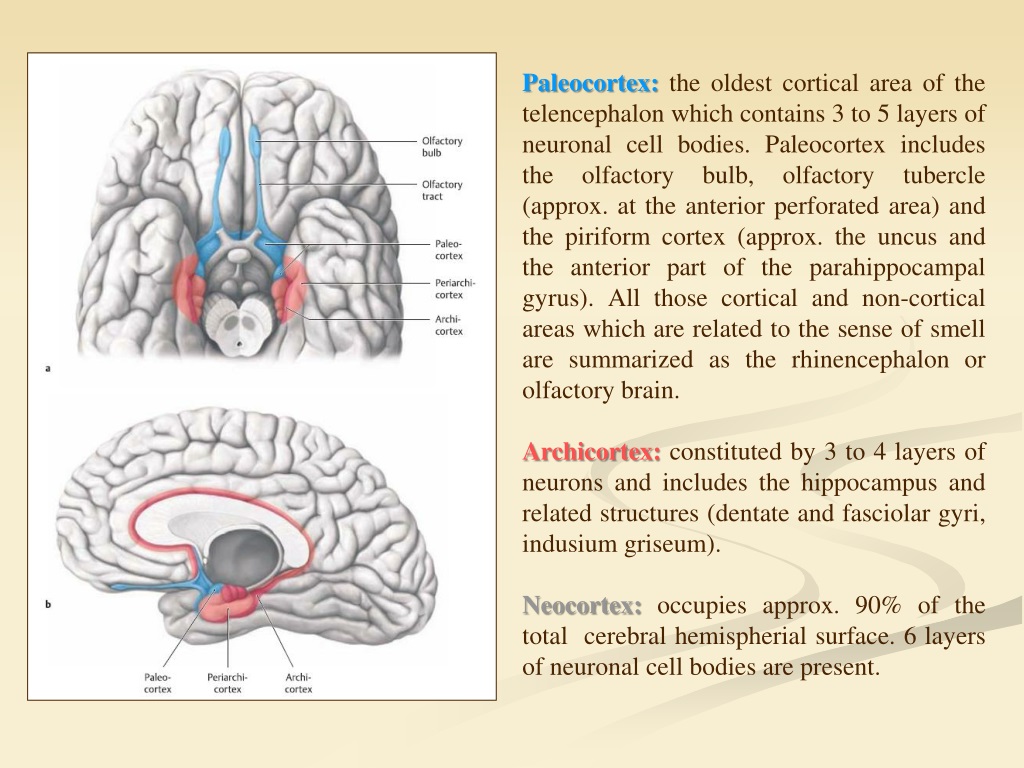
the limbic region is = ?
paleocortex + boundary area (what like the mesial temporal cortex?)
the limbic system has close connections to the…
hypothalamus and the olfactory area, which is why the limbic system can influencing the:
autonomic NS, eg. → goose-bumps triggered by a thought
endocrine system, eg. → perceiving and responding to sexual stimuli
emotion and memory
regulated by the primary limbic system
components → the amygdala, hippocampus, thalamus, hypothalamus, basal ganglia, and cingulate gyrus
amygdala function → to establish the emotional and motivational value of incoming sensory information
since its connected to the hypothalamus, it means that the autonomous NS is triggered by the emotional cues
if it were able to function entirely unchecked, every stimulus would initiate a strong impulsive response but it is inhibited by the frontobasal cortex → enables the adaptation of impulsive behaviour
however, a stimulus that is not immediately recognized can elicit a strong impulse response
the hippocampus is also located close to the amygdala → plays a central role in memory formation and therefore temporal orientation (measurement of memory?)
The amygdala processes incoming information from the sensory association areas (fig. 8.1-9) and attaches (often persistent) emotional significance to it (supplementary response by the amygdala). Memories are not retained in the hippocampus for long, however. Instead, the processed data is returned to the cortex regions that the ‘raw’ information came from. Thus, if similar information is perceived again in the future, appropriate associations can quickly be made, so that something may be immediately recognized as ‘nice’, ‘frightening’, or ‘horrid
i think ^ is like the hippo keeps getting short term and changes them into long term associated with somethin else an sends them to be stored elsewhere?
what inhibits the amygdala
frontobasal cortex
… is the part of the brain involved when it comes to behaviours we need for survival: feeding, reproduction and caring for our young, and fight or flight responses
limbic system
8.1.5???***
aphasia
can occur in isolation but is usually accompanied by a loss of the ability to read (alexia) and write (agraphia) and quire often by motor disorders affecting one half of the body (usually the dominant side)
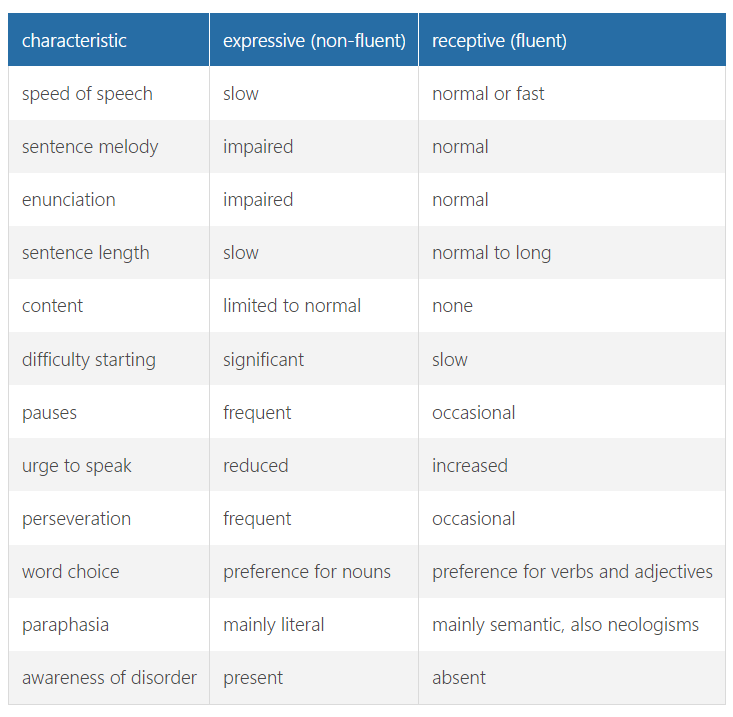
can be loosely split into mainly expressive and mainly receptive disorders, this is based mainly on the ability to speak easily and articulately (fluency)
motor aphasia = mainly expressive/fluent lesion:
usually localised towards the front of the posterior frontal cortex (of the dominant hemisphere), specifically in the inferior frontal gyrus/brocas speech centre = broca’s aphasia
able to understand language but cannot put thoughts into words (not adequately)
starting to speak is hard, speech is slow and full of pauses, right word is hard to find, words get muddled up, repetition is frequent
letters or letter groups are often revered = literal paraphasia
preference for nouns
patient is aware of their inability to express themselves normally → liable to become distraught or angry
sensory aphasia = mainly receptive/non fluent lesion:
usually localised towards the back of the dominant hemisphere = temporal lobe, specifically in the superior temporal gyrus/wernicke’s speech centre
ag. wernicke’s aphasia
also known as jargon aphasia
understanding of language is seriously impaired
patient can speak (often fast w/ normal intonation) but construction of sentences is incomplete using fixed phrases and sometimes joins unrelated separate words together
preference for verbs and adjectives
words are used in the wrong sense (semantic paraphasia) or completely new words are formed (neologisms)
if serious → loses ability to read and write
if mild → reading ability is normal but they dont understand
usually unaware that anything is wrong and its hard to communicate with them
other forms
amnestic aphasia/anomia:
characterised mainly by difficulty remembering names and words in isolation
not always so obvious in spont. speech (typ. fluent) but recognisable if the patient is asked to name a series of objects or images
location of lesion is variable
conduction aphasia:
disorders of the arcuate fasciculus which connects the temporal and frontal language areas
unable to repeat a sentence, mild problems with findinf the right word + mild literal paraphasia
spont. speech is largely normal and comprehension is good but reading aloud and writing are impaired
transcortical aphasia:
transcortical motor aphasia → unable to form a complete sentence in answer to a question
transcortical sensory aphasia → unlike ^, complete answers can be formed but with lots of semantic paraphasias (when an entire word is substituted for the intended word)
ability to repeat is normal
mixed (possibly total) aphasia:
most common form
both expressive and receptive forms are expressed but one form may be more pronounced
usually due to extensive lesions or to deep-lying lesions that disrupt the pathways between the cortical speech areas
what is the most common type of aphasia
mixed
if aphasia is due to …, partial or even total recovery is possible
a non-progressive cerebral problem (cerebral infarction, traumatic brain injury)
gerstamann’s syndrome
a neuropsychological disorder characterised by:
agraphia (inability to write)
acalculia (inability to perform mathematical calculations)
finger agnosia (inability to name, discriminate, or identify fingers)
left-right disorientation (inability to distinguish left from right)
due to a problem in the posterior region of the angular gyrus
combo of symptoms is due to a problem in spatial awareness
apraxia
inability to perform purposive actions (despite having an intact plan of action) or make gestures, although there is no motor disorder and the instruction is understood
caused by a problem in the language-dominant hemisphere, but affects both hands (eg. if a R handed patient has a L hemisphere problem, they may also lose the ability to do things w/ both their L and R hands)
→ specifically in the inferior parietal gyrus
→ can also be a due to a problem in the connection between the inferior parietal gyrus and the secondary motor regions (!! the inferior parietal gyru is connected to the contralateral secondary motor region, so an injury in that connection can only cause CONTRALATERAL ideomotor apraxia)
ideomotor apraxia = inability to voluntarily perform a learned task when given the necessary objects (eg. if given a screwdriver, the may try to write with it)
mild cases → appear slightly clumsy or absent minded, ability to copy actions may be retained but instructions cannot be followed
ideational apraxia = only spontaneous action (making coffee, unwrapping a present) is impaired, or the patient is unable to follow instructions only when a series of actions is involved (which require a plan of action)
the term apraxia is also sometimes used to refer to problems of performing activities controlled from other parts of the brain
micturition apraxia and gait apraxia → attributable to problems in the deep frontal cortex
dressing apraxia and constructive apraxia (arise in the non dominant hemisphere)
apraxia of lid opening
verbal apraxia and buccofacial apraxia → often caused by injury to broca’s speech centre or a nearby area
typically accompanied by non fluent aphasia
agnosia
= inability to recognise and integrate sensory perceptions
diagnosis is only appropriate if the peripheral apparatus is reasonable intact (eg. it cant be visual agnosia if their eyesight is defective)
tactile agnosia:
due to lesions in the parietal lobe close to the primary sensory cortex
contralateral to the lesion its undetected or only in the test???
main symptoms is astereognosis = inability to recognise objects by touch
often aware of pain or tactile stimuli but cant accurately localise the source
A good way to test for tactile agnosia is to provide simultaneous, symmetrical stimuli to both halves of the body. Contralateral to the lesion, the stimulus will be undetected, even though the patient is able to discern the stimuli individually, because attention in the affected hemisphere is extinguished by attention in the healthy hemisphere = tactile extinction
anosognsoia = being unaware that one half of the body is dysfunction
occurs in cases of acute (usually vascular) injury to the non dominant parietal cortex, usually disappears after a few hours or days (the injury or being unaware???)
body scheme disorder???
autotopagnosia = inability to recognise and name parts of the one’s own body, likely to be due to a problem in the language-dominant hemisphere
eg. finger agnosia
→ regarded as part of a naming disorder
visual and acoustic agnosia → stimulus is perceived but not understood = sensory information is not correctly associated with other retained information in the heteromodal tertiary association areas (eg. will hear the sound of a bunch of keys being rattled, but identify the sound as falling marbles)
kluver-bucy syndrome
very rare form of agnosia
due to the limbic system not receiving the correct information or is deactivated (sensory limbic disconnection) → no emotional significant is attached to incoming stimuli, oral tendency, hypersexuality, memory loss, failure to recognise familiar objects and people (visual agnosia and prosopagnosia respectively), loss of fear and abnormal aggression (last 2 are due to disconnection of the amygdala)
= bilateral dysfunction of the frontal region of the temporal lobe (thats where the limbic system is right???), usually most pronounced on the right
can develop after bilateral neurosurgical procedures or an infection such as herpes simplex encephalitis, in the context of a degenerative syndrome such as frontotemporal dementia or following a traumatic brain injury or CVA
aprosody
= inability to recognise or produce affective vocal inflection or facial expressions of emotion
diagnosis is important to prevent patients with injuries to the non-dominant hemisphere from being perceived as dissatisfied or ill-tempered
cognitive symptoms that are lesions in the language vs non language dominant cortex
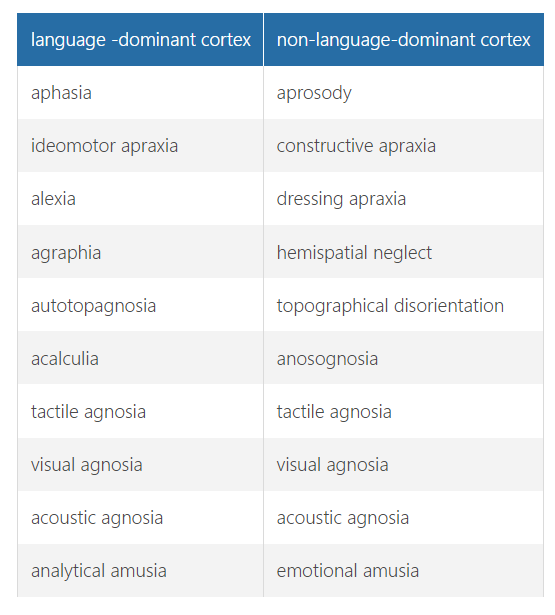
spatial disorders
due to problems in the posterior regions of the non dominant hemisphere
characterised by the inability to depict spatial relationships when copying or drawing
often accompanied by dressing apraxia
If a disorder in the posterior of the non-dominant hemisphere is suspected, confirmation can be sought by asking whether the patient often has problems finding their way when out and about in familiar places or even when at home ( topographical disorientation ), or is apt to forget the whereabouts of things they have put away