Short answer 2
1/6
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
7 Terms
Compare and contrast arteries and veins (blood vessels)
Similarities
Both are blood vessels that transport blood.
Both have three layers: tunica intima, tunica media, and tunica externa.
Both are essential for circulation and maintaining blood flow.
Differences
Feature | Arteries | Veins |
|---|---|---|
Function | Carry blood away from the heart | Carry blood toward the heart |
Oxygen Content | Usually oxygen-rich (except pulmonary arteries) | Usually oxygen-poor (except pulmonary veins) |
Wall Thickness | Thick, muscular, and elastic | Thin, less muscular, and less elastic |
Lumen Size | Narrow | Wide |
Pressure | High | Low |
Valves | Absent (except in large arteries) | Present to prevent backflow |
Explain the role of respiratory and skeletal pumps in veins (blood vessels)
The respiratory pump and skeletal muscle pump help push blood through veins, especially in low-pressure areas like the legs:
The respiratory pump assists venous return by creating pressure differences during breathing. When you inhale, the diaphragm contracts and moves downward, which increases intra-abdominal pressure and decreases intrathoracic pressure. This pressure gradient helps push blood from the abdominal veins into the thoracic veins and toward the heart. During exhalation, venous valves prevent backflow and maintain unidirectional blood flow.
The skeletal muscle pump helps propel blood through veins, especially in the legs. When skeletal muscles contract, they compress the veins, which increases pressure and pushes blood upward. One-way valves in veins prevent backflow and ensure that blood moves toward the heart. Both pumps are crucial for facilitating venous return, particularly in the lower extremities, where gravity can hinder blood flow back to the heart
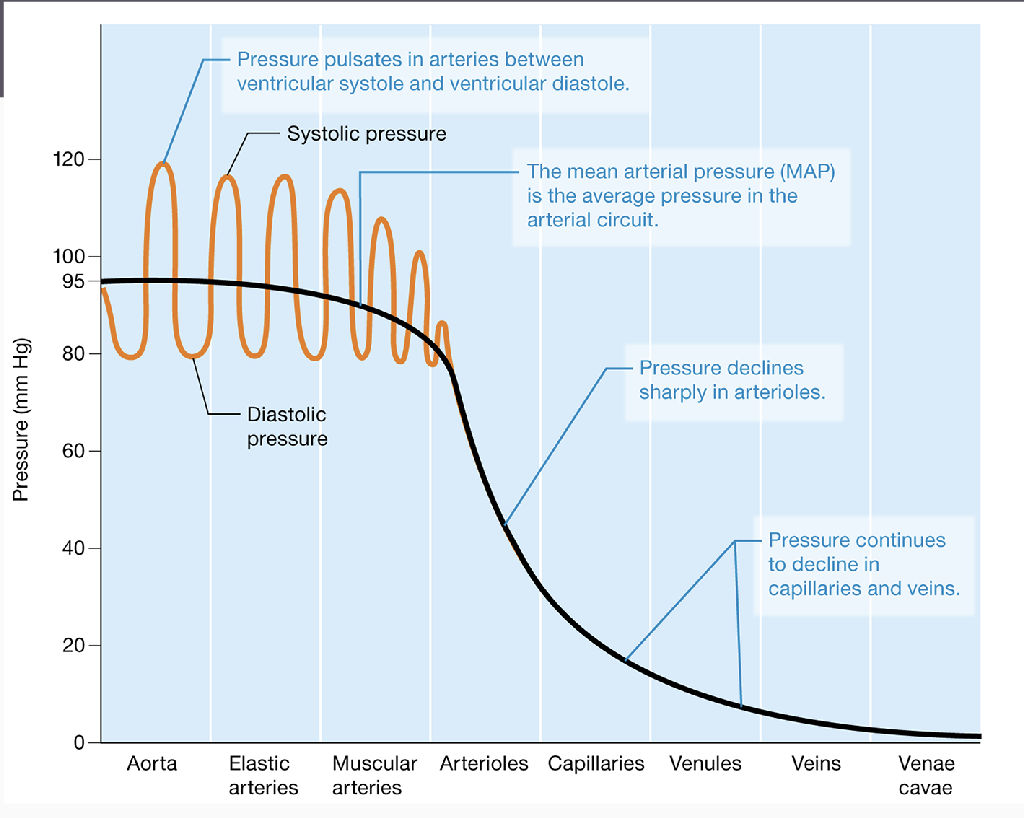
Explain blood pressure graphs and explain changes through the graphs (blood vessels)
Know how to draw
Systolic pressure-ventricles contracting
Diastolic pressure-ventricles relaxing
When moving away from arteries to arterioles, blood pressure is regulated and decreases significantly.
Pressure gets lower to go through capillaries.
Pressure remains low until the blood can be brought back to the heart.
Explain the role of platelets and steps to platelet plug formation (blood)
Platelets (thrombocytes) play a crucial role in hemostasis by helping to form a temporary platelet plug at the site of blood vessel injury, preventing excessive blood loss. Here's how platelet plug formation occurs:
Vascular Spasm
Blood vessels constrict to reduce blood flow at the injury site.Platelet Adhesion
Platelets stick to exposed collagen.Platelet Activation
Activated platelets release chemicals like ADP and thromboxane, attracting more platelets.Platelet Aggregation
Platelets stick together using fibrinogen, forming a temporary plug.Plug Stabilization
The coagulation cascade forms fibrin, strengthening and stabilizing the plug.
This process helps stop bleeding and begin the healing process.
Explain erythropoiesis and regulation of erythropoietin (EPO) (blood)
Erythropoiesis is the process of red blood cell (RBC) production, occurring in the bone marrow. It starts from hematopoietic stem cells, which differentiate into erythroblasts, then reticulocytes, and finally mature erythrocytes.
Regulation of Erythropoietin (EPO)
EPO is a hormone mainly produced by the kidneys in response to low blood oxygen (hypoxia). The regulation follows these steps:
Hypoxia detection – Kidney cells sense low oxygen levels.
EPO secretion – Increased EPO release stimulates erythropoiesis in the bone marrow.
RBC production – More RBCs increase oxygen-carrying capacity.
Negative feedback – Once oxygen levels normalize, EPO secretion decreases.
Factors affecting EPO production include anemia, high altitude, and chronic lung disease.
Cover anything we haven’t covered this exam
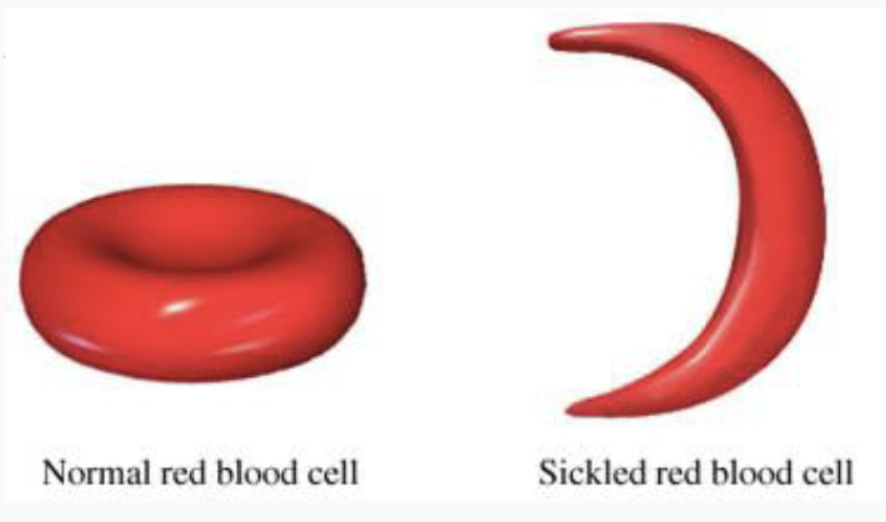
Sickle cell anemia results from genetically abnormal hemoglobin, which alters the shape of red blood cells (RBCs). This condition provides a survival advantage against malaria, particularly in regions like Africa where malaria is prevalent. Individuals with one sickle cell gene, known as the sickle cell trait, are less likely to suffer from severe malaria. As a result, the sickle cell trait has become more common in these populations, offering a protective effect against the disease.
Innate immunity and parts of it
responds to pathogens in a nonspecific way. responds to everything the same in a quick manner, always in the body ready to go.
Parts
1) barrier defenses-first line of defense (physical/chemical) against pathogens
2) complement system-network of proteins that enhance the body’s ability to eliminate pathogens/damaged cells
3) inflammation-innate immune cells detect infection/tissue injury
signs of inflammation are heat, redness, swelling, pain (hot red sweaty paint)