Tissue Structure
1/50
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
51 Terms
What is a tissue?
A collection of similar cells that are grouped together in an organised manner to fulfil a particular function
Structure and function are linked
What are tissues made from?
Cells in a tissue are arranged within an extracellular matrix which holds them in place, and forms the bulk of the tissue
What is the extracellular matrix?
The ECM is a structure outside the cells
Provides structural support
Made of proteins
What is the function of the extracellular matrix?
Supports cells
Maintains tissue structure
Provides strength and flexibility
How do extracellular matrix proteins vary between tissues?
The ECM proteins are shaped to match the function of the tissue:
Strong fibers in bones for support
Flexible fibers in skin for stretchability
Where do extracellular matrix proteins come from?
ECM proteins are produced and modified by cells
This allows tissues to adapt and maintain their properties.
Bones
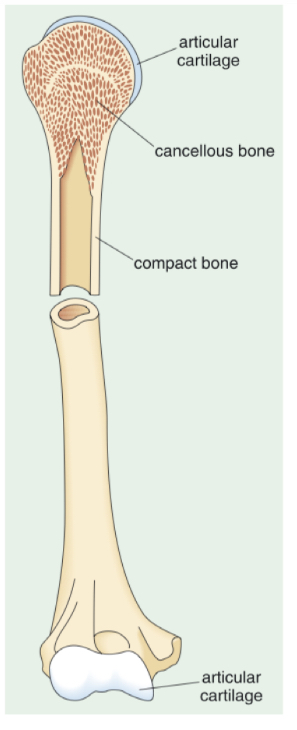
What is the structure of long bones?
Contain 2 types of bone tissue:
Compact (cortical) bone » dense and forms a hollow cylinder
Cancellous bone » within the cortical bone, less dense, honeycomb appearance
Contain cells
Contain numerous canals in which blood vessels, lymph vessels and nerves are located
Bones
Why might bones contain 2 types of bone rather than being entirely compact bone?
If entirely compact, bones would be too heavy and too brittle
Bones
What components does the extracellular matrix contain and what function does it have?
Contains collagen
A structural protein that provides flexibility and resistance to breaking
Collagen fibers are deposited by cells and form a framework that gives the bone strength
Mineral component, mainly calcium phosphate
Makes bones rigid and hard
Acts as a reservoir for Ca2+ » so if you become calcium deficient, Ca2+ can leak out of bones
Bones
2 types of bone cells
Osteoblasts
Ostcleoblasts
Bones
Osteoblasts
Form bone
Secret collagen
Organise the mineralisation process to give bones hardness
Bones
Osteoclasts
Break down (resorb) bone to remodel it onto an optimal shape
Maintain bone health
Bones
Why is the balance between osteoblasts and osteoclasts important?
The balance maintains normal bone structure and function
Allowing the bone to respond to growth, repair, and mechanical loading.
Bones
How does bone remodelling change during life?
During growth (e.g., in children), osteoblast activity is higher to build bone
The balance between osteoblasts and osteoclasts shifts with aging, hormonal changes, reduced activity, or conditions like osteoporosis.
Bones
What factors can disrupt the balance between osteoblasts and osteoclasts?
Osteoporosis
Reduced mechanical loading
Hormonal changes
Corticosteroid drugs
Bones
What cells does the bone marrow contain
Stem cells
Hematopoietic stem cells » make leukocytes, erythrocytes and thrombocytes
Mesenchymal stem cells » multipotent
Adipose tissue
Bones
What allows bones to flex at the joints?
The ends of bones are coated with articular cartilage
These are smooth and lack the mineral component
Which allows bones to bend
Skeletal Muscle
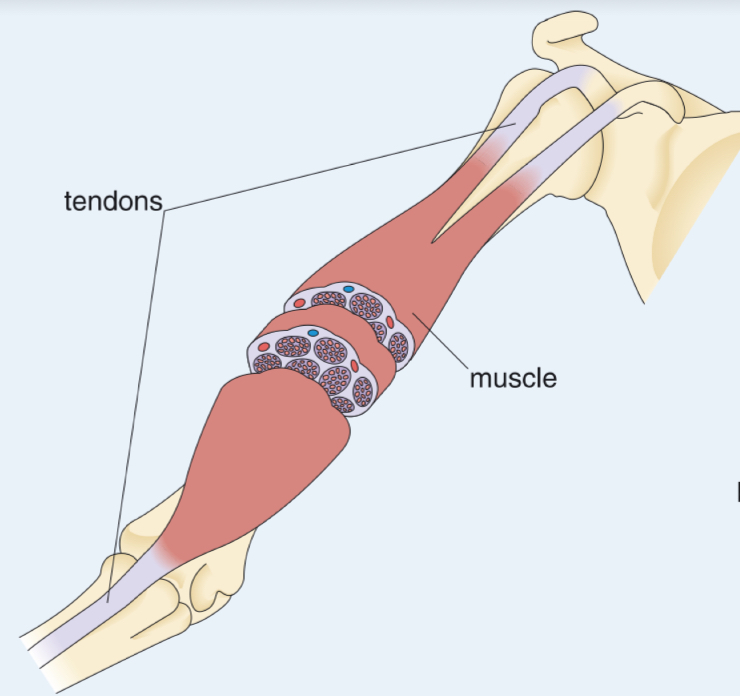
Where are skeletal muscles located?
Skeletal muscles are attached to bones via tendons
Skeletal Muscle
Structure
Skeletal muscles consist of bundles of myofibres
Myofibres are long, thin, multinucleated cells
They are packed together in a highly aligned manner with a supporting extracellular matrix
Contain lots of mitochondria
Myofibres contain myofibrils

Skeletal Muscle
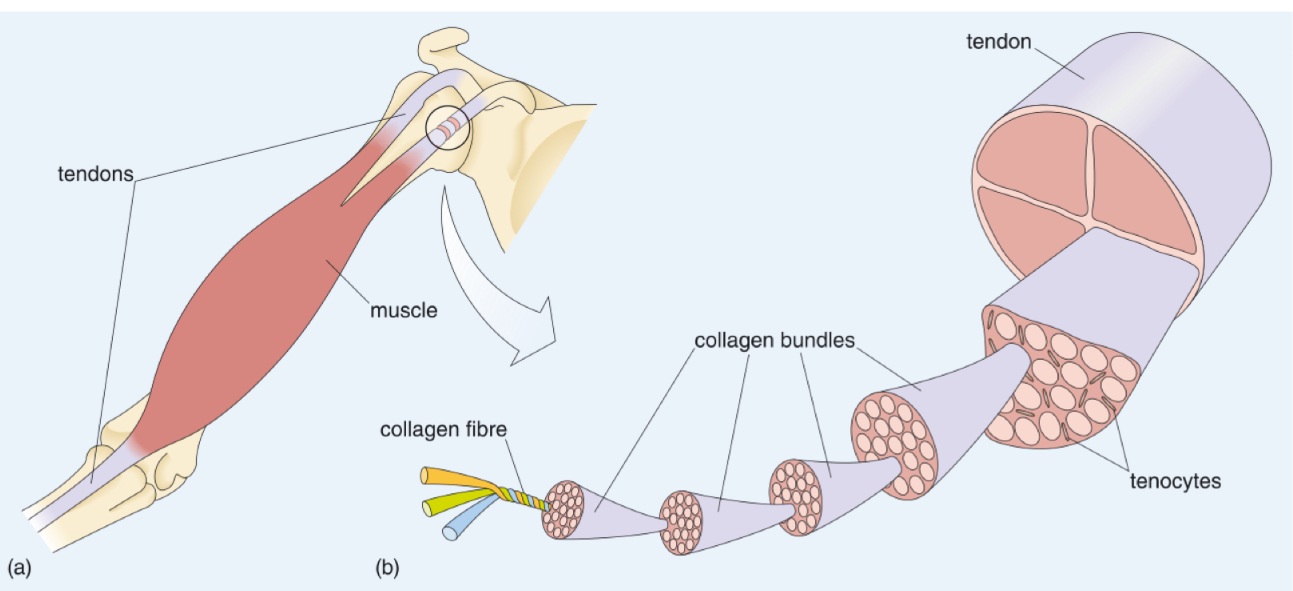
What surrounds the myofibres?
A network of collagen surrounds individual myofibres
The collagen fibres gather together at the ends of the muscle to form tendons that join muscle to bone
Skeletal Muscle
Characteristics of tendons
Mainly formed from collagen (plus some elastic fibres)
High tensile strength
» Made of densely packed collagen fibers
» Which makes them resistant to stretching
Variety of shapes and sizes depending on function and location
» Short and thick (e.g., Achilles tendon in the ankle)
» Long and thin (e.g., tendons in the fingers)
Skeletal Muscle
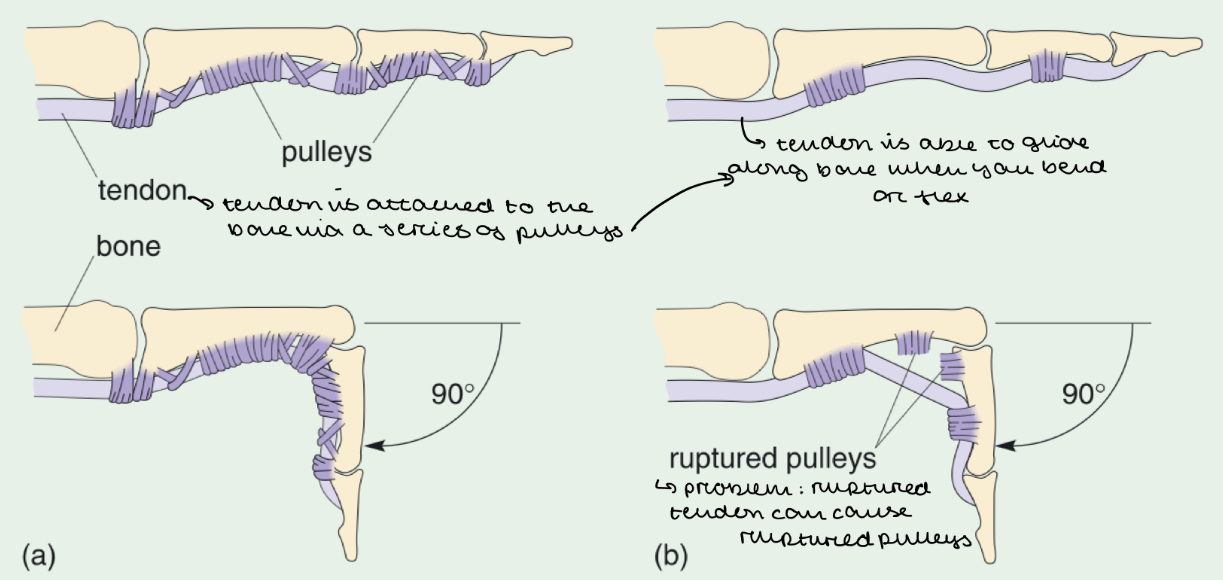
Explain how tendons facilitate movement of bone
Tendons operate using a pulley system
Tendons are attached to bones via a series of pulleys
When you flex or bend your fingers, the tendons slide along the bone
The pulleys act like loops through which the tendons pass, keeping them aligned with the bone
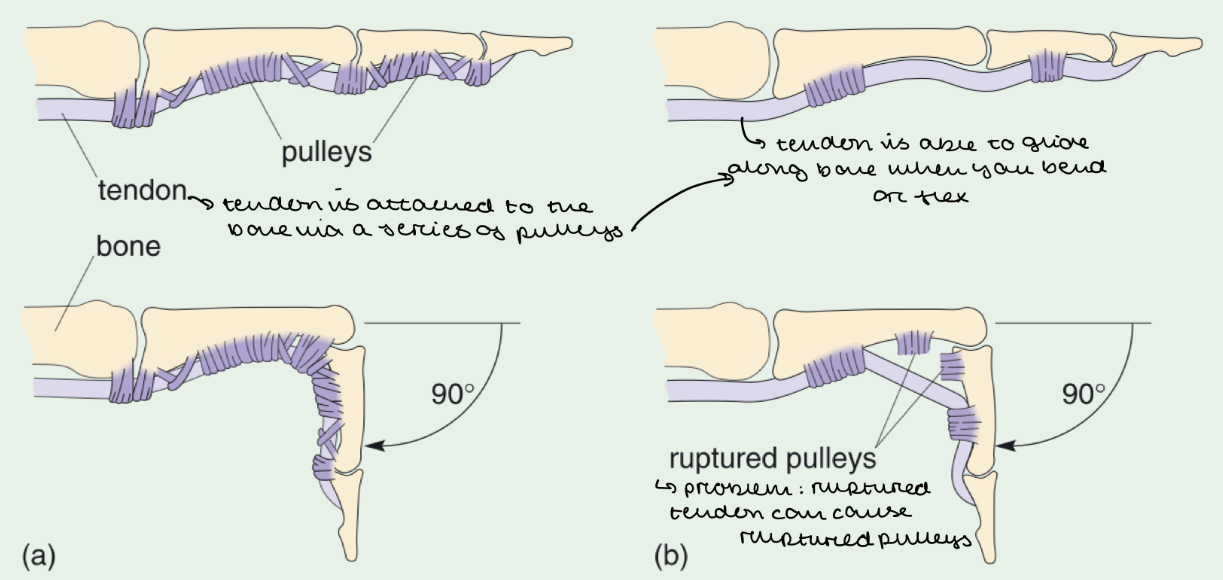
Skeletal Muscle
What happens if pulleys rupture?
The tendons lose its guiding structure
So they are unable to slide along the bone
Skeletal Muscle
What cells do tendons contain?
Tenocyte cells
Responsible for maintaining tendon structure
Sparsely populated
Limited blood supply
Skeletal Muscle
Why are tendons slow to heal?
Tenocyte cells have limited blood supply
Skeletal Muscle
Dinference between tendons and ligaments
Tendons: connect muscle to bone
Ligaments: connect bone to bone
Musculoskeletal System
How do muscles work?
Muscles can only contract and relax
This means muscles always work in antagonistic pairs where one muscle contracts (flexor) and the other muscle relaxes (extensor)
Musculoskeletal System
2 main types of muscles
Flexors » bend the joint e.g. biceps in the arm
Extensors » straighten the joint e.g. triceps in the arm
Musculoskeletal System
Explain how the arm bends and straightens
Flexion (bending): biceps contract, triceps relax
Extension (straightening): triceps contract, biceps relax
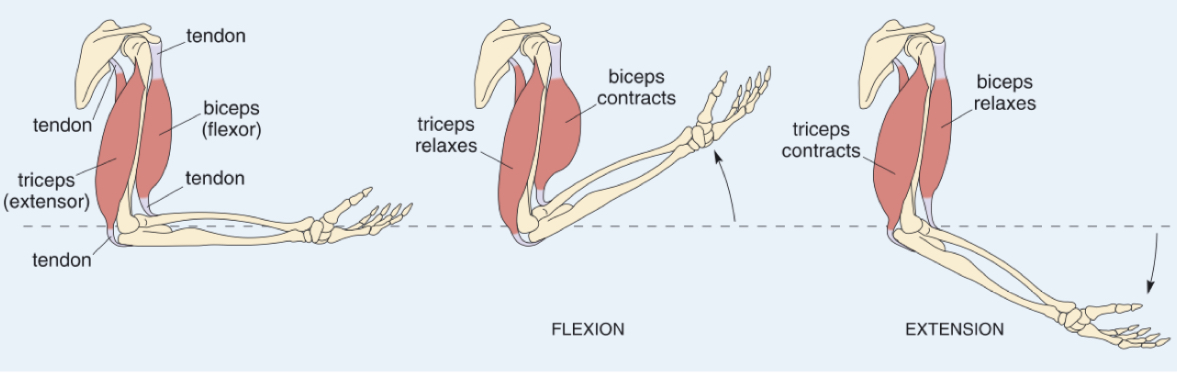
Musculoskeletal System
Why are there different classes of levers in the body?
Depending on the position of the load, effort and fulcrum
Musculoskeletal System
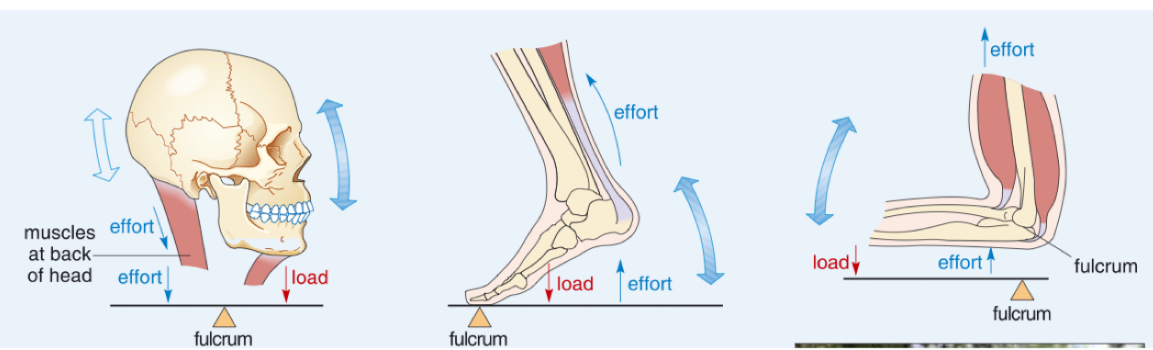
Give examples of the different classes of levers in the body
Class 1 Lever:
Head / Neck
Fulcrum in the middle, effort and load on either side (like a seesaw)
Class 2 Lever:
Foot / Ankle
Load is between the effort and the fulcrum
Class 3 Lever:
Arm / Elbow
Effort is between load and fulcrum
Skin
2 parts of the skin
Epidermis » contains flat, thin, dead keratinocytes which are full of keratin
Dermis » contains collagen, elastic fibres with fibroblasts, capillaries, nerve endings, sweat glands, hair
Blood Vessels (Capillaries)
Structure
Formed from flat endothelial cells
Blood Vessels (Capillaries)
Function
Network throughout tissues, providing nutrients and oxygen which diffuse out of blood and into tissues
Blood Vessels (Capillaries)
How much tissue fluid drains into the lymphatic system
10%
What is the difference between tissue repair and tissue regeneration?
Repair: problem is fixed but the tissue cannot go back to its original state
Regeneration: tissue is returned to its original state
How does the skin repair itself e.g. from a cut or wound?
Blood from damaged vessels fills the wound and clots to stop bleeding.
The clot is comprised mesh of fibrin fibers (formed from circulating fibrinogen) which creates a temporary barrier.
White blood cells migrate to the wound site to prevent infection, causing inflammation
Fibrin scaffold gets infiltrated with blood vessels and fibroblasts which produce new extracellular matrix proteins
Healed skin may have a scarred appearance due to the excess deposition of collagen (fibrosis).
How does the bone repair itself?
Blood from broken vessels forms a clot, creating a fibrin scaffold.
This scaffold supports the migration of stem cells and osteoblasts to form new bone
The fibrin scaffold is gradually replaced with collagen, which acts as a framework for new bone growth.
Gradually, the newly formed bone extracellular matrix (ECM) completely replaces the fibrin scaffold
The ECM becomes mineralized, giving it strength.
Over time, the new bone undergoes continuous natural remodeling, strengthening it.
The healed bone can look and function like undamaged bone.
Difference between skin repair and bone repair
Skin repair often leaves a scar due to fibrosis.
Bone repair can fully restore structure and function due to continuous remodeling.
Explain how muscles repair themselves
When muscle tissue is damaged, a fibrin scaffold forms at the injury site.
The fibrin scaffold is quickly populated by capillaries (to supply oxygen and nutrients), and fibroblasts (cells that help form connective tissue).
Stem cells present in the muscle tissue multiply and differentiate into myoblasts (muscle precursor cells).
These new myoblasts can either:
Fuse with the damaged myofibres to repair them.
Merge with other myoblasts to form new myofibres, helping to rebuild the muscle.
Once the new or repaired myofibres are formed, they integrate into the existing muscle structure.
The temporary fibrin scaffold is then replaced by collagen and other extracellular matrix (ECM) molecules
Explain how tendons repair themselves
A fibrin scaffold forms at the site of tendon injury. This scaffold supports the growth of tiny capillaries and fibroblasts, which are involved in repairing connective tissue.
Over time, the fibrin scaffold is replaced by collagen, the primary structural protein in tendons
The collagen gradually is remodelled to become strong and aligned
In some cases, fibrosis (excessive scar tissue formation) can occur. This can lead to the development of adhesions, (e.g. between tendon, pulley and bone) which can limit movement and function.
Why is tendon repair a slow process?
Replacing fibrin with collagen takes longer than in muscles because tendons have a poor blood supply, slowing the delivery of necessary nutrients and removal of waste.
How do nerves become damaged?
If the injury cuts the axon, then the distal part of the axon (on the far side) degenerates
This means the person loses any motor/sensory function associated with that nerve
How do nerves repair themselves?
Debris of degenerated axon are cleared away by macrophages (which cause inflammation)and Schwann cells
Schwann cells form a pathway for axon regeneration
Axons begin to regrow towards their target tissues
What is the creation of new blood vessels called?
Angiogenesis
When is angiogenesis important?
Embryonic develop,ent
Wound healing
Female reproductive cycle
In what conditions does excessive angiogenesis occur?
Cancer
Age-related macular degeneration
Psoriasis
Endometriosis
In what conditions is there insufficient angiogenesis?
Chronic wounds
Ischaemic heart diseases
What is the predominant ECM protein in most tissues?
Collagen

What is seen in this picture?
Collagen » looks stripy to the eye
What is tropocollagen
Made of 3 polypeptide alpha chains
Each chain has a regularly repeating amino acid motif Gly-X-Y
X and Y can be any amino acid but mostly proline and hydroxyproline