postural control
1/56
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
57 Terms
postural control
controlling the body’s position in space for the dual purposes of stability and orientation
required by all tasks
postural orientation
the ability to maintain an appropriate relationship btwn the body segments and btwn the body and environment for a task
includes biomechanical alignment of body segments relative to environment to accomplish a task
postural stability
ability to control COM in relationship to BOS
COM
a point at the center of total body mass
COG
vertical projection of COM
BOS
area of body in contact w/ support surface
COP (center of pressure)
center of distribution of the total force applied to the supporting surface
moves continuously around COM to keep COM w/in support base
orientation and stability demands of a task
influenced by task and environment
requirements vary according to ^
individual contraints/factors for postural control
postural control system
neural components
postural control results from complex interaction among many systems taht control both orientation & stability
task constraints
balance control
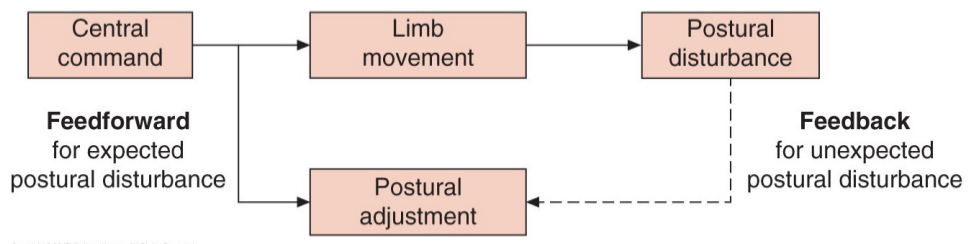
feedback control
feed-forward control
most fxl tasks require all 3 aspects of balance control at some point
environmental constraints
support surfaces
sensory context
cognitive load
steady-state (not static) balance
body alignment can minimize effect of gravitational forces
muscle tone keeps body from collapsing in response to pull of gravity
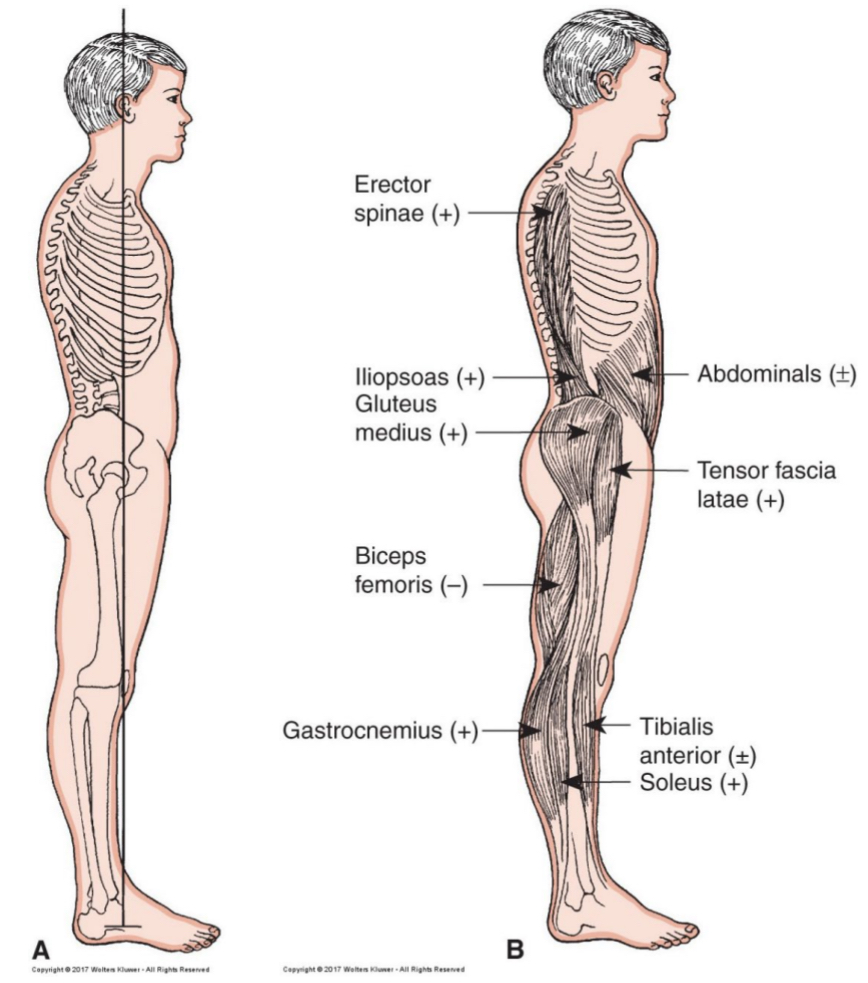
postural tone
increase activity in antigravity postural muscles when we stand upright
muscles tonically active during steady state balance/quiet stance
static postural control is actually dynamic
limits of stability
not fixed boundaries
best understood by looking at position and velocity of COM relative to BOS
affected by perceptual and cognitive factors
ankle and hip strategies
reactive balance control
motor patterns at ankle, hip; step, reach to grasp strategies
fixed support vs change in support
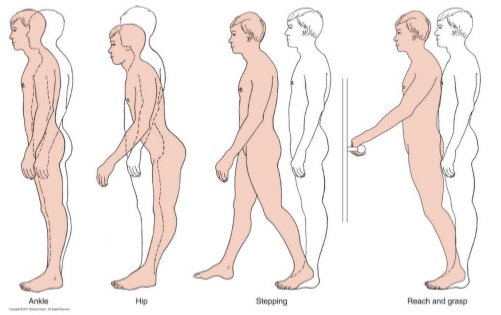
anteroposterior stability
ankle strategy, hip strategy, change in support strategies
medioalteral and multidirectional stability
alignment of body segments & muscles require activation of forces at different joints and in different directions to recover stability
ankle strategy—minimally involved
hip and trunk, change in support strategies
refining and tuning muscle synergies
stereotyped reactions
in response to changing demands in task and environment=adaptation
very quick response
reactive balance control in sitting
recovery of stability in seated position controlled similarly to that in stance
individual muscles change relative activation depending on direction of instability
why do corrective strategies occur proximal→distal?
energy conservation
it’s easier to fix balance closer to sensory input
go back and watch the panopto for this one i actually dont know why he siad proximal to distal
proactive/anticipatory balance control
CNS uses anticipatory processes in controlling action
critical to LE activities
posture anticipates voluntary movement
sensory inputs for steady state balance
vision, vestibular, somatosensory
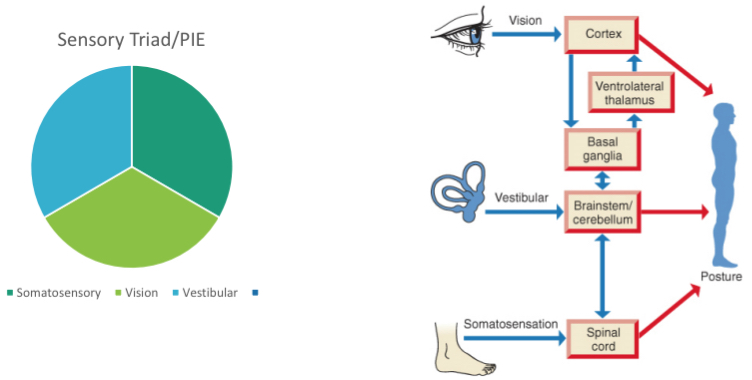
visual inputs for steady-state balance
position and motion of head with respect to surrounding objects
reference for verticality
self-motion
somatosensory contributions for steady-state balance
provide CNS w/ position & motion info about body w/ reference to supporting surfaces
report info about relationship of body segments to one another
somatosensory info integrated for steady-state balance
vestibular inputs for steady state balance
provides CNS info about position and movement of head w/ respect to gravity & inertial forces
sensory integration
reweighting
stability in variety of environments
sensory triad
visual info gathered
somatosensory inputs
cnotribution of vestibular system smaller than somatosensory
all 3 systems play a role in recovering stability after an unexpected perturbation
sensory inputs for proactive balance
visual inputs typically most critical, depending on individual and task
cognitive systems in postural control
attentional resources
dual-task interference
dual task interference in postural control
attentional demands vary as function of sensory context
performance of secondary task not always detrimental to posture
important to assess balance under both single and dual task conditions
spinal contributions to postural orientation and stability
tonic activation of extensor muscles for weight support
directionally specific responses to perturbations present at spinal cord level
brainstem contributions to postural orientation and stability
regulation of postural tone and automatic postural synergies
basal ganglia and cerebellar contributions to postural orientation and stability
cerebellum: controls adaptation of postural responses
basal ganglia: control of postural set
fall statistics
5th leading cause of death in elderly
¾ of deaths from falls occur in ppl 65+
1/3 of ppl 65+ fall each yr
RFs for falls
muscle weakness
fall hx
gait deficits
balance deficits
AD use
visual deficits
arthritis
impaired ADLs
depression
cognitive impairment
80+ y/o
presence of stairs
throw rugs
slippery surfaces
poor lighting
4+ meds
and many others
age related changes to postural control
MSK
ROM
somatosensory
vision
vestibular
progressive supranuclear palsy
BG pathology related/similar to PD
lack brainstem involvement, limiting postural control
mainly struggle with backwards postural responses
falls in ppl w/ neuro pathology
prevalence varies by diagnosis and setting
associated w/ mobility, occuring during walking, transfers, stair climbing
impaired balance found to be most consistent RF for indiv who have neuro path who fall
alignment
relationship of body segments to one another as well as to position of body w/ reference to gravity and BOS
determiens constellation of movement strategies effective in controlling posture
infl how muscles recruited and coord for recovery of stability
examination: verticality, symmetry
postural sway
assessing stability during quiet stance
pathology in cerebellum—directionally specific incr postural sway
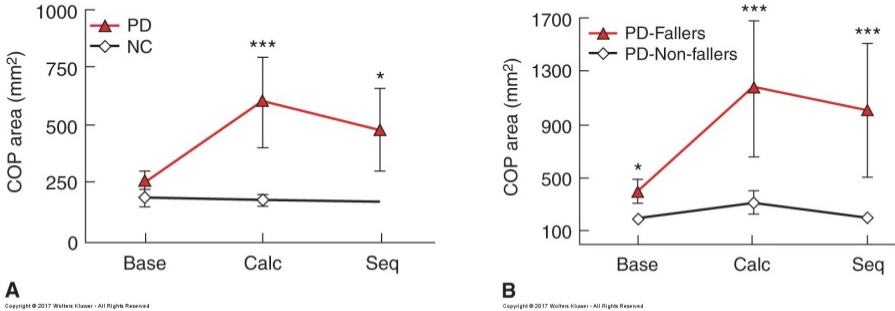
postural sway in PD and levodopa replacement therapy
keep in mind effects of medication state when seeing pt
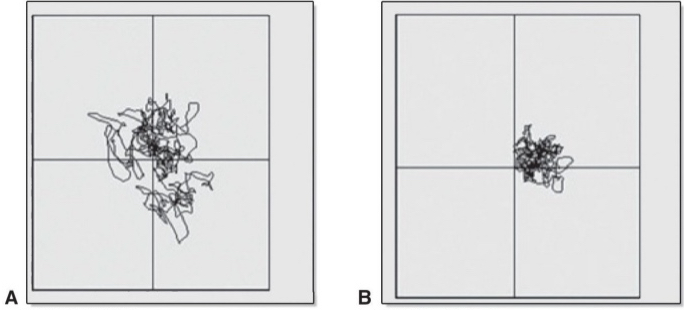
fxl stability limits
determined by biomechanics of body, postural control abilities, environmental factors
exam: COP excursion during voluntary leaning (reduced in MS and PD)
limits of stability: reactive balance
sequencing problems
problems w timely activation of postural responses
problems adapting postural activity to changing task and environmental demands
impaired in-place strategies: sequencing problems, co-activation, delayed onset of postural responses, problems modifying postural strategies (postural adaption), impaired central set
sequencing
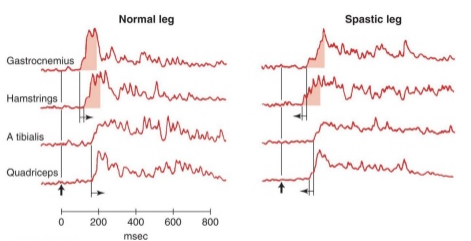
co-activation
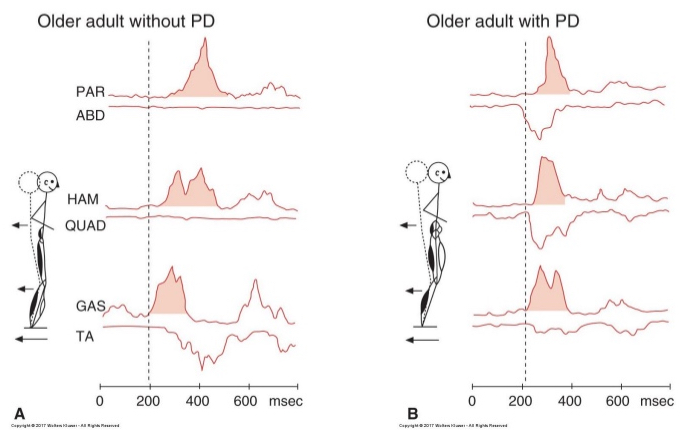
problems modifying postural strategies
sway (see picture)
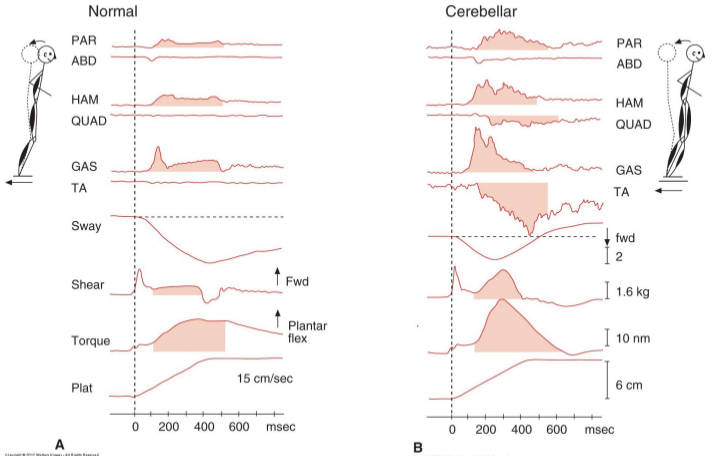
delayed onset of postural responses
reaction time
most common across different populations
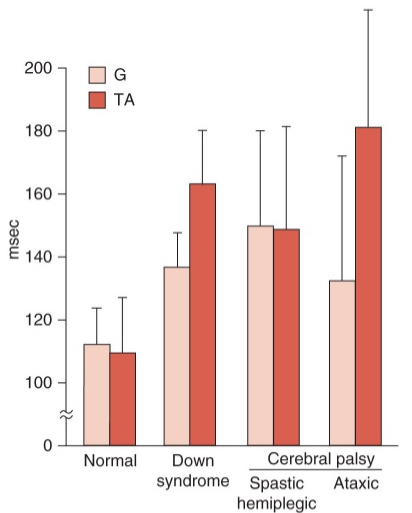
impaired central set
similar recruitment pattern regardless of task being performed
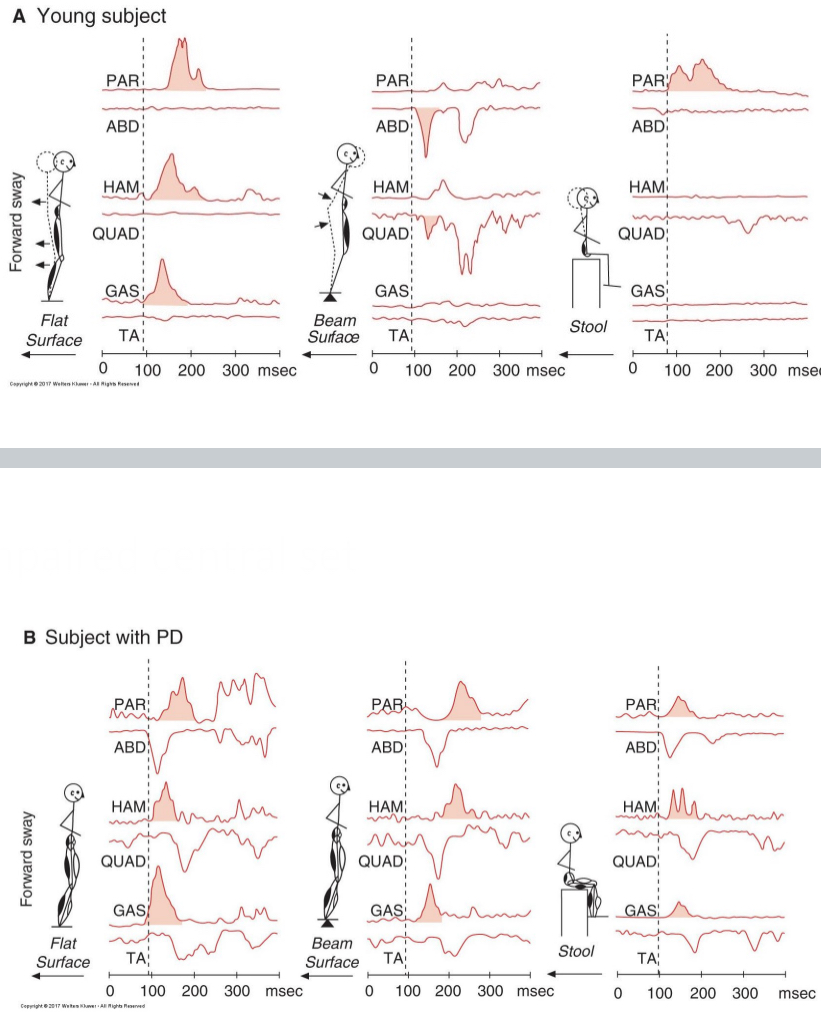
anticipatory postural control
loss of anticipatory processes that activate postural adjustments in advance of potentially destabilizing voluntary movements
dependent on previous experience & learning
activating muscles before stabilized→destabilization in anticipated motion
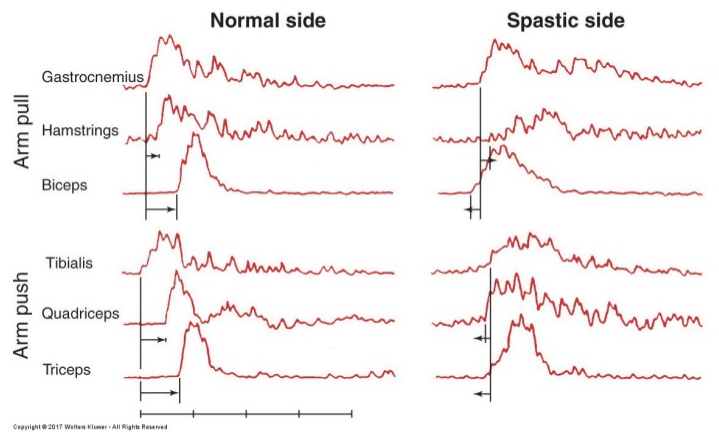
sensory problems affecting steady-state balance
detect position of body in space, accurate orientation cues in environment, sensory weighting
disrupt ability to adapt sensory inputs to changes in task and environmental demands
disrupt development of accurate internal models and perceptions of body
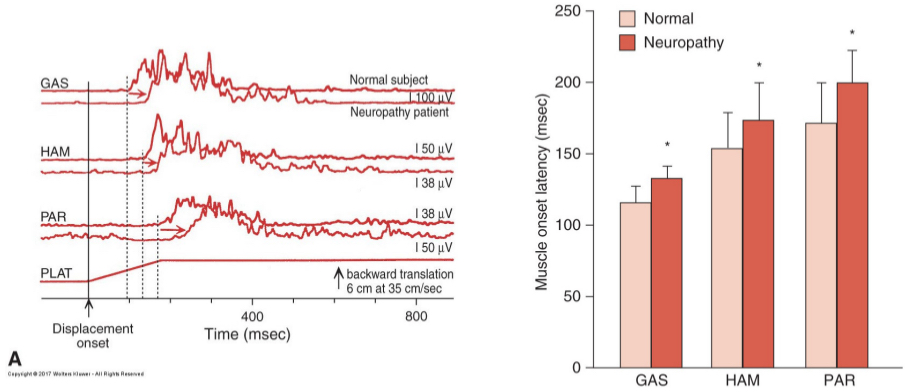
somatosensory inputs from LEs in reactive balance
trigger centrally organized postural synergies
provide direct sensory feedback
loss of somatosensory inputs can result in
profound changes in motor adaptation
earlier activation of anticipatory postural adjustments as a compensatory strategy
perceptual problems affecting postural control
perceptions of verticality: subjective visual vertical, haptic or kinesthetic vertical, subjective postural vertical
balance and falls self-efficacy
confidence/fear
avoidance
major factor predicting participation in community mobility
activity & participation are limited not only by person’s actual balance abilities but also by perceived balance abilities
impaired postural stability and dual-task interference
attentional capacity
neurologic pathology produces deficits in executive attention
neuro pathology deficits in executive attention (dual task)
infl allocation of attention under dual task conditions impairing balance
maintaining stability requires more attentional resources
may contribute to instability under dual task conditions