RMS - Pulmonary and Nasal Drug Delivery
1/9
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
10 Terms
What is Pulmonary Drug delivery?
- Pulmonary drug delivery involves administration of therapeutic agents via the respiratory system (into the lungs or via the lungs)
- Drugs may or may not enter systemic circulation
- Most commonly the pulmonary route is used for Asthma, COPD, Cystic Fibrosis, Pulmonary hypertension and lung infections
- Drugs can be delivered as gases or aerosols: "smokes" (solids suspended in air) or "mists" (liquids suspended in air)
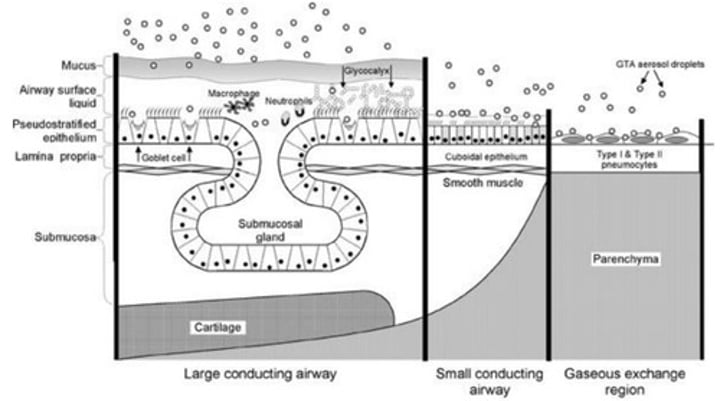
How is the anatomy of the Lungs involved in Pulmonary Drug delivery?
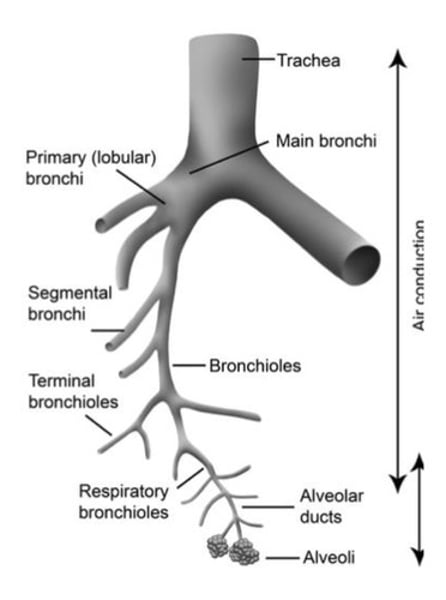
- Targets of Pulmonary drug delivery can either be the central airways (gas transport - trachea, bronchi and upper bronchioles) or the peripheral airways (gas exchange - terminal bronchioles, respiratory bronchioles and alveoli)
- The decreasing diameter of the airways increases resistance to air flow deeper in the lungs (1% diameter decrease = 4% resistance increase)
- To reach the respiratory alveoli, particles must be <5microns, and to reach the alveoli, particles must be <2microns
How do different disease states affect the lungs?
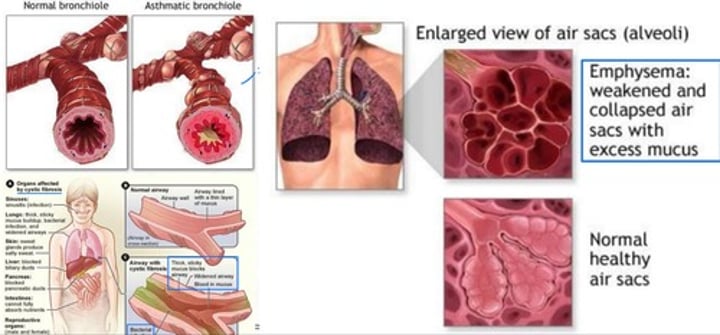
- Diseases such as Asthma can cause reduced airflow due to decrease in diameter of the airways, caused by inflammation, constriction and excess mucus production
- Diseases such as Emphysema can reduce gas exchange, and volume of air exchanged, caused by weakened and collapsed alveoli with excess mucus
- Diseases such as Cystic Fibrosis can reduce airflow due to mucus build up in airways, bacterial infections causing inflammation, and irregular diameters from widening of airways
What are the types of particle deposition observed in the Lungs?
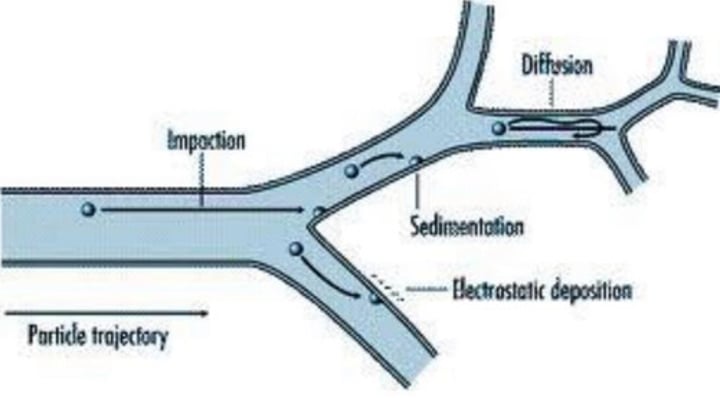
- Inertial Impaction = (5microns<) chance of impaction is higher the larger the particle is, and generally occurs at the upper divisions of the airway, particles impact into epithelia
- Gravitational Sedimentation = (0.5<x<5microns) most dominant deposition in lower divisions of airway, particles slow down gradually and sediment from gravity
- Diffusion = (<0.5microns) deposition in alveoli and furthest airway divisions, particles are affected brownian motion due to size (can be breathed out, absorbed or cleared macrophages)
- Aerodynamic diameter = geometric diameter * sqrt(density of solid)
What are the factors influencing particle deposition in the Lungs?
- Particle size = decreasing particle size leads to deeper deposition into lungs
- Particle size distribution = the more monodisperse distribution is, the more likely for deeper deposition into lungs
- Particle density = lower density mean lower aerodynamic diameter, so deeper deposition into lungs
- Particle shape = more spherical particles are able to flow better, but size is more important for deeper deposition into lungs
- Particle hygroscopicity = lower hygroscopicity (less water adherence to particle) leads to smaller particles, so deeper deposition into lungs
What happens once a drug has deposited in the Lungs?
- Particles that deposit in the upper airways are cleared by the mucociliary escalator (reduced drug concentration), or the drug is dissolved in the mucus (increased drug concentration)
- Particles that reach the lower airways are cleared by macrophages or undergo translocation (reduced drug concentration for both)
- Particles that reach lower airways are more likely to be absorbed due to flatter epithelia and looser tight junctions
Describe the advantages and disadvantages of Local delivery to the lungs
- Advantages = rapid onset, fewer systemic side effects, lower doses required, drug delivery to target organ, and non-invasive delivery
- Disadvantages = low delivery efficiency, difficulty with device technique + breathing technique, corticosteroid cause immunosuppression and possible throat irritation
Describe the advantages and disadvantages of Systemic delivery via the lungs
- Advantages = rapid onset of action, bypasses first pass metabolism, non-invade delivery, and good for biopharmaceuticals
- Disadvantages = low delivery efficiency, difficult with device technique + breathing technique, may need very low/exact doses, expensive with oral therapies
What is an example of advanced Pulmonary Drug delivery?
- Pulmonary vaccine delivery is an advanced application using Pulmonary Drug delivery
- Traditionally vaccines are delivered SC or IM, inducing systemic immunity, but no sufficient protection of mucosal surfaces (first point of contact for most pathogens)
- Mucosal vaccines induce both mucosal and systemic immunity (for all mucosal surfaces, not just the locally targeted surface)
- Targets are the MALT (mucosal-associated lymphoid tissue), which include the nose, rectum, vagina, gut and lungs
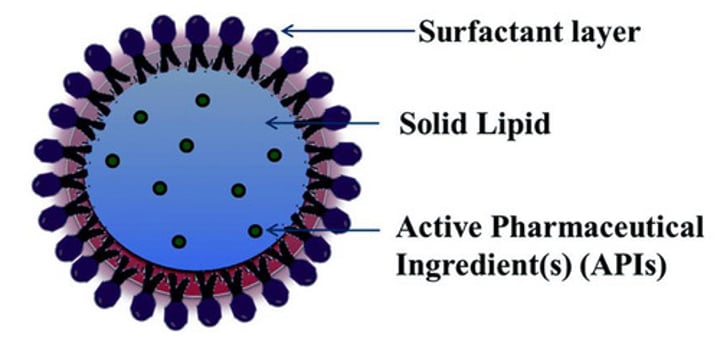
- Example carriers for vaccine delivery include nanoparticles (made with lipids), with mimic normal uptake of pathogens
Describe the immune system in the Lungs
- First line defence = physical barriers like mucociliary escalator, tight junctions between epithelia cells and surfactant
- Second line defence = innate immune system (macrophages and antigen-presenting cells) and adaptive immune system (activated by APCs, and include T + B cells, where B cells release IgA antibodies at mucosal surfaces)