Nodules & Neoplasms
1/73
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
74 Terms
what is bronchogenic carcinoma?
cancer that begins in the tissue that lines or covers the airways or the lungs
what is the leading cause of cancer related deaths in men & women?
bronchogenic carcinoma
what are the categories of bronchogenic carcinoma?
- small cell lung cancer (SCLC)
- non small cell lung cancer (NSCLC)
small cell lung cancer (SCLC)
- more likely to spread
- rarely amendable to surgery
- tends to originate in the central bronchi & metastasize to regional lymph nodes
- prone to early metastasis & has aggressive clinical course
non-small cell lung cancer (NSCLC)
- more common
- grows more slowly
- more amendable to surgery
- includes: squamous cell carcinoma, adenocarcinoma, & large cell carcinoma
types of NSCLC
- squamous cell carcinoma
- adenocarcinoma
- large cell carcinoma
which is more common?
a. SCLC
b. NSCLC
b. NSCLC
adenocarcinoma
- typically metastatic to distant organs
- arises from mucous glands
- usually appears in the periphery of the lung
- not amendable to early detection through sputum examination
squamous cell carcinoma
- bronchial in origin
- centrally located mass
- more likely to present w/ hemoptysis & therefore more likely to be diagnosed via sputum cytology
what is bronchoalveolar cell carcinoma (BAC)?
subtype of adenocarcinoma
- rare
- low grade (grows/spreads more slowly)
large cell carcinoma
- heterogeneous group of undifferentiated types that do not fit elsewhere
- cytology typically shows large cells & doubling time is rapid
- metastasis is early
- may be central or peripheral masses
what is the most common type of NSCLC?
adenocarcinoma
what are the risk factors for bronchogenic carcinomas?
- tobacco (even secondhand smoke)
- asbestos
- radon
- HIV
- idiopathic pulmonary fibrosis
- COPD
- TB
- hx of chemotherapy, chest radiotherapy, or lung cancer
- older age
- genetic mutations (ex: EGFR is present in 20% of adenocarcinomas)
the majority of patients who present w/ clinical s/s due to lung cancer have advanced disease; therefore, the most common presenting manifestations are the following:
- cough (particularly new onset or change in cough)
- hemoptysis
- dyspnea
- chest pain
what clinical features may suggest SCLC over NSCLC?
rapidly progressive sx
- which may include bone pain from metastases
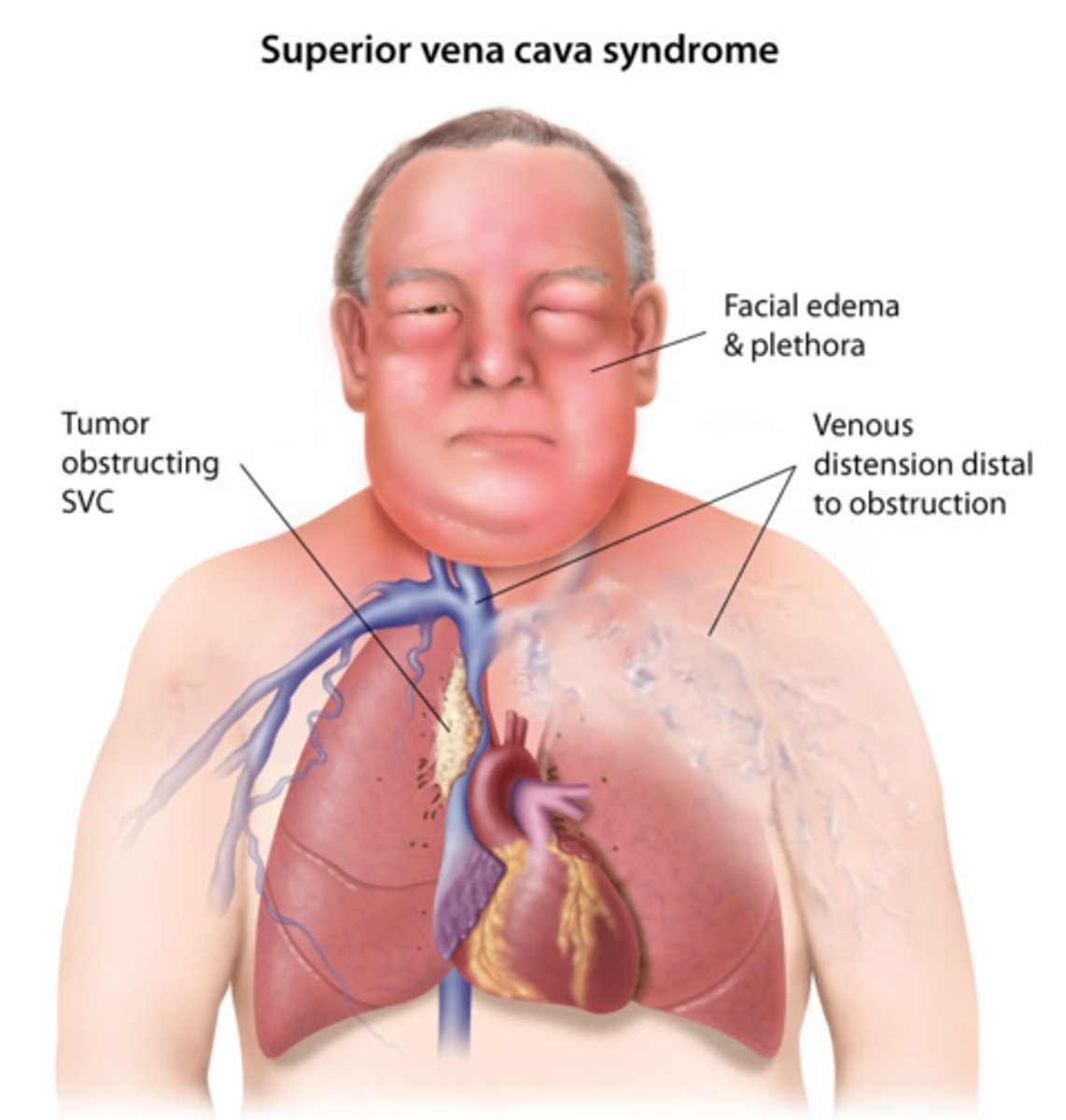
what is superior vena cava syndrome?
s/s resulting from either partial or complete obstruction of blood flow through the SVC
- which may be result of a thrombus formation or tumor infiltration of the vessel wall
pancoast tumors are a type of ________.
NSCLC
1 multiple choice option
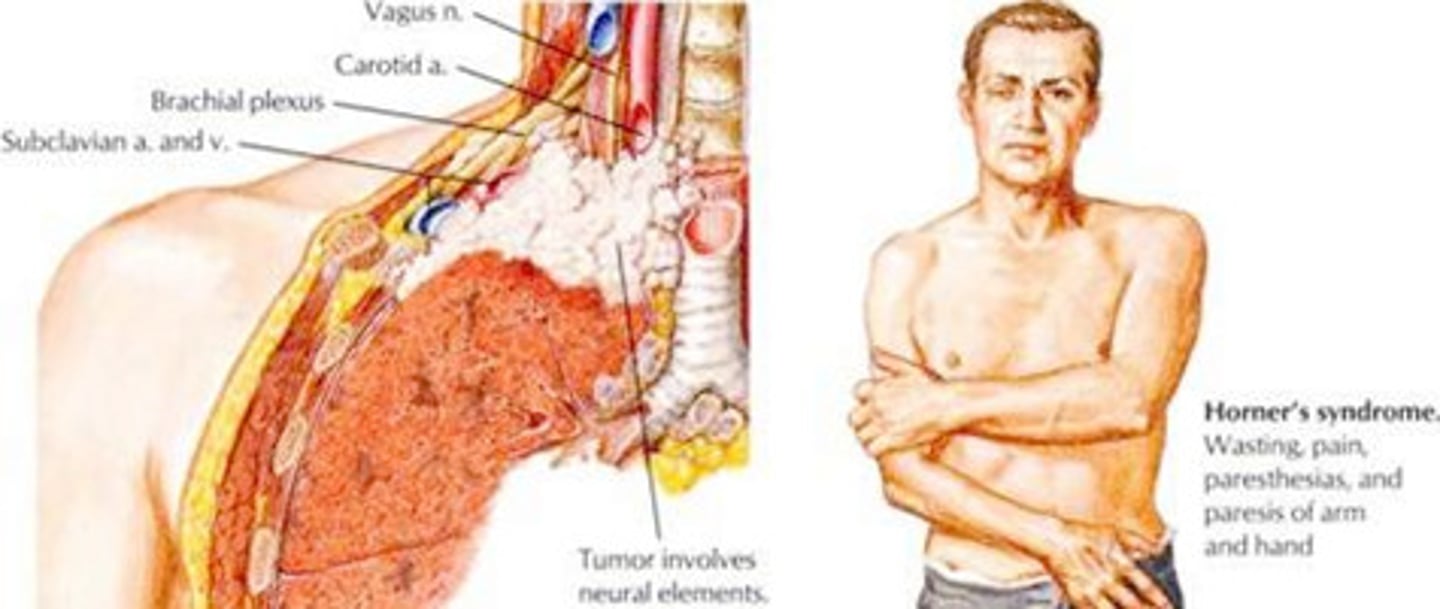
what are pancoast tumors?
tumors that arise from the apical pleuropulmonary groove
- located superior to the first rib
what is pancoast syndrome?
when pancoast tumors involve surrounding structures,
such as:
the branchial plexus, cervical paravertebral sympathetic nervous system, & stellate ganglion & cause a group of s/s
s/s of pancoast syndrome
- ipsilateral (same side) shoulder & arm pain
- paresthesias
- paresis
- atrophy of the thenar muscles of the hand
- horner's syndrome (ptosis, miosis, & anhidrosis)
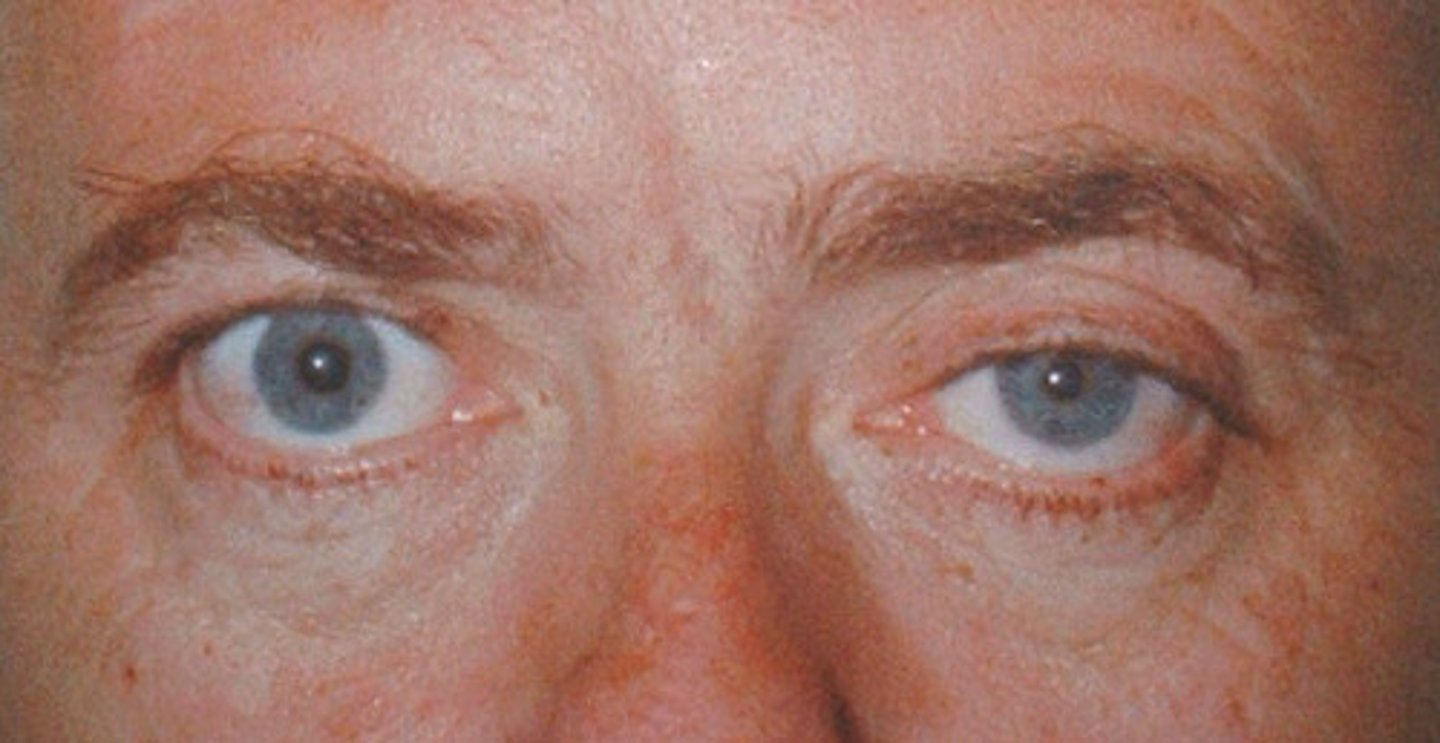
what is horner's syndrome?
ptosis, miosis, anhidrosis
- symptom of pancoast syndrome
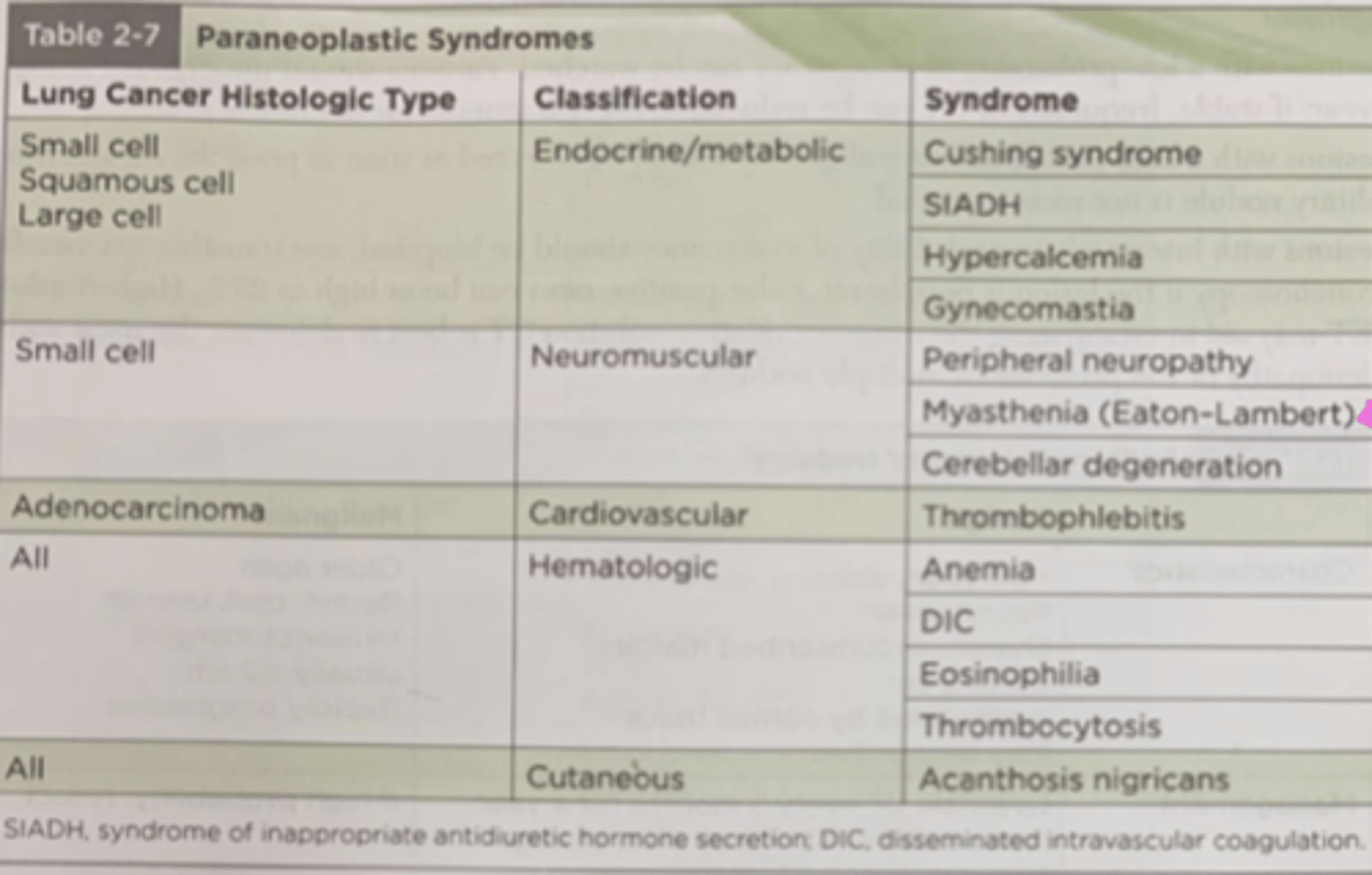
when does a paraneoplastic syndrome occur?
when a malignant tumor releases a hormone/protein that affects a certain body system or when the body's immune system releases a substance (antibody) meant to kill the tumor but also damages healthy body immune cells (autoimmune response)
paraneoplastic syndromes
what is the initial imaging for patients w/ sx concerning for lung cancer?
chest XR
what imaging should be conducted to further evaluate findings suggestive of cancer?
CT w/ contrast
can you rule out lung cancer w/ a CXR?
NO
1 multiple choice option
which type of pleural effusion is more suggestive of cancer when taken into consideration w/ the other s/s present?
a. exudative
b. transudative
a. exudative
what is the benefit of a cytologic examination of sputum?
can permit a definitive diagnosis of malignancy in some cases
if the sputum culture comes back normal, does this rule out malignancy?
NO
1 multiple choice option
which imaging modalities can be used to establish a diagnosis by looking at specific cell types through direct visualization &/or biopsy?
- bronchoscopy
- exam of pleural fluid
- biopsy
which type of imaging is done to evaluate for metastasis?
PET scan
why may tumor tissue analysis be done?
to look for epidermal growth factor receptor (EGFR) & K-RAS mutations
what specific therapy may those w/ EGFR mutation be candidates for?
targeted molecular therapy
how is a definitive diagnosis of lung cancer made?
based upon pathologic evaluation of fluid or tissue specimens
what is the treatment of choice for NSCLC?
surgery
- additional chemo/radiation may be considered as well
- needs oncology/pulmonology/surgical evlauation
what is the treatment of choice for SCLC?
combo therapy w/ chemo & radiation
which has a better survival rate?
a. NSCLC
b. SCLC
a. NSCLC
what is the 5 yr survival rate of NSCLC?
- localized: 63%
- regional spread: 35%
- distant spread: 25%
what is the 5 yr survival rate of SCLC?
- localized: 27%
- regional spread: 16%
- distant spread: 7%
how can lung cancer be prevented?
by reducing risk factors
- NO SMOKING!
who does the USPSTF recommend yearly lung cancer screening w/ a low-dose screening CT (LDSCT) for?
>/= 20 pack year smoking history
and
smoke now or have quit w/i past 15 yrs
and
are between 50-80 y/o
when can the patient STOP having their annual LDSCT?
once they have not smoked for 15 yrs or have a health problem that limits life expectancy
what is a pulmonary nodule?
small (< 30 mm), well defined lestion completely surrounded by pulmonary parenchyma
how are pulmonary nodules classified?
as solid or subsolid
lesions that measure ____mm are considered masses
> 30 mm
which have a much higher likelihood of being malignant?
a. pulmonary nodules
b. pulmonary masses
b. pulmonary masses
common causes of malignant nodules include:
- primary lung cancer
- lung metastases
- carcinoid tumors
rank the types of NSCLC from most common to least common:
1. adenocarcinoma
2. squamous cell carcinoma
3. large cell carcinoma
common causes of benign nodules include:
- infectious granulomas
- pulmonary hamartoma
what causes ~80% of benign nodules?
infectious granulomas
what are the most frequently recognized causes of infectious granulomas?
- fungi
- mycobacteria (TB or non-TB)
what is a pulmonary hamartoma?
benign neoplasm
- composed of: cartilage, connective tissue, muscle, fat & bone
what are the fleischner society guidelines?
guidelines for how to follow up based on type & size of pulmonary nodule
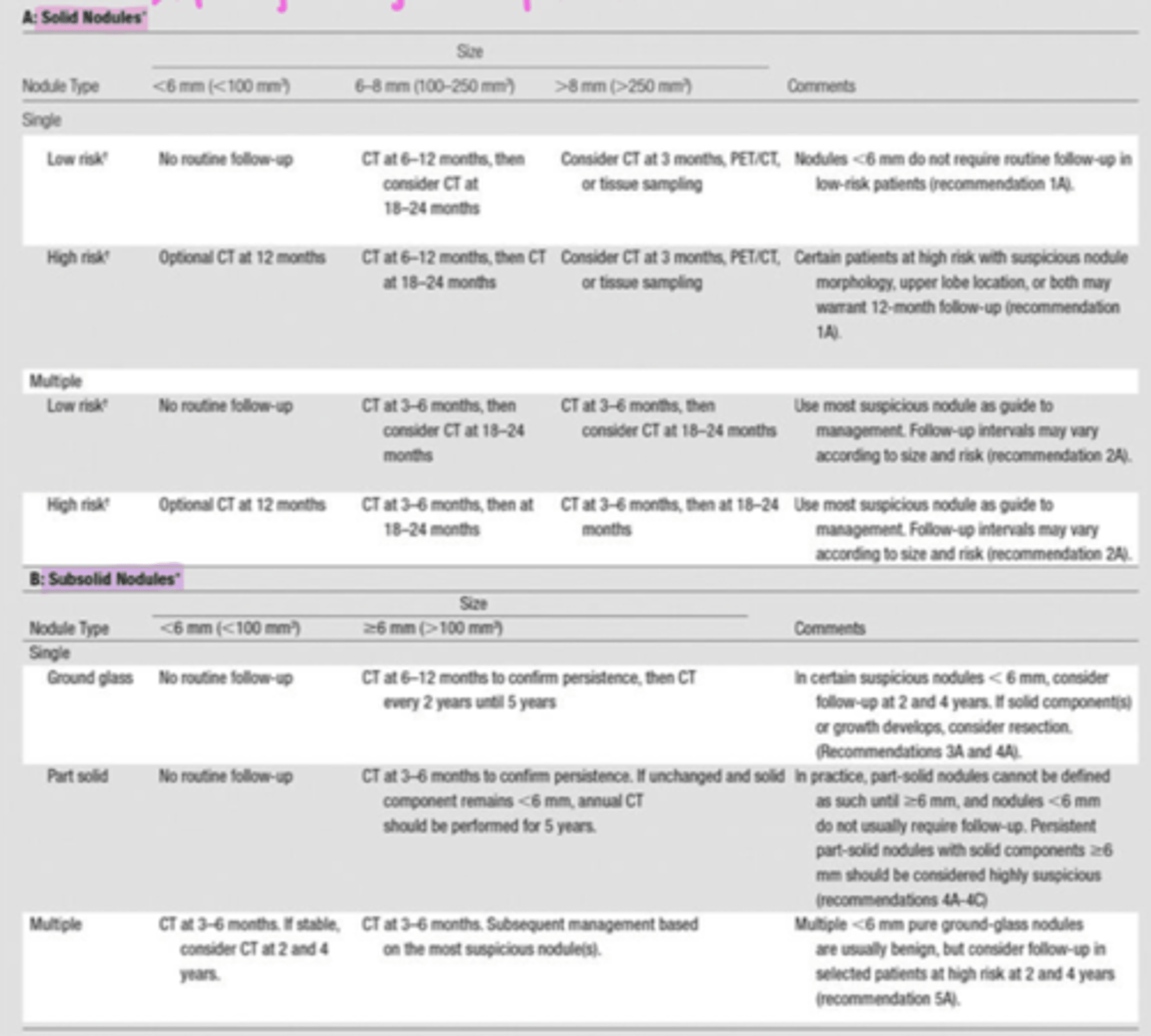
high risk factors include:
- older age
- hx of tobacco use &/or exposure
- irregular or speculated margins
- upper lobe location
- family hx of lung cancer
single, solid nodule of 5mm was found on CT.
pt is 70 y/o & has a hx of smoking.
using the fleischner society guidelines, what is the follow up for this patient?
optional CT at 12 months
single, subsolid, ground glass nodule of 5mm was found on CT.
using the fleischner society guidelines, what is the follow up for this patient?
no routine follow-up
multiple, solid nodules of 9mm were found on CT.
pt has no risk factors.
using the fleischner society guidelines, what is the follow up for this patient?
CT at 3-6 months
- then consider CT at 18-24 months
the fleischner society guidelines do NOT apply to patients younger than ________.
35 y/o
the term "carcinoid," has generally been applied to..
well-differentiated neuroendocrine tumors (NETs)
what is a carcinoid tumor?
a type of neuroendocrine tumor that grows from neuroendocrine cells which receive & send messages through hormones to help the body function
- rare
- usually start in the lining of the digestive tract or lungs (but rarely kidneys or ovaries)
- grow slowly & don't produce sx in early stages
where do carcinoid tumors usually start?
in the lining of the digestive tract or lungs
since carcinoid tumors grow slowly & don't produce sx in the early stages, what is the average age of diagnosis of digestive or lung carcinoids?
60 y/o
if in the pulmonary system, where are carcicinoid tumors usually found?
in the bronchi (endobronchial)
- 20% present as a peripheral, well-circumscribed pulmonary nodule
where may carcinoid tumors be found in children?
appendix
which genetic condition is associated w/ a higher risk of developing a carcinoid tumor?
multiple endocrine neoplasia type 1 (MEN1)
s/s of carcinoid tumors
can be asymptomatic
- pulmonary sx (hemoptysis, cough, focal wheezing, & recurrent pneumonia)
- GI sx (abdominal pain or discomfort, N/V/D, rectal bleeding, rectal pain)
carcinoid syndrome occurs in 10% of patients, & consists of:
- flushing
- diarrhea
- wheezing
- hypotension
what will bronchoscopy reveal w/ a carcinoid tumor?
a pink or purple, central lesion that is well vascularized
- lesion may be pedunculated or sessile
what is octreotide scintigraphy used for?
localization of primary & metastatic neuroendocrine tumors bearing somatostatin receptors
what do CTs/MRIs help w/ in work-up of carcinoid tumors?
localization of lesion as well as monitoring for growth
how is the diagnosis of a central carcinoid tumor/lesion confirmed?
bronchoscopic biopsy
how is the diagnosis of a peripheral carcinoid tumor/lesion confirmed?
transthoracic needle biopsy
how are carcinoid tumors treated?
surgery
- lesions are resistant to chemo & radiation
what can be used to treat the sx associated w/ a carcinoid tumor?
octreotide (somatostatin analog)
- which blocks hormone secretion