Dental Anatomy - Exam 1
1/68
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
69 Terms
What is the name of the system of teeth for chewing?
Masticatory System
What approach should you have in complete dentistry?
Identify and treat causative factors rather than just the symptoms (in these cases, it may be occlusal interference)
4 Parts of Complete Dentistry
Optimum Oral Health
Anatomic Harmony
Functional Harmony
Occlusal Stability
Optimum Oral Health
Plaque control
Periodontal status
Finding cause of problems
Fixing misdirected occlusal forces
Anatomic Harmony
Muscles and TMJ function as expected w/o interference
Anatomic shape of teeth corresponds with function
Functional Harmony
Mastication w/o interference
Can easily function to limit or remain at peace
Occlusal Stability
Horizontal stability of teeth (tongue muscle)
Vertical stability of teeth (opposing arch)
Benefits of Complete Dentistry
Increased patient comfort
Restoration longevity
Occlusal stability
More accurate treatment planning
Improved esthetics
Increased productivity
Decreased stress
Diagnostic Appointment Steps
Chief Complaint
Medical History
Conditions affecting treatment methodology
Systemic Conditions w/ Oral manifestations
Conditions affecting treatment plan
Risk factors to dentist and auxiliary personnel
Review of systems
Dental History
Comprehensive Dental Exam
Maxillary/Mandibular Alginate Impressions (one of many tests done to examine oral health)
Alginate Impression General Info
Irreversible Hydrocolloid where alginic acid solution is converted to calcium alginate as gel
Water makes up 50% of composition
Hydrocolloid should be poured 12 minutes before removal
Alginate Impression Tools
Impression material
Rubber bowl
Beaver Spatula
Disposable Tray
Adhesive for Alginate
PPE
Any other equipment for modifications like Hanau Torch or rope wax
Impression Tray Details
Perforated for retention
Need adhesive
Can be disposable or metal and size small, medium, or large
Ideally have ¼ inch alginate thickness
Alginate Impression Technique
Select tray and adhesive
Add powder to water and mix for 45-60 seconds
Load the tray
Position yourself in front of patient for mandibular and behind patient for maxillary
Use mirror to retract cheek and seat tray in rolling motion from posterior to anterior without applying pressure
Remove tray carefully with fingers under vestibular flange
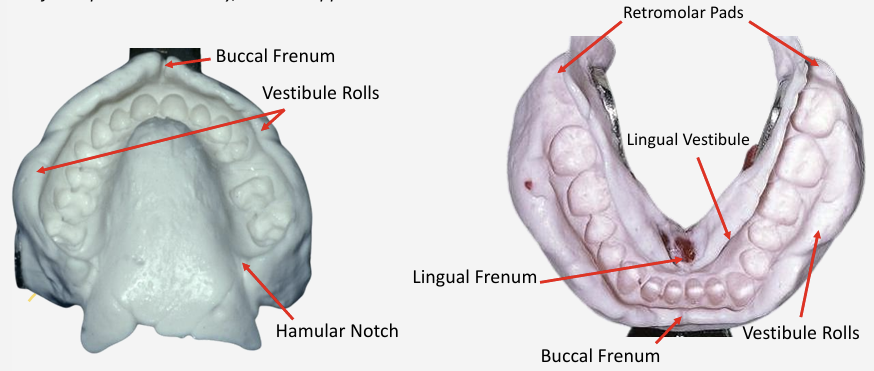
Features to see in Impressions
Maxillary
Vestibule Roll
Buccal Frenulum
Hamular Notch
Mandibular
Vestibule Roll
Buccal Frenulum
Lingual Frenulum
Lingual Vestibule
Retromolar Pads
Pouring and Making Cast
Impression must be removed within 12 minutes of being made
Rinse disinfectant from impression and remove excess water
Use exact W/P ratio
Vacuum mix stone for 15 seconds
Carefully vibrate into impression and use 2-step pour technique
Remove from alginate in 45-60 minutes
Trim casts to fit base former
Use super-sep to index grooves
Facebow
Instrument to record spatial relationship of maxillary arch to reference point
Orients dental cast to opening axis of articulator
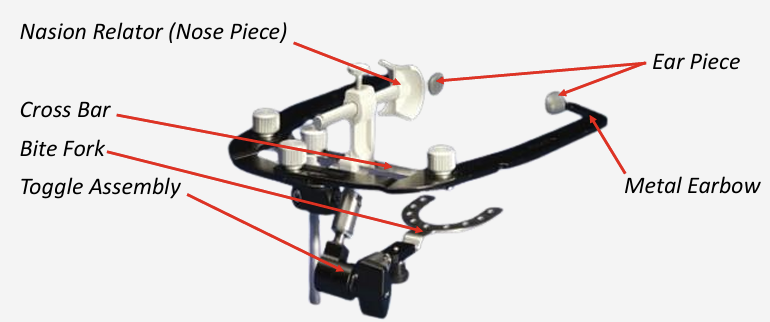
Components of Facebow
Nasion Relator
Ear Piece
Metal Earbow
Cross Bar
Bite Fork
Toggle Assembly
Facebow Record Equipment
Clean facebow and bitefork
Toggle Assembly
Blue Mousse
Red Handle Knife
Necessary PPE
Interocclusal Record
Spatial relationship between max and man teeth
Reproduces patient’s occlusal plane and arc of closure
Reference points used: Maximal Intercuspal Position and Centric Relation
Articulator Classes
Class 1 - Vertical motion only and non-adjustable
Class 2 - Permits horizontal and vertical motion but no TMJ movement
Class 3 - Simulates condylar pathway using mechanical equivalents of motion (semi-adjustable)
Arcon type have adjustable Bennet angle corners
Class 4 - 3D dynamic registrations used to orientate the cast to TMJ and simulate mandibular movements (adjustable)
Articulator Settings
Condylar Guidance is 30 degrees
Immediate Sideshift should be set to 0
Latch is closed
Pin set to 0 mm
Temporomandibular Joints
Right and left TMJs are interdependent
Changes in occlusion, attrition, or loss of teeth affects loading patterns of TMJ
Structures around TMJ
Mandibular Fossa
Has V-shaped contour to allow medial pole of condyle to fit and have rotational movement
Articular Surface of Condyle
Posterior aspect has greater articular surface
Soft Tissue Components
Articular Disc
Retrodiscal tissue
Muscles of Mastication and other structures
Deep Portion
Lateral Pterygoid
Superior head
Inferior head
Medial Pterygoid
Superficial Portion
Temporalis
Masseter
Suprahyoids
Tongue muscle
Buccinator
Capsule of Temporomandibular Joint
Temporalis
Origin - Inferior temporal line and fossa
Insertion - Coronoid Process and anterior ramus
Action - Elevates mandible (anterior and middle fibers) or retrudes mandible (posterior fibers)
Masseter
Origin - Zygomatic Arch
Insertion - Lateral surface of ramus and angle of mandible
Action - Elevates mandible
Medial Pterygoid
Origin - Medial surface of lateral pterygoid plate, pyramidal process of palatine, maxillary tuberosity
Insertion - Medial surface of ramus and angle of mandible inferior to mandibular foramen
Action - Elevates Mandible
Superior Head of Lateral Pterygoid
Origin - Greater wing of sphenoid and infratemporal crest
Insertion - Articular disc and neck of condyle
Action - Protrudes, moves mandible side to side
Inferior Head of Lateral Pterygoid
Origin - Lateral surface of lateral pterygoid plate
Insertion - Pterygoid fovea on the neck of condyle
Action - Depresses mandible
Which muscle is responsible for elevating, closing, or raising jaw?
All muscles of mastication except inferior head lateral pterygoid.
Which muscle is responsible for depressing or opening jaw?
Inferior head of lateral pterygoid and suprahyoid muscles.
What is responsible for elevation, depression, retrusion, protrusion, and lateral excursion?
Elevation
Ipsilateral Medial Pterygoid
Contralateral Masseter
Contralateral Temporalis
Depression
Contralateral Inferior Head of Lateral Pterygoid
Suprahyoid (such as anterior belly digastric and mylohyoid)
Infrahyoid
Retrusion
Temporalis
Masseter (deep)
Protrusion
Lateral Pterygoid
Medial Pterygoid
Masseter
Lateral Excursion
Ipsilateral Masseter
Contralateral Medial Pterygoid
Condylar Movement in Working and Balancing Side
Working Side
Rotation
Balancing Side
Orbiting (involved in translation and rotation of condyle)
Full Intercuspation, Opening Phase, End of Closing Phase
Full Intercuspation
Buccal cusps of mandibular molars are medial to buccal cusps of maxillary molars
Opening Phase
Buccal cusps of mandibular molars on working side is more lateral than usual
End of Closing Phase
Mandible is drawn toward midline
Bolus is subjected to vertical and horizontal shear forces by opposing molar cusps
What is considered as the power stroke during mastication?
The end of the closing step when teeth are crushing food bolus while resting between opposing cusps and fossae
Random Additional Info at the end of Spears Lecture
Articular disc rotates relative to condyle
Forces are transmitted to mandibular condyle during chewing and biting
Temporomandibular Disorder (TMD) causes clicking, internal derangement, joint degeneration, limited movement, and pain
Anatomical (occlusal contact area, malocclusion), physiological (muscle strength, gender, age), and psychological components all affect occlusion
Masticatory performance is objective and affects, food breakdown, nutrition, digestion, and much more
Number of occlusal contacts influences maximum bite force
Class II and III patients have lower masticatory performance but not cared for clinically if patient is not compromised
Occlusion and Determinants of Occlusion
Occlusion - Contact between maxillary and mandibular teeth
Determinants - Both TMJs, permanent dentition, and neuromusculature
Anterior teeth are active determinants; posterior teeth are passive determinants
Intercuspation and Interdigitation
Intercuspation is the cusp-to-fossa relationship of upper and lower teeth
Interdigitation is intercuspation but for multiple teeth
Each tooth interdigitates with two opposing teeth (provides dental arch stability)
Less distinct in molar region than other regions
Mandibular teeth interdigitate with same tooth and tooth medial to it (maxillary do opposite)
Exceptions are mandibular central incisors and maxillary third molars
Centric Occlusion
Occlusion of teeth when mandible is in centric relation
Maxillary buccal cusps line up with buccal embrasures and developmental grooves
Mandibular lingual cusps line up with lingual embrasures and developmental grooves
Maximal Intercuspation
Complete intercuspation of opposing teeth independent of condylar position
Used in articulators when occlusions can be restored in current mandibular position and no changes are planned on occlusal plane or vertical dimension
Centric Relation
Position independent of tooth contact
Condyles are in anterior-superior position against posterior slopes of articular eminence
Mandible can only rotate in this position
Bone-to-disk-to-bone relationship
Use in articulators when you plan to reorganize occlusion, when you plan to use extensive indirect restorations, or you want to make a new occlusal plane
Centric Stop
Opposing cusp/fossae contacts maintaining occlusal vertical dimension between opposing arches
Take the form of cusp to marginal ridge, cusp to fossa, or cusp to occlusal embrasure
They are usually found under or over line of central groove
Which teeth are classified as closure stoppers? What teeth protect others during protrusive movement? What teeth protect others in lateral excursion?
Closure Stoppers - Posterior Teeth
Protect anterior teeth in Centric Occlusion
Minimize load on TMJ’s
Protrusive Movement - Incisors
Lateral Excursions - Canines
Canine Protected Articulation (form of Canine Guidance or Cuspid Rise) is involved in lateral movement
Uses vertical and horizontal overlap of tooth as well as canine eminence (thick facial plate of bone) for protection
Has longest root in mouth
Anterior Guidance
Anterior teeth protect the posterior teeth and TMJs during excursive movements through posterior disclusion
Anterior teeth are considered steering wheel of occlusion
Effects of anterior guidance are most on premolars
Effects of condylar guidance are most in molars
Anterior teeth are protected by distance from TMJ because forces are closest near joint
What happens when canine guidance fails?
Group function occurs, causing contacts between several teeth and distributing occlusal forces
Restorative dentists consider modifying condylar guidance so no working contacts occur on buccal cusps of first and second molars
Condylar Guidance
Functional relation of hard and soft tissue in TMJ
The flatter the articular eminence, the shorter the cusps must be
The steeper the articular guidance, the taller the cusps may be
Anterior guidance must be equal to or greater than condylar guidance for excursive movements
Supporting Cusps vs Non-supportive cusps
Supporting Cusps
They contact opposing centric stops and do most of grinding during mastication
Non-supportive Cusps
Overlap supporting cusps
In CO, there is 0.5-1.0 mm of space between supportive and non-supportive cusps
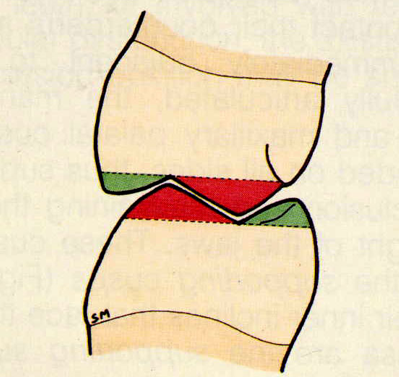
What protects the cheeks and the tongue during mastication?
Cheeks - Maxillary Buccal Cusps
Tongue - Mandibular Lingual Cusps
Posselt’s Diagram
Movement of mandibular incisal edge viewed from mid-sagittal plane
Does not represent mechanics of TMJ because in condylar position, CO may be posterior to CR
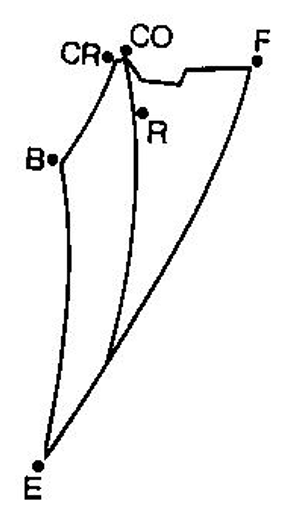
Steps of Opening Jaw from Centric Relation
First - Condyle hinges/rotates about fixed axis (hinge axis)
Responsible for recording CR at a vertical dimension
End of opening is 20-25 mm from centric relation
Second - Condyles translate or slide down articular eminences until they are over crests of articular eminences
End of opening is 40-60 mm of total opening
Working Side vs Balancing Side
Working Side
Same side as lateral excursive movement
Working side condyle rotates (moves forward/backward and upward/downward)
Bennett Movement or Immediate Sideshift
Balancing Side
Opposite side of lateral excursive movement
Balancing side condyle orbits (moving downward, forward, and medially)
Bennett Angle or Progressive Sideshift (measured around 15 degrees) corresponding to angulation of medial wall from lateral checkbite of superior wall
Tracking of Cusps in Working Side and Balancing Side
Working Side
Mesiolingual cusps of maxillary molars track out of lingual groove of mandibular molars
Distobuccal cusps of mandibular molars track out of buccal groove of maxillary molars
Balancing Side
Mesiolingual cusp of maxillary first molars track over distobuccal groove of mandibular first molars
Working vs Balancing Interferences
Working Interference
Working interferences occur between inner incline of non-supporting cusps and outer incline of supporting cusps
Cross-tooth balancing interference is a working interference between maxillary and mandibular lingual cusps
Balancing Interference
Balancing interferences occur between inner inclines of supporting cusps
Protrusive Movement
Condyles slide forward and downward on articular eminence
Mandibular incisal edges slide down lingual surfaces of maxillary incisors
Gothic Arch Tracing
Aka Gysi’s tracing or crow’s foot
Detects border movements of articulator in horizontal plane
CR-CO should be down midline and be short
If adjusted, long centric or freedom in centric may occur which is undesirable and may need othodontic treatment
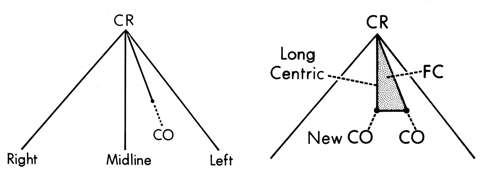
Maxillary vs Mandibular Crow’s Foot
Blue - Working
Green - Non-working
Black - Protrusive
Yellow - Lateral Protrusive
Maxillary
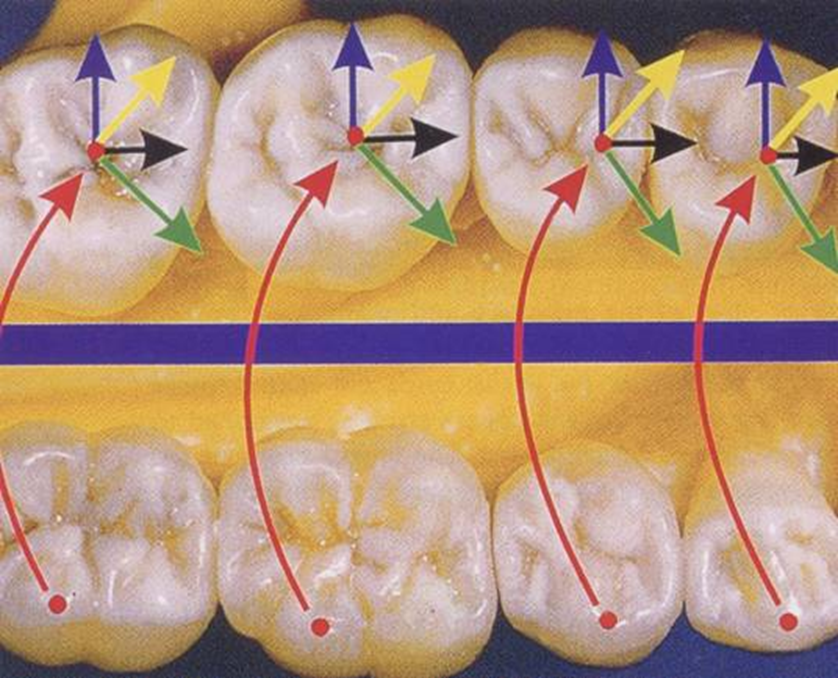
Mandibular
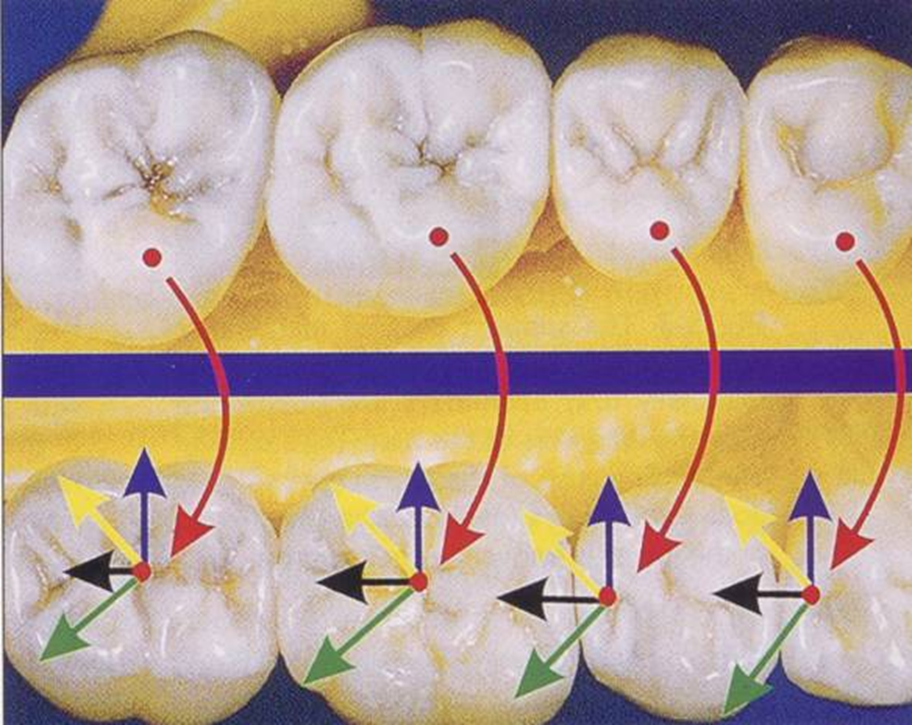
Curve of Spee
Curvature beginning in canine and following buccal cusp tips of premolars and molars
Flatter curve has less excursive interferences
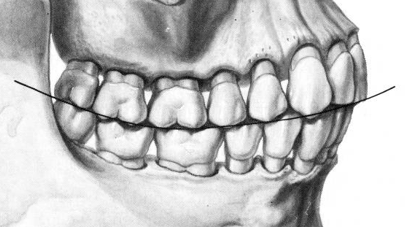
Curve of Wilson
Mediolateral curvature of occlusal plane of posterior teeth
Depresses non-supporting cusps and prevents working interferences
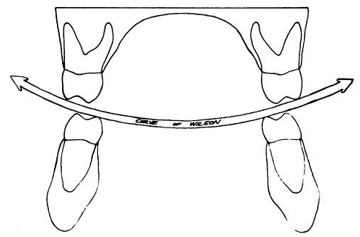
Curve of Spee + Curve of Wilson
Compensating Occlusal Curvature or Sphere or Monson
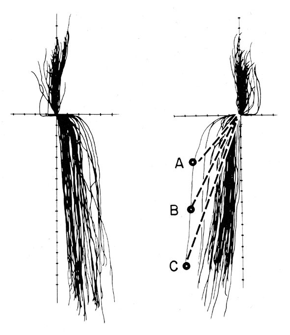
Shape of Immediate and Progressive Side Shifts
Not like A, B, or C in this image
These tracings were made using chinpoint guidance
Immediate side shift is as much as 3 mm because condyles may be distracted (CR detracts from natural seated position) which can harm TMJ
Orbiting Pathway vs Protrusive Pathway
Orbiting Pathway is steeper than protrusive pathway to prevent balancing interference
Since protrusive path is flatter, superior wall settings on protrusive record can be used for all excursive movements which can save chair time when casting restoration
Frontal Plane Border Movements
Masticatory Loop is vertical and teardrop shaped
If lateral pterygoid is paralyzed, the mandible will open to affected side
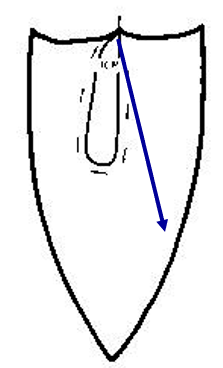
Physiologic Rest Position
Position of mandible when muscles are at minimal contraction
Freeway Space
Distance between occluding surfaces of maxillary and mandibular teeth when mandible is in rest position
Usually 2-4 mm
Malocclusion
Deviation from normally acceptable contact between opposing dental arches
Occlusal Prematurity
Contact of opposing teeth before planned intercuspation
Brain is signaled and brought to a “new” maximum intercuspation
Occlusal Forces
Should be borne along long axes of teeth to promote stability of occlusion
Primary and Secondary Occlusal Traumatism
Primary occlusal traumatism - Abnormal force placed on normal structure
This causes fremitus (tooth mobility)
After being corrected, may take several days to stabilize
Secondary occlusal traumatism - Normal force on abnormal supporting structures
Other defects that may be found because of occlusal traumatism
Anterior Diastema
Gingival Cleft
The rest of examples are not part of the exam