BIOS 1310 lab quiz 6
1/122
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
123 Terms
Respiration
aka breathing
the process by which the body exchanges gases w/ the environment
oxygen in
CO2 out
essential for maintaining body’s supply of oxygen while eliminating waste gases produced by cellular activity
Inhalation
Breathing IN
diaphragm contracts and moves downward
increases volume with chest cavity —→ allows lungs to expand
Inhalation pathway
air drawn into body through nose/mouth
air travels down windpipe (trachea) and into branching airways of the lungs
Once inside lungs air reaches alveoli
passes through alveolar walls and enters blood within capillaries
CO2 moves from the capillaries into the alveoli
Alveoli
tiny air sacs surrounded by capillaries
walls are very thin
allows gases to move easiy between them
Exhalation
diaphragm and muscles between ribs relax
reduces volume of the chest cavity and causes the lungs to deflate
as lungs contract, CO2 that moved into alveoli is pushed out through the trachea and exits through nose or mouth
Why is respiration necessary?
cells of the body require oxygen to produce energy needed for normal function and survival
How is CO2 produced?
as cells generate energy, CO2 is produced as a waste product
makes the blood acidic
Upper respiratory tract
nasal cavity
paranasal sinuses
pharynx
larynx
lie outside the thoracic cavity
conduct and condition incoming air
Nasal cavity
main entry point for air
contains hair follicles and mucous membranes
trap dust and other particulate matter
contains:
nasal conchae
olfactory receptors
Nasal conchae
curved bony structures
increase surface area
warm and humidify air as it moves through passages
Olfactory receptors
in the posterosuperior aspect of the nasal cavity
detect odorant molecules and transmits signals to brain
allows for sense of smell
Pharynx
funnel-shaped muscular tube
pathway for both air and food
divided into 3 regions
nasopharynx
oropharynx
laryngopharynx
Nasopharynx
functions only as an airway
Oropharynx
allows passage of both food and air
Laryngopharynx
where the repiratory and digestive systems separate
Larynx
voicebox
contains vocal cords
produce sound
includes the epiglottis
Epiglottis
closes over airway during swallowing to prevent food or liquid from entering the lower respiratory tract
known as aspiration
Lower repiratory tract
trachea
bronchi
bronchioles
lungs
Trachea
windpipe
rigid tube supported by C shaped rings of cartilage
keep the airway open as air travels from the larynx toward lungs
Where and how does the trachea divide?
the level of the sternal angle
two main bronchi
one to each lung
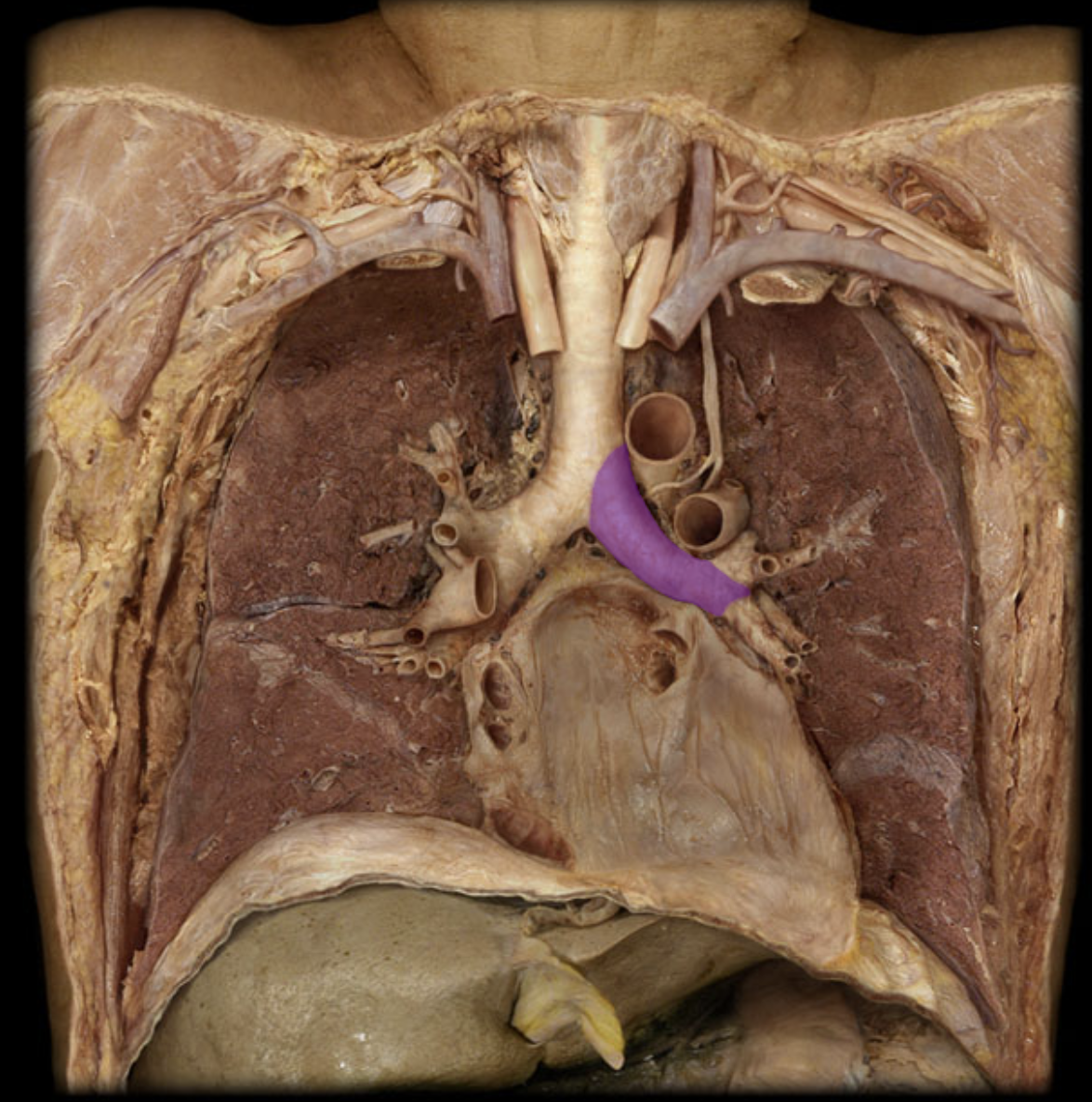
Carina
landmark junction where trachea splits
one of the most sensitive regions for triggering a cough
Right main bronchus
wider
short
more vertically oriented than the left
more susceptible to foreign body obstruction
Inside the lungs…
the main bronchi continue branching into lobar and segmental bronchi
eventually into bronchioles
even smaller airways
eventually end in alveoli
Bronchial tree
formed from the branching of bronchi in the lungs
Alveoli
clusters of microscopic air sacs
surrounded by capillaries
primary site of gas exchange
Gas exchange in alveoli
O2 from inhaled air diffuses across thin alveolar walls into blood within capillaries
CO2 moves from the blood into alveoli to be exhaled
Lungs
spongy
cone shaped
located in throacic cavity
each is surrounded by pleura
Right lung
3 lobes
Left lung
2 lobes
to accommodate space occupied by the heart
pleura
double layered membrane
reduces friction
allows lungs to move smoothly during breathing
Diaphragm
dome-shaped sheet of muscle located beneath lungs
primary muscle for breathing
When the diaphragm contracts…
flattens and increases volume of the throacic cavity
draws air into lungs
Intercostal muscles
located between ribs
assist by expanding and contracting the rib cage during inhalation and exhalation
2 zones of respiratory system
conducting zone
respiratory zone
conducting zone
nose
pharynx
larynx
trachea
bronchi
terminal bronchioles
primarily:
transport
filter
warm
humidify incoming air
Respiratory zone
respiratory bronchioles
alveoli
where gas exchange takes place
Lung volumes and capacities
measurements used to describe the amount of air contained in the lungs during different stages of the breathing cycle
provide important info about respiratory mechanics and overall lung function
Lung volumes
individual amounts of air present during specific phases of respiration
Lung capacities
combinations of two or more lung volumes
derived by combining two or more of these volumes
represent the functional limits of lung expansion and contraction
Tidal volume
amount of air inhaled or exhaled during a normal breathing cycle
typically ranges from 300-500 mL or 6-8 mL per kilogram of body weight
reflects:
activity of respiratory centers
strength of the respiratory muscles
mechanical properties of lungs and chest wall
can increase due to deep breathing or exercise
Inspiratory reserve volume (IRV)
the additional amount of air that can be forcibly inhaled after normal inhalation
becomes important for deep breathing or physcial exertion
usually not used during quiet breathing
normal range from 1900-3300 mL
Expiratory Reserve Volume (ERV)
extra amount of air that can be forcefully exhaled after normal exhalation
normal value typically 700-1200 mL
certain conditions such as:
obesity
abdominal pressure
recent abdominal surgery
can reduce ERV
Residual Volume (RV)
amount of air that remains in the lungs after maximal exhalation
this air cannot be voluntarily expelled
helps prevent lung collapse by keeping the alveoli partially inflated
average is 1200 mL
cannot be measured directly by spirometry
estimated using other lung measurments
In obstructive lung diseases….
such as emphysema
RV may increase due to air trapping and incomplete emptying of lungs
Inspiratory Capacity (IC)
maximum amount of air that can be inhaled following a normal exhalation
calculated as IC=TV +IRV
Vital capacity
represents the total volume of air that can be exhaled after a maximal inhalation
VC = TV + IRV + ERV
averages around 3100-4800 mL
varies depending on body size, age, and sex
reflects the ability to take deep breaths and produce an effective cough (important for clearing secretions from respiratory tract)
Functional Residual Capacity (FRC)
the volume of air remaining in the lungs at the end of a normal exhalation
FRC = RV + ERV
represents the resting position of the lungs where the inward elastic recoil of the lungs is balanced by the outward recoil of the chest wall
Total lung capacity (TLC)
maximum volume of air the lungs can contain after a maximal inhalation
sum of all four primary lung volumes ( TLC = TV+IRV+ERV+RV)
averages 4-6 L
Changes in TLC
may indicate certain pulmonary disorders
may increase in obstructive diseases such as emphysema
may decrease in restrictive conditions such as pulmonary fibrosis or ches wall abnormalities
Lung sounds
aka respiratory sounds
produced by air moving through the repiratory tract
can provide important info about lung health
Vesicular sound
soft, low pitched rustling noise heard over most of the lung fields
Bronchovesicular sounds
medium pitched
heard near major airways
Bronchial sounds
louder, high pitched
heard over trachea
adventitious breath sounds
abnormal sounds
may indicate underlying respiratory problems
Wheezes
high-pitched, musical sounds
caused by narrowed airways
commonly associated w conditions such as asthma or COPD
Crackles (rales)
bubbling or clicking sounds
produced when fluid is present in alveoli
may occur w pneumonia or heart failure
Rhonchi
low-pitched snoring like sound heard during inspiration
caused by mucus or obstruction within the larger airways
Stridor
harsh, high pitched sound heard during inspiration
often signals a seruous upper airway obstruction
Pleural friction rub
grating or creaking noise
compared to walking on fresh snow
caused by inflamed pleural surfaces rubbing together during breathing
Spirometry
measurments of lung volumes and capacities
noninvasive pulmonary function test
measures both the volume and speed of air moving in and out of lungs
helps evaluate lung function and diagnose respiratory conditions
2 Key measurments during spirometry
Forced Vital Capacity (FVC)
Forced expiratory volume in one second (FEV1)
help distinguish between obstructive diseases and restrivtive diseases
Forced Vital capacity (FVC)
total amount of air that can be forcefully exhaled after a deep inhalation
Forced Expiratory volume in 1 second (FEV1)
measures how much air can be expelled during the first second of exhalation
Obstructive disease
airway narrowing and reduced airflow
Restrictive disease
limit lung expansion
Largest amount of CO2 is…
hydrated and carried in the form of bicarbonate in the blood plasma
In red blood cell, CO2…
reacts w water to form carbonic acid in a reaction catalyzed by carbonic anhydrase
dissociates into
H+
binds to hemoglobin—→ forms deoxydemoglobin
bicarbonate
exchanged for chloride and pumped out of the red blood cell into plasma
also found in blood plasma from CO2 diffusing into bloodstream
This occurs slowly due to no carbonic anhydrase in blood plasma
CO2 can be…
bound to hemoglobin in RBCs
CO2 enters red blood and attaches to hemoglobin —→forms carbaminohemoglobin (HbCO2)
second most common way CO2 is carried in blood
CO2 can also enter the blood as…
dissolved gas similar to carbonated beverages
the more dissolved CO2 present in blood, the more H+ will be released into plasma and the lower the pH will be
least common way CO2 is carried from tissues to lungs
Arterial blood gas (ABG)
arterial blood test
usually drawn from radial artery
used to assess CO2, O2, pH levels
measures the amount of gas pressure in an artery
PaCO2
partial pressure of CO2 in an artery
normal range is 35-45 mmHg
PaO2
partial pressure of oxygen in an artery
normal range is 80-110 mmHg
SaO2
oxygen saturation level
percent of hemoglobin molecules saturated w oxygen
Normal is 95-100%
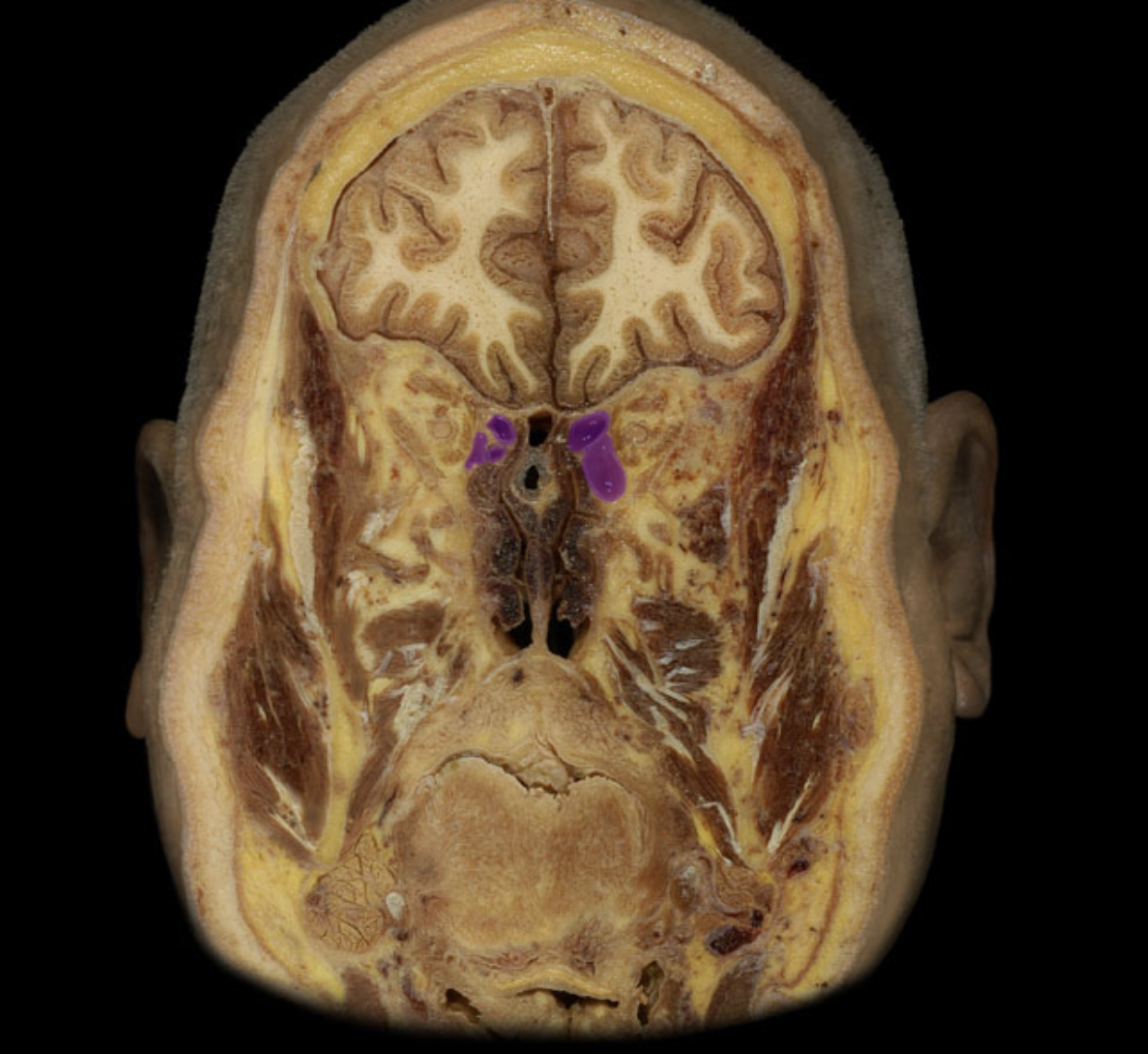
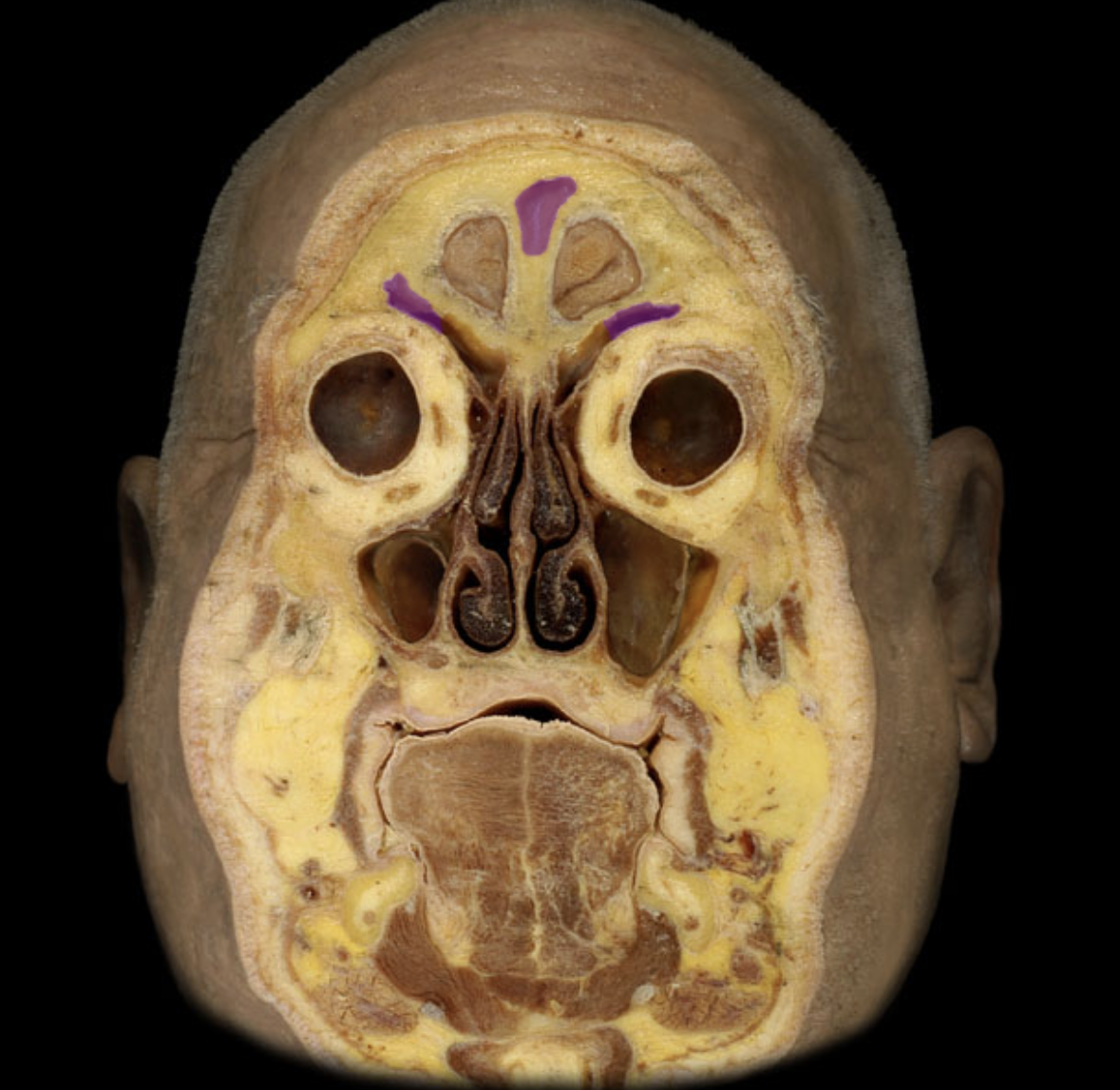
Ethmoid cells
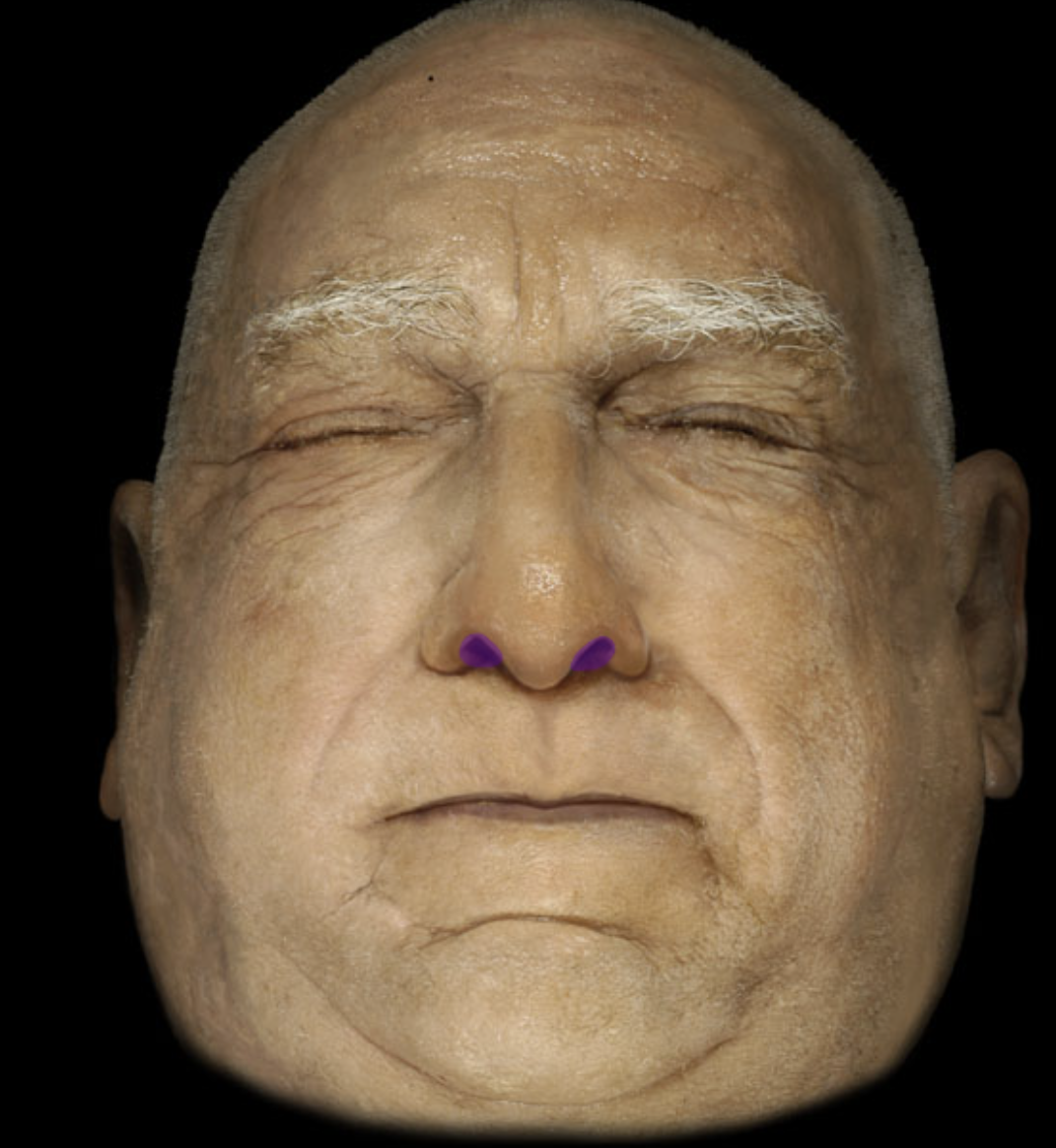
External naris
Frontal sinus
hard palate
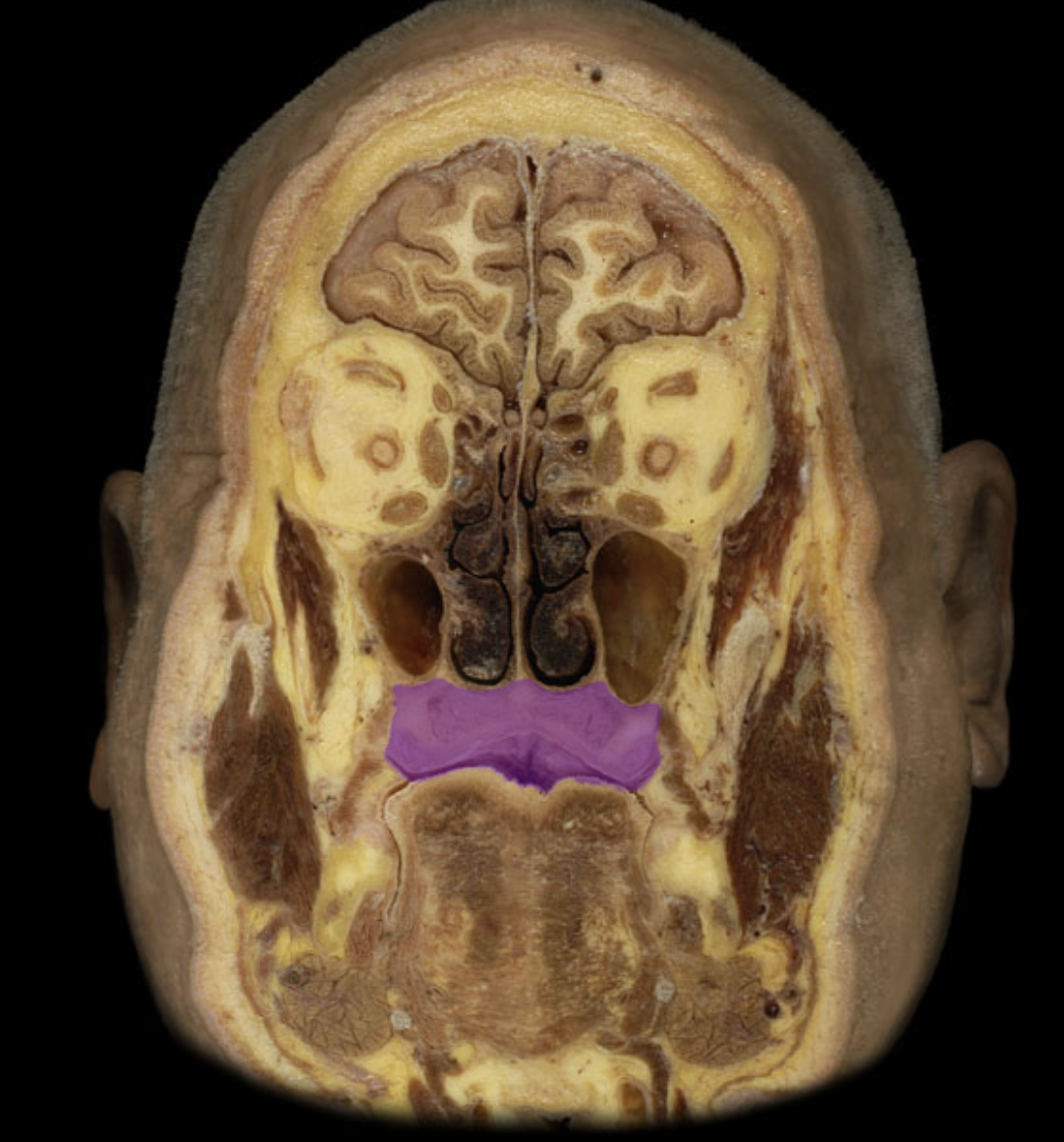
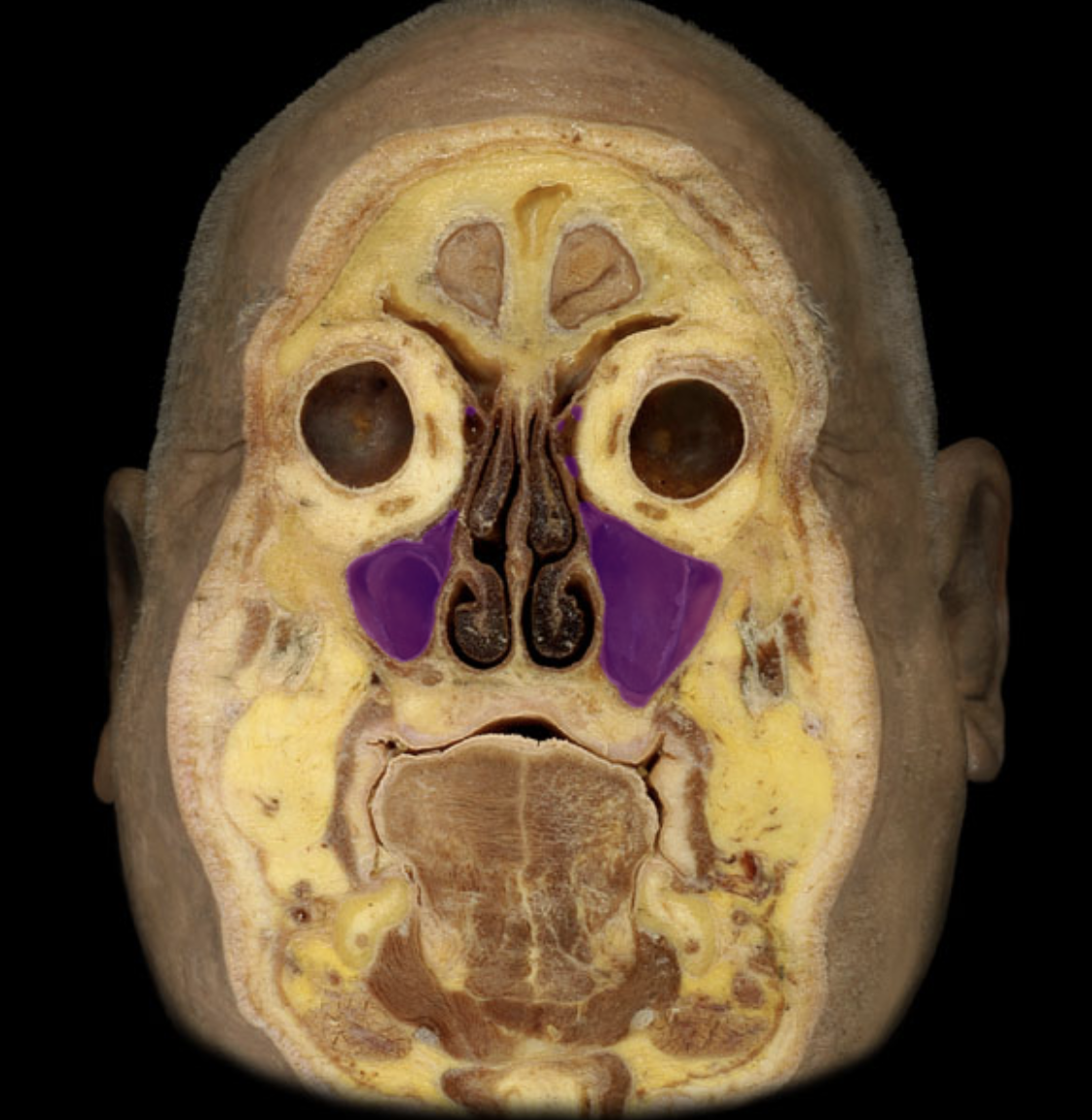
maxillary sinus
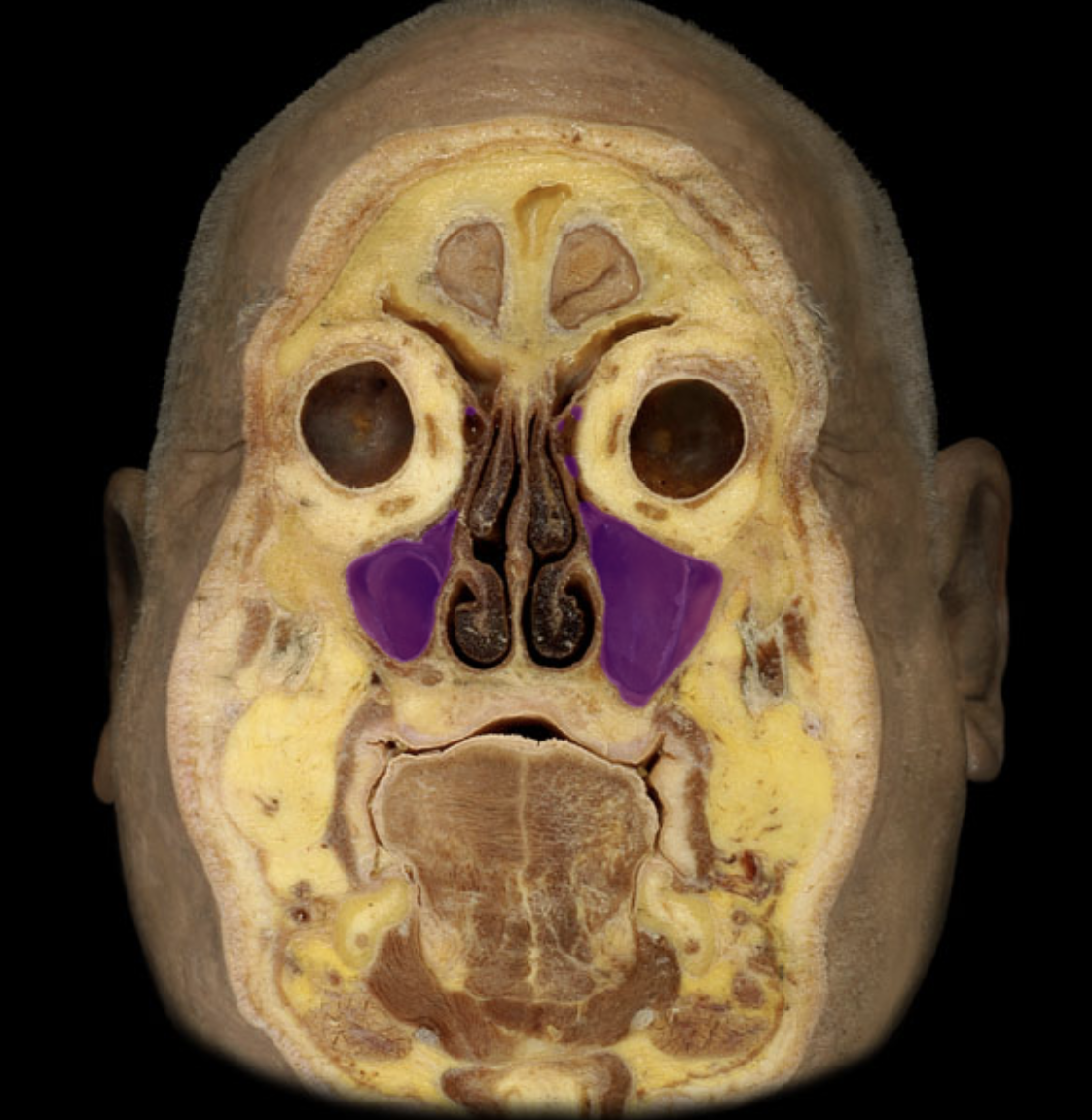
nasal cavity
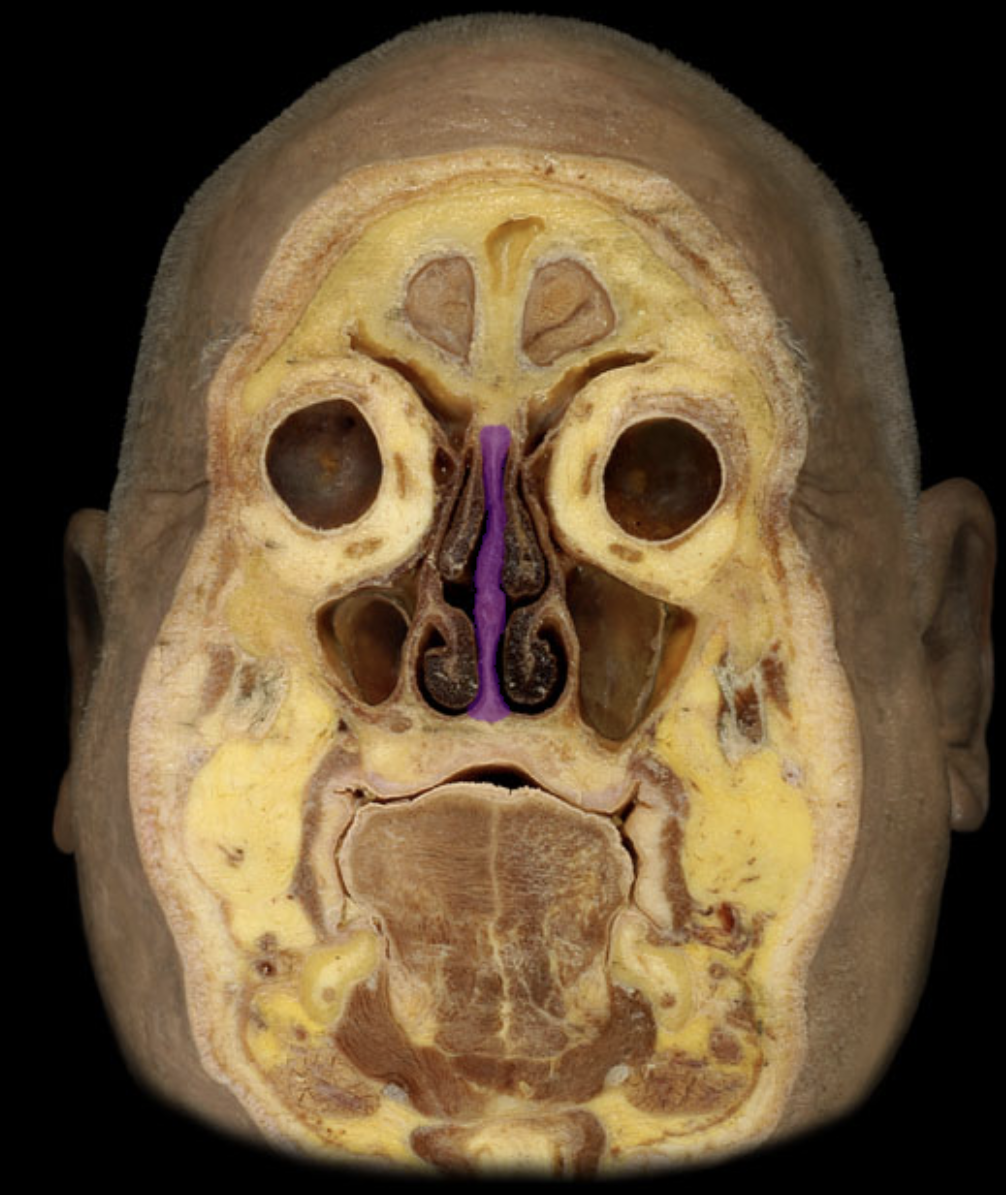
nasal septum
sphenoidal sinus
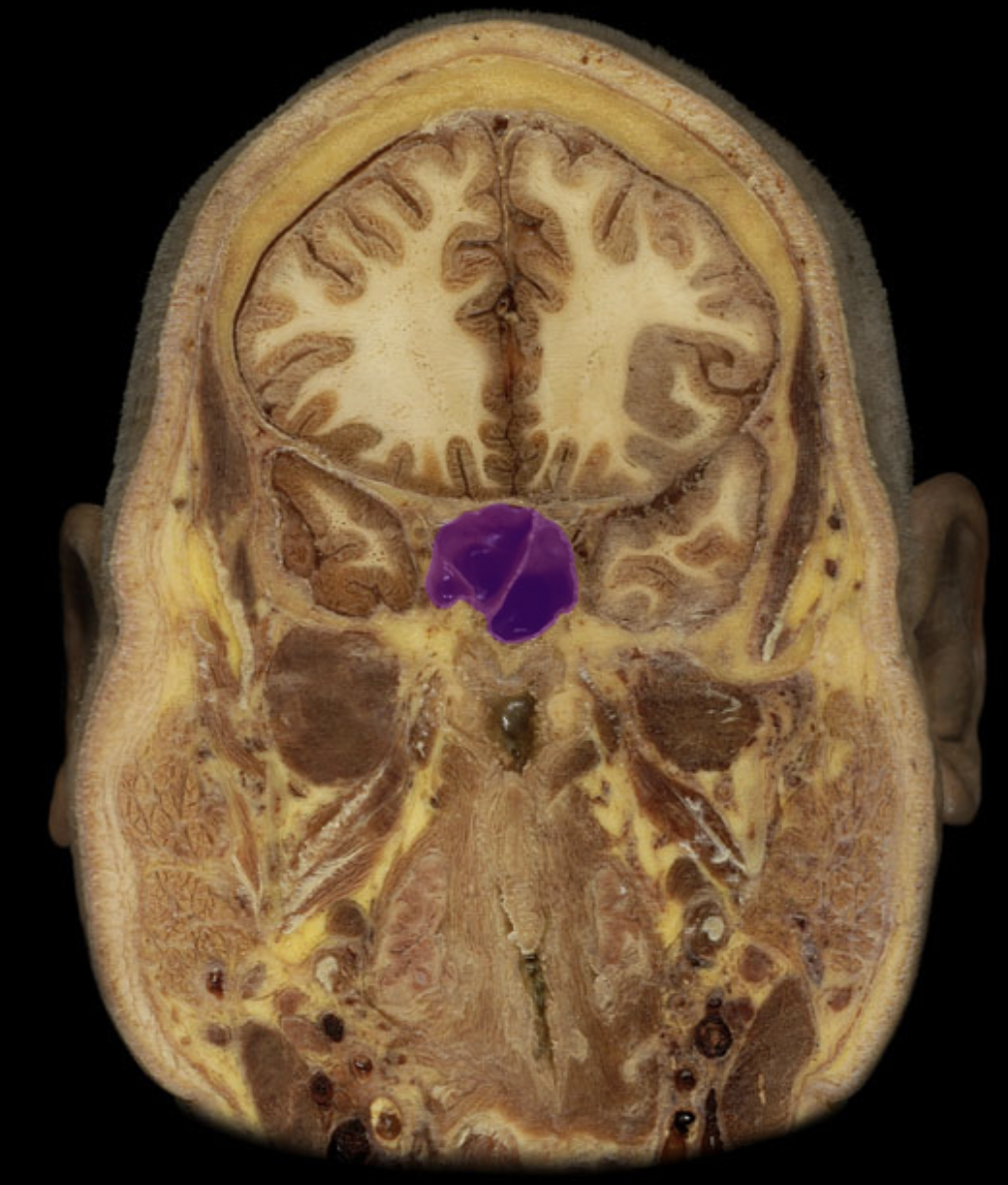
Uvula
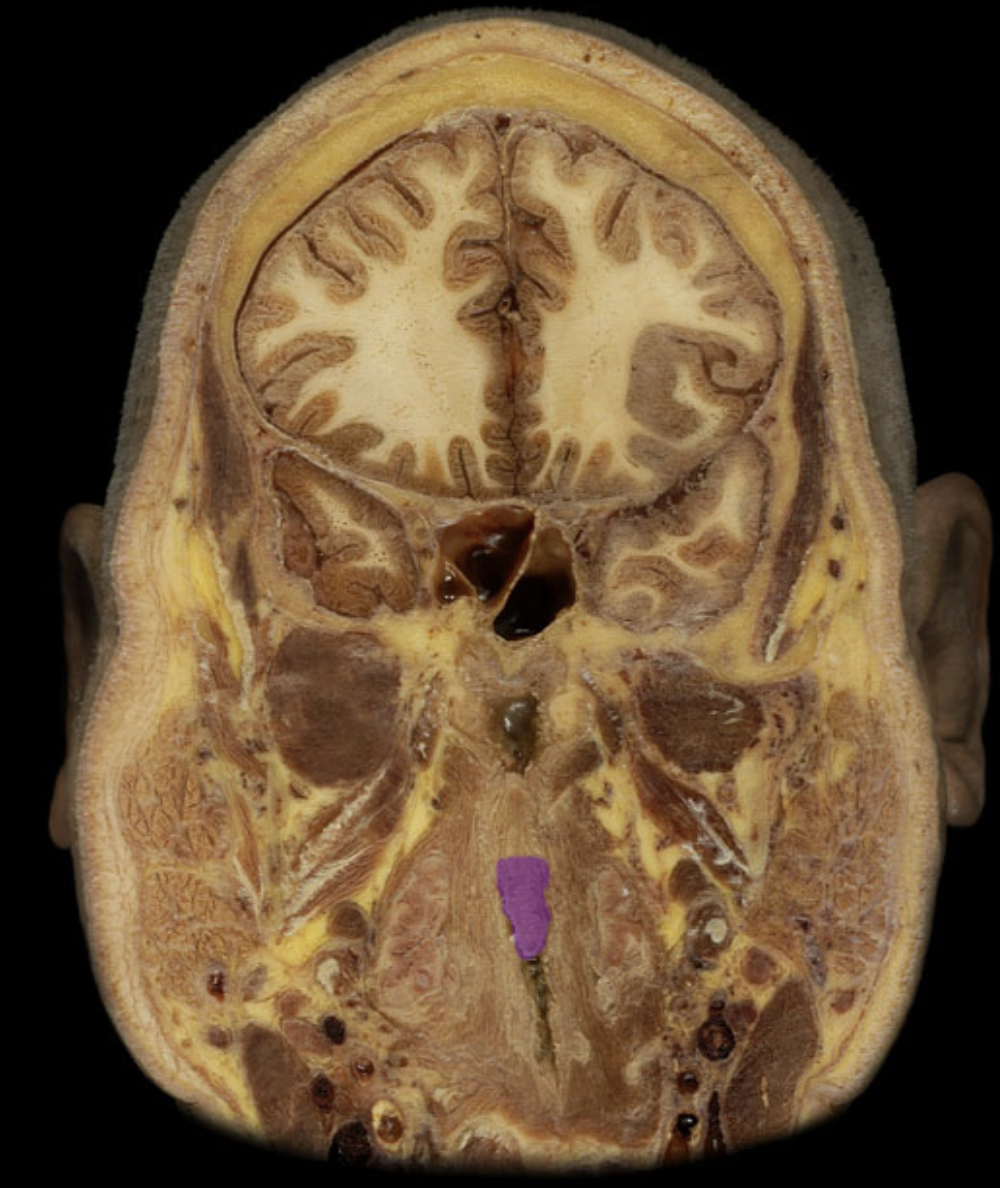
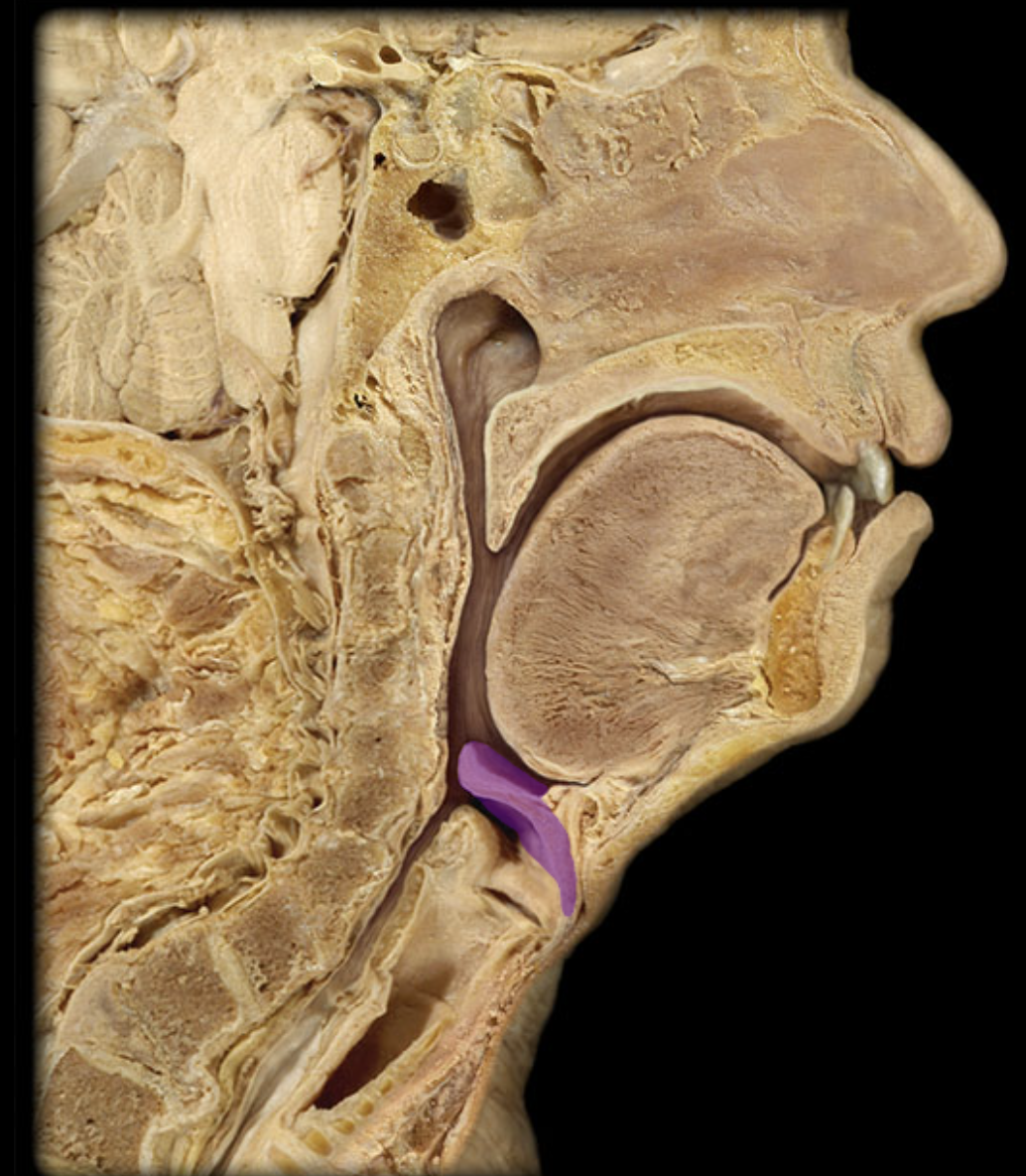
Epiglottis
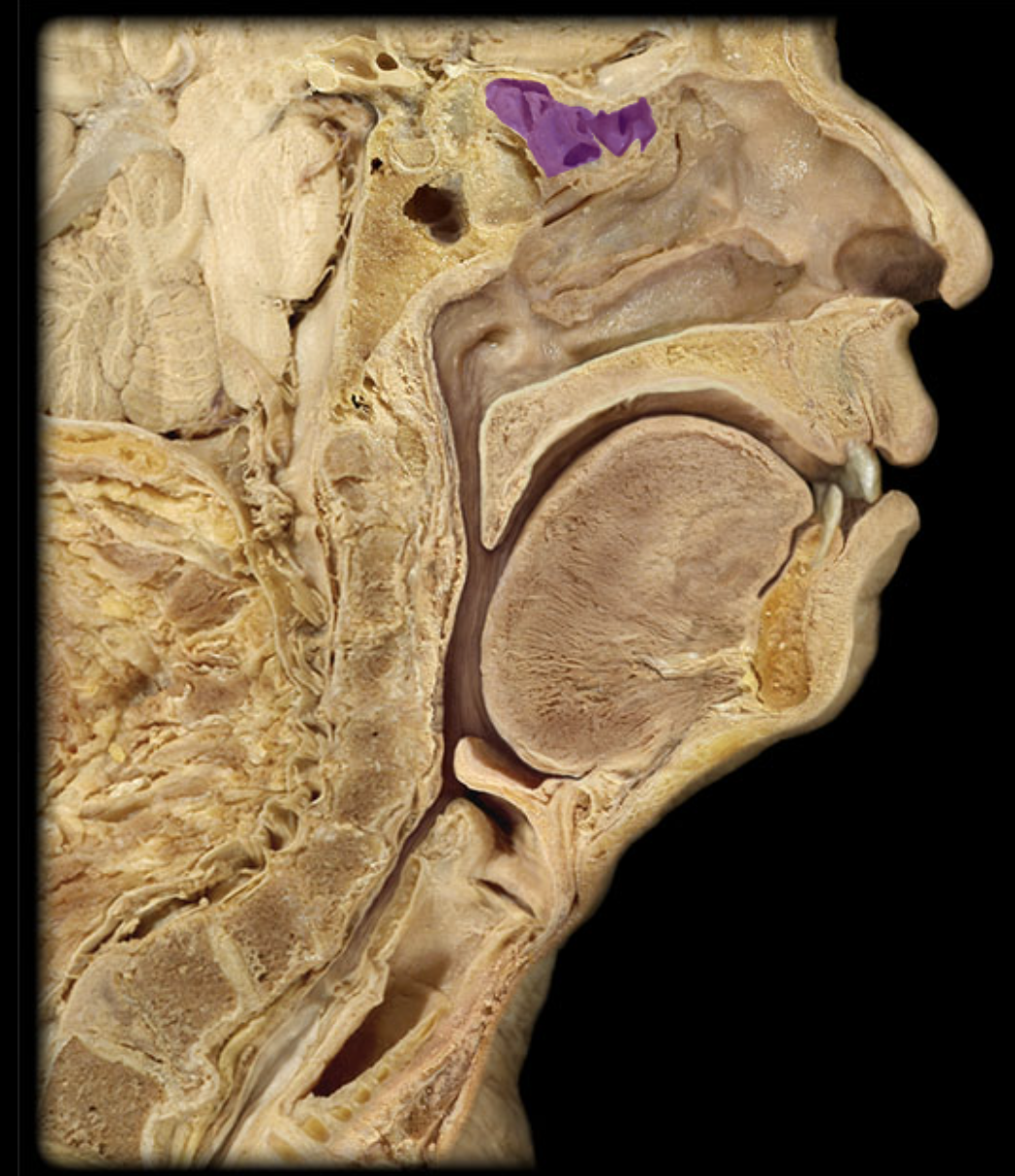
Ethmoid cells
inferior nasal concha
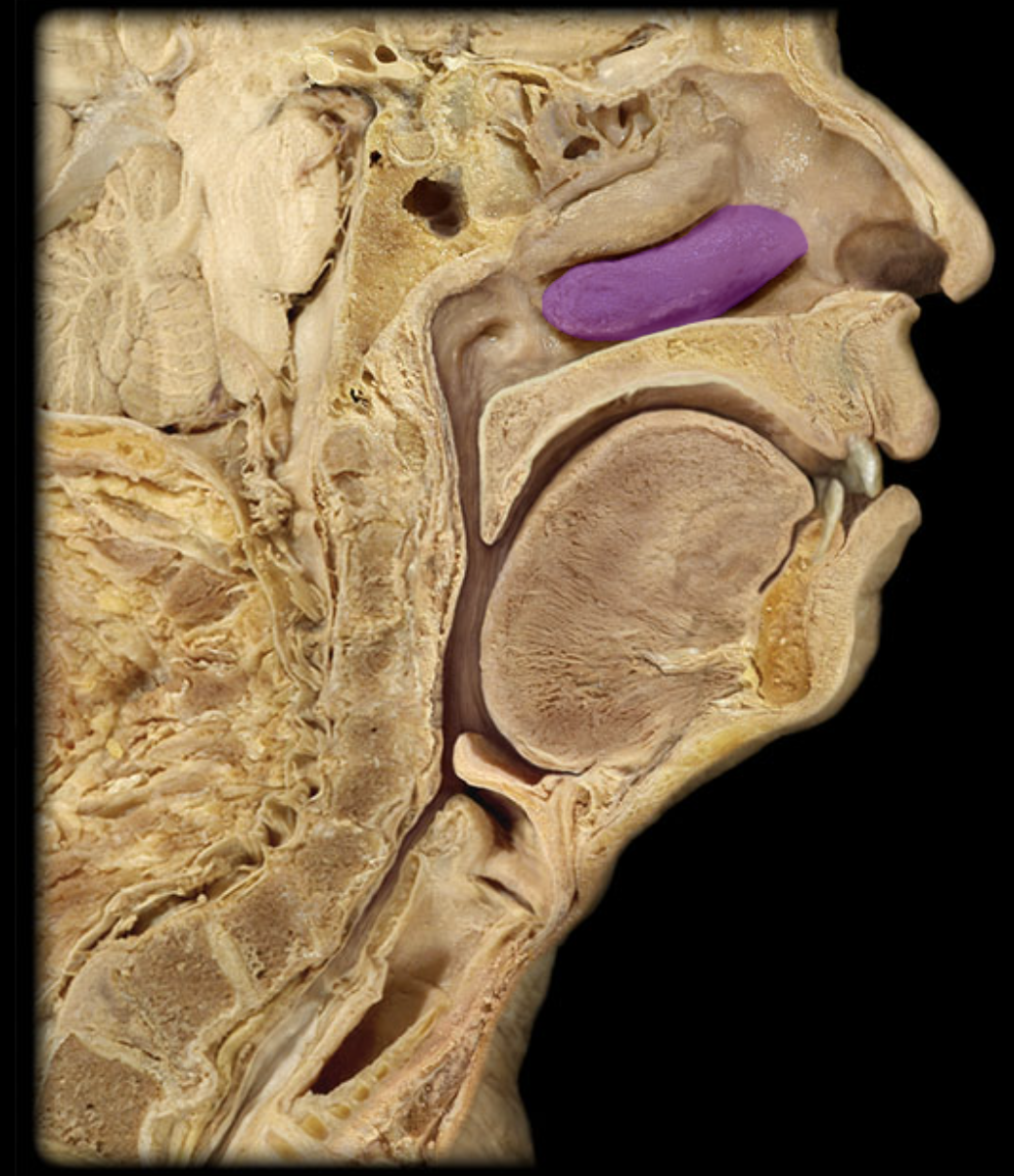
Hard palate
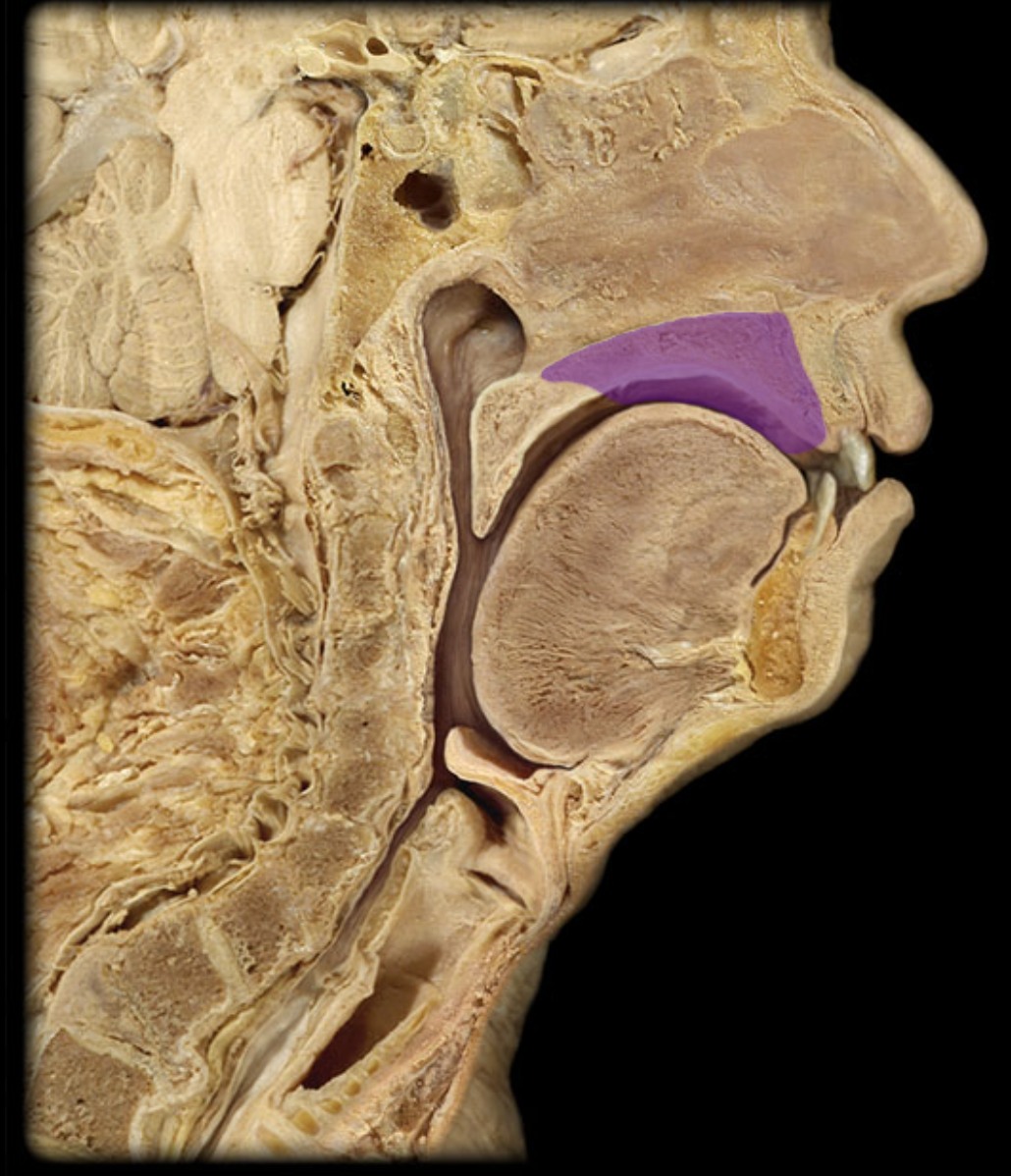
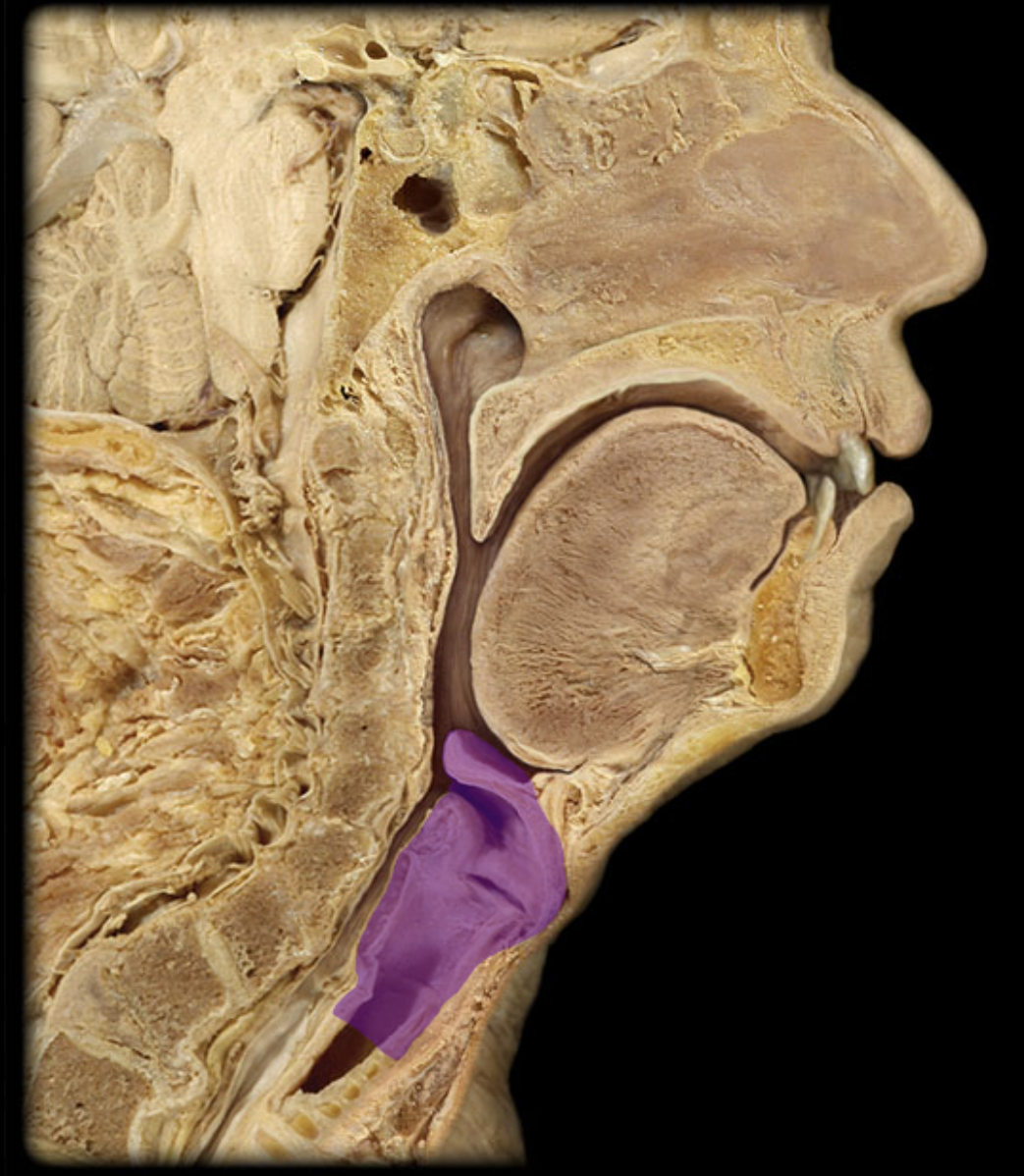
laryngopharynx
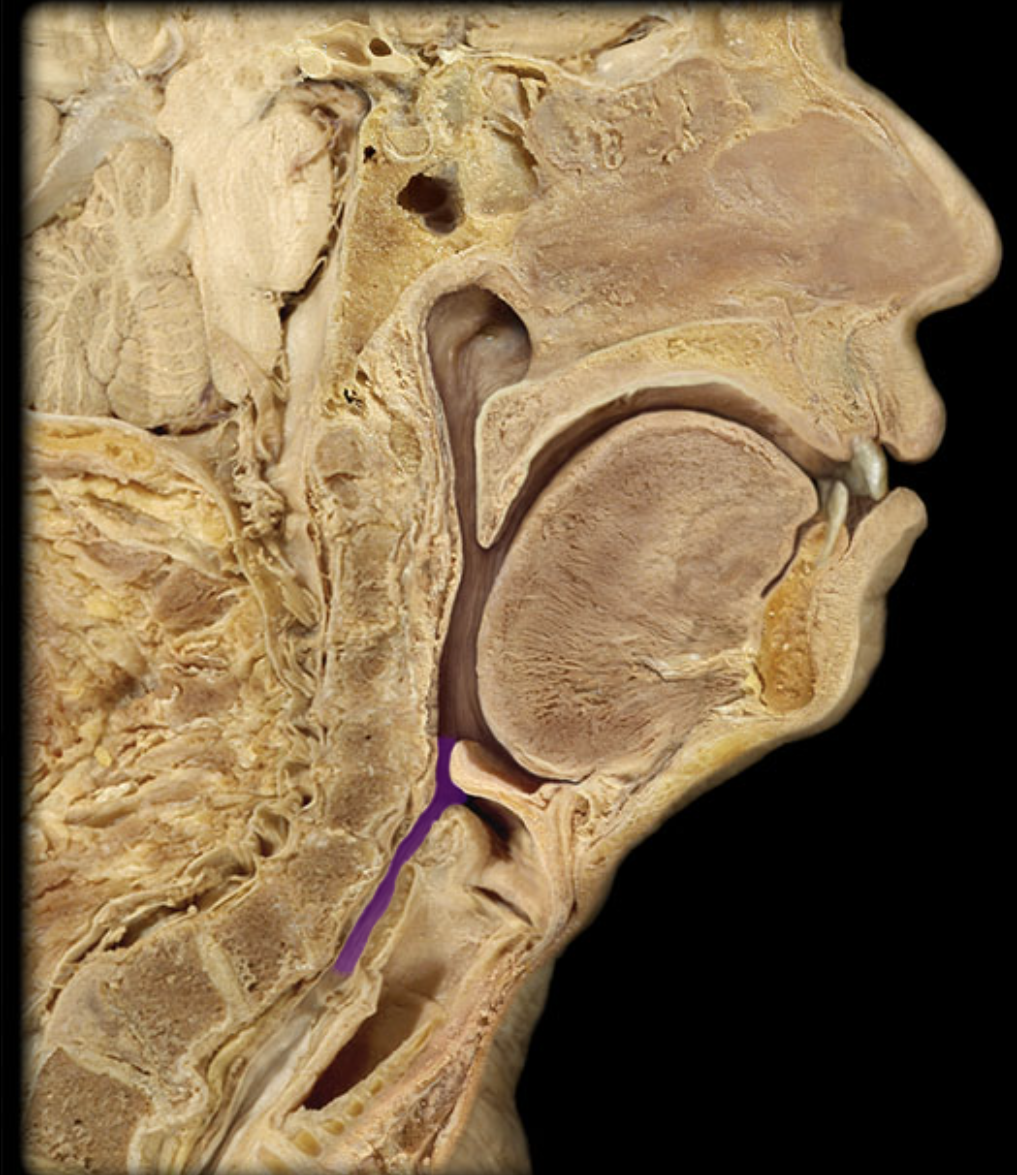
larynx
Middle nasal concha
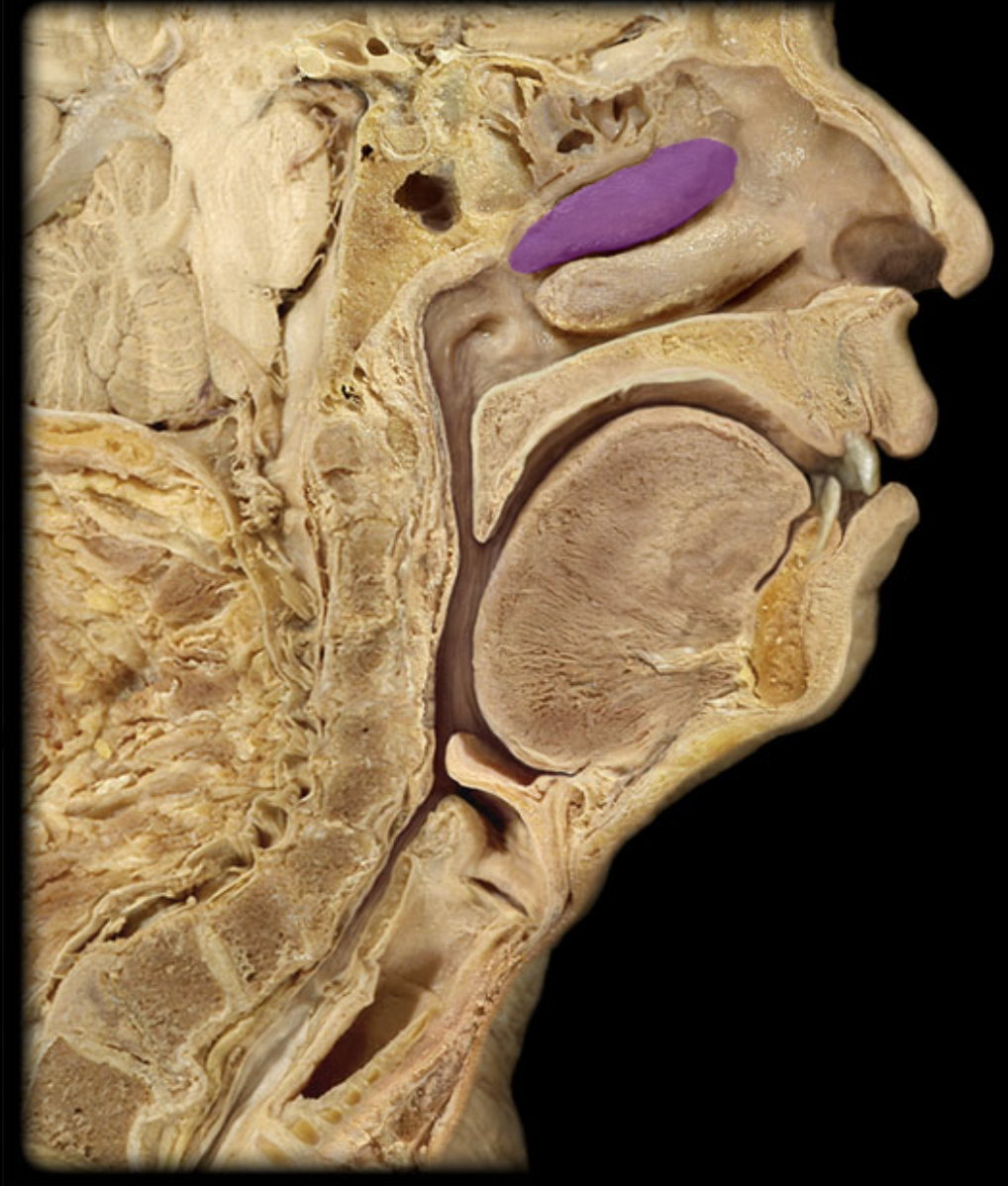
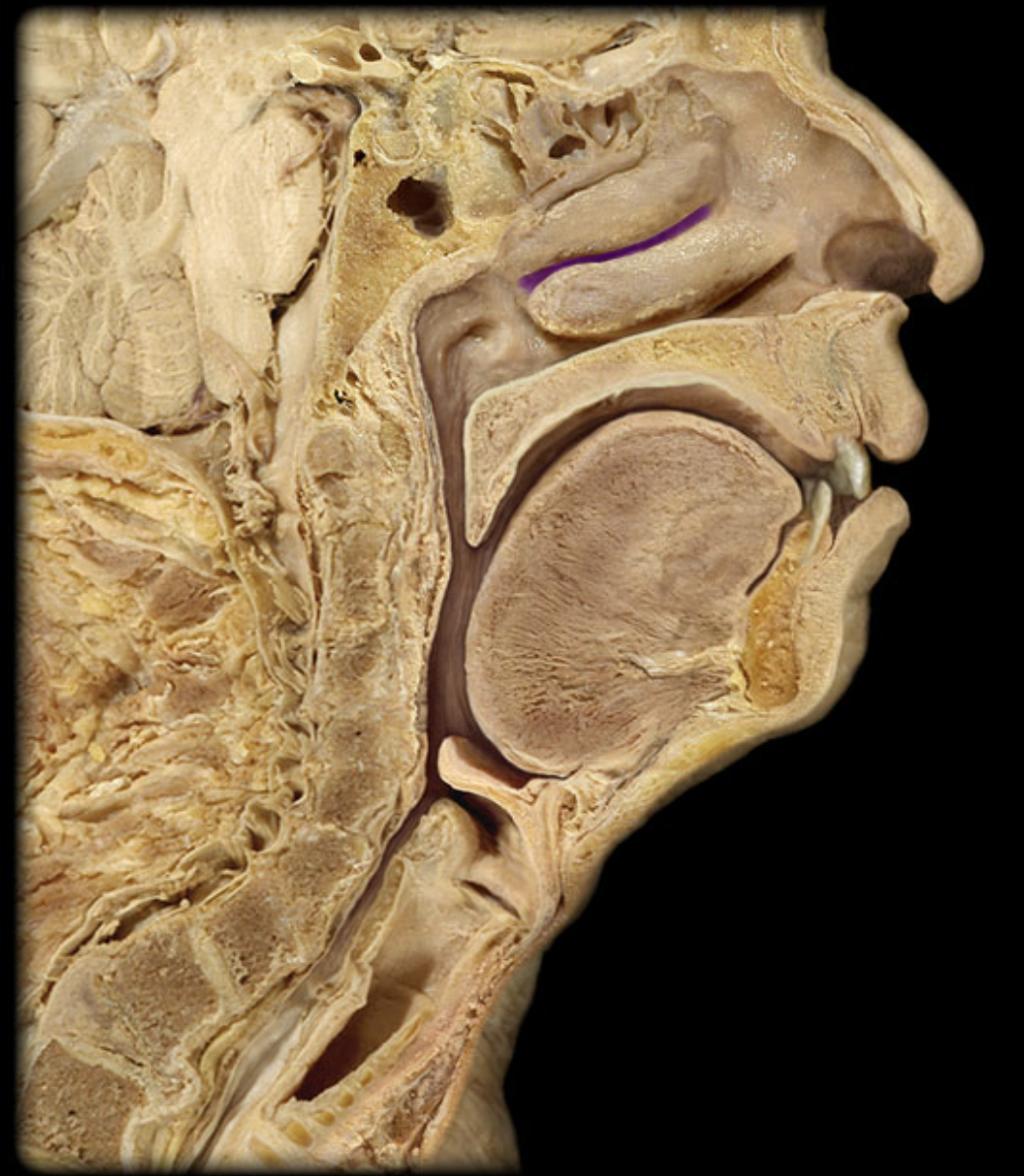
middle nasal meatus
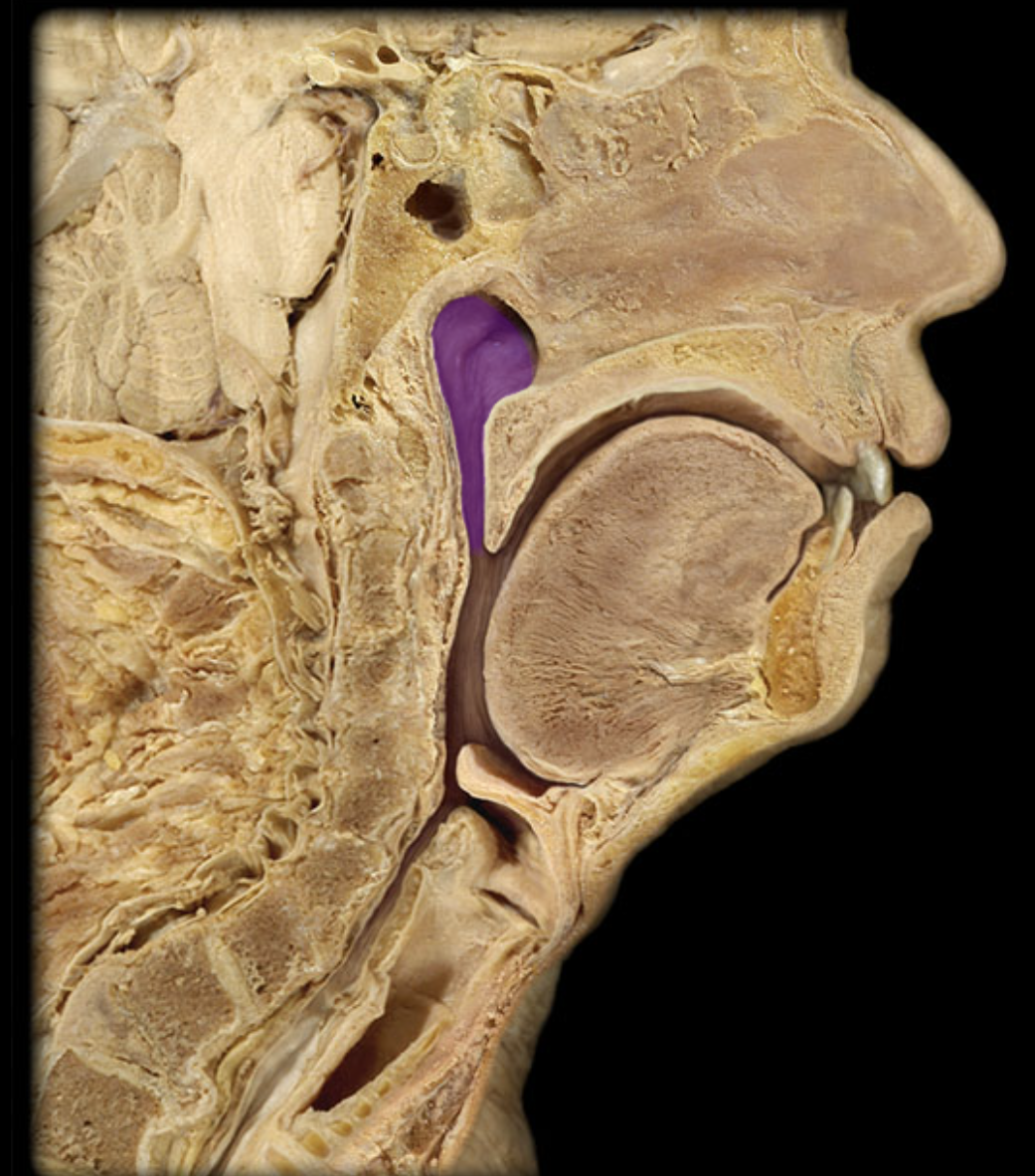
nasopharynx
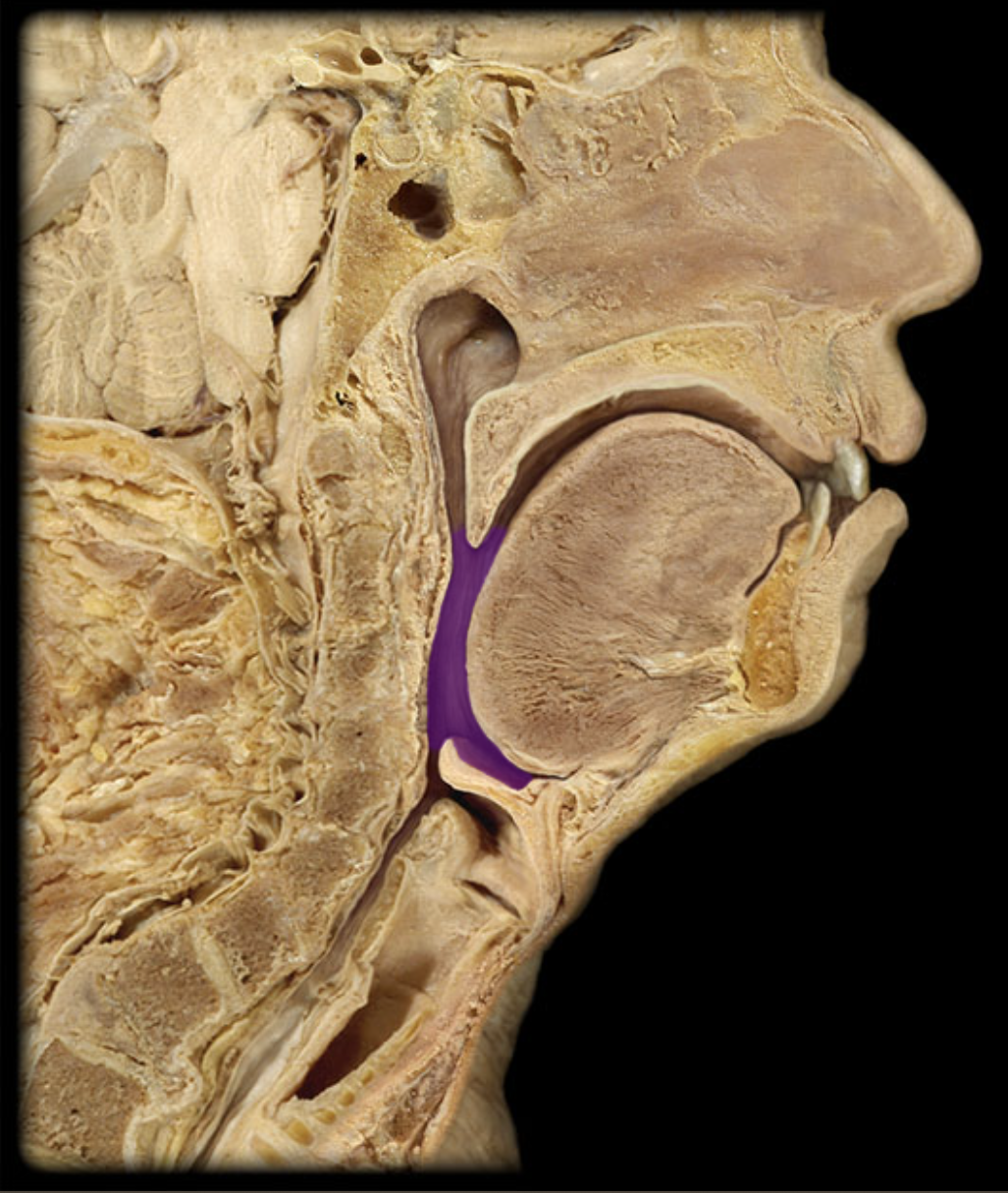
oropharynx
soft palate
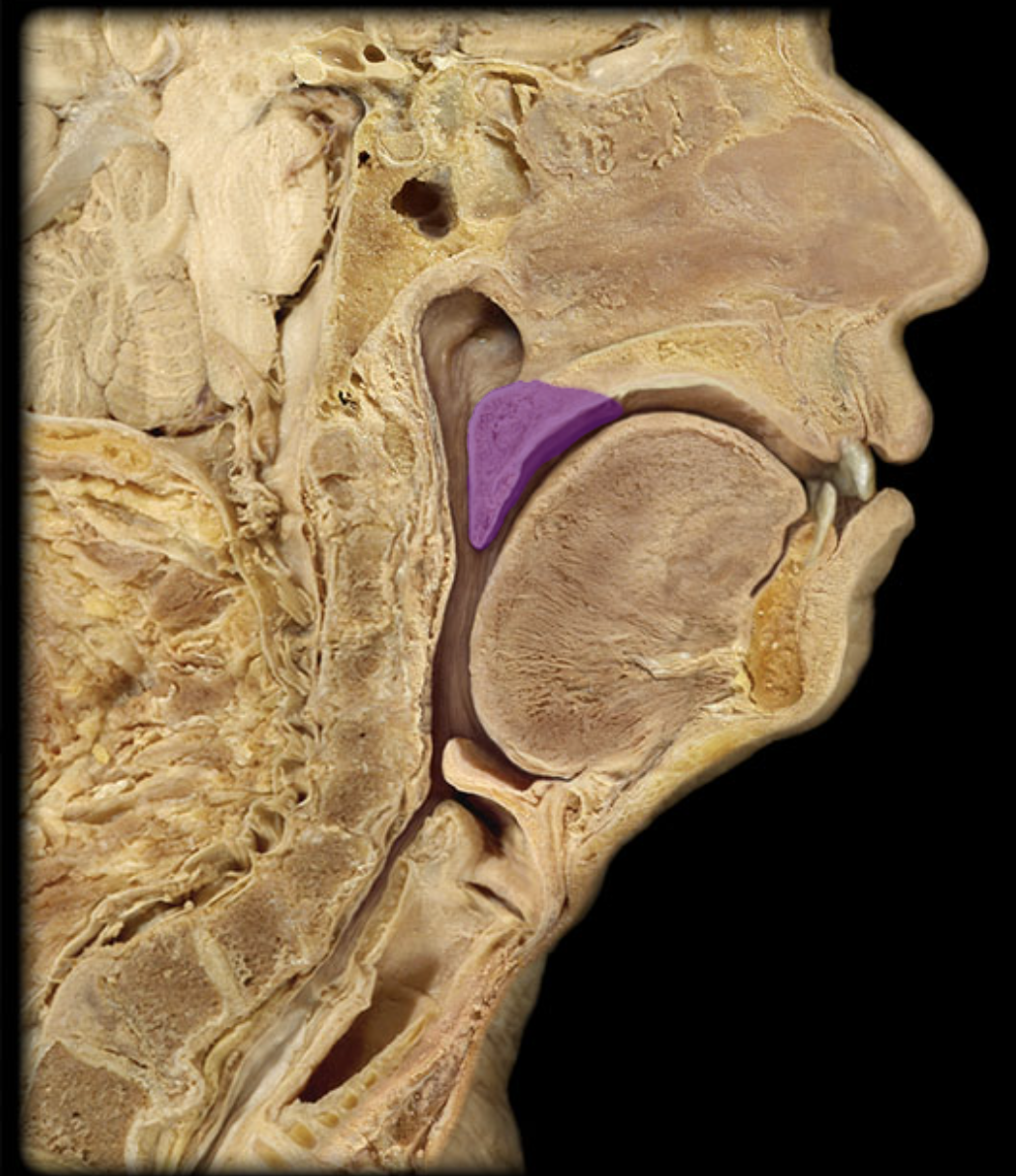
superior nasal concha
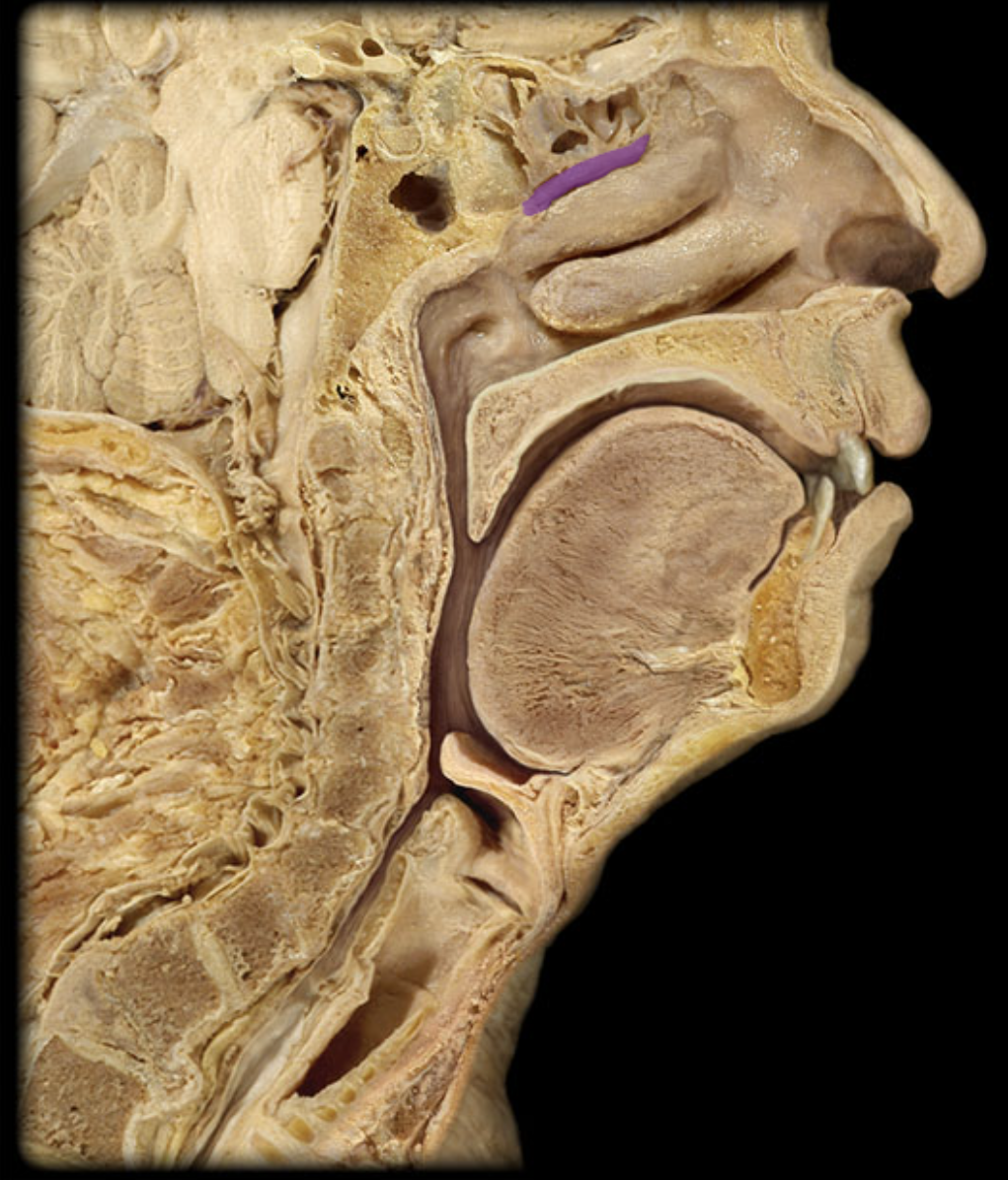
uvula
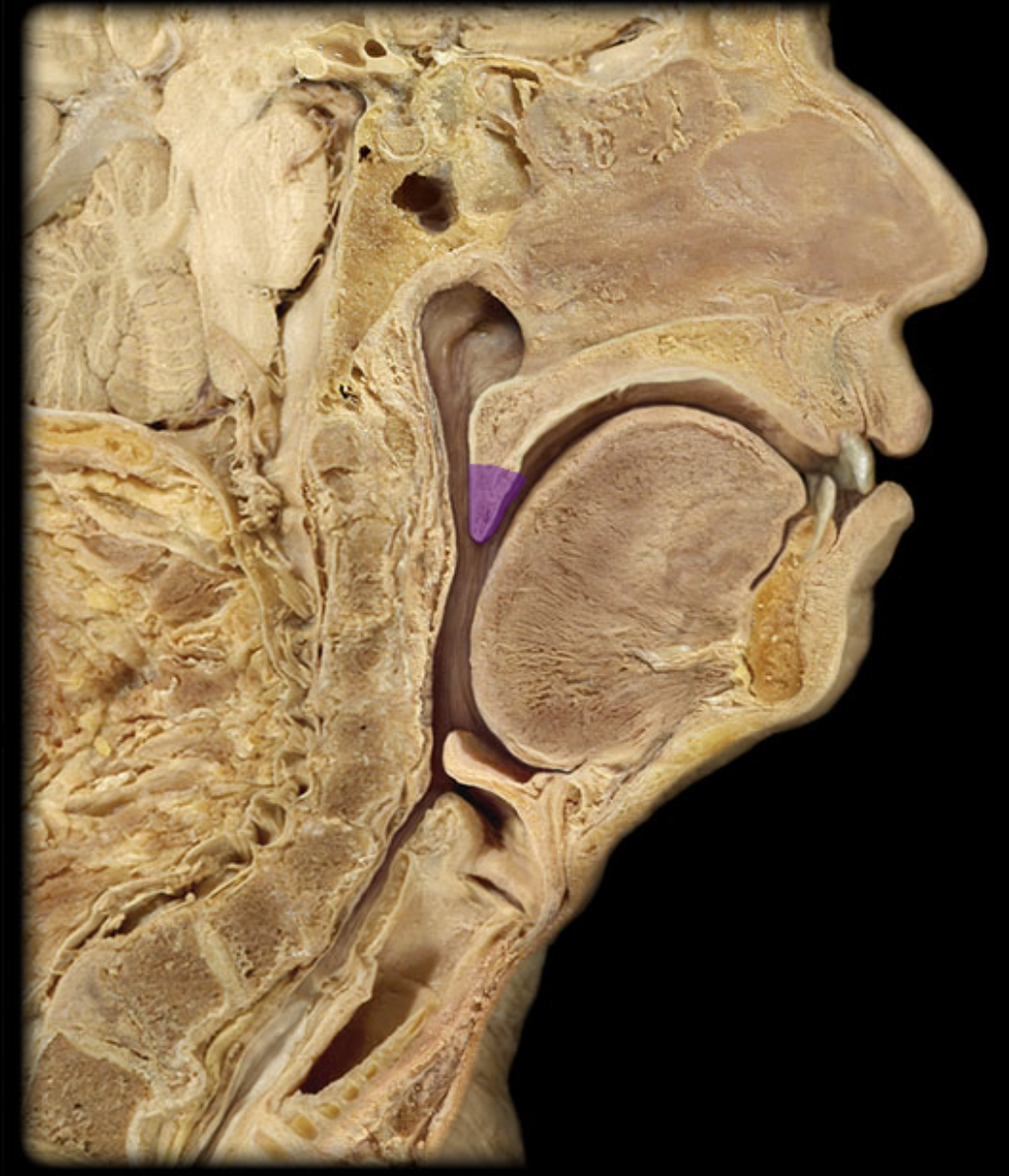
vocal fold
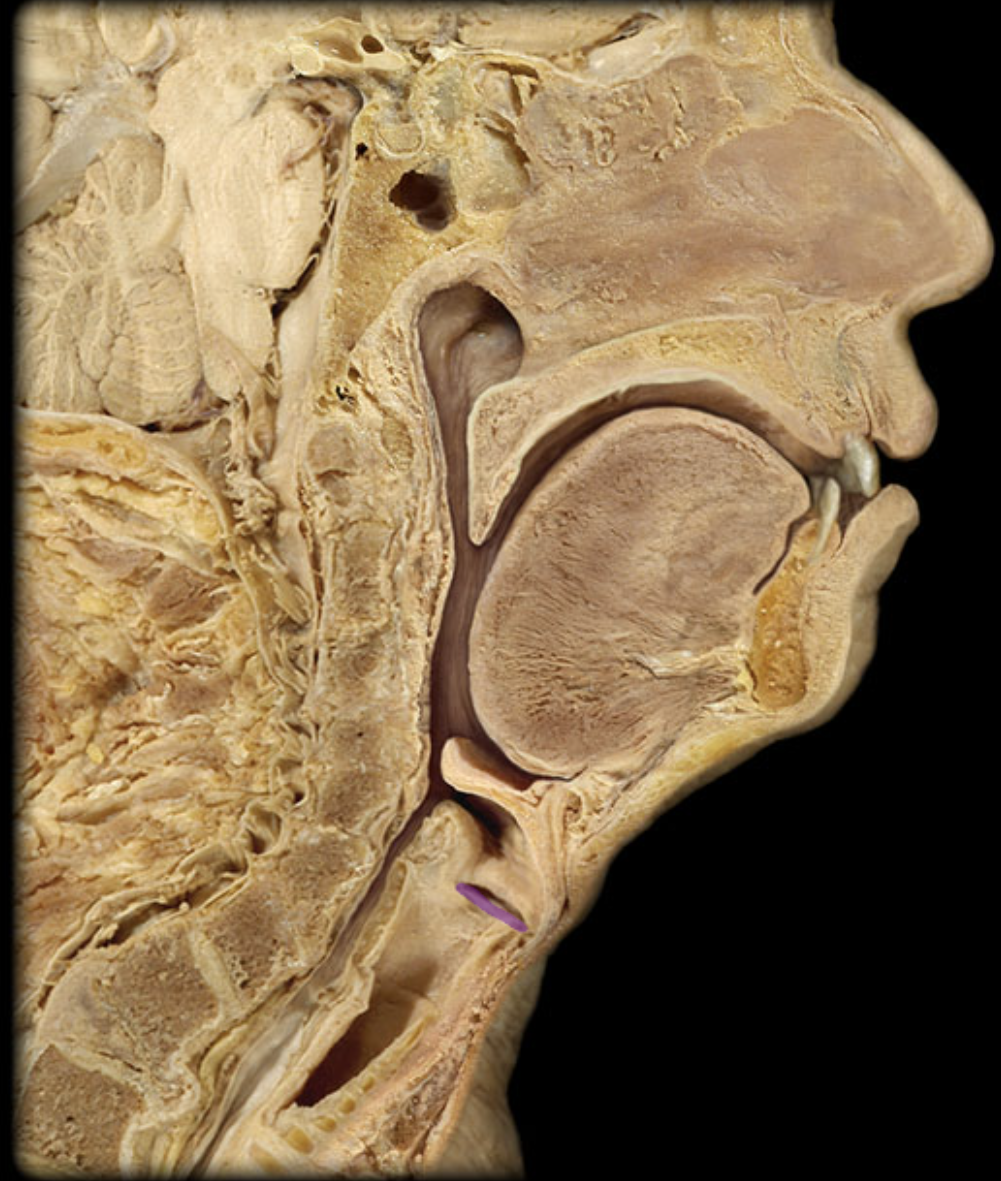
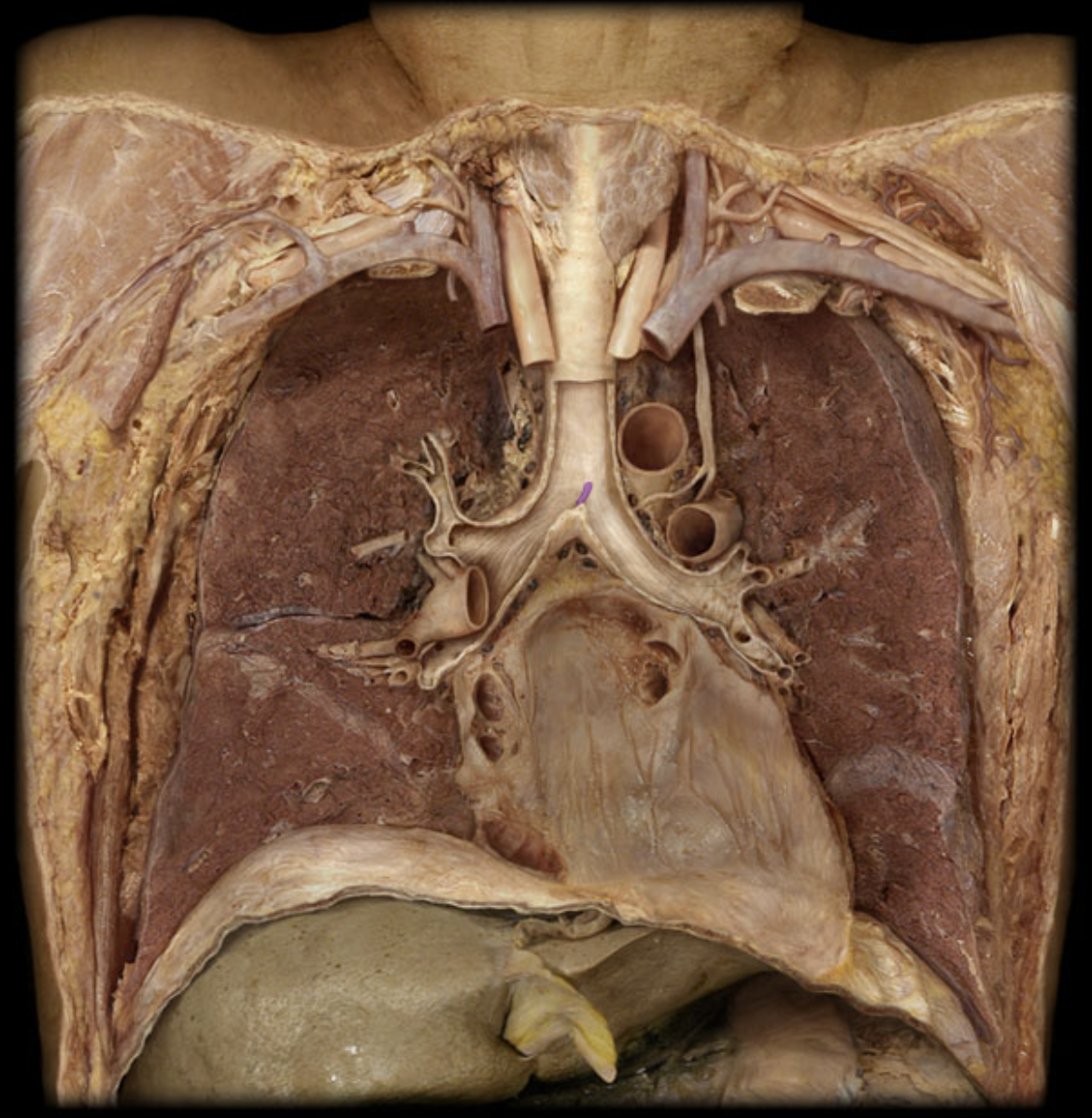
Carina
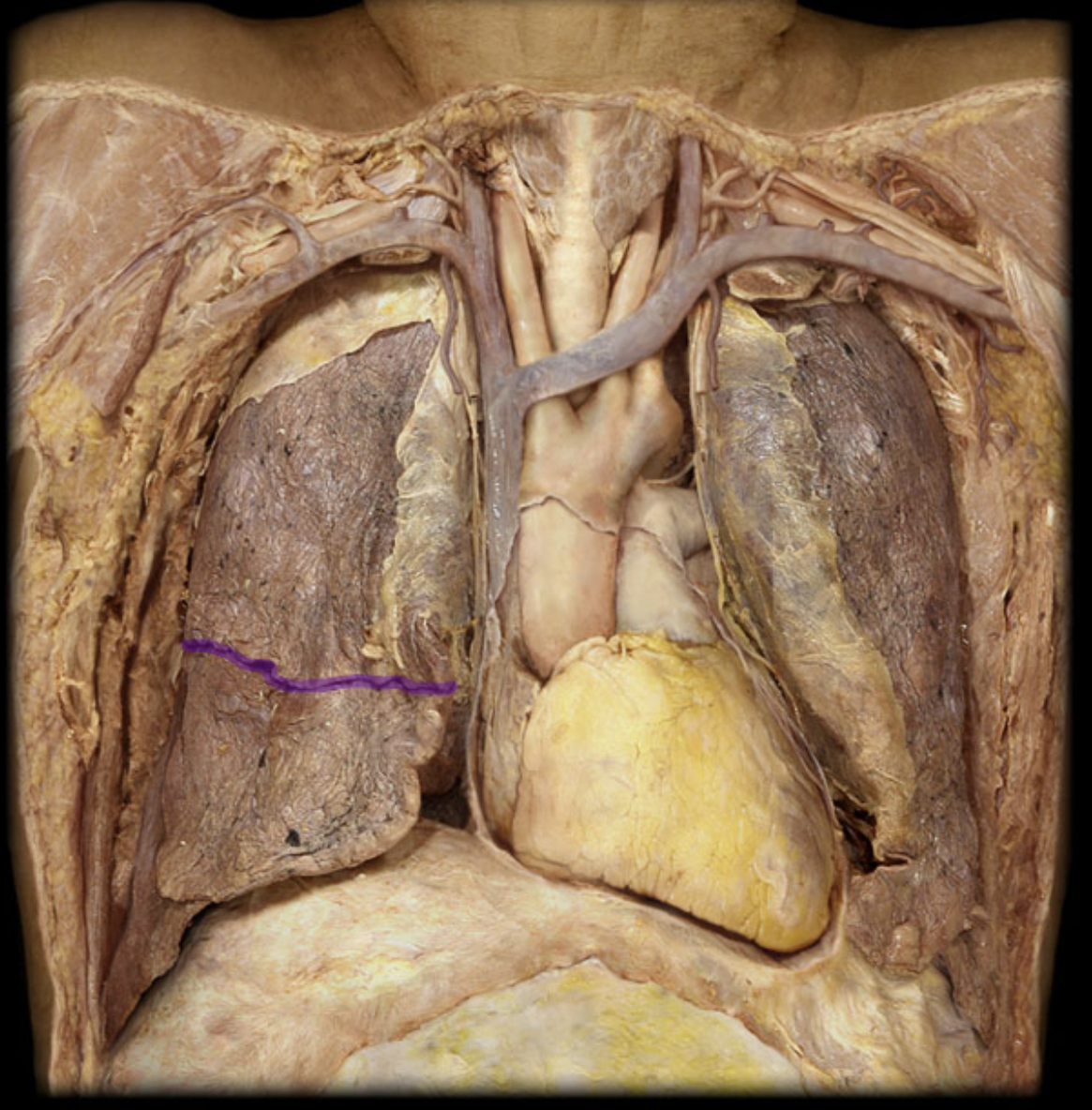
Horizontal fissure R lung
L lung
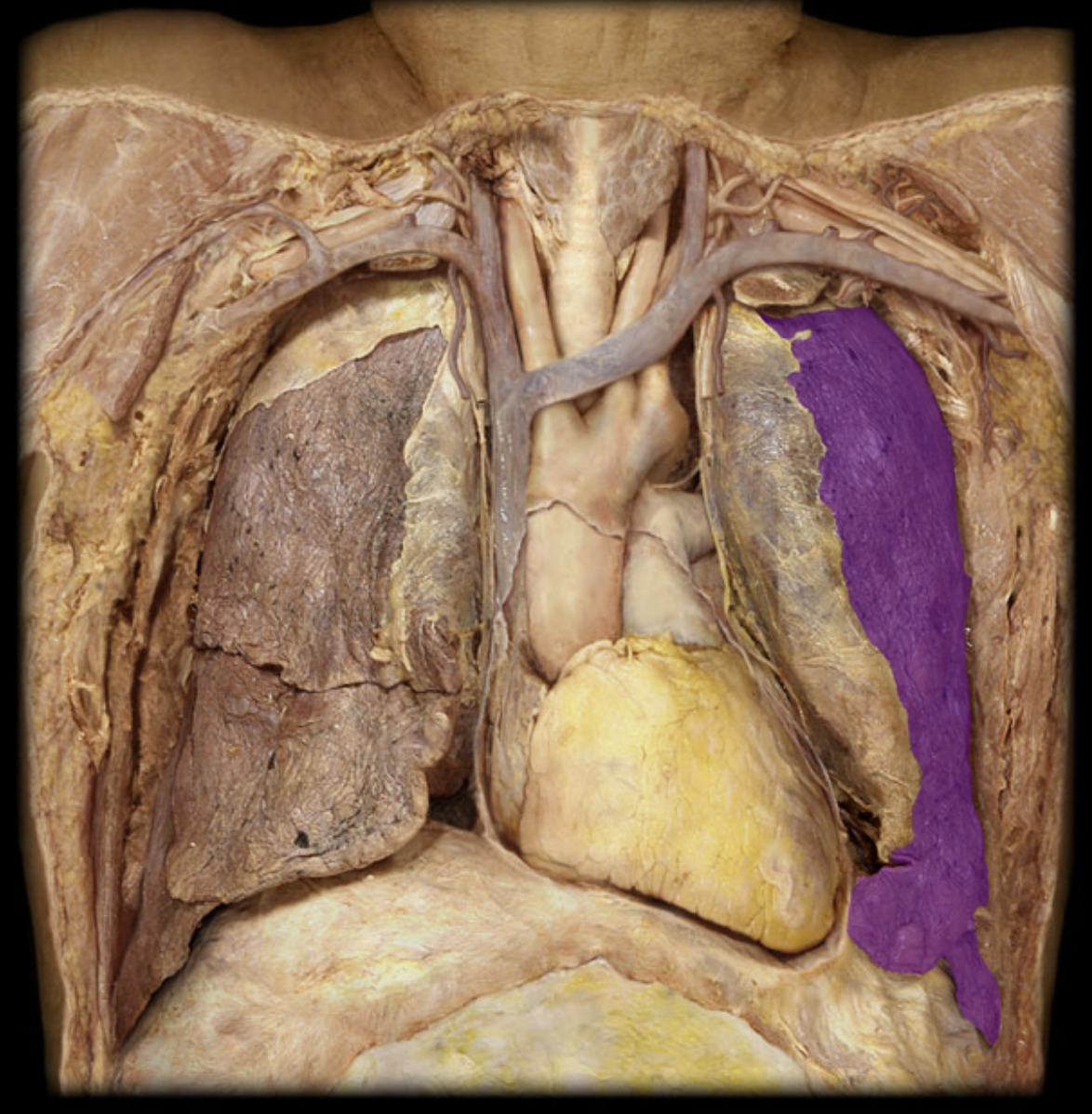
L main bronchus