Liver/Digestion Anat/Reg
1/122
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
123 Terms
What increases surface area in the stomach?
gastric glands (invaginations)
What increases surface area in the small intestine?
finger like villi and invaginations called crypts
What creates mucosa? What does it do?
Mucusoal epithelium, lamina propria, and muscular is mucosae. Modifications to mucosa increase surface area.
What are Peyer’s Patches? Where can they be found?
Are organized lymphoid follicles; can be found in distal jejunum an ileum (and sometimes duodenum of SI.
What contains the submucosal plexus of the ENS? What is it made out of?
Submucosa; connective tissue.
What contains the myenteric plexus of the ENS? What is it made out of?
Muscularis Plexus; two layers of smooth muscle.
What is the serosa?
smooth epithelial membrane of mesothelioma that lines the walls of internal organs (like the SI and Liver)
What are the four basic processes of the digestive system?
Digestion , absorption, secretion, motility.
What are some challenges of the digestive system?
Avoiding auto digestion, mass balance, fluid loss via vomiting and diarrhea, defense from pathogens.
What produces mucins in the stomach?
mucous cells
What produces mucins in the salivary glands?
serous cells
What produces mucins in the intestines?
goblet cells
_____ are sustained for minutes or hours, occurs in some smooth muscle sphincters + anterior potion of stomach, and keeps the bolus from moving.
Tonic contractions
______ lasts a few seconds and occurs in the posterior region of the stomach and in the SI.
Phasic Contractions
What is peristalsis and what does it do?
Automatic, wave-like movement of muscle that line GI tract. Moves the bolus forward from when you swallow to esophagus, stomach, and intestines.
Where does the muscle contract in peristaltic contractions?
Behind the bolus
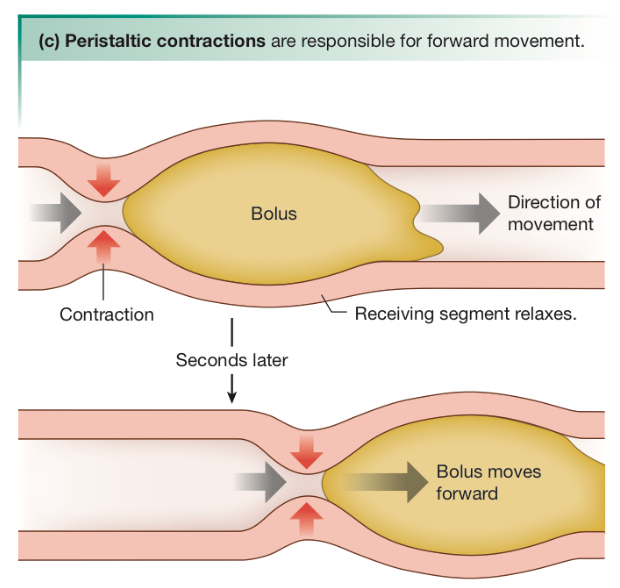
What are segmental contractions? What do they do?
Segments of the intestine that alternately contract and relax, which mixes the content of the bolus (keeping it in contact with the absorptive epthelium)
_____ contractions move the bolus forward, ____ contractions mixes the bolus.
Peristaltic, Segmental
What are extrinsic neurons?
Autonomic neurons that bring signals from CNS to the digestive system.
Where are longs reflexes integrated?
the CNS.
Where do long reflexes originated?
Some can be from outside the GI tract, some can be from ENS
Which reflex is carried out entirely within the gut wall?
Short reflexes.
Short reflexes originate in the ___
ENS
What does the oral cavity and esophagus secrete?
Saliva
What does the oral cavity/esophagus digest?
Carbohydrates.
What does the oral cavity/esophagus absorb?
nothing lol
What moves the bolus in the oral cavity and esophagus?
Chewing and swallowing, respectively.
What does the stomach secrete?
HCL, Pepsinogen, gastric lipase, mucus, bicarbonate, gastrin, histamine.
What does the stomach digest?
Proteins, MINIIMAL fats.
What does the stomach absorb?
lipid-soluble substances.
What moves the bolus in the stomach?
Peristaltic contractions.
What’s secreted in the SI?
Enzymes, mucus, hormones, bicarbonate, bile.
What’s digested in the SI?
Polypeptides, carbs, fats, nucleic acids.
What moves the bolus in the SI?
Segmental contractions, SOME peristalsis.
What’s secreted by the LI?
Mucus
What’s digested in the LI?
nothing.
What’s absorbed in the LI?
ions, minerals, vitamins, water, small organic molecules.
What moves the bolus in the SI?
Segmental contractions, mass movement for propulsion.
What are extrinsic neurons?
Autonomic neurons that bring signals from CNS to digestive system.
Which reflex is integrated in the ENS? Where does this typically originate?
Short reflex; originates entirely in the wall of the gut.
Which reflex is integrated in the CNS? Where does this typically originate?
Long reflex; can originate outside GI tract/in ENS.
Are bile salts hydrophilic or lipophilic?
Neither, its ambiphilic.
What’s gastrin’s stimulus for release?
Peptides and AAs; neural reflexes.
What’s gastrin’s primary target? What’s its primary effect?
ECL cells and Parietal cells. It stimulates gastric acid secretion and mucosal growth.
Where is gastrin released?
The stomach.
What’s CCK’s stimulus for release?
Fatty acids and some AAs.
What’s CCK’s primary target? What’s its primary effect?
Gallbladder, pancreas, stomach. Stimulates gallbladder contraction and enzyme secretion; inhibits gastric emptying and acid secretion.
What’s secretin’s stimulus for release?
Acid in SI.
What’s secretin’s primary target? What’s its primary effect?
Pancreas, stomach; stimulates HCO3 secretion, inhibits gastric emptying and acid secretion.
What’s motilin’s stimulus for release?
Fasting, periodic release ever 1.5-2 hours.
What’s motilin’s primary target? What’s its primary effect?
Gastric and intestinal smooth muscle; stimulates migrating motor complex.
What’s GIP’s stimulus for release?
Glucose, fatty acids, and AAs (in SI).
What’s gastrin’s primary target? What’s its primary effect?
Beta cells of pancreas; stimulates insulin, inhibits gastric emptying and acid secretion.
What’s GLP-1’s stimulus for release?
Mixed meal that includes carbs or fats in the lumen.
What’s GLP-1’s primary target? What’s its primary effect?
Endocrine pancreas; stimulates insulin release, inhibits glucagon release and gastric function.
Where does mechanical and chemical digestion begin?
The mouth.
Another name for ‘chewing’ is…
mastication.
Another name for ‘swallowing’ is…
Deglutition
Sequence the swallowing reflex:
Tongue pushes bolus against soft palate and back of mouth
Breathing is inhibited as the bolus passes the closed airway
Food moves downward into the esophagus, propelled by peristaltic waves & gravity.
What are the 3 functions of the stomach?
Storage, Digestion, Defense against pathogens.
How does digestive activity in the stomach begin?
Long vagal reflex of cephalic phase.
What does mucous surface cell secrete? What is the function of it?
Mucus; physical barrier between lumen and epithelium.
What’s mucous surface cells’ stimulus for release?
Tonic secretion; inhibition of mucosa.
What does mucous neck cells secrete? What is the function of it?
Bicarbonate, buffers gastric acid to prevent damage to epithelium.
What’s mucous neck cells’ stimulus for release?
Secreted with mucus.
What does parietal cells secrete? What is the function of it?
Gastric acid and intrinsic factor; activates pepsin and kills bacteria - complexes with vitamin B12 to permit absorption.
What’s parietal cells’ stimulus for release?
Ach, Gastrin, Histamine.
What does enterochromaffin-like cell secrete? What is the function of it?
Histamine; Stimulates gastric acid secretion.
What’s enterochromaffin-like cells’ stimulus for release?
Ach, gastrin.
What does chief cells secrete? What is the function of it?
Pepsinogen, Gastric lipase; Digests proteins and fats, respectively.
What’s chief cells’ stimulus for release?
Ach, acid secretion.
What does D cells secrete? What is the function of it?
Somatosatin; inhibits gastric acid secretion.
What’s D cell’s stimulus for release?
Acid in stomach.
What does G cells secrete? What is the function of it?
Gastrin; stimulates gastric acid secretion.
What’s G cell’s stimulus for release?
Ach, Peptides, AAs.
Why is bicarbonate secreted?
Acts as a barrier that neutralizes acid.
What does pancreas endocrine release?
Secretes insulin and glucagon.
What does pancreas exocrine release?
Secretes digestive enzymes and bicarb.
What are digestive enzymes secreted as in the SI?
zymogens, activated in SI.
What’s the purpose of bile?
Fat digestion.
Sequence isotonic NaCl secretion
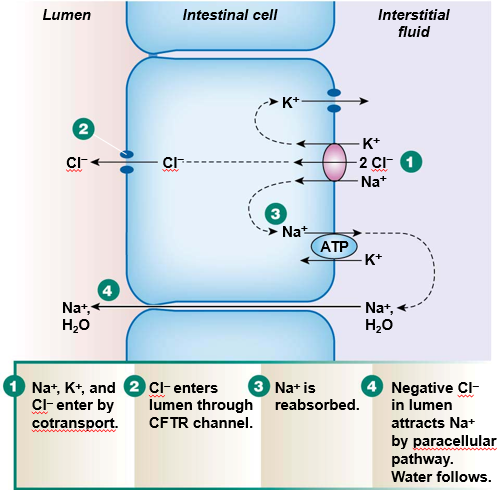
Sequence bicarbonate secretion in the pancreas and duodenum.
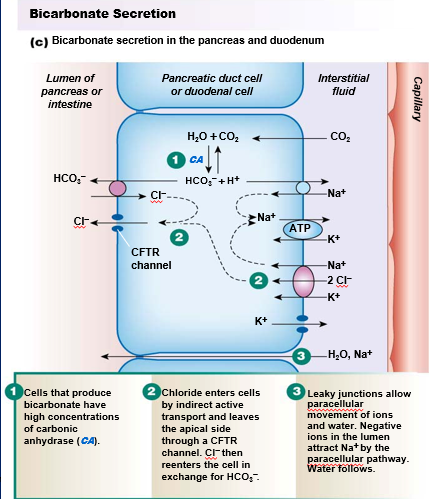
What’s the largest of internal organs?
The liver.
What’s the function of the common hepatic duct?
takes bile made in the liver to the gallbladder for storage.
What’s the function of the common bile duct?
Takes bile from the gallbladder to the lumen of the SI.
What’s the function of the hepatic artery?
Brings oxygenated blood containing metabolites from peripheral tissues to the liver.
What’s the function of the hepatic portal vein?
Hepatic portal vein blood is rich in absorbed nutrients from the GI tract and contains hemoglobin breakdown products from the spleen. Blood leaves liver from this vein.
What’s the function of the Sphincter of Oddi?
Controls the release of bile and pancreatic secretions in the duodenum.
Where does the majority of the blood supply come from?
Portal vein in the liver.
What is the largest visceral organ in the body?
The liver.
What are lobules?
Irregula hexagonal units comprised of hepatocytes.
What are hepatocytes?
Liver cells.
Blood entering the liver chart.
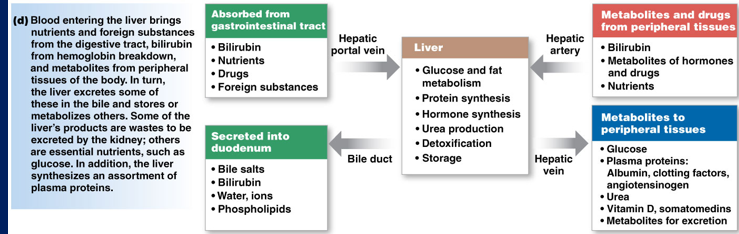
What are the functions of the liver?
Metabolic
storage
excretory/secretory
protective
circulatory
coagulation