BMA End of Semester Test
1/86
Earn XP
Description and Tags
Topics 5-8, Pracs 3-5
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
87 Terms
Spinal Cord
Communication highway between the brain and nerves
linking peripheral receptors to the brain
then to the effector muscles and glands
External Anatomy of the Spinal Cord
Long, thin and delicate tubular structure
Protected by the vertebral column, passes through the vertebral foramen
ends at L1-2
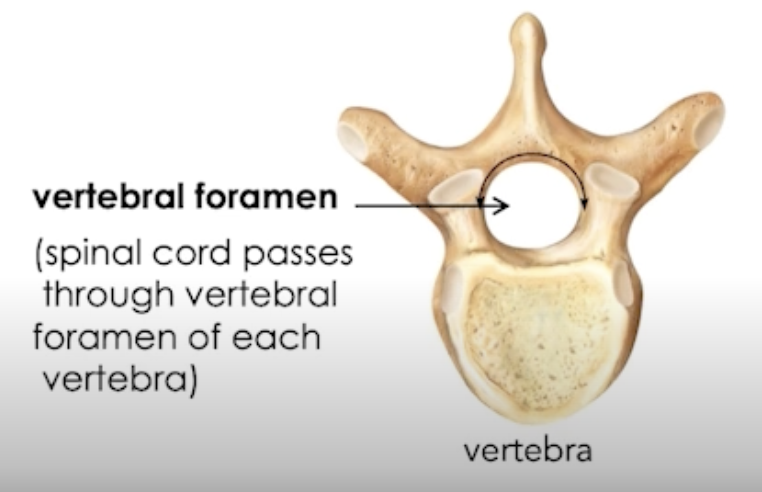
Regions of the Spinal Cord
Cervical (C1-8)
Thoracic (T1-12)
Lumbar (L1-5)
Sacral (S1-5)
Coccygeal (1)
→ Spinal cord ends at L1-2, therefore, L1-5, S1-5 and 1 coccygeal lie between T12-L2 of the VERTEBRAL COLUMN
not located in their corresponding regions, but will extend out to them
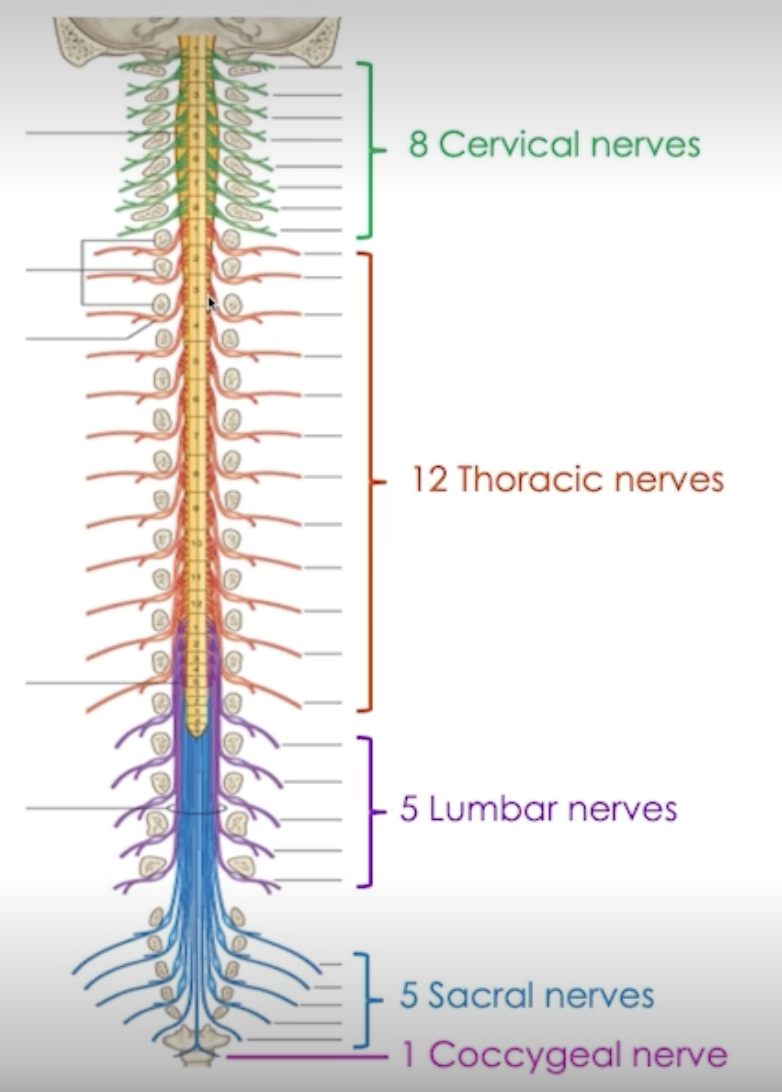
Spinal Nerves
Pairs of spinal nerves → axons
Dorsal (back) = sensory
sensory neurons = UNIPOLAR
Ventral (front) = motor
autonomic and somatic motor neurons
→ Mixed nerves (sensory + motor)
Protection of Spinal Cord
Mechanical forces, protected by:
Vertebral column
CSF
Spinal Meninges
Parts of the Spinal Cord
Caude Equina: Collection of nerve Roots (L1-5, S1-5, 1 coccygeal)
That extend beyond the conus medullaris (End structure of spinal cord)
emerge out of corresponding vertebral column
Filum Terminale: extends from the conus medullaris → coccyx vertebral column
Anchors the spinal cord in place
so that spinal cord isn’t affected by mechanical forces
Internal Anatomy of Spinal Cord
Neural tissue divided into left and right: separated by 2 grooves
Anterior (front) median fissure
*THINK → front = deeper into body, = deeper groove
Posterior (back) median sulcus
Grey matter surrounded by White matter
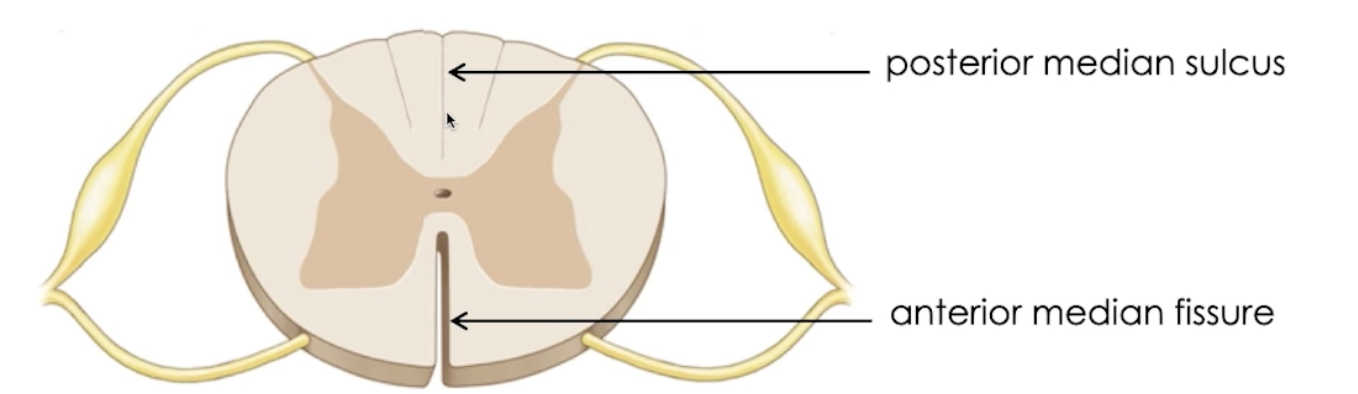
Grey Commissure
Axons cross from one side to the other
Explains why right brain = left movement, vice versa
Central Canal = contains CSF, nourishing neural tissue
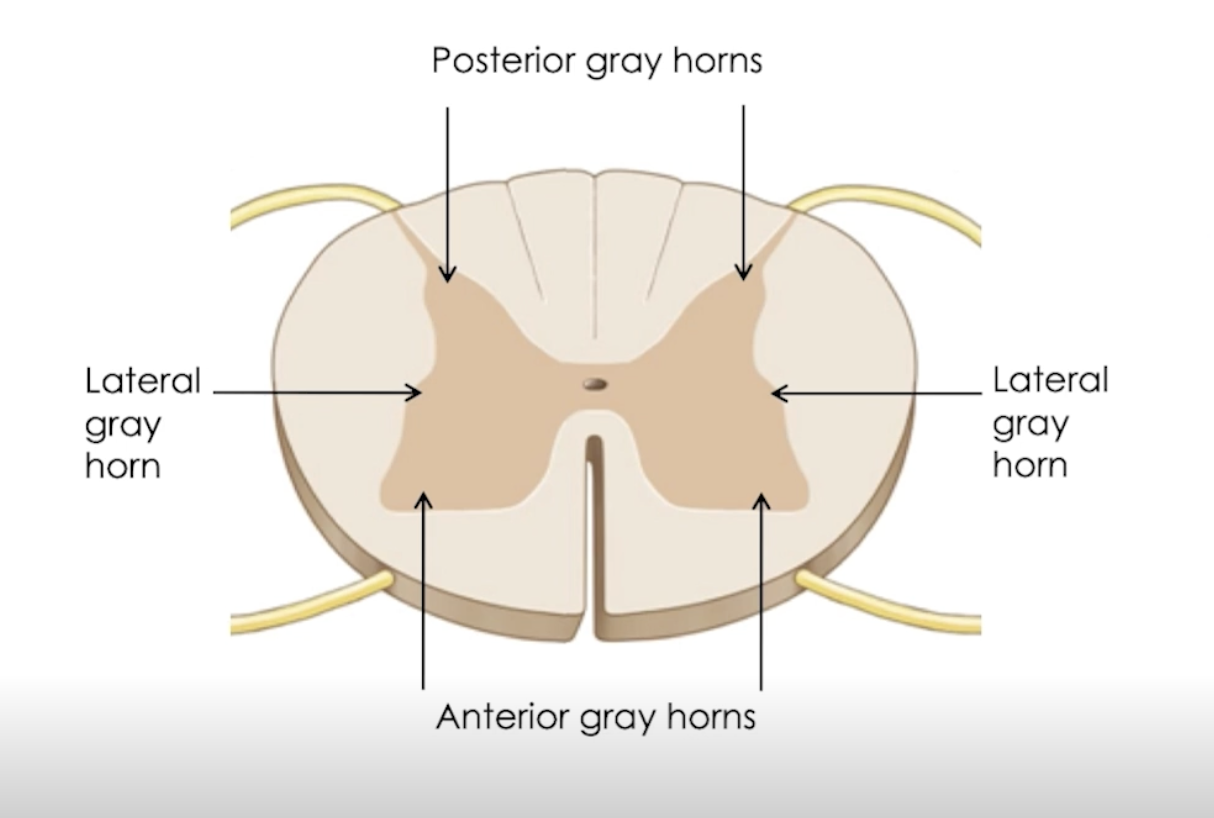
Subdivided into gray horns: → Processing
Anterior
Somatic motor function
cell bodies of lower motor neurons
Lateral → only thoracic and lumbar
Autonomic motor function
cell bodies of preganglionic neurons
Posterior = sensory input
cell bodies of spinal interneurons
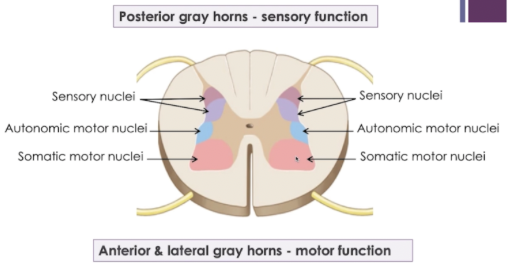
White Commissure
“Conduction highway”
→ Myelinated and unmyelinated axons
→ Anterior white commissure = axons cross from one side to the other
White columns, subdivided into:
Anterior
Posterior
Lateral
→ Ascending and descending spinal cord tracts (axons)
Ascending Spinal Cord Tracts
Sensory input → BRAIN
Posterior White Columns:
Fasciculus Gracillus
Fasciculus Cuneatus
Fine touch, light pressure, vibration, conscious proprioception
Lateral White Columns:
Lateral Spinothalamic
Pain and temperature
Anterior + Posterior Spinocerebellar
Unconscious proprioception
Anterior White Columns:
Anterior Spinothalamic
crude touch, deeep pressure
*THINK → more INSIDE = deep
Fine Touch vs Crude Touch
Fine touch = discriminative -> sense and identify location of touch stimulus on the skin
Details like texture, size and shape
Crude touch = non-discriminative -> cannot precisely locate the stimulus
No specific details, e.g. when someone bumps into you
Descending Spinal Cord Tracts
Lateral White Columns
Lateral Corticospinal
Somatic motor output - skeletal muscles of LIMBS
Anterior White Columns
Anterior Corticospinal
Somatic motor output - skeletal muscles of AXIAL
Somatosensory Neural Pathways
Connect receptors to brain
Conduct general sensory input
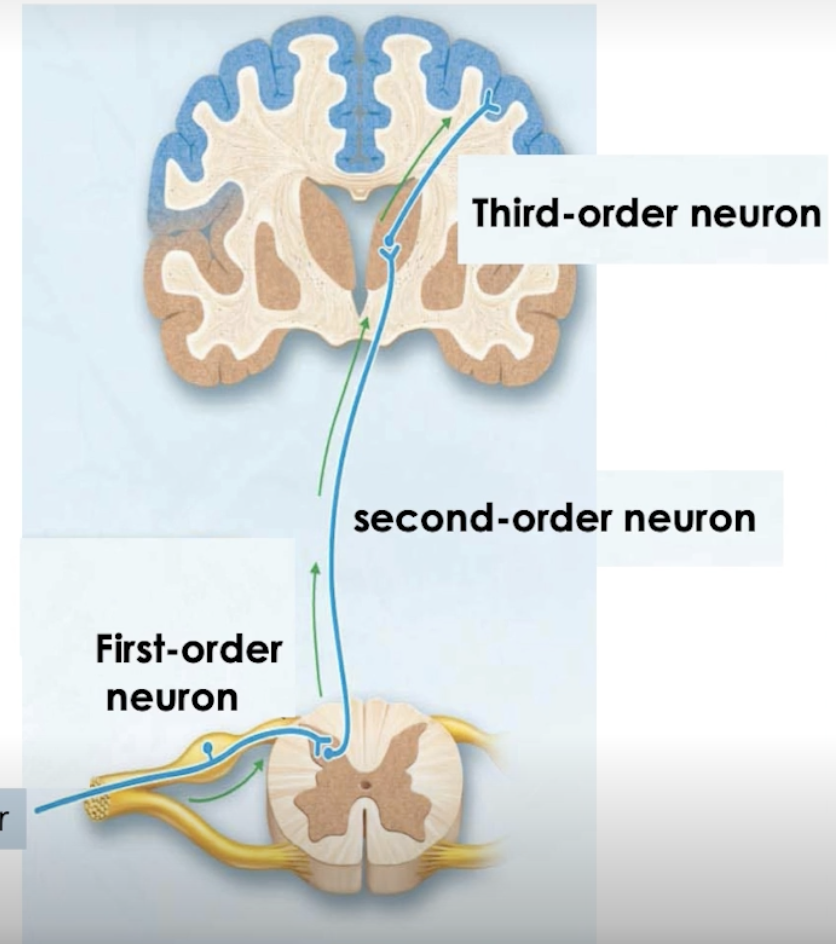
Relay of neurons:
First-order - sensory input from receptors → posterior gray horns
synapses with second-order, within sensory nucleus
Second-order - sends sensory input to designated area of brain
ascends through spinal cord tracts
synapses with third-order, within region of brain
Third-order
sensory input to designated cortex of the area of the brain
3 Main Somatosensory Pathways
Spinothalamic (crude touch, deep pressure - anterior)
(pain and temperature - lateral)
First order - sensory input from tactile, nociceptors and thermoreceptors into posterior gray horn
Second order - sensory input to thalamus
through anterior/lateral
Third order - sensory input from thalamus to PSC
Spinocerebellar (unconscious proprioception)
Maintains posture, balance, standing sitting and walking, ensure smooth coordinated movements
First order - sensory input from proprioceptors to posterior gray horn
Second order - sensory input to cerebellum
NO THIRD ORDER
Fasciculus G/C (fine touch, light pressure, vibration and proprioception)
First order - sensory input from proprioceptors and tactile into posterior gray horn
Synapses w second in medulla oblongata
Second order - sensory input to thalamus
Third order - sensory input to PSC
Somatic Motor Pathways
Conducting somatic motor output from PMC to skeletal muscles
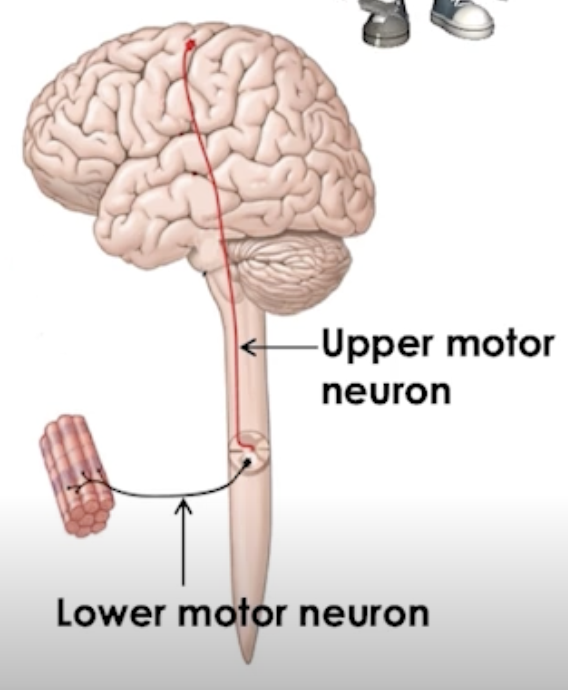
Relay of 2 neurons:
lower motor
upper motor
Main Somatic Motor Pathways
Lateral corticospinal
Upper motor neurons: somatic motor output from PMC to anterior gray horn
Descending spinal cord in tract
Lower motor neurons: Somatic motor output to skeletal muscles of limbs
Anterior corticospinal
Upper motor neurons: somatic motor output from PMC to anterior gray horn
Descending spinal cord in tract
Lower motor neurons: Somatic motor output to axial muscles
Spinal Reflex Arcs
Neural pathways that produce a rapid, predictable, involuntary somatic/autonomic reflex response to stimulus
5 components
Receptors
Sensory neurons
Integration centre
Lower motor neurons
Skeletal Muscles
Somatic Reflexes
Mediated by reflex integration centres (in spinal cord)
Stimulates skeletal muscle contractions
Lower motor neurons (LMN)
Motor output to skeletal muscles → can be modified by the PMC
Can be modified by the PMC (upper motor neurons)
Can diagnose disorders of the Nervous System
Patellar Reflex - Knee Jerk
Normal response = extension of the knee
Damage to spinal segments L2-4 OR Lower Motor Neurons → loss of reflex
Damage to Primary Motor Cortex or Corticospinal Tracts → hyperreflexia
Plantar Reflex
Normal response = flexion of toes
Damage to spinal segments L4-S2 or LMN = loss of reflex
Damage to PMC or corticospinal tracts = Bakinski sign
Spinal Cord Injuries
Sensory and/or motor losses → at or below level of injury
Damage to posterior gray horns (ascending) = loss of sensation
Damage to anterior gray horns (descending) = spastic or flaccid paralysis
Spastic Paralysis
Upper Motor neurons are damaged
Lateral White Columns affected
Loss of voluntary movement
Reflex activity intact → abnormal (hyper reflexia)
Flaccid Paralysis
Lower Motor neurons are damaged
Loss of voluntary movement and reflex activity
Complete Transaction of Spinal Cord
Loss of all sensations and voluntary movement
Both sides of body are affected
Transection in cervical region = quadriplegia (electric wheelchair)
Transection in thoracic or lumbar regions = paraplegia (leg muscles)
Reflex activity below level of Transection = present but abnormal
Spinal shock: transient period of complete sensory and motor loss
loss of all reflexes below level of lesion
reflex activity will slowly restore
Autonomic Nervous System
Dual innervation
Most effector organs are innervated by both sympathetic and parasympathetic divisions
ANS divisions can work independently or together
Opposing effects, counterbalance
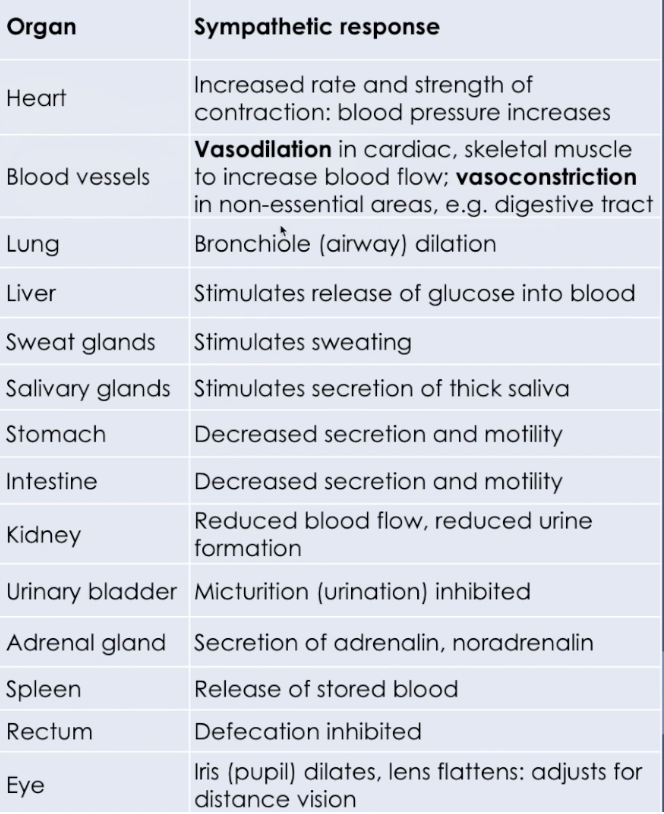
Sympathetic Nervous System
Preparing the body for heightened activity
Exercises, excitement, emergency, embarrassment (fight or flight)
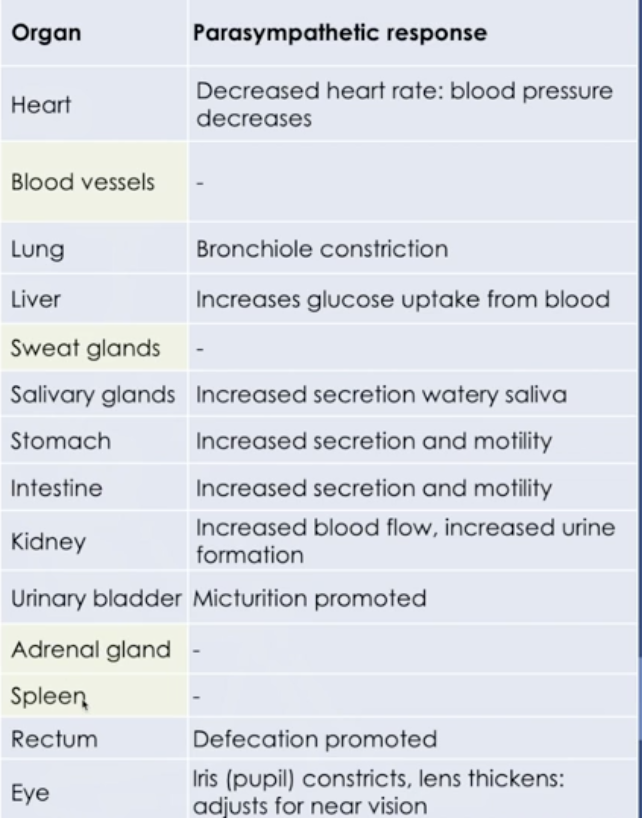
Parasympathetic Nervous System
Stimulating abdominal visceral activity
Conserving energy, rest and digest
Blood vessels, sweat glands, adrenal and spleen do not have parasympathetic function
Somatic vs Autonomic NS: General
Similarities
Both are efferent divisions
CNS to effectors
Differences
Neural pathways
Effectors - target organs
Organ responses
Neurotransmitters
Somatic vs Autonomic NS: Pathways
Somatic
Corticospinal pathway
Upper motor neurons cell bodies are in PMC
Travel down the spinal cord to LMN in anterior grey horn
Ventral root of spinal nerve to skeletal muscles
Autonomic
Peripheral pathways
Visceral motor nuclei in the hypothalamus (cerebral cortex ~ limbic system)
Preganglionic neurons → synapse with postganglionic neurons and innervate target organs
Smooth muscles, glands, cardiac muscles
Peripheral Motor Neurons
Somatic
Targets skeletal muscle fibres
Lower motor neuron cell body
spinal cord motor nucleus (anterior gray horn)
axon exists through ventral root
Brain stem nucleus (Cranial Nerve)
Autonomic
Targets smooth muscles, glands, cardiac muscles
2 different peripheral motor neurons
Preganglionic
cell bodies in brain stem nucleus, axon exits through CNs
OR motor nucleus → cell body in lateral gray horns, exits the ventral root
Postganglionic
found in peripheral ganglion
Neurotransmitters
Transmits nervous signal across a synapse OR between neuron and target
Somatic NS
NT is ALWAYS ACH → acetylcholine
binding receptors on targets, causing greater potential = action potential
Excitatory NTs, increasing target activity
Autonomic NS
Synapsing between pre- and postganglionic neurons, NTs is always ACH
Cross the synapse, binding receptors of the cell body of postganglionic
Depolarises to (- to +) to neuron, causing graded potential and leading to an action potential
Signals to be transmitted across synapse + reach target
The synapse between postganglionic and target organs
Acetylcholine
Noradrenalin released by postganglionic neuron
Depending on type of receptor that target has, NA:
Excitatory → increasing target activity
Inhibitory → reducing target activity
Sympathetic vs Parasympathetic NS
Similarities:
Serving many of the same organs
Pre- and postganglionic neurons
Preganglionic release Acetylcholine
Presence of ganglia (cell bodies in PNS)
Differences:
Both divisions don’t innervate ALL organs
Location of preganglionic cell bodies + axons exit points
Length of axons, location of ganglia
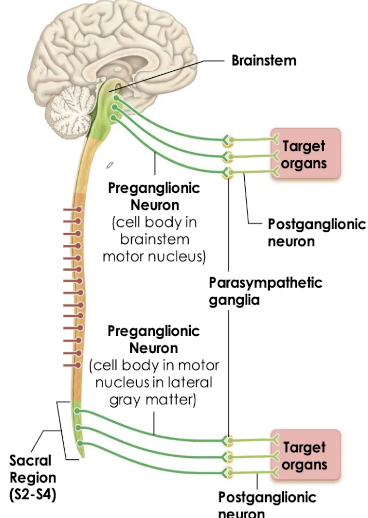
Parasympathetic NS - Craniosacral Division
Preganglionic neurons arise from opposite ends of the CNS
Preganglionic: Long Axons → postganglionic
Postganglionic: Short axons → target organs
Brain stem (cranial nerves)
Cranial pathways
CN III: Oculomotor nerve
CN VII: Facial nerve
CN IX: Glossopharyngeal nerve
CN X: Vagus nerve (organs)
Sacral region (S2-S4), (spinal nerves) -> lateral grey matter
Pelvic organs
Distal portion of large intestine
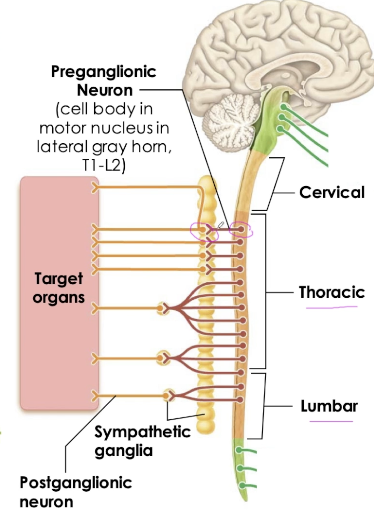
Sympathetic NS - Thoracolumbar Division
Preganglionic fibres arise from T1-L2
Cell bodies in motor nuclei of lateral grey horns, axons exit through spinal nerves
Ganglia is close to spinal cord
Pre- axon: short
Post- axon: long
Chain of 23 connected by fibres,
to form sympathetic trunk
Located on both sides of vertebral column
Extend from neck to pelvis
Segments T1-T6 innervate the head and thorax
Segments T5-L2 innervate abdominopelvic organs
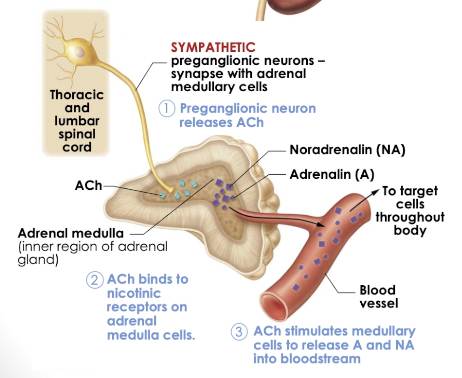
Adrenal Medulla
Adrenal glands are located on top of the kidneys
Medulla - inner region
Release Adrenaline and Noradrenaline into blood
Axons innervates adrenal medulla
release ACH when an action potential reaches axon terminal
Stimulates medullary cells to release adrenaline and noradrenaline
Affecting any cell bearing adrenergic receptors
Enhance and prolong sympathetic response → widespread
Single preganglionic neuron can synapse with many postganglionic, to active multiple effectors
CHOLINERGIC RECEPTORS (NTs)
Acetylcholine (ACh)
Cholinergic receptors
Nicotinic : EXCITATORY
increasing target activity
ALL ANS postganglionic neurons
Skeletal muscles
Sympathetic Division
Muscarinic : EXCITATORY OR INHIBITORY
excitation of most targets (Increasing activity)
Inhibition of cardiac muscles (decreasing activity)
ADRENERGIC RECEPTORS (NTs)
Alpha (1-2)
A1: blood vessels (except heart, liver, skeletal muscles) - all sympathetic targets
Excitatory and increasing activity
constricting blood vessels and visceral organs, dilating pupils
Beta (1-3)
B1: Heart
Excitatory, increases heart rate and force of contraction
B2: Airways, blood vessels (heart, liver, skeletal muscles), digestive tract, urinary organs
Inhibitory, decreasing activity → relaxing smooth muscles
Dilates airways, blood vessels, relaxes muscles in digestive and urinary organs
Receptors → Symp + Parasym
Preganglionic releases ACh = cholinergic receptors
ACh binds to cell bodies of postganglionic neurons = cholinergic nicotinic receptors
Postganglionic
Sympathetic = Noradrenaline
Adrenergic receptors, Alpha or Beta
Parasympathetic = ACh
Cholinergic receptors, Muscarinic
Effects of NTs on Targets
Synaptic Transmission
Action potential arrives at axon terminal
Voltage-gated Calcium 2+ channels open, Ca2+ ions enters
Ca+ entering, triggering the vesicles (filled with NT) to fuse with the plasma membrane of the terminal, releasing NTs into synaptic cleft
NT diffuses across the cell to bind receptors (chemically gated ion channels) on the postsynaptic membrane
Binding of the NT open the ion channels, graded potential, threshold = action potential
NT effects end when diffuses away, through enzymatic degradation or taken back up by axon terminal to be stored and reused
Postsynaptic Potential
AKA graded potential
EPSP - Excitatory Postsynaptic Potential
Neurotransmitters bind receptors on the postsynaptic membrane
Opens gated ion channels
Graded depolarisation (Na+ ions entering the cell, - to +)
Postsynaptic cells are EXCITED!!, membrane potential closer to threshold
Action potential is more likely to occur
= Increased target activity
IPSP - Inhibitory Postsynaptic Potential
Neurotransmitters bind receptors on the postsynaptic membrane
Open gated ion channels
Graded hyperpolarisation (K+ exit the cell, - to --)
Postsynaptic cell are INHIBITED, membrane potential further from threshold
Action potential is less likely to occur
= Decreased target activity
Drugs with Target Neurotransmitter Receptors
Agonists - mimicking the action of the NT
Antagonists - bind to receptor and block the action of NT
Affect the sympathetic targets
Adrenergic
B1 receptors -> Cardiac muscle
Normal response: increasing cardiac activity = increasing BP
Typical agonist drug (increasing) = dobutamine
Type antagonist drug (blocking) = beta blockers -> propranolol or timolol
B2 receptors -> smooth muscles in airways, blood vessels
Normal response: dilation of airways, blood vessels to increase airflow + blood flow
Typical agonist drug = Albuterol (Asthma puffers)
Typical antagonist drug = Beta blockers -> propranolol
Central NTs and Major Effects
(in the CNS)
Induce excitatory or inhibitory responses in the postsynaptic membranes -> 50 neurotransmitters identified
Neuropsychological disorders are traditionally thought to be caused by imbalances in neurotransmitters, but now questionable
Acetylcholine (ACh)
Motor control outside CNS
Released by:
Somatic lower motor neurons
Parasympathetic postganglionic neurons
Within the CNS
cerebral cortex - cognition
hippocampus - memory
brain stem - consciousness
Low levels of ACh found in Alzheimer's patients
Biogenic Amines
broadly distrbuted in the brain, emotional behaviours
Regulate our biological clocks
Imbalances associated with mental illness (no consistent evidence)
However, drugs that enhance the release of these neurotransmitters or block the uptake are associated with relief of symptoms -> but we don’t know how they work :(
Noradrenaline
(feel good)
Stimulates brain reward and pleasure centres
Involved in reducing stress, enhancing attention
Amphetamines: stimulant for CNS
Can treat ADHD, help to improve cognitive control
Dopamine
Stimulating brain reward, pleasure centres
High levels noted with schizophrenia
Deficient in Parkinson's disease
Serotonin
Mood regulation, sleep, appetite, nausea, migraines/headaches
GABA
Main inhibitory neurotransmitter in brain
Regulate sleep and wakefulness
Involve in motor control -> regulate skeletal muscle tone, by dampening activity
GABA blockers: convulsions, rapid repeated muscle contractions
Enhancing GABA (alcohol intake) = increase in dampening effect, impaired motor coordination
Glutamate
Excitatory neurotransmitter
Involved in learning and memory
Excessive release = excitotoxicity, overexcited and kill surrounding neurons
CVA, Alzheimer's disease
Substance P
Produced by damaged tissue
Stimulates peripheral nociceptors (pain)
Mediates pain transmission to the CNS
Endorphins
Includes endorphins and enkephalins
Inhibit perception of pain in CNS
Natural opiates, chemically similar to morphine (agonist), reduces pain, induce sleepiness, wellbeing
Special Senses
Smell, taste, see, hear and maintain balance
Specific information to specialised receptors
Stimuli detected by special senses:
Chemical molecules → taste and smell, chemoreceptors
Movement of fluids → hearing and balance, mechanoreceptors
Light (vision) → photoreceptors
Physiology + Neural Pathway of Olfaction
Smell → olfactory sensory neurons
located in the olfactory epithelium
hav cilia, surrounded by mucus
Odourant must be gaseous / volatile
Must reach olfactory epithelium, dissolved in mucus
odourant binds and opens gated channels → generating action potential
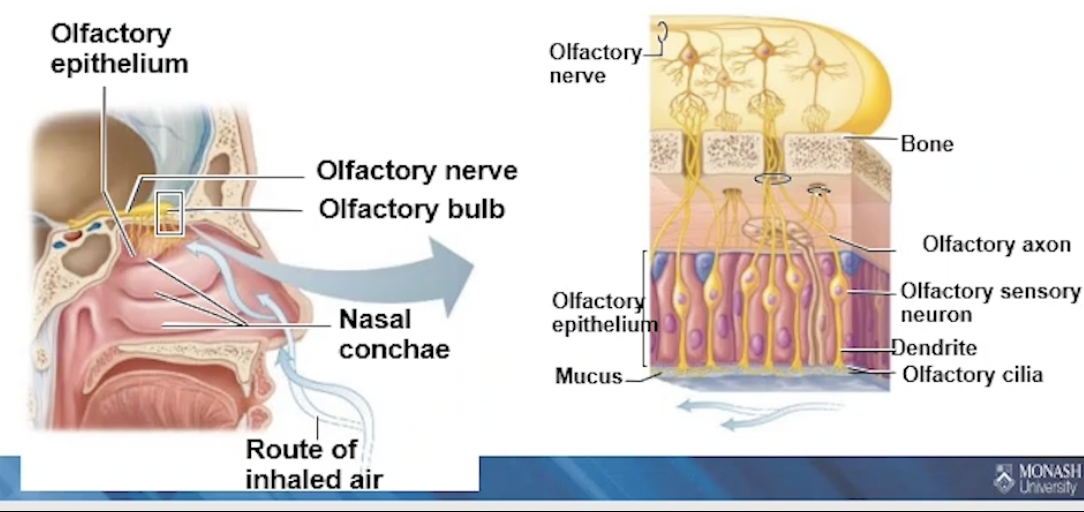
Olfactory Pathway
Olfactory sensory neurons (CN 1)
Action potentials travel to olfactory cortex of temporal lobe
2 different pathways
Frontal lobe
Hypothalamus + limbic system: emotional response to odour elicited
Role of Nose and Smell
Nociceptors
Thermoreceptors
→ smells can also signal danger: smoke/gas
Triggering fight or flight response
Protection by triggering sneezing and choking → in response to unpleasant odourants
Physiology + Neural Pathway of Gustation
Taste
Gustatory epithelial cells in taste buds
→ microvilli (gustatory hairs)
Food chemicals dissolved in saliva (chemoreceptors)
Gustatory Pathway
Cranial Nerves:
VII → Facial
IX → Glossopharyngeal
X → Vagus
→ all carry action potentials from taste buds to:
gustatory cortex in the insula
hypothalamus nd limbic system (appreciation of taste)
Role of Mouth and Taste
Taste sensations
Nociceptors
Thermoreceptors
Triggering reflexes involved in digestion
secretion of saliva, gastric juice
Protective reactions
gagging, reflexive vomiting
5 tastes -> homeostatic value
Influence food choices that help satisfy our body's needs
Control quality of food that will be ingested
Sweet = energy, carbohydrates
Bitter = warning (vomiting)
Sour = unripen, or spoilt food
Salty = mineral and water balance
Umami = protein rich foods
Influence of Smell on Taste
Combined effect when interpreted in cerebral cortex → 80% of taste is smell
Anatomy of the Ear
External → hearing
Middle → hearing
Internal → hearing and balance
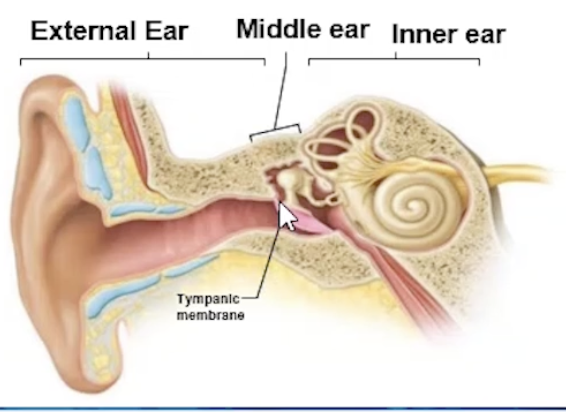
External Ear: Structures and Functions
Auricle / Pinna 👂
Funnels sound waves into the external acoustic meatus
External Auditory Meatus
Sound waves enter EAM, travel to vibrate the tympanic membrane
Tympanic Membrane (Eardrum)
Thin, translucent membrane
Vibrates in response to sound waves, transfers sound energy to bones of middle ear
Mechanical energy to auditory ossicles
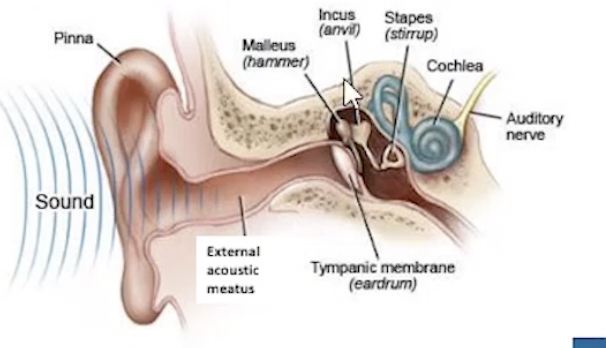
Middle Ear: Structures and Functions
Tympanic Cavity
air-filled cavity in temporal bone
Tympanic membrane is lateral to CAVITY
Bony wall is MEDIAL to cavity
i.e. cavity lies in between both
Bony wall = oval and round window
Auditory ossicles = malleus, incus, stapes
Pharyngotympanic tube: connects middle ear to nasopharynx
Equalises air pressure in middle ear cavity
→ open to nose and throat, microorganisms can travel and cause infections
*middle ear infections can cause tympanic membrane to be inflamed and red
more common in children
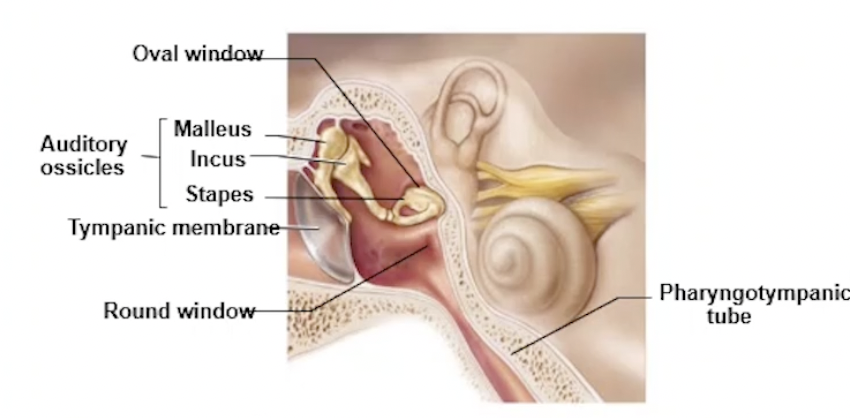
Auditory Ossicles (mid ear)
Malleus
Incus
Stapes
→ transmit and amplify the vibratory motions of tympanic membrane to the oval window
Bony Wall: Oval and Round Window (mid ear)
Oval
Opening in the bone, partitions middle ear to start of cochlea
Movement causes pressure waves within perilymph
Round
thin membrane that separates end of cochlea from middle ear
absorbs pressure waves
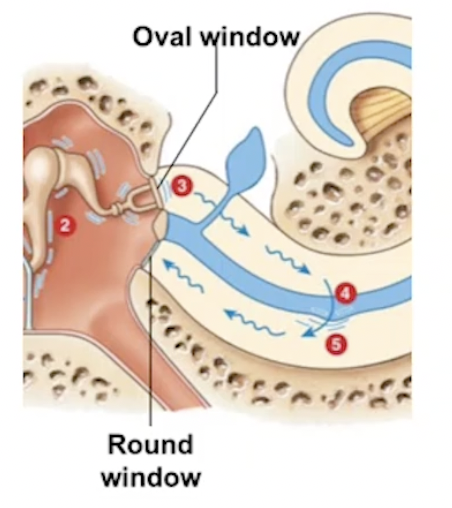
Inner Ear: Structures and Functions
Temporal Bone
2 divisions of internal ear
Bony Labyrinth
Vestibule
Semicircular canals
Cochlea
Filled with perilymph
Membranous Labyrinth
Series of interconnecting sacs and ducts
Within the bony labyrinth
Filled with endolymph
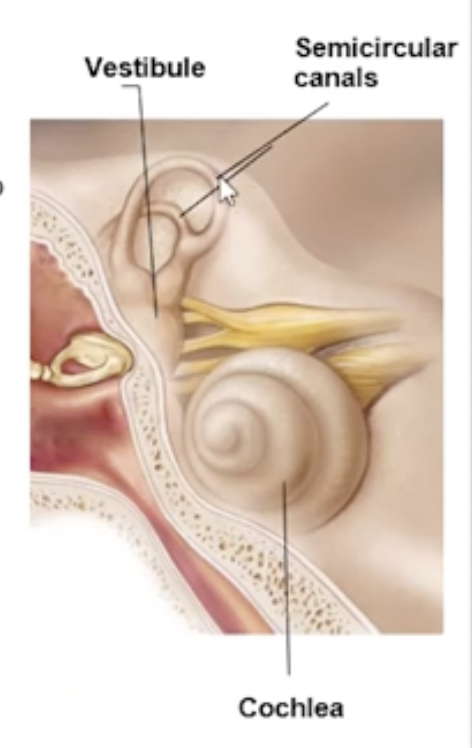
Cochlea (inner ear)
Spiral, bony chamber, extends from vestibule
→ contains the cochlear duct, housing the spiral organ of corti
Cochlear Nerve → Cranial Nerve VIII: Vestibulocochlear
→ contains 3 chambers:
2 perilymph, 1 endolymph
→ Membranous Labyrinth → cochlear duct (endolymph)
basilar membrane = floor of duct
Spiral Organ: on top of basilar membrane, with cochlear duct
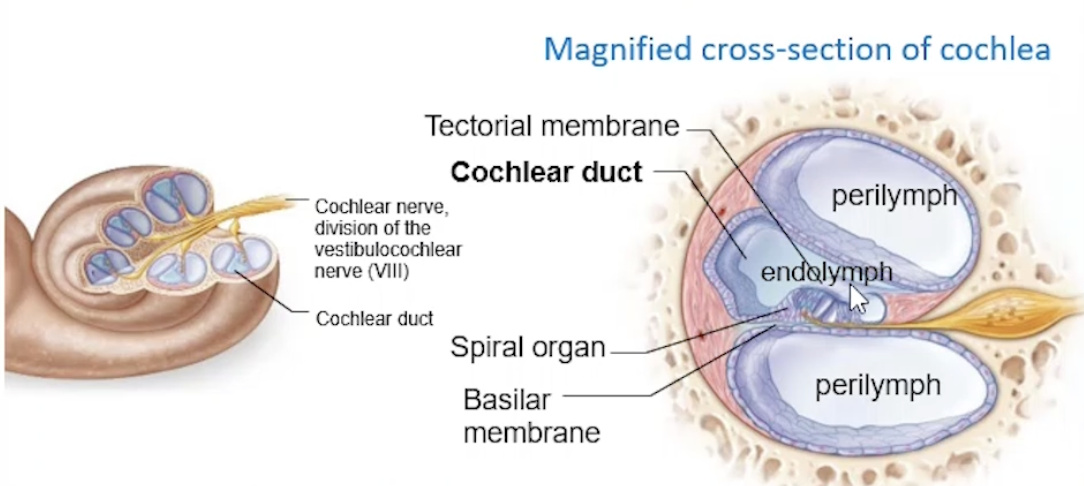
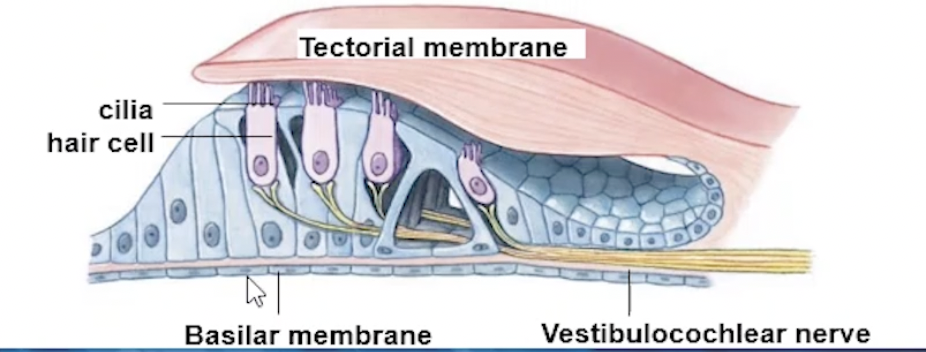
Spiral Organ (within Membranous Labyrinth)
Detects sound, organ of hearing
Composed of cochlear/cilia hair cells
Embedded in tectorial membrane
mechanoreceptors, auditory receptors
Pressure waves travel through perilymph of cochlea = movement of basilar membrane
this causes the hair cells to move or bend against tectorial membrane
= initiating a depolarisation = generating action potentials
sent to CN VIII: Vestibulocochlear nerve for interpretation
Cochlea + Stapes
Embedded in oval window, wall of bony labyrinth
stapes moves back and forth in response to mechanical movement
sound waves hit tympanic membrane
When moving back and forth, pressure waves are created within perilymph (in vestibule)
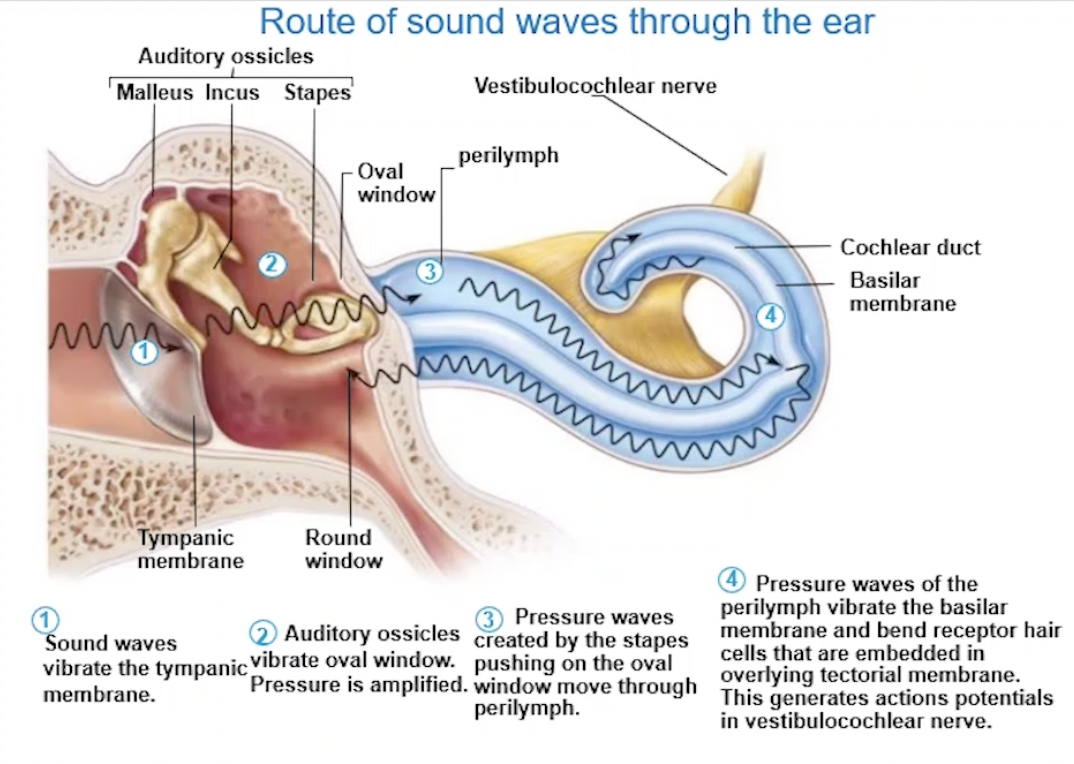
Route of Sound Waves Through Ear
Sound waves vibrate the tympanic membrane (funnelled through by pinna and EAM)
Auditory ossicles vibrate oval window + pressure is amplified
Pressure waves created by stapes pushing on oval window move through perilymph
Pressure waves of perilymph vibrate basilar membrane
Receptor hair cells embedded in tectorial membrane get moved/bent
Creating action potentials in vestibulocochlear nerve
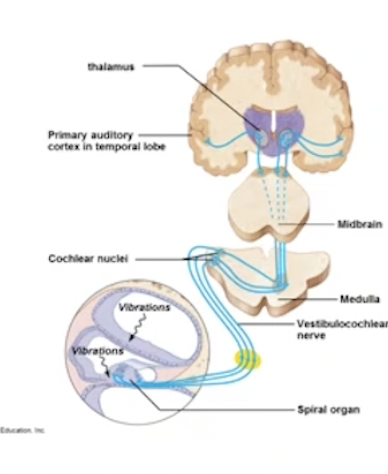
Auditory Pathway to Brain
Bending of hair cells in Spiral Organ
opens sodium ion channels, sodium rushes in = generating action potentials in auditory neurons
Axons of auditory neurons for the cochlear branch of CN VIII
Action potential travels to:
Medulla oblongata → auditory reflex centre of midbrain
To the auditory cortex (temporal lobe) → stimulus interpreted as sound
Balance / Equilibrium
Response felt by head movements
Role of equilibrium: providing information about location and movement of head
Equilibrium depends on inputs from external ear
As well as: Vision and Information from proprioceptors of muscles nd tendons
Mechanoreceptors for equilibrium are found in the inner ear, specifically:
Vestibule
Semicircular Canals
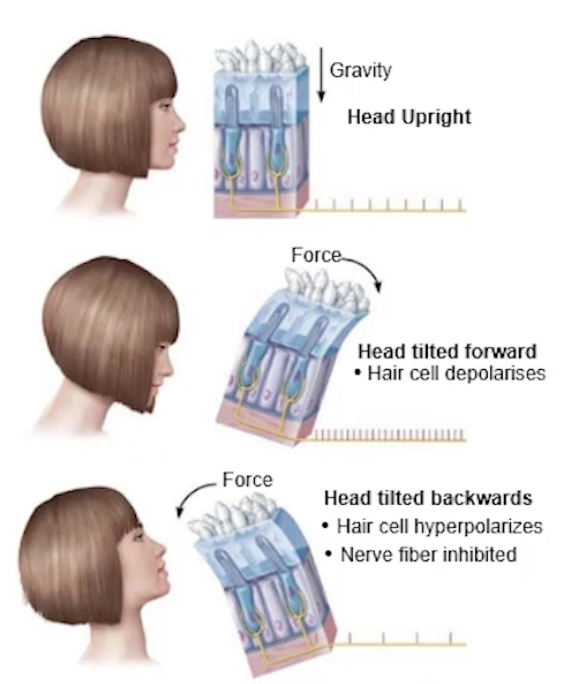
Static vs Dynamic Equilibrium
Static
Position of head, relative to gravity + forwards/backwards
motionless, moving in a straight line
→ when head positions move, gravity pulls on stones, distorting jelly
→ Bending the hair cells in the vestibule
Forward = depolarisation
Backward = hyperpolarisation
Dynamic
Evaluating position of head while it is rotating, or moving in an angular direction
→ detected by hair cells in the semi circular canals
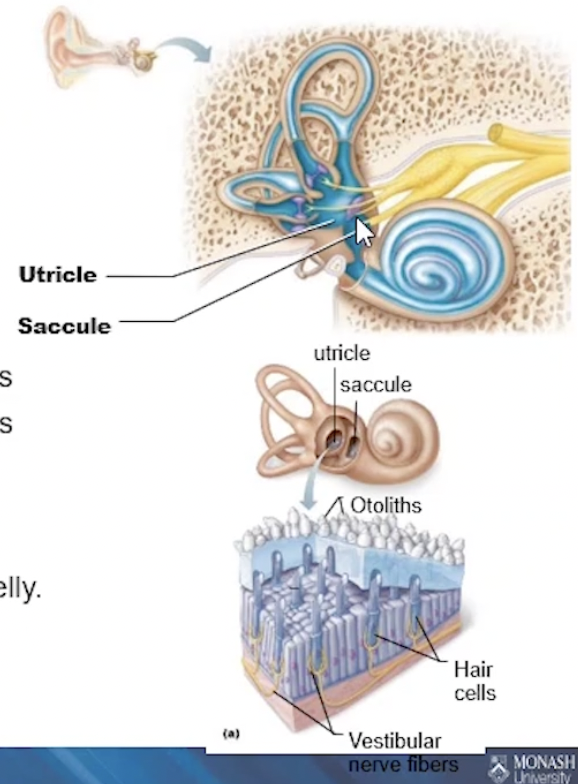
Vestibule
2 membranous sacs, containing equilibrium receptors
→ embedded in jelly-like substance
→ Ear stones (called otoliths) embedded into the jelly
Saccules: continuous with the cochlear duct = static
Utricles: continuous with the semicircular canals = dynamic
Semicircular Canals
3 fluid filled canals
Equilibrium hair cells respond to the rotational movement of head
Hair cells are surrounded by endolymph
Angular movement moves the endolymph, bending and distorts hair cells
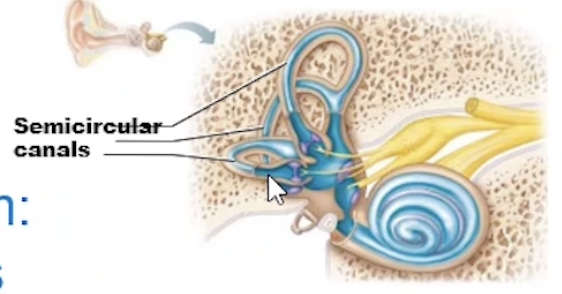
Equilibrium Pathway
Distortion of the hair cells stimulates depolarisation of vestibular division (CN VIII)
Action potentials travel to the:
Reflex centres of brainstem (vestibular nuclei)
Cerebellum
Vestibular cortex of insula
Maintaining Balance
Hair cells distorted in response to stimulus
Linear movement (vestibule) and rotational movement (semicircular canal)
Stimulate depolarisation of the vestibular division (CN VIII) + cochlea division -> sent to brain
Action potentials travel to vestibular nuclei (brain stem)
Integrative centre for balance
Sends commands to brain stem motor centres
Direct eye movement and reflex actions of the neck, limbs and trunk
Adjust body positions to maintain/regain balance
Sends information to the cerebellum
Comparing where the body is now to where it should actually be
Reaches vestibular cortex of the insula, becoming consciously aware of our balance (where position is in space)
Vision
Dominant sense
→ 70% of our sensory receptors are found in eye
→ half of the cerebral cortex is involved in some aspect of visual processing
Movement of the Eyeball
6 eye muscles
Innervated by Cranial Nerves:
III - Oculomotor
IV - Trochlear
VI - Abducens
Motor movement of eyeballs**
Enables eyes to be fixed on objects
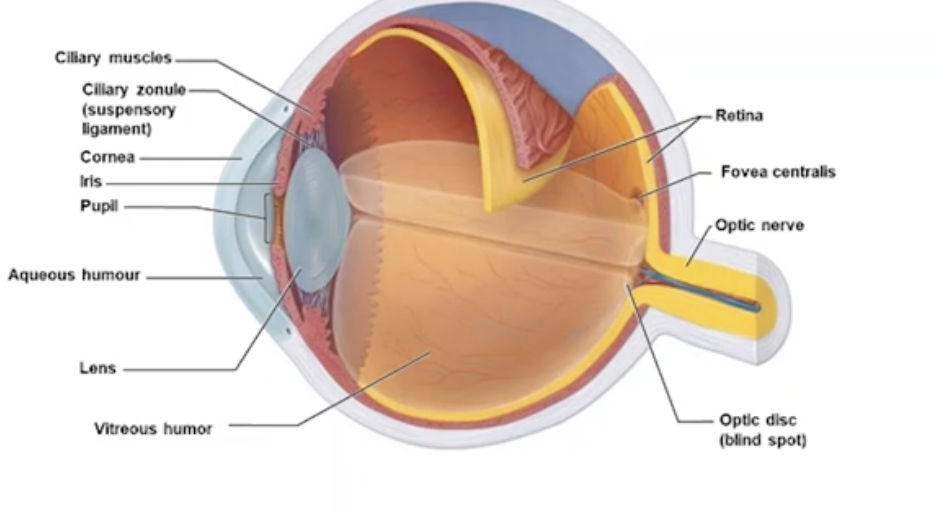
Structure of the Eyeball
Cushion of fat and walls of bony orbit
Cornea
most exposed, transparent layer of the eye
Forms window to let light in, no blood
Transplanted between individuals
Well-supplied with nerve endings → nociceptors
Reflexive blinking when touched
Iris
Coloured part of the eye
Adjustable diaphragm, controls the diameter of round central opening (pupil)
Contains muscles that constrict and dilate
Controlled by Sympathetic/Parasympathetic
Lens
Transparent and flexible, changing shape to focus light on the retina
Suspensory ligaments hold in place
Round and thickened
Pupil
Round and central
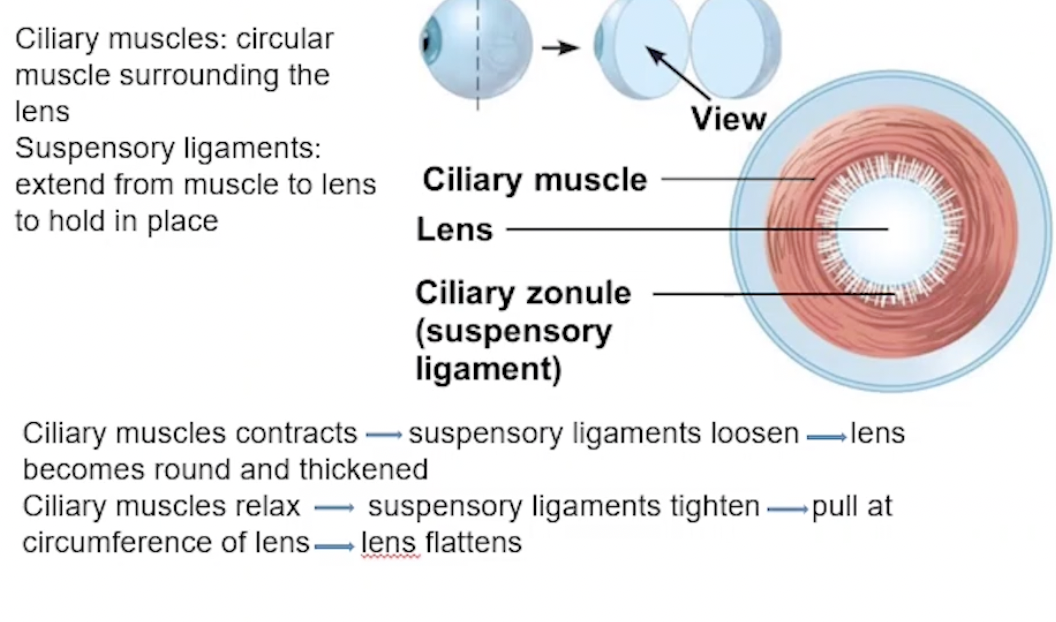
+ Ciliary Muscles and Zonules
Ciliary Muscles - Distant and Close Vision
Suspensory ligaments (zonules) - extend from ciliary muscle to lens to hold in place
Round and thick lens = ciliary muscles contract, suspensory ligaments loosen
Close vision, parasympathetic NS
6 metres>, reflect lights on divergent paths
Requires refraction to direct onto retina
Accommodation = lens gets fatter
Convergence of eyeballs required
Constriction of pupil, decreasing diameter to prevent the MOST divergent rays from entering
Flattened lens = ciliary muscles relax, suspensory ligaments tighten
Distant vision, sympathetic NS
6 metres<, light rays that are parallel to each other
Light rays will focus on retina, lens flattened
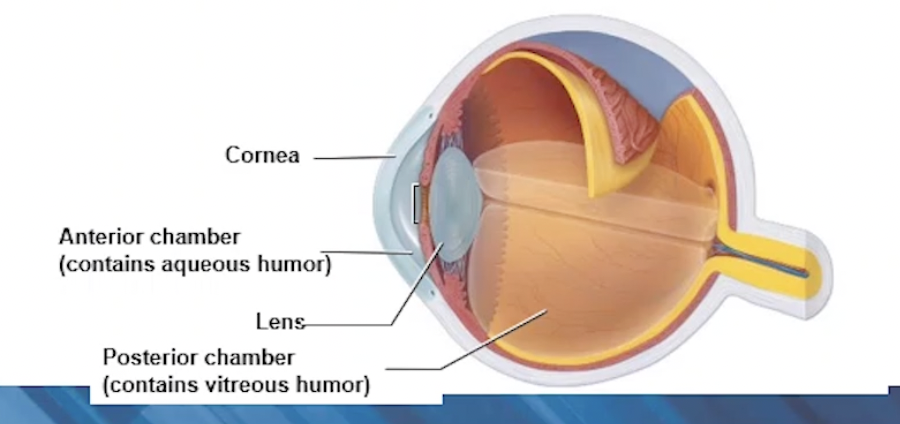
Internal Chambers and Fluids of Eyeball
2 Chambers:
Anterior (between cornea and lens)
Aqueous humour → nutrients and oxygen to lens and cornea
Posterior (behind the lens)
Vitreous humour: gelatinous substance, supporting posterior surface of eye → retina
Layers of the Eyeball
Fibrous (outer layer)
Sclera
White, tough connective tissue
Continuous with dura mater of brain
Cornea
Transparent region of front of eye
Vascular
Choroid
Vascularised area
Blood vessels nourish all layers
Brown pigment produced by melanocytes
absorbs light, prevents from scattering and reflecting inside eye
Ciliary Body
forms ciliary muscle rings around lens
Iris
Adjustable muscle layer
Retina (inner)
Nervous layer
Contains photoreceptors - light detecting receptor cells
Rods → dim light, peripheral vision
Cones → bright light, colour and visual activity
Fovea centralis → visual activity
Most cones, enhanced visual activity and detailed colour
Optic disc → blind spot
Optic nerve exits eye
Lacks photoreceptors
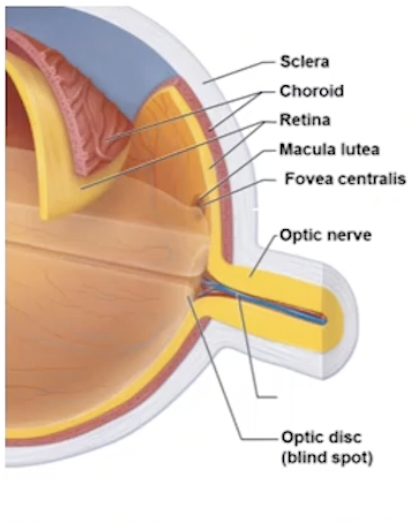
Light on the Retina
Refraction
Bending of light through different mediums → cornea, aqueous humour, lens, vitreous humour
Light travels in a straight line, until hitting an object or medium
Light reflects off of objects
Light gets refracted/bent through mediums
Pathway of Light into Eye
Cornea
Aqueous Humour
Lens
Vitreous Humour
→ combined effect of all refractions = focus on the image in retina
refraction is constant for all, EXCEPT the lens
Lens is highly elastic, can change shape to focus
More convex and fat = bigger refraction
Converting light to Action Potentials
Focused on retina (photoreceptors)
Rods contain Rhodopsin, which is sensitive to light
Light promotes breakdown of Rhodopsin = cell membrane depolarises = action potential
Cones are similar, with a different type of Rhodopsin
Pathway of signals from Eye to Brain
Light Into the Eye
Cornea → Aqueous Humour → Lens → Vitreous Humour → Retina
Photoreceptors of retina create action potential, travelling through Cranial Nerve II - Optic Nerve
Light through the Brain
Optic nerve → Optic chiasma → Optic Tract → Thalamus
→ Optic Radiations to Primary Visual Cortex in the Occipital Lobe
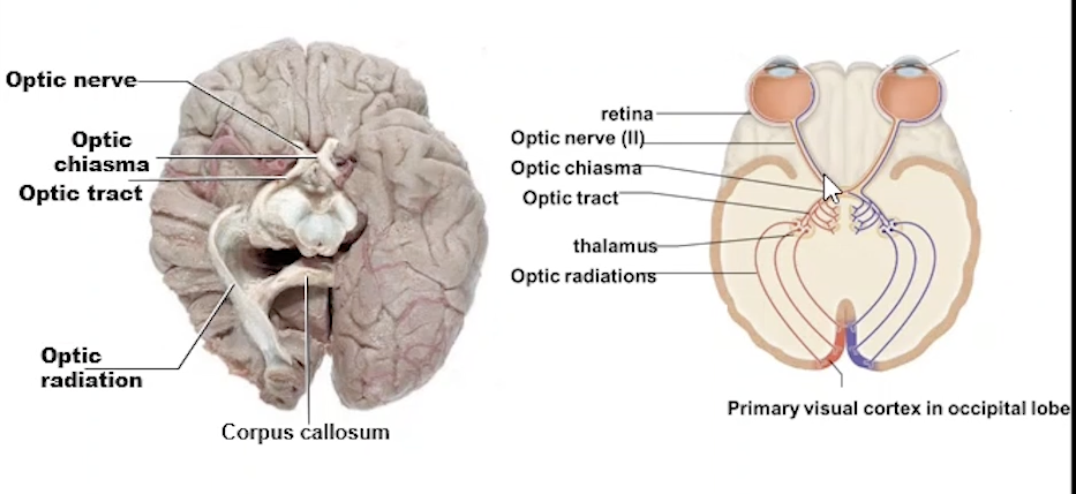
Binocular Vision and Depth Perception
Field of vision overlaps
2 optic nerves meet at the Optic Chiasma (overlapping point)
Medial fibres cross to the other side
Both hemispheres of brain receive visual images (from both eyes)
Visual cortex fuses the 2 images, providing depth perception